Professional Documents
Culture Documents
Acantosis Nigricans Maligna
Acantosis Nigricans Maligna
Uploaded by
David BravoCopyright:
Available Formats
You might also like
- Rectal Cancer With Synchronous Tonsillar Metastasis: A Case Report and Literature ReviewDocument3 pagesRectal Cancer With Synchronous Tonsillar Metastasis: A Case Report and Literature ReviewKresna ArdinugrahaNo ratings yet
- 69 63 PBDocument8 pages69 63 PBsepputriNo ratings yet
- Circulating Cell-Free DNA or Circulating Tumor DNA in The Management of Ovarian and Endometrial CancerDocument14 pagesCirculating Cell-Free DNA or Circulating Tumor DNA in The Management of Ovarian and Endometrial CancerSergio J Calleja FreixesNo ratings yet
- Analysis of Clinicopathological Features of Cervical MucinouDocument9 pagesAnalysis of Clinicopathological Features of Cervical MucinouFlaviu Ionuț FaurNo ratings yet
- Spectrum of Histomorphological Diagnosis in Cystoscopic Bladder BiopsiesDocument4 pagesSpectrum of Histomorphological Diagnosis in Cystoscopic Bladder BiopsieskushalNo ratings yet
- Pi Is 1474442217300595Document1 pagePi Is 1474442217300595Zulvina FaozanudinNo ratings yet
- Urachal Carcinoma With Liver Lung and Brain MetastDocument5 pagesUrachal Carcinoma With Liver Lung and Brain Metast7fkqx7zh7pNo ratings yet
- BIBL 12 Liver MetastasisDocument3 pagesBIBL 12 Liver Metastasisstoia_sebiNo ratings yet
- Tomlinson Acp2010Document1 pageTomlinson Acp2010Rayan BossNo ratings yet
- 1 s2.0 S2210261221006337 MainDocument5 pages1 s2.0 S2210261221006337 MainRubén LimaNo ratings yet
- Tabrizi An 2009Document4 pagesTabrizi An 2009Dung Tran HoangNo ratings yet
- 10.1016@S1470 20451930318 3Document10 pages10.1016@S1470 20451930318 3FistiNo ratings yet
- Van Nieuwenhove Et Al 2021 Imaging of Traumatic and Atraumatic Penile LumpsDocument2 pagesVan Nieuwenhove Et Al 2021 Imaging of Traumatic and Atraumatic Penile LumpsThesisaurus IDNo ratings yet
- Diagnosis and Treatment of Radiation ProctitisDocument2 pagesDiagnosis and Treatment of Radiation ProctitispatNo ratings yet
- VASC 014 - Bilateral Testicular Cancer A Rare Case ReportDocument1 pageVASC 014 - Bilateral Testicular Cancer A Rare Case ReporttiopanNo ratings yet
- Jurnal 1Document5 pagesJurnal 1Nur Syamsiah MNo ratings yet
- Histopathologic Analysis of Appendectomy Specimens: Shrestha R, Ranabhat SR, Tiwari MDocument5 pagesHistopathologic Analysis of Appendectomy Specimens: Shrestha R, Ranabhat SR, Tiwari Mmau tauNo ratings yet
- Journal Reading Tahap 2 Sub Bagian Gastroentero HepatologiDocument27 pagesJournal Reading Tahap 2 Sub Bagian Gastroentero HepatologiherdianNo ratings yet
- Group 12 Revisi 3Document7 pagesGroup 12 Revisi 3Nur Apipa DaudNo ratings yet
- Gervaz Et Al - Squamous Cell Carcinoma of The Anus - Another Sexually Transmitted DiseaseDocument9 pagesGervaz Et Al - Squamous Cell Carcinoma of The Anus - Another Sexually Transmitted DiseasenamirohsamiyahNo ratings yet
- Usg ToaDocument6 pagesUsg ToaMuhammad Nugie ZifiNo ratings yet
- Ijn S232777Document14 pagesIjn S232777BHUMI BHATTNo ratings yet
- P0710 1116 Acute Liver Failure Due To Severe.767Document1 pageP0710 1116 Acute Liver Failure Due To Severe.767Marselya GaniNo ratings yet
- Feature: 106 Emergency MedicineDocument8 pagesFeature: 106 Emergency MedicinehakimNo ratings yet
- Aydin 2016Document5 pagesAydin 2016nurfitriaNo ratings yet
- Derrame Pleural 2015Document16 pagesDerrame Pleural 2015MARIA NEGRETE MOSCOTENo ratings yet
- Malignant Acanthosis Nigricans: An Early Diagnostic Clue: Case ReportDocument3 pagesMalignant Acanthosis Nigricans: An Early Diagnostic Clue: Case Reportilham raymanaNo ratings yet
- Paraneoplastic PCaDocument12 pagesParaneoplastic PCaBrendan DiasNo ratings yet
- Janczak Et Al. - 2016 - An Evaluation of The Diagnostic Efficacy of Fine NDocument5 pagesJanczak Et Al. - 2016 - An Evaluation of The Diagnostic Efficacy of Fine NHaziel CorroNo ratings yet
- Endoscopic Ultrasound Staging of Gastric LymphomaDocument3 pagesEndoscopic Ultrasound Staging of Gastric LymphomaEvainoirNo ratings yet
- Nasopharyngeal Carcinoma: Imaging Features of Unusual Cancer in ChildrenDocument5 pagesNasopharyngeal Carcinoma: Imaging Features of Unusual Cancer in ChildrenDevanti EkaNo ratings yet
- Paraneoplastic Syndromes Associated With LaryngealDocument15 pagesParaneoplastic Syndromes Associated With Laryngealandre halimNo ratings yet
- Adult Desmoid Tumors: Biology, Management and Ongoing TrialsDocument7 pagesAdult Desmoid Tumors: Biology, Management and Ongoing TrialsGustavo GasperiNo ratings yet
- Ijwh 178349 Triple Negative Breast Cancer Current Perspective On The EvDocument7 pagesIjwh 178349 Triple Negative Breast Cancer Current Perspective On The EvMuhammad FauzanNo ratings yet
- Ameboma of Colon Simulating Colonic Adenocarcinoma: Case ReportDocument3 pagesAmeboma of Colon Simulating Colonic Adenocarcinoma: Case ReportJulio BarajasNo ratings yet
- Ijpd 24 221Document2 pagesIjpd 24 221intan yunni aztiNo ratings yet
- DuodenalcarcinoidDocument5 pagesDuodenalcarcinoidMudassar SattarNo ratings yet
- Shi 2017Document8 pagesShi 2017Claudia Ivette Villarreal OvalleNo ratings yet
- Hernandez 2008Document2 pagesHernandez 2008asialoren74No ratings yet
- Unknown Primary Cancer of The Head and Neck - A MultidisciplinaryDocument10 pagesUnknown Primary Cancer of The Head and Neck - A MultidisciplinaryFreddy Eduardo Navarro BautistaNo ratings yet
- Primary Congenital Choledochal Cyst With Squamous Cell Carcinoma: A Case ReportDocument6 pagesPrimary Congenital Choledochal Cyst With Squamous Cell Carcinoma: A Case ReportRais KhairuddinNo ratings yet
- Renal Cell Carcinoma: Diagnosis, Staging, and SurveillanceDocument18 pagesRenal Cell Carcinoma: Diagnosis, Staging, and SurveillanceMutia IsanaNo ratings yet
- Is Surveillance Necessary For Inverted Papilloma in The Urinary Bladder and Urethra?Document5 pagesIs Surveillance Necessary For Inverted Papilloma in The Urinary Bladder and Urethra?Денис КрахоткинNo ratings yet
