Professional Documents
Culture Documents
DDS, MSC: Version of Record Doi: 10.1002/JPER.19-0606
DDS, MSC: Version of Record Doi: 10.1002/JPER.19-0606
Uploaded by
Phương Thảo TrầnOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
DDS, MSC: Version of Record Doi: 10.1002/JPER.19-0606
DDS, MSC: Version of Record Doi: 10.1002/JPER.19-0606
Uploaded by
Phương Thảo TrầnCopyright:
Available Formats
Correlation between alveolar bone morphology and volumetric dimensional changes in immediate
maxillary implant placement: a 1-year prospective cohort study.
Tiago Borges*, DDS, MSc, PhD, Danilo Fernandes†, DDS, Bruno Almeida‡, DDS, MSc, Miguel
Pereira‡, DDS, MSc, David Martins†, DDS, Luís Azevedo†, DDS, Tiago Marques‡, DDS, MSc
* Assist. Prof, Universidade Católica Portuguesa, Center for Interdisciplinary Research in Health
(CIIS), Institute of Health Sciences (ICS), Viseu, Portugal
† Universidade Católica Portuguesa, Institute of Health Sciences (ICS), Viseu, Portugal
‡ Universidade Católica Portuguesa, Center for Interdisciplinary Research in Health (CIIS), Institute of
Health Sciences (ICS), Viseu, Portugal
Correspondence to:
DDS MSc PhD, Tiago Borges
Universidade Católica Portuguesa
Estrada da Circunvalação
3504-505 Viseu, Portugal
Phone: (00351) 917411447
Fax: (00351) 273328639
Email: geral@cmeb.pt
Word count: 3,669; Figures: 3; Tables: 3; References: 48
Running title: Alveolar changes and immediate implants
Summary: The current study illustrated the influence of the buccal bone plate thickness in the
dimensional changes that affects the peri-implant tissues after immediate maxillary implant
placement procedures. Findings also show the continuous alveolar volume reduction, mainly during
the first month of healing.
This is the author manuscript accepted for publication and has undergone full peer review but has not
been through the copyediting, typesetting, pagination and proofreading process, which may lead to
differences between this version and the Version of Record. Please cite this article as doi:
10.1002/JPER.19-0606.
This article is protected by copyright. All rights reserved.
Authors contribution: All authors have made substancial contributions to conception and design of
the study. TB has been involved in surgical procedures, data collection and dafting the manuscript.
DF has been involved in data collection, data analysis, data interpretation and drafting the
manuscript. BL, MP, DS, LA and TM have been involved in revising the manuscript and have given the
final approval of the version to be published.
ABSTRACT
Background: After a single tooth extraction, remodelling processes are initiated and
morphological changes occur in the alveolar bone. It has been suggested that implant
placement in a fresh extraction socket may parrtly reduce the alveolar ridge contraction and
that several factors like the thickness of the buccal bone wall and the size of the gap between
the implant and the facial bone wall may play a role on peri-implant tissues dimensional
alterations.
Methods: Twenty-six patients treated with single-tooth maxillary implants were included in this
study. A CBCT exam allowed to access the initial buccal bone thickness (BT). Digital impressions
were taken prior to extractions (T0), one month (T1), four months (T2) and 12 months (T3) after
implant insertion and superimposed with a computer software allowing to quantitatively analyse the
three-dimensional changes occurred in the adjacent tissues. Variables related to thickness, area and
volume were computed.
Results: Participants with BT ≤ 1mm exhibited a significantly increased buccal peri-implant tissue
thickness change than patients with BT > 1mm (p = 0.049). At T3 patients representing BT ≤ 1 mm
exhibited a total volume change of -8.53±5.47% compared with patients presenting BT > 1 mm, -
4.37±2.08%. No statistical significance was found on the distance between implant shoulder and the
buccal bone plate (BID) effect.
Conclusion: After the first year of treatment peri-implant tissues showed continuous changes
resulting in a higher thickness and volume reduction at thin buccal bone plates.
This article is protected by copyright. All rights reserved.
Key Words: dental implants, alveolar ridge augmentation, alveolar bone loss, three-dimensional
imaging, treatment outcome, wound healing.
Introduction
After a single-tooth extraction, the remodelling processes that occur in the alveolar bone have been
proved to take place horizontally, mostly on the buccal aspect of the ridge, followed by the
appearance of a vertical defect.1-4 These outcomes may result in an aesthetic compromise which can
manifest as either a vertical recession in the mid-facial or interdental area, loss of buccal contours in
the horizontal dimension, or differing tissue colour and surface texture.5 These changes to the hard
tissues and surrounding mucosa can be more challenging in the anterior maxilla due to the demand
for satisfactory results.
The literature has suggested that an implant placement in a fresh extraction socket may partly
reduce the alveolar ridge contraction after a tooth extraction,6 but recent clinical evidence shows
that the resorption of the buccal plate will still happen, both vertically and horizontally.7-9 In previous
publications, investigators stated that a careful case selection with intact bone walls, a lingualized
position of the implant, adequate primary stability and the clinician’s expertise need to be
considered as essential parameters to achieve a solid aesthetic outcome with this treatment
modality.10, 11 Several factors have been suggested as affecting the resorption of alveolar bone crest
in immediate implantation including the thickness of the buccal bone wall, the gingival
thickness/biotype, flap or flapless technique, distance from the implant platform to the crestal bone,
surface coating/design, and the size of the gap between the implant and the wall of the alveolar
socket.1, 12, 13 Over the years, strategies have been refined for the reduction of the bone remodelling
and peri-implant mucosal changes in immediate implant insertion in the maxilla. The treatment
modalities described include the placement of autogenous bone to fill the space between the
implant and the buccal bone wall, the placement of deproteinised bovine bone mineral (DBBM) in
This article is protected by copyright. All rights reserved.
the marginal gap between an immediate implant and the socket walls and the use of a connective
tissue graft.14-16
Although several authors14-16 report that there are some advantages with the use of these
techniques, it is difficult to predict with precision what will happen after immediate implant
placement in the aesthetic zone of the maxilla since it involves hard and soft tissue volume changes.
