Professional Documents
Culture Documents
Pacemaking-A Technique: Transvenous
Pacemaking-A Technique: Transvenous
Uploaded by
Gerry ValdyCopyright:
Available Formats
You might also like
- ACLS Answer KeyDocument23 pagesACLS Answer KeyKirana Budhiarta94% (17)
- Pathophysiology of Congestive Heart Failure: Predisposing Factors Precipitating/Aggravating FactorsDocument1 pagePathophysiology of Congestive Heart Failure: Predisposing Factors Precipitating/Aggravating Factorsguillermojerry100% (2)
- Easy Hypertension ClassificationDocument1 pageEasy Hypertension ClassificationGirish WaruNo ratings yet
- Ventricular Tachycardia: Jçrgen Schreieck, Gabriele Hessling, Alexander Pustowoit, Claus SchmittDocument28 pagesVentricular Tachycardia: Jçrgen Schreieck, Gabriele Hessling, Alexander Pustowoit, Claus SchmittFuad AlamsyahNo ratings yet
- Idiopathic Fascicular Left Ventricular Tachycardia: Linear Ablation Lesion Strategy For Noninducible or Nonsustained TachycardiaDocument6 pagesIdiopathic Fascicular Left Ventricular Tachycardia: Linear Ablation Lesion Strategy For Noninducible or Nonsustained TachycardiaRahmi SyuadzahNo ratings yet
- Konecny 2015Document5 pagesKonecny 2015Iszlai Matyas JenoNo ratings yet
- Kalyanam Shivkumar Catheter Ablation of VentricularDocument10 pagesKalyanam Shivkumar Catheter Ablation of Ventricularrvp.180088No ratings yet
- 1 s2.0 S2589790X20300998 MainDocument3 pages1 s2.0 S2589790X20300998 MainAlbert EinsteinNo ratings yet
- 1 s2.0 S1880427607800184 MainDocument4 pages1 s2.0 S1880427607800184 MainVimal NishadNo ratings yet
- Askep Ps DGN Tindakan Invasif & INB KD 2021Document91 pagesAskep Ps DGN Tindakan Invasif & INB KD 2021gayuspatarru123No ratings yet
- Electrocautery-Induced Complete Heart BlockDocument3 pagesElectrocautery-Induced Complete Heart BlockTheUdoNo ratings yet
- Pacemaker 180508042454Document86 pagesPacemaker 180508042454padmaNo ratings yet
- How To Perform A Transseptal Puncture: Mark J EarleyDocument9 pagesHow To Perform A Transseptal Puncture: Mark J EarleyAttilio Del RossoNo ratings yet
- CazuriDocument4 pagesCazuriIbănescu Iulia AndreeaNo ratings yet
- Journal of ElectrocardiologyDocument3 pagesJournal of ElectrocardiologyFederico FalsettiNo ratings yet
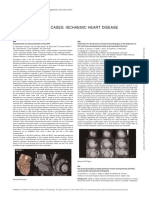
- Clinical Cases: Ischaemic Heart DiseaseDocument4 pagesClinical Cases: Ischaemic Heart DiseaseLADY JOWAHER ALLASNo ratings yet
- Arritmia SVDocument17 pagesArritmia SVCésar Lobo TarangoNo ratings yet
- MSCARDIODocument6 pagesMSCARDIOmark OrpillaNo ratings yet
- Frugal Innovation in The Cardiac Catheter Laboratory: Retrograde Balloon Mitral Valvuloplasty Using Extra Back-Up Guide CatheterDocument4 pagesFrugal Innovation in The Cardiac Catheter Laboratory: Retrograde Balloon Mitral Valvuloplasty Using Extra Back-Up Guide CatheterGisselle RomeroNo ratings yet
- ContentServer Asp3Document7 pagesContentServer Asp3ganda gandaNo ratings yet
- Pacemaker Invasive Cardiac PacingDocument57 pagesPacemaker Invasive Cardiac PacingAhmad Khalil Ahmad Al-SadiNo ratings yet
- Salerno (1978) - Monitoring of Electroencephalogram During Open-Heart SurgeryDocument4 pagesSalerno (1978) - Monitoring of Electroencephalogram During Open-Heart SurgeryVanessaNo ratings yet
- An Important Cause of Wide Complex Tachycardia: Case PresentationDocument2 pagesAn Important Cause of Wide Complex Tachycardia: Case PresentationLuis Fernando Morales JuradoNo ratings yet
- Iatrogenic Acute Aortic Dissection During PPCIDocument4 pagesIatrogenic Acute Aortic Dissection During PPCISajjad HussainNo ratings yet
