Professional Documents
Culture Documents
2012 - A Rat Model of Cigarette Smoke Abuse Liability
2012 - A Rat Model of Cigarette Smoke Abuse Liability
Uploaded by
Ana Karen CarneiroOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
2012 - A Rat Model of Cigarette Smoke Abuse Liability
2012 - A Rat Model of Cigarette Smoke Abuse Liability
Uploaded by
Ana Karen CarneiroCopyright:
Available Formats
Comparative Medicine Vol 62, No 5
Copyright 2012 October 2012
by the American Association for Laboratory Animal Science Pages 395–399
Original Research
A Rat Model of Cigarette Smoke Abuse Liability
Petros Ypsilantis,1,* Maria Politou,1 Constantinos Anagnostopoulos,2 Alexandros Kortsaris,2 and Constantinos Simopoulos1
We sought to develop a rat model of cigarette smoke exposure (CSE) that created cotinine serum levels comparable to those
of smokers and induced conditioned place preference (CPP) suggestive of cigarette smoke abuse liability. Rats were exposed to
sidestream cigarette smoke delivered semicontinuously for 2 periods of 20 (group S20), 40 (group S40), or 60 (group S60) min daily
for 12 wk. Serum cotinine concentration in blood samples was determined at 1 and 20 h after CSE. A biased (black versus white
chamber) CPP paradigm was used. In the high CSE group (group S60), serum cotinine at 1 h (250 to 300 ng/mL) was comparable
to average cotinine levels reported for addicted smokers (around 300 ng/mL). Cotinine levels at 20 h after CSE were higher than
the smoker–nonsmoker cut-off value (greater than 14 ng/mL) in all smoking groups, with the S60 group having the highest levels.
All rats preferred the black chamber to the white chamber during the preexposure CPP test. The time spent in the white chamber
was increased compared with 0-wk values in group S40 at 8 wk, group S60 at 4 and 8 wk, and the control group at 4 and 8 wk but
not at 12 wk; however, the shift in CPP was significantly higher at 8 wk in group S60 compared with other groups. In conclusion,
interrupted 2-h daily CSE for 8 wk induced serum cotinine levels in rats comparable to those of smokers and induced CPP sugges-
tive of cigarette smoke abuse liability.
Abbreviations: CPP, conditioned place preference; CSE, cigarette smoke exposure.
The devastating consequences of smoking on health have been its cessation. In toxicity studies, animals are exposed to tobacco
studied extensively in numerous clinical and animal studies over smoke for various periods, which depend on the side effect un-
time. This chronic habit leads to dependence on tobacco smoke, der investigation.18,25,27 Smoke exposure timetables usually do not
with nicotine, a main active ingredient of tobacco products, being involve weekends for practical reasons, and addiction of animals
recognized as the basic addictive substance.32 to tobacco smoke is not assessed in current models.
The known health benefits of smoking cessation motivate In our opinion, an ideal animal model of cigarette smoke abuse
smokers to quit tobacco use. However, unaided efforts usually liability suitable for the study of smoking cessation resembles
are unsuccessful, resulting in smoking relapse. The fight against the clinical situation in terms of chronic daily inhalation of ciga-
nicotine addiction may be undermined by potential weight gain rette smoke sufficient to attain blood nicotine levels compara-
after smoking cessation, potentially discouraging those attempt- ble to those of smokers and in cessation of the CSE period after
ing to quit smoking and contributing to relapse. During the past achieving tobacco smoke abuse liability. In the present project,
few years, research has been focused on 2 main areas of inter- we sought to establish such a model in rats by defining the daily
est toward this direction: understanding the underlying biologic timetable of CSE to induce serum levels of cotinine, nicotine’s
mechanisms related to nicotine addiction to effectively design major proximate metabolite, comparable to those of smokers and
therapeutic strategies to support those who wish to quit smok- by determining the minimum total CSE period required to induce
ing and investigating the hormonal and molecular mechanisms abuse liability to cigarette smoke. We assessed the CSE period by
responsible for weight gain after smoking cessation. using a biased conditioned place preference (CPP) paradigm.8
So far, animal models used to study the consequences of smok-
ing cessation involved the administration of nicotine as a sole
Materials and Methods
agent until addiction was achieved.23 However, nicotine-ad-
Animals. Male Wistar rats (Rattus norvegicus; n = 42; age, 5 to 6
ministration models do not completely represent the toxic and
mo; weight, 380 to 420 g) provided by our laboratory’s inhouse
addictive effects of cigarette smoke, given that smoke contains
breeding colony were used. They were the 20th inbred generation
more than 4000 chemicals whose actions or coactions have not
of Wistar rats obtained from the conventional breeding facility
been thoroughly evaluated yet.1 Cigarette smoke exposure (CSE)
of the Democritos National Center of Physics Research (Athens,
animal models have been used in studies investigating the met-
Greece). Colony health status was monitored semiannually, and
abolic changes conferred by smoking10-12 but not in those after
rats were found to be free of Mycoplasma spp., adventitious virus-
es, respiratory and enteric bacteria, and ecto- and endoparasites.
