Professional Documents
Culture Documents
De37 PDF
De37 PDF
Uploaded by
Eka JuliantaraOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
De37 PDF
De37 PDF
Uploaded by
Eka JuliantaraCopyright:
Available Formats
Diabetic Neuropathy and Diabetic Foot
The Diabetic Foot—Imaging Options and Considerations
a report by
D a k s h i n G a n g a d h a ra m u r t h y , M B B S , M P H , Pe r r y H o r w i c h , M D and R o b e r t L G re e n m a n , P h D
Department of Radiology, Beth Israel Deaconess Medical Center, and Harvard Medical School
DOI: 10.17925/USE.2007.00.2.75
Patients with diabetes may present with an array of foot disorders that periosteal reaction and post-traumatic changes can be non-specific. For
include, but are not limited to, neuropathy, ulceration, and osteomyelitis. example, the appearance of Charcot osteoarthropathy can be mistakenly
Ischemia and infection are common clinical concerns as either, or both, may identified as osteomyelitis on radiographs.6
be involved in the pathogenesis of these disorders. Management choices
can be difficult to make and diagnostic imaging is often sought to help Radionucleotide Scans
clarify the clinical picture. The imaging options available all have strengths Four radionucleotide studies are discussed here:
and weaknesses in terms of their clinical relevance. A common problem
encountered with imaging is distinguishing inflammation that is due to • technetium Tc-99m (99mTc)-labeled diphosphonate bone scanning;
trauma—e.g. surgical, mechanical or Charcot arthropathy—from soft-tissue • indium In-111 white blood cell (WBC);
or osseous infection. This article reviews the most common imaging options • non-specific human immunoglobulin (HIG) labeled with Tc-99; and
available to clinicians and summarizes the benefits and drawbacks of each. • 18-flourodeoxyglucose positron emission tomography (18-FDG-PET).
No single imaging modality can answer all the clinical questions that arise in
the setting of the diabetic foot, but knowing the features of the imaging
choices available to you may help answer the most pressing questions. Dakshin Gangadharamurthy, MBBS, MPH, is a Research Fellow
in the Division of Magnetic Resonance Research at Beth Israel
Deaconess Medical Center/Harvard Medical School in Boston.
Pathogenesis of Ischemia and Infection His research interests include magnetic resonance imaging of
While foot ulcers are the most common complication in the diabetic foot, atherosclerotic plaque and non-invasive assessment of
cardiovascular lesions. He is a member of the American
infections rank a close second.1 Sensory neuropathy in the distal regions of Roentgen Ray Society (ARRS). Dr Gangadharamurthy received
the extremities predisposes many diabetics to traumatic insults that can lead his MPH from Johns Hopkins University, Baltimore, and his
to skin breakdown, ulceration, and infection. Impaired perfusion due to MBBS from Bangalore Medical College, Bangalore, India.
peripheral vascular disease and microvascular abnormalities reduces the
Perry Horwich, MD, is an Instructor of Radiology at Harvard
patient’s capacity to heal wounds and recover from infection.2 In the
University Medical School and a Staff Radiologist in the
diabetic foot, infected skin ulcers, the development of cellulitis, Musculoskeletal Section at the Beth Israel Deaconess Medical
osteomyelitis, and abscess are major sources of morbidity. Center in Boston. His research interests include image processing
and feature extraction. He is a co-investigator for ongoing
research studies that focus on the assessment of the diabetic
The management of patients with diabetic foot disorders can vary foot by functional metabolic magnetic resonance imaging.
substantially depending on the presence and extent of infection, necrosis, Dr Horwich is a member of the International Society of Magnetic
Resonance in Medicine (ISMRM) and the Radiological Society of
and osteomyelitis.3 Imaging of the diabetic foot may provide information
North America (RSNA). He completed a residency in radiology at Beth Israel Medical Center, New
that can aid the clinician in making patient management decisions. York, and a fellowship in magnetic resonance imaging at Beth Israel Deaconess Medical Center in
Diagnostic imaging procedures may also provide information that helps Boston. He received his BSc in chemistry from Cornell College and his MD from Rush University
Medical College.
guide surgical planning.
Radiographs Robert L Greenman, PhD, is an Instructor of Radiology at
Harvard University Medical School and a scientist in the Division
This basic modality may be indicated when bone involvement is suspected. of Magnetic Resonance Imaging Research at the Beth Israel
Radiographs can detect cortical fragmentation, osteomyelitis, fractures, Deaconess Medical Center in Boston. His research interests
arterial calcifications, and soft-tissue gas and articular deformities, including include the non-invasive assessment of metabolism in skeletal
muscle and the myocardium in disease states and magnetic
Charcot osteoarthropathy (see Figure 1).1,4 While radiography is often used resonance imaging (MRI) of atherosclerotic plaques. He is the
initially, an early diagnosis of osteomyelitis may be difficult to make as principal investigator for ongoing research studies that focus on
changes on radiographs are often subtle, or absent, in the early stages of the the assessment of the diabetic foot by functional metabolic
MRI. Dr Greenman is a member of the International Society of Magnetic Resonance in Medicine
disease process.5 Thus, this imaging modality is useful for detecting changes (ISMRM) and the American Diabetes Association (ADA). He received his BSc in physics from the
associated with the later stages of osseous infection (typically two or more State University of New York, an MSc in electrical engineering from Cornell University, and a PhD
weeks from onset) (see Figure 2).6 This limitation is partly responsible for the in biochemistry and molecular biophysics from the University of Pennsylvania.
