Professional Documents
Culture Documents
Subarachnoid Hemorrhage: Clinical Practice
Subarachnoid Hemorrhage: Clinical Practice
Uploaded by
Nancy Romero QuirosOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Subarachnoid Hemorrhage: Clinical Practice
Subarachnoid Hemorrhage: Clinical Practice
Uploaded by
Nancy Romero QuirosCopyright:
Available Formats
The n e w e ng l a n d j o u r na l of m e dic i n e
Clinical Practice
Caren G. Solomon, M.D., M.P.H., Editor
Subarachnoid Hemorrhage
Michael T. Lawton, M.D., and G. Edward Vates, M.D., Ph.D.
This Journal feature begins with a case vignette highlighting a common clinical problem. Evidence
supporting various strategies is then presented, followed by a review of formal guidelines, when they exist.
The article ends with the authors’ clinical recommendations.
A 17-year-old boy had a sudden headache and briefly lost consciousness while at soccer From the Department of Neurosurgery,
practice. On arrival at the emergency department, he appeared drowsy and reported Barrow Neurological Institute, St. Joseph’s
Hospital and Medical Center, Phoenix, AZ
having the worst headache he had ever had. His blood pressure was 186/92 mm Hg. (M.T.L.); and the Department of Neuro-
The neurologic examination was normal. Computed tomography (CT) of the head surgery, University of Rochester Medical
without contrast enhancement showed diffuse subarachnoid hemorrhage and en- Center, Rochester, NY (G.E.V.) Address
reprint requests to Dr. Lawton at the De-
largement of the temporal horns of the lateral ventricles. How should this patient be partment of Neurosurgery, Barrow Neu-
further evaluated and treated? rological Institute, St. Joseph’s Hospital
and Medical Center, 350 W. Thomas Rd.,
Phoenix, AZ 85013, or at m ichael.lawton@
The Cl inic a l Probl em barrowbrainandspine.com, or to Dr. Vates
S
at the University of Rochester Medical
ubarachnoid hemorrhage without a preceding trauma is caused Center, Department of Neurosurgery,
601 Elmwood Ave., Box 670, Rochester,
by the rupture of an intracranial aneurysm in 80% of cases; other causes in- NY 14642, or at edward_vates@ urmc
clude vascular malformations and vasculitis. Subarachnoid hemorrhage ac- .rochester.edu.
counts for 5 to 10% of all strokes in the United States,1 and affected patients tend N Engl J Med 2017;377:257-66.
to be younger than those affected by other subtypes of stroke, which results in a DOI: 10.1056/NEJMcp1605827
greater loss of productive life.2 Among the patients with aneurysmal subarachnoid Copyright © 2017 Massachusetts Medical Society.
hemorrhage who survive, half suffer long-term neuropsychological effects and
decreased quality of life.3 Early identification and treatment of the aneurysm can
prevent aneurysm rerupture and can address sequelae from the initial rupture.
Intervention may be appropriate in cases of subarachnoid hemorrhage that are not
An audio version
caused by aneurysms (e.g., cases involving arteriovenous malformation), but up to of this article is
10% of cases of nonaneurysmal subarachnoid hemorrhage involve no vascular ab- available at
normality, and surgical or endovascular treatment is not considered to be necessary.4 NEJM.org
Intracranial Aneurysms
Intracranial aneurysms occur in 1 to 2% of the population.5 Aneurysms typically
form at branch points along intracranial arteries (Fig. 1 and the interactive graph-
ic); hemodynamic stress on the wall between the two exiting branches weakens
that region.6 The risk of intracranial aneurysms is increased among persons with
a family history (defined as at least one first-degree relative who has had an
intracranial aneurysm, with a greater risk if two or more first-degree relatives
have had such an event), among persons with certain connective-tissue disorders
(e.g., the Ehlers–Danlos syndrome), and among persons with polycystic kidney
disease.7,8 Factors associated with an increased risk of aneurysm rupture include
black race, Hispanic ethnic group, hypertension, current smoking, alcohol abuse,
use of sympathomimetic drugs, and an aneurysm larger than 7 mm.7,9
n engl j med 377;3 nejm.org July 20, 2017 257
The New England Journal of Medicine
Downloaded from nejm.org on July 19, 2017. For personal use only. No other uses without permission.
Copyright © 2017 Massachusetts Medical Society. All rights reserved.
The n e w e ng l a n d j o u r na l of m e dic i n e
Key Clinical Points
Subarachnoid Hemorrhage
• Subarachnoid hemorrhage from a ruptured intracranial aneurysm is a life-threatening stroke that affects
younger patients than those affected by other forms of stroke.
• Aneurysmal subarachnoid hemorrhage is diagnosed by confirmation of subarachnoid hemorrhage on
a computed tomographic (CT) scan of the head and by confirmation of an aneurysmal source by CT
angiography of the head, catheter angiography of the head, or both.
• The prevention of aneurysm rerupture is the first goal of treatment. Randomized, controlled trials suggest
that aneurysms that are judged to be treatable by either open surgery or endovascular intervention are
better treated by the latter; however, open surgery is preferred in certain cases.
• Vasospasm and delayed cerebral ischemia contribute to the occurrence of complications and death
after successful occlusion of an aneurysm and remain the major challenge of aneurysmal subarachnoid
hemorrhage.
• Decisions about treatment for aneurysms and about the management of aneurysmal subarachnoid
hemorrhage sequelae are best made at high-volume centers by experienced surgeons, interventionalists,
and neurologic intensive care experts.
The rate of detection of unruptured intracra- When an aneurysm ruptures, it is an intracra-
nial aneurysms has increased as the use of CT nial catastrophe. Blood pushes into the subarach-
and magnetic resonance imaging (MRI) has be- noid space at arterial pressure until the intracra-
come more common.10 The treatment of unrup- nial pressure equalizes across the rupture site and
tured intracranial aneurysms remains controver- stops the bleeding, with thrombus formation at
sial and is not addressed here. the bleeding site. The reported case fatality rate
The reported incidence of aneurysmal sub- is 25 to 50%,15 owing to consequences of either
arachnoid hemorrhage varies widely across the the original bleeding or rerupture; this estimate
world, from 2.0 cases per 100,000 persons in does not fully account for patients who die be-
China to 22.5 cases per 100,000 persons in Fin- fore receiving medical attention.16
land11; variation may in part reflect differences
in the rates of detection across countries.12,13 The Signs and Symptoms
2003 Nationwide Inpatient Sample estimated 14.5 The hallmark presenting symptom of aneurysmal
An interactive hospitalizations for aneurysmal subarachnoid subarachnoid hemorrhage is “the worst headache
graphic showing hemorrhage per 100,000 U.S. adults per year.14 of my life.”17 The onset of the headache is sudden,
management of Aneurysmal subarachnoid hemorrhage is more and the headache is severe and reaches maximal
subarachnoid
hemorrhage is
common among women than among men, and intensity in seconds (known as a thunderclap
available at the incidence increases with age to a peak among headache). In 10 to 40% of patients, this head-
NEJM.org persons in their 50s.14 ache is preceded by a warning leak or “sentinel”
Figure 1 (facing page). Repair of Aneurysms That Have Caused Subarachnoid Hemorrhage.
The anatomy of the subarachnoid space and the circle of Willis is shown in Panel A. A major artery (the internal carotid artery) enters the
skull from below and then follows a course through the subarachnoid space, giving off perforating branches that supply the parenchyma.
