Professional Documents
Culture Documents
Mechanisms of Laser-Tissue Interaction: I. Optical Properties of Tissue
Mechanisms of Laser-Tissue Interaction: I. Optical Properties of Tissue
Uploaded by
Aleksandar JokicOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Mechanisms of Laser-Tissue Interaction: I. Optical Properties of Tissue
Mechanisms of Laser-Tissue Interaction: I. Optical Properties of Tissue
Uploaded by
Aleksandar JokicCopyright:
Available Formats
Review Article
Mechanisms of Laser-Tissue Interaction:
I. Optical Properties of Tissue
Mohammad Ali Ansari, Ezeddin Mohajerani
Laser Research Institude, Shahid Beheshti University, Tehran, Iran.
Abstract:
Today, lasers are widely used in biology and medicine, and the majority of health
centers and hospitals utilize modern laser systems for diagnosis and therapy applications.
Researchers have introduced different medical applications for different lasers used
in surgeries and other medical treatments. Medical lasers can be categorized in both
diagnosis and therapy branches. Main difference between diagnosis and therapy
applications is the type of laser-tissue interactions. In diagnosis, one tries to arrange
a noninvasive method to study the normal behavior of tissue without any damage or
clear effect on tissue. But in therapy, such as surgery, a surgeon uses laser as a knife
or for affecting a specific region. So, the medical laser applications are defined by
the interaction type between laser light and tissues. The knowledge of laser-tissue
interaction can help doctors or surgeons to select the optimal laser systems and
modify the type of their therapy. Therefore, we seek to review the mechanisms of
laser- tissue interaction. In this paper, the optical properties of biological tissue such
as absorption, scattering, penetration and fluorescence are reviewed. Also, the effects
of these properties on laser penetration in tissue have been explained.
Keyword: medical optics; lasers; scattering; absorption; fluorescence
Please cite this article as follows:
Ansari MA, Mohajerani E. Mechanisms of laser-tissue interaction: I. optical properties of tissue. J Lasers Med Sci
2011; 2(3):119-25
*Corresponding Author: Ezeddin Mohajerani, PHD; Laser Research Institude, Shahid Beheshti University, Tehran, Iran.
Tel: +98-2122431987; Fax: +98-2122431987; Email: e-mohajerani@sbu.ac.ir
tissues on laser parameters and optical properties
Introduction
of tissues (26). Therefore, each biological tissue
After the invention of laser, many researches were has individual impulse response functions when
performed investigating potential interaction on irradiated by laser light. This impulse response is
tissue by means of all types of lasers and biological complicated and many groups around the world
tissues (1-24). While the number of feasible work in this field (27-32). This scientific subject
combinations for the experimental parameters is is called medical optics and has important role in
unlimited, mainly five groups of interaction types are laser surgery, optical imaging, and photodynamic
categorized. These are: photochemical interactions, therapy (33). Each of the interaction mechanisms
thermal interactions, ablative photodecomposition, will be carefully discussed in the next sections of
plasma-mediated ablation, and photo- disruption this review in later volumes. Emphasis is placed
(25). Before focusing on these interactions, it on microscopic mechanisms controlling various
is important to study the optical properties of processes of laser energy conversion. Each type of
biological tissues. The importance is due to the interaction will be introduced in separate papers
dependency of light penetration inside biological by common macroscopic observations including
Journal of Lasers in Medical Sciences Volume 2 Number 3 Summer 2011 119
Optical Properties of Tissue in Laser-Tissue Interaction
typical experimental data and/or histology of tissue
samples after laser exposure.
In this review, we will talk about basic phenomena
occurring when biological tissue is irradiated by
laser light. In principle, four phenomena exist
which govern on undistributed propagation of
light in tissue: reflection, scattering, absorption
and fluorescence. Reflection can be studied by
Fresnel’s law (34). Most part of laser energy
penetrates into biological tissue. The penetration of
laser light in biological tissue depends on optical Figure 1. Schematic of scattering in turbid media (15).
properties of biological tissue, such as index of
refraction, scattering and anisotropic factor, and
also the absorption of laser light in tissue. These and particle beam of photon.) of lasers diffuse and
optical properties determine the mechanism of attenuate in biological tissues.