- 1 s2.0 S0022522312009099 MainDocument9 pages1 s2.0 S0022522312009099 MainFayaNuraldaSitompulNo ratings yet
- Ablation of Ventricular Tachycardia in Chronic Chagasic Cardiomyopathy With Giant Basal AneurysmDocument3 pagesAblation of Ventricular Tachycardia in Chronic Chagasic Cardiomyopathy With Giant Basal AneurysmjjsanchezmunozNo ratings yet
- S2405500X20305983 MainDocument10 pagesS2405500X20305983 MainMSNo ratings yet
- A Rare Case of PJRT Ablated On The Roof of The Left Atrium 2012Document4 pagesA Rare Case of PJRT Ablated On The Roof of The Left Atrium 2012Võ Từ NhấtNo ratings yet
- Basics of The 12-Lead ECG - CE Article - NursingCenterDocument13 pagesBasics of The 12-Lead ECG - CE Article - NursingCenterتمارا مقداديNo ratings yet
- Bertini 2019Document7 pagesBertini 2019Marcos DuarteNo ratings yet
- Ventricular Tachycardic Storm With A Chronic Total Coronary Artery Occlusion Treated With Percutaneous Coronary InterventionDocument4 pagesVentricular Tachycardic Storm With A Chronic Total Coronary Artery Occlusion Treated With Percutaneous Coronary InterventionRJMNo ratings yet
- Revchilanestv 5007101119Document4 pagesRevchilanestv 5007101119Javier HdezNo ratings yet
- Mitral Annulus VT PDFDocument10 pagesMitral Annulus VT PDFNarendra KumarNo ratings yet
- Atrial Flutter An Update PDFDocument17 pagesAtrial Flutter An Update PDFPriska FebiolaNo ratings yet
- Ecg Junctionalventriculararrhythmias 140109180429 Phpapp02Document21 pagesEcg Junctionalventriculararrhythmias 140109180429 Phpapp02Morad KananNo ratings yet
- 247 FullDocument6 pages247 FullBryan FarrelNo ratings yet
- 6.V3 (2) 105 112Document8 pages6.V3 (2) 105 112Hima HuNo ratings yet
- Unusual Variants of Pre Excitation 2019Document19 pagesUnusual Variants of Pre Excitation 2019Võ Từ NhấtNo ratings yet
- Abstract Avrtcad2vd MuhammadakhiruddinDocument2 pagesAbstract Avrtcad2vd MuhammadakhiruddinNanank Akhiruddin SyamsaNo ratings yet
- Belhajsoulami 2018Document3 pagesBelhajsoulami 2018rédaNo ratings yet
- J HRTHM 2014 10 002Document9 pagesJ HRTHM 2014 10 002cpagtchadNo ratings yet
- Atrial Flutter: An Update: Revista Espa de Cardiologia September 2006Document17 pagesAtrial Flutter: An Update: Revista Espa de Cardiologia September 2006siensimuNo ratings yet
- Case Report - Aortic Valve Replacement Due To Aortic Valve Leaflet Perforation After PCIDocument3 pagesCase Report - Aortic Valve Replacement Due To Aortic Valve Leaflet Perforation After PCIInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- AR Yang Komplikasi Menjadi Gagal Jantung PDFDocument5 pagesAR Yang Komplikasi Menjadi Gagal Jantung PDFFitriani AlawiyahNo ratings yet
- Ailoaei Et Al 2021 Zero Fluoroscopy Ablation For Atrial Re Entry Via A Vein of Marshall Connection Using A VisibleDocument5 pagesAiloaei Et Al 2021 Zero Fluoroscopy Ablation For Atrial Re Entry Via A Vein of Marshall Connection Using A VisibleAndrés AllaucaNo ratings yet
- Case: Stenting of A Critical Internal Carotid Artery Stenosis With String SignDocument9 pagesCase: Stenting of A Critical Internal Carotid Artery Stenosis With String SignCarol ArtigasNo ratings yet
- Supraventricular TachycardiDocument8 pagesSupraventricular TachycardiHairunisa 0049No ratings yet
- Cardiac Surgery For Arrhythmias: Naspe 25 A SDocument13 pagesCardiac Surgery For Arrhythmias: Naspe 25 A SJuan José Sánchez MuñozNo ratings yet
- Ecmo Cannula Size JournalDocument9 pagesEcmo Cannula Size Journalbreaking nurseNo ratings yet
- (03241750 - Acta Medica Bulgarica) Multiple Congenital Heart AbnormalitiesDocument4 pages(03241750 - Acta Medica Bulgarica) Multiple Congenital Heart AbnormalitiesTeodorNo ratings yet
