Professional Documents
Culture Documents
Lectura FX Cinética1
Lectura FX Cinética1
Uploaded by
Jeraldiin BeltranCopyright:
Available Formats
You might also like
- Pharmaco KineticsDocument427 pagesPharmaco KineticsMehrdad AvestaNo ratings yet
- Biopharmaceutics - BrahmankarDocument414 pagesBiopharmaceutics - Brahmankarmatin586% (58)
- Post Anesthesia-Recovery Skills ChecklistDocument6 pagesPost Anesthesia-Recovery Skills Checklistnorthweststaffing100% (1)
- Case ConferenceDocument30 pagesCase Conferenceridazaheer29No ratings yet
- Brahmakar - Biopharmaceutics & PharmacokineticsDocument374 pagesBrahmakar - Biopharmaceutics & PharmacokineticsSamritiNo ratings yet
- Pharmacokinetics by Hanna AbrahamDocument27 pagesPharmacokinetics by Hanna AbrahamRom EonNo ratings yet
- BioPharm Midterms ReviewerDocument26 pagesBioPharm Midterms ReviewerCHARLES RONALD GENATONo ratings yet
- BIOPHARMACEUTICSDocument132 pagesBIOPHARMACEUTICSTahaniNo ratings yet
- Biopharmaceutics Note 7th SemDocument38 pagesBiopharmaceutics Note 7th Semmj.vinoth@gmail.comNo ratings yet
- What The Body Does To A Drug: PharmacokineticsDocument14 pagesWhat The Body Does To A Drug: PharmacokineticsSabrina JonesNo ratings yet
- Topic 1 - Introduction Tophysical Pharmacy and Principles of Biopharmaceutics I. Physical PharmacyDocument13 pagesTopic 1 - Introduction Tophysical Pharmacy and Principles of Biopharmaceutics I. Physical PharmacyAi LoveeiNo ratings yet
- Biopharmaceutics - 1 2022Document24 pagesBiopharmaceutics - 1 2022Varshini VarshaNo ratings yet
- Biopharmaceutics: GSDMSFI - BS Pharmacy 3Document11 pagesBiopharmaceutics: GSDMSFI - BS Pharmacy 3Majeddah Aliudin TalambunganNo ratings yet
- Introduction To Biopharmaceutics and PharmacokineticsDocument3 pagesIntroduction To Biopharmaceutics and PharmacokineticsSyeda Eshaal JavaidNo ratings yet
- BiokimmDocument42 pagesBiokimmAdeliaNo ratings yet
- Pharmacology Prelims ReviewerDocument21 pagesPharmacology Prelims ReviewerAntonette Africa MercadoNo ratings yet
- Drug Delivery On Rectal Absorption: Suppositories: Review ArticleDocument7 pagesDrug Delivery On Rectal Absorption: Suppositories: Review ArticleNindah IkaNo ratings yet
- Pharmacokinetics 1: AbsorptionDocument15 pagesPharmacokinetics 1: AbsorptionCecilia GrayebNo ratings yet
- Pharmacology - Pharmacology en PDFDocument386 pagesPharmacology - Pharmacology en PDFMaksym DemianchukNo ratings yet
- Document 2Document9 pagesDocument 2zoha fatimaNo ratings yet
- Pilapil PharmacologyDocument6 pagesPilapil PharmacologyIza FaboresNo ratings yet
- Chapter 1Document32 pagesChapter 1Czerwin JualesNo ratings yet
- NSG 105 Module 3Document22 pagesNSG 105 Module 3Alaminah MULOKNo ratings yet
- Ocular Pharmacology 2Document10 pagesOcular Pharmacology 2cornelia cindy SRDNo ratings yet
- Unit #1 IntroductionDocument22 pagesUnit #1 IntroductionSaima VictorNo ratings yet
- Basics of Biopharmaceutics: A Mini Review: Bioequivalence & Bioavailability International JournalDocument5 pagesBasics of Biopharmaceutics: A Mini Review: Bioequivalence & Bioavailability International JournalLina WinartiNo ratings yet
- Introduction To Pharmacology Part 2Document10 pagesIntroduction To Pharmacology Part 2jason fiasonNo ratings yet
- Unit One of PharmacologyDocument63 pagesUnit One of PharmacologyAbdinaasir MohamedNo ratings yet
- Cclec Drug MonitoringDocument14 pagesCclec Drug MonitoringAndrea Gail GutierrezNo ratings yet
- Unit #1 IntroductionDocument22 pagesUnit #1 IntroductionSaima VictorNo ratings yet
- Pharmacokinetic and Pharmacodynamic2021Document12 pagesPharmacokinetic and Pharmacodynamic2021STEFANIA AYA DIAZNo ratings yet
- Pharma Chapter 2_modDocument57 pagesPharma Chapter 2_modAlex CheungNo ratings yet
- EXERCISE#2Document5 pagesEXERCISE#2Ana GarciaNo ratings yet
- 4-Pharmacokinetics IDocument88 pages4-Pharmacokinetics IMarc Imhotep Cray, M.D.No ratings yet
- Pharmacokinetics: The Absorption, Distribution, and Excretion of DrugsDocument14 pagesPharmacokinetics: The Absorption, Distribution, and Excretion of DrugsAriiNo ratings yet
- Handbk of Basic Pharmacokinetics Chap. 2Document3 pagesHandbk of Basic Pharmacokinetics Chap. 2MoonGalaxyNo ratings yet
- Pharmacology Unit 1Document58 pagesPharmacology Unit 1Asif Ali LashariNo ratings yet
- Introduction To BiopharmaceuticsDocument27 pagesIntroduction To BiopharmaceuticsAmina Akther Mim 1821179649No ratings yet
- Biopharmaceutics BrahmankarDocument413 pagesBiopharmaceutics BrahmankarsrivathsavapNo ratings yet
- Ladmer SystemDocument26 pagesLadmer SystemAbdul Mannan80% (5)
- Pharmacokinetics PDFDocument14 pagesPharmacokinetics PDFLea PesiganNo ratings yet
- Pharmacology: B.Pharm, 2011, M.Pharm, 2016Document19 pagesPharmacology: B.Pharm, 2011, M.Pharm, 2016علي عبد اللطيفNo ratings yet
- Unit#1principle of PharmacologyDocument58 pagesUnit#1principle of PharmacologySaima VictorNo ratings yet
- تصميم كويزDocument73 pagesتصميم كويزHemo HindiNo ratings yet
- 01.25.01 Principles of Pharmacokinetics - Absorption and DistributionDocument10 pages01.25.01 Principles of Pharmacokinetics - Absorption and DistributionMikmik DGNo ratings yet
- Pharmacokinetic Lecture NotesDocument45 pagesPharmacokinetic Lecture NotesAmy Wu0% (1)
- Morgan 140 149Document10 pagesMorgan 140 149Marta DumitracheNo ratings yet
- Overview of Factors Affecting Oral Drug AbsorptionDocument11 pagesOverview of Factors Affecting Oral Drug Absorptionmahveen balochNo ratings yet
