Professional Documents
Culture Documents
0 ratings0% found this document useful (0 votes)
19 viewsCarpal Tunnel Syndrome
Carpal Tunnel Syndrome
Uploaded by
SereinCarpal tunnel syndrome is caused by compression of the median nerve as it travels through the carpal tunnel in the wrist. Early symptoms include pain, numbness and tingling in the thumb, index, middle and radial half of the ring finger. Treatment options include splinting, manual therapy techniques and physical therapy modalities. Skier's thumb refers to a sprain of the ulnar collateral ligament of the thumb caused by forced abduction and hyperextension. It is graded based on the severity of the ligament tear and treated initially with immobilization followed by range of motion and strengthening exercises.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You might also like
- DraftNutritionPlan1 PDFDocument25 pagesDraftNutritionPlan1 PDFJanine Tee100% (5)
- Animal Product ManualDocument720 pagesAnimal Product Manualjq_senNo ratings yet
- Alternative Treatment For Wildlife PDFDocument46 pagesAlternative Treatment For Wildlife PDFPaula Andrea Rodriguez100% (1)
- Dis HandDocument11 pagesDis HandSteven OwensNo ratings yet
- Carpal Tunnel SyndromeDocument5 pagesCarpal Tunnel SyndromeCatherine Camille AvelinoNo ratings yet
- Musculoskeletal Disorders of Elbow, Wrist and HandsDocument59 pagesMusculoskeletal Disorders of Elbow, Wrist and Handssaroj yadavNo ratings yet
- Carpal Tunnel Syndrome InforDocument5 pagesCarpal Tunnel Syndrome InforAnonymous uTEAEbugNo ratings yet
- الفصل الثاني محاضرات PDFDocument20 pagesالفصل الثاني محاضرات PDFAZOZ 19No ratings yet
- Shoulder PathologiesDocument33 pagesShoulder PathologiesjermaineNo ratings yet
- Physical Therapy For Sports Injuries (2012-2013)Document66 pagesPhysical Therapy For Sports Injuries (2012-2013)Mohammad EsmatNo ratings yet
- Carpal Tunnnel Syndrome: EtiologyDocument3 pagesCarpal Tunnnel Syndrome: EtiologyEga FlorenceNo ratings yet
- Carpal Tunnel SyndormeDocument6 pagesCarpal Tunnel SyndormeMAE THERESE MONICITNo ratings yet
- What Is Carpal Tunnel SyndromeDocument3 pagesWhat Is Carpal Tunnel SyndromerutipuspitaNo ratings yet
- Hand & WristDocument56 pagesHand & WristAbdallah Samir Mostafa٢٠١٩٠٢١٥٩No ratings yet
- Trigger Thumb: A. IntroductionDocument6 pagesTrigger Thumb: A. IntroductionrifkizidnyNo ratings yet
- Surgery Ortho - TaskDocument4 pagesSurgery Ortho - TasknicewanNo ratings yet
- Carpal Tunnel SyndromeDocument5 pagesCarpal Tunnel SyndromeBenjo ObsequioNo ratings yet
- Carpal Tunnel SyndromeDocument6 pagesCarpal Tunnel SyndromeRACHELLE ANNE L LUISNo ratings yet
- MSK Viva Voce Lateral EpicondylitisDocument7 pagesMSK Viva Voce Lateral EpicondylitisTing ChenNo ratings yet
- EXP Carpal TunnelDocument7 pagesEXP Carpal TunnelRomelyn OrdillasNo ratings yet
- Carpal Tunnel SyndromeDocument22 pagesCarpal Tunnel SyndromePinimNo ratings yet
- 6 - Injuries To The Ulnar Collateral Ligament o - 2018 - Clinical Orthopaedic Re PDFDocument4 pages6 - Injuries To The Ulnar Collateral Ligament o - 2018 - Clinical Orthopaedic Re PDFTolo CantallopsNo ratings yet
- Rotator Cuff Disorders: Salami Oluwaseyi ODocument16 pagesRotator Cuff Disorders: Salami Oluwaseyi OSalami OluwaseyiNo ratings yet
- DJSJKSDDF FisjDocument16 pagesDJSJKSDDF FisjsharenNo ratings yet
- Acquired DeformitiesDocument6 pagesAcquired DeformitiesAnonymous fVtDc9hNo ratings yet
- Shoulder PainDocument5 pagesShoulder Paindrraj07No ratings yet
- Elbow Injuries and FracturesDocument9 pagesElbow Injuries and FracturesJyoti MaheshwariNo ratings yet
- Elbow Pain.Document47 pagesElbow Pain.salmankhan09215No ratings yet
- OT8 - Thumb Immobilization SplintDocument4 pagesOT8 - Thumb Immobilization SplintAnnbe Barte100% (1)
- Jake PPDocument31 pagesJake PPapi-323342594No ratings yet
- Muscle: Assessed Through Dynamometry, Manual Muscle Strength and Functional StrengthDocument12 pagesMuscle: Assessed Through Dynamometry, Manual Muscle Strength and Functional StrengthArifa ShehzadiNo ratings yet
- Carpal Tunnel SyndromeDocument2 pagesCarpal Tunnel SyndromeHejar A.No ratings yet
- Carpal Tunnel SyndromeDocument6 pagesCarpal Tunnel SyndromeNau HasNo ratings yet
- Referat Claw and Club Hand: Ribka Theodora - Hand 3 Mentor: Dr. Betha Egih Riestiano, Spbp-ReDocument25 pagesReferat Claw and Club Hand: Ribka Theodora - Hand 3 Mentor: Dr. Betha Egih Riestiano, Spbp-ReRibka TheodoraNo ratings yet
- Carpal Tunnel SyndromeDocument7 pagesCarpal Tunnel SyndromeNeecel PastoralNo ratings yet
- Dr. Bramantya SP Ot - Diagnosis and Management in Upper Extremity ProblemDocument3 pagesDr. Bramantya SP Ot - Diagnosis and Management in Upper Extremity ProblemChristian HarnatNo ratings yet