modality having low sensitivity in the detection of osteomyelitis. While E: rgreenma@bidmc.harvard.edu
studies show radiographs typically have a higher specificity than sensitivity,
© TOUCH BRIEFINGS 2007 75
Diabetic Neuropathy and Diabetic Foot
Figure 1: Radionucleotide Studies an increase in bone turnover—such as neuropathic osteoarthropathy,
fracture, or surgery—may produce abnormal uptake, making these
A entities difficult to distinguish from osteomyelitus (see Figure 2).8,9
However, its high sensitivity contributes to a high negative predictive
value, and a negative bone scan typically provides convincing evidence for
ruling out infection.1
Indium In-111 White Blood Cell
In-111-labeled WBC scintigraphy combined with bone scintigraphy can
improve the specificity for osteomyelitus beyond that of bone
scintigraphy alone.10 Drawbacks associated with this option are that the
In-111-labeled WBC scintigraphy is expensive, is not readily available,
and involves time-consuming preparation of labeled WBCs,11 which may
take up to 48 hours.8,12,13
99 Tc Human Immunoglobulin
This technique has the potential to differentiate cellulitis from
B C
osteomyelitis.17 The disadvantage of HIG is its non-specific uptake in both
infection and non-infectious inflammation;14,18,19 also, recent trauma may
interfere with a diagnosis of infection in the diabetic foot.20 Similar to
99Tc WBC scans, 99Tc HIG scans are associated with false-positive results
in conditions such as rheumatoid arthritis (RA), osteoarthropathy, and
healing fracture.17
A: Lateral radiograph of the foot shows mid-foot osseous disorganization and destruction (white
arrow), typical of Charcot arthropathy. Arrow heads point out atherosclerotic arterial Flourodeoxyglucose Positron Emission Tomography
calcifications. FDG-PET imaging has the advantage of relatively short preparation and
B: 99mTc bone scan reveals corresponding abnormal uptake of radiotracer. This appearance can
be seen with either osseous fracture or osteomyelitis duration, and higher target-to-background contrast ratio than other
C: In-111 white blood cell scan depicts corresponding abnormal uptake of radiotracer, techniques of nuclear medicine.21 Despite having high sensitivity for
confirming the diagnosis of osteomyelitis.
imaging areas of active infection, PET may not be as specific in identifying
areas of abnormal tracer accumulation, which may be partly attributed to
Figure 2: Foot Radiographs
low spatial resolution. This limitation can be mitigated by combining PET
A B with computed tomography (PET/CT), which improves diagnostic accuracy
by allowing the co-registration of abnormal 18F-FDG uptake with specific
anatomical structures.22
Studies using the combined modalities of PET and CT have demonstrated
the ability to accurately differentiate between soft-tissue infection and
osteomyelitis. 22 The hybrid PET/CT technique provides accurate
registration of metabolic and structural data in a single examination,
resulting in improved diagnosis and localization of infection. The PET
component uses 18F-FDG as a tracer, which accumulates at the sites of
both infection and inflammation.21,23,24
Radionucleotide Scans—General Limitations
There are several general limitations of radionucleotide techniques. Poor
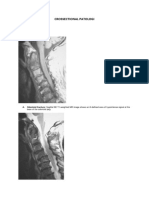
Compared with image A, image B shows interval cortical destruction of the first metatarsal spatial resolution may make it difficult to identify osetomyelitis when it is
head (black arrows) in this patient with osteomyelitis and septic arthritis of the first metatarsal–
adjacent to sites of soft-tissue infection.8,13,25 False-negative results, in the
phalangeal joint. The arrow heads in image A identify atherosclerotic arterial calcifications, a
common finding in patients with diabetes. setting of peripheral vascular disease, are attributable to diminished
regional delivery of isotope. The negative predictive value may thus be
Nuclear medicine techniques, such as 99mTc-labeled diphosphonate bone limited in the setting of local ischemia. Finally, these examinations
scanning and indium In-111 WBC scanning, are capable of detecting are expensive.4,25,26
changes of osteomyelitis earlier than plain radiographs.
Computed Tomography
99m Tc-labeled Diphosphonate Bone Scanning Much like radiographs, CT uses X-rays to generate an image. CT, while
Multiphase bone scintigraphy has very high sensitivity for diagnosing more sensitive than radiographs for detecting osteomyelitis, may still fail
osteomyelitis, but suffers from low specificity.7 Any condition that causes to detect osteomyelitis in the early stage of disease. Additionally, CT may
76 US ENDOCRINE DISEASE 2007
The Diabetic Foot—Imaging Options and Considerations
not be able to distinguish neuropathic osteoarthropathy from the Figure 3: Magnetic Resonance Imaging of the Foot
sequelae of chronic infection.
A B
Contrast-enhanced CT can detect soft-tissue and osseous abscess
formation. The discovery of an abscess may alter clinical management, as
treatment for abscess is typically surgical debridement. CT lacks
sensitivity for differentiating changes associated with infection, edema,
fibrosis, and granulation tissue.27 The risk of use of iodinated contrast in
diabetic patients may not be a trivial one as chronic renal insufficiency is
commonly a comorbidity in patients with diabetes.
