Professional Documents
Culture Documents
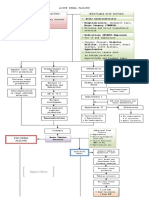
Pathophysiology of Acute Renal Failure
Pathophysiology of Acute Renal Failure
Uploaded by
Aina HaravataOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Pathophysiology of Acute Renal Failure
Pathophysiology of Acute Renal Failure
Uploaded by
Aina HaravataCopyright:
Available Formats
ACUTE RENAL FAILURE
NON-MODIFIABLE RISK FACTORS: MODIFIABLE RISK FACTORS:
IncreasedOliguric
age (72y.o.)
Phase
Family History of kidney disease Acute
Maintenance
Renal Injury
Gastroenteritis
Established
Obesity Phase
Hospitalization: Intensive
Smoking Care, Major Surgery (TAHBSO)
Endothelial cells
Bleeding and blood
necrosis andtransfusion
reaction sloughing
Medications (NSAIDS:Naproxen)
Tubular destruction
Use of ACE Inhibitors
MEDICAL MANAGEMENT:
Objectives: Chronic Increase
disease: tubular
Diabetes
permeability
Restore normal chemical Mellitus, kidney disease, heart
balance disease, liver disease,
Prevent complications hypertension
Low GFR (5-10mL/m)
as benign prostatic
Recognition and treatment of
High Creatinine
hypertrophy and bladder tumor
underlying cause
High BUN
BP monitoring
I and O monitoring, including Oliguria
drainage
Monitoring of electrolyte Decreased nephron
levels ability to
ECG Trauma/Injury in Dehydration
Inhibit COX-1 and eliminate waste
ABG and Serum bicarbonate levelMuscle
COX-2 production
monitoring
May have blood transfusion Azotemia
Decreased BP
Rhabdomyolosis
Fluid retention
Decrease
May initiate
renaldialysis Electrolyte
prostaglandin
Pharmacologic Therapy:
imbalance
Cation-exchange resins Release
production for of Kidney release
hyperkalemia Myoglobin and Renin Metabolic
Hemoglobin acidosis
IV dextrose 50%
Insulin Angiotensinogen
Vasoconstriction from liver
Calcium
of renal replacement
afferent
arteriole
Albuterol Sulfate nebule pH is <5.6
Diuretic Phase
Avoidance of nephrotoxic If managed Angiotensin
Kidneys I
have a remarkable
agents: radiocontrast ability to recover
Becomes ACE from Pulmonary and
agents, antibiotics with
ferrihemate Renal Endothelium
nephrotoxic potential, heavy
metal preparations, cancer
chemotherapeutic agents,
Free hydroxyl Angiotensin II Aldosterone
nonsteroidal anti- Growth factors
radicals Recovery
inflammatory drugs [NSAIDs] released
production Phase
Diuretic agents
Nutritional therapy: Vasoconstriction Na reabsorption
Repair and
Weigh patient daily Vasoconstriction Hypertension K of
excretion
regeneration
Dietary proteins Na reabsorption Water retention
renal tissue
High carbohydrate diet
Low salt, potassium, low
Recover tubular
phosphorus food function
Restrict potassium intake Ischemia Additional Risk
Factors:
Hypotension Recover renal
Blood transfusion function
Acute Tubular
IfPRE-RENAL
not managed Necrosis
reactions
FAILURE Severe Infection
(WBC:23.81) Increase Urine
output
Dye/Contrast use Decreased urea
Prolonged damage
to kidney tubules Decreased
Injured tubular Creatinine
Initiation epithelial cells
Phase
End-stage Renal
Disease Cell death and
detachment from
basement membrane
Decrease renal
perfusion
Oliguric Phase
Tubular necrosis
Decrease blood
volume
Low GFR
High Creatinine
High BUN
You might also like
- Diuretic Cases and Self-Test Questions With AnswersDocument19 pagesDiuretic Cases and Self-Test Questions With AnswersRoxana CaravețeanuNo ratings yet