- Degenerative Disc Disease by Dr. BBTDocument11 pagesDegenerative Disc Disease by Dr. BBTBhusan TamrakarNo ratings yet
- Fractures: Pathophysiology and EtiologyDocument5 pagesFractures: Pathophysiology and EtiologyHafid JuniorNo ratings yet
- Carpal Tunnel SyndromeDocument17 pagesCarpal Tunnel SyndromeAstrid IndriatiNo ratings yet
- Skiers ThumbDocument7 pagesSkiers ThumbMufassar NishatNo ratings yet
- Carpal Tunnel Syndrom Wesam Aljabali - 1Document38 pagesCarpal Tunnel Syndrom Wesam Aljabali - 1مركز ريلاكس للعلاج الطبيعيNo ratings yet
- Carpal Tunnel SyndromeDocument2 pagesCarpal Tunnel SyndromeTony HermawanNo ratings yet
- DiagnosissdhDocument6 pagesDiagnosissdhMplusWNo ratings yet
- Johs Trigger DigitsDocument12 pagesJohs Trigger DigitsDanielz FranceNo ratings yet
- Long Bone Fracture Management - Dr. ImanDocument20 pagesLong Bone Fracture Management - Dr. ImanYuliusNo ratings yet
- Lateral Epicondylitis.Document11 pagesLateral Epicondylitis.rabia khalidNo ratings yet
- Carpal Tunnel SyndromeDocument1 pageCarpal Tunnel SyndromekenthepaNo ratings yet
- About Traumatic Brachial Plexus InjuriesDocument5 pagesAbout Traumatic Brachial Plexus InjuriesdoruntineNo ratings yet
- Ulnar Nerve PalsyDocument63 pagesUlnar Nerve PalsyArben Cenollari100% (1)
- Carpal Tunnel Syndrome Fact SheetDocument6 pagesCarpal Tunnel Syndrome Fact SheetTissa RanatungeNo ratings yet
- Arthritis: OsteoarthritisDocument8 pagesArthritis: OsteoarthritisAlex DaniNo ratings yet
- Carpal Tunnel SyndromeDocument29 pagesCarpal Tunnel SyndromeAnn Heerah100% (2)
- Klumpke's ParalysisDocument20 pagesKlumpke's ParalysisRajath Kumar K R KNo ratings yet
- Fractures of Clavicle AserDocument44 pagesFractures of Clavicle AserHeba ElgoharyNo ratings yet
- Carpal Tunnel Syndrome FinalDocument4 pagesCarpal Tunnel Syndrome Finalcatherine_suganob6496100% (2)
- Most Common Diseases of Upper ExtremitiesDocument22 pagesMost Common Diseases of Upper ExtremitiesEliazar Alumbro Peniton Jr.No ratings yet
- 2008 Article 9145-2 PDFDocument7 pages2008 Article 9145-2 PDFDeborah González GarcíaNo ratings yet
- Evaluation and Treatment of Common Musculoskeletal Disorder of The ShoulderDocument42 pagesEvaluation and Treatment of Common Musculoskeletal Disorder of The ShoulderhdthhhhNo ratings yet
- Clavicle FractureDocument27 pagesClavicle FractureOves Patni100% (1)
- Carpal Tunnel SyndromeDocument2 pagesCarpal Tunnel SyndromejunkyardNo ratings yet
- What Is Carpal Tunnel Syndrome?Document4 pagesWhat Is Carpal Tunnel Syndrome?Muhammad Fachry HidayatNo ratings yet
- Cubital Tunnel Syndrome, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandCubital Tunnel Syndrome, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Carpal Tunnel Syndrome, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandCarpal Tunnel Syndrome, A Simple Guide To The Condition, Treatment And Related ConditionsRating: 5 out of 5 stars5/5 (1)
- Acromioclavicular Joint Injuries and Physical Therapy ManagementDocument12 pagesAcromioclavicular Joint Injuries and Physical Therapy ManagementSereinNo ratings yet
- Body CompositionDocument22 pagesBody CompositionSereinNo ratings yet
- Lung SurgeriesDocument43 pagesLung SurgeriesSereinNo ratings yet
- Principles of Fitness Training ProgramDocument8 pagesPrinciples of Fitness Training ProgramSereinNo ratings yet
- Exercise Stress TestingDocument18 pagesExercise Stress TestingSereinNo ratings yet
- Diagnostic Accuracy of Provocative Tests in Lateral EpicondylitisDocument10 pagesDiagnostic Accuracy of Provocative Tests in Lateral EpicondylitisPutu OkaNo ratings yet
- INTRODUCTION of Tuberculosis Final NewDocument2 pagesINTRODUCTION of Tuberculosis Final Newbatch1No ratings yet
- Position Paper ECOFINDocument3 pagesPosition Paper ECOFINGhina N. TashaNo ratings yet
- Bone Mineral Density Test - 2Document2 pagesBone Mineral Density Test - 2Wira DatNo ratings yet
- Music POINTERS TO REVIEWDocument2 pagesMusic POINTERS TO REVIEWRacielle Dame RamiloNo ratings yet
- Caregiving Lesson Quarter ExamsDocument3 pagesCaregiving Lesson Quarter ExamsGlaiza FloresNo ratings yet
- Diseases From AnimalsDocument8 pagesDiseases From AnimalsKash K. AsdaonNo ratings yet
- Test Bank Maternal Child Nursing Care Womens Health 2nd Edition Ward HisleyDocument28 pagesTest Bank Maternal Child Nursing Care Womens Health 2nd Edition Ward Hisleyjeremiahhartfozxmbqayn100% (19)
- Cure AllDocument38 pagesCure AllDanja TešićNo ratings yet
- Dutta 1Document667 pagesDutta 1Jeel GaralaNo ratings yet
- JurnalDocument10 pagesJurnalekalapaleloNo ratings yet
- Eccrine SpiradenomaDocument6 pagesEccrine SpiradenomaDeba P SarmaNo ratings yet
- Biocredit Kores PDFDocument8 pagesBiocredit Kores PDFHeru SubrotoNo ratings yet
