Professional Documents
Culture Documents
Indomethacin Is The Drug of Choice For Closing
Indomethacin Is The Drug of Choice For Closing
Uploaded by
Ramos, Janica De VeraOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Indomethacin Is The Drug of Choice For Closing
Indomethacin Is The Drug of Choice For Closing
Uploaded by
Ramos, Janica De VeraCopyright:
Available Formats
MATERNAL AND CHILD HEALTH NURSING LECTURE
CONGENITAL HEART ANOMALIES A. DEFECTS WITH INCREASED PULMONARY BLOOD
A. CONGENITAL HEART DISEASES FLOW
Review the Fetal Circulation
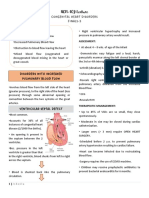
• Ductus venosus: carries oxygenated blood from PATENT DUCTUS ARTERIOSUS (PDA)
the placenta to the inferior vena cava; it by passes n This is the failure of the ductus arteriosus to close;
the liver; it closes at 8-weeks of life characterized by machinery murmurs and wide
• Ductus Arteriosus: bypasses flow of blood pulse pressure
through lungs by shunting oxygenated blood from n This allows a portion of oxygenated blood from
pulmonary artery to aorta; it closes at 7-10 days the left heart to flow back to the lungs by flowing
after birth from the aorta, which has a higher pressure, to
• Foramen ovale: connects right and left atria; the pulmonary artery
allows blood flow from right atrium (RA) to left n It causes congestive heart failure (CHF)
atrium (LA); bypasses the right ventricle (RV) and n Acyanotic
pulmonary circuit; closes by 2 to 3 months n Pulmonary vascular congestion is the risk.
Indomethacin is the drug of choice for closing
THE NORMAL HUMAN CIRCULATION the PDA
• superior vena cava and inferior vena cava
• Right Atrium VEBTRICULAR SEPTAL DEFECT (VSD)
• Tricuspid valve n Most common CHD characterized by abnormal
• Right Ventricle opening between the left and the right ventricles.
• Pulmonary valve n This results to right sided CHF because the blood
• Pulmonary Artery shunts from the left side of the heart (higher
• Lungs for oxygenation pressure) to the right side of the heart (lower
• Pulmonary veins pressure).
• Left Atrium n This results failure to thrive (FTT) due to
• Mitral valves decreased oxygenation and metabolism
• Left ventricle S&SX
• Aortic valve o Patient will have an increased RR; dyspnea;
• Aorta easy fatigability- these are signs that patient is
• To different parts of the body developing CHF
Failure to thrive
Organic: the body cannot cope up with the normal G&D;
poor nutrition
Nonorganic: caused by a certain disease; ventricular
septal defect
ATRIAL SEPATAL DEFECT (ASD)
n This is characterized by abnormal opening
between the left atria and right atria
n This results to right-sided CHF (shunting of blood
from the left to the right side of the heart
n Prepare child for x-ray and echocardiogram-
these are generally performed to demonstrate if
there is an increase in the size and location and
size of the defect
1 CONGENITAL HEART DISEASE
MATERNAL AND CHILD HEALTH NURSING LECTURE
B. OBSTRUCTIVE DEFECTS TRANSPOSITION OF THE GREAT VESSELS
n This is characterized by exchange of position of
COARCTATION OF AORTA the aorta and the pulmonary artery the aorta is
n This is presence of narrowing in the aorta located in the right ventricle, and the pulmonary
artery is located in the left ventricle. This is a
S&SX mixed defect
o HPN in the upper extremities; lower BP in the n Two- non communicating circulations
lower extremities; weak or absent pulse in the n There is severe cyanosis upon birth
lower extremities
o acyanotic COLLABORATIVE MANAGEMENT FOR CHILDREN
Surgical treatment: WITH CARDIOVASCULAR DEFECTS
o removal of the coarctation or balloon angioplasty o Monitor VS, respiratory status, I and O , and
weight
AORTIC STENOSIS o Administer O2 therapy (100% oxygen by face
n This is the narrowing of the aortic valve mask) to improve tissue oxygenation
n It leads to left side congestive heart failure o During hypercyanotic spells, place the infant in
knee-chest position
PULMONIC STENOSIS o Administer morphine sulfate as prescribed to
n this narrowing of pulmonic valve. It leads to reduce cardiac workload
right-sided congestive heart failure o Indomethacin to close PDA as prescribed
o Provide adequate nutrition. Malnutrition occurs
C. DEFECT WITH DECREASED PULMONARY BLOOD due to decreased metabolism that results from
FLOW inadequate tissue oxygenation
o Administer IV fluids as prescribed
TETRALOGY OF FALLOT: o Provide adequate rest. To reduce oxygen
4 defects namely: demands of tissues
1. pulmonic stenosis o Poor feeding and activity intolerance are
2. ventricular septal defect common in children with congenital heart disease
3. overriding aorta (the aorta is located in the right o Surgery to correct the defects. This is the most
