Professional Documents
Culture Documents
2.6 Patient Safety, Errors & Complications
2.6 Patient Safety, Errors & Complications
Uploaded by
Miguel C. DolotCopyright:
Available Formats
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5825)
- FULL Download Ebook PDF International Trauma Life Support For Emergency Care Providers 9th Edition PDF EbookDocument51 pagesFULL Download Ebook PDF International Trauma Life Support For Emergency Care Providers 9th Edition PDF Ebookcarl.helbling11891% (53)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1093)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (852)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (903)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (541)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (349)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (823)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (403)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- CODE of Construction Safety PracticeDocument291 pagesCODE of Construction Safety PracticeBala Praveen97% (119)
- A. Bron, R. Tripathi, B. Tripathi - Wolff's Anatomy of The Eye and Orbit-CRC Press (1998) PDFDocument724 pagesA. Bron, R. Tripathi, B. Tripathi - Wolff's Anatomy of The Eye and Orbit-CRC Press (1998) PDFPS NI100% (1)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- 4.4 Acute AbdomenDocument6 pages4.4 Acute AbdomenMiguel C. Dolot100% (1)
- Dr:Khalid MiladDocument27 pagesDr:Khalid MiladMohsen Elzobna0% (1)
- 4.2 Abdominal Wall Hernia (Jerome Villacorta's Conflicted Copy 2014-03-22)Document7 pages4.2 Abdominal Wall Hernia (Jerome Villacorta's Conflicted Copy 2014-03-22)Miguel C. DolotNo ratings yet
- Nucleotide MetabolismDocument17 pagesNucleotide MetabolismMiguel C. DolotNo ratings yet
- 02.03-01 CNS II - General AnesthesiaDocument9 pages02.03-01 CNS II - General AnesthesiaMiguel C. DolotNo ratings yet
- Basic Ocular Surgeries: Fatima Medical Center Dr. Vicente O. Santos JR., MDDocument53 pagesBasic Ocular Surgeries: Fatima Medical Center Dr. Vicente O. Santos JR., MDMiguel C. DolotNo ratings yet
- Diabetes Mellitus 1Document47 pagesDiabetes Mellitus 1Miguel C. DolotNo ratings yet
- 4.3 Peritonitis (Lecture-Based)Document5 pages4.3 Peritonitis (Lecture-Based)Miguel C. DolotNo ratings yet
- Shoulder Dystocia: Ina S. Irabon, MD, Fpogs, FPSRM, FpsgeDocument25 pagesShoulder Dystocia: Ina S. Irabon, MD, Fpogs, FPSRM, FpsgeMiguel C. DolotNo ratings yet
- Cornea and External DiseasesDocument18 pagesCornea and External DiseasesMiguel C. DolotNo ratings yet
- 02.01-04 CNS I - AntiepilepticsDocument10 pages02.01-04 CNS I - AntiepilepticsMiguel C. DolotNo ratings yet
- Basic Neuro-Ophthalmology: Common Problems SeenDocument6 pagesBasic Neuro-Ophthalmology: Common Problems SeenMiguel C. DolotNo ratings yet
- 02.01-03 CNS I - AlcoholsDocument5 pages02.01-03 CNS I - AlcoholsMiguel C. DolotNo ratings yet
- 02.03-03 CNS II - Skeletal Muscle RelaxantsDocument7 pages02.03-03 CNS II - Skeletal Muscle RelaxantsMiguel C. DolotNo ratings yet
- 02.03-02 CNS II - Local AnesthesiaDocument5 pages02.03-02 CNS II - Local AnesthesiaMiguel C. DolotNo ratings yet
- Angeline D. Alabastro, M.D. Angeline D. Alabastro, M.D. Angeline D. Alabastro, M.DDocument7 pagesAngeline D. Alabastro, M.D. Angeline D. Alabastro, M.D. Angeline D. Alabastro, M.DMiguel C. DolotNo ratings yet
- Angeline D. Alabastro, M.D.: CNS Pharmacology I: AntiepilepticsDocument10 pagesAngeline D. Alabastro, M.D.: CNS Pharmacology I: AntiepilepticsMiguel C. DolotNo ratings yet
- 02.05. Patient-Doctor Relationship and Interviewing TechniquesDocument10 pages02.05. Patient-Doctor Relationship and Interviewing TechniquesMiguel C. DolotNo ratings yet
- 02.01-01 CNS I - Central NeurotransmittersDocument3 pages02.01-01 CNS I - Central NeurotransmittersMiguel C. DolotNo ratings yet
- Los Baños: Mental Status ExamDocument5 pagesLos Baños: Mental Status ExamMiguel C. DolotNo ratings yet
- 02.04. Physical Examination and Laboratory Tests in PsychiatryDocument12 pages02.04. Physical Examination and Laboratory Tests in PsychiatryMiguel C. DolotNo ratings yet
- Psychiatric History: Doc Los BañosDocument6 pagesPsychiatric History: Doc Los BañosMiguel C. DolotNo ratings yet
- Qbank FormatDocument5 pagesQbank FormatpashaNo ratings yet
- Brachial Plexus InjuryDocument39 pagesBrachial Plexus InjurymariaNo ratings yet
- Q2-Activity in Science-Bones, Joint, MusclesDocument2 pagesQ2-Activity in Science-Bones, Joint, MusclesMaggie DreuNo ratings yet
- The Bony Thorax Ana - Positioning. ReviewerDocument8 pagesThe Bony Thorax Ana - Positioning. Reviewercorrainnejimenez.24No ratings yet
- Stretching Exercises For Seniors Over 60Document134 pagesStretching Exercises For Seniors Over 60Sal OtNo ratings yet
- Tutorial Report Physiology and Work Measurement BiomechanicsDocument17 pagesTutorial Report Physiology and Work Measurement Biomechanicsalma millaniaNo ratings yet
- Deland 2005Document10 pagesDeland 2005DavidNo ratings yet
- Eor-2058-5241 1 000052Document13 pagesEor-2058-5241 1 000052Alfian PramuditaNo ratings yet
- Pathophysiology of Acute PainDocument12 pagesPathophysiology of Acute PainMuhammad Ghilman NurizzanNo ratings yet
- Biomechanics of TennisDocument7 pagesBiomechanics of Tennismiruna.stanescu12No ratings yet
- Data For Scaffolding JsaDocument8 pagesData For Scaffolding JsaRaza Muhammad SoomroNo ratings yet
- Chapter 3 - Physical Activity FitnessDocument44 pagesChapter 3 - Physical Activity FitnessSharmila KrishnaswamyNo ratings yet
- Article 261-265Document10 pagesArticle 261-265BOBIS, FRIALYN N.No ratings yet
- Accident ReportDocument2 pagesAccident Reportberj.garbouchiansbcglobal.netNo ratings yet