High pulsatile pressure at branching points of the proximal artery (arrow, Panel B) soon after the arterial wall sheds much of its support-
ing adventitia can promote the formation of saccular aneurysms in susceptible persons. In such cases, an aneurysm forms at the branch
point of an artery, where the arterial pulsation stress is maximal. Most lesions remain silent until rupture occurs, at which time blood is rap-
idly released into the subarachnoid space, leading to early effects such as intracranial pressure elevation, parenchymal irritation, edema,
and hydrocephalus and delayed effects, such as vasospasm and delayed cerebral ischemia. Open surgical repair of such an aneurysm
(Panel C) involves exposing the aneurysm and the adjacent normal arteries so that the surgeon can apply a titanium clip on the neck of
the aneurysm, which effectively excludes it from arterial circulation. Removal of portions of the skull base provides improved access and
operative exposure for the surgeon without the need for substantial brain retraction. The aneurysm is then collapsed and the field in-
spected to make sure that no branches are compromised by the clip placement. The inner walls of the aneurysm base are approximated
by the clip, which generally provides a lifelong cure of the lesion. Endovascular repair of such an aneurysm (Panel D) involves the naviga-
tion of an intraarterial catheter through the circulation under fluoroscopic guidance until the catheter tip is in the lumen of the aneurysm.
With the use of the catheter, platinum coils are delivered and packed into the lumen of the aneurysm, which slows or prevents blood flow
into the aneurysm and leads to thrombus formation, effectively blocking arterial blood from entering the aneurysm. Angiographic exami-
nation of the result confirms flow through the normal arterial branches. Not all aneurysms can be treated with endovascular repair (some
will have to be treated with surgery), but endovascular repair can treat many aneurysms without a visible scar.
258 n engl j med 377;3 nejm.org July 20, 2017
The New England Journal of Medicine
Downloaded from nejm.org on July 19, 2017. For personal use only. No other uses without permission.
Copyright © 2017 Massachusetts Medical Society. All rights reserved.
Clinical Pr actice
A C Craniotomy
flap Ruptured
Craniotomy aneurysm
LEFT
A N TER IO R
Aneurysm
V IEW
Left posterior
C I R C L E OF Left anterior
WILLIS cerebral artery
cerebral
artery
Left posterior Brain
communicating
Left anterior artery Left internal
cerebral artery Reflected carotid
Basilar artery skin flap artery Left middle
cerebral
Left middle artery
Left internal cerebral artery
carotid artery
Deflated
aneurysm
B
Vessel Vessel Weakened intracranial Temporary
wall lumen arterial wall clip
Permanent
Left anterior clip
cerebral artery HE M ODY NA M I C
STRESS
Branching point between
the left internal carotid Temporary clips are placed on
artery, left anterior adjacent arteries to soften the
cerebral artery, and B L OOD aneurysm for permanent
F L OW A permanent titanium clip is clipping
left middle cerebral placed across the neck of the
artery aneurysm to preserve blood flow
in adjacent arteries
Left middle
Left internal cerebral
carotid artery artery D
Coils are deposited into the
aneurysm sac through the
microcatheter
Brain
Ruptured
aneurysm Coil Aneurysm
SUB A R A C H NOI D
SP A C E Microcatheter
I NT R A A NE UR Y S M A L
B L OOD F L OW
A microcatheter is
introduced into the Coil-filled
femoral artery and aneurysm
advanced to the
location of the
aneurysm
Coils fill the aneurysm,
Femoral arresting intraaneurysmal
B LO O D artery blood flow and inducing
FLO W
thrombus formation
n engl j med 377;3 nejm.org July 20, 2017 259
The New England Journal of Medicine
Downloaded from nejm.org on July 19, 2017. For personal use only. No other uses without permission.
Copyright © 2017 Massachusetts Medical Society. All rights reserved.
The n e w e ng l a n d j o u r na l of m e dic i n e
headache,18 which typically occurs within 2 to 8 the major determinant of grade. Aneurysm rup-
weeks before overt subarachnoid hemorrhage.9,10 ture produces immediate widespread brain dys-
Although hemorrhage can occur during physical function and “late” events days after the rupture,
or psychological stress, it occurs more com- both of which affect the outcome through mech-
monly during activities of daily living.19 Associated anisms that are only partially understood.25,26
symptoms or signs include nausea, vomiting, or
both; photophobia; neck stiffness; focal neuro- Imaging
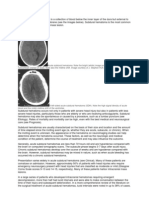
logic deficits; and a brief loss of consciousness.20 CT of the head without contrast enhancement is
More severely affected patients present with altered the first essential step in the diagnosis of sub-
mental status, from mild lethargy to profound arachnoid hemorrhage (Fig. 2).20,27 In the first
coma; the degree of encephalopathy at presenta- 3 days after the onset of symptoms, the sensitiv-
tion is the major determinant of the prognosis. ity of the CT scan is close to 100%, but it subse-
Aneurysmal subarachnoid hemorrhage ac- quently declines to 50% by 5 to 7 days after the
counts for only 1% of all headaches evaluated in onset of symptoms.28,29 CT of the head may also
the emergency department.21 Consequently, a sen- show a space-occupying hematoma or acute hy-
tinel headache may be dismissed as a migraine drocephalus — consequences of aneurysm rup-
headache or other headache without further ture for which patients are considered to require
evaluation; the likelihood of death or disability immediate surgical attention. If the CT of the
is four times as high among patients in whom a head is negative but clinical suspicion is high,
sentinel headache is misdiagnosed as it is among additional tests are indicated.
patients in whom a sentinel headache is cor- Lumbar puncture has been used to detect
rectly diagnosed.22 Therefore, a high index of blood or xanthochromia in cerebrospinal fluid,30
suspicion for aneurysmal subarachnoid hemor- but lumbar puncture performed after a negative
rhage from the patient’s history is warranted CT of the head is now of debated value owing to
and potentially lifesaving. the low prevalence of subarachnoid hemorrhage
and the difficulty in distinguishing between
subarachnoid hemorrhage and trauma related to
S t r ategie s a nd E v idence
the lumbar puncture.29 MRI, with fluid-attenuat-
Evaluation ed inversion recovery, proton density, and gradi-
Initial Stabilization ent-echo sequences, is exquisitely sensitive to
If a patient survives the initial rupture of the heme in the cerebrospinal fluid.31 CT angiogra-
aneurysm and reaches medical attention, manage- phy, which is now commonly performed at the
ment of the aneurysmal subarachnoid hemor- time of the initial CT, can show that an aneu-
rhage is directed at reversing or stabilizing acute rysm is present and can provide the essential
life-threatening sequelae, particularly in the case information in the case of patients who present
of comatose patients. Establishing a secure air- in extremis with a large intraparenchymal clot
way, normalizing cardiovascular function, and that is thought to require immediate surgical
treating seizures are common first steps before evacuation.32 CT angiography can now reliably
diagnostic studies are pursued. detect aneurysms as small as 2 mm, but tiny
blister aneurysms or aneurysms filled with
Grading Systems Used for Patients thrombi may be missed.
with Subarachnoid Hemorrhage Digital subtraction angiography remains the
A variety of grading systems correlate the clinical standard for diagnosing an aneurysm and for
status of the patient at the time of presentation defining relevant anatomy for treatment
with the long-term neurologic outcome. The two (Fig. 3).32 The combination of three-dimensional
most commonly used grading systems are the angiography reconstructions with two-dimen-
Hunt–Hess classification and the World Federation sional angiography in digital subtraction angi-
of Neurosurgical Societies classification (Table ography is more sensitive for detecting aneu-
S1 in the Supplementary Appendix, available with rysms and provides more detailed anatomical
the full text of this article at NEJM.org).23,24 In data than digital subtraction angiography alone
both systems, the severity of encephalopathy is and also helps in planning treatment.