- A Survey of Cross-Infection Control Procedures: Knowledge and Attitudes of Turkish DentistsDocument5 pagesA Survey of Cross-Infection Control Procedures: Knowledge and Attitudes of Turkish Dentistsbie2xNo ratings yet
- Placenta Previa Case Study: Adefuin, Jay Rovillos, Noemie MDocument40 pagesPlacenta Previa Case Study: Adefuin, Jay Rovillos, Noemie MMikes CastroNo ratings yet
- Fracture FemurDocument28 pagesFracture FemurKulsoom ShahNo ratings yet
- PharmacologyDocument53 pagesPharmacologyapi-3743565No ratings yet
- Klasifikasi Penyebab KomaDocument19 pagesKlasifikasi Penyebab KomaNoni JacksonNo ratings yet
- A Research Paper Prepared To Fulfill The Requirements of ENGL201 CourseDocument7 pagesA Research Paper Prepared To Fulfill The Requirements of ENGL201 CourseHashem ZohbiNo ratings yet
- Krok Review: How To Prepare Krok TestDocument84 pagesKrok Review: How To Prepare Krok Testgaurav100% (2)
- NBOG's Best Practice Guide: Page 1 of 7Document7 pagesNBOG's Best Practice Guide: Page 1 of 7hitham shehataNo ratings yet
- Drug Study (Vancomycin)Document4 pagesDrug Study (Vancomycin)Jared Niles SantosNo ratings yet
- Veterinary MedicineDocument16 pagesVeterinary Medicineapi-359846566No ratings yet
- Uace Biology Paper 2 2018 Marking GuideDocument7 pagesUace Biology Paper 2 2018 Marking GuideArthurNo ratings yet
- Early Identification and Remediation For Infants With Poor SuckDocument10 pagesEarly Identification and Remediation For Infants With Poor SuckMara CadinoiuNo ratings yet
- Takudzwa Mhishi's SpeechDocument5 pagesTakudzwa Mhishi's SpeechRomeo Mhakayakora100% (1)
- Ob2 Sas 14Document5 pagesOb2 Sas 14Ralph Louie ManagoNo ratings yet
Carpal Tunnel Syndrome
Carpal Tunnel Syndrome
Uploaded by
Serein0 ratings0% found this document useful (0 votes)
19 views27 pagesCarpal tunnel syndrome is caused by compression of the median nerve as it travels through the carpal tunnel in the wrist. Early symptoms include pain, numbness and tingling in the thumb, index, middle and radial half of the ring finger. Treatment options include splinting, manual therapy techniques and physical therapy modalities. Skier's thumb refers to a sprain of the ulnar collateral ligament of the thumb caused by forced abduction and hyperextension. It is graded based on the severity of the ligament tear and treated initially with immobilization followed by range of motion and strengthening exercises.
Original Description:
Original Title
CARPAL TUNNEL SYNDROME
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCarpal tunnel syndrome is caused by compression of the median nerve as it travels through the carpal tunnel in the wrist. Early symptoms include pain, numbness and tingling in the thumb, index, middle and radial half of the ring finger. Treatment options include splinting, manual therapy techniques and physical therapy modalities. Skier's thumb refers to a sprain of the ulnar collateral ligament of the thumb caused by forced abduction and hyperextension. It is graded based on the severity of the ligament tear and treated initially with immobilization followed by range of motion and strengthening exercises.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
0 ratings0% found this document useful (0 votes)
19 views27 pagesCarpal Tunnel Syndrome
Carpal Tunnel Syndrome
Uploaded by
SereinCarpal tunnel syndrome is caused by compression of the median nerve as it travels through the carpal tunnel in the wrist. Early symptoms include pain, numbness and tingling in the thumb, index, middle and radial half of the ring finger. Treatment options include splinting, manual therapy techniques and physical therapy modalities. Skier's thumb refers to a sprain of the ulnar collateral ligament of the thumb caused by forced abduction and hyperextension. It is graded based on the severity of the ligament tear and treated initially with immobilization followed by range of motion and strengthening exercises.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
You are on page 1of 27
CARPAL TUNNEL SYNDROME
Carpal tunnel syndrome (CTS) is an entrapment
neuropathy caused by compression of the median
nerve as it travels through the wrist's carpal
tunnel.
It is the most common nerve
entrapment neuropathy, accounting for 90%
of all neuropathies.
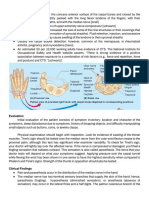
Early symptoms of carpal tunnel syndrome
include pain, numbness, and paraesthesia.
Symptoms typically present, with some
variability, in the thumb, index finger, middle
finger, and the radial half (thumb side) of the
ring finger.
Pain also can radiate up the affected arm.
With further progression, hand weakness,
decreased fine motor coordination,
clumsiness, and thenar atrophy can occur.
