Professional Documents
Culture Documents
CH 13 CongenitalHeartDefect
CH 13 CongenitalHeartDefect
Uploaded by
Carlo TorresCopyright:
Available Formats
You might also like
- Siretokituzisi Kinobody Superhero Download Xonanub PDFDocument5 pagesSiretokituzisi Kinobody Superhero Download Xonanub PDFRafaela Gomes33% (3)
- Medicine in Brief: Name the Disease in Haiku, Tanka and ArtFrom EverandMedicine in Brief: Name the Disease in Haiku, Tanka and ArtRating: 5 out of 5 stars5/5 (1)
- Essential Principle Checklist For Medical Device Conformity Assessment Other Than IVDDocument3 pagesEssential Principle Checklist For Medical Device Conformity Assessment Other Than IVDkhang baointlNo ratings yet
- Pectus Carinatum, (Pigeon Chest) A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandPectus Carinatum, (Pigeon Chest) A Simple Guide To The Condition, Treatment And Related ConditionsNo ratings yet
- ASEAN Anthem PDFDocument1 pageASEAN Anthem PDFCarlo TorresNo ratings yet
- Midterms Group 5Document25 pagesMidterms Group 5Karina MadriagaNo ratings yet
- Patent Ductus ArteriosusDocument3 pagesPatent Ductus ArteriosusMika SaldañaNo ratings yet
- Patent Ductus ArteriosusDocument6 pagesPatent Ductus ArteriosusnidyaparasayuNo ratings yet
- Atrial Septal DefectDocument5 pagesAtrial Septal DefectAnonymous MWd5UOUuiyNo ratings yet
- Patent Ductus ArteriosusDocument49 pagesPatent Ductus Arteriosusarchana vermaNo ratings yet
- Atrial Septal Defects: What Is It?Document3 pagesAtrial Septal Defects: What Is It?WahyuIrawanNstNo ratings yet
- Patent Ductus Arteriosus NewDocument16 pagesPatent Ductus Arteriosus NewchelNo ratings yet
- Description: Congestive Heart FailureDocument22 pagesDescription: Congestive Heart FailurePinklet Arleena CubianNo ratings yet
- 1.congenital Heart DiseaseDocument60 pages1.congenital Heart Diseasemerzi farooq ahmadkhanNo ratings yet
- Arteriosus Fails To Close After Birth. Early Symptoms Are Uncommon, But in The First Year of Life IncludeDocument3 pagesArteriosus Fails To Close After Birth. Early Symptoms Are Uncommon, But in The First Year of Life IncludeFranz Josef ArnucoNo ratings yet
- Tetralogy of Fallot: What Is It?Document3 pagesTetralogy of Fallot: What Is It?Anditha Namira RSNo ratings yet
- Atrial Septal Defect (ASD)Document12 pagesAtrial Septal Defect (ASD)anggiehardiyantiNo ratings yet
- Patent Ductus Arteriosus (PDA)Document19 pagesPatent Ductus Arteriosus (PDA)putri avriantiNo ratings yet
- Ncma 219 - Alterations in OxygenationDocument1 pageNcma 219 - Alterations in OxygenationKayNo ratings yet
- Ateneo de Zamboanga University College of Nursing NCM 103 DeliverablesDocument6 pagesAteneo de Zamboanga University College of Nursing NCM 103 DeliverablesNoelle HarrisonNo ratings yet
- Coarctation of The AortaDocument4 pagesCoarctation of The AortaChristine Joy CamachoNo ratings yet
- Patent Ductus Arteriosus ClosureDocument7 pagesPatent Ductus Arteriosus ClosureDard TongNo ratings yet
- Atrial Septal DefectDocument3 pagesAtrial Septal Defectmu_crNo ratings yet
- Congenital Heart Disease: PathophysiologyDocument21 pagesCongenital Heart Disease: PathophysiologyChin Chan100% (1)
- Tetralogy of FallotDocument3 pagesTetralogy of FallotyasminNo ratings yet
- Atrial Septal DefectDocument5 pagesAtrial Septal DefectalmorsNo ratings yet
- Tetralogy of Fallot: Normal Heart FunctionDocument4 pagesTetralogy of Fallot: Normal Heart FunctionSoekarno HattaNo ratings yet
- PAVSDMAPCAsDocument3 pagesPAVSDMAPCAsRajesh SharmaNo ratings yet
- Atrial Septal Defect - A ReviewDocument5 pagesAtrial Septal Defect - A ReviewInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Atrial Septal DefectDocument7 pagesAtrial Septal DefectRis Amy AyaNo ratings yet
- Congenital Heart DefectDocument10 pagesCongenital Heart DefectShubhamNo ratings yet
- Congenital HDDocument19 pagesCongenital HDNikhil YadavNo ratings yet
- Congenital Cardiac DefectsDocument40 pagesCongenital Cardiac Defectsstrawberry pieNo ratings yet
