Professional Documents
Culture Documents
How To Do Internal Jugular Vein Cannulation - Critical Care Medicine - MSD Manual Professional Edition
How To Do Internal Jugular Vein Cannulation - Critical Care Medicine - MSD Manual Professional Edition
Uploaded by
naveenCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
How To Do Internal Jugular Vein Cannulation - Critical Care Medicine - MSD Manual Professional Edition
How To Do Internal Jugular Vein Cannulation - Critical Care Medicine - MSD Manual Professional Edition
Uploaded by
naveenCopyright:
Available Formats
Brought to
ABOUT MSD MSD CAREERS RESEARCH WORLDWIDE
you by
MSD MANUAL
Professional Version
How To Do Internal Jugular Vein
Cannulation
By Paula Ferrada
, MD, VCU Health System
Last full review/revision Jun 2020| Content last modified Jun 2020
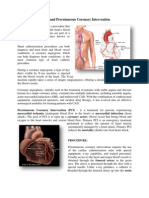
Percutaneous cannulation of the internal jugular vein uses anatomic landmarks to guide venipuncture
and a Seldinger technique to thread a central venous catheter through the internal jugular vein and into
the superior vena cava. Three approaches (central, anterior, and posterior) are used; the central approach
is described here.
An internal jugular central venous catheter (CVC) or a peripherally inserted central catheter (PICC)
is usually preferred to a subclavian CVC (which has a higher risk of bleeding and pneumothorax) or
a femoral CVC (which has a higher risk of infection).
Ultrasonographic guidance for placement of internal jugular lines increases the likelihood of
successful cannulation and reduces the risk of complications. When ultrasonographic guidance
and trained personnel are available, this method of placement is preferred.
(See also Vascular Access, Central Venous Catheterization, and How To Do Internal Jugular Vein
Cannulation, Ultrasound-Guided.)
Indications for Internal Jugular Vein Cannulation
Secure or long-term venous access that is not available using other sites
Inability to obtain peripheral venous access or intraosseous infusion
IV infusion of fluids and drugs for patients in cardiac arrest
IV infusion of concentrated or irritating fluids
IV infusion of high flows or large fluid volumes beyond what is possible using peripheral
venous catheters
Monitoring of central venous pressure (CVP)
Hemodialysis or plasmapheresis
Transvenous cardiac pacing (see video How to Insert a Transvenous Pacemaker) or pulmonary
arterial monitoring (Swan-Ganz catheter)*
Placement of inferior vena cava filter
* For transvenous cardiac pacing or pulmonary arterial monitoring, a right internal jugular
cannulation or a left subclavian vein cannulation typically is preferred.
Contraindications to Internal Jugular Vein Cannulation
Absolute contraindications
Internal jugular vein thrombosis
Local infection at the insertion site
Antibiotic-impregnated catheter in allergic patient
Relative contraindications
Coagulopathy, including therapeutic anticoagulation*
Local anatomic distortion, traumatic or congenital, or gross obesity
Superior vena cava syndrome
Severe cardiorespiratory insufficiency or increased intracranial or intraocular pressure
(patients will be compromised by Trendelenburg [head down] positioning)
History of prior catheterization of the intended central vein
Uncooperative patient (should be sedated if necessary)
Left bundle branch block (a guidewire or catheter in the right ventricle can induce complete
heart block)
* Therapeutic anticoagulation (eg, for pulmonary embolism) increases the risk of bleeding with
internal jugular vein cannulation, but this must be balanced against the increased risk of
thrombosis (eg, stroke) if anticoagulation is reversed. Discuss any contemplated reversal with the
clinician managing the patient's anticoagulation and then with the patient. A femoral line may be
preferred.
Complications of Internal Jugular Vein Cannulation
(See also Complications of central venous catheterization.)
Complications include
Arterial puncture
Hematoma
Pneumothorax
Damage to the vein
Hemothorax
Air embolism
Catheter misplacement*
Arrhythmias or atrial perforation, typically caused by guidewire or catheter
Nerve damage
Infection
Thrombosis
* Rare complications due to catheter misplacement include arterial catheterization, hydrothorax,
hydromediastinum, and damage to the tricuspid valve.
