Professional Documents
Culture Documents
Difficulty Sleeping, Increased Drooling, or Increased Fussiness
Difficulty Sleeping, Increased Drooling, or Increased Fussiness
Uploaded by
Won Vi0 ratings0% found this document useful (0 votes)
45 views6 pagesThe document provides instructions for various pediatric medical conditions and procedures. It includes recommendations for positioning and monitoring for procedures like femoral venipuncture, lumbar puncture and cardiac catheterization. It also provides guidance for caring for conditions like cystic fibrosis, Kawasaki disease, neutropenia and more. The document offers tips for assessments, treatments, medications, activities and education topics for infants and children of various ages.
Original Description:
Peds
Original Title
PEDS Proctor
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThe document provides instructions for various pediatric medical conditions and procedures. It includes recommendations for positioning and monitoring for procedures like femoral venipuncture, lumbar puncture and cardiac catheterization. It also provides guidance for caring for conditions like cystic fibrosis, Kawasaki disease, neutropenia and more. The document offers tips for assessments, treatments, medications, activities and education topics for infants and children of various ages.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
0 ratings0% found this document useful (0 votes)
45 views6 pagesDifficulty Sleeping, Increased Drooling, or Increased Fussiness
Difficulty Sleeping, Increased Drooling, or Increased Fussiness
Uploaded by
Won ViThe document provides instructions for various pediatric medical conditions and procedures. It includes recommendations for positioning and monitoring for procedures like femoral venipuncture, lumbar puncture and cardiac catheterization. It also provides guidance for caring for conditions like cystic fibrosis, Kawasaki disease, neutropenia and more. The document offers tips for assessments, treatments, medications, activities and education topics for infants and children of various ages.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
You are on page 1of 6
1.
Femoral venipuncture on a toddler position: supine
2. Cystic fibrosis: admin pancreatic within 30 mins of meals and snacks, if they have
steatorrhea they should get pancreatic enzyme, increase fat content in the child’s diet to
40 percent of total cal, their diet is high protein meal and snacks
3. Kawasaki disease in toddler expect: increased temperature, xerophthalmia, cervical
lymphadenopathy, strawberry tongue, cracked lips and edema in the oral mucosa and
pharynx, tachycardiac (not bradycardia)
4. Tunneled central venous access device intervention: use a semipermeable transparent
dressing to cover the site, avoid scissors, flush lumen with heparin not a sodium chloride
5. 10 year old with neutropenia: give a book about adventure to challenge them???
6. Preschool: large puzzle
7. Juvenile idiopathic arthritis: encourage them to perform independent self care!
8. Lumbar puncture: side lying/ or supine for 30 min to 1 hr after lumbar puncture
9. Semi recumbent: gavage feeding
10. DKA with a current glucose of 250 mg/dl: administer 5% dextrose in 0.9% sodium
chloride by continuous IV infusion 250 to 300 must be given that. If not, they might get
hypoglycemia
11. Lower leg cast 24 hours, what you report? Restricted ability to move the toes.
12. SO A PHYSICAL NEGLECT FOR 18 MONTH OLD IS POOR PERSONAL HYGIENE.
Multiple bruises on knees is normal because they run and fall all the time.
13. Cheiloplasty: lip surgery, apply antibiotic ointment on their suture line for 3 days, report
excessive swallowing, avoid placing objects in mouth, use sterile water in sutures
nothing else
14. Hypopituitarism: prescribe RECOMBINANT GROWTH HORMONE
15. Hyposecretion of Antidiuretic hormone: desmopressin
16. Hypothyroid: levothyroxine
17. Cardiac cath: wait 3 days before taking a bath, they can attend school but just avoid
strenuous activities, resume regular diet, remove pressure dressing day after procedure
and put bandage strip daily for the next 2 days
18. Epiglottitis: ABC first so monitor o2 sat
19. Abdominal trauma- mononucleosis should avoid activities because they might result in
trauma
20. Pulse oximetry for infant secure sensor : great toe
21. If you have a superficial burn: DO NOT LEAVE IT OPEN TO AIR, apply antimicrobial to
the affected area, do not ice it
22. Tinea pedis: the sweating in the feet, so wear sandals or something open
23. The nurse should inform the guardian that teething can result in discomfort for the
infant. Therefore, the guardian should look for indications such as pulling on the ears,
difficulty sleeping, increased drooling, or increased fussiness.
