Professional Documents
Culture Documents
Caz Patologie
Caz Patologie
Uploaded by
Barbulescu Anca DianaCopyright:
Available Formats
You might also like
- Arts and Design - Q1 - Mod2 - ArtistryRelatedInjuries - Version1 by Romel SabidorDocument26 pagesArts and Design - Q1 - Mod2 - ArtistryRelatedInjuries - Version1 by Romel SabidorJayson Paul Dalisay Datinguinoo100% (2)
- Necrotizing Sialometaplasia of The Palate: A Case Report: Ashwarya Trivedi, Mysore K Sunil, Sonam Gupta, Shaveta GargDocument4 pagesNecrotizing Sialometaplasia of The Palate: A Case Report: Ashwarya Trivedi, Mysore K Sunil, Sonam Gupta, Shaveta Gargandrianiputri916No ratings yet
- Granuloma ArticleDocument3 pagesGranuloma ArticleRamanpreet KourNo ratings yet
- Acharya 2011Document4 pagesAcharya 2011andreia ichimNo ratings yet
- Lobular Capillary Hemangioma of TongueDocument3 pagesLobular Capillary Hemangioma of TongueShreya DasguptaNo ratings yet
- Pyogenic GranulomaDocument13 pagesPyogenic GranulomaPiyusha SharmaNo ratings yet
- Journal Occlusal 2Document4 pagesJournal Occlusal 2Felianda ThaliaNo ratings yet
- Unusual Large and Abiding Fibroepithelial Polyp in Oral Cavity: A Case ReportDocument4 pagesUnusual Large and Abiding Fibroepithelial Polyp in Oral Cavity: A Case ReportmuharrimahNo ratings yet
- Gingival Epulis: Report of Two Cases.: Dr. Praful Choudhari, Dr. Praneeta KambleDocument5 pagesGingival Epulis: Report of Two Cases.: Dr. Praful Choudhari, Dr. Praneeta KambleAnandNo ratings yet
- Dental Journal: Peripheral Ossifying Fibroma of The Anterior Maxillary GingivaDocument5 pagesDental Journal: Peripheral Ossifying Fibroma of The Anterior Maxillary Gingivaanugraha GanendraNo ratings yet
- Peripheral Giant Cell Granuloma - A Case ReportDocument4 pagesPeripheral Giant Cell Granuloma - A Case ReportAziz IkbalNo ratings yet
- V 7 Aop 191Document3 pagesV 7 Aop 191Sekar EkaperdanaNo ratings yet
- October 2018 1538385165 481 PDFDocument4 pagesOctober 2018 1538385165 481 PDFKiyRizkikaNo ratings yet
- Clinical: Idiopathic Gingival Fibromatosis Associated With Generalized Aggressive Periodontitis: A Case ReportDocument5 pagesClinical: Idiopathic Gingival Fibromatosis Associated With Generalized Aggressive Periodontitis: A Case Reportchakriy9No ratings yet
- Gingival Abscess Case ReportDocument4 pagesGingival Abscess Case ReportKrishan GuliaNo ratings yet
- Management of Necrotizing Ulcerative Gingivitis in A Pregnant Patient - A Rare Case ReportDocument6 pagesManagement of Necrotizing Ulcerative Gingivitis in A Pregnant Patient - A Rare Case ReportAZWAN RAHMADHAN PUTRANo ratings yet
- 243 674 1 PB PDFDocument2 pages243 674 1 PB PDFsurgaNo ratings yet
- InflammatoryGingivalEnlargement ACaseReport PDFDocument5 pagesInflammatoryGingivalEnlargement ACaseReport PDFMardianiPutriPutriNo ratings yet
- Pyogenic GranulomaDocument6 pagesPyogenic GranulomaRini TiaraNo ratings yet
- 63 - CASE REPORT Epulis GranulomaDocument3 pages63 - CASE REPORT Epulis GranulomaRina NovitrianiNo ratings yet
- A Parulis-Like Soft Tissue Tumor in Relation With A Dental Implant: Case ReportDocument3 pagesA Parulis-Like Soft Tissue Tumor in Relation With A Dental Implant: Case ReportDr. AtheerNo ratings yet
- Periapical GranulomaDocument3 pagesPeriapical GranulomaLina BurduhNo ratings yet
- Giant Cell Epulis: Report of 2 Cases.: Oral PathologyDocument11 pagesGiant Cell Epulis: Report of 2 Cases.: Oral PathologyVheen Dee DeeNo ratings yet
- 8978 22741 1 SMDocument3 pages8978 22741 1 SMDhita AndanaNo ratings yet
- Gingival Squamous Cell Carcinoma Presenting As Periodontal Lesion in The Mandibular Posterior RegionDocument4 pagesGingival Squamous Cell Carcinoma Presenting As Periodontal Lesion in The Mandibular Posterior RegionThái BìnhNo ratings yet
- Plasma Cell Gingivitis With Aggressive Periodontitis: A Rare Presentation of An Uncommon ConditionDocument4 pagesPlasma Cell Gingivitis With Aggressive Periodontitis: A Rare Presentation of An Uncommon Conditionratih agridithaNo ratings yet
- Peripheral Ossifying Fi Broma: ASE EportDocument4 pagesPeripheral Ossifying Fi Broma: ASE Eporterr3sNo ratings yet
- Artículo de Periodoncia 2Document7 pagesArtículo de Periodoncia 2Margareth Roxanna Mendieta GirónNo ratings yet
- 7 CR 2 ArjunDocument4 pages7 CR 2 Arjunkiara wardanaNo ratings yet
- 3 RdarticleDocument5 pages3 RdarticleAmira Pradsnya ParamitaNo ratings yet
- Bi Bi: Fibrous Epulis - Case ReportDocument6 pagesBi Bi: Fibrous Epulis - Case Reportemmanuellagrace06No ratings yet
- Fibrous Hyperplasia A Case ReportDocument4 pagesFibrous Hyperplasia A Case ReportBramita Beta ArnandaNo ratings yet
