Professional Documents
Culture Documents
Benson, D. Et Al. (1988) Posterior Cortical Atrophy
Benson, D. Et Al. (1988) Posterior Cortical Atrophy
Uploaded by
Luis GómezCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Benson, D. Et Al. (1988) Posterior Cortical Atrophy
Benson, D. Et Al. (1988) Posterior Cortical Atrophy
Uploaded by
Luis GómezCopyright:
Available Formats
Posterior Cortical Atrophy
D. Frank Benson, MD; R. Jeffrey Davis, DO; Bruce D. Snyder, MD
\s=b\ Five patients had progressive de- case was discovered by one of us (B.D.S.). one three-word sentence to dictation, but
mentia heralded by disorders of higher None had hypertension, diabetes, hyperlip¬ paraphasic substitutions intruded into
visual function. All eventually developed idemia, clinical encephalitis, heavy metal other attempts. Simple calculations were
alexia, agraphia, visual agnosia, and com- exposure, or known medical cause. Prima¬ poor and not aided by paper and pencil.
ponents of Balint's, Gerstmann's, and ry motor and sensory modalities, including Right-left orientation was almost perfect
visual fields, were intact. Causes other for his own body but was otherwise ran¬
transcortical sensory aphasia syndromes.
than a primary degenerative process were dom. His ability to name and recognize
Memory, insight, and judgment were rela- sought. All patients underwent a routine fingers was severely impaired. Registra¬
tively preserved until late in the course. complete blood cell count; thyroid, liver, tion of new information could not be strin¬
Predominant parieto-occipital atrophy and renal function tests; glucose, serum gently assessed because of word-finding
was demonstrated on both computed calcium, and phosphorus determinations; impairment and visual problems, but
tomography and magnetic resonance and determinations of sedimentation rate recall of verbal material was nearly per¬
imaging in two of the patients; posterior and folate and vitamin B12 levels. Twenty- fect if multiple choice responses were pro¬
circulation was normal by angiography in four-hour urine samples were collected to vided. Behaviorally, a considerable degree
the three studied. To date, no pathologic determine the levels of heavy metals and of preserved memory function was indi¬
other toxic substances. All patients under¬ cated by the content of his continued
specimen is available for study; specula- went lumbar punctures. No abnormalities attempts at interpersonal discourse.
tions on the underlying pathologic condi- were demonstrated. Despite language problems, he correctly
tion include an atypical clinical variant of Computed tomography (CT) and mag¬ interpreted similarities, differences, and
Alzheimer's disease, a lobar atrophy anal- netic resonance imaging (MRI) were per¬ proverbs. He easily performed verbally
ogous to Pick's disease, or some previ- formed in all patients, and three under¬ commanded praxis tasks unless visual
ously unrecognized entity. went angiography of the carotid and verte¬ mediation to an outside object was
(Arch Neurol 1988;45:789-793) brobasilar systems (Table 1). An electroen¬ required. For instance, he easily oriented
cephalogram (EEG) was performed on all the telephone receiver to his ear but could
patients and a full battery of neuropsycho¬ not replace the receiver on the hook. He
Pouring evaluation of large popula¬
a logical tests supplemented clinical exami¬ could not copy, trace, or perform line orien¬
tion of patients with dementia, a nation in the three patients who were tation tasks. He drew a circle, square, and
few individuals with slowly progres¬ testable. triangle on command, but the productions
sive deterioration stood out because of were poor and he failed more complex
REPORT OF CASES
early visual dysfunction. Despite dis¬ figures, su&h as a bicycle. He competently
abling visual problems, both visual
Case 1.—A 64-year-old former bank tapped out rhythms and performed recip¬
executive presented with episodes of anxi¬ rocal rhythm tasks.
acuity and visual fields remained ety that complicated a slowly progressive The only problem noted on basic neuro¬
intact until late when unilateral qua¬ disturbance of vision and language. About logic examination was an inconsistent and
drante visual extinction could be eight years earlier, he had noted difficulty questionable diminution of visual acuity in
demonstrated. Agnosia, alexia, anom¬ reading; he remained at his job, but his the right lower quadrant, best demon¬
ia, Balint's syndrome (sticky fixation, secretary had to read for him. Although strated by double-simultaneous stimula¬
ocular dysmetria, and simultanagno- still able to write, he could not read what tion. He accurately counted fingers at 45
sia), Gerstmann's syndrome (right- he produced. Eventually, he also lost the cm, but was slow and uncertain. There was
left disorientation, finger agnosia, ability to write and had difficulty finding neither paresis nor alteration of sensation.
his way in familiar areas (environmental He walked as though blind but could navi¬
acalculia, and agraphia), and trans- agnosia) and in performing visually medi¬ gate the room without colliding into any¬
cortical sensory aphasia eventually ated tasks. The problems slowly pro¬ thing. When offered a chair, he had diffi¬
developed. Memory, insight into their gressed; he stated that what he saw disap¬ culty finding it and when he did, sat on the
problems, and motivation to improve peared before he could sense what it was. arm before correctly seating himself.
themselves were preserved until late Progressive worsening of his expressive A strong tendency to fix his gaze on a
in the course. ability was observed, though his family single object (sticky fixation) was present.
remained convinced that he understood Full lateral and vertical gaze were possible
PATIENT SELECTION AND EVALUATION what was said. if he followed a moving object, but jerky,
Four patients from neurologic and psy¬ On examination, he was alert, oriented, hypometric saccades and tendency to over¬
chiatric clinics at UCLA were noted to attentive, and in reasonably good physical shoot were noted. When asked to touch a
have a history of slowly progressive health. His manner was gracious and his stationary object held in front of him, he
dementing illness, with the most promi¬ insight was painfully apparent. Conversa¬ initially missed by 7.5 or 10 cm (ocular
nent cognitive and functional deficits tional speech was hesitant, with word- dysmetria). With repeated attempts, his
referable to visual processing. A similar finding pauses and occasional semantic performance improved but remained
and verbal paraphasic substitutions. Artic¬ uncertain. He routinely failed to find all
ulation and prosody were intact and he objects in an array (simultanagnosia).
