Professional Documents
Culture Documents
Woman Stroke
Woman Stroke
Uploaded by
paola nabhanCopyright:
Available Formats
You might also like
- Headache Syndromes, Oxford, 2020Document561 pagesHeadache Syndromes, Oxford, 2020luizmiranda108No ratings yet
- Pathophysiology of Migraine.5Document11 pagesPathophysiology of Migraine.5Bryan100% (1)
- Endovascular Treatment of Acute Ischemic Stroke.7-1 PDFDocument22 pagesEndovascular Treatment of Acute Ischemic Stroke.7-1 PDFCristina GhizdavetNo ratings yet
- Endovascular Treatment of Acute Ischemic Stroke.7 PDFDocument22 pagesEndovascular Treatment of Acute Ischemic Stroke.7 PDFchristinaNo ratings yet
- HSA ContinuunDocument35 pagesHSA ContinuunJose DavidNo ratings yet
- Chronic Traumatic Encephalopathy.12Document21 pagesChronic Traumatic Encephalopathy.12wmtxbbNo ratings yet
- Cluster Headache and Other Trigeminal Autonomic CephalalgiasDocument19 pagesCluster Headache and Other Trigeminal Autonomic CephalalgiasBryan100% (1)
- 7-Vertigo Related To Central Nervous System.-CompressedDocument21 pages7-Vertigo Related To Central Nervous System.-CompressedOlga Manco GuzmánNo ratings yet
- Cerebrovasc - ContinuumDocument239 pagesCerebrovasc - ContinuumRafael100% (1)
- Ataxia 10Document19 pagesAtaxia 10Cristina GhizdavetNo ratings yet
- Subarachnoid Hemorrhage: Continuumaudio Interview Available OnlineDocument35 pagesSubarachnoid Hemorrhage: Continuumaudio Interview Available OnlineJose DavidNo ratings yet
- Clinically Isolated Syndrome and Early Relapsing.8Document19 pagesClinically Isolated Syndrome and Early Relapsing.8juanmontoyaseNo ratings yet
- Neuromyelitis Optica Spectrum Disorder and Other.15Document30 pagesNeuromyelitis Optica Spectrum Disorder and Other.15Doaa Mokhtar100% (1)
- TraducirChiasmal and Postchiasmal - DiseaseDocument19 pagesTraducirChiasmal and Postchiasmal - DiseasejacquelineNo ratings yet
- Management of Stroke in The NCCUDocument25 pagesManagement of Stroke in The NCCUsaudNo ratings yet
- Charcot-Marie-Tooth Disease and Other Hereditary NeuropathiesDocument33 pagesCharcot-Marie-Tooth Disease and Other Hereditary NeuropathiesTallulah Spina TensiniNo ratings yet
- 2019-Epilepsy EmergenciesDocument23 pages2019-Epilepsy EmergenciesBryanNo ratings yet
- The Evolving Concept of Cryptogenic Stroke.9Document10 pagesThe Evolving Concept of Cryptogenic Stroke.9Toma BichirNo ratings yet
- Periferico - ContinuumDocument239 pagesPeriferico - ContinuumRafaelNo ratings yet
- Brain Death Death by Neurologic Criteria.15Document21 pagesBrain Death Death by Neurologic Criteria.15Anusha PervaizNo ratings yet
- Behavioral Variant Frontotemporal Dementia.7Document25 pagesBehavioral Variant Frontotemporal Dementia.7Nícolas CavalcanteNo ratings yet
- Neoplastic Myelopathies: Continuumaudio Interviewavailable OnlineDocument22 pagesNeoplastic Myelopathies: Continuumaudio Interviewavailable OnlineDalwadi1No ratings yet
- Diabetes and Metabolic Disorders and The.5 PDFDocument23 pagesDiabetes and Metabolic Disorders and The.5 PDFTallulah Spina TensiniNo ratings yet
- Neurologic Manifestations of Severe Acute.14Document15 pagesNeurologic Manifestations of Severe Acute.14Henry DanielNo ratings yet
- Brain Death Death by Neurologic Criteria.15Document21 pagesBrain Death Death by Neurologic Criteria.15Angy PalaciosNo ratings yet
- Cefaleia - ContinuumDocument195 pagesCefaleia - ContinuumRafaelNo ratings yet
- Otorrino ContinuumDocument220 pagesOtorrino ContinuumRafaelNo ratings yet
- Neurologic Complications of Lyme Disease: Review ArticleDocument11 pagesNeurologic Complications of Lyme Disease: Review ArticleHenry DanielNo ratings yet
- 1 AURa MIGRDocument9 pages1 AURa MIGRjerejerejereNo ratings yet
- Management of Cerebral Edema, Brain Compression,.4Document29 pagesManagement of Cerebral Edema, Brain Compression,.4Jorge MontenegroNo ratings yet
- Predatory Journals and Conferences: Why Fake Counts: ReviewDocument6 pagesPredatory Journals and Conferences: Why Fake Counts: ReviewFIA SlotNo ratings yet
- Predatory Journals and Conferences: Why Fake Counts: ReviewDocument6 pagesPredatory Journals and Conferences: Why Fake Counts: ReviewenriquegarciagalianaNo ratings yet
- Rapidly Progressive Dementia.16Document36 pagesRapidly Progressive Dementia.16tottocupNo ratings yet
- Preventive Migraine Treatment.7Document20 pagesPreventive Migraine Treatment.7Javıera MoyaNo ratings yet
- StrokeDocument23 pagesStrokepaola nabhanNo ratings yet
- Update On Antiseizure Medications 2022.13Document36 pagesUpdate On Antiseizure Medications 2022.13Ana Castro MondacaNo ratings yet
- 2020 Neuroimaging - in - Acute - Stroke.6Document23 pages2020 Neuroimaging - in - Acute - Stroke.6BryanNo ratings yet
- Chorea 9Document35 pagesChorea 9Cristina GhizdavetNo ratings yet
- Stroke TreatmentDocument19 pagesStroke Treatmentpaola nabhanNo ratings yet
- Disorders of The Cauda Equina: Continuum Audio Interviewavailable OnlineDocument20 pagesDisorders of The Cauda Equina: Continuum Audio Interviewavailable OnlineDalwadi1No ratings yet
- Autonomic Peripheral Neuropathy.7Document14 pagesAutonomic Peripheral Neuropathy.7thomashenrryNo ratings yet
- Palliative Care and Shared Decision Making in The.14Document14 pagesPalliative Care and Shared Decision Making in The.14AmitShettyNo ratings yet
- Psiquiatria - ContinuDocument288 pagesPsiquiatria - ContinuRafaelNo ratings yet
- Scientific American - World View 2016 (Gnv64)Document88 pagesScientific American - World View 2016 (Gnv64)Musa Rahim KhanNo ratings yet
- Low Back Pain.11-1Document20 pagesLow Back Pain.11-1Cristina GhizdavetNo ratings yet
- Continnumm Cerebrovascular Disease.2020Document316 pagesContinnumm Cerebrovascular Disease.2020CAMILA ALMENDRA VILCHES100% (2)
- Status Epilepticus, Refractory Status Epilepticus, and Super-Refractory Status EpilepticusDocument25 pagesStatus Epilepticus, Refractory Status Epilepticus, and Super-Refractory Status EpilepticusAlvaro EstupiñanNo ratings yet
- Rubber Band LigationDocument5 pagesRubber Band LigationZaeem KhalidNo ratings yet
- Charcot-Marie-Tooth Disease and Other Genetic PolyneuropathiesDocument18 pagesCharcot-Marie-Tooth Disease and Other Genetic PolyneuropathiesCristina GhizdavetNo ratings yet
- ArchitecturalDocument11 pagesArchitecturalvirnmontalesNo ratings yet
- 2020 The Place of Extracorporeal Life Support In.98996Document8 pages2020 The Place of Extracorporeal Life Support In.98996Miky DinuNo ratings yet
- Moderate and Severe Traumatic Brain Injury.7Document23 pagesModerate and Severe Traumatic Brain Injury.7gabrielpineiro14No ratings yet
- Dap - Volume 10 Issue 3 - A Resilient EconomyDocument37 pagesDap - Volume 10 Issue 3 - A Resilient Economyamirshehzad.ue.faisalabadNo ratings yet
- MODULE 9 (CARDIO 1 - THE HEART) .DrawioDocument1 pageMODULE 9 (CARDIO 1 - THE HEART) .DrawiohananpangonotanNo ratings yet
- A545 160 16 43 DI 0003 - Rev 0Document11 pagesA545 160 16 43 DI 0003 - Rev 0manishaNo ratings yet
- Acute Migraine Treatment.6Document16 pagesAcute Migraine Treatment.6BryanNo ratings yet
- Autonomic Peripheral Neuropathy: Review ArticleDocument14 pagesAutonomic Peripheral Neuropathy: Review ArticleAlaa MishrifNo ratings yet
- Rosemount 3308 Wireless Level Radar and Liquid Level Transmitter Process Connection TypesDocument3 pagesRosemount 3308 Wireless Level Radar and Liquid Level Transmitter Process Connection TypesUsman AliNo ratings yet
- Terrenos Del Estado: Municipalidad Distrital de Padre MarquezDocument1 pageTerrenos Del Estado: Municipalidad Distrital de Padre MarquezSting RiosNo ratings yet
- Medical Management of StrokeDocument6 pagesMedical Management of StrokemehakNo ratings yet
- Evaluation of Headache in Adults - UpToDateDocument18 pagesEvaluation of Headache in Adults - UpToDateSebastianNo ratings yet
- Cerebral Venous Thrombosis PDFDocument7 pagesCerebral Venous Thrombosis PDFd dNo ratings yet
- Cerebral Venous Thrombosis in Sub-Saharan Africa: A Systematic ReviewDocument7 pagesCerebral Venous Thrombosis in Sub-Saharan Africa: A Systematic ReviewDenise MacieNo ratings yet
- Cerebral Venous Thrombosis-Treatment & PrognosisDocument37 pagesCerebral Venous Thrombosis-Treatment & PrognosisMUHAMMAD09No ratings yet
- Jurnal RadiologiDocument8 pagesJurnal RadiologiNia Nurhayati ZakiahNo ratings yet
- Recognizing Vaccine-Induced Immune Thrombotic ThrombocytopeniaDocument7 pagesRecognizing Vaccine-Induced Immune Thrombotic Thrombocytopenialagopatis4No ratings yet
- Postpartum Headache: Diagnostic Considerations: Sue Yin Lim, Nikos Evangelou, Sibylle JürgensDocument8 pagesPostpartum Headache: Diagnostic Considerations: Sue Yin Lim, Nikos Evangelou, Sibylle JürgensJamie LittleNo ratings yet
- Pembimbing: Dr. Partodji, SP - Rad Oleh: 1. Ira Rahmawati 2. Pradnya Ayu 3. LimastaniDocument32 pagesPembimbing: Dr. Partodji, SP - Rad Oleh: 1. Ira Rahmawati 2. Pradnya Ayu 3. Limastaniira rahmaNo ratings yet
- Anatomic Variants and Artefacts in Non Enhanced MRDocument8 pagesAnatomic Variants and Artefacts in Non Enhanced MRlouloupavelNo ratings yet
- Headache ReviewDocument8 pagesHeadache Reviewoscar nieblesNo ratings yet
- Acute Multifocal Placoid Pigment EpitheliopathyDocument8 pagesAcute Multifocal Placoid Pigment EpitheliopathyremotmNo ratings yet
- Duration of Anticoagulation After Cerebral Venous Sinus Thrombosis 2012 Neurocritical CareDocument8 pagesDuration of Anticoagulation After Cerebral Venous Sinus Thrombosis 2012 Neurocritical Caremorris_tyoNo ratings yet
- Thesis MedicineDocument110 pagesThesis MedicineVenkatesh Korapaka100% (3)
- Literature Review On DVTDocument4 pagesLiterature Review On DVTaflsdefaq100% (1)
- A Clinical Approach To Hemiplegia: Dr. A.P.Ndondo Paediatric Neurology Department Red Cross Children's HospitalDocument62 pagesA Clinical Approach To Hemiplegia: Dr. A.P.Ndondo Paediatric Neurology Department Red Cross Children's HospitalGabrielle ElequiareNo ratings yet
- Intracerebral Hemorrhage - 2021Document32 pagesIntracerebral Hemorrhage - 2021Katherine Poma RamosNo ratings yet
- Cerebral Sinus ThrombosisDocument23 pagesCerebral Sinus ThrombosisHerinanda Fahmy FahlevieNo ratings yet
- A Pictorial Review of Postpartum ComplicationsDocument25 pagesA Pictorial Review of Postpartum ComplicationsGabriela Serra del CarpioNo ratings yet
- Conclusion: Long-Term Follow-Up ForDocument31 pagesConclusion: Long-Term Follow-Up ForHima HuNo ratings yet
- Klasifikasi Penyebab KomaDocument19 pagesKlasifikasi Penyebab KomaNoni JacksonNo ratings yet
- CEFALEA Evaluation of Headache in Adults - UpToDateDocument23 pagesCEFALEA Evaluation of Headache in Adults - UpToDateJOSE ANTONIO ALBARRAN MENDOZANo ratings yet
- Persuasive EssayDocument7 pagesPersuasive EssayJessica HopperNo ratings yet
- Stroke Associated With COVID-19 VaccinesDocument23 pagesStroke Associated With COVID-19 VaccinesTUTO TUTONo ratings yet
- ACR Criteria PDFDocument18 pagesACR Criteria PDFquickdannyNo ratings yet
- Headache Diagnosis and Treatment of 2609Document77 pagesHeadache Diagnosis and Treatment of 2609Reza Badruun Syahrul HakimNo ratings yet
- Cerebral Venous Sinus ThrombosisDocument34 pagesCerebral Venous Sinus ThrombosisNeurologia homicNo ratings yet
- Cerebral Venous and Dural Sinus ThrombosisDocument11 pagesCerebral Venous and Dural Sinus Thrombosislakshminivas PingaliNo ratings yet
- 2017 06 16 Stroke in PregnancyDocument49 pages2017 06 16 Stroke in PregnancyayubahriNo ratings yet
Woman Stroke
Woman Stroke
Uploaded by
paola nabhanOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Woman Stroke
Woman Stroke
Uploaded by
paola nabhanCopyright:
Available Formats
Stroke in Women REVIEW ARTICLE
By Hanne Christensen, MD, PhD, DMSci; Cheryl Bushnell, MD, MHS C O N T I N U UM A U D I O
I NT E R V I E W A V A I L AB L E
ONLINE
ABSTRACT
PURPOSE OF REVIEW: This
article reviews sex differences in stroke risk and
CITE AS:
presentation, with a particular emphasis on the unique risk factors women CONTINUUM (MINNEAP MINN)
experience throughout the lifespan.