- Clinocopathological Features and Prognosis of Patients With de Novo Versus Nevus Associated Melanoma in TaiwanDocument16 pagesClinocopathological Features and Prognosis of Patients With de Novo Versus Nevus Associated Melanoma in Taiwanira nurinaNo ratings yet
- Anoscopy: Top 10 Forgotten Diagnostic ProceduresDocument1 pageAnoscopy: Top 10 Forgotten Diagnostic ProceduresI G. A. Ratna DewiNo ratings yet
- Cirugi A Espan Ola: Approach and Management of Traumatic Retroperitoneal InjuriesDocument10 pagesCirugi A Espan Ola: Approach and Management of Traumatic Retroperitoneal InjuriesGrace TeweNo ratings yet
- WorldJColorectalSurg8379-1147446 031114Document5 pagesWorldJColorectalSurg8379-1147446 031114Pavan JonnadaNo ratings yet
- Efficacy and Safety of Endoscopic Nasopharyngectomy Combined With Low-Dose Radiotherapy For Primary T1-2 Nasopharyngeal CarcinomaDocument7 pagesEfficacy and Safety of Endoscopic Nasopharyngectomy Combined With Low-Dose Radiotherapy For Primary T1-2 Nasopharyngeal CarcinomaRoger J MorenoNo ratings yet
- Gynecologic Oncology: Yipin Cai, Weiqi Sheng, Libing Xiang, Xiaohua Wu, Huijuan YangDocument5 pagesGynecologic Oncology: Yipin Cai, Weiqi Sheng, Libing Xiang, Xiaohua Wu, Huijuan YangMarcella Bastos PersianoNo ratings yet
- Ultrasonographic Features of Tuberculous Cervical LymphadenitisDocument6 pagesUltrasonographic Features of Tuberculous Cervical LymphadenitisAisahNo ratings yet
- S155876732100080XDocument7 pagesS155876732100080XArais AraisNo ratings yet
- (2018) Aggresiveness of Solid Pseudopapillary Neoplasm Literature Review and MetanalysisDocument7 pages(2018) Aggresiveness of Solid Pseudopapillary Neoplasm Literature Review and MetanalysispengadaanNo ratings yet
- Appendiceal Mucinous Adenocarcinoma With Concurrent Tuberculous Appendix: An Unusual Overlap of Two Rare DiseasesDocument1 pageAppendiceal Mucinous Adenocarcinoma With Concurrent Tuberculous Appendix: An Unusual Overlap of Two Rare DiseasesKhei Jazzle LimNo ratings yet
- Spontaneous Regression of Pancreatic Cancer: A Case Report and Literature ReviewDocument5 pagesSpontaneous Regression of Pancreatic Cancer: A Case Report and Literature ReviewHitomi-No ratings yet
- Appendicitis 2021Document13 pagesAppendicitis 2021JorgeNo ratings yet
- (Ayuda) Surg2 Le1 RecallsDocument11 pages(Ayuda) Surg2 Le1 RecallsFrances DeiNo ratings yet
- Follicular Thyroid Carcinoma Presenting With EndobDocument5 pagesFollicular Thyroid Carcinoma Presenting With EndobSmriti LakraNo ratings yet
- 9 PDFDocument4 pages9 PDFtriNo ratings yet
- Anal Cancer, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandAnal Cancer, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- A Simple Guide to Nasopharyngeal Cancer, Diagnosis, Treatment, and Related ConditionsFrom EverandA Simple Guide to Nasopharyngeal Cancer, Diagnosis, Treatment, and Related ConditionsNo ratings yet
- G.G.GUPTA & Associates Advocates & Tax Consultants (GST & Custom) Office:-302, Aggrawal Tower, Netaji Subesh Place, Pitampura, New Delhi-34 Mobile No 8459466042Document6 pagesG.G.GUPTA & Associates Advocates & Tax Consultants (GST & Custom) Office:-302, Aggrawal Tower, Netaji Subesh Place, Pitampura, New Delhi-34 Mobile No 8459466042Utkarsh KhandelwalNo ratings yet
- Research Methods in Clinical PsychologyFINISHED AllanDocument33 pagesResearch Methods in Clinical PsychologyFINISHED AllanAllan DiversonNo ratings yet
- Nirav Industrial Training Ppt-1.NewDocument15 pagesNirav Industrial Training Ppt-1.NewMehul ThakkarNo ratings yet
- Chapter 1Document30 pagesChapter 1Melaku WalelgneNo ratings yet
- Module 3 - SociologyDocument74 pagesModule 3 - SociologyakshayaNo ratings yet
- Plan A 2025 CommitmentsDocument20 pagesPlan A 2025 CommitmentsReswinNo ratings yet
- South Carolina In-Patient Drug & Alcohol Treatment ProgramsDocument2 pagesSouth Carolina In-Patient Drug & Alcohol Treatment ProgramsABC News 4100% (1)
- Mater Maternity Booking Form V2 - March17 (Not For Record)Document1 pageMater Maternity Booking Form V2 - March17 (Not For Record)Oliver JanevNo ratings yet
- ALT GPT (IFCC) Single Vial: BiolaboDocument2 pagesALT GPT (IFCC) Single Vial: Biolabowindy ajengNo ratings yet
- Matching Heading PDFDocument6 pagesMatching Heading PDFUyen TranNo ratings yet
- Tamil Nadu National Law School: TiruchirappalliDocument14 pagesTamil Nadu National Law School: Tiruchirappallidynamo vjNo ratings yet
- Book - Health and WellnessDocument10 pagesBook - Health and WellnessWill AsinNo ratings yet
- Policloropreno FDADocument4 pagesPolicloropreno FDAAlejandro ZagalNo ratings yet
- Physical Inactivity TestDocument66 pagesPhysical Inactivity TestNHEMSTERS xoxoNo ratings yet
- Mavalli Tiffin Room (MTR) : A Brand HistoryDocument12 pagesMavalli Tiffin Room (MTR) : A Brand HistoryRohit GunwaniNo ratings yet
- CREP GuidelinesDocument32 pagesCREP Guidelinesamol76No ratings yet
- Risk For Impaired Skin IntegrityDocument4 pagesRisk For Impaired Skin IntegrityArelys Rodriguez100% (2)
- AnthropometryDocument6 pagesAnthropometryNRheena NJane NSenidoNo ratings yet
- Microbiology TortoraDocument33 pagesMicrobiology TortoraLaizaEuniceT.Monte100% (1)
- SenaDocument2 pagesSenaRejzl Awit100% (1)
- CAPSTONE2022Document170 pagesCAPSTONE2022Charisse Jean PelominoNo ratings yet
- Hepatitis B Cases StudiesDocument53 pagesHepatitis B Cases Studiesrieza_huseinNo ratings yet
- 114 247 1 SMDocument6 pages114 247 1 SMAzhar FauzanNo ratings yet
- Memorandum - Circular - No - 21-32 (DTI Operational Capacity Under Alert Level System)Document11 pagesMemorandum - Circular - No - 21-32 (DTI Operational Capacity Under Alert Level System)Brian TomasNo ratings yet
- Alison Morton-Cooper Health Care and The Autism Spectrum A Guide For Health Professionals, Parents and Carers 2004Document130 pagesAlison Morton-Cooper Health Care and The Autism Spectrum A Guide For Health Professionals, Parents and Carers 2004lillouana100% (1)
- Bisex Couple Tbilisi Escort From Tbilisi - EscortHubDocument1 pageBisex Couple Tbilisi Escort From Tbilisi - EscortHubsmallsabi226No ratings yet
- Dental BooklistDocument14 pagesDental Booklistالمكتبة المليونيةNo ratings yet