To understand the behaviour of peri-implant tissues, three-dimensional imaging methods have been
increasingly used to obtain a digital evaluation of the area.16-21 These comparison methods have the
potential to dynamically assess the changes that occur in a pre-defined alveolar area during a
timeline of treatment, as well as correlate them with distinct variables that potentially influence the
treatment outcomes. Initial alveolar bone features like the buccal plate thickness, the size of the gap
between the inner buccal bone cortical and the implant, or the buccal-lingual distance at the fresh
socket area, have been described as influencing peri-implant tissue changes.9, 22, 23
However,
different conclusions can be found in the literature regarding the importance of the bone
morphology as a predictor factor in terms of treatment outcome in maxillary immediate implant
placement.24
The purpose of this investigation is to correlate the initial alveolar bone features with the alveolar
volumetric changes that occur in post-extraction maxillary immediate implant installation in the
aesthetic zone after the first year of treatment.
Material and methods
Study design
The present investigation was designed as a prospective cohort study of implants placed in fresh
post-extraction sites. Twenty-six consecutive patients in need of a single-implant restoration in the
maxillary arch following tooth extraction were enrolled in this study. Patients were treated between
January 2018 and January 2019 at the Dentistry School of the Catholic University of Portugal, Viseu,
This article is protected by copyright. All rights reserved.
Portugal. The protocol for the present study was reviewed and approved by the Institute of
Bioethics of the Catholic University of Portugal (ERS 10A.2018). All patients included were previously
informed and agreed with written consent to participate in this study in accordance with the 1975
Declaration of Helsinki, revised in 2013. Patients’ inclusion criteria were: 1) ≥18 years of age; 2)
patients who had a failing tooth and needed an implant placing therapy in the aesthetic zone
(between 15-25); 3) the failing tooth has adjacent and opposing natural teeth; 4) sufficient mesial–
distal and inter-occlusal space for placement of the implant and definitive restoration; 5) had an
intact socket wall previously to the extraction; and 6) had sufficient apical bone to place an
immediate implant with a minimum primary stability of 30 N/cm. Exclusion criteria were: individuals
diagnosed with periodontal disease; medical and general contraindications for the surgical
procedure; heavy smokers (> 10 cigarettes/day); and an active infection at the implant site. A
STROBE checklist was performed in order to consider an appropriate guideline for observational
studies.25
Surgical protocol
The surgical procedure was conducted under local anaesthesia 4% articaine
•
UbistesinTM, 3M-ESPE, St. Paul, MN, USA;
*
OsseoSpeed EV™, AstraTech Implant System, Dentsply Implants, Möhndal, Sweden.
# ®
Symbios , Dentsply Implants, Möhndal, Sweden;
** ®
Mucograf Seal , Geistlish Biomaterials, Wolhusen, Switzerland;
TM
Seralon , Serag-Wiessner, Nalia, Germany;
†
Cerec Omnicam®, Sirona Dental Systems GmbH, Bensheim, Germany;
‡
Ortophos XG 3D®, Sirona Dental Systems GmbH, Bensheim, Germany;
§
PCB 12; Hu-Friedy, Chicago, IL, USA.
Geomagic Control X®, Geomagic, Inc., North Carolina, USA
Materialise Magics®, Materialise, Leuven, Belgium
Materialise Mimics®, Materialise, Leuven, Belgium
¥
SPSS™, Statistical Package for the Social Sciences, version 21.0, IBM Corporation, Armonk, NY, USA
This article is protected by copyright. All rights reserved.
with adrenaline 1:100000•. Flapless tooth extractions were performed after sectioning the tooth,
followed by the use of periotomes and elevators to separate the two parts of the tooth, avoiding
damage to the buccal and palatal bone plates. The socket was inspected to search for any
fenestration or dehiscence of the bone walls, which would have led to exclusion of the patient. All
patients were treated with cylindrical shape implants* with a narrow diameter internal connection
platform following the surgical sequence protocol provided by the manufacturer. The implant was
placed in a correct three-dimensional position, engaging the palatal and apical bone to achieve high
primary stability.26 After implant insertion, a gap of at least 2 mm between the inner cortical buccal
bone plate and the implant surface was filled with a DBBM material# and the socket was sealed with
a resorbable collagen membrane** stabilised with single interrupted 6/0 polyamide sutures. All
surgical procedures were performed by one experienced surgeon (T.B.). The patients had provisional
resin bonded crowns to the adjacent teeth on the same day as the implant surgery; these were in
place for 16 weeks. Postoperative instructions were given to the patients, which included oral
hygiene procedures, chlorhexidine 0.12% rinsing and medication (Paracetamol 1000 mg, ibuprofen
600 mg and amoxicillin 500 mg three times per day for five days). Sutures were removed 10 days
after surgery. A screw-retained provisional crown was delivered after four months of healing and
definitive restorations were inserted at the six-month appointment.
Clinical examination and image acquisition
Examination protocol and data collection consisted of four appointments: 1) T0 (flapless tooth
extraction and implant insertion; 2) T1 (1-month follow-up after implant placement; 3) T2 (4-month
follow-up after implant insertion) and 4) T3 (1-year postoperative follow-up). An intraoral optical
scan† of the upper arch and a CBCT‡ radiographic evaluation were performed followed by tooth
extraction and implant placement (T0). At this point, two clinical parameters were assessed with a
periodontal probe§ to the nearest millimetre: BID (distance between implant shoulder and the
buccal bone plate) and KM (distance between the gingival groove and the mucogingival junction).
This article is protected by copyright. All rights reserved.
Intraoral scans were completed post-implant placement at one month (T1), four months (T2) and
twelve months (T3). In all follow-up appointments hygiene instructions were given to the patients
and a periodontal care was executed when necessary.
Matching digital models
All digital models were exported from the intraoral optical scan† in STL format and were viewed with
Geomagic Control X. The T0 and T1, T0 and T2, and T0 and T3 STL files were overlapped and a strict
alignment was made into one common coordinate system. A final alignment was done through the
best fit alignment algorithm for a perfect match of digital models and executed with settings
adjusted to the oral cavity.27, 28
Examiner calibration method of digital measurements
A protocol was developed to study the variables of interest in three different computer softwares, ,
. One examiner (D.F), blinded for the surgical procedure, was calibrated by a specialist in the three
software programs used in this study. Calibration was only accepted when 90% of the registers were
within a 0.2 mm difference. Also, an intra-examiner calibration was achieved by Dahlberg d-value
through a double consecutive data collection of 10 randomly chosen patients included in this study.
An intra-class coefficient of 0.91 was obtained.