Downloaded from https://journals.lww.com/continuum by l59nLqSCmRHonh5BIcVReAOwUDBfjaleiuqlNZQtzuAR+yVsUOXYmXs2wjUL2c5RzTj6fvKae/3MmGsH4vhnmFEuKGh6iQK1MAwZqr+EHUTZhbcteGmw6xL1+aR8QIlD on 04/02/2020
2020;26(2, CEREBROVASCULAR
DISEASE):363–385.
RECENT FINDINGS: Although prior studies suggested women have worse
Address correspondence to
outcomes after stroke, it is now clear that age, prestroke functional status, Dr Cheryl Bushnell, Department
and comorbidities explain many of the differences between men and women of Neurology, Wake Forest
School of Medicine, Medical
in stroke severity, functional outcomes, and mortality. Several meta-analyses
Center Blvd, Winston-Salem,
and large cohort studies have evaluated the risk factors for women related NC 27157, cbushnel@wakehealth.
to reproductive factors and found that fewer years between menarche and edu.
menopause, pregnancy complications (preeclampsia/eclampsia, preterm RELATIONSHIP DISCLOSURE:
delivery, and stillbirth), oophorectomy, hormone replacement therapy use, Dr Christensen has served on
and younger age at menopause all increase the risk of stroke. Although the the advisory board of
Boehringer Ingelheim
nonreproductive risks of stroke overlap between men and women, those International GmbH and has
with greater impact on women include age, hypertension, atrial fibrillation, received personal
socioeconomic status, and depression. compensation for speaking
engagements from Bayer AG,
Boehringer Ingelheim
SUMMARY: Significant sex differences are observed in risk factors of stroke International GmbH,
Bristol-Myers Squibb Company,
and stroke outcome. Including this information in the clinical assessment and Daiichi-Sankyo. Dr
of the individual patient may support development of more effective Christensen has received
prevention plans. research/grant support from
the Lundbeck Foundation,
Toyota Fonden Denmark, the
TrygFonden, and the Velux
INTRODUCTION Foundations and publishing
U
nderstanding sex differences and factors unique to each sex is essential royalties from Gyldendal Forlag.
Dr Bushnell has received
for neurologists and other providers to offer optimal personalized and research/grant support from
holistic care of patients with stroke throughout the continuum. the Agency for Healthcare
Research and Quality
Significant advances have been made in the field of sex differences in (1R01HS025723-01), the National
stroke in the past decade, in particular, identification of the factors that Institutes of Health/National
confound stroke outcomes. We have overwhelming evidence that age, prestroke Institute of Neurological
Diseases and Stroke
functional status, and comorbidities explain many of the differences between men (1U24NS107235-01), and the
and women in stroke severity, functional outcomes, and mortality. However, sex Patient-Centered Outcomes
differences also exist in stroke presenting symptoms and the likelihood of a stroke Research Institute
(PCS-11403-14531) and publishing
mimic, which can affect the timeliness of the acute stroke evaluation. In addition, royalties from Henry Stewart
unique biological factors throughout the lifespan that affect stroke in women, such Talks Ltd and Oxford
University Press.
as age at menarche, use of hormonal contraception, pregnancy, menopause, and use
of hormone replacement therapy, have been relatively well studied recently. This UNLABELED USE OF
article reviews the impact of these factors and highlights stroke risk factors that PRODUCTS/INVESTIGATIONAL
USE DISCLOSURE:
women and men share that may be more prevalent in women. Drs Christensen and Bushnell
report no disclosures.
EPIDEMIOLOGY OF STROKE IN WOMEN
Worldwide, stroke incidence, prevalence, and mortality are higher in men than © 2020 American Academy
women in developing countries, except in Arab countries in the Middle East of Neurology.
CONTINUUMJOURNAL.COM 363
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
STROKE IN WOMEN
and North Africa, where the stroke mortality is higher in women.1 In Israel,
women have a higher stroke mortality than men, and in western Europe, the
stroke incidence is higher or similar in women compared with men.1
In the United States, important sex differences are seen in stroke epidemiology
by age and ethnic groups. For example, the prevalence of stroke is similar
between men and women from 20 to 59 years of age but higher in men
between 60 and 79 years of age (6.5% in men versus 5.4% in women) and
higher in women older than 80 years of age (13.4% in women versus 11.5% in
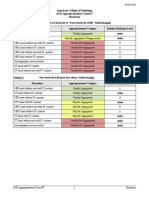
men) (FIGURE 7-1).2 The probability of death in the first year after stroke in
men and women differs widely by age and ethnicity, with the highest rate
observed in white women older than 75 years of age (36%), followed by white
men (33%), black women (27%), and black men (25%).2
An analysis of the Greater Cincinnati/Northern Kentucky Stroke Study, a
study that is representative of the general US population, was done to assess
sex-specific stroke trends from 1993–1994, 1999, 2005, and 2010. Overall, women
were about 4 years older than men at the time of stroke (72.4 years versus
68.2 years). However, when analyzing the stroke incidence trends in this cohort
over these time points, it was apparent that the incidence of stroke decreased in
men but not in women. This was despite an equivalent (and significant) trend for
increasing risk factors such as hypertension, diabetes mellitus, and hyperlipidemia
over time in both sexes. This study was not designed to assess the quality of
risk factor management, so whether this was a factor in the trends of incidence
is not known. The conclusion from this time trend study was that the overall
decrease in stroke incidence was driven by the decrease in men, but not women
(FIGURE 7-2).3
FIGURE 7-1
Prevalence of stroke by age and sex.
Reprinted with permission from Benjamin EJ, et al, Circulation.2 © 2019 American Heart Association, Inc.
364 APRIL 2020
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
KEY POINT
● Although the incidence of
stroke up to 2010 appeared
to be decreasing overall,
this trend is driven by a
decrease in incidence in
men, not women.
FIGURE 7-2
Ischemic stroke incidence rates and trends over time by sex. Incidence rates were adjusted
by age and race. P values for comparisons made between 1993/1994 and 2010 were P<.001 in
men and P=.09 in women.
Reprinted with permission from Madsen TE, et al, Neurology.3 © 2017 American Academy of Neurology.
Since women live longer than men and have a higher lifetime risk of stroke
(17% versus 15% after age 50),4 it is important to focus on the epidemiology of
stroke in older women. By applying age-specific and sex-specific data from the
US Census Bureau and US stroke mortality data, 32,000 more stroke deaths
occurred in white women versus white men in the year 2000, and this number is
projected to reach 68,000 more deaths in white women than in white men by
2050.5 Projections yielded similar results in other ethnicities. INSTRUCT
(INternational STRoke oUtComes sTudy), a pooled analysis of 13 population-based
studies in Europe, Australasia, South America, and the Caribbean between 1987
and 2013, showed that the crude mortality rate was higher for women than men,
but this was reversed after adjustment for age, prestroke functional limitations,
stroke severity, and history of atrial fibrillation.6 This analysis clearly illustrates the
importance of including these variables in any outcome analysis of sex differences,
especially mortality.
Now that we are in the era of endovascular treatment for ischemic stroke
due to large vessel occlusions, the focus has shifted from mortality to survival
with mild to moderate disability.7–9 Because women obtain the same benefit
from this treatment as men based on a pooled analysis of the clinical trial
participants7 and successful revascularization appears to be more important
than age in predicting outcome,10 their increased survival will likely lead
to more women with cognitive and physical disability from stroke in the
future.
RISKS UNIQUE TO WOMEN ACROSS THE REPRODUCTIVE LIFESPAN
Women have unique biological and pharmacologic factors that pose potential
risks for stroke based on reproductive and hormonal changes throughout the
CONTINUUMJOURNAL.COM 365
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
STROKE IN WOMEN
lifespan. These include age of menarche, use of hormonal contraception,
pregnancy, and menopause.
The relationship between the onset of menarche and stroke is of interest but
varies depending on the outcome of incidence versus mortality. One of the
largest studies to attempt to examine this was the United Kingdom Million
Women Study, which included more than 1 million middle-aged UK women
between 60 and 64 years of age. Interestingly, a U-shaped relationship was seen
TABLE 7-1 Causes of and Risk Factors for Stroke in Pregnancya
Ischemic Hemorrhagic
Cause/Risk Factor Stroke Stroke
African American race X X
Amniotic fluid embolism X
Antiphospholipid antibody syndrome X
b
Arteriovenous malformation X
Atrial fibrillation X
Cardioembolism/congenital heart defects X
Cerebral aneurysmb X
Cervical artery dissection X
Choriocarcinoma X
Chronic kidney disease X X
Coagulopathy X X
Congestive heart failure X
Diabetes mellitus X
HELLP (hemolysis, elevated liver enzymes, and X X
low platelet count) syndrome
Hypertensive disorders of pregnancyc X X
Migraine X X
Older age X X
Peripartum cardiomyopathy X
Peripartum infection X X
Posterior reversible encephalopathy syndrome (PRES) X X
Primary thrombocytopenia X X
Reversible cerebral vasoconstriction syndrome X X
Systemic lupus erythematosus X
a
Data from Swartz RH, et al, Int J Stroke15 and Hovsepian DA, et al, Stroke.18
b
Subarachnoid hemorrhage.
c
Includes prepregnancy hypertension.
366 APRIL 2020
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
between age at menarche and risk of incident stroke.11 Those women with onset KEY POINT
of menarche at age 13 had the lowest risk of cerebrovascular disease, whereas
● Age at menarche at
those with onset earlier than age 10 or after age 17 had the highest risks. The 10 years of age or younger
pattern for incident coronary heart disease was similar, but a higher relative risk increases the risk of stroke
was seen for coronary heart disease than for cerebrovascular disease.11 Similarly, later in life by about 25%.
the Nurses’ Health Study showed that menarche at an extremely early age
(10 years or younger) was associated with a 1.25 times greater risk of nonfatal or
fatal stroke (odds ratio, 1.25; 95% confidence interval [CI], 1.07 to 1.46).12
However, a systematic review of age at menarche and risks of all-cause and
cardiovascular death found no association between age at menarche and death
from stroke.13 One possible explanation for the stroke and cardiovascular disease
risk associated with very early age at menarche could be childhood obesity,
which is associated with higher exposure to endogenous estradiol and earlier
onset of puberty.14
PREGNANCY-RELATED STROKE
Although it is uncommon, pregnant and postpartum women are at 3 times
higher risk of stroke than other young adults.15 A 2017 systematic review and
meta-analysis of 11 studies reported a crude incidence rate of 30.0 per 100,000
pregnancies (95% CI, 18.8 to 47.9), and the rates for ischemic stroke, cerebral
venous sinus thrombosis, and intracerebral hemorrhage are roughly equal within
this combined rate.15 Incidence according to the timing of stroke is approximately
18.3 per 100,000 during the antepartum (before delivery)/peripartum
(immediately before and during delivery) period and 14.7 per 100,000 during
the postpartum (after delivery) period.15 However, pregnancy-related stroke
incidence has been increasing over time, particularly postpartum, as shown by
an 83% increase from 1994 to 2007. This was related to a concurrent increase in
heart disease and hypertension during this same time period.16
Hypertensive disorders of pregnancy, including preeclampsia, eclampsia, and
gestational hypertension, are associated with both ischemic and hemorrhagic
stroke as well as underlying vasculopathies leading to both stroke types, such as
reversible cerebral vasoconstriction syndrome (RCVS) and posterior reversible
encephalopathy syndrome (PRES).15 In addition, preeclampsia/eclampsia is
associated with both preterm birth and late-term/postpartum complications.
