Professional Documents
Culture Documents
Trauma I Initial Eval PDF
Trauma I Initial Eval PDF
Uploaded by
Esmareldah Henry SirueOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Trauma I Initial Eval PDF
Trauma I Initial Eval PDF
Uploaded by
Esmareldah Henry SirueCopyright:
Available Formats
ACS/ASE Medical Student Core Curriculum
Trauma I - ABCs of Trauma
Trauma I – ABCs of Trauma
Triage and Transport
Trauma patients are initially evaluated in the field by pre-hospital personnel. They are stabilized
and transported to a suitable facility based on clinical status and the capabilities of the center.
The method of transport is based on the severity of injury and the distance to the receiving
facility. On arrival, patients are triaged based on the mechanism of injury, severity of injury,
hemodynamic stability and resources available. In situations involving multiple victims, those
with the most severe or life-threatening injuries are generally treated first. In situations where
casualties overwhelm resources, however, patients that are unlikely to survive may receive
expectant management in order to devote resources to patients with survivable injuries. Once
appropriately triaged, trauma patients undergo assessment of vital signs, primary survey,
secondary survey, resuscitation and definitive care.
Primary Survey
The first component of the systematic approach to the trauma patient is called the primary
survey. The purpose of the primary survey is to identify life-threatening injuries and initiate
appropriate resuscitation. A simple mnemonic, ABCDE, is used to guide the steps of the primary
survey. Evaluation of the severely injured patient must occur quickly and methodically to
decrease the risk of missed injuries. Any decline in a patient’s status warrants repeating the
primary survey as clinical conditions in trauma can shift rapidly (1).
A- Airway Maintenance with Cervical Spine Protection
The airway must be rapidly assessed for patency in all trauma patients. This can be done simply
in awake patients by asking them to state their name and what occurred during the incident. If
the patient has difficulty or is unable to speak, maneuvers include suctioning the oropharynx,
searching for and removing foreign bodies, and identification of significant facial trauma or
evidence of burn injury. Definitive airway management is required in the following scenarios:
• Patients with depressed mental status or unable to protect their airway, such as patients
with Glasgow Coma Scale (GCS) of 8 or lower.
• Patients with significant maxillofacial trauma at high risk for airway obstruction,
• Patients with severe hemodynamic instability.
In preparation for endotracheal intubation, simple maneuvers for opening the airway can be
performed to improve oxygenation and ventilation. A jaw-thrust (chin-lifts are not used in blunt
trauma patients given the need to protect the cervical spine) may be the most important initial
procedure for an obtunded patient. An oral airway or nasal trumpet can be inserted. Finally,
supplemental oxygen must be administered, usually by bag valve mask. In general, for
obtunded or severely injured patients it is preferable to establish a definitive airway with a cuffed
endotracheal tube. Such tubes allow for oxygenation and ventilation in addition to preventing
gastric contents or blood from entering the lower airways.
Methods for management of the airway include:
Laryngeal mask airway (LMA) - In cases where endotracheal intubation has been
unsuccessful, a laryngeal mask airway can be placed as an advanced airway. This device is
American College of Surgeons Division of Education Page 1 of 16
Blended Surgical Education and Training for Life
ACS/ASE Medical Student Core Curriculum
Trauma I - ABCs of Trauma
placed over the larynx and does not provide a definitive airway. Trauma patients who arrive
from the field with an LMA require definitive airways upon arrival to a trauma center.
Surgical airway - In situations where endotracheal intubation is not feasible or unsuccessful
after several attempts, a surgical airway can be performed. The most common emergent airway
is obtained by incising the cricothyroid membrane and placing an endotracheal tube into the
airway. In the case of cricothyroidotomy, the airway remains in place until a more definitive
airway is established.
Figure 1. Cricothyroidotomy performed via vertical skin incision. The cricothyroid membrane is
incised transversely and an endotracheal tube is inserted into the airway. (2)
Endotracheal Intubation - The most common definitive airway in trauma is endotracheal
intubation. This can be performed with the aid of direct laryngoscopy, fiberoptic bronchoscopy,
video laryngoscopy, or a number of other methods.
As trauma patients are at high risk for aspiration, rapid sequence intubation is recommended to
decrease likelihood of aspiration of gastric contents. Patients undergo pre-oxygenation, cricoid
pressure, administration of rapid-onset sedative or hypnotic agents, neuromuscular-blockade to
induce paralysis, followed immediate introduction of the endotracheal tube. Following placement
of the endotracheal tube, the first priority is to confirm its position within the trachea. End-tidal
CO2 verification with disposable testing devices or continuous monitors provide the most reliable
means of accomplishing this.
Regardless of the intervention utilized to evaluate and establish the airway, great care must be
taken to avoid exacerbating a potential cervical spine injury. Hard collars and neck
immobilization can prevent spinal cord injury in these patients. Collars should remain in place
American College of Surgeons Division of Education Page 2 of 16
Blended Surgical Education and Training for Life
ACS/ASE Medical Student Core Curriculum
Trauma I - ABCs of Trauma
until injury to the cervical spine is effectively ruled out. Manual in-line stabilization can be
performed if the collar needs to be removed for intubation (1).
B- Breathing and Ventilation
After assessing and securing the airway, the next step is to ensure there are no barriers
preventing ventilation and oxygenation. The examiner should evaluate for symmetrical chest
rise, tracheal position, jugular venous distention, audible breath sounds, and evidence of trauma
to the chest wall. There are several specific injuries that must be rapidly identified and dealt with
should they be present. They include tension pneumothorax, massive hemothorax, and open
pneumothorax (also referred to as “sucking” chest wound).
Diagnosis of each is based on clinical findings and prompts immediate intervention.