ventricle together with the pulmonary artery. The definitive treatment
aorta transports a combination of oxygenated
and unoxygenated blood CARE OF CHILD BEFORE CARDIAC SURGERY
4. right ventricular hypertrophy: the right ventricle ² VS for baseline values
enlarges to accommodate increased workload ² Accurate height and weight are also recorded
caused by shunting of blood from the left to the ² Laboratory values must be checked specially
right ventricle due to the presence of VSD chemistry hematology and coagulation values
² Blood products must be typed and
² The child with TOF experiences “Tet spell” or cross-matched
hypoxic episode. This child should be put into ² Pregnancy test for girls who are menstruating
“knee-chest” position to improve return f blood ² Informed consent must be secured for
from lower extremities to the heart-thereby anesthesia and surgery
improving the cardiac output and tissue ² Prepare parents for the amount of equipment that
oxygenation. To older children the “squatting” will surround the child after the surgery such as
position is typical to compensate for hypoxemia cardiac monitor Oxygen tanks, IV equipment,
² Primary clinical manifestation of acute cyanosis chest tube, ventilator and the noise these
or tet spell in TOF is anxiousness and irritability machines may bring.
2 CONGENITAL HEART DISEASE
MATERNAL AND CHILD HEALTH NURSING LECTURE
² Discuss the surgical procedure to parents and • Ensuring the suction control chambers
with the child to lessen worries and answer are filled or set for the ordered amount of
misconceptions suctioning. If a fluid filled system, ensure
² Discuss coughing and deep breathing exercise bubble are in the chamber
and use of spiromentry during post op should be • Ensure the water seal chamber is filled
discussed preoperatively to manufacturer’s recommended level
² Take parents and older children to the ICU where • Monitoring for bubbles in the water seal
they will return after surgery and show the chamber which can indicate either a leak
equipment that will surround them in the drainage system or an air leak
from the patient’s lungs.
CARE OF CHILD AFTER CARDIAC SURGERY • Assessing and documenting the amount
² Taking accurate vital signs is essential in the color and consistency in the drainage
immediate post-operative period system routinely and as ordered. Report
² Continuous cardiac monitoring and assisted any drainage that changes in volume
ventilation with endotracheal intubation is color or bloodiness
frequently necessary • Keep tubes freely draining, do NOT milk
² Hemodynamic monitoring through the central or rub the tubes
venous catheter to carefully evaluate the preload • Ensure adequate pain control that
will help determine which type of therapy is allows the child to be awake and
necessary interactive
² IV fluids monitored NURSING INTERVENTIONS WHEN INFANT IS IN THE
ROUTINE CARE UNIT
NURSING INTERVENTION • Watch out for blood loss
o Endotracheal suctioning is necessary to prevent • Prevent infection
obstruction of the tube • Maintain lung expansion
o Assist with the chest physiotherapy to help lung • Encourage mobility
secretion mobile • Encourage healthy eating
o As soon as the ET tube and ventilator are • Include family in care
removed encourage the child to cough and
breathe deeply and use and incentive spirometer NURSING INTERVENTION
at hourly interval to mobilize secretions. a. PREVENT INFECTION
o Coughing and Deep breathing may be painful – Antibiotic therapy for 24 to 48 hours after
post-op so pain relievers are given as prescribed chest closure
o Teach children how to use pillow as splint while – Check the surgical incision site and the
coughing and deep breathing points of insertion for possible beginning
o Be certain parents understand that games infection
blowing cotton or bubbles using the incentive – Let infant wear shirts and bibs when feeding
spirometer as important exercises to help to prevent formula from dropping into the
achieve lung expansion incision site
o Chest tube drainage is attached to allow the b. MANAGE PARENTAL ANXIETY
drainage and collection of fluid or air from the – Encourage child to be out of bed and
chest but also to prevent air or fluid from ambulate once they are hemodynamically
returning to the chest stable and free from cumbersome equipment
• Keep the system closed and below – Encourage parents to participate in the care
chest level of their child (feeding breathing exercises
and ambulating)
3 CONGENITAL HEART DISEASE
MATERNAL AND CHILD HEALTH NURSING LECTURE
– Show to parents how to pick up child properly is snug and intact and no bleeding is present.