Patients can be diagnosed quickly and
respond well to treatment but the best means
of integrating clinical, functional, and
anatomical information for selecting
treatment choices have not yet been
identified.
Aetiology
Carpal tunnel syndrome results from
increased pressure in the carpal tunnel and
subsequent compression of the median
nerve. The most common causes of carpal
tunnel syndrome include genetic
predisposition, history of repetitive wrist
movements such as typing, or machine work
as well as obesity, autoimmune disorders
such as rheumatoid arthritis, and pregnancy.
Pathophysiology
There is a wide spectrum of causative
pathologies, converging on two mechanisms
of disease, both of which lead to entrapment:
A decrease in the size of the carpal tunnel
caused by such conditions as:
Mechanical overuse (considered the
most common association)
Osteoarthritis
Trauma
Acromegaly
Disease states leading to augmentation of
carpal tunnel contents:
Masses, For example, ganglion cysts,
primary nerve sheath tumours
Deposition of foreign material,
e.g., amyloid
Synovial hypertrophy in rheumatoid
arthritis
Clinical Presentation
CTS onset is generally gradual with tingling or
numbness in the median nerve distribution of
the affected hand.
Patients may notice aggravation of symptoms
with static gripping of objects such as a phone
or steering wheel but also at night or early in
the morning. Many patients will report an
improvement of symptoms following shaking
or flicking of their hand.
As the disorder progresses, the feeling
of tingling or numbness may become
constant and patients may complain of
burning pain.
The final symptoms are weakness and
atrophy of muscles of the thenar eminence.
These combined effects of sensory
deprivation and weakness may result in a
complaint of clumsiness and loss of grip and
pinch strength or dropping things,
Physical Therapy Management
Patients with mild to moderate symptoms can
be effectively treated in a primary care
environment
Physical therapists should give advice
on modifications of activities and the
workplace (ergonomic modifications), task
modification, for example, taking sufficient
rest and variation of movements.
Often simple obvious alterations to the
working practice can be beneficial in
controlling milder symptoms of CTS.
Manual therapy techniques
include mobilisation of
Soft tissue
Carpal bone
Median nerve
Other modalities include: ultrasound and
electromagnetic field therapy and splinting.
Research findings (varies)
Physiotherapy modalities
(TENS and ultrasound) have little useful
effects on hand sensory discomfort.
The evidence of the effectiveness of the
exercise and mobilization interventions is
limited and very low in quality.
Evidence about post-operative
rehabilitation is also limited. None of
them seems to have a prevailing benefit
SKIER’S THUMB
Skier's thumb is an acute partial or complete
rupture of the ulnar collateral ligament (UCL)
of the thumb’s metacarpophalangeal joint
(MCPJ) due to a hyperabduction trauma of
the thumb.
Whilst both terms are often used
interchangeably, skier’s thumb refers to the
cause as being acute injury. Gamekeeper’s
thumb specifically refers to the cause being
associated with a chronic injury to the UCL in
which it became attenuated through
repetitive stress.
UCL damage caused by Chronic injury may
have a serious risk of disabling instability,
pinch strength, and pain-free motion if not
treated adequately.
Aetiology
Skier’s thumb is caused by forced abduction
and hyperextension of the thumb. The UCL
tears mostly find place at the distal
attachment of the proximal phalange. But
proximal avulsion, proximal and distal bony
avulsion, isolated mid-substance tears and
mid-substance tears with bony avulsion do
also occur.
Mechanism of Injury
It is important to note that this injury is not
exclusive to skiers and can occur to anyone
where there is an extreme valgus stress force
applied to the thumb in abduction and
extension.
An acute UCL injury occurs following a
sudden, hyperabduction and hyperextension
forces at the MCP joint, whereas a forced
adduction movement would cause injury to
the RCL.
With regards to skiing, the injury often occurs
when a person lands on an outstretched hand
while holding a ski pole, which causes forced
abduction of the thumb with extension.
It is called skier’s thumb but can also occur in
football, handball, basketball, rugby, soccer
and even a handshake. If the injury to the UCL
is not treated properly this can lead to chronic
laxity, joint instability, pain, weakness and
arthritis in the MCPJ.
Clinical Presentation
The most common presentation is pain over
the ulnar aspect of the MCPJ of the thumb. If
the injury is acute there will be bruising and
inflammation.
There may be tenderness with palpation,
which localizes the injury to the ulnar aspect
of the thumb where the UCL is lesioned. In
more chronic cases the patients typically
complain of pain and weakness when using a
pincer grip. There also can be instability of the
thumb while doing these tasks. In the
instance of a Stenner lesion, there may also
be a palpable mass proximal to the adductor
aponeurosis.
Symptoms
These symptoms may occur minutes to hours
after the fall that created the injury:
Pain at the base of the thumb in the web
space between thumb and index finger.
Swelling of your thumb.
Inability to grasp or weakness of grasp
between your thumb and index finger.
Tenderness to the touch along the index
finger side of your thumb.
Blue or black discoloration of the skin over
the thumb.
Thumb pain that worsens with movement
in any or all directions.
Pain in the wrist (which may be referred
pain from your thumb).
Grades of thumb sprains.
Thumb sprains are ranked by how much the
ligament is pulled or torn away from the
bone.
Grade 1: Ligaments are stretched, but not
torn. This is a mild injury. It can improve
with some light stretching.
Grade 2: Ligaments are partially torn (less
than 3mm). This injury may require
wearing a splint or a cast for 5 to 6 weeks.
Grade 3: Ligaments are completely torn or
more than 3mm. This is a severe injury
that usually requires surgery.