- Dentj 38 2 02Document4 pagesDentj 38 2 02Alfonsius JeriNo ratings yet
- Periapical Granuloma Associated With Extracted Teeth: Original ArticleDocument4 pagesPeriapical Granuloma Associated With Extracted Teeth: Original ArticleDinar Sukma PamungkasNo ratings yet
- Pyogenic Granuloma A Case ReportDocument9 pagesPyogenic Granuloma A Case ReportSafira HlwNo ratings yet
- Granuloma Pyogenicum - A Case ReportDocument4 pagesGranuloma Pyogenicum - A Case ReportInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Radicular Cyst With Primary Mandibular Molar A RarDocument5 pagesRadicular Cyst With Primary Mandibular Molar A RargarciadeluisaNo ratings yet
- Case Report Necrotizing Ulcerative Gingivitis, A Rare Manifestation As A Sequel of Drug-Induced Gingival Overgrowth: A Case ReportDocument7 pagesCase Report Necrotizing Ulcerative Gingivitis, A Rare Manifestation As A Sequel of Drug-Induced Gingival Overgrowth: A Case ReportPutri Dwi AnggrainiNo ratings yet
- Focal Reactive OvergrowthsDocument5 pagesFocal Reactive OvergrowthsLjubomirErdoglijaNo ratings yet
- Periapical GranulomaDocument6 pagesPeriapical GranulomaEzza RiezaNo ratings yet
- Post Covid 19 Mucoromycosis of MandibleDocument5 pagesPost Covid 19 Mucoromycosis of MandibleDr Yamuna RaniNo ratings yet
- Management of Chronic Gingivitis PDFDocument5 pagesManagement of Chronic Gingivitis PDFliaamNo ratings yet
- 2017 FrogDocument4 pages2017 FrogUma DatarNo ratings yet
- 10866-Article Text-52118-1-10-20220425Document10 pages10866-Article Text-52118-1-10-20220425Trianita DivaNo ratings yet
- Jurnal Porio 1Document3 pagesJurnal Porio 1Neo YustindraNo ratings yet
- Lobular Capillary Hemangioma An Extremely Rare Entity in The Retromolar Region Case ReportDocument5 pagesLobular Capillary Hemangioma An Extremely Rare Entity in The Retromolar Region Case ReportInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Palatal SwellingsDocument6 pagesPalatal Swellingsopi akbarNo ratings yet
- Case Report Endo Perio Lesions-A Synergistic ApproachDocument5 pagesCase Report Endo Perio Lesions-A Synergistic ApproachRyanka Dizayani PutraNo ratings yet
- Jomp039-01-07 2Document5 pagesJomp039-01-07 2azkaziyan14No ratings yet
- Irritational Fibroma A Case ReportDocument2 pagesIrritational Fibroma A Case ReportquikhaaNo ratings yet
- Torus InglesDocument5 pagesTorus InglespaolaNo ratings yet
- Ijcpd 12 68Document5 pagesIjcpd 12 68lily oktarizaNo ratings yet
- GINGIVEKTOMIDocument6 pagesGINGIVEKTOMIAstrid ChrisanditaNo ratings yet
- Chronic Inflammatory Gingival Enlargement: A CaseDocument3 pagesChronic Inflammatory Gingival Enlargement: A CaseArida Khoiruza Asy'ariNo ratings yet
- DR Bhaumik Nanavati Proof ApprovedDocument6 pagesDR Bhaumik Nanavati Proof ApprovedFahmi FirmansyahNo ratings yet
- Dental Implant Therapy in A Patient With Acromegaly: A Clinical ReportDocument6 pagesDental Implant Therapy in A Patient With Acromegaly: A Clinical ReportAkanksha MahajanNo ratings yet
- Pulpitis JurnalDocument2 pagesPulpitis JurnalIsmail YusufNo ratings yet
- Pemphigus Vulgaris Confined To The Gingiva: A Case ReportDocument16 pagesPemphigus Vulgaris Confined To The Gingiva: A Case ReportAlmasulah Al-akmaliyahNo ratings yet
- Berglundh Et Al (2018) - Peri Implant Diseases and Conditions - Consensus Report of Workgroup 4 - 1Document9 pagesBerglundh Et Al (2018) - Peri Implant Diseases and Conditions - Consensus Report of Workgroup 4 - 1FelipeOyarceSalazarNo ratings yet
- Peri-Implant Complications: A Clinical Guide to Diagnosis and TreatmentFrom EverandPeri-Implant Complications: A Clinical Guide to Diagnosis and TreatmentNo ratings yet
- Amelogenesis Imperfecta: Case Study: Operative Dentistry September 2017Document14 pagesAmelogenesis Imperfecta: Case Study: Operative Dentistry September 2017Barbulescu Anca DianaNo ratings yet
- Rampant Caries in Adolescence: December 2019Document4 pagesRampant Caries in Adolescence: December 2019Barbulescu Anca DianaNo ratings yet
- Direct Laminate Veneers With Resin Composites: Two Case Reports With Five-Year Follow-UpsDocument3 pagesDirect Laminate Veneers With Resin Composites: Two Case Reports With Five-Year Follow-UpsBarbulescu Anca DianaNo ratings yet
- Partial Edentulism : Exploring Partial Edentulism Patterns in Mandibular Arch Among Patients of KarachiDocument5 pagesPartial Edentulism : Exploring Partial Edentulism Patterns in Mandibular Arch Among Patients of KarachiBarbulescu Anca DianaNo ratings yet
- Post-Operative Complications PresentationDocument37 pagesPost-Operative Complications PresentationChrisNeop0% (1)
