Professional Documents
Culture Documents
Hypoxic-Ischemic Encephalopathy (HIE)
Hypoxic-Ischemic Encephalopathy (HIE)
Uploaded by
Ritu VermaOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Hypoxic-Ischemic Encephalopathy (HIE)
Hypoxic-Ischemic Encephalopathy (HIE)
Uploaded by
Ritu VermaCopyright:
Available Formats
What Is Hypoxic-Ischemic Encephalopathy (HIE)?
What is hypoxic-ischemic encephalopathy (HIE)?
Hypoxic-ischemic encephalopathy (HIE) is a type of newborn brain damage caused by oxygen
deprivation and limited blood flow. HIE is a type of birth injury; this is a broad term used to
refer to any harm that a baby experiences at or near the time of birth. Other terms used for
HIE include birth asphyxia, perinatal asphyxia, and neonatal encephalopathy.
In some cases, therapeutic hypothermia can prevent or minimize permanent brain damage,
although it must be given within just hours of the baby’s birth/oxygen-depriving injury (see
“Treatment for HIE” for more information). However, with and without therapeutic
hypothermia, many infants with HIE go on to develop permanent health conditions and
disorders. These include cerebral palsy (CP), cognitive disabilities, epilepsy, hearing and
vision impairments, and much more.
What Is Hypoxic-Ischemic Encephalopathy (HIE)? | 1
What Is Hypoxic-Ischemic Encephalopathy (HIE)?
The full extent of damage from HIE is typically not apparent immediately after birth, for two
major reasons:
Brain injury from HIE is an evolving process. When blood flow is cut off to parts of the brain,
cells begin to break down, die, and release substances which are toxic to other cells. These
cells then begin to die off and continue the chain reaction, which causes brain injury to
spread over a period of hours or days. Therapeutic hypothermia can help to disrupt this chain
reaction.
Damage from HIE may occasionally not become apparent until a child has developmental
delays. For example, impacts on mobility may not be noticed until the child struggles to meet
milestones such as crawling or walking.
Once there is permanent brain damage, there is no cure for HIE . However, there are many
treatments and therapies that can improve symptoms and function in children with HIE.
What are the causes of HIE?
HIE can be caused by a variety of medical complications around the time of birth. In many
cases, medical malpractice also plays a role. For example, doctors may fail to properly
monitor the health of the mother and baby and identify potential issues. Alternatively, they
What Is Hypoxic-Ischemic Encephalopathy (HIE)? | 2
What Is Hypoxic-Ischemic Encephalopathy (HIE)?
may recognize problems but not take them seriously enough/fail to intervene. Learn more
information on the association between HIE and malpractice, as well as legal options.
For over 20 years, our legal team has fought on behalf of children with HIE as a result of
medical malpractice.
Get a free legal consultation
The following health problems and negligent actions can lead to HIE (these are just a few
examples; for more information please see this page):
Mismanagement of a high-risk pregnancy: Women with conditions such as preeclampsia
and gestational diabetes require more extensive monitoring and treatment.
Umbilical cord complications: The umbilical cord is like a lifeline between mother and
baby, supplying oxygen and nutrients and removing fetal waste. Anything that compresses
the cord or reduces its function puts the baby at risk of HIE.
Placental or uterine complications: The placenta and uterus also play very important roles
in providing oxygenated blood to the baby. Examples of placental and uterine issues that
may cause HIE include:
Placental abruption: when the placenta separates from the uterus before the baby is
born
Placenta previa: when the placenta attaches too close to the cervix; this can cause
dangerous bleeding and oxygen deprivation during delivery
Placental insufficiency: when the placenta is unable to deliver enough blood to the baby
Uterine rupture: when the uterus tears, partially or completely
Infections: Infections in the mother can spread to the baby during labor and delivery,
especially if the medical team do not take adequate precautions (such as doing indicated
What Is Hypoxic-Ischemic Encephalopathy (HIE)? | 3
What Is Hypoxic-Ischemic Encephalopathy (HIE)?
infection screening and prescribing antibiotics when needed).
Improper fetal heart monitoring: If a baby shows signs of fetal distress on the fetal heart
monitor, doctors and nurses can often intervene so that their oxygen supply is restored. If
necessary, this may involve an emergency C-section. However, if monitoring is sporadic or
does not occur, important signs of danger may be missed.