24. The nurse should use the FACES pain rating scale for pediatric clients who are 3 years
old and older.
25. Mama can breastfeed while sample heel stick is being obtained
26. Nonheme iron: raisins (juice is vit c, milk is calcium, carrots does not have iron)
27. Bacterial meningitis: The nurse should plan to maintain the adolescent on droplet
precautions for at least 24 hr following initiation of antimicrobial therapy. This
practice will ensure that the adolescent is no longer contagious, which protects family
members and the personnel caring for the client.
28. Faculty should plan to teach challenging academic subjects in the morning when
students who have ADHD are most able to focus and their medication is most likely to
be effective.
29. Sunburn protection: avoid playing outside between 10am to 2pm, choose waterproof
sunscreen min of spf 15, dress in cotton, reapply sunscreen more often like 2 hrs instead
of 4 hrs
30. The nurse should identify that irritability, inability to follow commands, and difficulty
concentrating are manifestations of increased intracranial pressure due to
decreased blood flow within the brain and pressure on the brainstem.
31. The nurse should monitor the adolescent's serum potassium level following the
administration of sodium polystyrene sulfonate. This medication is used to treat
hyperkalemia by exchanging sodium ions for potassium ions in the intestine.
32. The nurse should instruct the parents to brush the child's teeth after administering
digoxin to prevent tooth decay caused by the medication, which comes as a
sweetened liquid to enhance the taste. Do not double the dose. Do not repeat dose if
child vomits. Use calibrate device to measure medication, not a teaspoon!
33. Following surgical repair of a hypospadias, the infant is at increased risk for infection at
the operative site. The nurse should instruct the parents to administer a prophylactic
antibiotic as prescribed to help prevent infection. Not a hydrocortisone
34. HYpospadias: The nurse should instruct the parents to ensure that the stent drains
directly into the infant's diaper to prevent kinking or twisting that can interfere
with urine flow.
35. Controlling impulsive feelings is an expected behavior of school-age children. A
toddler is more likely to have difficulty controlling strong and impulsive feelings as they
try to assert their independence and gain control of situations. The nurse should include
that expressing likes and dislikes is an expected behavior of toddlers. This is the
time in life when a toddler is developing autonomy and self-concept. They will try to
assert themselves and frequently refuse to comply. The parent should allow the child to
have some control, but also set limits for them so they learn from their behavior and
learn to control their actions.
36. The nurse should expect Kussmaul respirations in a child who has diabetic
ketoacidosis. These deep and rapid respirations are the body's attempt to eliminate
excess carbon dioxide and achieve a state of homeostasis.
37. HR 106 to 186/min for a 3- to 5-month-old infant.
38. When using the urgent vs. nonurgent approach to client care, the nurse should assess
this child first. An episode of forceful vomiting is an indication of increased intracranial
pressure in a toddler who has a concussion.
39. After establishing an airway and stabilizing the child's respirations, the next action the
nurse should take when using the airway, breathing, and circulation approach to client
care is to establish IV access to maintain the child's circulatory volume.
40. The nurse should identify that an erythrocyte sedimentation rate of 18 mm/hr is above
the expected reference range of up to 10 mm/hr and is an indication of osteomyelitis.
41. Bicycle safety: The child should be able to stand on the balls of their feet when sitting on
the bike and wear light colored clothing duh!
42. To assess peripheral edema: palpate DORSUM OF FEET
43. Generalized edema assessment: observe for periorbital swelling
44. Impetigo contagiosa is a bacterial infection: apply topical antibacterial ointment to the
lesion, wash the bed linen daily with hot water, wash hands before and after contact with
affected area. Dont let the crust to remain intact, you have to wash it.
45. Up and back- children 3 yr and up
46. Down and back- children younger than 3
47. Severe dehydration? ABSENCE OF TEARS (If decreased only, that’s moderate.) Deep,
rapid respirations
48. To feed infant with cleft palate, use A CUP for 7 to 10 days. At least BURP THEM 2 to 3
times during feeding because baby might swallow air. They are expected to feed noisily.