Received: 20 Feb 2012. Revision requested: 03 Apr 2012. Accepted: 13 May 2012. The rats were housed in polycarbonate cages, 3 rats per cage, at 20
1
Laboratory of Experimental Surgery and Surgical Research and 2Laboratory of
to 22 °C, on a 14:10-h light:dark cycle and were given commercial
Biochemistry, School of Medicine, Democritus University of Thrace, Alexandroupolis,
Greece. pelleted diet (4RF25, Mucedola, Milan, Italy) and tap water ad
*
Corresponding author. Email: pipsil@med.duth.gr libitum. The facilities were in accordance with Directive 86/609/
395
cm12000025.indd 395 10/3/2012 10:55:55 AM
Vol 62, No 5
Comparative Medicine
October 2012
EEC, which refers to “the protection of animals used for experi-
mental and other scientific purposes.”13
Experimental design. We randomly assigned 24 rats to 3 smok-
ing (groups S20, S40, and S60) and a nonsmoking control group
(group C) that consisted of 6 rats each. Rats in the smoking groups
were exposed to interrupted sidestream cigarette smoke for vari-
ous periods on a daily basis for 12 wk. Three rats at a time were
confined in a white smoking chamber for 2 periods of 20 (group
S20), 40 (group S40), or 60 (group S60) min each, with a 60-min
interval between exposures. The color of the chamber was that
of the ‘nonpreferred’ side (white), as defined through a preex-
posure, black compared with white chamber, CPP test. Rats in
the control group were confined on a daily basis in an identical
chamber without smoke for 2 periods of 60 min, with a 60-min
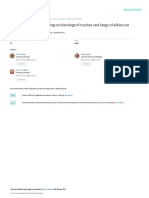
Figure 1. The smoke-exposure system.
interval, for 12 wk. Blood samples were collected around 20 h
after the first smoking session at 0, 5, and 9 wk during the CSE
period, as well as 2 d after the end of the CSE period, to determine side. CPP tests were considered to be biased and were conducted
serum cotinine concentration. Every 4 wk, rats were subjected to in the same manner.
a biased CPP test to assess abuse liability to cigarette smoke. In Determination of serum cotinine concentration. Blood samples
a separate set of smoking control experiments, 3 groups of 6 rats were collected from the tail artery under sevoflurane anesthesia.
each (groups SC20, SC40, SC60) were assigned to 1 wk of CSE Collection of blood samples for cotinine measurement in rats that
exposure as described earlier, and blood samples were collected underwent CSE was performed at 1 h after CSE (that is, 1400).
at 1 h after the last day’s smoking session to determine cotinine Control samples were collected between 0800 and 0900, approxi-
levels. The experimental protocol was approved by the Animal mately 20 h after their last session. Serum was separated by cen-
Care and Ethics Committee of the local Veterinary Service and trifugation at 3000 × g for 20 min and then stored at −70 °C until
was in compliance with Directive 86/609/EEC.13 later analyzed. The concentration of cotinine was determined by
CSE system. The system used to expose rats to sidestream ciga- using a commercially available ELISA kit (Cotinine Direct ELISA,
rette smoke consisted of a ventilator, a smoke-generating cham- BioQuant, San Diego, CA) according to the manufacturer’s in-
ber, and a whole-body CSE chamber that were serially connected structions. The lower limit of detection was 1 ng/mL.
via silicone tubes interlined by Heimlich valves (Becton Dickin- Statistical analysis. Data were analyzed by using SPSS 13.0 sta-
son, Franklin Lakes, NJ) to avoid smoke regression (Figure 1). The tistical software (SPSS, Chicago, IL). Data were expressed as mean
ventilator (Veterinary anesthesia ventilator model 2000, Hallowell ± SE and underwent repeated-measures ANOVA followed by
EMC, Pittsfield, MA) was set to provide 150 mL of air every 10 s. the Student t test for comparisons between 2 groups or the Least
The smoke-generating chamber consisted of an acrylic cylinder Significant Difference test for multiple comparisons. A probabil-
(radius, 8 cm; height, 27 cm) corresponding to 5430 cm3 total vol- ity of less than 5% (P < 0.05) was considered to be statistically
ume into which one cigarette (tar, 8 mg; nicotine, 0.6 mg; carbon significant.
monoxide, 9 mg) at a time was constantly kept lit. Smoke then
was delivered to an acrylic white chamber (length, 40 cm; width, Results
20 cm; height, 25 cm) of 20,000 cm3 total volume and exhausted All rats survived the 12-wk experimental period.
through a hole. The level of carbon monoxide inside the CSE Serum cotinine levels. Serum cotinine levels at 1 h after CSE
chamber was kept between 150 and 250 ppm by transient inter- ranged between 147 and 167 ng/mL (mean ± SE, 160.0 ± 4.1 ng/
ruption, if necessary, of the diluted sidestream smoke delivery. mL) for group SC20, 171 and 221 ng/mL (195.8 ± 11.2 ng/mL) for
The carbon monoxide concentration in air samples collected from group SC40, and 248 and 305 ng/mL (276.5 ± 12.7 ng/mL) for
the chamber interior at 15-min intervals was determined by using group SC60.
a portable carbon monoxide analyzer (piCO Smokerlyzer Breath At 20 h after CSE, serum cotinine concentration in all smoke-
CO monitor, Bedfont Scientific, Kent, UK). Rats were exposed to exposed rats was increased above 14 ng/mL, which is the cut-off
cigarette smoke between 0900 and 1300. value for being defined as a smoker.20 Cotinine concentrations
CPP test. The CPP apparatus consisted of 2 acrylic chambers, a were significantly (P < 0.001) higher in group S60 compared with
black and a white, that were connected by a door (height, 10 cm; groups S20 and S40. Cotinine returned to preexposure levels 2
width, 7 cm). The dimensions of each chamber were the same d after completion of the smoke-exposure period (Figure 2). No
with that of the CSE chamber (length, 40 cm; width, 20 cm; height, changes were noted in the cotinine levels of control rats (data not
25 cm; volume, 20,000 cm3). Each rat was placed individually in shown). Serum cotinine concentration did not differ among time
the apparatus, at the level of the interconnecting door, and the points within each smoke-exposed group, suggesting that the
time the rat spent in each chamber was recorded for a period of CSE setup induced a reliable and reproducible increase in serum
10 min (600 s). The chamber in which the rat spent less than 300 s cotinine.