Accepted for publication Feb 15, 1988. readily repeated and comprehended simple Meaningful neuropsychological testing
From the Department of Neurology, UCLA sentences; with complex or abstract could not be performed because of the
School of Medicine; and the Neurobehavior Unit, descriptions of objects or actions, however, severe impairment present at the time of
West Los Angeles Veterans Administration Med- comprehension became faulty. Confronta¬ the initial visit. Computed tomography
ical Center (Brentwood Division) (Drs Benson tion naming was markedly impaired but and MRI of the head revealed bilaterally
and Davis); and the Department of Neurology, St
Paul-Ramsey Medical Center, St Paul, Minn (Dr improved with palpation of the object. symmetrical atrophy, most prominent in
When offered multiple choices, he selected the parieto-occipital region, with enlarge¬
Snyder).
Reprint requests to UCLA Department of Neu- the names of colors better than objects or ment of both the ventricles and the cortical
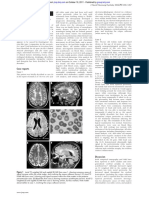
rology, 710 Westwood Plaza, Los Angeles, CA simple shapes. He could not read words, sulci (Fig 1). An EEG showed a generalized
90024-1769 (Dr Benson). letters, or numbers. He wrote his name and 6- to 7-Hz pattern without evidence of focal
Downloaded From: http://archneur.jamanetwork.com/ by a DALHOUSIE UNIVERSITY-DAL-11762 User on 05/18/2015
dysfunction.
Case 2.—A 59-year-old bookkeeper
sought help for "increasing memory diffi¬
culty" but presented his own history with
only minimal additions from family mem¬
bers. His problem had surfaced the previ¬
ous year with progressive difficulty in fol¬
lowing a line of print. Problems in calcula¬
tion, even in keeping the family checkbook,
developed and he became lost while driving
in his community. He was unable to main¬
tain his job.
Mental status examination demon¬
strated an alert man with a digit span of
six and an intact memory for the chronolo¬
gy of his symptoms and for general infor¬
mation concerning both remote and cur¬
rent events. Comprehension and repetition
of spoken language were normal. Confron¬
tation naming of high-frequency items was
intact, but less common items were missed. Fig 1.—Magnetic resonance imaging scan (case 1) demonstrating ventricular enlargement,
Both reading and writing were limited to particularly of occipital horns, and cortical atrophy, most pronounced in parieto-occipital
simple statements (eg, "The weather is areas.
nice"). Calculations were totally failed.
Right-left orientation was poor, but finger
identification was adequate. Neurologic Table 1.—Patient Data*
examination revealed no focal abnormali¬
ty; visual acuity was normal, visual fields Patients
were full to confrontation, and the extra¬
ocular movements were intact.
Over the next three years, his mental age of onset, y 56 54 67 53
Approximate
state progressively deteriorated. Although Duration of disorder, y
able to feed himself, he could not identify Anomia
the food until it was in his mouth. Similar¬ Alexia
ly, although able to dress himself, he Memory impairment
needed guidance and encouragement. Sim¬ Gerstmann's syndrome
ple tasks, such as opening a jar or using a Agraphia_
tool such as a hammer or screwdriver,
Acalculia
became impossible. He developed total
Finger agnosia
alexia, agraphia, and acalculia plus com¬ R-L disorientation
plete right-left disorientation and finger
agnosia (Gerstmann's syndrome). The Balint's syndrome
aphasia worsened considerably, particu¬ Sticky fixation
larly naming, which was almost totally Ocular dysmetria
failed. Some difficulty with language com¬ Simultanagnosia
prehension developed, but he still repeated Visual field extinction RLQ RHH LLQ LLQ
well. A full Balint's syndrome could be Environmental agnosia
demonstrated. Emotional symptoms
Neuropsychological testing on two occa¬ Full scale IQ NT 83
sions early in the course demonstrated a Verbal IQ NT 91 85 NT
depressed full scale IQ, with a significant Performance IQ NT 63 63 NT 44
difference between verbal (VIQ) and per¬
Wechsler memory quotient NT Impairedt 59 NT 79
formance (PIQ) subscores (VIQ 91; =
Computed tomography PA GA NEG PA
PIQ 63). Serial EEGs consistently dem¬
=
NEG
onstrated slow (6- to 7-Hz) background Magnetic resonance imaging scan PA GA PA PA
without focal abnormalities. Repeated CT Angiography NL NL NL
scans and a single MRI scan showed only a Electroencephalography SL SL SL SL SL
mild, progressive atrophy. *NT indicates not testable; GA, generalized atrophy: PA, posterior atrophy: SL, slow; NL, normal: ?, not
Case 3.—A 57-year-old woman com¬
reported; +, present; ±, mild; —, absent; RLQ, right lower quadrant; RHH, right homonymous hemianopsia;
plained of slowly progressive difficulty LLQ, left lower quadrant; NEG, negative.
with vision. Three changes of glasses over tNumbers not given in report and raw data subsequently lost.
a 2!/2-year period had not helped. She could
not drive, had difficulty reading, and com¬
plained of forgetting where she had placed "thread" used to sew a button). She could cal tests was most remarkable for its dem¬
her belongings. comprehend written material only at the onstration of visually oriented impair¬
Examination revealed a healthy individ¬ level of a three- or four-word sentence. ments reflected in a 22-point difference in
ual without basic medical or neurologic Writingwas severely impaired; only her the VIQ and PIQ subscores. A CT scan was
difficulty. There was no paresis, sensory own name was correctly spelled. She easily read as normal, but EEGs were abnormal,
loss, or visual field disturbance, and learned and retained new verbal informa¬ with generalized slowing and disorganized
extraocular movements were intact. She tion and retrieved information from the background frequencies.
was alert but not fully oriented. Verbal past. She was almost totally unable to Evaluation at several additional diag¬
output was fluent but empty, with circum¬ calculate. Right and left were discrimi¬ nostic centers with repeated laboratory
locutions and occasional paraphasic sub¬ nated with fair accuracy, but mistakes of tests produced similar results. Five and
stitutions. Comprehension and repetition finger identification were consistently not¬ one-half years following the original
were normal. On confrontation naming, ed. She could not copy drawings, except for examination, she was reevaluated. She now
she had difficulty with low-frequency a circle. acted as though blind and had to be led.
words (eg, the "bridge" of her glasses, the A complete battery of neuropsychologi- Visual acuity was normal, however, and
Downloaded From: http://archneur.jamanetwork.com/ by a DALHOUSIE UNIVERSITY-DAL-11762 User on 05/18/2015
visual fields were full to confrontation
testing although an inconsistent right
visual extinction was noted. Her eyes
moved in all directions when following a
finger, but hypometric saccades were
prominent. Neither paresis nor primary
sensory loss was evident. She was now
severely aphasie with a fluent, anomic
output, significantly disturbed comprehen¬
sion, almost total inability to name on
confrontation, and total alexia and
agraphia but intact repetition of spoken
language (transcortical sensory aphasia).