- PowerpointDocument12 pagesPowerpointapi-585922320No ratings yet
- CHD Updated March 20Document69 pagesCHD Updated March 20Jibran Jones GarciaNo ratings yet
- Patent Ductus Arteriosus: Patient InformationDocument4 pagesPatent Ductus Arteriosus: Patient InformationPamela JumpNo ratings yet
- Congenital Cardiac Disease: A Guide To Evaluation, Treatment and Anesthetic ManagementDocument87 pagesCongenital Cardiac Disease: A Guide To Evaluation, Treatment and Anesthetic ManagementJZNo ratings yet
- Coarctation of The AortaDocument7 pagesCoarctation of The Aortamharz_astillo100% (1)
- CausesDocument3 pagesCausesCitra WulandariNo ratings yet
- LESSON 3. Congenital Heart DefectsDocument9 pagesLESSON 3. Congenital Heart DefectsEdmarie P. TabacoldeNo ratings yet
- Cardiovascular PDFDocument15 pagesCardiovascular PDFGenki Fay B. LequiganNo ratings yet
- Congenital Heart Disease 1223958712449685 9Document58 pagesCongenital Heart Disease 1223958712449685 9RinaNo ratings yet
- Congenital Heart DefectsDocument13 pagesCongenital Heart DefectsGheluzee Herrera100% (2)
- Congenital Heart Disease (2011)Document17 pagesCongenital Heart Disease (2011)drheay100% (1)
- Tetralogy of FallotDocument5 pagesTetralogy of FallotNoor FadhilaNo ratings yet
- Jurnal Kedokteran Dan Kesehatan IndonesiaDocument10 pagesJurnal Kedokteran Dan Kesehatan IndonesiaIrna WatiNo ratings yet
- Pineda, Jennica BSN 4 Os Dec 17, 2017Document18 pagesPineda, Jennica BSN 4 Os Dec 17, 2017Denise EspinosaNo ratings yet
- PBL 4 - Acyanotic Heart DiseaseDocument27 pagesPBL 4 - Acyanotic Heart DiseaseNadiah Abdul HalimNo ratings yet
- Jurnal Kedokteran Dan Kesehatan Indonesia: Indonesian Journal of Medicine and HealthDocument7 pagesJurnal Kedokteran Dan Kesehatan Indonesia: Indonesian Journal of Medicine and HealthElison J PanggaloNo ratings yet
- Facts About Atrial Septal DefectDocument3 pagesFacts About Atrial Septal DefectBeuty SavitriNo ratings yet
- Congenital Heart Disease: Hema Rajendran B.SC (N) NICU Staff NurseDocument23 pagesCongenital Heart Disease: Hema Rajendran B.SC (N) NICU Staff NurseddNo ratings yet
- Congenital AnomaliesDocument26 pagesCongenital AnomaliesMaria VisitacionNo ratings yet
- Tetralogy of FallotDocument9 pagesTetralogy of FallotPaul MagbooNo ratings yet
- Congenital Heart DefectDocument12 pagesCongenital Heart Defectsangkularosmina837No ratings yet
- Pedia Ward Case ConDocument13 pagesPedia Ward Case ConAnthony Arcenal TarnateNo ratings yet
- Research Paper On Congenital Heart DefectsDocument8 pagesResearch Paper On Congenital Heart Defectspwvgqccnd100% (1)
- Atrial Septal DefectsDocument24 pagesAtrial Septal DefectsSaiaDaphiNo ratings yet
- Komplikasi Tetralogi FallotDocument5 pagesKomplikasi Tetralogi FallotIlhamAkbarNo ratings yet
- Carotid Artery Disease FlyerDocument2 pagesCarotid Artery Disease Flyerdinh son myNo ratings yet
- Anak PDFDocument2 pagesAnak PDFGheavita Chandra DewiNo ratings yet
- Congenital Heart Diseases, A Simple Guide to these Medical ConditionsFrom EverandCongenital Heart Diseases, A Simple Guide to these Medical ConditionsNo ratings yet
- Ventricular Septal Defect, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandVentricular Septal Defect, A Simple Guide To The Condition, Treatment And Related ConditionsNo ratings yet
- Trades Math WorkbookDocument32 pagesTrades Math WorkbookCarlo TorresNo ratings yet
- Harmonized Gender and Development Guidelines (HGDG)Document39 pagesHarmonized Gender and Development Guidelines (HGDG)Carlo Torres100% (3)
- Bneo BGPMSDocument26 pagesBneo BGPMSCarlo TorresNo ratings yet
- Batangan Clincher 2nd QuarterDocument8 pagesBatangan Clincher 2nd QuarterCarlo TorresNo ratings yet
- Vigan SupportDocument1 pageVigan SupportCarlo TorresNo ratings yet
- Sacred Heart College HymnDocument2 pagesSacred Heart College HymnCarlo Torres100% (1)
- Barangay FDPDocument17 pagesBarangay FDPCarlo Torres100% (1)
- BGPMS 2011 5 AreasDocument53 pagesBGPMS 2011 5 AreasCarlo TorresNo ratings yet
