Professional Documents
Culture Documents
Abscess, Cyst & Haematoma
Abscess, Cyst & Haematoma
Uploaded by
Aqsa Zahoor Ahmad Nadeem0 ratings0% found this document useful (0 votes)
23 views36 pages1. An abscess is a localized collection of pus caused by bacterial infection, while a cyst is a sac containing fluid or semi-solid material. A hematoma is a collection of blood under the skin caused by damaged blood vessels.
2. Abscesses are treated through maturation and drainage - draining pus and removing debris. Cysts are drained by puncturing and injecting iodine to destroy the membrane. Hematomas are drained by removing blood and ligating bleeders.
3. Differentiation is based on aspirated contents - pus for abscesses, fluid for cysts, blood for acute hematomas and serum for chronic hematomas. History and physical exam also help determine
Original Description:
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Document1. An abscess is a localized collection of pus caused by bacterial infection, while a cyst is a sac containing fluid or semi-solid material. A hematoma is a collection of blood under the skin caused by damaged blood vessels.
2. Abscesses are treated through maturation and drainage - draining pus and removing debris. Cysts are drained by puncturing and injecting iodine to destroy the membrane. Hematomas are drained by removing blood and ligating bleeders.
3. Differentiation is based on aspirated contents - pus for abscesses, fluid for cysts, blood for acute hematomas and serum for chronic hematomas. History and physical exam also help determine
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
0 ratings0% found this document useful (0 votes)
23 views36 pagesAbscess, Cyst & Haematoma
Abscess, Cyst & Haematoma
Uploaded by
Aqsa Zahoor Ahmad Nadeem1. An abscess is a localized collection of pus caused by bacterial infection, while a cyst is a sac containing fluid or semi-solid material. A hematoma is a collection of blood under the skin caused by damaged blood vessels.
2. Abscesses are treated through maturation and drainage - draining pus and removing debris. Cysts are drained by puncturing and injecting iodine to destroy the membrane. Hematomas are drained by removing blood and ligating bleeders.
3. Differentiation is based on aspirated contents - pus for abscesses, fluid for cysts, blood for acute hematomas and serum for chronic hematomas. History and physical exam also help determine
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
You are on page 1of 36
Abscess, Cyst & haematoma
Dr. Abdul Mateen
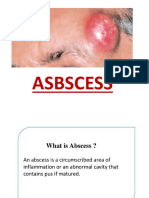
Abscess
• It is circumscribed area of inflammation which
is invaded by pus forming organisms or it is
localized collection of pus surrounded by
inflamed or pyogenic membrane. Size of the
abcess is variable from few mm to foot ball
size.
• Classification: basis of cardinal sign of
inflammation there are 2 types of abcess
• Acute and Chronic
• Both may be superficial or deep.
• Etiology: Pyogenic organisms; Irritant drugs,
Orgnsms Like staph., srept., corynebacterium
pyogenes, E coli,Helminthes; FungusProtozoa.
Irritantdrugs:Oilbase;drugs,e.goxytetracycline,
chloral hydrate or Mg sulfate etc these are not
given I/M or S/C always give these medicine
I/V.Then foreign bodies can be cause which
could be endogenous and exogenous bodies.
Continue…
Endogenous are the substances which are produced by own
body i.e bone, dead tissue
Exogenous are outside body which enter through any accident
e.g piece of wood
Acute superficial abscess:
• Appear within 3-5 days after entry of microbe. Appear as
small pockets underneath the skin. Then with the passage of
time these small pockets are converted into big pocket due to
necrosis of inflammatory membrane. Then pus move upward
and put pressure on the weak tissue making pointing of
abscess.
Continue…
• Acute deep abscess: Abscess develops in deeper tissue e.g
muscle which is not visible. The superficial area feels tense
and painful. No visible signs are seen apparently unless it
becomes superficial. Sometimes it burst in deeper tissue.
Sometimes abscess burst in other cavities and if pus reach to
the blood it may lead to pyemia or toxemia. If abscess is well
diagnosed by a surgeon in time drainage may be applied
surgically.