Failure to prevent a premature birth: Premature babies are at higher risk for HIE and other
birth injuries because their lungs are so underdeveloped. Therefore, it is very important
that doctors do what they can to prevent premature birth, such as performing a cervical
cerclage (a stitch placed in the cervix to stop it from opening too early) or providing
progesterone treatment.
Allowing prolonged labor to continue: Labor is stressful for babies because uterine
contractions compress the placenta and umbilical cord that supply their oxygen. If
something is preventing labor from progressing, and physicians do not offer intervention
(such as an emergency C-section), this is negligence. Prolonged labor is more likely to
occur when a baby is larger than normal, or the mother’s pelvis is smaller than normal.
Medication problems: Sometimes physicians prescribe medications such as Pitocin and
Cytotec in order to induce or enhance labor. Unfortunately, these medications can also
cause uterine contractions to become so strong and frequent that the baby is dangerously
deprived of oxygen.
Mismanagement of a neonatal condition: Hypoxic-ischemic injury can be caused by
complications during the neonatal period, i.e. a baby’s first month of life. Problems such as
respiratory distress, jaundice, and neonatal hypoglycemia can all contribute to an HIE
diagnosis, especially if mismanaged.
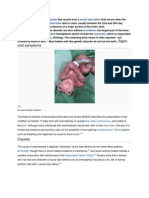
What are the signs and symptoms of HIE?
Babies with HIE may exhibit any of the following signs (among others):
Breathing problems
Feeding problems
Missing reflexes (for example, the baby does not respond to loud noises)
Seizures
What Is Hypoxic-Ischemic Encephalopathy (HIE)? | 4
What Is Hypoxic-Ischemic Encephalopathy (HIE)?
Low Apgar scores
Low or high muscle tone
Altered level of consciousness (e.g. not alert)
How do you pronounce hypoxic-ischemic encephalopathy (HIE)?
Treatment for HIE
HIE is managed using a treatment called therapeutic hypothermia, where the baby’s brain or
body is cooled down below normal temperatures to slow the cascade effect that causes
widespread damage. This allows the baby’s brain to recover and reduces the level of
disability they may have as they grow. According to current guidelines, the treatment must
be given within six hours of birth, although there is some evidence to suggest it may be
beneficial when given up to 24 hours.
Therapeutic hypothermia lasts for around 72 hours, allowing the baby’s metabolic rate to
slow. This prevents further damage known as reperfusion injury, which occurs when normal
oxygenation and blood flow are restored too quickly to the brain’s cells. While it may seem
counter-intuitive that restoring flow quickly could cause further injury, the brain’s cells react
differently to rapid oxygenation after being oxygen deprived. After oxygen deprivation injury,
rapid oxygenation can cause more inflammation and the release of certain harmful
compounds. Hypothermia treatment works to stabilize the brain’s cells and prevent or limit
damaging inflammation.
In addition to therapeutic hypothermia, medical staff should provide supportive care, which
can mean helping the baby breathe, controlling and preventing seizures and low blood sugar,
minimizing brain swelling, and more. In the long term, babies with brain damage from HIE
may benefit from a wide variety of treatments and therapies. Although these are not
What Is Hypoxic-Ischemic Encephalopathy (HIE)? | 5
What Is Hypoxic-Ischemic Encephalopathy (HIE)?
curative, they can minimize symptoms and maximize function. Click here for more
information.
Types and forms of HIE
If they suspect HIE, medical staff can conduct brain imaging, such as ultrasound and MRI, to
see how badly tissue in the brain is damaged. Caregivers also do a blood gas test to
determine the pH of the baby’s blood, which can also provide some information about the
baby’s oxygen levels.
The severity of HIE is determined using Sarnat staging, which takes into account clinical
presentation, exam results, seizure presence, and illness duration. Mild HIE is classified as
Sarnat Grade I, and severity increases up to a maximal Stage III (1).
Prevalence and incidence of HIE
HIE is estimated to occur in between 2 to 9 per 1,000 live births. The advent of therapeutic
hypothermia has significantly reduced rates of death and disability, but outcomes can still be
What Is Hypoxic-Ischemic Encephalopathy (HIE)? | 6
What Is Hypoxic-Ischemic Encephalopathy (HIE)?
severe. In one study, nearly half of newborns with HIE either died or had a major
neurodevelopmental disability at an 18-month follow-up. However, 40 percent of babies in
this study had normal early development (2).
