Professional Documents
Culture Documents
0 ratings0% found this document useful (0 votes)
5 viewsH. Pylori H. Pylori
H. Pylori H. Pylori
Uploaded by
Perplexed CeleryIn obese individuals, adipokines released from fat depots decrease insulin sensitivity in peripheral tissues, causing hyperglycemia and hyperinsulinemia. This triggers lipid uptake and lipogenesis in the liver, leading to non-alcoholic fatty liver disease (NAFLD) and non-alcoholic steatohepatitis (NASH), characterized by oxidative stress and hepatocellular damage. Chronic damage can progress to cirrhosis and hepatocellular carcinoma. NASH is diagnosed after ruling out other causes in patients without heavy alcohol use.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You might also like
- Test Certificate of BitumenDocument1 pageTest Certificate of BitumenAmit Prasad50% (2)
- Logbook KoDocument13 pagesLogbook KoMarkmar AnchetaNo ratings yet
- Parts of A Bar.Document3 pagesParts of A Bar.MARY JOY VILLARUEL100% (1)
- Khawater Makki Cover Letter.ADocument1 pageKhawater Makki Cover Letter.AAnonymous miK3qJxNo ratings yet
- Uworld Summary NotesDocument6 pagesUworld Summary Notesnavneet mannNo ratings yet
- Gi Study GuideDocument31 pagesGi Study Guidebsmodi98No ratings yet
- Dr. Ali's Uworld Notes For Step 2 CK: GastroDocument32 pagesDr. Ali's Uworld Notes For Step 2 CK: GastrouyesNo ratings yet
- Day 7 Gal Bladder StonesDocument12 pagesDay 7 Gal Bladder StonesShreyash HaritwalNo ratings yet
- Pancreatitis: Pancreatitis Is Inflammation of The Pancreas. It Occurs When Pancreatic Enzymes (Especially Trypsin)Document6 pagesPancreatitis: Pancreatitis Is Inflammation of The Pancreas. It Occurs When Pancreatic Enzymes (Especially Trypsin)tianallyNo ratings yet
- Set 3 COMP-2Document71 pagesSet 3 COMP-2Appu ayyalaNo ratings yet
- Cirrosis HepaticaDocument10 pagesCirrosis Hepaticaadriel710No ratings yet
- Cirrosis Adnd Its ComplicationDocument50 pagesCirrosis Adnd Its Complicationnathan asfahaNo ratings yet
- Assessment of Jaundice in The Hospitalized Patient PDFDocument16 pagesAssessment of Jaundice in The Hospitalized Patient PDFlaura canoNo ratings yet
- Gall Bladder Diseases by - DR Arun Aggarwal GastroenterologistDocument53 pagesGall Bladder Diseases by - DR Arun Aggarwal GastroenterologistDr. Arun Aggarwal GastroenterologistNo ratings yet
- UlcerativecolitisDocument27 pagesUlcerativecolitisMohamed Abdulrazaq100% (1)
- Doc.6th TopicDocument100 pagesDoc.6th TopicBibinNo ratings yet
- Msn-Small Bowel Disorder - SeminarDocument71 pagesMsn-Small Bowel Disorder - SeminarSarithaRajeshNo ratings yet
- DyspepDocument2 pagesDyspepGeorge WinchesterNo ratings yet
- Case 5 - Pancreatitis-1Document4 pagesCase 5 - Pancreatitis-1ngNo ratings yet
- Disorders of Motility2Document46 pagesDisorders of Motility2valdomiroNo ratings yet
- Biliary System and Pancreatic DisorderDocument59 pagesBiliary System and Pancreatic DisorderAlda AdeliaNo ratings yet
- Chronic Liver FailureDocument4 pagesChronic Liver FailureJasmine Faith SilvaNo ratings yet
- Gallbladder IIDocument22 pagesGallbladder IIAli SafaaNo ratings yet
- Hepatic Cirrhosis and Hepatitis: Dr. Lubna DwerijDocument69 pagesHepatic Cirrhosis and Hepatitis: Dr. Lubna DwerijNoor MajaliNo ratings yet
- Nu'man AS DaudDocument23 pagesNu'man AS DaudHidayat BazeherNo ratings yet
- Digestive System Disorder AssessmentDocument50 pagesDigestive System Disorder AssessmentTaate MohammedNo ratings yet
- Liver CirrhosisDocument38 pagesLiver Cirrhosisfeeo8266No ratings yet
- Pancreatitis Ercp Pain Amylase Lipase ErcpDocument24 pagesPancreatitis Ercp Pain Amylase Lipase ErcpPerplexed CeleryNo ratings yet
- Cholelithiasis and Cholecystitis: de Villa Dennis Fernando M. Level IVDocument38 pagesCholelithiasis and Cholecystitis: de Villa Dennis Fernando M. Level IVsimongarciadevillaNo ratings yet