was designated as the nonpreferred side. CPP. During the preexposure CPP test, all rats preferred the
Before commencement of the CSE period, rats underwent a black over the white chamber (Figure 3 A). The time spent in the
preexposure CPP test to determine their place preference. There- white chamber was significantly increased in group S40 at 8 wk
after, CSE (and control exposure) took place in acrylic chambers (P < 0.05) and group S60 at 4 wk (P < 0.05) and 8 wk (P < 0.001)
identical in color and dimensions as those of the nonpreferred but not at 12 wk of exposure. Similarly, the time control rats spent
396
cm12000025.indd 396 10/3/2012 10:55:55 AM
Cigarette smoke abuse liability model
Figure 2. Mean serum cotinine concentration (n = 6) of rats at 20 h after
daily smoke exposure during the CSE period (0, 1, 5, 9 wk) and at 2 d
after cessation of the CSE period (C2d). Error bars represent standard
errors. Values of 1 ng/mL or less are denoted as 1 ng/mL (minimum
detection limit). The dotted line depicts the 14 ng/mL cut-off limit for
being considered a smoker. CSE, cigarette smoke exposure; *, significant
(P < 0.001) difference between S20 and S40.
in the white chamber was increased at 4 wk (P < 0.01) and 8 wk (P
< 0.05). The white chamber remained the nonpreferred side (time
spent, less than 300 s) in all groups studied (Figure 3 A).
To compare the shift in place preference among groups at each
time point, the relative increase (%) of the initial time spent in the
white chamber was calculated. This percentage was significantly
higher (P < 0.05) in group S60 compared with group S20 and con- Figure 3. (A) Time spent in the white chamber (P values indicate dif-
trol rats after 8 wk of exposure (Figure 3 B). ferences compared with value at 0 wk) and (B) relative shift (%) of the
initial time spent in the white chamber after white compared with black
chamber-biased CPP test of rats exposed to cigarette smoke. Data are
Discussion presented as the mean of 6 rats; error bars represent standard error. The
In the present study, daily exposure of rats to freshly generated dotted line depicts the time limit that characterized place preference.
sidestream cigarette smoke delivered semicontinuously for 120 Total test time, 600 s.
min into a whole-body CSE chamber for an 8-wk period induced
serum cotinine levels comparable to those of addicted smokers people or animals to repeated self-administration of the drug.
and that remained over the smoker–nonsmoker cut-off value The likelihood that the self-administration of a drug will result
throughout the day. The model also led to the development of in persistent use or abuse is associated with its psychoactive or
CPP suggestive of tobacco smoke abuse liability. CNS effects, which can have both positive and negative subjec-
In a cigarette smoke abuse liability animal model, tobacco tive effects; its reinforcing effects; and its ability to induce toler-
smoke inhalation needs to result in serum nicotine levels equiva- ance, craving, and withdrawal-associated effects after repeated
lent to those of smokers. Cotinine has a longer half-life (18 to 20 h) use of the drug.32 A broad range of tests can provide scientifically
than that of nicotine (1 to 2 h)6 and therefore is considered a more validated basis for predicting the likelihood that a drug will be
reliable biomarker for smoking status. In our study, the smok- abused or cause addiction. In the experimental setting, these tests
ing habit was simulated in terms of serum cotinine levels, which include assessment of intravenous self-administration, condi-
were around 250 to 300 ng/mL in the high-CSE rats at 1 h after tioned place preference, and drug discrimination and the mea-
exposure, because these levels are comparable to average blood surement of withdrawal disturbances.22
cotinine concentration reported for addicted smokers (around 300 Abuse liability of animals to cigarette smoke is essential to be
ng/mL).5 Moreover, cotinine concentrations in our rats remained established when addiction-related side effects are to be studied.
above the accepted cut-off limit for being considered a smoker Nicotine is a highly addictive psychoactive substance and can
(14 ng/mL)20 throughout the day, according to measurements in induce enhanced reinforcement, as shown by behavioral tests
blood samples taken 20 h after CSE; data at this time point also in animals, after only 3 d of intraperitoneal,7 7 d of continuous
ensured that rats began subsequent days at a nonzero cotinine subcutaneous,23 or 8 d of intravenous infusion in adult rodents33
concentration. Recent studies in humans have lowered the smok- and after a single subcutaneous injection in early adolescent ro-
er–nonsmoker cut-off point to 3 ng/mL to better discriminate ac- dents.3 Although inhalation of tobacco smoke rapidly elevates
tive smokers from nonsmokers exposed to secondhand smoke.4 blood nicotine levels,26 abuse liability of rats to cigarette smoke,
Abuse liability is the potential that a drug has for addiction. A as suggested by CPP, took considerably more time to be estab-
drug meets criteria for abuse liability if it produces effects medi- lished in the current study compared with the time needed for
ated by the brain sufficient to lead a substantial proportion of nicotine addiction after its infusion as a sole agent, as reported in
397
cm12000025.indd 397 10/3/2012 10:55:56 AM
Vol 62, No 5
Comparative Medicine
October 2012
previous studies.7,23,33 In the current study, the diluted sidestream effects at high or sometimes the same dose.22 The reinforcing ef-
smoke delivery of nicotine and other smoke constituents were fect derived from cigarette smoke inhalation is a complex proce-
sufficient to support the development of CPP in our rat model af- dure, during which the rewarding properties of cigarette smoke
ter 8 wk of CSE. In humans, addiction to nicotine due to cigarette overcome the aversive nature of smoke constituents. A number of
smoking is a progressive procedure, starting with the use of 1 to 2 compounds, including acetaldehyde, act in concert with nicotine
cigarettes daily and followed by a gradual escalation of smoking to potentiate its brain-rewarding function,28,30 whereas others,
frequency. In addition, nicotine overload is known to produce including ammonia, acrolein, and acetone, act as irritant toxins.19
conditioned place or taste aversion.22 Because the rats in the cur- In addition, combustion products are aversive because of eye or
rent study were exposed to cigarette smoke for a standard exten- airway irritation, and repeated nicotine intake may induce toler-
sive daily period from the beginning of the study, they may have ance to its anxiolytic-like effects29 or place aversion due to poten-
experienced nicotine overload that was sufficient to have delayed tial residual anxiogenic effects.8 Furthermore, although repeated
CPP development. Repeated CSE, and therefore nicotine intake, CPP testing enable us to identify the time point with maximal
for 8 wk may then have led to CPP development suggestive of CPP shift, repetition of place conditioning might have affected
abuse liability. In addition, cigarette smoke contains numerous behavioral outcomes.
