Professional Documents
Culture Documents
0 ratings0% found this document useful (0 votes)
33 viewsPathology of Spine Shoulder and Elbow
Pathology of Spine Shoulder and Elbow
Uploaded by
Mei BejeranoThis document summarizes several common disorders of the spine and shoulder. For the spine, it describes the pathophysiology, manifestations, and management of cervical spondylosis, spondylolisthesis, ankylosing spondylitis, slipped discs, Pott's disease, and scoliosis. For the shoulder, it outlines the mechanism, manifestations, and treatment approaches for rotator cuff tears, supraspinatus tendinitis, subacromial bursitis, shoulder dislocations, and adhesive capsulitis.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You might also like
- Revalida Compi Velez PDFDocument248 pagesRevalida Compi Velez PDFKenneth Irving MocenoNo ratings yet
- Spine PDFDocument7 pagesSpine PDFDRAHMEDFAHMYORTHOCLINIC100% (1)
- Ch4 en Cover 2017Document23 pagesCh4 en Cover 2017Ramakant Singh100% (1)
- Cast and TractionsDocument3 pagesCast and TractionsMacaRonie PepeRownie del RioNo ratings yet
- Flex UK - July 2018Document132 pagesFlex UK - July 2018安建平 澳门南湖区100% (3)
- Lower Back Pain DDDocument9 pagesLower Back Pain DDjermaineNo ratings yet
- Aging Spine: A Degenerative Cascade: TH STDocument4 pagesAging Spine: A Degenerative Cascade: TH STChristi EspinosaNo ratings yet
- Bms2 k8 Kuliah Nyeri Punggung 2022Document54 pagesBms2 k8 Kuliah Nyeri Punggung 2022103Juffry PrayogaNo ratings yet
- "Hip Dislocation": Short CaseDocument38 pages"Hip Dislocation": Short CaseGusty BahyNo ratings yet
- Common Conditions of The Lumbar SpineDocument4 pagesCommon Conditions of The Lumbar SpineJames KNo ratings yet
- Low Back Pain Numbness: Strain SciaticaDocument5 pagesLow Back Pain Numbness: Strain SciaticaCarol KayasNo ratings yet
- Nyeri Punggung Bawah (Low Back Pain) : DefinisiDocument10 pagesNyeri Punggung Bawah (Low Back Pain) : DefinisiheruNo ratings yet
- Prolapsed Intervertebral Disc: By: Diksha Solanki Bot 4 YearDocument37 pagesProlapsed Intervertebral Disc: By: Diksha Solanki Bot 4 YearISIC IRS100% (1)
- Disc HerniationDocument32 pagesDisc HerniationMadalina DragoiNo ratings yet
- Posterior, Lateral, and Anterior Hip Pain Due To Musculoskeletal OriginDocument4 pagesPosterior, Lateral, and Anterior Hip Pain Due To Musculoskeletal Origin楊畯凱No ratings yet
- The Spine SummaryDocument6 pagesThe Spine SummaryAnnelieNo ratings yet
- Refrat Remato LBPDocument33 pagesRefrat Remato LBPwulanNo ratings yet
- Sacroiliac Joint Dysfunction and Piriformis Syndrome PDFDocument37 pagesSacroiliac Joint Dysfunction and Piriformis Syndrome PDFDevi SiswaniNo ratings yet
- AnatomyDocument6 pagesAnatomyVarsha Mol MohananNo ratings yet
- Duttons Libro 2Document1 pageDuttons Libro 2GUSTAVO ANDRÉS RIVERA-DAVIDNo ratings yet
- Problem of SpineDocument99 pagesProblem of SpineSashwini Dhevi100% (1)
- Varieties of Spondylolisthesis: (A) Normal, (B) Congenital, (C) Isthmic, (D) Traumatic, (E) Degenerative, and (F) PathologicalDocument5 pagesVarieties of Spondylolisthesis: (A) Normal, (B) Congenital, (C) Isthmic, (D) Traumatic, (E) Degenerative, and (F) PathologicalYashaswi ANo ratings yet
- Spodylolysthes IsDocument70 pagesSpodylolysthes IsshravaniNo ratings yet
- Low Back PainDocument100 pagesLow Back Painchandrusai100% (1)
- Back PainDocument18 pagesBack PainCabdiladif Ahmed McrfNo ratings yet
- Dylan Sciara Catergory 1Document4 pagesDylan Sciara Catergory 1api-508474347No ratings yet
- Dysfunction of The Sacroiliac Joint and Its Treatment : Richard L. Dontigny, BS, PTTDocument13 pagesDysfunction of The Sacroiliac Joint and Its Treatment : Richard L. Dontigny, BS, PTTferryNo ratings yet
- Mus Culo SkeletalDocument7 pagesMus Culo SkeletalJessica Abella SohNo ratings yet
- DegenerativeDiskDisease (HNP) IDocument2 pagesDegenerativeDiskDisease (HNP) Iapi-3822433No ratings yet
- Lee Zu Ying Problem of The Spine 541-16-17Document25 pagesLee Zu Ying Problem of The Spine 541-16-17Star CruiseNo ratings yet