The severity of the mental deterioration
made neuropsychological testing impossi¬
ble. Gerstmann's syndrome and a full Bal¬
int's syndrome were present. Repeated CT
and MRI scans demonstrated atrophy,
greatest in the occipital and parietal
regions bilaterally, without evidence of a
mass lesion or focal lucency (Fig 2). Angi¬
ography showed normal vessels in both (case 4) demonstrating striking enlargement of occipital
anterior and posterior vascular systems. Fig 2.—Computed tomographic scan
The EEG remained generally slow. Despite horns bilaterally.
marked disability, she retained consider¬
able insight, frequently manifested by cry¬
ing and despondency concerning her fear although extinction in the left lower quad¬ a detailed description of her problems with
of progressive disability. rant with double simultaneous stimulation only an occasional paraphasic substitution.
Case 4.—A 75-year-old, college-educated was noted late in the course. The advanced Despite intact functional speech, she could
author was evaluated for progressive intel¬ state of deterioration at the time she was write nothing but her name. All visual
lectual impairment of seven years' dura¬ first seen in our clinic precluded meaning¬ tasks were severely impaired, particularly
tion. She first noted that her typing slowed ful neuropsychological testing. A CT scan attempts to integrate a complex visual
and typographical errors increased. Her was considered normal for her age, but an picture into a meaningful whole (simul-
handwriting deteriorated, eventually be¬ EEG showed diffuse slowing. tanagnosia). Spelling aloud was severely
coming illegible. She continued typing a Case 5.—A 54-year-old housewife com¬ impaired. New learning was limited and
novel, which was published, and then plained that "my vision is hazy and fades she could perform only the simplest arith¬
wrote another. Grammatical structure and in and out." Ophthalmologic examination metic.
the general content were satisfactory, but demonstrated normal visual acuity, but After three years, her speech became
the more recent work was not accepted for she noted increasing difficulty in sewing, increasingly circumstantial. She no longer
publication. By then, she also noted diffi¬ playing cards, and in playing the piano. handled money and could not perform seri¬
culty with many daily tasks but remained She found herself uncertain about which al threes. Her neighborhood was now unfa¬
independent. direction to take in her own home and miliar and she became lost if unaccompa¬
On examination, she was alert and became lost in previously familiar sur¬ nied. New learning was profoundly
expressed herself clearly, although some roundings. She could no longer perform the impaired. Although she experienced diffi¬
word-finding pauses and circumlocution simple arithmetic required to balance her culty getting clothing on correctly, she still
were present. Comprehension, though gen¬ checkbook. Despite these difficulties, she attended ballet class for exercise, applied
erally intact, broke down with complex held telephone conversations, entertained her own makeup, and managed some
grammatical constructions. Repetition was guests, performed most household chores, household duties. She remained socially
intact to an extended span length. She planned meals, and attended a dance appropriate and retained insight into the
exhibited a profound confrontation anom¬ class. nature of her problems with no change in
ia, failing even the first few items on the On mental status examination, she was personality or mood.
Boston Naming Test. She appeared unable alert and oriented, articulated clearly, and On examination three years after initial
to recognize objects visually but also had showed good verbal reasoning. She was examination, calculations and right-left
difficulty providing a name when the fluent and repeated and comprehended discrimination were clearly impaired and
item's function was described. Phonemic well. She read aloud, but with difficulty. her ability to find objects in space was
cues did not help. When an object was Knowledge of current events was mildly poor. Visual fields were intact to confron¬
placed in her hand, she could pick its impaired and both registration and tation, but she showed greater difficulty
function from multiple-choice offerings retrieval of verbal and nonverbal material localizing objects in the left visual field,
but could not select the name from several was imperfect. The line bisection task was and fairly consistent extinction to double
choices. Her only writing was a barely performed slowly but correctly and with¬ simultaneous stimulation could be demon¬
legible signature. Memory testing was out omission. She drew a clock but could strated in the left inferior quadrant. Cra¬
complicated by the severe anomia, but not set the specified time. Her copy of a nial nerves were otherwise intact, there
when offered multiple-choice responses cube lacked three-dimensional quality. was no dysarthria or motorimpairment,
concerning current news, she was fully Neurological examination revealed no reflexes were brisk and symmetrical, and
correct, even for obscure details. Calcula¬ abnormalities of the cranial nerves, motor toes were downgoing. Sensation, balance,
tion was profoundly impaired, right-left strength, sensation, or coordination. and coordination testing were unreveal-
orientation was totally disturbed, and she Visual acuity was normal, eye movements ing.
could not differentiate fingers. She failed were full, optokinetic nystagmus was Neuropsychological testing was per¬
to copy even the simplest geometric draw¬ equal, and no visual neglect was demon¬ formed on several occasions, providing
ing and even had difficulty finding the strated with double simultaneous visual supportive data for the observations of far
model on the page. She distinguished stimulation. An EEG demonstrated theta greater visual than verbal disorder. Com¬
between a thick and a thin line but could activity. Computed tomography without puted tomographic scanning showed ven¬
not name or choose a color from multiple and with contrast showed only mild sulcal tricular size to be somewhat larger than
choice. Ocular fixation was intense; visual widening. Neuropsychological testing average for age, particularly in the posteri¬
recognition was so limited that simul- showed a clear discrepancy between VlQ or-superior parietal regions bilaterally. An
tanagnosia could not be tested. No visual and PIQ scores (Table 1). MR scan demonstrated atrophy that was
field defect could be demonstrated Two years later, she could still articulate most pronounced posteriorly. Brain-stem,
Downloaded From: http://archneur.jamanetwork.com/ by a DALHOUSIE UNIVERSITY-DAL-11762 User on 05/18/2015
in thesepatients deserves comment.