Tension Pneumothorax - Clinical signs associated with tension pneumothorax include absent
breath sounds, jugular venous distention, tracheal deviation away from the injured side, and
hypotension. Tension pneumothorax differs from simple pneumothorax in that the injured
portion of lung parenchyma acts as one-way valve allowing air to enter the pleural space with
each breath. The flap closes with exhalation resulting in ever increasing intrathoracic pressure.
The trachea and mediastinal structures may deviate away from the affected side which
ultimately occludes the superior and inferior vena cava. The loss of venous return to the heart
results in obstructive shock and hypotension.
The diagnosis of tension pneumothorax should be made before obtaining a chest radiograph.
Prompt tube thoracostomy should be performed to decompress the chest and reestablish
normal venous return. Needle decompression, usually with a 14-guage catheter in the second
intercostal space, mid-clavicular line, may be performed in the field, but is generally not
appropriate in the trauma bay where a chest tube can be placed rapidly (1).
Hemothorax - Hemothorax is defined as blood contained within the pleural cavity. The source
bleeding may be from an injured intercostal vessel in the setting of rib fractures, pulmonary
laceration, pulmonary hilar injury, or great vessel laceration. The quantity of blood may range
from an amount barely visible on chest radiograph, to several liters resulting in compression of
the lung and “white-out” of the affected side on chest x-ray. Patients with massive hemothorax
may have flat neck veins, absent breath sounds on the affected side, and hemodynamic
instability secondary to hemorrhagic shock.
Initial management includes aggressive resuscitation and replacement of blood products and
decompression of the chest with a chest tube. Patients with large volumes of blood evacuated
will often require urgent thoracotomy for hemorrhage control (1, 2). Typical indication for
thoracotomy include initial evacuation of 1500 mls. of blood or ongoing output of 250 ml/hour for
three consecutive hours.
American College of Surgeons Division of Education Page 3 of 16
Blended Surgical Education and Training for Life
ACS/ASE Medical Student Core Curriculum
Trauma I - ABCs of Trauma
Figure 2. Chest x-ray of hemothorax in supine (A) and upright (B) positions. Blood layers
posteriorly while the patient is supine. It can be seen collecting dependently in the upright
position (2).
Open Pneumothorax (“Sucking” Chest Wound) - A defect in the chest wall that allow air to
enter into the thoracic cavity is termed open pneumothorax. If the wound is 2/3 of the diameter
of the trachea or larger, air will preferentially enter through the chest wall defect inhibiting
ventilation. A simple procedure to restore normal respiratory mechanics is placement of an
occlusive dressing taped on three sides over the defect. A flutter valve is created preventing air
from entering the chest on inspiration while allowing it to evacuate during exhalation. A
completely occlusive dressing without the presence of a chest tube could result in a tension
pneumothorax. Chest tubes should be placed in a location remote from the chest wound.
A chest x-ray should be performed as part of the assessment of breathing after the primary
survey is completed and can help to confirm proper endotracheal or chest tube placement and
recognition of pneumothorax or hemothorax not detected on exam. Treatment of these serious
injuries if there is clinical suspicion should not be delayed for x-ray (1).
C- Circulation with Hemorrhage Control
Assessment of circulation entails evaluating a patient’s volume status as well as obtaining
adequate intravenous access and controlling sources of bleeding. Vital signs provide valuable
information regarding a patient’s physiologic response to an injury. Tachycardia in adults is
defined as a heart rate of 100 beats per minute or greater. A trauma patient may become
tachycardic due to pain or stress, but shock as a result of hemorrhage must be suspected in any
injured patient. Changes in blood pressure such as a decreased systolic pressure or widened
pulse pressure can also suggest that a patient is in some degree of hemorrhagic shock.
Hypotension is defined as systolic pressure less than 90 mm Hg. The combination of
hypotension and tachycardia is often referred to as hemodynamic instability. Prompt recognition
of stability is important as it strongly affects the management of trauma patients.
Whenever possible, it is important to obtain a report from first responders. This may aid in
understanding mechanisms of injury that may help identify injury patterns. General physical
exam findings of a patient in hemorrhagic shock include altered level of consciousness or
anxiety, pallor or coolness of the skin, or a rapid or weak central pulse. While external
American College of Surgeons Division of Education Page 4 of 16
Blended Surgical Education and Training for Life
ACS/ASE Medical Student Core Curriculum
Trauma I - ABCs of Trauma
hemorrhage is a common source of significant blood loss, these injuries are usually easily
identified in the field or trauma bay. External hemorrhage can often be controlled with direct
pressure or a tourniquet until definitive control can be obtained in the operating room. This is
more common in penetrating trauma.
If the source of hemorrhage is not evident, which is more often the case in blunt trauma, there
are five compartments that can accommodate large enough volumes of blood to result in
hemodynamic instability:
• thoracic cavity
• peritoneal cavity
• retroperitoneum
• pelvis
• long bones (usually femur fractures)
Patient history, vital signs, and physical exam findings will help the astute clinician make an
assessment of volume status. Physical exam findings such as a distended abdomen, unstable
pelvis, or lower extremity deformity must alert the examiner to the possibility of significant
hemorrhage. Adjuncts to the physical exam should be employed to evaluate each area. In the
unstable patient blunt trauma patient, chest x-ray, pelvis x-ray and FAST (Focus Assessment
with Sonography in Trauma) can be performed quickly in most situations. It is difficult to identify
hemorrhage in the retroperitoneum with these modalities and it may require exploratory
laparotomy for diagnosis and treatment. Computed tomography is effective for identifying
sources of hemorrhage in hemodynamically stable patients. However, this imaging modality is
generally contraindicated in cases of hemodynamic instability.