- Physical Pharmacy ReviewerDocument23 pagesPhysical Pharmacy ReviewerChrister Jon AcostaNo ratings yet
- Makalah KBM Kel 3Document32 pagesMakalah KBM Kel 3Novia RozadiNo ratings yet
- College of Pharmacy Biopharmaceutics and Pharmacokinetics Assignment No. 1Document6 pagesCollege of Pharmacy Biopharmaceutics and Pharmacokinetics Assignment No. 1ERIKA JADE TORRESNo ratings yet
- Biopharmaceutics and PharmacokineticDocument4 pagesBiopharmaceutics and PharmacokineticRiyaz AliNo ratings yet
- 2.principles of Pharmacokinetics Pharmacodynamic SlidesDocument13 pages2.principles of Pharmacokinetics Pharmacodynamic Slidesran8384080No ratings yet
- Drug Absorption-DistributionDocument60 pagesDrug Absorption-DistributionRuqayya AdamuNo ratings yet
- Learning Packet in Level 1-NCM 106 NURSING PHARMACOLOGY: College of Nursing School Year 2020-2021Document15 pagesLearning Packet in Level 1-NCM 106 NURSING PHARMACOLOGY: College of Nursing School Year 2020-2021Nur Sanaani100% (1)
- Share Pharmacology Book 1Document101 pagesShare Pharmacology Book 1Jmcle AhmedNo ratings yet
- Pharmacology- The Molecular Dance: Understanding Drug Interactions: Harmony and Chaos: The Symphony of Drug InteractionsFrom EverandPharmacology- The Molecular Dance: Understanding Drug Interactions: Harmony and Chaos: The Symphony of Drug InteractionsNo ratings yet
- Handbook of Drug Interaction and the Mechanism of InteractionFrom EverandHandbook of Drug Interaction and the Mechanism of InteractionRating: 1 out of 5 stars1/5 (1)
- Translational ADMET for Drug Therapy: Principles, Methods, and Pharmaceutical ApplicationsFrom EverandTranslational ADMET for Drug Therapy: Principles, Methods, and Pharmaceutical ApplicationsRating: 1 out of 5 stars1/5 (1)
- Border MoldingDocument39 pagesBorder MoldingRachelAngelaGabrielGalsimNo ratings yet
- GUY Et Al 1994 - Regulation of Colostrum Formation in Beef and Dairy CowsDocument6 pagesGUY Et Al 1994 - Regulation of Colostrum Formation in Beef and Dairy CowsMonique IndNo ratings yet
- Megaloblastic AnaemiaDocument11 pagesMegaloblastic AnaemiaJesmin_36No ratings yet
- PRI Breathing TechniquesDocument4 pagesPRI Breathing Techniqueskrserre5934100% (2)
- Basic Embryology Series-1-1Document229 pagesBasic Embryology Series-1-1davidbenedict870No ratings yet
- Bpoc Si Comorbiditati: Dr. Ursarescu Bianca Medic Rezident Pneumologie An IIIDocument35 pagesBpoc Si Comorbiditati: Dr. Ursarescu Bianca Medic Rezident Pneumologie An IIIBabii Alin Adrian100% (1)
- Grand Case PresentationDocument50 pagesGrand Case PresentationJean Michelle100% (1)
- Raven Biology of Plants: Eighth EditionDocument43 pagesRaven Biology of Plants: Eighth EditionMoath EnnabNo ratings yet
- RPI System Krol 1973 JPDDocument19 pagesRPI System Krol 1973 JPDMahadevan Ravichandran100% (1)
- Semi-Detailed Lesson Plan Multi Grade Grade 4&5 Lesson PlanDocument6 pagesSemi-Detailed Lesson Plan Multi Grade Grade 4&5 Lesson Plandianie joyNo ratings yet
- Skinny Helpers Cheat SheetDocument12 pagesSkinny Helpers Cheat SheetJennifer AllenNo ratings yet
- Neuropsychology 2O23Document8 pagesNeuropsychology 2O23farhaanah.abdullah02No ratings yet
- National Hal PG RopsDocument32 pagesNational Hal PG RopsRade NovakovicNo ratings yet
- Chapter 2. The Biological PerspectiveDocument40 pagesChapter 2. The Biological Perspectiveberk.turbil1457No ratings yet
- Nephron ColoringDocument3 pagesNephron ColoringkishoreddiNo ratings yet
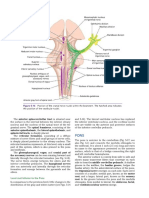
- Snell's Clinical Neuroanatomy Chapter PonsDocument6 pagesSnell's Clinical Neuroanatomy Chapter PonstsidazizyNo ratings yet
- Cephalosomatic LinkageDocument8 pagesCephalosomatic LinkageBrijeshNo ratings yet
- AcsDocument103 pagesAcsVikrant WankhedeNo ratings yet
- Mutant Formation PDFDocument5 pagesMutant Formation PDFMohan BalajiNo ratings yet
- Drug Study Final 1Document47 pagesDrug Study Final 1Nik2No ratings yet
- Science Exam Part I. Write The Parts of The Excretory System. (4 Points)Document5 pagesScience Exam Part I. Write The Parts of The Excretory System. (4 Points)Siria PinedaNo ratings yet
- New Scientist Essential Guide - No7 - The Human BrainDocument100 pagesNew Scientist Essential Guide - No7 - The Human BrainHieu Trinh100% (4)
- Aqa Y2 P2 Jun 19 MSDocument19 pagesAqa Y2 P2 Jun 19 MSestee.onyeNo ratings yet
- BC-2600 - Service Training - V2.0 - ENDocument157 pagesBC-2600 - Service Training - V2.0 - ENsandeep ntNo ratings yet
- Abdominal Aortic AneurysmDocument23 pagesAbdominal Aortic AneurysmHani AbulkhairNo ratings yet
- Bryant and Monie 2012Document10 pagesBryant and Monie 2012Le Uyen NguyenNo ratings yet
- Retic MethodDocument18 pagesRetic MethodFaty DearNo ratings yet
- GP MCQ 11Document4 pagesGP MCQ 11Marta MoreiraNo ratings yet
Lectura FX Cinética1
Lectura FX Cinética1
Uploaded by
Jeraldiin BeltranOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Lectura FX Cinética1
Lectura FX Cinética1
Uploaded by
Jeraldiin BeltranCopyright:
Available Formats
Introduction to
Pharmacokinetics
Part 1: Basic Concepts
MICHAEL E. BURTON
ave you wondered what happens to a drug products will be discussed. Pharmacokinetic models,
H within the patient's body after it has been admin
istered? Have you questioned how the medica
tion finds its way from the site of administration to pro
dosing methods, and factors which m a y necessitate
alteration of drug therapy will be discussed so pharmacy
technicians will understand the rationale of dosage
duce an effect? This article will review the science of individualization.
