Professional Documents
Culture Documents
NCP For Hiatal Hernia
NCP For Hiatal Hernia
Uploaded by
Lalaine Nadulpit100%(2)100% found this document useful (2 votes)
2K views3 pagesThe nursing care plan addresses a patient experiencing hiatal hernia symptoms including regurgitation, dyspnea, coughing and chest pain. Short term goals are to provide relief from symptoms within an hour and help the patient experience less regurgitation. Interventions include monitoring for aspiration signs, modifying diet and position, and administering antacids. Long term goals are for the patient to reduce aspiration risk and experience no regurgitation or pain, to be evaluated within 2 days.
Original Description:
www
Original Title
NCP for Hiatal Hernia
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThe nursing care plan addresses a patient experiencing hiatal hernia symptoms including regurgitation, dyspnea, coughing and chest pain. Short term goals are to provide relief from symptoms within an hour and help the patient experience less regurgitation. Interventions include monitoring for aspiration signs, modifying diet and position, and administering antacids. Long term goals are for the patient to reduce aspiration risk and experience no regurgitation or pain, to be evaluated within 2 days.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
100%(2)100% found this document useful (2 votes)
2K views3 pagesNCP For Hiatal Hernia
NCP For Hiatal Hernia
Uploaded by
Lalaine NadulpitThe nursing care plan addresses a patient experiencing hiatal hernia symptoms including regurgitation, dyspnea, coughing and chest pain. Short term goals are to provide relief from symptoms within an hour and help the patient experience less regurgitation. Interventions include monitoring for aspiration signs, modifying diet and position, and administering antacids. Long term goals are for the patient to reduce aspiration risk and experience no regurgitation or pain, to be evaluated within 2 days.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
You are on page 1of 3
NURSING CARE PLAN FOR HIATAL HERNIA
ASSESSMENT NURSING INFERENCE PLAN OF INTERVENTIONS RATIONALE EVALUATION
DIAGNOSIS CARE
Subjective Data: Risk for Dyspnea and Short Term 1. Monitor respiratory rate, depth, 1. Signs of aspiration should be Short Term Goal:
The patient aspiration coughing are Goal: and effort. Note any signs of detected as soon as possible Within an hour of
complained of related to caused by aspiration such as dyspnea, to prevent further aspiration nursing
frequent recurrent gastric acids Within an hour cough, cyanosis, wheezing, or and to initiate immediate interventions,
regurgitation after regurgitation that have of nursing fever. treatment. the client was able
meals and of gastric entered the interventions, 2. Auscultate for lung sounds 2. To determine presence of to demonstrate
vomiting of blood. contents lungs. The the client will 3. Assess patient’s ability to secretions in the lungs. relief from dyspnea
“Maasim ang regurgitation of demonstrate swallow and the presence 3. Loss of the gag reflex and coughing. The
panlasa ko at gastric acids relief from of gag reflex. increases the risk of client was able to
mahapdi sa cause swelling dyspnea and 4. Avoid placing patient aspiration. experience less
lalamunan ang of the airways coughing. The in supine position, have the 4. Supine position after meals and clear
pakiramdam. and stimulates client will also patient sit upright after meals. can increase regurgitation of regurgitation of
Nauubo ako dahil coughing experience 5. Elevate HOB while in bed.. acid. gastric acids.
may mahapdi sa reflex. less and clear 6. Instruct the patient to chew food 5. To prevent aspiration by
lalamunan ko. May regurgitation thoroughly and eat slowly. preventing the gastric acid to
konting dugo din of gastric 7. Assist/instruct in relaxation flow back in the esophagus.
po sa suka ko.” acids. techniques, e.g., deep/slow 6. Well-masticated food is easier
breathing to swallow. Food should be cut Long Term Goal:
Long Term into small pieces.
