Professional Documents
Culture Documents
Surface Anatomy of The Heart: ND RD
Surface Anatomy of The Heart: ND RD
Uploaded by
allenh016Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Surface Anatomy of The Heart: ND RD
Surface Anatomy of The Heart: ND RD
Uploaded by
allenh016Copyright:
Available Formats
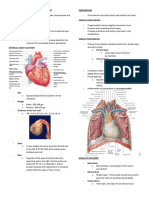
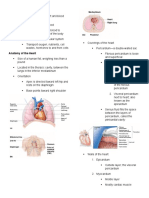
SURFACE ANATOMY OF THE HEART
Approximately in the middle of the thorax
Laterally & posteriorly by the lungs
Anteriorly by sternum & central part of thoracic cage
Borders of the heart
Variable and depend on position of diaphragm & build and physical condition of person
Superior border
Line connecting inferior border of 2nd costal cartilage to superior border of 3rd right costal
cartilage
Right border
Line drawn from 3rd right costal cartilage to 6th right costal cartilage
Slightly convex to the right
Inferior border
Line drawn from inferior end of right border to a point in 5th intercostal space
Close to left MCL
Left end corresponds to location of apex of heart and apex beat
Left Border
Line connecting left ends of the lines representing superior & inferior borders
Valves -> located posterior to sternum
Sounds produced are projected to areas (see figure)
Where stethoscope is placed to avoid intervening bone
APEX BEAT
Mitral Area
Results from apex of heart forced against anterior thoracic wall when LV contracts
Located in 4th or 5th intercostal spaces, 6-10cm from anterior median line
AUSCULTATORY AREAS
Aortic Area
Pulmonary Areas
Tricuspid Area
Mitral Area
© AKMH, Kromos 2023
1
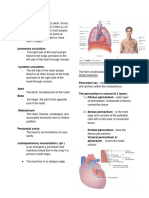
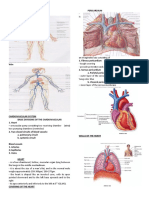
PERICARDIUM Transverse pericardial sinus
Transversely running passage between these 2 groups of vessels and reflections of serous
Found in middle mediastinum pericardium around them
Fibroserous membrane Oblique pericardial sinus
Covers heart & beginning of great vessels Reflection of serous pericardium around 2nd group of vessel
Aortic aorta carries pericardium superiorly beyond heart to level of sternal angle Folding of primordial heart tube
Situated obliquely approximately 2/3 to left and 1/3 to right of median plane Formation of pericardial sinuses during development of heart
Closed sac composed of two layers Venous end moves posterosuperiorly; end lies adjacent to arterial end
Bare area of pericardium -> Separated by transverse pericardial sinus
Serous pericardium Posterior to intrapericardial parts of pulmonary trunk & ascending aorta
Composed mainly of mesothelium Anterior to superior vena cava
Parietal layer Superior to atria of heart
Lines internal surface of fibrous pericardium Developing veins of heart
Visceral layer Surrounded by pericardial reflection forming oblique pericardial sinus
Reflects parietal layer onto heart at great vessels Wide pocket-like recess in pericardial cavity posterior to base of heart
Formed by left atrium
FIBROUS PERICARDIUM
Bounded laterally by pericardial reflections around pulmonary veins & IVC
Tough, external layer Posteriorly by pericardium overlying anterior aspect of esophagus
Continuous with central tendon of diaphragm Can be entered inferiorly & admit several fingers
Continuous superiorly with tunica adventitia of great vessels entering & leaving heart Cannot pass around any of these structures because sinus is blind sac
Also with pretracheal layer of deep cervical fascia
Attached anteriorly to posterior surface of sternum by sternopericardial ligaments
Bound posteriorly by loose connective tissues to structures in posterior mediastinum
Continuous inferiorly with central tendon of the diaphragm
Inseparable; firmly attached and confluent
Tethers heart in place inside fibrous pericardial sac
Floor of diaphragm
Pericardiacophrenic ligament -> site of continuity
Influenced by movement of heart & great vessels, sternum, and diaphragm
Protects heart against sudden overfilling
Due to being unyielding and relation to great vessels piercing it superiorly
PERICARDIAL CAVITY / SINUSES
Potential space between opposing parietal & visceral layers of serous pericardium
Contains fluid enabling heart to move & beat in a frictionless environment
Visceral layer
Forms epicardium
Extends onto beginning of great vessels
Continuous with parietal layer in locations where:
Aorta & pulmonary cavity leave heart
Superior vena cava, inferior vena cava and pulmonary veins enter heart
© AKMH, Kromos 2023
2
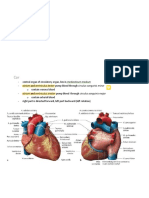
HEART EXTRAS
APEX OF HEART Coronary Sulcus -> demarcates atria from ventricles
Anterior & Posterior Interventricular Sulci -> demarcates right & left ventricle
Formed by inferolateral part of left ventricle
Lies posterior to left 5th intercostal space in adults (insert pictures here)
