Professional Documents
Culture Documents
Erythema Dyschromicum Perstans A Case Report 2376 0427 1000266
Erythema Dyschromicum Perstans A Case Report 2376 0427 1000266
Uploaded by
Batra MourinhoOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Erythema Dyschromicum Perstans A Case Report 2376 0427 1000266
Erythema Dyschromicum Perstans A Case Report 2376 0427 1000266
Uploaded by
Batra MourinhoCopyright:
Available Formats
See discussions, stats, and author profiles for this publication at: https://www.researchgate.
net/publication/322856914
Erythema Dyschromicum Perstans: A Case Report
Article in Journal of Pigmentary Disorders · January 2017
DOI: 10.4172/2376-0427.1000266
CITATIONS READS
0 139
5 authors, including:
Koray Durmaz İlkay Özer
Bozuyuk State Hospital Necmettin Erbakan Üniversitesi
17 PUBLICATIONS 14 CITATIONS 46 PUBLICATIONS 55 CITATIONS
SEE PROFILE SEE PROFILE
Sıddıka Fındık Pembe Oltulu
Necmettin Erbakan Üniversitesi Necmettin Erbakan University Meram Faculty of Medicine
60 PUBLICATIONS 187 CITATIONS 89 PUBLICATIONS 178 CITATIONS
SEE PROFILE SEE PROFILE
Some of the authors of this publication are also working on these related projects:
Dermatologic Emergencies View project
Epidemiological and localization characteristics of non-melanoma skin cancers: Retrospective analysis of 400 cases View project
All content following this page was uploaded by Koray Durmaz on 19 May 2020.
The user has requested enhancement of the downloaded file.
of
en
Pigm tary D Durmaz et al., Pigmentary Disorders 2017, 4:2
DOI: 10.4172/2376-0427.1000266
Journal of Pigmentary Disorders
iso
al
Journ
rder
s
World Health Academy
ISSN: 2376-0427
Case Report Open Access
Erythema Dyschromicum Perstans: A Case Report
Koray Durmaz1, İlkay Özer1, Sıddıka Fındık2, Pembe Oltulu2* and Arzu Ataseven1
1
Department of Dermatology, Necmettin Erbakan University, Turkey
2
Department of Pathology, Necmettin Erbakan University, Turkey
Abstract
Erythema dyscromicum perstans (EDP) or Ashy dermatosis is an uncommon pigmentary disorders which
characterized with asymptomatic gray symmetric confluent macules over the body. It usually starts between first to
three decades of the life and has a slow onset. This ailment can affect the palms, soles, scalp, nails and mucous
membranes. Despite the definition of some etiological factors, the exact etiology of EDP is not clear. In this paper, we
present a 24 years old patient with EDP.
Introductıon
Ashy dermatosis is an uncommon dermatosis which has unknown
etiology [1,2]. There is no accord on the description of EDP and some
different terms like EDP, ashy dermatosis, lichen planus pigmentosus
and idiopathic eruptive macular pigmentation have being used
interchangeably in the literature for this dermatosis [3].
Case Report
A 24 year old woman with type III phototype complexion presented
with numerous asymptomatic slate-grey macules on her trunk and back
with a 6 year history. Firstly,the lesions had started right side of trunk
and new lesions seemed increasingly to involve other areas of trunk
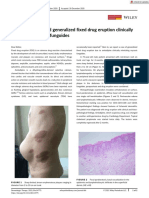
and back (Figure 1). There were no identifiable triggers or associated
family history. She had no known family history of skin or autoimmune
disease either. At the physical examination we noticed brown-grey
coloured pigmented macules and patches on the trunk and back. Some
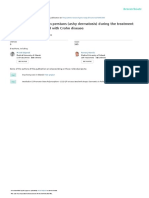
of the lesions appeared on her back were encircled by an erythematous Figure 2: Basal hyperpigmentation (blue arrow), dermal perivascular
halo and had a little elevated borders. The lesions were scaly and also she lymphocytic infiltrate with melanophages (red arrow) (H&E stain, 400x
had mild pruritus on the lesional areas. Histopathological findings of magnification).
biopsy specimen from trunk showed mild hyperkeratosis, melanocytic
hyperplasia at the basement membrane and perivascular lymphocytic emollients were also added to the therapy. After this 12 weeks period,
infiltrate with melanophages in dermis (Figure 2). Pityriasis rosea was a betterment of the erythematous violaceous component of lesions was
ruled out by reason of spongiosis absence. The patient was diagnosed noticed.
as EDP with clinical and histopathological findings. Routine laboratory
tests including glucose, liver enzymes, thyroid hormones, complete Discussion
blood count, were normal and Antinuclear antibody (ANA) test
Erythema Dyschromicum Perstans (EDP) or Ashy dermatosis
was negative. She was treated with narrowband ultraviolet B therapy
is an uncommon acquired and chronic dermatosis,characterized
three times a weekly for 12 weeks. Topical mometasone furoate and
by asymptomatic and progressive hyperpigmented oval, polycyclic
macules of various size on the trunk, face and extremities. These
brown-grey macules sometimes show erythematous borders [4,5].