- Barangay Assembly DayDocument2 pagesBarangay Assembly DayCarlo TorresNo ratings yet
- Sociology and AnthropologyDocument8 pagesSociology and AnthropologyCarlo Torres100% (1)
- Namcya HandbookDocument64 pagesNamcya HandbookCarlo TorresNo ratings yet
- Patef Program - NC 2010Document2 pagesPatef Program - NC 2010Carlo TorresNo ratings yet
- Rosary Meditations of Montfort PDFDocument16 pagesRosary Meditations of Montfort PDFCarlo Torres0% (1)
- 7sacraments 100331090022 Phpapp01Document37 pages7sacraments 100331090022 Phpapp01Carlo TorresNo ratings yet
- Current Trends and Practices in Social Studies Assessment For The Early GradesDocument4 pagesCurrent Trends and Practices in Social Studies Assessment For The Early GradesCarlo TorresNo ratings yet
- p3 Science Summary Chapter 3, 4, and 5Document3 pagesp3 Science Summary Chapter 3, 4, and 5wilson100% (1)
- Sputum ExamDocument14 pagesSputum ExamJuan MorseNo ratings yet
- Daftar Pustaka Poster PimfiDocument1 pageDaftar Pustaka Poster PimfiRohaniNo ratings yet
- Bio Cls 12 ProjectDocument11 pagesBio Cls 12 ProjectHimani VatsNo ratings yet
- Open University Isced Department of Education Sciences Portuguese Teaching Degree CourseDocument14 pagesOpen University Isced Department of Education Sciences Portuguese Teaching Degree CourseValdemiro NhantumboNo ratings yet
- NExit EssayDocument8 pagesNExit EssayNek Arthur JonathanNo ratings yet
- Country Profile: Philippines: Philippines Community Health Programs JANUARY 2015Document37 pagesCountry Profile: Philippines: Philippines Community Health Programs JANUARY 2015JB VillanuevaNo ratings yet
- EFDA Organogram English VersionDocument6 pagesEFDA Organogram English VersionRobsan YasinNo ratings yet
- Oral Dysfunction in Patients With Head and Neck.10Document14 pagesOral Dysfunction in Patients With Head and Neck.10Yeni PuspitasariNo ratings yet
- OGL 482 Pro-Seminar II Module 6 Assignment: Career Plan TemplateDocument12 pagesOGL 482 Pro-Seminar II Module 6 Assignment: Career Plan Templateapi-410456179No ratings yet
- Heat Stress PlanDocument34 pagesHeat Stress Plan01095902062ahmedNo ratings yet
- Guardian - Dental PPO Plan Summary 2022Document4 pagesGuardian - Dental PPO Plan Summary 2022Jessi ChallagullaNo ratings yet
- Upper GI BleedingDocument30 pagesUpper GI BleedingBibek GhimireNo ratings yet
- Accepted Manuscript: Epilepsy ResearchDocument14 pagesAccepted Manuscript: Epilepsy ResearchSyedNo ratings yet
- Cert IV OHS - WHS Responsibilities and Legislative RequirementsDocument4 pagesCert IV OHS - WHS Responsibilities and Legislative Requirementsdanieljohn810No ratings yet
- Form 2D Health Plan Implementation Pregnancy Prenatal CareDocument2 pagesForm 2D Health Plan Implementation Pregnancy Prenatal CareLora CarpioNo ratings yet
- BIO 155 Spring 2021 SyllabusDocument9 pagesBIO 155 Spring 2021 SyllabusMaria CNo ratings yet
- Ahead,: Is What We AreDocument10 pagesAhead,: Is What We AreKothapalli ChiranjeeviNo ratings yet
- 7 Warning Signs of An Eating DisorderDocument3 pages7 Warning Signs of An Eating DisordermelodyfathiNo ratings yet
- CHN 113 LecDocument5 pagesCHN 113 LecGEOMHAI CATBAGANNo ratings yet
- Disease Impact 2Document31 pagesDisease Impact 2Seed Rock ZooNo ratings yet
- MSDS Cocoa Powder PDFDocument3 pagesMSDS Cocoa Powder PDFkemang 35No ratings yet
- Somatic Therapy: Reporter: Daryl S. AbrahamDocument10 pagesSomatic Therapy: Reporter: Daryl S. AbrahamBiway RegalaNo ratings yet
- E PortfolioDocument6 pagesE Portfolioapi-534188113No ratings yet
- Hao Medical Clnic Family Medicine: Buhangin, Davao CityDocument2 pagesHao Medical Clnic Family Medicine: Buhangin, Davao CityJulie Ann LacandulaNo ratings yet
- BTEC FIRST IN SPORT UNIT 1 Assignment BookletDocument8 pagesBTEC FIRST IN SPORT UNIT 1 Assignment BookletMagin1981No ratings yet
- IPSF Statement:member State Mechanism On SubstandardDocument1 pageIPSF Statement:member State Mechanism On SubstandardInternational Pharmaceutical Students' Federation (IPSF)No ratings yet
