Professional Documents
Culture Documents
Echocardiography in The Emergency Assessment of Acute Aortic Syndromes
Echocardiography in The Emergency Assessment of Acute Aortic Syndromes
Uploaded by
Dumitru GrozaOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Echocardiography in The Emergency Assessment of Acute Aortic Syndromes
Echocardiography in The Emergency Assessment of Acute Aortic Syndromes
Uploaded by
Dumitru GrozaCopyright:
Available Formats
European Journal of Echocardiography (2009) 10, i31–i39
doi:10.1093/ejechocard/jen251
Echocardiography in the emergency assessment
of acute aortic syndromes
E. Louise Meredith and Navroz D. Masani*
Department of Cardiology, University Hospital of Wales, Heath Park, Cardiff CF14 4XW, UK
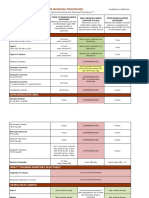
KEYWORDS Acute aortic syndrome (AAS) is a collective term for several life-threatening acute aortic conditions:
Acute aortic syndromes; aortic dissection, intramural haematoma (IMH), penetrating atherosclerotic ulcer, and traumatic tran-
Acute aortic dissection; section. Mortality from acute ascending aortic (type A) dissection increases rapidly immediately after
Intramural haematoma; presentation, reaching 1–2% per hour for the first 48 h. Early surgical intervention is recommended
Transthoracic for type A aortic dissection and has been shown to improve outcome. Transthoracic echocardiography
echocardiography; is an extremely valuable, often overlooked, clinical tool in diagnosing and assessing AAS in the emer-
Transoesophageal gency setting. Although diagnostic sensitivity is suboptimal, it is very useful in assessing potential
echocardiography high risk features or complications, such as pericardial effusion, and diagnosing potential differential
conditions. A negative transthoracic echocardiography (TTE), however, does not exclude AAS. In
patients with a high risk of type A dissection or IMH (identified clinically or by TTE), the safest and
most rapid ‘gold standard’ investigation is transoesophageal echocardiography, ideally performed
with the cardiac surgical team standing by. This is of particular importance in the haemodynamically
unstable patient. Transoesophageal echocardiography, helical CT, and MRI have similar diagnostic accu-
racy and, when there is diagnostic uncertainty or no indication for immediate intervention, should be
used according to clinical need, local availability, and expertise.
Introduction radiate to the neck in ascending aortic disease or the back
in descending aortic disease.2 The chest pain may have a
In this article, we review the role of echocardiography in the pleuritic or pericarditic nature. In type A dissection or
emergency management of acute aortic syndromes (AAS). IMH, there may be acute aortic regurgitation (AR) and
We focus on the importance of echocardiography in associated cardiac failure. There may be differences in
the early assessment of patients with suspected AAS in the upper limb blood pressure, pulse deficits, and evidence of
emergency and critical care settings. In particular, the end-organ ischaemia.3 Transient loss of consciousness is an
value of transthoracic echocardiography (TTE), often over- important presenting feature of type A dissection. Well-
looked, in the immediate management of such patients is recognized risk factors include longstanding hypertension
explored. The pivotal role of transoesophageal echocardio- and atherosclerosis as well as collagen disorders such as
graphy (TEE) is reviewed, with particular emphasis on its Marfan’s syndrome (Table 1). These patients often have sig-
value in patients requiring cardiac surgery. Finally, we nificant co morbid disease such as hypertension, coronary
describe a locally developed approach that optimizes the artery disease, and renal impairment.3
strengths of TTE, TEE, and other imaging modalities.
Acute aortic syndrome (AAS) is a collective term for
several life-threatening acute aortic conditions: aortic Pathophysiology, classification, and
dissection, intramural haematoma (IMH), penetrating ather- implications for management
osclerotic ulcer (PAU), and traumatic transection.1 Trau-
matic transection does not share pathophysiological or Aortic dissection
clinical features with the other conditions and will not be Aortic dissection occurs as a result of a tear in the intimal
considered in this article. lining of the aorta resulting in intimal exposure to elevated
Patients with AAS may have similar presenting symptoms, aortic pressures. The intima separates from the aortic wall
clinical features, and co morbid disease. Classically, AAS forming a false lumen, which runs alongside the true
patients present with severe acute chest pain which can lumen (Figure 1). The elevated pressures lead to pro-
pagation of the dissection proximally, distally or in both
* Corresponding author. Tel: þ44 2920744086; fax: þ44 2920743916. directions. A re-entrant tear may allow blood to circulate
E-mail address: navroz.masani@cardiffandvale.wales.nhs.uk through the false lumen.
Published on behalf of the European Society of Cardiology. All rights reserved. & The Author 2009.
For permissions please email: journals.permissions@oxfordjournals.org.
Downloaded from https://academic.oup.com/ehjcimaging/article-abstract/10/1/i31/2465433
by guest
on 18 December 2017
i32 E.L. Meredith and N.D. Masani
Table 1 Risk factors for the development of acute aortic
syndrome
Hypertension
Atherosclerosis
Collagen disorders
Marfans
Turners
Noonans
Ehlers danlos
Osteogenesis imperfecta
Bicuspid aortic valve
Coarctation of the aorta
Pregnancy
Trauma
Deceleration injuries, blunt trauma, penetrating injuries
Iatrogenic
Post-cardiac surgery
Cross-clamping
Coronary cannulation
Aortic valve replacement
Post-coronary angiography/angioplasty
Post-renal angioplasty
Inflammatory
Giant cell arteritis, Bechets, syphilis, aortitis
The entry tear occurs at sites of greatest wall stress. This
is most commonly within a few centimetres of the aortic
valve on the right lateral wall of the ascending aorta or
close to the ligamentum arteriosum in the descending
aorta. Sixty-five per cent of the cases occur within 3 cm of
the coronary ostia, 10% occur within the arch, and 10% in
the descending thoracic aorta.
Figure 1 Intimal flap and tear in a patient with acute type A aortic
Classification systems have been developed to describe
dissection. (A) In the transoesophageal echocardiography short-axis
the anatomic location of aortic dissection, which are view, a mobile linear flap is seen in the aortic root, just above
useful in determining prognosis and guiding management. the aortic valve leaflets (which can also be seen). The tear in the
The Stanford classification was developed from a functional flap, where the small central true lumen communicates with the
approach based on whether the ascending aorta was false lumen, is shown by the white arrow. (B) In the same patient,
involved. Type A refers to dissections involving the ascend- a 26-year-old man with no other co-morbidities, a short-axis view
ing aorta and type B the remainder.4 just below the origin of the flap, showing a bicuspid aortic valve.