- Radlink Issue 1 2008Document8 pagesRadlink Issue 1 2008RadlinkSingaporeNo ratings yet
- Depression: by Aroosha Abdul RasheedDocument9 pagesDepression: by Aroosha Abdul RasheedArushar 24No ratings yet
- 1h. Chapter-1-Introduction To First Aid-HighlightedDocument25 pages1h. Chapter-1-Introduction To First Aid-HighlightedMohamed BinNo ratings yet
- Stroke Hemoragik: Yusi Rizky N 1 6 1 0 2 1 1 0 5 1Document19 pagesStroke Hemoragik: Yusi Rizky N 1 6 1 0 2 1 1 0 5 1Yusi RizkyNo ratings yet
- Tarea 2 de Ingles 2Document6 pagesTarea 2 de Ingles 2Rosa RamosNo ratings yet
- Delta VariantDocument1 pageDelta VariantKurt Alec Richmond SALANGUITNo ratings yet
- Transfusion Reaction PDFDocument1 pageTransfusion Reaction PDFKah Man GohNo ratings yet
- Gastrointestinal SystemDocument218 pagesGastrointestinal Systemnursereview92% (12)
- DR Nazri - Covid-19 (CME) PDFDocument46 pagesDR Nazri - Covid-19 (CME) PDFKok Hui DiongNo ratings yet
- Optic Disc CuppingDocument14 pagesOptic Disc CuppingAsri Kartika AnggraeniNo ratings yet
- Differential Diagnosis of Low Back Pain: Elizabeth Huntoon, MD, and Marc Huntoon, MDDocument7 pagesDifferential Diagnosis of Low Back Pain: Elizabeth Huntoon, MD, and Marc Huntoon, MDGangsar DamaiNo ratings yet
- LidocaineDocument2 pagesLidocaineLeigh Marie LastimosaNo ratings yet
- Statistical TreatmentDocument9 pagesStatistical TreatmentCiv NortubNo ratings yet
- Heart Failure Treatment Algorithm: Diagnosis and ClassificationDocument7 pagesHeart Failure Treatment Algorithm: Diagnosis and ClassificationLorreine Elisa FaruqNo ratings yet
- Medicare Inpatient 2017Document8,939 pagesMedicare Inpatient 2017Shashi Shirke100% (1)
- Ineffective Breathing Pattern - NCPDocument2 pagesIneffective Breathing Pattern - NCPHsintan HsuNo ratings yet
- Sexually Transmitted Diseases HEALTH TEACHING 1 Copy 1Document41 pagesSexually Transmitted Diseases HEALTH TEACHING 1 Copy 1Pauline FabiañaNo ratings yet
- Physical & Multiple Disability ChecklistDocument3 pagesPhysical & Multiple Disability ChecklistGheylhu AmorNo ratings yet
- IMNCIDocument84 pagesIMNCIAyenew100% (1)
- Neoplastic Proliferation of White Blood CellDocument35 pagesNeoplastic Proliferation of White Blood Cellnighat khanNo ratings yet
- Infective EndocarditisDocument58 pagesInfective EndocarditisTok KeawkaewNo ratings yet
- Examination of Cerebellum and MeningesDocument4 pagesExamination of Cerebellum and MeningesAngelaTrinidadNo ratings yet
- 4th Quarter Summative Test Mapeh 7Document3 pages4th Quarter Summative Test Mapeh 7Theness BonjocNo ratings yet
- Perioperative Management of AdrenalectomyDocument13 pagesPerioperative Management of AdrenalectomyTJ LapuzNo ratings yet
- Massive HemorrhageDocument17 pagesMassive HemorrhageShannen Madrid Tindugan100% (1)
- NVHR - 211045 - 090821 - Mask Mandate Flyer - v1.1 - FDocument1 pageNVHR - 211045 - 090821 - Mask Mandate Flyer - v1.1 - FFOX5 VegasNo ratings yet
- Dictionary of Pharmaceutical Dosage FormsDocument169 pagesDictionary of Pharmaceutical Dosage FormsNguyễn Trần LinhNo ratings yet
- Drug Study AmlodipineDocument3 pagesDrug Study AmlodipineKristine ChampnessNo ratings yet
Caz Patologie
Caz Patologie
Uploaded by
Barbulescu Anca DianaOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Caz Patologie
Caz Patologie
Uploaded by
Barbulescu Anca DianaCopyright:
Available Formats
Published online: 2019-04-26
THIEME
46 Case Report
A Case Report: Aggressive Pyogenic Granuloma
Dipanshu Kumar1 Tanya Agarwal2
1 Department of Pedodontics & Preventive Dentistry, Inderprastha Address for correspondence Tanya Agarwal, Department of
Dental College and Hospital, Ghaziabad, Uttar Pradesh, India pedodontics & preventive dentistry, Institute of Dental Studies and
2Department of Pedodontics & Preventive Dentistry, Institute of Dental Technologies, Kadrabad, Modinagar, Uttar Pradesh 201204, India
Studies and Technologies, Kadrabad, Modinagar, Uttar Pradesh, India (e-mail: tanyapedo@gmail.com).
Dent J Adv Stud 2019;7:46–50
Abstract Soft-tissue growths of the oral cavity offer a diagnostic dilemma because of the
pathologic processes produced by such lesions. Pyogenic granuloma (PG) is one such
soft-tissue swelling that originates from the reactive inflammatory course in which
an exuberant fibrovascular expansile growth of the connective tissue of the skin or
mucous membrane occurs. This case report documents a rare case in which the size
and the site of the PG were different from the usual. The treatment included the
Keywords extraction of the involved tooth in addition with the surgical removal of the lesion.