- Unit 2 - Role of Social Worker in Health FieldDocument10 pagesUnit 2 - Role of Social Worker in Health FieldDharek IleshNo ratings yet
- Induction Program ScriptDocument2 pagesInduction Program ScriptAl-var A AtibingNo ratings yet
- BioavailabilityDocument15 pagesBioavailabilitywriter noreenNo ratings yet
Acantosis Nigricans Maligna
Acantosis Nigricans Maligna
Uploaded by
David BravoCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Acantosis Nigricans Maligna
Acantosis Nigricans Maligna
Uploaded by
David BravoCopyright:
Available Formats
OncoTargets and Therapy Dovepress
open access to scientific and medical research
Open Access Full Text Article
C A S E R E P O RT
Malignant Acanthosis Nigricans with Recurrent
Bladder Cancer: A Case Report and Review of
OncoTargets and Therapy downloaded from https://www.dovepress.com/ by 157.44.15.237 on 13-Mar-2021
Literature
This article was published in the following Dove Press journal:
OncoTargets and Therapy
Rongxin Zhang Abstract: Acanthosis nigricans (AN) is a rare cutaneous condition that may be
Meiya Jiang a manifestation of certain endocrinological or autoimmune diseases, as well as a potential
Wenyi Lei marker for underlying undiagnosed cancer. AN is classified as either benign or malignant
Aoxue Wang based on its clinical associations. Malignant acanthosis nigricans (MAN), which tends to be
For personal use only.
extensive and develops rapidly, is considered to be a paraneoplastic syndrome associated
Department of Dermatology, The Second
with advanced cancer, commonly accompanied by intra-abdominal malignancies. Bladder
Hospital of Dalian Medical University,
Dalian, Liaoning, 116027, People’s cancer with AN concomitant with tripe palms (TP) and/or mucosal involvement is relatively
Republic of China rare and, to our knowledge, only seven cases of AN with bladder cancer have been reported
in the English literature. However, to date, there have been no reports of bladder cancer with
AN concomitant with TP, skin and mucosal involvement. Here, we present a case of a 71-
year-old male diagnosed with AN coexisting with recurrent bladder cancer and simultaneous
TP and oral AN. In addition, we provide a brief review of the available literature on this
topic. Early recognition of skin features associated with internal malignancies provides an
opportunity for early diagnosis, treatment of the internal malignancy and monitoring of
tumor recurrence.
Keywords: malignant acanthosis nigricans, bladder cancer, tripe palms, oral acanthosis
nigricans
Introduction
Acanthosis nigricans (AN) is characterized by thick velvety hyperpigmented plaques
of the intertriginous areas, and less commonly, extensor areas of the skin. AN
represents a rare cutaneous condition that may be a manifestation of certain endocri
nological or autoimmune diseases, and even serve as a potential marker for underlying
undiagnosed cancer.1 There are two forms of AN, benign or malignant, which are
based upon clinical associations. Malignant acanthosis nigricans (MAN) is considered
as a paraneoplastic syndrome coexistent with advanced cancer. It is usually associated
with intra-abdominal malignancies, with gastric adenocarcinoma being the most
common, followed by pancreatic, ovary, lung, esophageal, breast, renal cell and
bladder cancers.2 MAN lesions mainly appear as hyperpigmented foci which later
Correspondence: Aoxue Wang
Department of Dermatology, The Second transform into papillary lesions. MAN tends to be extensive, with rapidly developing
Hospital of Dalian Medical University, changes in the skin often accompanied by mucosal involvement, seborrheic keratoses
Dalian, Liaoning, 116027, People’s
Republic of China and tripe palms (TP).1 TP, which is generally related to pulmonary and gastric
Tel +86-17709875795 carcinoma, rarely appears on the skin surface of the hands. Due to the similarities in
Fax +86-411-84672130
Email wangaxdl@163.com histopathological characteristics with AN, some investigators consider TP as a subtype
submit your manuscript | www.dovepress.com OncoTargets and Therapy 2021:14 951–957 951
DovePress © 2021 Zhang et al. This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.
http://doi.org/10.2147/OTT.S290124
php and incorporate the Creative Commons Attribution – Non Commercial (unported, v3.0) License (http://creativecommons.org/licenses/by-nc/3.0/). By accessing the
work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For
permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms (https://www.dovepress.com/terms.php).
Powered by TCPDF (www.tcpdf.org)
Zhang et al Dovepress
of AN. However, TP is generally more discernable and does medical history, he was initially diagnosed with urinary
not involve the soles.2 Moreover, the location and probabil bladder cancer in 2007. At that time, he received TUR-BT
ity of mucosal involvement differ in AN, and hyperpigmen surgery followed by regular administrations of intravesical
tation is often absent on mucosal sites. chemotherapy. In 2013, he was diagnosed with rectal cancer
Of the two forms of AN, MAN has a lower incidence and underwent laparoscopic surgery followed by regular
and is more frequently observed in the middle-aged and chemotherapy. He was then diagnosed with urinary bladder
elderly. According to the literature, an association of MAN cancer in 2014, and again underwent TUR-BT surgery fol
with bladder cancer is relatively rare. Here, we report one lowed by intravesical chemotherapy. Additionally, the patient
OncoTargets and Therapy downloaded from https://www.dovepress.com/ by 157.44.15.237 on 13-Mar-2021
such rare case of a patient with mucosal and cutaneous AN had a history of hypertension for more than 10 years. There
and TP along with recurrent bladder cancer. In addition, we was no history of steroid medication use, endocrine abnorm
present a brief review of the available literature on this topic. alities, hepatitis, other autoimmune diseases or familial her
editary diseases. Family members were unaffected.