- Seminar On PacemakerDocument14 pagesSeminar On Pacemakerjyothi50% (4)
- TachycardiaDocument7 pagesTachycardiamikiNo ratings yet
- Multimodality Imaging in Sepsis Related Myocardial CalcificationDocument5 pagesMultimodality Imaging in Sepsis Related Myocardial CalcificationRakhmat RamadhaniNo ratings yet
- AT Vs AVNRT ECGDocument10 pagesAT Vs AVNRT ECGRushil NundlallNo ratings yet
- Clinmed 23 5 442Document7 pagesClinmed 23 5 442Mey TalabessyNo ratings yet
- 58-63 DallAra JIC 2020 Feb WMDocument6 pages58-63 DallAra JIC 2020 Feb WMJose Manuel Ornelas-AguirreNo ratings yet
- Ablation Above The Semilunar Valves: When, Why, and How?: Mahmoud Suleiman, MD, Samuel J. Asirvatham, MDDocument6 pagesAblation Above The Semilunar Valves: When, Why, and How?: Mahmoud Suleiman, MD, Samuel J. Asirvatham, MDkaushikNo ratings yet
- VT CriteriaDocument8 pagesVT CriterianitipatNo ratings yet
- Crite RiosDocument8 pagesCrite RiosNilson Morales CordobaNo ratings yet
- TSV Con Aberrancia o TVDocument7 pagesTSV Con Aberrancia o TVOliverVasconcelosNo ratings yet
- Prominent Epsilon Waves in A Patient With Cardiac SarcoidosisDocument6 pagesProminent Epsilon Waves in A Patient With Cardiac Sarcoidosisdaniel gallegoNo ratings yet
- Decoding Cardiac Electrophysiology: Understanding the Techniques and Defining the JargonFrom EverandDecoding Cardiac Electrophysiology: Understanding the Techniques and Defining the JargonAfzal SohaibNo ratings yet
- CardiologyDocument83 pagesCardiologyAshutosh SinghNo ratings yet
- Cardiac Insufficiency Bisoprolol Study (CIBIS III) TrialDocument6 pagesCardiac Insufficiency Bisoprolol Study (CIBIS III) TrialClaudia TiffanyNo ratings yet
- Lippincott Antiarrhythmics 7Document2 pagesLippincott Antiarrhythmics 7Wijdan HatemNo ratings yet
- Permanent Pacemaker Implantation / Box Change - A Guide To The ProcedureDocument5 pagesPermanent Pacemaker Implantation / Box Change - A Guide To The ProcedureSapna thakurNo ratings yet
- Cardiovascular Examination IBDDocument6 pagesCardiovascular Examination IBDTRINIDAD, ALYANNA V.No ratings yet
- MKSAP13-Cardiovascular MedicineDocument102 pagesMKSAP13-Cardiovascular MedicineManisha DesaiNo ratings yet
- Elsevier ElectronicJournalPrices2024Document129 pagesElsevier ElectronicJournalPrices2024atanu.ece.citulubNo ratings yet
- 5-Heart FailureDocument12 pages5-Heart FailureJericho De GuzmanNo ratings yet
- Surgery (EACTS)Document116 pagesSurgery (EACTS)Sergio Vidal Mamani VillarrealNo ratings yet
- Ecg in DogsDocument107 pagesEcg in DogsPLABITA GOSWAMI100% (2)
- Serum Zinc Values in Children With Congenital Heart DiseaseDocument6 pagesSerum Zinc Values in Children With Congenital Heart DiseaseTri Novita SariNo ratings yet
- EcgDocument45 pagesEcgkamel6No ratings yet
- Webinar Flyer IACA Prof DR MuralidharDocument4 pagesWebinar Flyer IACA Prof DR Muralidharalvionita fitrianaNo ratings yet
- Aortic StenosisDocument8 pagesAortic Stenosisikbal rambalinoNo ratings yet
- Rido, Rudini - Paediatric ECGDocument51 pagesRido, Rudini - Paediatric ECGFikriYTNo ratings yet
- Evaluation and Management of Premature Ventricular ComplexesDocument15 pagesEvaluation and Management of Premature Ventricular ComplexesJohnbray Castellanos DiazNo ratings yet
- Cardiovascular DiseaseDocument73 pagesCardiovascular DiseaseAli SherNo ratings yet
- Ambulatory Elaphic MonitoDocument3 pagesAmbulatory Elaphic Monitocap tainNo ratings yet
- Cardiac GlycosidesDocument8 pagesCardiac GlycosidesShan Sicat100% (1)
- Naif SMLE QshareDocument319 pagesNaif SMLE QshareHuzaif KhatibNo ratings yet
- 991111 EUS教學 (6) 重點式急診心臟超音波之應用Document67 pages991111 EUS教學 (6) 重點式急診心臟超音波之應用juice119100% (5)