- Gastro-Oesophageal Reflux Disease: EpidemiologyDocument6 pagesGastro-Oesophageal Reflux Disease: EpidemiologyRehan RiyazNo ratings yet
- Gastrointestinal System: Paul Tang, MD, DPAMSDocument30 pagesGastrointestinal System: Paul Tang, MD, DPAMSThakoon Tts100% (1)
- Cholecystitis FinalDocument57 pagesCholecystitis FinalRajendra DesaiNo ratings yet
- Peptic Ulcer Disease: Palangka Raya University Faculty of MedicineDocument70 pagesPeptic Ulcer Disease: Palangka Raya University Faculty of MedicineMITHA100% (1)
- Inflammatoray Bowel DiseaseDocument14 pagesInflammatoray Bowel DiseaseSadr AkrmNo ratings yet
- Abdominal Swelling and Ascites: Global ConsiderationsDocument5 pagesAbdominal Swelling and Ascites: Global ConsiderationsJacob BorongNo ratings yet
- Medical Progress: N F L DDocument11 pagesMedical Progress: N F L DndocNo ratings yet
- Pancreatic Diabetes Mellitus: Frequency and DiagnosisDocument10 pagesPancreatic Diabetes Mellitus: Frequency and DiagnosisRutDanNo ratings yet
- Dr. S.P. Hewawasam (MD) Consultant Gastroenterologist/Senior Lecturer in PhysiologyDocument33 pagesDr. S.P. Hewawasam (MD) Consultant Gastroenterologist/Senior Lecturer in PhysiologyAjung SatriadiNo ratings yet
- 2009 Pearl SheetDocument19 pages2009 Pearl Sheetmikez100% (1)
- Small and Large IntestinesDocument44 pagesSmall and Large IntestinespempuladesmondsimfukwelNo ratings yet
- Ald & MasldDocument19 pagesAld & MasldAli SafaaNo ratings yet
- Pancreatitis: 1 Signs and SymptomsDocument6 pagesPancreatitis: 1 Signs and SymptomsZiedTrikiNo ratings yet
- Esophageal StrictureDocument6 pagesEsophageal StrictureŽäíñäb ÄljaÑabìNo ratings yet
- Bile, Bile Duct and Pancreatic DiseaseDocument82 pagesBile, Bile Duct and Pancreatic Diseaseshahrul rahmanNo ratings yet
- Dissertation ON A Clinical Study On Obstructive JaundiceDocument66 pagesDissertation ON A Clinical Study On Obstructive JaundicePravat SatpathyNo ratings yet
- Intestinal Obstruction in Pediatric SurgeryDocument69 pagesIntestinal Obstruction in Pediatric Surgeryabhinay_1712No ratings yet
- Acute & Chronic Pancreatitis - DoneDocument7 pagesAcute & Chronic Pancreatitis - DoneAriana ValenciaNo ratings yet
- Wa0093.Document27 pagesWa0093.EvaNo ratings yet
- CSS Ulcerative ColitisDocument28 pagesCSS Ulcerative ColitisAthiyyah HasnaNo ratings yet
- Revisao ColecistiteDocument16 pagesRevisao ColecistiteAndrés Menacho AbularachNo ratings yet
- Hepatobiliary Tract and Pancreatic Pathology Assignment - PAYSONDocument22 pagesHepatobiliary Tract and Pancreatic Pathology Assignment - PAYSONRodrigo Joseph PaysonNo ratings yet
- Stomach Ulcers (Peptic Ulcers)Document25 pagesStomach Ulcers (Peptic Ulcers)Irtza MajeedNo ratings yet
- Essay SuryaDocument5 pagesEssay SuryadewasayogaNo ratings yet
- Hepatobiliary DiseaseDocument52 pagesHepatobiliary DiseaseMelissa Laurenshia ThenataNo ratings yet
- CholecystitisDocument12 pagesCholecystitisMariela HuertaNo ratings yet
- Presentation Metabolic SyndromeDocument56 pagesPresentation Metabolic SyndromeAbdulhakeem Tleimat100% (1)
- Motility Disorders of The GITDocument57 pagesMotility Disorders of The GITMahmoud AjinehNo ratings yet
- Pancreatic Diabetes Mellitus: Frequency and DiagnosisDocument10 pagesPancreatic Diabetes Mellitus: Frequency and Diagnosisbalthier37No ratings yet
- Acutep 1Document45 pagesAcutep 1api-19916399No ratings yet
- Disorders of Esophagus and StomachDocument29 pagesDisorders of Esophagus and StomachSamuel kuriaNo ratings yet
- Cholelithiasis and Choledocholithiasis Infos ..Document5 pagesCholelithiasis and Choledocholithiasis Infos ..Franzia Izandra Alkuino MojicaNo ratings yet
- Prot LoseDocument7 pagesProt LoseAkbarian NoorNo ratings yet