pharmacokinetics and answer these questions. This review is meant to be an overview, not an in
In order to understand the importance of pharmacoki depth discussion of pharmacokinetics. M o r e complex
netics, the definition of this science is required. In addi systems often are used in practice to describe the phar
tion, understanding the application of pharmacokinetics macokinetic modeling of drugs than those described in
is essential for better comprehension of drug therapy. this article. Because of the depth of the subject, the
Pharmacokinetics has been described as the study and readers are referred to the references for more detailed
characterization of the time course of drug absorption, explanation. In addition, a glossary is provided to define
distribution, metabolism, and elimination, as well as the terminology. (All italicized words are included in the
relationship of these processes to the intensity and time glossary.) Part I of this article will deal with basic con
course of therapeutic and adverse effects of drugs. 1
cepts; part II will address clinical application of phar
Application of the science of pharmacokinetics to the macokinetic methods.
collection of clinical research data has produced a clin
ical health science, clinical pharmacokinetics. One prac Absorption
tical use of this clinical science is to enhance drug dosing
Absorption is the process by which a drug enters the
and thereby therapeutics. Individualization of drug ther
systemic blood circulation; it m a y occur via many
apy using clinical pharmacokinetic methods has been
routes of administration. The routes of administration
proven to decrease toxic and subtherapeutic effects,
2
requiring absorption include oral, intramuscular, sub
thereby improving therapeutics. Thus, the purpose of
cutaneous, rectal, sublingual, transdermal, and inhala
this article is to discuss the basic concepts of phar
tion. The administration of a drug through two other
macokinetics. In addition, concepts of bioavailability
routes, intravenous and intraarterial (directly into the
and the use of bioavailability data to select drug
systemic blood circulation), does not require absorp
tion. A drug and the delivery method (e.g., tablet, cap
sule, injection) must have certain characteristics to
MICHAEL E. BURTON, PharmD, is Clinical Pharmacist, Phar ensure adequate absorption by the desired route of
macology Section (HE), Veterans Administration Med administration. These characteristics will be discussed
ical Center, Dallas, TX, and Clinical Assistant Professor in subsequent paragraphs.
of Pharmacy, College of Pharmacy, The University of
As an example of the effect of the route of adminis
Texas, Austin, TX.
tration upon absorption, the most c o m m o n route of
journal of Pharmacy Technology Mar/Apr 1986 67
administration, oral, will be discussed. Absorption via intestine, the duodenal and jejunal segments are the pre
the oral route m a y be influenced b y the characteristics dominant absorption sites. S o m e absorption may occur
of the drug, the characteristics of the dosage form, and in the ileal segment. Presentation of a drug to the duode
gastrointestinal (GI) function. Figure 1 provides a num and jejunum is dependent upon the rate of gastric
representation of oral drug absorption and T a b l e 1 out emptying. Generally, the faster the rate of gastric emp
3
lines the factors modifying drug a b s o r p t i o n . As seen tying, the m o r e rapid the rate of absorption. O n c e in
in Figure 1, any dosage form must disintegrate into the small intestine, the drug must cross through the lipid
molecular particles forming a solution before a drug can membranes of the epithelial cell to reach the systemic
cross the lipid membranes (epithelial cell membranes) circulation. Lipid soluble molecules, small hydrophilic
of the GI tract. T h e processes of disintegration and dis molecules, and ions readily pass through this lipid bar
solution depend on the physical properties of both the rier. S o m e drugs m a y even be metabolized by enzymes
drug and the particular type of dosage form. For exam within the epithelial cell before reaching the systemic
ple, disintegration time for tablets depends on tablet circulation. Levodopa is an example of a drug metabo
compression and various excipients that facilitate dis lized b y an enzyme present within the epithelial cell. 4
integration. Generally, the rate-limiting step for absorp
tion is considered to be the dissolution rate. Dissolution
depends upon the salt form of the drug, crystal size, sur
Absorption takes place through two
face area of the particles, particle size, and manufac
turing variables. processes, passive diffusion and active
Additional factors m a y limit absorption of the dis transport.
solved drug. T h e drug must be stable in stomach acid
and resist enzymatic hydrolysis from pancreatic
enzymes in order to be available for absorption in the Absorption takes place through two processes, pas
small intestine or stomach. In addition, some drugs may sive diffusion and active transport. Passive diffusion is
complex with gastric content such as food or mucins, a first-order process (absorption is proportional to con-
which reduce the amount of drug available for absorp
tion. An example of complexation is calcium (a diva
lent ion and component of milk) forming a complex with
tetracycline, an antibiotic, thus inactivating the tetracy Table 1 .
cline and reducing the amount of active drug absorbed. Factors Modifying Drug Absorption
It is the nonionized form of a drug that is absorbed,
Physical properties of the drug
whether in the stomach or the small intestine. Since ioni lipid solubility (partition coefficient)
zation is dependent upon pKa (pH at which 5 0 percent pKa (ionization)
solubility
of the drug is ionized), absorption m a y be limited b y
stability (i.e., in gastric fluid, water, air)
this physiochemical property of a drug. For example, molecular weight
acidic drugs m a y be partially absorbed in the stomach Properties of the dosage form
because they are nonionized at gastric pH, even though disintegration time
tablet compression
the stomach is not the primary site for absorption. T h e
excipients added for disintegration
primary site of absorption is the small intestine due to dissolution rate
the large surface area available. Since m a n y drugs are particle surface area
crystal size
either weak acids or bases and not ionized at a pH near
salt form
neutral (pH 7 . 0 ) , the neutral pH of the small intestine manufacturing variables
can facilitate absorption of some drugs. Within the small Properties of lumen fluid
pH
enzymes
complexing or solubilizing agents
viscosity
effects of other drugs
absorbants (activated charcoal)
antacids
complexing agents
Factors affecting gastric transit
motility
gastric emptying
drugs altering peristalsis
Factors at absorption site
surface drug
blood flow membrane permeability (lipid solubility)
Figure 1 . A representation of oral absorption with some of the various factors that carrier-mediated transport (glucose)
may affect drug absorption. For further explanations of factors influencing drug local blood flow
absorption, refer to text. Reproduced with permission from Barr WH. Principles epithelial cell metabolism (levo-dopa)
of biopharmaceutics. Am J Pharmaceut Ed 1968;52:958-81.
68 journal of Pharmacy Technology Mar/Apr 1986
5
centration; Figure 2 ) . The force that drives drugs Table 2. Disease-Induced Alteration
through the epithelial cell is the concentration difference of Drug Absorption
on either side of the cell membrane. T h e rate of drug
penetration depends on lipid solubility, surface area of Delayed stomach emptying (decreased rate of absorption)
the small intestines, and concentration difference. Active atrophic gastritis
gastric carcinoma
transport or facilitated diffusion, being carrier-dependent pyloric stenosis
processes, have a capacity-limited mechanism for trans migraine
gastric ulcer
port of drugs across membranes. A s seen in Figure 2,
pancreatitis
the greater the concentration, the more limited the surgical procedures
absorption of a drug becomes until finally a maximal Enhanced stomach emptying (increased rate of absorption)
rate is reached (i.e., all carriers are employed). celiac disease
calculer cholecystitis
Changes in GI motility m a y alter absorption. Slow duodenal ulcer
ing tends to increase absorption, while increasing motil stress
ity may decrease absorption. Table 2 outlines disease gastroenterostomy
states that may change GI motility and thus drug Alterations in absorption
6
diarrhea—decreased
absorption. In addition, various drugs can alter GI celiac disease—variable
motility and therefore drug absorption. Some classic Crohn's disease—variable
examples include metoclopramide, which increases GI food—variable
fluid intake (increased volume increase rate and extent
motility, and propantheline or opiate analgesics which of absorption)
slow gastrointestinal motility.
