Professional Documents
Culture Documents
0 ratings0% found this document useful (0 votes)
20 views11lect Muscle2 Summary2017
11lect Muscle2 Summary2017
Uploaded by
Dan ChoiThis document summarizes the key characteristics of the three main types of muscle tissue - skeletal, cardiac, and smooth muscle. Skeletal muscle is voluntarily controlled and innervated by motor neurons at the neuromuscular junction. Calcium release triggers muscle fiber contraction. Cardiac muscle forms the heart walls and contracts involuntarily through electrical coupling between cardiomyocytes. Smooth muscle lines organs like blood vessels and intestines and contracts through autonomic innervation and gap junction coupling between fibers without striations. Clinical examples of muscle diseases are also discussed.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You might also like
- @anesthesia Books 2019 Hensley's PDFDocument1,175 pages@anesthesia Books 2019 Hensley's PDFAurora Herrera100% (1)
- Molecular Biology of The Cell, Sixth Edition Chapter 16: The CytoskeletonDocument37 pagesMolecular Biology of The Cell, Sixth Edition Chapter 16: The CytoskeletonJeanPaule Joumaa100% (1)
- Gen Bio 2 Lec PPT - 1795379778Document502 pagesGen Bio 2 Lec PPT - 1795379778Rey Ann ConcepcionNo ratings yet
- MCAT ReviewDocument162 pagesMCAT ReviewYukiC123No ratings yet
- AP I 2013 Exam 3 AnswersDocument13 pagesAP I 2013 Exam 3 AnswerssunilsheelavantNo ratings yet
- The Adaptations To Strength Training - Morphological and Neurological Contributions To Increased Strength PDFDocument24 pagesThe Adaptations To Strength Training - Morphological and Neurological Contributions To Increased Strength PDFLeonNo ratings yet
- Muscle PhysiologyDocument50 pagesMuscle PhysiologyJoyce Adjei-boateng100% (1)
- Muscle PhysiologyDocument24 pagesMuscle PhysiologyArmando AlehandroNo ratings yet
- Musculoskeletal PhysiologyDocument5 pagesMusculoskeletal PhysiologyKhairul IkhwanNo ratings yet
- PhysiologyDocument7 pagesPhysiologyLe Maurice CiminiNo ratings yet
- MuscleDocument5 pagesMuscleAbdulrahman AqraNo ratings yet
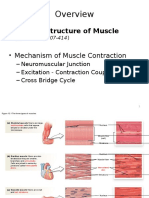
- Cellular Structure of Muscle: - Neuromuscular Junction - Excitation - Contraction Coupling - Cross Bridge CycleDocument44 pagesCellular Structure of Muscle: - Neuromuscular Junction - Excitation - Contraction Coupling - Cross Bridge CycleJon SteinerNo ratings yet
- Skeletal MusclesDocument7 pagesSkeletal MusclesAhmed OudahNo ratings yet
- Muscoskeletal SystemDocument5 pagesMuscoskeletal SystemJeevikaGoyalNo ratings yet
- 46 MusclesDocument5 pages46 Musclesuddim004100% (2)
- 6 Contraction of Skeletal MuscleDocument109 pages6 Contraction of Skeletal MuscleHaslinNo ratings yet
- G. Muscle Physiology - 1Document45 pagesG. Muscle Physiology - 1Milimo MweembaNo ratings yet
- Daftar Pustaka (Mini Projek)Document18 pagesDaftar Pustaka (Mini Projek)herfikaNo ratings yet
- (L2) - Locomotion and Movement - Sept 25, 2019 - WednesdayDocument45 pages(L2) - Locomotion and Movement - Sept 25, 2019 - WednesdayRofiul HussainNo ratings yet
- Muscle Tissue OutlineDocument4 pagesMuscle Tissue OutlinePeachy PieNo ratings yet
- Muscular TissuesDocument46 pagesMuscular TissuesDAVE CANALETANo ratings yet
- Physiology of Skeletal & Smooth MusclesDocument10 pagesPhysiology of Skeletal & Smooth MusclesAli AlhamadNo ratings yet
- Y Yyy Yy Yyyy YyyDocument5 pagesY Yyy Yy Yyyy YyyCzarina CatambingNo ratings yet
- Muscular System - 2Document77 pagesMuscular System - 2JB AriasdcNo ratings yet
- Chapter 7 - Muscular SystemDocument50 pagesChapter 7 - Muscular SystemZea Mae AgirNo ratings yet
- Histology of Cardiac and Smooth MuscleDocument73 pagesHistology of Cardiac and Smooth MuscleShehryar AbbasNo ratings yet
- Histology of Cardiac and Smooth MuscleDocument73 pagesHistology of Cardiac and Smooth MuscleShehryar AbbasNo ratings yet
- Smooth MuscleDocument51 pagesSmooth Musclefilza farheenNo ratings yet
- MUSCLE CELL PHYSIOLOGY MBCHB YEAR 1 2016-2Document289 pagesMUSCLE CELL PHYSIOLOGY MBCHB YEAR 1 2016-2AdminNo ratings yet
- SDL MuscularDocument6 pagesSDL MuscularMonique Eloise GualizaNo ratings yet
