Professional Documents
Culture Documents
Almansour2020 - Article - PyogenicSpondylodiscitisPyogen Clinica Radiologia
Almansour2020 - Article - PyogenicSpondylodiscitisPyogen Clinica Radiologia
Uploaded by
Thais LudenaCopyright:
Available Formats
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5822)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1093)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (852)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (898)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (540)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (349)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (822)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (403)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Short Notes in Periodontics A HandbookDocument172 pagesShort Notes in Periodontics A HandbookFarheen Tajammal100% (9)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Medication: Expected Pharmacological Action Therapeutic UseDocument1 pageMedication: Expected Pharmacological Action Therapeutic Useclarimer100% (1)
- Ujjayi Pranayama Benefits and Steps - Big Chi Theory PDFDocument4 pagesUjjayi Pranayama Benefits and Steps - Big Chi Theory PDFakshra7gjNo ratings yet
- Gayatri Dengale FinalDocument38 pagesGayatri Dengale FinalTarwade NileshNo ratings yet
- Clinical, Immunological, and Molecular Findings in 57 Patients With Severe Combined Immunodeficiency (SCID) From IndiaDocument16 pagesClinical, Immunological, and Molecular Findings in 57 Patients With Severe Combined Immunodeficiency (SCID) From IndiaYeni PuspitasariNo ratings yet
- Disorders of Iron Kinetics and Heme MetabolismDocument12 pagesDisorders of Iron Kinetics and Heme MetabolismJoanne JardinNo ratings yet
- Calcium Metabolism-Board Questions 2018: Azar Khosravi April 2018Document55 pagesCalcium Metabolism-Board Questions 2018: Azar Khosravi April 2018Abdullah SiddiqiNo ratings yet
- PollutionDocument30 pagesPollutionMuhammed Althaf VKNo ratings yet
- Actual Listening Test For English Major StudentsDocument2 pagesActual Listening Test For English Major StudentsBayissa BekeleNo ratings yet
- Proton Pump InhibitorDocument24 pagesProton Pump InhibitorApurba Sarker ApuNo ratings yet
- Analysis of Satisfaction Level Regarding Fixed Partial Denture: A Clinical StudyDocument3 pagesAnalysis of Satisfaction Level Regarding Fixed Partial Denture: A Clinical StudySkAliHassanNo ratings yet
- Time To Ditch Toxic Positivity,' Experts Say: It's Okay Not To Be Okay'Document5 pagesTime To Ditch Toxic Positivity,' Experts Say: It's Okay Not To Be Okay'Ivana VelickovicNo ratings yet
- ECG ArrhythmiaDocument27 pagesECG ArrhythmiaSrikitta DanieliaNo ratings yet
- 3.6.2020 Final Final Manual - Logbook For Students For Adult 2Document34 pages3.6.2020 Final Final Manual - Logbook For Students For Adult 2Drmirfat AlkashifNo ratings yet
- TelepsychiatryDocument406 pagesTelepsychiatrychrisNo ratings yet
- Evaluation of Allergenicity of Genetically Modified FoodsDocument30 pagesEvaluation of Allergenicity of Genetically Modified FoodsChirag EducationNo ratings yet
- List of Journals Approved by UGC-2024: January 2024Document1,401 pagesList of Journals Approved by UGC-2024: January 2024Jordan PetersonNo ratings yet
- Plain Film and HRCT Diagnosis of Interstitial Lung Disease: Sujal R. Desai, Helmut Prosch, and Jeffrey R. GalvinDocument9 pagesPlain Film and HRCT Diagnosis of Interstitial Lung Disease: Sujal R. Desai, Helmut Prosch, and Jeffrey R. GalvinVictor ChiabaiNo ratings yet
- Taking Charge of Your Health: © 2021 Cengage. All Rights ReservedDocument46 pagesTaking Charge of Your Health: © 2021 Cengage. All Rights ReservedTimothy MontgomeryNo ratings yet
- Atrial FibrillationDocument28 pagesAtrial FibrillationKrisianne Mae Lorenzo FranciscoNo ratings yet
- Bi Support Groups1Document6 pagesBi Support Groups1api-301357752No ratings yet
- TDM Slides NicholsDocument39 pagesTDM Slides NicholsGordon BongNo ratings yet
- Defecation - Rectum - Control - TeachMePhysiologyDocument2 pagesDefecation - Rectum - Control - TeachMePhysiologyLaiba AliNo ratings yet
- PriyankarefDocument6 pagesPriyankarefapi-19985983No ratings yet
- 8 - 030 - Fathan - Akbar - Al - Bahri - Outcome 1 2Document8 pages8 - 030 - Fathan - Akbar - Al - Bahri - Outcome 1 2Fathan FathanNo ratings yet
- Icardin - Your First Choice For A Second OpinionDocument3 pagesIcardin - Your First Choice For A Second OpinionHounkonnou JacquesNo ratings yet
- Nutrients and Botanicals For Erectile Dysfunction: Examining The EvidenceDocument13 pagesNutrients and Botanicals For Erectile Dysfunction: Examining The EvidencefinaNo ratings yet
- Hepbd J Met Hepatitis B Surface Antigen 508Document18 pagesHepbd J Met Hepatitis B Surface Antigen 508Gom LinusNo ratings yet
- Catalog Knee CapsDocument3 pagesCatalog Knee CapskrastromanNo ratings yet
- Infectious Diseases Affecting The GitDocument64 pagesInfectious Diseases Affecting The GitGeraldine MaeNo ratings yet
Almansour2020 - Article - PyogenicSpondylodiscitisPyogen Clinica Radiologia
Almansour2020 - Article - PyogenicSpondylodiscitisPyogen Clinica Radiologia
Uploaded by
Thais LudenaOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Almansour2020 - Article - PyogenicSpondylodiscitisPyogen Clinica Radiologia
Almansour2020 - Article - PyogenicSpondylodiscitisPyogen Clinica Radiologia
Uploaded by
Thais LudenaCopyright:
Available Formats
Der Orthopäde
Übersichten
Orthopäde 2020 · 49:482–493 H. Almansour · W. Pepke · M. Akbar
https://doi.org/10.1007/s00132-019-03836-0 Department of Orthopaedic Surgery, Trauma Surgery and Spinal Cord Injury, Heidelberg University,
Published online: 13 November 2019 Heidelberg, Germany
© Springer Medizin Verlag GmbH, ein Teil von
Springer Nature 2019
Pyogenic spondylodiscitis
The quest towards a clinical-radiological
classification
Introduction been also documented. This could be ex- ence pain at initial presentation [15]. In
plained byincreased life expectancyofthe a systematic review and meta-analysis on
Pyogenic spondylodiscitis (PS) encom- general population and of patients with PS, Taylor et al. showed that the lumbar
passes osteomyelitis of the vertebra and predisposing comorbidities as well as the spine is the most common site of infec-
intervertebral discs [1]. A multitude of rising number of spinal surgeries and im- tion followed by the thoracic spine and
terms are used to describe the same debil- proved diagnostic methods [2, 11]. The the cervical spine [6]. Radiculopathy or
itating condition, such as septic discitis, routes of PS infections include hematoge- sharp back pain could indicate the pres-
spinal osteomyelitis, disc space infection nous seeding, contiguous spreading from ence of an epidural abscess [16]. Spinal
and vertebral osteomyelitis [1, 2]. The neighboring soft tissue infections and tenderness on percussion is considered
PS has far-reaching clinical implications from direct inoculation in the context the most common sign elicited on clinical
for patients by increasing disability re- of spine surgery [1, 12]. Staphylococcus examination [17]. Fever is not uniformly
flected in lower health-related quality of aureus is the most common non-tubercu- reported. In one case series, fever was
life (HRQoL) scores [3]. It could result losis pathogen incriminated in PS. In the reported in 8 patients out of 59 [17].