Magnetic Resonance Imaging
The wide range of tissue contrast that is integral to magnetic resonance
imaging (MRI) makes it well suited for visualizing the extent of soft-tissue
A: Sagital T1-weighted magnetic resonance image of the foot shows a skin ulcer overlying the
infection as well as bone infection (see Figure 3). MRI is used, with posterior calcaneous (white arrow).
increasing frequency, to assess the complications associated with the B: Sagital fluid-sensitive image reveals high signal edema (white arrow heads) throughout the
calcaneous, representing the inflammatory changes seen with osteomyelitis.
diabetic foot.1,28 Due to the high spatial resolution that is achievable and its
ability to accurately evaluate the extent of inflammation, it is usually
preferred over CT to investigate the presence of osteomyelitis.1 The ability quantify the burden of occlusive disease and can identify targets for
of MRI to visualize the extent of osseous and soft-tissue infection also vascular bypass.
facilitates its use in pre-operative planning.28
When prescribing imaging studies that involve iodinated contrast materials
Gadolinium (Gd)-based contrast agents improve the detection of soft- for patients with diabetes, the risk of contrast-induced nephropathy (CIN)
tissue infection and help to determine its extent. It is also used to should be considered. Of all causes of acute renal failure (ARF) among all
improve the delineation of necrotic tissues and sinus tracts and the hospitalized patients, CIN ranks third.31,32
detection of abscesses. The excellent contrast characteristics of MRI and
the ability to visualize infection in multiple planes with good anatomical Digital Subtraction Angiography
detail using contrast enhancement makes MRI the preferred modality for As its name implies, digital subtraction angiography (DSA) is performed by
evaluating for the presence of abscess. Recently, a serious adverse subtracting a pre-injection image from a contrast-enhanced post-injection
reaction called nephrogenic systemic fibrosis (NSF) has been observed. image. This process removes distracting background anatomical structures.
NSF has been associated with the administration of MRI contrast agents The resulting angiograph has high contrast resolution compared with
and patients with renal dysfunction.29 NSF is characterized by widespread standard non-subtracted angiography, and allows for the use of lower
tissue fibrosis. Since renal dysfunction is a common complication of concentrations of contrast materials relative to other vascular imaging
diabetes, this relative contraindication for Gd-enhanced MRI may methods. DSA allows for the visualization of patent vessels beyond a
disqualify a number of patients. At the time of this publication, decision proximal occlusion better than non-subtracted angiography, which may
paradigms addressing who is and who is not a good candidate for make DSA better suited for evaluating diabetic patients with chronic severe
Gd-enhanced MRI are institution-specific and evolving. resting ischemia.32
While MRI has high sensitivity for identifying inflammation, it too can lack DSA is still considered to be the gold standard imaging study for assessing
specificity. For example, a patient may present with an ulcer that is in close peripheral artery disease.32,33 DSA is an invasive technique that requires the
proximity to a broken bone associated with Charcot osteoarthropathy. In insertion and direction of an intra-vascular catheter to the site that is to be
this hypothetical—yet commonly seen—case, the inflammation associated assessed, where injection of a radio-opaque contrast agent is made. The
with the skin ulcer may overlap with the inflammation that surrounds the procedure therefore involves some risk to the patient, including hemorrhage
Charcot-related osseous fracture. In such a case, it can be difficult to identify at the site of vascular puncture, distal embolization, and mural
the boundaries of the inflammation associated with infection from the dissection.30,32 One limitation of aniography occurs when multiple stenoses
inflammation associated with trauma. are present, as is common in diabetes. In such cases, small peripheral vessels
of the foot may not be seen in DSA.33
While MRI has high diagnostic accuracy for delineating both bone and soft-
tissue infections, the Infectious Disease Society of America (IDSA) and the Duplex Ultrasound
Clinical Practice Guideline Diabetes Panel4 of the American College of Foot Duplex ultrasound (DSU) can depict vascular flow with directional and
and Ankle Surgeons (ACFAS)1 recommends radiographs as the initial velocity-related information. This information can be superimposed on the
imaging study when infection is suspected. standard grayscale ultrasound image using color and is sometimes referred
to as ‘color Doppler.’ Longitudinal and cross-sectional depiction of medium
Angiography and large arteries and veins is possible. DSU is a non-invasive method of
Diabetic patients are at significantly higher risk of developing peripheral documenting artery morphology and vascular flow.30 DSU is not as sensitive
vascular disease than the general population.1,30 Angiography may help to as DSA in depicting small vessels with slow flow.
US ENDOCRINE DISEASE 2007 77
Diabetic Neuropathy and Diabetic Foot
Computed Tomography Angiography disease (PVD) in chronic resting ischemia than conventional angiography,
CT angiography (CTA) is beginning to be used more frequently to assess since it has been shown to visualize distal vessels in the presence of
peripheral vascular disease as it is less invasive than DSA and can provide numerous stenoses and occlusions.33 Thus, MRA may identify suitable
3D images. Multidetector CT (MDCT) is a recent technological advance target vessels for pedal bypass surgery.33
in CTA that can decrease acquisition time and increase spatial
resolution. This method can produce high-spatial-resolution images of Summary and Conclusions
the entire extremity in several seconds.33 MDCT does use iodine-based Many studies describing imaging of the diabetic foot provide assessments
contrast agents and, as with the use of all such contrast agents, there is of the specificity, sensitivity, positive predictive value (PPV), and negative
a risk of CIN. predictive value (NPV) for investigating specific foot disorders. The
published values of these measures vary substantially among studies. These
Magnetic Resonance Angiography measures are highly dependent on the circumstances that are related to
MRI scanners can be used to perform MR angiography (MRA). While MRI the individual studies. The patient population, whether or not patients
provides anatomical detail of the soft tissue and bones, MRA also allows have peripheral vascular disease, the stage of the specific disorder, and
the visualization of flowing blood within the vessels.30 Both 2D and 3D other factors all affect the cited quantified results of these imaging studies.
