Professional Documents
Culture Documents
Case Study 2
Case Study 2
Uploaded by
oumou80Original Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Case Study 2
Case Study 2
Uploaded by
oumou80Copyright:
Available Formats
Case Study 2
History:
Ester is a 75-year-old female who is not active.
Presentation and Examination
The patient presents with Parkinson’s disease (PD). She was diagnosed at the age of 35. This
was considered early for her age range. She first saw signs when she was tripping on small
cracks. Parkinson’s disease is a neurodegenerative (loss of neutrons in brain cell) disorder
affecting the motor skill of a person. Which can then affect a person's physical, functional and
mental activity. With age, Parkinson’s disease will later take over the body. The patient is now
in stage 5.
However, symptoms are bradykinesia, rigidity, hyperkinesia and resting tremor (Mestre, 2010).
Tremor is looking at the patient fingers. Rigidity is looking at the limb movement in a jerking
increment, and looking if the neck is stiff or trunk. Bradykinesia when a patient takes longer to
complete most activities such as, rising from a sitting position or turning in bed. Hyperkinesia
causes abnormally diminished movement. At a later stage patient suffering from PD have a
higher chance of falling, less control of motor function, dementia and a loss of autonomy. My
client is in the last stage. In my experience usually, they are very stiff from their head to there
entire body. Her face is mask-like and expressionless. Her speech is soft, slurred and less
audible. The patient has problems with muscle and joint function. She develops dysphagia
because she drools, and is at risk for choking or aspiration. I have to do everything for her. That
is why I'm here to assist them with everything she needs help with. But it takes a lot of work
doing it by myself. So usually I have another aid to assist me. She has an issue with
hypertension. Taking care of an elderly with Parkinson's takes a lot of work, it is usually not
easy to hold them up by yourself, she can not walk anymore and we need a wheelchair to move
her around. Even though I am tired and sometimes impatient, I remember that the best part of
my day is knowing I did everything for my patients. Sometimes seeing my patient sick, I feel
bad, but I try forgetting that so I can help them become healthy person. I strive to help them live
and enjoy the next day.
Diagnosis:
Diagnostic for Parkinson’s disease is PET scanning which is used in evaluating levodopa uptake
and conversion to dopamine in the corpus striatum. The doctors will look at patient history and
their daily activities. The doctor can do a neurologic examination.
Treatment and Outcomes:
There are no medical or surgical approaches that prevent PD. They are ways to slow down the
progression of the disease. There is pharmacologic therapy such as she is taking dopamine
agonists (immediate release, controlled release, and patch). She is being treated with
levodopa-carbidopa 100/25 mg. Also, one and a half pills q.i.d., and non-ergot derivative of
ropinirole. She also takes benztropine which is acetylcholine blocking drugs. The patient had
surgical interventions which they implanted a pacemaker. It's like a brain implant showing
promising results in relieving tremors. She had physical therapy 2 times a week. Sometimes she
went to swimming therapy to help her balance.
Cite:
Hayes, L. “Early Onset Parkinson’s Disease. Part 1: The Patient’s Story.” Canadian Family
Physician 40 (1994): 506–508. Print.
Mestre, Tiago, and Joaquim J Ferreira. “Pharmacotherapy in Parkinson's disease: case
studies.” Therapeutic advances in neurological disorders vol. 3,2 (2010): 117-26.