- Neurologic Disorders Associated With Mitral Valve ProlapseDocument6 pagesNeurologic Disorders Associated With Mitral Valve Prolapsegeorgiana_884431330No ratings yet
- (02.12) CM Valvular Heart Diseases (TG20) - Anne Gabrielle LiuDocument18 pages(02.12) CM Valvular Heart Diseases (TG20) - Anne Gabrielle LiuMikmik DGNo ratings yet
- PACKRAT Cardio Questions PDFDocument63 pagesPACKRAT Cardio Questions PDFkat100% (1)
- The Client With A Cardiovascular AlterationDocument15 pagesThe Client With A Cardiovascular AlterationDana Erica D. CarandangNo ratings yet
- Position Paper: A B C D e F G H CDocument11 pagesPosition Paper: A B C D e F G H CNico IonaşcuNo ratings yet
- Acute Coronary Syndrome (Sindroma Koroner Akut) : Zulfikri MukhtarDocument32 pagesAcute Coronary Syndrome (Sindroma Koroner Akut) : Zulfikri MukhtarWina DeskyNo ratings yet
Pacemaking-A Technique: Transvenous
Pacemaking-A Technique: Transvenous
Uploaded by
Gerry ValdyOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Pacemaking-A Technique: Transvenous
Pacemaking-A Technique: Transvenous
Uploaded by
Gerry ValdyCopyright:
Available Formats
British Heart Journal, I97I, 33, I9I-I92.
Br Heart J: first published as 10.1136/hrt.33.2.191 on 1 March 1971. Downloaded from http://heart.bmj.com/ on April 28, 2021 by guest. Protected by copyright.
Transvenous pacemaking-a bedside technique
Charles L. Baird
From Cardiovascular Division, Department of Medicine, Medical College of Virginia,
Richmond 23219, U.S.A.
A technique, termed 'pacing' method, is describedfor the blind insertion of temporary transvenous
*pacemakers. Advantage may be taken of cardiac pacing with minimal risk in situations where
X fluoroscopic control is not available.
The introduction of endocardial electrode
* catheters for cardiac pacing has significantly
altered the management of cardiac arrhyth-
Blind Insertion of the
,,mias. Temporary transvenous pacemaking is Transvenous Pacemaker Catheter
frequently indicated in patients with AV
,block and uncontrolled tachyarrhythmias. In ("Pacing Method")
the acutely ill patients, where fluoroscopy is
not available, flexible unipolar pacemaker MUSCLE
catheters have been inserted blindly by re- CONTRACTIONC
cording the intracavitary electrocardiogram
Jfrom the tip of the catheter electrode (Kim-
ball and Killip, I965). However, knotted LT
ATRA
catheters, difficulty with interpretation of the CApi TU RE w
intracavitary electrocardiogram, and incon-
stant pacing have been problems with this VENTRICULAR
unipolar catheter technique. Therefore, a < JiCAPTURE
7<1
blind technique (Siddons and Sowton, I967)
using stiff bipolar electrode catheters' without
intracavitary electrocardiography was em-
ployed in 3I patients.
Method
The transvenous bipolar pacemaker catheter is
introduced under sterile conditions into the MUSCLE
median basilic, external jugular, or saphenous CON TRACTI ON
s venous systems (Fig.) while the patient is under-
going continuous electrocardiographic monitoring.
--4he catheter is advanced until the right heart is
entered or an obstruction is met. At this time the
-two terminals ofthe catheter electrode are attached
to the external pulse generator2, and I-3 MA im-
- pulses at a slow rate are initiated. The position of
the catheter if lodged outside the heart is recog-
..,nized by skeletal muscle contractions induced by
pacemaker stimuli. Appropriate repositioning of
*e catheter allows for further advancement
toward the right atrium. As the catheter ap-
proaches the right heart the pacemaker stimuli
- Received 23 January 1970.