Objective Data: Goal: DEPENDENT/ COLLABORATIVE: 7. Helpful in decreasing The client was
T: 36.5 C discomfort and difficulty in able to reduce the
PR: 83 bpm The client will 8. Administer Antacids as ordered. breathing. risk of aspiration
RR: 10 cpm be able to 9. Instruct patient to avoid highly as evidenced by
BP:120/80 mmHg reduce the seasoned food, acidic juices, DEPENDENT/ COLLABORATIVE: effective breathing
O2 Sat.: 95% risk of alcoholic drinks, bedtime 8. To minimize gastric and no coughing
aspiration as snacks, and foods high in fat. hyperacidity and minimize within 2 days of
Patient is observed evidenced by episodes of regurgitations. nursing
with discomfort, effective 9. These can reduce the lower interventions. The
dyspnea and breathing and esophageal sphincter pressure client also
coughing. no coughing and decrease the production experienced no
within 2 days of gastric acids. regurgitation of
of nursing gastric acids.
interventions.
The client will
also
experience no
regurgitation
of gastric
acids
ASSESSMENT NURSING INFERENCE PLAN OF INTERVENTIONS RATIONALE EVALUATION
DIAGNOSIS CARE
Subjective Data: Acute pain Short Term 1. Assess for heartburn. 1. To determine the presence of Short Term Goal:
The patient related to Goal: (characteristic, severity, GERD. Heartburn is the most
complained of irritation in frequency) common feature of GERD. Within an hour of
regurgitation of the Within an hour 2. Carefully assess pain location 2. Pain of esophageal spasm nursing
acid and esophageal of nursing and discern pain from GERD resulting from reflux interventions,
heartburn. mucosa as interventions, and angina pectoris. esophagitis tends to be the client was able
evidenced by the client will 3. Avoid placing patient chronic and may mimic angina to report relief from
“Maasim ang regurgitation report relief in supine position, have the pectoris: radiating to the neck, pain as evidenced
panlasa ko at of acid and from pain as patient sit upright after meals. jaws, and arms. by a decrease in
mahapdi sa heart burn. evidenced by 4. Elevate HOB while in bed.. 3. Supine position after meals the rating of chest
lalamunan ang a decrease in 5. Instruct the patient to chew food can increase regurgitation of pain by 7/10 to
pakiramdam. the rating of thoroughly and eat slowly. acid. 5/10.
Nauubo ako dahil chest pain by 6. Assist/instruct in relaxation 4. To prevent aspiration by
may mahapdi sa 7/10 to 5/10. techniques, e.g., deep/slow preventing the gastric acid to Long Term Goal:
lalamunan ko. breathing flow back in the esophagus.
Mainit at masakit Long Term 5. Well-masticated food is easier The client was
ang pakiramdam Goal: to swallow. Food should be cut able to feel
sa dibdib ko. DEPENDENT/ COLLABORATIVE: into small pieces. relieved from pain
Nararamdaman ko The client will 7. Administer Antacids as ordered. 6. Helpful in decreasing and did not
din ang sakit sa be relieved 8. Instruct patient to avoid highly discomfort and difficulty in experience
may braso ko.” from pain and seasoned food, acidic juices, breathing. heartburn and
will not alcoholic drinks, bedtime regurgitation within
experience snacks, and foods high in fat 2 days of nursing
Objective Data: heartburn and . DEPENDENT/ COLLABORATIVE: interventions.
T: 36.5 C regurgitation 7. To minimize gastric
PR: 83 bpm within 2 days hyperacidity and minimize
RR: 10 cpm of nursing episodes of regurgitations and
BP:120/80 mmHg interventions. heartburn
O2 Sat.: 95% 8. These can reduce the lower
esophageal sphincter pressure
Patient is observed and decrease the production
with discomfort of gastric acids.
and guarding
behavior in the
chest.
Pain Scale of 7/10.
ASSESSMENT NURSING INFERENCE PLAN OF INTERVENTIONS RATIONALE EVALUATION
DIAGNOSIS CARE
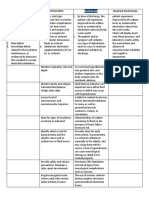
Subjective Data: Knowledge Limited health Short Term 1. Assess patient for information 1. Provides a basis for patient Short Term Goal:
“Hindi ko alam deficit related literacy skills Goal: needed and ability to perform teaching.