in septicemia, irreversible spinal cord in- context of postspinal fusion PS, the main This could be because analgesic medica-
jury, neurologic deficits, has a mortality causative pathogens are coagulase-nega- tions are administered [1]. Neurological
which of 4–29% [4, 5] and spinal de- tive staphylococci and Cutibacterium ac- deficits such as motor or sensory loss as
formity with debilitating complications nes [1, 10, 12]. In the setting of chronic well as loss of sphincter control are also
as a result of prolonged vertebral disc bacteremia, low-virulence bacteria, such commonly associated with PS [18]. Di-
destruction from chronic infections [6]. as coagulase-negative bacteria [1, 13] are agnosing PS remains challenging due to
The PS primarily impacts older people implicated. The avascular nature of the its insidious course and high incidence
with underlying comorbidities, such as intervertebral disc provides a safe milieu and prevalence of back pain in the gen-
diabetes, heart disease, immunosuppres- for bacterial seeding. Moreover, bacte- eral population [1]. Healthcare providers
sive disorders, use of intravenous drugs, rial seeding at the arterioles of vertebral should exercise a high index of suspicion
renal failure necessitating hemodialysis endplates paves the way for an increased of this condition and should apply sound
and cancer [1, 7, 8]. The incidence of intraosseous pressure which contributes clinical judgement on the basis of clini-
PS has been documented at 2.4 cases per to lower blood flow in the infected re-
100,000 population and increases with gion [6, 14]. Hence, prolonged antibiotic
Abbreviations
age (from 0.3 per 100,000 among patients treatment for PS is warranted to eradi-
ASIA American Spinal Injury Association
under 20 years of age to 6.5 per 100,000 cate the infection [6, 14]. In a multicenter
among patients older than 70 years) [1, study of 253 patients with PS, McHenry CRP C-reactive protein
9]. It has also been shown that it could et al. delineated the primary source of CT Computed tomography
affect any age group. Some studies have infection. The predominant infection fo-
reported a bimodal age distribution with cus was urinary tract, skin, or soft tissue ESR Erythrocyte sedimentation rate
peaks in patients whose age is less than infection such as endocarditis or septic HRQoL Health-related quality of life
20 years and in the group of patients aged arthritis or an intravenous access [1, 12].
IDSA Infectious Disease Society of
over 50 years [1, 10, 11]. It mainly af- Symptomatology of PS is insidious [1]. America
fects males with a male to female ratio The most common initial clinical feature
MRI Magnetic resonance imaging
of 1.5–2:1 [1, 10, 11]. An increase of is back pain and the location correlates
PS incidence in Europe and the USA has with the site of infection [1]. Exacerba- PS Pyogenic spondylodiscitis
tion of pain at night could be considered ROM Range of motion
The manuscript does not contain information an warning sign; however, it was reported
about medical device(s)/drug(s). that up to 15% of patients did not experi- SEA Spinal epidural abscess
482 Der Orthopäde 6 · 2020
cal manifestation, laboratory results and report: 7 papers whose main focus was cases with epidural abscess formation
imaging characteristics [1, 4]. In the light back pain and not spondylodiscitis were without vertebral or disc involvement.
of the broad differential diagnosis of low excluded. In total, three major classi- Treatment of this subtype was posterior
back pain even in the context of a febrile fication systems were proposed in the decompression via hemilaminectomy
patient with neurologic deficits, many PS literature. These classifications were de- and drainage of epidural abscess.
diagnoses are missed. A delay in the di- signed to encompass the most important
agnosis of almost 2 months has been re- clinical, anatomical and biomechanical Type 2. Patients with a physiological
ported [19]. For example, the initial diag- factors essential to decide the next best sagittal alignment but with neurologic
nosis of PS in a study of 109 patients with step in management. deficits and epidural abscess with ver-
Staphylococcus aureus bacteremia was ac- In total five criteria were proposed: tebral disc involvement. Treatment of
curately done in only 5% [15, 20]. Even in 1. Neurological deficits choice is decompression, stabilization
cases of correct diagnosis, management 2. Abscess formation and vertebral body replacement via cage
is still controversial. Many classification 3. Segmental instability implantation.
systems and algorithms of management 4. C-reactive protein (CRP)
have been reported [11, 21, 22]; how- 5. Pain Type 3. Includes patients withabscess for-
ever, these systems could be considered 6. MRI morphological findings. mation without specification of abscess
too complex and immature to reach con- type. Furthermore, this type includes
sensus. The Infectious Diseases Society PS classification systems cases with compression fracture of less
of America (IDSA) published the first than 50% of the vertebral body and seg-
guidelines on antibiotic treatment of PS Akbar et al. developed a classification of mental kyphosis of less than 25°. De-
and paved the way for more standardized PS based on a retrospective clinical and pending on the neurological symptoms,
treatment [4]; however, in the absence of radiological analysis of 221 patients who this type is subclassified into A) no neu-
a straightforward, evidence-based surgi- underwent surgical treatment [21]. They rologic deficits and B) with neurologic
cal classification of PS, the management concluded that spondylodiscitis without deficits. Treatment of choice was an-
approach is still too complex, controver- significant bone destruction, deformity terior debridement with vertebral body
sial and is reliant on the best judgment or neurologic deficits should be treated replacement and stabilization for type A
of the surgeon. with immobilization and antibiotic ther- and posterior decompression and stabi-
The aim of this paper was to review apy and that treatment should be dictated lization for type B.
the most recent classification systems and by the extent of the inflammation. Fur-
critically appraise the classification cri- thermore, they argued that that choice of Type 4. includes cases with more severe
teria suggested to healthcare providers surgical approach should be performed spinal deformation encompassing com-
when faced with a case of PS. according to the philosophy of the spine pression fracture of more than 50% and
center. Criteria for surgical treatment en- segmental kyphosis with abscess forma-
Material and methods compassed intractable pain, abscess for- tion with or without neurologic deficits.
mation, neurological status and spinal Treatment of this type included decom-
Search methodology instability with segmental kyphosis of pression anterior and posterior stabiliza-
more than 25° and vertebral compres- tion
An advanced PubMed search of titles ab- sion fracture. As a result, 7 subtypes Furthermore, Akbar et al. modified
stracts was conducted utilizing the terms were proposed: their classification to include spondy-
Classification AND Spondylodiscitis OR lodiscitis of the cervical spine [23]. Simi-
septic discitis OR spinal osteomyelitis OR Type 0. No neurologic deficits, no ab- larly, type 0 is without abscess formation
vertebral osteomyelitis OR vertebral in- scess formation and no bony destruc- or bony destruction. The treatment of
fection OR spinal infection. No filters tion. Treatment of choice is immobi- choice is a cervical brace and immobi-
pertaining to language of publication or lization with an orthosis and antibiotic lization and antibiotic treatment. Type 1
date of publication were applied. The bib- treatment. includes cases with neurologic deficits,
liographies of the relevant papers were epidural abscess and vertebral disc in-
retrieved and manually scanned for rele- Type 1 A. No neurologic deficits. This volvement; however, patients with type 1
vance. Furthermore, systematic reviews type encompassed cases with psoas ab- have a physiological sagittal profile with
on the different criteria for classifying PS scess without vertebral or disc involve- no bony destruction or deformity. The
were manually searched and discussed. ment. Treatment of this subtype was CT- treatment of choice is anterior or pos-
guided drainage of abscess or surgical de- terior decompression and stabilization.
Results bridement and drainage depending on Type 2 includes cases with bony destruc-
the size of the abscess. tion and segmental kyphosis with neuro-
A total of 43 articles were retrieved com- logic deficits (type 2A) or without neu-
prising 23 retrospective case series, 5 re- Type 1 B. Patients who presented with rologic deficits (type 2B). If the case was
views, 2 letters to the editor and 1 case neurologic deficits and encompassed monosegmental or bisegmental spondy-
Der Orthopäde 6 · 2020 483
Abstract · Zusammenfassung
Orthopäde 2020 · 49:482–493 https://doi.org/10.1007/s00132-019-03836-0
© Springer Medizin Verlag GmbH, ein Teil von Springer Nature 2019
H. Almansour · W. Pepke · M. Akbar
Pyogenic spondylodiscitis. The quest towards a clinical-radiological classification
Abstract
Background. Pyogenic spondylodiscitis (PS) is spondylodiscitis and its classification. No too complex for interdisciplinary clinical
a debilitating condition laden with orthopedic restrictions regarding language of publication practice and do not adequately address
and neurological complications. The choice of or date of publication were applied. unique entities, such as PS of the cervical
the best step in management is often delayed Results. A total of 43 papers with 5 encom- spine, anterolisthesis and retrolisthesis. Most
due to the controversy encompassing its passing 3 main classifications were found importantly, some criteria must be utilized in
multiple facets. Several classification systems in the literature. These classifications were concert with recently published guidelines
were proposed in the literature to define overlapping but different. They encompassed and should be re-assessed for validity and
optimal management; however, consensus neurologic deficits, abscess formation and reliability. A uniform orthopedic parlance is
was not achieved. segmental instability, laboratory parameters required to optimize the management of this
Objective. The aim of this study was to review and morphological changes in magnetic debilitating and life-threatening condition.