Case Presentation Physical examination revealed numerous grey and
A 71-year-old male presented with a history of AN lesions on brown skin papillary papules or verrucous nodules
the hands, feet, fold areas, face and oral cavity that had been observed in the axillary and inguinal areas, along with
present for approximately 4 months. The initial lesions diffuse hyperkeratosis and waxy-yellow lesions in the
appeared as hyperpigmentation, with a rough and thickened palms and plantar surfaces. Clinical examination of the
skin surface and mild pruritus, present on the hands, feet, oral cavity revealed hypertrophic lesions and papillomato
For personal use only.
axillary and inguinal regions. Subsequently, lesions also sis on the buccal mucosa, gingiva and a glossy tongue
emerged on the face, neck, back of the ears and oral cavity. without moss (Figure 1A–G). There were no apparent
He was treated with an oral administration of avermectin abnormalities in the toenails and hair.
A and traditional Chinese medicines along with topical ster Based on these findings and the exclusion of other
oids and urea vitamin E ointment with no clinical improve diseases, there was a suspicion of AN resulting from malig
ment. The skin lesions gradually thickened, developing nant tumors. Accordingly, assays for specific serum tumor
into wart-like hyperplasias or tumor-like lesions and addi markers and endocrine measurements were performed,
tional lesions associated with burning sensations surfaced on including AFP, CEA, CA125, CA19-9 and CYFRA 21–1,
the buccal mucosa and tongue. According to the patient’s along with an assessment of hypothalamic/pituitary/adrenal
Figure 1 Acanthosis nigricans on the surfaces of hands (A), feet (B), axilla (C and D), inguinal area (E) and oral cavity (F and G).
952 submit your manuscript | www.dovepress.com OncoTargets and Therapy 2021:14
DovePress
Powered by TCPDF (www.tcpdf.org)
Dovepress Zhang et al
(HPA) gland axis secretory function. Assay results of these
tumor markers indicated slight increases in CYFRA21-1
(3.84 ng/mL) and CEA (6.39 ng/mL), with levels of all
other tumor markers being within normal limits. Similarly,
tests of HPA gland secretory function (such as serum tes
tosterone, thyrotrophic hormone, adrenocorticotropic hor
mone and cortisol), as well as routine biochemical
indicators, were all within normal limits. Ultrasound exam
OncoTargets and Therapy downloaded from https://www.dovepress.com/ by 157.44.15.237 on 13-Mar-2021
ination of superficial lymph nodes revealed enlarged lymph
nodes in the left inguinal region, with the largest being
35 mm in diameter. Results from PET-CT imaging
showed: 1) that metabolic status of the bladder wall could
not be evaluated due to the concentration of urine in the
bladder, 2) the presence of multiple hypermetabolic lymph
nodes in the paravertebral, retroperitoneal and bilateral iliac
vessels, which along with those present in the bilateral
pelvic wall and left inguinal region, were considered as
sources for metastasis, 3) that the medial tubercle of the
For personal use only.
left paravertebral erector muscle was also considered as
a source for metastasis, and 4) that the diffuse increases in
metabolic activity present in the esophagus require further
endoscopy examination (Figure 2). Gastroscopy revealed
multiple esophageal eminences, with pathological findings
being consistent with AN (Figure 3A–D). Pathology exam
inations of the left inguinal lesion revealed hyperkeratosis
of the epidermis, papillomatous hyperplasia and sparse
lymphocyte infiltration in the superficial dermis, also con
sistent with AN (Figure 4). Results from HE-staining of the
biopsied left inguinal lymph node revealed that nested
masses of cancer cells were present. Immunohistochemical
staining for GATA-3, P40, CK7 and CK20 were positive,
Villin was partially positive and CDX2 was negative in the
cancer cells of the inguinal lymph node. When combining
the staining results from the biopsied left inguinal lymph
node and the patient’s history, the origin of metastasis is
considered to be urothelial cancer (Figure 5A–G).
When collating this information on history, skin lesions
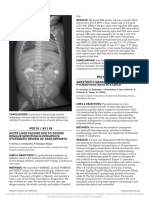
Figure 2 PET-CT results showing multiple hypermetabolic lymph nodes considered
and pathology, PET-CT and lymph node biopsy, a clinical metastatic within paravertebral, retroperitoneal, bilateral iliac vessels, bilateral
diagnosis of MAN with recurrent bladder cancer was con pelvic wall, left inguinal area and medial tubercle of the left paravertebral erector
muscle.
firmed. After diagnosis, the patient was transferred to the
Oncology Department for systemic chemotherapy. He
monoclonal antibody, tislelizumab, and follow-up in the
underwent a chemotherapy regimen consisting of gemci
Oncology Department.
tabine and cisplatin every 3 weeks for 5 cycles. After three
cycles, hyperkeratosis of the hands and feet, hyperpigmen
tation and verrucous hyperplasia in the axillary and ingu Discussion
inal regions and lesions in the oral cavity were all AN, also known as melanokeratosis, was first described by
significantly improved (Figure 6A–F). Currently, the Pollitzer.3 It is a rare skin disease characterized by hyperpig
patient is receiving immunotherapy with the anti-PD-1 mentation, hyperkeratosis, velvety thickening and verrucous
submit your manuscript | www.dovepress.com
OncoTargets and Therapy 2021:14 953
DovePress
Powered by TCPDF (www.tcpdf.org)
Zhang et al Dovepress
OncoTargets and Therapy downloaded from https://www.dovepress.com/ by 157.44.15.237 on 13-Mar-2021
For personal use only.
Figure 3 Gastroscopy revealing multiple esophageal eminences (A and B), and the pathological findings of esophageal hyperplasia (C and D) which were consistent with AN
(HE stain ×100).
induced and mixed-type.4 The main histological features of
AN are hyperkeratosis and papillomatosis.2 The principal
interest in AN resides in its association with malignancy,
along with the clinical manifestations of skin lesions and
the rapid and potentially lethal nature of the disease. With
regard to MAN, the malignant form of AN, this condition is
common in the middle-aged and elderly and almost always
involves visceral tumors. The most common histological
types of MAN-associated tumors involve adenocarcinomas,
especially gastric adenocarcinoma, followed by pancreatic,
ovary, lung, esophageal, breast, renal cell and bladder can
cers. In most cases of MAN (61.3%), there is a simultaneous
diagnosis of cancer. AN occurs prior to cancer diagnosis in
Figure 4 Pathological findings of the left inguinal lesion revealed hyperkeratosis of approximately 17.6% of cases and follows a cancer diagnosis
the epidermis, papillomatous hyperplasia, and sparse lymphocyte infiltration in the in approximately 21.1% of cases.2,5
superficial dermis (HE stain ×100).
