Professional Documents
Culture Documents
Lecture Notes - BIOS 1168 Functional Musculoskeletal Anatomy A Revision (Sydney)
Lecture Notes - BIOS 1168 Functional Musculoskeletal Anatomy A Revision (Sydney)
Uploaded by
SK AuOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Lecture Notes - BIOS 1168 Functional Musculoskeletal Anatomy A Revision (Sydney)
Lecture Notes - BIOS 1168 Functional Musculoskeletal Anatomy A Revision (Sydney)
Uploaded by
SK AuCopyright:
Available Formats
lOMoARcPSD|1668352
Bios1168 Functional Musculoskeletal Anatomy A Revision - 1
Functional Musculoskeletal Anatomy A (University of Sydney)
StuDocu is not sponsored or endorsed by any college or university
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
BIOS1168 Functional Musculoskeletal Anatomy A
Module 1 – Introduction, Soft Tissues, Shoulder and Elbow Regions
1. Introduction to Anatomy and Osteology
Objectives
1.1 Define the anatomical position
The erect position of the body with the face, eyes and toes directed forward, the
arms at the side, and the palms of the hands facing forward, used as a reference in
describing the relation of body parts to one another.
1.2 Define the following terms of position and direction which are related to the
standardised anatomical position:
I. Sagittal plane
The longitudinal plane that divides the body
into right and left portions. This does not have
to occur symmetrically.
II. Median (midsagittal) plane
A longitudinal plane along the midline of the
body dividing the body into right and left
halves. This creates symmetrical halves.
III. Coronal (frontal) plane
A longitudinal plane at right angles to a sagittal
plane, dividing the body into anterior and
posterior portions.
I. Horizontal (transverse) plane
A latitudinal plane passing horizontally through
the body, at right angles to the sagittal and
coronal planes, and dividing the body into
upper and lower portions.
II. Anterior (ventral)
Situated on the front surface the body.
Posterior (dorsal)
Situated on the rear surface of the body.
III. Superior (cephalic)
Situated on the upper region of the body.
Inferior (caudal)
Situated on the lower region of the body.
IV. Proximal
Away from the midline/trunk/origin of the body.
Usually regarding limbs.
Distal
Toward the midline/trunk/origin of the body. Usually
regarding limbs.
V. Medial
Situated toward the midline of the body.
Lateral
Situated away from the midline of the body.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
VI. Superficial
Nearer to the surface of the body.
Deep
Away from the surface of the body.
VII. Unilateral
On one side of the body, relative to the midline.
Bilateral
On both sides of the body, relative to the midline.
Ipsilateral
Pertaining to the same side
Contralateral
Pertaining to the opposite side.
1.3 List the major bones comprising the two divisions of the skeleton: the
appendicular and axial divisions.
Axial Skeleton
Cranium, mandible, hyoid bone, ear ossicles, rib cage, vertebral column.
Appendicular Skeleton
Pelvic girdle and lower limbs – pelvis, femur, tibia, fibula, patella, tarsals,
metatarsals and phalanges.
Shoulder girdle and upper limbs – scapula, clavicle, humerus, ulna, radius, carpals,
metacarpals, phalanges.
1.4 List five functions of the skeleton.
1. Protect vital organs
2. Support the body
3. Provide a basis for movement
4. Produce red blood cells
5. Store minerals
1.5 Classify bones according to shape and give an example of each type.
1. Short
Cancellous bone (spongy) covered by compact bone
eg. Carpals
2. Long
Shaft comprised of compact bone with ends comprised of cancellous
bone
eg. Femur
3. Flat
Layer of cancellous bone surrounded by compact bone. No bone
marrow cavity.
eg. Scapula
4. Irregular
Cancellous bone surrounded by compact bone
eg. Vertebrae
5. Sesamoid
Embedded in tendons and increase the efficiency of muscle
movement
eg. Patella
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
1.6 Illustrate the following features of a typical long bone: diaphysis, epiphysis,
metaphysis, articular surfaces.
1.7 Describe and state the functions of bone markings (bony projections and
depressions) and find an example of each type of marking.
Function of irregularities/bone markings:
1. Strengthen bone
2. Provide passage through bone
3. Promote bone to bone articulation
4. Provide attachment sites
5. Provide surface landmarks
Types of bony projections:
1. Trochanter Very large round process
2. Tubercle Small round process
3. Tuberosity Roughened process
4. Head Single terminal enlargement
5. Condyle Knuckle shaped terminal enlargement
6. Epicondyle Projection above condyle
7. Crest Prominent ridge
8. Line Low ridge
9. Spine Sharp process
10. Ramus Process projecting from main part of the bone
Types of depressions
1. Facet Small, flat and smooth area
2. Fossa Socket on a bone
3. Fovea Small pit
4. Sulcus Groove on a bone
5. Foramen Hole through a bone
6. Meatus Canal in a bone
7. Fissure Slit through a bone
8. Sinus Cavity within a bone
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
9. Notch Deep indentation in a bone
Aims
At the end of this topic you should be able to:
a) Explain basic anatomical terms related to position and direction
b) State the divisions and functions of the skeleton
c) Classify bones
d) Describe and state the functions of bone markings
2. Introduction to Tissues (Histology) and Imaging Anatomy
Objectives
2.1 Define the terms ‘tissue’ and ‘organ’
‘Tissues’ are an aggregation of similarly specialized cells that together perform
specific, limited functions.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
‘Organs’ are mixtures of cellular tissues and their associated extracellular matrix.
They are a differentiated part of the body that performs various functions.
2.2 Briefly describe the main histological characteristics and general functions of the
four basic tissues of the body:
I. Epithelia
Histology
Made of many cells close to each other (little extracellular material
between cells).
No blood vessels within the epithelial layer.
Often characterized by frequent cell division because they are
exposed to wear and tear and injury, necessitating replacement.
Function
Protect underlying tissues against physical damage, drying out,
chemical injury and infection.
Allow and regulate the passage of materials (diffusion, absorption,
filtration, secretion, excretion) into and out of the deeper tissues of
the body which they cover or line.
Specialized epithelia form sensory parts of organs such as the eye,
ear, mouth (taste buds), and nose (olfactory epithelium).
Examples
Skin or inside/linings of passageways.
II. Connective tissue
Histology
Most abundant tissue
Cells of the connective tissues are far apart, separated by an abundant
amount of extracellular material, also called extracellular matrix.
The properties of the cells and the composition and arrangement of
the extracellular matrix elements vary tremendously, giving rise to an
amazing diversity of connective tissues, each uniquely adapted to
perform its specific function in the body.
Four classes: blood, bone, cartilage, and connective tissue.
Function
Binding, support and packaging of muscles, epithelia, nerves, and
organs.
Protection, defense and repair.
Insulation of adipose tissue.
Transportation through blood.
Examples
Cartilage, blood, bone, tendons and ligaments.
III. Muscle tissue
Histology
Made of many cells close together (there is little extracellular material
between muscle cells).
Well vascularized (lots of blood vessels).
Cells are elongated.
Cells contain myofilaments (contractile proteins).
Function
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Movement
Maintenance of posture
Joint stabilization
Heat generation
Examples
Skeletal, Smooth and Cardiac
IV. Neural tissue
Histology
Made of many cells packed closely together (little extracellular
material between cells).
Most of the cells are strongly branching.
Two main groups of cells:
NEURONS –
Respond to stimuli; conduct electrical impulses to and from all
body organs and from one area of the CNS to another.
GLIAL CELLS –
Support, protect and bind neurons.
Function
Regulates and controls body functions.
Constantly monitors changes occurring both inside and outside of the
body.
Processes and interprets information and makes decisions about what
should be done at each moment.
Carries the order of what should be done to muscles and glands.
Examples
The brain, spinal cord, nerves and their associated ganglia.
2.3 Describe how the following techniques may be used for imaging the basic
tissues:
I. Radiography (X-ray)
X-rays are a form of radiant energy which can penetrate the body. This
imaging creates pictures of bones and internal organs of the body. The
image is produced on photographic film (radiographs) or TV or computer
monitor. The x-ray images are able to show hard tissues (compact and
spongy bone) but have poor discrimination of soft tissues. They are also
limited as they only shows a two-dimensional view of the human body.
Structures are superimposed on top of one another (i.e. can’t tell if
looking from front or back).
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
II. Fluoroscopy
This method requires an injection of contrast material (eg. barium, iodine,
gadolinium). It is used to visualise the anatomy and function of joints
(arthrogram) and internal body organs. The images of the body are
displayed in “real time".
III. Computed tomography (CT)
This method involves computer reconstructed images, available in a
variety of body planes (3mm cross sectional ‘slices’). CT scans use x-rays
to produce an image which means the patient is exposure to radiation.
The images are always displayed as if viewer were at the supine (face up)
patient’s feet. There is greater discrimination of soft tissues than
conventional radiography (plain films). This therefore makes it good for
looking at shoulder joint space, cartilage, labrum and tendons. CT scans
are widely available, faster, cheaper and less likely to require person to be
sedated or anaesthetized.
IV. Magnetic resonance imaging (MRI)
In this method, powerful magnets and radiowaves are used to create a
magnetic field. It DOES NOT use x-rays. A computer reconstructs images
based on the distribution of hydrogen atoms in tissues. These images can
be in various planes of the body (3mm ‘slices’). The imaging is direct
without the use of contrast media, making this method good for soft
tissues around joints (e.g. ganglions, bursitis) and tumours. MRI’s are not
as widely available, slower, very expensive, person may need to be
sedated or anaethetised. There are no known side effects.
V. Bone Scans
Show images of specific organs following IV injection of trace amounts of
radioactive substances. These images can be viewed as the whole organ
or in cross sections. The degree of uptake of IV fluid is dependent on local
blood flow and rate of bone metabolic activity. Bone scans allows
screening of entire skeleton and can be used to diagnose: cancer, trauma,
degenerative disease, metabolic disease, prosthetic joint, and sports
injuries.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
VI. Ultrasound
Use high frequency sound waves. These reflected sound wave echo’s are
recorded and then displayed as a visual image (sonogram). This technique
enables the examination of complex joints (e.g. the shoulder) non-
invasively. Real-time images show movement, function and anatomy of
internal tissues and organs.
Aims
At the end of this topic you should be able to understand:
a) That organs of the body are a series of different specialised structures composed of
specific arrangements of only four basic tissues.
b) The role of anatomical imaging techniques in differentiating the basic tissue types.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
3. Bones of the Shoulder Region
Objectives
3.1 Identify and classify the humerus.
The humerus is the upper arm bone and is classified as a long bone. A long bone’s
length is superior to their width, and the bone consists of a shaft (diaphysis) and two
expanded ends (epiphysis).
3.2 On the humerus identify:
I. Proximal end:
a) Head*
Rounded, articulating surface which is contained within the joint
capsule.
b) Anatomical neck*
Margin of joint capsule
c) Surgical neck*
The narrow part distal to the tubercles
d) Greater tubercle*
Lateral and forms tip of shoulder
e) Lesser tubercle*
Anterior and medial
f) Intertubercular (bicipital) groove*
Superior
g) Medial lip of intertubercular groove*
Superior
h) Lateral lip of intertubercular groove*
Superior
II. Shaft:
a) (Spiral) groove for radial nerve
For Radial nerveand posterior to Deltoid tuberosity
b) Deltoid tuberosity*
A bulge in the shaft, which attaches to the deltoid muscle
III. Distal end:
a) Medial epicondyle*
Larger than lateral side.
b) Lateral epicondyle*
Small, tuberculated projection.
c) Capitulum*
Smooth, rounded projection articulates with head of radius.
d) Trochlea*
Medial portion of the articular surface articulates with the trochlear
notch on the ulna.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
III.3Relate the markings of the humerus (objective 3.2) to the planes of the body in
order to side (orientate) a disarticulated humerus.
Sagittal Plane Coronal Plane Transverse
Medial Lateral Anterior Posterio Superior Inferior
r
Head, Deltoid Coronoid Radial Head, Trochlea,
Medial tuberosity Fossa Groove Surgical Capitulum
Epicondyl , Neck
e Lateral
Epicondyl
e
III.4Identify and classify the other bones of the shoulder girdle: clavicle and scapula.
The scapula is the shoulder blade and is classified as a flat bone. It is broader than it
is long and triangular shaped, and it articulates with the arm and clavicle.
The clavicle is the collarbone and is classified at a long bone. Its length is superior to
its width and is s-shaped. It originates at the manubrium (sternal end) and
articulates with the scapulae (acromial end).
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
III.5On the scapula identify:
I. Costal surface
Concave and forms a large subscapular fossa which is an attachment for
fleshy muscle.
II. Dorsal surface
Convexand divided unevenly by spine of the scapula, supraspinous fossa
and infraspinous fossa, which are attachments for fleshy muscles.
III. Superior, medial and lateral borders*
Superior – top of scapula
Medial – opposite side where the humerus attaches
Lateral – same side where humerus attaches
IV. Superior, inferior and lateral angles*
Superior – top of scapula opposite side where humerus attaches
Inferior – bottom tip of scapula
Lateral – top of scapula same side where humerus attaches, lower Glenoid
fossa
V. Spine*
Long prominent ridge runs across the upper dorsal surface of the bone,
attachment for trapezius and deltoid muscles.
VI. Acromion process*
Flat expanded continuation of the spine, articulates with acromioclavicular
joint.
VII. Coracoid process*
Most anterior process, smaller projection for muscle and ligament
attachments.
VIII. Glenoid fossa*
Slightly concavity at the lateral angle, forms socket for humerus head.
IX. Subscapular, supraspinous and infraspinous fossae*
Subscapular fossa – slightly depressed region in middle of the anterior
surface.
Supraspinous fossa – slightly depressed area superior to the spine on dorsal
surface.
Infraspinous fossa – large slightly depressed area inferior to the spine.
X. Suprascapular notch*
Where the superior border joins base of coracoid process.
XI. Supraglenoid and infraglenoid tubercles*
Supraglenoid tubercle - Superior to Glenoid fossa, allows for muscle
attachment.
Infraglenoid tubercle - Inferior to Glenoid fossa, allows for muscle
attachment.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
III.6Relate the markings of the scapula (objective 3.5) to the planes of the body in
order to orientate a disarticulated scapula.
Sagittal Plane Coronal Plane Transverse
Medial Lateral Anterior Posterior Superior Inferior
Superior Glenoid Coracoid Spine, Glenoid Inferior
angle, Fossa, Process, Acromion Fossa, angle
Medial Acromion Subscapular Process Acromion
border Process Fossa Process
III.7On the clavicle identify:
I. Acromial end*
Lateral and superior, flattened process.
II. Sternal end*
Medial and superior, bulbous process.
III. Superior surface
Smooth subcutaneous, rough at its medial part.
IV. Inferior surface
Smooth subcutaneous, oval impression at medial end.
V. Roughened area for costoclavicular ligament
Inferior and medial, roughened process.
VI. Trapezoid line
Lateral and inferior, further lateral than the Conoid tubercle.
VII. Conoid tubercle
Lateral and inferior, less lateral than the trapezoid line.
VIII. Curvatures
Lateral 1/3 – concave forwards
Medial 2/3 - convex forwards
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
III.8Identify the bony features listed above on X-rays of the shoulder region.
Aims
At the end of this topic you should be able to:
a) Identify and classify the bones of the shoulder region.
b) State the functions of markings on the bones of the shoulder region.
c) Orientate (side) the bones of the shoulder region using bony markings.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
4. Introductory Athrology
Objectives
4.1 Define a joint (articulation).
A joint or articulation is a place in the body where two bones come together,
creating a location where movement (articulation) occurs.
4.2 Describe two (2) main functions of a joint.
1. To allow articulation between two or more bones – holding the skeleton
together.
2. To permit movement by contraction of attached muscles.
4.3 Describe the general structure of, and the relative amount of movement available
at, each of the following types of joints:
I. Fibrous
Fibrous material joins the bone ends together. The amount of movement
between the bones depends on the length of the fibres.
a) Suture
Immovable
E.g. Skull bone sutures
b) Syndesmosis
Slightly movable
E.g. Interosseous membrane between tibia and fibula
II. Cartilaginous
Cartilage tissue involved in joint.
a) Primary cartilaginous or synchondrosis
Hyaline cartilage
Immovable
E.g. Costochondral joint
b) Secondary cartilaginous or symphysis
Fibrocartilage
Slightly movable
E.g. Intervertebral disc
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
III. Synovial
Freely movable joints (most common type of joint)
Synovial Membrane - Lines joint capsule and produces synovial fluid.
Fibrous Joint Capsule – Unites bones creating synovial joint cavity.
Articular Cartilage – cover the bone ends within joint capsule, allows the
bones to slide on one another without friction.
Joint Cavity - Contains synovial fluid (a lubricant) which assists in frictionless
movement of bones and nutrients to cartilage.
4.4 Describe the factors which determine the amount of friction occurring between
articular surfaces during movement at synovial joints.
Co-efficient of friction – shear force (frictional resistance)
Compression force depends on:
I. Compressive load
II. Surfaces involved
III. Articular cartilage
IV. Lubricant synovial fluid
Examples:
I. Rubber tyre on dry road (CF = 1.0)
II. Ice skate on ice (CF = 0.03)
III. Cartilage on cartilage (CF = 0.02 – 0.001)
4.5 Describe the 3 principal axes of movement about synovial joints.
Plane Axis Movements Examples
Sagittal Transverse Flexion/Extension Shoulder/Hip
Side to Side
Coronal Anteroposterior Abduction/Adduction Shoulder/Hip
Front to Back
Transverse Vertical Medial/Lateral Shoulder/Hip
Rotation
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
4.6 Classify synovial joints according to:
I. Degrees of freedom
II. According to number of axes about which movement occurs:
Anteroposterior axis, Transverse axis, Longitudinal axis
a) Uniaxial
1°
b) Biaxial
2°
c) Multiaxial
3°
III. Structure
a) Hinge
Uniaxial
b) Pivot
Uniaxial
c) Ellipsoid
Biaxial
d) Condyloid
Biaxial
e) Saddle
Biaxial
f) Ball and socket
Multiaxial
g) Plane (gliding)
Multiaxial
4.7 List and identify examples of each type of joint in objectives 4.3 and 4.6
Fibrous Joint Cartilaginous Joint
Suture Syndesmosis Synchondrosis Symphysis
Cranium sutures Interosseous Costochondral Intervertebral
membrane joint (ribs and discs
between tibia and costal cartilage)
fibula (inferior
tibiofibular
articulation)
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Synovial Joints
Example Plane/Axis Movement
Hinge Interphalangeal Sagittal/Transverse Flex/Ext
Pivot Radioulna Transverse/ Pronate/Supinate
Vertical
Ellipsoid Radiocarpal Sagittal/Transverse Flex / Ext
Coronal/AP Add / Abd
Condyloid Metacarpophalangea Sagittal/Transverse Flex / Ext
l (MCP) Coronal/AP Add / Abd
Saddle Carpometacarpal of Sagittal/Transverse Flex / Ext
the thumb Coronal/AP Add / Abd
Ball and Socket Glenohumeral Sagittal/Transverse Flex / Ext
Coronal/AP Add / Abd
Transverse/ Rotation
Vertical
Plane (Gliding) Acromioclavicular Transverse/ Protract/Retract
Vertical Elevate/Depress
Coronal/AP Rotation
Sagittal/Transverse
4.8 Define and demonstrate the following types of movement about synovial joints:
I. Active
The movements that are produced by muscle contraction. These muscle
contractions create:
a) Angular movements
Flexion/extension Transverse axis
Adduction/abduction Anteroposterior axis
b) Rotational movements
Internal (medial)/external (lateral) Longitudinal axis
II. Passive
a) Physiological
The movements that are produced by an external force, but they can
be produced actively.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
b) Accessory
The movements that can’t be produced actively, it is the movement of
articular surfaces within the joint capsule. These movements are
generally rolling and gliding motions.
4.9 Define and demonstrate the terms used to describe active movement about
joints:
I. Flexion; extension
Movements occur in the sagittal plane – Transverse axis.
Flexion is the act of bending a joint or limb in the body by the action of
flexors. Flexors are located anteriorly (except for flexion of the knee –
posterior).
Extension is the act of straightening a joint of limb in the body by the action
of extensors. Extensors are located posteriorly (except for extension of the
knee – anterior).
II. Abduction; adduction
Movements occur in the coronal plane – Anteroposterior axis.
Adduction is the act of moving a joint or limb towards the midline of the
body by the action of adductors. Adductors are located inferiorly
(underneath).
Abduction is the act of moving a joint of limb away from the midline of the
body by the action of the abductors. Abductors are located superiorly (on
top).
III. Medial rotation; lateral rotation
Movements occur in the transverse plane – Vertical axis.
Medial rotation is the act of moving a joint or limb around its long axis
towards the midline of the body.
Lateral rotation is the act of moving a joint or limb around its long axis
towards the midline of the body.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
4.10 Relate active movements about joints to the anatomical planes and axes for
movement.
Plane Axis Movement
Sagittal Transverse Flexion/Extension
Coronal Anteroposterior Adduction/Abduction
Transverse Vertical Medial/Lateral Rotation
4.11 Explain the functions of ligaments:
I. Mechanical
a) Prevent unwanted movements at joints
Ligaments are restrictive and therefore are able to prevent unwanted
movements at joints that could cause damage or injury.
b) Limit wanted movements at joints
Ligaments are also assistive and therefore are able to limit wanted
movements at joints in order to allow movement whilst preventing
damage and injury.
II. Sensory (proprioceptive)
Ligaments are sensory organs and are responsible for the body’s perception
of the joint in space, including the joints position and movement
(proprioception).
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
4.12 Define and give an example of each of the following types of ligament:
I. Capsular
Ligaments that form part of the joint capsule.
Eg. The anterior, posterior and medial components of the sternoclavicular
ligament.
II. Extracapsular
Ligaments that lie outside the joint capsule.
Eg. Coracohumeral ligament.
III. Intracapsular
Ligaments that lie inside the joint capsule.
Eg. The ACL of the knee.
4.13 Define and list five (5) possible functions of articular discs.
Articular discs are fibrocartilaginous structures in some synovial joints.
The functions of these discs are to:
I. Act as shock absorbers
II. Aid mechanical fit between articular surfaces
III. Restrain movement
IV. Assist lubrication
V. Permit different movement to occur simultaneously at the joint
4.14 Define and list the functions of bursae.
Bursae are closed sacs of synovial membranes which contain synovial fluid, situated
in tissues where friction would otherwise occur.
Its functions are to:
I. Cushion space between bones and tendons and/or muscles.
II. Reduces friction between bones, allowing free movement.
III. Produce synovial fluid
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
4.15 Identify examples of different ligament and disc types as listed in 4.12 and 4.13.
Extracapsular Capsular Intracapsular
Coracohumeral ligament The anterior, posterior The ACL of the knee.
and medial components
of the sternoclavicular
ligament.
Aims
At the end of this topic you should be able to understand the:
a) Definition of a joint.
b) System of joint classification.
c) Terms used to describe movements at joints.
d) Structure and function of the components of synovial joints.
5. Joints of the Shoulder Region
Objectives
5.1 Classify the shoulder (glenohumeral) joint and identify and/or describe its:
The glenohumeral joint is a synovial, multiaxial, ball and socket joint. Its function is
to move the hand in different positions. It permits greatest range of motion of any
joint. The shoulder demonstrates that stability must be sacrificed for mobility.
Movements that occur at the glenohumeral joint:
I. Flexion/extension (transverse axis),
160˚/50˚
II. Adduction/abduction (anteroposterior axis)
160˚/30˚
III. Medial and lateral rotation (longitudinal axis).
>90˚/80˚
I. Articular surfaces
a) Humeral Head
- ½ sphere that is 3 times size of glenoid fossa.
- Only 25-30% contact (allowing greater mobility)
b) Glenoid fossa
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
- Glenoid labrum - fibrous structure around glenoid fossa increases
Glenoid concavity.
- Facilitates mobility
II. Glenoid labrum
Fibrous structure around glenoid fossa. It facilitates mobility by protecting
the edges of the fossa and creates double the depth of the glenoid cavity to
create stability. This therefore increases the glenoid concavity, and also
provides attachment for joint capsule, ligaments, muscles.
III. Joint capsule
The joint capsule is very thin and lax (loose) to facility mobility
(compromises stability). On the scapula, the capsule attaches to the glenoid
labrum. On the humerus, the capsule attaches to the anatomical neck
(reflected inferiorly onto the medial shaft). The joint is reinforced by: the
rotator cuff tendons and the glenohumeral and coracohumeral ligaments
(capsular ligaments). It communicates with: subscapula bursa,
intertubercular groove, and the synovial membrane of the joint is
continuous with these two.
IV. Synovial membrane
Lines joint capsule and bony surfaces inside joint capsule which are not
covered by articular cartilage. Also secretes synovial fluid which lubricates
the joint.
V. Ligaments:
a) Coracohumeral
Ligament joining the coracoid process to the humeral head.
Capsular is the distal part and extracapsular is the proximal part. In the
upper limb pendant position, the glenoid fossa is directed superiorly and
laterally. Prevents lateral and therefore inferior dislocation of the
humerus.
b) Glenohumeral
Capsular ligament
Superior
Prevents lateral, and therefore inferior dislocation of the humerus.
Limits external rotation.
Middle
Limits external rotation. 30% of people do not have this part.
Inferior
Prevents anterior dislocation of the humerus when fulled
flexed/abducted. Usually best developed of the three ligaments.
c) Coracoacromial
Extracapsular ligament joining the coracoid process and the acromion.
Prevents superior dislocation of the humerus. Very thick and strong.
d) Transverse humeral
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Capsular ligament joining the greater and lesser tubercles on the upper
end of the intertubercular groove (humerus). Keeps the long head of the
biceps brachii in the intertubercular groove.
5.2 Identify and state the functions of the glenoid labrum.
4mm thick fibrous structure around the glenoid fossa.
Functions:
I. Increases glenoid concavity i.e. deepens the glenoid fossa slightly.
II. Faciliates movement – allows the humerus to move the joint without
damaging the rim.
III. Provides attachment for joint capsule, ligaments and muscles.
5.3 Describe the precise direction in which the glenoid fossa faces when the upper
limb is in the anatomical position (i.e. pendant position) and explain the
significance of this alignment.
Glenoid fossa faces laterally, anteriorly and slightly superiorly due to the orientation
of the humeral head. This is so the scapula can move and allow largest range of
movement of the shoulder. Its position assists in preventing inferior dislocation of
the humerus.