In the DeBakey classification, type 1 originates in the
ascending aorta and extends to the arch or beyond. Type 2 disruption.8,9 Blood collects within the aortic media
is confined to the ascending aorta. Type 3 originated distal without the presence of a tear in the intimal lining and is
to the left subclavian and propagates to the distal descend- caused by rupture of the vasa vasorum or possibly athero-
ing thoracic (3A) or abdominal (3B) aorta.5 We will use the sclerotic plaque (Figure 2). Intramural haematoma has a
Stanford system in this article. higher rate of rupture (35%) than dissection due to its
More recently, a classification based on the pathophysiolo- closer relationship to the adventitia.10,11 Extension
gical features of the aortic lesion rather than its location has towards the lumen may result in dissection in up to 33% of
been proposed:6 Class 1: classic aortic dissection with true the cases and therefore surgical management is usually
and false lumen without communication of the two required in cases involving the ascending aorta.12
lumina; class 2: intramural haemorrhage or haematoma;
class 3: ulceration of aortic plaque following plaque Penetrating aortic ulcer
rupture; class 4: subtle or discrete aortic dissection with
bulging of the aortic wall; class 5: iatrogenic or traumatic Penetrating atherosclerotic ulcer is caused by erosion of an
aortic dissection, illustrated by a catheter induced separ- intimal atherosclerotic plaque into the media (Figure 3).
ation of the intima. Erosion into the vasa vasorum may lead to IMH formation
Thus, it is recommended that AAS be classified according and possibly dissection. Adventitial erosion may cause
to both lesion type and location.7 aneurysm formation or rupture. Rupture has been reported
in up to 42% of cases.10
Intramural haematoma Life-threatening effects of acute aortic syndrome
Intramural haematoma accounts for 3–5% of the cases of Mortality from acute ascending aortic (type A) dissection
aortic dissection that occur without apparent intimal increases rapidly immediately after presentation, reaching
Downloaded from https://academic.oup.com/ehjcimaging/article-abstract/10/1/i31/2465433
by guest
on 18 December 2017
Echocardiography in the emergency assessment of AAS i33
In the emergency setting, the clinical presentation of
patients with AAS may include chest pain, dyspnoea, hypo-
tension, and signs of heart failure. The chest X-ray may or
may not reveal a widened mediastinal contour. ECG
changes (non-specific, pericarditic, ischaemic, or infarction)
are common. Thus, there is an important differential
diagnosis, which includes acute coronary syndrome, acute
myocardial infarction (MI), pericarditis, and pulmonary
embolism (PE). Not only may consideration of these con-
ditions result in crucial delay in the diagnosis of type A
AAS, but also their initial management (in three of the
above) includes anti-platelet, anticoagulant, and thrombo-
lytic therapies, with potential disastrous results.
Therefore, a high index of clinical suspicion and the rapid
availability of diagnostic tests that are safe, sensitive, and
Figure 2 Intramural haematoma. In the transoesophageal echocar- specific are required to make the correct diagnosis and
diography short-axis view, a cross-section of the aortic root is identify those patients who need early surgery.
shown. The aortic wall is markedly thickened (white arrowheads).
The intima has areas of focal echo brightness, characteristic of
atherosclerosis—this is one method of distinguishing IMH from
thrombus within the lumen of aortic aneurysm. There is an area
Emergency assessment of suspected aortic
of echo lucency within the haematoma, but no dissection flap or dissection: the role of transthoracic
false lumen is seen. An echo free rim is seen around the aorta, echocardiography
suggestive of free blood.
Transthoracic echocardiography is safe, rapid, and readily
available in the emergency department. It should be per-
formed without delay in patients with suspected AAS, to
evaluate the presence or absence of several important fea-
tures. An ascending aortic dissection flap may be visible:
TTE has a reported sensitivity of 59–83% and a specificity of
63–93% for the diagnosis of aortic dissection.4,14,15 However,
there are no recent studies, using modern ultrasound technol-
ogy, assessing the diagnostic accuracy of TTE in AAS. It is
important to note that its sensitivity is 78–100% in type A
dissection (in which the diagnosis needs to be made most
rapidly) but is only 31–55% in dissection of the descending
aorta (in which there is less urgency, since there is a lower
early mortality and no indication for early surgery). Regardless
of the visualization of a dissection flap, TTE is useful in
almost all such patients: the presence of a bicuspid aortic
valve (particularly in a young patient with chest pain), AR, a
dilated aortic root with associated pericardial effusion, or
regional wall motion abnormality (particularly inferior hypoki-
Figure 3 Penetrating atherosclerotic aorta. A transoesophageal
nesia) is suggestive of acute type A dissection, whereas their
echocardiography image of the descending aorta showing severe
absence is reassuring (but cannot definitely exclude AAS).
atheroma with a localized, bulge associated with plaque rupture
(white arrow). Transthoracic echocardiography is also useful in establish-
ing or excluding the differential diagnosis in the acutely
1–2% per hour for the first 48 h,13 i.e. there is an approximate unwell patient, particularly in the absence of aortic root
50% mortality rate after 48 h. Ascending aorta IMH and PAU dilatation: MI (large regional wall motion abnormality), peri-
are likewise at increased risk of lethal complications. cardial effusion, and PE (right heart dilatation, etc.).
In all AAS, death can ensue from aortic rupture. In Finally, in those patients in whom a dissection flap can be
addition, the potential lethal complications of type A dissec- seen, TTE can identify those features of type A dissection
tion arise from (i) its proximity to the heart, (ii) the intra- that indicate high risk—severe proximal aortic dilatation or
pericardial nature of the aortic root, and (iii) proximity to pericardial effusion (suggestive of impending rupture),
the head and neck vessels. Thus, the effects of type A dis- associated regional wall motion abnormality (coronary occlu-
section may include acute severe AR (acute dilatation of sion), and AR—facilitating immediate surgical referral and
the aortic root, aortic leaflet prolapse, dissection flap pro- appropriate emergency management. If there is high clinical
lapse, pre-existing disease, e.g. bicuspid valve), coronary suspicion and the TTE provides direct or corroborative evi-
ostial occlusion, haemorrhagic pericardial effusion and tam- dence for type A dissection, we recommend transfer of the
ponade, or extension to the head and neck vessels causing patient immediately to a cardiothoracic unit, where further
stroke. For these reasons, early surgical intervention is rec- pre- and intra-operative echocardiographic (TEE) imaging
ommended for type A aortic dissection and has been shown (or alternatively CT or MRI) can take place. This approach
to improve prognosis; delays in surgical treatment subject minimizes any delays, particularly while the patient is in an
the patient to a mortality risk of 1% per hour. environment in which potentially life-saving cardiac surgery
Downloaded from https://academic.oup.com/ehjcimaging/article-abstract/10/1/i31/2465433
by guest
on 18 December 2017
i34 E.L. Meredith and N.D. Masani
cannot take place, and ensures that emergency management
is undertaken by appropriate experts—cardiologists, cardiac
anaesthetists, and surgeons.