Life expectancy for people with HIE and cerebral palsy
The life expectancy of people with hypoxic-ischemic encephalopathy depends greatly on the
extent to which they are affected and their access to treatments and therapies. For this
reason, it’s difficult provide an “average” lifespan for people with HIE. Because many children
with HIE are also diagnosed with cerebral palsy, it may be more useful to look at life
expectancies for people with cerebral palsy.
People with very mild cerebral palsy are typically expected to live as long as their peers in
the general population. Overall, life expectancy for a person with cerebral palsy depends on
the extent to which they are affected:
Lifespan of mild cerebral palsy: For people with fairly mild cerebral palsy (defined as
walking unaided), life expectancy in females has been estimated at 70-80 years, and in
males at 66-76 years.
Lifespan of severe cerebral palsy: For those who are more severely affected (defined as an
inability to lift the head and being fed through a tube), life expectancies have been
estimated to be shorter for both females and males, depending on the quality of medical
care received.
These lifespan numbers were extracted from a 2008 study in Developmental Medicine and
Child Neurology. Click here to view the paper, which contains a detailed table on life
expectancy for people with cerebral palsy. It takes into account age, sex, movement ability,
and feeding mechanism (3).
What Is Hypoxic-Ischemic Encephalopathy (HIE)? | 7
What Is Hypoxic-Ischemic Encephalopathy (HIE)?
More detailed information on HIE
For more information on HIE, please visit our Medical Information section.
About the HIE Help Center and ABC Law Centers
The HIE Help Center is run by ABC Law Centers, a medical malpractice firm exclusively
handling cases involving HIE and other birth injuries. Our lawyers have over 100 years of
combined experience with this type of law, and have been advocating for children with HIE
and related disabilities since the firm’s inception in 1997.
We are passionate about helping families obtain the compensation necessary to cover their
extensive medical bills, loss of wages (if one or both parents have to miss work in order to
care for their child), assistive technology, and other necessities.
If you suspect your child’s HIE may have been caused by medical negligence, please contact
us today to learn more about pursuing a case. We provide free legal consultations, during
which we will inform you of your legal options and answer any questions you have. Moreover,
you would pay nothing throughout the entire legal process unless we obtain a favorable
settlement.
You are also welcome to reach out to us with inquiries that are not related to malpractice. We
cannot provide individualized medical advice, but we’re happy to track down informational
resources for you.
Citations
Sarnat, H. B., & Sarnat, M. S. (1976). Neonatal encephalopathy following fetal distress: a
What Is Hypoxic-Ischemic Encephalopathy (HIE)? | 8
What Is Hypoxic-Ischemic Encephalopathy (HIE)?
clinical and electroencephalographic study. Archives of neurology, 33(10), 696-705.
(n.d.). Retrieved January 15, 2019, from
https://www.uptodate.com/contents/clinical-features-diagnosis-and-treatment-of-neonatal-en
cephalopathy
Strauss, D., Brooks, J., Rosenbloom, L., & Shavelle, R. (2008). Life expectancy in cerebral
palsy: an update. Developmental Medicine & Child Neurology, 50(7), 487-493.
