Professional Documents
Culture Documents
1 The Role of Computed Tomography As A Prognostic Tool in Traumatic Brain Trauma - Imaging in Medicine
1 The Role of Computed Tomography As A Prognostic Tool in Traumatic Brain Trauma - Imaging in Medicine
Uploaded by
cral1124Original Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
1 The Role of Computed Tomography As A Prognostic Tool in Traumatic Brain Trauma - Imaging in Medicine
1 The Role of Computed Tomography As A Prognostic Tool in Traumatic Brain Trauma - Imaging in Medicine
Uploaded by
cral1124Copyright:
Available Formats
RESEARCH PAPER
The role of computed tomography as
a prognostic tool in traumatic brain
trauma
Traumatic brain injury (TBI) is a critical public health problem. It represents one of the most important medical-
surgical pathology worldwide. The occurrence indicate that this kind of injury cause a large number of deaths and
impairments leading to permanent disabilities, that is why is necessary to triage the patient and identify the injury
extension. Imaging has become a significant tool not only in the diagnosis of patients with TBI, but also as a patient
outcome predictor. This review of literature provides evidence of the current state of TBI imaging as to what is
considered to be the indications, benefits and limitations of computed tomography (CT).
KEYWORDS: computed tomography traumatic brain injury prognosis
25 using PubMed and EMBASE databases. Search Cristian Rincon-Guio1,
Introduction
terms used included “traumatic brain injury” Ana M Gómez2 & José D
Traumatic brain injury (TBI) is defined as any
and “computed tomography” and “prognosis”. Charry3*
structural skull traumatic injury with alterations
Search was filtered for articles in English, on
of cerebral physiology as a result of an external 1
Department of Engineering,
human subjects and published in the last ten Fundación Universitaria Navarra-
force either in the form of mechanical energy, Uninavarra, Colombia
years. Articles were assessed based on information
chemical, electrical or thermal heating [1]. Department of Health Science,
gleaned from the titles and abstracts initially. If 2
Fundación Universitaria Navarra-
The annual incidence of TBI in the United they seemed appropriate for the purpose of this Uninavarra, Colombia
States is frequently stated to be 200 cases per review, complete articles were obtained for further 3
Research Department, Fundación
100,000 people [2]. In low- and medium- assessment. References from these selected papers Universitaria Navarra- Uninavarra,
Colombia
income countries, burden of disease is quite were also examined to identify any article which
*Author for correspondence:
high and the few available data do not identify could be included in this study.
danielcharry06@gmail.com
the extent of the problem [3]. The main inclusion criteria were the used of
Brain imaging is crucial in the attention of computed tomography in traumatic brain injury,
patients who suffer traumatic brain injury. clinical findings and outcome. Studies included
Computed tomography (CT) is recommended must have clearly definition to determine
for the initial assessment in the emergency diagnosis and prognosis in TBI by imaging.
services. It provides information and diagnosis Abstracts, case reports, molecular studies, and
to identify the need of surgery, but it also helps neurologic or psychiatry comorbidities like
in the following of the patient and the evolution dementia were excluded.
of pathology. Research suggests that CT can be
used to predict patient outcomes. [4,5]. Results
Based on the search terms mentioned before,
Many classifications have been proposed 45 papers were initially identified. Twenty
to predict clinical outcomes among patients papers were selected for further scrutiny of their
with traumatic brain injury using computed titles and abstracts. Upon further scrutiny, only
tomography, however there are still limitations 12 studies met the inclusion criteria of this
to find the best tool to perform an accurate study. (FIGURE 1) illustrated the flow of paper
prognosis [6]. selection based on PRISMA guidelines.
Therefore, this review aims to assess the The studies characteristics are name in
current literature on the role of Computed (TABLE 1), taking into account the title, the
tomography and the classifications available to name of the author, year and study purpose.
predict outcome in traumatic brain injury. History of computed tomography
The development of CT is the result of the
Methods
observations and theoretical correlations of
A literature search was performed in October
ISSN 1755-5191 Imaging Med. (2017) 9(6) 171
RESEARCH PAPER Rincon-Guio, Gómez, Charry
Figure 1. PRISMA flow diagram.
many men throughout history, from Democritus
reaching Comarck’s ideas, until Hounsfield’s
advance of a practical device in the late 1960s [19].
The first clinical CT on a patient took
place on October 1971 at Atkinson Morley's
Hospital. An English woman with a suspected
frontal lobe tumor was scanned with a prototype
scanner, which produced an image with an 80
× 80 matrix, taking about 5 min for each scan
(FIGURE 2) with a similar time required to
process the image data [20].
CT device consists of a tube that emits
X-ray, which passes through the patient and
impresses the detectors on the opposite side.
The attenuated radiation that is received will
be the attenuation coefficients or "densities"
of the tissues, which will be interpreted by the
CT device as Hounsfield units (UH). This range
Figure 2. The first clinical scan: Atkinson Morley's
of attenuation varies between gray, from white Hospital, October 1971.