by placing hand behind the neck and n Reassess site after first ambulation and then a
scooping under the buttocks. minimum of 4 hourly prior to discharge.
– To prevent pain, do not pull the child’s arms n Patients should be kept lying flat for several
when attempting to carry an older child hours after the procedure so that any serious
– Use seatbelts at car seats to ensure safety bleeding can be avoided and that the artery can
– Do not place child on prone heal.
n It is advised that diagnostic catheterisation
CARE OF THE CHILD AFTER CARDIAC SURGERY patients are kept on bed rest for four hours, and
² The child should avoid the following: interventional catheterisation patients stay on
– Outside play or activities for 6 weeks. To bed rest for six hours.
prevent trauma and healing of the incision.
– Crowd for 2 weeks. To prevent development NURSING INTERVENTION
of infections a. Priority nursing intervention here is to prevent
– Activities that could cause fall (e.g. bleeding at the puncture site. Apply direct
bike-riding) for 4 to 6 weeks pressure to the catheterization site for at least 15
– Creams, lotions, or powders on the incision minutes, IF bleeding should occur at the insertion
until healed. To prevent infection site.
– Submersion underwater in tub or pool b. Distal pulses will be checked to ensure peripheral
– The child usually allowed to return to tissue perfusion. If a pulse cannot be palpated a
school after 3 weeks Doppler should be used. Notify physician for
– Advise parents to discipline child any loss of pulses
normally and avoid over protectiveness. c. An anticoagulant maybe initiated as ordered
This allows normal growth and d. Provide detailed education regarding the
development of the child. symptoms of an infection to the family.
– Dental visit should be done every 3 months e. Sponge bath is recommended or quick shower.
after age 3 years. To prevent dental caries Submersion to tub baths or pools are strictly
which may harbor microorganisms prohibited.
especially streptococcus (Group A
beta-hemolitic streptococcus may trigger CONGESTIVE HEART FAILURE (CHF)
autoimmune response that causes n Congestive heart failure (CHF) is a condition in
rheumatic heart disease which the heart does not pump as well as it
– Emphasize to parents the importance of should. The most common symptoms in
regular follow-up care for the child young children are difficulty feeding,
– Assistance with dressing and bathing for sweating and poor weight gain. Older children
several weeks buti will soon independent may present with fatigue and exercise
again. intolerance
n Clinical manifestations of CHF is tachypnea,
CARDIAC CATHETERIZATION dyspnea, fatigue
n is a procedure used to diagnose and treat certain n Edema due to poor circulation of blood
cardiovascular conditions secondary to heart failure, edema increases
n A long thin tube called a catheter is inserted in an weight
artery or vein in groin, neck or arm and threaded
through blood vessels to heart
n Assess puncture site 30 minutely for 4 hours then
hourly until ambulation. Ensure that the dressing
4 CONGENITAL HEART DISEASE
MATERNAL AND CHILD HEALTH NURSING LECTURE
confusion, anxiety, or hallucinations,
halos around bright objects; (fast,
forceful heartbeats in an irregular
rhythm) weakness
n Instruction of cardiopulmonary resuscitation (cpr)
increases parental confidenc and prapare thento
handle emergency
HYDROCEPHALUS
n It is caused by an imbalance in the production
and absorption of CSF in the ventricular
PRIORITY NURSING DIAGNOSIS system. When production is greater than the
o Decreased Cardiac Output: Inadequate blood absorption, CSF accumulates within the
pumped by the heart to meet metabolic demands ventricular system, usually under increased
of the body pressure producing passive dilatation of the
§ Administer Digoxin (Lanoxin) ventricles. It is detected through prenatal
Increases contractility of the heart sonogram
and force of contraction Two types:
§ provide optimum rest and good 1. COMMUNICATING hydrocephalus
Oxygenation (Extraventricular)
o The child may tire easily: n This is due to impaired absorption of CSF
§ Provide nipples of their bottles with within the subarachnoid space (due to
easy-to suck nipples malformations, tumors, hemorrhage, infection,
§ Eating may tire the child easily, so it trauma) .