- Frozen ShoulderDocument18 pagesFrozen Shoulderhemnath rajendranNo ratings yet
- Herniated Nucleus PulposusDocument4 pagesHerniated Nucleus Pulposuszeverino castilloNo ratings yet
- Peripheral Nerve ExaminationDocument30 pagesPeripheral Nerve ExaminationMalvinder Singh DhillonNo ratings yet
- Neurodynamics-Foster 08Document30 pagesNeurodynamics-Foster 08Tahira RajputNo ratings yet
- Bms2-k6 Kuliah Back Pain 08 03 17 FK UsuDocument50 pagesBms2-k6 Kuliah Back Pain 08 03 17 FK UsuFred RickNo ratings yet
- LaminectomyDocument16 pagesLaminectomyNicole John C. BolanteNo ratings yet
- Week 8 Category 2Document4 pagesWeek 8 Category 2api-468093714No ratings yet
- Neuro DynamicsDocument30 pagesNeuro DynamicsAnnisa Rahma SariNo ratings yet
- Lumbar Disc HerniationDocument4 pagesLumbar Disc HerniationChester NicoleNo ratings yet
- 7.PT Management of LBADocument11 pages7.PT Management of LBASapna ChaudharyNo ratings yet
- Lower Back PainDocument9 pagesLower Back PainKrishelle Kate PannigNo ratings yet
- Conservative Management of Selected Shoulder ProblemsDocument8 pagesConservative Management of Selected Shoulder ProblemsDr Franklin Shoenholtz100% (3)
- Herniated Nucleus PulposusDocument21 pagesHerniated Nucleus PulposusKianah ReyesNo ratings yet
- Sport Injuries: ShoulderDocument67 pagesSport Injuries: ShoulderNabiha AjmalNo ratings yet
- Swimmer's ShoulderDocument85 pagesSwimmer's ShoulderAbdallah Samir Mostafa٢٠١٩٠٢١٥٩No ratings yet
- HNP - OutputDocument3 pagesHNP - OutputStephany ZamorasNo ratings yet
- Degenerative DiseasesDocument8 pagesDegenerative Diseasesadrian kristopher dela cruz100% (1)
- Nursing Care: Fracture Jay VillasotoDocument11 pagesNursing Care: Fracture Jay VillasotoJay VillasotoNo ratings yet
- Exercise 1 Differential Chart: Ddx-Hip Region of Pain Risk Factors Aggravating/Relieving Treatment OsteoarthritisDocument2 pagesExercise 1 Differential Chart: Ddx-Hip Region of Pain Risk Factors Aggravating/Relieving Treatment Osteoarthritisapi-479720222No ratings yet
- Pemeriksaan Fisik Tulang BelakangDocument35 pagesPemeriksaan Fisik Tulang BelakangLeaf CloverNo ratings yet
- Exercise 1 Differential Chart: CHIR12007 Clinical Assessment and Diagnosis Portfolio Exercises Week 9 & 10Document12 pagesExercise 1 Differential Chart: CHIR12007 Clinical Assessment and Diagnosis Portfolio Exercises Week 9 & 10api-455408952No ratings yet
- Unstable Cervical InjuriesDocument15 pagesUnstable Cervical Injuriesanggi dwi puteraNo ratings yet
- Prolapse of Lumbar Intervertebral Disc: Li JieruoDocument36 pagesProlapse of Lumbar Intervertebral Disc: Li JieruoWai Kwong ChiuNo ratings yet
- Physical Rehabilitation 2.2 Rehabilitation of Lower Limb Musculoskeletal DisordersDocument6 pagesPhysical Rehabilitation 2.2 Rehabilitation of Lower Limb Musculoskeletal DisordersJAIRISH YZABELLE SALVADORNo ratings yet
- Cyriax ConceptDocument30 pagesCyriax ConceptSarah Khawar ButtNo ratings yet
- Intervertebral Disc ProlapseDocument46 pagesIntervertebral Disc Prolapsehellosir8273No ratings yet
- CH 41 LBP - Braddom's Physical Medicine & RehabilitationDocument46 pagesCH 41 LBP - Braddom's Physical Medicine & RehabilitationPyrectic WilliamsNo ratings yet
- Case 4-ObturatorDocument7 pagesCase 4-Obturatoranr.encarnacionNo ratings yet
- Cad wk9-10 QsDocument10 pagesCad wk9-10 Qsapi-468597987No ratings yet
- Abnormal ToneDocument14 pagesAbnormal Toneapi-442568656No ratings yet
- Musculoskeletal Disorders (For Students)Document5 pagesMusculoskeletal Disorders (For Students)Chaina MacaspacNo ratings yet
- Spinal Stenosis And Pinched Nerve A Simple Guide to These conditionsFrom EverandSpinal Stenosis And Pinched Nerve A Simple Guide to These conditionsRating: 5 out of 5 stars5/5 (1)
- Muscle Stretching in Manual TherapyDocument3 pagesMuscle Stretching in Manual TherapyEmad Eldin Mohamed AbdelatiefNo ratings yet
- Metacarpal Fractures1Document23 pagesMetacarpal Fractures1H100% (2)