doi:10.1177/1756285609352366
You might also like
- Focus On Nursing Pharmacology 6th Edition Karch Test BankDocument16 pagesFocus On Nursing Pharmacology 6th Edition Karch Test BankElizabethGomezxepgk100% (17)
- Mock Oral CasesDocument6 pagesMock Oral Casestcbarot100% (1)
- Biology Investigatory Parkinson's PDFDocument16 pagesBiology Investigatory Parkinson's PDFaneesh100% (2)
- HM-325-Service Guide (01-14)Document14 pagesHM-325-Service Guide (01-14)Carlos Rea100% (1)
- Parkinson's DiseaseDocument11 pagesParkinson's Diseaseleeyan2wenty6100% (3)
- The Headache Healer’s Handbook: A Holistic, Hands-On Somatic Self-Care Program for Headache and Migraine Relief and PreventionFrom EverandThe Headache Healer’s Handbook: A Holistic, Hands-On Somatic Self-Care Program for Headache and Migraine Relief and PreventionNo ratings yet
- My Sister's Keeper Reaction Paper - Moral DilemmaDocument2 pagesMy Sister's Keeper Reaction Paper - Moral DilemmaJanelle Leano MarianoNo ratings yet
- Case Study 2FDocument2 pagesCase Study 2Foumou80No ratings yet
- Intensive Nursing Practicum: Bachelor of Science in NursingDocument9 pagesIntensive Nursing Practicum: Bachelor of Science in NursingMichelle Gliselle Guinto MallareNo ratings yet
- A Simple Guide to Parkinson's Disease and Related Brain ConditionsFrom EverandA Simple Guide to Parkinson's Disease and Related Brain ConditionsNo ratings yet
- This Study Resource Was: ScenarioDocument3 pagesThis Study Resource Was: ScenarioIrish Jane GalloNo ratings yet
- PD WRDocument20 pagesPD WRepeydenfajardoNo ratings yet
- Laporan Tutorial Edit 2Document21 pagesLaporan Tutorial Edit 2Magenda BismaNo ratings yet
- HomeoDocument34 pagesHomeoSrinivas SrinuNo ratings yet
- Psychiatry Topic - WPS OfficeDocument9 pagesPsychiatry Topic - WPS OfficeJs JsNo ratings yet
- An Essay On The Shaking Palsy: Five Stages of Parkinsons DiseaseDocument16 pagesAn Essay On The Shaking Palsy: Five Stages of Parkinsons DiseaseBindu NairNo ratings yet
- Homoeopathic Treatment of Parkinson DieseDocument23 pagesHomoeopathic Treatment of Parkinson DieseNidhi SrivastavaNo ratings yet
- Parkinson Disease Grand Case PresDocument25 pagesParkinson Disease Grand Case PresLord Allen B. GomezNo ratings yet
- TG 4 Parkinson (NL)Document20 pagesTG 4 Parkinson (NL)Novi AdriNo ratings yet
- Parkinsons HTR English 20-ns-139 508cDocument36 pagesParkinsons HTR English 20-ns-139 508cMaria Madel AquinoNo ratings yet
- BDDKP 1Document35 pagesBDDKP 1Chidube UkachukwuNo ratings yet
- Skenario 1 Kaku Dan Tremor: Disusun Oleh: Nama: Risnasari Stambuk: G 501 11 011 Kelompok: 3 (TIGA)Document22 pagesSkenario 1 Kaku Dan Tremor: Disusun Oleh: Nama: Risnasari Stambuk: G 501 11 011 Kelompok: 3 (TIGA)Risna SariNo ratings yet
- Parkinson's Disease: Prepared by Bhawana ShresthaDocument12 pagesParkinson's Disease: Prepared by Bhawana ShresthaDiksha SapkotaNo ratings yet
- A Nurse Is CaringDocument2 pagesA Nurse Is CaringChubs RiegoNo ratings yet
- Parkinsons Disease PHD ThesisDocument5 pagesParkinsons Disease PHD Thesischristinawestcharleston100% (2)
- Parkinson's DiseaseDocument3 pagesParkinson's DiseaseRachelle Ann E. De FelixNo ratings yet
- Administrator, Journal Manager, 368-1206-1-CEDocument3 pagesAdministrator, Journal Manager, 368-1206-1-CESameer KhanNo ratings yet
- Mental Health Case StudyDocument15 pagesMental Health Case Studyapi-508142358No ratings yet
- Aileen Mccabe: Human Development Psy. 127 4W2Document12 pagesAileen Mccabe: Human Development Psy. 127 4W2EarlNo ratings yet
- Conversion Disorder TreatmentDocument9 pagesConversion Disorder Treatmentapi-241111102No ratings yet
- Parkinson S DiseaseDocument91 pagesParkinson S DiseaseTrisha Tolentino100% (1)