Linear and volumetric measurements
After the superimposition of digital models, a colour map was created to quantitatively analyse the
three-dimensional changes occurring in the surgical areas and adjacent tissues. Green areas
correspond to the perfect alignment of the model. The variation between yellow and red represents
changes of volumetric increase, whereas the variations between light blue and dark blue represent
the changes of volumetric decrease. A region of interest (ROI) with 10 section planes, perpendicular
to the coronal section of the tooth, was computed at buccal and palatal aspect (Figure 1). These
sections were set at the most apical point of the gingival margin and ended 5 mm above it. Mesially
This article is protected by copyright. All rights reserved.
and distally, a line passing through the interproximal area limited the region of interest. The same
ROI was used in each patient, at the different comparison points. The intersection of these sections
with the overlapping models allowed the linear changes to be obtained in each area. The Mean
Buccal Change (MBC0-1, MBC0-2, and MBC0-3) and Mean Total Change (MTC0-1, MTC0-2 and MTC0-3)
were calculated in millimetres (mm) to evaluate the changes that occurred in peri-implant contour
(Figure 2).
Digital models were superimposed in a computer software, and then exported to a different
computer software for volumetric assessement. A volumetric ROI was manually selected with “Cut
or Punch” function using interproximal areas as mesial and distal limits. All cuts were performed in
the same way in all digital models so that all measurements were carried out in the same areas. ROI
volume at T0 was computed for further comparison with consecutive volume change values (Figure
3). The 3D-analysis was conducted with “Boolean” functions, which allowed researchers to obtain
the volume change in each time point from different variables like the Buccal Volume Change (BVC0-1,
BVC0-2, and BVC0-3) and Total Volume Change (TVC0-1, TVC0-2, e TVC0-3), computed in cubic millimetres
(mm3). To allow a direct comparison of different sites at different time points, relative percentages
of these variables were calculated based on the ROI volume at T0.20 All measurements were
recorded to the nearest 0.01 mm.
Radiographic assessment
The acquisition of radiographic images was performed with a volumetric dimension of 8 x 8 cm for
14s with the XG 3D tomography acquisition protocol, with a voxel size of 0.1 mm in HD mode. The
CBCT images were imported in a DICOM format to a computer software to perform the
measurements. Buccal plate thickness (BT) was assessed for 3D radiographic analysis to evaluate the
initial features of the alveolar bone. All measurements were obtained through coronal slice
reconstructions, using an adjacent line to the sinus/nasal plate as a reference. BT was measured 1
mm above the coronal bone margin using a central slice, as well at the mesial and distal slices,
This article is protected by copyright. All rights reserved.
ranging 1 mm from the central slice. Mean BT values were obtained as the average values of the
three slices. One independent examiner who was not involved in the study executed all
measurements.
Statistical analysis
The outcome variables were presented as mean values, standard deviation and 95% confidence
interval. Measurement time (T1, T2 and T3) was considered as a factor and the following as
covariates: age, gender, KM height, location, implant length, BID and BT. The statistical analysis was
performed using a computer software¥. The Mann–Whitney U-test was used to disclose differences
for continuous non-paired variables. Moreover, the paired Wilcoxon test was used when the normal
distribution of the groups was proved. A multiple linear regression model, using the stepwise
forward method, was built to analyse the effect of the tested treatment in the main outcome
variables throughout the study. All hypothesis tests were conducted at the 5% level of significance.
Results
Patients and implants
Details regarding patient characteristics at baseline are shown in Table 1. Twenty-six patients with a
mean age of 53.04 +/- 12.11 (range from 34 to 85) who had been treated with 26 single-tooth
immediate implants were examined. In all, 46.15% of the patients (n=12) were males and 53.85%
were females (n=14). No biological complications occurred in any included patients or implant sites
during the follow-up period. No technical complications were recorded during the 12-month follow-
up. Sample size and power calculation were computed taking into consideration a significance value
of α = 0.05 (type I error) and the power at β = 5.09% (type II error) obtaining a sample size power of
94,9%.
Radiographic measurements
This article is protected by copyright. All rights reserved.
A CBCT analysis allowed computing the BT values through the three measurements from three
adjacent slices. This variable showed a mean value of 1.02±0.62 mm (ranging from 0.10 to 2.53). The
vast majority of the buccal bone walls (57.7%) presented a BT ≤ 1 mm, whereas 42.3% exhibited a BT
> 1 mm.
Linear and volumetric changes over time
Linear and volumetric changes in BT ≤ 1 mm and BT > 1 mm classes are presented in Table 2. The
linear measurements showed a buccal mean change in thickness at 1-year follow-up of -
0.48±0.28mm when BT ≤ 1 mm and -0.17±0.11mm when BT > 1 mm (p = 0.049). Although mean
total change only revealed significant statistical results at T2 (p = 0.015), after one year of treatment
it was observed a change of -0.59±0.40mm in BT ≤ 1 mm class compared with -0.31±0.12mm
observed when BT > 1 mm, demonstrating almost a two times bigger difference between each
group.
Regarding the volumetric analysis, patients representing BT > 1 mm exhibited again better results
than patients with BT ≤ 1 mm, presenting a significant different BVC (%) at T1 (p = 0.018), BVC (%)
(p = 0.010) and TVC (%) at T2 (p = 0.012) (see Supplementary Figure 1 in online Journal of
Periodontology). At the one-year follow-up appointment, buccal volume change was -11.27 ± 7.72
% when BT ≤ 1 mm compared with the observed -4.27 ± 3.39 %, when BT > 1 mm.
Regarding BID values, less changes could be found when BID > 2 mm. At 1-year follow-up it was
observed a total volume change of -10.88±6.59% when BID ≤ 2 mm and when BID > 2 mm, -
5.80±3.54%. Nevertheless, BID values showed no significant difference on thickness and volume
change of the peri-implant tissue contour over one, four and twelve months of observation (see
Supplementary Table 1 in online Journal of Periodontology).
Correlations
A multi-variate regression analysis was conducted to evaluate BT and BID effect on buccal peri-
implant tissue thickness and volume changes (Table 3). Although no significant influence of BID on
This article is protected by copyright. All rights reserved.
MBC and BVC at T1 or T3 were found, this analysis proved a statistical significant influence of BT on
buccal peri-implant tissue thickness and volume changes over time. BT values influenced MBC after
1 year of treatment (p = 0.016) and BVC at T1 (p = 0.015) and T3 (p = 0.009), respectively.