260 n engl j med 377;3 nejm.org July 20, 2017
The New England Journal of Medicine
Downloaded from nejm.org on July 19, 2017. For personal use only. No other uses without permission.
Copyright © 2017 Massachusetts Medical Society. All rights reserved.
Clinical Pr actice
Medical Interventions to Reduce the Risk
of Rerupture
Patients in whom aneurysm rerupture occurs
have a much higher risk of death and neurologic
injury than patients who have a single aneurysm Blood filling the
subarachnoid cisterns
rupture.33 The risk of rerupture is 4 to 14% in the and extending into the sylvian
first 24 hours after aneurysmal subarachnoid fissures bilaterally
hemorrhage,34,35 but the risk remains elevated for
30 days after the initial rupture if the aneurysm
is not treated.
Hypertension can increase the risk of rerup-
ture, but the goals of treatment remain poorly Enlarged temporal horns
defined, with few trial data available to support
specific blood-pressure targets.36 Antifibrinolytic
therapy may stabilize the initial thrombus at the Trace of intraventricular blood
bleeding site. In a randomized, controlled trial,
the incidence of aneurysm rerupture was 2%
among the patients who received antifibrinolytic
therapy as compared with 11% among patients
who did not receive such therapy.37 Although
antifibrinolytic therapy may have benefit when
aneurysm treatment is delayed (e.g., when a pa- Figure 2. CT Scan of the Head Showing Evidence
of Subarachnoid Hemorrhage.
tient is transferred to another facility), its use did
Subarachnoid hemorrhage, as seen on axial CT, varies
not improve overall outcomes and is associated
from none detected, to diffuse deposition of a thin layer
with an increased risk of deep venous thrombo- of blood (<1 mm thick) in the cerebrospinal fluid–filled
sis and delayed cerebral ischemia.38 Seizures oc- cisterns at the base of the brain, to a thick blood clot
cur in up to 20% of patients, especially in pa- (≥1 mm thick) in the cerebrospinal fluid–filled cisterns
tients with intraparenchymal bleeding, and can around the circle of Willis, as seen in this patient from
the vignette. Subarachnoid hemorrhage can extend be-
cause hemodynamic instability that precipitates
yond the basal cisterns into the sylvian fissures or into
aneurysm rerupture39; however, data are lacking the ventricles or brain parenchyma. The distribution of
from randomized trials to support routine ad- blood offers clues to the location of the aneurysm. The
ministration of antiseizure medication, and rou- greater amount of blood in the left basal cisterns than
tine prophylaxis is not recommended. in the right points to a likely location of the aneurysm
on the left side of the cerebral circulation. The enlarged
temporal horns are evidence of hydrocephalus; in most
Treatment of Ruptured Cerebral Aneurysms patients (and especially in younger patients) the tem-
Clinical experience and randomized trials have poral horns should not be visible.
shown that treatment for ruptured aneurysms is
safe and eliminates the immediate risk of aneu-
rysm rerupture.40-43 Treatment can be achieved by chanically close the sac at its neck while preserv-
means of open surgical clipping or endovascular ing blood flow through the adjacent normal ar-
aneurysm obliteration; both treatments should teries.
be provided by specialized, experienced practi- Endovascular treatment of a ruptured aneu-
tioners at high-volume centers.44 rysm involves navigating a catheter under fluo-
Surgical clipping of a ruptured aneurysm re- roscopic guidance from an entry point in the
quires opening the skull (craniotomy). With the arterial circulation (typically the femoral artery
use of the operating microscope, the subarach- in the groin) up to the parent artery of the aneu-
noid spaces around the cerebral arteries are rysm (Figs. 1 and 3). A microcatheter is then
opened at the base of the skull to mobilize deli- advanced into the aneurysm sac and metal coils
cate brain tissue without injury (Figs. 1 and 3). are deposited into the aneurysm lumen through
Once the aneurysm is exposed, a titanium clip is the microcatheter, a process that arrests intra-
placed across the neck of the aneurysm to me- aneurysmal blood flow and induces thrombus
n engl j med 377;3 nejm.org July 20, 2017 261
The New England Journal of Medicine
Downloaded from nejm.org on July 19, 2017. For personal use only. No other uses without permission.
Copyright © 2017 Massachusetts Medical Society. All rights reserved.
The n e w e ng l a n d j o u r na l of m e dic i n e
A B
Aneurysm
ACA
MCA
Aneurysm
ACA
MCA
ICA
C D
Aneurysm
MCA
ACA ACA MCA
Clip
ICA
ICA
E
Coil mass
occluding the
aneurysm
Figure 3. Angiogram Showing Internal Carotid Artery Aneurysms before and after Treatment.
An angiogram obtained in the patient in the vignette shows an aneurysm in the left internal carotid artery (ICA).
The aneurysm originates at the point where the ICA bifurcates into the arterial cerebral artery (ACA) and the middle
cerebral artery (MCA) (Panel A). At the time of surgery, the aneurysm was exposed and was shown to be multilobu-
lated, very thin-walled, and with friable daughter lobules (Panel B; the inset shows the location of the aneurysm in
the patient’s brain). CT angiography shows the placement of a surgical clip and complete obliteration of the aneurysm
(Panel C). An angiogram obtained in a different patient shows a similarly located ICA aneurysm (Panel D) and the
results obtained with endovascular treatment (Panel E).
formation, thereby occluding the aneurysm and national Subarachnoid Aneurysm Trial (ISAT) and
eliminating the immediate risk of rerupture. the Barrow Ruptured Aneurysm Trial (BRAT).40-43
Two randomized trials have compared endo- Despite a significantly higher rate of obliteration
vascular treatment with open-surgical treatment and greater durability with open-surgical treat-
for ruptured intracranial aneurysms: the Inter- ment than with endovascular treatment, both tri-
262 n engl j med 377;3 nejm.org July 20, 2017
The New England Journal of Medicine
Downloaded from nejm.org on July 19, 2017. For personal use only. No other uses without permission.
Copyright © 2017 Massachusetts Medical Society. All rights reserved.