should be not more than 45 minutes n Ventricles communicate
§ Do not give large meals at feeding time
§ Organize nursing interventions in such a 2. NON-COMMUNICATING hydrocephalus
way that the child will have an (Intraventricular)
uninterrupted rest and sleep periods n This is due to obstruction of CSF flow within the
to reduce cardiac demands and ventricular system.
workloads n The ventricles do not communicate
§ Diet is low sodium, high calorie
3 MAIN REASONS WHY CSF ACCUMULATES:
DIGOXIN THERAPY 1. Overproduction of fluid by the choroid plexus in
n stronger heart contraction, edema is gradually the first or second ventricle as could occur from a
resolved because of better circulation growing tumor (rare).
n Digoxin increases the force of contraction of the 2. Obstruction of the passage of fluid in the
muscle of the heart by inhibiting the activity of narrow aqueduct of Sylvius (most common) or
an enzyme (ATPase) that controls movement of the foramina of Magendie and Luschka, the
calcium, sodium, and potassium into heart openings that allow fluid to leave the 4th ventricle.
muscle. Inhibiting ATPase increases calcium 3. Interference with the absorption of CSF from
in heart muscle and therefore increases the the subarachnoid space if a portion of the
force of heart contractions. subarachnoid membrane has been removed (like
n Digoxin toxicity: surgery of meningocele or extensive
o Early signs: lack of appetite, nausea, subarachnoid hemorrhage)
vomiting, or diarrhea; headache,
5 CONGENITAL HEART DISEASE
MATERNAL AND CHILD HEALTH NURSING LECTURE
ASSESSMENT OF HYDROCEPHALUS motor function becomes impaired because of
• Rapid head growth both neurologic impairment and atrophy caused
• Bulging fontanels by the inability to move such a heavy head.
• Dilated scalp veins n Skull x-ray will reveal the separating sutures and
• Separated sutures thinning of the skull
• MacEwan sign (cracked pot sound on n Transillumination will reveal that the skull is filled
percussion with fluid rather than solid brain tissue
• Thinning of skull bones
• Frontal enlargement (bossing) THERAPEUTIC MANAGEMENT
• “sunset eyes” o IF CAUSED BY OVERPRODUCTION OF CSF:
• Child shows signs of increased intracranial – Acetazolamide (Diamox) a diuretic may
pressure such as decrease pulse and respiration, be prescribed to promote the excretion
increased temperature and blood pressure, of the excess fluid
hyperactive reflexes, strabismus and optic – Destruction of a portion of the choroid
atrophy plexus may be attempted by ventricular
• Irritable or lethargic with typical shrill, high pitched endoscopy; if a tumor is responsible for
cry the overproduction of CSF the tumor
should be removed
MACEWEN'S SIGN OR MACEWEN SIGN o IF CAUSED BY OBSTRUCTION
n is a sign used to help to diagnose hydrocephalus] – Shunting procedure
(accumulation of excess cerebrospinal fluid) and
brain abscesses. Tapping (percussion) the skull NURSING INTERVENTION PRE-OPERATIVELY
near the junction of the frontal, temporal and a. Assess if infant is able to turn freely because of
parietal bones will produce cracked pot sound. increased head size
Positive test is indication of separated sutures. b. Provide an environment for child that is
This is due to raised intracranial tension. stimulating yet not tiring
n The “setting sun” sign is an ophthalmologic c. Arrange for consultation for mother with
phenomenon where the eyes appear driven neurosurgeon to discuss surgery and child’s
downward bilaterally. The inferior border of the prognosis
pupil is often covered by the lower eyelid,
creating the “sunset” appearance. This finding VENTRICULOPERITONEAL SHUNT (VP SHUNT)
is classically associated with hydrocephalus in INSERTION
infants and children n Involves threading a thin polyethylene catheter
under the skin from the ventricles to the
PAPILLEDEMA peritoneum. Fluid drains by this route from the
n a serious medical condition where the optic nerve ventricles to the peritoneum where it is absorbed
at the back of the eye becomes swollen. across the peritoneal membrane into the body
Symptoms can include visual disturbances, circulation--eventually reduces intracranial
headaches, and nausea. Papilledema occurs pressure.