- Active Recreation: PE4 QuarterDocument43 pagesActive Recreation: PE4 QuarterIrish Marie BatoctoyNo ratings yet
CH 13 CongenitalHeartDefect
CH 13 CongenitalHeartDefect
Uploaded by
Carlo TorresCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
CH 13 CongenitalHeartDefect
CH 13 CongenitalHeartDefect
Uploaded by
Carlo TorresCopyright:
Available Formats
Patton: Structure & Function of the
Human Body
Connect It!
Congenital Heart Defects
A congenital heart defect is an abnormality of the anatomy of the heart or vessels at birth and is one of
the most common types of birth defects. The defect may disrupt the normal blood flow through the heart
or may have no symptoms. It is estimated that about 8 out of 1,000 live births have this defect. The
causes may range from genetic to environmental. Environmental causes that can alter the development
of the fetal heart include teratogens such as radiation, maternal infection or uncontrolled diabetes, drugs,
and chemicals. Table 1 gives a list of congenital heart defects.
Malformation Incidence per 1 Million Live %
Births
Ventricular septal defect 4,482 42
Atrial septal defect 1,043 10
Pulmonary stenosis 836 8
Patent ductus arteriosus 781 7
Tetralogy of Fallot 577 5
Coarctation of aorta 492 5
Atrioventricular septal defect 396 4
Aortic stenosis 388 4
Transposition of great arteries 388 4
Truncus arteriosus 136 1
Total anomalous pulmonary 120 1
venous connection
Tricuspid atresia 118 1
Total 9,757
Data from Hoffman JI, Kaplan S: The incidence of congenital heart disease. J Am Coll Cardiol 39:1890,
2002. In Kumar V, Abbas AK, Aster JC: Robbins basic pathology, ed 9, Philadelphia, 2013, Saunders.
Because of early detection and surgical techniques, there are many people who survive heart disease
and are able to have productive and healthy lives. A 2010 Olympic gold medal winner had surgery for a
congenital heart defect when he was an infant, showing that early surgical solutions are very successful.
Others patients will need to be monitored and may have to seek medical interventions more frequently.
The future possibility of fetal gene tests and stem cells implanted before birth may be the next level of
treatment.
Exams and Tests
Some structural heart defects may be identified while the fetus is still in the uterus, while others are
identified after the baby is born. Tests include fetal echocardiography using ultrasound, as well as
listening for heart murmurs or extra heart sounds with a stethoscope or using echocardiography after
Copyright © 2020, Elsevier Inc. All rights reserved.
birth. Medical interventions may occur shortly after the baby is born, while some may have heart surgery
before birth. Catheters may also be used to confirm defects.
Symptoms
Severe heart defects may be determined in newborns based on symptoms which include cyanosis (bluish
tint to lips, skin, and fingernail beds), rapid breathing, fatigue, or poor blood circulation. Some children
have no symptoms and do not require treatment.
Treatment
Treatment depends on the type of defect and may include medicines, catheter procedures in which a
small tube is inserted into a vessel to the heart, surgery, and heart transplants. The severity of the
condition as well as the age and health of the child may determine the type of intervention used.
Specific Defects
Two of the congenital heart defects shown in Table 1 are actually normal anatomy for a fetus that fails to
change in the months after birth. While not the most common, they are some of the ones that are the
most reversible. Once condition is patent ductus arteriosus (PDA) (PAT-ent DUK-tus ar-teer-ee-OH-sus
[pee dee ay]). PDA occurs when a vessel between the pulmonary artery and aorta that bypasses the
lungs remains open or patent. The other condition is called patent foramen ovale (PFO) (PAT-ent foh-
RAY-men oh-VAL-ee [pee ef oh]). PFO is an atrial septal defect in which the normal fetal opening
between the right and left atrium fails to close.