MRA techniques are available. One method, known as time-of-flight, In particular, prevalence of disease in a given study population can widely
allows for visualization of blood flow without the use of an injected skew reported values for PPV and NPV.
contrast agent. Gd-enhanced MRA is a more sensitive method of
demonstrating blood flow that is not perpendicular to the plane of The imaging modalities described in this article vary substantially in cost.
imaging. As previously mentioned in the section on MRI, it has become As indicated, none of the imaging modalities that have been discussed
important to screen patients for renal insufficiency, which may disqualify here is 100% sensitive or specific for diagnosing or ruling out infection.
them for Gd-enhanced MRA studies. However, of all of the techniques MRI typically has the best sensitivity,
PPV, and NPV compared with other modalities in the detection of
MRA has been recognized as a useful non-invasive tool for analyzing the osteomyelitis. It may be able to differentiate bone infection from soft-
peripheral arteries in the diabetic foot, particularly for the non-healing tissue infection and has the potential to detect both osseous and
ulcer.34 MRA may be better suited for evaluating peripheral vascular soft-tissue abscess.35 ■
1. Frykberg RG, Zgonis T, Armstrong DG, et al., Diabetic foot 14. Datz FL, Anderson CA, Ahluwalia R, The efficacy of Indium the foot in diabetic patients: value of 111In-leukocyte
disorders. A clinical practice guideline (2006 revision), J Foot 111polyclonal IgG for the detection of infection and scintigraphy, Am J Roentgenol, 1991;157:527–31.
Ankle Surg, 2006;45:S1–66. inflammation, Semin Nucl Med, 1994;35:74. 26. Shults DW, Hunter GC, McIntyre KE, Parent FN, Value of
2. Zlatkin Z, Pathra M, Sartoris D, Resnick D, The Diabetic Foot, 15. Rubin RH, Fischman AJ, The use of radiolabelled non-specific radiographs and bone scans in determining the need for
Radiol Clin North Am, 1987;25:1095–1105. immunoglobulin in the detection of focal inflammation, Semin therapy in diabetic patients with foot ulcers, Am J Surg,
3. Ledermann HP, Morrison WB, Schweitzer ME, Pedal abscesses Nucl Med, 1994;24. 1989;158:525–30.
in patients suspected of having pedal osteomyelitis: analysis 16. Sella EJ, Grosser DM, Imaging modalities of the diabetic foot, 27. Tomas MB, Patel M, Marwin SE, Palestro CJ, The diabetic foot,
with MR imaging, Radiology, 2002;224:649–55. Clin Podiatr Med Surg, 2003;20:729–40. Br J Radiol, 2000;73:443–50.
4. Lipsky BA, Berendt AR, Embil J, De Lalla F, Diagnosing and 17. Unal SN, Birinci H, Baktiroglu S, Cantez S, Comparison of Tc- 28. Morrison WB, Ledermann HP, Work-up of the diabetic foot,
treating diabetic foot infections, Diabetes Metab Res Rev, 99m methylene diphosphonate, Tc-99m human immune Radiol Clin North Am, 2002;40:1171–92.
2004;20(Suppl. 1):S56–64. globulin, and Tc-99m-labeled white blood cell scintigraphy in 29. Thomsen HS, Nephrogenic systemic fibrosis: A serious late
5. Marcus CD, Ladam-Marcus VJ, Leone J, et al., MR imaging of the diabetic foot, Clin Nucl Med, 2001;26:1016–21. adverse reaction to gadodiamide, Eur Radiol, 2006;16:2619–21.
osteomyelitis and neuropathic osteoarthropathy in the feet of 18. Demirkol MO, Adalet I, Unal SN, et al., 99Tc(m)-polyclonal IgG 30. Dyet JF, Nicholson AA, Ettles DF, Vascular imaging and
diabetics, Radiographics, 1996;16:1337–48. scintigraphy in the detection of infected hip and knee intervention in peripheral arteries in the diabetic patient,
6. Kapoor A, Page S, Lavalley M, et al., Magnetic resonance prostheses, Nucl Med Commun, 1997;18:543–8. Diabetes Metab Res Rev, 2000;16(Suppl. 1):S16–22.
imaging for diagnosing foot osteomyelitis: a meta-analysis, 19. Palermo F, Boccaletto F, Paolin A, et al., Comparison of 31. Kramer C, Budoff M, Fayad Z, et al., ACCF/AHA 2007 clinical
Arch Intern Med, 2007;167:125–32. technetium-99m-MDP, technetium-99m-WBC and technetium- competence statement on vascular imaging with computed
7. Palestro CJ, Torres MA, Radionuclide imaging in orthopaedic 99m-HIG in musculoskeletal inflammation, J Nucl Med, tomography and magnetic resonance, Circulation, 2007;116:
infections, Semin Nucl Med, 1997;27:334. 1998;39:516–21. 1318–35.
8. Seabold JE, Flickinger FW, Kao SC, et al., Indium-111- 20. Oyen WJ, Netten PM, Lemmens JA, et al., Evaluation of 32. Gates J, Hartnell GG, Optimized diagnostic angiography in
leukocyte/technetium-99m-MDP bone and magnetic resonance infectious diabetic foot complications with indium-111-labeled high-risk patients with severe peripheral vascular disease,
imaging: difficulty of diagnosing osteomyelitis in patients with human nonspecific immunoglobulin G, J Nucl Med, 1992;33: Radiographics, 2000;20:121–33.
neuropathic osteoarthropathy, J Nucl Med, 1990;31:549–56. 1330–36. 33. Lapeyre M, Kobeiter H, Desgranges P, et al., Assessment of
9. Elgazzar HA, Dayem AJC, Multimodality of osteomyelitis, Eur J 21. Bleeker-Rovers CP, de Kleijn EM, Corstens FH, et al., Clinical critical limb ischemia in patients with diabetes: comparison of
Nucl Med, 1995;22:1043–63. value of FDG PET in patients with fever of unknown origin and MR angiography and digital subtraction angiography, Am J
10. Schauwecker DS, Park HM, Burt RW, Combined bone patients suspected of focal infection or inflammation, Eur J Nucl Roentgenol, 2005;185:1641–50.