Grade 4: Failed immobilization and
required surgery as did all of those with a
Stenner lesion
Physical Therapy Management
The treatment of skier’s thumb is different for
partial and a complete rupture. Partial
ruptures are treated conservatively. The MCP
joint is immobilized, with the MCP fixed and
the IP joint remaining free to prevent
unnecessary stiffness. A navicular cast or
brace is usually used.
Swelling can be controlled with elevation
while supine and the use of cold compresses
as needed.
The primary goal of rehabilitation is
enhancing the patients' function and reducing
the time of functional recovery, the reported
treatment presents potential advantages in
the management of this frequent acute hand
injury.
Conservative treatment
Partial UCL injuries like ligament strains,
partial tears, low-demand patients and poor-
operative candidates, including patients with
degenerative MCP joint disease are effectively
treated conservatively.
Controversy also exists about treating a bony
skier’s thumb without surgery. The literature
however shows that if the MCP joint is stable
during testing and there is no dislocation of
the fragment, this injury can be treated
conservatively without reason for concern.
For patients with:
less than 30 degrees of valgus laxity of
extension of the MCPJ
Less than 15 degrees difference
between sides and no signs of avulsion
fracture on radiographs.
Immobilisation
From 10 days up to 6 weeks, depending on
the degree of laxity during the initial
examination. Authors of a recent review on
skier’s thumb agreed on a 4-week period,
suggestions:
A short-arm thumb spica cast
Thermoplastic splint: allows for the
patient to begin movement of the
interphalangeal joint.
A hand-based removable thumb spica
orthosis. The MCP joint is immobilized,
with the MCP fixed and the IP joint
remaining free to prevent unnecessary
stiffness.
Wearing a splint will avoid putting radial
stress on the thumb and gives the
ligament time to heal. The optimal
positioning for the splint involves holding
the MCPJ in slight flexion with a slight
ulnar deviation; the interphalangeal joints
should not be immobilized in the splint
After the period of immobilization is over, the
therapy can be started. Most likely the
patient will perform exercises that help
strengthen and stretch the joint in order to
regain full function in your thumb. The
patient should begin supervised hand therapy
during the period of immobilization.
Gentle flexion and extension range of motion
exercises can begin after about four weeks,
with the patient continuing to wear the splint
between therapy sessions. After 8 weeks
progressive strengthening exercises may
begin, but unrestricted activity is not allowed
until after 12 weeks.
Gripping and pinching activities should not
start until 10-12 weeks and should be
advanced as tolerated; forceful gripping
activities are typically not tolerated until
about week 12
Treatment after surgery
The content of the physical therapy after
surgery is the same as those of the
conservative treatment, besides:
Duration of Immobilisation: usually 6
weeks is applied
Control radiograph after immobilisation
Following surgery, a splint is usually worn for
four to five weeks. Immediate postoperative
motion of the operated joint produced faster
and better functional results. Therefor the use
of a functional splint is preferred, as well as
the early progressive start with moving within
the boundaries of pain. Athletes whose
injuries require surgery can usually return to
play in about three to four months. The study
of Derkash, considering pain, stability,
muscular force (tweezers grip) and
functionality in ADL, shows that less than 5%
of the patients experience a weakened
tweezers grip and stiffness. Pain was absent
or mild in 99% of the cases. 96% of the
treated patients were satisfied with the
results of the operation. When a secondary
operation is required, results were less
successful.
When the pain has subsided and the range of
motion has completely returned, the hand
can be completely used again. Usually this
takes about 3 months.
Exercises
Thumb active range of motion
With your palm flat on a table or other
surface, move your thumb away from your
palm as far you can. Hold this position for 5
seconds and bring it back to the starting
position. Then rest your hand on the table in a
handshake position. Move your thumb out to
the side away from your palm as far as
possible. Hold for 5 seconds. Return to the
starting position. Next, bring your thumb
across your palm toward your little finger.
Hold this position for 5 seconds. Return to the
starting position. Repeat this entire sequence
15 times. Do 2 sets of 15.
Wrist range of motion
Flexion: Gently bend your wrist forward.
Hold for 5 seconds. Do 2 sets of 15.
Extension: Gently bend your wrist
backward. Hold this position 5 seconds.
Do 2 sets of 15
Side to side: Gently move your wrist from
side to side (a handshake motion). Hold
for 5 seconds in each direction. Do 2 sets
of 15
Thumb strengthening: Pick up small
objects, such as paper clips, pencils, and
coins, using your thumb and each of your
other fingers, one at a time. Practice this
exercise for about 5 minutes
Finger spring: Place a large rubber band
around the outside of your thumb and
fingers. Open your fingers to stretch the
rubber band. Do 2 sets of 15.
Grip strengthening: Squeeze a soft rubber
ball and hold the squeeze for 5 seconds.
Do 2 sets of 15.
Wrist flexion: Hold a can or hammer
handle in your hand with your palm facing
up. Bend your wrist upward. Slowly lower
the weight and return to the starting
position. Do 2 sets of 15. Gradually
increase the weight of the can or weight
you are holding.
Wrist extension: Hold a soup can or
hammer handle in your hand with your
palm facing down. Slowly bend your wrist
up. Slowly lower the weight down into the
starting position. Do 2 sets of 15.
Gradually increase the weight of the
object you are holding.
DUPUYTRENS CONTRACTURE
Dupuytren contracture is a benign,
myeloproliferative progressive disease of the
palmar fascia which results in shortening,
thickening, and fibrosis of the fascia and
aponeurosis of the palm.
Dupuytren disease is predominantly a
myofibroblast disease that affects the
hand/fingers and results in contracture
deformities.
The most commonly affected digits are
the third and fourth digits.