- Muscular SystemDocument12 pagesMuscular SystemChrisjohn Aster OsioNo ratings yet
- Muscle Tissue 2012Document13 pagesMuscle Tissue 2012ST. Fatimah KadirNo ratings yet
- DhruvalHow Is Strength of Contraction Regulated in Different Types of MuscleDocument5 pagesDhruvalHow Is Strength of Contraction Regulated in Different Types of MuscleDhruvalNo ratings yet
- Locomotion and MovementDocument9 pagesLocomotion and Movementpoojari.dedeepyaNo ratings yet
- Excitable Tissue MuscleDocument45 pagesExcitable Tissue MuscleGrace NdutaNo ratings yet
- The Muscular SystemDocument9 pagesThe Muscular SystemKathleenJoyGalAlmasinNo ratings yet
- Human Muscular & Skeletal System - Grade 11 & 12Document24 pagesHuman Muscular & Skeletal System - Grade 11 & 12Ishita SinghNo ratings yet
- Smooth Muscle Explained FreeDocument22 pagesSmooth Muscle Explained FreeOmphile DansonNo ratings yet
- Types of Muscle TissueDocument11 pagesTypes of Muscle TissueAndrea Louise ReyesNo ratings yet
- Tell Them What You're Going To Tell Them. Tell Them. Tell Them What You Just Told Them. AristotleDocument17 pagesTell Them What You're Going To Tell Them. Tell Them. Tell Them What You Just Told Them. AristotleSafiya JamesNo ratings yet
- Muscle PDFDocument42 pagesMuscle PDFleti332100% (1)
- 6.muscular TissueDocument40 pages6.muscular Tissuemero wowNo ratings yet
- MascularDocument39 pagesMascularAive BelistaNo ratings yet
- Chapter 7 - Muscular SystemDocument29 pagesChapter 7 - Muscular SystemlNo ratings yet
- Muscle Tissue: Thomas A. Marino, PH.DDocument86 pagesMuscle Tissue: Thomas A. Marino, PH.DzellaNo ratings yet
- 10lect Muscle1 Summary2017Document3 pages10lect Muscle1 Summary2017Dan ChoiNo ratings yet
- ch9 NotesDocument31 pagesch9 NotesChris Baden HadawayNo ratings yet
- Skeletal Muscle Contraction and The Motor UnitsDocument4 pagesSkeletal Muscle Contraction and The Motor UnitsAnonymous vnv6QFNo ratings yet
- B Muscle Tissue HistologyDocument55 pagesB Muscle Tissue HistologyAffie SaikolNo ratings yet
- Nerve and Muscle Lecture 6 paraDocument24 pagesNerve and Muscle Lecture 6 paraTatenda SibandaNo ratings yet
- Bio 215 Topic 5 MusclesDocument88 pagesBio 215 Topic 5 MusclesYara BeainiNo ratings yet
- Muscular TissueDocument65 pagesMuscular TissueMitzel SapaloNo ratings yet
- Section SurnameFirstname Worksheet Week 4 Muscle PhysiologyDocument9 pagesSection SurnameFirstname Worksheet Week 4 Muscle PhysiologyZoe FormosoNo ratings yet
- Electromyogram - Principles and ApplicationsDocument12 pagesElectromyogram - Principles and ApplicationsIoana PetreNo ratings yet
- Muscular TissueDocument6 pagesMuscular TissueChezkaMayC.OliverosNo ratings yet
- Module 10 Kin 267 Muscle TissueDocument4 pagesModule 10 Kin 267 Muscle TissueJ aNo ratings yet
- Handout MusclesDocument3 pagesHandout Musclesirene9tan9ailianNo ratings yet
- Azantee Yazmie Abdul Wahab Dept. of Obstetrics & Gynaecology Kulliyyah of Medicine IIUM KuantanDocument51 pagesAzantee Yazmie Abdul Wahab Dept. of Obstetrics & Gynaecology Kulliyyah of Medicine IIUM KuantanNur ShafilaNo ratings yet
- Zoology PPT Muscular SystemDocument68 pagesZoology PPT Muscular SystemDian O. Velasquez100% (1)
- Muscle PhysiologyDocument7 pagesMuscle PhysiologyNicole Erin TomaquinNo ratings yet
- Chapter 12 - Muscle PhysiologyDocument21 pagesChapter 12 - Muscle PhysiologyAlec McIntoshNo ratings yet
- Muscle Tissue Slides C 20152016Document39 pagesMuscle Tissue Slides C 20152016brennan12345No ratings yet
- Cellular CardiomyocyteDocument37 pagesCellular CardiomyocyteHiba PNo ratings yet
- MUSCLE and NERVOUSHISTOLOGYDocument78 pagesMUSCLE and NERVOUSHISTOLOGYAerielle De GuzmanNo ratings yet
- 12lect Nerve1 Summary2017Document4 pages12lect Nerve1 Summary2017Dan ChoiNo ratings yet
- 10lect Muscle1 Summary2017Document3 pages10lect Muscle1 Summary2017Dan ChoiNo ratings yet
- 09lect Bone Summary2017Document3 pages09lect Bone Summary2017Dan ChoiNo ratings yet
- 05lect Adhesion Summary2017Document5 pages05lect Adhesion Summary2017Dan ChoiNo ratings yet
- 07lect EpitheliumCTissue Summary2017Document4 pages07lect EpitheliumCTissue Summary2017Dan ChoiNo ratings yet