other compounds, in addition to the well-known addictive agent During the first 8 wk, we also noted an increase in the time that
nicotine,9 whose potential addictive or aversive actions have not control rats spent in the white chamber, which were confined for
yet been investigated thoroughly. 2 h daily to that chamber. This finding suggests an acquaintance
The biased CPP paradigm we used here evaluates the reward- of the animals to the nonpreferred environment after chronic
ing effect of an agent or procedure in terms of an increase in the daily confinement, and this possibility should be considered
time spent in the initially preferred or nonpreferred environment when evaluating addiction by using a biased CPP paradigm. In
(for example, black compared with white chamber) after repeated longitudinal studies involving long-term pairing of a test sub-
pairing with the agent or procedure under investigation. This test stance or procedure with a certain type of environment, one can-
has been previously used to evaluate rewarding effects of nicotine not rule out the possibility that repeated exposure of animals
and other abused agents.7,8,14,21,24 However, the magnitude of the may gradually decrease aversion to, for example, an enclosure
effect of nicotine is generally small and affected by environmen- of a specific color. In addition, diverse ‘natural’ stimuli, includ-
tal stimuli or previous handling history, suggesting its weaker ing food, water, and wheel-running, can condition an increase in
reinforcing effect compared with that of other agents.22 Accord- place preference.2
ing to previous experimental setups, chambers used to evaluate The present experimental protocol involved daily exposure
nicotine-induced CPP differed in both color and floor texture.8,34 of rats to cigarette smoke, whereas this procedure in other rel-
In our study, rats showed a definite preference against the white evant models was interrupted during the weekends for practical
chamber (only a 50- to 150-s stay in the white chamber during a reasons.10,11 Undetectable serum cotinine levels at 2 d after ter-
600-s total test period) during the preexposure CPP test, even in mination of the CSE period confirmed the cessation of CSE and
the absence of a difference in floor texture. Therefore, we presume emphasized the importance of the uninterrupted CSE procedure.
that sufficient time was available for the manifestation of a CPP Although demanding, our time schedule closely resembled the
shift after CSE, especially after having incorporated a biased CPP human smoking habit and excluded the possibility of inducing
procedure by pairing CSE with the less-preferred enclosure. The short-term behavioral or organic effects due to transient cessation
time spent in the nonpreferred white chamber increased after of nicotine intake. Evidence indicates that nicotine withdrawal
8 wk of pairing it daily with 2-h interrupted CSE. According to is followed by behavioral abstinence signs, which appear within
our results, the magnitude of the increase proved to be depen- the first 24 h,23 whereas the hypothalamic expression of orexigenic
dent on the CSE period and subsequently on the dose of addictive neuropeptides increases after only 3 d.17
agents taken in, when compared with shorter exposure periods. In conclusion, we here describe a rat model of chronic CSE that
Accordingly, 4-h daily exposure of rats to tobacco smoke has been induced serum cotinine levels comparable to those of smokers
reported to induce nicotine dependence after 4 wk.28 Several stud- and led to the development of CPP suggestive of cigarette smoke
ies have found a dose-dependent CPP to nicotine-paired environ- abuse liability. This model may be useful in the study of the mech-
ments.8 In addition to the rewarding effect of nicotine in tobacco anism and side effects related to tobacco smoke abuse liability
smoke, the anxiolytic effect of nicotine may have contributed to and smoking cessation.
the development of CPP in our rats. Nicotine alleviates stress,
as shown by a reduction in aversion toward a previously non- References
preferred environment in the CPP procedure31 and according to 1. Ambrose JA, Barua RS. 2004. The pathophysiology of cigarette
results of the social interaction test,16 a fear-conditioning model,29 smoking and cardiovascular disease: an update. J Am Coll Cardiol
and the elevated plus-maze test.15 43:1731–1737.
We collected blood samples from rats after they had been anes- 2. Bardo MT, Bevins RA. 2000. Conditioned place preference: what
thetized briefly with sevoflurane. The remote possibility that does it add to our preclinical understanding of drug reward? Psy-
chopharmacology (Berl) 153:31–43.
sevoflurane anesthesia, even of a short duration (1 to 2 min) and
3. Belluzzi JD, Lee AG, Oliff HS, Leslie FM. 2004. Age-dependent
at such a sparse interval (4 wk), promoted place conditioning effects of nicotine on locomotor activity and conditioned place
due to potential residual effects was counterbalanced by simi- preference in rats. Psychopharmacology (Berl) 174:389–395.
larly anesthetizing control animals before collecting their blood 4. Benowitz NL, Bernert JT, Caraballo RS, Holiday DB, Wang J.
samples. 2009. Optimal serum cotinine levels for distinguishing cigarette
Time spent in the nonpreferred chamber was reduced at the smokers and nonsmokers within different racial/ethnic groups
12th week of CSE. Nicotine has both reinforcing and aversive in the United States between 1999 and 2004. Am J Epidemiol
169:236–248.
