Professional Documents
Culture Documents
Urethral Pathology: Case 1 Case 2
Urethral Pathology: Case 1 Case 2
Uploaded by
HardiTariqHamma0 ratings0% found this document useful (0 votes)
31 views2 pages1. A 43-year-old woman presents with urinary incontinence and vaginal pain with intercourse. Imaging reveals a female urethral diverticulum, which commonly causes dysuria, dribbling, and dyspareunia.
2. During a pelvic exam, a small protrusion from the urethral meatus is seen and diagnosed as a urethral caruncle, a benign growth caused by reduced estrogen support of the urethral mucosa.
3. Cystoscopy for hematuria reveals urothelial carcinoma of the urethra in a male, which has risk factors like bladder cancer, inflammation, and is most commonly seen
Original Description:
Original Title
uroso19-spottest
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Document1. A 43-year-old woman presents with urinary incontinence and vaginal pain with intercourse. Imaging reveals a female urethral diverticulum, which commonly causes dysuria, dribbling, and dyspareunia.
2. During a pelvic exam, a small protrusion from the urethral meatus is seen and diagnosed as a urethral caruncle, a benign growth caused by reduced estrogen support of the urethral mucosa.
3. Cystoscopy for hematuria reveals urothelial carcinoma of the urethra in a male, which has risk factors like bladder cancer, inflammation, and is most commonly seen
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
0 ratings0% found this document useful (0 votes)
31 views2 pagesUrethral Pathology: Case 1 Case 2
Urethral Pathology: Case 1 Case 2
Uploaded by
HardiTariqHamma1. A 43-year-old woman presents with urinary incontinence and vaginal pain with intercourse. Imaging reveals a female urethral diverticulum, which commonly causes dysuria, dribbling, and dyspareunia.
2. During a pelvic exam, a small protrusion from the urethral meatus is seen and diagnosed as a urethral caruncle, a benign growth caused by reduced estrogen support of the urethral mucosa.
3. Cystoscopy for hematuria reveals urothelial carcinoma of the urethra in a male, which has risk factors like bladder cancer, inflammation, and is most commonly seen
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
You are on page 1of 2
SPOT TEST
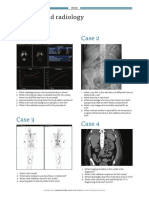
Urethral pathology
Case 1 Case 2
A 43-year-old lady presents with urinary incontinence and vaginal On performing a
pain associated with intercourse. An initial CT scan is performed. pelvic examination in
a female you see the
following.
Case courtesy of Radswiki, Radiopaedia.org, rID: 12056.
1. What is the clinical diagnosis from the imaging?
2. How common are these in women? 1. What is the diagnosis?
3. How do they usually present? 2. Define this condition.
4. How are these diagnosed? 3. What is the underlying pathophysiology?
5. How are they classified? 4. What is the differential diagnosis?
5. What are the treatment options?
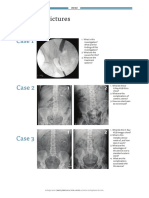
Case 3
While performing a cystoscopy for haematuria, the following are encountered in the
male urethra:
1. What is the likely diagnosis?
2. What are the risk factors for this?
3. How common is this?
4. What is the T-stage classification?
5. What factors affect overall disease survival?
urology news | SEPTEMBER/OCTOBER 2019 | VOL 23 NO 6 | www.urologynews.uk.com
SPOT TEST
Urethral pathology: answers oestrogens, anti-inflammatories or References
steroids. Surgery: excision if conservative 1. Greenwell TJ, Spilotros M. Urethral diverticula in women.
Nature Reviews Urology 2015; 12:671-80.
methods failed, symptomatic or
Case 1 2. Clark J, Olson L, Kujawa M. A review of the diagnosis
diagnostic uncertainty
and management of urethral caruncles. Urology News
2017;22(1):28-29.
1. Female urethral diverticulum.
2. 0.02–6%.
Case 3 3. Gakis G, Witjes JA, Compérat E, et al. EAU Guidelines on
Primary Urothral Carcinoma. Eur Urol 2013;64(5):823-30.