5.4 State the specific mechanical function(s) of the ligaments listed in objective 5.1(v)
ligaments.
Structure Mechanical Function
Glenoid Labrum Facilitates mobility by protecting the
fossa when the humerus glides.
Slightly increases the concavity of the
glenoid cavity.
Provides attachment for joint capsule,
ligaments, muscles.
Coracoacromial ligament Prevents superior dislocation of humerus
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Coracohumeral ligament Prevents lateral and therefore inferior
dislocation of humerus
Superior glenohumeral ligament Prevents lateral and therefore inferior
dislocation of humerus
Limits external rotation
Middle glenohumeral ligament Limits external rotation
Inferior glenohumeral ligament Prevents anterior dislocation of humerus
when fully flexed/abducted.
Transverse humeral ligament Keeps long head of biceps brachii in the
bicipital (intertubercular) groove.
Does not actually limit movement – not
a real ligament, no mechanical function.
5.5 Describe the relationship of the subacromial and subscapular bursae with the
cavity of the shoulder (glenohumeral) joint.
Subacromial bursa:
I. Non-communicating with the cavity of the shoulder.
II. Lies between, and separates, the coracoacromial arch and deltoid from the
superolateral part of the shoulder joint.
III. Acts to prevent friction between the bony projections of the scapula
(acromion and coracoid process) and the joint capsule and its ligaments.
Subscapular bursa:
I. Communicates with the shoulder as the synovial membrane of the bursa is
continuous with the joint cavity’s synovial membrane.
II. Lies between the joint capsule and subscapularis tendon.
III. Acts to prevent friction between the Subscapularis and bony projections of
the scapula and RC muscles.
5.6 Define and demonstrate movements at the shoulder joint and movements of the
scapula.
Movements at the shoulder joint:
I. Flexion and extension (transverse axis)
II. Abduction and adduction (AP axis)
III. Medial (internal) and lateral (external) rotation (longitudinal axis)
Movements at the scapula:
I. Elevation and depression (coronal plane) – glenoid fossa moves up or down.
II. Protraction (sagittal plane) – glenoid fossa faces forward.
III. Retraction (sagittal plane) – glenoid fossa faces more laterally.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
IV. Medial rotation – rotation of scapula so that the inferior angle moves
towards the midline.
V. Lateral rotation – rotation of scapula so that the inferior angle moves away
from midline.
5.7 Describe the relationship between scapular and clavicular movements.
All movements of the scapula involve movement at both the AC and SC joints. The
scapula rotates superiorly when you abduct the humerus > 90˚.
When the scapular laterally rotates, the coracoclavicular ligament becomes taut and
rotates the clavicle (anterior surface goes up).
Any impairment of the clavicle to rotate at either end joints will interfere with the
free movement of the shoulder blade and upper limb as a whole.
5.8 Identify and classify the joints of the shoulder girdle:
I. Sternoclavicular joint
Synovial, multiaxial and plane (gliding).
II. Acromioclavicular joint
Synovial, multiaxial and plane (gliding).
5.9 At the sternoclavicular joint identify and/or describe its:
I. Articular surfaces
The sternal (medial) end of clavicle articulates with the clavicular notch of
sternum and the costal cartilage of 1st rib.
II. Joint capsule and synovial membrane
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
The joint capsule is strong and reinforced by capsular ligaments. An intra-
articular disc (vertical disc) divides the joint cavity into medial and lateral
compartments, resulting in two separate synovial membranes. This disc acts
as a shock absorber.
III. Articular disc
Intra-articular; fibrocartilaginous; vertical disc. It divides the joint cavity into
medial and lateral cavities. Attached to joint capsule; superiorly and
posterior to the upper border of the sternal end of the clavicle; and
inferiorly to the 1st costal cartilage.
Functions:
a) Improves congruency and acts as a shock absorber
b) Prevents superior dislocation of the clavicle.
c) Acts as a ‘pivot’ about which elevation and depression occur.
IV. Ligaments
a) Costoclavicular
Extracapsular ligament attached to 1st costal cartilage and the sternal
end of the clavicle - bilaminar (two-layered).
It prevents superior dislocation of the humerus by limiting elevation of
the clavicle. Limits retraction – anterior layer. Limits protraction –
posterior layer.
b) Sternoclavicular
Anterior sternoclavicular (capsular):
Attached to the superior and anterior parts of the sternal end of the
clavicle, and to the front of the upper part of the manubrium (upper
part of the sternum).
Limits retraction.
Posterior sternoclavicular (capsular):
Attached to the superior and posterior parts of the sternal end of
the clavicle, and to the back of the upper part of the manubrium.
Limits protraction.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
5.10 At the acromioclavicular joint identify and/or describe its:
I. Articular surfaces
Acromial (lateral) end of the clavicle and anteromedial border of acromion
process.
II. Joint capsule and synovial membrane
Joint capsule is loose allowing a greater range of gliding movement. The
joint is reinforced by capsular ligaments.
An intra-articular, fibrocartilaginous disc partially divides the cavity. The disc
is attached to the upper inner part of the capsule and dips down between
the two articulating surfaces. The synovial membrane lines the inner surface
of the capsule attaching the margins of the articular surfaces.
III. Coracoclavicular ligament
This ligament is extremely powerful. It attaches to the acromial end of
clavicle and to coracoid process of the scapula. It is medial to the AC joint.
a) Conoid part
Extracapsular ligament that is located vertically and posteromedially. It
prevents superior dislocation of the clavicle and limits protraction of
scapula. It produces (posterior) axial rotation of the clavicle.
When the arm abducts, clavicle rotates back (posterior axial
rotation).
When the arm adducts, clavicle rotates forward (anterior axial
rotation).
Coordinates movement of scapula with the clavicle.
b) Trapezoid part
Extracapsular ligament that is oblique. It limits retraction of scapula and
prevents superior and lateral dislocation of the clavicle.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
5.11 State the specific mechanical function(s) of the ligaments listed in objectives 5.9
and 5.10.
Ligament Mechanical Function
Costoclavicular Limits elevation of clavicle
Limits protraction
Limits retraction
Anterior sternoclavicular Limits retraction
Posterior sternoclavicular Limits protraction
Interclavicular Limits retraction
Conoid part of coracoclavicular Limits superior movement of
clavicle
Limits protraction of scapula
Produces axial rotation of clavicle
(unusual – produces movement)
Trapezoid part of coracoclavicular Limits retraction of scapula
Prevents lateral dislocation of
clavicle
5.12 List the ligaments which attach to the:
I. Coracoid process of the scapula
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Coracoacromial ligament
Coracohumeral ligament
Coracoclavicular ligament
II. Acromion process of the scapula
Coracoacromial ligament
III. Glenoid labrum
Glenohumeral ligament
IV. Greater tubercle of the humerus.
Coracohumeral ligament
Glenohumeral ligament
Transverse humeral ligament
Aims
At the end of this topic you should be able to:
a) Identify, classify and describe the specific structure and movements of all the joints
of the shoulder region.
b) Identify and state the mechanical functions of the ligaments of the joints of the
shoulder region.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
6. Introductory Myology
Objectives
6.1 Describe the following types of external appearance (form) of skeletal muscles:
I. Parallel
These are the muscle fibres that run from one attachment of muscle to the
skeleton to the other attachment (i.e. parallel to the line of pull of muscle
organ)
a) Strap
Long and thin muscle fibres.
b) Fusiform
Bulging muscle fibres.
c) Triangular (radiate)
Triangular shaped muscle fibres.
d) Flat (quadrilateral)
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Rectangular or square shaped muscle fibres.
II. Oblique
These are the muscle fibres that run oblique to the line of pull of the muscle
organ (angled). The muscles are pennated in form and therefore are better
adapted to produce powerful contractions.
a) Unipennate
Muscle fibres that form one angle towards the line of pull.
b) Bipennate
Muscle fibres that form two angle towards the line of pull.
c) Multipennate
Muscle fibres that form three angle towards the line of pull.
III. Circular
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
These are the muscles that surround a body opening or ‘tube’. These tubes
are called sphincters.
6.2 Examine the specimens to find an example of each type of skeletal muscle listed in
objective 6.1.
Parallel Oblique/Pennate Circular
Type Example Type Example Example
Strap-like Sartorius Unipennate Extensor Obicularis Oris
digitorum
Fusiform Biceps Brachii Bipennate Rectus
Femoris
Triangular/ Pectoralis Major Multipennate Deltoid
Radiate
Quadrilateral Quadratus
/Flat Femoris
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
6.3 Discuss the effect of the form of a muscle to:
I. Its final contracted length
In a muscles final contracted length, the muscle fibres will be shortened
compared to its relaxed stage where muscle fibres are longer.
II. The force it can exert
Your muscles have thin and thick filaments, which are organized into
contractile units called sarcomeres. The sarcomeres have an optimal length
at which the number of possible binding sites between the filaments is
maximized. If your muscle fibers are shorter or longer than this optimal
length, they do not have as much force-producing potential because there
are fewer available binding sites between the filaments. For example, when
your elbow is fully bent, the length of your biceps muscle fibers is shorter
and less capable of producing force than when your elbow is extended.
6.4 Describe and identify examples of each type of muscle attachment:
I. Tendinous
A cord of fibrous tissue attaching muscle fibres to bone.
E.g. deltoid muscle attaching to the anterior and lateral acromion.
II. Aponeurotic
A sheet of fibrous tissue attaching muscle fibres to bone.
E.g. palmar aponeurosis is the continuation of the tendon of palmaris
longus.
III. "Fleshy" or "Muscular"
A muscle fibre that attaches to bone via epimysium.
E.g. the intercostal muscles.
IV. Raphe
A muscle fibre that attaches to another muscle – forms a floor
(interdigitate).
E.g. mandible.
6.5 Define the following terms related to muscles:
I. Origin
End of a muscle that attaches to a relatively immovable part – ‘stable end’.
Proximal.
II. Insertion
End of a muscle that attaches to a movable part. Always moves toward the
origin – ‘moving end’. Distal.
III. Action
The movement that is produced when a muscle contracts concentrically in
isolation.
IV. Torque
The active force generated by muscle contraction is response to resist
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
external or internal forces. The moment of a force; the measure of a force's
tendency to produce turning and rotation about an axis.
Torque = force x movement arm
V. Function
The action of muscle, which is principally contraction.
VI. Bursa
Closed sacs of synovial membrane which contain synovial fluid, allowing
muscles to slide over other structures without friction.
VII. Tendon sheath
Tubular synovial sacs around tendons, allowing tendons to slide over other
structures without friction.
6.6 Define the term ‘muscle contraction’.
A process leading to shortening and/or development of tension in muscle tissue.
Muscle contraction occurs by a sliding filament mechanism whereby actin filaments
slide inward among the myosin filaments.
6.7 Define the following terms relating to different types of muscle contraction:
I. Static/isometric
Muscle contracts and no movement in produced. The length of the muscle
stays the same.
II. Dynamic/isotonic
Muscle contracts and enough force to produced to move an object. Muscle
maintains its tension throughout the whole movement. There are two
types:
a) Concentric
Muscle shortens as it contracts. Contracts in the opposite direction of
the pull of gravity.
E.g. Pectoral muscles in the pushing-up phase of a push-up
b) Eccentric
Muscle lengthens as it contracts. Contracts in the direction of the pull of
gravity, as long as the speed of movement is less than the speed of
gravity.
E.g. Pectoral muscles in the lowering phase of a push-up.
Aims
At the end of this topic you should be able to understand the:
a) General structure of skeletal muscles and their accessory structures.
b) Implications of the external appearance of a skeletal muscle to its function.
c) Types of skeletal muscle contraction.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
7. Muscles of the Shoulder Region
Objectives
7.1 Identify, state the attachments and deduce the actions of the muscles of the
axillary and scapular regions (complete table at end of workbook):
I. AXIOSCAPULAR muscles connecting the axial skeleton and shoulder girdle:
a) Trapezius
Identify Attachments Actions
External Occipital Upper – Elevation
Protuberance - T12, and Lateral Rotation
Spine of Scapula, Middle – Retraction
Acromion Process Lower – Retraction
and Later Rotation
b) Rhomboid major
Identify Attachments Actions
T2-5 Spinal Process, Retraction
medial border of Medial Rotation
scapula
c) Rhomboid minor
Identify Attachments Actions
C7-T1 Spinal Process, Retraction
medial border of Medial Rotation
scapula
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
d) Levator scapulae
Identify Attachments Actions
C1-4 Transverse Elevation
Process, superior Medial Rotation
angle of scapula
e) Pectoralis minor
Identify Attachments Actions
Coracoid Process, Protraction
Ribs 3-5 Medial Rotation
Forward Tilting
f) Serratus anterior
Identify Attachments Actions
Coracoid Process, Protraction
Ribs 3-5 Medial Rotation
Forward Tilting
II. AXIOCLAVICULAR muscles connecting the axial skeleton to the clavicle:
a) Subclavius
Identify Attachments Actions
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Rib 1, Subclavian Depresses Shoulder
Groove, lateral Inferior and
aspect of clavicle Anterior Pull of
Clavicle
III. AXIOHUMERAL muscles connecting the axial skeleton and the humerus:
a) Pectoralis major - sternal head
Identify Attachments Actions
Intertubercular Adduction
Groove – attaches Medial Rotation
axial skeleton Flexion
(sternum) to humerus (Bench press,
punching,
throwing)
b) Latissimus dorsi
Identify Attachments Actions
Intertubercular Adduction
Groove, T6-S5, Iliac Medial Rotation
Crest, Ribs 9-12, Extension of GHJ
inferior angle of (swimming,
scapula – attaches climbing)
axial skeleton to
humerus
IV. SCAPULOHUMERAL (SH) and CLAVICULOHUMERAL (CH) muscles
connecting the shoulder girdle and the humerus:
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
a) Pectoralis major - clavicular head (CH)
Identify Attachments Actions
Intertubercular Adduction
Groove – attaches Medial Rotation
shoulder girdle Flexion
(clavicle) to humerus (Bench press,
punching,
throwing)
b) Deltoid (CH and SH)
Identify Attachments Actions
Deltoid Tuberosity, Anterior – Flexion,
Scapula Spine, Abduction
Acromion, Clavicle – Middle – Abduction
attaches shoulder Posterior –
girdle to humerus Extension,
Abduction, External
Rotation
(Arm raises, flies)
c) Coracobrachialis (SH)
Identify Attachments Actions
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Mid shaft of humerus, Adduction
coracoid process – Flexion
attaches shoulder
girdle to humerus
d) Teres major (SH)
Identify Attachments Actions
Intertubercular Adduction
Groove, inferior angle Medial Rotation
of scapula – attaches Extension
shoulder girdle to
humerus
e) Biceps brachii (SH)
Identify Attachments Actions
Long head (lateral) – Flexion of GHJ
Supraglenoid Tubercle Flexion and
Short head (medial) – Supination of Elbow
Coracoid Process (radioulna joint)
Distal attachment
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
f) Triceps brachii (SH)
Identify Attachments Actions
Olecranon Process, Extension of GHJ and
Infraglenoid Tubercle elbow (radioulna
– attaches shoulder joint)
girdle to humerus
2 joint muscle
g) Supraspinatus (SH – Rotator Cuff)
Identify Attachments Actions
Greater Tubercle, Externally Rotate
Supraspinatus Fossa Abduction
h) Infraspinatus (SH – Rotator Cuff)
Identify Attachments Actions
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Greater Tubercle, Externally Rotate
Infraspinatus Fossa
i) Teres minor (SH – Rotator Cuff)
Identify Attachments Actions
Greater Tubercle, Externally Rotate
lateral border of
scapula
j) Subscapularis (SH – Rotator Cuff)
Identify Attachments Actions
Lesser Tubercle, Internally Rotate
Subscapular Fossa
7.2 List the muscles which attach to the:
I. Scapula at the:
a) Coracoid process
Biceps Short Head Coracobrachialis Pectoralis Minor
b) Acromion process
Trapezius Deltoid
c) Spine
Trapezius Deltoid
d) Vertebral (medial) border
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Inferior to Superior
Rhomboid Major Rhomboid Minor
Superficial to Deep
Rhomboid Major Serratus Anterior Subscapularis
e) Inferior angle
Latissimus Dorsi Teres Major
II. Clavicle
Subclavius Pectoralis Major Deltoid
III. Humerus at the:
a) Greater tubercle
Supraspinatus Infraspinatus Teres Minor
b) Lesser tubercle
Subscapularis
c) Intertubercular (bicipital) groove – lateral lip
Pectoralis Major
d) Intertubercular (bicipital) groove- floor
Latissimus Dorsi
e) Intertubercular (bicipital) groove- medial lip
Teres Major
7.3 List the muscles which produce:
I. Movements of the scapula
a) Elevation
Upper Trapezius Levator Scapular
b) Depression
Lower Trapezius
c) Protraction
Serratus Anterior Pectoralis Minor
d) Retraction
Rhomboid Major Rhomboid Minor Middle Trapezius
slightly Upper and Lower Trapezius
e) Lateral Rotation
Upper Trapezius Lower Trapezius Serratus Anterior
f) Medial Rotation
Levator Scapulae Rhomboid Major Rhomboid Minor
Pectoralis Minor
II. Movements of the humerus (shoulder joint)
a) Flexion
Pectoralis Major Anterior Deltoid Coracobrachialis
Biceps Brachii
b) Extension
Latissimus Dorsi Posterior Deltoid Teres Major
Triceps Brachii
c) Abduction
Middle Deltoid Posterior Deltoid Anterior Deltoid
Supraspinatus
d) Adduction
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Pectoralis Major Latissimus Dorsi Coracobrachialis
Teres Major
e) Lateral Rotation
Posterior Deltoid Supraspinatus Infraspinatus
Teres Minor
f) Medial Rotation
Pectoralis Major Latissimus Dorsi Teres Major
Subscapularis
Aims
At the end of this topic you should be able to:
a) Identify and describe the attachments and actions of all the muscles of the shoulder
region.
b) List the muscles responsible for each movement of the shoulder region.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
8. Muscle Tissue
Objectives
8.1 Describe the functions of muscle tissue.
Muscles are composed of tubular muscle cells called myocytes. Myocytes are
composed of many chains of myofibrils. Myofibrils are composed of repeating
sections of sarcomeres (actin, myosin and titin that are organized into thick and thin
filaments). Sarcomeres appear under the microscope as dark and light bands.
Muscles contract by sliding the thin (actin) and thick (myosin) filaments along each
other.
Skeletal Muscle Cardiac Muscle Smooth Muscle
Functions Moves or stabilizes Circulates blood. Moves food, urine
the position of the Maintains blood and reproductive
skeleton. (hydrostatic) tract secretions.
Guards entrances pressure. Controls diameter
and exists to the of respiratory
digestive, passageways.
respiratory and Regulates
urinary tracts. diameter of blood
Generates heat vessels.
Protects internal
organs.
8.2 Understand the distribution and organisation of skeletal, smooth and cardiac
muscle tissue.
Skeletal Muscle Cardiac Muscle Smooth Muscle
Organisation Cells are long, Cells are short, Cells are short,
cylindrical, branched, and spindle-shaped,
striated, and striated, usually and nonstriated,
multinucleate. with a single with a single
nucleus; cells are central nucleus.
interconnected by
intercalates discs.
Location Combines with Heart Found in the walls
connective tissues of blood vessels
and neural tissue and in digestive,
in skeletal muscles. respiratory,
urinary, and
reproductive
organs.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Organisation of Skeletal Muscles -
Epimysium Layer of connective tissue, which covers the entire muscle.
Perimysium Sheath of connective tissue that groups muscle fibres into
bundles or fascicles.
Fascicle Bundle of skeletal muscle fibres.
Endomysium Connective tissue that surrounds each muscle fibre.
Muscle Fibre A muscle cell.
Myofibrils Contractile protein organelles.
Myofilaments Contractile proteins composed of:
Thick filaments Made of myosin.
Thin filaments Made of actin.
8.3 Describe the following features of skeletal muscle tissue:
Skeletal muscle fibres (myofibres) are long and narrow cells that often span the
entire length of a muscle. The cytoplasm of skeletal muscle fibres is called
sarcoplasm. Most of the sarcoplasm is occupied by myofibrils.
I. Myofibrils
Myofibrils are cylindrical bundles of contractile proteins. Each myofibril
extends the length of a fibre. Living muscle fibres usually contain hundreds
to thousands of myofibrils.
Along the surface, skeletal muscle fibres appear striated. The alternating
dark and light bands are due to the length, thickness and alignment of the
protein filaments in the myofibrils.
II. A bands
The myofilament myosin (thick filament) and actin (thin filament) overlap
zone. Appear dark under microscope.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
III. I bands
The myofilament actin and titin overlap zone. Appear light under
microscope.
IV. Z line
The joint line between adjacent sarcomeres – actin and titin.
V. Sarcomere
The smallest functional unit of muscle that change their length, which is the
driving force in muscular contraction.
8.4 Describe the role played in muscle contraction by each of the following
components of skeletal muscle fibres:
I. Sarcoplasm
Myofibrils and myofilaments are components of the sarcoplasm.
Muscle contraction begins when stored Ca 2+ ions are released into the
sarcoplasm (from the sarcoplasmic reticulum). Ions then diffuse into
individual contractile units called sarcomeres. Ca 2+ weakens troponin and
tropomyosin rotates so myosin can bind to actin (the contracting filaments
slide/ interdigitate between one another).
II. Sarcolemma
Action potentials (AP) are generated here which leads to muscle
contraction. The sarcolemma is the name of the cell membrane that
encloses each muscle cell/fibre. It contains tunnel-like extensions, which
pass across muscle fibres from side to side (transverse). These extensions of
the sarcolemma are called transverse tubules (T tubules).
Electrical impulse AP simultaneous contraction
III. Myofilament
Thin filaments (actin) slide to the centre of the sarcomere, alongside thick
filaments (myosin). When thick filaments are adjacent to the Z lines, this is
the end point of muscle contraction.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
IV. Myofibril
Myofibril is the name given to one of the components of skeletal muscle
cells that are particular to muscle tissue (contract). These are cylindrical
structures that extend along the complete length of the muscle fibre/cell.
Each myofibril consists of two types of protein filaments called thick
filaments (myosin), and thin filaments (actin). There are hundreds of
myofibrils in each muscle fibre.
V. A band
H band gets smaller and zone of overlap gets larger. The width of A band
remains constant during muscle contraction.
VI. I band
I band gets smaller during muscle contraction.
Titin helps keep the thick and thin filaments in proper alignments, aids in
restoring resting sarcomere length, and prevents extreme stretching
(damage contraction mechanism).
VII. Z line
Moves closer together during muscle contraction.
VIII. Sarcomere
Becomes shorter when muscle contracts.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
8.5 Briefly describe the differences between fast fibres, slow fibres and intermediate
fibres in skeletal muscle tissue.
Slow Twitch Intermediate Fast Twitch
Cross-sectional Small Intermediate Large
diameter
Tension Low Intermediate High
Contraction Slow Fast Fast
Speed
Fatigue High Intermediate Low
Resistance
Colour Red Pink White
Myoglobin High Low Low
content
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Capillary supply Dense Intermediate Scarce
Mitochondria Many Intermediate Few
Glycolytic Low High High
enzyme
concentration in
sarcoplasm
Substrates used Lipids, Primarily Carbohydrates
for ATP carbohydrates, carbohydrates (anaerobic)
generation amino acids (anaerobic)
during (aerobic)
concentration
Alternative Type I, S (slow), Type II-A, FR (fast Type II-B FF (fast
names red, SO (slow resistant), fast- fatigue), white,
oxidative), slow- twitch oxidative fast-twitch
twitch oxidative glycolytic
Aims
At the end of this topic you should be able to:
a) Understand the function of muscle tissue.
b) Describe the microscopic structure of the three types of muscle tissue.
c) Understand the mechanism of contraction of the three types of muscle tissue.
d) Describe the biochemical classification of skeletal muscle and its functional
significance.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
9. Introduction to the Anatomical Analysis of Movement
Objectives
9.1 Distinguish between alternative terms to describe motion of body parts:
A joint reference is the best to use in most cases where it can apply. However in
some cases, other references are more suitable (e.g. adduction of fingers,
protraction of the scapula).
I. Segments
General part of the body.
Eg. Arm, forearm.
II. Joints
The fulcrum which the bone moves upon.
Eg. Shoulder, elbow, wrist, scapulothoracic.
III. Bones
The actual bone that is moving.
Eg. Humerus, radius/ulna, carpals, scapula.
9.2 Distinguish between ‘open chain’ and ‘closed chain’ motions.
I. Open Chain
This is the default position and is non weight bearing. An open chain is a
mechanical description of a system of links in which only one end of system
is attached to a relatively immobile structures (ie. the body, and the other
end is free to move in mid-air).
For example, in an open chain motion of the knee, there is no change in hip
and ankle position required. Flex the knee by bending it and lifting the leg
and foot posteriorly so the foot is non weight bearing.
II. Closed Chain
A closed chain is a mechanical description of a system of links in which both
ends of the system are attached to relatively fixed structures. The moving
joint of focus (ie. The knee, elbow) lies between the relatively immoveable
loads of the body and the floor or another non-moving object. A closed
chain motion will change what is happening with nearby joints.
For example, in a closed chain motion of the knee, the hip and ankle
position changes. Flex the knee by flexing hip and ankle to form a squat
position, foot is weight bearing.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
9.3 Briefly define terms relating to motion in the anatomical planes:
I. Rotary
These movements involve turning around an axis. Movements can occur in
isolation (pure) – eg. flexion/extension of MCP joints.
Movements can occur simultaneously with translator movements – eg.
flexion/extension of glenohumeral joint.
II. Translational
These movements involve sliding along the plane. They do not usually occur
in isolation during active movements. These movements accompany rotary
motions in many synovial joints (called accessory movements; essential for
normal joint function). One focus of passive joint mobilisation techniques –
problems in movement can be due to too long translational movement in
joints.
For example, the shoulder joint will undergo rotary movements when
flexing and extending in the sagittal plane but at the same time the head of
the humerus will slide up or down, forward or back on the Glenoid fossa to
increase movement.
III. Circumduction
These movements occur between anatomical planes such that the distal
end of the moving segment traces a circle. This is not rotation.
IV. Cross-planar motion
The motions occur across anatomical planes and are rarely ‘pure’ rotary
motions. Uniaxial – rotary motions across one axis (eg. flexion of elbow in
sagittal plane). Biaxial – rotary motions across two axis (eg wrist in sagittal
and coronal plane). Multiaxial – rotary motions across three axis (eg
shoulder and hip).