Guidewire or catheter embolism also rarely occurs.
To reduce the risk of venous thrombosis and catheter sepsis, CVCs should be removed as soon as
they are no longer needed.
Equipment for Internal Jugular Vein Cannulation
Sterile procedure, barrier protection
Antiseptic solution (eg chlorhexidine alcohol chlorhexidine povidone iodine alcohol)
Antiseptic solution (eg, chlorhexidine-alcohol, chlorhexidine, povidone iodine, alcohol)
Large sterile drapes, towels
Sterile head caps, masks, gowns, gloves
Face shields
Seldinger (catheter-over-guidewire) technique
Cardiac monitor
Local anesthetic (eg, 1% lidocaine without epinephrine, about 5 mL)
Small anesthetic needle (eg, 25 to 27 gauge, about 1 inch [3 cm] long)
Large anesthetic/finder* needle (22 gauge, about 1.5 inches [4 cm] long)
Introducer needle (eg, thin-walled, 18 or 16 gauge, with internally beveled hub, about 2.5
inches [6 cm] long)
3- and 5-mL syringes (use slip-tip syringes for the finder and introducer needles)
Guidewire, J-tipped
Scalpel (#11 blade)
Dilator
Central venous catheter (adult: 8 French or larger, minimum length for internal jugular
catheter is 15 cm for right side, 20 cm for left side)
Sterile gauze (eg, 4 × 4 inch [10 × 10 cm] squares)
Sterile saline for flushing catheter port or ports
Nonabsorbable nylon or silk suture (eg, 3-0 or 4-0)
Chlorhexidine patch, transparent occlusive dressing
* A finder needle is a thinner needle used for locating the vein before inserting the introducer
needle. It is generally recommended for nonultrasound–guided internal jugular vein cannulation.
Having an assistant or two is helpful.
Additional Considerations
Cannulation attempts sometimes fail. Do not exceed 2 or 3 attempts (which increases the risk
of complications), and use new equipment with each attempt (ie, do not re-use needles,
catheters, or other equipment because they may have become blocked with tissue or blood).
During cardiopulmonary arrest, or even low blood pressure and hypoxia, arterial blood may
be dark and not pulsatile and may be mistaken for venous blood.
If the internal jugular artery is errantly cannulated by either the tissue dilator or the CVC,
leave the dilator or catheter in place and obtain surgical consultation for possible surgical
removal.
Relevant Anatomy for Internal Jugular Vein Cannulation
The anterior cervical triangle is bordered by the clavicle inferiorly and by the sternal and
clavicular heads of the sternocleidomastoid muscle medially and laterally.
The carotid artery is usually palpated near the lateral side of the sternal head of the
sternocleidomastoid, and the internal jugular vein usually lies superficial and lateral (often
minimally lateral) to the carotid artery. However, variant orientation of these vessels occurs
regularly (in 9 to 19% of patients). The orientation of the carotid artery and internal jugular
egu a y ( 9 to 9% o pat e ts). e o e tat o o t e ca ot d a te y a d te a jugu a
vein to each other also may change if the position of the patient’s head changes.
Most commonly, the central approach to the internal jugular vein is used, which may
decrease the chance of pleural or carotid arterial puncture. The introducer needle is inserted
at about a 30 to 40° angle to the skin at the apex (superior angle) of the anterior cervical
triangle, aiming toward the ipsilateral nipple.
The right internal jugular vein is usually preferred over the left for cannulation because it has
a larger diameter and affords a straighter path to the superior vena cava.
Vascular Anatomy of the Right
Neck Area
3D MODEL
Positioning for Internal Jugular Vein Cannulation
Raise the bed to a comfortable height for you (ie, so you may stand straight while doing the
procedure).
Place the patient supine and in Trendelenburg position (bed tilted head down 15 to 20°) to
distend the internal jugular vein and prevent air embolism.
Turn the patient's head only slightly (or not at all) to the contralateral side to expose the
internal jugular vein but not cause overlap with the carotid artery.
Stand at the head of the bed.
Step-by-Step Description of Procedure
Do a preliminary inspection (nonsterile) to identify the anterior cervical triangle, palpate the
carotid arterial pulse, and (optionally) mark the lateral border of the carotid.