3. A high index of clinical suspicion aids
the diagnosis. Classically they present 1. Urothelial carcinoma (UC) of the urethra.
with dysuria, dribble and dyspareunia 2. Bladder UC, chronic inflammation after
(3Ds) – 20% of female cases. Urinary clean intermittent self catheterisation
incontinence, recurrent urinary tract (CISC) / urethroplasty, radiotherapy, SECTION EDITOR
infections (UTIs), frequency, urgency, radioactive seeds, chronic urethral
urethral / vaginal lump may be other inflammation post sexually transmitted Nick Rukin,
symptoms. infection (i.e. HPV 16 related). In female Consultant Urological
4. MRI is the imaging of choice, but they specifically urethral diverticulum and Surgeon, Metro North
can be diagnosed on micturating recurrent UTIs. Hospitals and Health
Service, Brisbane, Australia.
cystourethrogram, video urodynamics, 3. Estimated to be 1.6 per million (males)
and 0.6 per million females. E: nicholas.rukin@
cystourethroscopy, ultrasound, CT health.qld.gov.au
imaging and clinically detected. 4. Tx Primary tumour cannot be assessed.
Twitter: @nickrukin
5. Multiple classifications have been Tis Carcinoma in situ.
reported [1-3] but an anatomical T0 No evidence of primary tumour.
classification via MRI is often helpful. Ta Non-invasive papillary carcinoma.
This incorporates: simple, horseshoe or T1 Tumour invades subepithelial
circumferential diverticula. connective tissue.
T2 Tumour invades any of the following
structures: corpus spongiosum, prostate,
Case 2
peri-urethral muscle.
T3 Tumour invades any of the following
1. Urethral caruncle.
structures: corpus cavernosum, invasion
2. A small single quadrant urethral
beyond prostatic capsule, anterior
prolapse, typically affecting the posterior
vaginal wall, bladder neck.
urethral meatus.
T4 Tumour invades other adjacent
3. Reduced oestrogen levels, causing the
organs.
urethral smooth muscle to lack support
5. Age, tumour stage and grade, nodal
for the urethral mucosa. Another
stage, presence of distant metastasis,
theory is secondary to an inflammatory
histological type, tumour size, tumour
process following recurrent or chronic
location, and type and modality of
inflammation
treatment.
4. Urethral prolapse / polyp, para-urethral
cyst, urethral diverticulum, condyloma,
urethral carcinoma.
5. Conservative therapy: sitz-bath, topical
urology news | SEPTEMBER/OCTOBER 2019 | VOL 23 NO 6 | www.urologynews.uk.com
You might also like
- Irvine Welsh Ecstasy Three Tales of Chemical RomanceDocument43 pagesIrvine Welsh Ecstasy Three Tales of Chemical RomanceClara RuizNo ratings yet
- UROLOGY OSCE Skills English NT Version 2Document1 pageUROLOGY OSCE Skills English NT Version 2HardiTariqHammaNo ratings yet
- TB of The TestesDocument2 pagesTB of The Testesntambik21No ratings yet
- Research Protocol Form, Approval Deraw DR - 1Document12 pagesResearch Protocol Form, Approval Deraw DR - 1HardiTariqHammaNo ratings yet
- Presentation Fabrication of Storage TankDocument43 pagesPresentation Fabrication of Storage TankAbdul Manaf100% (1)
- Urological Science: Jiun-Hung Geng, Chun-Nung HuangDocument4 pagesUrological Science: Jiun-Hung Geng, Chun-Nung Huangyerich septaNo ratings yet
- A Rare Case of Endometriosis in Turners SyndromeDocument3 pagesA Rare Case of Endometriosis in Turners SyndromeElison J PanggaloNo ratings yet
- Utd 13 1 74 77Document4 pagesUtd 13 1 74 77Abhishek Soham SatpathyNo ratings yet
- Case Report Aditya - Jurnal VancoverDocument6 pagesCase Report Aditya - Jurnal VancoverAditya AirlanggaNo ratings yet
- Review of Aetiology and Management of Testicular Abscess and Case Reports On Testicle Sparing Management of Testicular AbscessDocument5 pagesReview of Aetiology and Management of Testicular Abscess and Case Reports On Testicle Sparing Management of Testicular AbscessBodat BodatsNo ratings yet