9cm from median plane
Remains motionless throughout cardiac cycle
Sounds of mitral valve closure are maximal -> apex beat
Underlies mitral area
BASE OF HEART
Posterior aspect of heart; opposite of apex
Formed mainly by left atrium; right atrium has small contribution
Posteriorly faces bodies of T6-T9 vertebrae
Separated by pericardium; oblique pericardial sinus & aorta
Extends superiorly to bifurcation of pulmonary trunk &
inferiorly to coronary sulcus
Receives
Right & left side of left atrial portion: pulmonary veins
Superior & inferior ends of right atrial portion: SVC & IVC
SURFACES OF THE HEART
Anterior (Sternocostal): formed by right ventricle
Diaphragmatic (Inferior): formed mainly by left ventricle & partly by right ventricle
Related to central tendon of diaphragm
Right Pulmonary: formed by right atrium
Left Pulmonary: formed by left ventricle
Forms cardiac impression of left lung
BORDERS OF THE HEART
Right: right atrium extending between SVC & IVC; slightly convex
Inferior: right ventricle & little left ventricle; nearly horizontal
Left: left ventricle & little left auricle; oblique; nearly vertical
Superior: right & left atria and auricles in anterior view
Ascending aorta & pulmonary trunk emerge from this border
SVC enters right side of this border
Forms inferior boundary of transverse pericardial sinus
© AKMH, Kromos 2023
3
CHAMBERS OF THE HEART LEFT ATRIUM
RIGHT ATRIUM Forms most of the base of the heart
Valveless pairs of right & left pulmonary veins enter the atrium
Forms right border of the heart Wall of embryonic pulmonary vein & 4 of its tributaries -> incorporated into wall of left atrium
Receives venous blood from SVC, IVC & coronary sinus Part derived from embryonic pulmonary vein -> smooth walled
Right auricle Left auricle
Projects from right atrium; conical muscular pouch Wall trabeculated with pectinate muscles
Increases capacity of atrium as it overlaps ascending aorta Forms superior part of left border of heart
Interior of right atrium contains: Remains of left part of primordial atrium
Sinus venarum Semilunar depression in interatrial septum -> floor of oval fossa
Vena cavae & coronary sinus open Valve of oval fossa -> surrounding ridge of semilunar depression
Bringing poorly oxygenated blood into heart Interior of left atrium contains:
Pectinate muscles Larger smooth-walled part & smaller muscular auricle containing pectinate muscles
Composes rough, muscular anterior wall 4 pulmonary veins entering smooth posterior wall
Right AV orifice Thicker wall than right atrium
Poorly oxygenated blood into right ventricle Interatrial septum
Smooth & rough parts of atrial wall are separated by: Sloping posteriorly and to the right
Sulcus terminalis (terminal groove) externally; shallow vertical groove Left AV orifice
Crista terminalis (terminal crest) internally; vertical ridge Oxygenated blood from pulmonary veins into left ventricle
Superior vena cava
Opens into superior part at level of right 3rd costal cartilage
Inferior vena cava
Opens into inferior part at level of 5th costal cartilage; almost in line with SVC
Opening of coronary sinus
Between right AV orifice and intraventricular orifice
Interatrial septum
Separates atria
Oval fossa
Oval, thumbprint-size depression
Remnant of oval foramen & its valve in fetus
© AKMH, Kromos 2023
4
RIGHT VENTRICLE Inferiorly -> interventricular septum
Superiorly -> atrioventricular septum
Largest part of anterior surface of heart Separates right atrium from left ventricle
Small part of diaphragmatic surface; entire inferior border of heart Septomarginal trabecula -> curved muscular bundle
Conus arteriosus Traverses right ventricular chamber from inferior part of IVS to base of APM
Leads into pulmonary trunk Carries part of right branch of AV bundle
Interior of right ventricle contains Part of conducting system of heart to APM
Trabeculae carneae -> irregular muscular elevations Facilitate conduction time -> coordinated contraction of APM
Supraventricular crest -> thick muscular ridge Empty & relaxed right ventricle -> contraction of right atrium
Separates ridged muscular wall of inflow part from smooth wall of conus arteriosus Blood forced through () orifice into right ventricle
Inflow part Cusps pushed aside like curtains
Receives blood from right atrium into right AV (tricuspid) orifice Inflow tract -> inflow of blood into right ventricle
Located posterior to body of sternum at level of 4th-5th intercostal spaces Enters posteriorly
Surrounded by one of fibrous rings of fibrous skeleton of the heart Contracting right ventricle
Keep caliber of orifice constant -> large enough to admit tips of three fingers Outflow tract -> outflow of blood into pulmonary trunk
Resist dilation that result from blood being forced through at varying Leaves superiorly and to the left; U-shaped path through right ventricle, 1400