Hypertensive disorders of pregnancy, which increased in prevalence from 1994
to 2011, confer a more than a fivefold increase in the risk of stroke compared
to women without these conditions.17 If women have congenital heart disease
(odds ratio, 13.1; 95% CI, 9.90 to 18.90), atrial fibrillation (odds ratio, 8.1; 95%
CI, 4.4 to 14.9), primary thrombocytopenia (odds ratio, 5.5; 95% CI, 3.05 to 9.93),
or migraine (odds ratio, 4.5; 95% CI, 3.4 to 5.9) in addition to one of these
hypertensive disorders, the risk increases substantially.17 Of note, if
anticoagulation for stroke prevention is indicated, as with atrial fibrillation or
stroke from a hypercoagulable state before pregnancy, guidelines recommend
low-molecular-weight heparin with or without low-dose aspirin (less than
100 mg/d) for thromboprophylaxis during pregnancy. The causes of and risk
factors for ischemic stroke and hemorrhagic stroke during pregnancy and
postpartum are listed in TABLE 7-1.15,18 The most common causes of ischemic
stroke are cardioembolism, coagulopathy, and preeclampsia/eclampsia, whereas
aneurysm, arteriovenous malformation, preeclampsia/eclampsia, HELLP
(hemolysis, elevated liver enzymes, and low platelet count) syndrome, and
CONTINUUMJOURNAL.COM 367
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
STROKE IN WOMEN
coagulopathy are the most common causes of hemorrhagic stroke during
pregnancy.15 Risk factors for both stroke types during pregnancy overlap with
those noted for nonpregnant young adults, but those unique to pregnancy
include peripartum cardiomyopathy, choriocarcinoma, and amniotic fluid
embolus, the latter of which is very rare.
Given the fact that peripartum stroke affects young mothers and families, data
related to mortality and disability are important. An administrative study of
hospital discharges reported a case fatality rate of 4.1% and mortality rate of 1.4
per 100,000 deliveries for pregnancy-related stroke. Also, 22% of women with
pregnancy-related strokes were discharged to facilities other than home, which
was significantly higher than the 3% of all other pregnancy-related discharges.19
For hypertensive disorders of pregnancy, cerebrovascular complications make
up about 40% of maternal deaths.20 In an analysis of women with hypertensive
disorders of pregnancy and stroke compared to women without hypertensive
disorders of pregnancy and stroke, a 29% increased risk of death during
hospitalization (odds ratio, 1.29; 95% CI, 1.02 to 1.64), a 93% increased risk of
mechanical ventilation (odds ratio, 1.93; 95% CI, 1.63 to 2.25), and a 23% increased
chance of discharge to a facility rather than home (odds ratio, 1.23; 95% CI, 1.08
to 1.40) were seen.17
Acute stroke imaging is critical for treatment decisions, and pregnant women
are no exception. Noncontrast CT imaging for acute stroke is acceptable during
all trimesters and postpartum, particularly because the risk of missing the
diagnosis of a stroke outweighs the risk of the radiation. Similarly, iodinated
contrast, which is required for CT angiography and perfusion, is considered
acceptable if the information, such as confirmation of a large vessel occlusion,
cannot be acquired without contrast. MRI without gadolinium is considered safe
in pregnant women regardless of gestational age when the information gained
from the imaging cannot be delayed until after delivery.21
Treatment of acute ischemic stroke in pregnancy has been somewhat
controversial because of a lack of randomized controlled trials and the ethical
issues surrounding mother and fetus. However, the Canadian Stroke Best
Practices Consensus Statement recently provided recommendations for the
management of pregnant women with an acute stroke.22 These guidelines state it
is reasonable to consider giving IV alteplase to a pregnant woman who otherwise
meets the thrombolysis criteria and has a disabling ischemic stroke, but this
should be performed with the guidance of an interdisciplinary team that includes
vascular neurology, maternal-fetal medicine, and interventional radiology or
vascular neurosurgery and consideration of the wishes of the patient and her
family or next of kin. Alteplase does not cross the placenta and is not expected to
increase the risk of intracranial or systemic bleeding in the fetus, so the decision
to administer this drug is based on maternal bleeding risk associated with the
acute stroke. Thrombolytics administered in the early postpartum period are
associated with an increased risk of bleeding, so this is another consideration in
women with stroke within 48 hours of delivery. Endovascular thrombectomy is
also an option for large vessel occlusions in a pregnant woman (with appropriate
abdominal shielding and limited use of x-ray exposure). It could be considered
reasonable to forgo IV alteplase for a woman with known large vessel occlusion
who meets criteria for thrombectomy after weighing all risks and benefits of both
options, if the increased risk of maternal bleeding is likely to outweigh the benefit
of adding IV alteplase to endovascular therapy.22 Recommendations are also
368 APRIL 2020
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
provided for treatment of pregnant women with hemorrhagic stroke, with a KEY POINTS
focus on blood pressure management for intracerebral hemorrhage and imaging
● Women with
to diagnose and treat aneurysms or arteriovenous malformations.22 preeclampsia have an
Secondary prevention of ischemic stroke for women with a stroke during increased risk of both
pregnancy or those who have a history of stroke and are at high risk (such as with ischemic and hemorrhagic
multiple strokes or the presence of atrial fibrillation) and wish to become stroke in the peripartum and
postpartum periods, and
pregnant is also covered in detail in the Canadian Stroke Best Practices Consensus
this risk increases with
Statement, again encouraging an interdisciplinary approach for management additional comorbidities
(TABLE 7-2 and CASE 7-1).23 such as atrial fibrillation,
Another risk of stroke unique to women is the long-term consequence of migraine, or congenital heart
disease.
pregnancy complications, specifically of hypertensive disorders of pregnancy.
Women who have had hypertensive disorders of pregnancy have 3.7 times the ● Pregnant women with an
risk of new-onset hypertension after 14 years of follow-up compared to women acute stroke may be
who have not had hypertensive disorders of pregnancy.24 A 2017 systematic candidates for either IV
review and meta-analysis reported that women who have had hypertensive thrombolysis or
thrombectomy; referral to a
disorders of pregnancy have 1.8 times the cumulative increased risk of stroke in center with multidisciplinary
the years following childbearing.25 Interestingly, the complications are not expertise is essential for
limited to stroke, but hypertensive disorders of pregnancy also confer a 4 times these treatment decisions.
greater risk for heart failure, a 2.5 times greater risk of coronary heart disease, and
● Hypertensive disorders of
a 2.2 times greater risk of cardiovascular death.25 Other important consequences
pregnancy increase the risk
of hypertensive disorders of pregnancy are a greater extent of white matter of multiple vascular
lesions (especially in the temporal lobe), altered microstructural integrity, and complications later in life,
reduced cortical volume compared to women without hypertensive disorders of including hypertension,
stroke, heart disease, heart
pregnancy.26 One population-based study of death certificates in Utah reported
failure, and cerebral
an increased risk of all-cause mortality (adjusted hazard ratio, 1.65; 95% CI, 1.57 to microvascular disease.
1.73) in women with hypertensive disorders of pregnancy. The greatest excess
mortality for women with hypertensive disorders of pregnancy was with death
from Alzheimer disease, diabetes mellitus, ischemic heart disease, and stroke.27
CEREBRAL VENOUS SINUS THROMBOSIS
Thrombosis of the cerebral veins or venous sinus is an uncommon cause of stroke
(less than 0.5% to 1% of all strokes) and tends to occur more frequently in young
adults. Women are affected by cerebral venous sinus thrombosis 3 times more
often than men. Cerebral venous sinus thrombosis may be associated with
acquired or genetic (ie, thrombophilias) risk factors; among those that are
acquired include transient triggers, such as pregnancy, puerperium, surgery,
trauma, or exogenous hormones. Cancer or antiphospholipid syndrome may be
considered a permanent trigger. Women with sex-specific risk factors have a far
better prognosis than men or older women.28
The most common presenting sign of cerebral venous sinus thrombosis is
headache, followed by seizure, but focal signs or symptoms are uncommon.
Cerebral venous sinus thrombosis is diagnosed with imaging that could include
CT and CT venography, or MRI and MR venography, although MRI is considered
more sensitive.29 Management of cerebral venous sinus thrombosis includes
parenteral anticoagulation, regardless of the presence of hemorrhage due to
venous congestion, and low-molecular-weight heparin is recommended as it may
be more safe and effective than unfractionated heparin to be followed by oral
anticoagulation with vitamin K antagonists or dabigatran etexilate generally
recommended for 3 to 12 months.30,31 During pregnancy, treatment of cerebral
venous thrombosis includes low-molecular-weight heparin subcutaneously at
CONTINUUMJOURNAL.COM 369
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
STROKE IN WOMEN
therapeutic doses. For women with a history of cerebral venous sinus
thrombosis, pregnancy is not contraindicated as long as prophylactic
low-molecular-weight heparin is administered during pregnancy.32
HORMONAL CONTRACEPTION
The risk of ischemic stroke is estimated to be about 2 times higher in those
who use estrogen-containing oral contraceptives than in nonusers, but this risk
TABLE 7-2 Approach to Secondary Prevention of Stroke for Women With a History of
Stroke During or Outside of Pregnancya
Approach Suggested Providers
Prepregnancy counseling
Discuss future pregnancy and risk of recurrent stroke Neurology, vascular neurology
Ensure previous stroke etiology was fully investigated and appropriate secondary Neurology, vascular neurology
prevention strategies are in place
Discuss contraception options: progesterone-only oral contraception, Gynecology, primary care, neurology
progesterone-only or nonhormonal intrauterine devices, or barrier contraception;
estrogen-containing contraceptives should be avoided in most cases
Stroke risk factor assessment and lifestyle factors: healthy diet, regular exercise, Obstetrics/gynecology, primary
normal body mass index, smoking cessation, alcohol use care, neurology, vascular neurology
Review medications for potential teratogenicity Obstetrics/gynecology, primary care
Communication between health professionals regarding care plan Obstetrics/gynecology, primary
care, neurology, vascular neurology
Antenatal and intrapartum risk factor screening for women with a history of stroke
Screen for and assess vascular risk factors, counsel for healthy lifestyle behaviors Obstetrics/gynecology, neurology,
vascular neurology
Individualized stroke prevention management plans developed based on medical High-risk obstetrics/gynecology
history, stage of pregnancy, stroke type/etiology, stroke recurrence risk, personal (maternal fetal medicine), neurology,
goals and preferences vascular neurology
Postpartum stroke prevention management for women with a history of stroke
Educate women on signs and symptoms of stroke and what to do (face, arm, speech, Neurology, vascular neurology,
time [FAST], and call 911) because the first 6 weeks postpartum is highest risk period obstetrics/gynecology, primary care
Women with diabetes mellitus, hypertension, preeclampsia, or other high-risk Obstetrics/gynecology, primary care
conditions may need close postpartum monitoring
Review long-term stroke prevention plan and breast-feeding Neurology, vascular neurology
Prior stroke is not a contraindication to breast-feeding
Women with a prior stroke may need assistance for this task and other tasks to
care for the baby
Stroke prevention medications should be evaluated for compatibility with
breast-feeding; if high risk for thromboembolism in the first 6 weeks postpartum,
anticoagulation with either low-molecular-weight heparin or warfarin is a safe option
a
Data from Swartz RH, et al, Int J Stroke.23
370 APRIL 2020
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
varies based on the estradiol dose, according to two meta-analyses and a large
population-based case-control study.33–35 A 2015 Cochrane Review confirmed a
1.7 times greater risk of stroke and a similar magnitude of increased risk with
increased doses of estrogen.36 However, progestin-only contraception (including
pills, injectables, implantables, and intrauterine devices) confer no significant
increased risk of stroke or acute myocardial infarction to users compared to
nonusers.37 A systematic review found no increased risk of arterial
A healthy 24-year-old woman, gravida 1, para 0, delivered a healthy baby CASE 7-1
boy by cesarean delivery. Twelve days after delivery, she developed right
leg weakness and had a seizure. On evaluation, she had very high blood
pressure, and her MRI showed two separate hemorrhages (not shown),
with fluid-attenuated inversion recovery (FLAIR) images showing
vasogenic edema suggestive of posterior reversible encephalopathy
syndrome (PRES) (FIGURE 7-3). She described later that she had been very
edematous in her face and her limbs, and her blood pressure had
increased before delivery but not to the typical cutoff to qualify as
preeclampsia (>140/90 mm Hg). She was treated for postpartum
eclampsia with IV magnesium and discharged with no neurologic deficits.
Two years after the eclamptic
event, she presented with intermittent
episodes of right-sided numbness.
MRI repeated at that time showed only
minimal changes as a result of the
prior hemorrhage. She was diagnosed
with partial seizures and treated with
lamotrigine. She then developed
extremely painful cystic ovaries and
was prescribed an oral contraceptive.
The oral contraceptive, however, led
to increased clearance of lamotrigine,
lowered blood levels, and, thus, an
increase in her seizures, so the oral
contraceptive was ultimately stopped.
After another 2 years, she became
FIGURE 7-3
pregnant again and struggled with Imaging of the patient in CASE 7-1.
lamotrigine dosing and seizure control Coronal fluid-attenuated inversion
during pregnancy. Near the time of recovery (FLAIR) MRI showing bilateral
posterior parietal hyperintensities
delivery, she again developed
consistent with vasogenic edema from
preeclampsia but did not have any posterior reversible encephalopathy
cerebrovascular complications. syndrome (PRES).
This case illustrates the immediate and long-term consequences of COMMENT
eclampsia; in addition, women who have had eclampsia are at risk for
hypertension, cardiovascular disease, and, most important, stroke within
10 years of childbearing.