- Dysphagia, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandDysphagia, A Simple Guide To The Condition, Treatment And Related ConditionsRating: 5 out of 5 stars5/5 (1)
- Vitamin B12 Malabsorption Syndrome Diarrhea Celiac Disease Iga Screening Test IgaDocument18 pagesVitamin B12 Malabsorption Syndrome Diarrhea Celiac Disease Iga Screening Test IgaPerplexed CeleryNo ratings yet
- Pancreatitis Ercp Pain Amylase Lipase ErcpDocument24 pagesPancreatitis Ercp Pain Amylase Lipase ErcpPerplexed CeleryNo ratings yet
- Anemia Hip Pain Sickle Cell DiseaseDocument9 pagesAnemia Hip Pain Sickle Cell DiseasePerplexed CeleryNo ratings yet
- Stomach Flu Prodromal Scleral Icterus Urine Fever TransaminasesDocument7 pagesStomach Flu Prodromal Scleral Icterus Urine Fever TransaminasesPerplexed CeleryNo ratings yet
- FST 01 PDFDocument12 pagesFST 01 PDFRitwika JanaNo ratings yet
- Super HDB Turbo 15W-40Document1 pageSuper HDB Turbo 15W-40izzybjNo ratings yet
- Single Aisle Technical Training Manual CMQ A330/A340 To A319/320/321 (IAE V2500/ME) T1 (LVL 2&3) DoorsDocument84 pagesSingle Aisle Technical Training Manual CMQ A330/A340 To A319/320/321 (IAE V2500/ME) T1 (LVL 2&3) DoorsjuanNo ratings yet
- English 9 Honors Independent ReadingDocument2 pagesEnglish 9 Honors Independent Readingapi-320461761No ratings yet
- Isa Cem: Comparatives and SuperlativesDocument7 pagesIsa Cem: Comparatives and SuperlativesAnonymous 7xhhVAWCXNo ratings yet
- Analysis of Stuck Pipe and Fishing Operations: Case Study of Olkaria Geothermal Field in KenyaDocument32 pagesAnalysis of Stuck Pipe and Fishing Operations: Case Study of Olkaria Geothermal Field in KenyaIgorCencičNo ratings yet
- Cmo 14Document33 pagesCmo 14Geraldine CaneteNo ratings yet
- Slide Presentation Passive DesignDocument24 pagesSlide Presentation Passive DesignNuratiqah Sharifah100% (1)
- Comparacion Polar y VO2 MaxDocument3 pagesComparacion Polar y VO2 MaxZilanyaid MontoyaNo ratings yet
- CMT Lab ReportDocument3 pagesCMT Lab ReportJohn Emerald GoloNo ratings yet
- Orth Update 2023 16 105-105Document1 pageOrth Update 2023 16 105-105jlkdsjfljsdlfNo ratings yet
- All About Bamboo: Information SheetDocument5 pagesAll About Bamboo: Information SheetQuang Minh NguyễnNo ratings yet
- Tereos Banner TFI Journey FINAL (6DEC23)Document1 pageTereos Banner TFI Journey FINAL (6DEC23)Jundi FaizyNo ratings yet
- Minetruck MT65: Underground Truck With 65-Tonne Load CapacityDocument5 pagesMinetruck MT65: Underground Truck With 65-Tonne Load CapacityAlvaro Patricio Garcia AlfaroNo ratings yet
- Maquina Do Wando PDFDocument76 pagesMaquina Do Wando PDFGlauber AquinoNo ratings yet
- FablesDocument33 pagesFablesAngela Halasan HinautanNo ratings yet
- HealthySFMRA - 03001 - San Francisco MRA Claim FormDocument3 pagesHealthySFMRA - 03001 - San Francisco MRA Claim FormlepeepNo ratings yet
- Turmeric Powder Coriander Powder and Chilli Powder Processing IndustryDocument107 pagesTurmeric Powder Coriander Powder and Chilli Powder Processing IndustryAlexNo ratings yet
- DiverDocument9 pagesDiverAli MinusNo ratings yet
- Eating Well Recipe BookDocument92 pagesEating Well Recipe Bookwhite.serafimNo ratings yet
- Activity No. 4 Module Cell Types and Cell ModificationsDocument7 pagesActivity No. 4 Module Cell Types and Cell ModificationsAryan Jovic DomingoNo ratings yet
- About Beximco Pharmaceuticals LimitedDocument9 pagesAbout Beximco Pharmaceuticals LimitedAsaduzzamannayanNo ratings yet
- Soilless Media MatthewDocument13 pagesSoilless Media MatthewmatthewNo ratings yet
- Quiz 6 Primer Intento Ingles2 07032021Document5 pagesQuiz 6 Primer Intento Ingles2 07032021Carlos CortesNo ratings yet
- Wages For ESICDocument10 pagesWages For ESICvai8havNo ratings yet