Clinical Pr actice
als showed better functional outcomes at 1 year Treatment of Complications Arising
with endovascular treatment than with open- from Subarachnoid Hemorrhage
surgical treatment (Table S2 in the Supplemen- and Aneurysm Treatment
tary Appendix). Vasospasm and Delayed Cerebral Ischemia
In ISAT, a multicenter trial involving patients Narrowing of angiographically visible cerebral
whose aneurysms were considered to be suitable arteries after aneurysmal subarachnoid hemor-
for either open-surgical treatment or endovascu- rhage (vasospasm) occurs in 70% of patients; the
lar treatment, rates of dependency or death at the process generally starts 3 to 4 days after aneu-
1-year follow-up were 23.5% in the endovascular- rysm rupture, peaks at 7 to 10 days, and resolves
coil group and 30.9% in the open-surgery group by 14 to 21 days.46 Delayed cerebral ischemia is
(absolute difference, 7.4 percentage points; 95% a clinical syndrome of focal neurologic deficits
confidence interval, 3.6 to 11.2). In addition, the that develops in one third of patients, typically
endovascular-coil group had a lower mortality 4 to 14 days after aneurysm rupture,25 and is a
rate and a lower risk of seizures through the major cause of death and disability after sub-
7-year follow-up than did the open-surgery group; arachnoid hemorrhage has occurred.47
rebleeding, although infrequent, was more com- Despite a general belief that vasospasm causes
mon in the endovascular-coil group than in the delayed cerebral ischemia, recent evidence sug-
open-surgery group. BRAT, a single-center trial, gests that a variety of vascular and neural
showed a similar benefit of endovascular treat- changes that take place after subarachnoid hem-
ment as compared with open-surgical treatment orrhage may contribute to its pathogenesis.48 De-
with respect to functional outcomes at 1 year, layed cerebral ischemia develops in fewer than
although the differences between the two groups one half of patients with angiographic vaso-
were no longer significant at year 3 or year 6. spasm, and ischemia does not occur consistently
Unlike ISAT, BRAT did not include as an entry in the territory supplied by the vessel undergoing
criterion the need for the anatomy of the aneu- spasm. The calcium-channel blocker nimodipine,
rysm to be suitable for either procedure, and the only drug known to reduce the risk of de-
more than a third of the patients who were ran- layed cerebral ischemia and improve neurologic
domly assigned to receive endovascular treatment outcome after subarachnoid hemorrhage (dis-
crossed over to the open-surgery group, the ma- cussed further below), does not alter the inci-
jority owing to the anatomy of the aneurysm or dence or severity of vasospasm. In clinical trials
to the surgeon’s preference for open-surgical of a drug that significantly reduced the risk of
treatment over endovascular treatment. angiographic vasospasm, no measurable effect
The results of ISAT, combined with the fact was observed on the development of delayed
that patients tend to prefer a minimally invasive cerebral ischemia or on clinical outcomes.25,26
approach to treatment, have resulted in a dramatic Consequently, possible sequelae of subarachnoid
shift toward endovascular treatment of ruptured hemorrhage other than vasospasm are being
aneurysms. However, open-surgical treatment may explored as mediators of poor outcome after
be preferred for patients who have increased in- aneurysm rupture and as potential targets for
tracranial pressure or focal neurologic deficits therapy.25,48,49
caused by intracerebral hematoma, for patients Currently, it is recommended that nimodipine
whose aneurysms are difficult to visualize angio- be administered orally to all patients from the
graphically or for whom revascularization with a time of presentation to 21 days after the occur-
bypass is deemed to be necessary, and for patients rence of subarachnoid hemorrhage. A Cochrane
younger than 40 years of age who have anterior review of randomized trials indicated that nimo
circulation aneurysms and good neurologic status, dipine reduced the risk of poor outcomes in pa-
given the greater durability and the lower risk of tients with subarachnoid hemorrhage by one
aneurysm rebleeding with open-surgical treatment third.50 The maintenance of normal circulating
than with endovascular treatment.45 Consequent- blood volume and normal hemoglobin level is
ly, patients should be treated at high-volume associated with a reduced risk of delayed cere-
cerebrovascular centers where surgeons who are bral ischemia, but prophylactic hypervolemia and
experienced and skilled in both open-surgical balloon angioplasty to treat angiographic vaso-
and endovascular procedures are present. spasm (in the absence of clinical or radiograph-
n engl j med 377;3 nejm.org July 20, 2017 263
The New England Journal of Medicine
Downloaded from nejm.org on July 19, 2017. For personal use only. No other uses without permission.
Copyright © 2017 Massachusetts Medical Society. All rights reserved.
The n e w e ng l a n d j o u r na l of m e dic i n e
ic evidence of delayed cerebral ischemia) is dis- Medical Complications
couraged.51,52 Patients who have had aneurysm rupture are at
The clinical examination may not detect de- risk for multiple medical complications that are
layed cerebral ischemia in an obtunded or coma- common with critical illness, and they should be
tose patient. Transcranial Doppler ultrasonogra- treated in an intensive care unit, preferably one
phy is widely used as a noninvasive test to detect that specializes in neurocritical care.53 A detailed
vasospasm after subarachnoid hemorrhage, but discussion of general medical management is
its usefulness remains debated. Perfusion CT can beyond the scope of this article, but the goals
be used to identify regions of possible brain include euvolemia, normothermia, avoidance of
ischemia in patients who have a new neurologic hypoglycemia or marked hyperglycemia, electro-
deficit. If clinically significant delayed cerebral lyte balance, and adequate ventilation (for coma-
ischemia, with or without vasospasm, is suspect- tose patients) that avoids exacerbating elevated
ed, induced hypervolemia and hypertension intracranial pressure. Because deep venous throm-
(double “H” therapy with intravenous adminis- bosis is relatively common after subarachnoid
tration of fluid and alpha-adrenergic agents) is hemorrhage, especially among immobilized pa-
recommended to improve cerebral perfusion. If tients, routine prophylaxis is recommended, with
delayed cerebral ischemia occurs in the territory intermittent pneumatic compression at all times
of a major cerebral artery in spasm, cerebral an- and with unfractionated heparin starting 24 hours
gioplasty, selective intraarterial vasodilator ther- after the ruptured aneurysm has been treated
apy, or both can be considered in cases in which and continuing until patients are mobilized.
no clinical improvement is observed with induced However, there is a risk associated with antico-
hypertension.27 agulation for prevention of deep venous throm-
bosis in cases in which patients may have to
Hydrocephalus undergo multiple invasive procedures.54
Hydrocephalus may develop soon after subarach-
noid hemorrhage, owing to the presence of ex- A r e a s of Uncer ta in t y
travasated blood blocking normal cerebrospinal
fluid circulation through the subarachnoid cis- The goals for blood pressure and volume status
terns that surround major arteries at the base of after intervention and the appropriate manage-
the brain. Estimates of the incidence of hydro- ment of delayed cerebral ischemia remain uncer-
cephalus range from 15 to 85%27; most cases are tain. There are few data from randomized, con-
not clinically significant. In cases in which hy- trolled trials to guide strategies for reducing the
drocephalus causes encephalopathy, management risk of subarachnoid hemorrhage. Screening pro-
of the hydrocephalus typically involves placement tocols designed to identify cases of asymptom-
of an external ventricular drain, a procedure that atic deep venous thrombosis are of unclear value.
generally results in neurologic improvement. Subarachnoid hemorrhage has effects on thyroid
Alternatively, lumbar drainage can be used to and adrenal function, but data are lacking to
treat acute hydrocephalus and is associated with a show a clear benefit of intervention.
reduced risk of vasospasm; however, obstructive Adjuncts to endovascular treatment, including
hydrocephalus and intraparenchymal hematoma, balloon-tipped microcatheters, stents, and flow-
which cause increased intracranial pressure, are diverting stents, have been developed to manage
contraindications to lumbar drainage. Chronic wide-necked and fusiform aneurysms, but these
symptomatic hydrocephalus occurs in up to one adjuncts often require treatment with antiplate-
third of patients in whom acute hydrocephalus let therapy, with an attendant risk of bleeding.
develops and is treated with a ventriculoperito- These adjuncts are evolving rapidly, and more data
neal shunt for permanent diversion of cerebro- are needed regarding their risks and benefits.
spinal fluid. Hydrocephalus may develop days to
weeks after subarachnoid hemorrhage and should Guidel ine s
be suspected in patients who have a good initial
recovery followed by a plateau or decline in their A writing group of the American Heart Associa-
condition. tion and American Stroke Association published
264 n engl j med 377;3 nejm.org July 20, 2017
The New England Journal of Medicine
Downloaded from nejm.org on July 19, 2017. For personal use only. No other uses without permission.
Copyright © 2017 Massachusetts Medical Society. All rights reserved.