Table 2.—Posterior Cortical Atrophy*
Although first described in 1909,2 the
Course Slowly progressive syndrome was rarely reported until
Not stepwise recent years. While still considered
Initial symptoms visual
rare, reviews by Hécaen and Albert3
Clinical findings Visual agnosia, constructional disturbance, environmental agnosia and Damasio4 document a number of
Transcortical sensory aphasia (alexia, agraphia, anomia, and
decreased comprehension but normal repetition) examples and present pertinent theo¬
Gerstmann's syndrome (acalculia, agraphia, R-L disorientation, and ries concerning the underlying mech¬
finger agnosia) anism. Damasio4 stressed obligatory
Balint's syndrome (ocular dysmetria, sticky fixation, and bilateral parieto-occipital abnormali¬
simultanagnosia)
Decreased verbal learning (late) ty, usually with accompanying inferi¬
Normal primary visual, motor, and sensory systems or quadrantanopia, and suggested two
Retention of insight, appropriate affect cortical areas of greatest importance:
Laboratory findings EEG: diffuse slowing in mid to late stages _
(1) Brodmann area 7 of the parietal
WAIS: PIQ 25-30 points lower than VIQ cortex appeared essential for direct¬
CT: posterior > anterior atrophy
MRI scan: posterior > anterior atrophy ing gaze to novel stimuli; (2) the supe¬
rior occipital cortex was thought nec¬
*EEG indicates electroencephalogram; WAIS, Wechsler Adult Intelligence Scale; CT, computed tomogra¬
phy; PIQ, performance IQ; MRI, magnetic resonance imaging; and VIQ, verbal IQ. essary to structure the full visual
field. Hécaen and Albert3 agree with
the observation of a mandatory bilat¬
eral, parieto-occipital pathologic con¬
Table 3.—Differential Diagnosis of Cortical Dementia dition but note the presence of frontal
Posterior
cortex or occipital-frontal pathway
Alzheimer's Pick's lesions in some cases. It has been
Features Disease Disease Cortical Atrophy
Amnesia Early Late Late
posited that a combined parieto-occip-
itofrontal dysfunction underlies the
Constructional disturbance Early Late Early full syndrome.5 All of the neuroana-
Environmental agnosia Early Early tomical areas said to be associated
Acalculia Early Late Early with Balint's syndrome are either
Anomia Early Early Early
association cortex or cortical-cortical
Alexia Moderately late Moderately late Early
Agraphia Moderately late Moderately late Early
connections, not primary visual cortex
or its efferent connections, a feature
Gerstmann's syndrome Moderately late Late Relatively early consistent with the lack of visual field
Balint's syndrome Absent Absent Present
defect in our cases. The three compo¬
Klüver-Bucy syndrome Absent or late Early Absent
nents essential for the diagnosis-
Loss of insight Early Early Late
Behavioral response Unconcerned Disinhibited Appropriately concerned
sticky fixation (also called optic
apraxia, oculomotor apraxia, ocular
apraxia, psychic paralysis of gaze, or
spasm of fixation), ocular dysmetria
visual, and somatosensory evoked re¬ for this dramatic disorder.1 Four (optic ataxia or misreaching), and
sponses were normal. An EEG showed patients developed a full Balint's syn¬ simultanagnosia (visual disorienta¬
intermittent (4- to 6-Hz) slowing superim¬ drome (sticky fixation, ocular dysme¬
posed on a 6- to 8-Hz background.
tion)—were fully present in four cases
tria, and simultanagnosia) and the and only partially present in one
COMMENT fifth showed optic ataxia and ocular (naming and pointing were too severe¬
dysmetria. All eventually developed ly disordered to prove simultanagno¬
Each of the patients showed a pro¬ all four components of Gerstmann's sia). The syndrome was incomplete in
gressive mental deterioration without syndrome (finger agnosia, right-left the early stages (cases 2, 3, and 5) but
evidence of basic motor or sensory disorientation, agraphia, and acalcu¬ developed into the complete clinical
dysfunction. The earliest clinical find¬ lia) and also developed the findings of picture over a course of several years.
ings (eg, alexia or visual agnosia) transcortical sensory aphasia (anom¬ When features of Balint's syndrome
implied visual-association malfunc¬ ia, comprehension disorder, alexia are present, a bilateral parieto-occipi¬
tion. Despite the early presence of and agraphia, and good repetition). As tal pathological condition is implied;
visual disturbances that progressed to an early finding, all had severe the progression into a full syndrome
severe disability, visual acuity re¬ impairment of the ability to copy may indicate additional involvement
mained intact and the only visual- drawings. Memory function was of frontal connections.
field discrepancies were extinction to abnormal but only to a limited degree Computed tomography and MRI
double-simultaneous stimulation and until late in the course. Each could revealed a degenerative process that
hemineglect noted late in the course present his or her own history, was appeared more prominent in the pos¬
of the illness, long after severe visual aware of current events, and showed terior cerebral hemispheres in three
disability was evident. Two showed considerable insight into his or her of the patients. There was no evidence
right- and two left-sided extinction predicament. While use of specific of vascular, neoplastic, or inflamma¬
and in none was it a consistent find¬ names was difficult, true abnormality tory disease. The EEGs of all patients
ing. An early complaint of each in memory function was mild until showed diffuse theta activity without
patient was a tendency to get lost in late in the course. No patient devel¬ focal slowing or epileptiform dis¬
familiar areas, such as an inability to oped a primary motor, auditory, or charge, patterns that resemble those
find their way in their neighborhood somatesthetic disturbance. Table 1 reported in the midstages of both
or difficulty finding their way from outlines the more important clinical Pick's and Alzheimer's disease.6·7 The
room to room in their own home. findings of the cases presented. neuropsychological test results of all
Environmental agnosia is a term used The presence of Balint's syndrome patients who could be tested showed a
Downloaded From: http://archneur.jamanetwork.com/ by a DALHOUSIE UNIVERSITY-DAL-11762 User on 05/18/2015
marked discrepancy between PIQ and posterior cortical atrophy, is suggest¬ the initial cerebral involvement.19 The
VIQ scales, probably reflecting the ed to identify the disorder until more syndrome described here may well
sensitivity of the PIQ subtests to definitive causative data become represent an aberrant onset of a more
visual dysfunction. available. common disorder. Table 3 lists clinical
The findings in these patients fit Several causative considerations findings that appear to distinguish
current definitions of dementia.8·9 The can be suggested. In that the disorder the syndrome reported here from the
constellation of findings suggests dis¬ begins as a progressive derangement two currently recognized types of cor¬
turbance of association cortex or con¬ of the association cortex, it resembles tical dementia.