- 08 Cartilage Summary2017Document2 pages08 Cartilage Summary2017Dan ChoiNo ratings yet
- 06lect ECM Summary2017Document5 pages06lect ECM Summary2017Dan ChoiNo ratings yet
- 03lect Cell2 Summary2017Document4 pages03lect Cell2 Summary2017Dan ChoiNo ratings yet
- 04lect Cell3 Summary2017Document5 pages04lect Cell3 Summary2017Dan ChoiNo ratings yet
- 01lect Intro Summary2017Document2 pages01lect Intro Summary2017Dan ChoiNo ratings yet
- 02lect Cell1 Summary2017Document4 pages02lect Cell1 Summary2017Dan ChoiNo ratings yet
- Muscles TransesDocument3 pagesMuscles TranseskimeehhNo ratings yet
- Anatomy and Physiology Midterm Chapter Quiz Skeletal and Muscular System Skeletal SystemDocument8 pagesAnatomy and Physiology Midterm Chapter Quiz Skeletal and Muscular System Skeletal SystemMartin ManuelNo ratings yet
- Biol 273 NotesDocument46 pagesBiol 273 NotesDivyaNo ratings yet
- Chapter-1 Structural OrissuesDocument18 pagesChapter-1 Structural OrissuesRama DeviNo ratings yet
- Anatomy and Physiology 6th Edition Gunstream Test Bank Full Chapter PDFDocument42 pagesAnatomy and Physiology 6th Edition Gunstream Test Bank Full Chapter PDFserenafinnodx100% (13)
- Histology World MCQDocument43 pagesHistology World MCQAziz100% (7)
- Physiology of Muscle ContractionDocument3 pagesPhysiology of Muscle ContractionAJ AbraganNo ratings yet
- Anatomy and Physiology of MuscleDocument51 pagesAnatomy and Physiology of Musclenandhini raguNo ratings yet
- Pre Release Scientific Article Jan 2024 IAL U5 Edexcel BiologyDocument25 pagesPre Release Scientific Article Jan 2024 IAL U5 Edexcel BiologyAliza JafriNo ratings yet
- Anatomy Lec 9 (Muscles)Document21 pagesAnatomy Lec 9 (Muscles)HumrazNo ratings yet
- Songs NewDocument16 pagesSongs NewEdmonLagarto100% (1)
- Sliding Filament Model of ContractionDocument3 pagesSliding Filament Model of ContractionRATU ZULFI AMALIAHNo ratings yet
- Chapter 10Document5 pagesChapter 10Nona PeriarceNo ratings yet
- 6.0 Muscular SystemDocument76 pages6.0 Muscular System[R2A] Khadijah AzlanNo ratings yet
- Chapter 2 5 - Development and Disease of Mouse Muscular - 2012 - The LaboratoryDocument31 pagesChapter 2 5 - Development and Disease of Mouse Muscular - 2012 - The LaboratoryAzmal Kabir SarkerNo ratings yet
- The Muscular System: Essentials of Anatomy & PhysiologyDocument74 pagesThe Muscular System: Essentials of Anatomy & PhysiologySwetaNo ratings yet
- 1 MusclesDocument29 pages1 MusclesGideon CavidaNo ratings yet
- General Histology and Embryology Midterms 1Document24 pagesGeneral Histology and Embryology Midterms 1rvinluan.dentNo ratings yet
- Exercise Physiology Lecture Note (Specialization)Document97 pagesExercise Physiology Lecture Note (Specialization)Shameem AliNo ratings yet
- Muscles NotesDocument13 pagesMuscles NotesGabrielle ThompsonNo ratings yet
- Muscular TissuesDocument46 pagesMuscular TissuesDAVE CANALETANo ratings yet
- The Complete Running and Marathon BookDocument194 pagesThe Complete Running and Marathon Bookmuuan1914100% (7)
- Anatomy and Physiology With Integrated Study Guide 5th Edition Gunstream Solutions ManualDocument10 pagesAnatomy and Physiology With Integrated Study Guide 5th Edition Gunstream Solutions Manualsamuelfintanult1jj100% (33)
- Anatomy, Physiology, KinesiologyDocument442 pagesAnatomy, Physiology, KinesiologyFloriza de Leon100% (4)
11lect Muscle2 Summary2017
11lect Muscle2 Summary2017
Uploaded by
Dan Choi0 ratings0% found this document useful (0 votes)
20 views4 pagesThis document summarizes the key characteristics of the three main types of muscle tissue - skeletal, cardiac, and smooth muscle. Skeletal muscle is voluntarily controlled and innervated by motor neurons at the neuromuscular junction. Calcium release triggers muscle fiber contraction. Cardiac muscle forms the heart walls and contracts involuntarily through electrical coupling between cardiomyocytes. Smooth muscle lines organs like blood vessels and intestines and contracts through autonomic innervation and gap junction coupling between fibers without striations. Clinical examples of muscle diseases are also discussed.