the literature and critically appraise the resonance imaging (MRI) as the most
classification systems of PS and the rationale important factors used to classify PS, assess Keywords
behind the classification criteria. the severity and guide treatment. Vertebral osteomyelitis classification ·
Methods. A literature search was conducted Conclusion. The current classification schemes Surgery · Neurologic deficits · Epidural
in PubMed. Titles and abstracts of articles overlap and encompass the most clinically abscess · Segmental instability
were searched using different synonyms of relevant factors; however, some could be
Pyogene Spondylodiszitis. Die Suche nach einer klinisch-radiologischen Klassifikation
Zusammenfassung
Hintergrund. Die pyogene Spondylodiszitis ihrer Klassifikation durchsucht. Sowohl dieser Klassifikationen könnten jedoch
(PS) ist eine lebensbedrohliche Erkrankung die Veröffentlichungssprache als auch für die interdisziplinäre klinische Praxis zu
mit zahlreichen orthopädischen und das Veröffentlichungsdatum stellten kein komplex und im klinischen Alltag schwere
neurologischen Komplikationen. Die Wahl Ausschlusskriterium dar. zu handhaben sein. Auch werden einzelne
des besten Therapieschrittes wird aufgrund Ergebnisse. Iinsgesamt wurden 43 Artikel Entitäten wie z. B. die PS der Halswirbelsäule,
der facettenreichen Darstellung des Krank- gefunden, von denen 5 Arbeiten 3 ver- die Antero- und die Retrolisthese nicht
heitsbilds häufig verzögert. In der Literatur schiedene Klassifikationen aufwiesen. Diese adressiert. Am wichtigsten ist, dass einige der
wurden mehrere Klassifikationssysteme zur Klassifikationen überschneiden sich, auch enthaltenen Kriterien in Übereinstimmung
Entscheidungsfindung vorgeschlagen, um wenn sie sich zum Teil unterscheiden. Sie mit den kürzlich veröffentlichten Leitlinien
ein optimales Therapie-Management zu umfassen die wichtigsten Parameter wie das verwendet werden müssen und auf ihre
definieren. Ein Konsens wurde jedoch nicht neurologische Defizit, die Abszessbildung und Validität und Reliabilität überprüft werden
erreicht. die segmentale Instabilität sowie Laborpara- sollten. Eine einheitliche orthopädische
Fragestellung. Das Ziel dieser Studie ist es, meter und morphologische Veränderungen Klassifikation ist erforderlich, um das
die Literatur bezüglich der vorhandenen in der Magnetresonanztomographie (MRT) Management dieser lebensbedrohlichen
Klassifikationen der PS zu überprüfen und zur Klassifizierung der PS, zur Einschätzung Erkrankung zu optimieren.
die Klassifizierungsparameter kritisch zu des Schweregrades und zur therapeutischen
bewerten. Entscheidungsfindung. Schlüsselwörter
Methoden. Eine Literaturrecherche wurde Schlussfolgerungen. Die aktuell publizierten Klassifikation · Operative Therapie · Neurologi-
mit PubMed durchgeführt. Titel und Abstracts Klassifikationen zeigen bezüglich des sche Defizite · Epiduraler Abszess · Segmentale
von Artikeln wurden mit verschiedenen Aufbaus Überlappungen und umfassen die Instabilität
Synonymen der Spondylodiszitis und klinisch relevantesten Parameter. Einige
lodiscitis (one vertebra), the treatment of tion. It was divided into three types A, B, Type B. Included cases withbonydestruc-
choice was anterior decompression with and C which were then subdivided into tion or instability without neurological
vertebral body replacement. If the infec- a total of 11 subtypes: impairment or abscess formation. This
tion was multisegmental, then posterior- type was further divided into B1–B3
anterior instrumentation with vertebral Type A. Cases with biomechanical insta- and included cases with bony destruc-
body replacement was chosen. Similarly, bility without abscess or neurological im- tion without instability, cases with bony
Pola et al. [11] recently suggested a clini- pairment. Divided into A1–A4, ranging destruction with paravertebral exposure
coradiological classification encompass- from simple discitis to bilateral intra- and bony destruction with segmental
ing the most important prognostic factors muscular abscesses. Management of this kyphosis. Segmental instability was de-
in the sphere of PS: neurologic deficits, type ranged from using a rigid orthosis fined as a segmental kyphosis of more
segmental instability and abscess forma- to percutaneous stabilization. than 25°. Management of this type
484 Der Orthopäde 6 · 2020
ranged from rigid orthosis and immo- ate and severe spondylodiscitis, respec- ties of patients which have a pivotal role
bilization to open stabilization. tively. Each category is given 3 points, in deciding the right treatment [25, 26];
CRP is given 0, 1, 2 and 3 points when however, this should not stand as an ob-
Type C. Encompassed cases with acute CRP (mg/dl) is under 10, between 10–50, stacle in the way of developing a common
neurological impairment or formation between 51–150 and over 150, respec- language that clinicians can utilize as ori-
of an epidural abscess. It was subdivided tively. Pain on a numerical rating scale entation, a lingua franca that is easy to
into four classes (C1–C4). The worst case is given 0, 1, 2 and 3 points when pain is handle and would be a part of the medi-
scenario was classified as C4 with pres- under 3, between 3–5, between 3–8, and cal parlance in terms of spondylodiscitis
ence of an epidural abscess, acute neu- over 8, respectively. The MRI morpho- [25, 26].
rological impairment and segmental in- logical changes are given 0, 1, 2 and 3
stability whose management ranged from points when there are no MRI changes Limitations of the current
rigid orthosis immobilization to open de- indicating PS, when there is a spondylitis classification systems
bridement and stabilization. or discitis, when there is spondylodisci-
Finally, Homagk et al. [22] intro- tis, and when there is spondylodiscitis Current classification systems lack im-
duced the spondylodiscitis severity score with abscess formation, respectively. In portant factors which could be consid-
(SSC) and classified PS cases of the tho- contrast to the other static classification ered pivotal for the next evolutionary
racic and lumbar spine into three grades schemes, they developed a dynamic eval- step of a PS classification. The reli-
of severity depending on clinical and uation score which could be utilized to ability of these classification has not
neurological status, morphological ver- modify treatment according to disease been tested. A classification should be
tebral destruction and instability. Each progression. considered a measurement instrument
severity grade is subclassified if neighbor- whose inter-rater and intra-rater relia-
ing tissue was involved in the inflamma- Discussion bility should be tested [28]. Moreover,
tion (A) or not involved (B). They sug- a sound psychometric evaluation of these
gested conservative treatment only for Principles and rationale behind the classifications has not been performed.
a low-grade spondylodiscitis (grade 1) genesis of a PS classification These classifications were developed as
and patients whose comorbidities pro- an expert opinion and retrospectively
hibit surgery [22]. Henceforth, six sub- A clinically relevant classification should validated on a patient series in a single
types were proposed: accurately delineate all potential varia- center. Hence, an objective validation
4 Severity grade I A/B: no neurologic tions of PS, assist in the documentation, did not occur. Content validity was also
deficits or segmental instability or enable an efficient lingua franca among not tested. This is type of validity that
spinal canal stenosis. The tratment international peers and assign clear steps examines the extent to which diagnostic
of choice is conservative or posterior in management. Most importantly, it parameters of the severity measure make
stabilization. should be able to prognosticate different intuitive sense [26]. Consensus building
4 Severity grade II A/B: no neurologic treatment outcomes [25]. Development approaches such as the Delphi surveys
deficits with segmental instability and of a classification is not a static process but were not conducted and hence no content
kyphosis due to vertebral destruction. a dynamic continuum requiring multi- validity of the classification criteria could
The treatment of choice is posterior ple recalibrations and modification until be established [26]. This introduces an-
stabilization in the thoracic and it gains acceptance of the international other limitation that these classifications
lumbar spine. After a 3-month community [26]. Mirza et al. summa- although somehow overlapping lack
interval, the necessity of anterior rized the principles underlying an ideal “globality”. Mirza et al. defined globality
stabilization was determined on CT classification system. These include fac- as the ability of a classification system
scans to check for anterior fusion. tors such as identification, comprehen- to transcend a single describing author’s
4 Severity grade III A/B: all cases siveness, inclusiveness, concise and de- vision and hold a consistently mean-
with neurologic deficits regardless of scriptive terminology, treatment guid- ingful application to interested parties
other factors. Treatment of choice is ance and ability to predict outcomes [26]. outside an organizational or geographic
immediate two-staged stabilization The Institute of Medicine stated that the philosophy [21, 26]. Neurologic deficits,
surgery with a short interval. following factors are critical to the de- abscess formation and segmental in-
velopment of sound treatment guidelines stability are generally accepted criteria
Homagk et al. then modified the SSC such as: validity, reliability, reproducibil- [29]; however, the minute details used
to spondylodiscitis diagnosis and treat- ity, clinical applicability, clinical flexi- to stratify patients should be validated
ment (SponDT) based on three charac- bility, clarity, multidisciplinary process, in a multicenter study.