kung bakit laging to lack of are often actions independently. 2. Provides knowledge and Client did not
samasakit ang information greater among Client will 2. Provide patient with information facilitates compliance. experience heart
sikmura at dibdib regarding certain groups; have an regarding disease 3. Gravity helps control reflux burn and
ko pagkatapos condition/dis older adults, increased process, health practices that and causes less irritation from regurgitation after
kumain.” as ease process people with knowledge can be changed, and reflux action into the 2 hours of nursing
verbalized by the as evidenced limited regarding medications to be utilized. esophagus. interventions.
patient. by presence education, actions 3. Instruct patient regarding eating 4. Promotes comfort by
of minority preventing the small amounts of bland food the decrease in Long Term Goal:
preventable population. occurrence of followed by a small amount of intra-abdominal pressure,
complication Clients with low heart burn water. Instruct to remain in which reduces the reflux of The client showed
s. literacy skills and upright position at least 1–2 gastric contents. full understanding
have less regurgitation hours after meals, and to avoid 5. Helps prevent reflux. and implemented
information after 2 hours eating within 2–4 hours of 6. These food items increase ways to prevent
about health of nursing bedtime. acid production that the occurrence of
promotion interventions. 4. Instruct patient to avoid bending precipitates heartburn and heart burn and
and/or over, coughing, straining at increased reflux. regurgitation after
management of Long Term defecations, and other activities 7. Promotes knowledge, 2 hours of nursing
a disease Goal: that increase reflux. facilitates compliance with interventions.
process for 5. Instruct patients to eat slowly, treatment, and allows for
themselves. The client will chew foods well and maintain a prompt identification of
be able to fully high-protein, low-fat diet. potential need for changes in
understand 6. Instruct patient to avoid medication regimen to prevent
and temperature extremes of food, complications.
implement the spicy foods, and citrus, and gas
ways to forming foods.
prevent the 7. Instruct patient in medications,
occurrence of effects, side effects, and to
heart burn report to physician if symptoms
and persist
regurgitation despite medication treatment.
after 2 hours
of nursing
interventions.
You might also like
- Musical Acoustics PDFDocument26 pagesMusical Acoustics PDFGino Mendoza0% (1)
- MPM TroubleshootingDocument34 pagesMPM TroubleshootingMustafaNo ratings yet
- Hiatal Hernia Nursing Care Plan - Risk For AspirationDocument1 pageHiatal Hernia Nursing Care Plan - Risk For AspirationCyrus De Asis100% (12)
- OCAMPO, Maria Cecilia R. BSN 3d2 - 8i / MS Nursing Care Plan Related To Hypercalcemia Assessment Diagnosis Planning Intervention Rationale EvaluationDocument2 pagesOCAMPO, Maria Cecilia R. BSN 3d2 - 8i / MS Nursing Care Plan Related To Hypercalcemia Assessment Diagnosis Planning Intervention Rationale Evaluationchurva_freak433533% (9)
- Coronary Artery Disease Care PlanDocument2 pagesCoronary Artery Disease Care PlanDanelle Harrison, RN100% (2)
- Synthesis Outline + Essay TemplateDocument7 pagesSynthesis Outline + Essay TemplatefirdausNo ratings yet