What Is Hypoxic-Ischemic Encephalopathy (HIE)? | 9
You might also like
- NUR 146 MCN2 RLE P2 ExamDocument22 pagesNUR 146 MCN2 RLE P2 ExamMarga WreatheNo ratings yet
- Hearing Loss in Term Newborn Infants With Hypoxic-Ischemic Encephalopathy Treated With Therapeutic Hypothermia PDFDocument8 pagesHearing Loss in Term Newborn Infants With Hypoxic-Ischemic Encephalopathy Treated With Therapeutic Hypothermia PDFstefanp89No ratings yet
- Case 9: 2-Week-Old With Lethargy - CrimsonDocument7 pagesCase 9: 2-Week-Old With Lethargy - Crimsonalwaysbeclosing52No ratings yet
- Holistic Treatment of Lyme DiseaseDocument54 pagesHolistic Treatment of Lyme Diseasefrederic9866No ratings yet
- Hypoxic Ischemic EncephalopathyDocument7 pagesHypoxic Ischemic EncephalopathyJennesse May Guiao IbayNo ratings yet
- Breathing For A Better Future: Addressing Hypoxia and Disability As Its ImpactDocument7 pagesBreathing For A Better Future: Addressing Hypoxia and Disability As Its ImpactMichelle ChristinaNo ratings yet
- Guidelines Made Simple 2017 HBPDocument68 pagesGuidelines Made Simple 2017 HBPAprilliaNo ratings yet
- Birth AsphyxiaDocument17 pagesBirth AsphyxiaFarhad AhmadNo ratings yet
- ResearchDocument3 pagesResearchapi-296915417No ratings yet
- HypoxicDocument2 pagesHypoxicHenry KaweesaNo ratings yet
- Post Asphyxia Mangement NewDocument21 pagesPost Asphyxia Mangement NewAb Imo Pectore EvanNo ratings yet
- Text Book Reading: Hipoxic Ischaemic EncephalopatyDocument23 pagesText Book Reading: Hipoxic Ischaemic EncephalopatyPanduRespatiNo ratings yet
- Prematurity: Signs and SymptomsDocument13 pagesPrematurity: Signs and SymptomsGladie Ann Dela RosaNo ratings yet
- عرض تقديميDocument24 pagesعرض تقديميAlibeyatliNo ratings yet
- Neonatal HypotoniaDocument8 pagesNeonatal Hypotoniazulfiqar aliNo ratings yet
- NewbornEmergenices2006 PDFDocument16 pagesNewbornEmergenices2006 PDFRana SalemNo ratings yet
- Sarnat HIEDocument45 pagesSarnat HIEnadi diraNo ratings yet
- Sudden Infant Death SyndromeDocument5 pagesSudden Infant Death SyndromeJanelle Gift SenarloNo ratings yet
- Hypoxic Ischemic EncephalopathyDocument13 pagesHypoxic Ischemic Encephalopathyscribdkhasa100% (1)
- PathophysiologyDocument9 pagesPathophysiologySuzette PipoNo ratings yet
- Sudden Infant Death Syndrome (SIDS)Document4 pagesSudden Infant Death Syndrome (SIDS)Julliza Joy PandiNo ratings yet
- NICU-by SreedharDocument18 pagesNICU-by SreedharSreedhar Nakka KenniNo ratings yet
- Catatan HIEDocument3 pagesCatatan HIERuni ArumndariNo ratings yet
- Post Asphyxia MangementDocument17 pagesPost Asphyxia MangementTania MahalNo ratings yet
- Management of Neonatal Seizures: AIIMS-NICU Protocols 2010Document18 pagesManagement of Neonatal Seizures: AIIMS-NICU Protocols 2010gitphillipNo ratings yet
- Cerebral PalsyDocument10 pagesCerebral PalsyGeorgina HughesNo ratings yet
- Seminar 2 Endocrine DisordersDocument44 pagesSeminar 2 Endocrine DisordersSuganthi ParthibanNo ratings yet
- Hypothermia For Newborns With Hypoxic-Ischemic Encephalopathy - Canadian Paediatric SocietyDocument9 pagesHypothermia For Newborns With Hypoxic-Ischemic Encephalopathy - Canadian Paediatric SocietylizjathanNo ratings yet
- Importance of Newborn ScreeningDocument14 pagesImportance of Newborn ScreeningSheilah Mae PadallaNo ratings yet
- Group 1Document35 pagesGroup 1Fitri IsnainiNo ratings yet
- Pul HyperDocument3 pagesPul HyperAbdul Ghaffar AbdullahNo ratings yet
- AnencephalyDocument10 pagesAnencephalyRm LavariasNo ratings yet