- Flexoplastia Con Dorsal Ancho 3Document11 pagesFlexoplastia Con Dorsal Ancho 3Jagu ShopNo ratings yet
- Low Back Pain: General InfoDocument4 pagesLow Back Pain: General InfoErlinda RamosNo ratings yet
- NUR11O1 Integrated Human Anatomy and Physiology Department of Biology Institute of Arts and Sciences Far Eastern UniversityDocument6 pagesNUR11O1 Integrated Human Anatomy and Physiology Department of Biology Institute of Arts and Sciences Far Eastern UniversityPrancheska Abigayle Peneyra SantiagoNo ratings yet
- Avascular Necrosis of The FootDocument30 pagesAvascular Necrosis of The FootFlorinSabouNo ratings yet
- Dry Needling (Workshop Fisiofit 2016)Document119 pagesDry Needling (Workshop Fisiofit 2016)Laode Iski IsmailNo ratings yet
- Physiological Principles of SotaiDocument13 pagesPhysiological Principles of SotaiBuyu IkkanNo ratings yet
- Journal Of: The Plantar Calcaneal Spur: A Review of Anatomy, Histology, Etiology and Key AssociationsDocument9 pagesJournal Of: The Plantar Calcaneal Spur: A Review of Anatomy, Histology, Etiology and Key AssociationsRizka DamayantiNo ratings yet
- MICB4454 Metacarpal Fracture PDFDocument2 pagesMICB4454 Metacarpal Fracture PDFZakiyuddin FathoniNo ratings yet
- Muscles of The Pelvic Floor - Anatomy and Function - KenhubDocument9 pagesMuscles of The Pelvic Floor - Anatomy and Function - KenhubDhikaNo ratings yet
- Self Massage Therapy - Ebook PDFDocument26 pagesSelf Massage Therapy - Ebook PDFMatthewNo ratings yet
- Meridians and Acupuncture Points: A. Lung Meridian of Hand Taiyin (Document169 pagesMeridians and Acupuncture Points: A. Lung Meridian of Hand Taiyin (Siti PatimahNo ratings yet
- Ch05a EHAP-LectDocument25 pagesCh05a EHAP-LectBea RossetteNo ratings yet
- Ultrasonografia em EquinosDocument8 pagesUltrasonografia em EquinosIngrid MachadoNo ratings yet
- Examination of ElbowDocument18 pagesExamination of Elbowharmohit singhNo ratings yet
- Abu Hureyra Abu HureyraDocument4 pagesAbu Hureyra Abu Hureyrabozana0405100% (1)
- Chapter 2 f5Document103 pagesChapter 2 f5Jo YeeNo ratings yet
- Tendon Injuries of Hand: DR Saumya AgarwalDocument101 pagesTendon Injuries of Hand: DR Saumya AgarwaltesfahuntekletilahunNo ratings yet
- Maisonneuve Fracture - Case PresentationDocument4 pagesMaisonneuve Fracture - Case Presentationtwinke1012No ratings yet
- Osho Savrseni PutDocument201 pagesOsho Savrseni PutStefan Putnik100% (1)
- Levy CV Feb 2011Document5 pagesLevy CV Feb 2011jonathan_levy9254No ratings yet
- Entrapment of The Posterior Interosseous Nerve - Ax ArticleDocument9 pagesEntrapment of The Posterior Interosseous Nerve - Ax ArticleNaz HossNo ratings yet
- HEP2GO Carpal Tunnel Program PDFDocument2 pagesHEP2GO Carpal Tunnel Program PDFBetty OberackerNo ratings yet
- altMeasuresMUST PDFDocument1 pagealtMeasuresMUST PDFmahunNo ratings yet
- Bromothymol Blue - C27H28Br2O5S - PubChemDocument15 pagesBromothymol Blue - C27H28Br2O5S - PubChemDeangelis DamasNo ratings yet
- Biofeedback Stabilizer Manual PDFDocument188 pagesBiofeedback Stabilizer Manual PDFEugenio López Recio100% (1)
- Ischiorectal Fossa Anatomy and It's Suppuration: DR - Niveditha S Dr.S.Chandak DR - Melissa P Dr.C.MahkalkarDocument18 pagesIschiorectal Fossa Anatomy and It's Suppuration: DR - Niveditha S Dr.S.Chandak DR - Melissa P Dr.C.MahkalkarSagarRathodNo ratings yet
Pathology of Spine Shoulder and Elbow
Pathology of Spine Shoulder and Elbow
Uploaded by
Mei Bejerano0 ratings0% found this document useful (0 votes)
33 views5 pagesThis document summarizes several common disorders of the spine and shoulder. For the spine, it describes the pathophysiology, manifestations, and management of cervical spondylosis, spondylolisthesis, ankylosing spondylitis, slipped discs, Pott's disease, and scoliosis. For the shoulder, it outlines the mechanism, manifestations, and treatment approaches for rotator cuff tears, supraspinatus tendinitis, subacromial bursitis, shoulder dislocations, and adhesive capsulitis.