laser-tissue interaction in that special case. So, Scattering of laser light by cells, nuclei,
first, we study the optical properties of biological mitochondria, lysosome, macromolecules,
tissue, followed by the study of the effect of these membranes and other components, results in
properties on penetration of laser light. diffusion of light in biological tissues. Optical
Mainly, the behavior of laser in its interaction scattering originates from light interaction with
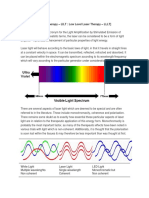
with tissue can be classified by its wavelength. biological structures ranging from cell membranes
Today, there are several lasers with wavelengths to whole cells. The size of this scattereres varies
between x-ray and infra-red (IR). Famous lasers from 10 nm to 10 microns. These scattereres are
like CO2, neodymium-doped yttrium aluminium distributed randomly in biological tissue; photons
garnet (Nd: YAG), fiber laser, and dye lasers usually encounter multiple scattering events. The
are frequently applied in medicine. The most scattering coefficient σ is defined as the probability
important difference that can be used to classify of photon scattering in a medium per unit path
lasers is their wavelength, because the molecular length. The scattering mean free path (spatial
absorption depends on this important parameter. interval between two adjacent scatterings) is the
For example, the 200 nm laser light is absorbed reciprocal of scattering coefficient σ. The scattering
only slightly by viruses; more is seen by bacteria coefficient of biological tissues depends on the
cells, and an entire absorption by mammalian cells. wavelength of laser, e.g. the scattering coefficient
This absorption is mainly due to the presence of liver for lambda of 515, 800 and 1064 nm is
of endogenous molecules that absorb heavily 285,200 and 150 cm-1, respectively. The scattering
near 200 nm such as DNA, genetic material and mean free path of liver for these wavelengths
proteins. Oxygen consumption is activated by is 35, 50 and 66 microns, which shows that the
illuminating with light at 365 nm. It is believed spatial interval between two scatterings increases
that mitochondria are the absorber of 630 nm (35). for longer wavelengths.
Therefore, in medical optics, the wavelength of The probability of no scattering after a photon
laser has an important role due to the absorption propagates over path length х can be written by
peaks of bio-molecules and tissues. Beer’s law (36):
(1)
In most biological tissues, the majority of
Medical optics
scattered light travels in forward direction. So,
400-1100 nm spectral region is called optical these biological tissues have anisotropy which is
window. Most biological tissues are classified by convenient to define a phase function p(θ) of a
strong optical scattering in this region. So, they photon to be scattered by an angle θ. If p(θ) is
are referred to as turbid media (Figure 1). In a constant and not dependent on θ, the media is
other words, the photons (The laser light can be called isotropic, otherwise, it is called anisotropic
simultaneously assumed as electromagnetic wave medium. Experiments show the mean value of
120 Journal of Lasers in Medical Sciences Volume 2 Number 3 Summer 2011
Optical Properties of Tissue in Laser-Tissue Interaction
phase function g is a number between -1 and +1. and pheomelanin which is red-yellow (39). The
Where g = 1 denotes purely forward scattering molar extinction coefficient spectra corresponding
and g = -1 purely backward scattering, and g = 0 to both types are shown in Figure 4. Melanin
isotropic scattering. Most biological tissues have absorbs ultraviolet strongly.
g > 0.7 (37). As an example, the absorption coefficients of
The absorption coefficient α is defined as the biological tissue at two wavelengths λ1,2 can be
probability of photon absorption in a medium per used to estimate the concentrations of Hb and
unit path length. The reciprocal of α is referred to HbO2 as in the following method (36):
at the mean absorption length. Optical absorption
in biological tissue originates from water, melanin (3)
and hemoglobin (Hb and HbO2). Figure 2 depicts
the molar extinction coefficient of oxy and
deoxyhemoglobin vs. wavelength. To convert the Here, eox and edx are the known molar extinction
molar extinction coefficient to absorption coefficient of oxy-and deoxyhemoglobin, respectively; C ox
in (cm-1), multiplied by the molar concentration and Cdx are the molar concentrations of oxy- and
and 2.303 (38): deoxy-hemoglobin, respectively, in tissue. The
oxygen saturation (SO2) and the total concentration
(2) (CHb) of hemoglobin can be computed as follows:
Where e and x are molar extinction coefficient
(cm-1/M) and number of gram per liter, a typical
value of x for whole blood is x = 150 g Hb/liter.
64500 (g Hb/mole) is gram molecular weight of
hemoglobin.
The absorption coefficient of natural water is
shown in Figure 3 (38). Melanin is a chromophore
that exists in the human epidermal layer of skin
responsible for protection from harmful UV
radiation. When melanocytes are stimulated by
solar radiation, melanin is produced (39). Melanin
is one of the major absorbers of light in some
biological tissue (although its contribution is
smaller than other components). There are two
types of melanin: eumelanin which is black-brown Figure 3. Absorption coefficient of natural water with penetration
depth (38).
Figure 2. Molar extinction coefficient of oxy and deoxyhemoglobin Figure 4. The molar extinction coefficient of eumelanin and
v.s. wavelength (38). pheomelanin v.s. wavelength (38).