- E Voting SystemDocument68 pagesE Voting Systemkeisha baby100% (1)
- Imbalanced NutritionDocument3 pagesImbalanced NutritionKM100% (6)
- NURSING-CARE-PLAN-Lung-Cancerxxx 1Document3 pagesNURSING-CARE-PLAN-Lung-Cancerxxx 1Caroline Cha100% (1)
- Nursing Care Plan For Peptic Ulcer NCPDocument2 pagesNursing Care Plan For Peptic Ulcer NCPJose Escobar100% (3)
- Myocarditis NCP 2Document8 pagesMyocarditis NCP 2astro_aaron117375% (4)
- NCP Peptic Ulcer DsDocument4 pagesNCP Peptic Ulcer Dsplug0650% (10)
- Nursing Care Plan For A Patient With Pleural EffusionDocument5 pagesNursing Care Plan For A Patient With Pleural Effusionmac042250% (4)
- GerDocument6 pagesGerLalaine NadulpitNo ratings yet
- The Civil War - The Universe of War (Episode 5)Document5 pagesThe Civil War - The Universe of War (Episode 5)ShreyaNo ratings yet
- Bullying, Stalking and ExtortionDocument17 pagesBullying, Stalking and ExtortionJLafge83% (6)
- NCP Hiatal HerniaDocument8 pagesNCP Hiatal HerniaLalaine NadulpitNo ratings yet
- Diarrhea (AGE)Document2 pagesDiarrhea (AGE)NursesLabs.com100% (1)
- Nursing Care Plan ConstipationDocument2 pagesNursing Care Plan ConstipationGio Baduria100% (1)
- NCP AfDocument3 pagesNCP AfAngelica Mercado SirotNo ratings yet
- Nursing Care Plan - CancerDocument3 pagesNursing Care Plan - CancerChristineAla0% (1)
- NCP PancreatitisDocument2 pagesNCP PancreatitisJeanelle Generoso100% (1)
- Nursing Care Plan Peptic UlcerDocument3 pagesNursing Care Plan Peptic UlcerJefferson Baluyot PalmaNo ratings yet
- Nursing Diagnosis Care Plan HyponitremiaDocument2 pagesNursing Diagnosis Care Plan HyponitremiaAbdallah AlasalNo ratings yet
- Nursing Care Plan UlcerDocument2 pagesNursing Care Plan Ulcerxrampley2100% (2)
- NCP Imbalanced NutritionDocument3 pagesNCP Imbalanced NutritionAav Canlas100% (1)
- Difficulty in SwallowingDocument1 pageDifficulty in SwallowingmawelNo ratings yet
- NCP - Acute Pain Related To EdemaDocument2 pagesNCP - Acute Pain Related To EdemaChenime Añana0% (1)
- Nursing Care Plan: Assessment Diagnosis Inference Planning Intervention Rationale EvaluationDocument3 pagesNursing Care Plan: Assessment Diagnosis Inference Planning Intervention Rationale EvaluationAbdallah AlasalNo ratings yet
- Nursing Care Plan Cues Nursing Diagnosis Scientific Analysis Objectives Nursing Interventions Rationale Evaluat IONDocument6 pagesNursing Care Plan Cues Nursing Diagnosis Scientific Analysis Objectives Nursing Interventions Rationale Evaluat IONAlex SilvanoNo ratings yet
- Lopez, Maria Sofia B. 10/07/2020 3-BSN-B Prof. Zoleta: Nursing Care Plan: PneumoniaDocument9 pagesLopez, Maria Sofia B. 10/07/2020 3-BSN-B Prof. Zoleta: Nursing Care Plan: PneumoniaSofia Lopez100% (2)
- Anxiety Related To Hospitalization and Disease Condition As Manifested by Fiscal Expression and VerbalizationDocument2 pagesAnxiety Related To Hospitalization and Disease Condition As Manifested by Fiscal Expression and VerbalizationmonaNo ratings yet
- Constipation NCPDocument2 pagesConstipation NCPAbby GonzalesNo ratings yet
- NCPDocument1 pageNCPJ. ishtelleNo ratings yet
- NCPDocument7 pagesNCPChris Denver BancaleNo ratings yet
- Imbalanced Nutrition Less Than Body Requirements Diabetes NCP PDFDocument5 pagesImbalanced Nutrition Less Than Body Requirements Diabetes NCP PDFashamy acolNo ratings yet