nections, with sparing of the primary Alzheimer's disease. Differences from Among other causative possibilities
sensory and motor pathways. The ear¬ the typical clinical features of Alz¬ considered in these cases, focal vascu¬
ly clinical picture suggests that the heimer's disease12 are obvious, howev¬ lar disease deserves strong consider¬
disorder initially involved occipital er. Memory and personal insight are ation. Most reported cases of Balint's
and parietal association cortices, par¬ relatively well retained in these syndrome have been based on multi¬
ticularly Brodmann areas 18 and 19. patients until late in the course, while ple vascular infarcts and the promi¬
Later findings suggest anterior visual agnosia, alexia, and acalculia nence of transcortical sensory apha¬
spread to involve the angular gyrus or are severe at early stages. Even if the sia, and the Gerstmann syndrome in
its connections bilaterally. Table 2 neuropathologic features of Alzheim¬ these cases suggests a posterior bor¬
lists the major clinical features noted er's disease are eventually demon¬ der-zone abnormality. However, no
in these patients. strated, the early clinical findings are evidence of a cerebrovascular disorder
The possibility that the visual strikingly atypical. Nonetheless, Alz¬ was uncovered by CT, MRI, or angio¬
symptoms presented by these patients heimer's disease is said to show con¬ graphie studies.
could be the result of a disconnection siderable variation in the initial pre¬ One remote causative possibility
disorder deserves consideration. Most sentation and these cases may well was suggested by the history that two
reports of alexia,10 visual agnosia,11 represent an atypical Alzheimer dis¬ of these patients had received exten¬
prosopagnosia,4 environmental agno¬ ease clinical pattern.13 sive (seven to eight years) tetracycline
sia,1 and Balint's syndrome2'4 describe A degenerative disorder with lobar therapy and a third had bronchial
structural defects that effectively dis¬ predilection, such as Pick's disease, problems treated with a variety of
connect the intact primary visual cor¬ offers a tempting alternative origin. antibiotics over a period of years. The
tical areas from various association Pick's disease has long been described other two did not receive such drugs,
cortices. Numerous brain-imaging as primarily affecting anterior struc¬ however, and, at most, any relation¬
studies in these patients revealed no tures, particularly frontal and anteri¬ ship between antibiotic therapy and
such structural defects. Demyeiin¬ or temporal cortex.9·1415 The patients this syndrome must be considered
ating disorders, such as multiple scle¬ in this report also appear to show a tenuous.
rosis or Schilder's disease, can lobar dysfunction, but one that pri¬ The possibility that each of these
produce visual symptoms; again, MRI marily affects occipital and posterior individuals suffers from the same dis¬
scans in these patients revealed no parietal cortex. Could these cases rep¬ order appears high. The findings and
evidence of demyelination. On the resent a posteriorly localized variant course, particularly the presence of a
basis of these observations, degenera¬ of Pick's disease? The answer must combination of rare clinical disorders
tion primarily affecting posterior await neuropathologic studies. such as Balint's, Gerstmann's, and
association cortex appears most prob¬ The recent reports of progressive transcortical sensory aphasia syn¬
able. aphasia1618 deserve note. These cases dromes, appear unique. These cases
In the proposed division between are also awaiting histological verifica¬ are sufficiently similar to each other
cortical and subcortical dementia syn¬ tion but are suspected to represent and the findings are sufficiently dif¬
dromes,9 this disorder presents with variations in the onset of traditional ferent from those typical for either
predominantly higher-function ab¬ dementing disorders. Alterations in Alzheimer's or Pick's disease to war¬
normalities that appear to originate the early clinical picture of degenera¬ rant classing them separately until
almost exclusively from the posterior tive dementia are well recognized, definitive pathologic information be¬
association cortex. A descriptive term, apparently dependent on the site of comes available.
References
1. Landis T, Cummings JL, Benson DF, et al: York, Grune & Stratton, 1975, pp 63-82. 14. Corsellis JAN: Aging and the dementias, in
Loss of topographic familiarity: An encironmen- 8. American Psychiatric Association: Diagnos- Blackwood W, Corsellis JAN (eds): Greenfield's
tal agnosia. Arch Neurol 1986;43:132-136. tic and Statistical Manual of Mental Disorders, Neuropathology. Chicago, Year Book Medical
2. Balint R: Die seelenlahmung des 'Schauens.' ed 3. Washington, DC, American Psychiatric Publishers Inc, 1976, pp 796-848.
Monatschr Psychiatr Neurol 1909;1:25-51. Association, 1980, pp 205-224. 15. Malamud N, Hirano A: Atlas ofNeuropath-
3. H\l=e'\caenH, Albert ML: Human Neuropsy- 9. Cummings JL, Benson DF: Dementia: A ology, ed 2. Berkeley, Calif, University of Califor-
chology. New York, John Wiley & Sons Inc, Clinical Approach. Stoneham, Mass, Butterworth nia Press, 1974.
1978. Publishers Inc, 1983. 16. Chawluk JB, Mesulam M-M, Hurtig H, et
4. Damasio A: Disorders of complex visual 10. Benson DF: Alexia, in Frederiks JAM (ed): al: Slowly progressive aphasia without general-
processing: Agnosias, achromatopsia, Balint's Handbook of Clinical Neurology, ed 2. Amster- ized dementia: Studies with positron emission
syndrome and related difficulties of orientation dam, Elsevier Science Publishers, 1985, vol 45: tomography. Ann Neurol 1986;19:68-74.
and construction, in Mesulam M-M (ed): Princi- Clinical Neuropsychology, pp 433-455. 17. Kirshner HS, Webb WG, Kelly MP, et al:
ples of Behavioral Neurology. Philadelphia, FA 11. Rubens AB: Agnosia, in Heilman KM, Language disturbance: An initial symptom of
Davis Co Publishers, 1985, pp 259-288. Valenstein E (eds): Clinical Neuropsychology. cortical degenerations and dementia. Arch Neu-
5. H\l=e'\caenH, de Ajuriaguerra J, David M, et al: New York, Oxford University Press Inc, 1979, pp rol 1984;41:491-496.
Paralysie psychique du regard de Balint au cours 233-267. 18. Mesulam M-M: Slowly progressive aphasia
de l'evolution d'une leuco-encephalite type Balo. 12. McKhann G, Drachman D, Folstein M, et without generalized dementia. Ann Neurol
Rev Neurol 1950;83:81-104. al: Clinical diagnosis of Alzheimer's disease: 1982;11:592-598.