►►pyogenic granuloma The present case report demonstrates that the treatment of choice varies according
►►oral cavity to individual case after the adequate analysis of clinical and radiographic findings and
►►posterior teeth should be managed appropriately to minimize further reoccurrence of the lesion and
►►reactive hyperplasia postsurgical complications.
Introduction Case Report
Pyogenic granuloma (PG) is a common non-neoplastic An 11-year-old female patient reported to the outpatient
inflammatory hyperplastic enlargement seen inside the oral Department of Pedodontics with the chief complaint of
cavity as a tissue reaction to irritation, trauma, or hormonal growth in the oral cavity pertaining to lower right back
imbalances and was first elaborated by Hullihen in 1844.1,2 tooth region which bled often and interfered with normal
It emanates as an elevated sessile or pedunculated growth, eating and brushing. She noticed the growth 20 days back
surfaced with red hemorrhagic and erythematous papules which started as a size of peanut and gradually increased
covered by a fibrinous membrane that usually shows to reach the present size. The medical and family history
ulcerations. The color divaricates from purple pink to red, were non-contributory. On extraoral examination, swelling
based on the vascularity of the lesion. The most common was seen on the lower right side of the face in relation to the
site in the oral cavity is gingiva, usually the marginal gingiva, inferior border of the mandible extending posteriorly. The
and is seen majorly in the maxillary gingiva. Moreover, the intraoral examination revealed a single growing exophytic
anterior areas are commonly affected than posterior areas lesion measuring approximately 2 by 2 cm which was
of the oral cavity. Clinically, the lesion rarely exhibits rapid attached to the marginal gingiva extending between the
growth, is symptomless, and does not cause pain.3 The radio- right mandibular first molar and second molar (►Fig. 1).
graphic findings are typically absent, but in long standing The lesion was reddish in color, oval in shape, pedunculated
gingival PGs, localized alveolar bone resorption can be seen.4 with a smooth surface, and bleeding was present on probing.
Biopsy findings have an important role and are definitive There was noticeable mobility of the mandibular first molar,
in establishing the diagnosis. The treatment involves and these findings were confirmed by palpation of the lesion.
excision of the lesion along with histopathological eval- Correlating the history and intra-oral findings, a provisional
uation to confirm the diagnosis. One important aspect diagnosis of pyogenic granuloma was made.
during the excision of PG is careful monitoring during Intraoral periapical radiograph of teeth no. 46 and
surgical removal because of its vascular nature leading to no. 47 and orthopantomogram revealed interproximal
profuse bleeding.5 The present case documents a rare case alveolar crestal bone loss and root resorption associated
of aggressive PG associated with the gingiva of mandibular with no. 46 (►Fig. 2A and B). After explaining the treat-
permanent first and second molar in an 11-year-old girl. ment plan to the parents and obtaining the consent, oral
received DOI https://doi.org/ ©2019 Bhojia Dental College and
August 24, 2018 10.1055/s-0039-1688102 Hospital affiliated to Himachal
accepted after revision ISSN 2321-1482. Pradesh University
February 27, 2019
A Case Report: Aggressive Pyogenic Granuloma Kumar, Agarwal 47
prophylaxis was done followed by the extraction of no. 46 tissue specimen was sent for histopathological assessment.
along with the surgical excision of the lesion (►Fig. 2C). The histological section at different magnification (10X
The postoperative instructions were given and the excised and 40X) showed hyperplastic parakeratinized stratified
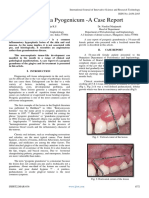
Fig. 1 Preoperative view showing pyogenic granuloma attached to the marginal gingiva extending between the right mandibular first molar
and second molar.
Fig. 2 (A, B) IOPA and OPG showing root resorption of right mandibular first molar and interproximal alveolar crestal bone loss. (C) Excised lesion.
Dental Journal of Advance Studies Vol. 07 No. 1/2019
48 A Case Report: Aggressive Pyogenic Granuloma Kumar, Agarwal
squamous epithelium with supporting fibrovascular Discussion
connective tissue consisting of many budding capillaries,
plump fibroblasts, extravasated red blood cells and dense PG is a type of inflammatory hyperplasia with various
chronic inflammatory cell infiltrate (►Fig. 3A and B). Thus, terminologies such as granuloma pyogenicum, eruptive
a final diagnosis of pyogenic granuloma was given. After hemangioma, and granuloma gravidarum.6 Moreover, PG
1 week, the patient was reviewed and an uneventful and is a misnomer since the lesion does not consist of any pus
satisfactory postoperative healing was noticed (►Fig. 4). and histologically also is not a granuloma.7
Fig. 3 Histological section of the lesion at (A) 10X (B) 40X. At 10x: low power view showing overlying ulcerated stratified squamous
epithelium with areas of high proliferation. Supporting connective tissue stroma demonstrates highly proliferative vascular tissue. Budding
vascular channels are arranged in lobular pattern. Evidence of inflammatory reaction with numerous inflammatory cell infiltration around
the capillaries and throughout the stroma can be seen. At 40x: high power view showing numerous budding capillaries engorged with red
blood cells. These capillaries are lined by plump endothelial cells. Proliferating endothelial cells are evident. These are surrounded by mixed
inflammatory cell infiltrate showing neutrophils, plasma cells and lymphocytes.
Fig. 4 Postoperative view showing uneventful healing after 1 week.