- A Premature Infant Is An Infant Born Before 37 WK GestationDocument5 pagesA Premature Infant Is An Infant Born Before 37 WK GestationKamila KawaiiNo ratings yet
- Cerebral Palsy: I. Definition/ DescriptionDocument5 pagesCerebral Palsy: I. Definition/ Descriptionfaye kimNo ratings yet
- Perinatal Jan-March 05Document4 pagesPerinatal Jan-March 05een265No ratings yet
- The Floppy Infant:: Evaluation of HypotoniaDocument13 pagesThe Floppy Infant:: Evaluation of HypotoniaminipredatorNo ratings yet
- IVHDocument2 pagesIVHHendra Boy SitumorangNo ratings yet
- Perinatal Asphyxia in Term and Late Preterm Infants - UpToDateDocument31 pagesPerinatal Asphyxia in Term and Late Preterm Infants - UpToDateRocio GNo ratings yet
- Causes Obstruction Causes CSF To Build Up in The Brain. If The Cause Is Congenital, Symptoms Such As AnDocument22 pagesCauses Obstruction Causes CSF To Build Up in The Brain. If The Cause Is Congenital, Symptoms Such As Anmhelandie100% (1)
- Risk Factors For Congenital CPDocument5 pagesRisk Factors For Congenital CPLucila E. AbsulioNo ratings yet
- Hypoxic-Ishchemic Encephalopathy (Hie)Document5 pagesHypoxic-Ishchemic Encephalopathy (Hie)Delphy VargheseNo ratings yet
- Cerebral Palsy: I. Definition/ DescriptionDocument4 pagesCerebral Palsy: I. Definition/ Descriptionfaye kim100% (1)
- DR - Rihab Pediatrics 04.hypothyroidismDocument7 pagesDR - Rihab Pediatrics 04.hypothyroidismMujtaba JawadNo ratings yet
- Pals HandoutDocument49 pagesPals HandoutYasir AshfaqNo ratings yet
- Birth Asphyxia: DefinitionDocument5 pagesBirth Asphyxia: DefinitionDella FerginaNo ratings yet
- Isk Factors: Short-Term ComplicationsDocument11 pagesIsk Factors: Short-Term Complicationsarju anshi kujurNo ratings yet
- Congenital Diseases: Name: Bernadette Anonoy Date: February 3, 2012 Year and Group: IV - Einstein RatingDocument7 pagesCongenital Diseases: Name: Bernadette Anonoy Date: February 3, 2012 Year and Group: IV - Einstein RatingBernadette Bithao AnonoyNo ratings yet
- Encephalo CeleDocument11 pagesEncephalo CeleMike Faustino SolangonNo ratings yet
- Newborn Screening TestDocument29 pagesNewborn Screening Testjinky_bsantos@yahoo.comNo ratings yet
- NIH Public Access: Author ManuscriptDocument15 pagesNIH Public Access: Author ManuscriptAna Rica Santiago Navarra-CruzNo ratings yet
- Jurnal 1 (2020)Document10 pagesJurnal 1 (2020)Inryuu ZenNo ratings yet
- Medical Management of Children With Down SyndromeDocument8 pagesMedical Management of Children With Down SyndromeMariana OrozcoNo ratings yet
- Newborn ScreeningDocument15 pagesNewborn ScreeningYzel Vasquez AdavanNo ratings yet
- Literature Review Pregnancy Induced HypertensionDocument4 pagesLiterature Review Pregnancy Induced HypertensionafmzaoahmicfxgNo ratings yet
- CAYABYAB Fetal-DistressDocument2 pagesCAYABYAB Fetal-DistressTrisha CayabyabNo ratings yet
- Neonatal Seizures 2014Document17 pagesNeonatal Seizures 2014akankshaNo ratings yet
- Shree Siddaganga Institute of Nursing Sciences and Research CentreDocument8 pagesShree Siddaganga Institute of Nursing Sciences and Research CentreSanthosh.S.UNo ratings yet
- What Is Hydrocephalus?Document8 pagesWhat Is Hydrocephalus?Urej BandiolaNo ratings yet
- CP NotesDocument7 pagesCP NotesKevin T. KatadaNo ratings yet
- Hypoxic-Ischemic Encephalopathy: Practice EssentialsDocument38 pagesHypoxic-Ischemic Encephalopathy: Practice EssentialsPasien ICU RSUINo ratings yet
- Thyroid Disease: Thyroid Disease at Different Ages: The most important information you need to improve your healthFrom EverandThyroid Disease: Thyroid Disease at Different Ages: The most important information you need to improve your healthNo ratings yet