(hyperdense) to black (hypodense); CT device
can identify more than 2000 shades of gray, Crania CT allows to evaluate the tissues
while the human eye only 30 shades [21,22]. with very good resolution (FIGURE 3), even
Current CT scanners can produce images though there are some difficulties at the base
with a 1024 × 1024 matrix, acquiring data for a of the skull, due to the artifacts generated by
slice in less than 0.3 s and are an integral part of the bone tissue in the posterior fossa, which
a modern hospital's imaging resources. can be observed as hypodense bands, projected
172 Imaging Med. (2017) 9(6)
The role of computed tomography as a prognostic tool in traumatic brain trauma
RESEARCH PAPER
Table 1. Summary of study characteristics.
Title Authors Year Study purpose
Review recent advances in neuroimaging and discuss how they
Imaging brain trauma are
Josh et al. [7] 2010
Helping to address these fundamental gaps.
The use of functional and metabolic imaging modalities can
Structural imaging of mild traumatic
provide information on pathological changes in mild TBI patients
brain injury
that may not be detected by structural imaging.
May not be enough: overview of
Samuel et al. [8] Each modality’s advantages and disadvantages are compared,
functional and metabolic imaging of
2017 and potential future applications of using combined modalities
mild traumatic brain injury
are explored.
Review the current state of TBI imaging including its indications,
Imaging evaluation of acute traumatic
Christopher et al. benefits and limitations of the modalities, imaging protocols, and
brain injury 2016
[9] imaging findings for each these pathoanatomic entities.
Current and future diagnostic The review is divided up into assessments based on specific goals,
tools for traumatic brain injury: CT, rather than based on scan modalities. It is not meant to supplant
conventional MRI, and diffusion David et al. [10] but rather to supplement the authoritative previous works on
2015
tensor imaging this topic.
This article identifies emerging neuroimaging measures
considered by the inter-agency Pediatric Traumatic Brain Injury
Emerging imaging tools for use with (TBI) Neuroimaging Workgroup. This article attempts to address
traumatic brain injury research Jill et al. [11] some of the potential uses of more advanced forms of imaging
in TBI as well as highlight some of the current considerations and
2012
unresolved challenges of using them.
A systematic review of factors
contributing to outcomes in patients Review systematically factors contributing to outcomes in
with traumatic brain injury Kim [12] 2010 patients with traumatic brain injury.
Both CT and MRI can be used to prognosticate clinical outcome,
and there is particular interest in advanced applications of
Imaging for the diagnosis and both techniques that may greatly improve the sensitivity of
Kim et al. [13]
management of traumatic brain injury 2011 conventional CT and MRI for both the diagnosis and prognosis
of TBI
Decompressive craniectomy is an operative option for the
Outcome of patients with severe neurosurgeon in cases of generalized traumatic brain edema.
head injury after decompressive While the outcome of patients after decompressive craniectomy
Lemcke et al. [14] 2010
craniectomy is often poor, we tried to identify predictors of a favorable course
of the injury through GOS, CT and MRI.
Classifications based on the presence or absence of intracranial
local lesions, diffuse injury, signs of subarachnoid or
Classification and prediction of intraventricular haemorrhage and fractures or foreign bodies
outcome in traumatic brain injury are considered, and their predictive value is discussed. Future
based on computed tomographic Zhu et al. [15] studies should address the complicated issue of how optimally to
2009
imaging combine CT characteristics for prognostic purposes and how to
improve on currently used CT classifications to predict outcomes
more accurately.
Prognostic models for predicting outcome after severe traumatic
Prediction of outcome in severe brain injury (TBI) may be useful in several areas. However,
Menon and Zahed
traumatic brain injury established risk prediction models for general critical illness show
[16] 2009
significant limitations in neurotrauma.
Predicting outcome after traumatic
To develop and validate practical prognostic
brain injury: practical prognostic
MRC CRASH Trial models for death at 14 days and for death or severe disability six
models based on large cohort of 2007
Collaborators [17] months after traumatic brain injury.
international patients
CT is the initial diagnostic test in TBI. Conventional MR imaging
Imaging of traumatic brain injury 2015 in the acute phase is used as a problem solver when CT does not
Uttam et al. [18]
explain the neurologic deficit.
Imaging Med. (2017) 9(6) 173
RESEARCH PAPER Rincon-Guio, Gómez, Charry
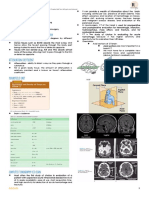
Figure 3. Current crania CT: A skull window and B brain tissue window.
Figure 4. Artifices in crania TC.
on the cerebellum. Other kinds of artifacts bone window if it is possible to position the
are due to patient movement, variations of patient for these. The crania CT provides a large
volume or presence of metal, which can cause amount of information and it has sensitivity
difficulties in diagnosis and lend themselves to for detection of acute hemorrhagic lesions for
misinterpretation, confusing these devices with surgical intervention, as long as it is used in a
images of hemorrhagic lesions (FIGURE 4). rational way under the indicate circumstances
[24-26].
The use of CT in TBI
Volume measurement is a determining factor
TBI represents a dynamic process with
for the management of intracranial lesions [27];
primary parenchymal damage from the moment
because of emergency surgery decisions are
of impact followed by a systemic response that
made for each type of collections or for cranial
involve local effects like hypoxia, hypotension,
decompression surgery to control cerebral
hypercarbia, brain swelling that combine lead to
edema.
secondary brain damage [1].
Volumetric measurements are performed by
Once determine the clinical state of the patient
the CT software and for its application use the
provides by the Glasgow Coma Scale (GCS)
following points (FIGURE 5).