CONTINUUMJOURNAL.COM 371
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
STROKE IN WOMEN
thromboembolism with contraceptive patches compared to oral contraceptives,
but venous thromboembolism was higher in patch users than in oral users.38
Women who have a history of stroke are generally recommended to avoid
estrogen-containing hormonal contraception (TABLE 7-2).39
MENOPAUSE, VASOMOTOR SYMPTOMS, AND HORMONE
REPLACEMENT THERAPY
Menopause can be defined as the absence of menstrual periods for at least 12
consecutive months. The average age of menopause is 51 years, ranging from
40 to 60 years.40 Reduced endogenous estrogen synthesis, which is a sign of
reproductive and somatic aging, is at the core of the physiologic changes of
menopause. Estrogen has a protective effect on vessels41; thus, longer deprivation
of this estrogen benefit as women age would theoretically occur with earlier age of
onset of menopause. Therefore, age of onset of menopause is an important
potential sex-specific risk factor for cardiovascular disease and stroke later in life.
Studies of age of spontaneous onset of menopause excluded women with
menopause as a result of hysterectomy/oophorectomy. The onset of menopause at
45 years or younger is considered early, but the risk of stroke is uncertain based on
mixed results.42 A meta-analysis of 32 studies reported no increased risk of overall
stroke with age at menopause younger than 45 years (relative risk, 0.99; 95% CI,
0.92 to 1.07) and a small but significant increased risk of stroke mortality (relative
risk, 1.19; 95% CI, 1.08 to 1.31).43 The risk of overall coronary heart disease, in
contrast, was 1.5 times higher for early menopause (relative risk, 1.5; 95% CI, 1.28
to 1.76).43 Age at menopause younger than 40 years, however, was associated with
a higher risk of cardiovascular disease (relative risk, 1.32; 95% CI, 1.16 to 1.51), total
stroke (relative risk, 1.25; 95% CI, 1.04 to 1.51), and total coronary heart disease
(relative risk, 1.37; 95% CI,1.14 to 1.63) in the Nurses’ Health Study,12 suggesting
that very early age of spontaneous menopause onset is an important factor.
In addition to studying the onset of menopause and stroke risk, some studies
have included an analysis of the reproductive lifespan. This is measured by
subtracting the age at menarche from the age at menopause. An analysis of the
Nurses’ Health Study found that a reproductive lifespan of 30 years or less was
independently associated with an increased risk of total stroke after adjustment
for relevant demographics, stroke risk factors, use of oral contraceptives or
hormone replacement therapy, and type of menopause (natural versus surgical)
(relative risk, 1.27; 95% CI, 1.06 to 1.52).12 In addition, reproductive lifespan, age
at menopause, and age at menarche were all significantly associated with total
cardiovascular disease risk in women who never used hormone therapy.12 Again,
the putative mechanisms for these risks likely pertain to the shortened exposure
to beneficial endogenous estradiol and subsequent increases in higher-risk lipid
profiles contributing to atherosclerosis.12
Vasomotor symptoms, which include hot flushes and night sweats, are
associated with the menopausal transition. Up to 82% of women undergoing
menopause experience these symptoms, and the intensity and duration
of the symptoms vary.44 A systematic review reported that women with
vasomotor symptoms had increased risks of coronary heart disease, stroke,
and cardiovascular disease compared to women without symptoms, but the
risk of stroke was attenuated after adjustment for established cardiovascular
risk factors.45 Vasomotor symptoms may be associated with a higher
prevalence of cardiovascular disease risk factors (such as hypertension and
372 APRIL 2020
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
hyperlipidemia), and the interrelationship between the autonomic nervous KEY POINT
system and other mental health aspects of menopause, such as anxiety,
● A reproductive lifespan of
depression, panic attacks, and poor sleep, could thereby increase the less than 30 years (age of
cardiovascular risk.46 menarche subtracted from
Hormone replacement therapy is presently used to reduce vasomotor the age at menopause) is
symptoms. The impact of hormone replacement therapy—especially with associated with an
increased risk of stroke.
estrogen—on thromboembolic diseases has been studied extensively. The
present understanding is that late (>10 years after menopause) introduction of
hormone replacement therapy increases risk of thromboembolic events, whereas
early introduction confers little to no risk.47,48 Further, transdermal estrogen is
safer than oral but remains underused.49,50 A practical guide to the
recommendation of hormone replacement therapy based on evidence from the
Women’s Health Initiative and other studies was published in 2014.51 This
algorithm guides the clinician based on the presence of vasomotor symptoms,
the patient’s history of cardiovascular disease or stroke, and the 10-year risk of
coronary heart disease based on the Framingham Risk Score. Key factors in
whether prescription may be safe include the degree of future coronary heart
disease risk and the years since the last menstrual period. In general, as stated
above, hormone replacement therapy should be avoided in women who are more
than 10 years from menopause or who have significant risk factors or have had a
cardiovascular disease event (FIGURE 7-4 and CASE 7-2).51
To summarize the unique risks for women, a systematic review and meta-
analysis assessed all sex-specific risks of stroke, including those relating to
preterm birth, spontaneous abortion, stillbirth, oophorectomy, hysterectomy,
and menopause.52 In addition, male-specific risks related to androgen-deprivation
therapy, orchiectomy, and erectile dysfunction were summarized, illustrating
FIGURE 7-4
Flowchart for identifying appropriate women for postmenopausal hormone therapy (HT).
CHD = coronary heart disease; TIA = transient ischemic attack.
Reprinted with permission from Manson JE, Fertil Steril.51 © 2014 American Society for Reproductive
Medicine.
CONTINUUMJOURNAL.COM 373
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
STROKE IN WOMEN
CASE 7-2 A 58-year-old woman with a history of type 1 diabetes mellitus since her
late twenties had multiple brief episodes of diplopia and vertigo over the
course of several weeks. She saw her primary care provider, who ordered
an MRI of the brain, which showed multiple small subacute infarcts in the
posterior circulation, multifocal microvascular disease, and old lacunar
infarcts.
Neurological consultation was obtained, and vascular workup with CT
angiography of her head and neck showed no evidence of vasculopathy.
A transthoracic echocardiogram showed a patent foramen ovale (PFO),
which was confirmed with a transesophageal echocardiogram, and
considered to be high risk for recurrent stroke. Her PFO was closed by an
interventional cardiologist, and she was placed on aspirin 325 mg/d and
clopidogrel 75 mg/d.
Her hematologic workup revealed a positive lupus anticoagulant
screen and confirmation assay, and her β2-glycoprotein I IgG was mildly
positive. She admitted that her diabetes mellitus had been poorly
controlled for the past 12 to 18 months, with a hemoglobin A1c of 8.3%. She
also admitted that she had been taking conjugated equine estrogen
0.3125 mg plus cyclic medroxyprogesterone since her early midforties for
vasomotor symptoms, but she had not revealed this to the neurologists
treating her for the stroke.
She stopped the hormone replacement therapy at the advice of her
neurologist and improved her diabetes control. Repeat antiphospholipid
testing performed 6 to 9 months after her stroke and after the initial
positive testing was normal.
Two years after her PFO closure, she stopped clopidogrel with
approval from her cardiologist. However, 2 weeks later, she had
recurrent diplopia and vertigo symptoms. MRI again showed new, tiny,
subacute infarcts in the posterior circulation, so she was started back on
clopidogrel.
Less than 1 year after the recurrent strokes, she was diagnosed with
ovarian cancer. She underwent surgical resection and received
chemotherapy, and her cancer went into remission.
COMMENT This case illustrates several important points about stroke in women. First,
a complete list of the patient’s medications should always be obtained,
and patients who are perimenopausal or postmenopausal should be asked
about the use of hormones of any kind. Second, antiphospholipid
antibodies can be positive in the setting of poorly controlled cardiovascular
risk factors (in this case, diabetes mellitus) and in cancer. Most likely, the
ovarian cancer and her hormone replacement therapy use (during the first
occurrence of strokes) contributed to her hypercoagulability. In a patient
with PFO, clots can form at the site; following PFO closure in this patient,
clot formation on the closure device after stopping the clopidogrel likely
contributed to the embolic-appearing strokes.
374 APRIL 2020
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
that men have a mild to moderately significant risk for stroke with these KEY POINT
conditions.52
● Women have strokes at
older ages and tend to have
UNMODIFIABLE RISK FACTORS COMMON TO MEN AND WOMEN lower levels of education
Some stroke risk factors, including age and socioeconomic status, than men, so it is important
are unmodifiable. to tailor necessary
resources accordingly.
Age
The risk of stroke increases with increasing age,53 and as women live longer
than men, their accumulated risk of stroke is greater. At the time of stroke,
women are older than men, but that does not lessen the importance of secondary
prevention. Individualized treatment decisions should include consideration of
multimorbidity and primary prevention, the risks of polypharmacy, and the lack
of evidence of benefit from some prevention strategies in the oldest-old (older
than 85 years of age) as well as in severe dementia.54 Involving the patient and
family members in these decisions and stating the pros and cons of a variety of
options often simplifies the issue, as many patients and their family members
already have preferences, including to what extent they are willing to accept the
burden of examinations and pharmacotherapy.
Socioeconomic Status
Socioeconomic status affects the risk of stroke, and the lowest income group has
a higher risk of stroke compared to the highest income group.55,56 Sex differences
have not been observed despite older age, lower education, and lower income
in women,57 although cardiovascular disease risk from low socioeconomic status
is higher in women.55 This observation of higher risk of cardiovascular disease
due to low socioeconomic status is partly, but not entirely, dependent on risk
factor profiles. Living in a deprived neighborhood, a less than adequate
household income, and a low level of education are related to a higher risk of
stroke in both men and women.58–60 In a large European study, low education
increased the likelihood of stroke in women (hazard ratio, 1.41; 95% CI, 1.16
to 1.71) with significant geographic variation in the degree to which this was
explained by risk factors.58 In US cohorts such as the Greater Cincinnati/
Northern Kentucky Stroke Study, women with stroke had consistently lower
levels of education compared to men with stroke.3 It is essential to recognize this
disparity and to ensure that educational materials are written at the lay level, that
free or low-cost medications are presented as options, and that local community
support services are identified, if available.
MODIFIABLE RISK FACTORS
Modifiable stroke risk factors are risk factors that can be modified by lifestyle
changes, pharmacotherapy, and interventions. Lifestyle varies between men and
women; further, some sex differences may exist with regard to impact on risk.
Physical Inactivity
Physical activity reduces the lifetime risk of cardiovascular diseases, including
stroke, in women at least to the same degree as in men and possibly more,61 with
one study suggesting a 25% reduction in risk of major cardiovascular disease in
high physical activity compared to low physical activity and a trend toward larger
effect sizes in women.62 Physical activity has a number of beneficial effects for
CONTINUUMJOURNAL.COM 375
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
STROKE IN WOMEN
primary and secondary prevention of stroke, including reduction of blood
pressure and increasing glycemic control.
Physical inactivity is extremely common among women: 41.6 % of women
from high-income countries are insufficiently physically active compared to
32% of men.63 Physical inactivity before stroke is a stronger predictor of poor
functional outcome than body mass index,64 and as more women than men
are physically inactive, poor functional outcome will affect more women than men.
The frequency of physical activity generally considered in studies is
75 minutes or more of vigorous intensity activity per week or 150 minutes or
more of any combination of moderate plus vigorous intensity activity per week.65
Clinicians are now being encouraged to routinely measure physical activity as a
“vital sign” in primary care, which is highly relevant for secondary stroke
prevention in the appropriate individuals.66 In addition, an important aspect of
recovery is that physical activity is positively associated with improving
cognition poststroke.67
Depression, Anxiety, and Stress
Depression is a recognized risk factor for stroke, and dose dependency exists
between the severity of the affective disorder and the risk of stroke.68 Interestingly,
the impact on stroke risk with depression may be higher in men.69 However,
women have a higher prevalence of depression than men. The mechanism
behind the relationship between depression and stroke risk is at least partially
explained by higher rates of poor health factors in patients with depression:
women with depression are more likely to be single, have a high body mass
index, smoke, and be physically inactive.43
Irritability; nervousness; anxiety; sleeplessness associated with problems
including health, family, finance, or job situation; and stressful life events are
associated with an increased risk of stroke and to a higher degree in women than
in men.70 Social isolation and loneliness are also risk factors for stroke and
acute myocardial infarction.71 This is important because women are more likely
to be living alone at the time of stroke. In addition, depression is associated
with worse outcomes after stroke.72
Women holding high-strain jobs characterized by high psychological stress
and low levels of control are reported to have a higher risk of stroke than women
with low-strain jobs, a difference not observed in men.73,74 This aspect of stroke
risk is underappreciated and as yet understudied.
Sex Differences in Risk Factors Modified Pharmacologically
A number of risk factors are modified pharmacologically in addition to
promotion of lifestyle changes. Several sex differences in prevalence of risk
factors have been observed, such as hypertension and atrial fibrillation. For other
topics such as sex differences and management of carotid artery disease, we
refer the reader to the respective articles in this issue.