- Accepted Manuscript: UrologyDocument12 pagesAccepted Manuscript: UrologyayunikmatulNo ratings yet
- Benign Paratesticlar Cyst - A Mysterical FindingDocument2 pagesBenign Paratesticlar Cyst - A Mysterical FindingInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Paraurethral Cyst: A Case Report: Central European Journal ofDocument3 pagesParaurethral Cyst: A Case Report: Central European Journal ofEltohn JohnNo ratings yet
- Case 1 Case 2: Bladder Outlet ObstructionDocument2 pagesCase 1 Case 2: Bladder Outlet ObstructionHardiTariqHamma100% (1)
- Ovarian TorsionDocument4 pagesOvarian TorsionRiko KuswaraNo ratings yet
- International Archives of Urology and Complications Iauc 8 086Document6 pagesInternational Archives of Urology and Complications Iauc 8 086Ikhsan PrialaksanaNo ratings yet
- Burud 2020Document8 pagesBurud 2020Wirda Elya SariNo ratings yet
- University of Colorado School of Medicine University of Colorado School of Medicine and Children's Hospital ColoradoDocument2 pagesUniversity of Colorado School of Medicine University of Colorado School of Medicine and Children's Hospital ColoradoashwiniNo ratings yet
- Rare Peritoneal Tumour Presenting As Uterine Fibroid: Janu Mangala Kanthi, Sarala Sreedhar, Indu R. NairDocument3 pagesRare Peritoneal Tumour Presenting As Uterine Fibroid: Janu Mangala Kanthi, Sarala Sreedhar, Indu R. NairRezki WidiansyahNo ratings yet
- Solitary Fibrous Tumor in The Retroperit 2024 International Journal of SurgeDocument5 pagesSolitary Fibrous Tumor in The Retroperit 2024 International Journal of SurgeRonald QuezadaNo ratings yet
- IVU in The ClinicDocument16 pagesIVU in The ClinicDaniela LSNo ratings yet
- Malignant Struma OvariiDocument4 pagesMalignant Struma Ovariixwahyu 108No ratings yet
- Intussusceptionis in Adult, Case Report of Acute Intussusceptionon Due To Metastasis From A Testicular TumorDocument4 pagesIntussusceptionis in Adult, Case Report of Acute Intussusceptionon Due To Metastasis From A Testicular TumorIJAR JOURNALNo ratings yet
- An Uncommon Poorly Differentiated Small Cell Neuro-Endocrine Carcinoma of Urinary Bladder A Review With Case ReportDocument3 pagesAn Uncommon Poorly Differentiated Small Cell Neuro-Endocrine Carcinoma of Urinary Bladder A Review With Case ReportInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Yang Et Al. - 2020 - Blunt Abdominal Trauma Resulting in Ovarian Mucinous Cystadenoma RuptureDocument2 pagesYang Et Al. - 2020 - Blunt Abdominal Trauma Resulting in Ovarian Mucinous Cystadenoma RuptureJamesLeeNo ratings yet
- Final-Galley Proof 2Document3 pagesFinal-Galley Proof 2rvfz9jw649No ratings yet
- Acute Scrotum PDFDocument9 pagesAcute Scrotum PDFthejaskamathNo ratings yet
- 60 TH Male Spermatic Cord HydroceleDocument2 pages60 TH Male Spermatic Cord HydroceleSofie HanafiahNo ratings yet
- Hepatic Echinococcus Granulosus. A Case ReportDocument2 pagesHepatic Echinococcus Granulosus. A Case ReportIngrid DuarteNo ratings yet
- 2014 Immature Uterine Teratoma Associated With Uterine InversionDocument3 pages2014 Immature Uterine Teratoma Associated With Uterine Inversionpaula rangelNo ratings yet
- Clear Cell Adenocarcinoma of Ovary About A Rare Case and Review of The LiteratureDocument3 pagesClear Cell Adenocarcinoma of Ovary About A Rare Case and Review of The LiteratureInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- 2016 Article 1454 PDFDocument3 pages2016 Article 1454 PDFHerlinda Puji LNo ratings yet
- An Infrequent Secondary Location of Renal Carcinoma About A CaseDocument7 pagesAn Infrequent Secondary Location of Renal Carcinoma About A CaseInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- El Nódulo TiroideoDocument8 pagesEl Nódulo Tiroideoemily peceroNo ratings yet