(TABLE 2), it is necessary to assess the type of
injury and its extension using brain imaging 1. Identify slice where the lesion with the
[23]. The image recommended for the initial largest diameter is evident.
assessment of TBI in emergency services is crania - A=Larger diameter of the lesion.
CT. This must be requested in its two windows
(bone window and tissue window). Currently, - B=Larger diameter measured at 90°
available technology allows TC scan in a few from the previous diameter in the same
seconds, with cross-sectional, coronal, multi- section.
planar and three-dimensional reconstructions. - C=Number of sections of 1 cm where
In patients with fronto-ethmoidal fractures, it the lesion is evident. (Cuts larger than
is important to request coronal sections of the 1cm are usually made by technical
174 Imaging Med. (2017) 9(6)
The role of computed tomography as a prognostic tool in traumatic brain trauma
RESEARCH PAPER
Table 2. Glasgow coma scale.
Eye opening response Verbal response Motor response
4: Spontaneous 5: Oriented 6: Obeys commands
3: To verbal stimuli 4: Confused 5: Localizes pain
2: To pain 3: Inappropriate words 4: Withdraws from pain
1: None 2: Incoherent 3: Flexion to pain or decorticate
1: None 2: Extension to pain or decerebrate
1: None
Figure 5. Acute epidural hematoma in a crania CT, it shows the larger diameter (A) and its diameter
at 90 degrees (B). In the left, there is an intracerebral hematoma, showing the larger diameter (A)
and its diameter at 90 degrees (B). These images will be the basis to apply the rule of measurement
of blood volumes in the other sections to determine the value of C, according to the formula
Vm=(A × B × C)/2.
requirement in diagnostic images above The classification of the severity of the TBI
the posterior fossa). according to the Glasgow coma scale and the
Each section should be compared with the correlation with the CT images have allowed to
associate prognosis and surgical indications in a
base one where the measurements were taken,
better-standardized way. One of the most used
to find the rule:
is the Marshall CT classification (TABLE 3),
- Hemorrhage greater than 75% of the which allows to correlate tomographic patterns
initial section volume is counted as 1. of injury that produce an important morbidity
- Hemorrhage between 25 and 75% of the and mortality, including diffuse and focal
volume of the initial section is counted lesions. The Marshall CT classification is a valid
as half (1/2 section). instrument, which is based on the CT findings
on the status of the mesencephalic cisterns,
- Hemorrhage less than 25% with respect the degree of midline shift and the presence or
to the base section is not taken into absence of local mass lesions [27,28].
account.
Marshal classification has limitation in patients
In addition to measuring the volume, the with multiple injuries, and its applications is
presence of lesions that determine prognosis and not linear, which difficult its use for severity. In
an urgent intervention in diffuse pathologies the other hand Rotterdam score (TABLE 4) is
with cerebral edema should be reviewed: based only in CT findings such as the presence
- Midline shift. of subarachnoid or intraventricular hemorrhage,
effacement of the basilar cisterns, midline shift
- Presence of traumatic subarachnoid
>5 mm, presence of subdural hemorrhage, and
hemorrhage in the basal cisterns.
absence of epidural hemorrhage, in an effort to
- Obliteration of cisterns of the base. predict 6-month mortality [29].
Imaging Med. (2017) 9(6) 175
RESEARCH PAPER Rincon-Guio, Gómez, Charry
Table 3. Marshal classification of head injury (Trauma coma data bank).
Category Definition Mortality*
Diffuse injury I
No visible intracranial pathology on CT scan. 10%
(no visible pathology)
Cisterns present with midline shift </=5 mm and/or lesion
densities present, no high- or mixed-density lesion >25 cc, 14%
Diffuse injury II
may include bone fragments and foreign bodies.
Cisterns compressed or absent with midline shift </=5 mm,
Diffuse injury III 34%
no high- or mixed-density lesion >25 cc
Diffuse injury VI Midline shift >5 mm, no high- or mixed-density lesion >25 cc 56%
Evacuated mass lesion Any lesion surgically evacuated 39%
No evacuated mass lesion High- or mixed-density lesion >25 cc, not surgically evacuated 53%
*Mortality at discharge
Table 4. Rotterdam score.
Predictor Score
Basal Cistern
Normal 0
Compressed 1
Absent 2
Midline Shift
No shift or shift </=5 mm 0
Shift >5 mm 1
Epidural mass lesion
Present 0
Absent 1
Intraventricular blood or subarachnoid
hemorrhage
Absent 0
Present 1
Sum score +1
In the Rotterdam scoring system, 1 point is added as a sum score to make the Rotterdam grade
numerically total 6 points, consistent with the motor core of the Glasgow Coma Scale and the
Marshal classification. From Maas et al. [37]
Even other prognostic tools exist, the Marshall scan, MRI may be helpful [15].
and Rotterdam score are the well standardized
To evaluate prognosis Glasgow Outcome Scale
and validated with CT findings.