- Available Fault Current Selective Coordination SpreadsheetDocument15 pagesAvailable Fault Current Selective Coordination SpreadsheetWISDOM TECHNOSOLUTIONSNo ratings yet
H. Pylori H. Pylori
H. Pylori H. Pylori
Uploaded by
Perplexed Celery0 ratings0% found this document useful (0 votes)
5 views3 pagesIn obese individuals, adipokines released from fat depots decrease insulin sensitivity in peripheral tissues, causing hyperglycemia and hyperinsulinemia. This triggers lipid uptake and lipogenesis in the liver, leading to non-alcoholic fatty liver disease (NAFLD) and non-alcoholic steatohepatitis (NASH), characterized by oxidative stress and hepatocellular damage. Chronic damage can progress to cirrhosis and hepatocellular carcinoma. NASH is diagnosed after ruling out other causes in patients without heavy alcohol use.
Original Description:
Original Title
GI4
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentIn obese individuals, adipokines released from fat depots decrease insulin sensitivity in peripheral tissues, causing hyperglycemia and hyperinsulinemia. This triggers lipid uptake and lipogenesis in the liver, leading to non-alcoholic fatty liver disease (NAFLD) and non-alcoholic steatohepatitis (NASH), characterized by oxidative stress and hepatocellular damage. Chronic damage can progress to cirrhosis and hepatocellular carcinoma. NASH is diagnosed after ruling out other causes in patients without heavy alcohol use.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
0 ratings0% found this document useful (0 votes)
5 views3 pagesH. Pylori H. Pylori
H. Pylori H. Pylori
Uploaded by
Perplexed CeleryIn obese individuals, adipokines released from fat depots decrease insulin sensitivity in peripheral tissues, causing hyperglycemia and hyperinsulinemia. This triggers lipid uptake and lipogenesis in the liver, leading to non-alcoholic fatty liver disease (NAFLD) and non-alcoholic steatohepatitis (NASH), characterized by oxidative stress and hepatocellular damage. Chronic damage can progress to cirrhosis and hepatocellular carcinoma. NASH is diagnosed after ruling out other causes in patients without heavy alcohol use.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
You are on page 1of 3
GI4
In obese individuals, adipokines released from fat depots decrease the insulin sensitivity of
peripheral tissue. Increased peripheral insulin resistance causes post-prandial hyperglycemia,
which, in turn, increases insulin secretion. This hyperinsulinemia triggers lipid uptake as well
as lipogenesis within hepatocytes (non-alcoholic steatosis). The precursors
of triglycerides (e.g., fatty acids, glycerols) and the byproducts of lipid metabolism can cause
hepatocellular damage (non-alcoholic steatohepatitis, NASH) by inducing oxidative stress.
Chronic hepatocellular damage eventually leads to cirrhosis and increased risk of hepatocellular
carcinoma. NASH is only diagnosed in patients with no history of heavy alcohol use and after
other causes of chronic liver disease have been ruled out.
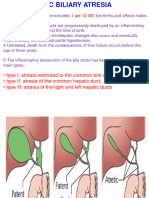
Primary biliary cholangitis (PBC; also known as primary biliary cirrhosis) is a chronic
progressive liver disease of autoimmune origin that is characterized by destruction of the
intralobular bile ducts. The pathogenesis of PBC is unclear; however, it primarily affects middle-
aged women and is frequently associated with other autoimmune conditions. In the early stages,
PBC is typically asymptomatic. Fatigue is the most common initial complaint. In advanced
disease, increased fibrotic changes lead to typical signs of cholestasis (e.g., jaundice) and portal
hypertension (e.g., ascites, gastrointestinal bleeding). Elevated cholestasis parameters (ALP, γ-
GT, bilirubin) as well as antimitochondrial antibodies (AMAs) help establish the diagnosis.