• Septic emboli may be carried to other parts of the body
producing abscess, pyemia and septicemia
• Chronic superficial abscess:
• In this type abcess is present but no cardinal signs it looks like
tumor due to fibrous tissue. Chronic abcess is not watery in
nature. It may be in the form of curdles, may be calcified or
inspissated (To undergo thickening ).
• Chronic deep abscess:
• Hard fibrous mass is present in deep tissue. Here surgery is
recommended.
• International treatment of abscess:
• Maturation .Drainage
• Maturation:
First of all mature the abcess by using irritant drugs or
naturally. Irritants only assist the natural maturity of the
abcess.
• Drainage:
Make incision for drainage and incision is always given
towards the gravity. If football like abcess is present on neck
here we do setoning for 5-6 days to maintain the patency (The
quality of being open, expanded, or unblocked) of abcess.
Ideal dressing material for abcess is MgSO4 because it has
lymph lavage action so it will absorb water.
• Case:
If acute abcess is at the neck site then we will
wait for some days for its maturation. We
apply counter irritant on the abcess site. After
maturation drainage is done by puncturing.
• Diagnosis:
Physical examination
Puncturing (aspiration)
• Physical examination:
• Soft at center and harder at periphery. When it matures it starts
fluctuation from periphery to centrei.e soft at all site.
• Puncturing:
• Use 16 Guage needle which is inserted right in the centre of abcess. Then
pus will come out.
• Confuse with abcess:
• Hematoma
• Cyst
• Tumors
• Bursitis
• Hernia
• Fibroma/granuloma
• Hematoma: Blood comes out after puncturing. In this case there is
accumulation of blood underneath the skin after rupturing of vessel. So in
acute form blood come out and in chronic form serum come out.
• Cyst:If watery fluid comes out then it is cyst. And you never see sign of
inflammation in it.
• Tumor:Always hard and after puncturing nothing comes out may be some
granular tissue come out but very rare.
• Bursitis: It is inflammation of bursa (it is space between two tendons, or
between tendon and muscle or between tendon and bone). It is always
close to the proximal or distal extremity of bone. In this case swelling
involving all signs of inflammation but nothing comes out after puncturing
but sometime serum come out.
Treatment
In acute mature abscess
• Hasten the maturation abscess by application
of counter irritant
• Like iodine ointment 5%
• In certain cases its advisable to open the
abscess as soon as its diagnose
Treatment
• The skin over the abscess should be clipped and
sheared and antiseptic application is done.
• An opening is made at the most dependant part of
the swelling which is fluctuating and its better in the
ventral part of the swelling to provide complete
drainage of the abscess cavity.
• After the pus is removed the cavity should be
checked for any F.B and necrotic T. should be
removed
• Then although flashing of the cavity should be made
by suitable antiseptic like 10% povidone iodine or 1%
chlorhexidene
Continue…
• Then the abscess cavity should be packed
completely with gauze saturated with ten.
Iodine 5%
• This ten. Iodine gauze help in destruction of
the lining membrane of abscess cavity and
reduce the number of microrganisms
• The gauze is removed in 24h and then the
cavity again flashed with mild antiseptic
solution
Cyst
• A sac containing liquid
and semi-solid substance
• It has an inner lining of
secretary membrane
• May contains a solid
substances like tooth and
hair
Types
• Retention cyst- due to
occlusion of duct or gland
e.g. salivary cyst
• Exudation cysts- due to
accumulation of fluid in existing
cavity e.g hydrocele
• Congenital cysts- present of at
birth due to failure of embryonic
cavity to close e.g urachal cyst
• Cyst due to misplaced
embryonic tissue e.g dermoid
cyst and dentigerous cyst
Diagnosis
• Cysts are non-
inflammatory and
develop slowly
• Fluid fluctuates in the cyst
• If contents are semi- solid
it fluctuate en masse
• May be differentiated
from abscess, swelling,
haematoma
Treatment
• Puncturing of cyst and evacuation of contents
• Tr. Iodine is injected to destroy the membrane
• Cyst may be incised to get the contents
evacuated
• Passing of seton
• Dentigerous cyst of temporal bone
• Tooth is extracted and sinus tract is cauterized
• Branchial cyst (honey cyst)
• Complete excision of the cyst
Contusion
• Deep wound in which skin remains intact. It is
very serious and involve:
• Muscle
• Blood vessels
• Nerves
• Bone
• Types:
• 1st degree contusion (ecchymosis)
• 2nd degree contusion (hematoma)
• 3rd degree contusion (gangrene)
1st degree contusion (ecchymosis):
• It is very mild type which is characterized by pin point
hemorrhages on skin and these hemorrhages are more
prominent in non pigmented area of body.