- Hope 2Document11 pagesHope 2Trisha Faye Tabuena PlanaNo ratings yet
- Unit 15Document3 pagesUnit 15Silent againNo ratings yet
- Causes and Investigation of Shock: Learning ObjectivesDocument3 pagesCauses and Investigation of Shock: Learning Objectivesstef lopezNo ratings yet
- USAP Continental Field ManualDocument146 pagesUSAP Continental Field Manualmvelilla12No ratings yet
- WALKING AIDS (Assistive Devices) : College of NursingDocument15 pagesWALKING AIDS (Assistive Devices) : College of NursingJojo JustoNo ratings yet
- MBA Thesis - MuruDocument79 pagesMBA Thesis - Murumurugeswaran.kpNo ratings yet
- Surgery QuestionsDocument19 pagesSurgery QuestionsdocaliNo ratings yet
- Sex Determination From Skeletal Remains - Forensic's BlogDocument10 pagesSex Determination From Skeletal Remains - Forensic's BlogReal AbrasNo ratings yet
- Prentice9e Im Chap18Document6 pagesPrentice9e Im Chap18api-281340024100% (1)
- Laboratory Manual For Anatomy and Physiology 6Th Edition Marieb Solutions Manual Full Chapter PDFDocument28 pagesLaboratory Manual For Anatomy and Physiology 6Th Edition Marieb Solutions Manual Full Chapter PDFJohnathanFitzgeraldnwoa100% (12)
- Forensic MedicineDocument32 pagesForensic Medicineferdosjm74No ratings yet
- BOSH SO2 Manual GovernmentDocument138 pagesBOSH SO2 Manual Governmentjasonrey.saysonNo ratings yet
2.6 Patient Safety, Errors & Complications
2.6 Patient Safety, Errors & Complications
Uploaded by
Miguel C. DolotOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
2.6 Patient Safety, Errors & Complications
2.6 Patient Safety, Errors & Complications
Uploaded by
Miguel C. DolotCopyright:
Available Formats
2.
6
September 19,2013
Hazel Z. Turingan, MD, FPCS, FPSGS, DPBTCVS, DMCC Patient Safety, Errors
Obedience is the mother of success and is wedded to safety. -Aeschylus & Complications
[TransGroup‘s Note: Texts in orange and tables and figures with
orange borders are those that have asterisks on Dr. Turingan‘s ppt.
Italicized texts are mostly Dr. Turingan‘s words.]
OUTLINE PAGE
Introduction 1
Types of Medical Errors 1
Creating a Culture of Safety 2
Communication Tools 2
Surgical Safety Checklist 3
Quality Patient Safety Indicators 4
Surgical Care Improvement Project Measures 4
National Quality Forum 4
Compliacations in Minor Procedures 5 If you see something, say it. Kahit mahina lang boses mo.
Organ System Complications Wag mong isipin na, “Ah, clerk pa lang ako, 4th year pa lang
Wounds, Drain and Infection ako.” You have to say what you saw because you might be
SIRS, Sepsis and MODS the only one who saw it. You‟re part of the medical team.
Issues in Caring for Obese Patients and
Patients at the Extremes of Ages TYPES OF MEDICAL ERRORS
INTRODUCTION Injury caused by medical management
Patient harm due to medical mistakes can be catastrophic rather than the patients‘s underlying
consequences for condition
o the patient Prolongs hospitalization, produces a
o the surgeon ADVERSE
disability at discharge, or both
o the institution EVENT
Classified as preventable or unpreventable
Patient safety It‟s not really part of the complication, it is
o science that promotes the use of evidence-based unexpected
medicine commonsense improvements in an attempt to Eg. MI in a very young patient
minimize the impact of human error on the routine Care that falls below a recognized standard
delivery of services of care
Poor communication contributes to approximately 70% of Standard of care
the sentinel events reported to the Joint Commission on o considered to be care a reasonable
Accreditation of Healthcare Organizations physician of similar knowledge, training,
Operating room briefings and experience would use in similar
o are team discussions of critical issues and potential NEGLIGENCE circumstances
hazards that can improve the safety of the operation eg. Surgeon transected the area where the
o shown to improve operating room culture decrease hernia is. He SHOULD know that he should
operating room delays not transect that area but rather isolate it,
Patient rapport retract it.. But he did it anyway. Under
o most important determinant of malpractice claims standard of care yung ginawa niya. He can
against a surgeon be sued here.
An error that does not result in patient
harm
Analysis of near misses provides the
opportunity to identify and remedy system
failures before the occurrence of harm
Ito, minor lang, it can be prevented.
Eg. The patient is coughing so you gave
him ambroxol. But it is actually secondary
NEAR MISS to the surgery kasi the patient was
intubated. Binigyan ng inhalation
anesthesia, so you expect a certain
atelectasis in the lungs. So the patient
cannot breathe well, hindi nageexpand
yung lungs niya so the patient keeps on
coughing. So you saw it, did something to
it, so the error was reversed. That‟s a near
miss. (in Filipino, kamuntikan na!)
Unexpected occurrence involving death or
SENTINEL serious physical or psychological injury,
EVENT injury involves loss of limb or function
requires immediate investigation and
Agatep. Detera. Doong. Rodriguez. Tejano. Villacorta Page 1 of 10
Patient Safety, Errors & Complications
response Pilipino, it may be awkward. But then now that I‟m a
Hemolytic transfusion reaction involving surgeon, I realized the importance of these things.”
administration of blood or blood products o Double check the patient‘s identification when they are
having major blood incompatibilities transferred between units.
Wrong-site, wrong-procedure, or wrong- o Re-check the patient‘s identification when they arrive
patient surgery at the O.R. and again in the O.R.