- Hydrocephalus Astrology: Navigating the Stars and Healing WatersFrom EverandHydrocephalus Astrology: Navigating the Stars and Healing WatersNo ratings yet
- Initial Full-Dose Heparin For Adult: 1-Venous Thromboembolism (DVT/PE), TreatmentDocument3 pagesInitial Full-Dose Heparin For Adult: 1-Venous Thromboembolism (DVT/PE), TreatmentLamNo ratings yet
- Childhood Traumatic GriefDocument85 pagesChildhood Traumatic Griefmoi5566No ratings yet
- IJP Mhca SupplementDocument7 pagesIJP Mhca Supplementgion.nandNo ratings yet
- JSA NEW FORM - Penarikan Kabel FO 37Document6 pagesJSA NEW FORM - Penarikan Kabel FO 37Muchamad SalafudinNo ratings yet
- Esophageal VaricesDocument3 pagesEsophageal VaricesSasa LuarNo ratings yet
- INTUSSUSCEPTIONDocument1 pageINTUSSUSCEPTIONAezyreal Anne MirallesNo ratings yet
- Predicting Mental Health Illness Using Machine Learning AlgorithmsDocument8 pagesPredicting Mental Health Illness Using Machine Learning AlgorithmsRuthuja B PNo ratings yet
- Uterine Sub InvolutionDocument1 pageUterine Sub Involutionkrystle0875% (4)
- Heart FailureDocument1 pageHeart FailureTrisha VergaraNo ratings yet
- Practical Review of Diagnosis and Management of Cutaneous Tuberculosis in IndonesiaDocument6 pagesPractical Review of Diagnosis and Management of Cutaneous Tuberculosis in IndonesiaAde Afriza FeraniNo ratings yet
- Program Pelayanan Lingkungan USAIDDocument313 pagesProgram Pelayanan Lingkungan USAIDioels100% (1)
- Kerala Floods - 2018: A Report by Archbishop Andrews ThazhathDocument31 pagesKerala Floods - 2018: A Report by Archbishop Andrews Thazhathsunil unnithanNo ratings yet
- Definition of A Stress: Crisis Management WorkshopDocument22 pagesDefinition of A Stress: Crisis Management WorkshopTubocurareNo ratings yet
- Amoebiasis DiseaseDocument10 pagesAmoebiasis Diseaseshruti ghordadeNo ratings yet
- The Economics of Animal Health and ProductionDocument385 pagesThe Economics of Animal Health and ProductionMarvelous Sungirai100% (2)
- Smart Covid Care System For PatientDocument8 pagesSmart Covid Care System For Patientvishalmate10No ratings yet
- The Asbestos Institute: Contractor / SupervisorDocument4 pagesThe Asbestos Institute: Contractor / Supervisordaniellewisat7387No ratings yet
- Bilateral Stimulation and AfterlifeDocument5 pagesBilateral Stimulation and AfterlifeLuiz AlmeidaNo ratings yet
- Research Essay Final Draft 1 1Document14 pagesResearch Essay Final Draft 1 1api-549221029No ratings yet
- Prevalence and Factors Associated With MalnutritioDocument21 pagesPrevalence and Factors Associated With Malnutritiolada emmanuelNo ratings yet
- Health Infrastructure and Economic Development in IndiaDocument9 pagesHealth Infrastructure and Economic Development in IndiaAkanksha PalNo ratings yet
- ISAAL 2020 Literary Contests-Pliant 14Document6 pagesISAAL 2020 Literary Contests-Pliant 14Noli CalderonNo ratings yet
- Kellgren and Lawrence Grading For Osteoartritis RadiographsDocument6 pagesKellgren and Lawrence Grading For Osteoartritis Radiographsnitu73100% (1)
- Procedures RationaleDocument3 pagesProcedures RationaleJamaica Leslie NovenoNo ratings yet
- Discharge InstructionsDocument2 pagesDischarge InstructionsNaneth CadisalNo ratings yet
- Status and Role of AYUSH and Local Health TraditionsDocument352 pagesStatus and Role of AYUSH and Local Health TraditionsSaju_Joseph_9228100% (1)
- Xceed 1 Slide Per PageDocument31 pagesXceed 1 Slide Per Pagemccarthy121677100% (1)
- Criteri 205 JohnesDocument7 pagesCriteri 205 JohnesTeodor ŞişianuNo ratings yet