(GOS) can be used. It categorizes the outcomes
Discussion of patients after traumatic brain injury, as follows
[31]: 1. Death, 2. Persistent vegetative state:
Role of CT in prognosis
Minimal responsiveness, 3. Severe disability:
CT is the brain imaging of choice for the Conscious but disabled; dependent on others for
initial assessment of TBI because it is fast, widely daily support, 4. Moderate disability: Disabled
available, and highly accurate in the detection but independent; can work in sheltered setting,
of skull fractures and intracranial lesions like 5. Good recovery: Resumption of normal life
hemorrhages, herniation and hydrocephalus, despite minor deficits.
which may necessitate immediate surgical
evacuation. However, in case of concussion, However, there are other elements valuable in
the role of CT is less well defined [30]. CT is the prognosis of TBI patients. Kim [12] described
recommended in patients with neurological in his paper that older age, severe injury measured
deterioration following TBI; studies have shown by GCS or injury severity score (ISS), no pupil
little benefit for routine follow up imaging. In reaction, hypotension or hypertension, elevated
rare cases where the clinical presentation is far ICP, hypoxia, hypoglycemia or hyperglycemia,
worse than can be explained based on the CT hypothermia or hyperthermia, low level of
176 Imaging Med. (2017) 9(6)
The role of computed tomography as a prognostic tool in traumatic brain trauma
RESEARCH PAPER
hemoglobin, coagulopathy, high level of lactate, outcome. Finally, intracranial hemorrhage has
electrolyte derangement, high level of Marshall an approximately 80% positive predictive value
CT classification and presence of subarachnoid, for poor functional outcome, with prognosis
epidural or subdural hemorrhage were identified worsening as the hematoma volume increases in
as predictors for poor GOS outcome. Even size. Of note, mortality is higher in patients with
though, it is recommended that GCS should be acute subdural hematomas compared with those
serially assessed even after emergency department with epidural hematomas [13,32].
stabilization and evaluated in company with Lemcke et al. [14] studied the outcome
the computed tomography (CT) finding for an of patients with severe head injury after
accurate prognosis [12]. It is notable that the decompressive craniectomy and found that the
majority of studies for Marshal CT classification shift of the midline on CT was significantly
show that patients with diffuse brain injury correlated with the quality of outcome. Patients
(I) had good outcomes, whereas patients in- with a poor outcome (GOS 1-3) had a mean
group IV or V having a mass lesion on CT had midline shift of 9.8 ± 6.7 mm, whereas patients
unfavorable outcome. Given that, there is a with a good outcome (GOS4-5) showed a mean
very strong relationship between Marshall CT midline shift of 6.7 ± 5.0 mm. The important
classification and outcome. Future studies need predictive value of this factor has been confirmed
to focus on combining the CT characteristics by Marshall et al. among others. The visibility of
and other predictors for increasing the prognostic the basal cisterns was also shown in this study to
value [31]. be very significantly connected to the quality of
The primary role of CT scanning has been outcome at follow-up [32].
the acute identification of focal injuries that may It is important to recognize that Marshall CT
require emergent neurosurgical interventions, classification has been extensively evaluated and
such as extra-axial or parenchymal hemorrhage, it is considered as many studies have showed a
midline shift and incipient herniation. tool in the prognosis. Nevertheless a number
Approximately 10% of patients with severe TBI of other CT classifications exist [33-35], which
require a craniectomy based on the findings can be an interesting alternative to examine the
from an initial CT scan. According to the Brain elements that Marshall CT classifications do not
Trauma Foundation guidelines, these findings consider.
include extra-axial hematomas (epidural or
Zhu et al. [15] described how in 2005, a
subdural hemorrhages) larger than 30 mL in size
study by Maas et al. compared alternative CT
or associated with greater than 5 mm of midline
models with the Marshall CT classification and
shift and parenchymal hematomas in a non-
found it was preferable to use combinations
eloquent cortex greater than 20 mL in size [32].
of individual CT predictors rather than the
Kim and Gean [13] showed that individual
Marshall CT classification for prognostic
predictors of poor outcome on conventional CT
purposes in TBI [36]. Later in 2007, Maas et
include compressed or absent basilar cisterns, the
al. [37] again evaluated the prognostic value of
presence of subarachnoid hemorrhage, midline
CT scan characteristics in TBI and found that
shift, and intracranial hemorrhagic lesions
individual CT characteristics added substantially
(e.g. subdural or epidural hematomas, shear
to the prognostic value of the CT classification
injury, and contusions). Compressed or absent
alone. They found that making greater use of
basilar cisterns indicate a threefold higher risk
individual CT characteristics allowed them
of increased ICP and are associated with a two-
to improve on the already sizeable predictive
to three-fold increase in mortality. Traumatic value of the original Marshall CT classification
subarachnoid hemorrhage is associated with a scheme. These findings need to be corroborated
twofold increase in mortality, and hemorrhage in through further prospective investigations.
the basilar cisterns has a 70% positive predictive
value for poor outcome. Midline shift indicates Limitations
increased ICP and is similarly associated Gray and non-English literature was
with a poor clinical outcome, although this excluded. In this review study, a comparison of a
association is somewhat complicated by the new classification for the use of tomography as a
fact that midline shift is caused by intracranial prognosis was not proposed or made.
hemorrhage that also negatively impacts
Imaging Med. (2017) 9(6) 177
RESEARCH PAPER Rincon-Guio, Gómez, Charry
Conclusion can improve the predictive value on the outcome
Brain imaging gives a landscape in outcome; taking into account the CT findings.
the application of CT classifications can be
Disclosure
helpful in the prognosis of TBI. Nevertheless,
The authors declare that there is no conflict
many elements may be consider in the evaluation
of interest, financial or otherwise, regarding the
of imaging and the development of new scores
publication of this paper.