Most joints do not have ‘pure’ planar motion because:
a) Axes of motion are not perfectly perpendicular to the anatomical
planes.
b) Joint surfaces are not perfectly spherical.
c) Therefore there are cross planar motion in all seemingly single plane
motions.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
9.4 Appreciate the joint motions involved in different styles of hand waving.
Style Joint Motions
Up and Down Wrist flexion and extension (sagittal)
Side to Side Wrist abduction and adduction (coronal)
Around and Around Circumduction of the wrist (moving
between sagittal and coronal)
Turn of the Spot No wrist motion, but fixed in extension,
supination and pronation of radioulnar
joints (transverse)
4 Finger Crunches No wrist motion but fixed in extension,
flexion and extension of 2-4 MCP joints
(sagittal)
Alternating Fingers No wrist motion but in slight extension,
alternating flexion and extension of 2-4
MCP joints (sagittal)
9.5 List the forces which can affect motion of body parts.
External to Body Internal From
Gravity Muscles (active)
Momentum Tendons
Friction Joint capsules
Ground Reaction Ligaments
Fascial Structures
9.6 Briefly define terms relating to skeletal muscle activity during motion of body
parts:
I. Action
Movement of joints which are produced when a muscle acts in isolation and
concentrically contracts. Usually referred to movement from the anatomical
position.
This is open chained. The default position is where the proximal attachment
is fixed and the distal attachment is moving towards the proximal
attachment when the muscle contracts concentrically (shortens).
II. ‘Reverse’ action
The action when the fixed and non-fixed parts are switched. This is a closed
chain. The proximal attachment becomes moveable and the distal
attachment becomes fixed.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
III. Uni-articular, bi-articular, multi-articular
a) Uni
Crosses and acts on one joint only (eg. brachialis).
b) Bi
Crosses and acts on two joints. Acts on the distal end first (eg. triceps
and biceps).
c) Multi
Crosses and acts on three joints (eg. wrist muscles/joints).
IV. Line of action
The directions of the lines of the muscles indicate the directions of the force
(pull) the muscles have on the joint – the end of the muscles moves towards the
origin of the muscles during contraction.
9.7 Briefly explain differences in function between uni-articular and bi-articular
muscles.
Uni-articular:
I. No synergist activity required for uni-articular muscles.
II. Optimal function is not restricted for uni-articular muscles.
Bi-articular:
I. Synergist activity required for bi-articular and multi-articular muscles if you
don’t not want the other joint motions to occur.
II. Optimal function is restricted for bi-articular muscles. The range of motion
at the most distal joints is affected by the position of the proximal joint.
III. Torque produced at the most distal joints is affected by the position of the
more proximal joint.
Aims
At the end of this topic you should be able to:
a) Define terms used in the anatomical analysis of movement.
b) Describe the components of a movement pattern or motor skill.
c) Briefly explain the steps involved in an anatomical analysis of a movement pattern
or motor skill.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
10. Functions of muscles and functional anatomy of the shoulder region.
Objectives
10.1Distinguish between the actions and the functions (functional roles of a muscle).
An action is defined as the movements produced when muscles contract concentrically
in isolation.
The functions of muscles is muscle co-ordination, which is achieved through the
various functional roles – agonist, antagonist, stabilizer, synergist.
10.2Define the following terms related to functional roles of muscles:
I. Agonist
The muscle producing the desired movement by either concentric or eccentric
contractions (eccentric contractions depend of gravity).
a) Prime mover
The muscle that contracts to produce a specific movement.
E.g. biceps brachii in elbow flexion
b) Assistant mover
Muscles that assist in the specific movement, albeit with less effect.
E.g. brachialis assist biceps brachii in elbow flexion.
II. Antagonist
The muscle that must relax (i.e. not contracting) to allow the desired
movement to occur.
E.g. triceps brachii in elbow flexion.
III. Synergist/neutralizer
The muscles that eliminate an undesired movement that would otherwise be
produced by the movers. Co-synergist act together to cancel out a movement.
E.g. flexion and extension of the deltoid cancel each other out.
IV. Stabilizer/fixator
The muscles that supports a body part so that another muscle will have a firm
base from which to act.
10.3Specifically describe the functional roles of the rotator cuff muscles group in
providing dynamic stability at the shoulder joint.
There are four rotator cuff muscles, each with a specific action:
I. Supraspinatus
Action – externally rotate the humerus (DOES NOT initiate abduction)
II. Infraspinatus
Action – externally rotates the humerus
III. Teres minor
Action – externally rotates the humerus
IV. Subscapularis
Action – internally rotates the humerus
The functional roles of these rotator cuff muscles is to provide dynamic stability at the
shoulder joint by:
I. Taking up slack in the shoulder joint capsule during movement – improved
capsular ligament function – improved proprioception.
II. Provide a medial force to the humeral head to accurately position it in the
centre of the Glenoid fossa during shoulder movement.
III. Prevent superior gliding in abduction caused by deltoid (will pull inferiorly)
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
IV. Prevent anterior gliding in flexion caused by deltoid/ pectoralis major (will pull
posteriorly)
V. Prevent posterior gliding in extension caused by deltoid/ latissimus dorsi (will
pull anteriorly)
10.4Specifically describe the functional roles of trapezius and serratus anterior during
lateral rotation of the scapula.
There are three parts to the trapezius muscles, and the serratus anterior, each with a
specific function:
I. Upper Trapezius
Actions – elevate and laterally rotate the scapula (cancels LT depression)
II. Middle Trapezius
Action – retracts the scapula (cancels SA protraction)
III. Lower Trapezius
Action – depress and laterally rotate the scapula (cancels UP elevation)
IV. Serratus Anterior
Action – protract and laterally rotate the scapula (cancels MT retraction)
The functional roles of the trapezius muscles and serratus anterior, for example during
lateral (upward) rotation of the scapula, is to:
I. Move the Glenoid fossa thus increasing the mobility of the shoulder, as there
is more articulating surface for the humerus to articulate on as it abducts.
II. Remove the obstruction caused by the acromion so that the humerus can
further abduct.
III. Reposition all the rotator cuff muscles enabling them to provide an
appropriate stabilizing force to humeral head throughout shoulder range of
movement.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
10.5Describe and state the functional significance of the scapulohumeral rhythm.
The scapulohumeral rhythm is the co-ordination between the humerus and scapular
movement. This requires significant muscle coordination.
Scapulohumeral rhythm serves at least two purposes:
I. It preserves the length-tension relationships of the glenohumeral muscles; the
muscles do not shorten as much as they would without the scapula's upward
rotation, and so can sustain their force production through a larger portion of
the range of motion.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
II. It prevents impingement between the humerus and the acromion. Because of
the difference in size between the Glenoid fossa and the humeral head,
subacromial impingement can occur unless relative movement between the
humerus and scapula is limited. Simultaneous movement of the humerus and
scapula during shoulder elevation limits relative (arthrokinematic) movement
between the two bones.
10.6List the functions of the clavicle and state the implications of its ‘crank-like’ shape for
the shoulder function.
Note: Produces movement of the clavicle.
Function:
I. Acts as a bar holding the scapula laterally, enabling the arm to be clear of the
trunk.
II. Transmits physical impacts from the upper limb to the axial skeleton.
Curved (“crank-like”) shape of clavicle increases shoulder region mobility.
Initially scapula lateral rotation produces posterior rotation of the clavicle at the SC
joint – due to tension in the conoid ligament.
Rotation at sternal end of clavicle creates a rotation with a much larger radius at the
acromial end of the clavicle.
As range of posterior axial rotation at the SC joint is exhausted, scapula lateral rotation
produces movement at the AC joint.
10.7Explain shoulder muscle recruitment patterns during full range abduction of the
upper limb.
Deltoid produces abduction of the shoulder joint by contracting, causing the humeral
head to glide superiorly. The synergist RC muscles (subscarpularis, infraspinatus, teres
minor), prevent superior glide by pulling inferiorly
Lateral rotation of the scapula accompanies abduction of the shoulder joint.
10.8List the features of the shoulder (glenohumeral) joint which contributes to its:
a) Stability
I. Ability of scapula to rotate, maintaining RC muscles in optimal position.
II. RC (dynamic) medial force to centralise humeral head.
III. Ligaments (glenohumeral, coracoacromial and coracohumeral).
IV. Synergist muscles.
V. Bone structure:
a) Acromion prevents superior dislocation.
b) Glenoid fossa faces slightly superiorly (stabilises head of humerus with
gravity and coracohumeral ligament).
c) Glenoid labrum increases concavity of the glenoid fossa – provides
more congruency.
b) Mobility
I. Ability of scapula to rotate, enabling glenoid fossa to continue articulating
with the humeral head.
II. Curved shape of clavicle (places scapula in more positions).
III. Shallow and small fossa.
IV. Loose, lax and thin capsule filled with synovial fluid.
V. Scapulohumeral rhythm – combination of scapular and humeral
movements.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
VI. Glenoid labrum increases flexibility without damaging the bone.
VII. Muscular structure.
VIII. Ball and socket joint (multiaxial synovial joint).
Aims
At the end of this topic you should be able to:
a) State the specified functional roles of all the muscles of the shoulder region.
b) Appreciate the concept of active stabilization of joints.
c) Explain muscle recruitment patterns during functional activities involving the shoulder
region.
d) List features which contribute to the stability and mobility of the shoulder region
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
11. Introduction to surface anatomy and surface anatomy of the shoulder region.
Objectives
XI.1 Outline the general principles of palpation.
I. Visual inspection
a) Identify anatomy structures.
b) Look for:
Alignment of head and neck
Levels of shoulder trapezius (dominant tends to be lower)
Clavicle alignment (swelling and deformity)
Muscle bulk (or lack of it) or muscle atrophy
Position
E.g. deltoid dislocation
Position of scapula
Depression/elevation upper trapezius?
Protraction Tight pectoralis major?
Inferior angle tilting Tight pectoralis minor?
Winging of scapula Weak serratus anterior
Bony landmarks
c) Static and dynamic movements.
II. Palpation
a) A method of feeling with the hands to identify anatomical structures
(bones, ligaments, tendons, muscle bodies, nerves and the vasculature).
Important to distinguish between structures in determining pain
source.
Important in AC and SC joint problems.
General palpation for temperature changes, palpable oedema and
sweating.
Palpation is firm but you feel more if less pressure is applied.
Visible and palpable anatomy forms the basis of any clinical examination and movement
analysis.
Relate visual anatomy and palpable anatomy to radiological examination, subjective
history and objective examination.
Must know ‘normal’ anatomy before you can assess ‘abnormal’ anatomy and hence
provide management strategies (exercise prescription and manual treatment).
XI.2 Identify the bony features (below) of the shoulder region on self, fellow students and
photographs:
I. Scapula:
a) Acromion
b) Spine
c) Vertebral border
d) Inferior angle
e) Coracoid process
Press firmly upwards and laterally below the junction of the middle and
lateral thirds of the clavicle
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
II. Clavicle:
a) Acromial end
b) Sternal end
c) Curvatures
III. Humerus:
a) Head
b) Greater tubercle
c) Lesser tubercle
d) Deltoid tuberosity
e) Medial and lateral epicondyles
IV. Sternoclavicular joint
V. Acromioclavicular joint
Anterior View - Bones
1. Clavicle
2. Sternal end – SC joint
2a. Acromial end – AC joint
3. Costoclavicular ligament
(not palpable)
4. Coracoid process
5. Coracoclavicular
ligament (not palpable)
6. Acromion
7. Humerus
8. Greater tubercle (look
for laterally)
9. Lesser tubercle (look for
medially and anteriorly)
10. Bicipital
(intertubercular) groove
(not palpable)
11. Head of humerus
12. Glenohumeral joint –
GHJ (not palpable)
13. Medial epicondyle
14. Lateral epicondyle
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Lateral View - Bones
1. Sternum
2. Manubrium
3. Clavicle
4. Coracoid process
5. Acromion
6. Greater tubercle
7. Lesser tubercle
8. Supracondylar ridge
9. Lateral epicondyle
10. Olecranon
Posterior View - Bones
1. Acromion
2. Spine of scapula
3. Medial border
4. Inferior angle
5. Base of spine
6. Superior angle
7. Glenoid fossa – for GHJ
(Can palpate from posterior view)
(Palpate ~ 1-2cm below acromion)
8. Humerus
XI.3 List the structures (muscle and/or ligaments) attaching to the:
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
I. Scapula
a) Corocoid process
Muscles Ligaments
Coracobrachialis Coracoacromial
Biceps brachii short head Coracohumeral
Pectoralis Minor Coracoclavicular - (conoid and
trapezoid)
b) Acromion
Muscles Ligaments
Deltoid Coracoacromial
Trapezius
c) Spine
Muscles Ligaments
Deltoid
Trapezius
d) Vertebral border
Muscles Ligaments
Rhomboid major
Rhomboid minor
Levator scapulae
Serratus anterior
e) Inferior angle
Muscles Ligaments
Latissimus Dorsi
Serratus Anterior
II. Humerus
a) Greater tubercle
Muscles Ligaments
Supraspinatus Coracohumeral
Infraspinatus Glenohumeral
Teres Minor Transverse humeral
b) Lesser tubercle
Muscles Ligaments
Subscapularis Transverse humeral
c) Intertubercular groove
Muscles Ligaments
Pectoralis Major
Latissimus Dorsi
Teres Major
d) Deltoid tuberosity
Muscles Ligaments
Deltoid
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
XI.4 Observe (photographs) and/or palpate the following muscles of the axillary and
scapular regions in a relaxed and contracted state on self, fellow students:
I. Muscles connecting the axial skeleton and the humerus:
a) Pectoralis major - sternal head (anterior axillary fold)
b) Latissimus dorsi (posterior axillary fold)
II. Muscles connecting the shoulder girdle and the humerus:
a) Pectoralis major - clavicular head (anterosuperior axillary fold)
b) Deltoid
c) Coracobrachialis
d) Teres major – (posterosuperior axillary fold)
e) Tendon of long head of biceps, biceps muscle belly
f) Triceps brachii
g) Tendon of suprapinatus
h) Infraspinatus
III. Muscles connecting the axial skeleton and shoulder girdle:
a) Trapezius
b) Rhomboid major
c) Serratus anterior
Anterior View – Muscle
Attachments
Coracoid process
1. Pectoralis minor
2. Coracobrachialis
3. Biceps brachii short
head
Greater tubercle
6. Supraspinatus,
infraspinatus and teres
minor
Lesser tubercle
7. Subscapularis
Intertubercular groove
8. Pectoralis major
(difficult to palpate)
9. Latissimus dorsi
(difficult to palpate)
10. Teres major (difficult
to palpate)
12. Deltoid
The biceps
14. Sternal head of
tendon runs over
pectoralis major
15. Clavicular head of
floor of bicipital
pectoralis major groove.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Anterior View – Muscle
Belly
Pectoralis major
4. Clavicular head
5. Sternal head
Palpable as the anterior
axillary fold and clearly
visible on suitable
specimens
More visible with resisted
adduction and medial
rotation
Biceps
4. long head
5. short head
Muscle belly palpable and
more visible with
supination and resisted
flexion
Lateral View – Muscles
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
14. Serratus anterior
15. Deltoid (anterior,
middle and posterior)
Deltoid attachments
16. Deltoid tuberosity
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Posterior View – Muscles
9. Trapezius
10. Deltoid
11. Latissimus dorsi –
posterior axillary fold
14. rhomboid major
16. infraspinatus
17. teres major
1. Supraspinatus
2. Infraspinatus
3. Teres minor
4. Teres major
5. Triceps brachii long
head
6. Triceps brachii lateral
head
7. Triceps brachii medial
head
9. Axillary nerve
10. Radial nerve
XI.5 Relate surface anatomy landmarks to the position of blood vessels and nerves.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Blood Vessels
1. Subclavian artery
2. Axillary artery
3. Brachial artery
6. Brachial plexus
8. Pectoralis minor
Aims
At the end of this topic you should be able to:
a) Relate surface anatomy landmarks to the gross anatomy of the shoulder region.
b) Observe and/or palpate major bony landmarks and joints of the shoulder region.
c) Observe and/or palpate most of the muscles of the shoulder region
d) Understand that blood vessels and nerves are important structures relating to the
surface anatomy
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
12. Generalised Connective Tissue.
Objectives
12.1Describe the properties and functions of the three components of connective tissues:
cells, fibres and ground substance.
There are three components of connective tissue - specialized cells, protein fibres and
ground substance. Protein fibres and ground substance make up the extracellular matrix.
Extracellular matrix makes up majority of tissue volume and determines specialised
function.
I. Specialised cells
a) Fibrocyte/Fibroblast (‘fixed’ active fibrous)
Most abundant type of cell in the body.
Found in all generalised connective tissue.
Produce and maintain intercellular matrix
Promote wound contraction
Secretes protein sub-units that complex together to form fibres.
Secretes molecules that spread out and contribute to the ground
substance.
Proliferate (increase in number) and migrate (relocate) in response to tissue
injury
Essential for healing (forms the scars)
b) Adipocytes (fatty tissue)
Contain large lipid droplet which pushes cytoplasm to one side (thin
nucleus)
Energy storage and insulation
Function to synthesise, store and release lipid.
c) Macrophage (‘fixed’ or ‘free’)
Mobile cells capable of phagocytosis
Eliminate micro-organisms and debris
Contribute to immune reactions
Directs the immune processes that lead to healing after injury
d) Mast Cells (‘fixed’ immune cells)
Produce anticoagulant (heparin-like)
Produce inflammatory substance (histamine), which increase vascular
permeability.
Function to facilitate migration of cells from blood to CTP
Stimulates inflammation after injury or infection
e) Plasma Cells (‘free’)
Produce antibodies to fight infection.
II. Fibres
a) Collagen Fibres
Very high tensile strength
Provide support and strength
Most common fibre in connective tissue proper
Fibres arranged in parallel bundles in tendons and ligaments
Long, straight and unbranched (rope like)
Resist tensional (tensile) forces as they are parallel
b) Reticular Fibres
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Branched network of interwoven fibres (stroma)
Thinner than collagen fibres
Strong and flexible
Network resist forces in many directions
Found in fascial sheaths around and between muscles.
c) Elastic Fibres
Easily sstretched branched and wavy fibres
Elastin core and mircofibrils.
Provides resilience and elasticity
Found in rare elastic ligaments and in structures that must withstand
repeated stretching (blood vessel walls (aorta), skin and lungs.
III. Ground Substance
This acts as a diffusion medium and provides support. It is a clear, colourless and
viscose fluid, filling spaces between connective tissue cells and fibres. The main
components are extra-cellular fluid and hydrated molecules (glycosaminoglycan’s –
GAGs).
a) Proteoglycans
Diverse group of soluble, large molecules
Hydrators – attract and hold water
Stabilise collagen networks – glue
Resist compressive forces
b) Glycoproteins
Link extra cellular matrix components (i.e. fibres, ground substance and
cells) – facilitate movement of cells through CT
Adhesion molecules provide the movement (binding and unbind to move).
Maintenance of ground substance is tightly regulated and controlled –
balance of synthesis and degradation of substances.
12.2Understand the structure and functions of the different types of generalised connective
tissue.
Connective Tissue
Provides support, touch and healing/repair
Support: Important component of normal functioning of musculoskeletal system –
shape for muscles.
Repair: Ligaments and tendons are damaged regularly – thus need to repaired/healed
by connective tissue.
Three types of connective tissue:
I. Supportive Connective Tissue
Bone and cartilage
II. Fluid Connective Tissue
Blood and Lymph
III. Connective Tissue Proper (generalised connective tissue)
Tendons: bone to muscle
Ligaments: bone to bone
Fascia: covering of organs
Reticular networks: structure for organ tissues
Adipose tissue: fat for cushioning and insulation
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
12.3Describe the listed features of the following generalised connective tissues:
Type of Tissue Description Features Examples
Loose (areolar) More cells and Collagen fibres Dermis of the skin
ground substance Elastic fibres
than fibre and is the Fibroblasts
only connective Other cells
tissue that contains
all cell types.
Responsible for
acute inflammatory
response. It is the
connective tissue
underlying all body
surfaces.
High Proteoglycans
Adipose Fat cells Fat cells Infrapatella fat pad
predominate which Fibroblasts
function to: insulate Reticular fibres
against heat loss;
provide mechanical
support; store and
release energy.
Regional differences
in distribution based
on age and gender.
Proteoglycans
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Dense Regular Predominance of Collagen fibres Ligaments and
fibres which lie in Fibroblasts Tendons
lines of stress. Very
high tensile strength
because: large
number of collagen
fibres and all fibres
oriented in same line
of stress.
Low Proteoglycans
12.4Describe how the arrangements of cells, fibres and ground substance vary to facilitate the
function of tissues such as ligament, tendon and fascia.
I. Ligaments
Resemble tendons, but connect one bone to another, or stabilise the positions
of organs.
II. Tendon
Cords of dense regular connective tissue that attach skeletal muscles to bones.
Predominantly made of collagen fibres. Some elastic fibres.
Collagen fibres are pack tightly in parallel to each other and aligned with the
forces applied to the tissue.
III. Superficial fascia (subcutaneous layer) and serous fascia
Layer of areolar tissue and fat (above/below deep fascia layer)
IV. Deep fascia
Consists of dense irregular connective tissue which strengthen and support
areas subjected to stresses from many directions
Predominantly made of collagen fibres. Some elastic fibres
Collagen fibres are in an interwoven meshwork with no consistent pattern – all
fibres of each layer run in the same direction, but the orientation changes from
layer to layer.
12.5Describe the general sequence of events during inflammation of connective tissue.
I. Inflammation
Local vasodilation (redness and heat)
White blood cells in blood vessels (lymphocytes and monocytes) are
attracted to site of injury/infection
Immune cells activated
Mast cells release inflammatory substance - increase in permeability of
blood vessel wall.
White blood cells pass into connective tissue (lymphocytes, plasma
cells, monocytes, macrophages)
Swelling and bruising occur due to “leakage” of red blood cells and
plasma as white blood cells enter connective tissue.
II. Migration
Macrophages accumulate and phagocytose debris
Plasma cells immobilise infectious organisms
III. Proliferation
Fibrocytes activated, divide and produce scar tissue
Results in fibres and ground substance.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
IV. Maturation
Scar matures then recedes
SUMMARY:
Damage to tissues and cells cells die inflammatory cells react to dead cells by
secreting inflammatory mediators eg. Histamine blood vessels respond more cells
migrate fibroblasts proliferate and migrate scar tissue formed by reticular and
collagen fibres remodelling of tissue healing complete.
12.6Describe the effect of inflammatory cells and mediators on the component of connective
tissue.
I. Inflammatory cells detect damage and begin clean up
II. Call for more help - chemotactic signals
III. Migratory cells respond to chemical messages
IV. Continue cleanup and begin scar formation
V. Re-modelling
VI. Normal function restored
12.7Describe how optimum connective tissue structure is maintained by the processes of
inflammation and healing.
Classification of generalised connective tissue:
I. Loose
More cells and ground substance than fibres.
Include areolar tissue and adipose tissue.
II. Dense
Predominance of fibres.
a) Regular
Fibres lie in lines of stress.
Large number of collagen fibres.
Include tendons and ligaments.
b) Irregular
No pattern of fibres.
Contains collagen and elastic fibres.
Functions to protect and support organs.
Aims
At the end of this topic you should be able to:
a) Understand the structure of connective tissue and the properties and functions of its
components.
b) Describe the functions of connective tissue.
c) Understand the role of connective tissue cells in the process of acute inflammation.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
13. Synovial Membrane and Synovial Fluid.
Objectives
13.1Describe the structure and functions of the synovial membrane.
I. Function:
Makes, secretes and absorbs synovial fluid – lubricant between moving surfaces
within the joint.
Provides a smooth and non adherent surface to facilitate movement.
Delivers nutrients to the joint.
II. Structure:
Vascular connective tissue with folds and villi (blood vessels)
This highly folded thin membrane increases surface area and promotes
distribution of synovial fluid.
Inner cellular layer with 2 types of cells:
a) Cells that promote hyaluronic acid (GAG)
b) Cells that phagocytose debris
Outer vascular/fibrous layer (blood vessels)
a) Contains varying amounts of adipose tissue (articular fat pad)
13.2Describe the components of normal synovial fluid and relate these components to its
functions.
I. Physical Characteristics
Clear, colourless to light yellow
Thick fluid = consistency of egg quite
Small volume in any joint (E.g. Knee 3.5mL)
II. Mechanical Properties
High viscosity – slipperiness
High elasticity - deforms under pressure and will move back to original shape
III. Major Components
Hyaluronan (a typical Proteoglycans) - viscous and elastic properties
Lubricin (Proteoglycans) - attaches to articular surfaces
Water and Small plasma proteins
a) Carries substance in solution
b) Diffuse from capillaries
c) Ultra filtrate of plasma
Glucose and other nutrients - provide nourishment and energy to joint and its
corresponding muscles
13.3Describe the structure and function(s) of the following specialised synovial associated
structures:
I. Synovial membrane associated with articulations
Lining the joint capsule and attaches to articular margin (inner surface).
II. Synovial bursae:
Sac like dilation lined with synovial membrane and filled with synovial fluid
Develops where undesirable friction could occur.
o Tendon and bone
o Tendon and joint capsule
o Tendon and tendon
o Tendon and skin
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Limited attachment to tendon and limited attachment to ‘other’ - free areas at
ends facilitate movement – allows sliding without trauma.
Can be communicating or non-communicating bursae.
o Communicating = if connected to joint capsule
o Non-communicating = free standing bursa, develops independently
a) Subcutaneous
Underneath the skin.
b) Subtendinous
Underneath tendons.
c) Submuscular
Underneath muscles.
III. Tendon synovial sheaths
Not all tendons have them – only in those that rub with bone/muscle
Synovial sac with tendons embedded in them – facilitates movement
May be a single tendon (e.g. flexor digital sheaths - fingers) or a number of
tendons embedded into the same sheath (e.g. common flexor synovial sheath -
wrist).
Tendon moves further and further in, so that the layer is pushed in as well (like
a balloon).
Visceral layer: next to tendon.
Parietal layer: secured to surround structures.
Mesotendon: transmits blood vessels (nutrients).
Synovial fluid in between visceral and parietal layers
Specific relationships between tendons and bursa – synovial sheath.