- The Westside Barbell Conjugate MethodDocument16 pagesThe Westside Barbell Conjugate Methodpflucho79% (19)
- Nuero and Musculo Set B Answer KeyDocument15 pagesNuero and Musculo Set B Answer KeyChristopher SarsozaNo ratings yet
- CASE-4-Pegad-Bea ScenarioDocument5 pagesCASE-4-Pegad-Bea Scenariobea pegadNo ratings yet
- Learning Exercise 5.9: To Float or Not To FloatDocument2 pagesLearning Exercise 5.9: To Float or Not To FloatZunnel Cortes100% (2)
- Term 3 Rationale Pharmacology and MCNDocument35 pagesTerm 3 Rationale Pharmacology and MCNKing KongNo ratings yet
- WPC in Ice CreamDocument5 pagesWPC in Ice CreamIvan MojsaNo ratings yet
- ARF PathoDocument3 pagesARF PathoNikki RodrigoNo ratings yet
- I. A. Brief Description: Chakinala, 2015)Document54 pagesI. A. Brief Description: Chakinala, 2015)Kacelyn QuibanNo ratings yet
- Biologic Crisis: Prepared By: Ronnie M. Amazona, RN, ManDocument162 pagesBiologic Crisis: Prepared By: Ronnie M. Amazona, RN, ManLex CatNo ratings yet
- Delegation: BY: Meilati Suryani, S.Kp.,M.KepDocument28 pagesDelegation: BY: Meilati Suryani, S.Kp.,M.Kepahmad rizalNo ratings yet
- Cva Power PointDocument167 pagesCva Power PointJen Passilan100% (14)
- Congestive Heart FailureDocument14 pagesCongestive Heart FailureBella Trix PagdangananNo ratings yet
- Pet CTDocument4 pagesPet CTKanishk R.SinghNo ratings yet
- Angina PectorisDocument8 pagesAngina PectorisJoanne LagusadNo ratings yet
- Coronary Artery Bypass SurgeryDocument12 pagesCoronary Artery Bypass SurgeryCarlos Eduardo Quisse SánchezNo ratings yet
- 780 Adult Cardio Resp Assess DSTDocument10 pages780 Adult Cardio Resp Assess DSTGursangeet Kaur100% (1)
- Test Quiz Hypo Kale MiaDocument6 pagesTest Quiz Hypo Kale MiaVivian Montesena BreganzaNo ratings yet
- NCM116 Module 3 Cerebrovascular Disease QuizDocument5 pagesNCM116 Module 3 Cerebrovascular Disease QuizIvan FernandezNo ratings yet
- Pneumonia and TuberculosisDocument18 pagesPneumonia and TuberculosisVincent QuitorianoNo ratings yet
- IschemicheartdiseaseDocument11 pagesIschemicheartdiseaseZaimon MaulionNo ratings yet
- Chronic Renal FailureDocument29 pagesChronic Renal Failuregeorgia.langNo ratings yet
- Cervical CA Case StudyDocument32 pagesCervical CA Case StudyCandy Mae Kabayao CuraNo ratings yet
- Professional AdjustmentDocument3 pagesProfessional Adjustmentkamae_27No ratings yet
- REVIEWERDocument12 pagesREVIEWERCynde KerrNo ratings yet
- Drills-1 Np4 AquinoDocument11 pagesDrills-1 Np4 AquinoSolah SalvatoreNo ratings yet
- Hepatic Encephalopathy and ComaDocument19 pagesHepatic Encephalopathy and ComaJas Castro JoveroNo ratings yet
- Cushing's SyndromeDocument5 pagesCushing's SyndromesummerduskNo ratings yet
- Kulit 5Document1 pageKulit 5Anonymous 12QYPATm3No ratings yet
- Dr. Sunatrio - Management Hypovolemic ShockDocument59 pagesDr. Sunatrio - Management Hypovolemic ShockArga Putra SaboeNo ratings yet
- Med-Surg Lecture 4th Year 1st Sem (Incomplete)Document70 pagesMed-Surg Lecture 4th Year 1st Sem (Incomplete)Raezhell Dianne RachoNo ratings yet
- NCM 103.1 FINAL - OkDocument99 pagesNCM 103.1 FINAL - OkElizalde HusbandNo ratings yet
- A. Gestational Diabetes Mellitus B. Secondary Diabetes Mellitus D. Type II Diabetes MellitusDocument32 pagesA. Gestational Diabetes Mellitus B. Secondary Diabetes Mellitus D. Type II Diabetes MellitusNebawNo ratings yet
- Asthma PDFDocument7 pagesAsthma PDFAlessandro Jr. ArellanoNo ratings yet