Although the etiology of EDP is unclear there are some probable
genetic factors related by genes located in the major histocompatibility
complex region [6]. There are also some predisposing triggers that
have been proposed, such as drugs (antibiotics, benzodiazepines,
pesticides), endocrinopathies or HIV and hepatitis like infectious
*Corresponding author: Pembe Oltulu, Necmettin Erbakan Universitesi Meram
Tip Fakultesi konya, Turkey, Tel: +903322236000; E-mail: drpembe@yahoo.com
Received July 12, 2017; Accepted September 13, 2017; Published September
20, 2017
Citation: Durmaz K, Özer İ, Fındık S, Oltulu P, Ataseven A (2017) Erythema
Dyschromıcum Perstans: A Case Report. Pigmentary Disorders 4: 266.
doi:10.4172/2376-0427.1000266
Copyright: © 2016 Durmaz K, et al. This is an open-access article distributed under
the terms of the Creative Commons Attribution License, which permits unrestricted
Figure 1: Slate-grey macules on trunk. use, distribution, and reproduction in any medium, provided the original author and
source are credited.
Pigmentary Disorders, an open access journal Volume 4 • Issue 2 • 1000266
ISSN: 2376-0427
Citation: Durmaz K, Özer İ, Fındık S, Oltulu P, Ataseven A (2017) Erythema Dyschromıcum Perstans: A Case Report. Pigmentary Disorders 4: 266.
doi:10.4172/2376-0427.1000266
Page 2 of 2
conditions [7-9]. In this case there wasn’t any triggers neither medical 3. Zaynoun S, Rubeiz N, Kibbi AG (2008) Ashy dermatoses-a critical review of
the literature and a proposed simplified clinical classification. Int J Dermatol
history nor laboratory findings [10]. The differential diagnosis includes
47: 542-544.
pigmented lichen planus, idiopathic eruptive macular pigmentation,
postinflammatory hyperpigmentation and Addison disease. Pigmented 4. Osswald SS, Proffer LH, Sartori CR (2001) Erythema dyschromicum perstans:
A case report and review. Cutis 68: 25-28.
lichen planus is the main considered differential diagnosis of EDP.
Lesions are usually characterized by bright violaceus-purple, flat, solid 5. Nieuweboer-Krobotova L (2013) Hyperpigmentation: types, diagnostics and
papules and often crossed by whitish lines (called as Wickham striae). targeted treatment options. J Eur Acad Dermatol Venereol 27: 2-4.
Lichen planus often involves mucous membranes by some different 6. Correa MC, Memije EV, Vargas-Alarcón G, Guzmán RA, Rosetti F, et al. (2007)
types and is related with mild pruritus, neither symptoms were present HLA-DR association with the genetic susceptibility to develop ashy dermatosis
in Mexican Mestizo patients. J Am Acad Dermatol 56: 617-620.
in our patient. Idiopathic eruptive macular pigmentation would be
another differential condition, however it presents typically with 7. Vásquez-Ochoa LA, Isaza-Guzmán DM, Orozco-Mora B, Restrepo-Molina
asymptomatic brownish nonconfluent lesions that involve the face, R, Trujillo-Perez J, et al. (2006) Immunopathologic study of erythema
dyschromicum perstans (ashy dermatosis). Int J Dermatol 45: 937-941.
trunk and proximal extremities in children and adolescents [11]. We
excluded postinflammatory hyperpigmentation and Addison disease as 8. Kontochristopoulos GJ, Aroni K, Anagnostopoulos G, Nakopoulou L,
Tassopoulos NC (2001) Erythema dyschromicum perstans and hepatitis C
a result of examination findings and the anamnesis. Treatment of EDP
virus infection. Int J Dermatol 40: 346-348.
include topical and systemic steroids, hydroquinone, dapsone, retinoids,
griseofulvin, ascorbic acid, chloroquine, estrogens, progesterone, 9. Cherobin AC, Oliveira FO, Baeta IG, Vale EC (2012) Case for diagnosis. Ashy
dermatosis. An Bras Dermatol 87: 151-152.
chemical peels, phototherapy, laser therapy, keratolytics, clofazimine
and nbUVB phototherapy [10,12]. 10. Novick NL, Phelps R, Tom C (1986) Erithema dyschromicum perstans. Int J
Dermatol 25:322-323.