Attach the cardiac monitor to the patient and turn it on.
Prepare the equipment
Place sterile equipment on sterilely covered equipment trays.
Dress in sterile garb and use barrier protection.
Draw the local anesthetic into a syringe.
Attach a finder needle to a 5-mL syringe with 1 to 2 mL of sterile saline in it.
Attach the introducer needle to a 5-mL syringe with 1 to 2 mL of sterile saline in it. Align the
bevel of the needle with the volume markings on the syringe.
Pre-flush all lines of the CVC with 3 to 5 mL of sterile saline and then close the ports with caps
or syringes.
When flushing a central line, use a 10-mL syringe (or one of equal or greater diameter) and do not push
too hard to avoid rupturing the line.
Prepare the sterile field
Swab a broad area of skin with antiseptic solution, encompassing the side of the neck,
clavicle, and anterior chest to below the ipsilateral nipple. Creating this broad sterile area
permits immediately switching to subclavian vein cannulation should the jugular cannulation
attempt fail.
Allow the antiseptic solution to dry for at least 1 minute.
Place sterile towels around the site, keeping the ipsilateral nipple exposed.
Place large sterile drapes (eg, a full-body drape) to establish a large sterile field.
Establish the needle insertion path (internal jugular vein, central approach)
Gently palpate the carotid arterial pulse using 3 fingers to appreciate the course of the artery.
Palpate gently so as not to compress the adjacent internal jugular vein (a compressed venous
lumen is difficult to cannulate).
The needle insertion path: Insert procedural needles (local anesthetic, finder, and introducer
needles) into the apical area (superior angle) of the anterior cervical triangle, just lateral to
the carotid pulse, at a 30 to 40° angle into the skin, aiming toward the ipsilateral nipple.
Maintain carotid artery palpation during needle insertions and keep the needle lateral to the artery to
avoid impaling the artery.
Anesthetize the cannulation site
Place a wheal of anesthetic at the needle entry site and then inject anesthetic into the skin
and soft tissues along the anticipated needle insertion path. Maintain gentle negative
pressure on the syringe plunger as you advance to identify intravascular placement and
prevent an intravascular injection.
If blood returns into the syringe, stop advancing, hold the syringe in place, and now regard
this needle as a finder needle. Proceed to Assess the blood return below.
Insert the finder needle
Insert the finder needle along the needle insertion path.
Maintain gentle negative pressure on the syringe plunger as you advance the needle.
Stop advancing when a flash of blood appears in the barrel of the syringe (you may feel the
needle pop through the wall as it enters the lumen). Hold the syringe motionless in this spot.
Even a slight movement may displace the needle tip from the vein.
If no flash of blood appears in the barrel after about 3 to 5 cm of insertion, withdraw the needle
slowly. If the needle had initially passed completely through the vein, a flash of blood may now
appear as you withdraw the needle tip back into the lumen. If a flash still does not appear,
withdraw the needle almost to the skin surface, change direction (usually slightly medially), and try
again to advance the needle into the vein. Do not change the direction of the needle while it is fully
inserted.
Assess the blood return
Continue to hold the syringe motionless.
Securely grasp the needle hub and also hold it motionless.
Remove the syringe from the needle hub and briefly let blood flow out to confirm that the
blood is venous (ie, dark red and flowing but not pulsatile). Then immediately cover the hub
b ood s e ous ( e, da ed a d o g but ot pu sat e). e ed ate y co e t e ub
with your thumb to stop the blood flow and prevent air embolism.
However, if the blood is bright red and pulsatile (arterial), terminate the procedure. Remove the
needle and use 4 × 4 gauze squares for 10 minutes to hold external pressure on the area and to
help prevent bleeding and hematoma.
Percutaneous Cannulation of the
Internal Jugular Vein
VIDEO
Insert the introducer needle, using the finder needle as a guide
Hold the introducer syringe with the needle bevel facing up.
Use one of two insertion methods: Either remove the finder needle and immediately insert
the introducer needle along the same path, or keep the finder needle in place and insert the
introducer needle underneath and roughly parallel to it (at a slightly shallower angle to the
skin).