Using research generated by
bioavailability studies, we can Bioavailability
evaluate product absorption or at The term bioavailability is used to describe the rate
least be aware of potential problems 7 9
and extent of absorption. " By comparing a drug prod
uct to a reference standard, bioavailability can be
with drug absorption.
directly measured. If the reference standard is com
pletely absorbed (i.e., intravenous dose), then the evalu
ation is an absolute bioavailability study. Comparison
With the many factors that may influence absorption, of a drug dosage form to another dosage form with the
how are we assured of complete or at least adequate same chemical composition is called a comparative
and consistent drug absorption? Using research gener bioavailability study. Usually, bioavailability studies
ated by bioavailability studies, we can evaluate prod involve giving human subjects a dose of a drug, then
uct absorption or at least be aware of potential problems measuring serum concentrations generated from that
with drug absorption. dose over a specific time period. The bioavailability of
a product is found by comparing the area under the
serum concentration-time curve ( A U C ) of one formu
lation with that of the reference product or standard
(Equation 1 ) . The ratio (F, or fraction absorbed) which
results is a decimal and c a n be converted to a percent
age by multiplying by 1 0 0 .
Extent of absorption (F) =
area under curve ( A U C ) [product]
area under curve ( A U C ) [standard] (Eq. 1)
Generally, A U C is determined by computer fitting of
7 9
data or simpler mathematical methods. "
Comparison of bioavailability of different formula
Concentration
tions of a drug is performed by assessing parameters that
Figure 2. A plot of concentration vs. initial rate of transport that illustrates the
difference between the linear passive diffusion and non-linear active (carrier medi represent the rate and exent of absorption. The param
ated) transport. As can be seen, carrier-mediated transport reaches a maximal
rate while, theoretically, passive diffusion does not. Most drugs are absorbed by eters that represent the rate of absorption of any for
passive diffusion; thus, absorption across the Gl wall is limited primarily by phys- mulation include the time required to reach maximal
iochemical factors and the concentration gradient across the cell membrane.
Reproduced with permission from Rowland M, Tozer T N . Clinical concentration and the maximal serum concentration.
pharmacokinetics—concepts and applications. Philadelphia: Lea and Febiger,
1980:19. The extent of absorption is represented by the A U C (Fig-
journal of Pharmacy Technology Mar/Apr 1986 69
ure 3 ) . Both the rate and extent of absorption must be (lipid solubility), blood flow to organs (organ size), and
10
similar for different formulations of the same drug for plasma and protein b i n d i n g . Since ionized drugs do
those formulations to be bioequivalent. For drugs that not cross membranes well, drugs that are ionized at the
are bioinequivalent, there must be a statistically signifi pH of the b l o o d will not penetrate through the wall of
cant difference in the rate and extent of absorption, but, these small b l o o d vessels called capillaries, and distri
for different formulations of a drug to have therapeu bution m a y be reduced. Drugs that are not lipid solu
tic equivalence, the drugs must have similar clinical ble penetrate cell m e m b r a n e barriers poorly. An
effectiveness and safety. Thus, in determining bioavail example would be penicillin, which is not lipid soluble
ability one must discern the ability of a particular dos and has p o o r penetration of the non-inflamed brain.
age form of a drug to be absorbed into the systemic Changes in the lipid membranes due to inflammation
circulation, then compare its absorption characteristics improve penicillin distribution to the brain. Disease
to the reference standard using the a b o v e three param states that can change systemic blood flow, such as
eters. Generally, important differences in bioavailabil myocardial infarction, produce a change in the volume
ity occur with drugs that have steep dose-response of distribution. An example of a drug with distributional
relationships, a poor or narrow therapeutic index, or changes due to myocardial infarction is lidocaine." Both
those drugs eliminated by capacity-limited biotransfor plasma and tissue binding can influence the magnitude
12
mation (at least a 2 0 percent difference in bioavailabil of volume of distribution. T h e plasma protein bind
ity is considered important). ing affects the amount of free drug available to disperse
into the tissues; the drug bound to tissue can represent
Distribution a large pool of drug with the resultant increase in the
magnitude of distribution. T h e relationship of tissue and
O n c e a drug crosses the epithelial cell m e m b r a n e of plasma protein binding to volume of distribution can
the GI tract and enters the splanchnic (GI) blood circu be understood by the following equation:
lation, the drug is distributed to the remainder of the
circulation. T h e rate-limiting step for distribution to the V d total = V b t e o d + V t i 5 5 u e fraction unbound (blood)
body is blood flow. O n c e a drug is distributed through
fraction unbound (tissue)
out the systemic circulation, it m a y diffuse to the
(Eq. 3)
extracellular fluid which bathes cells, bind to plasma
proteins, or bind to and enter red blood cells. Outside This equation relates the total distribution volume ( V d
of the systemic circulation and in the extracellular fluid, total) to the blood volume ( V ) and volume of other b k ) o d
a drug may bind to body tissues, drug receptors, or enter tissues in the b o d y ( V ) plus the fraction of the
tissue
the cell. This distribution of drug can be quantitated to unbound drug in the blood and the tissue. Thus, changes
provide an estimation of the apparent space in the body in binding to proteins in the b l o o d (plasma) will alter
that contains the drug. T h e pharmacokinetic parame total volume of distribution. Generally, a decrease in
ter which describes this distribution space is called the plasma protein binding without a change in tissue bind
volume of distribution. V o l u m e of distribution can be ing will increase volume of distribution (Table 3). Obvi-
imagined as the volume of drug in fluid at a specific con
centration it takes to fill a bucket. T h e distribution o f
each drug for the human b o d y would be represented
by a different size of bucket. Technically, the volume
of distribution is a proportionality constant relating
plasma concentration to the total amount of drug in the
5
body; it may range from 0.04 L / k g to 2 0 L / k g or m o r e .
Volume of distribution ( V ) = d
total amount of drug in the b o d y (dose)
concentration at time 0 (Eq. 2)
T h e above equation describes the relationship of vol
ume of distribution and dose to serum concentration.