pressures Supraventricular crest deflects:
Tricuspid valve Incoming flow into main cavity of ventricle
Guards right AV orifice Outgoing flow into conus arteriosus towards pulmonary orifice
Bases of valve cusps are attached to fibrous ring around orifice Pulmonary valve -> at apex of conus arteriosus -> level of left 3rd costal cartilage
Contact each other in same way with each heartbeat
Tendinous cords
Attach to anterior, posterior & septal cusps -> cords attaching to parachute
Arise from apices of papillary muscles
Tightened -> prevent separation of cusps & inversion during systole
Prevent cusps from prolapsing
Valve Cusps
Blocks backward flow of blood from right ventricle back to right atrium
During ventricular systole
Papillary muscles
Conical muscular projection with bases attached to ventricular wall
Begin to contract before contraction of right ventricle,
Tightening tendinous cords & draw cusps together
Anterior papillary muscle
Largest & most prominent
Arises from anterior wall of right ventricle
Cords attach to anterior & posterior cusps
Posterior papillary muscle
Smaller than APM (see above)
Arises from inferior wall of right ventricle
Cords attach to posterior & septal cusps
Septal papillary muscle
Arise from interventricular septum; cords attach to anterior & septal cusps
Interventricular septum -> composed of muscular & membranous parts
Partition between right & left ventricles -> forming part of walls of each
Muscular part
Majority of septum
Thickness of remainder of the wall of left ventricle (2-3x thicker than wall of RV)
Bulges into cavity of right ventricle
Membranous part
Found superiorly & posteriorly; smaller
Part of fibrous skeleton of heart
Septal cusp attaches to middle of membranous part
© AKMH, Kromos 2023
5
LEFT VENTRICLE SEMILUNAR VALVES
Forms apex; nearly all left (pulmonary) surface & most diaphragmatic surface Cusps -> concave when viewed superiorly
Performs more work than left ventricle -> systemic pressure > pulmonary pressure Do not have tendinous cords for support
Interior of left ventricle Smaller in area than AV valve cusps
Walls 2-3x thicker than walls of right ventricle Force exerted on them is less than half of tricuspid & mitral valve cusps
Walls covered with trabeculae carneae finer & numerous than right ventricle Project into the artery
Conical activity longer than right ventricle Pressed toward walls as blood leaves ventricle
Anterior & posterior papillary muscles -> larger than in right ventricle Diastole -> relaxation of ventricle
Aortic vestibule Elastic recoil of wall of pulmonary trunk / aorta forces blood back toward heart
Smooth-walled, nonmuscular, supero-anterior outflow part Cusps snap catching reverse blood flow
Leading from ventricular cavity to aortic orifice & aortic valve Close orifice; support each other as edges meet
Mitral valve -> double leaflet Prevent blood from returning to ventricle
Guards left AV orifice Lunule -> thickened edge of cusp in region of contact
Aortic orifice Nodule -> further thickened apex of angulated free edge
Lies in right posterosuperior part Aortic sinuses & sinuses of pulmonary trunk
Surrounded by fibrous ring Formed superior to semilunar cusps; dilated wall of origins of aorta & pulmonary artery
Right posterior & left cusps are attached Spaces at origin of pulmonary trunk & ascending aorta between dilated wall of vessel and each
Beginning of ascending aorta cusp of semilunar valves
Mitral valve Blood in sinuses & dilation of wall prevent cusps from sticking to the wall of vessel, which
Located posterior to sternum at level of 4th costal cartilage might prevent closure
Two cusps: anterior & posterior Right aortic sinus -> mouth of right coronary artery
Recieves tendinous cord from more than 1 papillary muscle Left aortic sinus -> mouth of left coronary artery
Support mitral valve, allows cusps to resist pressure during contractions of LV Posterior aortic sinus -> no artery
Cords become taut -> before & during systole -> cusps resist pressure in contraction
Bloodstream undergoes two right angle turns, result in 1800 change in direction
Takes place around anterior cusp of mitral valve; reversal of flow
Aortic valve -> semilunar valve
Between left ventricle & descending aorta
Located posterior to left side of sternum at level of 3rd intercostal space
© AKMH, Kromos 2023
6
ABNORMALITIES, DISEASES & INJURIES INVOLVING HEART & PERICARDIUM Always result of a valve abnormality; always a chronic process
Insufficiency or regurgitation -> failure of valve to close completely
POSITIONAL ABNORMALITIES OF HEART Owing to nodule formation on cusps -> edges do not meet or align
Result from pathology of valve itself or its supporting structures
Dextrocardia