In fact, nbUVB phototherapy decreases peripheral NK cell activity,
11. Oiso N, Tsuruta D, Imanishi H, Kobayashi H, Kawada A (2012) Erythema
lymphocyte proliferation, cytokine production as IL-2, IFN-g and IL- dyschromicum perstans in a Japanese child. Pediatr Dermatol 29:637-640.
10 [13,14]. NbUVB phototherapy stimulates pigment production and
12. (1997) An appraisal of narrow band (TL-01) UVB phototherapy. British
hides the dermal pigmentation [13,14]. In our case we used nbUVB Photodermatology Group Workshop Report (April 1996). Br J Dermatol 137:
phototherapy 3 times a weekly. 32730.
Refrences 13. Fabbrocini G, Di Costanzo L (2012) In vitro UVA irradiation decreases both
release ability and gene-expression of VEGF-A from mastcells. Photodermatol
1. Keisham C, Sarkar R, Garg VK, Chugh S (2013) Ashy dermatosis in an 8 year
Photoimmunol Photomed 28: 165-168.
old Indian child. Indian Dermatol Online J 4: 30-32.
14. Fabbrocini G, Cacciapuoti S, Izzo R, Mascolo M, Staibano S, et al. (2015)
2. Srivastava N, Solanki L, Chand S, Garbyal RS, Singh S (2008) Ashy dermatosis
Efficacy of narrowband UVB phototherapy in erythema dyschromicum perstans
like pigmentation due to ethambutol. Indian J Dermatol Venereol Leprol 74:
treatment: case reports. Acta Dermatovenerol Croat 23: 63-65.
281-282.
Pigmentary Disorders, an open access journal Volume 4 • Issue 2 • 1000266
ISSN: 2376-0427
View publication stats
You might also like
- Adult Development and Aging The Canadian Experience 1st Edition Harper Test BankDocument17 pagesAdult Development and Aging The Canadian Experience 1st Edition Harper Test Bankalexanderariellpu9q100% (30)
- Teleconsult Call SummaryDocument2 pagesTeleconsult Call SummaryJhade Ann CayanesNo ratings yet
- Generalized Eruptive Syringoma: Indian Journal of Dermatology March 2015Document3 pagesGeneralized Eruptive Syringoma: Indian Journal of Dermatology March 2015Yola TamngeNo ratings yet
- 10 1111@dth 14775Document2 pages10 1111@dth 14775dermatom dervenNo ratings yet
- PD Art 22401Document5 pagesPD Art 22401Haris TanNo ratings yet
- Epidermolytic Hyperkeratosis: Clinical Update: Clinical, Cosmetic and Investigational Dermatology DoveDocument12 pagesEpidermolytic Hyperkeratosis: Clinical Update: Clinical, Cosmetic and Investigational Dermatology DoveAri KurniawanNo ratings yet
- Inglés 2018Document7 pagesInglés 2018Luis GuzmánNo ratings yet
- Ashy Dermatosis and Lichen PlanusDocument27 pagesAshy Dermatosis and Lichen PlanusAthenaeum Scientific PublishersNo ratings yet
- A Case of Atrophoderma Vermiculatum Responding ToDocument3 pagesA Case of Atrophoderma Vermiculatum Responding ToToivo ToivonenNo ratings yet
- Implications of Adnexal Invasions in Primary Extramammary Paget's Disease: A Systematic ReviewDocument6 pagesImplications of Adnexal Invasions in Primary Extramammary Paget's Disease: A Systematic ReviewInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Papuloerythroderma of Ofuji - A Case ReportDocument4 pagesPapuloerythroderma of Ofuji - A Case ReportLidwina ApyakaNo ratings yet
- A Case Report of Eruptive Syringoma: Clinical, Dermoscopic and Histological FeaturesDocument5 pagesA Case Report of Eruptive Syringoma: Clinical, Dermoscopic and Histological FeaturesIJAR JOURNALNo ratings yet
- ErythrodermaDocument10 pagesErythrodermadennisadityaNo ratings yet
- Group 5 - Pathogenesis of ErythrodermaDocument20 pagesGroup 5 - Pathogenesis of Erythrodermaachmad billy hakiemNo ratings yet