The development of lesions associated with MAN are
rapid, serious and extensive, with the underlying mechan
hyperplasia that can occur on any part of the body, but isms for these effects remaining unclear. Results from
characteristically affects fold areas, such as axillae, neck, previous studies have indicated that these effects may be
inguinal, antecubital and popliteal surfaces. Clinically, as related to the secretion of certain cytokines by malignant
based upon the description of Schwartz, eight different tumors. Some examples of these cytokines include tumor-
types of AN have been described: benign, malignant, obe derived growth factor, alpha-melanocyte-stimulating fac
sity-associated, syndromic, acral, unilateral, medication- tor, peptide substances, platelet-derived growth factor,
954 submit your manuscript | www.dovepress.com OncoTargets and Therapy 2021:14
DovePress
Powered by TCPDF (www.tcpdf.org)
Dovepress Zhang et al
OncoTargets and Therapy downloaded from https://www.dovepress.com/ by 157.44.15.237 on 13-Mar-2021
Figure 5 Results of left inguinal lymph node biopsy revealed that nested mass cancer cells were present (A) (HE stain ×100). Cancer cells in the inguinal lymph node were
positive for GATA-3 (B), P40 (C), CK20 (D), CK7 (E), partially positive for Villin (F) and negative for CDX2 (G) (Immunohistochemical stain ×100).
For personal use only.
Figure 6 After three courses of chemotherapy, hyperkeratosis of the hands and feet (A–C), pigmentation and verrucous hyperplasia on the axillary (D) and inguinal (E)
regions and lesions in the oral cavity (F) were all significantly improved.
insulin-like growth factor-1 and, in particular, transform suddenly, progressed rapidly and was accompanied by
ing growth factor-alpha (TGF-α), whose effects on the mucosal involvement. Skin and esophageal histopathology
epidermal growth factor receptor (EGFR) lead to the pro were consistent with AN. There were no significant
liferation of keratinocytes and dermal fibroblasts.4,5 The abnormalities in the determination of cortical axis, islet
differentiation of keratinocytes can be partially inhibited function and blood sugar levels after admission. Due to
with activation of the ERK signaling pathway, which a high suspicion of malignant tumors in this AN patient,
results in a verrucous appearance of the epidermis. systematic examinations were performed. Multiple
The patient in our case report had a history of malig enlarged lymph nodes were detected in the left inguinal
nant tumors from the bladder and rectal cancer that were region by color Doppler ultrasonography and results of
treated surgically and with a regular follow-up of che PET-CT scans revealed multiple lymph node metastases.
motherapy. However, the AN in this patient occurred A diagnosis of MAN was confirmed based upon the skin
submit your manuscript | www.dovepress.com
OncoTargets and Therapy 2021:14 955
DovePress
Powered by TCPDF (www.tcpdf.org)
Zhang et al Dovepress
Table 1 Summary of Clinical Data on Patients with Bladder Cancer and AN and/or TP and/or Oral AN from 1983 to 2020
Case Age Gender Clinical Manifestations With Bladder Cancer Tumor Condition REF
Skin AN TP Oral AN Prior Follow Initial Recurrent Metastasis
1 65 F Y N Y Y Y Y [5]
2 69 F Y Y N Y Y Y [6]
3 70 M Y Y N Y Y Y [7]
4 78 F Y N Y Y Y [8]
OncoTargets and Therapy downloaded from https://www.dovepress.com/ by 157.44.15.237 on 13-Mar-2021
5 73 M Y N Y Y Y [9]
6 46 M Y N N Y Y [10]
7 40 F Y Unk N Y Y Unk [11]
8 71 M Y Y Y Y Y Y This case
Abbreviations: AN, acanthosis nigricans; TP, tripe palms; F, female; M, male; Y, yes; N, no; Unk, unknown; REF, reference.
lesions, histopathology and PET-CT findings. Results from accompanied with TP, skin and mucosal involvement. The
the biopsy of the left inguinal lymph nodes suggested that severity of skin lesions in MAN is closely related to the
the origin of metastases was urothelial carcinoma. Given occurrence and development of tumors, and these skin
the past history of two bladder cancers in this patient, we symptoms can significantly improve after the treatment
considered the recurrence of bladder cancer metastasis as of potential tumors, as was observed in our patient.
For personal use only.
leading to MAN. While digestive system tumors are com Although MAN usually has no specific treatment protocol,
mon in MAN-associated tumors, clinical reports of bladder AN may be treated with retinoic acid or PUVA (psoralen
cancer with AN are relatively rare. To our knowledge, only photochemotherapy), with limited effectiveness.
seven cases of AN have been reported in the English The degree of MAN malignancy is often greater when
literature as summarized in Table 1.5–11 However, there associated with tumors and, under such conditions, the
have been no such cases reported within China. Following disease progresses rapidly. Our case as reported here high
this diagnosis, the patient was transferred to the Oncology lights the relationship between the coexistence of skin
Department for systematic chemotherapy. After three markers and internal malignancies and thus the need to
courses of chemotherapy, the skin condition dramatically identify the source of the potential primary malignancy.
improved, likely through blocking the production of cyto Early recognition of these skin features provides an oppor
kines released by the tumors. In this way, AN can serve as tunity for early diagnosis, treatment of internal malignan
a principal cutaneous marker of internal malignancy and as cies and monitoring of tumor recurrence.
an index to evaluate the condition, efficacy and recurrence
of malignancy. We are reminded from this case that MAN, Conclusion
as associated with bladder cancer, should raise the suspi In summary, MAN represents an extensive and rapidly
cion of its metastasizing process. developing skin condition, which is considered to be
Lesions in the oral cavity are more common in patients a paraneoplastic syndrome associated with advanced cancer.
with MAN.5 Extensive papillary lesions of the lip, gingiva, In the present case, MAN was diagnosed based upon typical
palate and tongue are all characteristics of oral AN, which skin lesions, histopathology and PET-CT findings. While
may then spread to the nose, throat or esophagus.5,12 The MAN usually has no specific treatment protocol, the MAN
presence of mucosal involvement in MAN should be in this case improved after chemotherapy. The presence of
regarded as a significant clinical sign due to the high mucosal involvement and TP in MAN should alert the
incidence of tumors in patients with mucosal lesions.9 In clinicians to the possibility of a high incidence of tumors.
our current case, lesions were not only observed in the To our knowledge, there have been no case reports in the
buccal mucosa but also the esophagus. The presence of TP literature of bladder cancer with AN accompanied with TP
represents another potential skin manifestation of a tumor. along with skin and mucosal involvement. Our case as
While tumors with TP and/or mucosal involvement have reported here highlights the relationship between the coex
been reported extensively within the literature, to date, istence of skin markers and internal malignancies and thus
there has been no case report of bladder cancer with AN the need to identify the source of the potential primary
956 submit your manuscript | www.dovepress.com OncoTargets and Therapy 2021:14
DovePress
Powered by TCPDF (www.tcpdf.org)
Dovepress Zhang et al
malignancy. Early recognition of these skin features pro
vides an opportunity for early diagnosis, treatment of inter References
nal malignancies and monitoring of tumor recurrence. 1. Patel NU, Roach C, Alinia H, Huang WW, Feldman SR. Current
treatment options for acanthosis nigricans. Clin Cosmet Investig
Dermatol. 2018;11:407–413. doi:10.2147/CCID.S137527
2. Pentenero M, Carrozzo M, Pagano M, Gandolfo S. Oral acanthosis
Abbreviations nigricans, tripe palms and sign of leser-trélat in a patient with gastric
AN, acanthosis nigricans; MAN, malignant acanthosis adenocarcinoma. Int J Dermatol. 2004;43(7):530–532. doi:10.1111/
nigricans; TP, tripe palms; TUR-BT, transurethral blad j.1365-4632.2004.02159.x.