HYPERTENSION. After menopause, blood pressure levels increase in women, and
in patients with stroke, rates of hypertension are significantly higher in women
(60%) than in men (56%; P<.0001), as shown in a Swedish observational study.75
No differences are seen in the impact of hypertension on stroke risk between
men and women,76 but a disadvantage in awareness of treatment and control of
blood pressure in women has been reported,77 and older women, in particular,
376 APRIL 2020
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
have a significantly lower likelihood of achieving their target blood pressures.78 KEY POINTS
Major first-line antihypertensive classes, such as angiotensin-converting enzyme
● Compared to men,
inhibitors, calcium channel blockers, and diuretics, have comparable stroke risk women have a higher
reductions in men and women (CASE 7-3).79 The link between hypertension and prevalence of hypertension
atrial fibrillation is well documented in multiple studies showing a significantly over age 65, and women
higher incidence of new-onset atrial fibrillation in those with hypertension with stroke are more likely
to have hypertension,
compared to normotensive individuals.80 Given the higher prevalence of
probably due to older
hypertension in women older than 65 years of age and longer lifespans in women, age of stroke onset.
this may be one reason the combination of risk factors is more prevalent in
women than men with stroke, although this requires more study. ● Atrial fibrillation has a
higher impact on the risk of
stroke in women compared
ATRIAL FIBRILLATION. Atrial fibrillation has a higher impact on the risk of stroke to men. This can be
in women compared to men. This can be explained by the more advanced age explained by the more
in women at the time of stroke, that atrial fibrillation carries twice the risk advanced age in women at
of stroke in women in comparison to men, and, further, women have more the time of stroke, that atrial
fibrillation carries twice the
severe stroke presentations in stroke related to atrial fibrillation than men.81,82 risk of stroke in women in
Women may have more benefit from non–vitamin K antagonists than from comparison to men, and,
vitamin K antagonists compared to men,83 but women (and specifically older further, women have more
women) were underrepresented in trials, weakening this conclusion. A 2017 US severe stroke presentations
than men in stroke related to
report based on 691,906 people with atrial fibrillation reported that women were atrial fibrillation.
significantly less likely to receive oral anticoagulants at all levels of the
CHA2DS2VASc (congestive heart failure, hypertension, age 75 years or older, ● Women are more likely to
diabetes mellitus, stroke, vascular disease, age 65 to 74 years, sex category present with nontraditional
stroke symptoms and
[female sex]) score.84
mimics than men.
STROKE SIGNS AND SYMPTOMS IN WOMEN COMPARED WITH MEN
Studies that examined differences in stroke presenting symptoms published in
the past 10 years found that, in general, women are more likely to present with
nontraditional stroke symptoms compared to men.85–89 Nontraditional
symptoms included headache, fatigue, disorientation, lightheadedness, nausea,
hiccups, nonfocal weakness, chest pain, palpitations, shortness of breath,
difficulty understanding, change in vision, feeling “funny,” fatigue, malaise,
impaired or loss of consciousness, and altered mental status.86–89 Overall, no major
differences in the most common stroke symptoms are seen between men and
women.88 Nontraditional stroke symptoms could lead to delays in stroke recognition
and, thus, delays in brain imaging and acute stroke evaluation.85
In addition, women are more likely to present with stroke mimics, including
complicated migraine, seizure, neoplasm, metabolic disturbances, spinal cord
lesions, and psychiatric conditions (functional neurologic disorders). A
meta-analysis reported that female sex predicted a higher risk of nonorganic
stroke mimics90; in a large study of unselected stroke patients, 33% of women
versus 26% of men (P<.001) had a final stroke mimic diagnosis.91 Again, this is a
factor that can interfere with timely evaluation of possible strokes and
create delays.
It is, however, important to acknowledge that patients come “in packages,”
with age, multiple comorbidities, and physical limitations that may be associated
with their presentation when seen in the emergency setting. For example,
women tend to be older; live alone; have more comorbidities; and be more prone
to cardioembolic stroke, more severe strokes, and unusual presentations. Men,
on the other hand, tend to be slightly younger and more frequently have large
CONTINUUMJOURNAL.COM 377
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
STROKE IN WOMEN
vessel disease. Also, early studies of sex differences may not have adjusted for age
and prestroke comorbidities/function, which often explains much of the
variation between men and women.
ACCESS TO TREATMENT
In the acute stroke setting, women tend to have longer times from arrival to
imaging.85 Although study results vary, drawing definitive conclusions about sex
CASE 7-3 An 86-year-old woman was admitted with left hemiplegia and anosognosia.
She had likely been lying helpless on her kitchen floor for 10 hours before
being found. Before the stroke, she was a completely independent
widow living an active life. She had uncontrolled hypertension (treated
with a thiazide diuretic and candesartan) and hypercholesterolemia
(controlled by simvastatin) and used vaginal estradiol.
On admission, her blood pressure was 190/95 mm Hg, and her National
Institutes of Health Stroke Scale score was 12. Noncontrast head CT
showed a probable ischemic stroke with hemorrhagic conversion in the
right middle cerebral artery territory (FIGURE 7-5A). CT angiography showed
no large vessel occlusions or significant atherosclerosis in precerebral or
intracranial arteries (FIGURE 7-5B). Diffusion-weighted and fluid-attenuated
inversion recovery (FLAIR) MRI on day 3 confirmed the diagnosis of
ischemic infarct with hemorrhagic conversion (FIGURE 7-5C and FIGURE 7-5D).
All blood tests were within the normal range, but ECG revealed long
periods of atrial fibrillation, despite sinus rhythm on admission.
COMMENT In this case, the question is whether the patient’s blood pressure had been
controlled before the event, and, if not, why a more aggressive approach
to blood pressure reduction than a thiazide and candesartan had not been
used. Overwhelming evidence exists of the risk reduction from blood
pressure lowering, including in the elderly. Hypertension also increases the
risk of atrial fibrillation, and women with stroke have a higher prevalence of
both risk factors than men with stroke. This is essential information for
primary care providers to use for primary prevention of stroke in elderly
women.
378 APRIL 2020
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
differences is limited because not all studies were specifically designed to detect
sex differences and most were conducted in settings providing specialized stroke
care.85 Barriers to acute stroke treatment in women have been reported, but
studies showing longer door-to-needle times in women are conflicting. The
American Heart Association’s Get With The Guidelines-Stroke database found
delays in women,92,93 but this was not shown in European studies.94,95 Some
studies have also suggested women are less likely to receive diagnostic
FIGURE 7-5
Imaging of the patient in CASE 7-3. Axial noncontrast CT shows a probable ischemic
stroke with hemorrhagic conversion in the right middle cerebral artery territory (A). CT
angiography shows no large vessel occlusions or significant atherosclerosis in precerebral
or intracranial arteries (B). Axial diffusion-weighted (C) and fluid-attenuated inversion
recovery (FLAIR) (D) MRIs on day 3 confirm the diagnosis of ischemic infarct with
hemorrhagic conversion.
CONTINUUMJOURNAL.COM 379
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
STROKE IN WOMEN
investigations and acute treatment compared to men.96,97 The authors speculate
that this may be because of older age and less traditional presentations that are
not immediately recognized by emergency personnel. More strokes occur in
women older than 80 years of age, leading to more women being excluded from
receiving IV thrombolysis based on age criteria than men98 despite documented
benefit in this age group.99 More restricted access to secondary prevention has
also been reported in women, possibly because of an interaction with
socioeconomic variables.100–102
STROKE OUTCOMES
Women have been consistently reported to have worse outcomes after stroke
than men, but, again, this is a result of older age at the time of stroke onset, worse
prestroke functional status, and multiple comorbidities in women. Of these
factors, prestroke function appears to be the main contributor to outcome. Even
after adjustment for these confounding factors, however, women still do
worse.103 Rehabilitation after stroke is the key to better outcomes, specifically to
improving functional independence and reducing the risk of rehospitalization.104
Sex differences regarding access to rehabilitation have not been extensively
studied, but one study of Medicare claims showed that women were more likely
than men to be discharged to a skilled nursing facility rather than inpatient
rehabilitation, although women were also more likely to receive home health
agency visits and physical and occupational therapies than men.105
The physiologic differences that could affect recovery are still not clearly
understood. An Italian study matched men and women by age, stroke severity,
and time from stroke and found that women were more likely to walk with aids
and less likely to climb steps or perform activities of daily living independently
than men. A difference in depression by sex was not seen in the study
participants.106 These results suggest that sex differences could be related to
muscle recovery, physical activity before stroke, or approaches to disability, with
women perhaps feeling less secure, but the data could not prove any of these
possibilities.106
GENERALIZABILITY OF STROKE TRIALS TO WOMEN
Clear differences exist between males and females at the cellular level relating
to cell death pathways and how male and female cells respond to certain
neuroprotective drugs that target these pathways. This could be an important
factor in future drug development for stroke treatment.107
Unfortunately, representation of women in published stroke clinical trials is
lower than the general eligible population. The lack of real-world representation
in trials results in lack of knowledge of benefits and harms, especially in older
women, potentially leading to withholding a beneficial treatment or inflicting
harm. One example is thrombolysis; a population-based study (not a clinical
trial) reported that selecting 80 years as the upper age cutoff for thrombolysis
excluded 19% of all male patients but 44% of all female patients.97 Drugs may also
present different risk-benefit ratios in different demographics. Some evidence
shows that this is also the case in relation to drugs used in stroke: the risk
reduction from anticoagulation in atrial fibrillation (both in non–vitamin K oral
anticoagulants and vitamin K antagonists) is likely to be smaller in women than
in men.108,109 To address the inequities of biomedical research, the National
Institutes of Health (NIH) has issued requirements for inclusion of sex as a
380 APRIL 2020
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
biological variable in study designs and analyses.110 It is hoped that these review KEY POINTS
criteria will increase the reporting of data that are disaggregated by sex and allow
● Women have worse
more generalizability of results to the men and women eligible for new outcomes after stroke than
treatments for stroke in the real world. men, a result of older age at
the time of stroke onset,
worse prestroke functional
status, and multiple
CONCLUSION
comorbidities in women.
Stroke affects women differently than men, primarily because of their unique
reproductive issues and overall longer lifespan. Understanding these issues is ● Women are
important for clinicians, especially to recognize that women may have more underrepresented in many
confusing presenting symptoms and mimics that delay the acute stroke clinical trials of stroke
treatments, limiting the full
evaluation. In addition, outcomes after stroke in women are primarily influenced understanding of both
by older age and prestroke status, but this should lead to more personalized benefits and harm in
treatment, not less treatment. If we adopt a more holistic approach to prevention, women.
rehabilitation, support, and clinical trial representation, we will have a better
understanding of how these complex issues affect care for both men and women.
REFERENCES
1 Arnao V, Acciarresi M, Cittadini E, Caso V. Stroke 8 Albers GW, Marks MP, Kemp S, et al.
incidence, prevalence and mortality in women Thrombectomy for stroke at 6 to 16 hours with
worldwide. Int J Stroke 2016;11(3):287–301. selection by perfusion imaging. N Engl J Med
doi:10.1177/1747493016632245. 2018;378(8):708–718. doi:10.1056/NEJMoa1713973.
2 Benjamin EJ, Muntner P, Alonso A, et al. Heart 9 Nogueira RG, Jadhav AP, Haussen DC, et al.
disease and stroke statistics—2019 update: a Thrombectomy 6 to 24 hours after stroke with a
report from the American Heart Association. mismatch between deficit and infarct. N Engl J
Circulation 2019;139(10):e56–e528. doi:10.1161/ Med 2018;378(1):11–21. doi:10.1056/NEJMoa1706442.
CIR.0000000000000659.
10 Imahori T, Tanaka K, Arai A, et al. Mechanical
3 Madsen TE, Khoury J, Alwell K, et al. Sex-specific thrombectomy for acute ischemic stroke
stroke incidence over time in the Greater patients aged 80 years or older. J Stroke
Cincinnati/Northern Kentucky Stroke Study. Cerebrovasc Dis 2017;26(12):2793–2799.
Neurology 2017;89(10):990–996. doi:10.1212/ doi:10.1016/j.jstrokecerebrovasdis.2017.06.060.
WNL.0000000000004325.
11 Canoy D, Beral V, Balkwill A, et al. Age at
4 Seshadri S, Beiser AS, Kelly-Hayes M, et al. The menarche and risks of coronary heart and other
lifetime risk of stroke. Estimates from the vascular diseases in a large UK cohort. Circulation
Framingham Study. Stroke 2006;37:345–350. 2015;131(3):237–244. doi:10.1161/CIRCULATIONAHA.
doi:10.1161/01.STR.0000199613.38911.b2. 114.010070.
5 Reeves MJ, Bushnell CD, Howard G, et al. Sex 12 Ley SH, Li Y, Tobias DK, et al. Duration of
differences in stroke: epidemiology, clinical reproductive life span, age at menarche, and age
presentation, medical care, and outcomes. at menopause are associated with risk of
Lancet Neurol 2008;7(10):915–926. doi:10.1016/ cardiovascular disease in women. J Am Heart
S1474-4422(08)70193-5. Assoc 2017;6(11):e006713. doi:10.1161/JAHA.117.006713.
6 Phan HT, Blizzard CL, Reeves MJ, et al. Sex 13 Charalampopoulos D, McLoughlin A, Elks CE, Ong
differences in long-term mortality after stroke in KK. Age at menarche and risks of all-cause and
the INSTRUCT (INternational STRoke oUtComes cardiovascular death: a systematic review and
sTudy): a meta-analysis of individual participant meta-analysis. Am J Epidemiol 2014;180(1):29–40.
data. Circ Cardiovasc Qual Outcomes 2017;10(2): doi:10.1093/aje/kwu113.
e003436. doi:10.1161/CIRCOUTCOMES.116.003436.