Therefore, despite its relatively poor diagnostic accuracy,
TTE is an extremely valuable clinical tool in diagnosing and
assessing AAS in the emergency setting, identifying its
related complications and diagnosing potential differential
conditions. Most importantly, it has a vital role in identifying
patients at high risk and directing their referral to the
relevant cardiac surgical department promptly.
Performing transthoracic echocardiography
in suspected acute aortic syndrome
Where the clinical situation allows, a full TTE study should
be performed, as soon as possible, using standard and
off-axis views (Figure 4). Standard two-dimensional and
colour flow imaging in parasternal long axis (Figure 4A),
apical five- (Figure 4B) and three-chamber views are used
to image the aortic valve and root. In the parasternal and
modified apical two-chamber views, parts of the descending
aorta (behind the left atrium) can be visualized (Figure 4A).
Right parasternal or high left parasternal views allows visu-
alization of the ascending aorta in some patients. Using the
suprasternal view, the arch, origin of the head and neck
vessels, and proximal descending aorta can be imaged.
The subcostal view allows imaging of the abdominal aorta
in most patients (Figure 4C).
Transthoracic echocardiography should also be used to
assess the presence of pericardial or pleural effusions.
Assessment of any AR should be made, assessing the severity
and mechanism of AR. This may provide valuable infor-
mation to the surgeon about the need for aortic valve
repair or replacement. Left and right ventricular function
should be assessed. Regional wall abnormalities may
represent coronary involvement in the dissection flap or
pre-existing coronary disease.
Definitive imaging in acute aortic syndromes:
the role of transoesophageal echocardiography
The ideal diagnostic technique in AAS should be safe, rela-
tively rapid, and have high sensitivity and specificity. The
primary objectives are to immediately identify an intimal
tear (or haematoma) and delineate the extent of thoracic
dissection. Important secondary objectives are to evaluate
complications and, in type A dissection or IMH, provide
important information to cardiac surgeons: the presence Figure 4 Transthoracic echocardiography in a patient with
and mechanism of AR; branch occlusion, coronary/head Marfan’s syndrome and type A dissection. (A) Parasternal long-axis
and neck; extravasation of blood, pericardial/pleural view. There is severe dilatation of the aorta and a linear echo is
effusions. seen just above the aortic valve (white arrow). Note the normal
caliber and appearance of the descending thoracic aorta, posterior
Transoesophageal echocardiography, helical CT, and MRI
to the left atrium (black arrow). LV, left ventricle; LA, left atrium;
are all excellent imaging modalities in AAS.16 Transoesopha- Ao, aorta. (B) Apical five-chamber view. The dilated aortic root,
geal echocardiography is reported to have a sensitivity of with two reflections of the intimal flap, (white arrows) is seen.
94–100% and specificity of 77–100% for identifying an Severe aortic regurgitation (right panel) is seen with colour flow
intimal flap.16,17 The reduced specificity in early studies mapping. (C ) Subcostal view. Normal caliber, no dissection flap
relates to the false-positive interpretation of reverberation and normal flow are seen.
artefacts in the aortic root (discussed later),15 particularly
with the use of mono- or bi-plane TEE. In a comprehensive (probably the most widely used technique) is less accurate
meta-analysis16 of all three modalities, the most recent (sensitivity 83–94%, specificity 87–100%).16 In various
studies reported 100% sensitivity and 100% specificity for reports, the ‘TEE blindspot’ caused by the interposition of
TEE,18 helical CT, and MRI, whereas conventional CT the trachea between oesophagus and upper ascending
Downloaded from https://academic.oup.com/ehjcimaging/article-abstract/10/1/i31/2465433
by guest
on 18 December 2017
Echocardiography in the emergency assessment of AAS i35
aorta is mentioned as a potential disadvantage of TEE. In our
experience, this has not been a problem, given the extre-
mely low probability of dissection of IMH confined to this
precise location only.19 A detailed discussion of the relative
merits of each of these imaging modalities is beyond the
remit of this article and has been performed elsewhere,16
but is considered in brief in the final section.
Transoesophageal echocardiography is rapid and safe. It
may be performed at the bedside in a critical care environ-
ment: this is of particular importance in the haemodynami-
cally unstable patient and avoids the need to transfer the
patient to another department for imaging. When there is
a high degree of suspicion for type A dissection or IMH,
TEE can be performed in the operating room, with anaesthe-
tists and surgeons standing by. In such cases, unnecessary
and dangerous delays can be incurred by transferring
patients to CT or MRI scanners; expert TEE can provide all
of the required diagnostic and pre-surgical information.19 Figure 5 Reverberation artefact seen by M-mode transoesopha-
geal echocardiography. An apparent linear echo in the aorta is
There are anecdotal reports of deterioration of patients
seen (white arrow)—it mirrors the motion of the echo bright pos-
with aortic dissection, during TEE, possibly related to discom-
terior aortic wall, is twice the distance from the probe, and has
fort, gagging or distress.20 However, no mortality has been twice the amplitude of movement. PA, pulmonary artery; Ao, aorta.
reported in larger studies.16,17,19 Moreover, given the mor-
tality rate of 1–2% per hour, there is a high risk of fatal
deterioration while transferring patients for, or during, CT
or MRI. Nevertheless, it is vital that TEE is performed by They may be difficult to distinguish from intimal flaps and
suitably trained and experienced operators in this setting. account for some of the false-positive diagnoses of aortic
dissection. Reverberation artefacts in the aortic root can
Performing transoesophageal occur from the walls of the left atrium and in the ascending
echocardiography in suspected acute aorta from the right pulmonary artery. Using M-mode, the
artefact can be seen to be double the distance from
aortic syndrome
the probe as the original structure with movement,
Scrupulous attention must be paid to the medical and sup- which is in time but twice the amplitude of the original
portive treatment of the patient with AAS during TEE (and structure (Figure 5). Colour flow mapping, which shows
during CT, MRI, etc.).7 Careful and continuous monitoring differential flow between true and false lumens in true
of heart rate, blood pressure, and oxygen saturation is dissection, is also useful in recognizing reverberation
necessary. Adequate opiod analgesia should be given. Intra- artefacts.