Journal of Lasers in Medical Sciences Volume 2 Number 3 Summer 2011 121
Optical Properties of Tissue in Laser-Tissue Interaction
of endogenous fluorescence at physiologic PH are
(4) classified (where λa denotes maximum absorption
wavelength; e denotes molar extinction coefficient;
where λx denotes maximum excitation wavelength;
These parameters are essential for oximetry and where λm denotes maximum emission wavelength)
functional imaging. (36). Fluorescence can provide data about the
structure, and interaction of bimolecular structures.
For example, mitochondrial fluorophore NADH
Molecular absorption of laser light
(nicotinamide adenine dinucleotide) is an important
When tissue is irradiated by laser light, a small sign in cancer detection. The emission spectra of
fraction of light is reflected as shown in Figure 1, some biological components are shown in Figure 5.
but most of laser light penetrates into tissue, where
it is either absorbed or scattered by the molecules.
Effects of optical properties on penetration of
As it can be seen in the previous figures, water
laser light into biological tissue
has two regions of strong absorption, one in UV
and one in the IR region. The absorption peak The study of laser penetration in different
in the case of aromatic rings of proteins and the biological tissues is one of the aims in medical
nuclide acids is in the UV region between 260 and optics. For example the laser light propagation in
280 nm. Hence, in the UV region, the laser light skin is important for hair removal and other usage
is strongly absorbed by water and proteins in the of laser in dermatology. In references number (42)
tissue, resulting in a poor light penetration into the laser light transport in Asian and Caucasian
the tissue. The same is true in IR region starting at skins has been studied. Normalized reflectivity
about 1.3 microns. Blood absorbs light in a broad variation of Caucasian and Asian skins vs. volume
wavelength region up to red light (630 nm), and fraction of melanosome for wavelength of 694
above 600 nm, the absorption of blood is weak. nm of ruby laser is illustrated in Figure 6a-b. The
Melanin absorbs light in a region from UV to level of melanosome is assumed to vary from 1.3
near IR. Between 600 nm and 1.3 microns, the to 5.5% and from 10 to 15.5% for Caucasian and
absorption coefficient of the tissue molecules is Asian skins, respectively (38). The concentration
small, resulting an interesting optical window to of hemoglobin in Caucasian and Asian skins is
allow penetration of laser light into tissue. assumed to be 5% and 2%, respectively. The
When tissue is irradiated by laser light, most figures illustrate that reflectivity of both types
of the energy of light is absorbed by tissue of skins decreases for larger volume fraction of
molecules, and they are excited. Laser-excited
molecules can return to ground state by emitting
fluorescence or phosphorescence light, depending
on the lifetime of excited electron. The lifetime
of fluorescence is on the order of nanosecond,
but the lifetime of phosphorescence is longer
(millisecond or longer). In Table 1, the properties
Table 1. Properties of endogenous fluorescence at physiologic PH.
Fluoresence λα(nm) e(cm-1M-1) λx(nm) λm(nm)
NAD+ 260 18×103 - -
NADH 260 14.4×103 290 440
340 6.2×103 340 450
Phenylalanine 260 0.2×103 - 280
Figure 5. Emission spectra of some biological components. All
Tryptophan 280 5.6×103 280 350 compounds were measured in buffered (pH 7.2) saline solution,
Tyrosine 275 1.4×103 - 300 except retinol and cholecalciferol (vit D), which were measured
Ceriod - - 340-395 430-460 in EtOH. Riboflavin, cholecalciferol, and NADH were measured
Collagen, elastin - - 325 400 at 100 μM; retinol, folic acid, phylloquinone, pyridoxine, and
Lipofusion - - 340-395 430-460 nicotinamide were measured at 500 μM. (b) Emission spectra of
the compounds shown in a (measured in the same solvents) (41).
122 Journal of Lasers in Medical Sciences Volume 2 Number 3 Summer 2011
Optical Properties of Tissue in Laser-Tissue Interaction
Figure 6. Variation of normalized reflectance vs. volume fraction of melanosome from skin with hemoglobin volume fraction of 5% (a)
and 2% (b) (42)
melanosomes. But, for Caucasian skin, normalized not significant for different values of hemoglobin
reflection reduces down to 51% by increasing concentrations. Based on Mie theory, scattering
volume fraction of melanosome while, for Asian cross section depends on geometrical shape of
skin, this reduction is more pronounced and is scattering centers and the wavelength of incident
about 71.8%. Similar trends are observed for other light and its dependence on blood volume fraction
famous wavelengths, i.e. 775 (Alexanderit laser) can be neglected (38, 43). Therefore, blood volume
and 1064 nm (Nd:YAG laser). fraction only changes absorption coefficient
To study the effect of hemoglobin concentration of dermis layer. As the blood is assumed to be
on light propagation, the blood flow is assumed uniformly distributed in dermis layer, its absorption
to be uniformly distributed in the dermis layer coefficient, due to hemoglobin concentration,
(38). Figure 7 shows variation of normalized is expected to increase for larger blood volume
reflectance of skin vs. blood volume fraction fractions. But, hemoglobin absorption coefficient at
for Caucasian and Asian skins with melanosome 694 nm is about 0.2mm-1 and, therefore, variation
volume fraction of 1 and 10%, respectively. One of blood volume fraction does not significantly
can observe that the reduction of reflectivity is change dermis absorption of light.