scintigraphy and In-111leucocytes scans in neuropathic foot Med Mol Imaging, 2004;31:29–37. 34. Kreitner KF, Kalden P, Neufang A, et al., Diabetes and
disease, J Nucl Med, 1988;29:1651. 22. Keidar Z, Militianu D, Melamed E, et al., The diabetic foot: peripheral arterial occlusive disease: prospective comparison of
11. Roca M, Martin-Comin J, Becker W, et al., A consensus protocol initial experience with 18F-FDG PET/CT, J Nucl Med, contrast-enhanced three-dimensional MR angiography with
for white blood cells labelling with technetium-99m 2005;46:444–9. conventional digital subtraction angiography, Am J Roentgenol,
hexamethylpropylene amine oxime. International Society of 23. Zhuang H, Duarte PS, Pourdehnad M, et al., The promising role 2000;174:171–9.
Radiolabeled Blood Elements (ISORBE), Eur J Nucl Med, 1998;25: of 18F-FDG PET in detecting infected lower limb prosthesis 35. Enderle MD, Coerper S, Schweizer HP, et al., Correlation of
797–9. implants, J Nucl Med, 2001;42:44–8. imaging techniques to histopathology in patients with diabetic
12. Splittgerber GF, Spiegelhoff DR, Buggy BR, Combined leukocyte 24. De Winter F, Vogelaers D, Gemmel F, Dierckx RA, Promising role foot syndrome and clinical suspicion of chronic osteomyelitis.
and bone imaging used to evaluate diabetic osteoarthropathy of 18-F-fluoro-D-deoxyglucose positron emission tomography The role of high-resolution ultrasound, Diabetes Care, 1999;22:
and osteomyelitis, Clin Nucl Med, 1989;14:156–60. in clinical infectious diseases, Eur J Clin Microbiol Infect Dis, 294–9.
13. Schauwecker DS, Diagnosis with In-lll-labeled leukocytes, 2002;21:247–57.
Radiology, 1989;71:141–6. 25. Larcos G, Brown ML, Sutton RT, Diagnosis of osteomyelitis of
78 US ENDOCRINE DISEASE 2007
You might also like
- Cardiac Catheterization and Coronary Intervention (2nd Edition, 2020)Document353 pagesCardiac Catheterization and Coronary Intervention (2nd Edition, 2020)John Cancel50% (2)
- Essentials of Internal MedicineDocument832 pagesEssentials of Internal MedicineEmanuelMC100% (78)
- Allura Xper FD20 SpecificationsDocument28 pagesAllura Xper FD20 SpecificationsDewi Ratna Sari88% (8)
- CT For PE Breathing Technique PRESENTATIONDocument17 pagesCT For PE Breathing Technique PRESENTATIONEka JuliantaraNo ratings yet
- Short Syngo - Via - EngDocument5 pagesShort Syngo - Via - EngCeoĐứcTrườngNo ratings yet
- Abark PDFDocument73 pagesAbark PDFkeshavNo ratings yet
- De37 PDFDocument4 pagesDe37 PDFEka JuliantaraNo ratings yet
- NIH Public Access: Optical Imaging: New Tools For ArthritisDocument29 pagesNIH Public Access: Optical Imaging: New Tools For ArthritisMuhammad Fadli RobbyNo ratings yet
- The Importance of Magnetic Resonance Imaging in The Diagnosis and Treatment of Diabetic Foot SyndromeDocument7 pagesThe Importance of Magnetic Resonance Imaging in The Diagnosis and Treatment of Diabetic Foot SyndromeCentral Asian StudiesNo ratings yet
- Xray Mri Vs HistopaDocument9 pagesXray Mri Vs HistopaDinda SaviraNo ratings yet
- Osteomyelitis JamaDocument8 pagesOsteomyelitis Jamastevenvargas1No ratings yet
- Bone Tumor Risk Stratification and Management System A Consensus Guideline From The ACR Bone Reporting and Data System CommitteeDocument15 pagesBone Tumor Risk Stratification and Management System A Consensus Guideline From The ACR Bone Reporting and Data System CommitteeJuana GalloNo ratings yet
- Indicación de RX para DX TTMDocument12 pagesIndicación de RX para DX TTMenzoNo ratings yet
- Bornstein, M. M., Cionca, N., & Mombelli, A. (2009)Document17 pagesBornstein, M. M., Cionca, N., & Mombelli, A. (2009)tefaNo ratings yet
- Fneur 15 1360385Document11 pagesFneur 15 1360385arif 2006No ratings yet
- NIH Public Access: Author ManuscriptDocument15 pagesNIH Public Access: Author Manuscriptfidatahir93No ratings yet
- Correlation Between Radiograph Imaging and Degree of Chondrosarcoma HistopathologyDocument5 pagesCorrelation Between Radiograph Imaging and Degree of Chondrosarcoma HistopathologyPopyNo ratings yet
- Diagnostics 12 00618Document9 pagesDiagnostics 12 00618macox77No ratings yet
- SeminarDocument20 pagesSeminarricardojosesotofontalvoNo ratings yet
- (545. JAMP - Sushrit) 633-636 FinalDocument4 pages(545. JAMP - Sushrit) 633-636 FinalDinda SaviraNo ratings yet
- MRI Monitoring of Pathological Changes in The Spinal Cord in Patients With Multiple SclerosisDocument13 pagesMRI Monitoring of Pathological Changes in The Spinal Cord in Patients With Multiple SclerosisIreneNo ratings yet