Original Description:
Original Title
11Lect_Muscle2_Summary2017(1)
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document summarizes the key characteristics of the three main types of muscle tissue - skeletal, cardiac, and smooth muscle. Skeletal muscle is voluntarily controlled and innervated by motor neurons at the neuromuscular junction. Calcium release triggers muscle fiber contraction. Cardiac muscle forms the heart walls and contracts involuntarily through electrical coupling between cardiomyocytes. Smooth muscle lines organs like blood vessels and intestines and contracts through autonomic innervation and gap junction coupling between fibers without striations. Clinical examples of muscle diseases are also discussed.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
0 ratings0% found this document useful (0 votes)
20 views4 pages11lect Muscle2 Summary2017
11lect Muscle2 Summary2017
Uploaded by
Dan ChoiThis document summarizes the key characteristics of the three main types of muscle tissue - skeletal, cardiac, and smooth muscle. Skeletal muscle is voluntarily controlled and innervated by motor neurons at the neuromuscular junction. Calcium release triggers muscle fiber contraction. Cardiac muscle forms the heart walls and contracts involuntarily through electrical coupling between cardiomyocytes. Smooth muscle lines organs like blood vessels and intestines and contracts through autonomic innervation and gap junction coupling between fibers without striations. Clinical examples of muscle diseases are also discussed.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
You are on page 1of 4
Lecture
11 Muscle II – September 29, 2017 (Dr. Moukhles)
Ch 8:
3rd edition: pg. 168-184
4th edition: pg. 192-209
Somatic/Voluntary Motor Neuron Innervation
• Skeletal muscle: under voluntary control by motor neurons
• Motor unit: a motor neuron that originates in the ventral portion of the
spinal cord and all the muscle fibers that it innervates
• Neuromuscular junction (NMJ): the junction between the axon terminal of
the motor neuron and the motor endplate of the myofiber
o Axon terminal: the presynaptic portion of the NMJ and sends the
synaptic signal
o Motor endplate: the postsynaptic portion of the NMJ that receives the
synaptic signal. It is a specialized area of the sarcolemma/plasma
membrane of the skeletal myofiber
o Synaptic cleft: The depression in the sarcolemma of the myofiber
caused by the presence of the motor endplate
o Junctional folds: folds of the plasma membrane at the NMJ
Excitation-Contraction Coupling
• An action potential traveling down the axon of the neuron will depolarize the
neuronal plasma membrane
• Presynaptic vesicles containing the neurotransmitter, acetylcholine (ACh),
fuse with the plasma membrane of the axon terminal
• ACh is released into the synaptic cleft where it binds ACh receptors on the
sarcolemma of the motor end plate
• This triggers a depolarizing action potential in the muscle plasma membrane
that travels down the T-tubules to induce Ca++ release from the terminal
cisternae of the SR in the triad (10Lect – Muscle 1)
• The result is a contraction of the sarcomeres
• Contractions stop due to the action of an ATP-dependent Ca++ pump in the
SR
o Actively transports the released Ca++ in the cytoplasm back into the
SR
Please note: The motor neurons that are involved in this process are induced to
differentiate in the ventral portion of the developing spinal chord due to the
inductive action of the notochord as will be discussed in the Development lectures;
the specifics of neuron structure and function will be discussed in more detail in the
Nervous tissue lectures
Clinical correlations:
1) Botulism
• A multimeric toxin produced by the bacterium Clostridium botulinum that
prevents the release of ACh from axon terminals by inhibiting the fusion of
ACh-containing vesicles with the pre-synaptic axonal membrane at the NMJ
• Large quantities of botox leads to botulism à characterized by large scale
muscular paralysis, respiratory failure, and even death because muscle
contraction can’t occur
• For cosmetic purposes it is used in much smaller doses to paralyze muscle
contraction in order to decrease age-related wrinkling
2) Duchenne and Becker Muscular Dystrophy
• Disease that causes weakness and loss of muscle.