- NCP For HeadacheDocument1 pageNCP For HeadacheJohn MajanNo ratings yet
- NCP (Deficient Fluid VolumeDocument3 pagesNCP (Deficient Fluid VolumeNica RespondoNo ratings yet
- Body Weakness NCPDocument1 pageBody Weakness NCPtwicetrashNo ratings yet
- NCP DMDocument6 pagesNCP DMstara123No ratings yet
- Assessment Diagnosis Planning Intervention Rationale EvaluationDocument2 pagesAssessment Diagnosis Planning Intervention Rationale EvaluationVecky TolentinoNo ratings yet
- ASSESSMENT S: "Nanghihina Ako, Hindi Ko Magawa Yung Mga GustoDocument1 pageASSESSMENT S: "Nanghihina Ako, Hindi Ko Magawa Yung Mga GustoCherie MayNo ratings yet
- NCP: Acute GastroenteritisDocument3 pagesNCP: Acute GastroenteritishauteanicoleNo ratings yet
- Constipation NCPDocument2 pagesConstipation NCPDemilyn Olofernes-Fat100% (1)
- NCP Imbalanced NutritionDocument2 pagesNCP Imbalanced NutritionLyka Ngayan88% (8)
- Hyperkalemia: Ateneo de Naga University College of Nursing Nursing Care PlanDocument1 pageHyperkalemia: Ateneo de Naga University College of Nursing Nursing Care PlanRenie Serrano100% (1)
- Novilyn C. Pataray BSN - Ii Sickle Cell Anemia: St. Paul College of Ilocos SurDocument1 pageNovilyn C. Pataray BSN - Ii Sickle Cell Anemia: St. Paul College of Ilocos SurCharina AubreyNo ratings yet
- NCPDocument2 pagesNCPJhel NabosNo ratings yet
- Asthma Nanda DiagnosesDocument4 pagesAsthma Nanda DiagnosesZinya Robinson100% (1)
- Chronic Obstructive Pulmonary Disease (COPD)Document1 pageChronic Obstructive Pulmonary Disease (COPD)Bheru LalNo ratings yet
- NCP Liver CirrhosisDocument7 pagesNCP Liver CirrhosisIris Jimenez-BuanNo ratings yet
- Heart Failure Nursing Care Plans - 15 Nursing Diagnosis - NurseslabsDocument13 pagesHeart Failure Nursing Care Plans - 15 Nursing Diagnosis - NurseslabsJOSHUA DICHOSONo ratings yet
- Subjective: The Client's Grandmother Stated " Hindi Pa Nga Siya Dumudumi Simula Nung Nahospital Siya Ngayon. Mga Apat Na Araw Na Ata." ObjectiveDocument2 pagesSubjective: The Client's Grandmother Stated " Hindi Pa Nga Siya Dumudumi Simula Nung Nahospital Siya Ngayon. Mga Apat Na Araw Na Ata." ObjectiveAngelou MortosNo ratings yet
- Nursing Care Plan Rheumatoid ArthritisDocument3 pagesNursing Care Plan Rheumatoid ArthritisJashAnia MarIe EvArdo FloresNo ratings yet
- Activity 5 NCPDocument5 pagesActivity 5 NCPAl-Mujib TanogNo ratings yet
- Assessment Nursing Diagnosis Scientific Rationale Planning Intervention Rationale EvaluationDocument9 pagesAssessment Nursing Diagnosis Scientific Rationale Planning Intervention Rationale Evaluationclydell joyce masiarNo ratings yet
- Asthma Nursing Care Plan NCP Ineffective Airway Clearance CompressDocument2 pagesAsthma Nursing Care Plan NCP Ineffective Airway Clearance CompressMargarette GeresNo ratings yet
- Cap Nursing Care PlanDocument6 pagesCap Nursing Care PlanCharlene Grace ReginoNo ratings yet
- Final Na Jud Ni As In!Document19 pagesFinal Na Jud Ni As In!joyrena ochondraNo ratings yet
- Assesment Diagnosis Planning Intervention Rationale EvaluationDocument3 pagesAssesment Diagnosis Planning Intervention Rationale EvaluationTrisha Suazo100% (1)
- Cu 4Document3 pagesCu 4Paul SahagunNo ratings yet
- Romero, Deinielle Ingrid M. (Hiv)Document8 pagesRomero, Deinielle Ingrid M. (Hiv)Deinielle Magdangal RomeroNo ratings yet
- Paps NCPDocument8 pagesPaps NCPMerry Joy PapionaNo ratings yet