- Dr. Prudhvinathreddy. A: S/O A.M.Kondareddy 7/350-1A Bhaygya Nagar Colony Kadapa, Ysr Kadapa (DIST) Andhra PradeshDocument13 pagesDr. Prudhvinathreddy. A: S/O A.M.Kondareddy 7/350-1A Bhaygya Nagar Colony Kadapa, Ysr Kadapa (DIST) Andhra PradeshRachnaNo ratings yet
- Orthodontic Care For Medically Compromised Patients: ReviewDocument12 pagesOrthodontic Care For Medically Compromised Patients: ReviewAkram AlsharaeeNo ratings yet
- Struger WeberDocument6 pagesStruger WeberNicolas RodriguezNo ratings yet
- Evaluation and Management of Small-Bowel Obstruction: An Eastern Association For The Surgery of Trauma Practice Management GuidelineDocument8 pagesEvaluation and Management of Small-Bowel Obstruction: An Eastern Association For The Surgery of Trauma Practice Management GuidelineAndreia MattiuciNo ratings yet
- Wahlen 2020, Impact of Sarcopenia in Trauma and Surgical PatientDocument7 pagesWahlen 2020, Impact of Sarcopenia in Trauma and Surgical Patientdiana perezNo ratings yet
- Imaging in Osteoarthritis 2021 YjocaDocument22 pagesImaging in Osteoarthritis 2021 Yjocaal malikNo ratings yet
- Imaging For Osteoarthritis: SciencedirectDocument9 pagesImaging For Osteoarthritis: SciencedirectJesiandra isabel M WagiuNo ratings yet
- Use of Intravenous Iodinated Contrast Media in PatDocument10 pagesUse of Intravenous Iodinated Contrast Media in PatOrlin ZlatarskiNo ratings yet
- 111 PDFDocument8 pages111 PDFMaría José Díaz RojasNo ratings yet
- Systemic Diseases Affecting Osseointegration TherapyDocument7 pagesSystemic Diseases Affecting Osseointegration TherapyAlfred OrozcoNo ratings yet
- Radionuclide Imaging in The Diagnosis And.4Document9 pagesRadionuclide Imaging in The Diagnosis And.4cooperorthopaedicsNo ratings yet
- 586 2003 Article 613Document9 pages586 2003 Article 613Jossie AcuñaNo ratings yet
- The History of Clinical Musculoskeletal RadiologyDocument8 pagesThe History of Clinical Musculoskeletal RadiologyVALENTINA LOPEZ MARINNo ratings yet
- Future Trends Imaging in Bone TumorDocument7 pagesFuture Trends Imaging in Bone TumorTika wahyuNo ratings yet
- On The Brain PDFDocument6 pagesOn The Brain PDFNezrin BaxisliNo ratings yet
- Radiographic Imaging in Osteomyelitis The Role ofDocument11 pagesRadiographic Imaging in Osteomyelitis The Role ofEga AihenaNo ratings yet
- Zbojniewicz Sorger 2014 Posttreatment Imaging of Pediatric Musculoskeletal TumorsDocument18 pagesZbojniewicz Sorger 2014 Posttreatment Imaging of Pediatric Musculoskeletal Tumorsdinda indah AsmaraNo ratings yet
- Aerts 2016Document7 pagesAerts 2016Ishani Anushika JayakodyNo ratings yet
- Aslangul2013 PDFDocument8 pagesAslangul2013 PDFGilang PramanayudhaNo ratings yet
- Informed Appropriate Imaging For Low Back Pain Management: A Narrative ReviewDocument14 pagesInformed Appropriate Imaging For Low Back Pain Management: A Narrative ReviewstephanNo ratings yet
- Chapt 1 PeterDocument63 pagesChapt 1 PeterSamson PeterNo ratings yet
- Balogh 2012Document11 pagesBalogh 2012Fatrika DewiNo ratings yet
- CLN 75 1500Document7 pagesCLN 75 1500Hevin GokulNo ratings yet
- NIH Public Access: Author ManuscriptDocument26 pagesNIH Public Access: Author Manuscriptchrist_cruzerNo ratings yet
- Imaging Bone Tumor To Onco SurgDocument9 pagesImaging Bone Tumor To Onco SurgDinda SaviraNo ratings yet
- D0009DDocument7 pagesD0009DAmin AminiNo ratings yet
- Sajr 22 1316Document6 pagesSajr 22 1316Nafiatul MuasyarahNo ratings yet
- Osteosarcoma An Evolving Understanding of A.3Document12 pagesOsteosarcoma An Evolving Understanding of A.3cooperorthopaedicsNo ratings yet
- Controversias en Infecciones en CMFDocument9 pagesControversias en Infecciones en CMFDra.lupita LoMaNo ratings yet
- DX y TtoDocument13 pagesDX y TtoIvi HidalgoNo ratings yet
- Extra ExtraDocument24 pagesExtra ExtrabaoNo ratings yet
- Genetic Stroke Syndromes.16Document13 pagesGenetic Stroke Syndromes.16mhd.mamdohNo ratings yet
- Euro J of Neurology - 2023 - Abou Mrad - Central Vein Sign and Paramagnetic Rim Sign From Radiologically Isolated SyndromeDocument7 pagesEuro J of Neurology - 2023 - Abou Mrad - Central Vein Sign and Paramagnetic Rim Sign From Radiologically Isolated SyndromeRenju KuriakoseNo ratings yet
- Introduction To NeuroimagingDocument11 pagesIntroduction To NeuroimagingJojo LastNo ratings yet