3. Pollitzer S. Acanthosis nigricans. In: Unna PG, Morris M, Besnier E,
OncoTargets and Therapy downloaded from https://www.dovepress.com/ by 157.44.15.237 on 13-Mar-2021
der tumor resection; HPA, hypothalamus pituitary editors. Internal Atlas of Rare Skin Diseases. London, UK: Lewis and
adrenal gland; PET-CT, positron emission tomography- Co; 1891:1–3.
4. Schwartz RA. Acanthosis nigricans. J Am Acad Dermatol. 1994;31
computed tomography; CEA, carcinoembryonic anti (1):1–19.
gen; TGF-α, transforming growth factor-alpha; EGFR, 5. Olek-Hrab K, Silny W, Zaba R, Osmola-Mańkowska A, Mackiewicz-
epidermal growth factor receptor; ERK, extracellular Wysocka M, Dańczak-Pazdrowska A. Co-occurrence of acanthosis
nigricans and bladder adenocarcinoma-case report. Contemp Oncol
regulated protein kinases; PUVA, psoralen (Pozn). 2013;17(3):327–330. doi:10.5114/wo.2013.35287
photochemotherapy. 6. Möhrenschlager M, Vocks E, Wessner DB, Nährig J, Ring J. Tripe
palms and malignant acanthosis nigricans: cutaneous signs of immi
nent metastasis in bladder cancer? J Urol. 2001;165(5):1629–1630.
doi:10.1016/s0022-5347(05)66369-0.
Ethical Approval 7. Singh GK, Sen D, Mulajker DS, Suresh MS. Acanthosis nigricans asso
The patient’s informed consent for publication of the case ciated with transitional cell carcinoma of the urinary bladder. Indian
For personal use only.
details including the images was obtained. The study was J Dermatol. 2011;56(6):722–725. doi:10.4103/0019-5154.91837.
8. Canjuga I, Mravak-Stipetić M, Kopić V, Galić J. Oral acanthosis
approved by the Ethics Committee of the Second Hospital nigricans: case report and comparison with literature reports. Acta
of Dalian Medical University. Dermatovenerol Croat. 2008;16(2):91–95.
9. Cairo F, Rubino I, Rotundo R, Prato GP, Ficarra G. Oral Acanthosis
nigricans as a marker of internal malignancy. A case report.
J Periodontol. 2001;72(9):1271–1275. doi:10.1902/jop.2000.72.9.1271.
Acknowledgments 10. Gohji K, Hasunuma Y, Gotoh A, Shimogaki H, Kamidono S.
This work was supported by the Science and Technology Acanthosis nigricans associated with transitional cell carcinoma of
Innovation Foundation of Dalian, China (No.2020JJ the urinary bladder. Int J Dermatol. 1994;33(6):433–435.
doi:10.1111/j.1365-4362.1994.tb04046.x.
27SN073) and the Natural Science Foundation of Liaoning 11. Pinto WBVR, Badia BML, Souza PVS, Oliveira ASB, Silva LHL,
Province, China (No.2020-MS-262). Farias IB. Paraneoplastic motor neuronopathy and malignant
acanthosis nigricans. Arq Neuropsiquiatr. 2019;77(7):527. doi:10.
1590/0004-282X20190076.
12. Ramirez-Amador V, Esquivel-Pedraza L, Caballero-Mendoza E,
Disclosure Berumen-Campos J, Orozco-Topete R, Angeles-Angeles A. Oral mani
The authors declare no conflicts of interest in this work. festations as a hallmark of malignant acanthosis nigricans. J Oral Pathol
Med. 1999;28(6):278–281. doi:10.1111/j.1600-0714.1999.tb02039.x
OncoTargets and Therapy Dovepress
Publish your work in this journal
OncoTargets and Therapy is an international, peer-reviewed, open agents and protocols on patient perspectives such as quality of life,
access journal focusing on the pathological basis of all cancers, adherence and satisfaction. The manuscript management system is
potential targets for therapy and treatment protocols employed to completely online and includes a very quick and fair peer-review
improve the management of cancer patients. The journal also system, which is all easy to use. Visit http://www.dovepress.com/
focuses on the impact of management programs and new therapeutic testimonials.php to read real quotes from published authors.
Submit your manuscript here: https://www.dovepress.com/oncotargets-and-therapy-journal
submit your manuscript | www.dovepress.com
OncoTargets and Therapy 2021:14 957
DovePress
Powered by TCPDF (www.tcpdf.org)
Copyright of OncoTargets & Therapy is the property of Dove Medical Press Ltd and its
content may not be copied or emailed to multiple sites or posted to a listserv without the
copyright holder's express written permission. However, users may print, download, or email
articles for individual use.