Imaging Modality Common Findings Cause of instability Trauma Bay
Treatment
Chest X-ray Widened mediastinum, Pneumothorax, Chest tube
effusion, rib fractures, hemothorax, aortic
mediastinal deviation, injury
pneumothorax
Pelvis X-ray Pelvic fractures, Pelvic blood vessel Pelvic Binder
widened pubic disruption
symphysis (open
book)
FAST Fluid in pericardium, Pericardial tamponade, Transport to OR for
Morrison’s hemoperitoneum Sternotomy,
(hepatorenal) pouch, laparotomy
splenorenal space,
and pelvis
Extremity X-ray Long bone fracture Peripheral vascular Reduction/tourniquet
bleeding
Table 1. Imaging in unstable patients
Large bore, generally 16-gauge and larger, peripheral intravenous access is preferred for large
volume resuscitation. Internal diameter and length of the line determine the maximum rate at
which a fluid may be given. Short, large bore peripheral angiocatheters are therefore superior to
longer central venous catheters with smaller internal diameters for large volume resuscitation. If
peripheral venous access cannot be obtained, central resuscitative lines can be placed in the
American College of Surgeons Division of Education Page 5 of 16
Blended Surgical Education and Training for Life
ACS/ASE Medical Student Core Curriculum
Trauma I - ABCs of Trauma
internal jugular, subclavian or femoral veins. If this is not technically feasible, intraosseus lines
can be placed and used effectively for resuscitation (1).
Hemorrhagic shock is the most common form of shock seen in the trauma patient. Once
obstructive shock from tension pneumothorax or pericardial tamponade have been ruled out,
resuscitative efforts are directed towards replacing blood volume and control of hemorrhage.
Classes of Hemorrhage
Class I Class II (mild) Class III Class IV
(moderate) (severe)
Approximate blood <15% 15%-30% 31%-40% >40%
loss
Heart rate ↔ ↔/↑ ↑ ↑/↑↑
Blood pressure ↔ ↔ ↔/↓ ↓
Pulse pressure ↔ ↓ ↓ ↓
Respiratory rate ↔ ↔ ↔/↑ ↑
Urine output ↔ ↔ ↓ ↓↓
Glasgow Coma ↔ ↔ ↓ ↓
Scale core
Base deficit 0 to -2 mEq/L -2 to -6 mEq/L -6 to -10 mEq/L -10 mEq/L or
less
Need for blood Monitor Possible Yes Massive
products Transfusion
Protocol
Table 2. (1)
Unstable patients who have sustained significant blood loss may require large amounts of blood
product very rapidly. Massive transfusion protocols have been developed to efficiently supply
large amounts of blood product to the injured patient. Packed red blood cells, fresh frozen
plasma and platelets are generally given in a 1:1:1 ratio. Thromboelastography (TEG) guides
resuscitation by assessing the characteristics of a patient’s clot formation and breakdown (4).
Aberrations in these values can guide the surgeon in determining which blood products to use in
reeducation.
American College of Surgeons Division of Education Page 6 of 16
Blended Surgical Education and Training for Life
ACS/ASE Medical Student Core Curriculum
Trauma I - ABCs of Trauma
Figure 3. Diagram of thromboelastogram. R= reaction time, alpha= angle, MA= maximum
amplitude, TMA= time to maximal amplitude, LY= percentage amplitude reduction, CLT= clot
lysis time (7).
Emergency department thoracotomy can be performed in select patients presenting in extremis.
Goals of ED thoracotomy include evaluation of the pericardium with decompression of
tamponade, identification and repair of penetrating cardiac injury, and cross-clamping the
descending thoracic aorta. Indications for thoracotomy in the ED differ for blunt versus
penetrating mechanisms. In general, patients with penetrating injuries have a higher likelihood
of survival than patients with blunt injuries undergoing ED thoracotomy (5).
A newer method of temporizing severe hemorrhage below the level of the diaphragm is
resuscitative balloon occlusion of the aorta (REBOA). This technique involves placing a sheath
in the common femoral artery followed by deploying an endovascular balloon that can be
inflated in the lumen of the aorta to decrease arterial bleeding. REBOA allows for occlusion of
the aorta without the added morbidity opening the thoracic cavity (3).
American College of Surgeons Division of Education Page 7 of 16
Blended Surgical Education and Training for Life
ACS/ASE Medical Student Core Curriculum
Trauma I - ABCs of Trauma
Figure 4. REBOA with balloon inflated in zone I of the aorta. (6)
D- Disability (Neurologic Evaluation)
Rapid assessment of the patient’s neurologic status is an important part of the primary survey.
Details of the event such as loss of consciousness raise suspicion for potential intracranial
injury. Providers should also determine patient’s mental status and whether they take any
antiplatelet or anticoagulant medications.
Physical exam methods used to evaluate neurologic function include measuring pupillary size
and reaction, assessing level of consciousness, and application of the Glasgow Coma Scale.
The Glasgow Coma Scale can be utilized quickly and is useful for initial assessment as well as
prognosis. GCS can be repeated throughout the patient’s course to track progress or identify
signs of decompensation. The score is calculated by adding the best responses from each of
the three components of the scale.
American College of Surgeons Division of Education Page 8 of 16
Blended Surgical Education and Training for Life
ACS/ASE Medical Student Core Curriculum
Trauma I - ABCs of Trauma
A rapid assessment of the patient’s ability to move all extremities can provide information
regarding the presence of a spinal cord injury. If injury to the cord is suspected, a more detailed
exam can help determine the level at which the cord is affected.