- Dizziness - PPPD Information SheetDocument8 pagesDizziness - PPPD Information Sheettan_siqi100% (1)
- Biology Investigatory Project: Topic: Parkinson'S DiseaseDocument18 pagesBiology Investigatory Project: Topic: Parkinson'S DiseaseAneesh MoosaNo ratings yet
- Backup of Disorders - OverviewDocument7 pagesBackup of Disorders - OverviewmacaronloverNo ratings yet
- Conversion Disorder: Cynthia M. Stonnington, M.D. John J. Barry, M.D. Robert S. Fisher, M.D., PH.DDocument8 pagesConversion Disorder: Cynthia M. Stonnington, M.D. John J. Barry, M.D. Robert S. Fisher, M.D., PH.DLiza MelendrezNo ratings yet
- Capstone Case Study1 - Quiz 1studyDocument3 pagesCapstone Case Study1 - Quiz 1studyMary StrangeNo ratings yet
- Ocd-Treatment Publishing NardoneDocument62 pagesOcd-Treatment Publishing Nardoneneri100% (2)
- Disabilities Research PaperDocument8 pagesDisabilities Research Paperapi-662638224No ratings yet
- Psychological MasqueradeDocument32 pagesPsychological MasqueradeChen_scribeNo ratings yet
- Cerebral Palsy: I. Definition/ DescriptionDocument4 pagesCerebral Palsy: I. Definition/ Descriptionfaye kim100% (1)
- Reporter: Degenerative Diseases of The Central Nervous System (CNS) Parkinson's DiseaseDocument6 pagesReporter: Degenerative Diseases of The Central Nervous System (CNS) Parkinson's DiseaseMelody B. MiguelNo ratings yet
- CCJM Essential Tremor Choosing The Right Management Plan For Your PatientDocument8 pagesCCJM Essential Tremor Choosing The Right Management Plan For Your PatientBrian HarrisNo ratings yet
- AlzehiemerDocument40 pagesAlzehiemerdatumNo ratings yet
- Depressed MoodDocument3 pagesDepressed MoodlkdsjflsNo ratings yet
- A Rare Case of Obsessive-Compulsive Disorder WithDocument5 pagesA Rare Case of Obsessive-Compulsive Disorder WithAnand JhaNo ratings yet
- Functional Neurological Symptoms DisorderDocument18 pagesFunctional Neurological Symptoms DisorderWaqas Ahmed UsmaniNo ratings yet
- Depression Ad Cerebral PalsyDocument2 pagesDepression Ad Cerebral PalsyReinhaMaeDaduyaNo ratings yet
- Sujok For ParkinsonsDocument2 pagesSujok For ParkinsonsPranicHealingCentre75% (4)
- DR A.A.Ayu Meidiary, SPS: Department of Neurology, Sanglah General Hospital, Udayana University DenpasarDocument47 pagesDR A.A.Ayu Meidiary, SPS: Department of Neurology, Sanglah General Hospital, Udayana University DenpasarKertiasihwayanNo ratings yet
- Case Study Parkinsonism 2019 StudentDocument3 pagesCase Study Parkinsonism 2019 StudentAyman NabilNo ratings yet
- Research Paper Parkinson DiseaseDocument5 pagesResearch Paper Parkinson Diseasem0d1p1fuwub2100% (1)
- Parkinson'S Disease What Is Parkinson's Disease?Document6 pagesParkinson'S Disease What Is Parkinson's Disease?FadhilaKPNo ratings yet
- Psych Case StudyDocument13 pagesPsych Case Studyapi-732900066No ratings yet
- 10 Page Mental HealthDocument13 pages10 Page Mental Healthapi-736365670No ratings yet
- WHAT IS PARKINSONsDocument6 pagesWHAT IS PARKINSONsRPNNo ratings yet
- Pica Strok0Document1 pagePica Strok0Adel SalehNo ratings yet
- Casestudy 76 Case Study 24Document7 pagesCasestudy 76 Case Study 24Irish Jane GalloNo ratings yet
- Sleep Paralysis, (Parasomnia) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandSleep Paralysis, (Parasomnia) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Septiani de Vinta 154310618 III A D IV KebidananDocument5 pagesSeptiani de Vinta 154310618 III A D IV KebidananvintaNo ratings yet
- Ayurvedic Home Remedies For ParalysisDocument2 pagesAyurvedic Home Remedies For ParalysisPravin BholeNo ratings yet
- Paleracio Case StudyDocument18 pagesPaleracio Case StudySONY MANDAPNo ratings yet
- Gold 2021Document164 pagesGold 2021Rona Karmela BravoNo ratings yet