Patent Ductus Arteriosus (PDA)
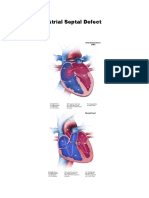
Figure 1, A, shows the normal heart after birth, with a ligament connecting the aorta to the pulmonary
artery where there used to be a vessel or duct in the fetus. This ligament forms within a few days after
birth. The duct in the fetus allows blood to bypass the lungs as the placenta is the organ that is used to
deliver oxygen to the fetus. After birth, the lungs take over the process of obtaining oxygen, requiring the
full delivery of blood from the pulmonary artery.
Copyright © 2020, Elsevier Inc. All rights reserved.
The fetal heart has a normal duct between the pulmonary artery and the aorta. When it remains open
after birth, the condition is called patent ductus arteriosus or simply PDA (Figure 1, B). This condition is
more common in girls, premature infants, babies with Down syndrome, and babies exposed to rubella
while they were in the uterus.
There may not always be symptoms of this condition. When symptoms occur, they may include rapid
breathing, poor feeding, fast heart rate, seating while feeding, poor growth, and fatigue. Diagnosis may
involve listening for murmurs or echocardiogram images. Some conditions are not identified until later in
childhood when symptoms may become more severe.
The duct may close on its own. In premature infants, a PDA may close within 2 years after birth. Other
infants should have closure of the PDA within a few days. PDA surgery may involve a catheter (small
hollow tube) threaded into a blood vessel leading to the heart. The catheter may be used to place a small
metal coil or another plugging device into the duct. If the catheter technique can’t be used, surgery may
be done to tie off the duct after making a small cut between the ribs to reach the PDA.
Medical intervention helps prevent more serious conditions, including heart failure, high blood pressure,
or infection of the inner lining of the heart, from developing. There may also be other congenital defects
that occur with PDA that require the duct to remain open until the other defects are addressed. Medicines
may be used to keep the duct from closing.
Patent Foramen Ovale (PFO) or Atrial Septal Defects (ASD)
The foramen ovale is a normal fetal structure found in the interatrial septum. This opening is another
method (see ductus arteriosus) that allows fetal blood to bypass the lungs which are not yet functioning in
the delivery of oxygen. Blood going from the right atrium into the left atrium will have oxygen obtained
from the placenta. Blood will leave the left atria and go to the left ventricle. The blood then moves out of
the aorta to the organ systems of the body.
Copyright © 2020, Elsevier Inc. All rights reserved.
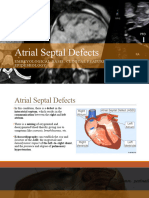
An atrial septal defect (ASD) (AYT-ree-al SEP-tal DEE-fekt [ay es dee]) such as PFO may be genetic or
may be caused by epigenetic changes of genes due to environmental factors. The opening should close
after birth, but 25% of people may have a PFO that doesn’t close and may not cause any symptoms.
An echocardiogram may be used to diagnose a PFO. A transesophageal echo (TEE), which uses a small
ultrasound probe placed in the esophagus, is used to obtain a clear image that avoids sending sound
waves through the outer chest wall. Sometime an infant with PFO will have a bluish skin color (cyanosis)
when straining while crying or having a bowel movement. This condition would indicate that a surgical
solution may be required to close the hole. The oxygen levels would be lower as the blood would travel
from the right atrium to the left atrium and bypass the lungs.
Treatment of PFO depends on the severity of the symptoms. Blood thinners may be used to prevent clots
from traveling to the brain in some patients, while a cardiac catheter can be used to deliver a blocking
device similar to that seen in PDA cases in some situations.
Copyright © 2020, Elsevier Inc. All rights reserved.