teristics: CRP, pain and MRI morpho- review of evidence, and documentation
logical changes [24]. The score is used [27]. It is of note, that there is no per-
to stratify the severity of PS. It ranges fect classification that could encompass
from 0 to 9. Scores under 3, 3–6 and the wide spectrum of individual cases
over 6 are classified as light, moder- and cover all variations and comorbidi-
Der Orthopäde 6 · 2020 485
Übersichten
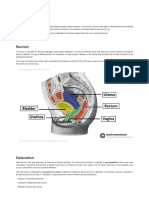
Fig. 1 8 a–k Different scenarios of abscess formation. a, c, e and g Schematic representations of a vertebra showing the spinal
canal and the spinal cord (blue) and the psoas muscle (brown). Paraspinal abscess and epidural abscess are shown (red). b, d,
fandh Axial MRIimages showingparaspinal andepidural abscesses.iSagittal schematic representationofthe spine depicting
an epidural abscess. j and k MRI of the cervical and lumbar spine of patients presenting with an epidural abscess
Critical appraisal of the discussed discussed did not take comorbidities spine surgeon [33]. It is clear that further
classification criteria into consideration. studies are warranted to determine who
benefits from whichintervention[33, 34];
Neurologic deficits Abscess formation however, ethical considerations hamper
A clearrecommendationechoing through A common complication of PS is infec- randomization efforts for treatment op-
the literature that the presence of pro- tion seeding from neighboring compart- tions of SEA. Some authors even admit
gressive neurologic deficits is a clear ments leading to epidural, paravertebral that conducting high-level evidence stud-
indication for surgical treatment. In or psoas abscess formation (. Fig. 1a–k). ies on this debilitating condition might
a systematic review of the clinical fea- In a multicenter study of 7 centers with be considered utopic [33, 34]. Hence,
tures of PS, the authors observed that 253 patients, an epidural abscess in was retrospective reviews might be the sole
38% of patients suffered from neurologi- found in 17% of cases and a paravertebral source of information upon which sound
cal dysfunction, such as sensory deficits, abscess in 26% [12]. Similar to PS, the in- clinical judgement and classification sys-
motor weakness or paralysis, radicu- cidence ofa spinal epidural abscess (SEA), tems could be built. Similar to PS, an
lopathy and loss of sphincter control. a debilitating and life-threatening com- SEA could be located in the cervical,
In almost one quarter of these patients, plication, is on the rise. The incidence of thoracic and lumbar spine with its own
paresis or paralysis was reported [10]. SEA was cited as being between 0.2 and unique characteristics; however, the cur-
Paralysis and severe muscular weak- 12.5 cases per 10,000 hospital admissions rent classification systems give general
ness were associated with certain risk [30, 31]. If treatment is delayed, the pa- expert opinion and criteria for surgi-
factors, such as increasing age at diagno- tient could be inflicted with irreversible cal treatment without discriminating be-
sis, steroid-induced immunosuppression neurological dysfunction [30, 32]. tween these unique entities [30]. Cervical
and diabetes. Therefore, considering the Many authors consider a SEA with- SEA has a lower infection rate than the
presence of neurologic deficits was an out neurologic deficits as an indication thoracic or lumbar spine; however, it has
important criterion to utilize in the clas- for surgery [15, 21]. In the literature been associated with a much more debil-
sification and treatment guidance of PS the decision for conservative versus sur- itating functional outcomes and higher
[4, 29], which was used in the three PS gical treatment seems to be contingent mortality [31]. Thus, some authors con-
classification systems discussed [11, 21, on patient’s neurological status, comor- sider it a unique entity the management
22]; however, the classification systems bidities, resources and preferences of the of which should not be the same as tho-
486 Der Orthopäde 6 · 2020
Fig. 2 9 a Sagittal
schematic representa-
tion of a spine with bone
destruction and epidural
abscess (red) without in-
stability. b and c Sagittal
CT and MRI of patients
presenting with PS without
instability
racic or lumbar SEA [30]. An explanation comes with immediate surgical interven- Spinal segmental instability
could be that the neurological level of in- tion and antibiotics [30]. Defining segmental instability is a con-
jury if one occurs is higher and hence the Hadjipavlou et al. analyzed neu- troversial topic [39]. Previous biome-
resulting spinal cord injury would have rological outcomes following spinal chanical studies defined instability in the
more dramatic consequences. In two of decompression for SEA and observed context of degenerative disease and not
the largest studies on cervical SEAs, it was a significantly higher rate of paraplegia/ inflammatory disease. Nonetheless, one
observed that 47–77% of patients with paraparesis prior to surgery and a sig- could utilize the established methods
cervical SEA presented with some form nificantly worse outcome postsurgical to build a consensus and then recali-
of a neurological deficit from a paresis of outcome in patients with SEA at the brate and reconfigure as the classification
one extremity to a complete tetraplegia thoracic level compared with the lumbar evolves. The concept of stability or in-
[30, 35, 36]. Furthermore, in a system- spine [34]. Hence, early identification stability seems to be a qualitative more
atic review and meta-analysis on cervical and a prompt surgical decompression in than a quantitative criterion that lacks
SEA, the authors noted that the major- the context of progressive neurological evidence-based recommendations and
ity of studies on SEA combined cervical, deterioration is a reasonable approach radiological thresholds [40]. The spine
thoracic, and lumbar abscesses together to mitigate morbidity or mortality in is a complex biomechanical apparatus
hindering conclusions specific to cervi- patient with cervical and thoracic SEA in which three-dimensional kinematics
cal SEA [30]. It was suggested that ear- [34]. are exerted [40, 41]. Furthermore, with
lier surgical intervention could be ben- Lumbar SEAs are less likely to cause its physiological cervical, thoracic and
eficial in safeguarding neurological out- complications in spondylodiscitis, result lumbar curvature the segmental range
come; however, it is an elusive matter in neurologic deficits or lead to symp- of motion (ROM) differs according to
to accurately define this patient popula- tomatic neural compression [33]. A sys- anatomical location. For instance, the
tion. This is because the rate of symptom tematic review of lumbar SEA demon- lumbar spine enables increased cephalo-
progression from back pain to complete strated that surgically treated patients caudal ROM while the lumbosacral joint
paralysis varies between individuals and presented more often with worse physical enables more sagittal ROM in flexion-
the current literature does not provide a symptoms and neurologic deficits evident extension. On the other hand, lateral
clear delineation of who profits from early in their worse ASIA motor level scores. bending and axial rotation ROM is almost
surgery vs. conservative treatment [30, Interestingly, there seem to be only a few equal along the entire spine with the ex-
37, 38]. Khanna et al. described a faster significant differences in treatment out- ception of the lumbosacral joints which
neurological deterioration in cervical and comes between surgically vs. medically exhibit the least lateral ROM [42]. Hence,
thoracic SEA than lumbar SEA due to the treated patients [33]. Noteworthy, is that In the context of inflammation it could
quicker compression of the spinal cord the most important prognostic factor of be postulated that the location of the in-
and smaller diameter of the spinal canal good neurological outcome was the ini- fected vertebra determines the pattern of
[38]. The aforementioned findings un- tial status before surgery. The authors instability (. Fig. 2a–c). A perturbation
derline a need for randomized clinical further noted that the current evidence of a spinal segment leads to dysfunc-
studies aimed at comparing the efficacy supporting surgical treatment of lumbar tional kinematics of multidirectional
of different surgical approaches based on SEA as the main recommendation lacks coupled motions of the spinal segment
location of the abscess. The majority of quality due to the deficiency of clinical [40]. To understand segmental stabil-
studies included reported improved out- trials comparing medical versus surgical ity or its opposite, instability, a sound
treatment [33]. understanding of spinal kinematics is
Der Orthopäde 6 · 2020 487
Übersichten
Fig. 3 8 a Sagittal schematic representation of the spine depicting anterolisthesis.b Sagittal CT of the spine illustrating an-
terolisthesis of L3–L4 with bone destruction. c Sagittal schematic representation of the spine depicting retrolisthesis.d Sagit-
tal CT of the spine illustrating anterolisthesis of L2–L3 with bone destruction
necessary [40, 41]. Each spinal motion tally unstable. This measurement could in vivo analysis was not conducted which
segment is comprised of two vertebral be done in normal resting radiographs. hampers their clinical utility.