A medication error or other treatment- Always check
related error resulting in death o Patient history, consent and other documents
Unintentional retention of a foreign body in o Radiological studies needed
a patient after surgery o Implants and prosthesis if required
Eg. You did an arterial line, or BP o Patient identification or arm band
monitoring, or arterial puncture for an ABG. Mark the procedure site
Tapos biglang nangitim yung kamay ng o A licensed independent practitioner (or other provider
bata, that‟s a sentinel event. Nagthrombose who is privileged or permitted by the organization to
yung artery that can lead to amputation of perform the intended procedure) marks the procedure
the hand. site.
o Use the surgeon‘s or proceduralist‘s initials
(preferably), with or without a line representing the
CREATING A CULTURE OF SAFETY proposed incision.
An acknowledgment of the high-risk, error-prone nature of o The type of mark made should be used consistently
an organization's activities throughout the organization.
A nonpunitive environment where individuals are able to Time out for the team
report errors or close calls without fear of punishment or o Correct patient
retaliation o Correct procedure
An expectation of collaboration across ranks to seek o Correct side and site
solutions to vulnerabilities o Agreement that we are set to go
A willingness on the part of the organization to direct Help prevent wrong side, wrong site, wrong patient, and
resources to address safety concerns wrong procedures in your organization with the help of our
In the Philippines, especially in government institutions, we "Time Out" Poster.
will see this recording of these errors because we‟re afraid. o Poster highlights all of the important steps that must
We try to cover it up. And covering it up will not actually be taken to prevent wrong side, wrong site, wrong
solve the problem. But when you report it, we would know patient and wrong procedures in your organization.
what should be done to prevent it from happening. o Poster should be hung in the OR staff lounge, in patient
pre-operative areas and procedure rooms, as any place
COMMUNICATION TOOLS: an invasive procedure may occur in your facility.
Operating Room Briefings o Help to ensure that staff is continuously reminded that
‗time out‘ will ensure or minimize surgical identification
FIVE-POINT OPERATING ROOM BRIEFING errors.
What are the names and roles of the team members?
o Pagpasok ng room: “Hi! I‟m Dr. Hazel Turingan. I am PRE OP CHECKLIST DAY OF SURGERY
a thoracic cardiovascular surgeon. And I‟ll be operating Client teaching completed
the patient.” Tapos sabihin mo naman: “Hi I‟m Dr. X, Consent form signed
5th year resident, and I‟ll be the first assist.” NPO
o Then usually, there are two nurses: one is a circulating o hindi dahil sadista yung mga nasa OR. You don‟t feed
nurse—the one you call when you need something and them because when you intubate the patient, they might
she takes care of everything in the OR—and the other aspirate. Because when you put something in your
is scrub nurse—the one who will take care of the throat, you‟re tendency is to cough, and the vomitus
instruments and hand it to the surgeon. Pag may ibang might obstruct your airway. Kahit fluids, bawal din.
tao dun, “Sino ka? Anong ginagawa mo dito?” In gown
Is the correct patient/procedure confirmed? Allergy & ID Bands on
[Joint Commission Universal Protocol (TIME-OUT)] o this is an example of a near miss. Ask the patient kung
Have antibiotics been given? (if appropriate) may allergy ba siya sa, let‟s say NSAIDs. You can prevent
What are the critical steps of the procedure? such to happen if you ask the patient.
What are the potential problems for the case? No jewelry-bands taped
o always remove jewelry. Because whenever you do
TIME OUT! cautery, whatever metal is on your body, it might burn
Is this the right patient? on those areas where the metal is. Your wrist where you
Do we have the right location? place your watch. Even the metal in your bra. That‟s why
Are we doing the right procedure? you don‟t wear bra or even the garter of the brief during
surgery. Cotton lang allowable.
Verify the person, site and procedure Voiding prior to transfer
o Whenever possible, always ask the patient—at o ―This happened to me when I was in college, second year
admission, during your pre-operative check and just or first year I guess, when I had my appendectomy. They
before the procedure—what procedure they are having didn‟t let me void prior to surgery, before putting my
and where spinal anesthesia. After the surgery, there were no
“Tanungin mo siya pasyente. Kahit sabihin niyang, eto sensations below my umbilicus. Well, I can move my feet
oh, nakasulat sa, let‟s say band ko. You have to ask to but I don‟t have control. I can feel my bladder about to
confirm. It might sound corny, alam mo naman mga burst to the point na I wanna sceam „Will somebody
Agatep. Detera. Doong. Rodriguez. Tejano. Villacorta Page 2 of 10
Patient Safety, Errors & Complications
please get me a foley catheter!‟ That bad! Because Difficult airway or aspiration risk?
someone didn‟t let me void prior to surgery. And then □ No
they‟re putting a lot of fluid to me, kasi when you‟re □ Yes, and equipment / assistance available
operating they‟re resuscitating you eh. So lahat yan, nasa Risk of >500 ml blood loss (7ml/kg in children)?
bladder ko. I was hold onto my capacity. So now, I‟m □ No
very aware of that to my patients. □ Yes, and two IVs / central access an fluids
PreOp meds planned
Side rails after PreOp
Contact lens out
Dentures/Bridges out 2. Before skin incision
o One time, the patient was not asked to remove her (With nurse, anaesthetist and surgeon)
dentures. And when they inserted the laryngoscope, the □ Confirm all team members have introduced
dentures were dislodged. The patient swallowed it. So the themselves by name and role.
team had to do surgery in the esophagus because of that □ Confirm the patient‘s name, procedure, and where
foreign body the incision will be made.
Nail polish removed Has the antibiotic prophylaxis been given within the last
o Bakit bawal? Kasi nangingitim ka na, hindi pa nakikita 60 minutes?
because you‟re wearing black nail polish. So tinatanggal □ Yes
yan prior to surgery □ Not applicable
Vitals within 4 hours of surgery or 30 minutes after PreOp Anticipated critical events
PreOp labwork on chart To surgeon:
Abnormal lab values □ What are the critical or non-routine steps?
o Always tell the surgeon. Kahit sa tingin mo insignificant □ How long will the case take?
lang naman, tell it pa rin. □ What is the anticipated blood loss?
Skin prep
Hx of Aspirin, Antidepressant, Steroid, NSAID‘s To anaesthetist:
□ Are there any patient-specific concerns?
WORLD HEALTH ORGANIZATION (WHO)
Developed a comprehensive perioperative checklist as a To nursing team:
primary intervention of the "Safe Surgery Saves Lives" □ Has sterility (including indicator results) been
program—an effort to reduce surgical deaths across the confirmed?
globe □ Are there equipment issues or any concerns?