- Articulo DiabetesDocument19 pagesArticulo DiabetesJosé Mario RodríguezNo ratings yet
- Arthritis in ColorDocument228 pagesArthritis in Colorpratham100% (1)
- Radiology For Maxillofacial Surgeons The EssentialDocument49 pagesRadiology For Maxillofacial Surgeons The EssentialAbdulkadir AwadhNo ratings yet
- JBO 19-1-010901 Medical Hiperspectral Imaging ReviewDocument24 pagesJBO 19-1-010901 Medical Hiperspectral Imaging ReviewJuan EstradaNo ratings yet
- Wilson 2017Document13 pagesWilson 2017DaniNo ratings yet
- Adi Wasis Prakosa - Poster AbstractDocument2 pagesAdi Wasis Prakosa - Poster AbstractAdi Wasis PrakosaNo ratings yet
- Radiol 13121947Document7 pagesRadiol 13121947Eduardo Agustín Vargas CamposNo ratings yet
- Perone 2020Document9 pagesPerone 2020Tenta Hartian HendyatamaNo ratings yet
- Wardlaw - 2013 Neuroimaging Standards For Research Into Small Vessel Disease SVDDocument17 pagesWardlaw - 2013 Neuroimaging Standards For Research Into Small Vessel Disease SVDDavid JuanNo ratings yet
- A 2022 Recurenta, RX,!!!Document8 pagesA 2022 Recurenta, RX,!!!Popescu MariaNo ratings yet
- Contrast Reverse DentalDocument4 pagesContrast Reverse DentalEka JuliantaraNo ratings yet
- Radiation Protection in Dental Radiology: Fundamentals of Panoramic RadiographyDocument51 pagesRadiation Protection in Dental Radiology: Fundamentals of Panoramic RadiographyEka JuliantaraNo ratings yet
- Journal of Clinical & Translational EndocrinologyDocument6 pagesJournal of Clinical & Translational EndocrinologyEka JuliantaraNo ratings yet
- Analysis of Ulcer Recurrences After Metatarsal Head Resection in Patients Who Underwent Surgery To Treat Diabetic Foot OsteomyelitisDocument6 pagesAnalysis of Ulcer Recurrences After Metatarsal Head Resection in Patients Who Underwent Surgery To Treat Diabetic Foot OsteomyelitisEka JuliantaraNo ratings yet
- Diffusion-Weighted Imaging (DWI) : Clinical Applications in Oncologic DiseaseDocument37 pagesDiffusion-Weighted Imaging (DWI) : Clinical Applications in Oncologic DiseaseEka JuliantaraNo ratings yet
- Diffusion-Weighted Imaging (DWI) : Clinical Applications in Oncologic DiseaseDocument37 pagesDiffusion-Weighted Imaging (DWI) : Clinical Applications in Oncologic DiseaseEka JuliantaraNo ratings yet
- Frequency and Distribution of Chest Radiographic F PDFDocument24 pagesFrequency and Distribution of Chest Radiographic F PDFEka JuliantaraNo ratings yet
- Imaging The Diabetic Foot: Skeletal Radiology December 1995Document10 pagesImaging The Diabetic Foot: Skeletal Radiology December 1995Eka JuliantaraNo ratings yet
- Frequency and Distribution of Chest Radiographic Findings in COVID-19 Positive PatientsDocument24 pagesFrequency and Distribution of Chest Radiographic Findings in COVID-19 Positive PatientsEka JuliantaraNo ratings yet
- Magnetic Resonance Imaging: The Diffusion and ADC Imaging WayDocument50 pagesMagnetic Resonance Imaging: The Diffusion and ADC Imaging WayEka JuliantaraNo ratings yet
- Analysis of Ulcer Recurrences After Metatarsal Head Resection in Patients Who Underwent Surgery To Treat Diabetic Foot OsteomyelitisDocument6 pagesAnalysis of Ulcer Recurrences After Metatarsal Head Resection in Patients Who Underwent Surgery To Treat Diabetic Foot OsteomyelitisEka JuliantaraNo ratings yet
- Abdominal MRI: Evaluation of Binomial Water Excitation For Fat SuppressionDocument1 pageAbdominal MRI: Evaluation of Binomial Water Excitation For Fat SuppressionEka JuliantaraNo ratings yet
- Coronavirus Webinar - Dr. Khaldun FINAL UPDATED 3.5.20 Final Slides 683083 7Document56 pagesCoronavirus Webinar - Dr. Khaldun FINAL UPDATED 3.5.20 Final Slides 683083 7Eka JuliantaraNo ratings yet
- NIH Public Access: Author ManuscriptDocument28 pagesNIH Public Access: Author ManuscriptEka JuliantaraNo ratings yet
- De37 PDFDocument4 pagesDe37 PDFEka JuliantaraNo ratings yet
- Digital Radiography. A Comparison With Modern Conventional ImagingDocument4 pagesDigital Radiography. A Comparison With Modern Conventional ImagingEka JuliantaraNo ratings yet
- Detector PDFDocument39 pagesDetector PDFEka JuliantaraNo ratings yet
- The Morphology, Characteristics, and Medicinal Properties of Camellia Sinensis' TeaDocument7 pagesThe Morphology, Characteristics, and Medicinal Properties of Camellia Sinensis' TeaEka JuliantaraNo ratings yet