Also transverse scattering of light from tissues
is studied in references number (42). Scattering
of light arises because of density variation. The
effect is due to the presence of different types
of molecules in tissue (36). Figure 8 illustrates
Maximum Scattered Beam Width (MSBW), i.e.
distance where fluence of the beam in transverse
direction reduces to 0.001% of its initial value
for Asian and Caucasian skins for different
wavelengths (optical properties of different skin
are mentioned in Table.2). The Figure shows that
MSBW parameter increases for longer wavelengths
for both skin types. That is because for longer
wavelengths, both scattering cross section and
reduced scattering coefficient decrease (44-36).
Furthermore, in NIR region absorption of melanin,
Figure 7. Normalized reflectance variation vs. hemoglobin volume
fraction for two different values of melanin volume fraction (42). as the most important absorbing element, decreases
Journal of Lasers in Medical Sciences Volume 2 Number 3 Summer 2011 123
Optical Properties of Tissue in Laser-Tissue Interaction
Table 2. Optical properties of Asian and Caucasian skins
λ(nm) 694 755 1064
Type Cau. / Asian Cau. / Asian Cau. / Asian
Absorp.of epi. (mm-1) 0.063 / 2.29 0.054 / 1.7 0.035 / 0.57
Absorp. of derm. (mm-1) 0.028 / 0.033 0.027 / 0.029 0.026 / 0.028
Scatt. of epi. (mm-1) 40 / 38 35 / 26 26 / 24
Scat. of derm. (mm-1) 20 / 19 17.5 / 13 13 / 12
6. Serebryakov VA, Boĭko EV, Petrishchev NN, Yan AV.
Medical applications of mid-IR lasers: Problems and
prospects. J Opt Technol 2010; 77(1):6-17.
7. Johnson FB. Optics and Pathology. Appl Opt 1969;
8(1): 49-52.
8. Guo H, Sato K, Takashima K, Yokoyama H. Two-photon
Bio-imaging with a Mode-locked Semiconductor Laser.
In 15th International Conference on Ultrafast Phenomena,
OSA Technical Digest Series (CD) (Optical Society of
America 2006), paper TuE8.
9. Fisher BT, Hahn DW. Real-time measurement of ArF
excimer laser corneal tissue ablation rates using cross-
correlation of laser waveforms. Opt Express 2011;
19(5):4231-41.
10. Flanagan GW, Binder PS. The theoretical vs. measured
laser resection for laser in situ keratomileusis. J Refract
Surg 2005; 21(1):18–27.
Figure 8. Maximum Scattered Beam Width (MSBW) for three
different wavelengths (42). 11. Pettit GH, Ediger MN, Weiblinger RP. Excimer laser
ablation of the cornea. Opt Eng 1995; 34(3):661–7.
for longer wavelengths (36). Therefore, moving 12. Pettit GH, Ediger MN. Pump/probe transmission
measurements of corneal tissue during excimer laser
toward longer wavelengths results in simultaneous ablation. Lasers Surg Med 1993; 13(3):363–7.
reduction of absorption coefficient and reduced
13. Dougherty PJ, Wellish KL, Maloney RK. Excimer laser
scattering coefficient and, consequently, increase ablation rate and corneal hydration. Am J Ophthalmol
in magnitude of diffusion coefficient. On the other 1994; 118(2):169–76.
hand, mean free path of tissue is proportional to 14. Vogel A, Noack J, Hüttman G, Paltauf G. Mechanism of
diffusion coefficient (26). Therefore, for longer femtosecond laser nanosurgery of cells and tissue. Appl
wavelengths, mean free path in transverse plane Phys B 2005; 81(8): 1015–47.
and, consequently, MSBW, increase. 15. Müller G, Chance B, Alfano R. Medical Optical
Tomography:Functional Imaging and Monitoring, IS11,
SPIE Press, Bellingham, WA, 1993.