venous beta-blockers, nitroprusside, or nitrates should be
used to maintain a low blood pressure (we avoid beta-
blockers in the presence of severe AR). We recommend False lumen
careful conscious sedation during TEE, using intravenous
midazolam. The aim is to introduce the TEE probe with It is important to be able to distinguish the true from the false
maximal patient cooperation and minimal agitation, follow- lumen. This has particular (surgical) relevance when the dis-
ing which further sedation may be given if needed. section extends to the origins of the coronaries and/or head
and neck vessels, which may originate from the false
lumen. In dissections of the descending aorta, visceral
Assessing the aorta arteries may be involved having surgical or endovascular
implications. The false lumen is often much larger than the
Intimal flap true lumen. Flow in the true lumen is usually greater than
The classic sign of aortic dissection is the intimal flap. This is in the false lumen, antegrade during systole, with the flap
seen as a mobile linear echo separating the true from the moving toward the false lumen. However, in cases where
false lumen with flow on either side. The false lumen is the proximal entry tear is large, flow in the false lumen
often much larger than the true lumen. The intimal flap may be similar to that in the true lumen with systolic
moves throughout the cardiac cycle. With chronic dissec- forward flow similar in velocity and timing along with dias-
tions, there is a decrease in mobility. It is important to be tolic reversal.21,22 With small or more distal entry tears,
able to identify the proximal extension of the dissection as flow in the false lumen is much slower and spontaneous
this determines whether an urgent surgical approach is echo contrast or thrombus may be identified. An aortic wall
used. It is not important to identify the distal extent of thickness of greater than 15 mm suggests dissection with
the flap, if this extends below the diaphragm, during the thrombosis in the false lumen (Figure 6). In this situation,
emergency presentation of AAS since this will not alter man- an aortic flap may not be identified—this is unusual in the
agement unless there is evidence of an intra-abdominal emergency setting. Thrombus formation is dependent on
complication or end-organ ischaemia. the flow within and location of the tear: it is more common
When the aorta is dilated, linear artefacts are common in the descending aorta and infrequent in the ascending
and may appear in the transverse or longitudinal plane. aorta, being described in only 7% of dissections.23,24
Downloaded from https://academic.oup.com/ehjcimaging/article-abstract/10/1/i31/2465433
by guest
on 18 December 2017
i36 E.L. Meredith and N.D. Masani
Figure 6 Thrombosis and spontaneous echo contrast in the Figure 7 Prolapsing intimal flap, causing severe aortic regurgita-
descending thoracic false lumen in a patient with repaired type A tion. Transoesophageal echocardiography in the same patient as in
dissection. The aorta is severely dilated. Characteristically, the Figure 1. The flap interferes with closure of the aortic valve. LA,
false lumen is much larger than the true lumen. In the right left atrium; LV, left ventricle; Ao, aortic root (which is severely
panel, colour flow mapping demonstrates vigorous flow in the true dilated, also contributing to aortic regurgitation).
lumen only.
Entry tears PAU extends to dissection, the dissection is usually shorter,
limited by neighbouring fibrosis and calcification. The flap
The intimal tear is usually .5 mm and is situated in the is usually thicker, may be calcified, and is less mobile than
proximal ascending aorta (Figure 1A) or in the descending in a true dissection.
aorta just distal to the left subclavian artery. A principal
aim of cardiac surgery in type A dissection is to obliterate
the entry tear in the ascending aorta, thereby preventing
Pericardial and pleural effusions
flow into the false lumen, encouraging thrombosis of the Pericardial effusions occur in 20–30% of ascending aorta and
false lumen and healing of the aorta.25 6% of descending aorta dissections.17,21,28 Pericardial effu-
Transoesophageal echocardiography identifies the intimal sions may occur due to rupture of the false lumen into the
tear in 78–100% of the cases.26,27 In cases where it is not pericardium or due to irritation of the pericardium second-
visualized by two-dimensional echocardiography, colour ary to aortic haematoma. The presence of a pericardial effu-
Doppler may show a turbulent jet directed toward the sion with an ascending aortic dissection is a sign of poor
false lumen. Using pulsed Doppler, flow velocity is usually prognosis.
,1.5 m/s in systole. Secondary tears, in up to 20% of the
cases,26,27 may be identified with TEE using colour Aortic regurgitation
Doppler. These are small communications between the
true and false lumen and occur more commonly in the Both TTE and TEE are able to accurately assess the severity
descending aorta. of AR. Transoesophageal echocardiography often gives
greater information about the mechanism of the AR. There
are several mechanisms that may contribute to the AR.
Intramural haematoma (Figure 2)
Echocardiography reveals an aortic wall thickness of over (1) Dilatation of the annulus, leading to incomplete valve
7 mm, with no dissection flap, entry tear, or false lumen. closure and resultant AR.
The thickened aorta in transverse section may have a cres- (2) Aortic leaflet prolapse occurs when the dissection
centic shape with distortion of the circular contour. Intra- extends into the root and disrupts the suspension of
mural echo-free spaces are seen. Intramural haematoma is one of the cusps. Abnormal leaflet coaptation occurs
more common in the descending aorta and there may be and there is eccentric AR. This is best seen in a long-axis
signs of more widespread arteriosclerosis. Intramural hae- view when the cusp is seen to prolapse back onto the
matoma may regress or progress to dissection or rupture. left ventricular outflow tract.
Supplementary imaging in the form of MRI or CT is often (3) Dissection flap prolapse can occur through the aortic
required and is used for serial imaging of these lesions. valve, during diastole, distorting the valve and causing
regurgitant flow (Figure 7). Prolapse of redundant
intimal flap tissue and the resultant AR may be intermit-
Penetrating aortic ulcer tent. This unusual mechanism of severe AR, in which the
Penetrating aortic ulcers occur predominantly in the des- valve itself may be inherently normal, is particularly
cending thoracic and abdominal aorta (Figure 3). They well visualized by TEE.29
occur more commonly in the elderly and there is often (4) Pre-existing valvular disease, for example, a bicuspid
widespread atheromatous disease. Penetrating athero- valve (Figure 1B), annular dilatation secondary to
sclerotic ulcer is usually a focal lesion appearing as an Marfan’s syndrome, or degenerative valve disease may
outpouching of the aortic wall with jagged edges. Concomi- cause significant AR. In these cases, the dissection may
tant aneurysms of the descending aorta may be found. If a be of the descending or ascending aorta.
Downloaded from https://academic.oup.com/ehjcimaging/article-abstract/10/1/i31/2465433
by guest
on 18 December 2017
Echocardiography in the emergency assessment of AAS i37
Figure 8 Visualization of the left coronary ostium. Transoesopha-
geal echocardiography short-axis view: in the left panel, a small
true lumen is seen, from which the left coronary artery (asterisk)
arises. Separate origins of the left anterior descending and circum-
flex branches can be seen—this was invaluable information for the
cardiac surgeon. In the right panel, colour flow mapping shows
unobstructed flow from true lumen into the left coronary branches.
It is critically important to provide accurate information
about the severity and mechanism of the aortic valve regurgi-
tation, as this will influence the surgical decision to repair or
replace the valve: in the first three mechanisms above, it is
usually possible to surgically ‘re-suspend’ the native valve.