Depressed neurologic status can be present secondary to direct injury to the central nervous
system, alcohol intoxication, shock, or a number of other factors. In the setting of traumatic brain
injury, initial priority is to avoid secondary brain injury resulting from hypoxemia and
hypoperfusion to the brain
The Glasgow Coma Scale guides the management of traumatic brain injury patients by
separating them into three degrees of severity. Patients with a score of 13-15 fall in the mild
traumatic brain injury category, those with a score of 9-12 are considered moderate, and scores
of 3-8 are described as severe. All patients in the moderate and severe categories require non-
contrast CT scans of the head after completion of the primary survey if they are
hemodynamically stable. Patients with a GCS of 13-15 should undergo CT scanning if they
have clinical evidence of open skull fracture, signs of basilar skull fracture (e.g.,
hemotympanum, raccoon eyes, CSF otorrhea or rhinorrhea, Battle’s sign), more than two
episodes of vomiting, or age greater than 65 years. The clinician should also consider
performing CT scan on patients with loss of consciousness greater than 5 minutes, retrograde
amnesia longer than 30 minutes, seizures, severe headaches, short term memory deficit,
intoxication, coagulopathy, focal neurological deficit, or dangerous mechanism such as
pedestrian struck by motor vehicle, ejection from motor vehicle, or fall from greater than 3 feet.
Children with head trauma run the risk of suffering poor outcomes if the injuries are not
evaluated and treated expeditiously. Secondary brain injury due to hypoxia, hypotension, or
other reductions in cerebral perfusion substantially increase the morbidity and mortality of
children with traumatic brain injuries. As in adults, the GCS score helps guide clinicians
regarding severity of injury. Not surprisingly, however, the scale is modified to account for
differences in children versus adults. Computed tomography scan of the head is the most useful
tool to look for evidence of intracranial injury. In general, children with GCS of 14 with altered
mental status, evidence of skull fracture, or seizure activity should have a head CT. Pediatric
patients with scalp hematomas, loss of consciousness, severe mechanism of injury, or
abnormal behavior according to the parents may either be observed or scanned based on
physician experience, multiple versus isolated findings, or parent preference.
(1).
Glasgow Coma Scale (GCS)
ORIGINAL SCALE REVISED SCALE SCORE
Eye Opening (E) Eye Opening (E)
Spontaneous Spontaneous 4
To speech To sound 3
To pain To pressure 2
None None 1
Non-testable NT
American College of Surgeons Division of Education Page 9 of 16
Blended Surgical Education and Training for Life
ACS/ASE Medical Student Core Curriculum
Trauma I - ABCs of Trauma
Verbal Response (V) Verbal Response (V)
Oriented Oriented 5
Confused conversation Confused 4
Inappropriate words Words 3
Incomprehensible sounds Sounds 2
None None 1
Non-testable NT
Best Motor Response (M) Best Motor Response (M)
Obeys commands Obeys Commands 6
Localizes pain Localizing 5
Flexion with withdrawal to pain Normal Flexion 4
Abnormal flexion (decorticate) Abnormal flexion 3
Extension (decerebrate) Extension 2
None (flaccid) None 1
Non-testable NT
Table 3. (1)
E- Exposure and Environmental Control
The final portion of the primary survey focuses on completely exposing the patient to avoid
missing injuries. All clothing is removed and the patient is turned in order to examine the back
and posterior surfaces. Once the patient is undressed, they should be covered with warm
blankets in order to prevent loss of body heat. Other means to prevent hypothermia in trauma
patients include increasing the ambient temperature of the trauma room, infusion of warmed
intravenous fluids, or placement of an external warming device.
Patients that have been exposed to skin irritants or other hazards substances should also be
decontaminated to prevent burns and progressive injury. Clothing soaked in gasoline is
promptly removed and discarded. Trauma centers also utilize decontamination rooms to wash
harmful substances from the patient’s body (1).
Secondary Survey
The secondary survey takes place once the primary survey is complete and resuscitation is in
progress. It includes a systematic, head-to-toe history and physical exam. Each body region is
examined carefully to avoid missing an injury. Radiography and computed tomography scans
are also utilized as part of the secondary survey.
Efforts must be taken to discover the patient’s medical background as well as details of the
event surrounding the trauma. A simple acronym to remember the important components of the
history is as follows:
S - Signs/symptoms
A - Allergies
M - Medications
P - Pertinent past medical history
L - Last oral intake
E - Events leading to the illness or injury
American College of Surgeons Division of Education Page 10 of 16
Blended Surgical Education and Training for Life
ACS/ASE Medical Student Core Curriculum
Trauma I - ABCs of Trauma
In the case of comatose or unresponsive patients, details of the history should be obtained from
family members or emergency medical personnel. A description of the patient’s mechanism of
injury is critical as the pattern of injury may guide the workup and management and avoid
missed injuries (1).
Secondary Survey
Anatomic Region Exam Findings Possible Injuries
Head Bleeding, skin defects, loss of Scalp laceration, trapped
vision, decreased extraocular extraocular muscle, basilar
motion, hemotympanum skull fracture
Face Midface stability, Facial and mandibular
malocclusion, skin defects, fractures, nasal septal
bleeding from nares hematoma, dental injury
Neck Cervical spine tenderness, Cervical spine fracture,
hematoma, bruit, tracheal penetrating and blunt
position, seat belt mark vascular injuries, esophageal
and tracheal injuries
Chest Breath sounds, crepitus, Pneumothorax, rib fractures,
chest wall stability, hemothorax, open
symmetrical chest wall pneumothorax, sternal
motion, chest wall defects fracture
Abdomen Distention, tenderness, Solid organ injury, hollow
peritoneal signs, seat belt viscus injury, vascular injury
mark
Pelvis and Perineum Pelvic stability, blood at Pelvic fracture, urethral
meatus, scrotal hematoma, disruption, rectal injury
rectal exam, high riding
prostate
Back Skin defects, thoracic or Spine fracture
lumbar spine tenderness or
step-offs, flank hematoma
Neurologic Mental status, strength, Intracranial injury, spinal cord
sensation injury, peripheral nerve
damage
Extremities Distal pulses, gross bone Long bone fractures,
deformity, joint stability, peripheral vascular injury,
compartment firmness compartment syndrome,
ligamentous injuries
Table 4. (1)
Tertiary Survey
The tertiary survey serves as the final means of identifying injury in the trauma patient. It
typically takes place within 24 hours of the injury. The primary and secondary surveys are
repeated and all laboratory and imaging date are reviewed. Any new injuries should be
identified and proper imaging obtained if indicated.