• Generally hereditary or result from mutations early at birth
- Caused by mutations in the cytoskeletal linker protein dystrophin
o Dystrophin is a vital part of the dystroglycan protein complex (See
Lect10 Muscle I). This complex acts as a linkage between the ECM and
the cytoskeleton via intracellular actin
- Mutations in dystrophin cause the complex to be released from the actin
cytoskeleton intracellularly.
o This disrupts the link of the muscle fibers to the basal lamina. Over
time this will cause damage to the sarcolemma and destruction of the
sarcomeres, ultimately leading to myofiber/muscle cell death. This
will induce inflammation (increased macrophages), followed by
increased collagenous CT and adipose tissue infiltration into the
muscle—known as fatty fibrosis.
o At the gross anatomical level this results in an initial swelling of the
muscle = pseudo-hypertrophy. This is followed by a gradual 'muscle
wasting' (i.e. loss of muscle mass/definition).
o Secondary effects are scholiosis (lateral curvature of the spine),
difficulties with clearing the respiratory tract and cardiac problems
• Attempts to correct the defect are being made using viral-mediated transfer of
the wild-type dystrophin gene into myofibers.
(Note: True 'hypertrophy' is an increase in tissue/organ size that is usually caused by
an increase in the size of the functional cells in the tissue/organ. Thus, the increased
muscle mass that occurs due to exercise in a healthy person is true hypertrophy as
opposed to the fake/pseudo hypertrophy that is a clinical symptom in DMD that is
caused by an increase in inflammation and fibrosis not an increase in actual myofiber
cell mass)
Inflammation will be described in some detail in the Lymphoid lectures.
Cardiac Muscle
• Found exclusively in the heart
• Cardiac muscle cells = cardiac myofibers = cardiomyocytes form the
'myocardium' (ie. the thick contractile walls of the heart's ventricles and the
atria).
• Cardiac myofibers are striated with true sarcomeres but they are mononuclear
(one central nucleus per cardiac myofiber/cardiac muscle cell)
• Contraction is involuntarily controlled (fibers contract spontaneously with
inherent rhythmicity).
• Cardiac myofibers are short and branched and they attach to each other by
intercalated disks that contain:
1) Transversely-located (across the fibers at right angles) adherens junctions
that are adhesive and anchor actin myofilaments of the terminal sarcomeres.
There are also desmosomes that anchor the adjacent cardiomyofibers to each
other.
2) Laterally-located (parallel to the myofilaments) gap junctions, which
electrically couple the cardiac myofibers by allowing for rapid flow of
information between fibers.
- This is important for the inherent rhythmicity of cardiomyocytes, as
the stimulation of one cell can lead to the stimulation of neighbouring
cells via gap junction transfer of ions.
• T tubules are present and prominent in cardiomyocytes. However, they have
sparse amounts of sarcoplasmic reticulum associated with them compared to
the situation in skeletal myofibers.
o Dyad/diad: One tubule usually has one associated cistern of sarcoplasmic
reticulum (dyad in cardiomyocytes vs triad in skeletal muscle).
• In cardiac muscle not as much calcium is stored in the sarcoplasmic reticulum,
therefore more calcium enters the cells to initiate contraction through coupled
calcium-sodium channels in the T-Tubule membrane as well as the sarcoplasmic
reticulum membrane.
Smooth Muscle
• Found in the walls of tube-based organs/structures where their contraction
decreases the diameter of the central lumen (eg. during rhythmic, peristaltic
contractions in the gastrointestinal and urogenital systems; to decrease blood
flow through small arteries and arterioles)
• Smooth muscle myofibers are mononucleated, spindle-shaped and tapered at
each end.
o There are no T-Tubules
• Contraction is involuntary and is initiated by multiple contacts from the axons
of neurons from the autonomic nervous system
o There are no well-defined neuromuscular junctions
• There are large numbers of gap junctions between smooth muscle myofibers to
allow direct electrical communication between adjacent smooth muscle fibers.
o This direct electrical communication facilitates slow rhythmic
contractions across many linked myofibers in smooth muscle tissues
§ Every individual smooth myofiber/muscle cell does not need
to be innervated to contract due to the gap junction-mediated
electrical coupling with neighbouring myofibers.
• There are no sarcomeres; therefore smooth muscle is not striated.
• Smooth myofibers have an extensive array of interweaving thin (actin) and
thick (myosin) filaments that give some multi-directionality to the contraction
(ie. they are arranged at oblique angles rather than in parallel arrays as is the
case in skeletal and cardiac myofiber sarcomeres).
o Thin filaments attach to aggregates of adapter/scaffold/linker proteins
called dense bodies that include actin bundling proteins (eg. alpha-
actinin) and act as an anchor for the filaments within the cytoplasm
(analagous to Z-lines/Z-plaques in skeletal/cardiac muscle).
o Actin filaments are also bundled and anchored to dense plaques at focal
adhesions at the plasma membrane.