bodies and the connecting ligaments. They also considered 2 mm of posterior Many studies have been conducted to
Each segment exhibits three types of translation to be the threshold of insta- assess the segmental instability of the tho-
kinematics, translation, angulation and bility. This threshold was suggested af- racic and cervical spine; however, these
rotation in six degrees of ROM. Hence, ter they conducted a thorough analysis criteria are not as comprehensive as the
stability or instability should be assessed of resting radiographs in the acute trau- criteria suggested by White and Pan-
accordingly [43]. Current classification matic setting and in the nonacute setting jabi and hence there is a certain reluc-
and recommendations take only sagittal of the lumbar spine [42, 44]. Further- tance to utilize them in future classifica-
instability into consideration. more, the authors studied segmental an- tions. Noteworthy, all proposed criteria,
Spinal stability is an instrumental req- gulation and after analyzing in vivo and including the ones by White and Pan-
uisite for its function in protecting neural in vitro studies of normal resting sagit- jabi [42], describe instability either in
structures [40]. Clinical instability was tal posture of the lumbar spine. sug- a physiological, traumatic or degenera-
defined by White and Panjabi [42] and gested that segmental angulation greater tive setting. None were described in the
Panjabi [44] as the inability of the spine of 22°should be considered unstable. In setting of vertebral osteomyelitis. Ak-
to safeguard its normal displacement un- the context of degenerative lumbar in- bar et al. [21] and Pola et al. [11]
der physiological loads in which there is stability Vaccaro and Ball considered an considered a sagittal kyphosis of more
no resulting neurologic deficits, incapac- angulation of more 10° as unstable [46]. than 25° as a threshold to define seg-
itating deformity or severe pain. In other In the context of dynamic radiographs, mental instability. It is, however, unclear
words, the American Academy of Ortho- authors suggested a segmental axial ro- why both groups of authors chose this
pedic Surgeons defined stability as “the tation of more than 15° at L2-L3, L3-L4, threshold highlighting the lack of objec-
capacity of the vertebrae to remain cohe- L4-L5 or greater than 25° at L5-S1 [42]. tivity and lack of quantifications meth-
sive and to preserve the normal displace- In the setting of cervical instability, John- ods regarding this controversial issue.
ments in all physiological body move- son et al. [47] defined instability as when Moreover, anterolisthesis and retrolisthe-
ments” [45]. There are many proposed there is 3.5 mm translation or when there sis (. Fig. 3a–d) were not considered [40].
techniques of measurement of instability is more than 11° of rotation difference Homagk et al. did not include segmental
in the literature. Albeit the most accepted of two subjacent vertebrae measured on instability in their severity score which
threshold was coined by White and Pan- lateral X-rays (resting or flexion-exten- could constitute a major limitation of us-
jabi [42, 44]. White and Panjabi consid- sion). In the context of thoracic insta- ing their classifying instrument [22, 24].
ered all the thresholds suggested in the bility, a horizontal translation of 2.5 mm Finally, in a systematic review by Her-
literature and suggested that 4.5 mm of (on lateral X-ray) or 5° of angulation of ren et al. they found the criterion for in-
anterior translation should be the thresh- two subjacent vertebrae may be consid- stability was segmental kyphosis greater
old upon which clinicians should con- ered as signs of instability [48]; however, than 15°. Similarly, this statement was
sider the lumbar spine to be segmen- these were biomechanical studies and an global and does not consider the loca-
488 Der Orthopäde 6 · 2020
Fig. 4 9 a Sagittal
schematic representa-
tion of the spine depicting
inflammation of vertebrae
and intervertebral disc
(red) as well as the result-
ing segmental kyphosis.
b Sagittal CT of the cervical
spine illustrating bone de-
struction with segmental
kyphosis. c Sagittal CT of
the thoracic spine illustrat-
ing bone destruction with
segmental kyphosis
tion of this kyphosis [29]. In light of aspect is mostly affected in advanced PS Defining failure of conservative
these discrepancies, it could be suggested [5]. Therefore, many surgeons prefer an- treatment
that segmental kyphosis of any degree in terior debridement in otherwise healthy
any spinal segment should be regarded patients who might not need posterior There is no consensus between authors on
as a criterion for instability (. Fig. 4a–c). stabilization [5]. To date and to the the exact definition of failure of PS treat-
This suggestion arises from the fact that best of the authors knowledge, there are ment. Unlike many published studies on
that the current knowledge about the no randomized controlled trial proving PS the IDSA guidelines considered per-
topic of spinal instability in general and the efficacy of a single surgical approach sistent pain, residual neurologic deficits,
especially in the setting of inflammation over another [4]. Hence, all suggested elevated markers of systemic inflamma-
is far too immature, which hampers its approaches by the authors of PS classi- tion or radiographic findings alone do
clinical and radiological utility [41]. On fications remain subjectively controver- not necessarily signify treatment failure
the other hand, an avalanche of biome- sial and an evidence-based answer to in treated PS patients [4]. Alternatively,
chanical and radiological studies is un- the superiority of an approach in a cer- the IDSA proposed a definition to stan-
derway to help enlighten the way towards tain clinical scenario remains unattained. dardize reporting of PS treatment out-
a more objective and clinically relevant The timing of surgery is also controver- comes. Failure of treatment was defined
definition of instability. sial. Segreto et al. retrospectively ana- as a persevering infection with a pos-
lyzed almost 34,500 patients with PS and itive microbiological detection in spite
Surgical management of PS and its stratified them according to the delay of of administration of targeted antibiotic
indications surgery. Subsequently, the authors an- treatment. The authors also noted that
alyzed the postoperative outcomes and defining failure based solelyonlaboratory
First-line treatment of PS is usually con- concluded that patients who underwent findings, radiographic surrogate markers
servative via antibiotics [5]; however, it surgery within 24 h after admission had and clinical status of the patient with-
has previously been reported that up to better outcomes than patients with de- out inclusion of microbiological detec-
40–50% of patients suffering from PS will layed surgery who suffered more postop- tion may overestimate treatment failure
eventually require surgical intervention erative complications and increased mor- and lead to exaggerated medicinal or sur-
[4, 5]. The goals of surgical treatment are bidity [5]. The IDSA guidelines stated gical treatment [4].
to eradicate the spinal infection, safe- that progressive neurologic deficits, im-
guard blood perfusion to the infected minent instability, persistent septicemia, Utility of inflammatory markers,
tissue, decrease pain and establish seg- adamant backpain and formation of an back pain and MRI as indices for
mental stability [15, 29]. There are many epidural abscess despite adequate antibi- assessing treatment
proposed surgical approaches in the lit- otic treatment constitute valid indica-
erature. These include anterior and/or tions for surgical treatment ([4], . Fig. 5). Inflammatory markers (CRP), pain and
posterior surgery, staged vs. single and MRI findings represented the main pil-
with or without stabilization. The ante- lars upon which the severity score of
rior aspect of the vertebrae is most af- Homagk et al. was designed [22, 24].