49. Intussusception: prepare barium enema, they may have VOMITING AND LETHARGY
50. Infant risk for electrolyte imbalance and dehydration is because they have LONGER
INTESTINAL TRACT
51. Pancreatic enzyme: cystic fibrosis
52. Calcium and iron: lead poisoned
53. If 4 month old baby, play with them by allowing them to splash in bathtub. If they are 9 to
12 month old, show them a board book with large pics or imitate sounds of animals or
push pull toys
54. Ileostomy: check bag for stool every 4 hours, they can lie on abdomen, tuck the
appliance into the diaper, replace appliance once a week
55. If patient has idiopathic juvenile arthritis, still encourage them to attend school regularly.
APPLY MOIST HEAT TO RELIEVE JOINT PAIN NOT COLD COMPRESS OK? TAKE
NSAIDS not OPIOIDS, THERE IS NO DIET FOR THIS ONE
56. For enema on infant, do not administer tap water, and if you insert the tubing it should be
2.5cm or 1 inch into the rectum, also be placed in supine position. Hold the buttocks
together after administering fluid
57. Jack in the box for infants
58. VP shunt complication: abdominal distention
59. 24 month old baby what you expect: they can build a tower of 6 blocks, they have
slightly bowed or curved leg appearance, 16 teeth, vocab will be 300 words and speak in
2 to 3 phrases, head circum is equal to chest
60. 3 year old? Coloring book and crayons
61. Snellen chart: position 10 ft away from the chart, wear prescribed glasses
62. Tumbling E: have them point the direction the E is facing
63. Teaching about measures to reduce risk of choking for toddlers: hot dog, grape, bagel,
marshmallow
64. Teaching about managing asthma and using a peak expiratory flow meter, which is an
understanding? “I will continue to take meds when my peak flow rate is in the green
zone”
65. Cerebral palsy teaching: “your child will need BOTULINUM TOXIN A INJECTION to
reduce muscle spasticity” , they can eat by mouth, they can participate in recreational
activities, do not use throw rugs
66. Infant who is breastfed and receiving amoxicillin for upper resp infection. Whitish
patches on the tongue that will not scrape off. : Administer an antifungal medication after
feeding to ensure oral mucosa and tongue safety ambot, no water
67. 6 year old child tx for pneumococcal pneumonia 4 days ago. What findings is indication
tx is treatment? HR 118 is expected for 6 yr old (75 to 118) . 18 to 25 respiratory rate for
6 to 11 yrs old
68. A nurse is creating a plan for a 6 mon old infant who requires continuous pulse oximetry
monitoring. Which intervention? COVER THE OXIMETRY SENSOR WITH CLOTHING
daw...to prevent false reading! Move the sensor every 4 to 8 hours. And place sensor
around the hand or foot for accurate reading. No conduction gel!
69. School aged child who has sickle cell anemia. What to do to help decrease risk of vaso
occlusive crisis? Provide fluid throughout the day. Oxygen not needed for anemia. Blood
transfusion is not for a crisis.
70. IM injection to a 2mon old infant, which site should the nurse plan to administer
injection? Vastus lateralis
71. Physical assessment on a 12 mon old. What do you report? Current weight is double. 12
mon is triple. 6 mos is double. Posterior fonatel should be closed at about 2 mos of age.
15 mos they can walk without assistance. 6 to 8 teeth present
72. Child overdose of acetaminophen- acetylcysteine
73. Opioid respiratory depression: naloxone
74. Allergy to medication: diphenhydramine
75. Hypoglycemia: glucagon
76. Acute asthma attack, what you administer? Albuterol
77. Assess 2 mon old infant with ventricular septal defect. What you report? Weight gain of
1.8 kg (4lb) . This is too much weight so report! - systemic murmur, hr 125, soft flat
fontanel are all normal and expected
78. Sickle cell anemia pt experiencing vaso-occlusive crisis PRIORITY- monitor the child’s
o2 sat level ABC is always PRIORITY
79. 6 mon old with moderate dehydration. What findings do you expect? Dry mucous
membranes
80. Severe dehydration: weight loss more than 10%, absent tears, lethargy
81. Child abuse. What example illustrate suggestive finding? Arm cast for a spiral fracture
on forearm. Not vague headache or stomach ache or bruising on knees coz this is
normal for children
82. Discharge teaching to guardians of adolescents with postoperative following a
tonsillectomy. What manifestations should you report? Constant clearing of the throat!!