14. Lemcke J, Ahmadi S, Meier U. Outcome 27. https://goo.gl/AWSFCV
REFERENCES of patients with severe head injury after
1. h t t p : / / g p c . m i n s a l u d . g ov. c o / g p c _ s i t e s / decompressive craniectomy. Acta. Neurochir. 28. Steyerberg EW, Mushkudiani N, Perel P et al.
Repositorio/Conv_563/GPC_trauma_craneo/ Suppl. 106, 231-233 (2010). Predicting outcome after traumatic brain injury:
CPG_TBI_professionals.pdf Development and international validation
15. Zhu GW, Wang F, Liu WG. Classification and of prognostic scores based on admission
2. h t t p s : / / e m e d i c i n e . m e d s c a p e . c o m / prediction of outcome in traumatic brain injury characteristics. PLoS. Med. 5, 165 (2008).
article/433855-overview#a4) based on computed tomographic imaging. J. Int.
Med Res. 37, 983-995 (2009). 29. Stein SC, Fabbri A, Servadei F et al. A critical
3. Byass P, de Courten M, Graham WJ et al. comparison of clinical decision instruments for
Reflections on the global burden of disease 2010 16. Menon DK, Zahed C. Prediction of outcome in computed tomographic scanning in mild closed
estimates. PLoS. Med. 10, 1477 (2013). severe traumatic brain injury. Curr. Opin. Crit. traumatic brain injury in adolescents and adults.
4. Hassan Z, Smith M, Littlewood S et al. Head Care. 15, 437-441 (2009). Ann. Emerg. Med. 53, 180-188 (2009).
injuries: A study evaluating the impact of the 17. MRC CRASH Trial Collaborators. Predicting 30. Ro YS, Shin SD, Holmes JF et al. Comparison
NICE head injury guidelines. Emerg. Med. J. outcome after traumatic brain injury: Practical of clinical performance of cranial computed
22, 845-849 (2005). prognostic models based on large cohort of tomography rules in patients with minor head
5. Metting Z, Rödiger LA, De Keyser J et al. international patients. Patients. BMJ. 28, 336- injury: A multicenter prospective study. Acad.
Structural and functional neuroimaging in mild- 425 (2007). Emerg. Med. 18, 597-604 (2011).
to-moderate head injury. Lancet. Neurol. 6, 699- 18. Uttam KB, Chandler S, Jiachen Z et al. Imaging 31. The Brain Trauma Foundation. The American
710 (2007). of traumatic brain injury. Radiol. Clin. N. Am. Association of Neurological Surgeons. The
6. David T. Head injury: Triage, assessment, 53, 695-715 (2015). joint section on neurotrauma and critical
investigation and early management of head care. Computed tomography scan features. J.
19. Ambrose J. Computerized transverse axial Neurotrauma. 17, 597-627 (2000).
injury in children, young people and adults scanning (tomography)-2. Clinical applications.
(NICE guideline CG 176). Arch. Dis. Child. Br. J. Radiol. 46, 1023-1047 (1973). 32. Marshall LF, Gautille T, Klauber MR et al.
Educ. Pract. Ed. 100, 97-100 (2015). The outcome of severe closed head injury. J.
20. Hounsfield, GN. Computerised transverse Neurosurg. 75, 28-36 (1991).
7. Josh LD, Robert DS. Imaging brain trauma. axial scanning (tomography)-1. Description of
Curr. Opin. Crit. Care. 16, 92-97 (2010). system. Br. J. Radiol. 46, 1016-1022 (1973). 33. Azian AA, Nurulazman AA, Shuaib L et
8. Samuel SS, James WB, Edward CD et al. al: Computed tomography of the brain in
21. Abdalla MR, Rubiano AM. Basic anatomy predicting outcome of traumatic intracranial
Structural imaging of mild traumatic brain applied to the interpretation of axial tomography
injury may not be enough: Overview of haemorrhage in Malaysian patients. Acta.
of the brain in emergency medicine in: Godoy Neurochir. 143, 711-720 (2001).
functional and metabolic imaging of mild DA. Int. Care. Neurol. Neurosurg. 2, 27-51
traumatic brain injury. Brain. Imaging. Behav. (2013). 34. Teasdale G, Teasdale E, Hadley D. Computed
11, 591-610 (2017). tomographic and magnetic resonance imaging
22. http://docplayer.net/10707822-Ferne-emra- classification of head injury. J. Neurotrauma. 9,
9. Christopher AM, Jason FT, GeanA. Imaging 2009-mid-atlantic-emergency-medicine-
evaluation of acute traumatic brain injury. 249-257 (1992).
medical-student-symposium-abcs-of-head-
Neurosurg. Clin. N. Am. 27, 409-439 (2016). ct-interpretation-heather-m-prendergast-md- 35. Schreiber MA, Aoki N, Scott BG et al.
10. David LB, Christine LMD, Joshua SS. Current mph.html Determinants of mortality in patients with
and future diagnostic tools for traumatic brain severe blunt head injury. Arch. Surg. 137, 285-
23. Hawryluk GW, Manley GT. Classification of 290 (2002).
injury: CT, conventional MRI and diffusion traumatic brain injury: Past, present and future.
tensor imaging. Handb. Clin. Neurol. 127, 267- Handb. Clin. Neurol. 127, 15-21 (2015). 36. Maas AI, Hukkelhoven CW, Marshall LF et al.