Clinical Pr actice
updated guidelines in 2012 for the management ment. However, open-surgical treatment (surgi-
of aneurysmal subarachnoid hemorrhage.27 The cal clipping) may be preferred on the basis of
recommendations in this article are generally certain features of the aneurysm (e.g., morpho-
consistent with these guidelines. logic characteristics of the aneurysm and an as-
sociated large hematoma) or in younger patients,
given the greater durability of the open-surgical
C onclusions a nd
R ec om mendat ions treatment in the randomized trials.55 Given this
patient’s age, his otherwise healthy status, and
The patient described in the vignette has clinical the location of the aneurysm in the anterior cir-
and radiographic findings that are consistent culation, we would recommend open-surgical
with subarachnoid hemorrhage. Catheter angi- treatment by a specialized, experienced surgeon.
ography is indicated to identify the source of his If a surgeon with expertise in open-surgical tech-
bleeding. An aneurysm is the most common nique is not available at the center, endovascular
cause and, if identified, is associated with a very treatment could be provided instead to eliminate
high risk of rerupture during the next 30 days; the immediate risk of rerupture.
thus, we would recommend immediate treat-
ment. Data from randomized trials have shown No potential conflict of interest relevant to this article was
reported.
better functional outcomes overall with endovas- Disclosure forms provided by the authors are available with
cular treatment than with open-surgical treat- the full text of this article at NEJM.org.
References
1. Rincon F, Rossenwasser RH, Dumont 9. Lall RR, Eddleman CS, Bendok BR, cranial aneurysms: a meta-analysis. Neu-
A. The epidemiology of admissions of non- Batjer HH. Unruptured intracranial aneu- rosurgery 2002;51:1101-7.
traumatic subarachnoid hemorrhage in rysms and the assessment of rupture risk 17. Bassi P, Bandera R, Loiero M, Tognoni
the United States. Neurosurgery 2013;73: based on anatomical and morphological G, Mangoni A. Warning signs in subarach-
217-22. factors: sifting through the sands of data. noid hemorrhage: a cooperative study.
2. Johnston SC, Selvin S, Gress DR. The Neurosurg Focus 2009;26(5):E2. Acta Neurol Scand 1991;84:277-81.
burden, trends, and demographics of mor- 10. Wiebers DO, Whisnant JP, Huston J III, 18. Polmear A. Sentinel headaches in an-
tality from subarachnoid hemorrhage. et al. Unruptured intracranial aneurysms: eurysmal subarachnoid haemorrhage: what
Neurology 1998;50:1413-8. natural history, clinical outcome, and risks is the true incidence? A systematic review.
3. Taufique Z, May T, Meyers E, et al. of surgical and endovascular treatment. Cephalalgia 2003;23:935-41.
Predictors of poor quality of life 1 year Lancet 2003;362:103-10. 19. Matsuda M, Watanabe K, Saito A,
after subarachnoid hemorrhage. Neuro- 11. Ingall T, Asplund K, Mähönen M, Matsumura K, Ichikawa M. Circumstances,
surgery 2016;78:256-64. Bonita R. A multinational comparison of activities, and events precipitating aneu-
4. Elhadi AM, Zabramski JM, Almefty subarachnoid hemorrhage epidemiology rysmal subarachnoid hemorrhage. J Stroke
KK, et al. Spontaneous subarachnoid hem- in the WHO MONICA stroke study. Stroke Cerebrovasc Dis 2007;16:25-9.
orrhage of unknown origin: hospital 2000;31:1054-61. 20. Meurer WJ, Walsh B, Vilke GM, Coyne
course and long-term clinical and angio- 12. de Rooij NK, Linn FH, van der Plas JA, CJ. Clinical guidelines for the emergency
graphic follow-up. J Neurosurg 2015;122: Algra A, Rinkel GJ. Incidence of sub- department evaluation of subarachnoid
663-70. arachnoid haemorrhage: a systematic re- hemorrhage. J Emerg Med 2016;50:696-701.
5. Brown RD Jr, Broderick JP. Unrup- view with emphasis on region, age, gender 21. Edlow JA. Diagnosing headache in the
tured intracranial aneurysms: epidemiol- and time trends. J Neurol Neurosurg Psy- emergency department: what is more im-
ogy, natural history, management options, chiatry 2007;78:1365-72. portant? Being right, or not being wrong?
and familial screening. Lancet Neurol 13. Korja M, Lehto H, Juvela S, Kaprio J. Eur J Neurol 2008;15:1257-8.
2014;13:393-404. Incidence of subarachnoid hemorrhage 22. Kowalski RG, Claassen J, Kreiter KT,
6. Kataoka K, Taneda M, Asai T, is decreasing together with decreasing et al. Initial misdiagnosis and outcome
Kinoshita A, Ito M, Kuroda R. Structural smoking rates. Neurology 2016;87:1118- after subarachnoid hemorrhage. JAMA
fragility and inflammatory response of 23. 2004;291:866-9.
ruptured cerebral aneurysms: a compara- 14. Shea AM, Reed SD, Curtis LH, Alex- 23. Report of World Federation of Neuro-
tive study between ruptured and unrup- ander MJ, Villani JJ, Schulman KA. Char- logical Surgeons Committee on a Univer-
tured cerebral aneurysms. Stroke 1999; acteristics of nontraumatic subarachnoid sal Subarachnoid Hemorrhage Grading
30:1396-401. hemorrhage in the United States in 2003. Scale. J Neurosurg 1988;68:985-6.
7. Bor AS, Koffijberg H, Wermer MJ, Neurosurgery 2007;61:1131-8. 24. Hunt WE, Hess RM. Surgical risk as
Rinkel GJ. Optimal screening strategy for 15. Nieuwkamp DJ, Setz LE, Algra A, related to time of intervention in the re-
familial intracranial aneurysms: a cost- Linn FH, de Rooij NK, Rinkel GJ. Changes pair of intracranial aneurysms. J Neuro-
effectiveness analysis. Neurology 2010;74: in case fatality of aneurysmal subarach- surg 1968;28:14-20.
1671-9. noid haemorrhage over time, according 25. Rowland MJ, Hadjipavlou G, Kelly M,
8. Broderick JP, Brown RD Jr, Sauerbeck to age, sex, and region: a meta-analysis. Westbrook J, Pattinson KT. Delayed cere-
L, et al. Greater rupture risk for familial as Lancet Neurol 2009;8:635-42. bral ischaemia after subarachnoid haem-
compared to sporadic unruptured intra- 16. Huang J, van Gelder JM. The probabil- orrhage: looking beyond vasospasm. Br J
cranial aneurysms. Stroke 2009;40:1952-7. ity of sudden death from rupture of intra- Anaesth 2012;109:315-29.
n engl j med 377;3 nejm.org July 20, 2017 265
The New England Journal of Medicine
Downloaded from nejm.org on July 19, 2017. For personal use only. No other uses without permission.
Copyright © 2017 Massachusetts Medical Society. All rights reserved.
Clinical Pr actice
26. Macdonald RL, Pluta RM, Zhang JH. 36. Ortega-Gutierrez S, Thomas J, Reccius lar approach to intracranial aneurysms.
Cerebral vasospasm after subarachnoid A, et al. Effectiveness and safety of nicar- Neurosurgery 2014;61:Suppl 1:121-9.
hemorrhage: the emerging revolution. Nat dipine and labetalol infusion for blood 46. Dorsch NW, King MT. A review of
Clin Pract Neurol 2007;3:256-63. pressure management in patients with cerebral vasospasm in aneurysmal sub-
27. Connolly ES Jr, Rabinstein AA, Car- intracerebral and subarachnoid hemor- arachnoid haemorrhage. I. Incidence and
huapoma JR, et al. Guidelines for the rhage. Neurocrit Care 2013;18:13-9. effects. J Clin Neurosci 1994;1:19-26.
management of aneurysmal subarachnoid 37. Hillman J, Fridriksson S, Nilsson O, 47. Kassell NF, Torner JC, Haley EC Jr,
hemorrhage: a guideline for healthcare Yu Z, Saveland H, Jakobsson KE. Immedi- Jane JA, Adams HP, Kongable GL. The Inter-
professionals from the American Heart ate administration of tranexamic acid and national Cooperative Study on the Timing
Association/American Stroke Association. reduced incidence of early rebleeding after of Aneurysm Surgery. 1. Overall manage-
Stroke 2012;43:1711-37. aneurysmal subarachnoid hemorrhage: ment results. J Neurosurg 1990;73:18-36.