Discussion
This investigation comprised a prospective cohort study of 26 dental implants, placed in the
maxillary arch immediately after tooth extraction. To minimise the impact that the surgeon’s skills
might have had in the final aesthetic result, all surgical procedures were carried out by an
experienced implant surgeon (T.B.) and patients were only included in the study group if they
received a dental implant with no associated defects of the alveolar bone walls. Implant placement
in fresh extraction sockets has been widely discussed and several studies show consistent favourable
results. Lops et al.29 addressed a prospective analysis of 46 post-extraction single implant
placements and clinical outcomes showed a 100% success rate. A growing number of studies confirm
these findings with post-extraction implant survival rates as predictable as in healed bone, even
when different implant morphologies are used.30-33 We also accept that the high predictability of
osseointegration is achieved when a specific set of selection criteria is applied, and a strict surgical
and restorative protocol is observed. In fact, the period from the surgical stage to the final
restoration step represents a critical time lapse for the tissue healing and the restoration option.34-36
Some literature reveals heterogeneity in the parameters used to evaluate the aesthetic outcomes of
an implant restoration.5, 37, 38 A great number of the indexes utilised to assess the results of implant
treatments in aesthetic areas are observer-dependent and reveal moderate reproducibility between
observers.39 The digital evaluation methods used in our investigation intend to provide an objective
and quantitative analysis of the peri-implant tissue evolution after immediate implant insertion, as
well as establish a possible correlation between the initial alveolar bone features and the alveolar
healing progression. The same ROI was used in each patient to compare thickness changes in a
uniform way. Also, since all ROI were different from each patient due to anatomical variations,
This article is protected by copyright. All rights reserved.
relative percentages of the areas and volumes were calculated to allow a direct comparison between
the different sites.40
Distinct variables have been described as factors that might influence the hard tissue dimensional
alterations following tooth extraction in the maxillary region. Ferrus et al.9 defined the location of
the implant, the thickness of the buccal bone crest, the extraction motive or the dimension of the
horizontal bone gap as predictable variables that potentially have an effect on peri-implant bone
resorption in fresh extraction sockets. Studies showed the outcomes of the hard-tissue graft, mainly
a bone substitute that was placed in the space between the implant surface and the inner surface of
the buccal bone wall.41, 42
The findings from these reports demonstrate that graft procedures,
combined with implant placement, may counteract ridge alterations following tooth extraction.
Similar findings had already been outlined by Araújo et al.43 in a study about socket preservation
procedures. According to the authors, the healing ridge contraction in fresh sockets filled with
bovine xenograft can be less conspicuous, not only for the buccal bone wall properties but also for
the four-wall defect-containing capacity, which may be more effective at incorporating the graft
material. All the sockets of our sample were grafted with DBBM, which filled the gap between the
inner buccal bone wall and the implant surface.
Januario et al.44 described the morphological features of the alveolar process in the anterior maxilla
(canine to canine) in humans, measuring the thickness of the buccal bone plate at three different
positions in relation to the buccal bone crest. Cone-beam computer tomograms were obtained from
this area showing that the buccal bone plate in most locations is ≤ 1 mm and up to 50% of the sites
had a bone plate of ≤ 0.5 mm. In the present study, almost half (N=11) of the consecutively included
patients had a buccal bone plate with a thickness of > 1 mm, which could be explained by the
inclusion of premolars in digital analysis.45
Almost no clinical studies have been found in the literature comparing the initial alveolar bone
morphology and the immediate implant installation outcomes in the aesthetic maxillary areas. To
This article is protected by copyright. All rights reserved.
test the influence that the buccal plate thickness may have in the healing process of the immediate
implant socket alteration, Arora et al.24 studied the possible correlation between preoperative
buccal cortical bone thickness and peri-implant tissue response following immediate implant
placement. The 18 patients with intact socket walls underwent a treatment strategy that involved a
flapless extraction procedure, implant placement and grafting of the implant-socket gap with a
xenograft material. The authors compared the preoperative bone width with the soft tissue and
aesthetic outcomes obtained by a Pink Esthetic Score, after a two-year follow-up period, and found
no significant correlation between both variables. These results are not in accordance with those
obtained from our investigation since the preoperative buccal cortical bone thickness proved to
influence the dimensional change that affects the peri-implant tissues after immediate implant
placement procedures (Table 2). Our data suggest that after one year of treatment, when BT ≤ 1 mm
we can expect a significant buccal tissue horizontal retraction compared with the implant sites that
presented BT > 1 mm (p = 0.049). The difference can be noticed by the diverse negative evolution of
the buccal section at the two BT classes at the 12-month follow-up (MBC T0 –T3 -0.48 ± 0.28 mm and
MBC T0 –T3 -0.17 ± 0.11 mm, when BT ≤ 1 and BT > 1 mm, respectively). In fact, it is clear that
individuals diagnosed with a thinner buccal bone plate undergo a marked reduction of the alveolar
tissues, from the first month of treatment. These findings are comparable with the results of Tomasi
et al.40, which point toward significantly higher alveolar volume reduction at sites with a thin buccal
bone wall (≤ 1 mm), a the 6-month evaluation.
It must be outlined that in the present investigation no separation was made in terms of soft tissue
and bone evaluation during the healing period, resulting in a lack of information towards the effect
of the grafting procedure in the hard tissues. Because of this, we can speculate that some of the
volumetric outcomes of the alveolar ridge might be due to compensatory variations of the mucosa,
has suggested by Chappuis et al.46
This article is protected by copyright. All rights reserved.
Despite of this, our study results are in accordance with several authors that emphatize the
importance of the thin labial bone plate as a predictor factor for higher rates of mucosal recession
and bone resorption around immediate implants inserted at the esthetic maxillary area.47 Also, we
must highlight the importance of a long-term follow-up of this treatment modality. Cosyn et al.,
concluded that after the 1-year evaluation, and despite the favourable early results obtained by
immediate maxillary implants in terms of survival rate and MBL, mid-facial recession and mid-facial
contour deterioration could be noticed48.
The appraisal beween different treatment options that potencially minimize the contraction of the
facial tissues, like the use of connective tissue grafts, or the comparison between different implant
insertion aproaches (immediate vs delayed) should be considered for future studies.
Conclusion
After the first year of treatment following single immediate implant placement in the maxilla, peri-
implant tissues showed a continuous alteration resulting in a thickness change that occurred mainly
in the first month and tended to be stable after the fourth month of follow-up. Linear section and
alveolar volume changes were significantly influenced by the buccal bone plate thickness.
Acknowledgments
The authors thank Dr. Celeste Morais, Professor of Statistics, for the support with the statistical
analysis.
Conflict of interest
The authors declare no conflict of interest in relation to this manuscript.
References
1. Araújo MG, Lindhe J. Dimensional ridge alterations following tooth extraction. An
experimental study in the dog. J Clin Periodontol 2005;32:212-218.