You might also like
- Rectal Cancer With Synchronous Tonsillar Metastasis: A Case Report and Literature ReviewDocument3 pagesRectal Cancer With Synchronous Tonsillar Metastasis: A Case Report and Literature ReviewKresna ArdinugrahaNo ratings yet
- 69 63 PBDocument8 pages69 63 PBsepputriNo ratings yet
- Circulating Cell-Free DNA or Circulating Tumor DNA in The Management of Ovarian and Endometrial CancerDocument14 pagesCirculating Cell-Free DNA or Circulating Tumor DNA in The Management of Ovarian and Endometrial CancerSergio J Calleja FreixesNo ratings yet
- Analysis of Clinicopathological Features of Cervical MucinouDocument9 pagesAnalysis of Clinicopathological Features of Cervical MucinouFlaviu Ionuț FaurNo ratings yet
- Spectrum of Histomorphological Diagnosis in Cystoscopic Bladder BiopsiesDocument4 pagesSpectrum of Histomorphological Diagnosis in Cystoscopic Bladder BiopsieskushalNo ratings yet
- Pi Is 1474442217300595Document1 pagePi Is 1474442217300595Zulvina FaozanudinNo ratings yet
- Urachal Carcinoma With Liver Lung and Brain MetastDocument5 pagesUrachal Carcinoma With Liver Lung and Brain Metast7fkqx7zh7pNo ratings yet
- BIBL 12 Liver MetastasisDocument3 pagesBIBL 12 Liver Metastasisstoia_sebiNo ratings yet
- Tomlinson Acp2010Document1 pageTomlinson Acp2010Rayan BossNo ratings yet
- 1 s2.0 S2210261221006337 MainDocument5 pages1 s2.0 S2210261221006337 MainRubén LimaNo ratings yet
- Tabrizi An 2009Document4 pagesTabrizi An 2009Dung Tran HoangNo ratings yet
- 10.1016@S1470 20451930318 3Document10 pages10.1016@S1470 20451930318 3FistiNo ratings yet
- Van Nieuwenhove Et Al 2021 Imaging of Traumatic and Atraumatic Penile LumpsDocument2 pagesVan Nieuwenhove Et Al 2021 Imaging of Traumatic and Atraumatic Penile LumpsThesisaurus IDNo ratings yet
- Diagnosis and Treatment of Radiation ProctitisDocument2 pagesDiagnosis and Treatment of Radiation ProctitispatNo ratings yet
- VASC 014 - Bilateral Testicular Cancer A Rare Case ReportDocument1 pageVASC 014 - Bilateral Testicular Cancer A Rare Case ReporttiopanNo ratings yet
- Jurnal 1Document5 pagesJurnal 1Nur Syamsiah MNo ratings yet
- Histopathologic Analysis of Appendectomy Specimens: Shrestha R, Ranabhat SR, Tiwari MDocument5 pagesHistopathologic Analysis of Appendectomy Specimens: Shrestha R, Ranabhat SR, Tiwari Mmau tauNo ratings yet
- Journal Reading Tahap 2 Sub Bagian Gastroentero HepatologiDocument27 pagesJournal Reading Tahap 2 Sub Bagian Gastroentero HepatologiherdianNo ratings yet
- Group 12 Revisi 3Document7 pagesGroup 12 Revisi 3Nur Apipa DaudNo ratings yet
- Gervaz Et Al - Squamous Cell Carcinoma of The Anus - Another Sexually Transmitted DiseaseDocument9 pagesGervaz Et Al - Squamous Cell Carcinoma of The Anus - Another Sexually Transmitted DiseasenamirohsamiyahNo ratings yet
- Usg ToaDocument6 pagesUsg ToaMuhammad Nugie ZifiNo ratings yet
- Ijn S232777Document14 pagesIjn S232777BHUMI BHATTNo ratings yet
- P0710 1116 Acute Liver Failure Due To Severe.767Document1 pageP0710 1116 Acute Liver Failure Due To Severe.767Marselya GaniNo ratings yet
- Feature: 106 Emergency MedicineDocument8 pagesFeature: 106 Emergency MedicinehakimNo ratings yet
- Aydin 2016Document5 pagesAydin 2016nurfitriaNo ratings yet
- Derrame Pleural 2015Document16 pagesDerrame Pleural 2015MARIA NEGRETE MOSCOTENo ratings yet
- Malignant Acanthosis Nigricans: An Early Diagnostic Clue: Case ReportDocument3 pagesMalignant Acanthosis Nigricans: An Early Diagnostic Clue: Case Reportilham raymanaNo ratings yet
- Paraneoplastic PCaDocument12 pagesParaneoplastic PCaBrendan DiasNo ratings yet
- Janczak Et Al. - 2016 - An Evaluation of The Diagnostic Efficacy of Fine NDocument5 pagesJanczak Et Al. - 2016 - An Evaluation of The Diagnostic Efficacy of Fine NHaziel CorroNo ratings yet
- Endoscopic Ultrasound Staging of Gastric LymphomaDocument3 pagesEndoscopic Ultrasound Staging of Gastric LymphomaEvainoirNo ratings yet
- Nasopharyngeal Carcinoma: Imaging Features of Unusual Cancer in ChildrenDocument5 pagesNasopharyngeal Carcinoma: Imaging Features of Unusual Cancer in ChildrenDevanti EkaNo ratings yet
- Paraneoplastic Syndromes Associated With LaryngealDocument15 pagesParaneoplastic Syndromes Associated With Laryngealandre halimNo ratings yet
- Adult Desmoid Tumors: Biology, Management and Ongoing TrialsDocument7 pagesAdult Desmoid Tumors: Biology, Management and Ongoing TrialsGustavo GasperiNo ratings yet
- Ijwh 178349 Triple Negative Breast Cancer Current Perspective On The EvDocument7 pagesIjwh 178349 Triple Negative Breast Cancer Current Perspective On The EvMuhammad FauzanNo ratings yet
- Ameboma of Colon Simulating Colonic Adenocarcinoma: Case ReportDocument3 pagesAmeboma of Colon Simulating Colonic Adenocarcinoma: Case ReportJulio BarajasNo ratings yet
- Ijpd 24 221Document2 pagesIjpd 24 221intan yunni aztiNo ratings yet
- DuodenalcarcinoidDocument5 pagesDuodenalcarcinoidMudassar SattarNo ratings yet
- Shi 2017Document8 pagesShi 2017Claudia Ivette Villarreal OvalleNo ratings yet
- Hernandez 2008Document2 pagesHernandez 2008asialoren74No ratings yet
- Unknown Primary Cancer of The Head and Neck - A MultidisciplinaryDocument10 pagesUnknown Primary Cancer of The Head and Neck - A MultidisciplinaryFreddy Eduardo Navarro BautistaNo ratings yet
- Primary Congenital Choledochal Cyst With Squamous Cell Carcinoma: A Case ReportDocument6 pagesPrimary Congenital Choledochal Cyst With Squamous Cell Carcinoma: A Case ReportRais KhairuddinNo ratings yet
- Renal Cell Carcinoma: Diagnosis, Staging, and SurveillanceDocument18 pagesRenal Cell Carcinoma: Diagnosis, Staging, and SurveillanceMutia IsanaNo ratings yet
- Is Surveillance Necessary For Inverted Papilloma in The Urinary Bladder and Urethra?Document5 pagesIs Surveillance Necessary For Inverted Papilloma in The Urinary Bladder and Urethra?Денис КрахоткинNo ratings yet
- Clinocopathological Features and Prognosis of Patients With de Novo Versus Nevus Associated Melanoma in TaiwanDocument16 pagesClinocopathological Features and Prognosis of Patients With de Novo Versus Nevus Associated Melanoma in Taiwanira nurinaNo ratings yet