You might also like
- Siretokituzisi Kinobody Superhero Download Xonanub PDFDocument5 pagesSiretokituzisi Kinobody Superhero Download Xonanub PDFRafaela Gomes33% (3)
- Medicine in Brief: Name the Disease in Haiku, Tanka and ArtFrom EverandMedicine in Brief: Name the Disease in Haiku, Tanka and ArtRating: 5 out of 5 stars5/5 (1)
- Essential Principle Checklist For Medical Device Conformity Assessment Other Than IVDDocument3 pagesEssential Principle Checklist For Medical Device Conformity Assessment Other Than IVDkhang baointlNo ratings yet
- Pectus Carinatum, (Pigeon Chest) A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandPectus Carinatum, (Pigeon Chest) A Simple Guide To The Condition, Treatment And Related ConditionsNo ratings yet
- ASEAN Anthem PDFDocument1 pageASEAN Anthem PDFCarlo TorresNo ratings yet
- Midterms Group 5Document25 pagesMidterms Group 5Karina MadriagaNo ratings yet
- Patent Ductus ArteriosusDocument3 pagesPatent Ductus ArteriosusMika SaldañaNo ratings yet
- Patent Ductus ArteriosusDocument6 pagesPatent Ductus ArteriosusnidyaparasayuNo ratings yet
- Atrial Septal DefectDocument5 pagesAtrial Septal DefectAnonymous MWd5UOUuiyNo ratings yet
- Patent Ductus ArteriosusDocument49 pagesPatent Ductus Arteriosusarchana vermaNo ratings yet
- Atrial Septal Defects: What Is It?Document3 pagesAtrial Septal Defects: What Is It?WahyuIrawanNstNo ratings yet
- Patent Ductus Arteriosus NewDocument16 pagesPatent Ductus Arteriosus NewchelNo ratings yet
- Description: Congestive Heart FailureDocument22 pagesDescription: Congestive Heart FailurePinklet Arleena CubianNo ratings yet
- 1.congenital Heart DiseaseDocument60 pages1.congenital Heart Diseasemerzi farooq ahmadkhanNo ratings yet
- Arteriosus Fails To Close After Birth. Early Symptoms Are Uncommon, But in The First Year of Life IncludeDocument3 pagesArteriosus Fails To Close After Birth. Early Symptoms Are Uncommon, But in The First Year of Life IncludeFranz Josef ArnucoNo ratings yet
- Tetralogy of Fallot: What Is It?Document3 pagesTetralogy of Fallot: What Is It?Anditha Namira RSNo ratings yet
- Atrial Septal Defect (ASD)Document12 pagesAtrial Septal Defect (ASD)anggiehardiyantiNo ratings yet
- Patent Ductus Arteriosus (PDA)Document19 pagesPatent Ductus Arteriosus (PDA)putri avriantiNo ratings yet
- Ncma 219 - Alterations in OxygenationDocument1 pageNcma 219 - Alterations in OxygenationKayNo ratings yet
- Ateneo de Zamboanga University College of Nursing NCM 103 DeliverablesDocument6 pagesAteneo de Zamboanga University College of Nursing NCM 103 DeliverablesNoelle HarrisonNo ratings yet
- Coarctation of The AortaDocument4 pagesCoarctation of The AortaChristine Joy CamachoNo ratings yet
- Patent Ductus Arteriosus ClosureDocument7 pagesPatent Ductus Arteriosus ClosureDard TongNo ratings yet
- Atrial Septal DefectDocument3 pagesAtrial Septal Defectmu_crNo ratings yet
- Congenital Heart Disease: PathophysiologyDocument21 pagesCongenital Heart Disease: PathophysiologyChin Chan100% (1)
- Tetralogy of FallotDocument3 pagesTetralogy of FallotyasminNo ratings yet
- Atrial Septal DefectDocument5 pagesAtrial Septal DefectalmorsNo ratings yet
- Tetralogy of Fallot: Normal Heart FunctionDocument4 pagesTetralogy of Fallot: Normal Heart FunctionSoekarno HattaNo ratings yet
- PAVSDMAPCAsDocument3 pagesPAVSDMAPCAsRajesh SharmaNo ratings yet
- Atrial Septal Defect - A ReviewDocument5 pagesAtrial Septal Defect - A ReviewInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Atrial Septal DefectDocument7 pagesAtrial Septal DefectRis Amy AyaNo ratings yet
- Congenital Heart DefectDocument10 pagesCongenital Heart DefectShubhamNo ratings yet
- Congenital HDDocument19 pagesCongenital HDNikhil YadavNo ratings yet
- Congenital Cardiac DefectsDocument40 pagesCongenital Cardiac Defectsstrawberry pieNo ratings yet
- PowerpointDocument12 pagesPowerpointapi-585922320No ratings yet
- CHD Updated March 20Document69 pagesCHD Updated March 20Jibran Jones GarciaNo ratings yet