- Cues Nursing Diagnosis Background Knowledge Goals of Care Intervention Rationale EvaluationDocument2 pagesCues Nursing Diagnosis Background Knowledge Goals of Care Intervention Rationale EvaluationCharles Dave AgustinNo ratings yet
- Cues Nursing Diagnosis Background Knowledge Goals of Care Intervention Rationale EvaluationDocument2 pagesCues Nursing Diagnosis Background Knowledge Goals of Care Intervention Rationale EvaluationCharles Dave AgustinNo ratings yet
- Final Thyroid Storm NCPDocument6 pagesFinal Thyroid Storm NCPoguitekim1No ratings yet
- DULNUANDocument2 pagesDULNUANJB tindonganNo ratings yet
- Patient Administered Sexual History QuestionnaireDocument1 pagePatient Administered Sexual History QuestionnaireLalaine NadulpitNo ratings yet
- Examples of Questions For The HOPE Approach To Spiritual AssessmentDocument3 pagesExamples of Questions For The HOPE Approach To Spiritual AssessmentLalaine NadulpitNo ratings yet
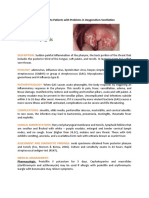
- Acute Pharyngitis: MODULE 2A: Nursing Care To Patients With Problems in Oxygenation-VentilationDocument2 pagesAcute Pharyngitis: MODULE 2A: Nursing Care To Patients With Problems in Oxygenation-VentilationLalaine NadulpitNo ratings yet
- I Belong To A ParishDocument18 pagesI Belong To A ParishLalaine NadulpitNo ratings yet
- Betty NeumanDocument1 pageBetty NeumanLalaine NadulpitNo ratings yet
- Loss & End of Life IssuesDocument4 pagesLoss & End of Life IssuesLalaine NadulpitNo ratings yet
- Ms - Castillo Ms - Castillo MR - Padua: Cycle 3 April 5-April 30 Monday T Wednesday TH Friday SaturdayDocument3 pagesMs - Castillo Ms - Castillo MR - Padua: Cycle 3 April 5-April 30 Monday T Wednesday TH Friday SaturdayLalaine NadulpitNo ratings yet
- NCP Hiatal HerniaDocument8 pagesNCP Hiatal HerniaLalaine NadulpitNo ratings yet
- Scrub Nurse Circulating NurseDocument2 pagesScrub Nurse Circulating NurseLalaine Nadulpit100% (3)
- As A Nurse Who Is in Charge of Caring The Clients With Altered Immune System Function, How Will You Promote and Maintain A Healthy Immune System?Document1 pageAs A Nurse Who Is in Charge of Caring The Clients With Altered Immune System Function, How Will You Promote and Maintain A Healthy Immune System?Lalaine NadulpitNo ratings yet
- What Is Inflammation?: Cellular Response To InjuryDocument10 pagesWhat Is Inflammation?: Cellular Response To InjuryLalaine NadulpitNo ratings yet
- JKHGKDocument1 pageJKHGKLalaine NadulpitNo ratings yet
- NCM 111 ForumDocument1 pageNCM 111 ForumLalaine NadulpitNo ratings yet
- Should The Nurse Do?Document1 pageShould The Nurse Do?Lalaine NadulpitNo ratings yet
- Apnea. (2020) - N.P.: Sciencedaily. Retrieved September 3, 2020, FromDocument9 pagesApnea. (2020) - N.P.: Sciencedaily. Retrieved September 3, 2020, FromLalaine NadulpitNo ratings yet
- Activity 1 Stating Your Research TopicDocument6 pagesActivity 1 Stating Your Research TopicLalaine NadulpitNo ratings yet
- GEM 101 - Bayaning Third World Analysis NadulpitBSN3ADocument2 pagesGEM 101 - Bayaning Third World Analysis NadulpitBSN3ALalaine NadulpitNo ratings yet
- CAD Concept Map FinalDocument4 pagesCAD Concept Map FinalLalaine NadulpitNo ratings yet
- FA 3 - Rizal's Homage To Luna and Hidalgo NadulpitBSN3ADocument2 pagesFA 3 - Rizal's Homage To Luna and Hidalgo NadulpitBSN3ALalaine NadulpitNo ratings yet