• Etiology: Blunt object, Compression of hard object, By
constant pressure
• Clinical signs:
• Pin point hemorrhages, Mild inflammation, slight pain
• Treatment:
• Auto recovery
• Apply all methods of acute inflammation
• Pain killer drugs (steroids, NSAID or non steroidal)
2nd degree contusion (hematoma):
• It is the accumulation of blood under beneath the
skin due to damage to major vassals. So blood
comes out and accumulates and looks like tumor,
abscess and appear as visible bulge. The
examples are swelling of on the caudal side of
horse, udder of the female, neck of the horse and
area where vassals are very superficial. Always
fluctuate uniformly and u will see movements of
fluid from one side to other. It has all the 4 signs
of acute inflammation.
Haematoma
• Diagnosis
• History (fight, automobiles, hit by blunt object)
• Physical examination (signs of inflammation)
• Differencial diagnosis that confuses with
• 1: Abscess 2: Tumor 3: Cyst 4: Bursitis
5: Herniation
• Aspiration test. Aspiration needle used to check the
acute or chronic hematoma. If by puncturing blood
come out it means acute hematoma. In chronic
haematoma case serum comes out after aspiration by
needle.
2nd degree contusion (hematoma):
• Accumulation of extravasated blood (the leakage of blood
from a vessel into tissues surrounding. There are two types
of hematoma: Acute and Chronic hematoma
• Acute and chronic hematoma:
• Acute is Fresh or recent case which has all cardinal signs of
inflammation. When blood is oozing out from artery. If
acute form is not treated then it is converted into chronic
after the passage of time. A crepitus (friction rub sound)
sound is there. If chronic stage persist for a long period of
time the serum is reabsorbed and clot remain there. If this
stage is contaminated by micro organisms then it leads to
abcess formation.
Treatment of acute hematoma:
• Two things are very important
• If the size of the hematoma continuously increasing and history
reveals that it is a recent case so it is acute heamatoma which
will indicate that damaged vessel is still bleeding we will never
open it and wait for 4-5 days with hydrotherapy untill bleeding
stops vassel heals and it is converted into chronic .
• If acute heamatoma is opened it may lead to hypovolemic shock
because of decrease in blood.
• If the size of the hematoma is constant and it is old case , we
open the area (long elliptical incision) remove blood, and main
bleeder is identified and ligated to stop the hemorrhage. In this
case hematoma is not sutured because we want drainage.
Treatment of chronic hematoma:
• first of all long incision is given and serum and clot is removed.
Sometime irrigation of hematoma is done for the proper drainage
purpose.
• If size of hematoma is 14 inch then never make long incision. On
buttock the size of the hematoma may reach upto 12 inch. In such
cases give two incisions one on proximal side and one distal side
then clear the wound with water.
• In big size hematoma setoning is done by giving two incisions for
proper drainage.
• Organs prone to chronic hematoma:
• Base of neck, Shoulder region, Buttock, Abdomen cranial to udder
and sheath, Caudal epigastric vein
Gangrene
• 3rd degree contusion (gangrene):
• Gangrene is the death of tissue in part of the body. It is
very severe type and blood vessels, muscles and nerves
damage and no life is there. Pinch the area to check
the response. It can also be checked by..