This particular equation assumes a one-compartment I I I I I I I I 1 I I ι ι I I
0 1 2 3 4 S 6 7 β 9 10 11 12 13 14
model with instantaneous input of a dose, e.g., an
intravenous bolus. T h u s , if one were to sample the Time (hours)
blood of a patient immediately following an intravenous
Figure 3. A plasma concentration-time curve representing the oral absorption of
dose, volume of distribution could be determined from a drug. By the evaluation of data found in this graph, estimates of bioavailability
8 can be determined. Time to peak concentration and peak height represent rate
the dose and blood (serum) c o n c e n t r a t i o n . of absorption. The area under the curve (AUC) from the plasma concentrations
Distribution is dependent upon factors that include determined at the various times represents the extent of absorption. The rate and
extent of absorption represents bioavailability. Comparative bioavailability can be
the pKa of a drug (ionization), the partition coefficient determined by comparing the rates and extent of absorption between products.
70 journal of Pharmacy Technology Mar/Apr 1986
ously, changes in tissue binding m a y alter volume of Table 3. Inverse Relationships between
distribution. For example, the greater the tissue bind Volume of Distribution and
ing (smaller the fraction unbound), the larger the vol Plasma Protein Binding
ume of distribution. Drugs such as digoxin that are
highly tissue bound have large volumes of distribution PLASMA PROTEIN
VOLUME OF DISTRIBUTION BINDING
(7-10 L / k g ) . T h u s , drug ionization, lipid solubility, DRUG (L/kg) (%)
blood flow, and plasma and tissue binding can influence Amitryptyline* 8.3 96.4
a drug's volume of distribution. Digoxin* 3-10 25
Propranolol* 3.9 93.3
Quinidine* 2.7 71
Cimetidine 2.1 19
Procainamide 1.9 16
When patients take multiple Carbamazepine 1.4 82
medications, one drug may decrease Diazepam 1.1 98.7
Phénobarbital 0.88 51
or enhance the metabolism of another Phenytoin 0.64 89
drug. Digitoxin 0.51 90
Theophylline 0.50 56
Gentamicin 0.25 <10
Tolbutamide 0.15 93
Warfarin 0.11 99
Furosemide 0.11 95.9
Metabolism and Elimination
"Highly tissue bound
As soon as the absorption process begins, elimina
tion starts. Elimination m a y occur by metabolism, then
lipid-soluble) forms. O n c e in these more soluble forms,
excretion of metabolites in the bile or urine; or elimi
drug metabolites m a y be excreted into the bile. In the
nation m a y occur b y renal excretion. S o m e drugs m a y
intestine these metabolites m a y be excreted in feces or
be eliminated b y other means, such as volatile sub
they m a y be altered b y enzymes or bacteria to an active
stances exhaled by the lung and drugs eliminated in per
form and recirculate throughout the b o d y . In addition,
spiration. T h e c o m b i n a t i o n of metabolism a n d / o r
drug metabolites m a y be excreted and possibly reab
elimination can be quantitated by measurement of drug
sorbed b y the kidney. T h r e e processes m a y affect renal
clearance. Clearance is the rate of elimination b y all
drug elimination: glomerular filtration, tubular secre
routes compared to the concentration of a drug in a n y
13
tion, and tubular reabsorption. T h e rate of glomerular
biologic fluid. In addition, clearance is additive in that
filtration depends on the volume of plasma filtered by
systemic clearance m a y be a combination of hepatic,
the glomeruli and the unbound concentraton of drug
renal, or other elimination. This rate of elimination may
in the plasma. T h e balance of tubular secretion and
be quantitated under steady state conditions b y Equa
reabsorption m a y account for a net renal secretion of
tion 4 .
drugs. T h e mechanism of secretion is an active process
that is saturable, while reabsorption is passive.
Clearance (CI) =
Often the metabolic and elimination processes m a y
dosing rate (must be continuous infusion) be altered b y other factors, including other drugs, dis
14
C s s (drug concentration at steady state) (Eq. 4) ease processes, diet, genetics, nutrition, e t c . W h e n
patients take multiple medications, one drug m a y
where steady state is the point in time that dosing rate decrease or enhance the metabolism of another drug.
of a drug to the systemic circulation equals the rate of A drug m a y decrease the metabolism of another drug
active drug elimination. Generally, this is considered b y competitive or complete inhibition of a particular
to be essentially complete at five times the biologic half- drug metabolizing enzyme. Alternatively, some drugs
life (tVi). enhance the metabolism of a drug b y inducement of
these same enzyme systems. In addition, by inheritance
Steady state = 5 X tVi (Eq. 5) (genetics), some drugs m a y not be metabolized as
rapidly (for example, acetylation enzymes), Thus, many
The primary sites of elimination are the liver and kid complex factors can alter the rate of drug metabolism.
ney. Within the liver, biotransformation or metabolism Measurement of metabolic rate can be performed b y
occurs. Most drugs are metabolized to some degree, examination of a serum concentration-time curve (Fig
usually to inactive metabolites, and then excreted in the ure 4 ) . Elimination can be seen b y the decline of plasma
bile. T h e basic metabolic pathways include oxidation, concentration over time which is measured b y the slope
reduction, conjugation, or hydrolysis. With some drugs, 10
(elimination rate c o n s t a n t ) . In addition, half-life can
multiple pathways m a y be used. Generally, metabolism be measured b y the time it takes for the serum concen
leads to conversion of drugs to more water-soluble (less trations to decrease by one-half (Figure 4 ) . B y multiply-
journal of Pharmacy Technology Mar/Apr 1986 71
ing volume of distribution ( V ) by elimination rate d small dosing change may produce a disproportionate
constant ( K J , clearance can be determined (Equation 6). rise in serum concentration with resultant toxicity.
Use of information obtained from studies of drug
Clearance (CI) = V d · K e (Eq. 6)
clearance, distribution, and half-life are helpful in
T w o , and preferably three or four, serum drug concen prediction of dose and dosage interval to obtain max
trations are used clinically to estimate these values for imal therapeutic response. (Use of this pharmacokinetic
a particular patient. In more formal research studies, information about a drug by using clinical pharmacoki
multiple serum drug concentration sampling requiring netics will be discussed in part II.)
1 0 - 2 0 samples at different times is performed.
Pharmacokinetic Modeling
Pharmacokinetic modeling is a Pharmacokinetic modeling is a method of describing
the processes of absorption, distribution, and elimina
method of describing the processes of tion within the body. Figures 4, 5, and 6 represent differ
absorption, distribution, and ent modeling methods. Figure 4 represents a linear,
elimination within the body. one-compartment model, which is the simplest mathe
matically to understand. W i t h a one-compartment
model, the b o d y represents one compartment. A drug
Figure 4 demonstrates a drug with first-order phar that just distributed to the blood volume would fit this
macokinetics. In other words, serum concentration is model. However, most drugs distribute to extracellu
proportional to dose. M a n y drugs behave according to lar water or b o d y tissue and are better described by a
first-order pharmacokinetics; however, some drugs such two-compartment model, as seen in Figure 6. In this
as phenytoin or ethanol (grain alcohol) best fit a model, the b o d y is represented as two compartments,
capacity-limited pharmacokinetic model. With capacity- a central compartment representing blood volume and
limited pharmacokinetics there may be a disproportion a peripheral compartment representing b o d y tissues or
ate rise in serum concentration in response to a dosage extracellular fluids. Elimination occurs from the central
increase. A s can be seen in Figure 5 , serum concentra compartment (Figure 6 ) . It m a y occur from the
tions decline in a non-linear manner. Dosing of drugs peripheral or both compartments, depending on how
with capacity-limited metabolism is difficult because a a drug is eliminated.