13.4Describe the effects of inflammatory cells and mediators on the structure and functions of
the synovial membrane.
Normal synovial fluid has If these factors are present it indicates
Little volume Large volume- effusion or edema (others
cells may be there)
No leukocytes (white blood cells) Inflammation
No mast cells Inflammation
No red blood cells Hemarthrosis (ruptured blood vessels)
No plasma clotting factors (no large Vascular dysfunction (blood vessel leaking)
proteins)
No culture or bacteria Septic
No chondrocytes (nothing to indicate Osteoarthritis Trauma (degradation of
cartilage is disintegrating) articular surface)
No Type A or Type B synovial cells Disintegration of membrane
13.5Describe changes in the characteristics of synovial fluid that occur as a result of immune-
mediated dysfunction.
There are two main types of joint disease:
I. Degenerative (osteoarthritis) – articular cartilage wears away with age.
II. Inflammatory (rheumatoid arthritis) – problem with synovial membrane.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Changes to synovial membrane in inflammatory joint disease:
I. Becomes more vascular and more permeable (joint swelling)
II. Becomes coated in dead cells (e.g. red blood cells) – too many macrophages
a) Decreased hyaluronic acid production – decreased viscosity
b) Decreased phagocytic activity – more debris (dead cells) to coat synovial
membrane.
Changes to synovial fluid in inflammatory joint disease:
Synovial fluid increases in amount due to increased number and permeability of vessels
in synovial membrane. Joint swelling occurs stretching the joint capsule and ligaments
making it less stable.
Hyaluronic acid content decreases leading to a decrease in viscosity and decreased joint
protection.
Not thixotropic creates no change in viscosity and decreased joint protection.
Protein content (e.g. fibrinogen) increases creating more plasma proteins due to
increased permeability of vessels in synovial membrane and decreased amount of
hyaluronic acid. This leads to clotting and increased joint damage from abrasion of
articular surfaces.
Decrease in nutrition and metabolic waste transfer to articular cartilage and discs.
Results in cartilage death and abrasion of articular surfaces by cartilage fragments.
13.6Describe how changes in the characteristics of synovial fluid can affect synovial joint
function.
Joint damage in inflammatory joint disease is due to abnormalities in synovial fluid. This
leads to:
Increase amounts of synovial fluid
Creates joint swelling, stretching of ligaments, rupture of ligaments, and joint instability
and deformation.
Decrease hyaluronan content of synovial fluid – reduced viscosity and elasticity
Increased protein content – clotting of synovial fluid
Creates decreased protection of articular surfaces, abrasions and cartilage erosion.
Decrease nutrition and metabolic waste transfer
Chondrocytes become starved of nutrients and die, fragments of cartilage float in fluid,
and abrasions of articular surfaces.
These changes in synovial fluid can lead to rheumatoid arthritis and synovitis – both
problems associated with synovial membrane.
Aims
At the end of this topic you should be able to understand the:
a) Structure and function of the synovial membrane and the properties of synovial fluid.
b) Structure and function of specialised synovial associated structures.
c) Changes in the synovial membrane and synovial fluid as a result of inflammatory
processes.
d) Consequences of these inflammatory changes for normal synovial joint function
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
14. Cartilage Tissue.
Objectives
14.1Describe the structure of cartilage tissue in terms of its components and their properties.
Cartilage tissue contains cells (chondrocytes) embedded in an intercellular (extracellular)
matrix. The chondrocytes are surrounded by lacunae (chambers).
Cartilage is usually avascular – it does not contain any blood vessels – due to anti-
angiogenesis factor.
Nutrition of chondrocytes occurs by diffusion (obtains nutrients from surrounding tissues).
Cartilage is aneural – it does not contain any nerves.
The intercellular matrix is composed of proteoglycans, collagen fibres and water and this
arrangement resists tensile forces and compressive forces.
14.2Describe the different types of cartilage and relate their function to their location in the
body.
I. Hyaline Cartilage
Epiphyseal plates - growing part of bones.
Walls of respiratory passage - allowing you to keep airways open without
muscular activity.
Stiff, flexible support which reduces friction between bones (articular cartilage).
Anterior end of ribs (costal cartilages) – connect to the sternum.
II. Articular Cartilage
Articular surfaces of bones - as low friction surface, and high tensile strength.
Similar in structure to hyaline cartilage, except for the organisation of its fibres.
Heavily hydrated tissue (75%).
III. Elastic Cartilage
Supportive but bends easily.
Found in external ear and epiglottis.
IV. Fibrocartilage
Intervertebral discs - greater tensile strength.
Articular discs (meniscus of knee)- greater tensile strength.
14.3Describe the listed features of different types of cartilage:
Type of Cartilage Feature
Hyaline – most Chondrocytes in lacunae
frequent in the Located in lacunae (depressions)
body Arranged in cell nests (groups of cells)
Intercellular matrix
Collagen fibres (cannot see them, same refractive index as
intercellular matrix)
Water (70% of the matrix) – diffusion of nutrients into cartilage.
Proteoglycans consists of GAGs attached to a core protein. Form
large molecules in cartilage tissues. Very strongly bind to water
due to their charge.
Fibrocartilage – Chondrocytes in lacunae
different structure Distributed individually or in pairs – not in groups as ‘cell nests’.
from other forms Many collagen fibres visible in intercellular matrix
of cartilage (more Collagen fibre content of its intercellular matric is much higher
collagen fibres than in other forms of cartilage.
compared to cells) Creates greater tensile strength than any other cartilage.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
14.4Describe the specific structure and function of articular cartilage.
Articular cartilage is located on the articular surfaces of bones.Similar in structure to hyaline
cartilage, except for the organisation of its fibres. The cartilage is heavily hydrated tissue
(75%).
I. Superficial zone
Highest concentration of collagen.
Collagen fibres run parallel to the articular surface. This creates a surface with a
very low coefficient of friction and a high tensile strength. Fibres act as a barrier
to the passage of hyaluronic acid, so it remains on the surface of the cartilage.
This limits the passage of large molecules between synovial fluid and cartilage.
II. Deep zone
Highest concentration of proteoglycans.
Collagen fibres run perpendicular to the articular surface. This forms a series of
overlapping arches, strengthens bond between articular cartilage and
underlying bone.
The network firms when the intercellular matrix binds water and swells due to
highest concentration of proteoglycan.
III. Load bearing
Some of this water is pushed out during loading of the cartilage.
When the load is removed, this water is reabsorbed by the cartilage. This
arrangement creates an ideal load-bearing surface which resists compression.
14.5Understand the differences between interfacial wear and fatigue wear of articular
cartilage.
Wear: removal of material from surfaces by mechanical action.
Interfacial wear: damage to the articular surfaces caused by lack of lubrication.
I. Abrasive: a softer surface is damaged by a harder one.
II. Adhesive: surface fragments adhere and are torn off during sliding – never
occurs in normal joints.
Example: osteoarthritis.
Fatigue wear: damage to the intercellular matrix caused by repetitive loading.
I. Occurs in normal joints.
Example: high impact activities.
14.6Discuss the likelihood of articular cartilage repairing itself.
Cartilage has a limited ability to repair itself.
I. Chondrocytes are bound in lacunae; they cannot migrate to damaged areas.
II. Avascular – oxygen and nutrients must diffuse from surrounding tissues.
III. Deposition of new matrix is slow.
IV. The growth of blood vessels into damaged cartilage is unlikely, since the forces
applied to cartilage are sufficient to collapse capillaries.
The solution to this requires intervention.
I. Surgical removal of damaged cartilage
II. Tissue grafts
III. Chondrocyte implantation
IV. Stem cell graft
The prevention to this can include glucosamine and chondroitin sulphate
supplementation.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Aims
At the end of this topic you should be able to:
a) Describe the manner in which the unique structure of cartilage permits it to perform
specific functions within the body.
b) Understand the similarities and differences between the various types of cartilage
present in the body.
c) Understand the particular structure and mechanisms of degeneration and repair of
articular cartilage.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
15. Bones and Joints of the Elbow Region.
Objectives
15.1Identify the elbow and three (3) radioulnar joints.
Elbow joint – Synovial, uniaxial, hinge. Works in the sagittal plane (flexion and extension of
the arm).
The articular surfaces of the elbow consist of the distal humerus, proximal ulna and
proximal radius.
Radioulnar joints – Synovial, uniaxial, pivot. Works in the horizontal plane (supination and
pronation)
Proximal radioulnar, intermediate (interosseous membrane) radioulnar and distal
radioulnar.
15.2Identify and briefly describe the articular surfaces of the:
I. Elbow joint
a) Trochlea of humerus
Medial, distal end of humerus.
Pulley-shaped like a groove in between the capitulum and medial
epicondyle.
b) Trochlear notch of ulna
Inside crescent shaped proximal end of the ulna.
Fits into the depression of the trochlea and articulates with the humerus in
a hinge joint formation.
c) Capitulum of humerus
Lateral, distal end of humerus .
Bony spherical protrusion that is medial to the lateral epicondyle.
d) Head of radius
Proximal end of radius.
Articulates with the Capitulum of humerus as well as the ulna.
II. Radioulnar articulations
a) Proximal (superior) radioulnar joint:
Radial notch of ulna
Lateral side of ulna.
Articulates with medial side of radius.
Head of radius
Proximal end of radius.
Articulates with radial notch on proximal end of ulna.
b) Distal (inferior) radioulnar joint:
Head of ulna
Distal end of bone.
Most medial bone in anatomical position.
Ulnar notch of radius
Distal, medial end of radius.
Lateral to ulna in anatomical position/supination.
In pronation it is on the medial side of the ulna.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Olecranon
15.3Classify and describe the movements available at the:
I. Elbow joint
Synovial hinge joint, allowing uni-axial movements of flexion and extension.
Contact areas:
The humeroulnar contact area increases from full extension to full flexion.
The head of the radius increases contact with the capitulum during flexion, with
no contact in full extension.
The closest total bony contact for the elbow joint occurs at 90˚ flexion in mid
range supination or pronation with an added load.
II. Radioulnar articulations:
a) Proximal (superior) radioulnar joint
Synovial pivot joint allows pronation and supination.
Radial head rotates against the ulna in the radial notch and is contained and
stabilised by the annular ligament.
The annular ligament wraps around the head of the radius, attaching to the
anterior and posterior margins of the radial notch on the ulna, forming an
articular surface for the radius.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
b) Intermediate radioulnar joint (interosseous membrane)
Radius and ulna are connected by the strong interosseous membrane.
A strong fibrous sheet with fibres running obliquely downwards and
medially from the radius to the ulna. Relaxed in pronation and supination
but taught in rotation.
This membrane transmits forces from the radius to ula.
Wrist: 20% load bearing ulna, 80% radius.
Elbow: 43% humeroulna joint, 57% humeroradial joint.
c) Distal (inferior) radioulnar joint
Synovial pivot joint.
Articular surfaces consists of the head of the ulna, ulnar notch of radius and
intra-articular disc (distal ulna).
Stability afforded by the interosseous membrane, intra-articular disc and
pronator quadratus.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
15.4Identify bony projections providing attachment for joint capsules, ligaments and muscles:
I. Elbow region:
Pony Projections Ligaments Joint Capsule Muscles
Medial and Ulna Collateral Ant. And Post. – Common Flexor
lateral Ligament comes Capsule joins to (CF) muscles
epicondyles of from M.E. articular margins attach to the CF
humerus Transverse band of both tendon of the
of UC runs epicondyles. M.E.
between ant. and Pronator Teres
post. attachment.
attachments. Common Extensor
Radial Collateral (CE) muscles
Ligaments comes attach to the CE
from ant., inf. tendon of the L.E.
Depression on Supinator
L.E. attachment and
anconeus.
Medial and NA Na Medial –
lateral Continued
supracondylar attachment of
ridges of humerus anconeus.
Lateral –
Brachioradialis
attachment.
Olecranon Posterior band of Not-covered Proximal
process of ulna Ulna Collateral attachment of
Ligament anconeus. Distal
attaches to attachment of
medial edge of triceps brachii.
Olecranon.
Coronoid process Anterior band of Covered One of two sites
of ulna Ulna Collateral of distal
Ligament attachment for
attaches to the brachialis
anterior surface. muscle.
Supinator crest of NA Not-covered Proximal
ulna attachment of
Supinator muscle
Radial tuberosity NA Not-covered Posterior aspect
of radius acts as distal
attachment for
biceps brachii
tendon.
Ulnar tuberosity Attachment of Not-covered Two of two sites
of ulna oblique cord of distal
ligament. attachment for
brachialis.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
II. Mid forearm
Pony Projections Ligaments Joint Capsule Muscles
Impression for NA Not-covered Distal attachment
pronator teres of pronator teres.
Note: Annular Ligament attaches to the Anterior and Posterior borders of the
Radial notch of the Ulna
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
15.5Identify and/or describe and state the functions of:
I. Joint capsules and synovial membranes of the elbow and radioulnar joints
Synovial joint surrounded by a synovial capsule shared between the
humeroulnar and radiohumeral articular components of the joint, and also
includes the proximal radioulnar articulation.
Elbow joint capsule provides part of the static soft tissue stabilising system.
No direct attachment of joint capsule to the radius so mobility at the superior
radioulnar joint is preserved.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
II. Olecranon, coronoid and radial fossae and their fat pads
a) Olecranon fossa
Depression above the back of the trochlea.
Function: Receives the olecranon process of the ulna during extension
of the forearm.
b) Coronoid fossa
Depression above trochlea.
Function: Receives coronoid process of the ulna during flexion of the
forearm.
c) Radial fossa
Depression above capitulum.
Function: Receives head of the radius at the elbow joint upon flexion of
the forearm.
d) Fat pads act as shock absorbers.
III. Ligaments of the elbow and proximal radioulnar joints
The medial and lateral collateral ligament complexes of the elbow assist in
stabilising the medial and lateral aspects of the joint.
The multidirectional nature of the ligament fibres allows effective limitations on
abduction and adduction throughout flexion and extension range of motion.
a) Ulnar (medial) collateral
Made up of several distinct bundles (anterior, posterior and transverse) to
allow the elbow joint to resist lateral forces applied to the forearm (valgus
direction – “pushing forces away from midline”) throughout flexion and
extension range.
Attaches from the medial epicondyle of the humerus to the coronoid
process (anterior) and the medial edge of the olecranon (posterior).
Function: Prevents abduction and rotation at the elbow.
b) Radial (lateral) collateral
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Passes from the lateral epicondyle of the humerus to blend with the annular
ligament on its insertion onto the radialnotch of the ulna.
This ligament protects the elbow joint from damage resulting from varus
forces (“oblique displacement of part of a limb towards the midline”)
applied to the forearm.
Function: Prevents adduction and rotations at the elbow.
c) Annular
The annular ligament wraps around the head of the radius, attaching to the
anterior and posterior margins of the radial notch on the ulna.
Function:
Prevents inferior dislocation.
Prevents lateral dislocation of proximal radioulnar joint.
Provides joint surface for proximal radioulnar joint.
IV. Interosseous membrane
A strong fibrous sheet with fibres running obliquely downwards and medially
from the radius to the lateral side of the ulna.
Functions:
Transmits forces from radius to ulna (distal radius is longer than distal ulna
and therefore receives greater impact of force).
Stabilises radius and ulna.
V. Articular disc of the distal radioulnar joint
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Triangular, fibrocartilaginous articular disc between the medial side of the
radius and lateral side of the ulna at the distal radioulnar joint (DRUJ).
The disc and radial components of the radioulnar ligaments maintain their
shape during pronation and supination while the ulnar components of the
ligaments change.
Disc is held between ligaments on both sides that extend from the ulna styloid
process to the medial aspect of the distal radius.
Functions:
Allows radius to glide and rotate over ulna during pronation/supination
movements.
Stabilises forearm and wrist and grip strength.
15.6Describe the structural relationships between the elbow joint and the superior radioulnar
joint.
The elbow joint and superior radioulnar joint share the same joint capsule and synovial
membrane that is continuous between the two joints. The radioulnar joint if connected to
the elbow joint through the annular ligament that blends with the fibres of the obliquely
oriented lateral collateral ligament of the medial epicondyle in the elbow joint.
15.7Describe the functional relationships between the radius and ulna during pronation and
supination.
Supine position: Ulna and radius are parallel to each other.
Supination is the movement that makes them parallel.
Prone position: Radius crosses anteriorly over the ulna.
Pronation is the movement that makes them cross.
Strongest pronation and supination is when elbow is flexed at 90˚.
Movements between the radius and ulna occur at the superior (proximal) and inferior
(distal) radioulnar joints:
Superior radioulnar joint – head of radius can rotate within radial notch and annular
ligament.
Inferior radioulnar joint – inferior end of radius rotates around the head of the ulna.
15.8Identify the bony features listed above on X-rays of the elbow region and forearm.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Aims
At the end of this topic, you should be able to:
a) Identify and state the functional roles of the major bony landmarks of the elbow region
b) Identify, classify and describe the specific structure and movements of the elbow and
the three (3) radioulnar joints.
c) Identify and state the functional roles of major ligaments of the elbow region.
16. Muscles of the Elbow Region.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Objectives
16.1Identify, list the attachments of, and deduce the actions of the muscles which move the
elbow and radioulnar joints (complete table at end of workbook):
I. Biceps brachii
Identify Attachments Actions
Short Head – Supination
Coracoid process Flexion of Elbow (in
(scapula), radial supination).
tuberosity (radius),
bicipital aponeurosis.
Long Head – Supination
Supraglenoid tubercle Flexion of GHJ
(scapula), Radial (weak)
tuberosity (radius),
bicipital aponeurosis.
II. Brachialis*
Identify Attachments Actions
Distal 2/3 of anterior Flexion of Elbow
shaft of humerus,
ulnar tuberosity
(ulna), coronoid
process (ulna).
III. Brachioradialis
Identify Attachments Actions
Upper 2/3 of lateral Flexion of Elbow
supracondylar ridge Supinate a pronated
(humerus) forearm to neutral
position (and
opposite).
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
IV. Triceps brachii
Identify Attachments Actions
Long Head – Extension of Elbow
Infraglenoid tubercle Adduction of GHJ
(scapula), olecranon Extension of GHJ
process (ulna). from flexed position.
Lateral Head – Extension of Elbow
Posterior shaft of
humerus (above and
lateral to spiral
groove), olecranon
process (ulna).
Medial Head – Extension of Elbow
Posterior shaft of
humerus (below and
medial to spiral
groove), olecranon
process (ulna).
V. Anconeus*
Identify Attachments Actions
Posterior lateral Extension of Elbow
epicondyle (humerus),
lateral surface of
olecranon process
(ulna), Proximal ¼
posterior ulna.
VI. Pronator teres
Identify Attachments Actions
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Medial supracondylar Pronate Forearm
ridge (humerus) via
medial epicondyle
(humerus), medial
proximal ulna,
impression on mid
shaft of radius.
VII. Pronator quadratus*
Identify Attachments Actions
Distal ¼ anterior ulna, Pronate Forearm
Distal ¼ anterior
radius.
VIII. Supinator
Identify Attachments Actions
Lateral epicondyle Supinate Forearm
(humerus), supinator Extension of Elbow
crest (ulna), proximal
shaft of radius
(posterior, lateral and
anterior).
[*uni-articular muscles]
16.2Identify the cubital fossa and state its boundaries and contents.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Boundaries:
Triangular hollow located on the anterior elbow.
Medial boundary: flexor/pronator muscle group (pronator teres)
Lateral boundary: extensor/supinators muscle group (brachioradialis)
Superior boundary = imaginary line from lateral epicondyle to medial epicondyle
Contents:
Biceps tendon
Brachial artery
Median nerve
Superficial layer (roof):
o Skin
o Fascia
o Median cubital vein
o Lateral and medial cutaneous nerve of forearm
o Bicipital aponeurosis
Deep boundary:
o Brachialis
o Supinator
16.3Describe the location and state the functions of the major elbow bursae:
A bursa is a fluid filled sac that reduces friction between a bone and the overlying muscles
or tendons.
I. Subcutaneous olecranon
Located between the skin and the olecranon process.
‘Cushions’ the olecranon process.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
II. Subtendinous olecranon
Lies between the triceps tendon attachment and the olecranon.
Reduces friction on the triceps tendon during elbow extension.
III. Radioulnar
Located between the extensor digitorum, radiohumeral articulation and the
supinators muscle.
Reduces friction between the radiohumeral joint and overlying muscles.
IV. Bicipitoradial
Between the biceps tendon and the radial tuberosity.
Reduces friction between the biceps tendon and proximal radius during
pronation and supination of the forearm.
16.4List the muscles which attach to the:
I. Distal humerus
a) Medial epicondyle
Pronator Teres
b) Lateral epicondyle
Anconeus Supinator
c) Medial supracondylar ridge
Pronator Teres
d) Lateral supracondylar ridge
Brachioradialis
II. Radius
a) Radial tuberosity
Biceps Brachii
b) Lateral surface of mid-shaft
Pronator Teres Supinator
III. Ulna
a) Olecranon process
Triceps Brachii Anconeus
b) Coronoid process
Brachialis
c) Ulnar tuberosity
Brachialis
16.5 List the muscles which produce:
I. Movements of the elbow
a) Flexion
Biceps Brachii Brachialis Brachioradialis
b) Extension
Triceps Brachii Anconeus
II. Movements of the radioulnar joints
a) Flexion
Biceps Brachii Supinator
b) Extension
Pronator Teres Pronator Quadratus
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Aims
At the end of this topic, you should be able to:
a) Identify and state the actions of the muscles responsible for each elbow and radioulnar
joint movement.
b) Identify and describe the cubital fossa.
c) Describe and state the functions of major elbow bursae
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
17. Functional Anatomy of the Elbow Region
Objectives
17.1Define the terms “spurt” and “shunt” as they apply to muscle function.
Shunt Muscles have a stability role. They direct contractile force along the bone and hence
act to press bones together rather than move them.
Spurt Muscles have a mobility role. They direct more contractile forces across the bone
rather than along it and hence act to move the bone. The fixed attachment of the muscle is
distant from the joint, whilst the moving attachment is closer to the joint.
17.2List the features that differentiate spurt and shunt muscles.
In shunt muscles: The fixed attachment of the muscle is close to the joint, whilst the moving
attachment is far from the joint.
In spurt muscles: The fixed attachment of the muscle is distant from the joint, whilst the
moving attachment is closer to the joint.
17.3List and identify elbow muscles that act as spurt and shunt muscles during elbow and
forearm movements.
Shunt muscles:
I. Brachioradialis – elbow flexion.
II. Common Extensor Origin and Common Flexor Origin – form part of static
constraints of elbow joint.
Spurt muscles:
I. Biceps brachii – elbow flexion and supination.
II. Brachialis – elbow flexion.
17.4Explain how muscle recruitment patterns for elbow region muscles vary with changing
conditions relating to:
Joint angles – a muscle is usually more efficient in mid range. This can be modified by
training.
I. Position of shoulder joint
Changing the upper arm elevation will change the muscles that work (e.g. the
effects of gravity on movement).
Long head of triceps roles in arm flexion/abduction.
II. Position of radioulnar joints
Pronated forearm – brachialis works mostly.
Neutral forearm – brachialis and brachioradialis work to flex the elbow.
Supinated forearm - brachialis and biceps brachii work together to flex the
elbow.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
III. Degree of elbow flexion
From 0-90degrees, brachialis and biceps perform elbow flexion as they
concentrically contract against gravity. More strength and torque at 90˚ elbow
flexion.
From 90-180degrees, gravity is pulling the arm down therefore muscles must try
to break down (slow) the contraction so eccentric contraction of the triceps
occurs.
IV. Load/resistance
Increased load will increase the amount of muscle fibres needed to perform the
task and thus may require additional input from synergist muscle groups
More muscles will be involved and will be contracting more muscle fibres.
For example, in elbow flexion against large resistance, you recruit more muscles
so that you have more power, thus you would use Brachialis, then
Brachioradialis, then Biceps, the Pronator Teres all to help the action.
V. Velocity of motion
Increased speed increases the role of the elbow stabiliser (shunt).
Increased speed of arm movements leads to co-activation of muscles around
the elbow.
This effect also applies to fast and complicated hand movements to ensure a
stable (lower arm) base for the hand action to best transmit forces.
Brachialis is the preferred dynamic stabiliser of the elbow during rapid
alternation of elbow flexion/extension because it is the closest to the joint and
requires the least synergistic activity.
17.5Analyse muscle recruitment patterns during:
I. Full elbow flexion with the shoulder held at 90abduction in the coronal plane
and in external rotation
0˚-90˚ elbow flexion –
Brachialis.
Biceps brachii.
90˚-180˚ elbow flexion –
Eccentric triceps brachii (moving with gravity so trying to break down and slow
the contraction).
II. Full elbow extension with the shoulder held at 30in the sagittal plane
Brachialis throughout range of movement.
Biceps brachii if supination.
17.6List the static and dynamic features of the elbow and radioulnar joints that contribute to
their:
I. Stability
Static Dynamic
Bony: Variable levels of muscle activation.
Olecranon fits snugly into olecranon Synergistic group arrangements
fossa (extension). depending on task.
Ridged shape of trochlear notch and Muscles positioned for shunt role to
trochlear of humerus. stabilise elbow joint during movement
Bony contact at superior and inferior (e.g. CEO, CFO, brachioradialis).
radioulnar joints.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Ligamentous:
Lateral (radial) and medial (ulnar)
ligament complex at elbow.
Interosseus membrane holding radius
and ulna together
Annular ligament containing radial
head in position.
Soft tissue contraints (CEO and CFO).
II. Mobility
The elbow moves in 2 directions (flexion/extension) as does the forearm
(pronation/supination) – bony alignment.
The muscles performing the elbow flexion and extension tasks are strong,
reflecting the typical lifting type demands on the arm.
Versatile arrangements of muscle groups allow the actions to occur in varying
orientations or elevations of the upper limb.
Aims
At the end of this topic you should be able to:
a) Define and differentiate spurt and shunt muscles as applied to the elbow and forearm.
b) Explain muscle recruitment patterns for functional activities involving the elbow and
forearm.
c) List features which contribute to the stability and mobility of the elbow and forearm
regions.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Module 2 – Hard Tissues, Distal Upper Limb, and Neurovascular Supply of Upper Limb
18. Bone Tissue and Growth of Bones
Objectives
18.1Describe the structure of bone tissue in terms of its organic and inorganic
components and their properties.