• Contractile units consist of myosin filaments connecting to the actin filaments:
o Thick filaments (myosin) act on thin filaments to cause contractions
between the dense bodies and dense plaques (brings them closer
together); this leads to shortening of the long, tapered, fusiform-shaped
cells as well as some cell twisting. In histological sections this contractile
twisting causes the nuclei to take on a 'corkscrew'-like appearance.
o a meshwork of intermediate filaments also courses through the
smooth muscle fibers
o Examples of sites of smooth muscle:
§ Arteries and veins: in some of these blood vessels they are found in the
central tunica media (Cardiovascular lecture for more detail)
§ Multiple layers in the wall of the stomach and intestines: that act together
to generate peristalsis (progressive and rhythmic contractions of the
smooth muscle that propel food through the digestive tract; see
Gastrointestinal lectures for more detail).
Please note: these arrangements of smooth muscle tissues will be discussed in detail
in the Circulatory and Gastrointestinal System lectures.
You might also like
- @anesthesia Books 2019 Hensley's PDFDocument1,175 pages@anesthesia Books 2019 Hensley's PDFAurora Herrera100% (1)
- Molecular Biology of The Cell, Sixth Edition Chapter 16: The CytoskeletonDocument37 pagesMolecular Biology of The Cell, Sixth Edition Chapter 16: The CytoskeletonJeanPaule Joumaa100% (1)
- Gen Bio 2 Lec PPT - 1795379778Document502 pagesGen Bio 2 Lec PPT - 1795379778Rey Ann ConcepcionNo ratings yet
- MCAT ReviewDocument162 pagesMCAT ReviewYukiC123No ratings yet
- AP I 2013 Exam 3 AnswersDocument13 pagesAP I 2013 Exam 3 AnswerssunilsheelavantNo ratings yet
- The Adaptations To Strength Training - Morphological and Neurological Contributions To Increased Strength PDFDocument24 pagesThe Adaptations To Strength Training - Morphological and Neurological Contributions To Increased Strength PDFLeonNo ratings yet
- Muscle PhysiologyDocument50 pagesMuscle PhysiologyJoyce Adjei-boateng100% (1)
- Muscle PhysiologyDocument24 pagesMuscle PhysiologyArmando AlehandroNo ratings yet
- Musculoskeletal PhysiologyDocument5 pagesMusculoskeletal PhysiologyKhairul IkhwanNo ratings yet
- PhysiologyDocument7 pagesPhysiologyLe Maurice CiminiNo ratings yet
- MuscleDocument5 pagesMuscleAbdulrahman AqraNo ratings yet
- Cellular Structure of Muscle: - Neuromuscular Junction - Excitation - Contraction Coupling - Cross Bridge CycleDocument44 pagesCellular Structure of Muscle: - Neuromuscular Junction - Excitation - Contraction Coupling - Cross Bridge CycleJon SteinerNo ratings yet
- Skeletal MusclesDocument7 pagesSkeletal MusclesAhmed OudahNo ratings yet
- Muscoskeletal SystemDocument5 pagesMuscoskeletal SystemJeevikaGoyalNo ratings yet
- 46 MusclesDocument5 pages46 Musclesuddim004100% (2)
- 6 Contraction of Skeletal MuscleDocument109 pages6 Contraction of Skeletal MuscleHaslinNo ratings yet
- G. Muscle Physiology - 1Document45 pagesG. Muscle Physiology - 1Milimo MweembaNo ratings yet
- Daftar Pustaka (Mini Projek)Document18 pagesDaftar Pustaka (Mini Projek)herfikaNo ratings yet
- (L2) - Locomotion and Movement - Sept 25, 2019 - WednesdayDocument45 pages(L2) - Locomotion and Movement - Sept 25, 2019 - WednesdayRofiul HussainNo ratings yet
- Muscle Tissue OutlineDocument4 pagesMuscle Tissue OutlinePeachy PieNo ratings yet
- Muscular TissuesDocument46 pagesMuscular TissuesDAVE CANALETANo ratings yet
- Physiology of Skeletal & Smooth MusclesDocument10 pagesPhysiology of Skeletal & Smooth MusclesAli AlhamadNo ratings yet
- Y Yyy Yy Yyyy YyyDocument5 pagesY Yyy Yy Yyyy YyyCzarina CatambingNo ratings yet
- Muscular System - 2Document77 pagesMuscular System - 2JB AriasdcNo ratings yet
- Chapter 7 - Muscular SystemDocument50 pagesChapter 7 - Muscular SystemZea Mae AgirNo ratings yet
- Histology of Cardiac and Smooth MuscleDocument73 pagesHistology of Cardiac and Smooth MuscleShehryar AbbasNo ratings yet