Original Description:
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document summarizes several common disorders of the spine and shoulder. For the spine, it describes the pathophysiology, manifestations, and management of cervical spondylosis, spondylolisthesis, ankylosing spondylitis, slipped discs, Pott's disease, and scoliosis. For the shoulder, it outlines the mechanism, manifestations, and treatment approaches for rotator cuff tears, supraspinatus tendinitis, subacromial bursitis, shoulder dislocations, and adhesive capsulitis.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
0 ratings0% found this document useful (0 votes)
33 views5 pagesPathology of Spine Shoulder and Elbow
Pathology of Spine Shoulder and Elbow
Uploaded by
Mei BejeranoThis document summarizes several common disorders of the spine and shoulder. For the spine, it describes the pathophysiology, manifestations, and management of cervical spondylosis, spondylolisthesis, ankylosing spondylitis, slipped discs, Pott's disease, and scoliosis. For the shoulder, it outlines the mechanism, manifestations, and treatment approaches for rotator cuff tears, supraspinatus tendinitis, subacromial bursitis, shoulder dislocations, and adhesive capsulitis.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
You are on page 1of 5
ABDUKADIL, AMIRA M.
L.I.: AFFECTATION PER REGION
DISORDERS OF THE SPINE
DISORDER PATHOPHYSIOLOGY MANIFESTATIONS MANAGEMENT
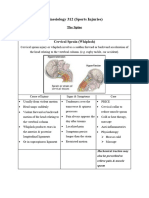
Cervical Multifactorial degenerative - Back pain that increases -Immobilization of cervical
Spondylosis changes in the intervertebral with movement spine
disks and facet joints of the -Stiffness -Mechanical traction
cervical spine cause narrowing -Better when inactive -Isometric exercises
of spinal canal and neural -Sensory dysfunction, if -Surgery, if with intractable
foramina. This causes with cervical pain and progressive
subsequent collapse as a result radiculopathy neurologic deficit
of biomechanical incompetence,
causing the annulus to bulge
outward. As the disk space
narrows, the annulus bulges, and
the facets override.
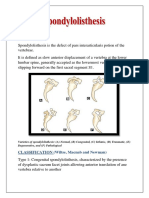
Spondylolisthesis Multifactorial events -May be asymptomatic -Rest
(degeneration, trauma) causes -Low back pain -Physical Therapy
anterior slippage of the vertebral -Hamstring tightness -Surgery, if not responding
body, pedicles, and superior -Tenderness (most often to conservative therapy or in
articular facets, leaving the L4 or L5) cases with progressive
posterior elements behind, neurologic deficit and
causing nerve root injury postural deformity
Ankylosing Inflammation, cartilage erosion, -Insidius onset of low -Exercise therapy to
Spondylitis and an additional process, which back pain which is maintain range of motion
is subsequent ossification of chronic -NSAIDs
sacroiliac joint and axial -Morning stiffness -Anti-TNF alpha drugs
skeleton. Inflammation is -Limited spinal mobility
initially dominated by -Improvement with
mononuclear cell infiltrates and exercise
by increased number of
osteoclast
Slipped Repetitive use of spine due to -Back pain aggravated by -Bed rest
(Herniated) Disc frequent heavy lifting causes motion or bending -Avoidance of strenuous
injury to intervertebral discs -Abnormal posture labor
(L4-L5 or L5-S1). With tear of -Limitation of spine -Strengthening and
ligament and posterior capsule motion stretching exercises
of disc, nucleus pulposus will -Focal neurologic deficit -Acetaminophen or NSAIDs
extrude with compression of -Weakness, atrophy, for pain
nerve root. fasciculations
Pott’s Disease Secondary infection from an -Back pain -Long-term
extraspinal source via -Stiffness antimycobacterial drugs
hematogenous spread. -Immobility -Patients with spinal
Progressive bone destruction -Mild fever instability or neural
leads to vertebral collapse and -Leukocytosis compression from
kyphosis. The spinal canal can epidural inflammatory
be narrowed by abscesses, tissue should undergo
granulation tissue, or direct debridement and fusion as
dural invasion, leading to spinal needed
cord compression and
neurologic deficits.