The disease begins in the palm as painless
nodules that form along longitudinal lines
of tension.
The nodules form cords that produce
contracture deformities within fascial
bands and tissues of the hand.
Dupuytren contracture is usually seen in
whites and the disorder is often bilateral;
when unilateral the right side is more
likely to be involved compared to the left.
In many individuals, there is a family
history with males being more likely to be
affected than females.
Aetiology
Dupuytren disease is a genetic disorder
expressed in an autosomal dominant fashion,
but most frequently seen with a multifactorial
aetiology. It is associated with diabetes,
seizure disorders, smoking, alcoholism, HIV,
and vascular disease.
Ectopic manifestations beyond the hand can
be seen in Lederhosen disease (plantar
fascia), 10% to 30%; Peyronie disease (Dartos
fascia of the penis), 2% to 8%; and Garrod
disease (dorsal knuckle pads), 40% to 50%.
Clinical Presentation
Dupuytren contracture occurs slowly and
typically progresses over the course of several
years, but can also develop more rapidly over
weeks or months.
It typically affects older men of European
descent. This condition most commonly
begins with thickening of the skin on the
palm, resulting in a puckering or dimpled
appearance. As the condition progresses,
bands of fibrotic tissue form in the palmar
area and may travel distally toward the
fingers. This tightening and shortening
eventually lead to the affected fingers being
pulled into flexion. Dupuytren contracture
typically occurs bilaterally, with one hand
being more severely affected than the other.
Physical findings:
Blanching of the skin when the finger is
extended
Proximal to the nodules, the cords are
painless
Pits and grooves may be present
The knuckle pads over the PIP joints may
be tender
If the plantar fascia is involved, this
indicates a more severe disease
(Lederhosen disease)
The patient may not be able to place the
palm flat on the table
Physical Therapy Management
Conservative Approach
Physical therapy may
include ultrasound waves: heat (early stage of
the disease); brace/splint to stretch the digits;
a range of motion of the fingers to prevent
adhesions.
Postoperative Care/Rehabilitation
Patients often enter hand therapy to:
Maintain the range of motion of the hand
and fingers is important (for many
activities of daily living), see hand
exercises
Extension splints often are used in
conjunction with other modalities.
Oedema and scar interventions.
Should be undertaken for at least 3
months to prevent contractures.
Maximal benefits of surgery are not
immediate, only become obvious after 6-8
weeks
A standard protocol for postoperative
management of Dupuytren disease is shown
below
Within the initial 5 days postoperative,
the primary interventions are to educate
the patient on decreasing oedema and the
importance of performing a range of
motion exercises on the uninvolved
fingers.
After 5-7 days postoperative, the primary
interventions shift to a range of motion
exercises and splinting.
The exercises are adapted to each
subject’s individual goals and are based
on their impairment, physical status, and
competency.
The types of splints used included volar
splints, dynamic extension splint, dynamic
flexion splints, exercise splints, and wrist
splints.
The key fact to appreciate is that not all patients
need treatment.
There are many treatments available for
Dupuytren contracture and none is ideal or
works consistently.
Only symptomatic patients should be offered
treatment because all treatments have
complications.
The patient must be educated about the
potential complications of treatments, which
are worse than the disorder itself.
Close communication between the team is
essential in order to improve outcomes.
Overall, only a few patients achieve a
desirable result.
In many cases, prolonged physical therapy is
required to restore functionality
You might also like
- DraftNutritionPlan1 PDFDocument25 pagesDraftNutritionPlan1 PDFJanine Tee100% (5)
- Animal Product ManualDocument720 pagesAnimal Product Manualjq_senNo ratings yet
- Alternative Treatment For Wildlife PDFDocument46 pagesAlternative Treatment For Wildlife PDFPaula Andrea Rodriguez100% (1)
- Dis HandDocument11 pagesDis HandSteven OwensNo ratings yet
- Carpal Tunnel SyndromeDocument5 pagesCarpal Tunnel SyndromeCatherine Camille AvelinoNo ratings yet
- Musculoskeletal Disorders of Elbow, Wrist and HandsDocument59 pagesMusculoskeletal Disorders of Elbow, Wrist and Handssaroj yadavNo ratings yet
- Carpal Tunnel Syndrome InforDocument5 pagesCarpal Tunnel Syndrome InforAnonymous uTEAEbugNo ratings yet
- الفصل الثاني محاضرات PDFDocument20 pagesالفصل الثاني محاضرات PDFAZOZ 19No ratings yet