References 16. Müller G, Roggan A (eds.) Laser-Induced Interstitial
Thermotherapy. PM25, SPIE Press, Bellingham, WA, 1995.
1. Katzir A. Laser and optical fibers in medicine. Optics
17. Tuchin VV, Selected Papers on Tissue Optics: Applications
Photonics News 1991; 2(2) 18-22.
in Medical Diagnostics and Therapy, 1994; MS102, SPIE
2. Lanigan SW. Lasers in dermatology. Springer- Verlag; Press, Bellingham, WA.
London, 2000.
18. Chance B, Cope M, Gratton E, Ramanujam N, Tromberg
3. Grundfest WS. Applications of pulsed ultraviolet lasers B. Phase Measurement of Light Absorption and Scatter in
in medicine. Biomedical Topical Meeting (BIO); 1999; Human Tissue. Rev Sci Instrum 1998; 69(10):3457–81.
Munich, Germany: OSA Technical Digest (Optical Society
19. Priezzhev AV, Tuchin VV, Shubochkin LP. Laser
of America, 1999), paper CWD1.
Diagnostics in Biology and Medicine. Nauka, Moscow;
4. Eichler J, Lenz H. Laser applications in medicine and 1989.
biology: a bibliography. Appl Opt 1977; 16 (1): 27.
20. Tuchin VV, Lasers and Fiber Optics in Biomedical
5. Wei-Chiang L, Motamedi M, Welch AJ. Dynamics of Science, Saratov University Press, Saratov; 1998.
tissue optics during laser heating of turbid media. Appl
21. Katzir A. Lasers and Optical Fibers in Medicine. Academic
Opt 1996; 35(19): 3413-20.
Press, San Diego; 1993.
124 Journal of Lasers in Medical Sciences Volume 2 Number 3 Summer 2011
Optical Properties of Tissue in Laser-Tissue Interaction
22. Tuchin V. Izatt JA. Coherence Domain Optical Methods 33. Vo-Dinh T. Biomedical Photonics Handbook. CRC
in Biomedical Science and Clinical Applications II. Proc Press; 2003.
SPIE 3251, 1998; 3598.
34. Hecht E. Optics. Addison-Wesley; 2002.
23. Tuchin VV. Lasers and Fiber Optics in Biomedicine.
35. Waynant RW. Lasers in Mediciene. Boca Raton: CRC
Laser Phys 1993; 3(5): 925–50.
Press; 2002.
24. Tuchin VV. Lasers Light Scattering in Biomedical
36. Wang LV, Wu HI. Biomedical optics: principles and
Diagnostics and Therapy. J Laser Appl 1993; 5(2):43–60.
imaging. Wiley-Interscience, New Jersey; 2007.
25. Neims MH. Laser-Tissue Interactions: Fundamentals and
37. Welch AJ, Gemert MVC. Optical- Response of Laser-
Applications. Springer-verlag, Berlin; 2004.
Irradiated Tissue. Springer; 1th rev; 1995.
26. Ansari MA, Massudi R, Hejazi M. Experimental and
38. http://omlc.ogi.edu/news/jan98/skinoptics.html
numerical study on simultaneous effects of scattering
and absorption on fluorescence spectroscopy of a breast 39. Vo-Dinh T. Biomedical Photonics Handbook. 2nd ed.Taylor
phantom. Opt Laser Technol 2009; 41(6):746-50. & Francis; 2002.
27. Cheong W, Prahl SA. A review of the optical properties 40. Zonios G, Dimou A, Bassukas J, Galaris D, Ysolakidis
of biological tissues. IEEE J Quantom Elec 1990; A, Kaxiras E. Melanin absorption spectroscopy: new
26(12):2166-85. method for noninvasive skin investigation and melanoma
detection. J. Biomed. Opt., Vol.13, 014017, 2008.
28. Brewster MQ, Yamada Y. Optical properties of thick,
turbid media from picosecond time-resolved light 41. Zipfel R, Williams RM, Christie R, Nikitin AY, Hyman
scattering measurement. Int J Heat Mass Transfer 1995; BT, Webb WW. Live tissue intrinsic emission microscopy
38(14):2569-81. using multiphoton-excited native fluorescence and second
harmonic generation. PNAS, 2003; 100(12) 7075–80.
29. Mitra K, Kumar S. Development and comparison of
models for light-pulse transport through scattering- 42. Ansari MA, Massudi R. Study of light propagation in
absorbing media. Appl Opt 1999; 38 (1):188-96. Asian and Caucasian skins by means of the boundary
element method. Opt Laser Eng 2009; 47(9):965-70.