6. Gordon EB, Sim M: The EEG in presenile Report of the NINCDS-ADRDA Work Group 19. Morris JC, Monroe C, Banker BQ, et al:
dementia. J Neurol Neurosurg Psychiatry 1967; under the auspices of Department of Health and Hereditary dysphasic dementia in the Pick-
30:285-291. Human Services Task Force on Alzheimer's Dis- Alzheimer spectrum. Ann Neurol 1984;16:455\x=req-\
7. Harner RN: EEG evaluation in the patient ease. Neurology 1984;34:939-944. 466.
with dementia, in Benson DF, Blumer D (eds): 13. Mayer-Gross W: Posterior involvement by
Psychiatric Aspects of Neurologic Disease. New DAT. Proc R Soc Med 1937;38:1443-1454.
Downloaded From: http://archneur.jamanetwork.com/ by a DALHOUSIE UNIVERSITY-DAL-11762 User on 05/18/2015
You might also like
- A Chamber of Secrets The Neurology of The Thalamus - Lessons From Acute StrokeDocument6 pagesA Chamber of Secrets The Neurology of The Thalamus - Lessons From Acute StrokeIvan Morales BarreraNo ratings yet
- Case Studies - NeurologyDocument12 pagesCase Studies - NeurologyNick MorettinNo ratings yet
- Neurology Multiple Choice Questions With Explanations: Volume IIIFrom EverandNeurology Multiple Choice Questions With Explanations: Volume IIIRating: 4.5 out of 5 stars4.5/5 (6)
- CB Final Project On K&N'sDocument35 pagesCB Final Project On K&N'sGOHAR GHAFFARNo ratings yet
- Slowly Generahed: Progressive Aphasia Without DementiaDocument7 pagesSlowly Generahed: Progressive Aphasia Without Dementiajonas1808No ratings yet
- Human Kluver-Bucy: SyndromeDocument6 pagesHuman Kluver-Bucy: SyndromeFlorencia RubioNo ratings yet
- Ingles Lobulo FrontalDocument10 pagesIngles Lobulo FrontalCentro De Copiado Luna RtNo ratings yet
- Demencia SemanticaDocument5 pagesDemencia SemanticaJesus DecepcionadoNo ratings yet
- How To Perform A Basic Neurological Examination - 2016 - MedicineDocument5 pagesHow To Perform A Basic Neurological Examination - 2016 - MedicinemateoNo ratings yet
- A Case of Posterior Cortical Atrophy With VerticalDocument7 pagesA Case of Posterior Cortical Atrophy With VerticalNataly CastañedaNo ratings yet
- CUSTODIO Y MONTESINOS 2020 Frontotemporal IMAGENDocument8 pagesCUSTODIO Y MONTESINOS 2020 Frontotemporal IMAGENMAXIMILIANO HEREDIANo ratings yet
- Primary Progressive Aphasia: A 25-Year RetrospectiveDocument4 pagesPrimary Progressive Aphasia: A 25-Year RetrospectiveDranmar AhmedNo ratings yet
- Summary Crossed WernickeDocument10 pagesSummary Crossed WernickeLourenço CoutoNo ratings yet
- The Logopenic/phonological Variant of Primary Progressive AphasiaDocument10 pagesThe Logopenic/phonological Variant of Primary Progressive AphasiaDranmar AhmedNo ratings yet
- Music and Mental Illness in Search of Lost Time From "Demonic Possession" To Anti-N-Methyl - Aspartate Receptor EncephalitisDocument2 pagesMusic and Mental Illness in Search of Lost Time From "Demonic Possession" To Anti-N-Methyl - Aspartate Receptor EncephalitisivanNo ratings yet
- Corticobasal Syndrome A Practical GuideDocument10 pagesCorticobasal Syndrome A Practical Guideerika avelina rodriguez jaureguiNo ratings yet
- Delong 1981 en Cefalo Pat I ADocument4 pagesDelong 1981 en Cefalo Pat I A__aguNo ratings yet
- Perceptual Dysfunction, Semantic Impairment?: Topographic Amnesia: Spatial SpecificDocument8 pagesPerceptual Dysfunction, Semantic Impairment?: Topographic Amnesia: Spatial SpecificMaca Martínez-CuitiñoNo ratings yet
- Rajput 2021Document4 pagesRajput 202120.009 Diki Permadi Pratama PutraNo ratings yet
- Mental Retardation, Epilepsy, Short Stature, and Skeletal DysplasiaDocument3 pagesMental Retardation, Epilepsy, Short Stature, and Skeletal Dysplasiajahfdfgsdjad asdhsajhajdkNo ratings yet
- Strub 1989Document4 pagesStrub 1989mgobiNo ratings yet
- Posterior Cortical Atrophy: A Brief Review: Howard S. Kirshner, MD, and Patrick J. M. Lavin, MB, BCH, Bao, MrcpiDocument4 pagesPosterior Cortical Atrophy: A Brief Review: Howard S. Kirshner, MD, and Patrick J. M. Lavin, MB, BCH, Bao, MrcpiEugenia FiginiNo ratings yet
- CrossedWernickesAphasia2003 SheehyandHainesDocument4 pagesCrossedWernickesAphasia2003 SheehyandHainesLourenço CoutoNo ratings yet
- The Neurologic Syndrome of Severe Alzheimer's DiseaseDocument11 pagesThe Neurologic Syndrome of Severe Alzheimer's DiseaseFlaviuNo ratings yet
- E100283 FullDocument4 pagesE100283 FullAulya isra KurniasariNo ratings yet
- Chamber of SecretsDocument7 pagesChamber of SecretsjavieroxbmxNo ratings yet
- Case 40-2021 - A 9-Year-Old - Enf - MoyamoyaDocument10 pagesCase 40-2021 - A 9-Year-Old - Enf - MoyamoyaJuan C. Salazar PajaresNo ratings yet
- (Bookflare - Net) - Neurological Foundations of Cognitive NeuroscienceDocument30 pages(Bookflare - Net) - Neurological Foundations of Cognitive Neurosciencethuraya aidNo ratings yet
- Posterior Cortical Dementia: Lost But Not ForgettingDocument2 pagesPosterior Cortical Dementia: Lost But Not ForgettingElisabet GobelliNo ratings yet