Old dry brown blood is normal, bad odor is normal, low grade fever is normal
83. Lab values for 6 month old infants with acute renal failure. What do you expect? Sodium
125 is bad so report. Bun level 5 is normal for infants. (infant bun is 5 to 18, newborn is 3
to 12 *google)
84. 4 month old with acute otitis media and a fever of 38.3 (101.1). What do you
administer? Amoxicillin,
85. Diphenhydramine is for allergic reactions
86. Furosemide is a diuretic to decrease edema
87. Ibuprofen are not for children under 6 months old. Acetaminophen is preferred
88. 1 year old with chronic otitis media. Risk of a delay in development? Speech patterns
89. School aged child who has hemophilia and fell on the playground. Pain is 4 to 10. What
you do? Apply an ice pack to the joint. Avoid giving aspirin or NSAID for hemophilia
patients.
90. Type 1 diabetes mellitus managing hypoglycemia. Teaching? 4oz OJ why OJ for
hypoglycemia. Research this! Also correct: 4 glucose tablets, 2 tsp of sugar, 6 oz of
regular soft drink
91. HIV preschool. Manifestations to expect? Chronic diarrhea, failure to thrive, weight loss
92. Preop education for 8 year old before cardiac surgery: USE A DOLL
93. Glomerulonephritis, school age child, BP of 160.78, receiving hydralazine, lunch choice:
3oz grilled chick, 1 cup pear slice, 120 or 4oz apple juice
94. Preop teaching for preschooler who is scheduled tonsillectomy. Intervention? Encourage
to bring toy
95. Ped unit child with autism. What you do? Ensure the staff visits with the child are kept
short. Because they have difficulty adjusting to new situations.
96. Schoolage child reports horseback riding 3 times per week and has injuries reportedly
related to falls from a horse: thin, frail extremities
97. Lab results fr children with manifestations of influenza. What you report? You report
WBC of 24 (5 to 10)
98. 1month old infant with gastroesophageal reflux. What is an understanding? Add rice
cereal to baby feeding
99. Give infant meds 30 mins before feeding, put them in an infant seat or at 30 degrees
angle 1 hour after feeding, avoid feeding before bedtime, rice cereal thickens the feeding
and prevent vomit
100. Preschool with terminal illness. What you expect? Believes that her own thoughts
can cause death. Because they are overacting!
101. Child maltreatment. What teaching? Premature kids are most maltreated
102. Body mass is 21.2. What is this? Healthy! (overweight is 25 to 29, 30 is obese,
under 18.5 is underweight)
103. 18 month old toddler otic meds: pull ear DOWN AND BACK!
104. “My child is suddenly not interested in certain food” what you do? KEEP A DIARY
OF THE FOOD THEY EAT!
105. Cystic fibrosis. What you do? HIGH FAT!
106. Otitis media and temperature is 39.1 or 102.4 = URGENT! administer an
antipyretic
107. FLACC 2months to 7 year old
108. FACES 3 year and older
109. Allergy, histamine, anaphylaxis: nausea, urticaria (hives), stridor (hoarse voice)
110. Parasitic disease: keep fingernails trimmed short.
111. Mild gastroesophageal reflux GER feeding therapy to recommend: thicken
feedings with rice cereal, keep clothing and diaper loose, hold infant upright at least 30
mins after each feeding
112. Toddler language development. What to expect in 18 month old? Vocabulary of
10 or more words, 2 years old they can say their name and complete simple commands,
they cannot name a color until 30 months of age
113. Glomerulophrenitis: weight once each day, check BP every 4 hours, no salt, bed
rest not required (that’s for nephrotic) , potassium restrict
114. Nosebleed what you do? Apply pressure to nose using thumb and forefinger,
keep child calm, seat forward, cold cloth to bridge of nose
115. Intussusception: abdominal ultrasound will confirm the pocket in the intestine
116. Encopresis is caused by stress or changes in environment