Management consists of slowing disease progression with ursodeoxycholic acid and relieving
symptoms. Liver transplantation is the only definitive treatment.
A combination of amoxicillin, clarithromycin, and omeprazole for a minimum of 7 days is used
for H. pylori eradication therapy. Multiple studies have demonstrated an association
between MALT lymphoma and H. pylori infection. In 60–80% of patients with H. pylori-
associated gastric MALT lymphoma, H. pylori eradication therapy causes complete regression of
the tumor.
Painless jaundice, together with a palpable gallbladder, should always raise suspicion
for pancreatic malignancy. This patient's smoking history is a risk factor for pancreatic
adenocarcinoma, which manifests with biliary tract obstruction as a late sign of infiltrative
disease. Dilated biliary and pancreatic ducts (the double duct sign) can be seen
on ultrasonography as a result of a stenosing tumor in the pancreatic head and subsequent
prestenotic dilation, as seen in this patient. Direct hyperbilirubinemia indicates obstructive
jaundice. The accumulation of serum bile acids, which causes pruritus, could explain the scratch
marks on this patient's extremities. His significant weight loss is another classic symptom of a
malignant process.
Abdominal x-ray is the preferred diagnostic modality for toxic megacolon and should be
ordered in all patients who present with bloody diarrhea, abdominal distention, and
signs of sepsis. Dilation of the transverse colon > 6 cm on plain abdominal x-
ray confirms the diagnosis. Loss of colonic haustration and multiple air-fluid levels
indicate colonic dilation and paralytic ileus. Patients with inflammatory bowel disease,
such as this patient, are at risk of developing toxic megacolon, especially early in the
course of disease (∼ 5% lifetime risk).
Zenker diverticulum is a pulsion-pseudodiverticulum and is caused by an inadequate relaxation
of the upper esophageal sphincter (UES) leading to increased intraluminal pressure that results in
outpouching of the pharyngeal wall. The condition usually forms in
the hypopharynx within Killian triangle, an area of weakness in the posterior pharyngeal wall.
This elderly man presents with classic symptoms of Zenker diverticulum, including dysphagia,
regurgitation of undigested food, halitosis, and a fluctuant neck mass.
Furosemide was likely prescribed to this patient to treat her ascites. If administered in
excess, furosemide can lead to a profound diuresis with water and electrolyte depletion, resulting
in hypokalemia, hypomagnesemia, hypocalcemia, hyponatremia, and ultimately the acute kidney
injury and metabolic alkalosis as seen in this patient. Hypokalemia and hypomagnesemia can
cause life-threatening arrhythmias, such as the ventricular tachycardia suffered by this patient. In
addition to correcting this patient's electrolyte levels, management would also include prompt
rehydration with intravenous fluids.
This patient with decompensated liver cirrhosis most likely has hepatorenal syndrome. As portal
hypertension worsens in patients with decompensated cirrhosis, vasodilatory mediators are
produced, leading to vasodilation of the splanchnic circulation. The altered hemodynamics result
in renal hypoperfusion, which in turn causes a decrease in GFR. Patients typically present with
gradual loss of kidney function, as seen in this patient who developed oliguria over a period of 1
month, an unremarkable urine sediment, and FENa < 1% and BUN/Cr ratio > 20. Treatment of
this condition includes administration of albumin, octreotide, and midodrine. A liver transplant is
the only curative option in advanced liver disease.