Acutely -> suddenly (e.g. rupture of cords)
Apex misplaced to right instead of left
Chronically -> over a relatively long time (e.g. scarring and retraction)
Complete reversion of heart position
Both result in increased workload for the heart
Due to abnormal folding of embryonic heart tube to left instead of right
Produces turbulence
Most common positional abnormality of heart; still relatively uncommon
Set up eddies (small whirlpools) -> produce vibrations audible as murmurs
Situs inversus; part of general transposition of thoracic & abdominal viscera
Superficial vibratory sensations (thrills) felt over area of turbulent skin
Low incidence of accompanying cardiac defects; heart functions normally
Clinical significance
Isolated dextrocardia; transposition only affects heart
Ranges from slight & insignificant to severe & rapidly fatal
Complicated by severe cardiac anomalies (e.g. transposition of great arteries)
Factors (e.g. degree, duration & etiology) -> affect secondary changes in heart, blood vessels &
PERICARDITIS, PERICARDIAL RUB & PERICARDIAL EFFUSION other organs, both proximal / distal to valve lesion
May be congenital or acquired
Pericarditis Mechanical problem
Inflammation of pericardium MITRAL VALVE INSUFFICIENCY / MITRAL VALVE PROLAPSE
Make serous pericardium rough -> calcify -> hamper cardiac efficiency Insufficient valve with 1 or both leaflets enlarged extend back to LA during systole
Pericardial friction rub -> rustle of silk over left sternal border & upper ribs Blood regurgitates into LA when LV contracts -> producing murmur
Pericardial effusion PULMONARY VALVE STENOSIS
Passage of fluid from pericardial capillaries into pericardial cavity (pus accumulation) Fused valve cusps -> forms dome with narrow central opening
Often occur with congestive heart failure Infundibular pulmonary stenosis -> underdeveloped conus arteriosus
Venous blood returns to heart at rate exceeding cardiac output Produce restriction of right ventricular outflow
Producing right cardiac hypertension PULMONARY VALVE INCOMPETENCE
Lunules of cusps of a semilunar valve thicken -> become inflexible/damaged by disease ->
CARDIAC TAMPONADE incomplete closure of valve
Results in backrush of blood under high pressure into right ventricle during diastole
Heart compression Produces pulmonic regurgitation -> heard through stethoscope
Increasingly compromised heart volume by fluid outside heart but inside pericardial cavity AORTIC VALVE STENOSIS -> most frequent valve abnormality
Extensive pericardial effusion -> compromised sac volume Result of degenerative calcification; coms to clinical attention in 6th decade of life
-> heart receives limited amount of blood -> reduced cardiac output Results in left ventricular hypertrophy
Hemopericardium -> blood in pericardial cavity -> produces cardiac tamponade AORTIC VALVE INSUFFICIENCY
Result from perforation of weak heart muscle area from previous myocardial infarction results in aortic regurgitation -> produces heart murmur & collapsing pulse
High pressure involved & rapidity of fluid accumulation -> lethal situation
Increasingly compressed heart & circulation fails
Veins become engorged due to blood backup, begins where SVC enters pericardium
Pneumopericardium -> air in pericardial sac
Complication of pneumothorax (air or gas in pleural cavity)
SEPTAL DEFECTS
Atrial Septal Defect (ASD)
Congenital anomaly of interatrial septum
Incomplete closure of oval foramen; patency present in 15-25% of adults
Cause no hemodynamic abnormalities by themselves
No clinical significants and not considered form of ASD by themselves
Clinically significant ASD -> large opening
Ventricular Septal Defect -> membranous part of IVS -> common site
VALVULAR HEART DISEASES
Disturbs pumping efficiency of heart; produces either
Stenosis -> failure of valve to open fully / slowing blood flow from a chamber
© AKMH, Kromos 2023
7
VASCULATURE OF HEART Left coronary artery
Arises from left aortic sinus of ascending aorta
CORONARY ARTERIES Passes between left auricle & left side of pulmonary trunk; runs in coronary sulcus
Typically supplies:
First branch of aorta Left atrium; most of left ventricle; part of right ventricle
Supply myocardium & epicardium Most of IVS
Right & left coronary arteries arise from corresponding aortic sinuses
AV bundle of conducting system of heart, via perforating IV septal branches
At proximal part of ascending aorta, superior to aortic valve, opposite sides of PT
SA node (40% chance)
Supply both atria & ventricles
SA nodal branch
Atrial branches are small and not readily apparent in cadaver
Arises from circumflex branch (40% chance)
Ventrical distribution not sharply demarcated
Divides into two branches at superior end of anterior IV groove
Right coronary artery