• Hammering the part
• Pinch the area by hand or traumatic object.
• Signs:
Dark red area
Black discoloration
No evidence of pain
Treatment:
Treatment:
• There are two methods
• If there is little bit response i.e 5% then we go for
treatment. If the area below knee is cold then we
do following procedures:
• Vigorous massage of area to ensure blood supply
• Flexion and extension
• Counter irritant drug is applied which induce:
• Blister
Treatment:
• Rubifaciant (A rubefacient is a substance for external
application that produces redness of the skin)These are
moderate type of counter irritant.
• If the part is not responding then amputation (remove
the part) is done. If for example in case of buffalo the
last two vertebra are damaged at tail region then we
remove the last two vertebra because the infected part
is source of infection and saprophytic bacteria
(clostridium) are present and lead to toxicity of blood
by reaching to blood. If in this case the infection reach
up to spinal cord then there is no treatment.
Auricular hematoma:
• An aural (ear) haematoma is a collection of blood or serum, and
sometimes a blood clot within the pinna or ear flap and ear flap become
thickened. The swelling may involve the entire ear flap or it may involve
only a small area.
• Dropping of ear
• Tilting of head
• Pain, discomfort and depression
• The first aim of treatment is to drain the haematoma to relieve the
pressure and pain associated with the build up of fluid within the ear flap.
This is achieved under general anesthesia where either a single incision or
multiple small biopsy holes are made on the inner surface of the ear. The
blood is drained and the ear flushed to remove any remaining blood clots.
These holes are left open to allow continued drainage of fluid whilst
waiting for the ear flap to heal.
• Reattachment of the ear cartilage is encouraged with the
use of multiple sutures placed through the ear flap (with or
without the use of a support to maintain the normal
architecture of the ear) and these sutures are left in place
for 3 weeks. The specific method used will depend on the
size, age and position of the haematoma.
Treatment:
• Any reason that causes the dog to shake its head can result
in the formation of an aural haematoma sh be treated first.
• Apply pressure (if hematoma is 1-2 mm)
• Drainage (aspiration is done by insulin syringe)
• Giving “S” shape incision
• Giving “+” shape incision
• Small and S-shape incision: mattress sutures are
applied in small incisions and knots are always
place on the outer side of ear. The inner side skin
of ear is very thin and it can cause infection on
that side that’s why we apply knots on outer side.
• In case of S-shape incision it has edge on elliptical
incision because in case of linear incision we can’t
expose more area while in case of S-shape
incision we can expose more area of infection.
• “+” shape incision (cruciate incision):
we never apply suture at this type of incision.
Here we apply undermining (separation of
skin from under lying tissue). Now apply gauze
and bandage. Here healing is done by 2nd
intension as an open wound.
WHAT HAPPENS IF YOUR DOG DOES
NOT HAVE SURGERY?
• If a haematoma is left untreated the blood in
the ear flap will separate into serum and a clot
and will gradually be absorbed over a period
of 10 days to 6 weeks. This is an
uncomfortable time for your dog and
unfortunately some scarring will take place
during this process. It also causes a deformity
of the ear flap resulting in a "cauliflower ear"
which may cause further problems.