WHO checklist includes Is essential imaging displayed?
o prompts to ensure that infection prevention measures □ Yes
followed □ Not applicable
o potential airway complications are precluded
e.g., anesthesia has necessary equipment and
3. Before patient leaves operating room
assistance for a patient with a difficult airway
(With nurse, anaesthetist and surgeon)
o groundwork for effective surgical teamwork is
Nurse verbally confirms:
established
□ The name of the procedure
e.g., proper introductions of all OR personnel
□ Completion of instrument, sponge and needle counts
o Aspects of the Joint Commission's preprocedure
□ Specimen labeling (read specimen labels aloud,
"Universal Protocol" (or "time-out") also are included in
including patient name)
the checklist
□ Whether there are any equipment problems to be
e.g., checks to ensure operation performed on
addressed
correct patient and correct site
o The circulating nurse counts how many instruments were
given and were used. She counts how many OS
SURGICAL SAFETY CHECKLIST: Universal Protocol (operating sponge) were given. Dati, eto yung ginagawa.
developed by WHO Example, the nurse gave you 5 OS. Eh you need more 5
OS then wala yung circulating nurse. So you ask the
1. Before induction of anesthesia intern or clerk to get 5 more OS. He/she‟s supposed to
(With at least nurse and anesthetist) tell it to the circulating nursekung ilan yung dinagdag.
Has the patient confirmed his/her identity, site, Bakit? Kapag kasi after the surgery, 9 ang bilang ng
procedure, and consent? nurse sa OS, eh 10 yung binigay at ginamit. Nasan na
□ Yes yung isa? So hanap sila ulit. They will open again the
Is the site marked? abdomen to search for the missing OS. Pero ngayon, the
□ Yes better hospitals, the tertiary hospitals use OS that are
□ Not applicable radilogic. They have this tag, usually blue or orange na
Is the anesthesia machine and medication check pag nag-xray, makikita, hence, alam agad na nasa loob
complete? ng patient yung OS.
□ Yes To surgeon, Anaesthetis and Nurse
Is the pulse oximeter on the patient and functioning? □ What are the key concerns for recovery and
□ Yes management of this patient?
Does the patient have a:
Known allergy?
□ No
□ Yes
Agatep. Detera. Doong. Rodriguez. Tejano. Villacorta Page 3 of 10
Patient Safety, Errors & Complications
Prophylactic antibiotics discontinued within 24 hrs after
surgery end time (48 hrs for cardiac patients)
Cardiac surgery patients with controlled 6 A.M.
postoperative serum glucose
Surgery patients with appropriate hair removal
Colorectal surgery patients with immediate postoperative
normothermia
VENOUS THROMBOEMBOLISM
Surgery patients with recommended venous
thromboembolism prophylaxis ordered
Surgery patients who received appropriate venous
thromboembolism prophylaxis within 24 hrs before surgery
to 24 hrs after surgery
CARDIAC EVENTS
Incidence of identification errors observed per 1000 Surgery patients on a beta blocker prior to arrival who
specimens (n = 21,351). received a beta blocker during the perioperative period
AGENCY FOR HEALTHCARE RESEARCH AND QUALITY PROPOSED OUTCOME MEASURES
PATIENT SAFETY INDICATORS
INFECTION
PROVIDER-LEVEL PATIENT SAFETY INDICATORS Postoperative wound infection diagnosed during index
Complications of anesthesia hospitalization
Death in low mortality diagnosis-related groups
Decubitus ulcer VENOUS THROMBOEMBOLISM
Failure to rescue Intra- or postoperative pulmonary embolism diagnosed
Foreign body left in during procedure during index hospitalization and within 30 days of surgery
Iatrogenic pneumothorax Intra- and postoperative deep vein thrombosis diagnosed
Selected infections due to medical care during index hospitalization and within 30 days of surgery
Postoperative hip fracture
Postoperative hemorrhage or hematoma CARDIAC EVENTS
Postoperative physiologic and metabolic derangements Intra- or postoperative acute myocardial infarction
Postoperative respiratory failure diagnosed during index hospitalization and within 30 days
Postoperative PE or DVT of surgery
Postoperative sepsis
Postoperative wound dehiscence in abdominopelvic surgical
GLOBAL MEASURES
patients
Accidental puncture and laceration Mortality within 30 days of surgery
Transfusion reaction Readmission within 30 days of surgery
Birth trauma – injury to neonate If the patient dies within one month after surgery, that‟s
Obstetric trauma – vaginal delivery with instrument still your mortality. The cause, regardless, is still your
Obstetric trauma – vaginal delivery without instrument surgery.
Obstetric trauma – cesarean delivery
NATIONAL QUALITY FORUM
AREA-LEVEL PATIENT SAFETY INDICATORS NEVER EVENTS
Foreign body left in during procedure Errors in medical care that are clearly:
Iatrogenic pneumothorax o Identifiable
Selected infections due to medical care o Preventable
Postoperative wound dehiscence in abdominopelvic surgical o Serious in their consequences for patients
patients Indicate a real problem in the safety and credibility of a
Accidental puncture and laceration health care facility
Transfusion reaction
Postoperative hemorrhage or hematoma SURGICAL NEVER EVENTS
Surgery performed on the wrong body part
THE SURGICAL CARE IMPROVEMENT PROJECT Surgery performed on the wrong patient
MEASURES Wrong surgical procedure performed in a patient
Unintended retention of a foreign object in a patient aftery
PROCESS OF PERFORMANCE MEASURES surgery or other procedure
Intraoperative or immediately postoperative death in an
ASA Class I patient (normaly healthy individual. Review the
INFECTION ASA Class in Trans 2.5. :D)
Prophylactic antibiotic received within 1 hr before
surgical incision
Prophylactic antibiotic selection for surgical patients
Agatep. Detera. Doong. Rodriguez. Tejano. Villacorta Page 4 of 10
Patient Safety, Errors & Complications
RETAINED SURGICAL ITEM • Central venous catheters should be exchanged only for
Refers to any surgical item that is found to be inside a specific indications (not as a matter of routine) and should
patient after he or she has left the OR requiring a second be removed as soon as possible.