Stop advancing the introducer needle when a flash of blood appears in the barrel of the
syringe. Hold the syringe motionless in this spot.
If the finder needle has not been removed, remove it now.
Assess blood flow from the introducer needle as described in Assess the blood return above.
Insert the guidewire
Carefully rotate the introducer syringe such that the bevel of the needle now faces medially
(ie, toward the heart and away from the subclavian vein).
Insert the J-curved end of the guidewire into the introducer needle, with the J curve facing
medially (ie, in the same direction as the needle bevel).
Advance the guidewire through the needle and into the vein. Do not force the wire; it should
slide smoothly. Advance the wire 10 to 15 cm for a right-sided internal jugular insertion, 15 to
20 cm for a left-sided insertion, or until ectopic heartbeats occur (withdraw from this point
until ectopy stops).
If you feel any resistance as you advance the guidewire, stop advancing it. Try to gently withdraw
the wire slightly, rotate it slightly, and then readvance it, or try to gently withdraw the wire entirely,
reestablish the needle tip within the vein (confirmed by venous blood return), and then reinsert
the wire.
However, if you feel any resistance as you withdraw the wire, terminate the procedure and
withdraw the needle and guidewire together as a unit (to prevent the needle tip from shearing
through the guidewire within the patient). Then use 4 × 4 gauze squares for 10 minutes to hold
external pressure on the area and to help prevent bleeding and hematoma.
Once the guidewire has been inserted, continue to hold it securely in place with one hand and maintain
control of it throughout the remainder of the procedure.
h i d dl f f l id i i i
Remove the introducer needle (after successful guidewire insertion)
First, securely hold the guidewire distal to the needle and pull the needle from the skin.
Then, securely hold the guidewire at the skin surface and slide the needle down the
remaining length of the guidewire to remove the needle.
Widen the insertion tract
Extend the skin insertion site: Using the scalpel, make a small stab incision (about 4 mm) into
the skin insertion site, avoiding contact with the guidewire, to enlarge the site and allow it to
accommodate the larger diameters of the tissue dilator and the catheter.
Advance the tissue dilator over the guidewire: First, grasp the guidewire at the skin and slide
the dilator down the length of the wire to the skin. Then grasp the wire just distal to the
dilator, hold the dilator near the skin surface, and use a corkscrew motion as needed to
stepwise insert the entire length of the dilator. Maintain your grasp on the wire at all times
during the insertion.
Remove the dilator: First, securely hold the guidewire distal to the dilator and pull the dilator
from the skin. When the guidewire is visible at the skin surface, completely remove the dilator
by sliding it down the remaining length of the guidewire.
Maintain your grasp on the guidewire at the skin surface.
Place the catheter
Advance the catheter over the guidewire to the skin surface: Hold the guidewire fixed at the
skin surface, thread the catheter tip over the distal end of the guidewire, and slide the
catheter down to the skin surface. The distal end of the guidewire should now be protruding
from the port hub.
If the distal end of the guidewire is not protruding from the port hub, inch the guidewire
outward from the skin surface while holding the catheter tip close to the skin surface until
the guidewire protrudes.
Continue to advance the catheter into the vein: Grasp and control the guidewire where it
protrudes from the hub. Hold the catheter near its tip and insert the tip through the skin.
Then, in increments of several centimeters and using a corkscrew motion as necessary,
stepwise advance the internal jugular catheter. If ectopic heartbeats occur, slowly withdraw
the catheter until ectopy stops.
Maintain your grasp on both the guidewire and the catheter.
Remove the guidewire: Withdraw the guidewire while holding the catheter securely in place
at the skin surface.
Flush each catheter port with saline: First, draw any air from the line and confirm venous
blood flow into the hub. Then, using a 10-mL syringe (or one of equal or greater diameter)
and nonexcessive force, push 20 mL of saline into the line to clear it.
Dress the site
If the patient is awake or minimally sedated, use 1% lidocaine to numb the skin at the
planned suture locations.
Place a chlorhexidine-impregnated disk on the skin at the catheter insertion point.
Suture the skin to the mounting clip on the catheter.