398
cm12000025.indd 398 10/3/2012 10:55:56 AM
Cigarette smoke abuse liability model
5. Benowitz NL, Henningfield JE. 1994. Establishing a nicotine thresh- 19. Jaakkola MS, Jaakkola JJ. 1997. Assessment of exposure to environ-
old for addiction. The implications for tobacco regulation. N Engl J mental tobacco smoke. Eur Respir J 10:2384–2397.
Med 331:123–125. 20. Jarvis MJ, Tunstall-Pedoe H, Feyerabend C, Vesey C, Saloojee Y.
6. Benowitz NL, Jacob P 3rd. 1993. Nicotine and cotinine elimination 1987. Comparison of tests used to distinguish smokers from non-
pharmacokinetics in smokers and nonsmokers. Clin Pharmacol Ther smokers. Am J Public Health 77:1435–1438.
53:316–323. 21. Le Foll B, Goldberg SR. 2005. Nicotine induces conditioned place
7. Biala G, Budzynska B. 2006. Reinstatement of nicotine-conditioned preferences over a large range of doses in rats. Psychopharmacology
place preference by drug priming: effects of calcium channel antago- (Berl) 178:481–492.
nists. Eur J Pharmacol 537:85–93. 22. Le Foll B, Goldberg SR. 2009. Effects of nicotine in experimental
8. Brielmaier JM, McDonald CG, Smith RF. 2008. Nicotine place pref- animals and humans: an update on addictive properties. Handb Exp
erence in a biased conditioned place preference design. Pharmacol Pharmacol 192:335–367.
Biochem Behav 89:94–100. 23. Malin DH. 2001. Nicotine dependence: studies with a laboratory
9. Carter LP, Stitzer ML, Henningfield JE, O’Connor RJ, Cummings model. Pharmacol Biochem Behav 70:551-559.
KM, Hatsukami DK. 2009. Abuse liability assessment of tobacco 24. Meehan SM, Schechter MD. 1998. LSD produces conditioned place
products including potential reduced exposure products. Cancer preference in male but not female fawn hooded rats. Pharmacol
Epidemiol Biomarkers Prev 18:3241–3262. Biochem Behav 59:105-108.
10. Chen H, Hansen MJ, Jones JE, Vlahos R, Anderson GP, Morris MJ. 25. Motz GT, Eppert BL, Sun G, Wesselkamper SC, Linke MJ, Deka
2008. Long-term cigarette smoke exposure increases uncoupling pro- R, Borchers MT. 2008. Persistence of lung CD8 T cell oligoclonal
tein expression but reduces energy intake. Brain Res 1228:81-88. expansions upon smoking cessation in a mouse model of cigarette
11. Chen H, Hansen MJ, Jones JE, Vlahos R, Bozinovski S, Anderson smoke-induced emphysema. J Immunol 181:8036–8043.
GP, Morris MJ. 2006. Cigarette smoke exposure reprograms the 26. Rotenberg KS, Miller RP, Adir J. 1980. Pharmacokinetics of
hypothalamic neuropeptide Y axis to promote weight loss. 2006. nicotine in rats after single-cigarette smoke inhalation. J Pharm Sci
Am J Respir Crit Care Med 173:1248–1254. 69:1087–1090.
12. Chen H, Vlahos R, Bozinovski S, Jones J, Anderson GP, Morris MJ. 27. Seagrave J, Barr EB, March TH, Nikula KJ. 2004. Effects of cigarette
2005. Effect of short-term cigarette smoke exposure on body weight, smoke exposure and cessation on inflammatory cells and matrix
appetite, and brain neuropeptide Y in mice. Neuropsychopharmacol- metalloproteinase activity in mice. Exp Lung Res 30:1–15.
ogy 30:713–719. 28. Small E, Shah HP, Davenport JJ, Geier JE, Yavarovich KR, Yamada
13. Council of the European Communities. 1986. Council Directive H, Sabarinath SN, Derendorf H, Pauly JR, Gold MS, Bruijnzeel
86/609/EEC of 24 November 1986 on the approximation of laws, AW. 2010. Tobacco smoke exposure induces nicotine dependence in
regulations, and administrative provisions of the Member States rats. Psychopharmacology (Berl) 208:143–158.
regarding the protection of animals used for experimental and other 29. Szyndler J, Sienkiewicz-Jarosz H, Maciejak P, Siemiatowski M,
scientific purposes. Off J Eur Communities L358:1–28 Rokicki D, Czlonkowska AI, Płaznik A. 2001. The anxiolytic-like
14. Davis CM, Roma PG, Dominguez JM, Riley AL. 2007. Morphine- effect of nicotine undergoes rapid tolerance in a model of contextual
induced place conditioning in Fischer and Lewis rats: acquisition fear conditioning in rats. Pharmacol Biochem Behav 69:511–518.
and dose–response in a fully biased procedure. Pharmacol Biochem 30. Talhout R, Opperhuizen A, van Amsterdam JG. 2007. Role of acet-
Behav 86:516-523. aldehyde in tobacco smoke addiction. Eur Neuropsychopharmacol
15. Elliott BM, Faraday MM, Phillips JM, Grunberg NE. 2004. Effects of 17:627–636.
nicotine on elevated plus maze and locomotor activity in male and fe- 31. Torrella TA, Badanich KA, Philpot RM, Kirstein CL, Wecker L.
male adolescent and adult rats. Pharmacol Biochem Behav 77:21–28. 2004. Developmental differences in nicotine place conditioning. Ann
16. File SE, Kenny PJ, Ougazzal AM. 1998. Bimodal modulation by N Y Acad Sci 1021:399–403.
nicotine of anxiety in the social interaction test: role of the dorsal 32. US Department of Health and Human Services. 1988. The health
hippocampus. Behav Neurosci 112:1423–1429. consequences of smoking: nicotine addiction. A report of the Surgeon
17. Fornari A, Pedrazzi P, Lippi G, Picciotto MR, Zoli M, Zini I. 2007. General. Rockville (MD): Center for Health Promotion and Educa-
Nicotine withdrawal increases body weight, neuropeptide Y, and tion.