- Rectovaginal Fistulae: Bidhan Das, MD Michael Snyder, MDDocument7 pagesRectovaginal Fistulae: Bidhan Das, MD Michael Snyder, MDNovaNo ratings yet
- Goh 2004Document3 pagesGoh 2004Brendan DiasNo ratings yet
- Striktur UrethraDocument24 pagesStriktur UrethraOktaviani Karo SekaliNo ratings yet
- Understanding Genitourinary System CytologyDocument130 pagesUnderstanding Genitourinary System Cytologyaaes2No ratings yet
- Care For Women: With Ovarian, Cerviacl, Vulvar and Endometrial CancerDocument26 pagesCare For Women: With Ovarian, Cerviacl, Vulvar and Endometrial CancerAhmad JradeenNo ratings yet
- Multiloculated Peritoneal Inclusion Cyst Treated Successfully With Laparoscopic SurgeryDocument3 pagesMultiloculated Peritoneal Inclusion Cyst Treated Successfully With Laparoscopic SurgerySreekumar SreekandanNo ratings yet
- Preceptor: Dr. Arief Effendi, SP - KK: OlehDocument13 pagesPreceptor: Dr. Arief Effendi, SP - KK: OlehriaNo ratings yet
- Malignant Mesothelioma of The Tunica Vaginalis Testis: Case ReportDocument2 pagesMalignant Mesothelioma of The Tunica Vaginalis Testis: Case ReportjamesyuNo ratings yet
- Testicular Torsion: A Urological EmergencyDocument4 pagesTesticular Torsion: A Urological EmergencycorsaruNo ratings yet
- 6703 23736 1 PBDocument3 pages6703 23736 1 PBReski Harlianty HarliNo ratings yet
- Lin 2019Document3 pagesLin 2019Mahmoud AbouelsoudNo ratings yet
- Bladder Cancer and Its MimicsDocument16 pagesBladder Cancer and Its MimicsmedicoscantareiraNo ratings yet
- Preprint Not Peer Reviewed: AuthorsDocument7 pagesPreprint Not Peer Reviewed: AuthorsАмина ПлотноваNo ratings yet
- University Journal of Surgery and Surgical Specialities: Dhivya Lakshmi S JDocument4 pagesUniversity Journal of Surgery and Surgical Specialities: Dhivya Lakshmi S JYonathanWaisendiNo ratings yet
- Intrathyroidal Lymphoepithelial (Branchial) Cyst: Diagnostic and Management Challenge of A Rare EntityDocument5 pagesIntrathyroidal Lymphoepithelial (Branchial) Cyst: Diagnostic and Management Challenge of A Rare EntityMeliNo ratings yet
- The Bartholin Cyst That Wasn't: A Case Report of Metastatic CancerDocument3 pagesThe Bartholin Cyst That Wasn't: A Case Report of Metastatic CancerihdinaNo ratings yet
- Testicular Microlithiasis1Document4 pagesTesticular Microlithiasis1Ioannis ValioulisNo ratings yet
- Jurnal P.acnesDocument4 pagesJurnal P.acnesFazlicha SyaradilaNo ratings yet
- Medicine: Intrauterine Device Found in An Ovarian TumorDocument5 pagesMedicine: Intrauterine Device Found in An Ovarian TumorRezky amalia basirNo ratings yet
- Congenital Disorders of Female Genital OrgansDocument73 pagesCongenital Disorders of Female Genital OrgansAmalNo ratings yet
- Undescended Testes:Embryological and Clinical Importance: Veena Vidya Shankar, Roopa KulkarniDocument3 pagesUndescended Testes:Embryological and Clinical Importance: Veena Vidya Shankar, Roopa KulkarniArgy RizkyNo ratings yet
- Krukenberg Tumour Simulating Uterine Fibroids and Pelvic Inflammatory DiseaseDocument3 pagesKrukenberg Tumour Simulating Uterine Fibroids and Pelvic Inflammatory DiseaseradianrendratukanNo ratings yet
- Adult Intussusception - A Surgical Dilemma: J Ayub Med Coll Abbottabad 2006 18Document4 pagesAdult Intussusception - A Surgical Dilemma: J Ayub Med Coll Abbottabad 2006 18edi_wsNo ratings yet
- Clinical Management of Ovarian Endometriotic Cyst (Chocolate Cyst) : Diagnosis, Medical Treatment, and Minimally Invasive SurgeryDocument9 pagesClinical Management of Ovarian Endometriotic Cyst (Chocolate Cyst) : Diagnosis, Medical Treatment, and Minimally Invasive SurgerymfaddhilNo ratings yet