- Brain Imaging in A Case of Capgras' SyndromeDocument6 pagesBrain Imaging in A Case of Capgras' SyndromeHusain RezaNo ratings yet
- Progressive: Primary AphasiaDocument7 pagesProgressive: Primary Aphasiamariafernanda portoNo ratings yet
- Cognitive FXN in PCADocument8 pagesCognitive FXN in PCAVincent OxenhamNo ratings yet
- Patient EVRDocument12 pagesPatient EVRJorge CastilloNo ratings yet
- Braga-13 EOAD PSEN1 Clinica de SCADocument3 pagesBraga-13 EOAD PSEN1 Clinica de SCAMARIA MONTSERRAT SOMOZA MONCADANo ratings yet
- Delayed Speech DevelopmentDocument5 pagesDelayed Speech DevelopmentShakirullah KhanNo ratings yet
- Agenesia CerebeloDocument5 pagesAgenesia CerebeloDiretoria CientíficaNo ratings yet
- Disconnecting The Cerebral Hemispheres: Bioscience Reports 2, 265-276 (1982) Printed in Great BritainDocument12 pagesDisconnecting The Cerebral Hemispheres: Bioscience Reports 2, 265-276 (1982) Printed in Great BritainNikhil NigamNo ratings yet
- AfasiaDocument23 pagesAfasiaAlexis A.No ratings yet
- Strasburger Et Al-2015-PsyCh JournalDocument8 pagesStrasburger Et Al-2015-PsyCh JournalPedro CardosoNo ratings yet
- ad vd ftdDocument8 pagesad vd ftdSakshi KharbandaNo ratings yet
- Abulia: No Will, No Way: SM Hastak, Pooja S Gorawara, NK MishraDocument5 pagesAbulia: No Will, No Way: SM Hastak, Pooja S Gorawara, NK MishraSaikat Prasad DattaNo ratings yet
- Apparently New Syndrome of Congenital Cataracts, Sensorineural Deafness, Down Syndrome-Like Facial Appearance, Short Stature, and Mental RetardationDocument5 pagesApparently New Syndrome of Congenital Cataracts, Sensorineural Deafness, Down Syndrome-Like Facial Appearance, Short Stature, and Mental Retardationjahfdfgsdjad asdhsajhajdkNo ratings yet
- Brain 2014 Yu Brain Awu239Document5 pagesBrain 2014 Yu Brain Awu239Angeles RbNo ratings yet
- Music, Memory, and Alzheimer's Disease: Is Music Recognition Spared in Dementia, and How Can It Be Assessed?Document7 pagesMusic, Memory, and Alzheimer's Disease: Is Music Recognition Spared in Dementia, and How Can It Be Assessed?Cami Sánchez SalinasNo ratings yet
- Alaskan 20 Husky 20 Encephalopathy 202Document13 pagesAlaskan 20 Husky 20 Encephalopathy 202Mao Tse Tung ToledoNo ratings yet
- Johnson 1996Document11 pagesJohnson 1996Ali AmokraneNo ratings yet
- Algoritmo Diferencial de Debilidad Proximal en Paciente Con Miopatia Adquirida Por Nemalina.Document7 pagesAlgoritmo Diferencial de Debilidad Proximal en Paciente Con Miopatia Adquirida Por Nemalina.Farid Santiago Abedrabbo LombeydaNo ratings yet
- Five Year Follow Up of A Patient With SPDocument9 pagesFive Year Follow Up of A Patient With SPasasakopNo ratings yet
- L&M AssignmentDocument11 pagesL&M AssignmentPayalNo ratings yet
- A Divided Mind. Observations On The Conscious Properties of Separated Hemispheres (1977)Document5 pagesA Divided Mind. Observations On The Conscious Properties of Separated Hemispheres (1977)Santiago Bermudez FeijooNo ratings yet
- Primary Progressive Aphasia: Neurological ProgressDocument8 pagesPrimary Progressive Aphasia: Neurological ProgressDranmar AhmedNo ratings yet
- A Case Report of Obsessive-Compulsive DisorderDocument6 pagesA Case Report of Obsessive-Compulsive DisorderfonsoalNo ratings yet
- Nancy Helm: Management of Palilalia With A Pacing BoardDocument4 pagesNancy Helm: Management of Palilalia With A Pacing BoardMacarena Paz ÁlvarezNo ratings yet
- Knowing Where and Knowinh Mhat A Double Dissociation Barbara Wilson & Linda Clare 1997Document13 pagesKnowing Where and Knowinh Mhat A Double Dissociation Barbara Wilson & Linda Clare 1997Registro psiNo ratings yet
- andreasenSINT NEG Y POSTIV EN ESQUIZODocument6 pagesandreasenSINT NEG Y POSTIV EN ESQUIZOmarielaNo ratings yet
- Journal of Child Neurology 11Document5 pagesJournal of Child Neurology 11NEUROLAB ESCALÓNNo ratings yet
- Screenshot 2023-09-17 at 3.26.16 PMDocument10 pagesScreenshot 2023-09-17 at 3.26.16 PMThana SnNo ratings yet
- Differentiating The Dementias: A Neurological Approach: ReviewDocument8 pagesDifferentiating The Dementias: A Neurological Approach: ReviewJemellee CanoNo ratings yet
- Developmental Dyscalculia: A Brief Report On Four Cases: Psychological Medicine, 1971, I, 292 29SDocument7 pagesDevelopmental Dyscalculia: A Brief Report On Four Cases: Psychological Medicine, 1971, I, 292 29SLejla HusicNo ratings yet
- Anomija PpaDocument11 pagesAnomija PpaMirna ZelicNo ratings yet
- The Epilepsy Aphasias: Landau Kleffner Syndrome and Rolandic EpilepsyFrom EverandThe Epilepsy Aphasias: Landau Kleffner Syndrome and Rolandic EpilepsyNo ratings yet
- (Macaulay, M. & Macmillan, M.) The Concept of Mental Age and MaturationDocument4 pages(Macaulay, M. & Macmillan, M.) The Concept of Mental Age and MaturationLuis GómezNo ratings yet
- Supplementary Figure 1. Negligible Effects of Covarying For Different Tracer Injection ParametersDocument6 pagesSupplementary Figure 1. Negligible Effects of Covarying For Different Tracer Injection ParametersLuis GómezNo ratings yet