- Anoscopy: Top 10 Forgotten Diagnostic ProceduresDocument1 pageAnoscopy: Top 10 Forgotten Diagnostic ProceduresI G. A. Ratna DewiNo ratings yet
- Cirugi A Espan Ola: Approach and Management of Traumatic Retroperitoneal InjuriesDocument10 pagesCirugi A Espan Ola: Approach and Management of Traumatic Retroperitoneal InjuriesGrace TeweNo ratings yet
- WorldJColorectalSurg8379-1147446 031114Document5 pagesWorldJColorectalSurg8379-1147446 031114Pavan JonnadaNo ratings yet
- Efficacy and Safety of Endoscopic Nasopharyngectomy Combined With Low-Dose Radiotherapy For Primary T1-2 Nasopharyngeal CarcinomaDocument7 pagesEfficacy and Safety of Endoscopic Nasopharyngectomy Combined With Low-Dose Radiotherapy For Primary T1-2 Nasopharyngeal CarcinomaRoger J MorenoNo ratings yet
- Gynecologic Oncology: Yipin Cai, Weiqi Sheng, Libing Xiang, Xiaohua Wu, Huijuan YangDocument5 pagesGynecologic Oncology: Yipin Cai, Weiqi Sheng, Libing Xiang, Xiaohua Wu, Huijuan YangMarcella Bastos PersianoNo ratings yet
- Ultrasonographic Features of Tuberculous Cervical LymphadenitisDocument6 pagesUltrasonographic Features of Tuberculous Cervical LymphadenitisAisahNo ratings yet
- S155876732100080XDocument7 pagesS155876732100080XArais AraisNo ratings yet
- (2018) Aggresiveness of Solid Pseudopapillary Neoplasm Literature Review and MetanalysisDocument7 pages(2018) Aggresiveness of Solid Pseudopapillary Neoplasm Literature Review and MetanalysispengadaanNo ratings yet
- Appendiceal Mucinous Adenocarcinoma With Concurrent Tuberculous Appendix: An Unusual Overlap of Two Rare DiseasesDocument1 pageAppendiceal Mucinous Adenocarcinoma With Concurrent Tuberculous Appendix: An Unusual Overlap of Two Rare DiseasesKhei Jazzle LimNo ratings yet
- Spontaneous Regression of Pancreatic Cancer: A Case Report and Literature ReviewDocument5 pagesSpontaneous Regression of Pancreatic Cancer: A Case Report and Literature ReviewHitomi-No ratings yet
- Appendicitis 2021Document13 pagesAppendicitis 2021JorgeNo ratings yet
- (Ayuda) Surg2 Le1 RecallsDocument11 pages(Ayuda) Surg2 Le1 RecallsFrances DeiNo ratings yet
- Follicular Thyroid Carcinoma Presenting With EndobDocument5 pagesFollicular Thyroid Carcinoma Presenting With EndobSmriti LakraNo ratings yet
- 9 PDFDocument4 pages9 PDFtriNo ratings yet
- Anal Cancer, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandAnal Cancer, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- A Simple Guide to Nasopharyngeal Cancer, Diagnosis, Treatment, and Related ConditionsFrom EverandA Simple Guide to Nasopharyngeal Cancer, Diagnosis, Treatment, and Related ConditionsNo ratings yet
- G.G.GUPTA & Associates Advocates & Tax Consultants (GST & Custom) Office:-302, Aggrawal Tower, Netaji Subesh Place, Pitampura, New Delhi-34 Mobile No 8459466042Document6 pagesG.G.GUPTA & Associates Advocates & Tax Consultants (GST & Custom) Office:-302, Aggrawal Tower, Netaji Subesh Place, Pitampura, New Delhi-34 Mobile No 8459466042Utkarsh KhandelwalNo ratings yet
- Research Methods in Clinical PsychologyFINISHED AllanDocument33 pagesResearch Methods in Clinical PsychologyFINISHED AllanAllan DiversonNo ratings yet
- Nirav Industrial Training Ppt-1.NewDocument15 pagesNirav Industrial Training Ppt-1.NewMehul ThakkarNo ratings yet
- Chapter 1Document30 pagesChapter 1Melaku WalelgneNo ratings yet
- Module 3 - SociologyDocument74 pagesModule 3 - SociologyakshayaNo ratings yet
- Plan A 2025 CommitmentsDocument20 pagesPlan A 2025 CommitmentsReswinNo ratings yet
- South Carolina In-Patient Drug & Alcohol Treatment ProgramsDocument2 pagesSouth Carolina In-Patient Drug & Alcohol Treatment ProgramsABC News 4100% (1)
- Mater Maternity Booking Form V2 - March17 (Not For Record)Document1 pageMater Maternity Booking Form V2 - March17 (Not For Record)Oliver JanevNo ratings yet
- ALT GPT (IFCC) Single Vial: BiolaboDocument2 pagesALT GPT (IFCC) Single Vial: Biolabowindy ajengNo ratings yet
- Matching Heading PDFDocument6 pagesMatching Heading PDFUyen TranNo ratings yet
- Tamil Nadu National Law School: TiruchirappalliDocument14 pagesTamil Nadu National Law School: Tiruchirappallidynamo vjNo ratings yet
- Book - Health and WellnessDocument10 pagesBook - Health and WellnessWill AsinNo ratings yet
- Policloropreno FDADocument4 pagesPolicloropreno FDAAlejandro ZagalNo ratings yet
- Physical Inactivity TestDocument66 pagesPhysical Inactivity TestNHEMSTERS xoxoNo ratings yet
- Mavalli Tiffin Room (MTR) : A Brand HistoryDocument12 pagesMavalli Tiffin Room (MTR) : A Brand HistoryRohit GunwaniNo ratings yet
- CREP GuidelinesDocument32 pagesCREP Guidelinesamol76No ratings yet
- Risk For Impaired Skin IntegrityDocument4 pagesRisk For Impaired Skin IntegrityArelys Rodriguez100% (2)
- AnthropometryDocument6 pagesAnthropometryNRheena NJane NSenidoNo ratings yet
- Microbiology TortoraDocument33 pagesMicrobiology TortoraLaizaEuniceT.Monte100% (1)
- SenaDocument2 pagesSenaRejzl Awit100% (1)
- CAPSTONE2022Document170 pagesCAPSTONE2022Charisse Jean PelominoNo ratings yet
- Hepatitis B Cases StudiesDocument53 pagesHepatitis B Cases Studiesrieza_huseinNo ratings yet
- 114 247 1 SMDocument6 pages114 247 1 SMAzhar FauzanNo ratings yet
- Memorandum - Circular - No - 21-32 (DTI Operational Capacity Under Alert Level System)Document11 pagesMemorandum - Circular - No - 21-32 (DTI Operational Capacity Under Alert Level System)Brian TomasNo ratings yet
- Alison Morton-Cooper Health Care and The Autism Spectrum A Guide For Health Professionals, Parents and Carers 2004Document130 pagesAlison Morton-Cooper Health Care and The Autism Spectrum A Guide For Health Professionals, Parents and Carers 2004lillouana100% (1)
- Bisex Couple Tbilisi Escort From Tbilisi - EscortHubDocument1 pageBisex Couple Tbilisi Escort From Tbilisi - EscortHubsmallsabi226No ratings yet
- Dental BooklistDocument14 pagesDental Booklistالمكتبة المليونيةNo ratings yet
- Unit 2 - Role of Social Worker in Health FieldDocument10 pagesUnit 2 - Role of Social Worker in Health FieldDharek IleshNo ratings yet
- Induction Program ScriptDocument2 pagesInduction Program ScriptAl-var A AtibingNo ratings yet
- BioavailabilityDocument15 pagesBioavailabilitywriter noreenNo ratings yet