American College of Surgeons Division of Education Page 11 of 16
Blended Surgical Education and Training for Life
ACS/ASE Medical Student Core Curriculum
Trauma I - ABCs of Trauma
References
1. Advanced Trauma Life Support Student Course Manual. American College of Surgeons
Committee on Trauma. 10e. 2018.
2. Burlew C, Moore E. Trauma. In: Brunicardi F, Andersen DK, Billiar TR, Dunn DL, Hunter JG,
Matthews JB, Pollock RE. eds. Schwartz's Principles of Surgery, 10e. New York, NY: McGraw-
Hill; 2014.
3. Dubose J, Scalea T, Brenner M, et al. The AAST prospective Aortic Occlusion for
Resuscitation in Trauma and Acute Care Surgery (AORTA) registry: Data on contemporary
utilization and outcomes of aortic occlusion and resuscitative balloon occlusion of the aorta
(REBOA). J Trauma Acute Care Surg. 2016.
4. Gonzalez E, Moore E, Moore H, et al. Goal-directed Hemostatic Resuscitation of Trauma-
induced Coagulopathy: A Pragmatic Randomized Clinical Trial Comparing a Viscoelastic Assay
to Conventional Coagulation Assays. Annals of Surgery. June 2016.
5. Seamon M, Haut E, Van Arendonk K, et al. Emergency Department Thoracotomy. J Trauma.
July 2015.
6. Katz N. REBOA: Resuscitative Endovascular Balloon Occlusino of the Aorta.
emottawablog.com/2017/02/reboa-resuscitative-endovascular-balloon-occlusion-of-the-aorta/.
February 2017.
7. Ronsholt F, Gerstoft J, Ullum H, et al. Thromboelastography on plasma reveals delayed clot
formation and accelerated clot lyses in HIV-1 infected persons compared with healthy controls.
BMC Infectious Diseases. September 2015.
American College of Surgeons Division of Education Page 12 of 16
Blended Surgical Education and Training for Life
ACS/ASE Medical Student Core Curriculum
Trauma I - ABCs of Trauma
Questions
1. A 26-year-old male presents to the trauma bay after being involved in a high-speed
motorcycle collision. You note that he is obtunded and has bilateral open lower extremity
fractures with exposed bone and muscle. What is the first priority when first assessing
this patient?
a. Place tourniquets on both lower extremities to control bleeding.
b. Place two large bore peripheral IV lines.
c. Assess the airway and, if necessary, perform endotracheal intubation.*
d. Send the patient to the CT scanner to look for intracranial injury.
2. You are evaluating a 22-year-old male following blunt trauma. His blood pressure is
84/47 and heart rate is 134. He is alert but anxious, complaining of abdominal pain. You
obtain intravenous access and begin transfusion of blood products. What is the next best
step?
a. Chest x-ray, pelvis x-ray and FAST exam to look for sources of hemorrhage.*
b. Emergent CT scan of the chest, abdomen, and pelvis.
c. Transport the patient to the operating room for exploratory laparotomy.
d. Place a pelvic binder.
3. You have completed the primary and secondary surveys for a 47-year-old man who was
struck by a motor vehicle while riding his bicycle. You found him to be hemodynamically
stable with a GCS of 15. His only obvious injury is a deformed right shoulder. The nurse
suddenly alerts you that the patient has become unresponsive and his systolic blood
pressure has now dropped into the 60’s with a palpable carotid pulse. What is the next
best step?
a. Call a code blue.
b. Begin chest compressions.
c. Re-evaluate the patient starting with another primary survey.*
d. Perform urgent reduction of his dislocated shoulder.
4. A 19-year-old male was struck by a truck while crossing the street. Blood pressure is
76/34 and heart rate is 122. You secure the airway and obtain a chest x-ray that
suggests pulmonary contusions on the right and a FAST exam showing a black stripe
between the liver and right kidney. What is the next best step?
a. Go to the operating room for abdominal exploration.*
b. Perform emergency department thoracotomy.
c. Place a central line, arterial line, and foley catheter.
d. Obtain CT scans of the chest, abdomen, and pelvis.
American College of Surgeons Division of Education Page 13 of 16
Blended Surgical Education and Training for Life
ACS/ASE Medical Student Core Curriculum
Trauma I - ABCs of Trauma
5. A 22-year-old male presents to the Emergency Department after being stabbed multiple
times in the chest and abdomen. He is hemodynamically stable. During the primary
survey, special attention must be given to which of the following:
a. Obtain a detailed history and physical.
b. Assess pelvis for stability to compression.
c. Expose and roll the patient to identify additional wounds.*
d. Draw CBC, CMP, and PT/INR.
American College of Surgeons Division of Education Page 14 of 16
Blended Surgical Education and Training for Life
ACS/ASE Medical Student Core Curriculum
Trauma I - ABCs of Trauma
Answers
1. A 26-year-old male presents to the trauma bay after being involved in a high-speed
motorcycle collision. You note that he is obtunded and has bilateral open lower extremity
fractures with exposed bone and muscle. What is the first priority when first assessing
this patient?