You might also like
- b53 07 Akash MudraDocument3 pagesb53 07 Akash Mudrashadowfalcon03No ratings yet
- Janez Rebol - Otoscopy Findings-Springer (2022)Document193 pagesJanez Rebol - Otoscopy Findings-Springer (2022)Thanh Long TrầnNo ratings yet
- Clinical Examination in Surgery PDFDocument40 pagesClinical Examination in Surgery PDFshanyiar100% (4)
- Lumps N BumpsDocument54 pagesLumps N BumpsAnis100% (1)
- Science 5 Sound Sample TestDocument2 pagesScience 5 Sound Sample TestNemie Christian Homer Custodio100% (2)
- Cerumen ImpactionDocument3 pagesCerumen ImpactionAira Alaro0% (1)
- Dr. Bruce Fogle - DogsDocument344 pagesDr. Bruce Fogle - DogsZana Maric67% (3)
- Ulcer: DR - Sunil Kumar Asst - Professor Dept - of Gen - Surgery MNR Medical College Sangareddy 01-05-2019Document83 pagesUlcer: DR - Sunil Kumar Asst - Professor Dept - of Gen - Surgery MNR Medical College Sangareddy 01-05-2019Aashmi ChandrikaaNo ratings yet
- BCM 229 Wounds and UlcersDocument20 pagesBCM 229 Wounds and UlcersTechnoveNo ratings yet
- UlcerDocument135 pagesUlcerMahir RathodNo ratings yet
- Wound PDFDocument70 pagesWound PDFIin MailoaNo ratings yet
- UlcersDocument42 pagesUlcersinfinitymedical08No ratings yet
- ABSCESSDocument35 pagesABSCESSlax prajapatiNo ratings yet
- Bartholin Gland Duct CystDocument16 pagesBartholin Gland Duct Cystsintia djafarNo ratings yet
- Skin UlcerDocument72 pagesSkin Ulcersahsweta67No ratings yet
- Hemorrhoids: Ginesha Hafidzy GarishahDocument35 pagesHemorrhoids: Ginesha Hafidzy GarishahrizqinadiaNo ratings yet
- Study Guide OstomyDocument6 pagesStudy Guide OstomyKennard Aristo ArifinNo ratings yet
- 09 Surgical Asepsis & Wound CareDocument44 pages09 Surgical Asepsis & Wound CareBobet ReñaNo ratings yet
- Incision and DrainageDocument33 pagesIncision and DrainagemathisyncNo ratings yet
- Wound HealingDocument47 pagesWound HealingdenekeNo ratings yet
- VagishaDocument60 pagesVagishavanshikaNo ratings yet
- Medical Themed PPTDocument32 pagesMedical Themed PPTRandom VibesNo ratings yet
- AbscessDocument3 pagesAbscessSandeep SinghNo ratings yet
- WoundDocument31 pagesWoundEnos ErastusNo ratings yet
- Wound Classification and Its Management: Presented By: Dr. Dhiren B. BhoiDocument48 pagesWound Classification and Its Management: Presented By: Dr. Dhiren B. BhoiBenita Janet AppajiNo ratings yet
- CIRCULATORY SYSTEM HAEMORRHAGE and Bleeding AutosavedDocument37 pagesCIRCULATORY SYSTEM HAEMORRHAGE and Bleeding AutosavedGerald Limo Arap ChebiiNo ratings yet
- Arterio-Venous Fistula: DR Bilal Ahmed TR Fcps UrologyDocument79 pagesArterio-Venous Fistula: DR Bilal Ahmed TR Fcps UrologyD M Shawkot HossainNo ratings yet
- Wounds and BleedingDocument22 pagesWounds and BleedingClark LlameraNo ratings yet
- Abscess 2Document4 pagesAbscess 2SANDEEP SINGHNo ratings yet
- Wounds and Wound Healing: DR Jithin MDocument73 pagesWounds and Wound Healing: DR Jithin Mshruthy rakeshNo ratings yet
- Wound Healing & BurnsDocument232 pagesWound Healing & BurnsdillaNo ratings yet
- Wound Care IntroductionDocument4 pagesWound Care IntroductionNikki Ann Kanapi FernandezNo ratings yet
- Sinus and FistulaDocument3 pagesSinus and FistulaAndrew BonusNo ratings yet