You might also like
- Test Certificate of BitumenDocument1 pageTest Certificate of BitumenAmit Prasad50% (2)
- Logbook KoDocument13 pagesLogbook KoMarkmar AnchetaNo ratings yet
- Parts of A Bar.Document3 pagesParts of A Bar.MARY JOY VILLARUEL100% (1)
- Khawater Makki Cover Letter.ADocument1 pageKhawater Makki Cover Letter.AAnonymous miK3qJxNo ratings yet
- Uworld Summary NotesDocument6 pagesUworld Summary Notesnavneet mannNo ratings yet
- Gi Study GuideDocument31 pagesGi Study Guidebsmodi98No ratings yet
- Dr. Ali's Uworld Notes For Step 2 CK: GastroDocument32 pagesDr. Ali's Uworld Notes For Step 2 CK: GastrouyesNo ratings yet
- Day 7 Gal Bladder StonesDocument12 pagesDay 7 Gal Bladder StonesShreyash HaritwalNo ratings yet
- Pancreatitis: Pancreatitis Is Inflammation of The Pancreas. It Occurs When Pancreatic Enzymes (Especially Trypsin)Document6 pagesPancreatitis: Pancreatitis Is Inflammation of The Pancreas. It Occurs When Pancreatic Enzymes (Especially Trypsin)tianallyNo ratings yet
- Set 3 COMP-2Document71 pagesSet 3 COMP-2Appu ayyalaNo ratings yet
- Cirrosis HepaticaDocument10 pagesCirrosis Hepaticaadriel710No ratings yet
- Cirrosis Adnd Its ComplicationDocument50 pagesCirrosis Adnd Its Complicationnathan asfahaNo ratings yet
- Assessment of Jaundice in The Hospitalized Patient PDFDocument16 pagesAssessment of Jaundice in The Hospitalized Patient PDFlaura canoNo ratings yet
- Gall Bladder Diseases by - DR Arun Aggarwal GastroenterologistDocument53 pagesGall Bladder Diseases by - DR Arun Aggarwal GastroenterologistDr. Arun Aggarwal GastroenterologistNo ratings yet
- UlcerativecolitisDocument27 pagesUlcerativecolitisMohamed Abdulrazaq100% (1)
- Doc.6th TopicDocument100 pagesDoc.6th TopicBibinNo ratings yet
- Msn-Small Bowel Disorder - SeminarDocument71 pagesMsn-Small Bowel Disorder - SeminarSarithaRajeshNo ratings yet
- DyspepDocument2 pagesDyspepGeorge WinchesterNo ratings yet
- Case 5 - Pancreatitis-1Document4 pagesCase 5 - Pancreatitis-1ngNo ratings yet
- Disorders of Motility2Document46 pagesDisorders of Motility2valdomiroNo ratings yet
- Biliary System and Pancreatic DisorderDocument59 pagesBiliary System and Pancreatic DisorderAlda AdeliaNo ratings yet
- Chronic Liver FailureDocument4 pagesChronic Liver FailureJasmine Faith SilvaNo ratings yet
- Gallbladder IIDocument22 pagesGallbladder IIAli SafaaNo ratings yet
- Hepatic Cirrhosis and Hepatitis: Dr. Lubna DwerijDocument69 pagesHepatic Cirrhosis and Hepatitis: Dr. Lubna DwerijNoor MajaliNo ratings yet
- Nu'man AS DaudDocument23 pagesNu'man AS DaudHidayat BazeherNo ratings yet
- Digestive System Disorder AssessmentDocument50 pagesDigestive System Disorder AssessmentTaate MohammedNo ratings yet
- Liver CirrhosisDocument38 pagesLiver Cirrhosisfeeo8266No ratings yet
- Pancreatitis Ercp Pain Amylase Lipase ErcpDocument24 pagesPancreatitis Ercp Pain Amylase Lipase ErcpPerplexed CeleryNo ratings yet
- Cholelithiasis and Cholecystitis: de Villa Dennis Fernando M. Level IVDocument38 pagesCholelithiasis and Cholecystitis: de Villa Dennis Fernando M. Level IVsimongarciadevillaNo ratings yet
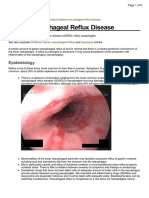
- Gastro-Oesophageal Reflux Disease: EpidemiologyDocument6 pagesGastro-Oesophageal Reflux Disease: EpidemiologyRehan RiyazNo ratings yet
- Gastrointestinal System: Paul Tang, MD, DPAMSDocument30 pagesGastrointestinal System: Paul Tang, MD, DPAMSThakoon Tts100% (1)
- Cholecystitis FinalDocument57 pagesCholecystitis FinalRajendra DesaiNo ratings yet
- Peptic Ulcer Disease: Palangka Raya University Faculty of MedicineDocument70 pagesPeptic Ulcer Disease: Palangka Raya University Faculty of MedicineMITHA100% (1)