117. Infant who has tetralogy of fallout experiencing hypercyanotic episode: place in
knee chest position, also admin morphine not acetaminophen, face mask also and iv
fluid is good
118. When caring for a child with tracheostomy, remove the catheter while applying
intermittent suction
119. 5-4 yr old: copy a square , 2-3 yr old: copy a circle
120. 5 yr old : tie shoes, draw stick figure with 7 parts, print letters of name
121. Preschooler: large pieces puzzle, building blocks
122. School age: chapter books, painting
123. Toddler: finger paint
124. When applying urine collection bag, always wash and dry genitalia, perineum
and surrounding skin FIRST
125. Anemia is for iron
126. Low platelet is encourage quiet play to children to prevent risk for injury and
excessive bleeding
127. If you have hypospadias: avoid tub bath, avoid clamping catheter any time,
increase fluid intake, and apply antibacterial ointment in penis
128. Nephrotic: provide thorough skin care, fluid restriction, diet requires protein
sodium fat restriction, AVOID INFECTED PEOPLE , corticosteroids first line treatment,
weight daily
129. Otitis media: ear infection, smoking is bad for this
130. Hyperopia: farsightedness should be reported
131. Dtap 5 years old
132. If an infant has acute gastroenteritis, report cap refill 5 seconds. The heart rate of
150 is expected in them
133. Google: Newborns 0 to 1 month old: 70 to 190 beats per minute. Infants 1 to 11
months old: 80 to 160 beats per minute. Children 1 to 2 years old: 80 to 130 beats per
minute. Children 3 to 4 years old: 80 to 120 beats per minute
You might also like
- Essential Intrapartum and Newborn CareDocument3 pagesEssential Intrapartum and Newborn CareMasterclass40% (5)
- of Newborn CareDocument42 pagesof Newborn CareGurpreet kaur100% (10)
- Pediatric Nursing NCLEX Questions!Document6 pagesPediatric Nursing NCLEX Questions!Javier Shields86% (7)
- Rufaida College of Nursing Jamia Hamdard (Hamdard University) Lesson Plan ONDocument16 pagesRufaida College of Nursing Jamia Hamdard (Hamdard University) Lesson Plan ONRaja100% (2)
- Neonatal ResuscitationDocument15 pagesNeonatal Resuscitationpriyanka91% (11)
- Safe Effective Care Environment For StudsDocument4 pagesSafe Effective Care Environment For Studscerelinamaratas100% (1)
- Nursing Process in The Care of The Preterm InfantDocument5 pagesNursing Process in The Care of The Preterm InfantizwanNo ratings yet
- General Objecti-Wps OfficeDocument3 pagesGeneral Objecti-Wps OfficeSumit YadavNo ratings yet
- Needs of New-Born CareDocument27 pagesNeeds of New-Born CarePruthviNo ratings yet
- Price: Pediatric Nursing, 10 Edition: Open Book Quizzes Chapter 8: Disorders of The InfantDocument2 pagesPrice: Pediatric Nursing, 10 Edition: Open Book Quizzes Chapter 8: Disorders of The InfantmickjagerNo ratings yet
- Postpartum ActDocument3 pagesPostpartum ActClafy DNo ratings yet
- FINAL ENC ChecklistDocument8 pagesFINAL ENC ChecklistRaven Torres100% (1)
- Einc-Word 054847Document4 pagesEinc-Word 054847Jane OrsalNo ratings yet
- NICU ReportDocument7 pagesNICU ReportoapsdoaksdokaNo ratings yet
- DLPDocument3 pagesDLPKathrina AlfonsoNo ratings yet
- NB Suctioning Heimlich Manuever 1Document13 pagesNB Suctioning Heimlich Manuever 1Sarah Shane Cortes CortesNo ratings yet
- Pedia 25Document5 pagesPedia 25Mar OrdanzaNo ratings yet
- Nursing Care of A Newborn and Family in The Post Partal Period ReviewerDocument2 pagesNursing Care of A Newborn and Family in The Post Partal Period ReviewerJo PigarNo ratings yet
- Nagogastric Tube FeedingDocument8 pagesNagogastric Tube FeedingSiwani raiNo ratings yet
- Capstone ATI EXIT EXAMDocument10 pagesCapstone ATI EXIT EXAMcarol50% (2)
- Pediatric Exam HESI Sample Questions PDFDocument10 pagesPediatric Exam HESI Sample Questions PDFSurendra Momidi100% (2)