A. Place tourniquets on both lower extremities to control bleeding.
B. Place two large bore peripheral IV lines.
C. Assess the airway and, if necessary, perform endotracheal intubation.
D. Send the patient to the CT scanner to look for intracranial injury.
2. You are evaluating a 22-year-old male following blunt trauma. His blood pressure is 84/47
and heart rate is 134. He is alert but anxious, complaining of abdominal pain. You obtain
intravenous access and begin transfusion of blood products. What is the next best step?
A. Chest x-ray, pelvis x-ray and FAST exam to look for sources of hemorrhage.
B. Emergent CT scan of the chest, abdomen, and pelvis.
C. Transport the patient to the operating room for exploratory laparotomy.
D. Place a pelvic binder.
3. You have completed the primary and secondary surveys for a 47-year-old man who was
struck by a motor vehicle while riding his bicycle. You found him to be hemodynamically
stable with a GCS of 15. His only obvious injury is a deformed right shoulder. The nurse
suddenly alerts you that the patient has become unresponsive and his systolic blood
pressure has now dropped into the 60’s with a palpable carotid pulse. What is the next
best step?
A. Call a code blue.
B. Begin chest compressions.
C. Re-evaluate the patient starting with another primary survey.
D. Perform urgent reduction of his dislocated shoulder.
American College of Surgeons Division of Education Page 15 of 16
Blended Surgical Education and Training for Life
ACS/ASE Medical Student Core Curriculum
Trauma I - ABCs of Trauma
4. A 19-year-old male was struck by a truck while crossing the street. Blood pressure is
76/34 and heart rate is 122. You secure the airway and obtain a chest x-ray that
suggests pulmonary contusions on the right and a FAST exam showing a black stripe
between the liver and right kidney. What is the next best step?
A. Go to the operating room for abdominal exploration.
B. Perform emergency department thoracotomy.
C. Place a central line, arterial line, and Foley catheter.
D. Obtain CT scans of the chest, abdomen, and pelvis.
5. A 22-year-old male presents to the Emergency Department after being stabbed multiple
times in the chest and abdomen. He is hemodynamically stable. During the primary
survey, special attention must be given to which of the following:
A. Obtain a detailed history and physical.
B. Assess pelvis for stability to compression.
C. Expose and roll the patient to identify additional wounds.
D. Draw CBC, CMP, and PT/INR.
American College of Surgeons Division of Education Page 16 of 16
Blended Surgical Education and Training for Life
You might also like
- Six-Foot Tiger, Three-Foot Cage - Take Charge of Your Health by Taking Charge of Your Mouth - Holistic Mouth Solutions For Sleep Apnea, Deficient Jaws, and Related Complications PDFDocument288 pagesSix-Foot Tiger, Three-Foot Cage - Take Charge of Your Health by Taking Charge of Your Mouth - Holistic Mouth Solutions For Sleep Apnea, Deficient Jaws, and Related Complications PDFTARAN .A.P.100% (6)
- Limmer Education Oxygen Administration FlowchartDocument1 pageLimmer Education Oxygen Administration FlowchartepraetorianNo ratings yet
- Swarthz TRAUMADocument26 pagesSwarthz TRAUMAAlexandra Niken Larasati75% (4)
- ATLS Case ScenarioDocument13 pagesATLS Case ScenarioJenny Schneider100% (2)
- Presentation 1Document25 pagesPresentation 1Nihar ShahNo ratings yet
- Primary and Secondary SurveyDocument10 pagesPrimary and Secondary SurveyBernadeth Meily100% (1)
- Lessonplan FinDocument14 pagesLessonplan Finx483xDNo ratings yet
- Normal and Pathological Bronchial Semiology: A Visual ApproachFrom EverandNormal and Pathological Bronchial Semiology: A Visual ApproachPierre Philippe BaldeyrouNo ratings yet
- Skills Netbook PDFDocument95 pagesSkills Netbook PDFPhilip100% (1)
- Thoracic TraumaDocument24 pagesThoracic TraumaOmar MohammedNo ratings yet
- Cap 19 Pre Hospital and Resuscitation CareDocument13 pagesCap 19 Pre Hospital and Resuscitation CareAvramescu Yoana100% (1)
- IntroductionDocument5 pagesIntroductionFarhan YulmiadiNo ratings yet
- PolytraumaDocument41 pagesPolytraumaFrederick Mars UntalanNo ratings yet
- Schellenberg 2018Document13 pagesSchellenberg 2018Juan Jesús Espinoza AmayaNo ratings yet
- Primary Survey KGD LBM 1Document9 pagesPrimary Survey KGD LBM 1Nur Azizah PermatasariNo ratings yet
- Chest Drains Learning ResourceDocument22 pagesChest Drains Learning ResourceSiriporn TalodkaewNo ratings yet
- Management of Chest InjuriesDocument13 pagesManagement of Chest Injuriesana9filimonNo ratings yet
- Thoracic Trauma Injuries Evaluation and TreatmentDocument17 pagesThoracic Trauma Injuries Evaluation and Treatmentnageur2017No ratings yet