This article is protected by copyright. All rights reserved.
2. Chappuis V, Engel O, Reiyes M, Shahim K, Nolte LP, Buser D. Ridge alterations post-extraction
in the esthetic zone: a 3D analysis with CBCT. J Dent Res 2013;92:195S-201S.
3. Lekovic V, Camargo PP, Klokkevold P, et al. Preservation of alveolar bone in extraction
sockets using bioabsorbable membranes. J Periodontol 1998;69:1044-1049.
4. Schropp L, Wenzel A, Kostopoulos L, Karring T. Bone healing and soft tissue contour changes
following single-tooth extraction: a clinical and radiographic 12-months prospective study. Int J
Periodontics Restorative Dent 2003;23:313-323.
5. Fϋrhauser R, Florescu D, Benesch T, Haas R, Mailath G, Watzek G. Evaluation of soft tissue
around single-tooth implant crowns: the pink esthetic score. Clin Oral Implants Res 2005;16:639-444.
6. Watzek G, Haider R, Mensdorff-Pouilly N, Haas R. Immediate and delayed implantation for
complete restoration of the jaw following extraction of all residual teeth: a retrospective study
comparing different types of serial immediate implantation. Int J Oral Maxillofac Implants
1995;10:561–567.
7. Arora H, Khzam N, Roberts D, Bruce WL, Ivanovski S. Immediate implant placement and
restoration in the anterior maxilla: Tissue dimensional changesafter 2-5 year follow up. Clin Implant
Dent Relat Res 2017;19:694-702.
8. Sanz M, Cecchinato S, Ferrus J, Pjertursson EB, Lang NP, Lindhe J. A prospective, randomized-
controlled clinical trial to evaluate bone preservation using implants with differente geometry placed
into extractio sockets in the maxilla. Clin Oral Implants Res 2010;21:13-21.
9. Ferrus J, Cecchinato D, Pjetursson EB, Lang NP, Sanz M, Lindhe J. Factors influencing ridge
alterations following immediate implant placement into extraction sockets. Clin Oral Implants Res
2010;21:22–29.
10. Lang NP, Pun L, Lau KY, Li KY, Wrong MC. A systematic review on survival and success rates
This article is protected by copyright. All rights reserved.
of implants placed immediately into fresh extraction sockets after at least 1 year. Clin Oral Implants
Res 2012;23:39-66.
11. Chen ST, Buser, D. Esthetic outcomes following immediate and early implant placement in
the anterior maxilla - a systematic review. Int J Oral Maxillofac implants 2014;29 Suppl:186–215.
12. Botticelli D, Persson LG, Lindhe J, Berglundh T. Bone tissue formation adjacent to implants
placed in fresh extraction sockets: An experimental study in dogs. Clin Oral Implants Res
2006;17:351–358.
13. Januário AL, Barriviera M, Duarte WR. Soft tissue cone-beam computed tomography: a novel
method for the measurement of gingival tissue and the dimensions of the dentogingival unit. J
Esthet Restor Dent 2008;20:366–373.
14. Becker W, Becker BE, Polizzi G, Bergstrom C. Autogenous bone grafting of bone defects
adjacent to implants placed into immediate extraction sockets in patients: a prospective study. Int J
Oral Maxillofac Implants 1994;9:389–396.
15. Sanz M, Lindhe J, Alcaraz J, Sanz-Sanchez I, Cecchinato D. The effect of placing a bone
replacement graft in the gap at immediately placed implants: a randomized clinical trial. Clin Oral
Implants Res 2017;28:902–910.
16. Poskevicius L, Sidlauskas A, Galindo-Moreno P, Juodzbalys, G. Dimensional soft tissue
changes following soft tissue grafting in conjunction with implant placement or around present
dental implants: a systematic review. Clin Oral Implants Res 2017;28:1–8.
17. Bienz SP, Jung RE, Sapata VM, Hämmerle CHF, Hüsler J, Thoma DS. Volumetric changes and
peri-implant health at implant sites with or without soft tissue grafting in the esthetic zone, a
retrospective case-control study with a 5-year follow-up. Clin Oral Implants Res 2017;28:1459–1465.
18. Sanz Martin I, Benic GI, Hämmerle CH, Thoma DS. Prospective randomized controlled clinical
This article is protected by copyright. All rights reserved.
study comparing two dental implant types: volumetric soft tissue changes at 1 year of loading. Clin
Oral Implants Res 2016;27:406–411.
19. Schneider D, Grunder U, Ender A, Hämmerle CH, Jung RE. Volume gain and stability of peri-
implant tissue following bone and soft tissue augmentation: 1-year results from a prospective cohort
study. Clin Oral Implants Res 2011;22:28–37.
20. Szathvary I, Caneva M, Bressen E, Botticelli D, Meneghello R. A volumetric 3-D digital analysis
of dimensional changes to the alveolar process at implants placed immediately into extraction
sockets. J Oral Sci Rehab 2015;1:62–69.
21. van Nimwegen WG, Goené RJ, Van Daelen AC, Stellingsma K, Raghoebar GM, Meijer HJ.
Immediate placement and provisionalization of implants in the aesthetic zone with or without a
connective tissue graft: a 1-year randomized controlled trial and volumetric study. Clin Oral Implants
Res 2018;29:671–678.
22. Tomasi C, Sanz M, Cecchinato D, Pjetursson B, Ferrus J, Lang NP, Lindhe J. Bone dimensional
variations at implants placed in fresh extraction sockets: a multilevel multivariate analysis. Clin Oral
Implants Res 2010;21:30-36.
23. Spray JR, Black CG, Morris HF, Ochi S. The influence of bone thickness on facial marginal
bone response: stage 1 placement through stage 2 uncovering. Ann Periodontol 2000;5:119–128.
24. Arora H, Ivanovski S. Correlation between pre-operative buccal bone thickness and soft
tissue changes around immediately placed and restored implants in the maxillary anterior region: a
2-year prospective study. Clin Oral Implants Res 2017;29:346–352.
25. von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP. The
Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement:
guidelines for reporting observational studies. J Clin Epidemiol 2008;6:344-349.
This article is protected by copyright. All rights reserved.
26. Buser D, Martin W, Belser UC. Optimizing esthetics for implant restorations in the anterior
maxilla: anatomic and surgical considerations. Int J Oral Maxillofac Implants 2004;19 Suppl:43-61.