275 (2015). Prediction of outcome in traumatic brain injury
24. Wei SC, Ulmer S, Lev MH et al. Value of coronal with computed tomographic characteristics: A
11. Jill VH, Elisabeth AW, Karen AT et al. Emerging reformations in the CT evaluation of acute head
imaging tools for use with traumatic brain injury comparison between the computed tomographic
trauma. Am. J. Neuroradiol. 31, 334-339 (2010). classification and combinations of computed
research. J. Neurotrauma. 29, 654-671 (2012).
25. Zacharia TT, Nguyen DD. Subtle pathology tomographic predictors. Neurosurg. 57, 1173-
12. Kim YJ. A systematic review of factors detection with multi-detector row coronal and 1182 (2005).
contributing to outcomes in patients with sagittal CT reformations in acute head trauma.
traumatic brain injury. J. Clin. Nurs. 20, 1518- 37. Maas AI, Steyerberg EW, Butcher I, et al.
Emerg. Radiol. 17, 97-102 (2010). Prognostic values of computerized tomography
1532 (2011).
26. Haacke EM, Mittal S, Wu Z et al. Susceptibility- scan characteristics in traumatic brain
13. Kim JJ, Gean AD. Imaging for the diagnosis weighted imaging: Technical aspects and clinical injury: Results from the IMPACT study. J.
and management of traumatic brain injury. applications, Part 1. Am. J. Neuroradiol. 30, 19- Neurotrauma. 24, 303-314 (2007).
Neurotherapeutics. 8, 39-53 (2011). 30 (2009).
178 Imaging Med. (2017) 9(6)
You might also like
- Machine Learning With Applications: Rajat Mehrotra, M.A. Ansari, Rajeev Agrawal, R.S. AnandDocument12 pagesMachine Learning With Applications: Rajat Mehrotra, M.A. Ansari, Rajeev Agrawal, R.S. AnandpavithrNo ratings yet
- JPM 10 00224 v3Document27 pagesJPM 10 00224 v3thouraya hadj hassenNo ratings yet
- Liew2 015Document3 pagesLiew2 015ThiagoSoaresNo ratings yet
- Texture Spectrum Coupled With Entropy and Homogeneity Image Fea-Tures For Myocardium Muscle CharacterizationDocument10 pagesTexture Spectrum Coupled With Entropy and Homogeneity Image Fea-Tures For Myocardium Muscle CharacterizationDimona MoldovanuNo ratings yet
- IJIRRDocument6 pagesIJIRRRajender RaoNo ratings yet
- 20 2 ImageDocument10 pages20 2 Imageakosuanyarko01No ratings yet
- 1 s2.0 S0010482522011131 MainDocument20 pages1 s2.0 S0010482522011131 MainZouhair MbarkiNo ratings yet
- A UWB Antenna For Microwave Brain ImagingDocument2 pagesA UWB Antenna For Microwave Brain ImagingPr eeTNo ratings yet
- Biomolecules 11 00090 v2Document4 pagesBiomolecules 11 00090 v2Windu KumaraNo ratings yet
- Paper RewriteDocument8 pagesPaper RewriteAsghar AliNo ratings yet
- JCM 10 02524Document11 pagesJCM 10 02524maribelNo ratings yet
- TAC en TraumaDocument9 pagesTAC en Traumasamuelfdiaz.0103No ratings yet
- Measurement Aging Atrophy CerebriDocument13 pagesMeasurement Aging Atrophy CerebriAnaqomNo ratings yet
- Image SegmentationDocument3 pagesImage SegmentationrajasekarNo ratings yet
- A Survey - Brain Tumor DetectionDocument14 pagesA Survey - Brain Tumor Detectionmunna.chalapathiNo ratings yet
- Application of An Improved U2 Net Model in UltrasoDocument9 pagesApplication of An Improved U2 Net Model in UltrasoNeon LeonNo ratings yet
- Basic Physical Principles and Clinical ApplicationDocument17 pagesBasic Physical Principles and Clinical ApplicationPopa Bogdan MihaiNo ratings yet
- Ieee 2Document15 pagesIeee 2mary sandros.jNo ratings yet
- Role of High Resolution Ultrasound in Assessment oDocument16 pagesRole of High Resolution Ultrasound in Assessment oilham Maulana ArifNo ratings yet
- Deep Learning For Chest X-Ray Analysis: A Survey: A A A A ADocument33 pagesDeep Learning For Chest X-Ray Analysis: A Survey: A A A A Amayank kumarNo ratings yet
- Rahayuddin 2019 J. Phys. Conf. Ser. 1341 082030Document7 pagesRahayuddin 2019 J. Phys. Conf. Ser. 1341 082030Saikat NandyNo ratings yet
- Diffusion Tensor Imaging, Intra-Operative Neurophysiological Monitoring and Small Craniotomy: Results in A Consecutive Series of 103 GliomasDocument11 pagesDiffusion Tensor Imaging, Intra-Operative Neurophysiological Monitoring and Small Craniotomy: Results in A Consecutive Series of 103 GliomasGeneration GenerationNo ratings yet
- An Efficient Visualization and Segmentation of Lung CT Scan Images For Early Diagnosis of CancerDocument5 pagesAn Efficient Visualization and Segmentation of Lung CT Scan Images For Early Diagnosis of Cancermaruthi631No ratings yet