- (Serbian Journal of Dermatology and Venereology) Dermoscopy Case of The Month PDFDocument5 pages(Serbian Journal of Dermatology and Venereology) Dermoscopy Case of The Month PDFArya NugrahaNo ratings yet
- Actaapa 2020 19Document3 pagesActaapa 2020 19iqbal dsNo ratings yet
- UntitledDocument10 pagesUntitledMarande LisaNo ratings yet
- Examining A Case: Carbamazepine-Triggered Drug Reaction With Eosinophilia and Systemic SymptomsDocument2 pagesExamining A Case: Carbamazepine-Triggered Drug Reaction With Eosinophilia and Systemic SymptomsInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Management of Stevens Johnson Syndrome Toxic Epidermal Necrolysis: Looking Beyond Guidelines!Document9 pagesManagement of Stevens Johnson Syndrome Toxic Epidermal Necrolysis: Looking Beyond Guidelines!anwarNo ratings yet
- Primary Extramammary Paget's Disease With Extensive Skeletal MetastasesDocument5 pagesPrimary Extramammary Paget's Disease With Extensive Skeletal MetastasesLaura PredescuNo ratings yet
- Slide Eritroderma 2Document7 pagesSlide Eritroderma 2Anonymous QqGJk2jK5No ratings yet
- TPD 47 127 enDocument2 pagesTPD 47 127 enNur AzizahNo ratings yet
- Case Study On Pemphigus VulgarisDocument2 pagesCase Study On Pemphigus VulgarisRanindya PutriNo ratings yet
- Dermoscopic Features of Pigmentary Disorders in Indian Skin: A Prospective Observational StudyDocument10 pagesDermoscopic Features of Pigmentary Disorders in Indian Skin: A Prospective Observational StudyIJAR JOURNALNo ratings yet
- Clinical and Dermoscopic Evaluation of PeriorbitalDocument6 pagesClinical and Dermoscopic Evaluation of Periorbitalruby.wryNo ratings yet
- A Study of Beetle Dermatitis: DermatologyDocument3 pagesA Study of Beetle Dermatitis: DermatologyKarina Terry AmartiniNo ratings yet
- What Is The Importance of Demodex Folliculorum in Behcet DiseaseDocument5 pagesWhat Is The Importance of Demodex Folliculorum in Behcet DiseaseRoxana SurliuNo ratings yet
- Rosacea 2022Document10 pagesRosacea 2022ucarecufinochiettoNo ratings yet
- Shikha Shah Acquired Dermal Macular HyperpigmentationDocument11 pagesShikha Shah Acquired Dermal Macular Hyperpigmentationsweetnam09No ratings yet
- Skin Biopsy Techniques For The Internist: Clinical ReviewDocument10 pagesSkin Biopsy Techniques For The Internist: Clinical ReviewUty PutriNo ratings yet
- Darier Disease A Fold (Intertriginous) DermatosisDocument5 pagesDarier Disease A Fold (Intertriginous) Dermatosisdaniel ayllonNo ratings yet
- Acrodermatitis Enteropathica - A Case Report: Rashmi Mittal, Sudha R, Murugan S, Adikrishnan, Shobana S, Anandan SDocument3 pagesAcrodermatitis Enteropathica - A Case Report: Rashmi Mittal, Sudha R, Murugan S, Adikrishnan, Shobana S, Anandan SMarcelitaTaliaDuwiriNo ratings yet
- PoikilodermaDocument5 pagesPoikilodermaDiana NunesNo ratings yet
- Dermoscopy of Pigmented Skin LesionsDocument44 pagesDermoscopy of Pigmented Skin LesionsCocoi Mella100% (2)
- Severe Dermatomyositis With Pronounced GeneralizedDocument4 pagesSevere Dermatomyositis With Pronounced Generalizedvasquezdario29No ratings yet
- International Journal of Infectious DiseasesDocument5 pagesInternational Journal of Infectious Diseasesduverney.gaviriaNo ratings yet
- Phenytoininduced DRESSDocument4 pagesPhenytoininduced DRESSCamille MalilayNo ratings yet
- What Is The Importance of Demodex Folliculorum in Behçet's Disease?Document6 pagesWhat Is The Importance of Demodex Folliculorum in Behçet's Disease?Ghea Tahara SugiantoNo ratings yet
- A Case of Ochronosis Successfully Treated With The Picosecond LaserDocument5 pagesA Case of Ochronosis Successfully Treated With The Picosecond LaserYohan WandishaNo ratings yet