27. Emir F, Piskin B, Sipahi C. Effect of dental technician disparities on the 3-dimensional
accuracy of definitive casts. J Prosthet Dent 2017;117: 410–418.
28. Nedelcu R, Olsson P, Nyström I, Rydén J, Thor A. Accuracy and precision of 3 intraoral
scanners and accuracy of conventional impressions: a novel in vivo analysis method. J Dent
2018;69:110–118.
29. Lops D, Chiapasco M, Rossi A, Bressan E, Romeo E. Incidence of inter-proximal papilla
between a tooth and an adjacent immediate implant placed into a fresh extraction socket: 1-year
prospective study. Clin Oral Implants Res 2008;19:1135-1140.
30. Cosyn J, Eghbali A, Hanselaer L, et al. Four modalities of single implant treatment in the
anterior maxilla: a clinical, radiographic, and aesthetic evaluation. Clin Implant Dent Relat Res
2013:15:517-530.
31. Noelken R, Kunkel M, Jung BA, Wagner W. Immediate nonfunctional loading of NobelPerfect
implants in the anterior dental arch in private practice – 5-year data. Clin Implant Dent Relat Res
2014;16:21-31.
32. Sanz M, Cecchinato D, Ferrus J, et al. Implants placed in fresh extraction sockets in the
maxilla: clinical and radiographic outcomes from a 3-year follow-up examination. Clin Oral Implants
Res 2014;25:321-327.
33. Cosyn J, De Lat L, Seyssens L, Doornewaard R, Deschepper E, Vervaeke S. The
effectiveness of immediate implant placement for single tooth replacement compared to delayed
implant placement: A systematic review and meta-analysis. J Clin Periodontol 2019;46 Suppl
21:224-241.
This article is protected by copyright. All rights reserved.
34. Borges T, Lima T, Carvalho À, Dourado C, Carvalho V. The influence of customized abutments
and custom metal abutments on the presence of the interproximal papilla at implants inserted in
single-unit gaps: a 1-year prospective clinical study. Clin Oral Implants Res 2014;25:1222-1227.
35. de Rouck T, Collys K, Cosyn J. Single-tooth replacement in the anterior maxilla by means of
immediate implantation and provisionalization: a review. Int J Oral Maxillofac Implants 2008;23:897-
904.
36. den Hartog L, Raghoebar GM, Stellingsma K, Vissink A, Meijer HJ. Immediate non-occlusal
loading of single implants in the aesthetic zone: a randomized clinical trial. J Clin Periodontol
2011;38:186-194.
37. Meijer HJA, Stellingsma K, Meijndert L, Raghoebar GM. A new index for rating aesthetics of
implant - supported single crowns and adjacent soft tissues – The Implant Crown Aesthetic Index.
Clin Oral Implants Res 2005;16:645-649.
38. Belser UC, Grütter L, Vailati F, Bornstein MM, Weber HP, Buser D. Outcome evaluation of
early placed maxillary anterior single-tooth implants using objective esthetic criteria: a cross-
sectional, retrospective study in 45 patients with a 2- to 4-year follow-up using pink and
white esthetic scores. J Periodontol 2011;72:1364-1371.
39. Hof M, Umar N, Budas N, Seemann R, Pommer B, Zechner W. Evaluation of implant esthetics
using eight objective indices-Comparative analysis of reliability and validity. Clin Oral Implants
Res 2018;29:697-706.
40. Tomasi C, Regidor E, Ortiz-Vigón A, Derks J. Efficacy of reconstructive surgical therapy at
peri-implantitis-related bone defects. A systematic review and meta-analysis. J Clin Periodontol
2019;46 Suppl 21:340-356.
41. Caneva M, Botticelli D, Morelli F, Cesaretti G, Beolchini M, Lang NP. Alveolar process
This article is protected by copyright. All rights reserved.
preservation at implants installed immediately into extraction sockets using desproteinized bovine
bone mineral – an experimental study in dogs. Clin Oral Implants Res 2012;23:789-796.
42. Caneva M, Botticelli D, Pantani F, Baffone GM, Rangel IG Jr, Lang NP. Deproteinized bovine
bone mineral in marginal defects at implants installed immediately into extraction sockets: an
experimental study in dogs. Clin Oral Implants Res 2012;23:106-112.
43. Araújo MG, da Silva JCC, de Mendonça AF, Lindhe J. Ridge alterations following grafting of
fresh extraction sockets in man. A randomized clinical trial. Clin Oral Implants Res 2015;26:407-412.
44. Januário AL, Duarte WR, Barriviera M, Mesti JC, Araújo MG, Lindhe J. Dimensional of the
facial bone wall in the anterior maxilla: a cone-beam computed tomography study. Clin Oral
Implants Res 2011;22:1168-1171.
45. Huynh-Ba G, Pjetursson BE, Sanz M, Cecchinato D, Ferrus J, Lindhe J, Lang NP. Analysis of
thee socket bone wall dimensions in the upper maxilla in relation to immediate implant placement.
Clin Oral Implants Res 2010;21:37-42.
46. Chappuis V, Engel O, Shahim K, Reyes M, Katsaros C, Buser D. Soft tissue alterations in
esthetic postextraction sites: A 3-dimensional analysis. J Dent Res 2015;94;187S-193S.
47. Yang X, Zhou T, Zhou N, Man Y. The thickness of labial bone affects the esthetics of
immediate implant placement and provisionalization in the esthetic zone: A prospective cohort
study. Clin Implant Dent Relat Res 2019;21:482-491.
48. Cosyn J, Eghbali A, Hermans A, Vervaeke S, De Bruyn H, Cleymaet R. A 5-year prospective
study on single immediate implants in the aesthetic zone. J Clin Periodontol 2016;43:702-709.
This article is protected by copyright. All rights reserved.
Figure 1. Determination of the region of interest (ROI) in superimposed models.
Figure 2. Buccal and palatal linear alterations.
This article is protected by copyright. All rights reserved.
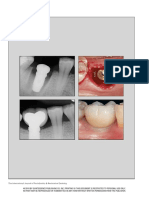
Figure 3. Selection of the ROI for volumetric evaluation; A: Buccal ROI; B: Palatal ROI; C: Buccal and
palatal ROI; D: Volumetric ROI for total alveolar volume assessment.
Table 1: Characterization of study sample in age, gender, implant site and dimension, BID and KM.
Patient N=26 (100.0%)
Age Mean SD Minimum Maximum
Male 58.18 12.49 37 85
Female 49.27 10.71 34 76
Total 53.04 12.11 34 85
Gender (N) (%)
Male 12 46.15
Female 14 53.85
Total 26 100.0
Implant site (N) (%)
This article is protected by copyright. All rights reserved.