Generalised Structure:
Various bone cells. The four types of bone cells make up only 2% of bone mass.
Osteocytes
o Mature bone cells that maintain the bone matrix (“cyte” means mature).
o Live in lacunae.
o Are between layers (lamellae) of matrix.
o Connect by cytoplasmic extensions through canaliculi in lamellae.
o Do not divide.
o Functions:
Maintain protein and mineral content of matrix.
Help repair damage bone.
Osteblasts
o Immature bone cells that secrete matrix compounds (osteogenesis).
o Osteoid – matrix produced by osteoblasts, but not yet calcified to form
bone.
o Osteoblasts surrounded by bone become osteocytes.
o Bone building is done by osteoblasts.
Osteoprogenitor cells
o Mesenchymal stem cells that divide to produce osteoblasts.
o Located in endosteum and the inner cellular layer of periosteum.
o Assist in fracture repair.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Osteoclasts
o Secrete acids and protein-digesting enzymes.
o Giant, multinucleate cells.
o Dissolve bone matrix and release stored mineral (osteolysis).
o Derived from stem cells that produce macrophages.
o Bone recycling is done by osteoclasts.
Intercellular matrix:
o Collagen fibres
Gives strength and resilience
o Proteoglycans, glycoproteins and phosphoproteins
All these are linked to bone growth
o Inorganic minerals (mainly calcium phosphate)
Lie along and between collagen fibres
If bone is demineralised (without minerals) the bone can bend
Resilience to all types of stresses
o Water only makes up 10% of total bone weight (thus bone must have its
own blood supply)
Organic Component:
o 25% of bone weight
o Cells and collagen fibres embedded in glycoproteins, phosphoproteins and
Proteoglycans
o Responsible for STRENGTH and RESILIENCE of bone
o Decreases with age which leads to bones becoming fragile in the elderly
Inorganic Component:
o 75% of total bone weight
o Mainly calcium phosphate in crystalline form (hydroxyapatite), plus water
o Responsible for HARDNESS and RIGIDITY of bone
o If lost the bone becomes dangerously flexible
18.2Describe the structure of the two types of bone tissue (spongy and compact) in
terms of their specific functions.
Spongy Bone
Does not have osteons
The matrix forms an open network of Trabeculae
Trabeculae have no blood vessels
The space between Trabeculae is filled with red bone marrow which has blood
vessels - forms red blood cellsand supplies nutrients to osteocytes.
Yellow bone marrow - in some bones, spongy bone holds yellow bone
marrow. It is yellow because it stores fat.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Compact Bone
Osteon (Haversian system) is the basic unit.
Osteocytes are arranged in concentric lamellae around a central canal
containing blood vessels.
Perforating (Volkmann's) canalsrun perpendicular to the central canal, carrying
blood vessels into bone and marrow.
Circumferential Lamellae - lamellae wrapped around the long bone, binding
osteons together.
Compact bone is covered with a membrane.
o Periosteum on the outside.
Covers all bones except parts enclosed in joint capsules.
Made up of an outer, fibrous layer and an inner, cellular layer.
Perforating fibres: collagen fibres of the Periosteum.
Connect with collagen fibres in bone.
Also connects with fibres of joint capsules – attaches
tendons and ligaments.
Functions:
Isolates bone from surrounding tissues.
Provides a route for circulatory and nervous supply.
Participates in bone growth and repair.
o Endosteum on the inside.
An incomplete cellular layer:
Lines the medullary (marrow) cavity.
Covers Trabeculae of spongy bone.
Lines central canals.
Contains osteoblasts, osteoprogenitor cells and
osteoclasts.
Active in bone growth and repair.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
18.3Describe the following features of bone tissue:
I. Compact Bone
For weight bearing activites. Found on outside of any bone – 80% of
skeleton made up of compact bone. Dense type of tissue because of
weight-bearing function. Organised into osteons (Haversian systems)
[longitudinal canals that run longitudinally through bone].
a) Haversian Canals
Central canals within osteons
Contain blood vessels
Lymph and nerves as a site for nutrient/waste exchange [not
enough liquid for diffusion]
b) Volkmann’s Canals
Contain blood vessels that also link osteons to one another.
Running horizontally through bone perpendicular to Haversian
canals and surface
c) Lacunae
Depressions in intercellular matrix
Contain osteocytes (one per lacunae)
d) Concentric Lamellae
Plates of bone
Concentric rings of intercellular matrix - strengthens bone
e) Canaliculi
Minute canals radiating out from each lacunae
Contain the cytoplasmic processes of osteocytes.
Radiating out from lacunae, allow osteocytes to communicate with
neighbours (inter-lacunae communication)
f) Bone Marrow
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Red bone marrow forms blood cells, 50% of marrow in adults, only
in axial skeleton.
Yellow bone marrow contains adipose tissue = vital energy reserve
and not found in children, in appendicular skeleton of adults and
skull
g) Periosteum
Covers the outer surface of the bones
Inner layer which is cellular and can form bone cells if required
Anchored to the bone by Sharpey’s fibres
Functions to:
Isolate the bone from surrounding tissues
Provide a route for the circulatory and nervous supply
Actively participate in bone growth and repair
II. Spongy Bone
Located where bones are not heavily stressed or where stress is from many
directions. Does not have osteons. Canaliculi contain the cytoplasmic
processes of osteocytes. No Haversian systems and no Volkmann’s canals
are present , therefore no blood vessels through (must rely on diffusion for
movement of nutrients IN and wastes OUT).
Finite point of growth of spongy bone due to limited blood supply - finite
point to which they can enlarge .
a) Trabeculae
Matrix of struts and plates
Isn’t completely solid = allows nutrients to diffuse in from
surrounding areas {no Haversian canals/Volkmann’s canals}
b) Lacunae
Depressions containing osteocytes, communicate with adjacent
osteocytes through Canaliculi (narrow passageways)
c) Marrow Spaces between Trabeculae
Contain either red or yellow bone marrow
18.4Briefly describe the mechanisms by which long bones grow in length and
diameter.
Bone growth and maintenance is assisted by the hormone calcitriol with helps
absorb calcium and phosphorus from digestion.
There are three phases of bone development:
I. Osteogenesis – bone formation
Nutrient Artery and Vein – a pair of large blood vessels that enter the
diaphysis through the nutrient foramen (the femur has more than one
pair).
Metaphyseal Vessels – supply the epiphyseal cartilage where bone
growth occurs.
Periosteal Vessels – blood supply to superficial osteons and secondary
ossification centres.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
The Periosteum also contains a network of lymphatic vessels and
sensory nerves.
II. Ossification – bone tissue replacement
Calcification occurs during ossification where calcium salts are
deposited.
Two forms of ossification:
o Endochondral
Ossifies bone that originate as hyaline cartilage (most bones).
Chondrocytes secrete Enzymes (alkaline phosphatase) to
begin the Process of mineralization.
Bone collar formation - blood vessels infiltrate and
osteoblasts secrete osteoid against the cartilage model
Internally, chondrocytessecrete vascular endothelial growth
factor (VEGF)promoting blood vessel invasion and bringing
osteoprogenitor cells, osteoblasts and osteoclasts
Medulla cavity forms
Same process occursin secondary ossification sites(epiphysis,
but no medulla)
Compact bone thickens and strengthens long bone with layers
of circumferential lamellae
When long bones stop growing after puberty, epiphyseal
cartilage disappears.
As long bones mature osteoclasts enlarge medullary (marrow)
cavity and osteons form around blood vessels in compact
bone.
o Intramembranous
Produces flat bones such as mandible and clavicle.
Formation of matrix within fibrous membrane
Formation of woven bone and Periosteum
Formation of compact bone plates
18.5Briefly describe the sequence of events occurring during repair of a fractured
bone.
Fractures are cracks or breaks in bones caused by physical stress.
They are repaired in four steps:
I. Bleeding
Produces a clot (fracture haematoma)
o Haematoma: localised mass of blood released from blood vessels
but confined within an organ or space.
Establishes a fibrous network.
Bone cells in the area die.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
II. Cells of the endosteum and periosteum.
Divide and migrate into fracture zone.
Calluses stabilise the break.
o External callus of cartilage and bone surrounds break.
o Internal callus develops in medullary cavity.
III. Osteoblasts
Replace central cartilage of external callus with spongy bone.
IV. Osteoblasts and osteocytes remodel the fracture for up to a year.
Reducing bone calluses.
Aims
At the end of this topic, you should be able to:
a) Describe the manner in which the unique structure of bone permits it to perform specific
functions within the body.
b) Describe the similarities and differences between the two types of bone tissue present in
the body.
c) Understand the sequence of events by which long bones grow in length and diameter.
d) Understand the mechanism of fracture repair.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
19. Bones and Joints of the Wrist and Hand
Objectives
19.1Identify the following bones of the wrist and hand, and some of their features:
I. Styloid processes of radius and ulna
Distal end on radius and ulna.
II. 8 carpal bones
She Looks Too Pretty Try To Catch Her (proximal – lateral to medial, then
distal row lateral to medial).
Proximal row:
a) Scaphoid and its tubercle
Most commonly fractured as it is direct point of impact when you fall
on your wrist – lateral.
b) Lunate
Most commonly dislocated, shaped like a crescent moon - middle of
proximal row.
c) Triquetrum
Sits below pisiform, articulates with 3 bones – medial.
d) Pisiform
Sits on top of triquetrum, easy to palpate sesamoid bone – medial.
Distal row:
a) Trapezium and its tubercle
Articulates with metacarpal of thumb – lateral.
b) Trapezoid
Named after shape – lateral.
c) Capitate
‘Captain’ carpal bone, base of middle finger, very stable, attachment
site, biggest bone, axis of hand goes through it.
d) Hamate and its hook
Shaped like a hammer, projects forward into palm – medial.
III. Heads, shafts and bases of metacarpals
Head is more distal, shaft is long body of the bone, base attaches to the
carpal bones. Named by roman numerals (I-V), starting at the thumb.
IV. Heads, shafts and bases of proximal, middle and distal phalanges
Each digit made up of three phalanges: proximal, middle and distal
Thumb only has two phalanges: proximal and distal
Again the head is more distal, shaft is long body of the bone, base attaches to
the metacarpal bones (proximal) and phalanges (middle, distal).
V. Sesamoid bones at base of proximal phalanx of thumb (on X-rays only)
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
19.2Identify and classify the radiocarpal (wrist) (RC) joint and:
Radiocarpal Joint is synovial, ellipsoid (biaxial) allowing flexion/extension and
adduction (ulnar deviation)/abduction (radial deviation).
I. Identify its articular surfaces
Articular disc of ulna, distal end of radius, scaphoid, lunate and triquetrum of
proximal row of carpal bones (carpal condyle).
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
II. Describe the attachments of its joint capsule
Fibrous joint capsule completely encloses joint. Distal edges of radius and
ulna anteriorly and posteriorly. Laterally and medially attached to the radial
and ulnar styloid processes respectively.
Distally – capsule firmly attached to margins of articular surfaces of proximal
row of carpal bones.
Medially – passes to the medial side of the triquetrum and laterally to the
lateral side of the Scaphoid.
III. Identify and state the functions of its ligaments:
a) Dorsal radiocarpal
Capsular ligament attaching from posterior edge of distal end of
radius to posterior surface of the scaphoid, lunate and triquetrum.
Fibres run downwards and medially, principally to the triquetrum and
continuous with dorsal intercarpal ligaments. This ligaments limits
flexion and ulnar deviation.
b) Palmar radiocarpal
Capsular ligament attaching the anterior edge of distal radius and
styloid process, to the anterior surface of proximal row of carpal
bones. Some of the fibres even attach to the Capitate (are extended).
Broad band of fibres passing downwards and slightly medially. This
ligament limits extension and ulnar deviation.
c) Palmar ulnocarpal
Capsular ligament attaching the anterior edge of articular disc and
the base of the ulnar styloid process, to the anterior surface of the
proximal carpal bones. Fibres extend downward and laterally. This
ligament limits extension of the radiocarpal joint.
d) Radial collateral carpal
Extracapsular ligament that attaches the tip of the radial styloid
process to the lateral side of the scaphoid, immediately adjacent to
it’s proximal articular surface and lateral side of the trapezium. This
ligament limits ulnar deviation and prevents rotation.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
e) Ulnar collateral carpal
Extracapsular (Rounded cord) that attaches the ulnar styloid process
to the base of the pisiform and the medial and posterior non-articular
surfaces of the triquetrals. This ligament limits abduction (radial
deviation) and prevents rotation.
IV. Demonstrate its movements
Flexion and extension about a transverse axis in the sagittal plane
Flexion:
o Greater range of motion than extension about 50°
Extension:
o Range of 35°
o Movements are limited by the margins of the radius because the
posterior margin extends further distally than the anterior margin.
Abduction and adduction about an Anteroposterior axis in the coronal plane
Abduction (radial deviation)
o Movement of the hand towards the radius
o Movement of proximal row of carpal bones in relation to the distal
end of the radius
o Quite limited due to long radial styloid process - only 7° of motion
Adduction (ulnar deviation)
o Movement of the hand towards the ulna
o Has greater range of about 30° until the Scaphoid tubercle impacts
on the radial styloid process
19.3Identify and classify the intercarpal joints.
Any joints between the 8 carpal bones are named according to bones involved (e.g.
scapho-lunate joint, capito-hamate joint). They are synovial, plane (multiaxial)
joints. Very little movement possible due to restrictions placed on them by
surrounding ligaments.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
19.4Identify the midcarpal (MC) joint and:
Synovial, ellipsoid, biaxial joint, between the proximal and distal rows of carpal
bones.
I. Identify its articular surfaces
Proximal and distal row carpal bones with each row acting like a single
articular surface.
II. Briefly describe its joint capsule
Fibrous joint capsule, composed mostly of irregular bands of fibres running
between the rows of bones.
Anteriorly – palmar ligaments
Posteriorly – dorsal ligaments
Sides of joint capsule are strengthened by collateral ligaments.
III. Identify and state the functions of its ligaments:
a) Palmar intercarpal
Also known as the radiate capitate ligament, attaches the bones of
the proximal row to the head of the capitate. This limits flexion and
ulnar deviation.
b) Dorsal intercarpal
Attaches the bones of one row the bones of the other. This limits
extension and ulnar deviation.
c) Radial collateral
Strong distinct band attaching the scaphoid to the trapezium. It is a
continuation of the radial collateral carpal ligament of the radiocarpal
joint. This ligament limits extension of the radiocarpal joint.
d) Ulnar collateral
Attaches the triquetrum to the hamate. It is a continuation of the
ulnar collateral carpal ligament of the radiocarpal joint. This limits
ulnar deviation and prevents rotation.
IV. Demonstrate its movements.
Flexion:
o Movement of the palm towards the anterior surface of the forearm
o 35° of movement past anatomical position
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Extension:
o Movement of the dorsal surface towards the posterior surface of
the forearm
o 50° of movement past anatomical position is usually possible
Abduction:
o Movement of the lateral carpals towards the radius
o 8° of movement past anatomical position
Adduction:
o Movement of the medial carpals towards the ulna
o 15° of movement past anatomical position
19.5State the relative contributions of radiocarpal and midcarpal joints to the
movements of the wrist joint complex.
Abduction (radial deviation)
o Radiocarpal joint provides 7° of movement
o Mid carpal joint provides 8° of movement
Adduction (ulnar deviation)
o Radiocarpal joint provides 30° of movement
o Midcarpal joint provides 15° of movement
Flexion
o Radiocarpal joint provides 50° of movement
o Midcarpal joint provides 35° of flexion
Extension
o Radiocarpal joint provides 35° of movement
o Midcarpal joint provides 50° of movement
19.6Identify and classify the common carpometacarpal (CM) joint and:
Multiaxial, Plane joint, does not include 1st metacarpal.
I. Identify its articular surfaces
Base of metacarpal II-V [most mobile towards metacarpal V], and the
Trapezoid, Capitate, Hamate [medial 3 carpal bones from distal row].
Together form CMC joint, which has an irregular joint line.
II. Identify and state the functions of its ligaments:
a) Palmar carpometacarpal
Attaches the distal row of carpal bones to the bases of the
metacarpals. This functions to thicken the joint capsule, holds the
metacarpals and carpals together.
b) Dorsal carpometacarpal
Attaches the distal row of carpal bones to the bases of the
metacarpals. Series of bands of fibres. In general, each metacarpal
receives 2 bands. This functions to thicken the joint capsule, holds
metacarpals and carpals together.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
III. Demonstrate its movements.
Very little movement at this joint. Second and Third Carpals are essentially
immobile. Slight amounts of gliding may occur between the fourth
metacarpal and the hamate. Fifth metacarpal shows the only appreciable
movements as it glides on the hamate due to the oblique joint surfaces.
Flexion/slight rotation during opposition experienced.
19.7Identify and classify the carpometacarpal (CM) joint of the thumb and:
Synovial, saddle and biaxial joint.
I. Identify its articular surfaces
1st metacarpal and Trapezium. Reciprocally shaped joint surfaces (concavo-
convex). Loose capsule.
II. Identify and state the functions of its ligaments:
a) Radial carpometacarpal
Attaches adjacent lateral surface of trapezium to the first metacarpal.
This functions to hold the bones together and prevent abduction.
b) Anterior Oblique
Attaches anterior surface of the trapezium to the medial side of the
first metacarpal, converging with the posterior oblique ligament as it
does so. This functions to prevent unwanted/excessive extension.
c) Posterior Oblique
Attaches the posterior surface of trapezium to the medial side of the
first metacarpal, converging with the anterior oblique ligament as it
does so. This functions to prevent unwanted/excessive flexion.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
III. Describe and demonstrate its movements using the plane of the hand as
the basic movement reference plane.
Abduction/Adduction (perpendicular to the palm of the hand)
Abduction – move thumb anteriorly away from the palm of the hand
Adduction – move thumb back to the palm of the hand
Flexion/Extension (in the plane of the palm of the hand)
Opposition
o Distal pad of the thumb brought against the distal pad of any other
digit
o Involves flexiona and abduction at CMC, rotation of the metacarpal
then adduction at the CMC joint.
o Stages:
19.8Identify and classify the metacarpophalangeal (MCP) joints and:
Synovial, Condyloid, Biaxial joint.
I. Identify its articular surfaces
Head of the metacarpal (biconvex, with unequal curvatures transversely and
anteroposteriorly) and the base of the proximal phalynx (biconcave, smaller
articular surface than metacarpal head).
II. Identify and state the functions of its ligaments:
a) Collateral
b) Attaches the tubercle and adjacent depression on the side of the
head of the metacarpal to the palmar aspect of the side of the base
of the proximal phalanx. Very strong and tight in flexion, loose in
extension.
Its function is to prevent/limit unwanted abduction and adduction of
the digits.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
c) Palmar
Attaches the anterior margin of the base of proximal phalanx to the
loosely attached to the neck of the metacarpal (proximally). Dense
fibrocartilaginous plate firmly attached. Receives some fibres from
the collateral ligaments. Moves with the proximal phalanx.
Its function is to increase surface area of the articulating surface of
the base of the proximal phalanx.
d) Deep Transverse Metacarpal
Series of short ligaments. Continuous with the palmar interosseous
fascia and blend with the fibrous tendons.
Attaches the palmar ligaments of the four metacarpophalangeal
joints of the fingers.
III. Describe and demonstrate its movements.
For the thumb:
o Flexion range of 45°
o Extension range of 0°
o Abduction range of 15°
o Adduction is negligible
o Axial Rotation - at MCP joint during opposition
For the digits:
o Flexion range of 90°
o Extension active range of 50° but may reach 90° during passive
extension
o Abduction/Adduction limited due to the width of the metacarpal
head, 30° in each direction limited by the bones and collateral
ligaments which become taught.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
19.9Identify and classify the interphalangeal (IP, PIP, DIP) joints and:
Synovial, hinge and uniaxial. Thumb only has 1 IP joint (2 phalanges) but the digits
have PIP and DIP (3 phalanges).
I. Identify its articular surfaces
PIP – head of proximal and base of middle phalynx
DIP – head of middle and base of distal phalynx
IP joint of thumb – pulley-shaped head of the proximal phalynx and the base
of the distal phalynx. Fibrocartilaginous plate (palmar ligament) attaches to
the anterior margin of the base of the distal phalynx.
II. Identify and state the functions of its ligaments:
a) Collateral
Attaches the sides of the head of the most proximal phalanx to the
sides of the base of the adjacent, more distal phalanx (blending with
the margins of the palmar ligament). Becomes increasingly tense with
flexion at the joint.
It functions to prevent adduction and abduction of the joint.
b) Palmar
Attaches the tubercle and adjacent depression on the side of the
head of the metacarpal to the palmar aspect of the side of the base
of the proximal phalanx. Very strong.
III. Describe and demonstrate its movements.
Flexion: moving the anterior surface of the more distal phalynx to the
anterior surface of more proximal phalynx
o Range greater than 90°
o PIP flexion >90° for all fingers, gradually increases towards little finger
(up to 135°)
o DIP flexion <90 °, decreases from 90 at little finger down to index
Extension: Moving the posterior surface of the more distal phalynx
towards the posterior surface of the more proximal phalynx
o Extension of IP, DIP and PIP is minimal (range less than 10°)
o DIP <5°
o PIP <2°
Small degrees of massive side to side movement (adduction/abduction) is
possible due to the nature of the joint
19.10 Describe accessory (operator-directed) movements of the joints of the hand.
I. Wrist Joint
Distal end radius can be moved anteroposteriorly when gripped
When the distal ends of the radius and ulna are firmly gripped the head
of the ulna can be moved anteroposteriorly
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
II. Intercarpal Joint
Anteroposterior gliding can occur between adjacent carpal bones if
gripped
III. Midcarpal Joints:
Anteroposterior movements can occur when the distal and proximal rows
are gripped separately
IV. Joints of the Fingers:
Common CMC Joints: slight anteroposterior gliding can be produced b/w
base of the metacarpal and its adjacent carpal bone with the right
pressure
MCP and IP Joints: Anteroposterior gliding and rotation
V. Joints of the Thumb
CMC Joint = base of MC I can be moved anteroposteriorly, mediolaterally
and longitudinal gapping and rotation
MCP and IP Joint = anteroposterior gliding and rotation and longitudinal
gapping at MCP joint.
19.11 Describe the location of the ‘axis of the hand’ and state the digital movements
that are made in reference to this axis.
Imaginary axis running the length of the hand – extends from distal phalynx of the
middle finger down the hand between Thenar and Hypothenar eminence
Digital Movements:
o Flexion and Extension of digits occur in sagittal plane
o Flexion and Extension of the thumb occurs in the coronal plane (in
anatomical position)
o Abduction and Adduction occur in coronal plane
o Index finger has a considerable degree of freedom
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
19.12 Explain ‘opposition’ in terms of the sequence of movements that occur at the:
Opposition is when the distal pad of the thumb is brought against the distal pad of
any of the remaining digits. It involves flexion, abduction, and rotation followed by
adduction at CMC joint.
I. CM, MCP and IP joints of the thumb
At CMC
Initially flexion and abduction of the thumb occur simultaneously due to
flexor pollicis longus, flexor pollicis Brevis and abductor pollicis longus.
CMC joint is flexed and abducted
Adduction (axial rotation) is later produced by adductor pollicis
At MCP
MCP joint abduction and flexion caused by flexor pollicis longus and
Brevis, abductor pollicis longus and opponens pollicis.
MCP Joint is flexed and abducted
At IP
Slight flexion
II. MCP, PIP and DIP joints of the digits
At MCP
Flexion caused by lumbricals
Passive axial rotation of little finger
Movements of little finger (5th digit)
At IP
Extension cause by lumbricals
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
19.13 Identify the bones, bony features and joints listed above on X-rays of the wrist
and hand.
Aims
At the end of this topic, you should be able to:
a) Identify the bones of the wrist and hand.
b) Identify and state the functions of the major markings of the bones of the wrist and hand.
c) Classify and describe the specific structure and movements of the joints of the wrist and
hand.
20. Muscles of the Forearm and Functional Anatomy of the Wrist Joint Complex
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Objectives
20.1Identify, list the attachments and deduce the action(s) of the muscles of the
forearm (on table at end of workbook) with particular attention to major muscles
that act on the wrist joint complex (shown in italics):
I. Flexor (anteromedial) group:
a) Superficial layer
These muscles attach to the medial epicondyle of the humerus (common
flexor origin) and spread across the forearm. 8 in total – 5 superficial, 3
deep.
i. Pronator teres
Identify Attachments Actions
Medial Pronate Forearm
supracondylar ridge Weak Flexor
(humerus) via medial
epicondyle
(humerus), medial
proximal ulna,
impression on mid
shaft of radius.
ii. Flexor carpi radialis
Identify Attachments Actions
Medial epicondyle Wrist Flexion
(humerus), bases of Wrist Abduction
metacarpal 2 and 3. (radial deviation)
Pronate
Flex Elbow Flexion
(Prevents
unwanted
extension of wrist
when extending
fingers)
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
iii. Palmaris longus
Identify Attachments Actions
Medial epicondyle Wrist Flexion
(humerus), palmar (weak)
aponeurosis, flexor
retinaculum
iv. Flexor digitorum superficialis
Identify Attachments Actions
Medial epicondyle of MCP and PIP
humerus, coronoid Flexion
process of ulna, Wrist Flexion
proximal 2/3
anterior radius
anteriorly,
bases of middle
phalanges of digits 2-
5
FDS splits to allow
FDP to attach more
distally.
v. Flexor carpi ulnaris
Identify Attachments Actions
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Medial epicondyle of Wrist Flexion
humerus, olecranon Wrist Adduction
process of ulna, (ulna deviation)
proximal 2/3 (Synergist in
posterior ulna extension of
posteriorly, via fingers, preventing
pisiform to hook of unwanted
hamate and base of extension)
metacarpal 5
b) Deep layer
i. Flexor digitorum profundus
Identify Attachments Actions
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Coronoid process of Flexion of DIP joint
ulna, Proximal ¾ Flexion of PIP,
ulna, Middle 1/3 MCP and wrist
interosseus joint.
membrane, Bases of
distal phalanges of
digits 2-5
ii. Flexor pollicis longus
Identify Attachments Actions
Anterior surface of Flexion of IP joint
radius, adjacent in thumb
interosseous Flexion MCP and
membrane, base of CMC joint of
distal phalanx of thumb
thumb
iii. Pronator quadratus
Identify Attachments Actions
Distal ¼ anterior ulna Pronate Forearm
anteriorly
Distal ¼ anterior
radius anteriorly
II. Extensor (posterolateral) group:
a) Superficial layer
These muscles attach to the lateral epicondyle of the humerus (common
extensor origin). 12 in total – 7 superficial, 5 deep.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
i. Brachioradialis
Identify Attachments Actions
Upper 2/3 of lateral Flexion of Elbow
supracondylar ridge Supinate a
(humerus), styloid pronated forearm
process of radius to neutral position
(and opposite).
ii. Extensor carpi radialis longus
Identify Attachments Actions
Lateral supracondylar Extension of wrist
ridge of humerus, Abduction of wrist
occasionally to lateral (radial deviation)
epicondyle of Flexion of elbow
humerus (via CEO),
base of metacarpal 2
iii. Extensor carpi radialis brevis
Identify Attachments Actions
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Lateral epicondyle of Extension of wrist
humerus (via CEO), Abduction of wrist
base of metacarpal 3 (radial deviation)
iv. Extensor digitorum
Identify Attachments Actions
Lateral epicondyle of Extension of MCP
humerus (via CEO), via Extension of PIP
dorsal digital and DIP
expansion (extensor Extension of wrist
aponeurosis) to bases
of middle and distal
phalanges of digits 2-5
v. Extensor digiti minimi
Identify Attachments Actions
Lateral epicondyle of Extension of MCP,
humerus (via CEO), via DIP and PIP of little
dorsal digital finger
expansion (extensor Adduction of Wrist
aponeurosis) to digit 5 (ulnar deviation)
Extension of wrist
vi. Extensor carpi ulnaris
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Identify Attachments Actions
Lateral epicondyle of Extension of wrist
humerus (via CEO), Adduction of Wrist
base of metacarpal 5 (ulnar deviation)
vii. Anconeus
Identify Attachments Actions
Posterior lateral Extension of
epicondyle Elbow
(humerus), lateral
surface of olecranon
process (ulna),
Proximal ¼ posterior
ulna.
b) Deep layer
i. Supinator
Identify Attachments Actions
Lateral epicondyle Supinate Forearm
(humerus), supinator Extension of Elbow
crest (ulna), proximal
shaft of radius
(posterior, lateral
and anterior).
