Professional Documents
Culture Documents
2004RwaringRwaring2004p5302004-06-04The Risk of Recurrent Venous
2004RwaringRwaring2004p5302004-06-04The Risk of Recurrent Venous
Uploaded by
Luciano McsCopyright:
Available Formats
You might also like
- 10 1038@nrdp20156Document17 pages10 1038@nrdp20156Desi DwiNo ratings yet
- Blom JW - Malignancies, Prothrombotic Mutations, and The Risk of Venous ThrombosisDocument8 pagesBlom JW - Malignancies, Prothrombotic Mutations, and The Risk of Venous ThrombosisFarid RakhmanNo ratings yet
- Helen K. Chew - Incidence of Venous Thromboembolism and Its Effect On SurvivalDocument7 pagesHelen K. Chew - Incidence of Venous Thromboembolism and Its Effect On SurvivalFarid RakhmanNo ratings yet
- Embolismo Pulmonar NejmDocument3 pagesEmbolismo Pulmonar NejmSaidNo ratings yet
- Venous Thrombotic Recurrence After Cerebral Venous ThrombosisDocument7 pagesVenous Thrombotic Recurrence After Cerebral Venous ThrombosisMartina Alarcon AcevedoNo ratings yet
- Thrombosis and Acute LeukemiaDocument6 pagesThrombosis and Acute Leukemiaannisa edwarNo ratings yet
- Caso TEP Bibliografia Bis 2023Document7 pagesCaso TEP Bibliografia Bis 2023Viviana MorenoNo ratings yet
- Study 1Document6 pagesStudy 1suhamkky8No ratings yet
- Meissner2007Document29 pagesMeissner2007dewiNo ratings yet
- Khorana AA - Thromboembolism in Hospitalized Neutropenic Cancer PatientsDocument8 pagesKhorana AA - Thromboembolism in Hospitalized Neutropenic Cancer PatientsFarid RakhmanNo ratings yet
- Blood 742304Document9 pagesBlood 742304Francieudo SampaioNo ratings yet
- Aspirina Después de Fractura Art Ing 2023Document4 pagesAspirina Después de Fractura Art Ing 2023roman rodriguezNo ratings yet
- 1 s2.0 S0006497120687596 MainDocument5 pages1 s2.0 S0006497120687596 MainnadaNo ratings yet
- 3144.full MoyamoyaDocument8 pages3144.full MoyamoyaDarren ZytkiewiczNo ratings yet
- JCTH 7 154Document11 pagesJCTH 7 154Andreea AlexandruNo ratings yet
- TEP Systemic Thrombolysis For Pulmonary Embolism Evidence, Patient Selection, and Protocols For ManagementDocument10 pagesTEP Systemic Thrombolysis For Pulmonary Embolism Evidence, Patient Selection, and Protocols For Managementbenitez1228No ratings yet
- DVT in India PDFDocument6 pagesDVT in India PDFKarthik KoneruNo ratings yet
- Jama Neal 2023 Ed 230070 1696973944.14124Document2 pagesJama Neal 2023 Ed 230070 1696973944.14124Luz Elena ValderramaNo ratings yet
- Postpartum Hemorrhage-Epidemiology, Risk Factors, and CausesDocument13 pagesPostpartum Hemorrhage-Epidemiology, Risk Factors, and CausesNilfacio PradoNo ratings yet
- Plueral Effusion and Ovarian CancerDocument5 pagesPlueral Effusion and Ovarian CancerAthenaeum Scientific PublishersNo ratings yet
- Management of Contraception in Adolescent Females With Hormone-Related Venous ThromboembolismDocument5 pagesManagement of Contraception in Adolescent Females With Hormone-Related Venous ThromboembolismInggrit DirgantariNo ratings yet
- Abnormaluterinebleeding Inyoungwomenwithblood Disorders: Kathryn E. Dickerson,, Neethu M. Menon,, Ayesha ZiaDocument18 pagesAbnormaluterinebleeding Inyoungwomenwithblood Disorders: Kathryn E. Dickerson,, Neethu M. Menon,, Ayesha ZiaSalvador ArredondoNo ratings yet
- VTE in Unusual Sites BJH - 2012Document11 pagesVTE in Unusual Sites BJH - 2012Chenuri Annamarie RanasingheNo ratings yet
- How We Diagnose and Treat Deep Vein Thrombosis.: Author InformationDocument18 pagesHow We Diagnose and Treat Deep Vein Thrombosis.: Author InformationligitafitranandaNo ratings yet
- Thromboprophylaxis after Extremity Fracture — Time for Aspirin? (2023)Document2 pagesThromboprophylaxis after Extremity Fracture — Time for Aspirin? (2023)ericdgNo ratings yet
- 01-16 Optimal Therapy For Unstable Pulmonar EmbolismDocument4 pages01-16 Optimal Therapy For Unstable Pulmonar EmbolismLesly Peinado TorresNo ratings yet
- Clinical Considerations in Recurrent Miscarriage: Journal ofDocument5 pagesClinical Considerations in Recurrent Miscarriage: Journal ofElena VisterniceanNo ratings yet
- Pregnancy, The Postpartum Period and Prothrombotic Defects: Risk of Venous Thrombosis in The MEGA StudyDocument6 pagesPregnancy, The Postpartum Period and Prothrombotic Defects: Risk of Venous Thrombosis in The MEGA StudyAlfa FebriandaNo ratings yet
- 1 s2.0 S2376060524000063 MainDocument4 pages1 s2.0 S2376060524000063 Mainifte5104385No ratings yet
- Venous Thromboembolism: What To Do After Anticoagulation Is StartedDocument10 pagesVenous Thromboembolism: What To Do After Anticoagulation Is StartedJuanMa Correa SanabriaNo ratings yet
- Highlow StudyDocument7 pagesHighlow StudySilvia IzvoranuNo ratings yet
- Evidence-Based Therapies For Pharmacologic Prevention and Treatment of Acute Deep Vein Thrombosis And  Pulmonary EmbolismDocument15 pagesEvidence-Based Therapies For Pharmacologic Prevention and Treatment of Acute Deep Vein Thrombosis And  Pulmonary EmbolismBolivar IseaNo ratings yet
- Jurnal 15Document5 pagesJurnal 15rifkipspdNo ratings yet
- A Comparison of Enoxaparin With Placebo For The Prevention ofDocument8 pagesA Comparison of Enoxaparin With Placebo For The Prevention ofjose luisNo ratings yet
- Mulatu Et Al 2020 Deep Venous Thrombosis Recurrence and Its Predictors at Selected Tertiary Hospitals in Ethiopia ADocument14 pagesMulatu Et Al 2020 Deep Venous Thrombosis Recurrence and Its Predictors at Selected Tertiary Hospitals in Ethiopia Amulatbirhanu100No ratings yet
- Schnatz 2011Document9 pagesSchnatz 2011Benjamin SiglicNo ratings yet
- GastroprofilaxisDocument13 pagesGastroprofilaxisDaniel Alejandro Lecaros BarríaNo ratings yet
- Tep 1Document16 pagesTep 1Yarlin MontoyaNo ratings yet
- Heit2008Document6 pagesHeit2008dewiNo ratings yet
- Dose-Adjusted Enoxaparin Thromboprophylaxis in Hospitalized CancerDocument7 pagesDose-Adjusted Enoxaparin Thromboprophylaxis in Hospitalized CancerAnonymous 9dVZCnTXSNo ratings yet
- Circulation 2014 Piazza 283 7Document6 pagesCirculation 2014 Piazza 283 7arthoclaseNo ratings yet
- Khorana AA - Frequency, Risk Factors, and Trends For Venous Thromboembolism Among Hospitalized Cancer PatientsDocument8 pagesKhorana AA - Frequency, Risk Factors, and Trends For Venous Thromboembolism Among Hospitalized Cancer PatientsFarid RakhmanNo ratings yet