- Marquardt Et Al 2014 Impact of The Design of The Built Environment On People With Dementia An Evidence Based ReviewDocument31 pagesMarquardt Et Al 2014 Impact of The Design of The Built Environment On People With Dementia An Evidence Based Reviewyfive soneNo ratings yet
- Disaster Management: by Ananda.SDocument34 pagesDisaster Management: by Ananda.SAnand gowda100% (2)
- Argumentati Ve Essay: Sri Rejeki, S.P D., M.PDDocument11 pagesArgumentati Ve Essay: Sri Rejeki, S.P D., M.PDRahma OktaviaNo ratings yet
- Literature Review On Quantitative EasingDocument5 pagesLiterature Review On Quantitative Easingaflrrefsn100% (1)
- Task 5 Banksia-SD-SE-T1-Hazard-Report-Form-Template-V1.0-ID-200278Document5 pagesTask 5 Banksia-SD-SE-T1-Hazard-Report-Form-Template-V1.0-ID-200278Samir Mosquera-PalominoNo ratings yet
- Are You A Psychopath-TestDocument3 pagesAre You A Psychopath-TestMalinaNo ratings yet
- Difficult Airway Management: By: Bereket Habtamu Advisor: Leulayehu AkaluDocument72 pagesDifficult Airway Management: By: Bereket Habtamu Advisor: Leulayehu AkaluagatakassaNo ratings yet
- Test Bank - Nutrition and Diet Therapy 7th EditionDocument14 pagesTest Bank - Nutrition and Diet Therapy 7th EditiongreygalaxyNo ratings yet
- Journal Pone 0255465Document15 pagesJournal Pone 0255465wonNo ratings yet
- CBSE Provisions For CWSNDocument20 pagesCBSE Provisions For CWSNManisha Verma100% (1)
- Questions and Answers From The Webinar Community Health Workers: Their Role in Preventing and Controlling Chronic ConditionsDocument13 pagesQuestions and Answers From The Webinar Community Health Workers: Their Role in Preventing and Controlling Chronic ConditionsGift EseNo ratings yet
- Camarin High School First Quarterly Examination - Mapeh 8: National Capital Region Division of Caloocan CityDocument3 pagesCamarin High School First Quarterly Examination - Mapeh 8: National Capital Region Division of Caloocan CityReynaldo Rolan Jr.No ratings yet
- Triage Scale For Post Stroke Patients A Basis For Improving Nurses PriortizationDocument13 pagesTriage Scale For Post Stroke Patients A Basis For Improving Nurses PriortizationLance RaphaelNo ratings yet
- Orientation Clinical HemaDocument10 pagesOrientation Clinical HemaPRECIOUS DIANNE BARDON-MEMPINNo ratings yet
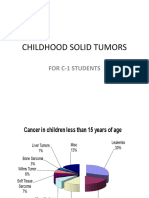
- Childhood Solid Tumors: For C-1 StudentsDocument72 pagesChildhood Solid Tumors: For C-1 StudentsYemata HailuNo ratings yet
- Genetics Class 10Document7 pagesGenetics Class 10Manjit KumarNo ratings yet
- Homeopathic Management of Ring WormDocument3 pagesHomeopathic Management of Ring WormEditor IJTSRDNo ratings yet
- Pölzl Et Al 2023 Association of High Sensitivity Cardiac Troponin T With 30 Day and 5 Year Mortality After CardiacDocument12 pagesPölzl Et Al 2023 Association of High Sensitivity Cardiac Troponin T With 30 Day and 5 Year Mortality After CardiacKardiologi ManadoNo ratings yet
- Effect of Kundalini Yoga On Alpha MSHDocument2 pagesEffect of Kundalini Yoga On Alpha MSHUniversal Saints CommunityNo ratings yet
- IT 9 - Arthritis in SLE - HMSDocument38 pagesIT 9 - Arthritis in SLE - HMSRurie Awalia Suhardi0% (1)
- Objective: Jamel Alaa - Dr. PorfDocument62 pagesObjective: Jamel Alaa - Dr. Porfhussain AltaherNo ratings yet
- Introduction+to+the+Health+System+2023 RPDocument42 pagesIntroduction+to+the+Health+System+2023 RPSibabalwe DlovasheNo ratings yet
- The Insecticidal Potency of Nee-Gano (Neem, Azadirachta Indica OreganoDocument9 pagesThe Insecticidal Potency of Nee-Gano (Neem, Azadirachta Indica Oreganostevenlloyd maybituinNo ratings yet
- Understanding StressDocument13 pagesUnderstanding StressMimi LabindaoNo ratings yet
- Leg Length Discrepancy (LLD) : H Fcmaf PM Ambcare AMB P AGE OFDocument1 pageLeg Length Discrepancy (LLD) : H Fcmaf PM Ambcare AMB P AGE OFanuragNo ratings yet