- 6 Lethal DeathsDocument4 pages6 Lethal Deathslina_m354No ratings yet
- Filosso 2017Document11 pagesFilosso 2017Allison DiêgoNo ratings yet
- Airway and Ventilatory ManagementDocument8 pagesAirway and Ventilatory ManagementAshen DissanayakaNo ratings yet
- Management of Maxillofacial Trauma in EmergencyDocument11 pagesManagement of Maxillofacial Trauma in EmergencyDicky Nanda KhaNo ratings yet
- Water Seal Drainage (WSD) : Entri-Entri BerikutnyaDocument12 pagesWater Seal Drainage (WSD) : Entri-Entri BerikutnyaputridwierlindaNo ratings yet
- Water Seal Drainage (WSD) : Entri-Entri BerikutnyaDocument7 pagesWater Seal Drainage (WSD) : Entri-Entri BerikutnyaputridwierlindaNo ratings yet
- Truma Slide 4 Chest TrumaDocument38 pagesTruma Slide 4 Chest TrumaadnanreshunNo ratings yet
- Walls 8093 CH 01Document7 pagesWalls 8093 CH 01Adriana MartinezNo ratings yet
- Maxillofacial Trauma: Dr. Azher A. Auda Bds CabsDocument17 pagesMaxillofacial Trauma: Dr. Azher A. Auda Bds CabsHaider F YehyaNo ratings yet
- NEJM VICM Viewers ChoiceDocument19 pagesNEJM VICM Viewers ChoiceAnonymous cQWavnNo ratings yet
- JRNL-Responding To Trauma Your Priorities in The First HourDocument8 pagesJRNL-Responding To Trauma Your Priorities in The First HourArs MoriendiNo ratings yet
- NYSORA Hazdics RegionalDocument8 pagesNYSORA Hazdics RegionalAishu BNo ratings yet
- Traum ManagementDocument7 pagesTraum Managementchinthaka18389021No ratings yet
- Edwardus T. Adar 1308012050: Consultant Dr. Stef D. Soka, SP.BDocument21 pagesEdwardus T. Adar 1308012050: Consultant Dr. Stef D. Soka, SP.BAlbert RanggaNo ratings yet
- Combined Tracheoesophageal Transection Following A 2024 International JournDocument4 pagesCombined Tracheoesophageal Transection Following A 2024 International JournRonald QuezadaNo ratings yet
- Chapter 4: Thoracic Trauma ObjectivesDocument29 pagesChapter 4: Thoracic Trauma ObjectivesDeborah Anasthasia PakpahanNo ratings yet
- Preliminary Management of Maxillofacial Injuries MADE EASYDocument9 pagesPreliminary Management of Maxillofacial Injuries MADE EASYMohammedNo ratings yet
- Pediatric and Adult Airway Management of AnesthesiaDocument141 pagesPediatric and Adult Airway Management of AnesthesiaMulatu MilkiasNo ratings yet
- Trauma and Emergency NursingDocument9 pagesTrauma and Emergency Nursingchinthaka18389021No ratings yet
- Atls by DR Moges - 082701Document64 pagesAtls by DR Moges - 082701moges beletachawNo ratings yet
- Thoracic Surgery Lec 3Document10 pagesThoracic Surgery Lec 3ahmedalbayati2002No ratings yet
- Name Yohanes Demisu ID 1003663: Tittle-Anesthesia Consideration For Tracheal RessectionDocument4 pagesName Yohanes Demisu ID 1003663: Tittle-Anesthesia Consideration For Tracheal Ressectionderba simintoNo ratings yet
- C CH He Es ST TT TR Ra Au Um Ma A PatientDocument7 pagesC CH He Es ST TT TR Ra Au Um Ma A Patientch4augustNo ratings yet
- 1 - Politrauma 2013 PDFDocument44 pages1 - Politrauma 2013 PDFJaimeNo ratings yet
- Tube Thoracostomy Chest Tube Implantation and Follow Up: Review ArticleDocument10 pagesTube Thoracostomy Chest Tube Implantation and Follow Up: Review ArticleAnasthasia hutagalungNo ratings yet
- Rapid Sequence Intubation ReportDocument55 pagesRapid Sequence Intubation Reportlorkan19100% (1)
- Thoracic Emergency Trauma QuestionnairesDocument7 pagesThoracic Emergency Trauma QuestionnairesMeliza BancolitaNo ratings yet
- ER JournalDocument7 pagesER JournalGab LandazabalNo ratings yet
- Chest TraumaDocument26 pagesChest TraumaNader SaadNo ratings yet
- Final Chest Tube CareDocument46 pagesFinal Chest Tube Careوجد عمرNo ratings yet
- Redbook - ASSESSMENT AND MANAGEMENT OF TRAUMA PDFDocument323 pagesRedbook - ASSESSMENT AND MANAGEMENT OF TRAUMA PDFrizka100% (1)
- Airway ManagementDocument28 pagesAirway ManagementghazyNo ratings yet
- Tracheostomy: Continuing Education ActivityDocument9 pagesTracheostomy: Continuing Education ActivityUlul IsmiNo ratings yet
- Final Chest Tube CareDocument46 pagesFinal Chest Tube Careوجد عمرNo ratings yet
- Polytrauma: DR A.R.Baka Department of Surgery Federal Medical Center, YolaDocument57 pagesPolytrauma: DR A.R.Baka Department of Surgery Federal Medical Center, YolaAbuhafezbaka100% (1)
- Cuello 1Document4 pagesCuello 1Lili Pérez ArtolaNo ratings yet
- Tratamiento Del Paciente TraumatizadoDocument10 pagesTratamiento Del Paciente TraumatizadomariaNo ratings yet
- Basic Airway Management in AdultsDocument7 pagesBasic Airway Management in AdultsBereket temesgenNo ratings yet
- Pneumothorax, Tension and TraumaticDocument24 pagesPneumothorax, Tension and TraumaticSatria WibawaNo ratings yet