- 2022 37 1 145 147 EngDocument3 pages2022 37 1 145 147 EngAri Tri UtamiNo ratings yet
- A Double-Blind Randomized Controlled Trial CompariDocument7 pagesA Double-Blind Randomized Controlled Trial CompariThe SangeNo ratings yet
- Fixed Drug Eruption Induced by Levocetirizine.11Document3 pagesFixed Drug Eruption Induced by Levocetirizine.11SamKingstoneNo ratings yet
- Ijms 22 05077 v2Document44 pagesIjms 22 05077 v2RIRINNo ratings yet
- Jurnal Kulit AccDocument7 pagesJurnal Kulit AccPutriiNusaGusmaliaNo ratings yet
- Bilgili2011 Nonsteroidal Anti-InflammatoryDocument5 pagesBilgili2011 Nonsteroidal Anti-InflammatoryShelaMaretaNo ratings yet
- Jurnal AccDocument4 pagesJurnal AccOlivia Chandra DeviNo ratings yet
- Simple Approach To Histological Diagnosis of Common Skin Adnexal TumorsDocument11 pagesSimple Approach To Histological Diagnosis of Common Skin Adnexal TumorsThiều Mạnh CườngNo ratings yet
- Ecthyma Gangrenosum in A Neonate Case Report: October 2020Document4 pagesEcthyma Gangrenosum in A Neonate Case Report: October 2020cuteNo ratings yet
- Received: 26/3/2017 Accepted: 22/7/2017Document7 pagesReceived: 26/3/2017 Accepted: 22/7/2017Sergio Revuelta HernándezNo ratings yet
- Clinico Morphological Evaluation of Melasma and Other Hyperpigmentary Disorders of SkinDocument25 pagesClinico Morphological Evaluation of Melasma and Other Hyperpigmentary Disorders of SkinBaru Chandrasekhar RaoNo ratings yet
- Successfull Treatment of Dermatophytosis With Combination of Itraconazole and IsotretinoinDocument5 pagesSuccessfull Treatment of Dermatophytosis With Combination of Itraconazole and IsotretinoinAlfaNo ratings yet
- 16 Exogenous-SharmaS PDFDocument3 pages16 Exogenous-SharmaS PDFlala putriNo ratings yet
- Perioral DermatitisDocument6 pagesPerioral DermatitisYeni OktaviaNo ratings yet
- See DiscussionsDocument8 pagesSee DiscussionsAjri AlonzoNo ratings yet
- Tacrolimus in DermatologyDocument4 pagesTacrolimus in DermatologyDimas PrajagoptaNo ratings yet
- Becker's Nevus With Neurofibromatosis Type 1: Annals of Indian Academy of Neurology February 2015Document4 pagesBecker's Nevus With Neurofibromatosis Type 1: Annals of Indian Academy of Neurology February 2015YesicaNo ratings yet
- 10 Differential Diagnosis of Neonatal ErythrodermaDocument13 pages10 Differential Diagnosis of Neonatal Erythrodermacgs08No ratings yet
- Challenges in Treating Genodermatoses: New Therapies at The HorizonDocument25 pagesChallenges in Treating Genodermatoses: New Therapies at The HorizonJhonnie Gaona CardonaNo ratings yet
- Use of Topical Corticosteroids in Dermatology: An Evidence-Based ApproachDocument14 pagesUse of Topical Corticosteroids in Dermatology: An Evidence-Based ApproachKorry Meliana PangaribuanNo ratings yet
- Topical Rapamycin Solution To Treat Multiple Facial Angiofibromas in A Patient With Tuberous SclerosisDocument3 pagesTopical Rapamycin Solution To Treat Multiple Facial Angiofibromas in A Patient With Tuberous Sclerosisw0rfNo ratings yet
- Diagnóstico en DermatologíaDocument4 pagesDiagnóstico en DermatologíaBrantorseinNo ratings yet
- A Simple Guide to Xeroderma Pigmentosa, Diagnosis, Treatment and Related ConditionsFrom EverandA Simple Guide to Xeroderma Pigmentosa, Diagnosis, Treatment and Related ConditionsNo ratings yet
- Apgenco 2012 Certificate of Fitness 22032012Document2 pagesApgenco 2012 Certificate of Fitness 22032012Veera ChaitanyaNo ratings yet
- Measures of Disease Frequency NOTESDocument22 pagesMeasures of Disease Frequency NOTESSJ Jung100% (1)