- Shoulder PathologiesDocument33 pagesShoulder PathologiesjermaineNo ratings yet
- Physical Therapy For Sports Injuries (2012-2013)Document66 pagesPhysical Therapy For Sports Injuries (2012-2013)Mohammad EsmatNo ratings yet
- Carpal Tunnnel Syndrome: EtiologyDocument3 pagesCarpal Tunnnel Syndrome: EtiologyEga FlorenceNo ratings yet
- Carpal Tunnel SyndormeDocument6 pagesCarpal Tunnel SyndormeMAE THERESE MONICITNo ratings yet
- What Is Carpal Tunnel SyndromeDocument3 pagesWhat Is Carpal Tunnel SyndromerutipuspitaNo ratings yet
- Hand & WristDocument56 pagesHand & WristAbdallah Samir Mostafa٢٠١٩٠٢١٥٩No ratings yet
- Trigger Thumb: A. IntroductionDocument6 pagesTrigger Thumb: A. IntroductionrifkizidnyNo ratings yet
- Surgery Ortho - TaskDocument4 pagesSurgery Ortho - TasknicewanNo ratings yet
- Carpal Tunnel SyndromeDocument5 pagesCarpal Tunnel SyndromeBenjo ObsequioNo ratings yet
- Carpal Tunnel SyndromeDocument6 pagesCarpal Tunnel SyndromeRACHELLE ANNE L LUISNo ratings yet
- MSK Viva Voce Lateral EpicondylitisDocument7 pagesMSK Viva Voce Lateral EpicondylitisTing ChenNo ratings yet
- EXP Carpal TunnelDocument7 pagesEXP Carpal TunnelRomelyn OrdillasNo ratings yet
- Carpal Tunnel SyndromeDocument22 pagesCarpal Tunnel SyndromePinimNo ratings yet
- 6 - Injuries To The Ulnar Collateral Ligament o - 2018 - Clinical Orthopaedic Re PDFDocument4 pages6 - Injuries To The Ulnar Collateral Ligament o - 2018 - Clinical Orthopaedic Re PDFTolo CantallopsNo ratings yet
- Rotator Cuff Disorders: Salami Oluwaseyi ODocument16 pagesRotator Cuff Disorders: Salami Oluwaseyi OSalami OluwaseyiNo ratings yet
- DJSJKSDDF FisjDocument16 pagesDJSJKSDDF FisjsharenNo ratings yet
- Acquired DeformitiesDocument6 pagesAcquired DeformitiesAnonymous fVtDc9hNo ratings yet
- Shoulder PainDocument5 pagesShoulder Paindrraj07No ratings yet
- Elbow Injuries and FracturesDocument9 pagesElbow Injuries and FracturesJyoti MaheshwariNo ratings yet
- Elbow Pain.Document47 pagesElbow Pain.salmankhan09215No ratings yet
- OT8 - Thumb Immobilization SplintDocument4 pagesOT8 - Thumb Immobilization SplintAnnbe Barte100% (1)
- Jake PPDocument31 pagesJake PPapi-323342594No ratings yet
- Muscle: Assessed Through Dynamometry, Manual Muscle Strength and Functional StrengthDocument12 pagesMuscle: Assessed Through Dynamometry, Manual Muscle Strength and Functional StrengthArifa ShehzadiNo ratings yet
- Carpal Tunnel SyndromeDocument2 pagesCarpal Tunnel SyndromeHejar A.No ratings yet
- Carpal Tunnel SyndromeDocument6 pagesCarpal Tunnel SyndromeNau HasNo ratings yet
- Referat Claw and Club Hand: Ribka Theodora - Hand 3 Mentor: Dr. Betha Egih Riestiano, Spbp-ReDocument25 pagesReferat Claw and Club Hand: Ribka Theodora - Hand 3 Mentor: Dr. Betha Egih Riestiano, Spbp-ReRibka TheodoraNo ratings yet
- Carpal Tunnel SyndromeDocument7 pagesCarpal Tunnel SyndromeNeecel PastoralNo ratings yet
- Dr. Bramantya SP Ot - Diagnosis and Management in Upper Extremity ProblemDocument3 pagesDr. Bramantya SP Ot - Diagnosis and Management in Upper Extremity ProblemChristian HarnatNo ratings yet
- Degenerative Disc Disease by Dr. BBTDocument11 pagesDegenerative Disc Disease by Dr. BBTBhusan TamrakarNo ratings yet
- Fractures: Pathophysiology and EtiologyDocument5 pagesFractures: Pathophysiology and EtiologyHafid JuniorNo ratings yet
- Carpal Tunnel SyndromeDocument17 pagesCarpal Tunnel SyndromeAstrid IndriatiNo ratings yet
- Skiers ThumbDocument7 pagesSkiers ThumbMufassar NishatNo ratings yet
- Carpal Tunnel Syndrom Wesam Aljabali - 1Document38 pagesCarpal Tunnel Syndrom Wesam Aljabali - 1مركز ريلاكس للعلاج الطبيعيNo ratings yet
- Carpal Tunnel SyndromeDocument2 pagesCarpal Tunnel SyndromeTony HermawanNo ratings yet
- DiagnosissdhDocument6 pagesDiagnosissdhMplusWNo ratings yet
- Johs Trigger DigitsDocument12 pagesJohs Trigger DigitsDanielz FranceNo ratings yet
- Long Bone Fracture Management - Dr. ImanDocument20 pagesLong Bone Fracture Management - Dr. ImanYuliusNo ratings yet
- Lateral Epicondylitis.Document11 pagesLateral Epicondylitis.rabia khalidNo ratings yet
- Carpal Tunnel SyndromeDocument1 pageCarpal Tunnel SyndromekenthepaNo ratings yet
- About Traumatic Brachial Plexus InjuriesDocument5 pagesAbout Traumatic Brachial Plexus InjuriesdoruntineNo ratings yet
- Ulnar Nerve PalsyDocument63 pagesUlnar Nerve PalsyArben Cenollari100% (1)
- Carpal Tunnel Syndrome Fact SheetDocument6 pagesCarpal Tunnel Syndrome Fact SheetTissa RanatungeNo ratings yet
- Arthritis: OsteoarthritisDocument8 pagesArthritis: OsteoarthritisAlex DaniNo ratings yet
- Carpal Tunnel SyndromeDocument29 pagesCarpal Tunnel SyndromeAnn Heerah100% (2)
- Klumpke's ParalysisDocument20 pagesKlumpke's ParalysisRajath Kumar K R KNo ratings yet