Agouti-related protein expression in the hypothalamus and de- 33. Wilkinson JL, Bevins RA. 2008. Intravenous nicotine conditions
creases uncoupling protein-3 expression in the brown adipose tissue a place preference in rats using an unbiased design. Pharmacol
in high-fat-fed mice. Neurosci Lett 411:72–76. Biochem Behav 88:256–264.
18. Fusby JS, Kassmeier MD, Palmer VL, Perry GA, Anderson DK, 34. Yamada H, Bishnoi M, Keijzers KF, van Tuijl IA, Small E, Shah
Hackfort BT, Alvarez GK, Cullen DM, Akhter MP, Swanson PC. HP, Bauzo RM, Kobeissy FH, Sabarinath SN, Derendorf H,
2010. Cigarette smoke-induced effects on bone marrow B-cell subsets Bruijnzeel AW. 2010. Preadolescent tobacco smoke exposure leads
and CD4+:CD8+ T-cell ratios are reversed by smoking cessation: to acute nicotine dependence but does not affect the rewarding effects
influence of bone mass on immune cell response to and recovery of nicotine or nicotine withdrawal in adulthood in rats. Pharmacol
from smoke exposure. Inhal Toxicol 22:785-796. Biochem Behav 95:401–409.
399
cm12000025.indd 399 10/3/2012 10:55:56 AM
You might also like
- Essentials of Abnormal Psychology 5th Canadian Edition Jeffrey SNevidDocument577 pagesEssentials of Abnormal Psychology 5th Canadian Edition Jeffrey SNevidQin Joey100% (3)
- Get Through MRCPsych Paper A1 MockDocument570 pagesGet Through MRCPsych Paper A1 MockFirdaus RafiNo ratings yet
- The Other Side of Eden - Life With John - SteinbeckDocument304 pagesThe Other Side of Eden - Life With John - SteinbeckFacundo Baró100% (3)
- What I Never Told You by Titus NdirituDocument102 pagesWhat I Never Told You by Titus NdirituLawrence Wawire100% (2)
- Reaction Paper MT Q1 Taghoynsa DilimDocument1 pageReaction Paper MT Q1 Taghoynsa DilimJuneth Billones100% (2)
- The Dog As A Passive Smoker: Effects of Exposure To Environmental Cigarette Smoke On Domestic DogsDocument6 pagesThe Dog As A Passive Smoker: Effects of Exposure To Environmental Cigarette Smoke On Domestic DogsBrandoNo ratings yet
- BCH413 2019-20 Harmattan 2Document11 pagesBCH413 2019-20 Harmattan 2idriscognitoleadsNo ratings yet
- Imid NocicepDocument13 pagesImid NocicepnikuNo ratings yet
- Toxicological Screening: Educational ForumDocument6 pagesToxicological Screening: Educational ForumeyobNo ratings yet
- Toxicology For The Twenty-First CenturyDocument5 pagesToxicology For The Twenty-First CenturymjkoNo ratings yet
- Jaalas 2022000181Document7 pagesJaalas 2022000181Harshad BargajeNo ratings yet
- What Can Radio Isotopes Do For Man?: Medicine and BiologyDocument10 pagesWhat Can Radio Isotopes Do For Man?: Medicine and Biologyvasukimp572No ratings yet
- Assessment of Antidiabetic Effect of 4-HIL in Type 2 Diabetic and Healthy Sprague Dawley RatsDocument11 pagesAssessment of Antidiabetic Effect of 4-HIL in Type 2 Diabetic and Healthy Sprague Dawley RatsMaxin BangsalNo ratings yet
- Efficacy of Hydroxocobalamin for the Treatment of Acute Cyanide Poisoning in Adult Beagle DogsDocument13 pagesEfficacy of Hydroxocobalamin for the Treatment of Acute Cyanide Poisoning in Adult Beagle DogsLaurent GouardoNo ratings yet
- The Total of Leukocytes Mice (Mus Musculus) Exposed To Secondhand Smoke Extract and Given Watermelon (Citrullus Vulgaris)Document5 pagesThe Total of Leukocytes Mice (Mus Musculus) Exposed To Secondhand Smoke Extract and Given Watermelon (Citrullus Vulgaris)tiaraNo ratings yet
- Electronic Nicotine Delivery SystemsDocument15 pagesElectronic Nicotine Delivery SystemsBrent StaffordNo ratings yet
- The Relative Risk of Cancer From Smoking and Vaping NicotineDocument25 pagesThe Relative Risk of Cancer From Smoking and Vaping Nicotineyfzsc5g7nmNo ratings yet
- Analytical Chemistry ReviewerDocument4 pagesAnalytical Chemistry ReviewerPrincess Aleia SalvadorNo ratings yet
- Cannabis y Convulsión en PerrosDocument18 pagesCannabis y Convulsión en PerrosAndres RodriguezNo ratings yet
- 196 202Document8 pages196 202waee0565No ratings yet
- Archeal PAHDocument4 pagesArcheal PAHukilabosNo ratings yet
- 4.3, 4.4, 4.5 Radiation Measurement HL MAppDocument15 pages4.3, 4.4, 4.5 Radiation Measurement HL MAppIvy Joyce BuanNo ratings yet
- 1966 MMR 3Document4 pages1966 MMR 3isomeraseNo ratings yet
- Acute Subacute ChronicDocument59 pagesAcute Subacute Chronicaziskf100% (1)
- Effect of Cigarette Smoke On Spermatogenesis in Rats: Sexual Dysfunction and InfertilityDocument5 pagesEffect of Cigarette Smoke On Spermatogenesis in Rats: Sexual Dysfunction and InfertilityAhmad AnzariNo ratings yet