- Parainfluenza VirusDocument9 pagesParainfluenza VirusLia Ayu Nur'ainiNo ratings yet
- 1 Benign and Malignant Lesions of The CervixDocument46 pages1 Benign and Malignant Lesions of The CervixRohitNo ratings yet
- BSN 1a Micro para ReportDocument2 pagesBSN 1a Micro para ReportJohn Steven Bringuelo FloroNo ratings yet
- Acute Abdomen (Modified From DR James Roring)Document18 pagesAcute Abdomen (Modified From DR James Roring)Arga KafiNo ratings yet
- Final Research - LeukemiaDocument20 pagesFinal Research - LeukemiaMohammed S. KhalilNo ratings yet
- Acute Diarrhea in Adults and Children A Global PerspectiveDocument10 pagesAcute Diarrhea in Adults and Children A Global PerspectiverobyNo ratings yet
- "Association Splitting" Versus Cognitive Remediation in Obsessive-Compulsive Disorder - A Randomized Controlled TrialDocument39 pages"Association Splitting" Versus Cognitive Remediation in Obsessive-Compulsive Disorder - A Randomized Controlled Trialmahashweta bhattacharyaNo ratings yet
- The Association Between Diabetic Retinopathy, Cognitive Impairment, and Quality of Life A Cross Sectional StudyDocument5 pagesThe Association Between Diabetic Retinopathy, Cognitive Impairment, and Quality of Life A Cross Sectional StudyppdsretinaNo ratings yet
- Black DeathDocument17 pagesBlack Deathapi-350807464No ratings yet
- Day 1 Patient's Name: Mr. X Age: 61 Address: Larap, Jose Panganiban, Camarines Norte Date / Time Focus Data, Action, Response Chest PainDocument4 pagesDay 1 Patient's Name: Mr. X Age: 61 Address: Larap, Jose Panganiban, Camarines Norte Date / Time Focus Data, Action, Response Chest PainJulliza Joy PandiNo ratings yet
- Safer Rimming BrochureDocument2 pagesSafer Rimming BrochureMichael_Bolen1306No ratings yet
- 2018-Rad, Bidi, Khaligh - 2018 - Causes of Late Referral To The Emergency Department in Patients With Myocardial Infarction in IranDocument9 pages2018-Rad, Bidi, Khaligh - 2018 - Causes of Late Referral To The Emergency Department in Patients With Myocardial Infarction in Irancipto susiloNo ratings yet
- Newborn RashDocument20 pagesNewborn RashshamaaroubaNo ratings yet
- Science DengvaxiaDocument2 pagesScience DengvaxiaJan Den Saul DalanNo ratings yet
- Array 3Document2 pagesArray 3api-247458670No ratings yet
- Art Integrated Test Class 4 Anita Pandey (Responses)Document4 pagesArt Integrated Test Class 4 Anita Pandey (Responses)Anita PandeyNo ratings yet
- Public Health & Preventive Medicine - Toronto Notes 2022Document35 pagesPublic Health & Preventive Medicine - Toronto Notes 2022AbdullaNo ratings yet
- Class 3 Anuj UPadhyayDocument3 pagesClass 3 Anuj UPadhyayaayush upadhyayNo ratings yet
- Reviewer - 1. Introduction To ZoonosesDocument4 pagesReviewer - 1. Introduction To ZoonosesGeriel QuidesNo ratings yet
- PhatophysiologyDocument1 pagePhatophysiologymenolzkiNo ratings yet
- Green Book FinalDocument115 pagesGreen Book Finalechspckhammam pcNo ratings yet
- Glomerulonefrita Intrainfectioasa de Cauza StafilococicaDocument7 pagesGlomerulonefrita Intrainfectioasa de Cauza StafilococicaDenisa Carmen ColiofNo ratings yet
- Diseases of The Human Body 6th Edition 6th Edition Ebook PDFDocument61 pagesDiseases of The Human Body 6th Edition 6th Edition Ebook PDFjerry.chadwick517100% (51)
- Data Sheet 2Document3 pagesData Sheet 2survery analysisNo ratings yet
- Case Presentation of Acute PyelonephritisDocument1 pageCase Presentation of Acute PyelonephritisANALYN ANUBNo ratings yet
- Screening IndustryDocument2 pagesScreening Industryrahaman.maNo ratings yet