30. Tuchin VV. Light interaction with biological tissues.
Proc. SPIE, 1993; 1884. 234-72. 43. Zonios G, Bykowski J, Kollias N. Skin melanin,
Hemoglobin, and light scattering properties can be
31. Kim AD. Transport theory for light propagation in
quantitatively assessed in vivo using diffuse reflectance
biological tissue. J Opt Soc Am A 004; 21 (5):820-7.
spectroscopy. J Invest Dermatol 2001; 117(6):1452-7.
32. Klose AD, Larsen EW. Light transport in biological tissue
44. Taroni P, Pifferi A, Torricelli A, Comelli D, Cubeddu R. In
based on the simplified spherical harmonics equations.
vivo absorption and scattering spectroscopy of biological
J Comput Phys 2006; 220(1):441-70.
tissues. Photochem Photobiol Sci 2003; 2(2):124-9.
Journal of Lasers in Medical Sciences Volume 2 Number 3 Summer 2011 125
You might also like
- Xray ReportDocument26 pagesXray Reports00uravNo ratings yet
- Infrared SpectrosDocument4 pagesInfrared SpectrosAna-Maria Pantazica50% (2)
- Global Reporting System User Manual GRS-Rig V4.0: TitleDocument161 pagesGlobal Reporting System User Manual GRS-Rig V4.0: Titlevikrant911No ratings yet
- Application of Diode Laser in Oral and Maxillofacial SurgeryDocument42 pagesApplication of Diode Laser in Oral and Maxillofacial SurgeryEng.MohamedNo ratings yet
- Studying Laser Tissue Interaction of Two Internal Organs of RatDocument7 pagesStudying Laser Tissue Interaction of Two Internal Organs of RaterpublicationNo ratings yet
- Unit I LfoDocument47 pagesUnit I LfoSinduNo ratings yet
- SBM1602Document61 pagesSBM1602Dhanalakshmi StridaraneNo ratings yet
- Prof. Tiina Karu's Research Paper Written Exclusively For UsDocument8 pagesProf. Tiina Karu's Research Paper Written Exclusively For Usmarty mcflyNo ratings yet
- Laser Applications in Bio-Medical FieldDocument11 pagesLaser Applications in Bio-Medical FieldJonNo ratings yet
- Technology of Lasers and Their Applications in Oral Surgery: Literature ReviewDocument7 pagesTechnology of Lasers and Their Applications in Oral Surgery: Literature ReviewLeonardoNo ratings yet
- Fixler 2012Document5 pagesFixler 2012Michael Rojas RuizNo ratings yet
- Laser in Oral and Maxillofacial Surgery 2023Document26 pagesLaser in Oral and Maxillofacial Surgery 2023يسر مكي وهاب المظفرNo ratings yet
- Medical Optics - 2 Marks With AnswerSDocument27 pagesMedical Optics - 2 Marks With AnswerSBharath V100% (3)
- Emerging Modalities in Veterinary Rehabilitation OkDocument21 pagesEmerging Modalities in Veterinary Rehabilitation OkIndyNo ratings yet
- Medical Optics (2016-2017) - 2 Marks With AnswerSDocument28 pagesMedical Optics (2016-2017) - 2 Marks With AnswerSBharath VNo ratings yet
- Bio Medical Optics Ch1Document16 pagesBio Medical Optics Ch1kgupta27No ratings yet
- 2 PDFDocument9 pages2 PDFhmsatNo ratings yet
- Microdosimetry of Internally Deposited Radionuclides: Int. J. Appl. Radiat. IsotDocument13 pagesMicrodosimetry of Internally Deposited Radionuclides: Int. J. Appl. Radiat. IsotHalaj AzadNo ratings yet
- Fundamentals of Tissue OpticsDocument14 pagesFundamentals of Tissue OpticsArturo FilemonNo ratings yet
- Law of Bergonie and TribondeauDocument7 pagesLaw of Bergonie and TribondeauRuelyn AcedoNo ratings yet
- FT-IR Spectroscopy in Medicine: National Technical University of Athens, NTUA GreeceDocument20 pagesFT-IR Spectroscopy in Medicine: National Technical University of Athens, NTUA Greeceroxana biricioiuNo ratings yet
- EE3018 Literature ReportDocument10 pagesEE3018 Literature ReportGoh Cai YuNo ratings yet
- Review Laser Ablation For Cancer: Past, Present and FutureDocument15 pagesReview Laser Ablation For Cancer: Past, Present and FutureSujin JiracheewanunNo ratings yet
- Laser TherapyDocument6 pagesLaser TherapyMuhammad FahmyNo ratings yet