operation to remove the item
Estimates of retained foreign bodies in surgical procedures
1/8,000 to 18,000 operations, or approximately 1,500
cases per year in the US
RISK FACTORS FOR RETAINED SURGICAL SPONGE
Emergency surgery
Unplanned changes in procedure
Patient with higher body-mass index
Multiple surgeons involved in same operation
Multiple procedures performed in same patient CENTRAL VENOUS CATHETER COMMON
Involvement of multiple operating room nurses / staff COMPLICATIONS
members Pneumothorax
Case duration covers multiple nursing ―shifts‖ o Occurrence 1 to 6%
o higher among the inexperienced operators
WRONG SITE SURGERY o stable, pneumothorax is small (<15%) observation
Any surgical procedure performed in the: may be adequate
o Wrong patient Arrhythmias
o Wrong body part Arterial Puncture
o Wrong side of the body o Carotid artery may be punctured
o Wrong level of a correctly identified anatomic site Lost Guidewire
Air Embolus >50ml
BEST PRACTICES FOR OPERATING ROOM SAFETY Pulmonary Artery Rupture
Conduct the Joint Commission Universal Protocol (―time- o ("Swan-Ganz") catheters
out‖) to prevent wront-site surgery pulmonary artery rupture due to excessive
Perform an operating room briefing (checklist) to identify advancement of the catheter into the pulmonary
and mitigate hazards early circulation
Promote a culture of speaking up about safety concerns o sentinel bleed noted when a PA catheter balloon is
Use a screening x-ray to detect foreign bodies in high-risk inflated
cases o uncontrolled hemoptysis
Benign patient sign-outs with the most likely immediate o Treatment :
safety hazard Re-inflation of the catheter balloon,
immediate airway intubation with mechanical
COMMON CAUSES OF LAWSUITS IN SURGERY
ventilation, urgent portable chest x-ray,
Positional nerve injury notification of the OR that an emergent
Common bile duct injury thoracotomy may be required.
Failure to diagnose or delayed diagnosis Central Venous Line Infection (CDC)
Failure to treat, delayed treatment, or wrong treatment o 12 to 25% mortality rate when a central venous line
Inadequate documentation infection becomes systemic
Inappropriate surgical indication o 15% of hospitalized patients will acquire central venous
Failure to call a specialist line sepsis.
Cases resulting in amputation / limb loss o once an infection is recognized as central line sepsis,
removing the line is adequate
COMPLICATIONS
o If your patient is having chiils, suspect already a
Individual errors catheter infection. Do culture na.
Cause minor or major complications during or after a o Staphylococcus aureus infections present a unique
surgical procedure problem due to its potential for metastatic seeding of
May not be publicized as much as wrong-site surgery or a bacterial emboli
retained surgical item o Treatment: 4 to 6 weeks antibiotic therapy
Can still lead to surgical complications that prolong the
course of illness, lengthen hospital stay, increase morbidity
ARTERIAL LINES
and mortality rates
Sa A-line, maglalagay ka ng probe, and this actually
measures second-by-second systolic and diastolic pressure.
COMPLICATIONS IN MINOR PROCEDURES
CENTRAL VENOUS CATHETERS
Steps to decrease complications include the following:
• Ensure that central venous access is indicated
• Experienced (credentialed) personnel should insert the
catheter, or should supervise the insertion.
• Use proper positioning and sterile technique.
Agatep. Detera. Doong. Rodriguez. Tejano. Villacorta Page 5 of 10
Patient Safety, Errors & Complications
ARTERIAL LINES COMPLICATIONS
Thrombosis
o AKA embolization of an extremity can result in the
loss of a digit, hand, or foot,
o Risk is nearly the same for both femoral and radial
cannulation.
o Treatment:
anticoagulation,
surgical intervention required to re-establish
adequate inflow
Bleeding
Hematoma
Arterial Spasm (nonthrombotic pulselessness)
Infection
The problem with stiff catheter (Seldinger technique), if you
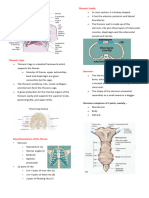
TRACHEOSTOMY hit it low, you might hit the bladder and may give you false
positive. When you hit it high, you might hit the stomach and
TRACHEO-INNOMINATE ARTERY FISTULA (TIAF) give you falce positive result as well. Dapat yan periumbilicus.
occurs rarely (~0.3%)
50 - 80% mortality rate ORGAN SYSTEM COMPLICATIONS
can occur as early as 2 days and as late as 2 mos. after
tracheostomy NEUROLOGIC SYSTEM
Neurapraxia
o improper positioning and/or padding during operations
o Treatment
clinical observation
spontaneous resolution 1 - 3 months
Direct injury to nerves during a surgical intervention:
NERVE SURGICAL INTERVENTION
facial nerve superficial parotidectomy
hypoglossal carotid endarterectomy
nerve
Prostatectomy
nervi erigentes
erectile impotence when injured
inguinal herniorrhaphy
THORACOSTOMY chronic groin pain at 6 months
ilioinguinal nerve groin numbness
postoperative sensory loss at the
groin region
DIAGNOSTIC PERITONEAL LAVAGE
Nasogastric and bladder catheter decompression is
mandatory before DPL to avoid injury during the procedure
The small or large bowel, or the major vessels of the The nerve injury
retroperitoneum also can be punctured inadvertently, and o stretch injury
these injuries require surgical exploration and repair o an unintentionally severed nerve
Consequence:
o loss of function
o severed nerves - painful neuroma that may require
subsequent surgery
Agatep. Detera. Doong. Rodriguez. Tejano. Villacorta Page 6 of 10
Patient Safety, Errors & Complications
EYES, EARS, NOSE RESPIRATORY SYSTEM
Corneal abrasions Pulmonary Atelectasis
o inadequate protection of the eyes during anesthesia o loss of functional residual capacity (FRC)
Conjunctivitis o can predispose to pneumonia
o overlooked contact lenses in a trauma patient o poor pain control in the postoperative period
contributes to poor inspiratory effort and collapse of
the lower lobes in particular
o Treatment:
increase in FRC by ≥ 700 mL
accomplished by sitting patients up >45°
mechanically ventilated patients, simply placing
the head of the bed at 30 to 45° elevation
improves pulmonary outcomes
Inclusion Criteria for Acute Respiratory Distress
Syndrome (ARDS)
Acute onset
Predisposing condition
PaO2:FiO2 < 200 (regardless of positive end-expiratory
Persistent epistaxis pressure)
o NGT placement or removal, Bilateral infiltrates
o Treatment: Pulmonary artery occlusion pressure < 18 mmHg
nasal packing No clinical evidence of right heart failure
persistent direct pressure on external nares
CARDIAC SYSTEM
Atrial fibrillation
o most common arrhythmia
o occurs between 3-5 postoperative day high-risk
patients
o when patients begin to mobilize their interstitial fluid
into the vascular fluid space