'Bipolar Pacemaker Catheter, Electro-Catheter Cor-
Lporation, 932 East Elizabeth Avenue, Linden, N. J.
2 Medtronic Model 5840 External Pacemaker,
Med-
tronic, Inc., 3055 Old Highway Eight, Minneapolis,
Minnesota.
192 Charles L. Baird
Br Heart J: first published as 10.1136/hrt.33.2.191 on 1 March 1971. Downloaded from http://heart.bmj.com/ on April 28, 2021 by guest. Protected by copyright.
become visible on the oscilloscope. Successful cardiogram confirmed the extrusion of the
entrance of the catheter into the right atrium is
pacemaker catheter tip by recording an epi-
manifested by atrial pacing, i.e. an artificial stimu-
cardial lead pattern before withdrawal back
lus or 'spike' preceding each P wave at a rate de-
into the right ventricular chamber. The
termined by the external pulse generator. The
catheter may then be passed into the right ven-patient tolerated this complication, as in most
cases of catheter perforation, without peri-
tricle where ventricular pacing is recognized by
the stimuli preceding the widened QRS com- cardial tamponade. It is entirely possible that
a greater incidence of cardiac perforation
plexes. 'Overdrive' of the atrial or ventricular
rhythm is easily accomplished by adjustment of during temporary pacing may be detected by
the rate and milliamperage control. the use of intracavitary electrocardiography.
The blind techniques using an intracavitary
Discussion electrocardiogram and the 'pacing' method
The 'pacing' method of blind insertion of described in this paper will eventually become
transvenous pacemaker catheters was success- obsolete with the wider use of portable fluor-
fully employed in 28 of 33 instances (3I oscopy and intensive care units equipped with
patients). Complications such as vessel per- image intensification. However, the distinct
foration, pacemaker-induced arrhythmias, or advantages of cardiac pacing in the control
patient intolerance to the skeletal muscle arrhythmias by fixed rate, demand, or coupled
stimulation were not observed during the in- stimulation warrant continued use of the
sertion. Prolonged or unsuccessful catheter blind insertion technique in situations where
insertion was attributed to soft or floppy fluoroscopy is not available.
catheters as well as extensive manipulation
required by the indirect approaches of the References
median basilic or external jugular venous Kimball, J. T., and Killip, T. (I965). A simple bedside
systems. However, recent experience with the method for transvenous intracardiac pacing.
American Heart Journal, 70, 35.
newly introduced Elecath 'semi-floating' bi- Siddons, H., and Sowton, E. (I967). Cardiac Pace-
polar pacemaker catheter has resulted in a makers. Charles C. Thomas, Springfield, Illinois.
high percentage of successful insertions from
the median basilic venous system. It must be Addendum
added that one patient in this group developed Approximately 100 additional patients have had
cardiac perforation manifested by diaphrag- successful semifloating bipolar pacemaker inser-
matic twitching. The intracavitary electro- tion with the method described.
You might also like
- ACLS Answer KeyDocument23 pagesACLS Answer KeyKirana Budhiarta94% (17)
- Pathophysiology of Congestive Heart Failure: Predisposing Factors Precipitating/Aggravating FactorsDocument1 pagePathophysiology of Congestive Heart Failure: Predisposing Factors Precipitating/Aggravating Factorsguillermojerry100% (2)
- Easy Hypertension ClassificationDocument1 pageEasy Hypertension ClassificationGirish WaruNo ratings yet