- Caos PaperDocument6 pagesCaos PaperMauricio Lopez MejiaNo ratings yet
- 19 TEP Tak2019Document12 pages19 TEP Tak2019Juan Carlos Uribe CaballeroNo ratings yet
- Nej M 199603213341203Document4 pagesNej M 199603213341203Krinta AlisaNo ratings yet
- Seminar: Faizan Khan, Tobias Tritschler, Susan R Kahn, Marc A RodgerDocument14 pagesSeminar: Faizan Khan, Tobias Tritschler, Susan R Kahn, Marc A RodgerJuan Camilo Morales TabordaNo ratings yet
- Inpatient Inherited Thrombophilia Testing: Choosing Wisely: Things We Do For No ReasonDocument4 pagesInpatient Inherited Thrombophilia Testing: Choosing Wisely: Things We Do For No Reasonkishore kumar meelNo ratings yet
- Risk of ThrombosisDocument13 pagesRisk of ThrombosisNataliaHermosilloNo ratings yet
- Streptokinase in The Treatment of Pleural Controlled Trial of IntrapleuralDocument7 pagesStreptokinase in The Treatment of Pleural Controlled Trial of IntrapleuraltomgasoneNo ratings yet
- Assessing Hypercoagulability and VTE Risk Using Thromboelastography and Khorana Score in Women With Cancers Receiving Chemotherapy 2024Document9 pagesAssessing Hypercoagulability and VTE Risk Using Thromboelastography and Khorana Score in Women With Cancers Receiving Chemotherapy 2024myqrwd464kNo ratings yet
- Leunase and TrombolismDocument12 pagesLeunase and TrombolismSanta UlinaNo ratings yet
- The Coagulopathy of Cancer: ReviewDocument7 pagesThe Coagulopathy of Cancer: ReviewlucyishakNo ratings yet
- Malignant Mesothelioma Presenting With Unexplained Recurrent Pleurisy EpisodesDocument4 pagesMalignant Mesothelioma Presenting With Unexplained Recurrent Pleurisy EpisodesNurul NingrumNo ratings yet
- Jurnal 9Document9 pagesJurnal 9Atikah AbayNo ratings yet
- New England Journal Medicine: The ofDocument9 pagesNew England Journal Medicine: The ofHila AmaliaNo ratings yet
- Seminar: PathophysiologyDocument12 pagesSeminar: PathophysiologyBeni KurniawanNo ratings yet
- Hypercoagulable and TestingDocument14 pagesHypercoagulable and TestingSri HartiniNo ratings yet
- Our Experience With Bicytopenia in Patients Treated at The Ankara Hospital Pediatric ClinicDocument5 pagesOur Experience With Bicytopenia in Patients Treated at The Ankara Hospital Pediatric ClinicRonny DoankNo ratings yet
- Thrombophilia-Associated Pregnancy Wastage: Modern TrendsDocument10 pagesThrombophilia-Associated Pregnancy Wastage: Modern TrendspogimudaNo ratings yet
- Anatomy Muscular System BrochureDocument2 pagesAnatomy Muscular System Brochureapi-462608096No ratings yet
- CVS - BloodDocument30 pagesCVS - BloodQuimson KennethNo ratings yet
- PMLS2 EsentialsDocument38 pagesPMLS2 EsentialsKen Novero100% (1)
- HematologyDocument2 pagesHematologyMohammed Al-RahmaweeNo ratings yet
- hssb2101t SecquizDocument2 pageshssb2101t Secquizfhhgghhg hggghgNo ratings yet
- Normal Laboratory ValuesDocument40 pagesNormal Laboratory ValuesPrincess Nasima M. Usngan100% (1)
- Untitled4 PDFDocument13 pagesUntitled4 PDFElizabeth LeonNo ratings yet
- Anemia in TropicsDocument7 pagesAnemia in TropicsAsnaafii BantiiNo ratings yet
- 3 PracticalDocument47 pages3 PracticalT NNo ratings yet
- CBCDocument3 pagesCBCDicky DamaraNo ratings yet
- Hemostasis - TrombositDocument28 pagesHemostasis - TrombositNovi AndrianiNo ratings yet
- Invitro Anticoagulant Activity of Emblica Officinalis Leaf Extract On Normal Healthy Blood PlasmaDocument4 pagesInvitro Anticoagulant Activity of Emblica Officinalis Leaf Extract On Normal Healthy Blood PlasmaInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- CBCDocument1 pageCBCAhmed GaberNo ratings yet
- Alveolar BoneDocument8 pagesAlveolar BoneClarisse MendozaNo ratings yet
- Itp 210530123628Document26 pagesItp 210530123628Sakthi DeviNo ratings yet
- Blood TransfusionDocument5 pagesBlood Transfusionrupali gahalianNo ratings yet
- Ruby BrochureDocument8 pagesRuby BrochureNalan SezerNo ratings yet
- Memo Re Blood donationBJMPDocument1 pageMemo Re Blood donationBJMPptsievccdNo ratings yet
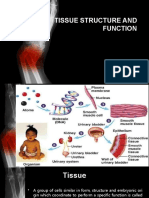
- Tissue Structure & FunctionDocument74 pagesTissue Structure & FunctionTaufiqurrahman Sidqi100% (1)
- SGD Case: Hematology Weakness: Dizziness: Anorexia: Vomit: Numbness: TinglingingDocument10 pagesSGD Case: Hematology Weakness: Dizziness: Anorexia: Vomit: Numbness: TinglingingEveryday FundayNo ratings yet
- Blood TransfusionDocument21 pagesBlood TransfusionAnup GouravNo ratings yet
- Physical Characteristics: C. PlateletsDocument6 pagesPhysical Characteristics: C. PlateletsGwyneth Marie DayaganNo ratings yet
- G5 - Bones and MusclesDocument4 pagesG5 - Bones and MusclesrababNo ratings yet
- Kell Blood Group System: Muhammad Asif Zeb Lecturer Hematology Ipms-Kmu PeshawarDocument11 pagesKell Blood Group System: Muhammad Asif Zeb Lecturer Hematology Ipms-Kmu PeshawarMaaz KhanNo ratings yet
- HEMOSTASISDocument12 pagesHEMOSTASISRyan PedregosaNo ratings yet
- (K5-1) Kuliah Anemia Hemolitik (Dr. Riza)Document21 pages(K5-1) Kuliah Anemia Hemolitik (Dr. Riza)Puti Callistha IchsanNo ratings yet
- Hemorrhagic Shock (Anestesi)Document44 pagesHemorrhagic Shock (Anestesi)Dwi Meutia IndriatiNo ratings yet
- 13 OCTOBER, 2021 Wednesday Biology Transport SystemDocument12 pages13 OCTOBER, 2021 Wednesday Biology Transport SystemOyasor Ikhapo AnthonyNo ratings yet
- Skeletal Guided NotesDocument4 pagesSkeletal Guided Notesapi-591284844No ratings yet
- ThrombocytopeniaDocument49 pagesThrombocytopeniaMaria EnjelinaNo ratings yet
2004RwaringRwaring2004p5302004-06-04The Risk of Recurrent Venous
2004RwaringRwaring2004p5302004-06-04The Risk of Recurrent Venous
Uploaded by
Luciano McsOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
2004RwaringRwaring2004p5302004-06-04The Risk of Recurrent Venous
2004RwaringRwaring2004p5302004-06-04The Risk of Recurrent Venous
Uploaded by
Luciano McsCopyright:
Available Formats
The new england journal of medicine
original article
The Risk of Recurrent Venous
Thromboembolism in Men and Women
Paul A. Kyrle, M.D., Erich Minar, M.D., Christine Bialonczyk, M.D.,
Mirko Hirschl, M.D., Ansgar Weltermann, M.D., and Sabine Eichinger, M.D.