when there is a build-up of pressure in or around n After VP shunt insertion, place the child in supine
the brain, which causes the optic nerve to swell; position with head of bed flat for the first 24 hours
Late sign of increased ICP to prevent too rapid reduction in CSF pressure.
n If surgery is anticipated, IV infusion should A rapid decrease in the size of the ventricles may
not be placed in a scalp vein in a child with cause subdural hematoma
hydrocephalus. n After 24 hours, the child may be turned to the
n As the head continues to enlarge the child’s unaffected side; may be put in semi-fowler’s
6 CONGENITAL HEART DISEASE
MATERNAL AND CHILD HEALTH NURSING LECTURE
position 10-20degree angle if there is sustained – Observe mother’s interaction with infant
increase in ICP and remind her that congenital disorders
occur in a proportion of all births for
Ventriculoperitoneal (VP) shunt complications unknown reasons
• include blockage and infection – early and – Review care of child and assure parents
prompt detection of shunt dysfunction is vital as healthcare providers can be contacted
delay can lead to markedly raised intracranial anytime if they have questions.
pressure, which may result to death. – Establish a convenient follow up care
• signs of shunt malfunction: (there is decreased appointment
absorption of CSF—due to blockage of VP or – Make referral for home care if needed.
infection/swelling Also refer parents to support group of
– Headaches. other parents of children with
– Vomiting. hydrocephalus
– Lethargy (sleepiness)
– Irritability. SPINAL CORD ANOMALIES
– Swelling or redness along the shunt • It is the failure of the neural tube to close
tract. • detected through amniocentesis and prenatal
– Decreased school performance. sonogram; characterized by elevated alpha-feto
– Periods of confusion. protein (AFP).
– Seizures • Degrees of Spinal cord anomalies: 1) Spina
• Monitor abdominal girth, enlargement of Bifida, 2) Meningocele , and 3)
abdominal girth signifies that the CSF is NOT Meningomyelocele
adequately absorbed in the abdominal cavity
1. SPINA BIFIDA OCCULTA
NURSING INTERVENTION POSTOPERATIVELY n The posterior portion of the lamina failed to close
a. Assess infant’s neurologic status postoperatively but the spinal cord or the meninges do NOT
including response to sound pupillary response protrude through the defect. The defect is not
increasing irritability or lethargy visible externally. It is characterized by skin
b. Position infant with head of bed slightly elevated; depression or dimple; port-wine angiomatous
prevent flexion or rotation of the head. Record nevi, dark tufts of hair, soft subcutaneous lipomas.
cerebral perfusion pressure as prescribed. It is simply a surface of bone is missing, and the
c. Assess head circumference and anterior spinal cord is intact
fontanelles for tenseness every 4 hours as
prescribed.
d. Document head circumference and appearance
of anterior fontanelles.
e. Observe how mother feeds the baby. Assist
mother and teach how to position the baby during
feeding
f. Monitor intake and output closely
g. Administer osmotic diuretic and corticosteroid as
prescribed
NURSING INTERVENTION
a. Psychosocial/Spiritual/ Emotional Need
2. MENINGOCELE– THE EXTERNAL SAC
7 CONGENITAL HEART DISEASE
MATERNAL AND CHILD HEALTH NURSING LECTURE
n (the three layers of meninges: pia mater needed.
arachnoid and the dura mater) protrude as a
circular mass, about the size of an orange ASSESSMENT
through the defect in the vetebral column. The • Discovery of increased AFP (alpha feto-protein)
protrusion generally occurs I the lower lumbar in amniotic fluid
and lumbosacral region, although it might be • Observe and record whether an infant born with
present anywhere along the spinal canal. The neural tube disorder has spontaneous movement
protrusion is either covered y a layer of skin or of the lower extremities
ore frequently only the clear dura mater. No • Asses the nature and pattern of voiding (whether
sensory or motor deficits accompany the disorder wet every 2-3 hours or continually wet). Infants
unless the membrane sack should rupture. without motor or sphincter control void
continually. This pattern is same for defecation.