- Ventricular Tachycardia: Jçrgen Schreieck, Gabriele Hessling, Alexander Pustowoit, Claus SchmittDocument28 pagesVentricular Tachycardia: Jçrgen Schreieck, Gabriele Hessling, Alexander Pustowoit, Claus SchmittFuad AlamsyahNo ratings yet
- Idiopathic Fascicular Left Ventricular Tachycardia: Linear Ablation Lesion Strategy For Noninducible or Nonsustained TachycardiaDocument6 pagesIdiopathic Fascicular Left Ventricular Tachycardia: Linear Ablation Lesion Strategy For Noninducible or Nonsustained TachycardiaRahmi SyuadzahNo ratings yet
- Konecny 2015Document5 pagesKonecny 2015Iszlai Matyas JenoNo ratings yet
- Kalyanam Shivkumar Catheter Ablation of VentricularDocument10 pagesKalyanam Shivkumar Catheter Ablation of Ventricularrvp.180088No ratings yet
- 1 s2.0 S2589790X20300998 MainDocument3 pages1 s2.0 S2589790X20300998 MainAlbert EinsteinNo ratings yet
- 1 s2.0 S1880427607800184 MainDocument4 pages1 s2.0 S1880427607800184 MainVimal NishadNo ratings yet
- Askep Ps DGN Tindakan Invasif & INB KD 2021Document91 pagesAskep Ps DGN Tindakan Invasif & INB KD 2021gayuspatarru123No ratings yet
- Electrocautery-Induced Complete Heart BlockDocument3 pagesElectrocautery-Induced Complete Heart BlockTheUdoNo ratings yet
- Pacemaker 180508042454Document86 pagesPacemaker 180508042454padmaNo ratings yet
- How To Perform A Transseptal Puncture: Mark J EarleyDocument9 pagesHow To Perform A Transseptal Puncture: Mark J EarleyAttilio Del RossoNo ratings yet
- CazuriDocument4 pagesCazuriIbănescu Iulia AndreeaNo ratings yet
- Journal of ElectrocardiologyDocument3 pagesJournal of ElectrocardiologyFederico FalsettiNo ratings yet
- Clinical Cases: Ischaemic Heart DiseaseDocument4 pagesClinical Cases: Ischaemic Heart DiseaseLADY JOWAHER ALLASNo ratings yet
- Arritmia SVDocument17 pagesArritmia SVCésar Lobo TarangoNo ratings yet
- MSCARDIODocument6 pagesMSCARDIOmark OrpillaNo ratings yet
- Frugal Innovation in The Cardiac Catheter Laboratory: Retrograde Balloon Mitral Valvuloplasty Using Extra Back-Up Guide CatheterDocument4 pagesFrugal Innovation in The Cardiac Catheter Laboratory: Retrograde Balloon Mitral Valvuloplasty Using Extra Back-Up Guide CatheterGisselle RomeroNo ratings yet
- ContentServer Asp3Document7 pagesContentServer Asp3ganda gandaNo ratings yet
- Pacemaker Invasive Cardiac PacingDocument57 pagesPacemaker Invasive Cardiac PacingAhmad Khalil Ahmad Al-SadiNo ratings yet
- Salerno (1978) - Monitoring of Electroencephalogram During Open-Heart SurgeryDocument4 pagesSalerno (1978) - Monitoring of Electroencephalogram During Open-Heart SurgeryVanessaNo ratings yet
- An Important Cause of Wide Complex Tachycardia: Case PresentationDocument2 pagesAn Important Cause of Wide Complex Tachycardia: Case PresentationLuis Fernando Morales JuradoNo ratings yet
- Iatrogenic Acute Aortic Dissection During PPCIDocument4 pagesIatrogenic Acute Aortic Dissection During PPCISajjad HussainNo ratings yet
- 1 s2.0 S0022522312009099 MainDocument9 pages1 s2.0 S0022522312009099 MainFayaNuraldaSitompulNo ratings yet
- Ablation of Ventricular Tachycardia in Chronic Chagasic Cardiomyopathy With Giant Basal AneurysmDocument3 pagesAblation of Ventricular Tachycardia in Chronic Chagasic Cardiomyopathy With Giant Basal AneurysmjjsanchezmunozNo ratings yet
- S2405500X20305983 MainDocument10 pagesS2405500X20305983 MainMSNo ratings yet
- A Rare Case of PJRT Ablated On The Roof of The Left Atrium 2012Document4 pagesA Rare Case of PJRT Ablated On The Roof of The Left Atrium 2012Võ Từ NhấtNo ratings yet
- Basics of The 12-Lead ECG - CE Article - NursingCenterDocument13 pagesBasics of The 12-Lead ECG - CE Article - NursingCenterتمارا مقداديNo ratings yet
- Bertini 2019Document7 pagesBertini 2019Marcos DuarteNo ratings yet