abstract
background
From the Department of Internal Medi- Whether a patient’s sex is associated with the risk of recurrent venous thromboembo-
cine I, Division of Hematology and Hemo- lism is unknown.
stasis (P.A.K., A.W., S.E.), Ludwig Boltz-
mann-Institut für Thromboseforschung
(P.A.K.), and the Department of Internal methods
Medicine II, Division of Angiology, Medical We studied 826 patients for an average of 36 months after a first episode of spontane-
University of Vienna (E.M.); Wilhelminen-
spital (C.B.); and Hanusch Krankenhaus ous venous thromboembolism and the withdrawal of oral anticoagulants. We excluded
(M.H.) — all in Vienna. Address reprint pregnant patients and patients with a deficiency of antithrombin, protein C, or protein S;
requests to Dr. Kyrle at the Department of the lupus anticoagulant; cancer; or a requirement for potentially long-term antithrom-
Internal Medicine I, Division of Hema-
tology and Hemostasis, Währinger Gürtel botic treatment. The end point was objective evidence of a recurrence of symptomatic
18-20, A 1090 Vienna, Austria, or at venous thromboembolism.
paul.kyrle@meduniwien.ac.at.
N Engl J Med 2004;350:2558-63. results
Copyright © 2004 Massachusetts Medical Society. Venous thromboembolism recurred in 74 of the 373 men, as compared with 28 of the
453 women (20 percent vs. 6 percent; relative risk of recurrence, 3.6; 95 percent confi-
dence interval, 2.3 to 5.5; P<0.001). The risk remained unchanged after adjustment for
age, the duration of anticoagulation, and the presence or absence of a first symptomatic
pulmonary embolism, factor V Leiden, factor II G20210A, or an elevated level of factor
VIII or IX. At five years, the likelihood of recurrence was 30.7 percent among men, as
compared with 8.5 percent among women (P<0.001). The relative risk of recurrence
was similar among women who had had their first thrombosis during oral-contraceptive
use or hormone-replacement therapy and women in the same age group in whom the
first event was idiopathic.
conclusions
The risk of recurrent venous thromboembolism is higher among men than women.
2558 n engl j med 350;25 www.nejm.org june 17, 2004
Downloaded from www.nejm.org by MAURO L. KAUFMANN MD on June 17, 2004.
Copyright © 2004 Massachusetts Medical Society. All rights reserved.
the risk of recurrent venous thromboembolism in men and women
cer in 423; and the need for long-term treatment
t he annual incidence of venous
thromboembolism is 1 to 2 cases per 1000
persons,1,2 and the risk of the disorder
rises exponentially with age, from an annual rate of
less than 5 per 100,000 children to greater than 400
with antithrombotic drugs for reasons other than
venous thrombosis in 436.
The day of discontinuation of oral anticoagulants
was defined as the day of study entry. After three
per 100,000 adults older than 80 years.3 The overall weeks, patients were screened for the presence of
incidence of a first venous thromboembolism a deficiency of antithrombin, protein C, and protein
seems to be similar among men and women,1-3 but S; the lupus anticoagulant; factor V Leiden; and fac-
the risk is higher among women of childbearing age tor II G20210A. Levels of factors VIII and IX were
than among men in the same age group.2,4,5 This also determined. The 24 patients who had a defi-
difference probably relates to the association of ciency of antithrombin, protein C, or protein S or
venous thromboembolism with pregnancy or the in whom the lupus anticoagulant was detected were
use of oral contraceptives. By contrast, the risk excluded. Patients were observed at three-month
among older women is substantially lower than that intervals for the first year and every six months
among men in the same age group.2,4,5 thereafter. They were provided with detailed written
Venous thromboembolism has a recurrence rate information on the symptoms of venous thrombo-
of 5 to 10 percent per year.6-8 As for a first episode, embolism and were instructed to report to one of
the pathogenesis of recurrences is multifactorial, the thrombosis centers in case of symptoms. All
with risks that depend on the severity and number women were strongly discouraged from using con-
of hereditary and circumstantial factors. Whether a traceptive pills or hormone-replacement therapy
patient’s sex is associated with the risk of recurrent regardless of whether they had a history of an asso-
venous thromboembolism is uncertain. Large pro- ciation between the use of these hormones and the
spective studies of the incidence of recurrence did initial venous thromboembolism. At each visit, a
not address sex.6,8 In a study in Norway,7 proximal data form was completed regarding the patient’s
deep-vein thrombosis, cancer, and a history of ve- medical history.
nous thromboembolism, but not the person’s sex,
predicted an increased risk of recurrent thrombotic diagnosis of venous thromboembolism
events. In this report, we assessed the association of The diagnosis of deep-vein thrombosis was estab-
patient sex with the risk of recurrence in 826 pa- lished by venography or color-coded duplex sonog-
tients with a first episode of spontaneous venous raphy (in the case of proximal deep-vein thrombo-
thromboembolism. sis). If venography was used, one of the following
direct or indirect criteria had to be fulfilled: a con-
methods stant filling defect was present on two views; there
was an abrupt discontinuation of the contrast-filled
patients and study design vessel at a constant point in the vein; and the entire
The Austrian Study on Recurrent Venous Thrombo- deep-vein system failed to fill without an external
embolism is an ongoing prospective study involv- compressing process, with or without venous flow
ing four thrombosis centers in Vienna. Between through collateral veins. Diagnostic criteria for
July 1992 and June 2003, 2795 patients older than color-coded duplex sonography were the following:
18 years of age who had been treated with oral anti- visualization of an intraluminal thrombus in a deep
coagulants for at least three months after venous vein, lack of or incomplete compressibility, and lack
thromboembolism were enrolled after providing of flow spontaneously and after distal manipula-
written informed consent. All patients had been tion. The diagnosis of pulmonary embolism was
treated with standard heparin at doses designed to made by ventilation–perfusion lung scanning ac-
keep the activated partial-thromboplastin time 1.5 cording to the criteria of the Prospective Investiga-
to 2.0 times that of the control value or with subcu- tion of Pulmonary Embolism Diagnosis.9 Patients
taneous low-molecular-weight heparin at therapeu- with both deep-vein thrombosis and pulmonary
tic doses. A total of 1945 patients were excluded embolism were categorized as having pulmonary
because of the following conditions: previous ve- embolism.
nous thromboembolism in 451; surgery, trauma, or
pregnancy within the previous three months in 527; outcome measures
a known deficiency of antithrombin, protein C, or The end point of the study was recurrence of symp-
protein S in 65; the lupus anticoagulant in 43; can- tomatic venous thromboembolism confirmed by
n engl j med 350;25 www.nejm.org june 17, 2004 2559
Downloaded from www.nejm.org by MAURO L. KAUFMANN MD on June 17, 2004.