Arterial involvement
Figure 9 Visualization of the head and neck vessels. Off-axis trans-
In 10–20% cases of dissection, the intimal flap propagates oesophageal echocardiography view of the aortic arch. (A) A linear
retrogradely to involve the origin of one or both coronary dissection flap is seen. The origins of the left common carotid and
arteries,30 thereby obstructing flow. Coronary involvement subclavian arteries as seen to arise from the smaller, true lumen
is suggested by left ventricular regional wall abnormalities, (white arrows). (B) In the right panel, colour flow mapping shows
unobstructed flow from true lumen into the head and neck vessels.
although these may represent pre-existing coronary disease.
Transoesophageal echocardiography allows direct visualiza-
tion of the coronary ostia and their spatial relationship to
the proximal extent of the dissection flap; proximal flow Table 2 Transoesophageal echocardiography in
can be seen with colour Doppler. This is achieved in the mid- patients undergoing surgery for type A dissection:
oesophageal short- and long-axis views. It is possible to information for the surgeon
identify whether the coronaries originate from the true or
false lumen or whether the dissection extends into the cor- Proximal extent of dissection flap
onary (Figure 8). It should be remembered that coronary Site of entry tear(s)
Pericardial effusion/cardiac tamponade
angiography is hazardous, and therefore frequently not per-
Aortic regurgitation
formed, in patients with aortic dissection. Severity
In most cases, the upper oesophageal views of the aortic Mechanism
arch can be used to identify the origin of the head and Coronary involvement
neck vessels and assess whether flow is from the true or Head and neck vessel involvement
false lumen (Figure 9). Left ventricular function
Additional cardiac pathologies
Operative assessment: pre, intra, and post
Cardiac surgery is indicated in patients with acute type A Transthoracic echocardiography and, in particular, TEE
aortic dissection (or IMH), reducing 14-day mortality from provide the cardiac surgeon with invaluable information,
50% to 20%.31 The aims of cardiac surgery are to repair or as detailed in the above section (Table 2). When a diagnosis
replace the aortic root/ascending aorta, to obliterate the of type A dissection or IMH has already been made (by TTE,
entry site (tear) into the false lumen, to repair or replace TEE, CT, or MRI) before transfer to the operating room, we
a regurgitant aortic valve, and to secure antegrade flow to recommend the use of peri-operative TEE to augment and
the coronary and proximal head/neck vessels. review the available diagnostic information. Furthermore,
Downloaded from https://academic.oup.com/ehjcimaging/article-abstract/10/1/i31/2465433
by guest
on 18 December 2017
i38 E.L. Meredith and N.D. Masani
Figure 10 Algorithm for the use of echocardiography in acute aortic syndrome (see text for details). RWMA, regional wall motion abnorm-
alities; AR, aortic regurgitation; C-T unit, cardiothoracic unit; CCU, coronary care unit; OR, operating room.
dissection and IMH are dynamic and rapidly progressing con- If TTE identifies type A dissection or high-risk features in
ditions, and contemporaneous imaging at the time of association with a strong clinical suspicion, we recommend
surgery frequently provides important information (such as performing TEE with cardiac surgeons and anaesthetists
the development of pericardial effusion, rapid expansion standing by. If the diagnosis is confirmed, surgery can
of the aortic root, etc.). proceed with minimal delay. Importantly, TEE (and TTE)
Post-operatively, TEE is valuable in assessing competence allows the assessment of AR, its severity, mechanism, and
of the aortic valve, integrity of upper32 and lower anasta- need for replacement or repair.
moses of interposition grafts, and, in haemodynamically In the absence of TTE, suspicion of type A dissection (or
unstable patients, ventricular function and the presence of IMH) or high-risk features, there is less urgency. The defini-
pericardial collections. Because of the severe nature of tive imaging modality will depend upon clinical circum-
the presenting illness, often with cardiovascular collapse, stances, availability of facilities, and operators: helical CT,
and the complexity and duration of surgery required, post- MRI, and TEE are equally accurate and have relative
operative complications are common. The rapid availability strengths and weaknesses. Although both allow visualization
and portability of TEE (including in the operating room or of the entire aorta including branch vessel involvement, this
intensive care unit) are invaluable in assessing these is less important in the first few hours. Both CT and MRI may
complex patients.32 have time delays and practical difficulties in monitoring
patients whilst in the scanner. Occasionally, multiple modal-
ities may be needed to clarify suspicious or incongruous
Suggested approach for echocardiography in results. The choice of modality will depend on the resources
patients with suspected acute aortic syndrome available in individual centres and the expertise available.
In patients undergoing surgery, TEE offers invaluable
Untreated, AAS can be a rapidly fatal condition (Figure 10). information for the surgeon operating on these most
For this reason, prompt and accurate assessment is required challenging of patients.
to identify high-risk patients. A high index of clinical suspi-
cion is required, to distinguish AAS from other causes of
chest pain and dyspnoea. Conflict of interest: none declared.
We recommend TTE as the first-line imaging modality.
Where more definitive imaging (such as CT) is regarded as
the conventional first-line investigation, TTE can be per- References
formed in the emergency department, while the prep-
arations for the CT scan are being made. This serves to 1. Vilacosta I, San Roman J. Acute aortic syndrome. Heart 2001;85:365–8.
2. Ince H, Nienaber C. The concept of interventional therapy in acute aortic
highlight complications or high-risk features (such as peri- syndrome. J Card Surg 2002;17:135–42.
cardial effusion) that may alter the management plan—this 3. Ahmad F, Cheshire N, Hamady M. Acute aortic syndrome: pathology and
is particularly important in non-surgical centres. therapeutic strategies. Postgrad Med J 2006;82:305–12.
Downloaded from https://academic.oup.com/ehjcimaging/article-abstract/10/1/i31/2465433
by guest
on 18 December 2017
Echocardiography in the emergency assessment of AAS i39
4. Daily P, Trueblood H, Stinson, Wuerflein R, Shumway N. Management of 19. Banning AP, Masani ND, Ikram S, Fraser AG, Hall RJ. Transoesophageal
acute aortic dissections. Ann Thorac Surg 1970;10:237–47. echocardiography as the sole diagnostic investigation in patients with
5. DeBakey M, McCollum C, Crawford E, Morris G, Howell J, Noon G. Dissec- suspected thoracic aortic dissection. Br Heart J 1994;72:461–5.
tion and dissecting aneurysms of the aorta: twenty-year follow-up of five 20. Kristensen S, Ivarsen H, Egeblad H. Rupture of aortic dissection during
hundred twenty-seven patients treated surgically. Surgery 1982;92: attempted tranesophageal echocardiograph. Echocardiography 2007;
1118–34. 13:405–6.