- (Greenspan, N.) Autism, Evolution, and The Inadequacy of SpectrumDocument4 pages(Greenspan, N.) Autism, Evolution, and The Inadequacy of SpectrumLuis GómezNo ratings yet
- Neurobiology of AgingDocument11 pagesNeurobiology of AgingLuis GómezNo ratings yet
- Consensus Classification of Posterior Cortical AtrDocument15 pagesConsensus Classification of Posterior Cortical AtrLuis GómezNo ratings yet
- (Zimmerman, D., Et Al.) Independence of Hot and Cold Executive Function Deficits in High - Functioning Adults With Autism Spectrum DisorderDocument15 pages(Zimmerman, D., Et Al.) Independence of Hot and Cold Executive Function Deficits in High - Functioning Adults With Autism Spectrum DisorderLuis GómezNo ratings yet
- Author's Accepted Manuscript: Psychiatry ResearchDocument29 pagesAuthor's Accepted Manuscript: Psychiatry ResearchLuis GómezNo ratings yet
- Large-Scale Brain Networks in Cognition: Emerging Methods and PrinciplesDocument14 pagesLarge-Scale Brain Networks in Cognition: Emerging Methods and PrinciplesLuis GómezNo ratings yet
- Bruininks-Oseretsky Test of Motor Proficiency, Second Edition (BOT-2)Document2 pagesBruininks-Oseretsky Test of Motor Proficiency, Second Edition (BOT-2)Luis GómezNo ratings yet
- Annual Review Of: in Category Category Name in Category Factor Half-Life IndexDocument2 pagesAnnual Review Of: in Category Category Name in Category Factor Half-Life IndexLuis GómezNo ratings yet
- The Structure of The Individual Mental Lexicon From The Standpoint of L. S. Vygotsky's IdeasDocument15 pagesThe Structure of The Individual Mental Lexicon From The Standpoint of L. S. Vygotsky's IdeasLuis GómezNo ratings yet
- Software Manual Ifm 7391009UKDocument19 pagesSoftware Manual Ifm 7391009UKpatriciobenavidesmNo ratings yet
- Pa1 W2 S3 R2Document7 pagesPa1 W2 S3 R2Bubble PopNo ratings yet
- PoeticsDocument4 pagesPoeticsCalvin PenacoNo ratings yet
- Reguladores de Voltaje 79xxDocument13 pagesReguladores de Voltaje 79xxJuan Angel Cerda GuerraNo ratings yet
- Modal VerbsDocument13 pagesModal VerbsinmorichiNo ratings yet
- Bandarban at A GlanceDocument29 pagesBandarban at A GlanceShahriazAlamNo ratings yet
- Reading Circle 2 - Vocabulary EnricherDocument7 pagesReading Circle 2 - Vocabulary EnricherLee Jia XiNo ratings yet
- PhillipDocument4 pagesPhilliplucasdoriamaiaNo ratings yet
- Jade PresentationDocument11 pagesJade PresentationaaaaaaaNo ratings yet
- McDonald Family History v35Document45 pagesMcDonald Family History v35David McDonaldNo ratings yet
- Mental Health Services Data Set (MHSDS) Autism Statistics: Metadata FileDocument4 pagesMental Health Services Data Set (MHSDS) Autism Statistics: Metadata FileLauren-Jodie WilsonNo ratings yet
- Bidding Docs For DBWD Nlif May Final 2013projectDocument158 pagesBidding Docs For DBWD Nlif May Final 2013projectrain06021992No ratings yet
- Variable Unit-Linked Training Manual: Vul/Ulp Licensing Manual (December 2014) I 1Document57 pagesVariable Unit-Linked Training Manual: Vul/Ulp Licensing Manual (December 2014) I 1Gus Delfin100% (1)
- Greene, Big - Data - in - Medicine PDFDocument6 pagesGreene, Big - Data - in - Medicine PDFglitterglyptodonNo ratings yet
- Content and Contextual Analysis of The Parisian LifeDocument7 pagesContent and Contextual Analysis of The Parisian LifeSowla sidoNo ratings yet
- Differential Equations & Transforms (BMAT102L)Document19 pagesDifferential Equations & Transforms (BMAT102L)Venkat BalajiNo ratings yet
- Tables of Sign, Degree, Minute, Second For Horary KPDocument4 pagesTables of Sign, Degree, Minute, Second For Horary KPindrani royNo ratings yet
- Research Paper #6Document9 pagesResearch Paper #6Venice Claire CabiliNo ratings yet
- Quantitative Analysis of Carbohydrates by Nelson'S MethodDocument3 pagesQuantitative Analysis of Carbohydrates by Nelson'S MethodSeph CordovaNo ratings yet
- The Final JourneyDocument164 pagesThe Final JourneyMohammed Kamaluddeen YahyaNo ratings yet
- G.R. No. L-94Document2 pagesG.R. No. L-94wjdwbdiwbNo ratings yet
- Desires - How Are You Feeling Today Sir? If Huminto Po Si PT, Iallow Po Natin Siya & Bigyan Siya NG Time To Fully Undertand What He Is Feeling Right Now.Document19 pagesDesires - How Are You Feeling Today Sir? If Huminto Po Si PT, Iallow Po Natin Siya & Bigyan Siya NG Time To Fully Undertand What He Is Feeling Right Now.melodia gandezaNo ratings yet
- Final SampleDocument5 pagesFinal SampleTasaduqNo ratings yet
- Kaos GnosticismDocument1 pageKaos Gnosticismanton eNo ratings yet
- Azu TD 3132236 Sip1 MDocument218 pagesAzu TD 3132236 Sip1 MXi LinNo ratings yet
- Chap 13: Turning Customer Knowledge Into Sales KnowledgeDocument3 pagesChap 13: Turning Customer Knowledge Into Sales KnowledgeHEM BANSALNo ratings yet
- MSDS Full1 PDFDocument92 pagesMSDS Full1 PDFSunthron SomchaiNo ratings yet
- Nadine Rose DissertationDocument7 pagesNadine Rose DissertationWebsiteThatWillWriteAPaperForYouSavannah100% (1)