28. Cortnum S, Sørensen P, Jørgensen J. a prospective randomized study. J Neuro- 48. Lucke-Wold BP, Logsdon AF, Manoran
Determining the sensitivity of computed surg 2002;97:771-8. jan B, et al. Aneurysmal subarachnoid hem-
tomography scanning in early detection 38. Starke RM, Kim GH, Fernandez A, et orrhage and neuroinflammation: a com-
of subarachnoid hemorrhage. Neurosur- al. Impact of a protocol for acute antifi- prehensive review. Int J Mol Sci 2016;17:
gery 2010;66:900-3. brinolytic therapy on aneurysm rebleed- 497.
29. Sayer D, Bloom B, Fernando K, et al. ing after subarachnoid hemorrhage. Stroke 49. McConnell ED, Wei HS, Reitz KM, et
An observational study of 2,248 patients 2008;39:2617-21. al. Cerebral microcirculatory failure after
presenting with headache, suggestive of 39. Gilmore E, Choi HA, Hirsch LJ, Claas- subarachnoid hemorrhage is reversed by
subarachnoid hemorrhage, who received sen J. Seizures and CNS hemorrhage: hyaluronidase. J Cereb Blood Flow Metab
lumbar punctures following normal com- spontaneous intracerebral and aneurys- 2016;36:1537-52.
puted tomography of the head. Acad mal subarachnoid hemorrhage. Neurolo- 50. Dorhout Mees SM, Rinkel GJ, Feigin
Emerg Med 2015;22:1267-73. gist 2010;16:165-75. VL, et al. Calcium antagonists for aneurys-
30. Czuczman AD, Thomas LE, Bou- 40. Molyneux A, Kerr R, Stratton I, et al. mal subarachnoid haemorrhage. Cochrane
langer AB, et al. Interpreting red blood International Subarachnoid Aneurysm Database Syst Rev 2007;3:CD000277.
cells in lumbar puncture: distinguishing Trial (ISAT) of neurosurgical clipping ver- 51. Lennihan L, Mayer SA, Fink ME, et al.
true subarachnoid hemorrhage from trau- sus endovascular coiling in 2143 patients Effect of hypervolemic therapy on cere-
matic tap. Acad Emerg Med 2013;20:247-56. with ruptured intracranial aneurysms: bral blood flow after subarachnoid hem-
31. Shimoda M, Hoshikawa K, Shiramizu a randomised trial. Lancet 2002;360:1267- orrhage: a randomized controlled trial.
H, Oda S, Matsumae M. Problems with 74. Stroke 2000;31:383-91.
diagnosis by fluid-attenuated inversion 41. Molyneux AJ, Kerr RS, Yu LM, et al. 52. Zwienenberg-Lee M, Hartman J,
recovery magnetic resonance imaging in International Subarachnoid Aneurysm Trial Rudisill N, et al. Effect of prophylactic
patients with acute aneurysmal subarach- (ISAT) of neurosurgical clipping versus transluminal balloon angioplasty on cere-
noid hemorrhage. Neurol Med Chir (To- endovascular coiling in 2143 patients bral vasospasm and outcome in patients
kyo) 2010;50:530-7. with ruptured intracranial aneurysms: with Fisher grade III subarachnoid hem-
32. Agid R, Andersson T, Almqvist H, et al. a randomised comparison of effects on orrhage: results of a phase II multicenter,
Negative CT angiography findings in pa- survival, dependency, seizures, rebleed- randomized, clinical trial. Stroke 2008;
tients with spontaneous subarachnoid ing, subgroups, and aneurysm occlusion. 39:1759-65.
hemorrhage: when is digital subtraction Lancet 2005;366:809-17. 53. Samuels O, Webb A, Culler S, Martin
angiography still needed? AJNR Am J Neu- 42. Spetzler RF, McDougall CG, Albu- K, Barrow D. Impact of a dedicated neuro-
roradiol 2010;31:696-705. querque FC, et al. The Barrow Ruptured critical care team in treating patients with
33. Jane JA, Winn HR, Richardson AE. Aneurysm Trial: 3-year results. J Neuro- aneurysmal subarachnoid hemorrhage.
The natural history of intracranial aneu- surg 2013;119:146-57. Neurocrit Care 2011;14:334-40.
rysms: rebleeding rates during the acute 43. Spetzler RF, McDougall CG, Zabrams- 54. Nyquist P, Jichici D, Bautista C, et al.
and long term period and implication for ki JM, et al. The Barrow Ruptured Aneu- Prophylaxis of venous thrombosis in neu-
surgical management. Clin Neurosurg rysm Trial: 6-year results. J Neurosurg rocritical care patients: an executive sum-
1977;24:176-84. 2015;123:609-17. mary of evidence-based guidelines. Criti-
34. Kassell NF, Torner JC. Aneurysmal 44. Boogaarts HD, van Amerongen MJ, cal Care Med 2017;45(3):476-9.
rebleeding: a preliminary report from the de Vries J, et al. Caseload as a factor for 55. Mitchell P, Kerr R, Mendelow AD, Mo-
Cooperative Aneurysm Study. Neurosur- outcome in aneurysmal subarachnoid lyneux A. Could late rebleeding overturn
gery 1983;13:479-81. hemorrhage: a systematic review and the superiority of cranial aneurysm coil
35. Naidech AM, Janjua N, Kreiter KT, et meta-analysis. J Neurosurg 2014;120:605- embolization over clip ligation seen in
al. Predictors and impact of aneurysm re- 11. the International Subarachnoid Aneurysm
bleeding after subarachnoid hemorrhage. 45. Rosenwasser RH, Chalouhi N, Tjou- Trial? J Neurosurg 2008;108:437-42.
Arch Neurol 2005;62:410-6. makaris S, Jabbour P. Open vs endovascu- Copyright © 2017 Massachusetts Medical Society.
nejm clinical practice center
Explore a new page designed specifically for practicing clinicians,
the NEJM Clinical Practice Center, at NEJM.org/clinical-practice-center.
Find practice-changing research, reviews from our Clinical Practice series,
a curated collection of clinical cases, and interactive features
designed to hone your diagnostic skills.
266 n engl j med 377;3 nejm.org July 20, 2017
The New England Journal of Medicine
Downloaded from nejm.org on July 19, 2017. For personal use only. No other uses without permission.
Copyright © 2017 Massachusetts Medical Society. All rights reserved.