- Histology of Cardiac and Smooth MuscleDocument73 pagesHistology of Cardiac and Smooth MuscleShehryar AbbasNo ratings yet
- Smooth MuscleDocument51 pagesSmooth Musclefilza farheenNo ratings yet
- MUSCLE CELL PHYSIOLOGY MBCHB YEAR 1 2016-2Document289 pagesMUSCLE CELL PHYSIOLOGY MBCHB YEAR 1 2016-2AdminNo ratings yet
- SDL MuscularDocument6 pagesSDL MuscularMonique Eloise GualizaNo ratings yet
- Muscular SystemDocument12 pagesMuscular SystemChrisjohn Aster OsioNo ratings yet
- Muscle Tissue 2012Document13 pagesMuscle Tissue 2012ST. Fatimah KadirNo ratings yet
- DhruvalHow Is Strength of Contraction Regulated in Different Types of MuscleDocument5 pagesDhruvalHow Is Strength of Contraction Regulated in Different Types of MuscleDhruvalNo ratings yet
- Locomotion and MovementDocument9 pagesLocomotion and Movementpoojari.dedeepyaNo ratings yet
- Excitable Tissue MuscleDocument45 pagesExcitable Tissue MuscleGrace NdutaNo ratings yet
- The Muscular SystemDocument9 pagesThe Muscular SystemKathleenJoyGalAlmasinNo ratings yet
- Human Muscular & Skeletal System - Grade 11 & 12Document24 pagesHuman Muscular & Skeletal System - Grade 11 & 12Ishita SinghNo ratings yet
- Smooth Muscle Explained FreeDocument22 pagesSmooth Muscle Explained FreeOmphile DansonNo ratings yet
- Types of Muscle TissueDocument11 pagesTypes of Muscle TissueAndrea Louise ReyesNo ratings yet
- Tell Them What You're Going To Tell Them. Tell Them. Tell Them What You Just Told Them. AristotleDocument17 pagesTell Them What You're Going To Tell Them. Tell Them. Tell Them What You Just Told Them. AristotleSafiya JamesNo ratings yet
- Muscle PDFDocument42 pagesMuscle PDFleti332100% (1)
- 6.muscular TissueDocument40 pages6.muscular Tissuemero wowNo ratings yet
- MascularDocument39 pagesMascularAive BelistaNo ratings yet
- Chapter 7 - Muscular SystemDocument29 pagesChapter 7 - Muscular SystemlNo ratings yet
- Muscle Tissue: Thomas A. Marino, PH.DDocument86 pagesMuscle Tissue: Thomas A. Marino, PH.DzellaNo ratings yet
- 10lect Muscle1 Summary2017Document3 pages10lect Muscle1 Summary2017Dan ChoiNo ratings yet
- ch9 NotesDocument31 pagesch9 NotesChris Baden HadawayNo ratings yet
- Skeletal Muscle Contraction and The Motor UnitsDocument4 pagesSkeletal Muscle Contraction and The Motor UnitsAnonymous vnv6QFNo ratings yet
- B Muscle Tissue HistologyDocument55 pagesB Muscle Tissue HistologyAffie SaikolNo ratings yet
- Nerve and Muscle Lecture 6 paraDocument24 pagesNerve and Muscle Lecture 6 paraTatenda SibandaNo ratings yet
- Bio 215 Topic 5 MusclesDocument88 pagesBio 215 Topic 5 MusclesYara BeainiNo ratings yet
- Muscular TissueDocument65 pagesMuscular TissueMitzel SapaloNo ratings yet
- Section SurnameFirstname Worksheet Week 4 Muscle PhysiologyDocument9 pagesSection SurnameFirstname Worksheet Week 4 Muscle PhysiologyZoe FormosoNo ratings yet
- Electromyogram - Principles and ApplicationsDocument12 pagesElectromyogram - Principles and ApplicationsIoana PetreNo ratings yet
- Muscular TissueDocument6 pagesMuscular TissueChezkaMayC.OliverosNo ratings yet
- Module 10 Kin 267 Muscle TissueDocument4 pagesModule 10 Kin 267 Muscle TissueJ aNo ratings yet
- Handout MusclesDocument3 pagesHandout Musclesirene9tan9ailianNo ratings yet
- Azantee Yazmie Abdul Wahab Dept. of Obstetrics & Gynaecology Kulliyyah of Medicine IIUM KuantanDocument51 pagesAzantee Yazmie Abdul Wahab Dept. of Obstetrics & Gynaecology Kulliyyah of Medicine IIUM KuantanNur ShafilaNo ratings yet
- Zoology PPT Muscular SystemDocument68 pagesZoology PPT Muscular SystemDian O. Velasquez100% (1)
- Muscle PhysiologyDocument7 pagesMuscle PhysiologyNicole Erin TomaquinNo ratings yet
- Chapter 12 - Muscle PhysiologyDocument21 pagesChapter 12 - Muscle PhysiologyAlec McIntoshNo ratings yet
- Muscle Tissue Slides C 20152016Document39 pagesMuscle Tissue Slides C 20152016brennan12345No ratings yet
- Cellular CardiomyocyteDocument37 pagesCellular CardiomyocyteHiba PNo ratings yet