6. Svensson LG, Labib SB, Eisenhau JR. Intimal tear without haematoma. 21. Erbel R, Mohr-Kahaly S, Rennollet H, Brunier J, Drexler M, Wittlich N
Circulation 1999;99:1331–6. et al. Diagnosis of aortic dissection: the value of transesophageal
7. Erbel R, Alfonso F, Boileau C, Dirsch O, Eber B, Haverich A et al. Diagnosis echocardiography. Thorac Cardiovasc Surg 1987;35:126–33.
and management of aortic dissection. Recommendations of the Task 22. Mohr-Kahaly S, Erbel R, Rennollet H, Wittlich N, Drexler M, Oelert H et al.
Force on Aortic Dissection, European Society of Cardiology. Eur Heart J Ambulatory follow-up of aortic dissection by transesophageal two-
2001;22:1642–81.
dimensional and color-coded Doppler echocardiography. Circulation
8. Hirst A, Johns V, Kime S. Dissecting aneurysm of the aorta: a review of
1989;80:24–33.
505 cases. Medicine (Baltimore) 1958;37:217–79.
23. Ballal R, Nanda N, Gatewood R, D’Arcy B, Samdarshi T, Holman W et al.
9. Eichelberger J. Aortic dissection without intimal tear: case report and
Usefulness of transesophageal echocardiography in assessment of aortic
findings on transesophageal echocardiography. J Am Soc Echocardiogr
dissection. Circulation 1991;84:1903–14.
1994;7:82–6.
24. Armstrong W, Bach D, Carey L, Chen T, Donovan C, Falcone R et al. Spec-
10. Coady M, Rizzo J, Elefteriades J. Pathologic variants of thoracic aortic
trum of acute dissection of the ascending aorta: a transesophageal
dissections. Penetrating atherosclerotic ulcers and intramural hemato-
mas. Cardiol Clin North Am 1999;17:637–57. echocardiographic study. J Am Soc Echocardiogr 1996;9:646–56.
11. Eggebrecht H, Baumgart D, Schmermund A, Herold U, Hunold P, Jakob H. 25. Erbel R, Oelert H, Meyer J, Puth M, Mohr-Kahaly S, Hausmann D et al.
Penetrating atherosclerotic ulcer of the aorta: treatment by endovascu- Effect of medical and surgical therapy on aortic dissection evaluated
lar stent-graft placement. Curr Opin Cardiol 2003;18:431–5. by transesophageal echocardiography. Implications for prognosis and
12. Robbins R, McManus R, Mitchell R, Latter D, Moon M, Olinger G et al. therapy. The European Cooperative Study Group on Echocardiography.
Management of patients with intramural hematoma of the thoracic Circulation 1993;87:1604–15.
aorta. Circulation 1993;88:II1–10. 26. Evangelista A, Gonzalez-Alujas M, Garcia del Castillo H, Anivarro I,
13. Chirillo F, Marchiori M, Andriolo L, Razzolini R, Mazzucco A, Gallucci V Angel J, Salas A et al. Transesophageal echocardiography in the diagnosis
et al. Outcome of 290 patients with aortic dissection. A 12-year multicen- of aortic dissection. Revista Espanola de Cardiologia 1993;46:805–9.
tre experience. Eur Heart J 1990;11:311–9. 27. Chirillo F, Cavallini C, Longhini C, Ius P, Totis O, Cavarzerani A et al. Com-
14. Miller D. Surgical management of aortic dissections: Indications, perio- parative diagnostic value of transesophageal echocardiography and ret-
perative management and long term results. In: Doroghazi RM, rograde aortography in the evaluation of thoracic aortic dissection. Am
Slater EE, eds. Aortic Dissection. New York: McGraw-Hill; 1983. J Cardiol 1994;74:590–5.
pp. 193–243. 28. Keren A, Kim C, Hu B, Eyngorina I, Billingham M, Mitchell R et al. Accu-
15. Appelbaum A, Karp R, Kirklin J. Ascending vs descending aortic dissec- racy of biplane and multiplane transesophageal echocardiography in
tions. Ann Surg 1976;183:296–300. diagnosis of typical acute aortic dissection and intramural hematoma.
16. Shiga T, Wajima Z, Apfel C, Inoue T, Ohe Y. Diagnostic accuracy of trans- J Am Coll Cardiol 1996;28:627–36.
oesophageal echocardiography, helical computed tomography, and mag- 29. Geyik B, Ozeke O, Ozbakir C, Deveci B, Aras D. Aortic dissection with
netic resonance imaging for suspected thoracic aortic dissection: diastolic prolapse of intimal flap into left ventricle. European Journal
systematic review and meta-analysis. Arch Int Med 2006;166:1350–6. of Echocardiography 2005;6:311–2.
17. Nienaber C, von Kodolitsch Y, Nicolas V, Siglow V, Piepho A, Brockhoff C 30. Crawford E. The diagnosis and management of aortic dissection. JAMA
et al. The diagnosis of thoracic aortic dissection by noninvasive imaging 1990;264:2537–41.
procedures. N Engl J Med 1993;328:1–9.
31. Tsai T, Neinaber C, Eagle K. Acute aortic syndromes. Circulation 2005;
18. Pepi M, Campodonico J, Galli C, Tamborini G, Barbier P, Doria E et al.
112:3802–13.
Rapid diagnosis and management of thoracic aortic dissection and intra-
32. Cianciulli T, Fairman E, Saccheri M, Llanos Dethinne S, Prezioso H. Acute
mural haematoma: a prospective study of advantages of multiplane vs.
supravalvular aortic stenosis following the replacement of the ascending
biplane transoesophageal echocardiography. Eur J Echocardiogr 2000;1:
aorta. Eur J Echocardiogr 2007;8:232–4.
72–9.