Dental Journal of Advance Studies Vol. 07 No. 1/2019
A Case Report: Aggressive Pyogenic Granuloma Kumar, Agarwal 49
Pyogenic granuloma is a commonly occurring reactive Depending on the extent of the lesion management
lesion of the oral cavity. It is non-neoplastic in nature and varies and with increase in size of the lesion, occlusal
is hence referred to as a tumor-like lesion. Histologically, interference during brushing and eating is seen. As a result
it was described by Angelopoulos as hemangiomatous there will be release of angiogenic and endogenous factors
granuloma because of its inflammatory nature and presence leading to the rise in blood supply to the affected region
of multitudinal blood vessels.8,9 Histopathologically, pyogenic consequently resulting in bleeding. Levels of estrogen and
granuloma is classified into lobular capillary hemangioma progesterone hormones will be augmented during second
(LCH) and nonlobular capillary hemangioma (non-LCH). decade of life especially in females but it can be seen in
Proliferating blood vessels in lobular aggregates, with no all age groups. Cryosurgery, flash lamp pulsed dye laser,
specific changes such as edema and capillary dilatation sclera therapy, excision by Nd YAG laser, injection of cor-
is seen in LCH whereas in Non-LCH type a vascular core ticosteroid or ethanol are additional treatment modalities
resembling granulation tissue with foci of fibrous tissue for pyogenic granuloma.14 In the presented case the size of
is seen with greater number of blood vessels. Oral PGs are the lesion was moderate; therefore, surgical excision was
mainly of LCH type. The microscopic picture of pyogenic carried out which is also a recommended treatment in the
granuloma in general shows exuberant granulation tissue dental literature.
which is covered by atrophic/hyperplastic epithelium that While treating such lesions, importance on maintenance
may be ulcerated at times and reveals fibrinous exudates. of oral hygiene should be advised. This benign vascular
Presence of numerous endothelium-lined vascular spaces and neoplasm does not undergo malignant transformation, but it
proliferation of fibroblasts and budding endothelial cells are tends to recur occasionally after surgical excision usually as
the characteristic features of pyogenic granuloma. Presence a result from incomplete excision, failure to remove etiologic
of mixed inflammatory cell infiltration is also observed. factors, or reinjury of the area. It has also been noted that
At present it is now acknowledged that pyogenic granuloma gingival lesions show a much higher recurrence rate than
occurs as a consequence of different stimuli such as hormonal lesions from other oral mucosal sites.15,16 It was also observed
imbalances, low grade chronic irritation, trauma or certain that there was no reoccurrence of the lesion after 1 year of
type of drugs and oral contraceptives. Nonspecific bacterial follow-up.
infection is supposed to be of minor involvement rather than
being the main etiology of this lesion. The tissues respond
Conclusion
in a typical process ensuing in excessive and uncontrolled
growth of the vascular content of connective tissue.10 Oral Soft-tissue enlargements such as pyogenic granuloma
PGs can appear in all age groups from children to adults, but although non-neoplastic can be present at unusual site
commonly seen in females in the second decade of life due to with atypical size, consequently, appropriate management
the rise in levels of hormones. Pyogenic granuloma generally pertaining to its diagnosis, treatment, and further prevention
affects the gingiva primarily, especially the marginal gingiva is extremely imperative.
and is more common in maxillary than mandibular gingiva.
Authors’ Contributions
Anterior areas are more frequently affected than posterior
Dr. Dipanshu kumar conceived the idea, and helped in
areas. All these lesions are more common on the facial than
the analysis of data and final editing. Dr. Tanya Agarwal
the lingual aspect whereas in the present case report the
helped in collection of data, sample formation, analysis of
aggressive nature and the unusual presentation of the lesion
data, and manuscript preparation.
is evident from its location and size as it is seen in the mandib-
ular posterior region extending from buccal to lingual aspect. Conflict of Interest
It was also observed that the aggressive pyogenic granuloma None declared.
was causing alveolar bone resorption, thus displacing teeth
in the mandibular posterior region. Similar such finding was
reported by Saravana in his review of 137 cases reported four References
patients with extensive bone loss and mobility of teeth.11 1 Greenberg MS, Glick M. Burkett’s Oral Medicine: Diagnosis
Differential diagnosis includes hemangioma, peripheral and Treatment. 10stedn. Hamilton, Canada: BC Decker; 2003
2 Hullihen SP. Case of aneurism by anastomosis of the superior
giant cell granuloma, hyperplastic gingival inflammation,