To prevent pulling on the insertion site, suture the catheter at a second site so that a curved
or looped segment of catheter lies between the two sites.
Apply a sterile occlusive dressing. Transparent membrane dressings are commonly used.
Aftercare for Internal Jugular Vein Cannulation
Do a chest x-ray to confirm that the tip of a jugular (or subclavian) CVC lies in the superior
vena cava near its junction with the right atrium (the catheter can be advanced or retracted if
not in the appropriate position) and to confirm that pneumothorax has not occurred.
X-Ray of a Central Venous Catheter
Hide Details
The red arrow points to the tip of a left subclavian venous port catheter (placed appropriately
in the lower superior vena cava).
© 2017 Elliot K. Fishman, MD.
Warnings and Common Errors
The tip of a CVC must never lie in the right atrium because the atrium is thin-walled and
easily perforated.
Cardiac ectopy may be induced by a guidewire or catheter in the right atrium or ventricle.
Never lose grasp of the guidewire.
During cardiopulmonary arrest, or even low blood pressure and hypoxia, arterial blood may
be dark and not pulsatile and may be mistaken for venous blood.
To help prevent air embolism, CVCs should be inserted (and removed) with the vascular
cannulation site positioned dependant to the heart.
Tips and Tricks for Internal Jugular Vein Cannulation
A thin (finder, scout) needle often is used to first find the internal jugular vein (before
inserting the larger introducer needle) so that less bleeding and hematoma result if the
needle aberrantly impales the carotid artery. (Ultrasound guidance eliminates the need for a
finder needle.)
The orientation of the carotid artery and internal jugular vein to each other may change if the
position of the patient’s head changes; thus, to avoid impaling the artery, you should gently
palpate the carotid pulse during the needle insertions included in this procedure.
p p p g p
The size of the internal jugular vein varies with respiration (maximum diameter in patients
not intubated occurs just prior to inspiration [prior to expiration in intubated patients]) and is
increased by the Trendelenburg position, the Valsalva maneuver, humming, and external
abdominal compression. To increase your chance of successful internal jugular cannulation,
advance the introducer at moments of increased jugular diameter.
© 2022 Merck & Co., Inc., Rahway, NJ, USA and its affiliates. All rights reserved.
You might also like
- 18d Nls Use Manual EnglishDocument136 pages18d Nls Use Manual Englishneo carty100% (1)
- IV Cannulation and Fixation Infusion PumpDocument23 pagesIV Cannulation and Fixation Infusion PumpUday Kumar0% (1)
- Interventional CardiologyDocument36 pagesInterventional CardiologyRufus RajNo ratings yet
- Central Venous Pressure InsertionDocument22 pagesCentral Venous Pressure Insertionjeizy17No ratings yet
- Pharmacist Workup of Drug Therapy in Pharmaceutical Care: Problem Oriented Pharmacist RecordDocument22 pagesPharmacist Workup of Drug Therapy in Pharmaceutical Care: Problem Oriented Pharmacist RecordputihatauhitamNo ratings yet
- Critical Care ProtocolsDocument19 pagesCritical Care ProtocolsPrabhat KumarNo ratings yet
- Arteri LineDocument13 pagesArteri Linemuthia octavianaNo ratings yet
- CVP MonitoringDocument10 pagesCVP MonitoringRaghu RajanNo ratings yet
- Umbilical Vein CatheterizationDocument3 pagesUmbilical Vein CatheterizationrohitNo ratings yet