14 Zhai L, Liu J, Zhao J, et al. Association of obesity
7 Goyal M, Menon BK, van Zwam WH, et al. with onset of puberty and sex hormones in
Endovascular thrombectomy after large-vessel Chinese girls: a 4-year longitudinal study. PLoS
ischaemic stroke: a meta-analysis of individual One 2015;10:e0134656. doi:10.1371/journal.
patient data from five randomised trials. Lancet pone.0134656.
2016;387(10029):1723–1731. doi:10.1016/S0140-
15 Swartz RH, Cayley ML, Foley N, et al. The
6736(16)00163-X.
incidence of pregnancy-related stroke: a
systematic review and meta-analysis. Int J Stroke
2017;12(7):687–697. doi:10.1177/1747493017723271.
CONTINUUMJOURNAL.COM 381
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
STROKE IN WOMEN
16 Kuklina EV, Tong X, Bansil P, et al. Trends in 29 Saposnik G, Barinagarrementeria F, Brown RD Jr,
pregnancy hospitalizations that included a stroke et al. Diagnosis and management of cerebral
in the United States from 1994 to 2007: reasons venous thrombosis: a statement for healthcare
for concern? Stroke 2011;42(9):2564–2570. professionals from the American Heart
doi:10.1161/STROKEAHA.110.610592. Association/American Stroke Association.
Stroke 2011;42:1158–1192. doi:10.1161/STR.
17 Leffert LR, Clancy CR, Bateman BT, et al.
0b013e31820a836.
Hypertensive disorders and pregnancy-related
stroke: frequency, trends, risk factors, and 30 Ferro JM, Bousser MG, Canhão P, et al. European
outcomes. Obstet Gynecol 2015;125(1):124–131. Stroke Organisation guideline for the diagnosis
doi:10.1097/AOG.0000000000000590. and treatment of cerebral venous thrombosis.
Eur J Neurol 2017:24:1203–1213. doi:10.1177/
18 Hovsepian DA, Sriram N, Kamel H, et al. Acute
2396987317719364.
cerebrovascular disease occurring after hospital
discharge for labor and delivery. Stroke 2014; 31 Ferro JM, Coutinho JM, Dentali F, et al. Safety and
45(7):1947–1950. doi:10.1161/STROKEAHA. efficacy of dabigatran etexilate vs dose adjusted
114.005129. warfarin in patients with cerebral venous
thrombosis: a randomized clinical trial. JAMA
19 James AH, Bushnell CD, Jamison MG, Myers ER.
Neurol 2019;76(12):1457–1465. doi:10.1001/
Incidence and risk factors for stroke in
jamaneurol.2019.2764.
pregnancy and the puerperium. Obstet Gynecol
2005;106(3):509–516. doi:10.1097/01.AOG. 32 Aguiar de Sousa D, Canhão P, Crassard I, et al.
0000172428.78411.b0. Safety of pregnancy after cerebral venous
thrombosis: results of the ISCVT (International
20 MacKay AP, Berg CJ, Atrash HK. Pregnancy-
Study on Cerebral Vein and Dural Sinus
related mortality from preeclampsia and
Thrombosis)-2 PREGNANCY Study. Stroke 2017;
eclampsia. Obstet Gynecol 2001;97(4):533–538.
48:3130–3133. doi:10.1161/STROKEAHA.117.018829.
doi:10.1016/S0029-7844(00)01223-0.
33 Chan WS, Ray J, Wai EK, et al. Risk of stroke in
21 Tirada N, Dreizin D, Khati NJ, Akin EA, Zeman RK.
women exposed to low-dose oral contraceptives:
Imaging pregnant and lactating patients.
a critical evaluation of the evidence. Arch Intern
Radiographics 2015;35(6):1751–1765. doi.org/10.
Med 2004;164(7):741–747. doi:10.1001/archinte.
1148/rg.2015150031.
164.7.741.
22 Ladhani NNN, Swartz RH, Foley N, et al. Canadian
34 Gillum L, Mamidipudi SK, Johnston S. Ischemic
stroke best practice consensus statement: acute
stroke risk with oral contraceptives: a meta-
stroke management during pregnancy. Int J
analysis. JAMA 2000;284:72–78. doi:10.1001/
Stroke 2018;13(7):743–758. doi:10.1177/
jama.284.1.72.
1747493018786617.
35 Lidegaard Ø, Løkkegaard E, Jensen A, et al.
23 Swartz RH, Ladhani NNN, Foley N, et al. Canadian
Thrombotic stroke and myocardial infarction
stroke best practice consensus statement:
with hormonal contraception. N Engl J Med 2012;
secondary stroke prevention during pregnancy.
366(24):2257–2266. doi:10.1056/NEJMoa1111840.
Int J Stroke 2018;13(4):406–419. doi:10.1177/
1747493017743801. 36 Roach RE, Helmerhorst FM, Lijfering WM, et al.
Combined oral contraceptives: the risk of
24 Bellamy L, Casas JP, Hingorani A, Williams D.
myocardial infarction and ischemic stroke.
Pre-eclampsia and risk of cardiovascular disease
Cochrane Database Syst Rev 2015;(8):CD011054.
and cancer in later life: systematic review and
doi:10.1002/14651858.CD011054.pub2.
meta-analysis. BMJ 2007;335(7627):974.
doi:10.1136/bmj.39335.38530.BE. 37 Tepper NK, Whiteman MK, Marchbanks PA, et al.
Progestin-only contraception and
25 Wu P, Haththotuwa R, Kwok CS, et al.
thromboembolism: a systematic review.
Preeclampsia and future cardiovascular health: a
Contraception 2016;94(6):678–700. doi:10.1016/j.
systematic review and meta-analysis. Circ
contraception.2016.04.014.
Cardiovasc Qual Outcomes 2017;10(2):e003497.
doi:10.1161/CIRCOUTCOMES.116.003497. 38 Tepper NK, Dragoman MV, Gaffield ME, Curtis
KM. Nonoral combined hormonal contraceptives
26 Siepmann T, Boardman H, Bilderbeck A, et al.
and thromboembolism: a systematic review.
Long-term cerebral white and gray matter
Contraception 2017;95(2):130–139. doi:10.1016/j.
changes after preeclampsia. Neurology 2017;
contraception.2016.10.005.
88(13):1256–1264. doi:10.1212/WNL.
0000000000003765. 39 Caso V, Falorni A, Bushnell CD, et al. Pregnancy,
hormonal treatments for infertility, contraception,
27 Theilen LH, Fraser A, Hollingshaus MS, et al.
and menopause in women after ischemic stroke.
All-cause and cause-specific mortality after
Stroke 2017;48(2):501–506. doi:10.1161/
hypertensive disease of pregnancy. Obstet
STROKEAHA.116.013964.
Gynecol 2016;128(2):238–244. doi:10.1097/
AOG.0000000000001534. 40 te Velde E, Pearson PL. The variability of female
reproductive ageing. Hum Reprod Update 2002;
28 Coutinho JM, Ferro JM, Canhão P, et al. Cerebral
8(2):141–154. doi:10.1093/humupd/8.2.141.
venous and sinus thrombosis in women. Stroke
2009;40:2356–2361. doi:10.1161/STROKEAHA.
108.543884.
382 APRIL 2020
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
41 Mendelsohn ME, Karas R. The protective effects 53 GBD 2016 Lifetime Risk of Stroke Collaborators,
of estrogen on the cardiovascular system. N Engl Feigin VL, Nguyen G, et al. Global, regional, and
J Med 1999;340(23):1801–1811. doi:10.1056/ country-specific lifetime risks of stroke, 1990
NEJM199906103402306. and 2016. N Engl J Med 2018;379(25):2429–2437.
doi:10.1056/NEJMoa1804492.
42 Lisabeth L, Bushnell C. Stroke risk in women: the role
of menopause and hormone therapy. Lancet Neurol 54 Ramos R, Comas-Cufí M, Martí-Lluch R, et al.
2012;11(1):82–91. doi:10.1016/S1474-4422(11)70269-1. Statins for primary prevention of cardiovascular
events and mortality in old and very old adults
43 Muka T, Oliver-Williams C, Kunutsor S, et al.
with and without type 2 diabetes: retrospective
Association of age at onset of menopause and
cohort study. BMJ 2018;362:k3359. doi:10.1136/
time since onset of menopause with cardiovascular
bmj.k3359.
outcomes, intermediate vascular traits, and
all-cause mortality: a systematic review and 55 Backholer K, Peters SAE, Bots SH, et al. Sex
meta-analysis. JAMA Cardiol 2016;1(7):767–776. differences in the relationship between
doi:10.1001/jamacardio.2016.2415. socioeconomic status and cardiovascular
disease: a systematic review and meta-analysis.
44 Reed SD, Lampe JW, Qu C, et al. Self-reported
J Epidemiol Community Health 2017;71(6):
menopausal symptoms in a racially diverse
550–557. doi:10.1136/jech-2016-207890.
population and soy food consumption. Maturitas
2013;75(2):152–158. doi:10.1016/j.maturitas. 56 Andersen KK, Steding-Jessen M, Dalton SO,
2013.03.003. Olsen TS. Socioeconomic position and incidence
of ischemic stroke in Denmark 2003-2012. A
45 Muka T, Oliver-Williams C, Colpani V, et al.
nationwide hospital-based study. J Am Heart
Association of vasomotor and other menopausal
Assoc 2014;3(4):e000762. doi:10.1161/JAHA.
symptoms with risk of cardiovascular disease:
113.000762.
a systematic review and meta-analysis. PLoS One
2016;11(6):e0157417. doi:10.1371/journal.pone.0157417. 57 Andersen KK, Dalton SO, Steding-Jessen M,
Olsen TS. Socioeconomic position and survival
46 Brunner EJ, Shipley MJ, Britton AR, et al.
after stroke in Denmark 2003 to 2012: nationwide
Depressive disorder, coronary heart disease, and
hospital-based study. Stroke 2014;45:3556–3560.
stroke: dose-response and reverse causation
doi:10.1161/STROKEAHA.114.007046.
effects in the Whitehall II cohort study. Eur J Prev
Cardiol 2014;21(3):340–346. doi:10.1177/ 58 Ferrario MM, Veronesi G, Kee F, et al.
2047487314520785. Determinants of social inequalities in stroke
incidence across Europe: a collaborative analysis
47 Hodis HN, Mack WJ, Henderson VW, et al.
of 126635 individuals from 48 cohort studies.
Vascular effects of early versus late
J Epidemiol Community Health 2017;71(12):
postmenopausal treatment with estradiol.
1210–1216. doi:10.1136/jech-2017-209728.
N Engl J Med 2016;374(13):1221–1231. doi:10.1056/
NEJMoa1505241. 59 Xu X, Mishra GD, Dobson AJ, Jones M.
Progression of diabetes, heart disease, and
48 Harman SM, Black DM, Naftolin F, et al. Arterial
stroke multimorbidity in middle-aged women: a
imaging outcomes and cardiovascular risk
20-year cohort study. PLoS Med 2018;15(3):
factors in recently menopausal women: a
e1002516. doi:10.1371/journal.pmed.1002516.
randomized trial. Ann Intern Med 2014;161(4):
249–260. doi:10.7326/M14-0353. 60 Forsberg PO, Ohlsson H, Sundquist K. Causal
nature of neighborhood deprivation on individual
49 Canonico M, Carcaillon L, Plu-Bureau G, et al.
risk of coronary heart disease or ischemic stroke:
Postmenopausal hormone therapy and risk
a prospective national Swedish co-relative
of stroke: impact of the route of estrogen
control study in men and women. Health Place
administration and type of progestogen. Stroke
2018;50:1–5. doi:10.1016/j.healthplace.2017.12.006.
2016;47(7):1734–1741. doi:10.1161/STROKEAHA.
116.013052. 61 Kubota Y, Evenson KR, Maclehose RF, et al.
Physical activity and lifetime risk of
50 Renoux C, Dell’Aniello S, Garbe E, Suissa S.
cardiovascular disease and cancer. Med Sci
Transdermal and oral hormone replacement
Sports Exerc 2017;49(8):1599–1605. doi:10.1249/
therapy and the risk of stroke: a nested
MSS.0000000000001274.
case-control study. BMJ 2010;340:c2519.
doi:10.1136/bmj.c2519. 62 Lear SA, Hu W, Rangarajan S, et al. The effect of
physical activity on mortality and cardiovascular
51 Manson JE. Current recommendations: what is
disease in 130 000 people from 17 high-income,
the clinician to do? Fertil Steril 2014;101(4):916–921.
middle-income, and low-income countries: the
doi:10.1016/j.fertnstert.2014.02.043.
PURE study. Lancet 2017;390(10113):2643–2654.