Scoliosis Idiopathic: unknown etiology -High shoulder, prominent - Curves between
but may involve collagen hip, or projecting 30 and 40 degrees: Braces,
abnormalities, abnormal growth, Scapula -Curves greater than 40 to
or genetic bases with incomplete -Idiopathic scoliosis is 45 degrees: Surgery
penetrance usually painless - Combined anterior
Neuromuscular: not well and posterior surgery (for
understood but may be a result more severe curvatures)
of muscle weakness
DISORDERS OF THE SHOULDER
DISORDER MECHANISM MANIFESTATIONS MANAGEMENT
Rotator Cuff Forceful or repeated overhead or -Pain -Rest
Tears pulling movements produce -Tenderness - Pain management with
significant stress on the -Muscle atrophy NSAIDs
glenohumeral complex of the -Difficulty abducting or -Immediate surgery for
rotator cuff, causing it to tear. rotating the arm extensive acute traumatic
This will eventually lead to tears
instability of the shoulder joint. -Rehabilitation
a. Immobilization: using a
sling, 4-6 weeks after
surgery
b. Passive Exercise:
moving the arm n
different positions to
improve range of
motions, 4-6 weeks after
surgery
c. Active Exercise: more
than 4-6 weeks
d. Surgery: for acute
traumatic tears
Supraspinatus Trauma or repetitive stress on the -Pain -Range of motion exercises
Tendinitis shoulder allowing inflammatory -Tenderness -Strengthening exercises
fluid to accumulate causing -Muscle atrophy -Avoidance of overhead
swelling of the tendon and activities
thickening of its closing sheath. - Pain management with
NSAIDs
Subacromial Repetitive overhead activities or -Pain -Ice and rest
Bursitis causing inflammation of the -Tenderness -Immobilization with a sling
bursa. This causes synovial cells -Muscle atrophy - Pain management with
to multiply and thereby increases -Impaired arm abduction NSAIDs
collagen formation and fluid -Strengthening and range of
production motion exercises
Shoulder Physical trauma to the shoulder -Pain -Closed Reduction
Dislocation can cause the humeral head to be -Swelling -Immobilization with a sling
separated from the glenoid -Limited range of motion -Passive ROM exercises
cavity. Anterior dislocation (most -Joint deformity after initial period of
common) is due sudden violence -Minimal ability to immobilization
applied to the humerus with the elevate the arm
joint fully abducted, tilting the
humeral head downward onto the
inferior weak part of the capsule,
causing it to tear. The humeral
head comes to lie inferior to the
glenoid fossa.
Adhesive Inflammation in the joint -Insidious onset of pain -Usually self-limiting
Capsulitis capsule followed by development -Gradual decrease in -Physiotherapy
of adhesions and fibrosis of the active and passive range -Home exercise
synovial lining. Thickening and of motion - Pain management with
contraction of the glenohumeral NSAIDs
joint capsule and formation of
collagenous tissue surrounding
the joint reduces joint volume.
Following the synovial
inflammatory process, there is
contracture of the capsule of the
glenohumeral joint, which causes
pain and stiffness.
Impingement Chronic repetitive mechanical -Gradual increase in -Initial therapy will include
Syndrome process in which the conjoint shoulder pain with rest, NSAIDs, and physical
tendon of the rotator cuff overhead activities therapy
undergoes repetitive compression - Patients tend to -Injection of a local
and micro trauma as it passes externally rotate the arm anesthetic and a cortisone
under the coraco-acromial arch in order to allow the cuff preparation
to occupy the widest part -Bursectomy and
of the subacromial space subacromial decompression
thereby relieving the via acromioplasty (if
symptoms conservative treatment if
unsuccessful)
DISORDERS OF THE ELBOW
DISORDER PATHOPHYSIOLOGY MANIFESTATIONS MANAGEMENT
Tennis Elbow Overexertion of the extensor -Pain on the lateral aspect - Rest, ice, compression,