Downloaded from https://academic.oup.com/ehjcimaging/article-abstract/10/1/i31/2465433
by guest
on 18 December 2017
You might also like
- Guide To The Dissection of The Dog, 8th EditionDocument346 pagesGuide To The Dissection of The Dog, 8th Editionmaria da matosNo ratings yet
- Aortic DissectionDocument49 pagesAortic DissectionAnonymous ZUaUz1wwNo ratings yet
- Aortic Aneurysm & DissectionDocument51 pagesAortic Aneurysm & DissectionRashed ShatnawiNo ratings yet
- Aortic D RefferatDocument5 pagesAortic D RefferatRachman IbrahimNo ratings yet
- Acute Aortic Disecccion Type ADocument15 pagesAcute Aortic Disecccion Type AAnonymous envUOdVNo ratings yet
- Aneurism A de Aorta Es in Dromes Aortic AsDocument18 pagesAneurism A de Aorta Es in Dromes Aortic AsYgor AlbuquerqueNo ratings yet
- Rido, Rudini - Disease of Aorta and Trauma To The AortaDocument114 pagesRido, Rudini - Disease of Aorta and Trauma To The AortaFikriYTNo ratings yet
- Imaging of Cardiovascular Thoracic Emergencies Acute Aortic Syndrome and Pulmonary EmbolismDocument8 pagesImaging of Cardiovascular Thoracic Emergencies Acute Aortic Syndrome and Pulmonary EmbolismAlejandro ColombanoNo ratings yet
- Brain Strokes Related To Aortic Aneurysma - The Analysis of Three CasesDocument4 pagesBrain Strokes Related To Aortic Aneurysma - The Analysis of Three Casesdian asrianaNo ratings yet
- Patologia AorticaDocument18 pagesPatologia AorticaVALENTINASE17No ratings yet
- Jurnal Coronary Artery FistulaDocument3 pagesJurnal Coronary Artery FistulaRistinyaUnuyNo ratings yet
- Coarctation of The Aorta: P. Syamasundar Rao, MDDocument10 pagesCoarctation of The Aorta: P. Syamasundar Rao, MDAustine OsaweNo ratings yet
- Acute Aortic Syndrome – More in The SpectruDocument5 pagesAcute Aortic Syndrome – More in The Spectrufabiola shoshajNo ratings yet
- BJR Aortic Aciute SyndromeDocument19 pagesBJR Aortic Aciute Syndromefrancu60No ratings yet
- CCR 8 152Document6 pagesCCR 8 152ekafithraNo ratings yet
- Surgery Reviosn NotesDocument41 pagesSurgery Reviosn Noteshy7tn100% (1)
- Thoracic Aortic Aneurysm - Optimal Surveillance and TreatmentDocument12 pagesThoracic Aortic Aneurysm - Optimal Surveillance and TreatmentNguyễn Thời Hải Nguyên100% (1)
- Aorticemergencies: Kathleen WittelsDocument12 pagesAorticemergencies: Kathleen WittelsRavin DebieNo ratings yet
- Diseccion AortaDocument22 pagesDiseccion AortaPavel Salazar TacangaNo ratings yet
- KP 2.5.4.5 AortaDocument60 pagesKP 2.5.4.5 Aortanurul ramadhiniNo ratings yet
- Carrel (LAncet 2023)Document16 pagesCarrel (LAncet 2023)Batoul100% (1)
- Adriaans2019 Article PredictiveImagingForThoracicAoDocument9 pagesAdriaans2019 Article PredictiveImagingForThoracicAohengkileonardNo ratings yet
- Triaje Del Taponamiento Cardíaco ESC 2014Document6 pagesTriaje Del Taponamiento Cardíaco ESC 2014Adriana MendozaNo ratings yet
- Left Ventricular Diverticulum in Association With Bicuspid Aortic Valve and Pseudocoarctation: Hitherto Unreported AssociationDocument3 pagesLeft Ventricular Diverticulum in Association With Bicuspid Aortic Valve and Pseudocoarctation: Hitherto Unreported AssociationIsabella María GantivarNo ratings yet
- Aortic DissectionDocument26 pagesAortic DissectionMuhammad ZakyNo ratings yet
- Chest CT Angiography For Acute Aortic Pathologic Conditions: Pearls and PitfallsDocument26 pagesChest CT Angiography For Acute Aortic Pathologic Conditions: Pearls and PitfallsJelvis BofNo ratings yet
- Disección AorticaDocument12 pagesDisección AorticazapichitoNo ratings yet
- Aortic Dissection: DR Muhammad Burhan PashaDocument41 pagesAortic Dissection: DR Muhammad Burhan PashapashaNo ratings yet
- Saranteas 2016Document8 pagesSaranteas 2016Alejandro López LópezNo ratings yet
- Aortic Regurgitation: Clinical PracticeDocument8 pagesAortic Regurgitation: Clinical PracticeChintya Fidelia MontangNo ratings yet
- Acute Aortic Dissection Is A TimeDocument2 pagesAcute Aortic Dissection Is A TimeIuliana Ceban MașnicNo ratings yet
- Clinical Cases: Ischaemic Heart DiseaseDocument4 pagesClinical Cases: Ischaemic Heart DiseaseLADY JOWAHER ALLASNo ratings yet
- 2021 Article 2376Document6 pages2021 Article 2376Anna Sofía ParedesNo ratings yet
- Acute Arterial OcclusionDocument49 pagesAcute Arterial OcclusiondrvsvasuNo ratings yet
- Thoracic Aortic Aneurysm: A Rare Case Report: Torasik Aort Anevrizması: Nadir Görülen Bir VakaDocument3 pagesThoracic Aortic Aneurysm: A Rare Case Report: Torasik Aort Anevrizması: Nadir Görülen Bir VakaAlejandra LopezNo ratings yet
- Aortic Dissection Gary 2009Document22 pagesAortic Dissection Gary 2009Ciubuc AndrianNo ratings yet
- 1 s2.0 S0733865124000171 MainDocument19 pages1 s2.0 S0733865124000171 MainABRAHAM MANUEL MEDINA LEYTONNo ratings yet
- A Rare Case of Vertebral Artery Pseudoaneurysmas An Iatrogenic ComplicationDocument4 pagesA Rare Case of Vertebral Artery Pseudoaneurysmas An Iatrogenic ComplicationIOSRjournalNo ratings yet
- Intramural Haematoma of The Thoracic Aorta-Who's To Be Alerted The Cardiologist or The Cardiac SurgeonDocument7 pagesIntramural Haematoma of The Thoracic Aorta-Who's To Be Alerted The Cardiologist or The Cardiac SurgeonAlexandru CozmaNo ratings yet
- Dissection Octobre 2019Document48 pagesDissection Octobre 2019ARMVOPNo ratings yet
- s13019-020-01333-6Document6 pagess13019-020-01333-6deepi2408No ratings yet
- CazuriDocument4 pagesCazuriIbănescu Iulia AndreeaNo ratings yet
- Carotid Artery Stenosis ImagingDocument10 pagesCarotid Artery Stenosis ImagingCristhian RuizNo ratings yet
- Acute Limb Ischemia: EtiologyDocument6 pagesAcute Limb Ischemia: EtiologyCheysar Lufiana L RamadhaniNo ratings yet
- Linician Pdate: Acute Aortic DissectionDocument18 pagesLinician Pdate: Acute Aortic DissectionBagus DikaNo ratings yet
- Intramural Hematoma: Journal of Cardiothoracic and Vascular AnesthesiaDocument22 pagesIntramural Hematoma: Journal of Cardiothoracic and Vascular AnesthesiaRomeo GuevaraNo ratings yet