- Nursing Bullets 4Document12 pagesNursing Bullets 4kate annNo ratings yet
- Essential Intrapartum and Newborn Care (Einc) 2Document8 pagesEssential Intrapartum and Newborn Care (Einc) 2Alphine DalgoNo ratings yet
- NCM NewbornDocument3 pagesNCM NewbornAisa Janna Biston HabibNo ratings yet
- Neonatal ResuscitationDocument16 pagesNeonatal ResuscitationPrecilla C. Stephen100% (3)
- Post Assessment PediatricsDocument4 pagesPost Assessment Pediatricscuicuita100% (4)
- Essential Newborn CareDocument20 pagesEssential Newborn Carejanjan_cepilloNo ratings yet
- Case Study On Observation and Newborn CareDocument8 pagesCase Study On Observation and Newborn CarePiyush Dutta100% (1)
- Enbc RaniDocument24 pagesEnbc RaniRajaNo ratings yet
- Pedia PCADocument6 pagesPedia PCARamon Carlo Almiranez100% (1)
- 8Document7 pages8belleNo ratings yet
- Uep - Edu.ph: Nursing AssessmentDocument9 pagesUep - Edu.ph: Nursing AssessmentCzarina Mae Quinones TadeoNo ratings yet
- Care of Unconscious PatientDocument7 pagesCare of Unconscious PatientSallieNo ratings yet
- Chapter 2, 3 and 4Document19 pagesChapter 2, 3 and 4Ingrid Valerie A. GanirNo ratings yet
- Pediatric Board Cert Exam1Document6 pagesPediatric Board Cert Exam1acar0105No ratings yet
- NCM 109 SF Book QuestionsDocument12 pagesNCM 109 SF Book Questionsdunhill26labanNo ratings yet
- Case Study Baby HDocument6 pagesCase Study Baby HSharon Williams0% (1)
- E1 Fall 20Document10 pagesE1 Fall 20Alexander BarbechoNo ratings yet
- Child Evolve ExamDocument37 pagesChild Evolve Examfriendofnurse100% (14)
- ATI Comprehensive: Study Online atDocument6 pagesATI Comprehensive: Study Online atVanessaMUeller100% (1)
- Part 2 - NSG Care of A Family When A Child Needs Diagnostic or Therapeutic ModalitiesDocument38 pagesPart 2 - NSG Care of A Family When A Child Needs Diagnostic or Therapeutic ModalitiesJustine Jean GuillermoNo ratings yet
- Maternity Study Guide CH 21-24 & 29Document11 pagesMaternity Study Guide CH 21-24 & 29Vanessa Da CruzNo ratings yet
- Case Simulation in Pediatric Nursing Case Study 1Document4 pagesCase Simulation in Pediatric Nursing Case Study 1Cheska PalomaNo ratings yet
- Aspirin: Assess The Overall Condition of The SkinDocument4 pagesAspirin: Assess The Overall Condition of The SkinShaina Fe RabaneraNo ratings yet
- Discharge For InfantDocument3 pagesDischarge For InfantIra Krystel ReyesNo ratings yet
- Case StudyDocument7 pagesCase StudyCaren MarquezNo ratings yet
- Misc Review QsDocument4 pagesMisc Review QsAlvin L. RozierNo ratings yet
- PNC CareDocument2 pagesPNC CareAparna ChoudhuryNo ratings yet
- Chapter 3B Neonatal ResusDocument18 pagesChapter 3B Neonatal ResusAbood AboodshNo ratings yet
- Teaching ProgramDocument6 pagesTeaching ProgramLizly Letrondo-PinoteNo ratings yet
- Case Study On Observation and Newborn CareDocument38 pagesCase Study On Observation and Newborn CarePiyush Dutta100% (2)
- Nursing Care The NewbornDocument82 pagesNursing Care The NewbornLeamae AbayonNo ratings yet
- NSG 1405 Care PlansDocument3 pagesNSG 1405 Care PlansAshley CyriacNo ratings yet
- Assignment #1 - PEDIA (GIT)Document1 pageAssignment #1 - PEDIA (GIT)Kerima Danica Lising GayoNo ratings yet
- Management of New Born: Presented By: Riya Patel Shukal M.SC (OBGYN)Document27 pagesManagement of New Born: Presented By: Riya Patel Shukal M.SC (OBGYN)BBNo ratings yet
- Essential Intrapartum Newborn Care 181120082158 PDFDocument19 pagesEssential Intrapartum Newborn Care 181120082158 PDFDorinna Rizada BagaNo ratings yet
- Care NewbornDocument38 pagesCare NewbornRaja0% (1)
- The Care and Feeding of Children - A Catechism for the Use of Mothers and Children’s NursesFrom EverandThe Care and Feeding of Children - A Catechism for the Use of Mothers and Children’s NursesNo ratings yet