- Synovial Knee Disease: MRI Differential Diagnosis: Poster No.: Congress: Type: AuthorsDocument18 pagesSynovial Knee Disease: MRI Differential Diagnosis: Poster No.: Congress: Type: AuthorsEka JuliantaraNo ratings yet
- Dimond Iii: Image Quality and Dose Management For Digital RadiographyDocument137 pagesDimond Iii: Image Quality and Dose Management For Digital RadiographyEka JuliantaraNo ratings yet
- Ajr 14 12810Document5 pagesAjr 14 12810Eka JuliantaraNo ratings yet
- MicrosDocument11 pagesMicrosEka JuliantaraNo ratings yet
- Research ArticleDocument15 pagesResearch ArticleEka JuliantaraNo ratings yet
- Pub1532 WebDocument190 pagesPub1532 WebEka JuliantaraNo ratings yet
- Crossectional Patologi: I. Spine 1. Fraktur OdontoidDocument11 pagesCrossectional Patologi: I. Spine 1. Fraktur OdontoidEka JuliantaraNo ratings yet
- West African Journal of Radiology April 2005 Vol. 12 Number 1Document6 pagesWest African Journal of Radiology April 2005 Vol. 12 Number 1Eka JuliantaraNo ratings yet
- Sir OsisDocument8 pagesSir OsisEka JuliantaraNo ratings yet
- KCR 2019 Abstract Book-SE - NeuroradiologyDocument66 pagesKCR 2019 Abstract Book-SE - NeuroradiologyJANBADE PURVESH ATUL (PGP 2016-18)No ratings yet
- SCATh AnnexI v5.4Document80 pagesSCATh AnnexI v5.4chichaslocasNo ratings yet
- Vet Record Case Reports - 2022 - Cambruzzi - Anaesthetic Management of A Dog With Severe Pulmonary Stenosis and R2A RightDocument10 pagesVet Record Case Reports - 2022 - Cambruzzi - Anaesthetic Management of A Dog With Severe Pulmonary Stenosis and R2A RightYeny Paola Cruz RojasNo ratings yet
- Embolization of Bronchial Arteries For The Treatment of HEMOPTYSIS. Update and Literature ReviewDocument20 pagesEmbolization of Bronchial Arteries For The Treatment of HEMOPTYSIS. Update and Literature ReviewHai SheikhNo ratings yet
- Clinical Abbreviations List - SESLHDPR 282Document46 pagesClinical Abbreviations List - SESLHDPR 282VitusMpotwaNo ratings yet
- Contrast MediaDocument94 pagesContrast MediaJustin JoseNo ratings yet
- Med Surg Study GuideDocument98 pagesMed Surg Study Guideprogramgrabber100% (24)
- Biopsychology, 6/E: ISBN: 0-205-42651-4Document30 pagesBiopsychology, 6/E: ISBN: 0-205-42651-4Gînțăgan Denisa GabrielaNo ratings yet
- Clinical and Angiographic Profile of Coronary Artery Disease in Young Women - A Tertiary Care Centre Study From North Eastern IndiaDocument13 pagesClinical and Angiographic Profile of Coronary Artery Disease in Young Women - A Tertiary Care Centre Study From North Eastern IndiaIJAR JOURNALNo ratings yet
- DNB Radiology PapersDocument55 pagesDNB Radiology PaperskhanaknandoliaNo ratings yet
- Neurologic Disorder: By: Sandot, Alfrien BDocument25 pagesNeurologic Disorder: By: Sandot, Alfrien BAlfrien Ivanovich LarchsonNo ratings yet
- MJPJAY Procedures 996Document58 pagesMJPJAY Procedures 996bhushan adhariNo ratings yet
- Case Study 1 and 2 Ucm - 488417Document49 pagesCase Study 1 and 2 Ucm - 488417Monna Jane ObiedoNo ratings yet
- How To Do Radial Coronary AngiogramDocument5 pagesHow To Do Radial Coronary AngiogramnarasimhahanNo ratings yet
- NeuroradiologieDocument107 pagesNeuroradiologieOleg BalanNo ratings yet
- Seminar Bidang Ilmu Bedah Mulut: Arterivenous Malformation Pada Mandibula Dan Penanganannya Dalam Praktik Kedokteran GigiDocument41 pagesSeminar Bidang Ilmu Bedah Mulut: Arterivenous Malformation Pada Mandibula Dan Penanganannya Dalam Praktik Kedokteran GigiAbdul QaharNo ratings yet
- CPT Guide Diagnostic Radiology ProceduresDocument2 pagesCPT Guide Diagnostic Radiology ProceduresPavithra ManickamNo ratings yet
- Radiological Investigations of Urinary TractDocument78 pagesRadiological Investigations of Urinary Tractzoher al naeemeNo ratings yet
- Brochure Optima IGS 330 2016Document7 pagesBrochure Optima IGS 330 2016Mauricio Ernesto Andrade MaquilónNo ratings yet
- Case Study CvaDocument6 pagesCase Study Cvajing_elizabethNo ratings yet
- DCLT?Document5 pagesDCLT?My selfNo ratings yet
- Imaging of Central Nervous System Ischemia.6Document19 pagesImaging of Central Nervous System Ischemia.6Gabriela ArvelaezNo ratings yet
- Specifications ClarityFD20Document36 pagesSpecifications ClarityFD20Jonas Denis NGAMBANo ratings yet
- Carotid Artery Disease: Causes, Symptoms, Tests, and TreatmentDocument6 pagesCarotid Artery Disease: Causes, Symptoms, Tests, and TreatmentVijay Baskar SNo ratings yet
- healthcare-ANGIO-brochure-06 - 2023 WebDocument6 pageshealthcare-ANGIO-brochure-06 - 2023 WebkinatavintageNo ratings yet