- GEM 101 - Luneta Park 3D View NadulpitBSN3ADocument1 pageGEM 101 - Luneta Park 3D View NadulpitBSN3ALalaine NadulpitNo ratings yet
- What I Know What I Want To Know What I Have LearntDocument1 pageWhat I Know What I Want To Know What I Have LearntLalaine NadulpitNo ratings yet
- Execution and Legacy: M5 - Exile, Trial and DeathDocument4 pagesExecution and Legacy: M5 - Exile, Trial and DeathLalaine NadulpitNo ratings yet
- Heroism or Rizal InfographicsDocument1 pageHeroism or Rizal InfographicsLalaine NadulpitNo ratings yet
- Transfer of Balance-NLEXDocument1 pageTransfer of Balance-NLEXLalaine NadulpitNo ratings yet
- Lalaine G. Nadulpit Bs Nursing 3ADocument3 pagesLalaine G. Nadulpit Bs Nursing 3ALalaine NadulpitNo ratings yet
- A GUIDE TO TRULY RICH CLUB by BO SANCHEZDocument4 pagesA GUIDE TO TRULY RICH CLUB by BO SANCHEZRaymunda Rauto-avilaNo ratings yet
- Veterinary MicrobiologyDocument206 pagesVeterinary MicrobiologyHomosapienNo ratings yet
- Greece Education Foundation Courses and Gces 10 2010Document6 pagesGreece Education Foundation Courses and Gces 10 2010Stamatios KarapournosNo ratings yet
- Furosemide DSDocument2 pagesFurosemide DSjhanrey0810_18768No ratings yet
- Legal Reasoning For Seminal U S Texts Constitutional PrinciplesDocument13 pagesLegal Reasoning For Seminal U S Texts Constitutional PrinciplesOlga IgnatyukNo ratings yet
- Deed of DonationDocument2 pagesDeed of DonationMary RockwellNo ratings yet
- Kindergarten HandbookDocument5 pagesKindergarten HandbookElizabeth MoorlagNo ratings yet
- HABASIT 04 Guía Ingeniería HabasitLINKDocument100 pagesHABASIT 04 Guía Ingeniería HabasitLINKKyriakos MichalakiNo ratings yet
- Ia 2 Compilation of Quiz and ExercisesDocument16 pagesIa 2 Compilation of Quiz and ExercisesclairedennprztananNo ratings yet
- Academic Calendar Fall 19-Spring 20 & Summer 20-Final-1 PDFDocument3 pagesAcademic Calendar Fall 19-Spring 20 & Summer 20-Final-1 PDFAhmadNo ratings yet
- Usb MSC Boot 1.0Document19 pagesUsb MSC Boot 1.0T.h. JeongNo ratings yet
- Logging Best Practices Guide PDFDocument12 pagesLogging Best Practices Guide PDFbnanduriNo ratings yet
- PGDRD Mail Assignment 26 Feb PalitDocument8 pagesPGDRD Mail Assignment 26 Feb PalitDeepak PandeyNo ratings yet
- Informative Essays TopicsDocument9 pagesInformative Essays Topicsb725c62j100% (2)
- Print - Udyam Registration CertificateDocument2 pagesPrint - Udyam Registration CertificatesahityaasthaNo ratings yet
- Major Landforms of The Earth NotesDocument3 pagesMajor Landforms of The Earth NotesSIMMA SAI PRASANNANo ratings yet
- 11.02.2022-PHC ResultsDocument6 pages11.02.2022-PHC ResultsNILAY TEJANo ratings yet
- Affidavit - ERRONEOUS ENTRY - Alzate 2Document1 pageAffidavit - ERRONEOUS ENTRY - Alzate 2Diaz Law OfficeNo ratings yet
- p-37 Recovery of Gold From Its OresDocument33 pagesp-37 Recovery of Gold From Its OresRussell Hartill100% (6)
- OutDocument318 pagesOutBet HalNo ratings yet
- OSPE DU MedicineDocument101 pagesOSPE DU MedicinesaifNo ratings yet
- PROCERA: A New Way To Achieve An All-Ceramic CrownDocument12 pagesPROCERA: A New Way To Achieve An All-Ceramic CrownCúc Phương TrầnNo ratings yet
- Accounting For Managers: S. No. Questions 1Document5 pagesAccounting For Managers: S. No. Questions 1shilpa mishraNo ratings yet
- Trial in AbsentiaDocument12 pagesTrial in AbsentiaNahid hossainNo ratings yet