muscle while performing a of the elbow and elevation
backhand stroke in a game of -Local tenderness over the -Avoidance of painful
tennis or other activity causing lateral epicondyle activities
repetitive forearm muscle -Decreased movement on - Pain management with
contractions. passive elbow extension, NSAIDs
wrist flexion and ulnar -Elbow counterforce brace
deviation and pronation
Golfer’s Elbow Repeated wrist flexion or -Pain over the medial -Rest, ice, compression, and
forearm pronation and high- elbow elevation
energy valgus forces created by - Local tenderness over -Physical therapy to
the overhead throw seen in the medial epicondyle maintain range of motion
sports. -Weakness of hand and -Pain management with
wrist NSAIDs
-Elbow braces
Nursemaid Elbow Low-energy trauma occurring -A child will tend to hold -Immobilization
from brisk axial traction of the the elbow in slight flexion -Closed reduction
forearm, often by an adult who and the forearm pronated
holds the child’s hand as the -Pain and tenderness
child pulls away. May also be localized to the lateral
due to falls, wrestling, and abuse aspect of the elbow
You might also like
- Revalida Compi Velez PDFDocument248 pagesRevalida Compi Velez PDFKenneth Irving MocenoNo ratings yet
- Spine PDFDocument7 pagesSpine PDFDRAHMEDFAHMYORTHOCLINIC100% (1)
- Ch4 en Cover 2017Document23 pagesCh4 en Cover 2017Ramakant Singh100% (1)
- Cast and TractionsDocument3 pagesCast and TractionsMacaRonie PepeRownie del RioNo ratings yet
- Flex UK - July 2018Document132 pagesFlex UK - July 2018安建平 澳门南湖区100% (3)
- Lower Back Pain DDDocument9 pagesLower Back Pain DDjermaineNo ratings yet
- Aging Spine: A Degenerative Cascade: TH STDocument4 pagesAging Spine: A Degenerative Cascade: TH STChristi EspinosaNo ratings yet
- Bms2 k8 Kuliah Nyeri Punggung 2022Document54 pagesBms2 k8 Kuliah Nyeri Punggung 2022103Juffry PrayogaNo ratings yet
- "Hip Dislocation": Short CaseDocument38 pages"Hip Dislocation": Short CaseGusty BahyNo ratings yet
- Common Conditions of The Lumbar SpineDocument4 pagesCommon Conditions of The Lumbar SpineJames KNo ratings yet
- Low Back Pain Numbness: Strain SciaticaDocument5 pagesLow Back Pain Numbness: Strain SciaticaCarol KayasNo ratings yet
- Nyeri Punggung Bawah (Low Back Pain) : DefinisiDocument10 pagesNyeri Punggung Bawah (Low Back Pain) : DefinisiheruNo ratings yet
- Prolapsed Intervertebral Disc: By: Diksha Solanki Bot 4 YearDocument37 pagesProlapsed Intervertebral Disc: By: Diksha Solanki Bot 4 YearISIC IRS100% (1)
- Disc HerniationDocument32 pagesDisc HerniationMadalina DragoiNo ratings yet
- Posterior, Lateral, and Anterior Hip Pain Due To Musculoskeletal OriginDocument4 pagesPosterior, Lateral, and Anterior Hip Pain Due To Musculoskeletal Origin楊畯凱No ratings yet
- The Spine SummaryDocument6 pagesThe Spine SummaryAnnelieNo ratings yet
- Refrat Remato LBPDocument33 pagesRefrat Remato LBPwulanNo ratings yet
- Sacroiliac Joint Dysfunction and Piriformis Syndrome PDFDocument37 pagesSacroiliac Joint Dysfunction and Piriformis Syndrome PDFDevi SiswaniNo ratings yet
- AnatomyDocument6 pagesAnatomyVarsha Mol MohananNo ratings yet
- Duttons Libro 2Document1 pageDuttons Libro 2GUSTAVO ANDRÉS RIVERA-DAVIDNo ratings yet
- Problem of SpineDocument99 pagesProblem of SpineSashwini Dhevi100% (1)
- Varieties of Spondylolisthesis: (A) Normal, (B) Congenital, (C) Isthmic, (D) Traumatic, (E) Degenerative, and (F) PathologicalDocument5 pagesVarieties of Spondylolisthesis: (A) Normal, (B) Congenital, (C) Isthmic, (D) Traumatic, (E) Degenerative, and (F) PathologicalYashaswi ANo ratings yet
- Spodylolysthes IsDocument70 pagesSpodylolysthes IsshravaniNo ratings yet
- Low Back PainDocument100 pagesLow Back Painchandrusai100% (1)
- Back PainDocument18 pagesBack PainCabdiladif Ahmed McrfNo ratings yet
- Dylan Sciara Catergory 1Document4 pagesDylan Sciara Catergory 1api-508474347No ratings yet