maxillae. Am J Dent Sci 1844;4(3):160–162
pregnancy tumor, peripheral ossifying fibroma, bacillary
3 Regezi JA, Sciubba JJ, Jordan RC. Oral Pathology and Clinical
angiomatosis, angiosarcoma, metastatic cancer, Kaposi’s Pathological Considerations. 4th ed. Philadelphia, PA: W B
sarcoma, and non-Hodgkin’s kymphoma.12 Peripheral giant Saunders; 2003:115–6
cell granuloma is almost clinically identical to PG; however, 4 Ganesan A, Kumar NG, Azariah E, Asokan GS. Oral pyogenic
bone resorption in radiograph and appearance of the granuloma: a case report and a comprehensive review. SRM J
Res Dent Sci. 2015;6:250–256
multinucleated giant cell are differentiating features.3 Also,
5 Mahajan A, Singhal P, Poonam. Lobular capillary hemangioma
fibroma can be distinguished by the consistency, texture, and in a child: a case report and literature review. Open Access Sci-
the lighter color. Metastatic tumors, even though clinically entific Reports 2012;1:265. doi:10.4172/scientificreports.265
resembles PG, the microscopic features look like as the tumor 6 Jafarzadeh H, Sanatkhani M, Mohtasham N. Oral pyogenic
of origin.13 granuloma: a review. J Oral Sci 2006;48(4):167–175
Dental Journal of Advance Studies Vol. 07 No. 1/2019
50 A Case Report: Aggressive Pyogenic Granuloma Kumar, Agarwal
7 Bouquot JE, Nikai H. Lesions of oral cavity. In: Gnepp DR, ed. 13 Nirmala SVSG, Vallepu R, Babu M, Dasarraju RK. Pyogenic
Diagnostic Surgical Pathology of Head and Neck. Philadelphia, granuloma in an 8-year-old boy: a rare case report. J Pediatr
PA: W B Sanders; 2001:141–233 Neonatal Care 2016;4(2):00135
8 Angelopoulos AP. Pyogenic granuloma of the oral cavity: 14 Parajuli R, Maharjan S. Unusual presentation of oral
statistical analysis of its clinical features. J Oral Surg pyogenic granulomas: a review of two cases. Clin Case Rep
1971;29(12):840–847 2018;6(4):690–693
9 Gomes SR, Shakir QJ, Thaker PV, Tavadia JK. Pyogenic granuloma 15 Rosa CG, Lay AC, Torre ACL. Oral pyogenic granuloma
of the gingiva: A misnomer? A case report and review of diagnosis and treatment: a series of cases. Rev Odontol Mex
literature. J Indian Soc Periodontol 2013;17(4):514–519 2017;21(4):244–252
10 Shafer WG, Hyne MK, Lcvy HM. Shafer's textbook of Oral 16 Fowler EB, Cuenin MF, Thompson SH, Kudryk VL,
Pathology. 4stedn, Philadelphia, London, Toronto: WB Billman MA. Pyogenic granuloma associated with guided
Saunders; 1983 tissue regeneration: a case report. J Periodontol 1996;
11 Saravana GH. Oral pyogenic granuloma: a review of 137 cases. 67(10):1011–1015
Br J Oral Maxillofac Surg 2009;47(4):318–319
12 Neville BW, Damm DD, Allen CM, Bouquot JE. Oral and
Maxillofacial Pathology. 2nd ed. Philadelphia, PA: Saunders;
2002:437–95
Dental Journal of Advance Studies Vol. 07 No. 1/2019
You might also like
- Arts and Design - Q1 - Mod2 - ArtistryRelatedInjuries - Version1 by Romel SabidorDocument26 pagesArts and Design - Q1 - Mod2 - ArtistryRelatedInjuries - Version1 by Romel SabidorJayson Paul Dalisay Datinguinoo100% (2)
- Necrotizing Sialometaplasia of The Palate: A Case Report: Ashwarya Trivedi, Mysore K Sunil, Sonam Gupta, Shaveta GargDocument4 pagesNecrotizing Sialometaplasia of The Palate: A Case Report: Ashwarya Trivedi, Mysore K Sunil, Sonam Gupta, Shaveta Gargandrianiputri916No ratings yet
- Granuloma ArticleDocument3 pagesGranuloma ArticleRamanpreet KourNo ratings yet
- Acharya 2011Document4 pagesAcharya 2011andreia ichimNo ratings yet
- Lobular Capillary Hemangioma of TongueDocument3 pagesLobular Capillary Hemangioma of TongueShreya DasguptaNo ratings yet
- Pyogenic GranulomaDocument13 pagesPyogenic GranulomaPiyusha SharmaNo ratings yet
- Journal Occlusal 2Document4 pagesJournal Occlusal 2Felianda ThaliaNo ratings yet
- Unusual Large and Abiding Fibroepithelial Polyp in Oral Cavity: A Case ReportDocument4 pagesUnusual Large and Abiding Fibroepithelial Polyp in Oral Cavity: A Case ReportmuharrimahNo ratings yet
- Gingival Epulis: Report of Two Cases.: Dr. Praful Choudhari, Dr. Praneeta KambleDocument5 pagesGingival Epulis: Report of Two Cases.: Dr. Praful Choudhari, Dr. Praneeta KambleAnandNo ratings yet
- Dental Journal: Peripheral Ossifying Fibroma of The Anterior Maxillary GingivaDocument5 pagesDental Journal: Peripheral Ossifying Fibroma of The Anterior Maxillary Gingivaanugraha GanendraNo ratings yet
- Peripheral Giant Cell Granuloma - A Case ReportDocument4 pagesPeripheral Giant Cell Granuloma - A Case ReportAziz IkbalNo ratings yet
- V 7 Aop 191Document3 pagesV 7 Aop 191Sekar EkaperdanaNo ratings yet
- October 2018 1538385165 481 PDFDocument4 pagesOctober 2018 1538385165 481 PDFKiyRizkikaNo ratings yet
- Clinical: Idiopathic Gingival Fibromatosis Associated With Generalized Aggressive Periodontitis: A Case ReportDocument5 pagesClinical: Idiopathic Gingival Fibromatosis Associated With Generalized Aggressive Periodontitis: A Case Reportchakriy9No ratings yet
- Gingival Abscess Case ReportDocument4 pagesGingival Abscess Case ReportKrishan GuliaNo ratings yet