- The Care and Feeding of Children - A Catechism for the Use of Mothers and Children's NursesFrom EverandThe Care and Feeding of Children - A Catechism for the Use of Mothers and Children's NursesNo ratings yet
- ENEMADocument3 pagesENEMAdenNo ratings yet
- SequanceDocument481 pagesSequanceRite2summaiya SumiNo ratings yet
- Down Syndrome REG Last EditDocument60 pagesDown Syndrome REG Last EditJane NeduNo ratings yet
- List of Designated OfficersDocument56 pagesList of Designated OfficersPrabhakar Joy PalakurthiNo ratings yet
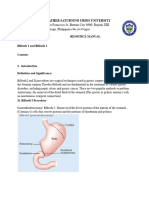
- Billroth 1 and 2 Resource ManualDocument8 pagesBillroth 1 and 2 Resource ManualMike AndersenNo ratings yet
- High-Efficiency and High-Flux Hemodialysis: Sivasankaran Ambalavanan Gary Rabetoy Alfred K. CheungDocument10 pagesHigh-Efficiency and High-Flux Hemodialysis: Sivasankaran Ambalavanan Gary Rabetoy Alfred K. CheungveiaNo ratings yet
- TaurodontDocument14 pagesTaurodontHameed WaseemNo ratings yet
- Pedia CardDocument4 pagesPedia CardPatricia Kate RegalaNo ratings yet
- LEARNING DIARY FOR NCM 105n/L-Nutrition and Diet Therapy Date: Name: Topics: Guide QuestionsDocument3 pagesLEARNING DIARY FOR NCM 105n/L-Nutrition and Diet Therapy Date: Name: Topics: Guide QuestionsWendell Gian GolezNo ratings yet
- Department of Education: Individual Workweek Plan August 2021Document5 pagesDepartment of Education: Individual Workweek Plan August 2021Jeffren P. MiguelNo ratings yet
- AIPGMEE 2006 Question PaperDocument96 pagesAIPGMEE 2006 Question PaperpavaniNo ratings yet
- Pedia NotesDocument3 pagesPedia NotesNikki DiocampoNo ratings yet
- Student Overview: # Question and Answer Choices Points CategoriesDocument17 pagesStudent Overview: # Question and Answer Choices Points CategoriesGabriel AndradeNo ratings yet
- Antipsychotic Drugs: Referance Book .Essential of Pharmacology by Shah NawazDocument47 pagesAntipsychotic Drugs: Referance Book .Essential of Pharmacology by Shah NawazLaiba ShahNo ratings yet
- Infection Control Measures in Pediatric Dental Practice During Covid - 19 - A Review ArticleDocument5 pagesInfection Control Measures in Pediatric Dental Practice During Covid - 19 - A Review ArticleInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Genital Tract InfectionsDocument4 pagesGenital Tract Infectionsmed.progressNo ratings yet
- Generic Name Brand Name Abbreviation: © 2017 Find Your Script HIV Medications - Drug Names Quick SheetDocument1 pageGeneric Name Brand Name Abbreviation: © 2017 Find Your Script HIV Medications - Drug Names Quick SheetMonica J Ortiz PereiraNo ratings yet
- Case Presentation SurgeryDocument9 pagesCase Presentation SurgeryFlora LawrenceNo ratings yet
- Jurnal 2 PDFDocument6 pagesJurnal 2 PDFviny206No ratings yet
- CARBUNCLEDocument11 pagesCARBUNCLEKesavanadh T M100% (1)
- Bioinstrument 7 (Respiratory System) 16-22Document7 pagesBioinstrument 7 (Respiratory System) 16-22vividmeNo ratings yet
- Endodontics ObturationDocument8 pagesEndodontics ObturationShameer Parambil100% (2)
- HypnotherapyDocument5 pagesHypnotherapyapi-585441161No ratings yet
- HY Immunology by Mehlaman - PDF Version 1Document41 pagesHY Immunology by Mehlaman - PDF Version 1Drekola KhanNo ratings yet
- Shock ManagementDocument17 pagesShock ManagementAmare EshetieNo ratings yet
- List of Nursing Abbreviations and Acronyms 1Document5 pagesList of Nursing Abbreviations and Acronyms 1Jay Debby RuizoNo ratings yet
- RLE - WK1 - Manarang, Kyla Mae SDocument1 pageRLE - WK1 - Manarang, Kyla Mae SKyla ManarangNo ratings yet
- Common Equations Used in Renal Physiology PDFDocument1 pageCommon Equations Used in Renal Physiology PDFAnonymous t5TDwdNo ratings yet
- Clinical Exam For OphthalmologyDocument6 pagesClinical Exam For Ophthalmologynuuraaisya50% (2)
- Natural Tea Give Health Benefits (A3 Size)Document8 pagesNatural Tea Give Health Benefits (A3 Size)itsjai1303m80No ratings yet