Anterior IV branch / LAD
Typically supplies:
Passes along IV groove to apex of heart
Right atrium; most of right ventricle
Turns around inferior border of heart
Diaphragmatic surface (left ventricle); posterior third of IV septum (part only)
Commonly anastomoses with posterior IV branch of RCA
SA node (60% of people); AV node (80% of people)
Supplies adjacent parts of both ventricles
Arises from right aortic sinus of ascending aorta
Passes to right side of pulmonary trunk, running in coronary sulcus Also anterior 2/3 of IVS via IV septal branches
Sino-atrial nodal branch; ascending Gives rise to lateral branch -> descends on anterior surface of heart
Given off near origin Circumflex branch
Supplies SA node Follows coronary sulcus around left border of heart to posterior surface of heart
Right marginal branch Left marginal border -> follows left margin of heart; supplies left ventricle
Given off in descent of RCA in coronary sulcus Terminates in coronary sulcus, but 1/3 continue to supply branch running or adjacent to
Supplies right border of heart as it runs toward apex of heart posterior IV groove
Atrioventricular nodal branch Variations of Coronary arteries
At junction of interatrial & interventricular septa between 4 heart chambers (cross) 67% -> right dominant pattern -> RCA & LCA share equal blood supply of heart
Supplies AV node 15% -> dominant LCA -> posterior IV branch is from circumflex artery
Posterior interventricular branch 18% -> codominance -> artery reach crux & give rise to branches near posterior groove
67% chance -> dominance is typical Few only have 1 coronary artery; 4% have accessory coronary artery
Supplies areas of both ventricles Coronary Collateral Circulation
Sends perforating interventricular septal branches into IV septum Functional end arteries -> coronary arteries
Supply regions of myocardium lacking sufficient anastomoses from other large branches
Maintain viability of tissue should occlusion occur
Anastomoses exist between
coronary arteries (subepicardial / myocardial) & extracardiac vessels (thoracic vessels)
Between terminations of right & left coronary arteries in coronary sulcus & between IV
branches around apex of heart in 10% of hearts
Potential for development of collateral circulation exists in all hearts
© AKMH, Kromos 2023
8
VENOUS DRAINAGE OF HEART INNERVATION OF HEART
Drained mainly by veins emptying into coronary sinus & small veins emptying right atrium Cardiac plexus -> supplies heart with autonomic nerve fibers
Coronary sinus -> main vein of heart Lies on anterior surface of bifurcation of trachea (carina)
Runs from left to right in posterior part of coronary sulcus Commonly observed in dissection after removal of ascending aorta & bifurcation of
Left end: great cardiac vein pulmonary trunk
Right end: middle cardiac vein & small cardiac veins Formed of both sympathetic & parasympathetic fibers en route to heart
Left posterior ventricular vein & left marginal veins also open into sinus As well as visceral afferent fibers - convey reflexive & nociceptive fibers from heart
Great cardiac vein -> main tributary of coronary sinus Divided into:
Anterior interventricular vein -> first part Superficial
Begins near apex of heart & ascends with anterior IV branch (LAD) of LCA Deep
Turns left at coronary sulcus -> second part Sympathetic supply
Runs around left side of heart w/ circumflex branch of LCA to reach coronary sinus From presynaptic fibers
Same direction of blood flow within paired artery & vein Cell bodies in intermediolateral cell column of superior 5/6 thoracic segments
Drains areas of heart supplied by LCA Also from postsynaptic sympathetic fibers
Middle cardiac vein -> accompanies posterior IV branch Cell bodies in cervical & superior thoracic paravertebral ganglia of sympathetic
Small cardiac vein -> accompanies right marginal branch of RCA trunks
Oblique vein of the left atrium (of Marshall) -> relatively unimportant postnatally Traverse cardiopulmonary splanchnic nerves & cardiac plexus
Descends over posterior wall of left atrium End in SA & AV nodes in relation to terminations of parasympathetic fibers
Merges with great cardiac vein to form coronary sinus on coronary arteries
Remnant of embryonic left SVC; atrophies during fetal period Sympathetic stimulation results to:
Occasionally persists in adults; replacing / augmenting SVC Increased heart rate; impulse conduction
Some veins do not drain via coronary sinus Force of contraction
Anterior cardiac vein Increased blood flow through coronary vessels -> support increased activity
Begin over anterior surface of right ventricle, cross coronary sulcus Adrenergic stimulation of SA node & conductive tissue
End directly in right atrium; sometimes enter cardiac vein