- Management of Necrotizing Ulcerative Gingivitis in A Pregnant Patient - A Rare Case ReportDocument6 pagesManagement of Necrotizing Ulcerative Gingivitis in A Pregnant Patient - A Rare Case ReportAZWAN RAHMADHAN PUTRANo ratings yet
- 243 674 1 PB PDFDocument2 pages243 674 1 PB PDFsurgaNo ratings yet
- InflammatoryGingivalEnlargement ACaseReport PDFDocument5 pagesInflammatoryGingivalEnlargement ACaseReport PDFMardianiPutriPutriNo ratings yet
- Pyogenic GranulomaDocument6 pagesPyogenic GranulomaRini TiaraNo ratings yet
- 63 - CASE REPORT Epulis GranulomaDocument3 pages63 - CASE REPORT Epulis GranulomaRina NovitrianiNo ratings yet
- A Parulis-Like Soft Tissue Tumor in Relation With A Dental Implant: Case ReportDocument3 pagesA Parulis-Like Soft Tissue Tumor in Relation With A Dental Implant: Case ReportDr. AtheerNo ratings yet
- Periapical GranulomaDocument3 pagesPeriapical GranulomaLina BurduhNo ratings yet
- Giant Cell Epulis: Report of 2 Cases.: Oral PathologyDocument11 pagesGiant Cell Epulis: Report of 2 Cases.: Oral PathologyVheen Dee DeeNo ratings yet
- 8978 22741 1 SMDocument3 pages8978 22741 1 SMDhita AndanaNo ratings yet
- Gingival Squamous Cell Carcinoma Presenting As Periodontal Lesion in The Mandibular Posterior RegionDocument4 pagesGingival Squamous Cell Carcinoma Presenting As Periodontal Lesion in The Mandibular Posterior RegionThái BìnhNo ratings yet
- Plasma Cell Gingivitis With Aggressive Periodontitis: A Rare Presentation of An Uncommon ConditionDocument4 pagesPlasma Cell Gingivitis With Aggressive Periodontitis: A Rare Presentation of An Uncommon Conditionratih agridithaNo ratings yet
- Peripheral Ossifying Fi Broma: ASE EportDocument4 pagesPeripheral Ossifying Fi Broma: ASE Eporterr3sNo ratings yet
- Artículo de Periodoncia 2Document7 pagesArtículo de Periodoncia 2Margareth Roxanna Mendieta GirónNo ratings yet
- 7 CR 2 ArjunDocument4 pages7 CR 2 Arjunkiara wardanaNo ratings yet
- 3 RdarticleDocument5 pages3 RdarticleAmira Pradsnya ParamitaNo ratings yet
- Bi Bi: Fibrous Epulis - Case ReportDocument6 pagesBi Bi: Fibrous Epulis - Case Reportemmanuellagrace06No ratings yet
- Fibrous Hyperplasia A Case ReportDocument4 pagesFibrous Hyperplasia A Case ReportBramita Beta ArnandaNo ratings yet
- Dentj 38 2 02Document4 pagesDentj 38 2 02Alfonsius JeriNo ratings yet
- Periapical Granuloma Associated With Extracted Teeth: Original ArticleDocument4 pagesPeriapical Granuloma Associated With Extracted Teeth: Original ArticleDinar Sukma PamungkasNo ratings yet
- Pyogenic Granuloma A Case ReportDocument9 pagesPyogenic Granuloma A Case ReportSafira HlwNo ratings yet
- Granuloma Pyogenicum - A Case ReportDocument4 pagesGranuloma Pyogenicum - A Case ReportInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Radicular Cyst With Primary Mandibular Molar A RarDocument5 pagesRadicular Cyst With Primary Mandibular Molar A RargarciadeluisaNo ratings yet
- Case Report Necrotizing Ulcerative Gingivitis, A Rare Manifestation As A Sequel of Drug-Induced Gingival Overgrowth: A Case ReportDocument7 pagesCase Report Necrotizing Ulcerative Gingivitis, A Rare Manifestation As A Sequel of Drug-Induced Gingival Overgrowth: A Case ReportPutri Dwi AnggrainiNo ratings yet
- Focal Reactive OvergrowthsDocument5 pagesFocal Reactive OvergrowthsLjubomirErdoglijaNo ratings yet
- Periapical GranulomaDocument6 pagesPeriapical GranulomaEzza RiezaNo ratings yet
- Post Covid 19 Mucoromycosis of MandibleDocument5 pagesPost Covid 19 Mucoromycosis of MandibleDr Yamuna RaniNo ratings yet
- Management of Chronic Gingivitis PDFDocument5 pagesManagement of Chronic Gingivitis PDFliaamNo ratings yet
- 2017 FrogDocument4 pages2017 FrogUma DatarNo ratings yet
- 10866-Article Text-52118-1-10-20220425Document10 pages10866-Article Text-52118-1-10-20220425Trianita DivaNo ratings yet
- Jurnal Porio 1Document3 pagesJurnal Porio 1Neo YustindraNo ratings yet
- Lobular Capillary Hemangioma An Extremely Rare Entity in The Retromolar Region Case ReportDocument5 pagesLobular Capillary Hemangioma An Extremely Rare Entity in The Retromolar Region Case ReportInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Palatal SwellingsDocument6 pagesPalatal Swellingsopi akbarNo ratings yet
- Case Report Endo Perio Lesions-A Synergistic ApproachDocument5 pagesCase Report Endo Perio Lesions-A Synergistic ApproachRyanka Dizayani PutraNo ratings yet
- Jomp039-01-07 2Document5 pagesJomp039-01-07 2azkaziyan14No ratings yet
- Irritational Fibroma A Case ReportDocument2 pagesIrritational Fibroma A Case ReportquikhaaNo ratings yet
- Torus InglesDocument5 pagesTorus InglespaolaNo ratings yet
- Ijcpd 12 68Document5 pagesIjcpd 12 68lily oktarizaNo ratings yet
- GINGIVEKTOMIDocument6 pagesGINGIVEKTOMIAstrid ChrisanditaNo ratings yet
- Chronic Inflammatory Gingival Enlargement: A CaseDocument3 pagesChronic Inflammatory Gingival Enlargement: A CaseArida Khoiruza Asy'ariNo ratings yet
- DR Bhaumik Nanavati Proof ApprovedDocument6 pagesDR Bhaumik Nanavati Proof ApprovedFahmi FirmansyahNo ratings yet