- MUSCLE and NERVOUSHISTOLOGYDocument78 pagesMUSCLE and NERVOUSHISTOLOGYAerielle De GuzmanNo ratings yet
- 12lect Nerve1 Summary2017Document4 pages12lect Nerve1 Summary2017Dan ChoiNo ratings yet
- 10lect Muscle1 Summary2017Document3 pages10lect Muscle1 Summary2017Dan ChoiNo ratings yet
- 09lect Bone Summary2017Document3 pages09lect Bone Summary2017Dan ChoiNo ratings yet
- 05lect Adhesion Summary2017Document5 pages05lect Adhesion Summary2017Dan ChoiNo ratings yet
- 07lect EpitheliumCTissue Summary2017Document4 pages07lect EpitheliumCTissue Summary2017Dan ChoiNo ratings yet
- 08 Cartilage Summary2017Document2 pages08 Cartilage Summary2017Dan ChoiNo ratings yet
- 06lect ECM Summary2017Document5 pages06lect ECM Summary2017Dan ChoiNo ratings yet
- 03lect Cell2 Summary2017Document4 pages03lect Cell2 Summary2017Dan ChoiNo ratings yet
- 04lect Cell3 Summary2017Document5 pages04lect Cell3 Summary2017Dan ChoiNo ratings yet
- 01lect Intro Summary2017Document2 pages01lect Intro Summary2017Dan ChoiNo ratings yet
- 02lect Cell1 Summary2017Document4 pages02lect Cell1 Summary2017Dan ChoiNo ratings yet
- Muscles TransesDocument3 pagesMuscles TranseskimeehhNo ratings yet
- Anatomy and Physiology Midterm Chapter Quiz Skeletal and Muscular System Skeletal SystemDocument8 pagesAnatomy and Physiology Midterm Chapter Quiz Skeletal and Muscular System Skeletal SystemMartin ManuelNo ratings yet
- Biol 273 NotesDocument46 pagesBiol 273 NotesDivyaNo ratings yet
- Chapter-1 Structural OrissuesDocument18 pagesChapter-1 Structural OrissuesRama DeviNo ratings yet
- Anatomy and Physiology 6th Edition Gunstream Test Bank Full Chapter PDFDocument42 pagesAnatomy and Physiology 6th Edition Gunstream Test Bank Full Chapter PDFserenafinnodx100% (13)
- Histology World MCQDocument43 pagesHistology World MCQAziz100% (7)
- Physiology of Muscle ContractionDocument3 pagesPhysiology of Muscle ContractionAJ AbraganNo ratings yet
- Anatomy and Physiology of MuscleDocument51 pagesAnatomy and Physiology of Musclenandhini raguNo ratings yet
- Pre Release Scientific Article Jan 2024 IAL U5 Edexcel BiologyDocument25 pagesPre Release Scientific Article Jan 2024 IAL U5 Edexcel BiologyAliza JafriNo ratings yet
- Anatomy Lec 9 (Muscles)Document21 pagesAnatomy Lec 9 (Muscles)HumrazNo ratings yet
- Songs NewDocument16 pagesSongs NewEdmonLagarto100% (1)
- Sliding Filament Model of ContractionDocument3 pagesSliding Filament Model of ContractionRATU ZULFI AMALIAHNo ratings yet
- Chapter 10Document5 pagesChapter 10Nona PeriarceNo ratings yet
- 6.0 Muscular SystemDocument76 pages6.0 Muscular System[R2A] Khadijah AzlanNo ratings yet
- Chapter 2 5 - Development and Disease of Mouse Muscular - 2012 - The LaboratoryDocument31 pagesChapter 2 5 - Development and Disease of Mouse Muscular - 2012 - The LaboratoryAzmal Kabir SarkerNo ratings yet
- The Muscular System: Essentials of Anatomy & PhysiologyDocument74 pagesThe Muscular System: Essentials of Anatomy & PhysiologySwetaNo ratings yet
- 1 MusclesDocument29 pages1 MusclesGideon CavidaNo ratings yet
- General Histology and Embryology Midterms 1Document24 pagesGeneral Histology and Embryology Midterms 1rvinluan.dentNo ratings yet
- Exercise Physiology Lecture Note (Specialization)Document97 pagesExercise Physiology Lecture Note (Specialization)Shameem AliNo ratings yet
- Muscles NotesDocument13 pagesMuscles NotesGabrielle ThompsonNo ratings yet
- Muscular TissuesDocument46 pagesMuscular TissuesDAVE CANALETANo ratings yet
- The Complete Running and Marathon BookDocument194 pagesThe Complete Running and Marathon Bookmuuan1914100% (7)
- Anatomy and Physiology With Integrated Study Guide 5th Edition Gunstream Solutions ManualDocument10 pagesAnatomy and Physiology With Integrated Study Guide 5th Edition Gunstream Solutions Manualsamuelfintanult1jj100% (33)
- Anatomy, Physiology, KinesiologyDocument442 pagesAnatomy, Physiology, KinesiologyFloriza de Leon100% (4)