o rate control more important than rhythm control
o First-line treatment: beta blockade and/or calcium
channel blockade
MUSCULOSKELETAL SYSTEM
Decubitus ulcers
o preventable complications of prolonged bedrest due to
VASCULAR PROBLEMS OF THE NECK traumatic paralysis, dementia, chemical paralysis, or
Carotid Sinus coma
o baroreceptors maintains blood pressure innervated by o ischemic changes in the microcirculation of the skin can
the Sinus nerve of Herring, branch of glossopharyngeal be significant after 2 hours of sustained pressure
nerve (IX)
Carotid Body Turning schedule
o small cluster of chemoreceptors at the bifurcation of
the CA
o detects changes in partial pressure of O2 & CO2
o sensitive to changes in pH and Temp
Carotid Endarterectomy
o Complications:
central or regional neurologic deficits
bleeding with an expanding neck hematoma
Agatep. Detera. Doong. Rodriguez. Tejano. Villacorta Page 7 of 10
Patient Safety, Errors & Complications
Pressure Ulcer Prevention Guide RATE OF VIRAL TRANSMISSION IN BLOOD PRODUCT
TRANSFUSIONS
HIV 1:1.9 million
HBV 1: 137,000
HCV 1: 1 million
Note that bacterial transmission is 50 to 250 times higher
than viral transmission per transfusion
WOUNDS, DRAIN AND INFECTION
WOUND (SURGICAL SITE) INFECTION
General trend toward providing a single preoperative
dose, as antibiotic prophylaxis may not impart any benefit
at all beyond the initial dosing
Irrigation of the operative field and the surgical wound with
saline solution has shown benefit in controlling wound
inoculum
Irrigation with an antibiotic-based solution has not
demonstrated significant benefit in controlling postoperative
infection
70% isopropyl alcohol:
o best bactericidal effect
o flammable
o hazardous when electrocautery used
chlorhexidine gluconate +isopropyl alcohol,
povidone-iodine, iodophor with alcohol
o more advantageous
WOUND (SOFT TISSUE) INFECTION
>105 CFU per gram of tissue
warrants expeditious & proper antibiotic/antifungal
treatment
clinical signs raise enough suspicion that the patient is
treated before a confirmatory culture is undertaken.
clinical signs of wound infection include rubor, tumor,
calor, and dolor (redness, swelling, heat, and pain),
most definitive treatment: remains open drainage
HEMATOLOGIC SYSTEM
The transfusion guideline
o maintaining the hematocrit level in all patients >30% is
NO longer valid
Only those patients who requires increased oxygen-carrying DRAIN MANAGEMENT
capacity to adequately perfuse end organs, requires higher Four Indications for applying a surgical drain are:
levels of hemoglobin: To collapse surgical dead space in areas of redundant
o symptomatic anemia tissue (e.g., neck and axilla)
o significant cardiac disease To provide focused drainage of an abscess or grossly
o critically ill patient infected surgical site
Other than those select patients, the decision to transfuse To provide early warning notice of a surgical leak (either
should generally not occur until the hemoglobin level bowel contents, secretions, urine, air, or blood)—the so-
reaches 7 mg/dL or hematocrit reaches 21% called sentinel drain
To control an established fistula leak
Agatep. Detera. Doong. Rodriguez. Tejano. Villacorta Page 8 of 10
Patient Safety, Errors & Complications
Treatment
o surgical emergency
o wide débridement of the necrotic tissue to the level of
bleeding, viable tissue
SYSTEMIC INFLAMMATORY RESPONSE SYNDROME,
SEPSIS, AND MULTI-ORGAN DYSFUNCTION SYNDROME
SIRS
result of proinflammatory cytokines related to tissue
malperfusion or injury
dominant cytokines
o interleukin-1,
o interleukin-6,
o tissue necrosis factor (TNF).
other mediators include
o nitric oxide
URINARY CATHETERS
o inducible macrophage-type nitric oxide
catheter be inserted its full length up to the hub o synthase
urine flow established before balloon inflated o prostaglandin I2
misplacement of the catheter in the urethra with premature
inflation of the balloon can lead to tears and disruption of INCLUSION CRITERIA
the urethra
Temperature >38OC or <36OC
Heart rate >90 beats/min
Respiratory rate >20 breathes/min or PaCO2 <32mmHg
White blood cell count of <4000 or >12000 cells/mm3 or
>10%immature forms
Mortality Associated with Patients Exhibiting Two or
More Criteria for SIRS
PROGNOSIS Mortality %
2 SIRS criteria 5
3 SIRS criteria 10
4 SIRS criteria 15-20
SEPSIS
Categorized as
o Sepsis
SIRS + infection
o Severe Sepsis
EMPYEMA sepsis + signs of cellular hypoperfusion or end-
(Gr. en, within + pyon, pus) organ dysfunction
infection of the pleural space (pyothrax) o Septic Shock
Etiology: sepsis associated with hypotension after adequate
o overwhelming pneumonia fluid resuscitation
o retained hemothorax,
o systemic sepsis, MULTIPLE-ORGAN DYSFUNCTION DYSNDROME (MODS)
o esophageal perforation from any cause, infections with culmination of septic shock and multiple end-organ failure
a predilection for the lung (e.g., tuberculosis)
SIRS/MODS
ABDOMINAL ABCESS Management
vague complaints intermittent abdominal pain o aggressive global resuscitation
fever o support of end-organ perfusion,
leukocytosis o correction of the inciting etiology,
change in bowel habits o control of infectious complications,
o management of iatrogenic complications
*CT scan usually required. When a fluid collection within the Adjuncts for supportive therapy
peritoneal cavity is found on CT scan, treatment options are o tight glucose control
antibiotics and percutaneous drainage of the collection. o low tidal volumes in ARDS
o vasopressin in septic shock
NECROTIZING FASCITIS o steroid replacement therapy
fulminant soft tissue infection
30 to 70% mortality GLYCEMIC CONTROL
o Group A streptococcal (M types 1, 3, 12, and 28) 50% reduction in mortality in the critical care setting
o Clostridium perfringens serum glucose was maintained between 80 and 110 mg/dL
o C. septicum with insulin infusion
Agatep. Detera. Doong. Rodriguez. Tejano. Villacorta Page 9 of 10
Patient Safety, Errors & Complications
Secondary findings included Pulmonary embolism
o an improvement in overall morbidity, Adrenal insufficiency
o decreased percentage of ventilator days, less renal Malignant Hyperthermia
impairment, o exposure to agents
o lower incidence of bloodstream infections succinylcholine
halothane-based inhalational anesthetics
PROBLEMS WITH THERMOREGULATION o Symptoms:
dramatic
HYPOTHERMIA with rapid onset of increased temperature
Core Temperature <35°C (95°F), rigors
myoglobinuria related to myonecrosis
Mild [35 to 32°C, (95 to 89.6°F)]
o Treatment:
Moderate [32 to 28°C (89.6 to 82.4°F)]
Medications must be discontinued immediately
Severe [<28°C, (<82.4°F)]
Dantrolene (2.5 mg/kg every 5 minutes) until
Shivering symptoms subside.