fected by the infection. The posterior Many authors consider adamant fever,
Der Orthopäde 6 · 2020 489
Übersichten
toms and inflammatory markers. The
IDSA recommends follow-up MRI spe-
cially to monitor paraspinal and epidu-
ral abscesses in patients not respond-
ing to treatment. An explanation could
be that MRI changes frequently perse-
vere or could even be aggravated during
treatment in spite of clinical improve-
ment [15, 56]. Performing a follow-up
MRI sooner than 4 weeks could lead to
a lower threshold of preforming surgery
and an unnecessary lengthy antibiotic
treatment [4, 57]. Interestingly, morpho-
Fig. 5 8 Suggested treatment algorithm for patients presenting with back pain and a clinical pre- logical changes on MRI indicating persis-
sentation suspicious of PS. This algorithm is inspired by the literature review and constitutes the core tentinfectioncould be evidentformonths
treatment plan in this university hospital. N Neurologic deficits, A Abscess formation, S Segmental in-
to years in patients otherwise showing
stability, (0) no, (1) yes. When a patient presents with no neurologic deficits (N0), no abscess formation
on MRI (A0), and no segmental instability (S0), the next best step would be conservative treatment. clinical improvement [4, 57–59]. This
When conservative treatment fails then surgery is indicated.When a patient presents with progressive is another criticism of the MRI criteria
neurologic deficits (N1), epidural abscess (A1) or segmental instability (S1), the best next step would used by Homagk et al. to monitor dis-
be surgery ease progression. Nonetheless, Homagk
et al. address this fact in their score dis-
back pain or continuously elevated in- suspected of having treatment failure. In cussion [24]. On the other hand, total
flammatory markers (CRP higher than summary, an orchestrated assessment of loss of gadolinium enhancement and os-
30 mg/l) as predictors of management clinical status with systemic inflamma- seous healing are revealed late on MRI
failure [49, 50]; however, the advantage of tory markers should be applied to ac- in the course of the healing process [60].
obtaining follow-up inflammatory labo- curately measure efficacy of treatment Moreover, a clear discrepancy between
ratory markers (ESR, CRP) under antibi- [4]. Intuitively, persistent back pain in clinical symptoms and radiological signs
otic treatment for PS has not been con- a patient undergoing treatment for PS has been previously reported. For in-
firmed [4]. The CRP level is elevated in is alarming. In the multicenter study of stance, epidural enhancement and spinal
the majority of cases with spondylodisci- McHenry et al. [12], the most reported canal stenosis were revealed in patients
tis [51]. In a systematic review and meta- finding in patients who failed treatment with improving clinical symptoms [59].
analysis on spondylodiscitis Taylor et al. was persistent backpain. On the other In summary, targeted and suitably timed
showed that CRP was high (>10 mg/l) in hand, many authors including McHenry MRI follow-up should be cautiously con-
85% of patients (1083/1272). Elevated et al. consistently reported that “cured” ducted. A follow-up MRI is indicated
leukocyte counts were observed only in patients with PS complained of persist- especially in cases with an epidural or
43% (457/1052) of patients [6]. More- ing back pain [4, 12, 54, 55]. Therefore, paraspinal abscess to document the mor-
over, Carrage et al. observed that patients interpreting back pain as a main criterion phological response to treatment espe-
who are 60 years or older and immuno- to assess efficacy of treatment might not cially in patients who did not show a clin-
compromized patients had an increased be the best approach. The gold standard ical improvement on administering an-
likelihood to have a normal leukocyte diagnostic modality of PS is MRI of the tibiotic treatment for a suitable duration
count in the setting of an active PS [52]. spine, which has a specificity of 93% and [4]. As a possible solution to the dilemma
This signifies that the leukocyte count a sensitivity of 97% [4]. Increased sig- of assessing treatment failure, the IDSA
seems tobe the leasthelpful inflammatory nal intensity on T2-weighted images, de- proposed image-guided biopsy for ob-
marker. It has already been shown that creased signal intensity on T1-weighted taining histological samples and micro-
CRP correlates with the clinical symp- images and loss of delineation of verte- biological testing [4]. Facing a patient
tomatology of patients with PS [4, 50]. bral endplates are distinctive features of with suspected treatment failure repre-
Notwithstanding, it has been reported PS-induced changes of the vertebral body sents a true challenge. An individual-
that the majority of patients with persis- and neighboring discs [4, 15]. The sys- ized case by case approach incorporat-
tently increased inflammatory markers tematic review of Taylor et al. [6] revealed ing all the aforementioned factors and an
in a 4–8 week follow-up had a favor- that MRI scans accurately detected PS in interdisciplinary multidimensional pro-
able clinical outcome [4, 53]. The IDSA 94% (980/1045). Homagk et al. consid- cess comprising spine surgeons, neuro-
guidelines recommended that inflamma- ered MRI changes to be essential in their surgeons, radiologists and infectious dis-
tory markers should be reassessed after score to diagnose and monitor treatment eases specialists is warranted to tackle this
4 weeks of antibiotic treatment. Patients [22, 24]; however, IDSA guidelines [4] complex problem [4].
with unchanged or worsening inflamma- advised against follow-up MRI in patients
tory markers after 4 weeks should be who exhibited improved clinical symp-
490 Der Orthopäde 6 · 2020
be validated in a multicenter study in For this article no studies with human participants
Conclusion or animals were performed by any of the authors. All
which multiple cases of PS are presented studies performed were in accordance with the ethical
A PS remains a real challenge despite to orthopedic surgeons of all career stages standards indicated in each case.
the recent advances in early diagnosis and tested for feasibility, validity, inter-
and treatment strategies. The goals of rater and intrarater reliability. Despite the
treatment are to eradicate the infection, fact that PS of the cervical spine is asso- References
safeguard neurological function and halt ciated with worse neurological outcome,
the progress of deformity. In the con- the discussed classification systems do 1. Zimmerli W (2010) Vertebral osteomyelitis. N Engl
J Med 362(11):1022–1029
text of interdisciplinary management of not take this point into consideration. 2. Pola E et al (2018) Multidisciplinary management
PS, a clinically utile orthopedic classi- Spinal epidural abscesses could be lo- of pyogenic spondylodiscitis: epidemiological
fication should be kept clinically and cated in the cervical, thoracic and lumbar and clinical features, prognostic factors and long-
term outcomes in 207 patients. Eur Spine J
radiologically as simple as possible to spine, each with its own unique charac- 27(2):229–236
suit spine professionals and surgeons of teristics; however, the current classifica- 3. Lu M-L et al (2015) Transforaminal lumbar
all training expertise. Thus far, there tion systems give general expert opinion interbody debridement and fusion for the
treatment of infective spondylodiscitis in the
is neither a uniform orthopedic classi- and criteria for surgical treatment ubiq- lumbar spine. Eur Spine J 24(3):555–560
fication system nor a treatment algo- uitously without discriminating between 4. Berbari EF et al (2015) 2015 Infectious Diseases
rithm to guide its management. This these unique entities. Lastly, none of Society of America (IDSA) clinical practice
guidelines for the diagnosis and treatment of
controversy could be the culprit behind the classifications considered concomi- native vertebral osteomyelitis in adults. Clin Infect
overtreatment or undertreatment result- tant patient comorbidities which could Dis 61(6):e26–e46
ing in increased postoperative complica- downplay their clinical utility. 5. Segreto FA et al (2018) Vertebral osteomyelitis:
a comparison of associated outcomes in early
tions and increased costs burden to the In summary, an orchestrated assess- versus delayed surgical treatment. Int J Spine Surg
health economic system [5]. Published ment of clinical signs, serological results, 12(6):703–712
classification systems encompass clini- radiographic changes on MRI and a well- 6. Taylor DG et al (2018) Presentation and outcomes
after medical and surgical treatment versus med-
cal and radiological criteria to classify defined approach to defining stability or ical treatment alone of spontaneous infectious
and guide the management of PS. The imminent segmental instability should be spondylodiscitis: asystematicliteraturereviewand
presence or lack of neurologic deficits, applied. In light of the current literature meta-analysis. Global Spine J 8(4_suppl):49S–58S
7. Stoeckle M et al (2008) The role of diabetes mellitus
abscess formation and segmental insta- and published guidelines, depending on inpatientswithbloodstreaminfections. SwissMed
bility, increased inflammatory markers surrogate markers alone could falsely sig- Wkly 138(35):512
and MRI morphological changes repre- nify a persistent infection without a clin- 8. SobottkeRetal(2009)Treatmentofspondylodisci-
tis in human immunodeficiency virus-infected
sent the main pillars of these classification ical correlation. Hence, this approach patients: a comparison of conservative and
systems. The aim of these classifications could lead to overtreatment with unnec- operative therapy. Spine 34(13):E452–E458
is to establish a process-based and multi- essary surgery or lengthy antibiotic treat- 9. Grammatico L et al (2008) Epidemiology of
vertebral osteomyelitis (VO) in France: analysis of
dimensional rethinking of PS; however, ment. Hitherto, there is a lot of room for hospital-discharge data 2002–2003. Epidemiol
these systems do not take all the clinically evolution and improvement for current Infect 136(5):653–660
relevant factors into account and some classification systems of PS to reach in- 10. Mylona E et al (2009) Pyogenic vertebral os-
teomyelitis: a systematic review of clinical charac-
definitions used could not be considered ternational consensus. teristics. Semin Arthritis Rheum 39(1):10–17
evidence based. For instance, evidence- 11. Pola E et al (2017) New classification for the
based thresholds of defining segmental treatment of pyogenic spondylodiscitis: validation
Corresponding address studyonapopulationof250 patientswithafollow-
instability should be utilized in a future up of 2 years. Eur Spine J 26(4):479–488
classification taking specific spinal kine- M. Akbar, MD 12. McHenryMC, EasleyKA, LockerGA(2002)Vertebral
Department of Orthopaedic osteomyelitis: long-term outcome for 253 patients
matics dictated by the anatomic location
Surgery, Trauma Surgery and from 7 Cleveland-area hospitals. Clin Infect Dis
of the inflamed segments into considera- Spinal Cord Injury, Heidelberg 34(10):1342–1350
tion. The current discrepancies pertain- University 13. Bucher E et al (2000) Spondylodiscitis associated
ing to instability could motivate clinicians Schlierbacher Landstraße with bacteraemia due to coagulase-negative
200A, 69118 Heidelberg, staphylococci. Eur J Clin Microbiol Infect Dis
to consider segmental kyphosis of any de- 19(2):118–120
Germany
gree in any spinal segment as a sign of 14. Bernard L et al (2015) Antibiotic treatment for
michael.akbar@ 6 weeks versus 12 weeks in patients with pyogenic
instability. Moreover, they only consider med.uni-heidelberg.de vertebral osteomyelitis: an open-label, non-
angular instability and do not take ante- inferiority, randomised, controlled trial. Lancet
rior or posterior translation as criteria for 385(9971):875–882
instability into consideration. Unfortu- 15. Gouliouris T, Aliyu SH, Brown NM (2010) Spondy-
Compliance with ethical lodiscitis: update on diagnosis and management.