Central incisor 5 19.23
Lateral incisor 5 19.23
First PM 12 46.15
Second PM 4 15.38
Total 26 100.0
Implant (N) (%)
EV 4.2x11 mm 6 23.08
EV 3.6 x 9 mm 1 3.85
EV 3.6x11 mm 18 69.23
EV 3.6x13 mm 1 3.85
Total 26 100.0
Intra-operative
Mean SD Minimum Maximum
measurements
BID 3.08 0.93 2 5
KM 3.88 1.21 2 6
Table 2: Alveolar tissue change from baseline to 1-year in relation with the buccal plate thickness.
Minimum;M CI(95%)
Variable N BT Mean SD P-value
aximum Lower;Upper
MBC T0-T1 15 ≤1mm -1.15;0.20 -0.32 0.37 -0.53;-0.12
0,061
(mm) 11 >1mm -0.44;0.19 -0.11 0.17 0.22;0.00
MBC T0-T2 15 ≤1mm -1.03;0.13 -0.46 0.37 -0-72;-0.21
0,017*
(mm) 11 >1mm -0.32;0.06 -0.14 0.10 -0.21;-0.70
MBC T0-T3 15 ≤1mm -0.97;-0.06 -0.48 0.28 -0.67;-0.28
0.049*
(mm) 11 >1mm -0.30;-0.04 -0.17 0.11 -0.35;0.01
MTC T0-T1 15 ≤1mm -1.62;0.10 -0.66 0.59 -1.05;-0.26
0.065
(mm) 11 >1mm -0.99;0.16 -0.25 0.34 -0.47;-0.01
This article is protected by copyright. All rights reserved.
MTC T0-T2 15 ≤1mm -1.37;-0.01 -0.65 0.47 -0.97;-0.34
0.015*
(mm) 11 >1mm -0.49;-0.11 -0.26 0.12 -0.34;-0.18
MTC T0-T3 15 ≤1mm -1.30;-0.06 -0.59 0.40 -0.92;-0.34
0.066
(mm) 11 >1mm -0.55;0.09 -0.31 0.22 -0.60;0.07
15 ≤1mm -53.32;9.73 -27.45 18.53 -39.22;-15.67
BVC T0-T1 (mm3) 0.012*
11 >1mm -34.29;7.81 -10.07 10.28 -16.97;-3.16
15 ≤1mm -70.07;7.05 -30.57 21.14 -44.78;-16.37
BVC T0-T2 (mm3) 0.012*
11 >1mm -30.42;3.42 -10.44 8.33 -16.04;-4.85
15 ≤1mm -69.26;7.05 -29.06 21.25 -43.45;-14.79
BVC T0-T3 (mm3) 0.219
11 >1mm -24.09;-3.29 -11.89 10.86 -25.49;3.03
15 ≤1mm -98.00;2.93 -46.53 32.51 -68.37;-24.70
TVC T0-T1 (mm3) 0.045*
11 >1mm -76.97;6.03 -20.90 22.74 -36.18;-5.63
15 ≤1mm -95.49;-7.37 -45.82 28.91 -65.24;-26.40
TVC T0-T2 (mm3) 0.017*
11 >1mm -52.05;-9.44 -21.30 11.69 -29.15;-13.45
15 ≤1mm -96.34;-16.12 -40.32 26.48 -58.11;-22.38
TVC T0-T3 (mm3) 0.302
11 >1mm -37.96;-11.80 -22.59 13.67 -40.43;3.23
BVC T0-T1 15 ≤1mm -19.16;3.53 -10.22 7.31 -14.86;-5.58
0.018*
(%) 11 >1mm -11.20;3.05 -3.91 3.84 -6.49;-1.33
BVC T0-T2 15 ≤1mm -25.68;2.56 -11.57 7.67 -16.72;-6.41
0.010*
(%) 11 >1mm -9.94;1.34 -4.08 3.03 -6.11;-2.05
BVC T0-T3 15 ≤1mm -25.38;2.56 -11.27 7.72 -16.83;-6.33
0.168
(%) 11 >1mm -7.87;-1.14 -4.27 3.39 -8.45;0.94
TVC T0-T1 15 ≤1mm -16.11;0.51 -8.39 6.02 -12.44;-4.35
0.088
(%) 11 >1mm -13.19;0.85 -4.42 4.22 -7.26;-1.59
TVC T0-T2 15 ≤1mm -20.15;-1.38 -9.24 5.40 -12.87;-5.61
0.012*
(%) 11 >1mm -8.92;-2.07 -4.42 2.06 -5.80;-3.04
TVC T0-T3 15 ≤1mm -20.33;-3.14 -8.53 5.47 -12.52;-5.05
0.239
(%) 11 >1mm -6.50;-2.35 -4.37 2.08 -7.35;0.32
This article is protected by copyright. All rights reserved.
MBC, Mean Buccal Change (mm); MTC, Mean Total Change (mm); BVC, Buccal Volume change (mm3/%); TVC, Total Volume
change (mm/%3); BT, Buccal bone thickness (mm); SD, Standard deviation; * statistically significant changes at the 5% level;
Ci, Confidence interval
Table 3: Multivariate regression analysis
2 F Statistical Standardized t Statistical (P-
Variable Regressors Adjusted R
(P) Coefficients value)
Constant -0.165 -0.539(0.038)
MBC T0-T1 2.622
BT 0.163 0.348 1.879 (0.071)
(mm) (0.076)
BID -0.013 -0.072 (0.361)
Constant -0.654* -2.138(0.046)
MBC T0-T3 3.928
BT 0.295 0.497* 2.663 (0.016*)
(mm) (0.026)
BID 0.175 0.938 (0.361)
Constant -12.533 -1.846(0.080)
BVC T0-T1 4.241
BT 0.306 0.477* 2.681 (0.015*)
(%) (0.019)
BID 0.159 0.891 (0.384)
Constant -15.561* -2.542(0.020)
BVC T0-T3 4.701
BT 0.346 0.526* 2.926 (0.009*)
(%) (0.014)
BID 0.173 0.960 (0.350)
MBC, Mean Buccal Change (mm); BVC, Buccal Volume change (%); * statistically significant changes at the 5% level.
This article is protected by copyright. All rights reserved.