Copyright © 2004 Massachusetts Medical Society. All rights reserved.
The new england journal of medicine
venography, ventilation–perfusion lung scanning, ment for potentially long-term antithrombotic treat-
or both, according to the aforementioned criteria. ment, a diagnosis of cancer, or pregnancy, who were
The diagnosis was established by an adjudication lost to follow-up, or who died were censored at the
committee consisting of independent clinicians and time of withdrawal. To test for homogeneity among
radiologists who were aware of the patient’s sex but the various groups of patients, we used the log-rank
unaware of the presence or absence of thrombotic test. Univariate and multivariate Cox proportional-
risk factors. Recurrent deep-vein thrombosis was hazards models were used to analyze the associa-
diagnosed if the patient had a thrombus in another tion of the patient’s sex with the risk of recurrent
deep vein in the leg involved in the previous event, venous thromboembolism. Analyses were adjusted
a thrombus in the other leg, or a thrombus in the for age, the presence or absence of symptomatic
same venous system involved in the previous event pulmonary embolism at the time of a first throm-
with a proximal extension of the thrombus if the botic event, the duration of anticoagulation, and the
upper limit of the original thrombus had been visi- presence or absence of factor V Leiden, factor II
ble or the presence of a constant filling defect sur- G20210A, and elevated levels of factors VIII and IX
rounded by contrast medium if it had not. (dichotomized at the 90th percentile [234 IU per
deciliter] and at the 75th percentile [138 IU per
laboratory analysis deciliter] of the patient population, respectively).
Venous blood was obtained after the patient had All computations were performed with the use of
fasted overnight, placed in 1/10 volume of 0.11 SPSS software, version 10.0.
mmol of trisodium citrate per liter, and centrifuged
for 20 minutes at 2000¬g. The plasma was stored at results
–80°C. Routine laboratory methods were used to
identify antithrombin, protein C, and protein S. study population
Screening for factor V Leiden and factor II G20210A We studied 826 patients (373 men and 453 women)
was carried out on genomic DNA as described pre- who had had a first episode of spontaneous venous
viously.10,11 Factor VIII and factor IX were measured thromboembolism. The mean ages of these men
by one-step clotting assays with the use of factor and women were 51±14 years and 45±18 years, re-
VIII– or factor IX–deficient plasma (Immuno Baxter) spectively (P<0.001). They were enrolled after the
and a Sysmex CA 6000 fully automated coagulation discontinuation of oral anticoagulants and followed
analyzer. The presence of the lupus anticoagulant for a median of 26 months. The median duration of
was established on the basis of the criteria of the follow-up was 23 months (interquartile range, 10 to
Subcommittee on Lupus Anticoagulant/Antiphos- 49) among the men and 28 months (interquartile
pholipid Antibody of the Scientific and Standardisa- range, 12 to 57) among the women (P=0.02). A total
tion Committee of the International Society on of 189 patients left the study: 125 required long-
Thrombosis and Haemostasis.12 The technicians term antithrombotic treatment for reasons other
were unaware of the patient’s characteristics, in- than venous thromboembolism (15 women and 10
cluding sex, at all times. men received anticoagulants because of atrial fibril-
lation and 54 women and 46 men were given aspirin
statistical analysis for arterial disease), 14 received a diagnosis of can-
Categorical data were compared between groups cer, 26 became pregnant and started prophylaxis
with use of contingency-table analyses (the chi- with low-molecular-weight heparin, and 24 were
square test), and continuous data (presented as lost to follow-up. Three patients died of cancer, six
means ±SD) were compared with use of Mann– of cardiac failure, and one of septicemia.
Whitney U tests. All P values were two-tailed. Sur-
vival-time methods were used to analyze the time recurrent venous thromboembolism
to recurrent venous thromboembolism among pa- A total of 102 of the 826 patients (12 percent) had
tients with a subsequent episode (uncensored ob- recurrent venous thromboembolism (deep-vein
servations) or the duration of follow-up among pa- thrombosis in 67 and pulmonary embolism in 35).
tients without recurrence (censored observations).13 Of these 102 patients, 74 (73 percent) were men
The probability of recurrence was estimated accord- and 28 (27 percent) were women. Table 1 shows
ing to the method of Kaplan and Meier.14 Data on the relative risk of a recurrence according to age,
patients who left the study because of a require- the presence of a previous symptomatic pulmonary
2560 n engl j med 350;25 www.nejm.org june 17 , 2004
Downloaded from www.nejm.org by MAURO L. KAUFMANN MD on June 17, 2004.
Copyright © 2004 Massachusetts Medical Society. All rights reserved.
the risk of recurrent venous thromboembolism in men and women
embolism, factor V Leiden, factor II G20210A, or an
Table 1. Relative Risk of Recurrent Venous Thromboembolism According to
elevated level of factor VIII or IX, and the duration Baseline Characteristics.*
of anticoagulation. When age was analyzed in a Cox
proportional-hazards model, the relative risk of Univariate Multivariate
Relative Risk Relative Risk
recurrent venous thromboembolism was 1.2 (95 Characteristic (95% CI) (95% CI)†
percent confidence interval, 1.1. to 1.4; P=0.001)
Age (per 10-yr increase) 1.2 (1.1–1.4) 1.1 (0.9–1.3)
for each 10-year increase and 1.1 (95 percent confi-
dence interval, 0.9 to 1.3; P=0.3) in the multivari- Symptomatic pulmonary embolism 1.7 (1.2–2.5) 1.7 (1.1–2.5)
(vs. deep-vein thrombosis)
ate analysis. An elevated level of factor VIII and a
Factor V Leiden (vs. absence of 1.0 (0.7–1.6) 1.2 (0.8–1.8)
first symptomatic pulmonary embolism were the mutation)
strongest determinants of recurrence. Factor II G20210A (vs. absence of 1.7 (0.9–3.1) 2.1 (1.1–3.8)
mutation)
recurrent venous thromboembolism Factor VIII ≥234 IU/dl (vs. <234 IU/dl) 3.4 (2.1–5.6) 2.9 (1.6–5.1)
and sex
Factor IX ≥138 IU/dl (vs. <138 IU/dl) 1.8 (1.2–2.7) 1.3 (0.8–2.0)
Venous thromboembolism recurred in 74 of the Duration of anticoagulation (per 3-mo 1.03 (0.99–1.07) 1.02 (0.98–1.05)
373 men, as compared with 28 of the 453 women increase)
(20 percent vs. 6 percent, P<0.001). Table 2 shows
the baseline characteristics of all patients. The men * CI denotes confidence interval.