- Annrcse01509 0sutureDocument3 pagesAnnrcse01509 0sutureNichole Audrey SaavedraNo ratings yet
- Jurnal Laryngeal TraumaDocument7 pagesJurnal Laryngeal TraumaadindaNo ratings yet
- Tindakan TorakosentesisDocument15 pagesTindakan TorakosentesisAyu Ayu AyuNo ratings yet
- Bmri2016 3741426Document7 pagesBmri2016 3741426MandaNo ratings yet
- Anesthesia in Thoracic Surgery: Changes of ParadigmsFrom EverandAnesthesia in Thoracic Surgery: Changes of ParadigmsManuel Granell GilNo ratings yet
- Post Exposure Prophylaxis (PEP) : - Thought To Reduce HIV Transmission by 80%Document3 pagesPost Exposure Prophylaxis (PEP) : - Thought To Reduce HIV Transmission by 80%SamNo ratings yet
- Xnip2021 02 23 - 13 58 07 OCRDocument1 pageXnip2021 02 23 - 13 58 07 OCRSamNo ratings yet
- Xnip2021 02 23 - 13 53 11 OCRDocument1 pageXnip2021 02 23 - 13 53 11 OCRSamNo ratings yet
- Text Message: Been Retrieved. You May Want To Contact TheDocument1 pageText Message: Been Retrieved. You May Want To Contact TheSamNo ratings yet
- I Stop To Cancel.: Placed. You Have Opted-In To Receive TXT MSG Updates. MSG 8 Msgs. Reply HELP 4 Help orDocument1 pageI Stop To Cancel.: Placed. You Have Opted-In To Receive TXT MSG Updates. MSG 8 Msgs. Reply HELP 4 Help orSamNo ratings yet
- Xnip2021 02 23 - 13 58 15 OCRDocument1 pageXnip2021 02 23 - 13 58 15 OCRSamNo ratings yet
- FailureDocument13 pagesFailureSamNo ratings yet
- ISBARQ (Or S-BAR + 2) PDFDocument1 pageISBARQ (Or S-BAR + 2) PDFSamNo ratings yet
- 5 PsDocument2 pages5 PsSamNo ratings yet
- Cefoxitin Sodium MefoxinDocument3 pagesCefoxitin Sodium MefoxinKristi WrayNo ratings yet
- NCP FAQsDocument16 pagesNCP FAQsEl Avion NoelNo ratings yet
- Brochure HyBase 6100 2010 PDFDocument6 pagesBrochure HyBase 6100 2010 PDFYun EdhiharsoNo ratings yet
- Diabetic Foot InfectionDocument40 pagesDiabetic Foot InfectionSuchie ILyasNo ratings yet
- Group 4 NCM 114Document14 pagesGroup 4 NCM 114ESTELLE VERA O. VELEZNo ratings yet
- Evolution of Prostate BrachytherapyDocument25 pagesEvolution of Prostate BrachytherapyStirNo ratings yet
- Slide Microteaching MM Iqbal 2Document40 pagesSlide Microteaching MM Iqbal 2RAJA HARAHAPNo ratings yet
- Viral Load Suppression in Children-STUDY UNICEF-2021Document34 pagesViral Load Suppression in Children-STUDY UNICEF-2021Desmond OtienoNo ratings yet
- FLUID & Electrolyte ManagementDocument49 pagesFLUID & Electrolyte ManagementYovitaNo ratings yet
- Chronic Suppurative Otitis Media Chronic Suppurative Otitis MediaDocument34 pagesChronic Suppurative Otitis Media Chronic Suppurative Otitis MediaMariappan RdNo ratings yet
- Cover LetterDocument1 pageCover Letterapi-530730346No ratings yet
- Alzheimers Disease Power Point Presentation FileDocument10 pagesAlzheimers Disease Power Point Presentation Filejoseph ndung'uNo ratings yet
- Allyson Lods ResumeDocument2 pagesAllyson Lods Resumeapi-301787076No ratings yet
- Approach To Neurologic InfectionsDocument18 pagesApproach To Neurologic InfectionsHabib G. Moutran Barroso100% (1)
- Ped CardioDocument18 pagesPed CardioIdioness100% (1)
- Our Lady of Fatima UniversityDocument7 pagesOur Lady of Fatima UniversityJess SyNo ratings yet
- Anemiile HemoliticeDocument4 pagesAnemiile HemoliticeIoana GalNo ratings yet
- Annexure 42 - Counselling Checklists-NewDocument18 pagesAnnexure 42 - Counselling Checklists-NewJay PaulNo ratings yet
- Name Age Gender Ic No/Passport Mysejahtera User Id Contact NumberDocument12 pagesName Age Gender Ic No/Passport Mysejahtera User Id Contact NumberAtuk golden fried chickenNo ratings yet
- NCP BurnDocument9 pagesNCP Burnbanyenye2533% (3)
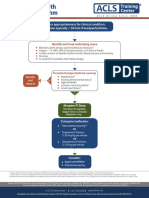
- Assess Appropriateness For Clinical Condition. Heart Rate Typically 50/min If BradyarrhythmiaDocument1 pageAssess Appropriateness For Clinical Condition. Heart Rate Typically 50/min If BradyarrhythmiaatikaNo ratings yet
- Injections - IdDocument3 pagesInjections - IdMariya DantisNo ratings yet
- FilariaDocument65 pagesFilarialunaghilvin2026No ratings yet
- A History of Medical Device Regulation & Oversight in The United States - FDADocument7 pagesA History of Medical Device Regulation & Oversight in The United States - FDAHector Tinoco GarciaNo ratings yet
- Pelvic Anatomy Slides FINALDocument36 pagesPelvic Anatomy Slides FINALRajashekharNo ratings yet
- 10 Things That Stopped My Thyroid Hair LossDocument115 pages10 Things That Stopped My Thyroid Hair LossAnonymous vI4dpAhcNo ratings yet
- The Lack of Physicians' Familiarity With LGBT Health and Its ConsequencesDocument13 pagesThe Lack of Physicians' Familiarity With LGBT Health and Its ConsequencesZachary ZydonikNo ratings yet