Increases pacemaker depolarization rate while increasing AV conduction
Smallest cardiac vein
Direct adrenergic stimulation + indirect suprarenal hormone stimulation
Begin in capillary beds of myocardium & open directly into chamber of heart (atria)
Increases atrial and ventricular contractility
Valveless communications with capillary beds of myocardium
Coronary blood vessel adrenergic receptors = B2 receptorsd
Carry blood from heart chambers to myocardium
Activated -> causes relaxation of vascular smooth muscle -> dilation of artery
LYMPHATIC DRAINAGE OF HEART more oxygen & nutrient supply to myocardium during increased activity
Parasympathetic supply
Subepicardial lymphatic plexus From presynaptic fibers of vagus nerve
Lymphatic vessels in myocardium & subendocardial connective tissue pass here Postsynaptic parasympathetic cell bodies (intrinsic ganglia)
Pass to coronary sulcus and follow coronary arteries Located in atrial wall & interatrial septum near SA & AV nodes & along CA
Lymphatic vessel -> formed by union of various lymphatic vessels of heart -> ascends between Release acetylcholine -> binds with muscarinic receptors
pulmonary trunk & left atrium -> ends in interior tracheobronchial lymph nodes (right side) Decreases pacemaker polarization rate & AV conduction
Decrease atrial contractility
© AKMH, Kromos 2023
9
STIMULATING, CONDUCTING & REGULATING SYSTEM OF HEART Lies on right side of superior mediastinum, anterolateral to trachea & posterolateral to
ascending aorta
Generates & transmits impulses producing coordinated contractions of cardiac cycle
Consist of
Nodal tissue -> initiates heartbeat & coordinates contractions
Conducting fibers -> conduct impulses rapidly to different areas of heart
-> impulses propagated by cardiac striated muscles -> simultaneous contraction
Sino-atrial node
Located anterolaterally, deep to epicardium at junction of SVC & RA, near superior end of
sulcus terminalis
Small collection of nodal tissue, specialized cardiac muscle fibers & associated fibro-elastic
connective tissue
Pacemaker of heart
Initiates and regulates impules for contractions of heart
Gives off an impulse 70x/min
Contraction signal spreads myogenically of both atria
Supplied by sino-atrial nodal artery
Arises either from RCA (60%) or LCA (40%)
Stimulated by sympathetic division of autonomic nervous system
To accelerate heart rate
Inhibited by parasympathetic division to return to / approach its basal rate
Atrioventricular node
Smaller than SA node
Located in postero-inferior region of interatrial septum near opening of coronary sinus
Signal from SA node -> wall of RA + cardiac muscle propagation -> AV node
Distributes signal to ventricles through AV bundle
Supplied by AV nodal artery
Largest & usually first IV septal branch of posterior IV artery
Branch of RCA in 80% of people
RCA usually supplies both SA & AV nodes
AV bundle / Bundle of His
Only bridge between atrial & ventricular myocardium
Passes from AV node through fibrous skeleton of heart along membranous part of IVS
Divides into left & right bundle at junction of membranous & muscular parts of IVS
Proceed on side of muscular IVS deep to endocardium
-> ramify into subendocardial branches -> extend into walls of respective ventricle
Right -> stimulate muscle of IVS, anterior papillary muscle through septomarginal
trabecula, wall of right ventricle
Left -> divides into 6 smaller tracts -> subendocardial branches
Stimulate IVS, anterior & posterior papillary muscles & wall of LV
Traverses center of IVS, anterior two thirds supplied by septal branches of LAD
1. SA node -> AV node -> AV bundle (Bundle of His)
GREAT VESSELS
Brachiocephalic veins (right & left)
Formed posterior to SC joints by union of IJV & subclavian veins
Unite to form SVC at level of inferior border of 1st right costal cartilage
Shunt blood from head, neck, & upper limbs to right atrium
Left is twice as long as right ->
Superior vena cava
Returns blood from all structures superior to diaphragm EXCEPT lungs & heart
Passes inferiorly and ends at level of 3rd costal cartilage -> enter right atrium
© AKMH, Kromos 2023
10
You might also like
- Chapter 12: Heart: Functions of The HeartDocument12 pagesChapter 12: Heart: Functions of The Heartchristian anchetaNo ratings yet
- Cardiovascular System Heart ReviewerDocument8 pagesCardiovascular System Heart ReviewerImmanuel Cris PalasigueNo ratings yet
- First Aid Emergencies: Call/DialDocument5 pagesFirst Aid Emergencies: Call/DialKhalilahmad Khatri100% (1)
- Blodd Cell Poster PDFDocument2 pagesBlodd Cell Poster PDFGustavo Adolfo Piñero BorgesNo ratings yet
- Third Spacing - Where Has All The Fluid GoneDocument14 pagesThird Spacing - Where Has All The Fluid Gonedbryant0101100% (15)
- Anatomy of The HeartDocument3 pagesAnatomy of The HeartCanan YilmazNo ratings yet