o body's attempt to reverse effects of hypothermia, Aggressive cooling methods
occurs 37 - 31°C (98.6 and 87.8°F) alcohol bath
o ceases at <31°C (87.8°F) packing in ice
Triad Severe Malignant Hyperthermia
o metabolic acidosis o mortality rate is nearly 30%
o coagulopathy Patients who are moderately hypothermic are at higher risk
o hypothermia for complications than are those who are more profoundly
commonly found in long operative cases patients hypothermic
with blood dyscrasias
The enzymes that contribute to the clotting cascade and ISSUES IN CARING FOR OBESE PATIENTS & PATIENTS
platelet activity are most efficient at normal body AT THE EXTREMES OF AGE
temperatures;
Surgery with multiple risks
therefore all measures must be used to reduce heat loss
Important to optimize prior to surgery
intraoperatively
Preoperatively:
Arrhythmia
o dietary modifications
o most common cardiac abnormality when body
o exercise
temperature drops below 35°C
o pulmonary toilet issues
Bradycardia
Obese Conditions
o occurs with temperatures below 30°C
o eccentric left ventricular hypertrophy,
Hypothermia may induce CO2 retention resulting in
o right ventricular hypertrophy
respiratory acidosis
o congestive heart failure.
Renal dysfunction of hypothermia manifests itself as a
o significant sleep apnea
paradoxic polyuria, related to an increased GFR,
o gastroesophageal reflux disease
potentially perplexing in patients undergoing resuscitation
o Poor Glycemic control
for hemodynamic instability,
o contributes significantly to infection & DM
brisk urine output provides a false sense of an adequate
o decrease in antithrombin III levels,
intravascular fluid volume
o higher risk of DVT and PE
Methods used to warm patients include
Measures to optimize physiologic function:
o warm air circulation over the patient,
o keep head of the bed elevated at all times.
o heated IV fluids,
can improve FRC by almost 1 liter
More Aggressive Measures
↓ atelectasis and pneumonia complications
o bilateral chest tubes with warm solution
o Proper glycemic control
o lavage
tight insulin sliding scale
o intraperitoneal rewarming lavage
o risk of DVT may be attenuated by
o extracorporeal membrane oxygenation
immediate use of prophylactic LMWH
rate of temperature rise of 2 to 4°C/h considered adequate,
early ambulation
Most common complication for nonbypass rewarming is
Elderly vs Very Young
arrhythmia with ventricular arrest
Elderly Very Young
HYPERTHERMIA End-organ underdeveloped or anomalous
insufficiency organ function
Immune response Immune response compromised
Common Causes Of Elevated Temperature In Surgical
compromised
Patients
may not be capable resolve fevers overnight, and
HYPERTHERMIA HYPERPYREXIA
of mounting a febrile the cause may remain
Environmental Sepsis
response undiagnosed
Malignant hyperthermia Infection
Extremes of Ages
Neuroleptic malignant syndrome Drug reaction
o other alterations in these groups include:
Thyrotoxicosis Transfusion reaction amount and distribution of
Pheochromocytoma Collagen disorder – total body water
Carcinoid syndrome Factitious syndrome – total body fat
Iatrogenic Neoplastic disorder o communication
Central/ hypothalamic response o involvement of family members
Agatep. Detera. Doong. Rodriguez. Tejano. Villacorta Page 10 of 10
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5825)
- FULL Download Ebook PDF International Trauma Life Support For Emergency Care Providers 9th Edition PDF EbookDocument51 pagesFULL Download Ebook PDF International Trauma Life Support For Emergency Care Providers 9th Edition PDF Ebookcarl.helbling11891% (53)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1093)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (852)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (903)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (541)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (349)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (823)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (403)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- CODE of Construction Safety PracticeDocument291 pagesCODE of Construction Safety PracticeBala Praveen97% (119)
- A. Bron, R. Tripathi, B. Tripathi - Wolff's Anatomy of The Eye and Orbit-CRC Press (1998) PDFDocument724 pagesA. Bron, R. Tripathi, B. Tripathi - Wolff's Anatomy of The Eye and Orbit-CRC Press (1998) PDFPS NI100% (1)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- 4.4 Acute AbdomenDocument6 pages4.4 Acute AbdomenMiguel C. Dolot100% (1)
- Dr:Khalid MiladDocument27 pagesDr:Khalid MiladMohsen Elzobna0% (1)
- 4.2 Abdominal Wall Hernia (Jerome Villacorta's Conflicted Copy 2014-03-22)Document7 pages4.2 Abdominal Wall Hernia (Jerome Villacorta's Conflicted Copy 2014-03-22)Miguel C. DolotNo ratings yet
- Nucleotide MetabolismDocument17 pagesNucleotide MetabolismMiguel C. DolotNo ratings yet
- 02.03-01 CNS II - General AnesthesiaDocument9 pages02.03-01 CNS II - General AnesthesiaMiguel C. DolotNo ratings yet