MICHAELIS-MENTEN KINETICS
10
Slope=
5h When Cp«K ,the m
linear portion of the
Iv Bolus
Semilogarithmic
Input Compartment
plot allows estimation of
V m a x ^ m i therefore, use
k-Elimlnatlon Rate Constant this r e p r e s e n t a t i o n at low
< serum concentrations
1 1 1
2
10
Slope of Line Equals -k ( ο
v Slope = -Vn.
5h When C p » K , m
the linear portion
of the L i n e a r plot
allows estimation of
v
m a s · therefore, use
this r e p r e s e n t a t i o n at
hiah serum concentrations
10 11 12 13 14 15
Iv Dose
I Given Instantly Time (hours)
TIME
Figure 4. A plot of serum concentrations vs. time following an instantaneous Figure 5. The upper figure represents a semilogarithmic (log) plot of serum con
intravenous dose. The linear decline in serum concentralions indicates that this centration vs. time following a dose of a drug displaying capacity-limited (Michaelis-
drug would fit a one-compartment pharmacokinetic model. This means that the Menten) pharmacokinetics. The linear portion o( the graph (serum concentration
body represents a single compartment to which the drug distributes. The concen <5) allows estimation of a slope of the line which equals V ( V in text)/K .m a x m m
tration at time zero (C ) may be determined by dividing the intravenous dose by
ç When plotted in a linear fashion (lower plot) - V can be estimated from the
m a i (
the volume of distribution; or, by rearranging the equation, volume of distribution linear portion of the plot. Thus with an adequate number of serum concentrations
may be determined. The slope of the line represents the elimination rate constant following a dose, the parameters V ( V in text) and K can be determined to
m a x m m
(K ). Half-life (tVj) may be determined directly by dividing 0.693 (Ln 2) by K (tV4
e e use for subsequent dosing. These plots demonstrate the non-linearity of capacity-
= 0.693/K ). The concentration at any time after the dose may be determined
5 limited metabolism. Thus, a small increase in a dose of a drug displaying this type
by multiplying C times the natural log θ raised to the negative exponent of Κ mul
0 of metabolism will produce a greater than proportional increase in serum concen
tiplied by the time since C . 0 tration because the metabolic rate may be maximal.
72 journal of Pharmacy Technology Mar/Apr 1986
Mathematical equations from these methods are used is a determinate of drug clearance (Equation 8 ) . 1 2
to predict the concentration of a drug at a particular
Cl = Q · Ε Eq. 8
time. For drugs where precise dosing is necessary to pro
duce desired response, the prediction of serum concen where CI — clearance, Q = blood flow, and Ε =
trations is particularly important for accurate dosing. extraction ratio (or fraction).
Drugs requiring precise dosing have a narrow therapeu
Extraction ratio is described by the equation:
tic index.
T~ CI intrinsic
Other models include the Michaelis-Menten or meta Ε —
c
Eq. 9
n
bolic capacity-limited model (Figure 5 ) . This model Q + CI intrinsic
describes the interactions of an enzyme system (which where CI intrinsic reflects the inherent ability of the
13
is saturable) upon a substrate. In the body, this m a y organ to remove the drug.
represent hepatic drug metabolizing enzymes and a drug This concept is similar to that of the Michaelis-Menten
(substrate). This model describes drugs like aspirin, model. Often, the intrinsic clearance of a drug may
phenytoin, and ethanol. This model is described by the exceed what would be expected as a result of blood flow.
Michaelis-Menten equation: Propranolol and lidocaine are notable examples, in that
the liver so avidly extracts the drug that clearance
K m + C ss (Eq. 7) depends on blood flow. Phenytoin can also be described
with this model, in that the intrinsic clearance is low.
where R = rate of elimination, V m = maximal meta
W h e n intrinsic clearance is small, clearance is more
bolic rate, C ss = steady state serum concentration, and
dependent upon the intrinsic ability of the liver to clear
K,,, = the serum concentration at which metabolic rate
a drug and extraction ratio instead of blood flow.
is one-half maximal.
These modeling systems can provide the basis to pre
By definition, at steady state serum concentrations,
dict dosing based on serum concentration data obtained
the rate of elimination must equal the rate of adminis
from a patient. The use of an individual's serum con
tration. By use of steady state serum concentrations a
centration data allows better prediction of dosage by
dosing rate may be predicted. (More on dosing estima
taking into account m a n y factors that m a y alter drug
tion will be discussed in part II of this article.) 2
pharmacokinetics.
A flow-type model assumes that a fraction of the drug
in the body will be extracted from the blood on each
pass through the eliminating organ and that blood flow
References
1. Gibaldi M. Biopharmaceutics and clinical pharmacokinetics.
2nd ed. Philadelphia: Lea and Febiger, 1977: vii.
2. Burton ME, Brater DC, Vasko MR. Comparison of drug dos
ing methods. Clin Pharmacokinet 1985:10:1-37.
3. Barr WH. Principles of biopharmaceutics. Am ] Pharmaceut
Ed 1968;52:958-81.
^ Peripheral 4. Riegelman S, Rowland M. Effect of route of administration on
Distribution drug disposition. / Pharmacokinet Biopharm 1973;1:419-34.
Compartment
5. Rowland M, Tozer TN. Clinical pharmacokinetics: concepts
and applications. Philadelphia: Lea and Febiger, 1980:16-33, 34-47.
6. Welling PG. Effects of gastrointestinal disease on drug absorp
tion. In: Benet LZ., Massoud N, Gambertoglio JG, eds. Pharmacoki
netic basis for drug treatment. New York: Raven Press, 1984:29-47.
7. Niazi S. Textbook of biopharmaceutics and clinical pharmacoki
netics. New York: Appleton-Century-Crofts, 1979:41-73.
8. Gibaldi M, Perrier D. Pharmacokinetics. New York: Marcel
Dekker, 1982:1-44, 145-98.
9. Metzler CM. Bioavailability—a problem in equivalence. Bio
metrics 1974;30:309-17.
10. Benet LZ. Effect of route of administration and distribution on
1 I I 1
I I I I I I I I I I I I I I drug action. / Pharmacokinet Biopharm 1978;6:559-85.
0 1 2 3 -, 5 6 7 8 9 10 11 12 13 14 15 11. Thompson PD, Melmon KL, Richardson JA, et al. Lidocaine
pharmacokinetics in advanced heart failure, liver disease, and renal
Time (hours) failure in humans. Ann Intern Med 1973;78:499-508.