- Dental Implant Therapy in A Patient With Acromegaly: A Clinical ReportDocument6 pagesDental Implant Therapy in A Patient With Acromegaly: A Clinical ReportAkanksha MahajanNo ratings yet
- Pulpitis JurnalDocument2 pagesPulpitis JurnalIsmail YusufNo ratings yet
- Pemphigus Vulgaris Confined To The Gingiva: A Case ReportDocument16 pagesPemphigus Vulgaris Confined To The Gingiva: A Case ReportAlmasulah Al-akmaliyahNo ratings yet
- Berglundh Et Al (2018) - Peri Implant Diseases and Conditions - Consensus Report of Workgroup 4 - 1Document9 pagesBerglundh Et Al (2018) - Peri Implant Diseases and Conditions - Consensus Report of Workgroup 4 - 1FelipeOyarceSalazarNo ratings yet
- Peri-Implant Complications: A Clinical Guide to Diagnosis and TreatmentFrom EverandPeri-Implant Complications: A Clinical Guide to Diagnosis and TreatmentNo ratings yet
- Amelogenesis Imperfecta: Case Study: Operative Dentistry September 2017Document14 pagesAmelogenesis Imperfecta: Case Study: Operative Dentistry September 2017Barbulescu Anca DianaNo ratings yet
- Rampant Caries in Adolescence: December 2019Document4 pagesRampant Caries in Adolescence: December 2019Barbulescu Anca DianaNo ratings yet
- Direct Laminate Veneers With Resin Composites: Two Case Reports With Five-Year Follow-UpsDocument3 pagesDirect Laminate Veneers With Resin Composites: Two Case Reports With Five-Year Follow-UpsBarbulescu Anca DianaNo ratings yet
- Partial Edentulism : Exploring Partial Edentulism Patterns in Mandibular Arch Among Patients of KarachiDocument5 pagesPartial Edentulism : Exploring Partial Edentulism Patterns in Mandibular Arch Among Patients of KarachiBarbulescu Anca DianaNo ratings yet
- Post-Operative Complications PresentationDocument37 pagesPost-Operative Complications PresentationChrisNeop0% (1)
- Radlink Issue 1 2008Document8 pagesRadlink Issue 1 2008RadlinkSingaporeNo ratings yet
- Depression: by Aroosha Abdul RasheedDocument9 pagesDepression: by Aroosha Abdul RasheedArushar 24No ratings yet
- 1h. Chapter-1-Introduction To First Aid-HighlightedDocument25 pages1h. Chapter-1-Introduction To First Aid-HighlightedMohamed BinNo ratings yet
- Stroke Hemoragik: Yusi Rizky N 1 6 1 0 2 1 1 0 5 1Document19 pagesStroke Hemoragik: Yusi Rizky N 1 6 1 0 2 1 1 0 5 1Yusi RizkyNo ratings yet
- Tarea 2 de Ingles 2Document6 pagesTarea 2 de Ingles 2Rosa RamosNo ratings yet
- Delta VariantDocument1 pageDelta VariantKurt Alec Richmond SALANGUITNo ratings yet
- Transfusion Reaction PDFDocument1 pageTransfusion Reaction PDFKah Man GohNo ratings yet
- Gastrointestinal SystemDocument218 pagesGastrointestinal Systemnursereview92% (12)
- DR Nazri - Covid-19 (CME) PDFDocument46 pagesDR Nazri - Covid-19 (CME) PDFKok Hui DiongNo ratings yet
- Optic Disc CuppingDocument14 pagesOptic Disc CuppingAsri Kartika AnggraeniNo ratings yet
- Differential Diagnosis of Low Back Pain: Elizabeth Huntoon, MD, and Marc Huntoon, MDDocument7 pagesDifferential Diagnosis of Low Back Pain: Elizabeth Huntoon, MD, and Marc Huntoon, MDGangsar DamaiNo ratings yet
- LidocaineDocument2 pagesLidocaineLeigh Marie LastimosaNo ratings yet
- Statistical TreatmentDocument9 pagesStatistical TreatmentCiv NortubNo ratings yet
- Heart Failure Treatment Algorithm: Diagnosis and ClassificationDocument7 pagesHeart Failure Treatment Algorithm: Diagnosis and ClassificationLorreine Elisa FaruqNo ratings yet
- Medicare Inpatient 2017Document8,939 pagesMedicare Inpatient 2017Shashi Shirke100% (1)
- Ineffective Breathing Pattern - NCPDocument2 pagesIneffective Breathing Pattern - NCPHsintan HsuNo ratings yet
- Sexually Transmitted Diseases HEALTH TEACHING 1 Copy 1Document41 pagesSexually Transmitted Diseases HEALTH TEACHING 1 Copy 1Pauline FabiañaNo ratings yet
- Physical & Multiple Disability ChecklistDocument3 pagesPhysical & Multiple Disability ChecklistGheylhu AmorNo ratings yet
- IMNCIDocument84 pagesIMNCIAyenew100% (1)
- Neoplastic Proliferation of White Blood CellDocument35 pagesNeoplastic Proliferation of White Blood Cellnighat khanNo ratings yet
- Infective EndocarditisDocument58 pagesInfective EndocarditisTok KeawkaewNo ratings yet
- Examination of Cerebellum and MeningesDocument4 pagesExamination of Cerebellum and MeningesAngelaTrinidadNo ratings yet
- 4th Quarter Summative Test Mapeh 7Document3 pages4th Quarter Summative Test Mapeh 7Theness BonjocNo ratings yet
- Perioperative Management of AdrenalectomyDocument13 pagesPerioperative Management of AdrenalectomyTJ LapuzNo ratings yet
- Massive HemorrhageDocument17 pagesMassive HemorrhageShannen Madrid Tindugan100% (1)
- NVHR - 211045 - 090821 - Mask Mandate Flyer - v1.1 - FDocument1 pageNVHR - 211045 - 090821 - Mask Mandate Flyer - v1.1 - FFOX5 VegasNo ratings yet
- Dictionary of Pharmaceutical Dosage FormsDocument169 pagesDictionary of Pharmaceutical Dosage FormsNguyễn Trần LinhNo ratings yet
- Drug Study AmlodipineDocument3 pagesDrug Study AmlodipineKristine ChampnessNo ratings yet