- Inflammatoray Bowel DiseaseDocument14 pagesInflammatoray Bowel DiseaseSadr AkrmNo ratings yet
- Abdominal Swelling and Ascites: Global ConsiderationsDocument5 pagesAbdominal Swelling and Ascites: Global ConsiderationsJacob BorongNo ratings yet
- Medical Progress: N F L DDocument11 pagesMedical Progress: N F L DndocNo ratings yet
- Pancreatic Diabetes Mellitus: Frequency and DiagnosisDocument10 pagesPancreatic Diabetes Mellitus: Frequency and DiagnosisRutDanNo ratings yet
- Dr. S.P. Hewawasam (MD) Consultant Gastroenterologist/Senior Lecturer in PhysiologyDocument33 pagesDr. S.P. Hewawasam (MD) Consultant Gastroenterologist/Senior Lecturer in PhysiologyAjung SatriadiNo ratings yet
- 2009 Pearl SheetDocument19 pages2009 Pearl Sheetmikez100% (1)
- Small and Large IntestinesDocument44 pagesSmall and Large IntestinespempuladesmondsimfukwelNo ratings yet
- Ald & MasldDocument19 pagesAld & MasldAli SafaaNo ratings yet
- Pancreatitis: 1 Signs and SymptomsDocument6 pagesPancreatitis: 1 Signs and SymptomsZiedTrikiNo ratings yet
- Esophageal StrictureDocument6 pagesEsophageal StrictureŽäíñäb ÄljaÑabìNo ratings yet
- Bile, Bile Duct and Pancreatic DiseaseDocument82 pagesBile, Bile Duct and Pancreatic Diseaseshahrul rahmanNo ratings yet
- Dissertation ON A Clinical Study On Obstructive JaundiceDocument66 pagesDissertation ON A Clinical Study On Obstructive JaundicePravat SatpathyNo ratings yet
- Intestinal Obstruction in Pediatric SurgeryDocument69 pagesIntestinal Obstruction in Pediatric Surgeryabhinay_1712No ratings yet
- Acute & Chronic Pancreatitis - DoneDocument7 pagesAcute & Chronic Pancreatitis - DoneAriana ValenciaNo ratings yet
- Wa0093.Document27 pagesWa0093.EvaNo ratings yet
- CSS Ulcerative ColitisDocument28 pagesCSS Ulcerative ColitisAthiyyah HasnaNo ratings yet
- Revisao ColecistiteDocument16 pagesRevisao ColecistiteAndrés Menacho AbularachNo ratings yet
- Hepatobiliary Tract and Pancreatic Pathology Assignment - PAYSONDocument22 pagesHepatobiliary Tract and Pancreatic Pathology Assignment - PAYSONRodrigo Joseph PaysonNo ratings yet
- Stomach Ulcers (Peptic Ulcers)Document25 pagesStomach Ulcers (Peptic Ulcers)Irtza MajeedNo ratings yet
- Essay SuryaDocument5 pagesEssay SuryadewasayogaNo ratings yet
- Hepatobiliary DiseaseDocument52 pagesHepatobiliary DiseaseMelissa Laurenshia ThenataNo ratings yet
- CholecystitisDocument12 pagesCholecystitisMariela HuertaNo ratings yet
- Presentation Metabolic SyndromeDocument56 pagesPresentation Metabolic SyndromeAbdulhakeem Tleimat100% (1)
- Motility Disorders of The GITDocument57 pagesMotility Disorders of The GITMahmoud AjinehNo ratings yet
- Pancreatic Diabetes Mellitus: Frequency and DiagnosisDocument10 pagesPancreatic Diabetes Mellitus: Frequency and Diagnosisbalthier37No ratings yet
- Acutep 1Document45 pagesAcutep 1api-19916399No ratings yet
- Disorders of Esophagus and StomachDocument29 pagesDisorders of Esophagus and StomachSamuel kuriaNo ratings yet
- Cholelithiasis and Choledocholithiasis Infos ..Document5 pagesCholelithiasis and Choledocholithiasis Infos ..Franzia Izandra Alkuino MojicaNo ratings yet
- Prot LoseDocument7 pagesProt LoseAkbarian NoorNo ratings yet
- Dysphagia, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandDysphagia, A Simple Guide To The Condition, Treatment And Related ConditionsRating: 5 out of 5 stars5/5 (1)
- Vitamin B12 Malabsorption Syndrome Diarrhea Celiac Disease Iga Screening Test IgaDocument18 pagesVitamin B12 Malabsorption Syndrome Diarrhea Celiac Disease Iga Screening Test IgaPerplexed CeleryNo ratings yet