Figure 6. A plot of serum concentrations vs. time following an instantaneous 12. Wilkinson GR, Shand DG. A physiological approach to hepatic
intravenous dose for a drug that fits a two-compartment model. The compartments drug clearance. Clin Pharmacol Ther 1975;28:377-90.
include a central compartment representing the blood volume and a peripheral
compartment representing the tissue. Elimination occurs from the central com
13. Benet LZ. Pharmacokinetic parameters: which are necessary
partment. The effects upon a serum concentration distribution are represented to define a drug substance? Eur ] Respir Dis 1984;65(suppl 134):45-61.
_ < ,
by the term Α β ' and the effects of elimination on a serum concentration by the 14. Mayer SE, Melmon KL, Gilman AG. Introduction: the
term Be~*. The term a represents a distribution rate constant and β represents
an elimination rate constant. From the equation C, = Ae + Be - , a serum con _ Λ dynamics of drug absorption, distribution, and elimination. In: Gil
centration can be determined at any time (t). The clinical utility of a two- man AG, Goodman LS, Gilman A, eds. The pharmacological basis
compartment model is limited to a computer because of mathematical complexity. of therapeutics. 6th ed. New York: Macmillan, 1980:1-27.
journal of Pharmacy Technology Mar/Apr 1986 73
You might also like
- Pharmaco KineticsDocument427 pagesPharmaco KineticsMehrdad AvestaNo ratings yet
- Biopharmaceutics - BrahmankarDocument414 pagesBiopharmaceutics - Brahmankarmatin586% (58)
- Post Anesthesia-Recovery Skills ChecklistDocument6 pagesPost Anesthesia-Recovery Skills Checklistnorthweststaffing100% (1)
- Case ConferenceDocument30 pagesCase Conferenceridazaheer29No ratings yet
- Brahmakar - Biopharmaceutics & PharmacokineticsDocument374 pagesBrahmakar - Biopharmaceutics & PharmacokineticsSamritiNo ratings yet
- Pharmacokinetics by Hanna AbrahamDocument27 pagesPharmacokinetics by Hanna AbrahamRom EonNo ratings yet
- BioPharm Midterms ReviewerDocument26 pagesBioPharm Midterms ReviewerCHARLES RONALD GENATONo ratings yet
- BIOPHARMACEUTICSDocument132 pagesBIOPHARMACEUTICSTahaniNo ratings yet
- Biopharmaceutics Note 7th SemDocument38 pagesBiopharmaceutics Note 7th Semmj.vinoth@gmail.comNo ratings yet
- What The Body Does To A Drug: PharmacokineticsDocument14 pagesWhat The Body Does To A Drug: PharmacokineticsSabrina JonesNo ratings yet
- Topic 1 - Introduction Tophysical Pharmacy and Principles of Biopharmaceutics I. Physical PharmacyDocument13 pagesTopic 1 - Introduction Tophysical Pharmacy and Principles of Biopharmaceutics I. Physical PharmacyAi LoveeiNo ratings yet
- Biopharmaceutics - 1 2022Document24 pagesBiopharmaceutics - 1 2022Varshini VarshaNo ratings yet
- Biopharmaceutics: GSDMSFI - BS Pharmacy 3Document11 pagesBiopharmaceutics: GSDMSFI - BS Pharmacy 3Majeddah Aliudin TalambunganNo ratings yet
- Introduction To Biopharmaceutics and PharmacokineticsDocument3 pagesIntroduction To Biopharmaceutics and PharmacokineticsSyeda Eshaal JavaidNo ratings yet
- BiokimmDocument42 pagesBiokimmAdeliaNo ratings yet
- Pharmacology Prelims ReviewerDocument21 pagesPharmacology Prelims ReviewerAntonette Africa MercadoNo ratings yet
- Drug Delivery On Rectal Absorption: Suppositories: Review ArticleDocument7 pagesDrug Delivery On Rectal Absorption: Suppositories: Review ArticleNindah IkaNo ratings yet
- Pharmacokinetics 1: AbsorptionDocument15 pagesPharmacokinetics 1: AbsorptionCecilia GrayebNo ratings yet
- Pharmacology - Pharmacology en PDFDocument386 pagesPharmacology - Pharmacology en PDFMaksym DemianchukNo ratings yet
- Document 2Document9 pagesDocument 2zoha fatimaNo ratings yet
- Pilapil PharmacologyDocument6 pagesPilapil PharmacologyIza FaboresNo ratings yet
- Chapter 1Document32 pagesChapter 1Czerwin JualesNo ratings yet
- NSG 105 Module 3Document22 pagesNSG 105 Module 3Alaminah MULOKNo ratings yet
- Ocular Pharmacology 2Document10 pagesOcular Pharmacology 2cornelia cindy SRDNo ratings yet
- Unit #1 IntroductionDocument22 pagesUnit #1 IntroductionSaima VictorNo ratings yet
- Basics of Biopharmaceutics: A Mini Review: Bioequivalence & Bioavailability International JournalDocument5 pagesBasics of Biopharmaceutics: A Mini Review: Bioequivalence & Bioavailability International JournalLina WinartiNo ratings yet
- Introduction To Pharmacology Part 2Document10 pagesIntroduction To Pharmacology Part 2jason fiasonNo ratings yet
- Unit One of PharmacologyDocument63 pagesUnit One of PharmacologyAbdinaasir MohamedNo ratings yet
- Cclec Drug MonitoringDocument14 pagesCclec Drug MonitoringAndrea Gail GutierrezNo ratings yet
- Unit #1 IntroductionDocument22 pagesUnit #1 IntroductionSaima VictorNo ratings yet
- Pharmacokinetic and Pharmacodynamic2021Document12 pagesPharmacokinetic and Pharmacodynamic2021STEFANIA AYA DIAZNo ratings yet
- Pharma Chapter 2_modDocument57 pagesPharma Chapter 2_modAlex CheungNo ratings yet
- EXERCISE#2Document5 pagesEXERCISE#2Ana GarciaNo ratings yet
- 4-Pharmacokinetics IDocument88 pages4-Pharmacokinetics IMarc Imhotep Cray, M.D.No ratings yet
- Pharmacokinetics: The Absorption, Distribution, and Excretion of DrugsDocument14 pagesPharmacokinetics: The Absorption, Distribution, and Excretion of DrugsAriiNo ratings yet
- Handbk of Basic Pharmacokinetics Chap. 2Document3 pagesHandbk of Basic Pharmacokinetics Chap. 2MoonGalaxyNo ratings yet
- Pharmacology Unit 1Document58 pagesPharmacology Unit 1Asif Ali LashariNo ratings yet
- Introduction To BiopharmaceuticsDocument27 pagesIntroduction To BiopharmaceuticsAmina Akther Mim 1821179649No ratings yet
- Biopharmaceutics BrahmankarDocument413 pagesBiopharmaceutics BrahmankarsrivathsavapNo ratings yet