- Aortic Coarctation Cardiology Clinics 2020Document15 pagesAortic Coarctation Cardiology Clinics 2020Angela OrozcoNo ratings yet
- Rheumatology 2006 Maksimovi Iv26 31Document6 pagesRheumatology 2006 Maksimovi Iv26 31Thio GifarnoNo ratings yet
- Anomalies D'origine CoronaireDocument4 pagesAnomalies D'origine Coronairealex mihneaNo ratings yet
- Instrumental MethodDocument24 pagesInstrumental Methodzerish0208No ratings yet
- Belhajsoulami 2018Document3 pagesBelhajsoulami 2018rédaNo ratings yet
- Acute Coronary Syndrome (ACS)Document12 pagesAcute Coronary Syndrome (ACS)swastikNo ratings yet
- Aortic DissectionDocument67 pagesAortic DissectionPIYALI BISWASNo ratings yet
- aortic dissectionDocument9 pagesaortic dissectionnaufalrahman145No ratings yet
- Kardo S 1998Document3 pagesKardo S 1998Sarly FebrianaNo ratings yet
- Pi Is 0003497516313285Document3 pagesPi Is 0003497516313285Gordana PuzovicNo ratings yet
- Causes of Stroke PDFDocument16 pagesCauses of Stroke PDFEmmanuel AguilarNo ratings yet
- Advancements in Acute Aortic Syndrome: From Pathophysiology to Personalized TherapeuticsFrom EverandAdvancements in Acute Aortic Syndrome: From Pathophysiology to Personalized TherapeuticsNo ratings yet
- Decoding Cardiac Electrophysiology: Understanding the Techniques and Defining the JargonFrom EverandDecoding Cardiac Electrophysiology: Understanding the Techniques and Defining the JargonAfzal SohaibNo ratings yet
- Atlas of Coronary Intravascular Optical Coherence TomographyFrom EverandAtlas of Coronary Intravascular Optical Coherence TomographyNo ratings yet
- Comprehensive Insights into Acute Coronary Syndrome: Pathways, Interventions, and Holistic RecoveryFrom EverandComprehensive Insights into Acute Coronary Syndrome: Pathways, Interventions, and Holistic RecoveryNo ratings yet
- AKI After CABG Vs PCIDocument10 pagesAKI After CABG Vs PCIDumitru GrozaNo ratings yet
- Risk Model DialysiddssssDocument7 pagesRisk Model DialysiddssssDumitru GrozaNo ratings yet
- Dialysis After CABG Ejcts 2013ddDocument6 pagesDialysis After CABG Ejcts 2013ddDumitru GrozaNo ratings yet
- Fate of A Coronary Artery Intramural Haematoma Complicating Aortic Root Surgery: A Case ReportDocument5 pagesFate of A Coronary Artery Intramural Haematoma Complicating Aortic Root Surgery: A Case ReportDumitru GrozaNo ratings yet
- Dry Citrasate Part A Acid Concentrate PowderDocument4 pagesDry Citrasate Part A Acid Concentrate PowderSubhrajit ChattopadhayayNo ratings yet
- Sistema Urinarius Blok 2.1 2021Document34 pagesSistema Urinarius Blok 2.1 2021Avika MuharrahmahNo ratings yet
- Rana Greene Neovascular GlaucomaDocument25 pagesRana Greene Neovascular GlaucomaGG INo ratings yet
- Abrams Urodynamics 4Th Edition Marcus Drake Full ChapterDocument67 pagesAbrams Urodynamics 4Th Edition Marcus Drake Full Chapternorma.fegley884100% (6)
- Rajiv Gandhi University of Health Sciences, Bangalore, Karnataka, Annexure Ii Proforma For Registration of Subject For DissertationDocument13 pagesRajiv Gandhi University of Health Sciences, Bangalore, Karnataka, Annexure Ii Proforma For Registration of Subject For DissertationGirish SubashNo ratings yet
- Cerebral AneurysmDocument69 pagesCerebral AneurysmDiksha chaudharyNo ratings yet
- MammographyDocument15 pagesMammographyPratik PatelNo ratings yet
- Cannula Versus Needle For Rejuvenation of The Perioribital RegionDocument9 pagesCannula Versus Needle For Rejuvenation of The Perioribital RegionAmanda Lopes100% (1)
- Cerebralangiography Jesppt 1Document17 pagesCerebralangiography Jesppt 1iqbalNo ratings yet
- Anticoagulation Guidelines For Neuraxial Procedures: Anticoagulants, InjectableDocument4 pagesAnticoagulation Guidelines For Neuraxial Procedures: Anticoagulants, InjectablepaulaNo ratings yet
- Glaucoma Drainage DevicesDocument6 pagesGlaucoma Drainage Devicesmax paxNo ratings yet
- Medical Prefixes and SuffixesDocument12 pagesMedical Prefixes and SuffixesKrishnanunni KLNo ratings yet
- Surgery Osteoplastic MaterialsDocument24 pagesSurgery Osteoplastic Materialssmile secretNo ratings yet
- Cardiogenic Shock Pathogenesis, Classification, and ManagementDocument20 pagesCardiogenic Shock Pathogenesis, Classification, and Managementjosh FaducNo ratings yet
- FX Pilon - 3tecnicasqx - 2001Document8 pagesFX Pilon - 3tecnicasqx - 2001Luis ChamanNo ratings yet
- Anesthesiology PrimerDocument10 pagesAnesthesiology PrimerJamesNo ratings yet
- Orbital ProsthesisDocument5 pagesOrbital ProsthesisdrsmritiNo ratings yet
- AVA Safer Anaesthesia Guildlines Booklet VET Web PDFDocument9 pagesAVA Safer Anaesthesia Guildlines Booklet VET Web PDFtinamalinkaNo ratings yet
- Acute CholecystitisDocument25 pagesAcute Cholecystitissri wula moniNo ratings yet
- Mechanical VentilationDocument18 pagesMechanical VentilationAlka GoyalNo ratings yet
- Coonrad Morrey ElbowDocument2 pagesCoonrad Morrey Elbowgcif88No ratings yet
- RadiologyDocument1 pageRadiologyMark Christian BentijabaNo ratings yet
- Resume - Parvin MoradiDocument3 pagesResume - Parvin Moradimohammadrezahajian12191No ratings yet
- Protocol Adult TTE SampleDocument4 pagesProtocol Adult TTE Samplemsukhan000No ratings yet
- User Guide For The Participant Use Data File: American College of Surgeons National Surgical Quality Improvement ProgramDocument40 pagesUser Guide For The Participant Use Data File: American College of Surgeons National Surgical Quality Improvement Programbobobobo12341212No ratings yet
- EndosDocument8 pagesEndosAli ZainNo ratings yet
- Flap Basics I Rotation and Transposition FlapsDocument9 pagesFlap Basics I Rotation and Transposition FlapsariskaNo ratings yet
- Nejmoa2206606 AppendixDocument41 pagesNejmoa2206606 AppendixAndikaputra Brahma WidiantoroNo ratings yet
- Answers To Exams - Acland's Video Atlas of Human Anatomy (Lower Extremity)Document72 pagesAnswers To Exams - Acland's Video Atlas of Human Anatomy (Lower Extremity)siddhantaNo ratings yet