- The Effects of Different Laser Doses OnDocument8 pagesThe Effects of Different Laser Doses OnАркадий ЖивицаNo ratings yet
- Overview of Lasers: Uddhav A. Patil, Lakshyajit D. DhamiDocument13 pagesOverview of Lasers: Uddhav A. Patil, Lakshyajit D. Dhamizidan ojaNo ratings yet
- Walt-low-Energy Laser Therapy As Quantum MedicineDocument4 pagesWalt-low-Energy Laser Therapy As Quantum Medicinemuitasorte9No ratings yet
- Raman Spectroscopy and Regenerative Medicine: A ReviewDocument10 pagesRaman Spectroscopy and Regenerative Medicine: A Reviewkr7wyddmw2No ratings yet
- LASER (LLLT) BASICS - "Mode of Action of Laser in Tissues"Document41 pagesLASER (LLLT) BASICS - "Mode of Action of Laser in Tissues"Dr. Mohammad Nazrul IslamNo ratings yet
- Laser TherapyDocument7 pagesLaser TherapyGustavo CabanasNo ratings yet
- DRAFT Physical Methods in Biology and Medicine Biophysics Finals RequirementsDocument16 pagesDRAFT Physical Methods in Biology and Medicine Biophysics Finals RequirementsALNo ratings yet
- Laser Tissue InteractionsDocument16 pagesLaser Tissue InteractionsDuchung TranNo ratings yet
- Particle Size AnalyzerDocument14 pagesParticle Size AnalyzermmmonmissionNo ratings yet
- Lasers in OphthalmologyDocument6 pagesLasers in OphthalmologyIJAR JOURNALNo ratings yet
- Principles of DiffuseDocument49 pagesPrinciples of DiffuseabocbellsNo ratings yet
- Laser Application: IntroductionDocument8 pagesLaser Application: IntroductionArjay CarolinoNo ratings yet
- Near Infrared (NIR) LightDocument11 pagesNear Infrared (NIR) LightVăn Hiền NguyễnNo ratings yet
- In Vivo Measumerent of Optical Properties of SkinDocument14 pagesIn Vivo Measumerent of Optical Properties of SkinCorynaNo ratings yet
- Effect of Different Wavelengths of Laser Irradiation On The Skin CellsDocument18 pagesEffect of Different Wavelengths of Laser Irradiation On The Skin CellsMat EckNo ratings yet
- Photobiology 1 - 231103 - 171019Document25 pagesPhotobiology 1 - 231103 - 171019eslam.h.mohamed1No ratings yet
- SpectrophotometryDocument22 pagesSpectrophotometryaziskfNo ratings yet
- Laserannals ComDocument8 pagesLaserannals ComveliNo ratings yet
- Clarifying Tissue ClearingDocument12 pagesClarifying Tissue ClearingJan GładkiNo ratings yet
- Ir Presentation PDFDocument17 pagesIr Presentation PDFMarr BarolNo ratings yet
- Laser TherapyDocument7 pagesLaser TherapylecturioNo ratings yet
- Infrared Spectroscopy: Theory and Interpretation of IR SpectraDocument33 pagesInfrared Spectroscopy: Theory and Interpretation of IR SpectraGerald See TohNo ratings yet
- PHY 278 - Linear Energy TransferDocument12 pagesPHY 278 - Linear Energy Transferbossbaby18105No ratings yet
- Modes of Vibration Basic Principles OfIR SpectrosDocument9 pagesModes of Vibration Basic Principles OfIR SpectrosMuhammad Hussnain100% (1)
- Lasers in Endodontics: ReviewDocument7 pagesLasers in Endodontics: ReviewShreya BagweNo ratings yet
- Laser in Orthodontics PDFDocument53 pagesLaser in Orthodontics PDFAly OsmanNo ratings yet
- Low Level Laser Therapy: Healing at The Speed of LightDocument24 pagesLow Level Laser Therapy: Healing at The Speed of LightcumbredinNo ratings yet
- Laser and IPL Technology in Dermatology and Aesthetic MedicineDocument434 pagesLaser and IPL Technology in Dermatology and Aesthetic MedicineMauricio MontemayorNo ratings yet
- 1 s2.0 S096522991930915X MainDocument6 pages1 s2.0 S096522991930915X MainltcgmoreiraNo ratings yet
- We Are Intechopen, The World'S Leading Publisher of Open Access Books Built by Scientists, For ScientistsDocument17 pagesWe Are Intechopen, The World'S Leading Publisher of Open Access Books Built by Scientists, For ScientistsJonathan YepesNo ratings yet
- TT115Document19 pagesTT115arexixNo ratings yet