52 Poorthuis MH, Algra AM, Algra A, et al. Female- doi:10.1016/S0140-6736(17)31634-3.
and male-specific risk factors for stroke: a
63 Guthold R, Stevens GA, Riley LM, Bull FC.
systematic review and meta-analysis. JAMA
Worldwide trends in insufficient physical activity
Neurol 2017;74(1):75–81. doi:10.1001/jamaneurol.
from 2001 to 2016: a pooled analysis of 358
2016.3482.
population-based surveys with 1·9 million
participants. Lancet Glob Health 2018;6(10):
e1077–e1086. doi:10.1016/S2214-109X(18)30357-7.
CONTINUUMJOURNAL.COM 383
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
STROKE IN WOMEN
64 Rist PM, Capistrant BD, Mayeda ER, et al. Physical 76 Peters SA, Huxley RR, Woodward M. Comparison
activity, but not body mass index, predicts less of the sex-specific associations between
disability before and after stroke. Neurology systolic blood pressure and the risk of
2017;88(18):1718–1726. doi:10.1212/WNL. cardiovascular disease: a systematic review and
0000000000003888. meta-analysis of 124 cohort studies, including
1.2 million individuals. Stroke 2013;44(9):2394–2401.
65 Meschia JF, Bushnell C, Boden-Albala B, et al.
doi:10.1161/STROKEAHA.113.001624.
Guidelines for the primary prevention of stroke: a
statement for healthcare professionals from the 77 Redfern A, Peters SAE, Luo R, et al. Sex
American Heart Association/American Stroke differences in the awareness, treatment, and
Association. Stroke 2014;45(12):3754–3832. control of hypertension in China: a systematic
doi:10.1161/STR.0000000000000046. review with meta-analyses. Hypertens Res Off
J Jpn Soc Hypertens 2019;42(2):273–283.
66 Berra K, Rippe J, Manson JE. Making physical
doi:10.1038/s41440-018-0154-x.
activity counseling a priority in clinical practice:
the time for action is now. JAMA 2015;314(24): 78 Keyhani S, Scobie J, Hebert P, McLaughlin M.
2617–2618. doi:10.1001/jama.2015.16244. Gender disparities in blood pressure control
and cardiovascular care in a national sample of
67 Oberlin LE, Waiwood AM, Cumming TB, et al.
ambulatory care visits. Hypertension 2008;51(4):
Effects of physical activity on poststroke
1149–1155. doi:10.1161/HYPERTENSIONAHA.
cognitive function: a meta-analysis of
107.107342.
randomized controlled trials. Stroke 2017;48(11):
3093–3100. doi:10.1161/STROKEAHA.117.017319. 79 Oparil S, Davis BR, Cushman WC, et al. Mortality
and morbidity during and after antihypertensive
68 Zahodne LB, Gilsanz P, Glymour MM, et al.
and lipid-lowering treatment to prevent heart
Comparing variability, severity, and persistence
attack trial: results by sex. Hypertension 2013;
of depressive symptoms as predictors of future
61(5):977–986. doi:10.1161/HYPERTENSIONAHA.
stroke risk. Am J Geriatr Psychiatry 2017;25(2):
111.00213.
120–128. doi:10.1016/j.jagp.2016.10.009.
80 Dzeshka MS, Shahid F, Shantsila A, Lip GYH.
69 Hamano T, Li X, Lönn SL, et al. Depression, stroke
Hypertension and atrial fibrillation: an intimate
and gender: evidence of a stronger association in
association of epidemiology, pathophysiology,
men. J Neurol Neurosurg Psychiatry 2015;86(3):
and outcomes. Am J Hypertens 2017;30(8):
319–323. doi:10.1136/jnnp-2014-307616.
733–755. doi:10.1093/ajh/hpx013.
70 Booth J, Connelly L, Lawrence M, et al. Evidence
81 Emdin CA, Wong CX, Hsiao AJ, et al. Atrial
of perceived psychosocial stress as a risk factor
fibrillation as risk factor for cardiovascular
for stroke in adults: a meta-analysis. BMC Neurol
disease and death in women compared with men:
2015;15:233. doi:10.1186/s12883-015-0456-4.
systematic review and meta-analysis of cohort
71 Hakulinen C, Pulkki-Råback L, Virtanen M, et al. studies. BMJ 2016;532:h7013. doi:10.1136/bmj.h7013.
Social isolation and loneliness as risk factors
82 Nezu T, Hosomi N, Kondo K, et al. Greater severity
for myocardial infarction, stroke and mortality:
of neurological defects in women admitted with
UK Biobank cohort study of 479 054 men and
atrial fibrillation-related stroke. Circ J 2016;80(1):
women. Heart 2018;104(18):1536–1542. doi:10.1136/
250–255. doi:10.1253/circj.CJ-15-0873.
heartjnl-2017-312663.
83 Ruff CT, Giugliano RP, Braunwald E, et al.
72 Aron AW, Staff I, Fortunato G, McCullough LD.
Comparison of the efficacy and safety of new
Prestroke living situation and depression
oral anticoagulants with warfarin in patients with
contribute to initial stroke severity and stroke
atrial fibrillation: a meta-analysis of randomised
recovery. J Stroke Cerebrovasc Dis 2015;24(2):
trials. Lancet 2014;383(9921):955–962. doi:10.1016/
492–499. doi:10.1016/j.jstrokecerebrovasdis.
S0140-6736(13)62343-0.
2014.09.024.
84 Thompson LE, Maddox TM, Lei L, et al. Sex
73 Huang Y, Xu S, Hua J, et al. Association between
differences in the use of oral anticoagulants for
job strain and risk of incident stroke: a meta-
atrial fibrillation: a report from the National
analysis. Neurology 2015;85(19):1648–1654.
Cardiovascular Data Registry (NCDR®) PINNACLE
doi:10.1212/WNL.0000000000002098.
Registry. J Am Heart Assoc 2017;6(7):e005801.
74 Toivanen S. Social determinants of stroke as doi:10.1161/JAHA.117.005801.
related to stress at work among working women:
85 Bushnell C, Howard VJ, Lisabeth L, et al. Sex
a literature review. Stroke Res Treat 2012;2012:
differences in the evaluation and treatment of
873678. doi:10.1155/2012/873678.
acute ischaemic stroke. Lancet Neurol 2018;17(7):
75 Ullberg T, Zia E, Petersson J, Norrving B. Changes 641–650. doi:10.1016/S1474-4422(18)30201-1.
in functional outcome over the first year after
86 Lisabeth LD, Brown DL, Hughes R, et al. Acute
stroke: an observational study from the Swedish
stroke symptoms: comparing women and men.
stroke register. Stroke 2015;46(2):389–394.
Stroke 2009;40(6):2031–2036. doi:10.1161/
doi:10.1161/STROKEAHA.114.006538.
STROKEAHA.109.546812.
384 APRIL 2020
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
87 Stuart-Shor EM, Wellenius GA, DelloIacono DM, 99 Mishra NK, Ahmed N, Andersen G, et al.
Mittleman MA. Gender differences in presenting Thrombolysis in very elderly people: controlled
and prodromal stroke symptoms. Stroke 2009; comparison of SITS International Stroke
40(4):1121–1126. doi:10.1161/STROKEAHA.108.543371. Thrombolysis Registry and Virtual International
Stroke Trials Archive. BMJ 2010;341:c6046. doi:
88 Gall SL, Donnan G, Dewey HM, et al. Sex
10.1136/bmj.c6046.
differences in presentation, severity, and
management of stroke in a population-based 100 Tanislav C, Milde S, Schwartzkopff S, et al.
study. Neurology 2010;74(12):975–981. doi:10.1212/ Secondary stroke prevention in atrial fibrillation:
WNL.0b013e3181d5a48f. a challenge in the clinical practice. BMC Neurol
2014;14:195. doi:10.1186/s12883-014-0195-y.
89 Jerath NU, Reddy C, Freeman WD, et al. Gender
differences in presenting signs and symptoms 101 Nilsson G, Samuelsson E, Söderström L, Mooe T.
of acute ischemic stroke: a population-based Low use of statins for secondary prevention in
study. Gend Med 2011;8(5):312–319. doi:10.1016/j. primary care: a survey in a northern Swedish
genm.2011.08.001. population. BMC Fam Pract 2016;17(1):110.
doi:10.1186/s12875-016-0505-0.
90 Jones AT, O’Connell NK, David AS. Epidemiology
of functional stroke mimic patients: a systematic 102 Sjölander M, Eriksson M, Asplund K, et al.
review and meta-analysis. Eur J Neurol 2020;27: Socioeconomic inequalities in the prescription
18–26. doi:10.1111/ene.14069. of oral anticoagulants in stroke patients with
atrial fibrillation. Stroke 2015;46(8):2220–2225.
91 Merino JG, Luby M, Benson RT, et al. Predictors
doi:10.1161/STROKEAHA.115.009718.
of acute stroke mimics in 8187 patients referred
to a stroke service. J Stroke Cerebrovasc 103 Lisabeth LD, Reeves MJ, Baek J, et al. Factors
Dis 2013;22:e397–e403. doi:10.1016/j. influencing sex differences in poststroke
jstrokecerebrovasdis.2013.04.018. functional outcome. Stroke 2015;46:860–863.
doi:10.1161/STROKEAHA.114.007985.
92 Asdaghi N, Romano JG, Wang K, et al. Sex
disparities in ischemic stroke care: FL-PR CReSD 104 Freburger JK, Li D, Fraher EP. Community use of
study (Florida-Puerto Rico Collaboration to physical and occupational therapy after stroke
Reduce Stroke Disparities). Stroke 2016;47(10): and risk of hospital readmission. Arch Phys Med
2618–2626. doi:10.1161/STROKEAHA.116.013059. Rehabil 2018;99(1):26–34.e5. doi:10.1016/j.apmr.
2017.07.011.
93 Kamal N, Sheng S, Xian Y, et al. Delays in
door-to-needle times and their impact on 105 Roth DL, Sheehan OC, Huang J, et al. Medicare
treatment time and outcomes in get with the claims indicators of healthcare utilization
guidelines-stroke. Stroke 2017;48(4):946–954. differences after hospitalization for ischemic
doi:10.1161/STROKEAHA.116.015712. stroke: race, gender, and caregiving effects.
Int J Stroke 2016;11(8):928–934. doi:10.1177/
94 Gattringer T, Ferrari J, Knoflach M, et al.
1747493016660095.
Sex-related differences of acute stroke unit
care: results from the Austrian stroke unit 106 Paolucci S, Bragoni M, Coiro P, et al. Is sex a
registry. Stroke 2014;45(6):1632–1638. doi:10.1161/ prognostic factor in stroke rehabilitation? A
STROKEAHA.114.004897. matched comparison. Stroke 2006;37(12):
2989–2994. doi:10.1161/01.STR.0000248456.
95 Lorenzano S, Ahmed N, Falcou A, et al. Does
41647.3d.
sex influence the response to intravenous
thrombolysis in ischemic stroke?: answers from 107 Chauhan A, Moser H, McCullough LD. Sex
safe implementation of treatments in differences in ischaemic stroke: potential
stroke—International Stroke Thrombolysis cellular mechanisms. Clin Sci (Lond) 2017;131(7):
Register. Stroke 2013;44(12):3401–3406. 533–552. doi:10.1042/CS20160841.
doi:10.1161/STROKEAHA.113.002908.
108 Hart RG, Eikelboom JW, Pearce LA. Sex, stroke,
96 Foerch C, Misselwitz B, Humpich M, et al. Sex and atrial fibrillation. Arch Neurol 2012;69(12):
disparity in the access of elderly patients to 1641–1643. doi:10.1001/archneurol.2012.2691.
acute stroke care. Stroke 2007;38(7):2123–2126.
109 Raccah BH, Perlman A, Zwas DR, et al. Gender
doi:10.1161/STROKEAHA.106.478495.
differences in efficacy and safety of direct oral
97 Foerch C, Czapowski D, Misselwitz B, et al. anticoagulants in atrial fibrillation: systematic
Gender imbalances induced by age limits in review and network meta-analysis.
stroke trials. Neuroepidemiology 2010;35(3): Ann Pharmacother 2018;52(11):1135–1142.
226–230. doi:10.1159/000319457. doi:10.1177/1060028018771264.
98 Fredwall M, Sternberg S, Blackhurst D, et al. 110 Clayton JA. Applying the new SABV (sex as a
Gender differences in exclusion criteria for biological variable) policy to research and clinical
recombinant tissue-type plasminogen activator. care. Physiol Behav 2018;187:2–5. doi:10.1016/j.
J Stroke Cerebrovasc Dis 2016;25(11):2569–2574. physbeh.2017.08.012.
doi:10.1016/j.jstrokecerebrovasdis.2016.06.012.
CONTINUUMJOURNAL.COM 385
Copyright © American Academy of Neurology. Unauthorized reproduction of this article is prohibited.