- MEDIASTINUMDocument3 pagesMEDIASTINUMlilac.poppy.48No ratings yet
- Cardiovascular SystemDocument9 pagesCardiovascular SystemCrazy StrangerNo ratings yet
- اشرف بيركارديوم اند هارتDocument35 pagesاشرف بيركارديوم اند هارتبيلسان 'نNo ratings yet
- Anatomia InimiiDocument5 pagesAnatomia InimiiMariaa MariutssaNo ratings yet
- HeartDocument7 pagesHeartlilac.poppy.48No ratings yet
- Hap - Circulatory System HeartDocument13 pagesHap - Circulatory System HeartKyle LumingkitNo ratings yet
- Cardiovascular SystemDocument8 pagesCardiovascular SystemHannah Grace CorveraNo ratings yet
- Four Chambers of The HeartDocument7 pagesFour Chambers of The HeartJohn TecsonNo ratings yet
- 10th Week Practical LessonsDocument11 pages10th Week Practical LessonstheodorastanerNo ratings yet
- Four Chambers of The HeartDocument7 pagesFour Chambers of The HeartJohn TecsonNo ratings yet
- Whitaker 2010Document3 pagesWhitaker 2010Gabriel Jose CarvajalNo ratings yet
- Cardiovascular SystemDocument57 pagesCardiovascular SystemSarah Shane Cortes CortesNo ratings yet
- ANPH Wk12 - Cardiovascular SystemDocument17 pagesANPH Wk12 - Cardiovascular SystemSin I GangNo ratings yet
- Heart Finals ReviewerDocument7 pagesHeart Finals ReviewershannenmaehfajanilanNo ratings yet
- Anatomi Kardio PDFDocument49 pagesAnatomi Kardio PDFDestrini Anjani LandaNo ratings yet
- Anatomy Heart PericardiumDocument34 pagesAnatomy Heart PericardiumMICHAEL KEPSEUNo ratings yet
- Surfacwe Anatomy of Cvs and Arterial Puls AreasDocument6 pagesSurfacwe Anatomy of Cvs and Arterial Puls AreasHisham ChomanyNo ratings yet
- Anatomy & Histology of PericardiumDocument2 pagesAnatomy & Histology of PericardiumDila Larasati100% (1)
- CARDIODocument17 pagesCARDIORayana Ubas100% (1)
- Anaphy HeartDocument6 pagesAnaphy HeartAngellene GraceNo ratings yet
- A12. MediastinumDocument29 pagesA12. MediastinumUmerNo ratings yet
- Cardiovascular System: The HeartDocument28 pagesCardiovascular System: The HeartTania Pal ChoudhuryNo ratings yet
- HEARTDocument11 pagesHEARTcatalinaNo ratings yet
- Cardiovascular System WordDocument18 pagesCardiovascular System WordLapitan Jared Anne S.No ratings yet
- CARDIO VASCULAR SYSTEM TransesDocument4 pagesCARDIO VASCULAR SYSTEM TransesBianca Paulyn CastilloNo ratings yet
- CIRCULATORY SYSTEM (Heart)Document4 pagesCIRCULATORY SYSTEM (Heart)Andrei NicoleNo ratings yet
- AP Heart ReviewerDocument7 pagesAP Heart Revieweryes noNo ratings yet
- Kuliah 1 OVERVIEW Titipan Dari (DR Pipiet)Document465 pagesKuliah 1 OVERVIEW Titipan Dari (DR Pipiet)Gangsar DamaiNo ratings yet
- Heart and Blood Vessels, BloodDocument13 pagesHeart and Blood Vessels, BloodDaniel DanielNo ratings yet
- Heart and Its External Features For Paramedical StudentsDocument26 pagesHeart and Its External Features For Paramedical Studentslakshmiraman1770No ratings yet
- 3 MAJOR OPENINGS /right Atirum: Cardiovascular System Serious PericardiumDocument3 pages3 MAJOR OPENINGS /right Atirum: Cardiovascular System Serious PericardiumAebee Alcaraz100% (1)
- CH - 10 - THE CARDIOVASCULAR SYSTEMDocument122 pagesCH - 10 - THE CARDIOVASCULAR SYSTEMCheska DillupacNo ratings yet
- Cardiovascular System - The HeartDocument37 pagesCardiovascular System - The HeartCecil AlbaNo ratings yet
- CARDIOLOGYDocument15 pagesCARDIOLOGYPatty RomeroNo ratings yet
- 9 PericardiumDocument19 pages9 PericardiumAuza Moses Ibrahim100% (2)
- The Cardiovascular SystemDocument17 pagesThe Cardiovascular SystemChris Deinielle Marcoleta Sumaoang100% (1)
- Cardiovascular SystemDocument103 pagesCardiovascular System2022105340No ratings yet
- Anaphy Lab CardioDocument3 pagesAnaphy Lab CardioRyan Dave UmayamNo ratings yet
- CH 21: Cardiovascular System - The HeartDocument21 pagesCH 21: Cardiovascular System - The HeartMadhuri DandamudiNo ratings yet
- Cardiovascular - SummaryDocument18 pagesCardiovascular - Summarys.tinaja.marieantonetteNo ratings yet
- CHAP11Document12 pagesCHAP11Crystal ARIETANo ratings yet
- Heart External AnatomyDocument6 pagesHeart External AnatomyKrissia BaasisNo ratings yet
- BY Ifenna Nnachi Salvator REG NO: 2019070000636Document35 pagesBY Ifenna Nnachi Salvator REG NO: 2019070000636nnachi ifennaNo ratings yet
- MC1 Lec12 13 CardiovascularDocument119 pagesMC1 Lec12 13 CardiovascularVERGEL, Sophia Luis V.No ratings yet
- AnatomyDocument8 pagesAnatomyOM BAWNENo ratings yet
- 1 Pericardium - MbbsDocument34 pages1 Pericardium - MbbsmwadramannNo ratings yet
- CARDIOVASDocument3 pagesCARDIOVASFrama Intan MiguelNo ratings yet
- HeartDocument11 pagesHeartAdamNo ratings yet
- Corazón AnatomicoDocument19 pagesCorazón Anatomicojoselyngarciaga2005No ratings yet
- Mammalian Heart PDFDocument5 pagesMammalian Heart PDFKhaled TurkNo ratings yet
- 1-Heart 2015Document27 pages1-Heart 2015smeersalalNo ratings yet