- Molecular ImagingDocument34 pagesMolecular ImagingShaher Bano MirzaNo ratings yet
- FluorimetryDocument24 pagesFluorimetryAhmed ZaghloulNo ratings yet
- 20 Bio Medical LasersDocument77 pages20 Bio Medical Laserskaushik4208No ratings yet
- Shining a Light on Cool Standards: Infrared Spectroscopy Theory Explored.From EverandShining a Light on Cool Standards: Infrared Spectroscopy Theory Explored.No ratings yet
- Laser / IPL Technology for Skin Care: A Comprehensive Technical and Informative TextbookFrom EverandLaser / IPL Technology for Skin Care: A Comprehensive Technical and Informative TextbookRating: 4 out of 5 stars4/5 (8)
- A guide to Phototherapy Practice: Theory and Underpinning ScienceFrom EverandA guide to Phototherapy Practice: Theory and Underpinning ScienceNo ratings yet
- Passive VoiceDocument2 pagesPassive Voicenguyen hong phuong63% (19)
- Latihan UtsDocument8 pagesLatihan UtsFadhli Aulia SNo ratings yet
- CURVESDocument30 pagesCURVESPHULARAM PEGUNo ratings yet
- The Fox Project, A ReappraisalDocument22 pagesThe Fox Project, A ReappraisalZemin OonNo ratings yet
- Bhubneshwor LeadsDocument4 pagesBhubneshwor LeadsCo2 RenuUNo ratings yet
- Miscellaneous Measurements: and ControlsDocument50 pagesMiscellaneous Measurements: and ControlsJeje JungNo ratings yet
- Philippines RegionsDocument5 pagesPhilippines RegionsKristine MercadoNo ratings yet
- HB 2016 - 2nd - Edition - 13 - 01 - 17Document293 pagesHB 2016 - 2nd - Edition - 13 - 01 - 17Vaidya NurNo ratings yet
- Captcha SeminarDocument35 pagesCaptcha SeminarSachin ItgampalliNo ratings yet
- BT08 PDFDocument4 pagesBT08 PDFAfdhalNo ratings yet
- BK Ambari InstallationDocument72 pagesBK Ambari InstallationFernovy GesnerNo ratings yet
- Chapter3 DC-DC Converters 2016Document113 pagesChapter3 DC-DC Converters 2016ShawnNo ratings yet
- C Program To Store Records of Students in An ArrayDocument5 pagesC Program To Store Records of Students in An ArrayAsh RafNo ratings yet
- Policy - Task 2 ContentDocument6 pagesPolicy - Task 2 ContentJadhav AmitNo ratings yet
- HE-210 P-2604A-B - DEBUTANIZER FEED PREHEATING - Rev 0CxDocument1 pageHE-210 P-2604A-B - DEBUTANIZER FEED PREHEATING - Rev 0CxMariaNo ratings yet
- Strategies Towards Comprehensive Hemophilia Care Services in Uttar Pradesh" SGPGIMS, LucknowDocument4 pagesStrategies Towards Comprehensive Hemophilia Care Services in Uttar Pradesh" SGPGIMS, LucknowsalmanNo ratings yet
- DLL Mathematics 6 q4 w6Document7 pagesDLL Mathematics 6 q4 w6Abegail CorpuzNo ratings yet
- Query ManualDocument37 pagesQuery ManualstraNo ratings yet
- Format For THC 10 10 10 10 Siomairice Sa SarapDocument24 pagesFormat For THC 10 10 10 10 Siomairice Sa SarapFrost ByteNo ratings yet
- Byzantine ArmyDocument7 pagesByzantine ArmyDimitris Mavridis100% (1)
- Text - Cambay BasinDocument58 pagesText - Cambay BasinBidyut MandalNo ratings yet
- GregormendelandhispeasreadingandquestionsDocument2 pagesGregormendelandhispeasreadingandquestionsapi-248015505No ratings yet
- Hizon, Czarina May CVDocument3 pagesHizon, Czarina May CVnotapernota101No ratings yet
- SPPU MA 2 SyllabusDocument43 pagesSPPU MA 2 SyllabusPranit JavirNo ratings yet
- Z-Transform Theory: Itm, GurgaonDocument85 pagesZ-Transform Theory: Itm, GurgaonkanchiNo ratings yet
- Santa 1Document3 pagesSanta 1Polipio SaturnioNo ratings yet
- 500kV Aluminum Welded Bus Pipe Terminal PDFDocument9 pages500kV Aluminum Welded Bus Pipe Terminal PDFMohakumar MaranNo ratings yet
- Weather ChangesDocument34 pagesWeather ChangesEmina PodicNo ratings yet
- A Guide To The Management of Tuberculosis in Patients With Chronic Liver DiseaseDocument12 pagesA Guide To The Management of Tuberculosis in Patients With Chronic Liver DiseaseMeldaNo ratings yet