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
ii. Abductor pollicis longus
Identify Attachments Actions
Proximal posterior Abducts Thumb
ulna, Middle 1/3 Extends Thumb at
posterior radius, CMC
Adjacent
interosseous SNUFF BOX
membrane, base of
metacarpal 1
iii. Extensor pollicis longus
Identify Attachments Actions
Middle 1/3 posterior Extends Thumb
ulna, Adjacent Extension and
interosseous Abduction of Wrist
membrane, base of
distal phalanx of SNUFF BOX
thumb
iv. Extensor pollicis brevis
Identify Attachments Actions
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Middle part of Extends CMC and
posterior radius, MCP of Thumb
adjacent Extension and
interosseous Abduction of Wrist
membrane, base of
proximal phalanx of SNUFF BOX
thumb
v. Extensor indicis
Identify Attachments Actions
Distal posterior ulna, Extends Index
adjacent (MCP joint) and via
interosseous dorsal digital
membrane, dorsal expansion (DIP and
digital expansion PIP)
(extensor Extends Wrist
aponeurosis) of digit
2
20.2List the muscles acting on the wrist which attach to the:
I. Humerus
a) Medial epicondyle
FCR, PL, FDS, FCU
b) Lateral epicondyle
ECRL, ECRB, ED, EDM, ECU
II. Carpals
a) Pisiform
FCU
III. Metacarpals
a) MC 2
FCR, ECRL
b) MC 3
FCR, ECRB
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
c) MC 5
FCU, ECU
20.3List the muscles which produce:
I. Wrist flexion (palmarflexion)
FCR, FCU, PL, FDS, FDP, FPL
II. Wrist extension (dorsiflexion)
ECRL, ECRB, RCU, ED, EI, EDM, EPL, EPB
III. Wrist abduction (radial deviation)
FCR, ECRL, ECRB, APL, EPL, EPB
IV. Wrist adduction (ulnar deviation)
FCU, ECU
20.4Describe the role of muscles in maintaining dynamic stability of wrist during hand
activities.
I. There is functional interdependence between wrist and hand – whatever
happens at the wrist affects the hand.
For example in the observed position of function:
The wrist is in 30-40° extension and 5° radial deviation.
The metacarpophalangeal joint is in 70° flexion.
The interphalangeal joints are flexed.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
The length tension relationship within the long finger flexors is in part
dependent on the position of the wrist:
Flexor muscles are lengthened passively
No slack in tendon
Contraction of finger flexors translated immediately into movement of
fingers.
In this observed position of function:
The wrist is in a neutral position (slight extension)
The metacarpophalangeal joints are very slightly flexed.
The interphalangeal joints are extended.
The length tension relationship within the long finger flexors is in part
dependent on the position of the wrist:
Flexor muscles slack
Contraction of finger flexors requires slack within the tendon to be taken
up and then pulling on bony attachments.
II. All movements of the hand are accompanied by movements within the wrist
joint complex.
Observation of normal finger/wrist movement:
Active insuffiency occurs when contraction of long finger flexor muscles
results in unwanted flexion of the wrist. A cause of active insufficiency is wrist
instability.
III. Stability of the wrist joint complex is essential for effective hand and finger
function – dynamic stability.
Observation of power grips:
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
The role of the wrist is to provide a stable base to grip and to move through
range to control the tool/object.
Observation of precision grips:
The role of the wrist is to provide a stable base to grip and optimise length-
tension relationship for long finger muscles by placing them in the position of
function.
Aims
At the end of this topic, you should be able to:
a) Identify and describe the attachments and actions of muscles, which move the wrist
joint complex.
b) List the muscles responsible for each movement of the wrist joint complex.
c) State the specified functional roles of muscles associated with the wrist joint complex
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
21. Muscles of the Hand
Objectives
21.1Identify, list the attachments of, and deduce the actions of the intrinsic muscles
of the hand (in table at end of workbook):
I. Muscles of the thenar eminence
a) Flexor pollicis brevis
Identify Attachments Actions
Flexor retinaculum, Flexion of thumb
distal row of carpal (MCP and CMC)
bones, base of Medial rotation of
proximal phalanx of the thumb
thumb
b) Abductor pollicis brevis
Identify Attachments Actions
Flexor retinaculum, Abducts thumb
tubercles of (CMC and MCP)
scaphoid and Flexion of MCP
trapezium, base of Extension of IP
proximal phalanx of
thumb Precision tasks that
require a pincer
grip
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
c) Opponens pollicis
Identify Attachments Actions
Flexor retinaculum, Oppositioon
tubercles of (adduction medial
trapezium, rotation, flexion
anterolateral surface and adduction at
of shaft of CMC)
metacarpal 1
Tip to tip contact
allowing precise
actions
II. Muscles of the hypothenar eminence
a) Flexor digiti minimi
Identify Attachments Actions
Flexor retinaculum, Flexion of MCP of
hook of hamate, little finger
base of proximal
phalanx of digit 5
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
b) Abductor digiti minimi
Identify Attachments Actions
Pisiform, tendon of Flexion of MCP
FCU, dorsal digital Extension of IP
expansion (extensor Abduction of little
aponeurosis) of digit finger
5, base of proximal
phalanx of digit 5 Grasp large objects
with outspread
fingers.
c) Opponens digiti minimi
Identify Attachments Actions
Flexor retinaculum, Opposition of little
hook of hamate, finger by pulling it
medial surface of towards palm and
shaft of metacarpal 5 laterally rotating it
at the CMC joint
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
III. Adductor pollicis
Identify Attachments Actions
Oblique head: bases Adduction of
of metacarpals 2-4, thumb
trapezoid and Later stages of
capitate, base of opposition
proximal phalanx of
thumb. Precision grip of
Transverse head: the hand
shaft of metacarpal 3
base of proximal
phalanx of thumb.
IV. Lumbricals
Identify Attachments Actions
Lateral sides of Flexion of MCP
tendons of FDP, via joint
dorsal digital Extension of IP (PIP
expansion to bases and DIP) joints of
of distal phalanges the corresponding
of digits 2-5 finger
Medial rotation of
index finger
Coordination of
finger movements
involving both
flexion and
extension (e.g.
writing)
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
V. Interossei
a) Dorsal
Identify Attachments Actions
Shafts of Abduct index,
metacarpals 1-5, via middle and ring
dorsal digital fingers
expansions to 1st DAb rotates
proximal phalanges index finger at MCP
of digits 2-4. 1st Dab adducts
thumb
Fexion of MCP and
extension of PIP
and DIP joints
DAb
b) Palmar
Identify Attachments Actions
Shafts of Adduct thumb,
metacarpals 1,2,4 index, ring and
and 5, via dorsal little finger towards
digital expansions to middle finger
proximal phalanges Flexion of thumb
of digits 1, 2, 4 and (MCP)
5. Flexion MCP
Extension IP (PIP
and DIP)
PAd
21.2List the muscles that attach to the:
I. Interosseous membrane of the forearm
Deep Flexors:
a) Flexor digitorum profundus
b) Flexor pollicis longus
Deep extensors:
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
a) Extensor indicis
b) Extensor pollicis longus
c) Extensor pollicis brevis
d) Abductor pollicis longus
II. Metacarpal 1
a) Base of abductor pollicis longus
b) Anterolateral surface of opponens pollicis
c) Shaft of palmar interossei
d) Shaft of dorsal interossei
III. Carpals
a) Proximal row
i. Flexor carpi ulnaris – pisiform
ii. Abductor pollicis brevis – scaphoid tubercle
iii. Abductor digiti minimi – pisiform
b) Distal row
i. Flexor carpi ulnaris – hook of hamate
ii. Flexor pollicis brevis – distal row of carpal bones
iii. Flexor digiti minimi – hook of hamate
iv. Abductor pollicis brevis – tubercle of trapezium
v. Adductor pollicis – trapezoid and capitate
vi. Opponens pollicis – tubercle of trapezium
vii. Opponens digiti minimi – hook of hamate
IV. Phalanges of the fingers
a) Proximal row
i. Abductor digiti minimi – base of digit 5
ii. Flexor digiti minimi – base of digit 5
iii. Palmar interossei – digits 1,2,4 and 5
iv. Dorsal interossei – digits 2-4
b) Middle row
i. Flexor digitorum superficialis
ii. Extensor digitorum
c) Distal row
i. Flexor digitorum profundus
ii. Extensor digitorum
V. Phalanges of the thumb
a) Proximal row
i. Extensor pollicis brevis – base
ii. Abductor pollicis brevis – base
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
iii. Flexor pollicis brevis – base
iv. Adductor pollicis – base
v. Palmar interossei
b) Distal row
i. Extensor pollicis longus – base
ii. Flexor pollicis longus - base
21.3List the muscles which produce:
I. Movement of CM, MCP and IP joints of the thumb:
a) Flexion
Flexor pollicis longus (IP, MCP and CMC)
Flexor pollicis brevis (MCP and CMC)
b) Extension
Extensor pollicis longus (IP, MCP and CMC)
Extensor pollicis brevis (MCP and CMC)
Abductor pollicis longus (CMC)
c) Abduction (CM and MCP)
Abductor pollicis longus (CMC)
Abductor pollicis brevis (MCP and CMC)
d) Adduction (CM and MCP)
Adductor pollicis (CMC)
e) Rotation (CM and MCP)
Opponens pollicis (CMC)
II. Movements of MCP, PIP and DIP joints of index, middle fingers:
a) Flexion
Flexor digitorum superficialis (PIP and MCP)
Flexor digitorum profundus (DIP, PIP and MCP)
Lumbricals (MCP)
Dorsal interossei (MCP)
Palmar interossei (MCP)
b) Extension
Extensor digitorum (DIP, PIP and MCP)
Extensor indicis (DIP, PIP and MCP) – index finger
Lumbricals (DIP and PIP)
Interossei (DIP and PIP)
c) Abduction (MCP)
Dorsal interossei (MCP)
d) Adduction (MCP)
Palmar interossei (MCP)
III. Movements of the MCP, PIP and DIP joints of the little finger:
a) Flexion
Flexor digitorum superficialis (MCP and PIP)
Flexor digitorum profundus (DIP, PIP and MCP)
Flexor digiti minimi (MCP)
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Lumbricals (MCP)
b) Extension
Extensor digitorum (DIP, PIP and MCP)
Extensor digiti minimi (DIP, PIP and MCP)
Lumbricals (DIP and PIP)
c) Abduction (MCP)
Abductor digiti minimi (MCP)
d) Adduction (MCP)
Palmar interossei (MCP)
e) Rotation (MCP)
Opponens digiti minimi (CMC)
IV. Tension in the palmar aponeurosis:
Palmaris Brevis
Palmaris Longus
21.4Identify, describe the location and state the function(s) of the following features
in facilitating, efficient functioning of the hand:
I. Movement of CM, MCP and IP joints of the thumb:
a) Flexor retinaculum
Anterior to carpals where it forms the roof of the carpal tunnel.
Attaches laterally to the scaphoid tubercle and trapezium.
Attaches medially to the pisiform and hook of hamate.
Acts as a strong band for retention of the long flexor tendons (and
prevents ‘bowstringing’) converting the carpal sulcus into a tunnel.
Carpal tunnel involves:
FDS tendon x 4
FDP tendon x4
FPL tendon
FCR tendon
Median nerve
Disease associated with flexor retinaculum: Carpal tunnel syndrome
Inflammation of the synovial sheaths in the carpal tunnel
compresses the median nerve.
b) Extensor retinaculum
A thickening of deep fascia on the back of the forearm and wrist.
Attaches laterally to the distal part of the anterior surface of the
radius.
Attaches medially to the distal end of the ulna, pisiform, triquetral and
ulnar collateral ligament of the wrist.
From medial to lateral, the compartments contain:
ECU
EDM
ED and EI
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
EPL
ECRL and ECRB
APL and EPB
Retains extensor tendons in their position preventing ‘bowstringing’.
c) Intertendinous connections of the extensor tendons
Run horizontally between extensor tendons.
Facilitates extension of all the digits.
Helps explain why none of the fingers can be flexed or extended
individually without movement in the other fingers.
d) Dorsal digital expansion
Also called extensor aponeurosis or extensor hood.
Formed by the tendon of the extensor digitorum, the interossei and
the lumbricals of each finger and acts as a movable hood around the
MCP joint.
The lumbricals and interossei act as ‘wings’ on the extensor digitorum
tendon.
Enables extrinsic extensor tendons to strongly extend the MCP joint.
Can extend IP joints when MCP joints are flexed by finger flexors.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
e) Palmar aponeurosis
Thick, triangular sheath towards the bases of the fingers.
Central part of the fascia is strong and covers the hand.
The medial and lateral parts of the aponeurosis are thin and cover the
muscles of the 1st and 5th digits.
Maintains correct position of tendon by fixing them at certain
positions.
Connected to all flexor tendons allowing communication between
them.
Longitudinal bands and horizontal fibres
Protection of underlying blood vessels and nerves.
Improves grip.
Vertical fibres
Form septa and compartments which facilitate movements
between muscles.
Disease associated with palmar aponeurosis: Dupuytren’s Contracture
Shortening and thickening of palmar aponeurosis that result in
clawing of the fingers.
Ring finger is affected most often, followed by little, middle and
index fingers.
Fingers flex towards palm and become difficult to extend.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
f) Synovial sheaths
Tubular synovial sacs enclosing tendons of FDS and FDP.
Extends proximal to A1 ligaments of the fibrous flexor sheath.
Allows tendons to slide over other structures without friction.
Irritation of synovial membranes.
Increased production of synovial fluid causes stiffness.
Change in quality of synovial fluid less viscous and less nutrients
(affects health of tendons inside.
Thickening of synovial membrane.
Causes of irritation
Trauma, overuse, system condition e.g. Rheumatoid arthritis.
Digits have individual synovial sheaths and do not connect to the
common synovial sheath, with the exception of the little finger.
g) Fibrous flexor sheaths
Fibrous flexor sheath
Annular ligaments A1-A5
A1, A3 and A5 attach to palmar plate.
A2 and A4 attach to bone.
Cruciate ligaments C1-C4
Fibres running obliquely (crossing over).
One fibre attaches to palmar plate
The other attaches to bone.
Loose connective tissue completes the sheath
Palmar ligaments
Fibrocartilage plate – part of joint capsule.
Concave anteriorly – guides the long flexor tendons.
Moves with its distal attachment.
Damaged in hyperextension injuries.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
During flexion, palmar plate moves proximally.
Fibro osseous canal
Involves fibrous flexor sheath, palmar plate and bone.
Prevents bow-stringing (bulging) of flexor tendons.
Occurs when A1 ligament becomes stretched
Flexor tendons are no longer adjacent to the phalanges.
Greater amount of muscle contraction is required to obtain the
same about of finger flexion.
21.5List the muscles which attach to the:
I. Palmar aponeurosis
Palmaris Longus
II. Flexor retinaculum of the wrist
PL, FPB, APB, OP, FDM and ODM.
III. Dorsal digital expansion
EDM, EI, ED, ADM, lumbricals, dorsal interossei and palmar interossei.
Aims
At the end of this topic, you should be able to:
a) Identify and describe the attachments and actions of muscles which move the fingers.
b) Identify and describe the attachments and actions of muscles which move the thumb.
c) Appreciate the structural features of the forearm, wrist joint complex and hand that
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
contribute to efficient functioning of the hand.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
22. Functional Anatomy of the Hand
Objectives
22.1Define the position of function of the hand and list the functional advantages
associated with this position.
Position of function of the hand
Wrist at 30-40˚ in extension and 5˚ in radial deviation.
MCP joints at 70˚ in flexion.
Functional advantages
Length-tension relationship – Optimal movement of the long finger flexors
depend on the position of the wrist joint.
Extended wrist
o Flexor muscles are lengthened.
o Optimal tension because there is not slack in the tendon.
Provides optimal finger movement from contraction of finger flexors.
Neutral wrist
o Flexor muscles tendons have slack.
o Contraction of finger flexor muscles need to first take up slack within the
tendon, and then they can pull on bony attachments.
22.2Explain the recruitment of the extrinsic and intrinsic muscles of the hand in
producing 'normal digital sweep' of the digits.
Digital sweep is the widest arc of movement of the tip of digit through flexion and
extension.
Lumbricals flex MCP joint (intrinsic) FDS flex PIP joint (extrinsic) FDP flex DIP
joint (extrinsic)
The ED performs digital sweep the other way.
22.3Demonstrate and describe the different types of grip and list the musculoskeletal
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
structures necessary to perform these grips effectively:
I. Precision grips
a) Pincer (terminal opposition)
Tips of the pads are used to pick up very fine objects (e.g. a pin).
b) Pad-to-pad (subterminal opposition)
Thumb and index (or other) finger come into contact with each other,
most common precision grip (e.g. holding a pen).
c) Key (subterminolateral opposition)
Pad of thumb presses against the side of the phalanges of a finger, is
less fine but is strong. Can replace the above two grips if distal phalynx
of index finger is lost.
d) Finger adduction
Usually index and middle fingers.
Palmar interossei.
Thumb plays no part, is weak and generally has little precision.
Thumb and radial digits form an O.
Opposition largely dependant on mobility of CMC joint.
II. Power grips
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
a) Palmar
Most powerful.
Whole hand wraps around object, it’s volume determines the strength
of grip which is maximal when the thumb can still touch the index
finger.
Thumb to counterpressure.
b) Hook
Large area of contact
FDS and FDP isometrically contracted
All fingers usually involved
IP extrinsic muscles flexed
MCP intrinsic muscles (lumbricals) flexed
Ulnar fingers flexed more than radial fingers
Is secure but only in one direction eg. Carrying a suitcase
22.4Explain the recruitment of muscles to perform ‘pad to pad opposition’ of the
thumb to the:
I. Index finger
Relative freedom of index finger is important in grasping (longitudinal arch
between thumb and index).
Used in simple lifting task with less manipulation or holding a very small
light object – thumb opposition, index finger flexion.
MCP joint abduction and flexion (FPL, FPB, AbPL, OP).
CMC joint abduction and flexion, axial rotation (AdP, FPL, FPB, AbPL).
II. Little finger
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
This is the only finger with active rotation.
Involves use of hypothenar and thenar muscles to bring these fingers
together – also cupping the palm of the hand.
MCP joint extension (lumbricals, flexor digiti minimi).
IP joint extension (lumbricals).
Opponens Digiti Minimi.
22.5Explain how the muscle recruitment patterns for wrist and hand movements vary
with changing conditions relating to the:
I. Intention of the movement
i.e. moving from:
a) Reach to grasp
e.g. Catching Reach Grasp
Thumb and fingers: Extensors Flexors
Wrist: Neutral Extension
b) Grasp to release
e.g. Throwing Grasp Reach
Thumb and fingers: Flexors Extensors
Wrist: Extension Neutral flexion
II. Velocity of the movement
As speed increases, muscles act eccentrically to stabilise, control and
protect joints.
III. Load of the object being moved
As load increases, more muscles are recruited and act:
Concentrically (shorten) to assist
Eccentrically (lengthen) to stabilise
Isometrically (no change in length) to stabilise
22.6Explain how the position of the wrist (flexion, neutral, extension) affects digital
movements.
During complex hand movements, proximal stabilisation is crucial to maintain task
accuracy distally – shunt muscles.
Co-activation of spurt muscles generally not desirable.
Fatigue in high speed performance can lead to compensatory motor patterns of
muscle recruitment.
E.g. Wrist muscles try to control and move.
E.g. bowing on a string instrument
Playing a finger board of a stringed instrument.
If a tendon is already tight, further contraction becomes more effective (force and
speed).
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Wrist flexion: flexor tendon loose and extensor tendon tight.
Wrist neutral: flexor and extensor tendons not too tight or loose.
Wrist extension: Flexor tendons tight, extensor tendons loose.
Speed of digital movement
Wrist flexion: fastest extension, slowest flexion.
Wrist neutral: middle group of fast and slow.
Wrist extension: Fastest flexion, slowest extension.
22.7Consider specific tasks that demonstrate aspects of hand function listed in 22.5
and 22.6.
Reach to grasp: Grasping – Catching a ball
Grasp to reach: Releasing – Throwing a ball
High speed: In wrist and hand – Bowing on a stringed instrument like the cello.
Dexterity: Fine motor movements – Drawing, buttoning shirts or threading a
needle.
22.8Describe the factors that maintain the normal position and function of the
metacarpophalangeal (MCP) joint of the index finger and the effect of loss of
integrity of one or more of these factors on joint structure and function.
Position and Function of MCP joint maintained by:
Muscles:
FDS, FDP, ED, EI, lumbricals, interossei (palmar and dorsal).
Ligaments:
Palmar ligament, collateral ligament, deep transverse metacarpal ligament.
Other:
Dorsal digital expansion.
Effect of loss of integrity of one or more factors on joint structure and function:
Slight loss of strength with FDS and FDP
Loose range of motion
Stiffness
Loose strength and power
22.9Discuss the relationship between proximal stability and distal mobility as applied
to the hand and wrist joint complex.
Proximal stability at the wrist joint is important for distal mobility at the hand and
fingers.
The origin of intrinsic muscles of the hand require fixation at the wrist by the
muscles of the forearm.
The more stable the proximal end, the more mobility the distal end has.
22.10 Describe the structure and function of the triangular fibrocartilaginous
complex.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Cartilage of TFCC is attaches by ligaments between the ulna styloid process and
medial border of distal radius. It involves the fibrocartilaginous disc (articular disc)
and the ligaments on the ulnar side of the wrist
Its function is to separate the ulna from the radiocarpal joint, stabilises the distal
radioulnar joint and acts as a buttress for supporting proximal carpals.
22.11 Describe the structure and function of the scapholunate ligament.
Intrinsic/interosseous wrist ligament between scaphoid and lunate.
Extrinsic wrist ligaments – connect carpal bones to other bones.
Intrinsic wrist ligament – between carpal bones (more elastic).
The scaphoid rotates the most with wrist flexion, lunate the least.
Its function is to maintain functional stability of the wrist.
22.12 Describe how the structures in objectives 22.10 and 22.11 contribute to carpal
stability.
TFCC: Concave shape stabilises carpal during ulna deviation (adduction).
Scapholunate ligament: Stabilises scaphoid and lunate and allows proximal row of
carpal bones to function as one unit.
Aims
At the end of this topic, you should be able to:
a) Define and describe the position of function of the hand.
b) State the specified functional roles of the muscles of the hand.
c) Explain muscle recruitment patterns during functional activities involving the wrist and
hand.
d) Describe the musculoskeletal requirements for the various types of grip
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
23. Surface Anatomy of the Elbow and Distal Upper Limb
Objectives
23.1Observe and palpate bony features of the elbow, forearm and hand on a living
subject and (if possible) identify on the photographs provided:
I. At the elbow
a) Medial epicondyle of the humerus
Large, easily palpable bump on the medial side of the elbow.
b) Lateral epicondyle of the humerus
Large, easily palpable on the lateral side of the elbow.
c) Olecranon process of the ulna
Large, easily palpable bump on the posterior surface of the elbow
‘funny bone’.
d) Head of the radius
Easiest to palpate with the middle and index fingers when approaching
the distal elbow from the lateral, posterior side.
II. At the wrist
a) Head of the ulna
Easily palpated on the medial, proximal side of the wrist joint.
b) Styloid process of the ulna
Easily palpated on the medial side of the wrist joint between the head
of the ulna and the triquetrals/pisiform bones of the proximal carpal
row.
c) Styloid process of the radius
Easily palpated on the lateral side of the wrist, between the distal end
of the radius and scaphoid bone.