- Karnan and LogeswariDocument9 pagesKarnan and LogeswariPrasanna ThiNo ratings yet
- A Deep Learning Model For Detection of Cervical SPDocument12 pagesA Deep Learning Model For Detection of Cervical SPOTSMANE ChaimaaNo ratings yet
- Review Bio Medical ImagingDocument23 pagesReview Bio Medical ImagingSweta TripathiNo ratings yet
- 10 1109@iccsp48568 2020 9182258Document4 pages10 1109@iccsp48568 2020 9182258mindaNo ratings yet
- Steady States and Stability Analysis of Brain Tumour Growth ModelDocument13 pagesSteady States and Stability Analysis of Brain Tumour Growth ModelInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Project Report On Primitive Diagnosis of Respiratory Diseases - Google Docs1Document13 pagesProject Report On Primitive Diagnosis of Respiratory Diseases - Google Docs1sasanknakka9No ratings yet
- Brain Tumor Diagnosis Using Machine Learning, Convolutional Neural Networks, Capsule Neural Networks and Vision Transformers, Applied To MRI: A SurveyDocument40 pagesBrain Tumor Diagnosis Using Machine Learning, Convolutional Neural Networks, Capsule Neural Networks and Vision Transformers, Applied To MRI: A Surveysumit2k4No ratings yet
- Review of MRI-based Brain Tumor Image Segmentation Using Deep Learning MethodsDocument8 pagesReview of MRI-based Brain Tumor Image Segmentation Using Deep Learning MethodsChandan MunirajuNo ratings yet
- Clinical Neurology and Neurosurgery: SciencedirectDocument15 pagesClinical Neurology and Neurosurgery: SciencedirectPedroNo ratings yet
- Deep Learning For Multigrade Brain Tumour Classification In-2Document18 pagesDeep Learning For Multigrade Brain Tumour Classification In-2j74770331No ratings yet
- Deep Learning Methods To Generate Synthetic CT From MRI in Radiotherapy A Literature ReviewDocument17 pagesDeep Learning Methods To Generate Synthetic CT From MRI in Radiotherapy A Literature ReviewColman SiuNo ratings yet
- Transfer Learning Based Deep Learning Framework For Identification of Type of Brain TumorDocument6 pagesTransfer Learning Based Deep Learning Framework For Identification of Type of Brain TumorTole SutiknoNo ratings yet
- The End of RadiologyDocument4 pagesThe End of RadiologyfreteerNo ratings yet
- Deep Learning and Artificial Intelligence in Radiology: Current Applications and Future DirectionsDocument4 pagesDeep Learning and Artificial Intelligence in Radiology: Current Applications and Future DirectionsFadhilWNo ratings yet
- IJMECE160531Document7 pagesIJMECE160531Senthil PNo ratings yet
- Brain Tumor and Glioma Grade Classification Using Gaussian Convolutional Neural NetworkDocument10 pagesBrain Tumor and Glioma Grade Classification Using Gaussian Convolutional Neural NetworkMohana LeelaNo ratings yet
- JNMT-2004-Seibert-X-ray Part 1Document10 pagesJNMT-2004-Seibert-X-ray Part 1Martin HaarbyeNo ratings yet
- KJN 12 47Document8 pagesKJN 12 47Khenza Nur HasanahNo ratings yet
- We Are Intechopen, The World'S Leading Publisher of Open Access Books Built by Scientists, For ScientistsDocument27 pagesWe Are Intechopen, The World'S Leading Publisher of Open Access Books Built by Scientists, For ScientistsMalikNo ratings yet
- Application of Physics in MedicineDocument9 pagesApplication of Physics in MedicineShreyash PolNo ratings yet
- Deep Learning For Brain Tumor Classification: A A A, C BDocument16 pagesDeep Learning For Brain Tumor Classification: A A A, C Bpuspa fr12No ratings yet
- Deep Learning Techniques For The Classification of Brain Tumor A Comprehensive SurveyDocument14 pagesDeep Learning Techniques For The Classification of Brain Tumor A Comprehensive SurveyManu KumarNo ratings yet
- Size of MCDocument11 pagesSize of MCFrancesco GualdiNo ratings yet
- Brain Tumor Detection and Classification Using IntDocument17 pagesBrain Tumor Detection and Classification Using IntZed LolNo ratings yet
- Pola Cco 2013Document3 pagesPola Cco 2013akivaNo ratings yet
- Diagnostics 11 01589 v2Document19 pagesDiagnostics 11 01589 v2sekharraoNo ratings yet
- Imaging For Neuro-Ophthalmic and Orbital Disease - A ReviewDocument24 pagesImaging For Neuro-Ophthalmic and Orbital Disease - A ReviewMashhoor AlfayezNo ratings yet