were on average older than the women (51±14 years † Multivariate relative risks were calculated with adjustment for age; the pres-
ence or absence of a first symptomatic pulmonary embolism, factor V Leiden,
vs. 45±18 years, P<0.001), and they had a shorter factor II G20210A, elevated factor VIII levels, or elevated factor IX levels; and
duration of follow-up (33±29 months vs. 38±33 the duration of anticoagulation.
months, P=0.02). There was no significant differ-
ence between men and women with regard to the
presence of factor V Leiden (31 percent and 29 per-
cent, respectively), factor II G20210A (7 percent and Table 2. Baseline Characteristics of the 826 Patients According to Sex.*
8 percent, respectively), elevated levels of factor VIII Women Men
(8 percent and 10 percent, respectively), elevated Characteristic (N=453) (N=373) P Value
levels of factor IX (25 percent and 22 percent, respec- Age — yr 45±18 51±14 <0.001
tively), or the duration of anticoagulation (eight Site of thrombosis — no. (%) 0.09
months and nine months, respectively). According Distal veins of the leg 102 (23) 58 (16)
to Kaplan–Meier analysis, there was a clear diver- Proximal veins of the leg 150 (33) 135 (36)
Axillary veins 19 (4) 14 (4)
gence between the rate of recurrence among men Pulmonary embolism 182 (40) 166 (45)
and the rate among women throughout the period
Duration of anticoagulation — mo 9±12 8±11 0.76
of observation (P<0.001) (Fig. 1). At five years, the
Follow-up — mo 38±33 33±29 0.02
cumulative probability of recurrence was 30.7 per-
Factor V Leiden — no. (%) 130 (29) 115 (31) 0.5
cent (95 percent confidence interval, 23.8 to 37.6)
among men, as compared with 8.5 percent (95 per- Factor II G20210A — no. (%) 36 (8) 25 (7) 0.5
cent confidence interval, 5.0 to 12.0) among wom- Factor VIII ≥234 IU/dl — no. (%) 44 (10) 28 (8) 0.5
en. According to the univariate analysis, male sex Factor IX ≥138 IU/dl — no. (%) 101 (22) 95 (25) 0.3
conferred a relative risk of recurrence of 3.6 (95 per-
cent confidence interval, 2.3 to 5.5; P<0.001). After * Plus–minus values are means ±SD.
adjustments for age, the duration of anticoagula-
tion, and the presence or absence of a first sympto-
matic pulmonary embolism, factor V Leiden, factor 11.1) among these women and 4.3 percent (95 per-
II G20210A, and an elevated level of factor VIII or cent confidence interval, 0 to 10.1; P=0.8) among
IX, the risk of recurrence among men, as compared the 60 women in the same age groups in whom the
with women, was 3.6 (95 percent confidence inter- first event was idiopathic (Fig. 2). Among women
val, 2.3 to 5.8; P<0.001). who were taking oral contraceptives, the relative
A first venous thromboembolism occurred dur- risk of recurrence was 0.8 (95 percent confidence
ing oral-contraceptive use in 175 women. The cu- interval, 0.1 to 4.0; P=0.8) and remained unchanged
mulative probability of recurrence at five years was after adjustment for age and other possibly con-
5.9 percent (95 percent confidence interval, 0.6 to founding factors.
n engl j med 350;25 www.nejm.org june 17, 2004 2561
Downloaded from www.nejm.org by MAURO L. KAUFMANN MD on June 17, 2004.
Copyright © 2004 Massachusetts Medical Society. All rights reserved.
The new england journal of medicine
replacement therapy had a relative risk of recurrent
50
thromboembolism of 1.6 (95 percent confidence
Cumulative Probability of Recurrence (%) P<0.001 interval, 0.4 to 6.0; P=0.5). In the multivariate analy-
40 sis, the relative risk of recurrence was 3.4 times as
Men great among men as among women who had not
30 received hormone-replacement therapy (95 percent
confidence interval, 2.1 to 5.5; P<0.001).
20
discussion
Women
10
Our study of 826 patients shows that the patient’s
sex is a major determinant of recurrent venous
0 thromboembolism after an initial episode of spon-
0 1 2 3 4 5 6
taneous venous thromboembolism. The risk of
Years after Withdrawal of Oral Anticoagulants
recurrence was almost four times as great among
No. at Risk
Men 373 263 183 133 95 65 42
men as among women. Five years after the with-
Women 453 342 248 193 142 103 72 drawal of oral anticoagulation, the likelihood of re-
current venous thrombosis was 30.7 percent among
Figure 1. Kaplan–Meier Estimates of the Likelihood of Recurrent Venous men and only 8.5 percent among women (with an
Thromboembolism According to Sex.
upper 95 percent confidence bound of 12.0 percent).
The cumulative probability of recurrent venous thromboembolism was great-
The risk of recurrent venous thrombosis is great-
er among men than women (P<0.001 by the log-rank test).
ly increased among patients who have had more
than one thromboembolic episode15 and among pa-
tients who have cancer,6 the lupus anticoagulant,16
or a hereditary deficiency of an inhibitor of coag-
50 ulation.17 Patients with these risk factors receive
P=0.8 long-term secondary thromboprophylaxis and were
40 therefore not included in our study. Arterial disease
Cumulative Probability
of Recurrence (%)
or atrial fibrillation developed in a relatively large
30 number of patients during follow-up, and these pa-
tients thus began antithrombotic treatment. Given
20 the evidence that oral anticoagulation and aspirin
Oral-contraceptive use reduce the risk of venous thrombosis and pulmo-
10 No oral-contraceptive use
nary embolism,15,18-20 data on these patients were
censored at the time antithrombotic therapy was
0
0 1 2 3 4 5 6
initiated.
Years after Withdrawal of Anticoagulant Therapy
We previously reported that a high level of factor
VIII or factor IX or a first symptomatic pulmonary
No. at Risk
No oral-contraceptive use 60 49 34 27 18 13 9 embolism increases the risk of recurrent venous
Oral-contraceptive use 175 139 105 79 63 45 32 thromboembolism.21-23 In the current study, how-
ever, the proportion of patients with a high level of
Figure 2. Kaplan–Meier Estimates of the Likelihood of Recurrent Venous
factor VIII or IX was similar among men and wom-
Thromboembolism among Women Who Had Their First Venous Thrombosis
during Oral-Contraceptive Use, as Compared with Women in the Same Age en. In addition, the higher risk of recurrence among
Group Who Were Not Taking Oral Contraceptives at the Time of a First men remained unchanged after adjustment for an
Thrombotic Event. elevated level of factor VIII or IX and the presence
The cumulative probability of recurrent venous thromboembolism did not of factor V Leiden, factor II G20210A, and a first
differ significantly between the two groups (P=0.8 by the log-rank test). symptomatic pulmonary embolism.
Advanced age is an important risk factor for
venous thrombosis.3 The men in our study were on
Sixty-one women had their first venous thrombo- average six years older than the women. The differ-
embolism during hormone-replacement therapy. ence in age between the two groups, however, does
As compared with these women, the 108 women in not explain the higher rate of recurrent venous
the same age groups who did not use hormone- thromboembolism among men, since the likeli-
2562 n engl j med 350;25 www.nejm.org june 17 , 2004
Downloaded from www.nejm.org by MAURO L. KAUFMANN MD on June 17, 2004.