III. In the hand
a) Scaphoid
Between the tendons of extensor pollicis longus and brevis.
b) Tubercle of scaphoid
At the proximal edge of the middle of the thenar eminence on the
distal flexion crease of the wrist.
c) Lunate
Protrudes slightly on the dorsum of the hand during palmarflexion
(wrist flexion).
d) Pisiform
The ‘heel’ of the hand.
e) Capitate - in a fossa just proximal to the base of the third metacarpal
In a fossa just proximal to the base of the third metacarpal.
f) Hook of hamate
Felt indistinctly on the medial edge of the hypothenar eminence.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
g) Joint lines
i. Midcarpal
Easier to palpate on the dorsum of the hand, just distal to
the extensor retinaculum.
ii. 1st carpometacarpal
Easy to palpate on the dorsum of the hand, between
tendons of extensor pollicis brevis and longus at the snuff
box.
iii. Metacarpophalangeal (MCP)
Knuckles of the hand. Very easy to palpate for all 5 joints.
iv. Interphalangeal (IP)
The knuckles of the fingers. Very easy to palpate on all 5
digits.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
23.2List all the structures (ligaments and/or muscles) which attach to the:
I. Distal humerus
a) Medial epicondyle
Muscles Ligaments
Pronator Teres (CFO) Ulnar (medial) Collateral
Flexor Carpi Radialis (CFO)
Flexor Carpi Ulnaris (CFO)
Palmaris Longus (CFO)
Flexor Digitorum Superficialis (CFO)
b) Lateral epicondyle
Muscles Ligaments
Extensor Carpi Radialis Brevis (CEO) Radial (lateral) Collateral
Extensor Carpi Radialis Longus (CEO)
Extensor Carpi Ulnaris (CEO)
Extensor Digitorum (CEO)
Extensor Digiti Minimi (CEO)
Anconeus
Supinator
c) Medial supracondylar ridge
Muscles Ligaments
Pronator Teres (CFO)
d) Lateral supracondylar ridge
Muscles Ligaments
Brachioradialis
Extensor Carpi Radialis Longus
II. Radius
a) Radial tuberosity
Muscles Ligaments
Biceps Brachii
Flexor Pollicus Longus
b) Lateral surface of mid-shaft
Muscles Ligaments
Pronator Teres
Supinator
c) Styloid process
Muscles Ligaments
Brachioradialis Palmar Radiocarpal
Radial Collateral Carpal
III. Ulna
a) Olecranon process
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Muscles Ligaments
Triceps Brachii Ulnar (medial) Collateral
Anconeus
Flexor Carpi Ulnaris
b) Coronoid process
Muscles Ligaments
Brachialis Ulnar (medial) Collateral
Flexor Digitorum Superficialis
Flexor Digitorum Profundus
Flexor Pollicus Longus
c) Ulnar tuberosity
Muscles Ligaments
Brachialis
d) Styloid process
Muscles Ligaments
Palmar Ulnocarpal
23.3Observe and palpate on a living subject, and identify on the photographs
provided, the following muscle bellies and tendons in both contracted (against
resistance) and relaxed states:
I. Muscles of the arm
a) Biceps brachii
i. Muscle belly of long head
ii. Muscle belly of short head
iii. Biceps tendon
iv. Bicipital aponeurosis
4 – long head
5 – short head
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
b) Triceps brachii
i. Muscle belly of long head
ii. Muscle belly of lateral head
iii. Muscle belly of medial head
iv. Triceps tendon
II. Muscles of the forearm
a) Muscle bellies of the flexor compartment (group) of the forearm
b) Tendon of flexor carpi radialis
c) Tendon of palmaris longus (if present)
d) Tendons of flexor digitorum superficialis
e) Tendon of flexor carpi ulnaris
f) Muscle belly of brachioradialis
g) Muscle belly of extensor carpi radialis longus
h) Muscle belly of extensor carpi radialis brevis
i) Muscle bellies of extensor digitorum
j) Tendons of extensor digitorum
k) Muscle belly of extensor carpi ulnaris
l) Tendon of extensor pollicis longus
m) Tendon of extensor pollicis brevis
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
n) Tendon of abductor pollicis longus
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
III. Muscles of the hand
a) Thenar eminence
b) Hypothenar eminence
c) 1st dorsal interosseous
d) Adductor pollicis
Aims
At the end of this topic you should be able to:
a) Relate surface anatomy landmarks to the gross anatomy of the elbow, forearm, wrist
and hand,
b) Observe and/or palpate major bony landmarks and joints of the elbow, wrist and hand.
c) Observe and/or palpate many of the muscles of the arm, forearm and hand
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
24. Adaptation of Tissues
Objectives
24.1Distinguish genetic and environmental factors determining the shape of adult
bones.
Genetics gives the overall gross shape of the bone (e.g. humerus head, neck shaft,
epicondyles, condyles). Activity alters the shape of adult bones – loading. Forces
may be compressive (weight bearing), tensile (muscle pull), or torsional
(fixed/twisting).
24.2Explain the major effects of increased physical activity on:
I. Compact bone
Becomes thicker and denser (e.g. Deltoid tubercle, Radial Tuberosity).
II. Spongy bone
Orientation of Trabeculae changes to resist mechanical forces (doesn’t get
thicker). Most obvious in weight bearing bones.
III. Muscles:
a) Skeletal muscle tissue
Hypertrophy, increase in cross-sectional area of Type 1 (slow) and Type 2
(fast), or transition from type 2 to type 1 (fast slow). Consistent with
increased strength and endurance.
Prolonged lengthening in the immobilised position results in production
of additional sarcomeres in series. This results in an increase in the
overall length of the muscle fibres which allows the muscle to maintain
its length-tension relationship.
b) Associated epimysium and perimysium
Type of connective tissue proper [ground substance, collagen fibres,
fibroblasts].
Increased collagen turnover [combination of synthesis and breakdown],
some degree of net collagen increase [synthesis > breakdown]. Gain in
collagen makes the structure stronger and load resistant.
c) Tendons
Type of connective tissue proper [ground substance, collagen fibres,
fibroblasts].
Same adaptations as epimysium and perimysium.
Increased collagen turnover (synthesis and degradation) - increase in
number of collagen fibrils, increase in collagen fibril density, and net
collagen synthesis.
Net effect decreases stress and make it load resistant – decrease injury.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
IV. Ligaments
Type of connective tissue proper [ground substance, collagen fibres,
fibroblasts].
Same adaptations as epimysium and perimysium.
V. Fascia (e.g. thoracolumbar fascia; iliotibial band)
Type of connective tissue proper [ground substance, collagen fibres,
fibroblasts].
Same adaptations as epimysium and perimysium.
24.3Explain the major effects of decreased physical activity (e.g. bed rest) on the
structures listed in 24.2.
I. Compact bone
Becomes thinner, less dense and more brittle. This makes it weaker and more
vulnerable to fractures/breaks.
II. Spongy bone
Demonstrates less Trabeculae. The bone is weaker and less able to withstand
multi-directional forces.
Can result in osteoporosis where the rate of bone reabsorption by osteoclasts
is greater than bone formation.
III. Muscles:
a) Skeletal muscle tissue
Atrophy (decrease in muscle size), decrease in cross sectional area of
Type 1 (slow) and Type 2 (fast), or transition from Type 1 to Type 2 fibres
(Slow Fast). Disuse atrophy results in loss of strength.
Prolonged shortening may occur which results in loss of sarcomeres,
decreasing the overall length of the muscle fibres. The normal number
and length is fully recovered when immobilisation is terminated.
b) Associated epimysium and perimysium
c) Increased osteoclastic activity at insertion site - increased frequency of
avulsion failure. Increase collagen turnover (synthesis and degradation) -
after 9 weeks no change in overall collagen mass, and after 12 weeks
reduced collagen mass and atrophy. Disorganisation of fibre orientation,
alteration in collagen fibre size, decreased water and GAGs - connective
tissue contractures. Reduced failure load and reduced stiffness.
d) Tendons
Overall there is a decrease in the production of collagen fibres and these
changes appear to be reversible.
IV. Ligaments
Overall there is a decrease in the production of collagen fibres and these
changes appear to be reversible.
V. Fascia (e.g. thoracolumbar fascia; iliotibial band)
Overall there is a decrease in the production of collagen fibres and these
changes appear to be reversible.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
24.4Describe the gross and histological structure of the myotendinous junction and
specific functions they serve.
A myotendinous junction is formed by skeletal muscles where they adhere to
tendons. The connective tissue in muscles is continuous with collagen fibres of a
tendon. Extensive folding of the muscle cell membrane (sarcolemma) –
interdigitation – occurs at the junction, and it is also the site of Golgi tendon organs
(mechanoreceptors). The muscle tendon interface is never flat and therefore the
junction is very strong. It also is the junction of blood supply from the muscle to
the tendon.
Epitenon – sheath of rough connective tissue surrounding entire tendon (attached
to epimysium).
Endotenon – a thin layer of connective tissue that contains lymphatics, blood
vessels and nerves.
24.5Describe the normal blood and nerve supply of the myotendinous junction.
Blood supply
Intrinsic Systems:
Blood Vessels from within muscle or from bone
If tendon is too long the blood won’t got the entire way , therefore long
tendons have an area of hypovascularity (blood supply isn’t consistent).
Used in both short tendons and long tendons.
Extrinsic Systems:
Occur along the course of the tendon
Enters at various stages along the tendon
Only needed in long tendons.
Micro Vascular Networks with Tendon Extensive
Area of hypovascularity is reliant upon diffusion from synovial sheaths.
Nerve supply
Golgi Tendon Organ (inside the tendon) – proprioceptive sensory receptor
organ.
Muscle spindles (stretch/length)
Pain
24.6Describe the results of disruption of the myotendinous junction in terms of
vascular changes, tissue oedema, effect of inflammatory mediators and influx of
inflammatory cells.
Vascular Changes - disrupt blood flow.
Tissue oedema (swelling) – increased.
Effect on inflammatory mediators – released.
Influx of inflammatory cells - more arrive at disrupted site.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
24.7Describe the resolution of disruption to the myotendinous junction in terms of
parameters of healing.
Re-establishing adequate blood supply.
Re-absorption of blood clot and tissue oedema.
Re-establish muscle-tendon connection.
Formation of scar tissue at site of injury (never as strong as original structure).
Repair and reconnect sensory components (Receptors - GTO and Afferent Nerves).
Aims
At the end of this topic you should be able to:
a) Understand the effects of changes in physical activity of the mechanical properties of
common structural tissues.
b) Describe the structure and function of the myotendinous junction.
c) Understand the cell and tissue events associated with disruption and subsequent
healing at this interface.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
25. Nerve Tissue and the Structure of Peripheral Nerves
Objectives
25.1Identify and state the functions of the major structural components of the
central and peripheral nervous systems.
Central Nervous System
CNS is composed of the brain and spinal cord.
The brain is the command centre and the spinal cord is located at the bottom.
Both are very delicate so they need protection (bone).
In the cross section of the Spinal Cord, it has:
I. Grey Matter (looks like a H), for sorting of incoming/outgoing information.
II. Hole in the middle of the grey matter is the central canal which holds the
cerebral spinal fluid.
III. White Matter (white due to the presence of myelin), contains columns:
pathways/tracts which are ascending and descending tracts.
Ascending tracts carry sensory information towards the brain.
Descending tracts carry motor commands to the spinal cord.
Functions CNS:
Integrating, processing and coordinating sensory data and motor commands.
Sensory commands: information about internal/external conditions received
from various receptors throughout the body (afferent pathways).
Motor commands: control or adjust the activities of peripheral organs like the
skeletal muscles (efferent pathways).
Peripheral Nervous System
Consists of all neural tissue outside the CNS.
Functions PNS:
Delivers sensory information to the CNS and carries motor commands to the
peripheral tissues and systems.
Afferent Division: brings sensory information to the CNS (touch, pressure, pain,
temperature, smell and sight).
Efferent Division: carries motor commands from the CNS to muscles, glands
and adipose tissues.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
25.2Describe the basic structure of a neurone (nerve cell):
I. Cell body
The portion of a nerve cell that contains the nucleus - the site of the cell's
metabolic reactions. It processes input from the dendrites and if input is large
enough relays to the axon, where an impulse is initiated.
II. Dendrites
The receptive parts of a neurone such that the direction of information flows
towards the cell body.
III. Axon
A long process which attaches to the cell body and the direction of
information flows from the cell body towards the axon terminal.
25.3Describe the basic structure and functions of sensory neurone and motor
neurone.
Sensory Neurone
The cell body is very close to the vertebral column, thus it is protected by the
vertebrae or skull. Axons are within the CNS and the dendrites acts as a receptor.
The nerve fibre can vary in length (very short – from neck or very long – from leg).
Nerve fibres can also branch.
Motor Neurone
Dendrites and cell body look like a 3D starfish. Dendrites act like a funnel to collect
information. This information travels in the direction from the cells body to the
axon terminal. Nerve fibres can branch.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
25.4Explain the term: ‘nerve fibre’.
A nerve fibre consists of the dendrite of a sensory neurone or an axon of a motor
neurone.
Afferent fibres (sensory information – touch, pressure)
Efferent fibres (motor information – muscles)
Nerve fibres bundle together to form nerves.
25.5Describe the components of a simple reflex (examples: biceps and triceps tendon
reflexes).
Reflex arc begins at a receptor and ends at a peripheral effector (e.g. muscle fibre).
In reflex actions, response is immediate and information doesn’t reach brain but
stops at Spinal Cord. An ‘arc’ is formed, as the brain is cut out of the information
processing.
Information bypasses the brain, travels along a sensory neuron via the dorsal root
and immediately along the motor neuron via the ventral root.
Biceps and Triceps Tendon Reflexes aim to test the integrity of the spinal segments
or any components of the reflex pathway.
25.6Describe the general structure and functions of a synapse and a neuromuscular
junction.
Synapse is a junction that permits a neuron to pass an electrochemical signal to
another cell.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
A neuromuscular junction is found between a motor nerve ending and a muscle
cell. Chemicals are released from the motor nerve ending which will cause the
muscle cells to contract. This is how the nerve controls the activity of muscles.
25.7Describe the location and functions of Schwann cells.
Schwann cells produce a white substance called myelin, which insulates nerve
fibres. As a result we have myelinated nerve fibres (myelination). Myelinated nerve
fibres conduct electrical signals more rapidly than unmyelinated cells.
25.8Describe the structure and general functions of individual peripheral nerve fibres:
myelinated and unmyelinated fibres.
Myelinated Fibres:
Axon of the neuron is covered by a layer of myelin (myelin sheath).
One Schwann cells wraps around one fibre/axon forming multiple layers of
myelin sheath.
Myelin increases the conduction speed of actions potentials (electrical signals)
along the axon.
Commonly present in white matter.
Unmyelinated Fibres:
The axon of the neuron isn’t completely covered by myelin (no myelin sheath).
One Schwann cell wraps around many axons, but doesn’t cover the entire axon
(not enclosed).
Are commonly present in the grey matter of the CNS.
25.9Describe the arrangement of neural and connective tissues within a peripheral
nerve and define the terms endoneurium, perineurium and epineurium.
A nerve is formed by nerve fibres.
Larger nerve fibres tend to be motor, smaller tend to be sensory.
Connective Tissue wraps around axons, fascicles and nerves to protect these
structures and allow anatomical distribution (i.e. orderly distributed)
Endoneurium: Innermost layer of connective tissue that surrounds each nerve
fibre.
Perineurium: Middle layer of connective tissue that surrounds each fascicle.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Epineurium: Outermost layer of connective tissue surrounds the whole nerve.
Contains fat and connects nerve to its surrounding tissue and connects with
dura mater.
25.10 Describe the segmental organisation of the spinal cord and spinal nerves and
the distribution of dorsal and ventral rami and the named nerves.
Sensory fibres go into the spinal cord and motor fibres come out of the spinal cord.
These fibres can bunch together and exit the vertebral column in a small hole.
When these fibres are bundles, they form a mixed spinal nerve. When spinal
nerves form a network it is called a plexus.
Spinal Cord
Roots
o Dorsal (sensory)
o Ventral (motor)
Primary Rami
o Dorsal Ramus – nerves of the back
o Ventral Ramus – nerves of the trunk (thorax and abdomen), nerves of the
limbs (brachial plexus and lumbosacral plexus).
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
25.11 Compare the level of spinal segments to that of the vertebral column. Note
the vertebral level of termination of the adult spinal cord.
Spinal column ends at the vertebral levels of L1/L2. Most of the spinal segments
and their corresponding vertebrae are not at the same level.
Regions of the Spinal Cord:
Cervical: 8
Thoracic: 12
Lumbar: 5
Sacral: 5
Coccygeal: 1
Aims
At the end of this topic, you should be able to identify and/or explain:
a) The major structural components: peripheral and central nervous systems and the main
components of each.
b) The structure of individual peripheral nerve fibres: myelinated and unmyelinated fibres.
c) The structure of peripheral nerves and their supporting connective tissues.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
26. The Brachial Plexus and Nerves of the Shoulder Region
Objectives
26.1Explain the term ‘spinal segment’.
Section of the spinal cord from which a nerve root (ventral rami) is produced.
Spinal segments and their corresponding vertebrae are not at the same
level/alignment [because the vertebral column continues to grow after birth but
the spinal cord doesn’t grow as much].
Consists of:
Vertebra
Spinal nerve
Dorsal root (sensory axons and cell bodies)
Ventral root (motor axons)
Dorsal rami (supplies muscles of the back and overlying skin)
Ventral rami (supplies muscles of the trunk and overlying skin)
26.2Identify and describe the following features of the brachial plexus:
Real Teenagers Drink Cold Beer (Rami, Trunks, Divisions, Cords, Branches).
I. Its formation from ventral rami
These stem from the Spinal cord. The dorsal and ventral root merge to
become the ventral rami. Five ventral rami of the lower four cervical nerves
and the first thoracic nerve give the root values C5, C6, C7, C8 and T1.
These are known as the roots of the plexus.
II. Its trunks
Roots C5 and C6 form the upper trunk. C7 continues as the middle trunk. C8
and T1 form the lower trunk.
III. Its divisions
Each of the three trunks divides into an anterior and posterior division.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
IV. Its cords
The anterior divisions from the upper and middle trunk form the lateral cord.
The posterior divisions from all three trunks form the posterior cord.
The anterior division from the lower trunk form the medial cord.
V. The position of its rami, trunks, divisions and cords in relation to
musculoskeletal structures and skin.
The ventral rami emerge from vertebral column.
The trunks are located between the scalene muscles and the clavicle.
The divisions are located posterior and inferiorly to the clavicle.
The cords are found under the pectoralis minor and the axillary artery.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
26.3Identify the following direct branches of the brachial plexus to the shoulder
region and state their sensory and motor distribution (* indicates found on most
specimens):
I. Dorsal scapular nerve (DSN)
Supplies levator scapulae, rhomboid major and rhomboid minor.
Branches from ventral ramus (C5)
II. Long thoracic nerve (LTN)
Supplies serratus anterior
Branches from ventral ramus (C5, C6 and C7)
III. *Suprascapular nerve (SS)
Supplies supraspinatus and Infraspinatus.
Branches from upper trunk with root value C5 and C6.
Goes through suprascapular notch.
IV. Nerve to subclavius
Supplies subclavius.
Branches from upper trunk with root value C5 and C6.
V. *Upper subscapular nerve (US)
Supplies upper part of subscapularis.
Branches from posterior cord with root value C5 and C6.
VI. *Lower subscapular (LS)
Supplies subscapularis and teres major.
Branches from posterior cord with root value C5 and C6.
VII. *Thoracodorsal (TD)
Supplies latissimus dorsi.
Branches from posterior cord with root value C6, C7 and C8.
VIII. Medial pectoral (MP)
Supplies pectoralis major and minor.
Branches from medial cord with root value C8 and T1.
IX. Lateral pectoral (LP)
Supplies pectoralis major.
Branches from lateral cord with root value C5, C6 and C7.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
26.4Identify and state the area of distribution of the following branches of the
brachial plexus supplying skin of the medial arm and forearm:
I. *Medial cutaneous nerve of arm
Supplies the skin and fascia on the medial side of the proximal half of the
arm.
Branches from medial cord with root value T1.
II. *Medial cutaneous nerve of forearm
Supplies skin over the lower part of biceps brachii, the medial side of the
forearm as far as the wrist and part of the medial side of the of the posterior
surface of the forearm.
Branches from the medial cord with root value C8 and T1.
26.5Identify the terminal branches of the brachial plexus:
My Aunt Raped My Uncle (Musculocutaneous, Axillary, Radial, Median and Ulnar –
lateral to medial).
These five nerves are informally referred to as the ‘W’. They are a starting point to
help identify all nerves in the brachial plexus.
Steps:
Find Coracobrachialis - the nerve entering is the musculocutaneous nerve
(upper limb of the ’W’)
Trace this nerve back to the plexus, pick up the ‘W’.
The middle limb of the “W” is the median nerve and the lower limb is the ulnar
nerve.
The feet of the ‘W’ are the medial and lateral cords.
Hold the musculocutaneous, median and ulnar nerves up from the plexus.
The two large remaining branches are the radial nerve (largest) and the axillary
nerve.
They come from the posterior cord.
For all remaining branches, find the nerve entering each muscle (figure out
what muscles they supply).
I. *Axillary nerve – posterior cord
Supplies deltoids and teres minor.
Branches from posterior cord with root value C5, C6 and C7.
II. *Radial nerve – posterior cord
Branches from posterior cord with root value C5, C6 and C7.
III. *Musculocutaneous nerve – lateral cord
Supplies biceps brachii, Coracobrachialis and brachialis.
Branches from lateral cord with root value C5, C6 and C7.
IV. *Median – lateral and medial cord
Branches from lateral and medial cords with root value C5, C6, C7, C8 and T1.
V. *Ulnar – medial cord
Branches from medial cord with root value C8 and T1.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
26.6Trace the course of the axillary nerve and state its:
Arises from posterior cord.
Runs below the axillary artery in the axillar.
In front of subscapularis.
Passes inferior shoulder joint.
Anterior branch winds around surgical neck of humerus as far as anterior
deltoid.
Posterior branch supplies teres minor and posterior deltoid.
Passes superficially to supply skin over deltoid.
I. Root value
C5 and C6.
II. Sensory distribution
a) To skin (cutaneous)
Skin over the deltoid and lateral triceps.
b) To joint(s) (articular)
Shoulder joint.
III. Motor distribution
Deltoids and teres minor.
IV. Site(s) of greatest vulnerable to injury
Anterior branch around humerus surgical neck.
26.7Trace the course of the suprascapular nerve and identify site(s) on the scapula
where it is most vulnerable to injury.
Arises from the upper trunk.
Passes inferolaterally parallel to trunks.
Goes through the suprascapular notch.
Runs deep to and supplies supraspinatus and infraspinatus.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
I. Root value
C5 and C6.
II. Sensory distribution
None.
III. Motor distribution
Supraspinatus and Infraspinatus.
IV. Site(s) of greatest vulnerable to injury
Suprascapular notch.
26.8List the nerves supplying the following joints of the upper limb:
I. Shoulder
Nerves with root values C5, C6, C7
Suprascapular nerve
Axillary nerve
Subscapular nerve
Lateral Pectoral nerve
Musculocutaneous Nerves
II. Elbow
Nerves with root values C5, C6, C7, C8
Musculocutaneous nerve
Median nerve
Radial nerve
III. Wrist
Nerves with root values C7, C8
Median nerve
Radial nerve
Ulnar nerve
26.9Deduce a general rule for nerve supply to joints (known as Hilton’s Law).
Hilton’s law states that the nerve that innervates joint also innervates the muscles
that move the joint and the skin over these muscles.
26.10 Explain the terms:
I. Root value
The ventral rami that contribute to the nerve.
II. Dermatome(s)
An area of skin supplied by a single nerve root (or spinal nerve).
There is an overlap and variation, so are less clinically reliable than
myotomes.
III. Dermatomal map
A map of dermatomes.
Embryologically-based – more closely related to study from embryological
development.
Clinically-based – more closely related to clinical findings.
IV. Myotome(s)
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
A group of muscles supplied by a single nerve root (or spinal nerve).
Often described in terms of the movements that these muscles bring about.
26.11 List the myotomes responsible for the following upper limb movements:
C5 Hi5.
C6,7,8.
5,6 pick up sticks.
7,8 lay them straight.
Sea-sick soup.
7,8 pronate.
Sea-sick seven.
C7 later m8.
C8, T1.
I. Abduction and lateral (external) rotation of the shoulder
C5.
II. Adduction and medial (internal) rotation of the shoulder
C6, C7 and C8.
III. Flexion of the elbow
C5 and C6.
IV. Extension of the elbow
C7 and C8.
V. Supination of the forearm
C6.
VI. Pronation of the forearm
C7 and C8.
VII. Wrist flexion (palmarflexion)
C6 and C7.
VIII. Wrist extension (dorsiflexion)
C6 and C7.
IX. Finger flexion and extension
C7 and C8.
X. Finger abduction and adduction
C8 and T1.
XI. Thumb movements
C8 and T1.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Aims
At the end of this topic, you should be able to:
a) Appreciate the concept of segmental innervation of the body.
b) List the dermatomes of the upper limb.
c) List the myotomes of the upper limb.
d) Understand the formation of the brachial plexus and identify its component parts.
e) Identify and state the distribution of the direct branches of the brachial plexus
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
27. Peripheral Nerves of the Upper Limb and Nerve Lesions in the Upper Limb
Objectives
27.1Identify and trace the course on the skin of the following nerves in the upper
limb:
I. Radial nerve and its branches:
Between long and medial heads of triceps brachii.
In radial groove on shaft of humerus.
Between brachialis and brachioradialis just above elbow.
Cross anterior aspect of elbow (cubital fossa).
Divides into superficial (radial) and deep (posterior interosseous)
branches.
a) Superficial radial nerve
Closest to skin.
b) Posterior interosseous nerve (PIN)
Deep branch winds around neck of radius to posterior forearm, then
passes between two heads of supinator.
Runs on posterior surface of interosseous membrane.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
II. Musculocutaneous nerve
Arises from lateral cord of the brachial plexus.
Initially it lies lateral to the axillary artery and then descends between the
artery and coracobrachialis which it supplies and pierces before running
distally between biceps and brachialis to reach the lateral side of the arm.
At the elbow, this nerve pierces the deep fascia between biceps and
brachioradialis as the lateral cutaneous nerve of the forearm.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
III. Median and its branches:
a) Anterior interosseous nerve (AIN)
Medial to brachial artery in lower half of arm.
Behind bicipital aponeurosis in front of brachialis.
Crosses anterior aspect of elbow (cubital fossa), then passes between
two heads of pronator teres, then deep to FDP.
At wrist, it is between FDS and FCR.
Passes deep to flexor retinaculum to enter the hand.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
IV. Ulnar
Medial to brachial artery in arm (more medial than the median nerve).
Passes through the medial head of triceps brachii to lie between the
medial epicondyle and olecranon (funny bone).
Descends on medial forearm on FDP.
Enters hand passing anterior to flexor retinaculum and runs around
medial side of hook of hamate.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
27.2For each of the nerves listed in objective 27.1, state (if applicable):
Radial Nerve
I. Its root value
C5, C6, C7, C8 and T1.