- Hemorrhoids and Anal ProblemsDocument64 pagesHemorrhoids and Anal ProblemsAhmed Noureldin Ahmed100% (4)
- Wound Healing and Its DisordersDocument39 pagesWound Healing and Its Disordersmahdi aljamalNo ratings yet
- Benign Gynecologic LesionsDocument103 pagesBenign Gynecologic Lesions201286% (7)
- Scrotal Swellings: Dr. A. D. IkobhoDocument65 pagesScrotal Swellings: Dr. A. D. IkobhoPrincewill SeiyefaNo ratings yet
- Anorectal DisorderDocument41 pagesAnorectal DisorderMuhammad100% (1)
- Examination of Lumps and BumpsDocument47 pagesExamination of Lumps and Bumpszoya shaikhNo ratings yet
- Surgical Incisions, Wound and Wound Closure-1Document78 pagesSurgical Incisions, Wound and Wound Closure-1Iwasokun GabrielNo ratings yet
- Introduction To First AidDocument61 pagesIntroduction To First AidLim Jun BinNo ratings yet
- Dry StationDocument3 pagesDry StationTala ArarNo ratings yet
- This Is The Blood and Guts of First Response, The Most Important Thing You Will DoDocument112 pagesThis Is The Blood and Guts of First Response, The Most Important Thing You Will DoEil AzNo ratings yet
- HemorrhoidectomyDocument5 pagesHemorrhoidectomydrnareshkumar3281100% (1)
- Wound Healing: Dr. Shaimaa Alaraby Specialist of General SurgeryDocument21 pagesWound Healing: Dr. Shaimaa Alaraby Specialist of General SurgeryOsama Fadel ahmedNo ratings yet
- First AidDocument61 pagesFirst AidShajin NNo ratings yet
- Hemorrhoids 1Document19 pagesHemorrhoids 1susulemani3No ratings yet
- Hydatidcyst 180609173228 PDFDocument60 pagesHydatidcyst 180609173228 PDFKarem MaaliNo ratings yet
- Primary Oral UlcerationDocument41 pagesPrimary Oral Ulcerationاحمد العزكيNo ratings yet
- HemerroidDocument24 pagesHemerroidVina WineNo ratings yet
- Sinus, FistulaDocument46 pagesSinus, Fistulaalia0% (1)
- Elearning Surgery 1Document100 pagesElearning Surgery 1daniyfondoNo ratings yet
- Mon Surgical Infections Boils, Abscess, Ulcer, Cellulitis, Curbuncle, Gangrene, Sinus, Fistula CDocument48 pagesMon Surgical Infections Boils, Abscess, Ulcer, Cellulitis, Curbuncle, Gangrene, Sinus, Fistula CPanna SahaNo ratings yet
- Preseptor: Hj. Liza Nursanty, DR., Sp. B., M. Kes., FinacsDocument30 pagesPreseptor: Hj. Liza Nursanty, DR., Sp. B., M. Kes., FinacsRosa NurkholidNo ratings yet
- ParasiticDocument106 pagesParasitichelloaNo ratings yet
- Ovarian Cyst As GroupDocument54 pagesOvarian Cyst As GroupZaynab Abdul WahidNo ratings yet
- Skin Integrity and Wound CareDocument47 pagesSkin Integrity and Wound CareCHALIE MEQUNo ratings yet
- AbscessDocument16 pagesAbscessPlày GameNo ratings yet
- Testicular SwellingDocument66 pagesTesticular SwellingbrnardNo ratings yet
- Bed Sore 48Document45 pagesBed Sore 48Sedaka DonaldsonNo ratings yet
- 03 Anal & Perianal DisordersDocument56 pages03 Anal & Perianal DisordersHafizah HoshniNo ratings yet
- Wounds and Their ManagementDocument26 pagesWounds and Their ManagementABBAM ABRAHAMNo ratings yet
- A Simple Guide to Blood in Stools, Related Diseases and Use in Disease DiagnosisFrom EverandA Simple Guide to Blood in Stools, Related Diseases and Use in Disease DiagnosisRating: 3 out of 5 stars3/5 (1)
- Castration of Large AnimalsDocument17 pagesCastration of Large AnimalsAqsa Zahoor Ahmad NadeemNo ratings yet