Copyright © 2004 Massachusetts Medical Society. All rights reserved.
the risk of recurrent venous thromboembolism in men and women
hood of recurrence among men and women re- the risk of recurrent venous thrombosis was more
mained unchanged after adjustment for age. than three times as great among men as among
Oral-contraceptive use increases the risk of ve- women in whom the initial episode of thrombosis
nous thrombosis.24 At the time of their first venous was not related to postmenopausal hormone use.
thrombosis, more than a third of the women were Why the women had a low risk of recurrent ve-
taking oral contraceptives, and they were advised nous thrombosis is unknown, but the finding may
to refrain from further oral contraceptive use. These have clinical implications. First, the sex-related dif-
women might have had a lower risk of recurrence ference in the risk of recurrence has to be taken into
— which could explain the low overall risk of re- account in the interpretation of past studies and the
currence among women — but the risk was low design of future trials. Second, the low risk among
among users and nonusers of oral contraception, women could influence decisions concerning the
and there was no significant difference between the duration of secondary thromboprophylaxis for
two groups. women, but independent confirmation of our find-
Hormone-replacement therapy more than dou- ings is required before they can be translated into
bles the risk of venous thrombosis.24 In our study, routine clinical practice. Third, future studies are
61 women had their first thrombotic event while warranted to determine whether there are risk fac-
they were taking postmenopausal hormones, but tors specific to men or protective factors specific to
the risk of recurrence among them did not differ women.
significantly from the risk among women who did Supported by grants from the Jubilaeumsfonds of the Öster-
reichische Nationalbank and the Medizinisch-Wissenschaftlicher
not use hormone-replacement therapy. Moreover, Fonds des Bürgermeisters der Bundeshauptstadt Wien.
after these women were excluded from the analysis, We are indebted to Dr. Marcus Muellner for expert statistical as-
sistance.
references
1. Anderson FA Jr, Wheeler HB, Goldberg 9. The PIOPED Investigators. Value of the lism in patients with familial thrombophilia.
RJ, et al. A population-based perspective of ventilation/perfusion scan in acute pulmo- Arch Intern Med 1997;157:2227-32.
the hospital incidence and case-fatality rates nary embolism: results of the Prospective In- 18. Kearon C, Gent M, Hirsh J, et al. A com-
of deep vein thrombosis and pulmonary em- vestigation of Pulmonary Embolism Diagno- parison of three months of anticoagulation
bolism: the Worcester DVT Study. Arch In- sis (PIOPED). JAMA 1990;263:2753-69. with extended anticoagulation for a first epi-
tern Med 1991;151:933-8. 10. Bertina RM, Koeleman BP, Koster T, et al. sode of idiopathic venous thromboembo-
2. Nordstrom M, Lindblad B, Bergqvist D, Mutation in blood coagulation factor V asso- lism. N Engl J Med 1999;340:901-7. [Erra-
Kjellstrom T. A prospective study of the inci- ciated with resistance to activated protein C. tum, N Engl J Med 1999;341:298.]
dence of deep-vein thrombosis within a de- Nature 1994;369:64-7. 19. Prevention of pulmonary embolism and
fined urban population. J Intern Med 1992; 11. Poort SR, Rosendaal FR, Reitsma PH, deep vein thrombosis with low dose aspirin:
232:155-60. Bertina RM. A common genetic variation in Pulmonary Embolism Prevention (PEP) trial.
3. White RH. The epidemiology of venous the 3'-untranslated region of the prothrom- Lancet 2000;355:1295-302.
thromboembolism. Circulation 2003;107: bin gene is associated with elevated plasma 20. Antiplatelet Trialists’ Collaboration. Col-
Suppl I:I-4–I-8. prothrombin levels and an increase in ve- laborative overview of randomised trials of
4. Oger E. Incidence of venous thrombo- nous thrombosis. Blood 1996;88:3698-703. antiplatelet therapy. III. Reduction in venous
embolism: a community-based study in 12. Brandt JT, Triplett DA, Alving B, Schar- thrombosis and pulmonary embolism by
western France. Thromb Haemost 2000;83: rer I. Criteria for the diagnosis of lupus anti- antiplatelet prophylaxis among surgical and
657-60. coagulants: an update. Thromb Haemost medical patients. BMJ 1994;308:235-46.
5. Silverstein MD, Heit JA, Mohr DN, 1995;74:1185-90. 21. Kyrle PA, Minar E, Hirschl M, et al. High
Petterson TM, O’Fallon WM, Melton J III. 13. Kalbfleisch JD, Prentice RL. The statisti- plasma levels of factor VIII and the risk of re-
Trends in the incidence of deep vein throm- cal analysis of failure time data. New York: current venous thromboembolism. N Engl J
bosis and pulmonary embolism: a 25-year John Wiley, 1980. Med 2000;343:457-62.
population-based study. Arch Intern Med 14. Kaplan EL, Meier P. Nonparametric esti- 22. Weltermann A, Eichinger S, Bialonczyk
1998;158:585-93. mation from incomplete observations. J Am C, et al. The risk of recurrent venous throm-
6. Prandoni P, Lensing AW, Cogo A, et al. Stat Assoc 1958;53:457-81. boembolism among patients with high fac-
The long-term clinical course of acute deep 15. Schulman S, Granqvist S, Holmström tor IX levels. J Thromb Haemost 2003;1:28-
venous thrombosis. Ann Intern Med 1996; M, et al. The duration of oral anticoagulant 32.
125:1-7. therapy after a second episode of venous 23. Eichinger S, Weltermann A, Minar E, et
7. Hansson PO, Sörbo J, Eriksson H. Re- thromboembolism. N Engl J Med 1997;336: al. Symptomatic pulmonary embolism and
current venous thromboembolism after deep 393-8. the risk of recurrent venous thromboembo-
vein thrombosis: incidence and risk factors. 16. Khamashta MA, Cuadrado MJ, Mujic F, lism. Arch Intern Med 2004;164:92-6.
Arch Intern Med 2000;160:769-74. Taub NA, Hunt BJ, Hughes GRV. The man- 24. Rosendaal FR, van Hylckama Vlieg A,
8. Baglin T, Luddington R, Brown K, Bag- agement of thrombosis in the antiphospho- Tanis BC, Helmerhorst FM. Estrogens, pro-
lin C. Incidence of recurrent venous throm- lipid-antibody syndrome. N Engl J Med 1995; gestogens and thrombosis. J Thromb Hae-
boembolism in relation to clinical and 332:993-7. most 2003;1:1371-80.
thrombophilic risk factors: prospective co- 17. van den Belt AG, Sanson BJ, Simioni P, Copyright © 2004 Massachusetts Medical Society.
hort study. Lancet 2003;362:523-6. et al. Recurrence of venous thromboembo-
n engl j med 350;25 www.nejm.org june 17, 2004 2563
Downloaded from www.nejm.org by MAURO L. KAUFMANN MD on June 17, 2004.
Copyright © 2004 Massachusetts Medical Society. All rights reserved.