- Ventricular Tachycardic Storm With A Chronic Total Coronary Artery Occlusion Treated With Percutaneous Coronary InterventionDocument4 pagesVentricular Tachycardic Storm With A Chronic Total Coronary Artery Occlusion Treated With Percutaneous Coronary InterventionRJMNo ratings yet
- Revchilanestv 5007101119Document4 pagesRevchilanestv 5007101119Javier HdezNo ratings yet
- Mitral Annulus VT PDFDocument10 pagesMitral Annulus VT PDFNarendra KumarNo ratings yet
- Atrial Flutter An Update PDFDocument17 pagesAtrial Flutter An Update PDFPriska FebiolaNo ratings yet
- Ecg Junctionalventriculararrhythmias 140109180429 Phpapp02Document21 pagesEcg Junctionalventriculararrhythmias 140109180429 Phpapp02Morad KananNo ratings yet
- 247 FullDocument6 pages247 FullBryan FarrelNo ratings yet
- 6.V3 (2) 105 112Document8 pages6.V3 (2) 105 112Hima HuNo ratings yet
- Unusual Variants of Pre Excitation 2019Document19 pagesUnusual Variants of Pre Excitation 2019Võ Từ NhấtNo ratings yet
- Abstract Avrtcad2vd MuhammadakhiruddinDocument2 pagesAbstract Avrtcad2vd MuhammadakhiruddinNanank Akhiruddin SyamsaNo ratings yet
- Belhajsoulami 2018Document3 pagesBelhajsoulami 2018rédaNo ratings yet
- J HRTHM 2014 10 002Document9 pagesJ HRTHM 2014 10 002cpagtchadNo ratings yet
- Atrial Flutter: An Update: Revista Espa de Cardiologia September 2006Document17 pagesAtrial Flutter: An Update: Revista Espa de Cardiologia September 2006siensimuNo ratings yet
- Case Report - Aortic Valve Replacement Due To Aortic Valve Leaflet Perforation After PCIDocument3 pagesCase Report - Aortic Valve Replacement Due To Aortic Valve Leaflet Perforation After PCIInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- AR Yang Komplikasi Menjadi Gagal Jantung PDFDocument5 pagesAR Yang Komplikasi Menjadi Gagal Jantung PDFFitriani AlawiyahNo ratings yet
- Ailoaei Et Al 2021 Zero Fluoroscopy Ablation For Atrial Re Entry Via A Vein of Marshall Connection Using A VisibleDocument5 pagesAiloaei Et Al 2021 Zero Fluoroscopy Ablation For Atrial Re Entry Via A Vein of Marshall Connection Using A VisibleAndrés AllaucaNo ratings yet
- Case: Stenting of A Critical Internal Carotid Artery Stenosis With String SignDocument9 pagesCase: Stenting of A Critical Internal Carotid Artery Stenosis With String SignCarol ArtigasNo ratings yet
- Supraventricular TachycardiDocument8 pagesSupraventricular TachycardiHairunisa 0049No ratings yet
- Cardiac Surgery For Arrhythmias: Naspe 25 A SDocument13 pagesCardiac Surgery For Arrhythmias: Naspe 25 A SJuan José Sánchez MuñozNo ratings yet
- Ecmo Cannula Size JournalDocument9 pagesEcmo Cannula Size Journalbreaking nurseNo ratings yet
- (03241750 - Acta Medica Bulgarica) Multiple Congenital Heart AbnormalitiesDocument4 pages(03241750 - Acta Medica Bulgarica) Multiple Congenital Heart AbnormalitiesTeodorNo ratings yet
- Seminar On PacemakerDocument14 pagesSeminar On Pacemakerjyothi50% (4)
- TachycardiaDocument7 pagesTachycardiamikiNo ratings yet
- Multimodality Imaging in Sepsis Related Myocardial CalcificationDocument5 pagesMultimodality Imaging in Sepsis Related Myocardial CalcificationRakhmat RamadhaniNo ratings yet
- AT Vs AVNRT ECGDocument10 pagesAT Vs AVNRT ECGRushil NundlallNo ratings yet
- Clinmed 23 5 442Document7 pagesClinmed 23 5 442Mey TalabessyNo ratings yet
- 58-63 DallAra JIC 2020 Feb WMDocument6 pages58-63 DallAra JIC 2020 Feb WMJose Manuel Ornelas-AguirreNo ratings yet
- Ablation Above The Semilunar Valves: When, Why, and How?: Mahmoud Suleiman, MD, Samuel J. Asirvatham, MDDocument6 pagesAblation Above The Semilunar Valves: When, Why, and How?: Mahmoud Suleiman, MD, Samuel J. Asirvatham, MDkaushikNo ratings yet