- Heart Failure NCLEX QuestionsDocument5 pagesHeart Failure NCLEX QuestionsMelodia Turqueza GandezaNo ratings yet
- Body Fluid DistributionDocument56 pagesBody Fluid DistributionZoya Morani100% (1)
- C C C M MMMM MM M MMM 3mm MMMMM MM M MMMMMDocument4 pagesC C C M MMMM MM M MMM 3mm MMMMM MM M MMMMMjohkieNo ratings yet
- GYNECOLOGICALNURSINGDocument4 pagesGYNECOLOGICALNURSINGSheana TmplNo ratings yet
- Patient Monitoring SheetDocument8 pagesPatient Monitoring SheetAndrea Sibayan SorianoNo ratings yet
- Acute Respiratory Distress Syndrome - NursingDocument14 pagesAcute Respiratory Distress Syndrome - Nursingyellowbyuns0% (1)
- Requirement in PathophysiologyDocument38 pagesRequirement in PathophysiologyckathreenahNo ratings yet
- Cerebral HemorrhageDocument10 pagesCerebral HemorrhageJayd Lorenz Vicente ChuanNo ratings yet
- Hemorrhagic Cerebro Vascular DiseaseDocument37 pagesHemorrhagic Cerebro Vascular Diseasejbvaldez100% (1)
- GenitoUri Post TestDocument5 pagesGenitoUri Post Testlourd nabNo ratings yet
- Post Operative ComplicationsDocument17 pagesPost Operative Complicationsdrhiwaomer100% (8)
- Acromegaly PDFDocument7 pagesAcromegaly PDFBudi AthAnza SuhartonoNo ratings yet
- Fluids and ElectrolytesDocument38 pagesFluids and ElectrolytesJohn Anthony de GùzmanNo ratings yet
- Metabolic EmergenciesDocument53 pagesMetabolic EmergenciesWengel Redkiss100% (1)
- Electrolyte ImbalanceDocument4 pagesElectrolyte ImbalanceDoneva Lyn MedinaNo ratings yet
- Chapter 11: Urological and Gynecological Disorders: Multiple ChoiceDocument4 pagesChapter 11: Urological and Gynecological Disorders: Multiple ChoiceJamieNo ratings yet
- Intracerebral HemorrageDocument13 pagesIntracerebral HemorrageChristian JuarezNo ratings yet
- Ethical Principles: Example: Surgery, or Any ProcedureDocument3 pagesEthical Principles: Example: Surgery, or Any ProcedureKevin Miguel Rivera100% (1)
- Activity 5 - Case StudyDocument2 pagesActivity 5 - Case StudyMary Hope BacutaNo ratings yet
- Practical Research 2 - ADocument1 pagePractical Research 2 - ABoyshin RebaldeNo ratings yet
- Pleural Fluid AnalysisDocument15 pagesPleural Fluid AnalysisNatalie Sarah MoonNo ratings yet
- CPT & Suctioning Rle ExamDocument2 pagesCPT & Suctioning Rle ExamJojo JustoNo ratings yet
- PlanningDocument30 pagesPlanningRajalakshmi BlessonNo ratings yet
- What Is Hypertensive NephropathyDocument11 pagesWhat Is Hypertensive NephropathyIvy Pamanian DeldaNo ratings yet
- Pleural Fluid Analysis: How The Test Is PerformedDocument4 pagesPleural Fluid Analysis: How The Test Is PerformedKevin LlorenteNo ratings yet
- Pathophysiology of Acute Renal FailureDocument2 pagesPathophysiology of Acute Renal Failureminangsung minangnengNo ratings yet
- Allopurinol (Drug Study)Document2 pagesAllopurinol (Drug Study)Daisy PalisocNo ratings yet
- TelmisartanDocument2 pagesTelmisartanRea LynNo ratings yet
- MATZ Maximilian P. Thesis BSCDocument79 pagesMATZ Maximilian P. Thesis BSCAina HaravataNo ratings yet
- Blake Jessica D 201407 MasterDocument154 pagesBlake Jessica D 201407 MasterAina HaravataNo ratings yet
- Drug Study SpironolactoneDocument2 pagesDrug Study SpironolactoneAina HaravataNo ratings yet
- MannitolDocument1 pageMannitolAina HaravataNo ratings yet
- 4 AnnotationsDocument8 pages4 Annotationsapi-243334002No ratings yet