- Peripherally Inserted Central CatheterDocument4 pagesPeripherally Inserted Central CatheterDivine Grace Arreglo AbingNo ratings yet
- Subclavian Centraline ManualDocument12 pagesSubclavian Centraline Manualqc.carcinovaNo ratings yet
- ACFrOgBJ11ZY9WD49wZ4mx Nu2QyGvK-qmOsUHKXVRSBkfEbfwWLzfDaE3L9 rejnh0YFVdwEJYzgZnIKRyT1AcSkbIft12Sqr5t7NCHqRd2MZQD7DJSwhSvGVKwQbTUPSaBLuf75yV EO1CV72IDocument8 pagesACFrOgBJ11ZY9WD49wZ4mx Nu2QyGvK-qmOsUHKXVRSBkfEbfwWLzfDaE3L9 rejnh0YFVdwEJYzgZnIKRyT1AcSkbIft12Sqr5t7NCHqRd2MZQD7DJSwhSvGVKwQbTUPSaBLuf75yV EO1CV72Iمحمد سعد طهNo ratings yet
- CVP MonitoringDocument64 pagesCVP MonitoringNárēsh Yadav GäddēNo ratings yet
- Central Venous Access: RSUD Duren SawitDocument48 pagesCentral Venous Access: RSUD Duren SawitMonica HerdiatiNo ratings yet
- Final HeartDocument6 pagesFinal HeartPrincess PlateroNo ratings yet
- (FEU) Central Venous Pressure Notes PDFDocument25 pages(FEU) Central Venous Pressure Notes PDFBryJos tiongsonNo ratings yet
- Intravenous CannulationDocument37 pagesIntravenous CannulationUday KumarNo ratings yet
- CVPDocument25 pagesCVPNikhil YadavNo ratings yet
- PericardiocintesisDocument20 pagesPericardiocintesisKarelau KarniaNo ratings yet
- Arterial LineDocument2 pagesArterial LineRaghav Goyal100% (1)
- Aqueductal StenosisDocument41 pagesAqueductal StenosisAnna SinghNo ratings yet
- Central Venous Catheterization: Maret 2021Document39 pagesCentral Venous Catheterization: Maret 2021Rudy SiahaanNo ratings yet
- Umbilical Artery CatheterizationDocument9 pagesUmbilical Artery CatheterizationrohitNo ratings yet
- Cap 2013 NejmDocument7 pagesCap 2013 NejmpaulaandreavargasbNo ratings yet
- PERICARDIOCENTESISDocument25 pagesPERICARDIOCENTESISrastaNo ratings yet
- Central Venous CatheterDocument5 pagesCentral Venous Catheterasmaa_gamal14No ratings yet
- CardiacDocument18 pagesCardiacAya Mohamed100% (1)
- Central Venous Central Venous Catheterization CatheterizationDocument25 pagesCentral Venous Central Venous Catheterization CatheterizationNobian AndreNo ratings yet
- Biofluid Assignment 3Document6 pagesBiofluid Assignment 3Dina AssefaNo ratings yet
- O o o o o o o o o o o oDocument9 pagesO o o o o o o o o o o oAshish PandeyNo ratings yet
- Angioplasty and Vascular StentingDocument8 pagesAngioplasty and Vascular Stentingrajnishpathak648No ratings yet
- Invasive Blood Pressure Monitoring: Group MembersDocument88 pagesInvasive Blood Pressure Monitoring: Group Membersallenshanique1999No ratings yet
- Common Procedures in Paediatric IcuDocument17 pagesCommon Procedures in Paediatric IcuNeethu Mariya MathewNo ratings yet
- Heart CareDocument14 pagesHeart CareArman CareNo ratings yet
- Central Venous LinesDocument34 pagesCentral Venous LinesManny TrujilloNo ratings yet
- Coronary Angiogram and Percutaneous Coronary InterventionDocument9 pagesCoronary Angiogram and Percutaneous Coronary Interventionellaine0024100% (2)
- Placement of Subclavian Venous CathetersDocument36 pagesPlacement of Subclavian Venous CathetersCourtneykdNo ratings yet
- CVPNSGDocument19 pagesCVPNSGmalathiNo ratings yet
- Vascular AccessDocument48 pagesVascular AccessJason Samuel Fredrick80% (5)
- DR Tarun BhatnagarDocument40 pagesDR Tarun Bhatnagararhim aljalyNo ratings yet
- Acesso VenosoDocument4 pagesAcesso VenosoAnderson AmaralNo ratings yet
- Venous and Arterial Catheterization: General PrinciplesDocument22 pagesVenous and Arterial Catheterization: General PrinciplesTibin JosephNo ratings yet