nately, current classification systems are guidelines J Antimicrob Chemother 65(suppl_3):iii11–iii24
only retrospectively validated in single 16. Sendi P, Bregenzer T, Zimmerli W (2008) Spinal
center retrospective studies and hence are epidural abscess in clinical practice. QJM
Conflict of interest H. Almansour, W. Pepke and 101(1):1–12
laden with biases signifying their lack of M. Akbar declare that they have no competing inter- 17. Wirtz DC et al (2000) Diagnostic and therapeutic
mature evolution which invites lack of ests. management of lumbar and thoracic spondy-
consensus. These classifications need to
Der Orthopäde 6 · 2020 491
Fachnachrichten
lodiscitis—an evaluation of 59 cases. Arch Orthop 40. Izzo R et al (2013) Biomechanics of the spine. Part I: Jetzt bewerben:
Trauma Surg 120(5-6):245–251 spinal stability. Eur J Radiol 82(1):118–126 RheumaPreis 2020
18. Eismont FJ et al (1983) Pyogenic and fungal 41. Izzo R et al (2013) Biomechanics of the spine. Part II:
vertebral osteomyelitis with paralysis. J Bone Joint spinal instability. Eur J Radiol 82(1):127–138 Beruflich aktiv trotz entzündlich-
Surg Am 65(1):19–29 42. White A, Panjabi MM (1990) Clinical biomechanics rheumatischer Erkrankung
19. BatemanJL,PevznerMM(1995)SpinalOsteomyeli- of the spine, 2nd edn. Lippincott Williams &
tis: a review of 10 years’experience. Orthopedics Wilkins, Philadelphia „Gemeinsam AufRheumen am Ar-
18(6):561–565 43. Gopinath P (2015) Lumbar segmental instability:
20. Jensen AG et al (1998) Bacteremic staphylo- points to ponder. J Orthop 12(4):165 beitsplatz“ – unter diesem Motto ruft
coccus aureus spondylitis. Arch Intern Med 44. Panjabi MM (1992) The stabilizing system of die Initiative RheumaPreis in diesem
158(5):509–517 the spine. Part II. Neutral zone and instability Jahr zum zwölften Mal dazu auf, sich
21. Akbar M et al (2011) Pyogenic spondylodiscitis hypothesis. J Spinal Disord 5:390–390
of the thoracic and lumbar spine: a new 45. Kirkaldy-Willis W (1985) Presidential symposium für die gleichnamige Auszeichnung
classification and guide for surgical decision- on instability of the lumbar spine: introduction. zu bewerben. Denn „aufzurheumen“
making. Orthopäde 40(7):614–623 Spine 10(3):254 gibt es noch immer vieles, wenn es
22. Homagk L et al (2016) Spondylodiscitis severity 46. Vaccaro AR, Ball ST (2000) Indications for in-
code: scoring system for the classification and strumentation in degenerative lumbar spinal darum geht, trotz einer entzündlich-
treatment of non-specific spondylodiscitis. Eur disorders. Orthopedics 23(3):260–271 rheumatischen Erkrankung weiter
Spine J 25(4):1012–1020 47. Johnson R, Panjabi M, Southwick W (1975) berufstätig zu sein.
23. Akbar M et al (2012) Pyogene Spondylodiszitis: Biomechanical analysis of clinical stability in the
Therapiealgorithmus und neue Klassifikation cervical spine. Clin Orthop Relat Res 109:85–96
zur therapeutischen Entscheidungsfindung (Leit- 48. Panjabi MM, Hausfeld JN, White AA (1981) A Die Initiative RheumaPreis in diesem Jahr
thema). Orthopäde 41(9):749–758 biomechanical study of the ligamentous stability
of the thoracic spine in man. Acta Orthop Scand
zum zwölften Mal dazu auf, sich für die
24. Homagk L et al (2019) SponDT (spondylodiscitis
diagnosisandtreatment): spondylodiscitisscoring 52(3):315–326 gleichnamige Auszeichnung zu bewer-
system. J Orthop Surg Res 14(1):100 49. Kowalski TJ et al (2006) Do follow-up imaging ex- ben. Die Initiative „RheumaPreis“ sucht
25. Chapman JR, Dettori JR, Norvell DC (2009) Spine aminations provide useful prognostic information
in patients with spine infection? Clin Infect Dis
auch in diesem Jahr wieder Menschen
classifications and severity measures. Thieme,
Stuttgart 43(2):172–179 mit Rheuma, denen es gemeinsam mit
26. Mirza SK et al (2002) Classifications of thoracic and 50. Khan MH et al (2006) Serum C-reactive protein ihren Arbeitgebern gelungen ist, ihr Ar-
lumbar fractures: rationale and supporting data. levels correlate with clinical response in patients
treated with antibiotics for wound infections after
beitsumfeld umzugestalten und so ihren
J Am Acad Orthop Surg 10(5):364–377
27. Field MJ, Lohr KN (1990) Clinical practice guide- spinal surgery. Spine J 6(3):311–315 Arbeitsplatz und die Freude am Beruf zu
lines: directions for a new program. National 51. Chelsom J, Solberg CO (1998) Vertebral os- erhalten. Die Bewerbung für den Rheuma-
Academies Press, Washington teomyelitis at a Norwegian university hospital
28. Audigé L, Bhandari M, Kellam J (2004) How reliable 1987–97: clinical features, laboratory findings and
Preis steht jedem offen, der an Rheuma
are reliability studies of fracture classifications? A outcome. Scand J Infect Dis 30(2):147–151 erkrankt ist und einer Berufstätigkeit nach-
systematic review of their methodologies. Acta 52. Carragee EJ (1997) Pyogenic vertebral osteomyeli- geht. Teams können sich ebenso melden
Orthop Scand 75(2):184–194 tis. J Bone Joint Surg Am 79(6):874–880
29. Herren C et al (2017) Spondylodiscitis: diagnosis 53. Carragee EJ et al (1997) The clinical use of
wie Einzelpersonen, Selbstständige ebenso
and treatment options: a systematic review. Dtsch erythrocyte sedimentation rate in pyogenic wie Auszubildende oder Angestellte. Der
Ärztebl Int 114(875):51–52 vertebral osteomyelitis. Spine 22(18):2089–2093 Preis wird von einer unabhängigen Jury an
30. Stricsek G et al (2018) Etiology and surgical 54. del Pozo JSG, Soto MV, Solera J (2007) Vertebral
management of cervical spinal epidural abscess osteomyelitis: long-term disability assessment
den Arbeitnehmer und seinen Arbeitgeber
(SEA): a systematic review. Global Spine J and prognostic factors. J Infect 54(2):129–134 vergeben. Das Preisgeld von 3000 Euro
8(4_suppl):59S–67S 55. O’Daly BJ, Morris SF, O’Rourke SK (2008) Long-term erhält der Arbeitnehmer.