- VT CriteriaDocument8 pagesVT CriterianitipatNo ratings yet
- Crite RiosDocument8 pagesCrite RiosNilson Morales CordobaNo ratings yet
- TSV Con Aberrancia o TVDocument7 pagesTSV Con Aberrancia o TVOliverVasconcelosNo ratings yet
- Prominent Epsilon Waves in A Patient With Cardiac SarcoidosisDocument6 pagesProminent Epsilon Waves in A Patient With Cardiac Sarcoidosisdaniel gallegoNo ratings yet
- Decoding Cardiac Electrophysiology: Understanding the Techniques and Defining the JargonFrom EverandDecoding Cardiac Electrophysiology: Understanding the Techniques and Defining the JargonAfzal SohaibNo ratings yet
- CardiologyDocument83 pagesCardiologyAshutosh SinghNo ratings yet
- Cardiac Insufficiency Bisoprolol Study (CIBIS III) TrialDocument6 pagesCardiac Insufficiency Bisoprolol Study (CIBIS III) TrialClaudia TiffanyNo ratings yet
- Lippincott Antiarrhythmics 7Document2 pagesLippincott Antiarrhythmics 7Wijdan HatemNo ratings yet
- Permanent Pacemaker Implantation / Box Change - A Guide To The ProcedureDocument5 pagesPermanent Pacemaker Implantation / Box Change - A Guide To The ProcedureSapna thakurNo ratings yet
- Cardiovascular Examination IBDDocument6 pagesCardiovascular Examination IBDTRINIDAD, ALYANNA V.No ratings yet
- MKSAP13-Cardiovascular MedicineDocument102 pagesMKSAP13-Cardiovascular MedicineManisha DesaiNo ratings yet
- Elsevier ElectronicJournalPrices2024Document129 pagesElsevier ElectronicJournalPrices2024atanu.ece.citulubNo ratings yet
- 5-Heart FailureDocument12 pages5-Heart FailureJericho De GuzmanNo ratings yet
- Surgery (EACTS)Document116 pagesSurgery (EACTS)Sergio Vidal Mamani VillarrealNo ratings yet
- Ecg in DogsDocument107 pagesEcg in DogsPLABITA GOSWAMI100% (2)
- Serum Zinc Values in Children With Congenital Heart DiseaseDocument6 pagesSerum Zinc Values in Children With Congenital Heart DiseaseTri Novita SariNo ratings yet
- EcgDocument45 pagesEcgkamel6No ratings yet
- Webinar Flyer IACA Prof DR MuralidharDocument4 pagesWebinar Flyer IACA Prof DR Muralidharalvionita fitrianaNo ratings yet
- Aortic StenosisDocument8 pagesAortic Stenosisikbal rambalinoNo ratings yet
- Rido, Rudini - Paediatric ECGDocument51 pagesRido, Rudini - Paediatric ECGFikriYTNo ratings yet
- Evaluation and Management of Premature Ventricular ComplexesDocument15 pagesEvaluation and Management of Premature Ventricular ComplexesJohnbray Castellanos DiazNo ratings yet
- Cardiovascular DiseaseDocument73 pagesCardiovascular DiseaseAli SherNo ratings yet
- Ambulatory Elaphic MonitoDocument3 pagesAmbulatory Elaphic Monitocap tainNo ratings yet
- Cardiac GlycosidesDocument8 pagesCardiac GlycosidesShan Sicat100% (1)
- Naif SMLE QshareDocument319 pagesNaif SMLE QshareHuzaif KhatibNo ratings yet
- 991111 EUS教學 (6) 重點式急診心臟超音波之應用Document67 pages991111 EUS教學 (6) 重點式急診心臟超音波之應用juice119100% (5)
- Neurologic Disorders Associated With Mitral Valve ProlapseDocument6 pagesNeurologic Disorders Associated With Mitral Valve Prolapsegeorgiana_884431330No ratings yet
- (02.12) CM Valvular Heart Diseases (TG20) - Anne Gabrielle LiuDocument18 pages(02.12) CM Valvular Heart Diseases (TG20) - Anne Gabrielle LiuMikmik DGNo ratings yet
- PACKRAT Cardio Questions PDFDocument63 pagesPACKRAT Cardio Questions PDFkat100% (1)
- The Client With A Cardiovascular AlterationDocument15 pagesThe Client With A Cardiovascular AlterationDana Erica D. CarandangNo ratings yet
- Position Paper: A B C D e F G H CDocument11 pagesPosition Paper: A B C D e F G H CNico IonaşcuNo ratings yet
- Acute Coronary Syndrome (Sindroma Koroner Akut) : Zulfikri MukhtarDocument32 pagesAcute Coronary Syndrome (Sindroma Koroner Akut) : Zulfikri MukhtarWina DeskyNo ratings yet