- Patent Ductus Arteriosus: Patient InformationDocument4 pagesPatent Ductus Arteriosus: Patient InformationPamela JumpNo ratings yet
- Congenital Cardiac Disease: A Guide To Evaluation, Treatment and Anesthetic ManagementDocument87 pagesCongenital Cardiac Disease: A Guide To Evaluation, Treatment and Anesthetic ManagementJZNo ratings yet
- Coarctation of The AortaDocument7 pagesCoarctation of The Aortamharz_astillo100% (1)
- CausesDocument3 pagesCausesCitra WulandariNo ratings yet
- LESSON 3. Congenital Heart DefectsDocument9 pagesLESSON 3. Congenital Heart DefectsEdmarie P. TabacoldeNo ratings yet
- Cardiovascular PDFDocument15 pagesCardiovascular PDFGenki Fay B. LequiganNo ratings yet
- Congenital Heart Disease 1223958712449685 9Document58 pagesCongenital Heart Disease 1223958712449685 9RinaNo ratings yet
- Congenital Heart DefectsDocument13 pagesCongenital Heart DefectsGheluzee Herrera100% (2)
- Congenital Heart Disease (2011)Document17 pagesCongenital Heart Disease (2011)drheay100% (1)
- Tetralogy of FallotDocument5 pagesTetralogy of FallotNoor FadhilaNo ratings yet
- Jurnal Kedokteran Dan Kesehatan IndonesiaDocument10 pagesJurnal Kedokteran Dan Kesehatan IndonesiaIrna WatiNo ratings yet
- Pineda, Jennica BSN 4 Os Dec 17, 2017Document18 pagesPineda, Jennica BSN 4 Os Dec 17, 2017Denise EspinosaNo ratings yet
- PBL 4 - Acyanotic Heart DiseaseDocument27 pagesPBL 4 - Acyanotic Heart DiseaseNadiah Abdul HalimNo ratings yet
- Jurnal Kedokteran Dan Kesehatan Indonesia: Indonesian Journal of Medicine and HealthDocument7 pagesJurnal Kedokteran Dan Kesehatan Indonesia: Indonesian Journal of Medicine and HealthElison J PanggaloNo ratings yet
- Facts About Atrial Septal DefectDocument3 pagesFacts About Atrial Septal DefectBeuty SavitriNo ratings yet
- Congenital Heart Disease: Hema Rajendran B.SC (N) NICU Staff NurseDocument23 pagesCongenital Heart Disease: Hema Rajendran B.SC (N) NICU Staff NurseddNo ratings yet
- Congenital AnomaliesDocument26 pagesCongenital AnomaliesMaria VisitacionNo ratings yet
- Tetralogy of FallotDocument9 pagesTetralogy of FallotPaul MagbooNo ratings yet
- Congenital Heart DefectDocument12 pagesCongenital Heart Defectsangkularosmina837No ratings yet
- Pedia Ward Case ConDocument13 pagesPedia Ward Case ConAnthony Arcenal TarnateNo ratings yet
- Research Paper On Congenital Heart DefectsDocument8 pagesResearch Paper On Congenital Heart Defectspwvgqccnd100% (1)
- Atrial Septal DefectsDocument24 pagesAtrial Septal DefectsSaiaDaphiNo ratings yet
- Komplikasi Tetralogi FallotDocument5 pagesKomplikasi Tetralogi FallotIlhamAkbarNo ratings yet
- Carotid Artery Disease FlyerDocument2 pagesCarotid Artery Disease Flyerdinh son myNo ratings yet
- Anak PDFDocument2 pagesAnak PDFGheavita Chandra DewiNo ratings yet
- Congenital Heart Diseases, A Simple Guide to these Medical ConditionsFrom EverandCongenital Heart Diseases, A Simple Guide to these Medical ConditionsNo ratings yet
- Ventricular Septal Defect, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandVentricular Septal Defect, A Simple Guide To The Condition, Treatment And Related ConditionsNo ratings yet
- Trades Math WorkbookDocument32 pagesTrades Math WorkbookCarlo TorresNo ratings yet
- Harmonized Gender and Development Guidelines (HGDG)Document39 pagesHarmonized Gender and Development Guidelines (HGDG)Carlo Torres100% (3)
- Bneo BGPMSDocument26 pagesBneo BGPMSCarlo TorresNo ratings yet
- Batangan Clincher 2nd QuarterDocument8 pagesBatangan Clincher 2nd QuarterCarlo TorresNo ratings yet
- Vigan SupportDocument1 pageVigan SupportCarlo TorresNo ratings yet
- Sacred Heart College HymnDocument2 pagesSacred Heart College HymnCarlo Torres100% (1)
- Barangay FDPDocument17 pagesBarangay FDPCarlo Torres100% (1)
- BGPMS 2011 5 AreasDocument53 pagesBGPMS 2011 5 AreasCarlo TorresNo ratings yet
- Barangay Assembly DayDocument2 pagesBarangay Assembly DayCarlo TorresNo ratings yet
- Sociology and AnthropologyDocument8 pagesSociology and AnthropologyCarlo Torres100% (1)