You might also like
- 10 1038@nrdp20156Document17 pages10 1038@nrdp20156Desi DwiNo ratings yet
- Blom JW - Malignancies, Prothrombotic Mutations, and The Risk of Venous ThrombosisDocument8 pagesBlom JW - Malignancies, Prothrombotic Mutations, and The Risk of Venous ThrombosisFarid RakhmanNo ratings yet
- Helen K. Chew - Incidence of Venous Thromboembolism and Its Effect On SurvivalDocument7 pagesHelen K. Chew - Incidence of Venous Thromboembolism and Its Effect On SurvivalFarid RakhmanNo ratings yet
- Embolismo Pulmonar NejmDocument3 pagesEmbolismo Pulmonar NejmSaidNo ratings yet
- Venous Thrombotic Recurrence After Cerebral Venous ThrombosisDocument7 pagesVenous Thrombotic Recurrence After Cerebral Venous ThrombosisMartina Alarcon AcevedoNo ratings yet
- Thrombosis and Acute LeukemiaDocument6 pagesThrombosis and Acute Leukemiaannisa edwarNo ratings yet
- Caso TEP Bibliografia Bis 2023Document7 pagesCaso TEP Bibliografia Bis 2023Viviana MorenoNo ratings yet
- Study 1Document6 pagesStudy 1suhamkky8No ratings yet
- Meissner2007Document29 pagesMeissner2007dewiNo ratings yet
- Khorana AA - Thromboembolism in Hospitalized Neutropenic Cancer PatientsDocument8 pagesKhorana AA - Thromboembolism in Hospitalized Neutropenic Cancer PatientsFarid RakhmanNo ratings yet
- Blood 742304Document9 pagesBlood 742304Francieudo SampaioNo ratings yet
- Aspirina Después de Fractura Art Ing 2023Document4 pagesAspirina Después de Fractura Art Ing 2023roman rodriguezNo ratings yet
- 1 s2.0 S0006497120687596 MainDocument5 pages1 s2.0 S0006497120687596 MainnadaNo ratings yet
- 3144.full MoyamoyaDocument8 pages3144.full MoyamoyaDarren ZytkiewiczNo ratings yet
- JCTH 7 154Document11 pagesJCTH 7 154Andreea AlexandruNo ratings yet
- TEP Systemic Thrombolysis For Pulmonary Embolism Evidence, Patient Selection, and Protocols For ManagementDocument10 pagesTEP Systemic Thrombolysis For Pulmonary Embolism Evidence, Patient Selection, and Protocols For Managementbenitez1228No ratings yet
- DVT in India PDFDocument6 pagesDVT in India PDFKarthik KoneruNo ratings yet
- Jama Neal 2023 Ed 230070 1696973944.14124Document2 pagesJama Neal 2023 Ed 230070 1696973944.14124Luz Elena ValderramaNo ratings yet
- Postpartum Hemorrhage-Epidemiology, Risk Factors, and CausesDocument13 pagesPostpartum Hemorrhage-Epidemiology, Risk Factors, and CausesNilfacio PradoNo ratings yet
- Plueral Effusion and Ovarian CancerDocument5 pagesPlueral Effusion and Ovarian CancerAthenaeum Scientific PublishersNo ratings yet
- Management of Contraception in Adolescent Females With Hormone-Related Venous ThromboembolismDocument5 pagesManagement of Contraception in Adolescent Females With Hormone-Related Venous ThromboembolismInggrit DirgantariNo ratings yet
- Abnormaluterinebleeding Inyoungwomenwithblood Disorders: Kathryn E. Dickerson,, Neethu M. Menon,, Ayesha ZiaDocument18 pagesAbnormaluterinebleeding Inyoungwomenwithblood Disorders: Kathryn E. Dickerson,, Neethu M. Menon,, Ayesha ZiaSalvador ArredondoNo ratings yet
- VTE in Unusual Sites BJH - 2012Document11 pagesVTE in Unusual Sites BJH - 2012Chenuri Annamarie RanasingheNo ratings yet
- How We Diagnose and Treat Deep Vein Thrombosis.: Author InformationDocument18 pagesHow We Diagnose and Treat Deep Vein Thrombosis.: Author InformationligitafitranandaNo ratings yet
- Thromboprophylaxis after Extremity Fracture — Time for Aspirin? (2023)Document2 pagesThromboprophylaxis after Extremity Fracture — Time for Aspirin? (2023)ericdgNo ratings yet
- 01-16 Optimal Therapy For Unstable Pulmonar EmbolismDocument4 pages01-16 Optimal Therapy For Unstable Pulmonar EmbolismLesly Peinado TorresNo ratings yet
- Clinical Considerations in Recurrent Miscarriage: Journal ofDocument5 pagesClinical Considerations in Recurrent Miscarriage: Journal ofElena VisterniceanNo ratings yet
- Pregnancy, The Postpartum Period and Prothrombotic Defects: Risk of Venous Thrombosis in The MEGA StudyDocument6 pagesPregnancy, The Postpartum Period and Prothrombotic Defects: Risk of Venous Thrombosis in The MEGA StudyAlfa FebriandaNo ratings yet
- 1 s2.0 S2376060524000063 MainDocument4 pages1 s2.0 S2376060524000063 Mainifte5104385No ratings yet
- Venous Thromboembolism: What To Do After Anticoagulation Is StartedDocument10 pagesVenous Thromboembolism: What To Do After Anticoagulation Is StartedJuanMa Correa SanabriaNo ratings yet
- Highlow StudyDocument7 pagesHighlow StudySilvia IzvoranuNo ratings yet
- Evidence-Based Therapies For Pharmacologic Prevention and Treatment of Acute Deep Vein Thrombosis And  Pulmonary EmbolismDocument15 pagesEvidence-Based Therapies For Pharmacologic Prevention and Treatment of Acute Deep Vein Thrombosis And  Pulmonary EmbolismBolivar IseaNo ratings yet
- Jurnal 15Document5 pagesJurnal 15rifkipspdNo ratings yet
- A Comparison of Enoxaparin With Placebo For The Prevention ofDocument8 pagesA Comparison of Enoxaparin With Placebo For The Prevention ofjose luisNo ratings yet
- Mulatu Et Al 2020 Deep Venous Thrombosis Recurrence and Its Predictors at Selected Tertiary Hospitals in Ethiopia ADocument14 pagesMulatu Et Al 2020 Deep Venous Thrombosis Recurrence and Its Predictors at Selected Tertiary Hospitals in Ethiopia Amulatbirhanu100No ratings yet
- Schnatz 2011Document9 pagesSchnatz 2011Benjamin SiglicNo ratings yet
- GastroprofilaxisDocument13 pagesGastroprofilaxisDaniel Alejandro Lecaros BarríaNo ratings yet
- Tep 1Document16 pagesTep 1Yarlin MontoyaNo ratings yet
- Heit2008Document6 pagesHeit2008dewiNo ratings yet
- Dose-Adjusted Enoxaparin Thromboprophylaxis in Hospitalized CancerDocument7 pagesDose-Adjusted Enoxaparin Thromboprophylaxis in Hospitalized CancerAnonymous 9dVZCnTXSNo ratings yet