- Central Venous CatheterizationDocument71 pagesCentral Venous CatheterizationNobel LaureateNo ratings yet
- UVC NewbornDocument6 pagesUVC NewbornMani VachaganNo ratings yet
- Oncology - Presentation EditedDocument71 pagesOncology - Presentation EditedSarah Racheal AkelloNo ratings yet
- Lumbar puncture senDocument6 pagesLumbar puncture senNeethupaulNo ratings yet
- Sop of Doing Inavsive Line (Ijv) in IcuDocument12 pagesSop of Doing Inavsive Line (Ijv) in Icuqc.carcinovaNo ratings yet
- Basic Ward ProceduresDocument209 pagesBasic Ward ProceduresNoopur SawarkarNo ratings yet
- Central Venous PressureDocument4 pagesCentral Venous Pressuremike_steven12No ratings yet
- Central Venous Pressure Monitoring.: DR Jyothsna Chairperson DR Sunil ChhabriaDocument24 pagesCentral Venous Pressure Monitoring.: DR Jyothsna Chairperson DR Sunil ChhabriaPriyanka MaiyaNo ratings yet
- Angiographic ThoracalisDocument22 pagesAngiographic ThoracalisermaendahNo ratings yet
- Subclavian Vein Catheterisation - Techniques and ComplicatonsDocument15 pagesSubclavian Vein Catheterisation - Techniques and ComplicatonsRaghavendra PrasadNo ratings yet
- Daftar Isi TesisDocument8 pagesDaftar Isi TesisArifHidayatNo ratings yet
- Coronary AngiogramDocument58 pagesCoronary AngiogramEllaine Jennel100% (3)
- Peripheral Venous Peripheral Venous Cannulation Cannulation Cannulation CannulationDocument45 pagesPeripheral Venous Peripheral Venous Cannulation Cannulation Cannulation CannulationKarthik SNo ratings yet
- Emergency Procedures: - Defibrillation in CPRDocument20 pagesEmergency Procedures: - Defibrillation in CPRDuy Phương NguyễnNo ratings yet
- Central Venous AccessDocument20 pagesCentral Venous AccessCarlos GuerreroNo ratings yet
- Cateter Venoso Central PDFDocument37 pagesCateter Venoso Central PDFClaris PachecoNo ratings yet
- Intra-Arterial Catheterization For Invasive Monitoring: Indications, Insertion Techniques, and Interpretation - UpToDateDocument40 pagesIntra-Arterial Catheterization For Invasive Monitoring: Indications, Insertion Techniques, and Interpretation - UpToDatejuanpbagurNo ratings yet
- Access Vascular FOR Hemodialysis: Dr. Sahal Fatah, SP - BTKVDocument28 pagesAccess Vascular FOR Hemodialysis: Dr. Sahal Fatah, SP - BTKVAnonymous wVgEAr6No ratings yet
- Cardiac Surgical Operative AtlasFrom EverandCardiac Surgical Operative AtlasThorsten WahlersNo ratings yet
- Todentj 2 73Document6 pagesTodentj 2 73naveenNo ratings yet
- Acute Naphthalene Poisoning Following The Non-Accidental Ingestion of MothballsDocument4 pagesAcute Naphthalene Poisoning Following The Non-Accidental Ingestion of MothballsnaveenNo ratings yet
- Management of Life-Threatening Acid-Base DisordersDocument10 pagesManagement of Life-Threatening Acid-Base DisordersnaveenNo ratings yet
- Consent For Diagnostic And/or Therapeutic ParacentesisDocument2 pagesConsent For Diagnostic And/or Therapeutic ParacentesisnaveenNo ratings yet
- Medical Management of Renal Stone: Review ArticleDocument4 pagesMedical Management of Renal Stone: Review ArticlenaveenNo ratings yet
- BAMS Students AdmittedDocument3 pagesBAMS Students AdmittednaveenNo ratings yet
- A Woman, Age 35, With New-Onset Ascites: Symptoms To DiagnosisDocument6 pagesA Woman, Age 35, With New-Onset Ascites: Symptoms To DiagnosisnaveenNo ratings yet
- FluDocument31 pagesFluSheril Sularte CasanesNo ratings yet