You might also like
- NBME 19 ExplanationsDocument96 pagesNBME 19 Explanationsmed student100% (2)
- VSIM Clinical Worksheet 07.16.2020Document6 pagesVSIM Clinical Worksheet 07.16.2020Jackie GriffisNo ratings yet
- A Case Study Presentation On Subarachnoid Hemorrhage: Presented byDocument78 pagesA Case Study Presentation On Subarachnoid Hemorrhage: Presented byNina100% (1)
- Hemorrhagic Stroke CBLDocument106 pagesHemorrhagic Stroke CBLJessica NadiaNo ratings yet
- Case Report-Hemorragic Stroke-Fitra RulianDocument29 pagesCase Report-Hemorragic Stroke-Fitra RuliannabiyaNo ratings yet
- Bacls PDFDocument23 pagesBacls PDFAngelo Domingo0% (1)
- Classification of Head InjuryDocument3 pagesClassification of Head InjuryAndreas LaseNo ratings yet
- Qtsoi Concept MapDocument5 pagesQtsoi Concept MapGenella BabantoNo ratings yet
- Chan, Johnson - TreatmentGuidelines PDFDocument0 pagesChan, Johnson - TreatmentGuidelines PDFBogdan CarabasNo ratings yet
- Case Report-Hemorragic Stroke-Fitra RulianDocument29 pagesCase Report-Hemorragic Stroke-Fitra RuliannabiyaNo ratings yet
- The Pathophysiology of Cocaine AbuseDocument13 pagesThe Pathophysiology of Cocaine AbuseAndy DixonNo ratings yet
- Aneurysmal Subarachnoid Hemorrhage.6Document19 pagesAneurysmal Subarachnoid Hemorrhage.6Aldy Setiawan PutraNo ratings yet
- Subarachnoid HemorrhageDocument3 pagesSubarachnoid HemorrhageTristan Cunanan0% (1)
- Epidural Hematoma Case ReportDocument48 pagesEpidural Hematoma Case ReportJansept Bruce Guinto67% (6)
- Subarachnoid Hemorrhage in The Emergency DepartmentDocument8 pagesSubarachnoid Hemorrhage in The Emergency DepartmentLuis octavio carranzaNo ratings yet
- STEMI - Case ReportDocument42 pagesSTEMI - Case ReportWarren LieNo ratings yet
- Subarachnoid HemorrhageDocument3 pagesSubarachnoid Hemorrhagetenaj_purpleNo ratings yet
- Diagnostic SAHDocument8 pagesDiagnostic SAHMohammadAwitNo ratings yet
- Subarachno Id Hemorrhag E: DONE BY: Rawan AlebousDocument54 pagesSubarachno Id Hemorrhag E: DONE BY: Rawan AlebousHiba AliNo ratings yet
- Ineffective Cerebral Tissue Perfusion Related ToDocument7 pagesIneffective Cerebral Tissue Perfusion Related TohannahNo ratings yet
- Brain AneurysmDocument26 pagesBrain AneurysmHu Eyong100% (1)
- Pathophysiology TBIDocument1 pagePathophysiology TBIChester ManaloNo ratings yet
- Thyroid Lobectomy and IsthmusectomyDocument12 pagesThyroid Lobectomy and IsthmusectomyAgustina100% (1)
- Head Trauma - CaseDocument74 pagesHead Trauma - CaseSardito PhanNo ratings yet
- Pathophysiology of Ischemic Stroke - UpToDateDocument11 pagesPathophysiology of Ischemic Stroke - UpToDateKarla AldamaNo ratings yet
- Laboratory and Diagnostic Findings: Small Cell CarcinomaDocument4 pagesLaboratory and Diagnostic Findings: Small Cell CarcinomaTheresa Sombilla FacunlaNo ratings yet
- A Subdural HematomaDocument12 pagesA Subdural HematomaGina Irene IshakNo ratings yet
- Increased ICPDocument7 pagesIncreased ICPK-La BreanneNo ratings yet
- PPPDocument3 pagesPPPJack BangcoyoNo ratings yet
- Pathophysiology ErDocument3 pagesPathophysiology ErAlexa A. AldayNo ratings yet
- Cva Concept MapDocument1 pageCva Concept MapAnn Justine OrbetaNo ratings yet
- Diagnosis and Management of Subarachnoid HemorrhageDocument25 pagesDiagnosis and Management of Subarachnoid HemorrhageMisael ClintonNo ratings yet
- Subdural HematomaDocument20 pagesSubdural HematomaArief Zamir100% (1)
- Au Di Minor Case Study Myasthenia GravisDocument17 pagesAu Di Minor Case Study Myasthenia Gravisapi-301816885No ratings yet
- Cerebral AneurysmDocument24 pagesCerebral Aneurysmcaptain_rafeNo ratings yet
- Subarachnoid HemorrhageDocument54 pagesSubarachnoid Hemorrhageganga2424No ratings yet
- Pulmonary EdemaDocument50 pagesPulmonary EdemaStacy LuceroNo ratings yet
- Traumatic Brain InjuryDocument14 pagesTraumatic Brain InjurySamuel Hananiel RoryNo ratings yet
- A Case Study ON Cerebrovascular Accident With Left HemiparesisDocument57 pagesA Case Study ON Cerebrovascular Accident With Left Hemiparesisdonheyzz_020% (1)
- Cerebrovascular Accident (Stroke)Document15 pagesCerebrovascular Accident (Stroke)mesdejen100% (1)
- Lacunar Stroke Guide - Causes, Symptoms and Treatment OptionsDocument6 pagesLacunar Stroke Guide - Causes, Symptoms and Treatment OptionsRismanto TorsioNo ratings yet
- Cerebral AneurysmDocument6 pagesCerebral AneurysmNavjot BrarNo ratings yet
- What Is Stroke?: BY: Luis Alberto Sanchez Hernandez Physical TherapistDocument12 pagesWhat Is Stroke?: BY: Luis Alberto Sanchez Hernandez Physical TherapistLidiaAMonroyRNo ratings yet
- Subarachnoid HemorrhageDocument16 pagesSubarachnoid HemorrhageErika NaingNo ratings yet
- NCP CvaDocument4 pagesNCP CvaMariquita BuenafeNo ratings yet
- Pathophysiology and Clinical Manifestation of StrokeDocument42 pagesPathophysiology and Clinical Manifestation of Strokedrg Riki Indra KusumaNo ratings yet
- Introduction - MIDocument10 pagesIntroduction - MIkhimiiiNo ratings yet
- CVA PathophysiologyDocument3 pagesCVA Pathophysiologyshmily_0810No ratings yet
- UGIBDocument1 pageUGIBgarrl100% (1)
- PathophysiologyDocument3 pagesPathophysiologyDimple BlancoNo ratings yet
- CVDDocument67 pagesCVDRachel PerandoNo ratings yet
- Ischemic Stroke Pathophysiology and Principles of Localization (1) G PDFDocument16 pagesIschemic Stroke Pathophysiology and Principles of Localization (1) G PDFGina Ayudia PutriNo ratings yet
- Nanda NCP BasedDocument14 pagesNanda NCP Baseddeliejoyce100% (1)
- Cva-Hypertension-Case-Analysis-Group-I FinalDocument59 pagesCva-Hypertension-Case-Analysis-Group-I FinalVhince Norben PiscoNo ratings yet
- Hyperosmolar Hyperglycemic State (HHS)Document21 pagesHyperosmolar Hyperglycemic State (HHS)Malueth AnguiNo ratings yet
- CASE REPORT Hip DislocationDocument42 pagesCASE REPORT Hip DislocationvereriNo ratings yet
- SUBarachnoid HemorrhageDocument4 pagesSUBarachnoid Hemorrhagekhadzx100% (2)
- Cerebrovascular Disease (Bleed)Document25 pagesCerebrovascular Disease (Bleed)Margaret Jenaw JenawNo ratings yet
- Mallory Weiss SyndromeDocument10 pagesMallory Weiss SyndromeGuilherme CaneverNo ratings yet
- 2017 HSA Clinical PracticeDocument10 pages2017 HSA Clinical PracticeAndrea MartinezNo ratings yet
- Hemorragia SubaracnoideaDocument10 pagesHemorragia SubaracnoideaAna TeresaNo ratings yet
- Spontaneous Intracerebral Hemorrhage - Nejmra2201449Document2 pagesSpontaneous Intracerebral Hemorrhage - Nejmra2201449Elena RamiroNo ratings yet