- Animals Chapter 9 Animal Use in Toxicity StudiesDocument15 pagesAnimals Chapter 9 Animal Use in Toxicity StudiesAshishNo ratings yet
- Research: Human Pathogens Abundant in The Bacterial Metagenome of CigarettesDocument7 pagesResearch: Human Pathogens Abundant in The Bacterial Metagenome of Cigarettes1eenahaNo ratings yet
- His To MetricDocument20 pagesHis To MetricEva Indreswari TandisallaNo ratings yet
- Serum Organochlorine Pesticides Residues and Risk - 2018 - Saudi Journal of BiolDocument7 pagesSerum Organochlorine Pesticides Residues and Risk - 2018 - Saudi Journal of BiolErick Dario P ChNo ratings yet
- Changes of Ghrelin and Leptin Levels in Plasma by Cigarette Smoke in RatsDocument8 pagesChanges of Ghrelin and Leptin Levels in Plasma by Cigarette Smoke in RatsramadanNo ratings yet
- Pesticidas en LarvasDocument9 pagesPesticidas en LarvasCAROLNo ratings yet
- Review JurnalDocument6 pagesReview JurnalNavida SeftianaNo ratings yet
- IC 50 Bixin 72,21 PPMDocument10 pagesIC 50 Bixin 72,21 PPMANNISANo ratings yet
- Why Short-Term Bioassays Are Not Meaningful-Effects of A Pesticide (Imidacloprid) and A Metal (Cadmium) On Pea Aphids (Acyrthosiphon Pisum Harris)Document8 pagesWhy Short-Term Bioassays Are Not Meaningful-Effects of A Pesticide (Imidacloprid) and A Metal (Cadmium) On Pea Aphids (Acyrthosiphon Pisum Harris)ArtemNo ratings yet
- Oxidative Damage Induced by Cigarette Sm-1Document10 pagesOxidative Damage Induced by Cigarette Sm-1Crys CaladoNo ratings yet
- Toxicology ReportsDocument7 pagesToxicology ReportsValeskaSenaNo ratings yet
- Anesthesia of C57BL6 MiceDocument3 pagesAnesthesia of C57BL6 MiceJoaquin Rojas FritzNo ratings yet
- Animal Toxicological StudiesDocument40 pagesAnimal Toxicological StudiesDeepika RaoNo ratings yet
- Effects of Cigarette Smoking On HistologDocument8 pagesEffects of Cigarette Smoking On HistologErisca AyuNo ratings yet
- Acute Toxicity of 31 Different Nanoparticles To Zebrafish Danio Rerio Tested in Adulthood and in Early Life Stages Comparative StudyDocument7 pagesAcute Toxicity of 31 Different Nanoparticles To Zebrafish Danio Rerio Tested in Adulthood and in Early Life Stages Comparative StudyMaruf MuhammadNo ratings yet
- Huclier-Markai - DOTA Labeling of Sc-44 - 2014Document8 pagesHuclier-Markai - DOTA Labeling of Sc-44 - 2014PAULINA MUNGUIANo ratings yet
- Toxicology ReportsDocument8 pagesToxicology ReportsImam HasanNo ratings yet
- (24508608 - Journal of Veterinary Research) Metaldehyde Poisoning of Companion Animals - A Three-Year Retrospective StudyDocument5 pages(24508608 - Journal of Veterinary Research) Metaldehyde Poisoning of Companion Animals - A Three-Year Retrospective StudySara Estefania Arango VasquezNo ratings yet
- 58db3199b6c51 PDFDocument6 pages58db3199b6c51 PDFNaeem AkhtarNo ratings yet
- 1 s2.0 S0753332223004298 MainDocument10 pages1 s2.0 S0753332223004298 MaingrcardossNo ratings yet
- Ratiometric Emission Fluorescent pH Probe for Imaging of Living Cells in Extreme AcidityDocument6 pagesRatiometric Emission Fluorescent pH Probe for Imaging of Living Cells in Extreme AcidityCalford ChanNo ratings yet
- Chapter 1 MJDocument14 pagesChapter 1 MJMidman LegitNo ratings yet
- Risk Assessment of Triclosan, A Cosmetic Preservative: Invited ReviewDocument18 pagesRisk Assessment of Triclosan, A Cosmetic Preservative: Invited ReviewMaja TastanoskaNo ratings yet
- 1 s2.0 S1570023222001064 MainDocument8 pages1 s2.0 S1570023222001064 MainFithriana RachmawatiNo ratings yet
- 1 s2.0 S0300483X23002706 MainDocument12 pages1 s2.0 S0300483X23002706 MainprunaldijayaNo ratings yet
- Tobaccocontrol 2013 051469Document6 pagesTobaccocontrol 2013 051469Indhira JarnuzylovaNo ratings yet
- 86 - 2024 - TCP - Zervas Et Al - Particle Emissions From Heated Tobacco ProductsDocument9 pages86 - 2024 - TCP - Zervas Et Al - Particle Emissions From Heated Tobacco ProductsmnlkpoNo ratings yet
- Influence of Washing Hands and Using Gloves During Hygienic OperationsInvolving Acupuncture NeedlesDocument2 pagesInfluence of Washing Hands and Using Gloves During Hygienic OperationsInvolving Acupuncture NeedlesBruna MoraesNo ratings yet
- Art 01Document12 pagesArt 01Cristian-Catalin GavatNo ratings yet
- Ikonomidis Et Al 2018 Electronic Cigarette Smoking Increases Arterial Stiffness and Oxidative Stress To A Lesser ExtentDocument4 pagesIkonomidis Et Al 2018 Electronic Cigarette Smoking Increases Arterial Stiffness and Oxidative Stress To A Lesser Extentvip.kirill.novikov.2001No ratings yet