- Dysfunction of The Sacroiliac Joint and Its Treatment : Richard L. Dontigny, BS, PTTDocument13 pagesDysfunction of The Sacroiliac Joint and Its Treatment : Richard L. Dontigny, BS, PTTferryNo ratings yet
- Mus Culo SkeletalDocument7 pagesMus Culo SkeletalJessica Abella SohNo ratings yet
- DegenerativeDiskDisease (HNP) IDocument2 pagesDegenerativeDiskDisease (HNP) Iapi-3822433No ratings yet
- Lee Zu Ying Problem of The Spine 541-16-17Document25 pagesLee Zu Ying Problem of The Spine 541-16-17Star CruiseNo ratings yet
- Frozen ShoulderDocument18 pagesFrozen Shoulderhemnath rajendranNo ratings yet
- Herniated Nucleus PulposusDocument4 pagesHerniated Nucleus Pulposuszeverino castilloNo ratings yet
- Peripheral Nerve ExaminationDocument30 pagesPeripheral Nerve ExaminationMalvinder Singh DhillonNo ratings yet
- Neurodynamics-Foster 08Document30 pagesNeurodynamics-Foster 08Tahira RajputNo ratings yet
- Bms2-k6 Kuliah Back Pain 08 03 17 FK UsuDocument50 pagesBms2-k6 Kuliah Back Pain 08 03 17 FK UsuFred RickNo ratings yet
- LaminectomyDocument16 pagesLaminectomyNicole John C. BolanteNo ratings yet
- Week 8 Category 2Document4 pagesWeek 8 Category 2api-468093714No ratings yet
- Neuro DynamicsDocument30 pagesNeuro DynamicsAnnisa Rahma SariNo ratings yet
- Lumbar Disc HerniationDocument4 pagesLumbar Disc HerniationChester NicoleNo ratings yet
- 7.PT Management of LBADocument11 pages7.PT Management of LBASapna ChaudharyNo ratings yet
- Lower Back PainDocument9 pagesLower Back PainKrishelle Kate PannigNo ratings yet
- Conservative Management of Selected Shoulder ProblemsDocument8 pagesConservative Management of Selected Shoulder ProblemsDr Franklin Shoenholtz100% (3)
- Herniated Nucleus PulposusDocument21 pagesHerniated Nucleus PulposusKianah ReyesNo ratings yet
- Sport Injuries: ShoulderDocument67 pagesSport Injuries: ShoulderNabiha AjmalNo ratings yet
- Swimmer's ShoulderDocument85 pagesSwimmer's ShoulderAbdallah Samir Mostafa٢٠١٩٠٢١٥٩No ratings yet
- HNP - OutputDocument3 pagesHNP - OutputStephany ZamorasNo ratings yet
- Degenerative DiseasesDocument8 pagesDegenerative Diseasesadrian kristopher dela cruz100% (1)
- Nursing Care: Fracture Jay VillasotoDocument11 pagesNursing Care: Fracture Jay VillasotoJay VillasotoNo ratings yet
- Exercise 1 Differential Chart: Ddx-Hip Region of Pain Risk Factors Aggravating/Relieving Treatment OsteoarthritisDocument2 pagesExercise 1 Differential Chart: Ddx-Hip Region of Pain Risk Factors Aggravating/Relieving Treatment Osteoarthritisapi-479720222No ratings yet
- Pemeriksaan Fisik Tulang BelakangDocument35 pagesPemeriksaan Fisik Tulang BelakangLeaf CloverNo ratings yet
- Exercise 1 Differential Chart: CHIR12007 Clinical Assessment and Diagnosis Portfolio Exercises Week 9 & 10Document12 pagesExercise 1 Differential Chart: CHIR12007 Clinical Assessment and Diagnosis Portfolio Exercises Week 9 & 10api-455408952No ratings yet
- Unstable Cervical InjuriesDocument15 pagesUnstable Cervical Injuriesanggi dwi puteraNo ratings yet
- Prolapse of Lumbar Intervertebral Disc: Li JieruoDocument36 pagesProlapse of Lumbar Intervertebral Disc: Li JieruoWai Kwong ChiuNo ratings yet
- Physical Rehabilitation 2.2 Rehabilitation of Lower Limb Musculoskeletal DisordersDocument6 pagesPhysical Rehabilitation 2.2 Rehabilitation of Lower Limb Musculoskeletal DisordersJAIRISH YZABELLE SALVADORNo ratings yet
- Cyriax ConceptDocument30 pagesCyriax ConceptSarah Khawar ButtNo ratings yet
- Intervertebral Disc ProlapseDocument46 pagesIntervertebral Disc Prolapsehellosir8273No ratings yet
- CH 41 LBP - Braddom's Physical Medicine & RehabilitationDocument46 pagesCH 41 LBP - Braddom's Physical Medicine & RehabilitationPyrectic WilliamsNo ratings yet
- Case 4-ObturatorDocument7 pagesCase 4-Obturatoranr.encarnacionNo ratings yet
- Cad wk9-10 QsDocument10 pagesCad wk9-10 Qsapi-468597987No ratings yet