- Urothelial Carcinoma of The Urinary Bladder in Young Adults - Clinical Experience at Taipei Veterans General HospitalDocument4 pagesUrothelial Carcinoma of The Urinary Bladder in Young Adults - Clinical Experience at Taipei Veterans General HospitaldrelvNo ratings yet
- 14 Vol. 11 Issue 11 Nov 2020 IJPSR RE 3646Document7 pages14 Vol. 11 Issue 11 Nov 2020 IJPSR RE 3646Ehwanul HandikaNo ratings yet
- TangDocument8 pagesTangPatricia BezneaNo ratings yet
- Surgical TechniquesDocument32 pagesSurgical TechniquesJackson Souza100% (1)
- Group 4 Anatomy Assignment SubmissionDocument24 pagesGroup 4 Anatomy Assignment SubmissionGraceNo ratings yet
- Endoscopic Ultrasound Management of Pancreatic Lesions: From Diagnosis to TherapyFrom EverandEndoscopic Ultrasound Management of Pancreatic Lesions: From Diagnosis to TherapyAntonio FacciorussoNo ratings yet
- Uroma16 Spot Test 2Document2 pagesUroma16 Spot Test 2HardiTariqHammaNo ratings yet
- Holep Masterclass 2012Document2 pagesHolep Masterclass 2012HardiTariqHammaNo ratings yet
- Urology News Jul Aug 2016 Spot TestDocument2 pagesUrology News Jul Aug 2016 Spot TestHardiTariqHammaNo ratings yet
- Urolithiasis - Metabolic Considerations: Case 1Document2 pagesUrolithiasis - Metabolic Considerations: Case 1HardiTariqHammaNo ratings yet
- 9 Summative Assessements Prof AntoniewiczDocument60 pages9 Summative Assessements Prof AntoniewiczHardiTariqHammaNo ratings yet
- Prostate Cancer: Case 1 Case 2Document2 pagesProstate Cancer: Case 1 Case 2HardiTariqHammaNo ratings yet
- A. Congenital Adrenal HyperplasiaDocument5 pagesA. Congenital Adrenal HyperplasiasewmehondesalegnNo ratings yet
- Uromj14 Spot Test NewDocument2 pagesUromj14 Spot Test NewHardiTariqHammaNo ratings yet
- Urology OSCEDocument10 pagesUrology OSCEHardiTariqHammaNo ratings yet
- Neurourology: Case 1 Case 3Document2 pagesNeurourology: Case 1 Case 3HardiTariqHammaNo ratings yet
- Case 1 Case 2: Bladder Outlet ObstructionDocument2 pagesCase 1 Case 2: Bladder Outlet ObstructionHardiTariqHamma100% (1)
- The Shouldice Natural Tissue Repair For Inguinal HerniaDocument12 pagesThe Shouldice Natural Tissue Repair For Inguinal HerniaHardiTariqHammaNo ratings yet
- Emphysematous Pyelonephritis (EPN)Document31 pagesEmphysematous Pyelonephritis (EPN)HardiTariqHammaNo ratings yet
- Radiology Quiz: by Jane BelfieldDocument4 pagesRadiology Quiz: by Jane BelfieldHardiTariqHammaNo ratings yet
- Paediatric Urology - Peno-Scrotal: Case 1 Case 2Document2 pagesPaediatric Urology - Peno-Scrotal: Case 1 Case 2HardiTariqHammaNo ratings yet
- Continuing Medical Education: CME Multiple Choice QuestionsDocument1 pageContinuing Medical Education: CME Multiple Choice QuestionsHardiTariqHammaNo ratings yet
- Case 1 Case 3: Technology - Part 1Document2 pagesCase 1 Case 3: Technology - Part 1HardiTariqHammaNo ratings yet
- Renal Quiz (12.8.2017)Document3 pagesRenal Quiz (12.8.2017)HardiTariqHammaNo ratings yet
- Case 1: Urological Trauma - Part 1Document2 pagesCase 1: Urological Trauma - Part 1HardiTariqHammaNo ratings yet
- Test Yourself: MCQ and Single Best AnswerDocument2 pagesTest Yourself: MCQ and Single Best AnswerHardiTariqHammaNo ratings yet
- 4 - ProstateDocument9 pages4 - ProstateHardiTariqHammaNo ratings yet
- Pyeloplasty (Anderson-Hynes)Document12 pagesPyeloplasty (Anderson-Hynes)HardiTariqHammaNo ratings yet
- Transurethral Resection of The ProstateDocument41 pagesTransurethral Resection of The ProstateHardiTariqHammaNo ratings yet
- Urology Case Reports: Shakhawan Hama Amin Said, Rezhin Yaseen Abdalla, Ismaeel Aghaways, Ari Mohammed AbdullahDocument3 pagesUrology Case Reports: Shakhawan Hama Amin Said, Rezhin Yaseen Abdalla, Ismaeel Aghaways, Ari Mohammed AbdullahHardiTariqHammaNo ratings yet