- Differntiation of Spinal TB and Metastatic Spinal TumorDocument8 pagesDifferntiation of Spinal TB and Metastatic Spinal TumorWilly DannyNo ratings yet
- Measurement: SensorsDocument6 pagesMeasurement: SensorsMohana LeelaNo ratings yet
- Brain Stroke Computed Tomography Images Analysis Using Image Processing: A ReviewDocument12 pagesBrain Stroke Computed Tomography Images Analysis Using Image Processing: A ReviewIAES IJAINo ratings yet
- Abdominal Musculature Segmentation and Surface Prediction From CTDocument6 pagesAbdominal Musculature Segmentation and Surface Prediction From CTLuma GallacioNo ratings yet
- Diffusion-Weighted Imaging Guided RadiotherapyDocument17 pagesDiffusion-Weighted Imaging Guided RadiotherapyAlberto Osa GarcíaNo ratings yet
- Radiology in Forensic Medicine: From Identification to Post-mortem ImagingFrom EverandRadiology in Forensic Medicine: From Identification to Post-mortem ImagingGiuseppe Lo ReNo ratings yet
- Emergency Management of Subdural Hematoma: Corresponding Author: Abdulrahman Mubarak Almutairi - 0564804048Document3 pagesEmergency Management of Subdural Hematoma: Corresponding Author: Abdulrahman Mubarak Almutairi - 0564804048Falon PapalangiNo ratings yet
- CV DR Dehnadi 14 Nov 22Document5 pagesCV DR Dehnadi 14 Nov 22mohammadrezahajian12191No ratings yet
- Mrcs NeurosurgeryDocument28 pagesMrcs NeurosurgeryAdebisiNo ratings yet
- DR Nachiket Vijay PotdarDocument42 pagesDR Nachiket Vijay PotdarNachiket Vijay PotdarNo ratings yet
- CT Scan NotesDocument97 pagesCT Scan NotesMr. Hrisab DebNo ratings yet
- Head TraumaDocument32 pagesHead TraumacokarisaNo ratings yet
- Intracranial HemorrhageDocument6 pagesIntracranial HemorrhagezuliaahmadNo ratings yet
- Basic Approch To CT BrainDocument62 pagesBasic Approch To CT BrainS B SayedNo ratings yet
- Skripsi Tanpa Pembahasan PDFDocument63 pagesSkripsi Tanpa Pembahasan PDFYudha NurulNo ratings yet
- (Ebook PDF) Emergency Radiology: The Requisites Second Edition. Edition Lucey - Ebook PDF All ChapterDocument69 pages(Ebook PDF) Emergency Radiology: The Requisites Second Edition. Edition Lucey - Ebook PDF All Chapterkukuiavfach2100% (22)
- Acute Subdural Hematoma Morbidity, Mortality and Operative TimingDocument7 pagesAcute Subdural Hematoma Morbidity, Mortality and Operative TimingNadia BordaşNo ratings yet
- Ped. SurgeryDocument262 pagesPed. SurgeryXerox medNo ratings yet
- FSM Final Doubts Shuvro DaDocument33 pagesFSM Final Doubts Shuvro DaSumanNo ratings yet
- Head Injury .Document26 pagesHead Injury .Lenjun100% (4)
- Acute Mild Traumatic Brain Injury (Concussion) in Adults - UpToDateDocument46 pagesAcute Mild Traumatic Brain Injury (Concussion) in Adults - UpToDateSinuhé RodríguezNo ratings yet
- Craniotomy CHR SDHDocument3 pagesCraniotomy CHR SDHAnnisa RahimNo ratings yet
- Rilley's Head Injury CompleteDocument492 pagesRilley's Head Injury CompleteAgung Anom Arie Wiradana100% (1)
- Yesterday's Tomorrow - Suvika PDFDocument223 pagesYesterday's Tomorrow - Suvika PDFSindhu Jhaveri100% (2)
- Stroke - Wikipedia, The Free EncyclopediaDocument31 pagesStroke - Wikipedia, The Free EncyclopediaRhonskiiNo ratings yet
- Neuropathology NotesDocument3 pagesNeuropathology NotesYağışBeyNo ratings yet
- Subdural HematomaDocument20 pagesSubdural HematomaArief Zamir100% (1)
- Insignis Surgery NeurosurgeryDocument15 pagesInsignis Surgery NeurosurgeryAla'a Emerald AguamNo ratings yet
- P R S S P: CT Kepala, Menyangkut Penyakit-PenyakitDocument76 pagesP R S S P: CT Kepala, Menyangkut Penyakit-Penyakitranz ibonkNo ratings yet
- PDF Emergency Radiology The Requisites Second Edition Edition Lucey Ebook Full ChapterDocument53 pagesPDF Emergency Radiology The Requisites Second Edition Edition Lucey Ebook Full Chapterlamar.jones949100% (5)
- CT Scan BasicsDocument28 pagesCT Scan BasicsPauline Burgos100% (1)
- 12 SeventhproblemDocument52 pages12 SeventhproblemAlicia TjinNo ratings yet
- MCN Week 16 17 BookDocument115 pagesMCN Week 16 17 BookJesena SalveNo ratings yet
- Subdural HematomaDocument8 pagesSubdural HematomaaaronmanullangNo ratings yet
- Pseudo-Subarachnoid Hemorrhage: A Potential Imaging PitfallDocument7 pagesPseudo-Subarachnoid Hemorrhage: A Potential Imaging PitfallNona HenNo ratings yet
- Head Injury PPT 160219094543Document49 pagesHead Injury PPT 160219094543Claire De VeraNo ratings yet