- Anatomy of The Heart & Its ValvesDocument9 pagesAnatomy of The Heart & Its ValvesJustine CastilloNo ratings yet
- Heart and Neck VesselsDocument31 pagesHeart and Neck Vesselsshellacayetano2No ratings yet
- Cardiology. Section 1. Anatomy of HeartDocument13 pagesCardiology. Section 1. Anatomy of HeartJennifer SteffiNo ratings yet
- CVS and Blood Anatomy - 2Document55 pagesCVS and Blood Anatomy - 2Tharushi PereraNo ratings yet
- Cardiovascular System 1Document66 pagesCardiovascular System 1Mary joy DavidNo ratings yet
- Immediate Life Support for healthcare Practitioners: A Step-By-Step GuideFrom EverandImmediate Life Support for healthcare Practitioners: A Step-By-Step GuideNo ratings yet
- DAN AG Monte Aribal Family Final PaperDocument81 pagesDAN AG Monte Aribal Family Final Paperallenh016No ratings yet
- Batch 2025 (Spirare) : Cebu Institute of Medicine Class ListDocument1 pageBatch 2025 (Spirare) : Cebu Institute of Medicine Class Listallenh016No ratings yet
- Hypothyroidism: Radioiodine Uptake and Thyroid ScanningDocument6 pagesHypothyroidism: Radioiodine Uptake and Thyroid Scanningallenh016No ratings yet
- 2021 Third Exam CoverageDocument3 pages2021 Third Exam Coverageallenh016No ratings yet
- Retinopathy of Prematurity & Retinoblastoma: Salinas & EstellaDocument23 pagesRetinopathy of Prematurity & Retinoblastoma: Salinas & Estellaallenh016No ratings yet
- DOTA 2 Rules Regulations Intramurals 2019Document3 pagesDOTA 2 Rules Regulations Intramurals 2019allenh016No ratings yet
- Strabismus and Amblyopia: Allen Habajab Samantha ReyesDocument23 pagesStrabismus and Amblyopia: Allen Habajab Samantha Reyesallenh016No ratings yet
- Ocular Pharmacology: Salinas EstellaDocument26 pagesOcular Pharmacology: Salinas Estellaallenh016No ratings yet
- MICROB3 - Chapter3 - Cell Structure and FunctionDocument40 pagesMICROB3 - Chapter3 - Cell Structure and FunctionAdriana Corrêa0% (1)
- L3, 16-18 Gross Anatomy of Pelvis and PerineumDocument37 pagesL3, 16-18 Gross Anatomy of Pelvis and PerineumБеатриса ШипNo ratings yet
- 404 - Lipid - ZC# 25-30Document47 pages404 - Lipid - ZC# 25-30fatehatun noorNo ratings yet
- Bahan SupervisiDocument21 pagesBahan SupervisiMeta BachtiarNo ratings yet
- Sepsis and Septic ShockDocument28 pagesSepsis and Septic ShockHayk MinasyanNo ratings yet
- Amino Acids Metabol Synth of UreaDocument32 pagesAmino Acids Metabol Synth of UreaAnastasiafynn100% (1)
- Cap. 06 - Avian Anatomy and PhysiologyDocument65 pagesCap. 06 - Avian Anatomy and PhysiologyNailson JúniorNo ratings yet
- Pain PathwayDocument46 pagesPain PathwayAnil Kumar ReddyNo ratings yet
- Postnatal AssessmentDocument9 pagesPostnatal Assessmentsaleha sultana100% (1)
- Medical For Athletes 1Document2 pagesMedical For Athletes 1Peachy FreezyNo ratings yet
- Lab 3 - Dissection Guide - EarthwormDocument15 pagesLab 3 - Dissection Guide - Earthwormbszool006No ratings yet
- Cell Structure and Functions: Class 8 NCERT Biology Chapter 4Document29 pagesCell Structure and Functions: Class 8 NCERT Biology Chapter 4Chitranshee RastogiNo ratings yet
- Chest PainDocument13 pagesChest Paing3murtulu100% (1)
- SMARTLYTE Quick Setup GuideDocument2 pagesSMARTLYTE Quick Setup GuideSandy KompengNo ratings yet
- Olmetec-Ci e PDFDocument3 pagesOlmetec-Ci e PDFAlyssa Dannah RodriguezNo ratings yet
- Biological Classification Class 11 Notes Biology CDocument14 pagesBiological Classification Class 11 Notes Biology Cdharun0704No ratings yet
- Blood Group Incompatibility RH DiseaseDocument35 pagesBlood Group Incompatibility RH DiseaseRay SadisNo ratings yet
- Chapter 1 The World Through Our SensesDocument18 pagesChapter 1 The World Through Our SensesNurul Ain RazaliNo ratings yet
- Anatomy - Board Ii: Abdomen - Oral PartDocument25 pagesAnatomy - Board Ii: Abdomen - Oral Partbadiuzzaman2010No ratings yet
- Such Thing As An Anion Gap Metabolic Alkalosis. There Is Also No Such ThingDocument3 pagesSuch Thing As An Anion Gap Metabolic Alkalosis. There Is Also No Such ThingMwanja MosesNo ratings yet
- Fatty Acid BiosynthesisDocument7 pagesFatty Acid BiosynthesisJeremiah Eyo AmanamNo ratings yet
- Rules and Regulations For BPTDocument54 pagesRules and Regulations For BPTSherin KNo ratings yet
- An Efficient Chronic Unpredictable Stress Protocol To Induce Stress-Related Responses in C57BL-6 MiceDocument11 pagesAn Efficient Chronic Unpredictable Stress Protocol To Induce Stress-Related Responses in C57BL-6 MiceVampyrgirlNo ratings yet
- Respiratory System ReviewerDocument7 pagesRespiratory System ReviewerVictoria Ellex TiomicoNo ratings yet
- JUJ Pahang SPM 2014 Biology K3 Set 2 SkemaDocument14 pagesJUJ Pahang SPM 2014 Biology K3 Set 2 SkemaCikgu FaizalNo ratings yet
- Test A AnsweredDocument15 pagesTest A AnsweredSarah FathimaNo ratings yet