You might also like
- Headache Syndromes, Oxford, 2020Document561 pagesHeadache Syndromes, Oxford, 2020luizmiranda108No ratings yet
- Pathophysiology of Migraine.5Document11 pagesPathophysiology of Migraine.5Bryan100% (1)
- Endovascular Treatment of Acute Ischemic Stroke.7-1 PDFDocument22 pagesEndovascular Treatment of Acute Ischemic Stroke.7-1 PDFCristina GhizdavetNo ratings yet
- Endovascular Treatment of Acute Ischemic Stroke.7 PDFDocument22 pagesEndovascular Treatment of Acute Ischemic Stroke.7 PDFchristinaNo ratings yet
- HSA ContinuunDocument35 pagesHSA ContinuunJose DavidNo ratings yet
- Chronic Traumatic Encephalopathy.12Document21 pagesChronic Traumatic Encephalopathy.12wmtxbbNo ratings yet
- Cluster Headache and Other Trigeminal Autonomic CephalalgiasDocument19 pagesCluster Headache and Other Trigeminal Autonomic CephalalgiasBryan100% (1)
- 7-Vertigo Related To Central Nervous System.-CompressedDocument21 pages7-Vertigo Related To Central Nervous System.-CompressedOlga Manco GuzmánNo ratings yet
- Cerebrovasc - ContinuumDocument239 pagesCerebrovasc - ContinuumRafael100% (1)
- Ataxia 10Document19 pagesAtaxia 10Cristina GhizdavetNo ratings yet
- Subarachnoid Hemorrhage: Continuumaudio Interview Available OnlineDocument35 pagesSubarachnoid Hemorrhage: Continuumaudio Interview Available OnlineJose DavidNo ratings yet
- Clinically Isolated Syndrome and Early Relapsing.8Document19 pagesClinically Isolated Syndrome and Early Relapsing.8juanmontoyaseNo ratings yet
- Neuromyelitis Optica Spectrum Disorder and Other.15Document30 pagesNeuromyelitis Optica Spectrum Disorder and Other.15Doaa Mokhtar100% (1)
- TraducirChiasmal and Postchiasmal - DiseaseDocument19 pagesTraducirChiasmal and Postchiasmal - DiseasejacquelineNo ratings yet
- Management of Stroke in The NCCUDocument25 pagesManagement of Stroke in The NCCUsaudNo ratings yet
- Charcot-Marie-Tooth Disease and Other Hereditary NeuropathiesDocument33 pagesCharcot-Marie-Tooth Disease and Other Hereditary NeuropathiesTallulah Spina TensiniNo ratings yet
- 2019-Epilepsy EmergenciesDocument23 pages2019-Epilepsy EmergenciesBryanNo ratings yet
- The Evolving Concept of Cryptogenic Stroke.9Document10 pagesThe Evolving Concept of Cryptogenic Stroke.9Toma BichirNo ratings yet
- Periferico - ContinuumDocument239 pagesPeriferico - ContinuumRafaelNo ratings yet
- Brain Death Death by Neurologic Criteria.15Document21 pagesBrain Death Death by Neurologic Criteria.15Anusha PervaizNo ratings yet
- Behavioral Variant Frontotemporal Dementia.7Document25 pagesBehavioral Variant Frontotemporal Dementia.7Nícolas CavalcanteNo ratings yet
- Neoplastic Myelopathies: Continuumaudio Interviewavailable OnlineDocument22 pagesNeoplastic Myelopathies: Continuumaudio Interviewavailable OnlineDalwadi1No ratings yet
- Diabetes and Metabolic Disorders and The.5 PDFDocument23 pagesDiabetes and Metabolic Disorders and The.5 PDFTallulah Spina TensiniNo ratings yet
- Neurologic Manifestations of Severe Acute.14Document15 pagesNeurologic Manifestations of Severe Acute.14Henry DanielNo ratings yet
- Brain Death Death by Neurologic Criteria.15Document21 pagesBrain Death Death by Neurologic Criteria.15Angy PalaciosNo ratings yet
- Cefaleia - ContinuumDocument195 pagesCefaleia - ContinuumRafaelNo ratings yet
- Otorrino ContinuumDocument220 pagesOtorrino ContinuumRafaelNo ratings yet
- Neurologic Complications of Lyme Disease: Review ArticleDocument11 pagesNeurologic Complications of Lyme Disease: Review ArticleHenry DanielNo ratings yet
- 1 AURa MIGRDocument9 pages1 AURa MIGRjerejerejereNo ratings yet
- Management of Cerebral Edema, Brain Compression,.4Document29 pagesManagement of Cerebral Edema, Brain Compression,.4Jorge MontenegroNo ratings yet
- Predatory Journals and Conferences: Why Fake Counts: ReviewDocument6 pagesPredatory Journals and Conferences: Why Fake Counts: ReviewFIA SlotNo ratings yet
- Predatory Journals and Conferences: Why Fake Counts: ReviewDocument6 pagesPredatory Journals and Conferences: Why Fake Counts: ReviewenriquegarciagalianaNo ratings yet
- Rapidly Progressive Dementia.16Document36 pagesRapidly Progressive Dementia.16tottocupNo ratings yet
- Preventive Migraine Treatment.7Document20 pagesPreventive Migraine Treatment.7Javıera MoyaNo ratings yet
- StrokeDocument23 pagesStrokepaola nabhanNo ratings yet
- Update On Antiseizure Medications 2022.13Document36 pagesUpdate On Antiseizure Medications 2022.13Ana Castro MondacaNo ratings yet
- 2020 Neuroimaging - in - Acute - Stroke.6Document23 pages2020 Neuroimaging - in - Acute - Stroke.6BryanNo ratings yet
- Chorea 9Document35 pagesChorea 9Cristina GhizdavetNo ratings yet
- Stroke TreatmentDocument19 pagesStroke Treatmentpaola nabhanNo ratings yet
- Disorders of The Cauda Equina: Continuum Audio Interviewavailable OnlineDocument20 pagesDisorders of The Cauda Equina: Continuum Audio Interviewavailable OnlineDalwadi1No ratings yet
- Autonomic Peripheral Neuropathy.7Document14 pagesAutonomic Peripheral Neuropathy.7thomashenrryNo ratings yet
- Palliative Care and Shared Decision Making in The.14Document14 pagesPalliative Care and Shared Decision Making in The.14AmitShettyNo ratings yet
- Psiquiatria - ContinuDocument288 pagesPsiquiatria - ContinuRafaelNo ratings yet
- Scientific American - World View 2016 (Gnv64)Document88 pagesScientific American - World View 2016 (Gnv64)Musa Rahim KhanNo ratings yet
- Low Back Pain.11-1Document20 pagesLow Back Pain.11-1Cristina GhizdavetNo ratings yet
- Continnumm Cerebrovascular Disease.2020Document316 pagesContinnumm Cerebrovascular Disease.2020CAMILA ALMENDRA VILCHES100% (2)
- Status Epilepticus, Refractory Status Epilepticus, and Super-Refractory Status EpilepticusDocument25 pagesStatus Epilepticus, Refractory Status Epilepticus, and Super-Refractory Status EpilepticusAlvaro EstupiñanNo ratings yet
- Rubber Band LigationDocument5 pagesRubber Band LigationZaeem KhalidNo ratings yet
- Charcot-Marie-Tooth Disease and Other Genetic PolyneuropathiesDocument18 pagesCharcot-Marie-Tooth Disease and Other Genetic PolyneuropathiesCristina GhizdavetNo ratings yet
- ArchitecturalDocument11 pagesArchitecturalvirnmontalesNo ratings yet
- 2020 The Place of Extracorporeal Life Support In.98996Document8 pages2020 The Place of Extracorporeal Life Support In.98996Miky DinuNo ratings yet
- Moderate and Severe Traumatic Brain Injury.7Document23 pagesModerate and Severe Traumatic Brain Injury.7gabrielpineiro14No ratings yet
- Dap - Volume 10 Issue 3 - A Resilient EconomyDocument37 pagesDap - Volume 10 Issue 3 - A Resilient Economyamirshehzad.ue.faisalabadNo ratings yet
- MODULE 9 (CARDIO 1 - THE HEART) .DrawioDocument1 pageMODULE 9 (CARDIO 1 - THE HEART) .DrawiohananpangonotanNo ratings yet
- A545 160 16 43 DI 0003 - Rev 0Document11 pagesA545 160 16 43 DI 0003 - Rev 0manishaNo ratings yet
- Acute Migraine Treatment.6Document16 pagesAcute Migraine Treatment.6BryanNo ratings yet
- Autonomic Peripheral Neuropathy: Review ArticleDocument14 pagesAutonomic Peripheral Neuropathy: Review ArticleAlaa MishrifNo ratings yet
- Rosemount 3308 Wireless Level Radar and Liquid Level Transmitter Process Connection TypesDocument3 pagesRosemount 3308 Wireless Level Radar and Liquid Level Transmitter Process Connection TypesUsman AliNo ratings yet
- Terrenos Del Estado: Municipalidad Distrital de Padre MarquezDocument1 pageTerrenos Del Estado: Municipalidad Distrital de Padre MarquezSting RiosNo ratings yet
- Medical Management of StrokeDocument6 pagesMedical Management of StrokemehakNo ratings yet
- Evaluation of Headache in Adults - UpToDateDocument18 pagesEvaluation of Headache in Adults - UpToDateSebastianNo ratings yet
- Cerebral Venous Thrombosis PDFDocument7 pagesCerebral Venous Thrombosis PDFd dNo ratings yet
- Cerebral Venous Thrombosis in Sub-Saharan Africa: A Systematic ReviewDocument7 pagesCerebral Venous Thrombosis in Sub-Saharan Africa: A Systematic ReviewDenise MacieNo ratings yet
- Cerebral Venous Thrombosis-Treatment & PrognosisDocument37 pagesCerebral Venous Thrombosis-Treatment & PrognosisMUHAMMAD09No ratings yet
- Jurnal RadiologiDocument8 pagesJurnal RadiologiNia Nurhayati ZakiahNo ratings yet
- Recognizing Vaccine-Induced Immune Thrombotic ThrombocytopeniaDocument7 pagesRecognizing Vaccine-Induced Immune Thrombotic Thrombocytopenialagopatis4No ratings yet
- Postpartum Headache: Diagnostic Considerations: Sue Yin Lim, Nikos Evangelou, Sibylle JürgensDocument8 pagesPostpartum Headache: Diagnostic Considerations: Sue Yin Lim, Nikos Evangelou, Sibylle JürgensJamie LittleNo ratings yet
- Pembimbing: Dr. Partodji, SP - Rad Oleh: 1. Ira Rahmawati 2. Pradnya Ayu 3. LimastaniDocument32 pagesPembimbing: Dr. Partodji, SP - Rad Oleh: 1. Ira Rahmawati 2. Pradnya Ayu 3. Limastaniira rahmaNo ratings yet
- Anatomic Variants and Artefacts in Non Enhanced MRDocument8 pagesAnatomic Variants and Artefacts in Non Enhanced MRlouloupavelNo ratings yet
- Headache ReviewDocument8 pagesHeadache Reviewoscar nieblesNo ratings yet
- Acute Multifocal Placoid Pigment EpitheliopathyDocument8 pagesAcute Multifocal Placoid Pigment EpitheliopathyremotmNo ratings yet
- Duration of Anticoagulation After Cerebral Venous Sinus Thrombosis 2012 Neurocritical CareDocument8 pagesDuration of Anticoagulation After Cerebral Venous Sinus Thrombosis 2012 Neurocritical Caremorris_tyoNo ratings yet
- Thesis MedicineDocument110 pagesThesis MedicineVenkatesh Korapaka100% (3)
- Literature Review On DVTDocument4 pagesLiterature Review On DVTaflsdefaq100% (1)
- A Clinical Approach To Hemiplegia: Dr. A.P.Ndondo Paediatric Neurology Department Red Cross Children's HospitalDocument62 pagesA Clinical Approach To Hemiplegia: Dr. A.P.Ndondo Paediatric Neurology Department Red Cross Children's HospitalGabrielle ElequiareNo ratings yet
- Intracerebral Hemorrhage - 2021Document32 pagesIntracerebral Hemorrhage - 2021Katherine Poma RamosNo ratings yet
- Cerebral Sinus ThrombosisDocument23 pagesCerebral Sinus ThrombosisHerinanda Fahmy FahlevieNo ratings yet
- A Pictorial Review of Postpartum ComplicationsDocument25 pagesA Pictorial Review of Postpartum ComplicationsGabriela Serra del CarpioNo ratings yet
- Conclusion: Long-Term Follow-Up ForDocument31 pagesConclusion: Long-Term Follow-Up ForHima HuNo ratings yet
- Klasifikasi Penyebab KomaDocument19 pagesKlasifikasi Penyebab KomaNoni JacksonNo ratings yet
- CEFALEA Evaluation of Headache in Adults - UpToDateDocument23 pagesCEFALEA Evaluation of Headache in Adults - UpToDateJOSE ANTONIO ALBARRAN MENDOZANo ratings yet
- Persuasive EssayDocument7 pagesPersuasive EssayJessica HopperNo ratings yet
- Stroke Associated With COVID-19 VaccinesDocument23 pagesStroke Associated With COVID-19 VaccinesTUTO TUTONo ratings yet
- ACR Criteria PDFDocument18 pagesACR Criteria PDFquickdannyNo ratings yet
- Headache Diagnosis and Treatment of 2609Document77 pagesHeadache Diagnosis and Treatment of 2609Reza Badruun Syahrul HakimNo ratings yet
- Cerebral Venous Sinus ThrombosisDocument34 pagesCerebral Venous Sinus ThrombosisNeurologia homicNo ratings yet
- Cerebral Venous and Dural Sinus ThrombosisDocument11 pagesCerebral Venous and Dural Sinus Thrombosislakshminivas PingaliNo ratings yet
- 2017 06 16 Stroke in PregnancyDocument49 pages2017 06 16 Stroke in PregnancyayubahriNo ratings yet