- Cerebral AneurysmsDocument12 pagesCerebral AneurysmsDyah Ayu Puspita AnggarsariNo ratings yet
- NEJM 2022 Sheth Review Article On ICHDocument8 pagesNEJM 2022 Sheth Review Article On ICHV ANo ratings yet
- Hyperglycemic CrisisDocument9 pagesHyperglycemic CrisisRoberto López MataNo ratings yet
- Best Clinical Practice: AnaphylaxisDocument6 pagesBest Clinical Practice: AnaphylaxisputriNo ratings yet
- Diuretic Treatment in Heart FailureDocument12 pagesDiuretic Treatment in Heart FailureRoberto López Mata100% (1)
- ADA 2018 Diabetes CareDocument150 pagesADA 2018 Diabetes CareRoberto López Mata100% (1)
- Diagnosis and Treatment of HyperkalemiaDocument9 pagesDiagnosis and Treatment of HyperkalemiaRoberto López MataNo ratings yet
- Uric Acid Is A Strong Risk Marker For Developing Hypertension From PrehypertensionDocument16 pagesUric Acid Is A Strong Risk Marker For Developing Hypertension From PrehypertensionRoberto López MataNo ratings yet
- Update On The Management of Venous ThromboembolismDocument8 pagesUpdate On The Management of Venous ThromboembolismRoberto López MataNo ratings yet
- Fluid Therapy Options and Rational SelectionDocument13 pagesFluid Therapy Options and Rational SelectionRoberto López MataNo ratings yet
- Pathophysiology of Septic ShockDocument19 pagesPathophysiology of Septic ShockRoberto López MataNo ratings yet
- A Test in Context - D-DimerDocument10 pagesA Test in Context - D-DimerRoberto López MataNo ratings yet
- 2015 ESC Guidelines For The Diagnosis and Management of Pericardial DiseasesDocument44 pages2015 ESC Guidelines For The Diagnosis and Management of Pericardial DiseasesRoberto López MataNo ratings yet
- Rivaroxaban Vs Warfarin Sodium in The Ultra-Early Period After Atrial Fibrillation-Related Mild Ischemic StrokeDocument10 pagesRivaroxaban Vs Warfarin Sodium in The Ultra-Early Period After Atrial Fibrillation-Related Mild Ischemic StrokeRoberto López MataNo ratings yet
- Acute Monocular Vision LossDocument9 pagesAcute Monocular Vision LossRoberto López MataNo ratings yet
- Delirium in Hospitalized Older AdultsDocument11 pagesDelirium in Hospitalized Older AdultsRoberto López MataNo ratings yet
- Evaluation and Management of Lower-Extremity UlcersDocument9 pagesEvaluation and Management of Lower-Extremity UlcersRoberto López MataNo ratings yet
- Will This Hemodynamically Unstable Patient Respond To A Bolus of Intravenous Fluids?Document12 pagesWill This Hemodynamically Unstable Patient Respond To A Bolus of Intravenous Fluids?Roberto López MataNo ratings yet
- Predicting 30-DayMortality For PatientsWith AcuteHeart Failure in The EmergencyDepartmentDocument14 pagesPredicting 30-DayMortality For PatientsWith AcuteHeart Failure in The EmergencyDepartmentRoberto López MataNo ratings yet
- Electrolyte Disturbances in Patients With Chronic Alcohol-Use DisorderDocument10 pagesElectrolyte Disturbances in Patients With Chronic Alcohol-Use DisorderRoberto López MataNo ratings yet
- Indications For and Adverse Effects of Red-Cell TransfusionDocument12 pagesIndications For and Adverse Effects of Red-Cell TransfusionRoberto López Mata100% (1)
- Acute Coronary Syndromes The Way Forward From Mechanisms To Precision TreatmentDocument13 pagesAcute Coronary Syndromes The Way Forward From Mechanisms To Precision TreatmentRoberto López MataNo ratings yet
- Ischemic Stroke Pathophysiology and Principles of Localization (1) G PDFDocument16 pagesIschemic Stroke Pathophysiology and Principles of Localization (1) G PDFGina Ayudia PutriNo ratings yet
- Anti Angina (Hany)Document51 pagesAnti Angina (Hany)Angga AhadiyatNo ratings yet
- Scientific Evidence-Based Effects of Hydrotherapy On Various Systems of The BodyDocument16 pagesScientific Evidence-Based Effects of Hydrotherapy On Various Systems of The Bodydonald duckNo ratings yet
- CVD and HTNDocument60 pagesCVD and HTNZsazsa100% (1)
- Uworld QuestionsDocument17 pagesUworld Questionsmoped00No ratings yet
- Ischemic Heart DiseaseDocument8 pagesIschemic Heart DiseaseNina Natalia Bautista100% (1)
- Drug Study AdalatDocument4 pagesDrug Study AdalatLea CelestialNo ratings yet
- Hridroga Samprapti and Modern Pathology of IhdDocument11 pagesHridroga Samprapti and Modern Pathology of IhdGAURAVNo ratings yet
- Cardiovascular Study GuideDocument19 pagesCardiovascular Study GuideLouise FraserNo ratings yet
- Aneurysm BJADocument17 pagesAneurysm BJAParvathy R NairNo ratings yet
- Endothelial Dysfunction and Vascular Disease - A 30th Anniversary UpdateDocument75 pagesEndothelial Dysfunction and Vascular Disease - A 30th Anniversary UpdateAna Clara RodriguesNo ratings yet
- Nervus 3Document3 pagesNervus 3Palneuro UnsriNo ratings yet
- Ischemic Heart DiseaseDocument31 pagesIschemic Heart DiseaseRohit SahNo ratings yet
- Mini Case Study 1Document14 pagesMini Case Study 1Casas, Jo-an Pauline A.No ratings yet
- Hemorragia SubaracnoideaDocument10 pagesHemorragia SubaracnoideaAna TeresaNo ratings yet
- Pharmacology Test 3 - Cardiovascular Drugs, Part I Flashcards - QuizletDocument10 pagesPharmacology Test 3 - Cardiovascular Drugs, Part I Flashcards - QuizletBhopesh Kadian0% (1)
- VASODILATORSDocument30 pagesVASODILATORSEvangelin MelvinNo ratings yet
- PharmaAntianginal DrugsDocument175 pagesPharmaAntianginal DrugsNidal AbboudNo ratings yet
- Kramer 2013Document8 pagesKramer 2013zixzaxoffNo ratings yet
- Antianginal Drugs: Claro M. Isidro M.DDocument34 pagesAntianginal Drugs: Claro M. Isidro M.DNikki ChauhanNo ratings yet
- Peripheral Vascular Diseases Practice QuizDocument12 pagesPeripheral Vascular Diseases Practice QuizErica Veluz LuyunNo ratings yet
- Cardiovascular Pharmacology: Ana Sharmaine S. Uera, MD DR PJGMRMC Anesthesiology Department 1st Year ResidentDocument68 pagesCardiovascular Pharmacology: Ana Sharmaine S. Uera, MD DR PJGMRMC Anesthesiology Department 1st Year ResidentLalay CabanagNo ratings yet
- Brain ICHDocument19 pagesBrain ICHAditya KurniantoNo ratings yet
- CV - Imaging of Heart Disease in Women - Review and Case PresentationDocument30 pagesCV - Imaging of Heart Disease in Women - Review and Case PresentationAndi Wetenri PadaulengNo ratings yet
- Ischemic Heart DiseaseDocument6 pagesIschemic Heart DiseaseApril Joy Villacorta PonceNo ratings yet
- Imitrex: (Sumatriptan) Nasal SprayDocument25 pagesImitrex: (Sumatriptan) Nasal Spray58TRONGNo ratings yet