- Fractures of Clavicle AserDocument44 pagesFractures of Clavicle AserHeba ElgoharyNo ratings yet
- Carpal Tunnel Syndrome FinalDocument4 pagesCarpal Tunnel Syndrome Finalcatherine_suganob6496100% (2)
- Most Common Diseases of Upper ExtremitiesDocument22 pagesMost Common Diseases of Upper ExtremitiesEliazar Alumbro Peniton Jr.No ratings yet
- 2008 Article 9145-2 PDFDocument7 pages2008 Article 9145-2 PDFDeborah González GarcíaNo ratings yet
- Evaluation and Treatment of Common Musculoskeletal Disorder of The ShoulderDocument42 pagesEvaluation and Treatment of Common Musculoskeletal Disorder of The ShoulderhdthhhhNo ratings yet
- Clavicle FractureDocument27 pagesClavicle FractureOves Patni100% (1)
- Carpal Tunnel SyndromeDocument2 pagesCarpal Tunnel SyndromejunkyardNo ratings yet
- What Is Carpal Tunnel Syndrome?Document4 pagesWhat Is Carpal Tunnel Syndrome?Muhammad Fachry HidayatNo ratings yet
- Cubital Tunnel Syndrome, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandCubital Tunnel Syndrome, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Carpal Tunnel Syndrome, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandCarpal Tunnel Syndrome, A Simple Guide To The Condition, Treatment And Related ConditionsRating: 5 out of 5 stars5/5 (1)
- Acromioclavicular Joint Injuries and Physical Therapy ManagementDocument12 pagesAcromioclavicular Joint Injuries and Physical Therapy ManagementSereinNo ratings yet
- Body CompositionDocument22 pagesBody CompositionSereinNo ratings yet
- Lung SurgeriesDocument43 pagesLung SurgeriesSereinNo ratings yet
- Principles of Fitness Training ProgramDocument8 pagesPrinciples of Fitness Training ProgramSereinNo ratings yet
- Exercise Stress TestingDocument18 pagesExercise Stress TestingSereinNo ratings yet
- Diagnostic Accuracy of Provocative Tests in Lateral EpicondylitisDocument10 pagesDiagnostic Accuracy of Provocative Tests in Lateral EpicondylitisPutu OkaNo ratings yet
- INTRODUCTION of Tuberculosis Final NewDocument2 pagesINTRODUCTION of Tuberculosis Final Newbatch1No ratings yet
- Position Paper ECOFINDocument3 pagesPosition Paper ECOFINGhina N. TashaNo ratings yet
- Bone Mineral Density Test - 2Document2 pagesBone Mineral Density Test - 2Wira DatNo ratings yet
- Music POINTERS TO REVIEWDocument2 pagesMusic POINTERS TO REVIEWRacielle Dame RamiloNo ratings yet
- Caregiving Lesson Quarter ExamsDocument3 pagesCaregiving Lesson Quarter ExamsGlaiza FloresNo ratings yet
- Diseases From AnimalsDocument8 pagesDiseases From AnimalsKash K. AsdaonNo ratings yet
- Test Bank Maternal Child Nursing Care Womens Health 2nd Edition Ward HisleyDocument28 pagesTest Bank Maternal Child Nursing Care Womens Health 2nd Edition Ward Hisleyjeremiahhartfozxmbqayn100% (19)
- Cure AllDocument38 pagesCure AllDanja TešićNo ratings yet
- Dutta 1Document667 pagesDutta 1Jeel GaralaNo ratings yet
- JurnalDocument10 pagesJurnalekalapaleloNo ratings yet
- Eccrine SpiradenomaDocument6 pagesEccrine SpiradenomaDeba P SarmaNo ratings yet
- Biocredit Kores PDFDocument8 pagesBiocredit Kores PDFHeru SubrotoNo ratings yet
- A Survey of Cross-Infection Control Procedures: Knowledge and Attitudes of Turkish DentistsDocument5 pagesA Survey of Cross-Infection Control Procedures: Knowledge and Attitudes of Turkish Dentistsbie2xNo ratings yet
- Placenta Previa Case Study: Adefuin, Jay Rovillos, Noemie MDocument40 pagesPlacenta Previa Case Study: Adefuin, Jay Rovillos, Noemie MMikes CastroNo ratings yet
- Fracture FemurDocument28 pagesFracture FemurKulsoom ShahNo ratings yet
- PharmacologyDocument53 pagesPharmacologyapi-3743565No ratings yet
- Klasifikasi Penyebab KomaDocument19 pagesKlasifikasi Penyebab KomaNoni JacksonNo ratings yet
- A Research Paper Prepared To Fulfill The Requirements of ENGL201 CourseDocument7 pagesA Research Paper Prepared To Fulfill The Requirements of ENGL201 CourseHashem ZohbiNo ratings yet
- Krok Review: How To Prepare Krok TestDocument84 pagesKrok Review: How To Prepare Krok Testgaurav100% (2)
- NBOG's Best Practice Guide: Page 1 of 7Document7 pagesNBOG's Best Practice Guide: Page 1 of 7hitham shehataNo ratings yet
- Drug Study (Vancomycin)Document4 pagesDrug Study (Vancomycin)Jared Niles SantosNo ratings yet
- Veterinary MedicineDocument16 pagesVeterinary Medicineapi-359846566No ratings yet
- Uace Biology Paper 2 2018 Marking GuideDocument7 pagesUace Biology Paper 2 2018 Marking GuideArthurNo ratings yet
- Early Identification and Remediation For Infants With Poor SuckDocument10 pagesEarly Identification and Remediation For Infants With Poor SuckMara CadinoiuNo ratings yet
- Takudzwa Mhishi's SpeechDocument5 pagesTakudzwa Mhishi's SpeechRomeo Mhakayakora100% (1)
- Ob2 Sas 14Document5 pagesOb2 Sas 14Ralph Louie ManagoNo ratings yet