- Referensi Elabscience T2Document12 pagesReferensi Elabscience T2Nandia SeptiyoriniNo ratings yet
- Artigo Samuel ValençaDocument5 pagesArtigo Samuel ValençaKleber DennisNo ratings yet
- Acute Toxicity Test of Pigeon Pea Leaves Extract (CajanusDocument4 pagesAcute Toxicity Test of Pigeon Pea Leaves Extract (CajanusEva AndariNo ratings yet
- Vansickel 2010 E-Cigarettes ClinicalDocument9 pagesVansickel 2010 E-Cigarettes ClinicalSam MunroNo ratings yet
- Articulo 2 2018Document15 pagesArticulo 2 2018Gabriela Hernández OrtizNo ratings yet
- Cyanide PoisoningDocument5 pagesCyanide Poisoningriz04_fortitudessa5178No ratings yet
- Carneiro Et Al 2014Document8 pagesCarneiro Et Al 2014LuizaNo ratings yet
- The Toxicity of Caffein: An experimental study on different species of animalsFrom EverandThe Toxicity of Caffein: An experimental study on different species of animalsNo ratings yet
- Zebrafish: Methods for Assessing Drug Safety and ToxicityFrom EverandZebrafish: Methods for Assessing Drug Safety and ToxicityPatricia McGrathNo ratings yet
- Literature Review Substance Abuse TreatmentDocument8 pagesLiterature Review Substance Abuse Treatmentafdtorpqk100% (1)
- 1final Drugs ThesisDocument36 pages1final Drugs ThesisEmmalyn DayagNo ratings yet
- Assessing and Treating Patients With Impulsivity, Compulsivity, and AddictionDocument8 pagesAssessing and Treating Patients With Impulsivity, Compulsivity, and AddictionAmber FatimaNo ratings yet
- DB01 Drug ClassificationDocument20 pagesDB01 Drug ClassificationMayank TewatiaNo ratings yet
- Ceramah 2 - Pengetahuan Dan Penilaian Ketagihan Merokok - DR LianaDocument29 pagesCeramah 2 - Pengetahuan Dan Penilaian Ketagihan Merokok - DR LianaMohd Zakaria Mohd YusaffNo ratings yet
- Aa Homework AssignmentsDocument8 pagesAa Homework Assignmentsh44f4068100% (1)
- Substance Use and Abuse Among AdolescentsDocument9 pagesSubstance Use and Abuse Among Adolescentssakshi agarwalNo ratings yet
- Problems Encountered by Police Personnel in Conducting DrugDocument5 pagesProblems Encountered by Police Personnel in Conducting DrugRanie MonteclaroNo ratings yet
- Drug Addiction: Biology Investigatory ProjectDocument18 pagesDrug Addiction: Biology Investigatory ProjectOmkar GhatageNo ratings yet
- Drug Awareness and PreventionDocument3 pagesDrug Awareness and PreventionRosielyn ParelNo ratings yet
- Cannabis EffectsDocument5 pagesCannabis EffectsIdarmis TorresNo ratings yet
- Drugs Abuse Among Youth in Maiduguri, Borno State, NigeriaDocument13 pagesDrugs Abuse Among Youth in Maiduguri, Borno State, NigeriaInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Adolescent Problems: Submitted By, Maria T M B.Ed, Natural ScienceDocument19 pagesAdolescent Problems: Submitted By, Maria T M B.Ed, Natural ScienceMaria T MNo ratings yet
- Mephentermine Abuse For Stamina, Resulting in Mania - A Case ReportDocument4 pagesMephentermine Abuse For Stamina, Resulting in Mania - A Case Reportgaurav sharmaNo ratings yet
- Psychoactive Drugs and Harm Reduction: From Faith To ScienceDocument5 pagesPsychoactive Drugs and Harm Reduction: From Faith To ScienceMel LissaNo ratings yet
- Amino Acid Therapy ChartDocument1 pageAmino Acid Therapy Chartdragonfly19722018No ratings yet
- NSTP ReviewerDocument4 pagesNSTP ReviewerDivine Samson CabanizasNo ratings yet
- Social Media Addiction and Empathy Moderating Impact of - 2021 - Telematics andDocument15 pagesSocial Media Addiction and Empathy Moderating Impact of - 2021 - Telematics andasia.calzavaraNo ratings yet
- XVFDocument16 pagesXVFJoaquín OlivaresNo ratings yet
- 2023-11 - Fentanyl Precursor Submission CDPCDocument12 pages2023-11 - Fentanyl Precursor Submission CDPCCDPCNo ratings yet
- Mapeh 4 (Health 4) : Third QuarterDocument22 pagesMapeh 4 (Health 4) : Third QuarterAaron Manuel MunarNo ratings yet
- The Matrix Model in Outpatiens Substances AbuseDocument9 pagesThe Matrix Model in Outpatiens Substances AbuseEduardo Garza GarzaNo ratings yet
- TEST 11th Grade - Compulsive ShoppingDocument3 pagesTEST 11th Grade - Compulsive Shoppingvalentina-serebreanuyandex.ruNo ratings yet
- Drug and Alcohol Awareness-Employee TrainingDocument59 pagesDrug and Alcohol Awareness-Employee TrainingRaymond M. LacsonNo ratings yet
- The Effect of Housing and Gender On Preference For Morphine-Sucrose Solutions in RatsDocument5 pagesThe Effect of Housing and Gender On Preference For Morphine-Sucrose Solutions in RatsqweqweqweqwzaaaNo ratings yet