- Meat Inspection For Wholesomeness The MeatDocument5 pagesMeat Inspection For Wholesomeness The MeatAqsa Zahoor Ahmad NadeemNo ratings yet
- Nephrectomy & Nephrotomy: Dr. Abdul MateenDocument19 pagesNephrectomy & Nephrotomy: Dr. Abdul MateenAqsa Zahoor Ahmad NadeemNo ratings yet
- Lameness in Bovines: Dr. Abdul MateenDocument37 pagesLameness in Bovines: Dr. Abdul MateenAqsa Zahoor Ahmad NadeemNo ratings yet
- Practical7236 208Document48 pagesPractical7236 208Aqsa Zahoor Ahmad NadeemNo ratings yet
- IV Catheter PlacementDocument10 pagesIV Catheter PlacementAqsa Zahoor Ahmad NadeemNo ratings yet
- Topic: Surgical Problems of Respiratory System: DR Abdul MateenDocument24 pagesTopic: Surgical Problems of Respiratory System: DR Abdul MateenAqsa Zahoor Ahmad NadeemNo ratings yet
- Sped in Mapeh FinalDocument30 pagesSped in Mapeh FinalAngelle Bahin100% (2)
- Aging Simulation PDFDocument2 pagesAging Simulation PDFramzan aliNo ratings yet
- Petrous Apex FinalDocument53 pagesPetrous Apex Finalpravinxyz100% (1)
- Knowledge Organiser: Properties of Waves Sound Waves HearingDocument1 pageKnowledge Organiser: Properties of Waves Sound Waves HearingLuisGamesNo ratings yet
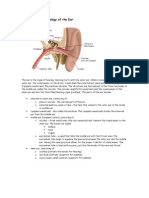
- Anatomy and Physiology of The EarDocument6 pagesAnatomy and Physiology of The EarrizzarNo ratings yet
- Assr, Vemp, VNG, OaeDocument8 pagesAssr, Vemp, VNG, OaeSuprit Sn100% (1)
- MCQsDocument13 pagesMCQsVinay BhatNo ratings yet
- Chapter 30: Health Assessment and Physical Examination: Test BankDocument23 pagesChapter 30: Health Assessment and Physical Examination: Test BankNurse UtopiaNo ratings yet
- Keratosis ObturansDocument12 pagesKeratosis ObturansRahma LuthfaNo ratings yet
- Diseases of EarDocument12 pagesDiseases of EartarshaNo ratings yet
- Ent Miniosce Group A3Document25 pagesEnt Miniosce Group A3frabziNo ratings yet
- Grade 3 2nd Quarter Unit 3 Lesson 1 Sense Organs and How To Care For ThemDocument89 pagesGrade 3 2nd Quarter Unit 3 Lesson 1 Sense Organs and How To Care For ThemRaul Rivera SantosNo ratings yet
- Ent MCQSDocument10 pagesEnt MCQSMuhammad SherazNo ratings yet
- Pathophysiology and Complications of CSOMDocument42 pagesPathophysiology and Complications of CSOMSalsabilla Ameranti PutriNo ratings yet
- Edt 313 - Science Concept PlannersDocument6 pagesEdt 313 - Science Concept Plannersapi-454812724No ratings yet
- Mastoid Obliteration January 2021Document7 pagesMastoid Obliteration January 2021Lovesickbut PrettysavageNo ratings yet
- Medai ReDocument0 pagesMedai RepatojaracNo ratings yet
- Chapter 5 Sensation NotesDocument5 pagesChapter 5 Sensation NotesAlicia Raptor Chen100% (1)
- Asius PosterDocument1 pageAsius PosterSteve Keeley0% (1)
- Dysmorphology Training ManualDocument23 pagesDysmorphology Training Manuale.K.e.kNo ratings yet
- Oxford Fajar 6 SoundDocument5 pagesOxford Fajar 6 SoundAqilah HazwaniNo ratings yet
- Meniere's DiseaseDocument63 pagesMeniere's DiseaseLaurice Grace Zamayla BaelNo ratings yet
- RNCM 101 Guidelines For Return Demonstration 2021Document24 pagesRNCM 101 Guidelines For Return Demonstration 2021Athena AlabadoNo ratings yet
- Otalgia by DrtbaluDocument13 pagesOtalgia by DrtbaluDr. T. Balasubramanian100% (2)