- Namcya HandbookDocument64 pagesNamcya HandbookCarlo TorresNo ratings yet
- Patef Program - NC 2010Document2 pagesPatef Program - NC 2010Carlo TorresNo ratings yet
- Rosary Meditations of Montfort PDFDocument16 pagesRosary Meditations of Montfort PDFCarlo Torres0% (1)
- 7sacraments 100331090022 Phpapp01Document37 pages7sacraments 100331090022 Phpapp01Carlo TorresNo ratings yet
- Current Trends and Practices in Social Studies Assessment For The Early GradesDocument4 pagesCurrent Trends and Practices in Social Studies Assessment For The Early GradesCarlo TorresNo ratings yet
- p3 Science Summary Chapter 3, 4, and 5Document3 pagesp3 Science Summary Chapter 3, 4, and 5wilson100% (1)
- Sputum ExamDocument14 pagesSputum ExamJuan MorseNo ratings yet
- Daftar Pustaka Poster PimfiDocument1 pageDaftar Pustaka Poster PimfiRohaniNo ratings yet
- Bio Cls 12 ProjectDocument11 pagesBio Cls 12 ProjectHimani VatsNo ratings yet
- Open University Isced Department of Education Sciences Portuguese Teaching Degree CourseDocument14 pagesOpen University Isced Department of Education Sciences Portuguese Teaching Degree CourseValdemiro NhantumboNo ratings yet
- NExit EssayDocument8 pagesNExit EssayNek Arthur JonathanNo ratings yet
- Country Profile: Philippines: Philippines Community Health Programs JANUARY 2015Document37 pagesCountry Profile: Philippines: Philippines Community Health Programs JANUARY 2015JB VillanuevaNo ratings yet
- EFDA Organogram English VersionDocument6 pagesEFDA Organogram English VersionRobsan YasinNo ratings yet
- Oral Dysfunction in Patients With Head and Neck.10Document14 pagesOral Dysfunction in Patients With Head and Neck.10Yeni PuspitasariNo ratings yet
- OGL 482 Pro-Seminar II Module 6 Assignment: Career Plan TemplateDocument12 pagesOGL 482 Pro-Seminar II Module 6 Assignment: Career Plan Templateapi-410456179No ratings yet
- Heat Stress PlanDocument34 pagesHeat Stress Plan01095902062ahmedNo ratings yet
- Guardian - Dental PPO Plan Summary 2022Document4 pagesGuardian - Dental PPO Plan Summary 2022Jessi ChallagullaNo ratings yet
- Upper GI BleedingDocument30 pagesUpper GI BleedingBibek GhimireNo ratings yet
- Accepted Manuscript: Epilepsy ResearchDocument14 pagesAccepted Manuscript: Epilepsy ResearchSyedNo ratings yet
- Cert IV OHS - WHS Responsibilities and Legislative RequirementsDocument4 pagesCert IV OHS - WHS Responsibilities and Legislative Requirementsdanieljohn810No ratings yet
- Form 2D Health Plan Implementation Pregnancy Prenatal CareDocument2 pagesForm 2D Health Plan Implementation Pregnancy Prenatal CareLora CarpioNo ratings yet
- BIO 155 Spring 2021 SyllabusDocument9 pagesBIO 155 Spring 2021 SyllabusMaria CNo ratings yet
- Ahead,: Is What We AreDocument10 pagesAhead,: Is What We AreKothapalli ChiranjeeviNo ratings yet
- 7 Warning Signs of An Eating DisorderDocument3 pages7 Warning Signs of An Eating DisordermelodyfathiNo ratings yet
- CHN 113 LecDocument5 pagesCHN 113 LecGEOMHAI CATBAGANNo ratings yet
- Disease Impact 2Document31 pagesDisease Impact 2Seed Rock ZooNo ratings yet
- MSDS Cocoa Powder PDFDocument3 pagesMSDS Cocoa Powder PDFkemang 35No ratings yet
- Somatic Therapy: Reporter: Daryl S. AbrahamDocument10 pagesSomatic Therapy: Reporter: Daryl S. AbrahamBiway RegalaNo ratings yet
- E PortfolioDocument6 pagesE Portfolioapi-534188113No ratings yet
- Hao Medical Clnic Family Medicine: Buhangin, Davao CityDocument2 pagesHao Medical Clnic Family Medicine: Buhangin, Davao CityJulie Ann LacandulaNo ratings yet
- BTEC FIRST IN SPORT UNIT 1 Assignment BookletDocument8 pagesBTEC FIRST IN SPORT UNIT 1 Assignment BookletMagin1981No ratings yet
- IPSF Statement:member State Mechanism On SubstandardDocument1 pageIPSF Statement:member State Mechanism On SubstandardInternational Pharmaceutical Students' Federation (IPSF)No ratings yet
- Active Recreation: PE4 QuarterDocument43 pagesActive Recreation: PE4 QuarterIrish Marie BatoctoyNo ratings yet