- Basic Ocular Surgeries: Fatima Medical Center Dr. Vicente O. Santos JR., MDDocument53 pagesBasic Ocular Surgeries: Fatima Medical Center Dr. Vicente O. Santos JR., MDMiguel C. DolotNo ratings yet
- Diabetes Mellitus 1Document47 pagesDiabetes Mellitus 1Miguel C. DolotNo ratings yet
- 4.3 Peritonitis (Lecture-Based)Document5 pages4.3 Peritonitis (Lecture-Based)Miguel C. DolotNo ratings yet
- Shoulder Dystocia: Ina S. Irabon, MD, Fpogs, FPSRM, FpsgeDocument25 pagesShoulder Dystocia: Ina S. Irabon, MD, Fpogs, FPSRM, FpsgeMiguel C. DolotNo ratings yet
- Cornea and External DiseasesDocument18 pagesCornea and External DiseasesMiguel C. DolotNo ratings yet
- 02.01-04 CNS I - AntiepilepticsDocument10 pages02.01-04 CNS I - AntiepilepticsMiguel C. DolotNo ratings yet
- Basic Neuro-Ophthalmology: Common Problems SeenDocument6 pagesBasic Neuro-Ophthalmology: Common Problems SeenMiguel C. DolotNo ratings yet
- 02.01-03 CNS I - AlcoholsDocument5 pages02.01-03 CNS I - AlcoholsMiguel C. DolotNo ratings yet
- 02.03-03 CNS II - Skeletal Muscle RelaxantsDocument7 pages02.03-03 CNS II - Skeletal Muscle RelaxantsMiguel C. DolotNo ratings yet
- 02.03-02 CNS II - Local AnesthesiaDocument5 pages02.03-02 CNS II - Local AnesthesiaMiguel C. DolotNo ratings yet
- Angeline D. Alabastro, M.D. Angeline D. Alabastro, M.D. Angeline D. Alabastro, M.DDocument7 pagesAngeline D. Alabastro, M.D. Angeline D. Alabastro, M.D. Angeline D. Alabastro, M.DMiguel C. DolotNo ratings yet
- Angeline D. Alabastro, M.D.: CNS Pharmacology I: AntiepilepticsDocument10 pagesAngeline D. Alabastro, M.D.: CNS Pharmacology I: AntiepilepticsMiguel C. DolotNo ratings yet
- 02.05. Patient-Doctor Relationship and Interviewing TechniquesDocument10 pages02.05. Patient-Doctor Relationship and Interviewing TechniquesMiguel C. DolotNo ratings yet
- 02.01-01 CNS I - Central NeurotransmittersDocument3 pages02.01-01 CNS I - Central NeurotransmittersMiguel C. DolotNo ratings yet
- Los Baños: Mental Status ExamDocument5 pagesLos Baños: Mental Status ExamMiguel C. DolotNo ratings yet
- 02.04. Physical Examination and Laboratory Tests in PsychiatryDocument12 pages02.04. Physical Examination and Laboratory Tests in PsychiatryMiguel C. DolotNo ratings yet
- Psychiatric History: Doc Los BañosDocument6 pagesPsychiatric History: Doc Los BañosMiguel C. DolotNo ratings yet
- Qbank FormatDocument5 pagesQbank FormatpashaNo ratings yet
- Brachial Plexus InjuryDocument39 pagesBrachial Plexus InjurymariaNo ratings yet
- Q2-Activity in Science-Bones, Joint, MusclesDocument2 pagesQ2-Activity in Science-Bones, Joint, MusclesMaggie DreuNo ratings yet
- The Bony Thorax Ana - Positioning. ReviewerDocument8 pagesThe Bony Thorax Ana - Positioning. Reviewercorrainnejimenez.24No ratings yet
- Stretching Exercises For Seniors Over 60Document134 pagesStretching Exercises For Seniors Over 60Sal OtNo ratings yet
- Tutorial Report Physiology and Work Measurement BiomechanicsDocument17 pagesTutorial Report Physiology and Work Measurement Biomechanicsalma millaniaNo ratings yet
- Deland 2005Document10 pagesDeland 2005DavidNo ratings yet
- Eor-2058-5241 1 000052Document13 pagesEor-2058-5241 1 000052Alfian PramuditaNo ratings yet
- Pathophysiology of Acute PainDocument12 pagesPathophysiology of Acute PainMuhammad Ghilman NurizzanNo ratings yet
- Biomechanics of TennisDocument7 pagesBiomechanics of Tennismiruna.stanescu12No ratings yet
- Data For Scaffolding JsaDocument8 pagesData For Scaffolding JsaRaza Muhammad SoomroNo ratings yet
- Chapter 3 - Physical Activity FitnessDocument44 pagesChapter 3 - Physical Activity FitnessSharmila KrishnaswamyNo ratings yet
- Article 261-265Document10 pagesArticle 261-265BOBIS, FRIALYN N.No ratings yet
- Accident ReportDocument2 pagesAccident Reportberj.garbouchiansbcglobal.netNo ratings yet
- Hope 2Document11 pagesHope 2Trisha Faye Tabuena PlanaNo ratings yet
- Unit 15Document3 pagesUnit 15Silent againNo ratings yet
- Causes and Investigation of Shock: Learning ObjectivesDocument3 pagesCauses and Investigation of Shock: Learning Objectivesstef lopezNo ratings yet
- USAP Continental Field ManualDocument146 pagesUSAP Continental Field Manualmvelilla12No ratings yet
- WALKING AIDS (Assistive Devices) : College of NursingDocument15 pagesWALKING AIDS (Assistive Devices) : College of NursingJojo JustoNo ratings yet
- MBA Thesis - MuruDocument79 pagesMBA Thesis - Murumurugeswaran.kpNo ratings yet
- Surgery QuestionsDocument19 pagesSurgery QuestionsdocaliNo ratings yet
- Sex Determination From Skeletal Remains - Forensic's BlogDocument10 pagesSex Determination From Skeletal Remains - Forensic's BlogReal AbrasNo ratings yet
- Prentice9e Im Chap18Document6 pagesPrentice9e Im Chap18api-281340024100% (1)
- Laboratory Manual For Anatomy and Physiology 6Th Edition Marieb Solutions Manual Full Chapter PDFDocument28 pagesLaboratory Manual For Anatomy and Physiology 6Th Edition Marieb Solutions Manual Full Chapter PDFJohnathanFitzgeraldnwoa100% (12)
- Forensic MedicineDocument32 pagesForensic Medicineferdosjm74No ratings yet
- BOSH SO2 Manual GovernmentDocument138 pagesBOSH SO2 Manual Governmentjasonrey.saysonNo ratings yet