- Urology Case Reports: Abdullah, Junping XingDocument3 pagesUrology Case Reports: Abdullah, Junping XingHardiTariqHammaNo ratings yet
- Di MCB DB Pricelist01!07!2018Document1 pageDi MCB DB Pricelist01!07!2018saurabhjerps231221No ratings yet
- Zulkurnain Et Al. - 2013 - Optimization of Palm Oil Physical Refining Process For Reduction of 3-Monochloropropane-1,2-Diol (3-MCPD) EstDocument10 pagesZulkurnain Et Al. - 2013 - Optimization of Palm Oil Physical Refining Process For Reduction of 3-Monochloropropane-1,2-Diol (3-MCPD) EstMoch Dimas Khoirul UmamNo ratings yet
- IntroductionDocument19 pagesIntroductionAkshay BhagatNo ratings yet
- Common Proper Noun Worksheet Underlining IntermediateDocument1 pageCommon Proper Noun Worksheet Underlining Intermediaterazeen_93No ratings yet
- Clinical Significance of para Lumbar FossaDocument11 pagesClinical Significance of para Lumbar FossaSUTHAN100% (1)
- METUS - Getting Started With VRF - White PaperDocument11 pagesMETUS - Getting Started With VRF - White PaperEltonNo ratings yet
- Earths Climate Past and Future 3rd Edition Ruddiman Test BankDocument14 pagesEarths Climate Past and Future 3rd Edition Ruddiman Test Bankraphaelbacrqu100% (25)
- Xi English Set 1Document4 pagesXi English Set 1aashirwad2076No ratings yet
- Stoichiometric CalculationsDocument13 pagesStoichiometric Calculationsandrew surajNo ratings yet
- Risk Based SupervisionDocument22 pagesRisk Based Supervisionsakshi819863200No ratings yet
- Welding-Standards 23-03-2014Document1 pageWelding-Standards 23-03-2014givali100% (7)
- Earth Compaction EquipmentDocument15 pagesEarth Compaction EquipmentÄmî Îíţ ŚHäh100% (1)
- Conservation of A Neolithic Plaster StatueDocument1 pageConservation of A Neolithic Plaster StatueJC4413No ratings yet
- Global Vaccine Action Plan: Tetanus & Difteri (TD/DPT)Document6 pagesGlobal Vaccine Action Plan: Tetanus & Difteri (TD/DPT)Gusti IndrakusumaNo ratings yet
- 1 PDFDocument103 pages1 PDF123qweNo ratings yet
- Contract Labour FORM XIIDocument1 pageContract Labour FORM XIIhdpanchal86100% (1)
- Line and Cable ModellingDocument23 pagesLine and Cable ModellingarunmozhiNo ratings yet
- Aksum University-Department of Nursing For 3 Yr BSC Nursing StudentsDocument21 pagesAksum University-Department of Nursing For 3 Yr BSC Nursing StudentsteklayNo ratings yet
- 150 de Thi Hoc Sinh Gioi Tieng Anh Lop 6Document59 pages150 de Thi Hoc Sinh Gioi Tieng Anh Lop 6K68G-Trần Hải HàNo ratings yet
- MS116-6.3 Manual Motor Starter: Product-DetailsDocument7 pagesMS116-6.3 Manual Motor Starter: Product-DetailsLeonardo Andres MagiNo ratings yet
- Q2-Module 1-The Healthy School and Community Invironments With SignatureDocument22 pagesQ2-Module 1-The Healthy School and Community Invironments With SignatureMark Euan B. DolosoNo ratings yet
- Research Methods in BusinessDocument28 pagesResearch Methods in Businessguptasoniya247No ratings yet
- Unit Operations of Bokaro Steel Plant and Their Environmental AspectsDocument52 pagesUnit Operations of Bokaro Steel Plant and Their Environmental AspectsGopalSingh100% (2)
- Cerebrovascular AccidentDocument42 pagesCerebrovascular AccidentGideon HaburaNo ratings yet
- Nuclear ChemistryDocument9 pagesNuclear ChemistryMaries San PedroNo ratings yet
- Ignition System Prototype Maintenance Manual and Safety ManualDocument15 pagesIgnition System Prototype Maintenance Manual and Safety ManualangeloNo ratings yet
- Jung Typology TestDocument2 pagesJung Typology TestPhuong Thanh ANNo ratings yet
- Caie A2 Level Geography 9696 Advanced Physical Geography v1Document21 pagesCaie A2 Level Geography 9696 Advanced Physical Geography v1j53846004No ratings yet