- Ladmer SystemDocument26 pagesLadmer SystemAbdul Mannan80% (5)
- Pharmacokinetics PDFDocument14 pagesPharmacokinetics PDFLea PesiganNo ratings yet
- Pharmacology: B.Pharm, 2011, M.Pharm, 2016Document19 pagesPharmacology: B.Pharm, 2011, M.Pharm, 2016علي عبد اللطيفNo ratings yet
- Unit#1principle of PharmacologyDocument58 pagesUnit#1principle of PharmacologySaima VictorNo ratings yet
- تصميم كويزDocument73 pagesتصميم كويزHemo HindiNo ratings yet
- 01.25.01 Principles of Pharmacokinetics - Absorption and DistributionDocument10 pages01.25.01 Principles of Pharmacokinetics - Absorption and DistributionMikmik DGNo ratings yet
- Pharmacokinetic Lecture NotesDocument45 pagesPharmacokinetic Lecture NotesAmy Wu0% (1)
- Morgan 140 149Document10 pagesMorgan 140 149Marta DumitracheNo ratings yet
- Overview of Factors Affecting Oral Drug AbsorptionDocument11 pagesOverview of Factors Affecting Oral Drug Absorptionmahveen balochNo ratings yet
- Physical Pharmacy ReviewerDocument23 pagesPhysical Pharmacy ReviewerChrister Jon AcostaNo ratings yet
- Makalah KBM Kel 3Document32 pagesMakalah KBM Kel 3Novia RozadiNo ratings yet
- College of Pharmacy Biopharmaceutics and Pharmacokinetics Assignment No. 1Document6 pagesCollege of Pharmacy Biopharmaceutics and Pharmacokinetics Assignment No. 1ERIKA JADE TORRESNo ratings yet
- Biopharmaceutics and PharmacokineticDocument4 pagesBiopharmaceutics and PharmacokineticRiyaz AliNo ratings yet
- 2.principles of Pharmacokinetics Pharmacodynamic SlidesDocument13 pages2.principles of Pharmacokinetics Pharmacodynamic Slidesran8384080No ratings yet
- Drug Absorption-DistributionDocument60 pagesDrug Absorption-DistributionRuqayya AdamuNo ratings yet
- Learning Packet in Level 1-NCM 106 NURSING PHARMACOLOGY: College of Nursing School Year 2020-2021Document15 pagesLearning Packet in Level 1-NCM 106 NURSING PHARMACOLOGY: College of Nursing School Year 2020-2021Nur Sanaani100% (1)
- Share Pharmacology Book 1Document101 pagesShare Pharmacology Book 1Jmcle AhmedNo ratings yet
- Pharmacology- The Molecular Dance: Understanding Drug Interactions: Harmony and Chaos: The Symphony of Drug InteractionsFrom EverandPharmacology- The Molecular Dance: Understanding Drug Interactions: Harmony and Chaos: The Symphony of Drug InteractionsNo ratings yet
- Handbook of Drug Interaction and the Mechanism of InteractionFrom EverandHandbook of Drug Interaction and the Mechanism of InteractionRating: 1 out of 5 stars1/5 (1)
- Translational ADMET for Drug Therapy: Principles, Methods, and Pharmaceutical ApplicationsFrom EverandTranslational ADMET for Drug Therapy: Principles, Methods, and Pharmaceutical ApplicationsRating: 1 out of 5 stars1/5 (1)
- Border MoldingDocument39 pagesBorder MoldingRachelAngelaGabrielGalsimNo ratings yet
- GUY Et Al 1994 - Regulation of Colostrum Formation in Beef and Dairy CowsDocument6 pagesGUY Et Al 1994 - Regulation of Colostrum Formation in Beef and Dairy CowsMonique IndNo ratings yet
- Megaloblastic AnaemiaDocument11 pagesMegaloblastic AnaemiaJesmin_36No ratings yet
- PRI Breathing TechniquesDocument4 pagesPRI Breathing Techniqueskrserre5934100% (2)
- Basic Embryology Series-1-1Document229 pagesBasic Embryology Series-1-1davidbenedict870No ratings yet
- Bpoc Si Comorbiditati: Dr. Ursarescu Bianca Medic Rezident Pneumologie An IIIDocument35 pagesBpoc Si Comorbiditati: Dr. Ursarescu Bianca Medic Rezident Pneumologie An IIIBabii Alin Adrian100% (1)
- Grand Case PresentationDocument50 pagesGrand Case PresentationJean Michelle100% (1)
- Raven Biology of Plants: Eighth EditionDocument43 pagesRaven Biology of Plants: Eighth EditionMoath EnnabNo ratings yet
- RPI System Krol 1973 JPDDocument19 pagesRPI System Krol 1973 JPDMahadevan Ravichandran100% (1)
- Semi-Detailed Lesson Plan Multi Grade Grade 4&5 Lesson PlanDocument6 pagesSemi-Detailed Lesson Plan Multi Grade Grade 4&5 Lesson Plandianie joyNo ratings yet
- Skinny Helpers Cheat SheetDocument12 pagesSkinny Helpers Cheat SheetJennifer AllenNo ratings yet
- Neuropsychology 2O23Document8 pagesNeuropsychology 2O23farhaanah.abdullah02No ratings yet
- National Hal PG RopsDocument32 pagesNational Hal PG RopsRade NovakovicNo ratings yet
- Chapter 2. The Biological PerspectiveDocument40 pagesChapter 2. The Biological Perspectiveberk.turbil1457No ratings yet
- Nephron ColoringDocument3 pagesNephron ColoringkishoreddiNo ratings yet
- Snell's Clinical Neuroanatomy Chapter PonsDocument6 pagesSnell's Clinical Neuroanatomy Chapter PonstsidazizyNo ratings yet
- Cephalosomatic LinkageDocument8 pagesCephalosomatic LinkageBrijeshNo ratings yet
- AcsDocument103 pagesAcsVikrant WankhedeNo ratings yet
- Mutant Formation PDFDocument5 pagesMutant Formation PDFMohan BalajiNo ratings yet
- Drug Study Final 1Document47 pagesDrug Study Final 1Nik2No ratings yet
- Science Exam Part I. Write The Parts of The Excretory System. (4 Points)Document5 pagesScience Exam Part I. Write The Parts of The Excretory System. (4 Points)Siria PinedaNo ratings yet
- New Scientist Essential Guide - No7 - The Human BrainDocument100 pagesNew Scientist Essential Guide - No7 - The Human BrainHieu Trinh100% (4)
- Aqa Y2 P2 Jun 19 MSDocument19 pagesAqa Y2 P2 Jun 19 MSestee.onyeNo ratings yet
- BC-2600 - Service Training - V2.0 - ENDocument157 pagesBC-2600 - Service Training - V2.0 - ENsandeep ntNo ratings yet
- Abdominal Aortic AneurysmDocument23 pagesAbdominal Aortic AneurysmHani AbulkhairNo ratings yet
- Bryant and Monie 2012Document10 pagesBryant and Monie 2012Le Uyen NguyenNo ratings yet
- Retic MethodDocument18 pagesRetic MethodFaty DearNo ratings yet
- GP MCQ 11Document4 pagesGP MCQ 11Marta MoreiraNo ratings yet