- Circulation 2014 Piazza 283 7Document6 pagesCirculation 2014 Piazza 283 7arthoclaseNo ratings yet
- Khorana AA - Frequency, Risk Factors, and Trends For Venous Thromboembolism Among Hospitalized Cancer PatientsDocument8 pagesKhorana AA - Frequency, Risk Factors, and Trends For Venous Thromboembolism Among Hospitalized Cancer PatientsFarid RakhmanNo ratings yet
- Caos PaperDocument6 pagesCaos PaperMauricio Lopez MejiaNo ratings yet
- 19 TEP Tak2019Document12 pages19 TEP Tak2019Juan Carlos Uribe CaballeroNo ratings yet
- Nej M 199603213341203Document4 pagesNej M 199603213341203Krinta AlisaNo ratings yet
- Seminar: Faizan Khan, Tobias Tritschler, Susan R Kahn, Marc A RodgerDocument14 pagesSeminar: Faizan Khan, Tobias Tritschler, Susan R Kahn, Marc A RodgerJuan Camilo Morales TabordaNo ratings yet
- Inpatient Inherited Thrombophilia Testing: Choosing Wisely: Things We Do For No ReasonDocument4 pagesInpatient Inherited Thrombophilia Testing: Choosing Wisely: Things We Do For No Reasonkishore kumar meelNo ratings yet
- Risk of ThrombosisDocument13 pagesRisk of ThrombosisNataliaHermosilloNo ratings yet
- Streptokinase in The Treatment of Pleural Controlled Trial of IntrapleuralDocument7 pagesStreptokinase in The Treatment of Pleural Controlled Trial of IntrapleuraltomgasoneNo ratings yet
- Assessing Hypercoagulability and VTE Risk Using Thromboelastography and Khorana Score in Women With Cancers Receiving Chemotherapy 2024Document9 pagesAssessing Hypercoagulability and VTE Risk Using Thromboelastography and Khorana Score in Women With Cancers Receiving Chemotherapy 2024myqrwd464kNo ratings yet
- Leunase and TrombolismDocument12 pagesLeunase and TrombolismSanta UlinaNo ratings yet
- The Coagulopathy of Cancer: ReviewDocument7 pagesThe Coagulopathy of Cancer: ReviewlucyishakNo ratings yet
- Malignant Mesothelioma Presenting With Unexplained Recurrent Pleurisy EpisodesDocument4 pagesMalignant Mesothelioma Presenting With Unexplained Recurrent Pleurisy EpisodesNurul NingrumNo ratings yet
- Jurnal 9Document9 pagesJurnal 9Atikah AbayNo ratings yet
- New England Journal Medicine: The ofDocument9 pagesNew England Journal Medicine: The ofHila AmaliaNo ratings yet
- Seminar: PathophysiologyDocument12 pagesSeminar: PathophysiologyBeni KurniawanNo ratings yet
- Hypercoagulable and TestingDocument14 pagesHypercoagulable and TestingSri HartiniNo ratings yet
- Our Experience With Bicytopenia in Patients Treated at The Ankara Hospital Pediatric ClinicDocument5 pagesOur Experience With Bicytopenia in Patients Treated at The Ankara Hospital Pediatric ClinicRonny DoankNo ratings yet
- Thrombophilia-Associated Pregnancy Wastage: Modern TrendsDocument10 pagesThrombophilia-Associated Pregnancy Wastage: Modern TrendspogimudaNo ratings yet
- Anatomy Muscular System BrochureDocument2 pagesAnatomy Muscular System Brochureapi-462608096No ratings yet
- CVS - BloodDocument30 pagesCVS - BloodQuimson KennethNo ratings yet
- PMLS2 EsentialsDocument38 pagesPMLS2 EsentialsKen Novero100% (1)
- HematologyDocument2 pagesHematologyMohammed Al-RahmaweeNo ratings yet
- hssb2101t SecquizDocument2 pageshssb2101t Secquizfhhgghhg hggghgNo ratings yet
- Normal Laboratory ValuesDocument40 pagesNormal Laboratory ValuesPrincess Nasima M. Usngan100% (1)
- Untitled4 PDFDocument13 pagesUntitled4 PDFElizabeth LeonNo ratings yet
- Anemia in TropicsDocument7 pagesAnemia in TropicsAsnaafii BantiiNo ratings yet
- 3 PracticalDocument47 pages3 PracticalT NNo ratings yet
- CBCDocument3 pagesCBCDicky DamaraNo ratings yet
- Hemostasis - TrombositDocument28 pagesHemostasis - TrombositNovi AndrianiNo ratings yet
- Invitro Anticoagulant Activity of Emblica Officinalis Leaf Extract On Normal Healthy Blood PlasmaDocument4 pagesInvitro Anticoagulant Activity of Emblica Officinalis Leaf Extract On Normal Healthy Blood PlasmaInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- CBCDocument1 pageCBCAhmed GaberNo ratings yet
- Alveolar BoneDocument8 pagesAlveolar BoneClarisse MendozaNo ratings yet
- Itp 210530123628Document26 pagesItp 210530123628Sakthi DeviNo ratings yet
- Blood TransfusionDocument5 pagesBlood Transfusionrupali gahalianNo ratings yet
- Ruby BrochureDocument8 pagesRuby BrochureNalan SezerNo ratings yet
- Memo Re Blood donationBJMPDocument1 pageMemo Re Blood donationBJMPptsievccdNo ratings yet
- Tissue Structure & FunctionDocument74 pagesTissue Structure & FunctionTaufiqurrahman Sidqi100% (1)
- SGD Case: Hematology Weakness: Dizziness: Anorexia: Vomit: Numbness: TinglingingDocument10 pagesSGD Case: Hematology Weakness: Dizziness: Anorexia: Vomit: Numbness: TinglingingEveryday FundayNo ratings yet
- Blood TransfusionDocument21 pagesBlood TransfusionAnup GouravNo ratings yet
- Physical Characteristics: C. PlateletsDocument6 pagesPhysical Characteristics: C. PlateletsGwyneth Marie DayaganNo ratings yet
- G5 - Bones and MusclesDocument4 pagesG5 - Bones and MusclesrababNo ratings yet
- Kell Blood Group System: Muhammad Asif Zeb Lecturer Hematology Ipms-Kmu PeshawarDocument11 pagesKell Blood Group System: Muhammad Asif Zeb Lecturer Hematology Ipms-Kmu PeshawarMaaz KhanNo ratings yet
- HEMOSTASISDocument12 pagesHEMOSTASISRyan PedregosaNo ratings yet
- (K5-1) Kuliah Anemia Hemolitik (Dr. Riza)Document21 pages(K5-1) Kuliah Anemia Hemolitik (Dr. Riza)Puti Callistha IchsanNo ratings yet
- Hemorrhagic Shock (Anestesi)Document44 pagesHemorrhagic Shock (Anestesi)Dwi Meutia IndriatiNo ratings yet
- 13 OCTOBER, 2021 Wednesday Biology Transport SystemDocument12 pages13 OCTOBER, 2021 Wednesday Biology Transport SystemOyasor Ikhapo AnthonyNo ratings yet
- Skeletal Guided NotesDocument4 pagesSkeletal Guided Notesapi-591284844No ratings yet
- ThrombocytopeniaDocument49 pagesThrombocytopeniaMaria EnjelinaNo ratings yet