31. Rigamonti D et al (1999) Spinal epidural abscess: functional outcome in pyogenic spinal infection.
contemporary trends in etiology, evaluation, and Spine 33(8):E246–E253
management. Surg Neurol 52(2):189–197 56. Euba G et al (2008) Long-term clinical and radi- Bewerbungsschluss
32. Howie BA et al (2018) Thoracic epidural ab- ological magnetic resonance imaging outcome ist der 30. Juni 2020.
scesses: a systematic review. Global Spine J of abscess-associated spontaneous pyogenic
8(4_suppl):68S–84S vertebral osteomyelitis under conservative man-
33. de Leeuw CN et al (2018) Lumbar epidural agement. Semin Arthritis Rheum 38(1):28–40 Die Bewerbung kann per Post
abscesses: a systematic review. Global Spine J 57. Carragee EJ (1997) The clinical use of mag- oder online eingereicht werden.
8(4_suppl):85S–95S netic resonance imaging in pyogenic vertebral
34. Hadjipavlou AG et al (2000) Hematogenous osteomyelitis. Spine 22(7):780–785
pyogenic spinal infections and their surgical 58. Wang Q et al (2010) Utility of MRI in the follow-up Bewerbungsunterlagen online:
management. Spine 25(13):1668–1679 of pyogenic spinal infection in children. Pediatr https://rheumapreis.de/bewerbung/
35. Ghobrial GM et al (2015) Surgical management Radiol 40(1):118
in 40 consecutive patients with cervical spinal
bewerbungsinformationen/
59. Kowalski T et al (2007) Follow-up MR imaging
epidural abscesses. Spine 40(17):E949–E953 in patients with pyogenic spine infections: lack
36. Alton TB et al (2015) Is there a difference in of correlation with clinical features. AJNR Am J
neurologic outcome in medical versus early Neuroradiol 28(4):693–699
operative management of cervical epidural
Informationen zu den Mitgliedern
60. Gillams A, Chaddha B, Carter A (1996) MR
abscesses? Spine J 15(1):10–17 appearances of the temporal evolution and und Initiatoren der Initiative
37. Tuchman A, Pham M, Hsieh PC (2014) The resolution of infectious spondylitis. AJR Am J „RheumaPreis“ finden Sie unter:
indications and timing for operative management Roentgenol 166(4):903–907
of spinal epidural abscess: literature review and
http://rheumapreis.de/partner/
treatment algorithm. Neurosurg Focus 37(2):E8
38. Khanna RK et al (1996) Spinal epidural abscess:
evaluation of factors influencing outcome.
Neurosurgery 39(5):958–964
S. Priester,
39. Szpalski M (1996) The mysteries of segmental Pressestelle RheumaPreis
instability. Bull NYU Hosp Jt Dis 55(3):147 www.rheumapreis.de
492 Der Orthopäde 6 · 2020
Hier steht eine Anzeige.
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5822)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1093)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (852)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (898)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (540)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (349)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (822)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (403)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Short Notes in Periodontics A HandbookDocument172 pagesShort Notes in Periodontics A HandbookFarheen Tajammal100% (9)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Medication: Expected Pharmacological Action Therapeutic UseDocument1 pageMedication: Expected Pharmacological Action Therapeutic Useclarimer100% (1)
- Ujjayi Pranayama Benefits and Steps - Big Chi Theory PDFDocument4 pagesUjjayi Pranayama Benefits and Steps - Big Chi Theory PDFakshra7gjNo ratings yet
- Gayatri Dengale FinalDocument38 pagesGayatri Dengale FinalTarwade NileshNo ratings yet
- Clinical, Immunological, and Molecular Findings in 57 Patients With Severe Combined Immunodeficiency (SCID) From IndiaDocument16 pagesClinical, Immunological, and Molecular Findings in 57 Patients With Severe Combined Immunodeficiency (SCID) From IndiaYeni PuspitasariNo ratings yet
- Disorders of Iron Kinetics and Heme MetabolismDocument12 pagesDisorders of Iron Kinetics and Heme MetabolismJoanne JardinNo ratings yet
- Calcium Metabolism-Board Questions 2018: Azar Khosravi April 2018Document55 pagesCalcium Metabolism-Board Questions 2018: Azar Khosravi April 2018Abdullah SiddiqiNo ratings yet
- PollutionDocument30 pagesPollutionMuhammed Althaf VKNo ratings yet
- Actual Listening Test For English Major StudentsDocument2 pagesActual Listening Test For English Major StudentsBayissa BekeleNo ratings yet
- Proton Pump InhibitorDocument24 pagesProton Pump InhibitorApurba Sarker ApuNo ratings yet
- Analysis of Satisfaction Level Regarding Fixed Partial Denture: A Clinical StudyDocument3 pagesAnalysis of Satisfaction Level Regarding Fixed Partial Denture: A Clinical StudySkAliHassanNo ratings yet
- Time To Ditch Toxic Positivity,' Experts Say: It's Okay Not To Be Okay'Document5 pagesTime To Ditch Toxic Positivity,' Experts Say: It's Okay Not To Be Okay'Ivana VelickovicNo ratings yet
- ECG ArrhythmiaDocument27 pagesECG ArrhythmiaSrikitta DanieliaNo ratings yet
- 3.6.2020 Final Final Manual - Logbook For Students For Adult 2Document34 pages3.6.2020 Final Final Manual - Logbook For Students For Adult 2Drmirfat AlkashifNo ratings yet
- TelepsychiatryDocument406 pagesTelepsychiatrychrisNo ratings yet
- Evaluation of Allergenicity of Genetically Modified FoodsDocument30 pagesEvaluation of Allergenicity of Genetically Modified FoodsChirag EducationNo ratings yet
- List of Journals Approved by UGC-2024: January 2024Document1,401 pagesList of Journals Approved by UGC-2024: January 2024Jordan PetersonNo ratings yet
- Plain Film and HRCT Diagnosis of Interstitial Lung Disease: Sujal R. Desai, Helmut Prosch, and Jeffrey R. GalvinDocument9 pagesPlain Film and HRCT Diagnosis of Interstitial Lung Disease: Sujal R. Desai, Helmut Prosch, and Jeffrey R. GalvinVictor ChiabaiNo ratings yet
- Taking Charge of Your Health: © 2021 Cengage. All Rights ReservedDocument46 pagesTaking Charge of Your Health: © 2021 Cengage. All Rights ReservedTimothy MontgomeryNo ratings yet
- Atrial FibrillationDocument28 pagesAtrial FibrillationKrisianne Mae Lorenzo FranciscoNo ratings yet
- Bi Support Groups1Document6 pagesBi Support Groups1api-301357752No ratings yet
- TDM Slides NicholsDocument39 pagesTDM Slides NicholsGordon BongNo ratings yet
- Defecation - Rectum - Control - TeachMePhysiologyDocument2 pagesDefecation - Rectum - Control - TeachMePhysiologyLaiba AliNo ratings yet
- PriyankarefDocument6 pagesPriyankarefapi-19985983No ratings yet
- 8 - 030 - Fathan - Akbar - Al - Bahri - Outcome 1 2Document8 pages8 - 030 - Fathan - Akbar - Al - Bahri - Outcome 1 2Fathan FathanNo ratings yet
- Icardin - Your First Choice For A Second OpinionDocument3 pagesIcardin - Your First Choice For A Second OpinionHounkonnou JacquesNo ratings yet
- Nutrients and Botanicals For Erectile Dysfunction: Examining The EvidenceDocument13 pagesNutrients and Botanicals For Erectile Dysfunction: Examining The EvidencefinaNo ratings yet
- Hepbd J Met Hepatitis B Surface Antigen 508Document18 pagesHepbd J Met Hepatitis B Surface Antigen 508Gom LinusNo ratings yet
- Catalog Knee CapsDocument3 pagesCatalog Knee CapskrastromanNo ratings yet
- Infectious Diseases Affecting The GitDocument64 pagesInfectious Diseases Affecting The GitGeraldine MaeNo ratings yet