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5834)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1093)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (852)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (903)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (541)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (349)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (824)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (405)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- 6th Central Pay Commission Salary CalculatorDocument15 pages6th Central Pay Commission Salary Calculatorrakhonde100% (436)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- 2006MockBoard Answers ReferencesDocument46 pages2006MockBoard Answers ReferencesAniket Potnis100% (2)
- Arnab Chowdhury AsDocument11 pagesArnab Chowdhury AsARNAB CHOWDHURY.No ratings yet
- NEET MDS 2021 Part 1 - Recalls, Analysis, Question Paper and ExplanationsDocument183 pagesNEET MDS 2021 Part 1 - Recalls, Analysis, Question Paper and ExplanationsMahima100% (1)
- Reconstructive Aesthetic Implant Surgery PDFDocument152 pagesReconstructive Aesthetic Implant Surgery PDFAnonymous p28Tktgl5No ratings yet
- Implants in The Esthetic Zone: Mohanad Al-Sabbagh, DDS, MSDocument17 pagesImplants in The Esthetic Zone: Mohanad Al-Sabbagh, DDS, MSNeil SchembriNo ratings yet
- Al-Juboori (2015), The Effect of Flapless and Full-Thickness Flap Techniques On Implant Stability During The Healing PeriodDocument7 pagesAl-Juboori (2015), The Effect of Flapless and Full-Thickness Flap Techniques On Implant Stability During The Healing PeriodPhương Thảo TrầnNo ratings yet
- Bornstein (2009), Early Loading of Nonsubmerged Titanium Implants With A Chemically Modified Sand-Blasted and Acid-Etched SurfaceDocument10 pagesBornstein (2009), Early Loading of Nonsubmerged Titanium Implants With A Chemically Modified Sand-Blasted and Acid-Etched SurfacePhương Thảo TrầnNo ratings yet
- Amato 1 (2018), Immediate Implant PlacementDocument8 pagesAmato 1 (2018), Immediate Implant PlacementPhương Thảo TrầnNo ratings yet
- Volume 11, Issue 1Document54 pagesVolume 11, Issue 1Phương Thảo TrầnNo ratings yet
- قائمة الكتبDocument18 pagesقائمة الكتبخالدعلمNo ratings yet
- Anthogyr:Axiom Implant CatalogDocument108 pagesAnthogyr:Axiom Implant CatalogDeb SNo ratings yet
- Dental Implants History and DefinitionDocument6 pagesDental Implants History and DefinitionRmz StudyNo ratings yet
- Ortho Perio NewDocument5 pagesOrtho Perio NewNingombam Robinson SinghNo ratings yet
- Alveolar Segmental Sandwich Osteotomy PDFDocument7 pagesAlveolar Segmental Sandwich Osteotomy PDFDeepak YadavNo ratings yet
- Periodontics Final Exam Questions - QuizletDocument12 pagesPeriodontics Final Exam Questions - Quizlethasnaa.makkawiNo ratings yet
- Reabilitarea Orală A Unor Cazuri Sociale Cu Edentaţie Parţială Clasa I KennedyDocument8 pagesReabilitarea Orală A Unor Cazuri Sociale Cu Edentaţie Parţială Clasa I KennedyBuzoianu Mihaela-AndreeaNo ratings yet
- Resume - Niloofar MojaradDocument2 pagesResume - Niloofar Mojaradmohammadrezahajian12191No ratings yet
- The IMZ Implant System: IMZ Original 3.3 & 4.0 Non-Hex Flat-TopDocument10 pagesThe IMZ Implant System: IMZ Original 3.3 & 4.0 Non-Hex Flat-TopReem Al BasNo ratings yet
- Correlation Between Placement Torque and Survival of Single-Tooth ImplantsDocument8 pagesCorrelation Between Placement Torque and Survival of Single-Tooth ImplantssheetalNo ratings yet
- Masticatory Performance of Denture Wearers With The Use of Denture Adhesives A Systematic ReviewDocument6 pagesMasticatory Performance of Denture Wearers With The Use of Denture Adhesives A Systematic Review박소영No ratings yet
- Management of Difficult Complete Denture CasesDocument78 pagesManagement of Difficult Complete Denture Casesmoh AshourNo ratings yet
- Section 019 EstheticsDocument10 pagesSection 019 EstheticsMohammed LafiNo ratings yet
- Product Catalog 2022Document40 pagesProduct Catalog 2022Tîrban Pantelimon FlorinNo ratings yet
- Introduction To Implant Prosthodontics CARINO MA NON ALLA TAWFIKDocument214 pagesIntroduction To Implant Prosthodontics CARINO MA NON ALLA TAWFIKOral SurgeonNo ratings yet
- Class of Medical DevicesDocument14 pagesClass of Medical DevicesDuck Mann-ConsulNo ratings yet
- Biocompatability of Dental Materials.Document93 pagesBiocompatability of Dental Materials.vadlamudi chakradhar100% (2)
- TUFTS - School of Dental Medicine - Continuing Education Fall 2009Document24 pagesTUFTS - School of Dental Medicine - Continuing Education Fall 2009Adrian MGNo ratings yet
- A Immediate Implant With Provisionaliztion Journal of Clinical PeriodontologyDocument12 pagesA Immediate Implant With Provisionaliztion Journal of Clinical PeriodontologyAhmed BadrNo ratings yet
- Digital DentistryDocument401 pagesDigital DentistryvcNo ratings yet
- Fet Ner 2015Document8 pagesFet Ner 2015Marco TeixeiraNo ratings yet
- Case Report Treatment of A Periodontic-Endodontic Lesion in A Patient With Aggressive PeriodontitisDocument10 pagesCase Report Treatment of A Periodontic-Endodontic Lesion in A Patient With Aggressive PeriodontitissulistiyaNo ratings yet
- Immediate or Early Placement of Implants Following Tooth Extraction: Review of Biologic Basis, Clinical Procedures, and OutcomesDocument14 pagesImmediate or Early Placement of Implants Following Tooth Extraction: Review of Biologic Basis, Clinical Procedures, and OutcomesJASPREETKAUR0410No ratings yet
- (Reduced) 24th BaSS PREFINAL Program 2019Document36 pages(Reduced) 24th BaSS PREFINAL Program 2019Vera Radojkova NikolovskaNo ratings yet
- Novel Bone Adhesives in Fracture Fixation & Its Possible Significance in Midfacial Surgery - A ReviewDocument6 pagesNovel Bone Adhesives in Fracture Fixation & Its Possible Significance in Midfacial Surgery - A ReviewInternational Journal of Innovative Science and Research TechnologyNo ratings yet