- Pancreatitis Ercp Pain Amylase Lipase ErcpDocument24 pagesPancreatitis Ercp Pain Amylase Lipase ErcpPerplexed CeleryNo ratings yet
- Anemia Hip Pain Sickle Cell DiseaseDocument9 pagesAnemia Hip Pain Sickle Cell DiseasePerplexed CeleryNo ratings yet
- Stomach Flu Prodromal Scleral Icterus Urine Fever TransaminasesDocument7 pagesStomach Flu Prodromal Scleral Icterus Urine Fever TransaminasesPerplexed CeleryNo ratings yet
- FST 01 PDFDocument12 pagesFST 01 PDFRitwika JanaNo ratings yet
- Super HDB Turbo 15W-40Document1 pageSuper HDB Turbo 15W-40izzybjNo ratings yet
- Single Aisle Technical Training Manual CMQ A330/A340 To A319/320/321 (IAE V2500/ME) T1 (LVL 2&3) DoorsDocument84 pagesSingle Aisle Technical Training Manual CMQ A330/A340 To A319/320/321 (IAE V2500/ME) T1 (LVL 2&3) DoorsjuanNo ratings yet
- English 9 Honors Independent ReadingDocument2 pagesEnglish 9 Honors Independent Readingapi-320461761No ratings yet
- Isa Cem: Comparatives and SuperlativesDocument7 pagesIsa Cem: Comparatives and SuperlativesAnonymous 7xhhVAWCXNo ratings yet
- Analysis of Stuck Pipe and Fishing Operations: Case Study of Olkaria Geothermal Field in KenyaDocument32 pagesAnalysis of Stuck Pipe and Fishing Operations: Case Study of Olkaria Geothermal Field in KenyaIgorCencičNo ratings yet
- Cmo 14Document33 pagesCmo 14Geraldine CaneteNo ratings yet
- Slide Presentation Passive DesignDocument24 pagesSlide Presentation Passive DesignNuratiqah Sharifah100% (1)
- Comparacion Polar y VO2 MaxDocument3 pagesComparacion Polar y VO2 MaxZilanyaid MontoyaNo ratings yet
- CMT Lab ReportDocument3 pagesCMT Lab ReportJohn Emerald GoloNo ratings yet
- Orth Update 2023 16 105-105Document1 pageOrth Update 2023 16 105-105jlkdsjfljsdlfNo ratings yet
- All About Bamboo: Information SheetDocument5 pagesAll About Bamboo: Information SheetQuang Minh NguyễnNo ratings yet
- Tereos Banner TFI Journey FINAL (6DEC23)Document1 pageTereos Banner TFI Journey FINAL (6DEC23)Jundi FaizyNo ratings yet
- Minetruck MT65: Underground Truck With 65-Tonne Load CapacityDocument5 pagesMinetruck MT65: Underground Truck With 65-Tonne Load CapacityAlvaro Patricio Garcia AlfaroNo ratings yet
- Maquina Do Wando PDFDocument76 pagesMaquina Do Wando PDFGlauber AquinoNo ratings yet
- FablesDocument33 pagesFablesAngela Halasan HinautanNo ratings yet
- HealthySFMRA - 03001 - San Francisco MRA Claim FormDocument3 pagesHealthySFMRA - 03001 - San Francisco MRA Claim FormlepeepNo ratings yet
- Turmeric Powder Coriander Powder and Chilli Powder Processing IndustryDocument107 pagesTurmeric Powder Coriander Powder and Chilli Powder Processing IndustryAlexNo ratings yet
- DiverDocument9 pagesDiverAli MinusNo ratings yet
- Eating Well Recipe BookDocument92 pagesEating Well Recipe Bookwhite.serafimNo ratings yet
- Activity No. 4 Module Cell Types and Cell ModificationsDocument7 pagesActivity No. 4 Module Cell Types and Cell ModificationsAryan Jovic DomingoNo ratings yet
- About Beximco Pharmaceuticals LimitedDocument9 pagesAbout Beximco Pharmaceuticals LimitedAsaduzzamannayanNo ratings yet
- Soilless Media MatthewDocument13 pagesSoilless Media MatthewmatthewNo ratings yet
- Quiz 6 Primer Intento Ingles2 07032021Document5 pagesQuiz 6 Primer Intento Ingles2 07032021Carlos CortesNo ratings yet
- Wages For ESICDocument10 pagesWages For ESICvai8havNo ratings yet
- Available Fault Current Selective Coordination SpreadsheetDocument15 pagesAvailable Fault Current Selective Coordination SpreadsheetWISDOM TECHNOSOLUTIONSNo ratings yet