- Abnormal ToneDocument14 pagesAbnormal Toneapi-442568656No ratings yet
- Musculoskeletal Disorders (For Students)Document5 pagesMusculoskeletal Disorders (For Students)Chaina MacaspacNo ratings yet
- Spinal Stenosis And Pinched Nerve A Simple Guide to These conditionsFrom EverandSpinal Stenosis And Pinched Nerve A Simple Guide to These conditionsRating: 5 out of 5 stars5/5 (1)
- Muscle Stretching in Manual TherapyDocument3 pagesMuscle Stretching in Manual TherapyEmad Eldin Mohamed AbdelatiefNo ratings yet
- Metacarpal Fractures1Document23 pagesMetacarpal Fractures1H100% (2)
- Flexoplastia Con Dorsal Ancho 3Document11 pagesFlexoplastia Con Dorsal Ancho 3Jagu ShopNo ratings yet
- Low Back Pain: General InfoDocument4 pagesLow Back Pain: General InfoErlinda RamosNo ratings yet
- NUR11O1 Integrated Human Anatomy and Physiology Department of Biology Institute of Arts and Sciences Far Eastern UniversityDocument6 pagesNUR11O1 Integrated Human Anatomy and Physiology Department of Biology Institute of Arts and Sciences Far Eastern UniversityPrancheska Abigayle Peneyra SantiagoNo ratings yet
- Avascular Necrosis of The FootDocument30 pagesAvascular Necrosis of The FootFlorinSabouNo ratings yet
- Dry Needling (Workshop Fisiofit 2016)Document119 pagesDry Needling (Workshop Fisiofit 2016)Laode Iski IsmailNo ratings yet
- Physiological Principles of SotaiDocument13 pagesPhysiological Principles of SotaiBuyu IkkanNo ratings yet
- Journal Of: The Plantar Calcaneal Spur: A Review of Anatomy, Histology, Etiology and Key AssociationsDocument9 pagesJournal Of: The Plantar Calcaneal Spur: A Review of Anatomy, Histology, Etiology and Key AssociationsRizka DamayantiNo ratings yet
- MICB4454 Metacarpal Fracture PDFDocument2 pagesMICB4454 Metacarpal Fracture PDFZakiyuddin FathoniNo ratings yet
- Muscles of The Pelvic Floor - Anatomy and Function - KenhubDocument9 pagesMuscles of The Pelvic Floor - Anatomy and Function - KenhubDhikaNo ratings yet
- Self Massage Therapy - Ebook PDFDocument26 pagesSelf Massage Therapy - Ebook PDFMatthewNo ratings yet
- Meridians and Acupuncture Points: A. Lung Meridian of Hand Taiyin (Document169 pagesMeridians and Acupuncture Points: A. Lung Meridian of Hand Taiyin (Siti PatimahNo ratings yet
- Ch05a EHAP-LectDocument25 pagesCh05a EHAP-LectBea RossetteNo ratings yet
- Ultrasonografia em EquinosDocument8 pagesUltrasonografia em EquinosIngrid MachadoNo ratings yet
- Examination of ElbowDocument18 pagesExamination of Elbowharmohit singhNo ratings yet
- Abu Hureyra Abu HureyraDocument4 pagesAbu Hureyra Abu Hureyrabozana0405100% (1)
- Chapter 2 f5Document103 pagesChapter 2 f5Jo YeeNo ratings yet
- Tendon Injuries of Hand: DR Saumya AgarwalDocument101 pagesTendon Injuries of Hand: DR Saumya AgarwaltesfahuntekletilahunNo ratings yet
- Maisonneuve Fracture - Case PresentationDocument4 pagesMaisonneuve Fracture - Case Presentationtwinke1012No ratings yet
- Osho Savrseni PutDocument201 pagesOsho Savrseni PutStefan Putnik100% (1)
- Levy CV Feb 2011Document5 pagesLevy CV Feb 2011jonathan_levy9254No ratings yet
- Entrapment of The Posterior Interosseous Nerve - Ax ArticleDocument9 pagesEntrapment of The Posterior Interosseous Nerve - Ax ArticleNaz HossNo ratings yet
- HEP2GO Carpal Tunnel Program PDFDocument2 pagesHEP2GO Carpal Tunnel Program PDFBetty OberackerNo ratings yet
- altMeasuresMUST PDFDocument1 pagealtMeasuresMUST PDFmahunNo ratings yet
- Bromothymol Blue - C27H28Br2O5S - PubChemDocument15 pagesBromothymol Blue - C27H28Br2O5S - PubChemDeangelis DamasNo ratings yet
- Biofeedback Stabilizer Manual PDFDocument188 pagesBiofeedback Stabilizer Manual PDFEugenio López Recio100% (1)
- Ischiorectal Fossa Anatomy and It's Suppuration: DR - Niveditha S Dr.S.Chandak DR - Melissa P Dr.C.MahkalkarDocument18 pagesIschiorectal Fossa Anatomy and It's Suppuration: DR - Niveditha S Dr.S.Chandak DR - Melissa P Dr.C.MahkalkarSagarRathodNo ratings yet