- Brain Cancer Vaccine Succeeds at Prolonging Survival in Phase 3 TrialDocument1 pageBrain Cancer Vaccine Succeeds at Prolonging Survival in Phase 3 TrialGlen RosselliNo ratings yet
- Pgi OpdDocument22 pagesPgi OpdajaydevmalikNo ratings yet
- NCH Safe Pregnancy BrochureDocument6 pagesNCH Safe Pregnancy BrochurenehahNo ratings yet
- Drugs:: Side Effects of Psychotropic MedicationsDocument32 pagesDrugs:: Side Effects of Psychotropic MedicationsMARIE ROSE L. FUNTANARNo ratings yet
- Presentation 11Document14 pagesPresentation 11stellabrown535No ratings yet
- GI MAP Interpretive GuideDocument52 pagesGI MAP Interpretive GuidedulceomNo ratings yet
- Management of Myelofibrosis: Alessandro M. VannucchiDocument9 pagesManagement of Myelofibrosis: Alessandro M. VannucchifrnksusNo ratings yet
- Weighing Babies On The Postnatal WardsDocument6 pagesWeighing Babies On The Postnatal WardsCallithya BentleaNo ratings yet
- Reflection On Bipolar DisorderDocument2 pagesReflection On Bipolar DisorderLaila GabrielNo ratings yet
- Assessment On Basic Post-Operative Tracheostomy Care in Intensive Care UnitDocument7 pagesAssessment On Basic Post-Operative Tracheostomy Care in Intensive Care UnitmochkurniawanNo ratings yet
- Re Sum MeDocument3 pagesRe Sum Medrckc821969No ratings yet
- HematocritDocument3 pagesHematocritMaybelle Acap PatnubayNo ratings yet
- Preparing For EnemaDocument11 pagesPreparing For Enemapassion26100% (1)
- Respiratory Quotient: Method of Determination: USING RESPIROMETERDocument4 pagesRespiratory Quotient: Method of Determination: USING RESPIROMETERNeethi KrishnanNo ratings yet
- Hypertension in Geriatrics 2010Document51 pagesHypertension in Geriatrics 2010Andre HawkNo ratings yet
- London Cancer Lung Radiotherapy Guidelines 2013 v1 0Document24 pagesLondon Cancer Lung Radiotherapy Guidelines 2013 v1 0Cosmin SaftaNo ratings yet
- تجميعات شهر مارس EmsDocument11 pagesتجميعات شهر مارس EmsMohamed MahmoudNo ratings yet
- Bihar HospitalDocument4 pagesBihar Hospitalmahwish khanNo ratings yet
- Pediatric Readiness Guidelines ChecklistDocument4 pagesPediatric Readiness Guidelines ChecklistsabirNo ratings yet
- Consanguinity As A Significant Risk Factor For Diabetes Mellitus: A Systematic ReviewDocument8 pagesConsanguinity As A Significant Risk Factor For Diabetes Mellitus: A Systematic ReviewIJAR JOURNALNo ratings yet
- NCP Nursing Care Plans For Aplastic AnemiaDocument3 pagesNCP Nursing Care Plans For Aplastic AnemiaTahir Ali0% (1)
- Morphometric Study of Frontal Horn of Lateral Ventricles of The Brain by Computed Tomography in Western Up PopulationDocument6 pagesMorphometric Study of Frontal Horn of Lateral Ventricles of The Brain by Computed Tomography in Western Up Populationrhegi isdiara FairuzNo ratings yet
- Auscultation of Fetal Heart RateDocument2 pagesAuscultation of Fetal Heart Rateraul nino MoranNo ratings yet
- Chapter 23: RadiologyDocument23 pagesChapter 23: RadiologypoddataNo ratings yet
- Dracunculus Medinensis Better Known As Guinea WormDocument2 pagesDracunculus Medinensis Better Known As Guinea WormTeresa SilvaNo ratings yet
- Neuro Linguistic Programming and Application in Treatment of Phobias 2010 Complementary Therapies in Clinical PracticeDocument5 pagesNeuro Linguistic Programming and Application in Treatment of Phobias 2010 Complementary Therapies in Clinical Practiceihlus_fardan89No ratings yet
- Physical Therapist: Entry Level: Please NoteDocument3 pagesPhysical Therapist: Entry Level: Please NoteMafe DiazNo ratings yet