- Proposed Rule: Medicare: Electronic Prescription Drug Program E-PrescribingDocument20 pagesProposed Rule: Medicare: Electronic Prescription Drug Program E-PrescribingJustia.comNo ratings yet
- Eaton - Internormen Wind Power SolutionsDocument12 pagesEaton - Internormen Wind Power SolutionsEaton FiltrationNo ratings yet
- Medical Marijuana: Social Construction of A Myth Theories, Findings, FutureDocument21 pagesMedical Marijuana: Social Construction of A Myth Theories, Findings, Futurejohn mark demetilloNo ratings yet
- Open Fracture Tibia Fibula FixDocument42 pagesOpen Fracture Tibia Fibula Fixannisaoktoviani100% (1)
- Compressed Air System Design, Operating and MaintenanceDocument29 pagesCompressed Air System Design, Operating and Maintenanceibrahim1961No ratings yet
- Irrigation Manual FAO Module 7Document169 pagesIrrigation Manual FAO Module 7Zac Mweb86% (7)
- Enviroline 199+ds+eng PDFDocument4 pagesEnviroline 199+ds+eng PDFMohamed NouzerNo ratings yet
- Chapter - 03 - PPT (Supplementary To ISpace)Document43 pagesChapter - 03 - PPT (Supplementary To ISpace)kjw 2No ratings yet
- Sydney Girls 2019 Chemistry Prelim Yearly & SolutionsDocument24 pagesSydney Girls 2019 Chemistry Prelim Yearly & SolutionsmabbuttbNo ratings yet
- Soal UNBK Bahasa Inggris SMPDocument13 pagesSoal UNBK Bahasa Inggris SMPfendiwaloyosugiartoNo ratings yet
- 8 19 Management of Snake Bites PDFDocument12 pages8 19 Management of Snake Bites PDFdawnkuruvillaNo ratings yet
- SF20 - OKL04 Risk Assessment WeldingDocument2 pagesSF20 - OKL04 Risk Assessment WeldingMike BoyesNo ratings yet
- 4 Dec - 24 WDsmalDocument24 pages4 Dec - 24 WDsmalrasbreedoagileNo ratings yet
- Form Hasil Pemeriksaan Laboratorium 2Document5 pagesForm Hasil Pemeriksaan Laboratorium 2puskesmas sarijadiNo ratings yet
- Technical Specifications: Type Pointek CLS 100 Pointek CLS 200 Pointek CLS 300Document8 pagesTechnical Specifications: Type Pointek CLS 100 Pointek CLS 200 Pointek CLS 300chochoroyNo ratings yet
- 304 Stainless Steel Chemical Compatibility Chart From IsmDocument11 pages304 Stainless Steel Chemical Compatibility Chart From IsmchenNo ratings yet
- Final Maintenance SheetDocument14 pagesFinal Maintenance SheetmanishrastogiNo ratings yet
- 066A3 HSE Bulletin Heat Illness PreventionDocument1 page066A3 HSE Bulletin Heat Illness PreventionOws AnishNo ratings yet
- Nucleobase: Nucleobases, Also Known As Nitrogenous BasesDocument5 pagesNucleobase: Nucleobases, Also Known As Nitrogenous BasesLuis Felipe Mera GrandasNo ratings yet
- Pengaruh Edukasi Gizi Menggunakan Instagram Terhadap PerubahanDocument9 pagesPengaruh Edukasi Gizi Menggunakan Instagram Terhadap PerubahanSiska WarnitaNo ratings yet
- Trade Queries 2020: S No. Company Particular Items Queried Export/ImportDocument16 pagesTrade Queries 2020: S No. Company Particular Items Queried Export/ImportINFO CEMARKINGNo ratings yet
- BOOSTDocument16 pagesBOOSTChristous PkNo ratings yet
- Introduction To VibrationsDocument36 pagesIntroduction To VibrationsMajid SattarNo ratings yet
- CBT 210Document1 pageCBT 210Carlos GutierrezNo ratings yet
- Biology MALNUTRITION ProjectDocument17 pagesBiology MALNUTRITION ProjectEbin Off16No ratings yet
- Menu Template - 02Document5 pagesMenu Template - 02Prashanna SapkotaNo ratings yet
- Advantages and Disadvantages of Working From Home - AnywhereDocument1 pageAdvantages and Disadvantages of Working From Home - AnywhereKerisia WayneNo ratings yet