II. Its sensory distribution
a) To skin (cutaneous)
Skin of posterior arm, forearm and hand.
b) To joint(s) (articular)
Elbow and wrist joints.
III. Its motor distribution
Before dividing (posterior arm) – triceps brachii, anconeus, brachioradialis,
ECRL and ½ brachialis.
(Posterior forearm) – supinator, extensors of the wrist (5 muscles – ECRB, ED,
EDM, ECU, EI), extensors of the thumb (EPL and EPB) and APL.
Located posterior entire length of arm
IV. Site(s) of greatest vulnerability to injury
In the spiral (radial) groove of the humerus.
Musculocutaneous Nerve
I. Its root value
C5, C6 and C7.
II. Its sensory distribution
c) To skin (cutaneous)
Lateral ½ of forearm as far as the ball of the thumb.
Variable area over extensor muscles of forearm, wrist and occasionally
metacarpal I.
d) To joint(s) (articular)
Shoulder joint.
III. Its motor distribution
Biceps brachii, brachialis (2/3) and Coracobrachialis.
Located anterior upper arm
IV. Site(s) of greatest vulnerability to injury
Where it enters the Coracobrachialis or the anterolateral forearm near the
elbow.
Median Nerve
I. Its root value
C5, C6, C7, C8 and T1.
II. Its sensory distribution
e) To skin (cutaneous)
Anterior surface of lateral 3 ½ digits, extending posteriorly to the distal
interphalangeal joint line and corresponding anterior palm.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
f) To joint(s) (articular)
Elbow and wrist joints.
III. Its motor distribution
All flexors of the wrist, fingers and thumb including PT (i.e. anterior
compartment of the forearm except 1 ½ muscles – FCU and ½ FDP), thenar
eminence (except AP) and lateral two lumbricals.
Located middle, thumb-side of anterior forearm – BUSIEST IN ARM
IV. Site(s) of greatest vulnerability to injury
Near cubital fossa as it passes through pronator teres. Proximal to flexor
retinaculum by laceration. Deep to flexor retinaculum in the carpal tunnel by
compression.
Ulnar Nerve
I. Its root value
C8 and T1.
II. Its sensory distribution
g) To skin (cutaneous)
Palmar and dorsal skin of the medial 1 1/2 digits and corresponding palm.
h) To joint(s) (articular)
Wrist joints.
III. Its motor distribution
Opposite of Median nerve
All intrinsic muscles of the hand (except for the lateral 2 lumbricals and
thenar eminence[not AP]) - hypothenar muscles, medial 2 lumbricals, AP and
all interossei, FCU and medial half of FDP.
Located pinky-side anterior forearm, BUSIEST IN HAND
IV. Site(s) of greatest vulnerability to injury
As it passes behind the groove of the medial epicondyle and at the wrist.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
27.3Describe the functional loss and deformity resulting from a complete lesion to
the following nerves:
I. Radial nerve
a) In the axilla
Forearm supination (turning keys), wrist extension (picking up cup), and
finger extension (picking up and releasing objects).
Deformity – wrist drop (loss of wrist extensors).
b) At the level of the spiral groove
As above.
II. Ulnar nerve
a) At the elbow
Loss of precision grip, reduced power in power grips, and all grips are
affected due to inability to feel objects on the medial side of the palmar
hand surface.
Deformity – claw hand (loss of intrinsics placing MCP in good position for
digital sweep – MCP extension, long flexors continue to pull fingers into
flexion).
b) Near pisiform
As above.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
III. Median nerve in the carpal tunnel
Loss of precision grips and power is severely affected.
Deformity – ape hand (loss of thenar muscles if lesion is in carpal tunnel).
27.4Appreciate the clinical significance of the segmental innervation pattern of the
upper limb.
In a nerve lesion, loss is seen distal to the lesion.
Segmental innervation is the distribution of nerves in a given region (dermatomes
and myotomes).
Clinically used to determine the spinal segments affected - to identify the site of
the lesion.
The differences in nerve supply can help distinguish between spinal nerve lesions
and peripheral nerve lesions.
27.5Distinguish between peripheral and spinal nerve lesions of the upper limb using
the following examples:
Peripheral Nerves Spinal Nerves
Motor List muscles supplied by the nerve List myotomes of the nerve
Sensory List areas of skin and joints List dermatomes of the nerve
supplied by nerve
Blue indicates actions produced by the peripheral nerve only.
Red indicates actions produced by the spinal nerve only.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
I. C5 vs. musculocutaneous nerve
Musculocutaneous nerve C5
Motor Coracobrachialis: Abduction of shoulder.
Flexion of shoulder, and abduction Lateral rotation of
of shoulder. shoulder.
Biceps brachii: Flexion of elbow.
Flexion of shoulder, flexion of
elbow and supination of forearm.
Brachialis (medial 2/3):
Flexion of elbow
Sensory Skin of lateral forearm Dermatome map
II. C6 vs. radial nerve
Radial nerve C6
Motor Abductor pollicus longus: Adduction and medial
Abducts the thumb. (internal) rotation of
Anconeus: shoulder joint.
Flexion of elbow joint
Elbow Extension.
Supination of radioulnar
Brachioradialis: joints.
Elbow flexion, supination of Flexion of wrist joints.
pronated forearm to neutral Extension of wrist joints.
position, pronation of supinated
forearm to neutral position.
Brachialis (lateral 1/3):
Flexion of elbow
Extensors of the fingers and wrist:
ECRL, ECRB, ED, EDM, ECU, EI.
Extensors of the thumb:
EPL, EPB
Supinator
Triceps brachii:
Extension of elbow joint
Long head extends shoulder joint.
Sensory Skin of posterior arm, forearm and Dermatome map
hand.
Elbow and wrist joints
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
III. C7 vs. median nerve
Median nerve C7
Motor Forearm FCR, FDS, lateral ½ FDP Wrist and finger flexion.
and FPL. Pronation.
PT and PQ Shoulder adduction and
medial rotation.
(does not include FCU and medial ½
Elbow extension.
FDP) Wrist and finger
Thenar eminence (FPB, OP, AbPB) extension.
Thumb flexion, thumb opposition
and thumb abduction
Lateral 2 lumbricals
Sensory Anterior surface of lateral 3 ½ Sensation in
digits. anterior/posterior
Posterior surface above lateral 3 ½ forearm, wrist and digit III
DIP joints
IV. C8 vs. ulna nerve
Ulna nerve C8
Motor All intrinsic muscles of the hand Adduction and medial
(except for lateral 2 lumbricals and (internal) rotation of
thenar eminence) - shoulder joint.
Hypothenar muscles (flexor digiti Extension of elbow joint.
minimi brevis, abductor digiti Pronation of radioulnar
minimi and opponens digiti minimi) joint.
Medial 2 lumbricals Flexion and extension of
Adductor pollicis digits.
All interossei Abduction, adduction and
opposition of digits.
Flexor carpi ulnaris:
Flexion and adduction of wrist joint
Medial ½ of flexor digitorum
profundus:
Flexes digits, and aids flexion of
wrist joint.
Sensory Palmar and dorsal skin of medial 1 Dermatome map
½ digits and corresponding palm,
and the wrist joint
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Aims
At the end of this topic, you should be able to:
a) Identify and state the sensory (cutaneous, articular) and motor distribution of the major
peripheral nerves of the upper limb.
b) Distinguish between the effects of peripheral and segmental nerve lesions on upper
limb function.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
28. Blood Vessels of the Upper Limb
Objectives
28.1Identify:
I. Ascending aorta
First artery taking blood out of the heart.
II. Aortic arch and its three major branches:
a) Brachiocephalic trunk
Supplies the upper limb via the right subclavian artery.
Supplies the right side of the head and neck via the right common carotid
artery.
b) Left common carotid artery
Supplies the left side of the head and neck.
c) Left subclavian artery
Supplies the left upper limb.
III. Right common carotid artery
Supplies the right side of the head and neck.
IV. Right subclavian artery
Supplies the right upper limb.
28.2Identify and describe the general areas of supply of the arteries of the upper
limb:
I. Axillary brachial
Continuation of the subclavian artery.
Supplies the shoulder and pectoral regions and lateral chest wall.
II. Profunda brachii
Supplies structures of the anterior arm (runs with the median nerve).
Ends in the cubital fossa opposite the neck of the radius.
Vulnerable at the supracondylar ridge.
III. Radial
Supplies structures of the lateral forearm. Starts in cubital fossa from the
brachial artery and ends by completing the deep palmar arch in the hand.
Radial pulse felt just distal to the tendon of FCR.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
IV. Ulnar
Supplies structures on the medial forearm.
Runs with the ulnar nerve, on top of FDP and under FCU.
Starts in the cubital fossa from the brachial artery and ends at the pisiform
where it divides into deep and superficial palmar arteries.
V. Superficial palmar arch
Major contribution – ulnar artery, small contribution – radial artery.
Supplies structures of the fingers.
VI. Deep palmar arch
Major contribution – radial artery, small contribution – ulnar artery.
Supplies structures of the palm.
2cm distal to crease on wrist.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
28.3State the functional significance of two venous systems (deep and superficial) for
draining blood from the upper limb.
Deep venous system
Runs with and takes the names of surrounding arteries. They have same pattern as
arteries, up to the brachial vein. It has vena commitantes – 2 veins per artery, on
either side of the artery. They also contain valves.
Superficial vein system
Located in skin, therefore are no seen on specimens. They have valves, but not as
many as deep veins. These veins anastomose (communicate) freely with deep
veins and are best identified in surface anatomy catalogues.
Functional Significance
Two ways to return blood to the heart, some in-built redundancy (i.e. if one
pathway is bleeding or has a blockage, the heart can still receive deoxygenated
blood from the other pathway).
Plays a role in temperature control. If the body is hot, blood goes through
superficial veins (cools body). If body is cold, blood goes through deep veins
(retains heat).
28.4Identify the deep veins of the upper limb:
I. Radial
Has vena commitantes with radial artery.
II. Ulnar
Has vena commitantes with the ulnar artery.
III. Brachial
Has vena commitantes with the brachial artery.
IV. Axillary
Continuation of the basilica vein at the lower border of teres minor. Lies
lateral to the axillary artery.
28.5Identify the superficial veins of the upper limb:
I. Dorsal venous arch
Network of veins on the dorsal (back) surface of the hand when you ‘pump’
the arm to expose the veins.
II. Cephalic
Runs laterally up the forearm until it joins the axillary vein. Most lateral vein.
Connected to the basilic vein by the median cubital vein near the cubital
fossa.
III. Basilic
Runs medially up the forearm. Most medial vein. Connected to the cephalic
vein by the median cubital vein near the cubital fossa.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
IV. Median cubital
Short, wide vein. Usually runs upwards and medially across the bicipital
aponeurosis. Communicates with the cephalic and basilic veins. Site where
blood is drawn commonly.
28.6Identify the veins returning blood from the upper limb to the heart:
I. Subclavian
Proximal continuation of the axillary vein.
Downloaded by Abery Au (auabery@yahoo.com.hk)
lOMoARcPSD|1668352
II. Brachiocephalic
Further continuation of subclavian vein once it penetrates the chest wall and
enters the thoracic cavity.
III. Superior vena cava
Major vein that directly enters the heart superiorly to drain blood into it.
Aims
At the end of this topic you should:
a) Understand the route by which oxygenated blood is distributed by the heart to the
upper limb.
b) Understand the routes by which deoxygenated blood is returned from the upper limb to
the heart.
Downloaded by Abery Au (auabery@yahoo.com.hk)
You might also like
- Human Body StructureDocument72 pagesHuman Body Structuredeepak dwivedi94% (16)
- Lecture Notes - BIOS1170B (Body Systems - (Structure and Function) ) (Sydney)Document86 pagesLecture Notes - BIOS1170B (Body Systems - (Structure and Function) ) (Sydney)SK AuNo ratings yet
- Anatomy Mnemonics 2Document50 pagesAnatomy Mnemonics 2Nourhan JamalNo ratings yet
- Wellness Massage PTDocument8 pagesWellness Massage PTJosephine Simpao100% (1)
- Veterinary Anatomy Lab MaterialDocument34 pagesVeterinary Anatomy Lab MaterialFira'ol BogalaNo ratings yet
- MBBS - Batch 29 - Group 1 (Introduction To Anatomy)Document14 pagesMBBS - Batch 29 - Group 1 (Introduction To Anatomy)thrrishaNo ratings yet
- 1st-Introduction To Anatomy1Document30 pages1st-Introduction To Anatomy1prasun_vNo ratings yet
- Lecture 1Document35 pagesLecture 1Mian Mudassar AkramNo ratings yet
- Tissue 2Document34 pagesTissue 2nneduchiemerieNo ratings yet
- General AnatomyDocument17 pagesGeneral AnatomyAbubakar Umar GaladanchiNo ratings yet
- Introduction To Veterinary AnatomyDocument118 pagesIntroduction To Veterinary AnatomyKhrys Hardy100% (1)
- Anatomy and Physiology Notes-3_074008Document77 pagesAnatomy and Physiology Notes-3_074008hossanathomas22No ratings yet
- Introduction To Veterinary AnatomyDocument22 pagesIntroduction To Veterinary AnatomyAbdulla Hil KafiNo ratings yet
- Chapter III SkeletalDocument26 pagesChapter III SkeletalTitoMacoyTVNo ratings yet
- Module 2 AnaphysioDocument32 pagesModule 2 AnaphysioJomarie RamirezNo ratings yet
- Unit 4 Introduction To Bones and The SkullDocument22 pagesUnit 4 Introduction To Bones and The SkullrynNo ratings yet
- Human Anatomy Physiology Chapter 4 Osseous System NotesDocument17 pagesHuman Anatomy Physiology Chapter 4 Osseous System Notesmanku9163No ratings yet
- Introduction To The Anatomy,: Sagittal PlaneDocument10 pagesIntroduction To The Anatomy,: Sagittal PlanemagholNo ratings yet
- Anatomy - Physiology of Animals - Skeletal System.Document3 pagesAnatomy - Physiology of Animals - Skeletal System.Erica MaeNo ratings yet
- Anatomy Learning Assessment 3Document13 pagesAnatomy Learning Assessment 3Jay Lure Gomez BaguioNo ratings yet
- 689general and Systems 2023 اسنان عامDocument36 pages689general and Systems 2023 اسنان عامking111newNo ratings yet
- 4th Report SkeletonDocument14 pages4th Report SkeletonAndi NurhidayahNo ratings yet
- Anatomy and Physiology Lecture Assignment (Skeletal System)Document4 pagesAnatomy and Physiology Lecture Assignment (Skeletal System)Destined UbaldoNo ratings yet
- Group2 - BSHM 1 BDocument43 pagesGroup2 - BSHM 1 BSAPILAN DENMARNo ratings yet
- Movement and Growth: Csec BiologyDocument25 pagesMovement and Growth: Csec BiologyYanique JonesNo ratings yet
- Anatomy 2019 1Document6 pagesAnatomy 2019 1YMORNo ratings yet
- Tissue and Supporting SystemDocument15 pagesTissue and Supporting SystemjolaolumolusinNo ratings yet
- Anatomy and Physiology of Farm AnimalsDocument157 pagesAnatomy and Physiology of Farm AnimalsOliver Talip100% (1)
- Grade 11 Biology Week 2 Lesson 1Document6 pagesGrade 11 Biology Week 2 Lesson 1NesiaNo ratings yet
- Musculoskeletal Anatomy and Physiology 4Document67 pagesMusculoskeletal Anatomy and Physiology 4Dennis Nabor Muñoz, RN,RM100% (1)
- Biology Review FebDocument16 pagesBiology Review FebSarahNo ratings yet
- Midterm Assignment 1Document5 pagesMidterm Assignment 1R Jay LagdaminNo ratings yet
- Bio Summary 1-10Document113 pagesBio Summary 1-10ShwwwwNo ratings yet
- Anatomy (Bones)Document48 pagesAnatomy (Bones)Jumrah KhumairahNo ratings yet
- Locomotion Handout 2023Document7 pagesLocomotion Handout 2023rheanna0076No ratings yet
- Anatomy and PhysiologyDocument65 pagesAnatomy and PhysiologyJosef BaroniNo ratings yet
- Body MovementsDocument54 pagesBody MovementsTapas BanerjeeNo ratings yet
- AnaPhy Module 2 - Copy - HIGHLIGHTEDDocument93 pagesAnaPhy Module 2 - Copy - HIGHLIGHTEDKristine Joy NolloraNo ratings yet
- Anatomical IntroductionDocument17 pagesAnatomical Introductionllazoozllbraa 7372No ratings yet
- 2.0 Tissues and Supporting SystemDocument39 pages2.0 Tissues and Supporting Systemwalterkalu385No ratings yet
- Life Sciences Grade 10 Term 2 Week 6 - 2020Document10 pagesLife Sciences Grade 10 Term 2 Week 6 - 2020fmsr7wmtd5No ratings yet
- Antome Bones (BONES)Document7 pagesAntome Bones (BONES)Sadon B AsyNo ratings yet
- P - 7 Science Lesson NotesDocument104 pagesP - 7 Science Lesson Notesmichaelopi63No ratings yet
- Anatomy and Physiology of Farm AnimalsDocument157 pagesAnatomy and Physiology of Farm AnimalsOliver TalipNo ratings yet
- P.7 Best Science Notes Term One - Teacher - AcDocument105 pagesP.7 Best Science Notes Term One - Teacher - AcMonydit SantinoNo ratings yet
- $R4UVS5TDocument32 pages$R4UVS5Tnechtech6No ratings yet
- Skripta Za Usmeni Iz EngleskogDocument15 pagesSkripta Za Usmeni Iz EngleskogElizabetaNo ratings yet
- Introduction To Human OsteologyDocument131 pagesIntroduction To Human OsteologyMiguel Angel Soto Gutierrez100% (1)
- 11LS The Skeleton NOTESDocument28 pages11LS The Skeleton NOTESAdhi PandayNo ratings yet
- Elzatona Anatomy 2023Document9 pagesElzatona Anatomy 2023mahmoud ezzeldeenNo ratings yet
- Skeletal System (2) - 2Document71 pagesSkeletal System (2) - 2alazarademe797No ratings yet
- 02 SkeletalsystemDocument18 pages02 SkeletalsystemhorozukaNo ratings yet
- Bones PDFDocument227 pagesBones PDFAtthapu ThirupathaiahNo ratings yet
- Orca Share Media1629098154770 6832932906945476564Document8 pagesOrca Share Media1629098154770 6832932906945476564Scar ShadowNo ratings yet
- Act08 The Skeletal System DiscussionDocument8 pagesAct08 The Skeletal System DiscussionSofia A.No ratings yet
- Skeletal System Lesson PlanDocument10 pagesSkeletal System Lesson PlanNicketa AndersonNo ratings yet
- ALVEOLAR BoneDocument72 pagesALVEOLAR BoneArchana50% (2)
- Anatomy ExamDocument9 pagesAnatomy ExamFoo FuuNo ratings yet
- 2 SkeletelDocument53 pages2 Skeletelsamuel mergaNo ratings yet
- داتا زتونة مديول الجينيرال أناتوميDocument69 pagesداتا زتونة مديول الجينيرال أناتوميAhmed MohamedNo ratings yet
- Advanced farriery knowledge: A study guide and AWCF theory course companionFrom EverandAdvanced farriery knowledge: A study guide and AWCF theory course companionNo ratings yet
- The Practical Guide to Drawing Anatomy: [Artist's Workbook]From EverandThe Practical Guide to Drawing Anatomy: [Artist's Workbook]Rating: 3.5 out of 5 stars3.5/5 (3)
- Welcome To: Oracle Spatial Workshop For ManagementDocument19 pagesWelcome To: Oracle Spatial Workshop For ManagementSK AuNo ratings yet
- Les03 - Spatial TunningDocument26 pagesLes03 - Spatial TunningSK AuNo ratings yet
- Sustainability 12 02443 v2Document15 pagesSustainability 12 02443 v2SK AuNo ratings yet
- Spatial Queries: Oracle Corporation, 2002. All Rights ReservedDocument47 pagesSpatial Queries: Oracle Corporation, 2002. All Rights ReservedSK AuNo ratings yet
- Les06 - ComparsionDocument7 pagesLes06 - ComparsionSK AuNo ratings yet
- Vdocument - in - Making A Decision Between Liferay and DrupalDocument36 pagesVdocument - in - Making A Decision Between Liferay and DrupalSK AuNo ratings yet
- Effect of Milk Production On Reproductive Performance in Dairy HerdsDocument10 pagesEffect of Milk Production On Reproductive Performance in Dairy HerdsSK AuNo ratings yet
- Make The Move From Ibm Lotus Notes and Optimize Your Business AppsDocument8 pagesMake The Move From Ibm Lotus Notes and Optimize Your Business AppsSK AuNo ratings yet
- Business Benefits of Transitioning From Lotus Notes To SharePointDocument7 pagesBusiness Benefits of Transitioning From Lotus Notes To SharePointSK AuNo ratings yet
- Oracle Spatial With Gis Application Training: Thinkspace IncDocument16 pagesOracle Spatial With Gis Application Training: Thinkspace IncSK AuNo ratings yet
- Exercise On GeoMedia Professional and Oracle SpatialDocument12 pagesExercise On GeoMedia Professional and Oracle SpatialSK AuNo ratings yet
- Compare Oracle Spatial Data Storage and Manipulation With Conventional GISDocument7 pagesCompare Oracle Spatial Data Storage and Manipulation With Conventional GISSK AuNo ratings yet
- Lecture Notes - Homeostasis-L1-4Document28 pagesLecture Notes - Homeostasis-L1-4SK AuNo ratings yet
- BIOL2024-Practical Notes (2018)Document31 pagesBIOL2024-Practical Notes (2018)SK AuNo ratings yet
- PWR 1.0Document25 pagesPWR 1.0Elizabeth SmithNo ratings yet
- Aiims Anatomy NotesDocument46 pagesAiims Anatomy Notesshalialoo22No ratings yet
- Medigrip Sizing ChartDocument1 pageMedigrip Sizing ChartKelly HuntNo ratings yet
- Free Preview An Athletes Guide To Chronic Knee PainDocument25 pagesFree Preview An Athletes Guide To Chronic Knee PaintylerdurdenmademeNo ratings yet
- Life 12 00188Document17 pagesLife 12 00188Ligia BoazuNo ratings yet
- The Complete Running and Marathon BookDocument194 pagesThe Complete Running and Marathon Bookozal udaya100% (4)
- Or A Piri Yakul 2018Document10 pagesOr A Piri Yakul 2018Luigi Paolo Zapata DelgadoNo ratings yet
- Ankle and Foot Complex 1aDocument19 pagesAnkle and Foot Complex 1afoziiiii100% (3)
- Both Bone # of ForearmDocument40 pagesBoth Bone # of ForearmSashmi Sareen ManandharNo ratings yet
- Peter Bellezza DPM, MS Midori Higashi DPM Jeffrey Christensen, DPM, FACFASDocument1 pagePeter Bellezza DPM, MS Midori Higashi DPM Jeffrey Christensen, DPM, FACFASbaoNo ratings yet
- DISTINGUISHING BETWEEN NORMAL AND ABNORMAL FETAL BONES AND EXTERMITIES - ISUOG LECTURE CUSP 2018.pdf MAINDocument29 pagesDISTINGUISHING BETWEEN NORMAL AND ABNORMAL FETAL BONES AND EXTERMITIES - ISUOG LECTURE CUSP 2018.pdf MAINBharti Pant GahtoriNo ratings yet
- Implants in OrthopaedicsDocument20 pagesImplants in OrthopaedicsDr. F. Abdul KhaderNo ratings yet
- Zogadi Cnebebi Zeda Kiduris SesaxebDocument8 pagesZogadi Cnebebi Zeda Kiduris Sesaxebsasa sasadzeNo ratings yet
- WRMS Amira Extra Credit Skeletal SystemDocument1 pageWRMS Amira Extra Credit Skeletal SystemWendy PinedaNo ratings yet
- Intro 70Document75 pagesIntro 70bockoneNo ratings yet
- The Scapulohumeral RhythmDocument3 pagesThe Scapulohumeral RhythmArun RamananNo ratings yet
- Nevralgia Cervico-BrahealaDocument17 pagesNevralgia Cervico-BrahealaAlex RăşcanuNo ratings yet
- Giannini SERIDocument9 pagesGiannini SERISeagate PramonoNo ratings yet
- Physiotherapy Neurological Assessment Form: Glasgow Coma Scale: /15Document6 pagesPhysiotherapy Neurological Assessment Form: Glasgow Coma Scale: /15PC LaptopNo ratings yet
- Soft Tissue Disorders and Fibromyalgia: Jaya Ravindran Consultant RheumatologistDocument54 pagesSoft Tissue Disorders and Fibromyalgia: Jaya Ravindran Consultant RheumatologistarunupadhayaNo ratings yet
- HEP2GO Carpal Tunnel Program PDFDocument2 pagesHEP2GO Carpal Tunnel Program PDFBetty OberackerNo ratings yet
- Shoulder DisocationDocument16 pagesShoulder DisocationLakshmanan PrakashNo ratings yet
- Peripheral NerveDocument6 pagesPeripheral NerveNur Atiqah ZainalNo ratings yet
- Large Resistance Bands - Ebook UK PDFDocument16 pagesLarge Resistance Bands - Ebook UK PDFSimão Pedro MartinsNo ratings yet
- Femoral Triangle - Borders, Contents and Mnemonics - KenhubDocument7 pagesFemoral Triangle - Borders, Contents and Mnemonics - Kenhubو عجلت اليك ربي لترضيNo ratings yet
- 3 RomDocument58 pages3 Romphysical therapy channel ptNo ratings yet
- 32 Standardized Simplified Sword FormDocument27 pages32 Standardized Simplified Sword FormCarvalhoNo ratings yet
- Bankart LesionDocument3 pagesBankart LesionFrnz RiveraNo ratings yet



















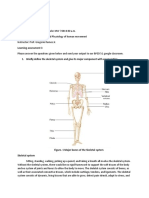









































![The Practical Guide to Drawing Anatomy: [Artist's Workbook]](https://imgv2-2-f.scribdassets.com/img/word_document/238627287/149x198/b1987107b7/1617237212?v=1)