MENINGOMYELOCELE • Differentiation is further established by CT scan
n most common birth defect affecting the central ultrasound or MRI.
nervous system and is viewed as the most
complicated birth defect
• Not only the meninges protrude through the THERAPEUTIC MANAGEMENT
vertebrae, but the spinal cord usually ends at the ² No surgical correction for Spina bifida occulta.
point of protrusion Just inform parents of the defect. They should
• Motor and sensory function is decreased or receive patient education so that they can
absent beyond this point. recognize more serious symptoms as the child
• The higher the defect is along the spine, the grows such as numbness weakness or pain
greater the degree of paralysis which may indicate a need for reevaluation.
• The child may have partial or complete paralysis, ² Immediate surgery is needed for Meningocele
partial or complete lack of sensation of the lower and encephalocele to replace the meninges and
extremities as well as loss of bowel and bladder to close the gap in the skin. This is done soon
control after birth if possible (within 24-48 hours) to
• Legs appear lax because infant cannot move prevent infection. Surgical risk: the child’s
them cognitive potential may be impaired; and if a
• Urine and stools continually dribble because of large portion of the meninges have to be
lack of sphincter control removed by the surgery—this could limit the rate
• Infant ay have accompanying Talipes disorder of absorption of CSF which could lead to build up
and developmental dysplasia of the hip of CSF and hydrocephalus.
• A hydrocephalus may also develop in ² Children with meningomyelocele have the same
• Many as 90% of these infants because of the lack surgery to return the meninges and close the gap
of sub arachnoid membrane in the skin surface—however complete or partial
paralysis of the lower extremities and loss of
ENCEPHALOCELE bladder and bowel function will not be resolved
n is a cranial meningocele, most often in the
occipital area of the skull but may occur as a NURSING INTERVENTION
nasal or nasopharyngeal disorder. Generally • Preoperative
covered by the skin. – Use sterile gloves and sterile linens when
n Transillumination of the sac will reveal whether caring for infants with either meningocele or
brain tissue is in the sac. A CT scan MRI or meningomyelocele
ultrasound will reveal the size of the skull – Use a sterile, wet, warm compress of saline,
disorder and help predict the extent of surgery antiseptic, or antibiotic gauze over the lesion
8 CONGENITAL HEART DISEASE
MATERNAL AND CHILD HEALTH NURSING LECTURE
to keep the sac moist. Add additional warm – Baby is placed on cardiorespiratory monitor
fluid as needed. and positioned on the abdomen until the
– Position infants carefully to prevent pressure skin incision has healed (about 7 days)
on the exposed meninges either in a prone – Continue same careful precautions against
position or supported on their side. Use rolled allowing urine or feces to touch the incision
blankets or diapers to support the back and area
prevent pressure on the lesion. Place folded – If defect repair is large and the risk of
diapers between legs to prevent skin picking up the infant is great, the infant may
surfaces from touching and rubbing in this be fed while lying on the side in an
position and to prevent hips from internally incubator or prone on a specialized bed
rotating. frame.
• Position infants on their abdomen will prevent – Raise infant’s head slightly by slipping a
urine and feces from flowing onto the lesion as folded diaper under it.
well as keeping the protruding meninges free – Do not pat/touch/stroke the incision area at
from pressure. anytime.
• Place a piece of plastic wrap below the • Continue to observe the child as well for signs of
protruding membranes on the child’s back to increased intracranial pressure such as bulging
prevent feces from touching the open lesion. fontanelles, variations in vital signs, neurologic
• Place a folded towel under the infants abdomen signs such as pupillary changes or behavioral
to help flex the infant’s hip while on prone position changes such as irritability or lethargy
to reduce pressure on the sac , and ensure good • Preserve skin integrity during preoperative and
leg position. Check if the infant’s leg is postoperative
comfortable in that position. – Reposition patient every 2 hours to prevent
• Make certain that the child is adequately warm. pressure ulcers
However do not put child under radiant heat – Use paper tape or stockinette for dressing
source because it may dry the lesion and cause changes or place a protective dressing
cracking. Use of incubator is advised for a better such as Stomahesive on the skin under the
heat source and allows the nurse to assess and area where the tape will touch.
monitor the lesion. – Change diaper frequently to prevent
• Watch out for any seepage of clear fluid from the excessive contact of acidic urine with skin
defect and should be reported promptly because
that is probably escaping CSF. If in doubt if fluid NURSING INTERVENTION
is urine or CSF check it against a glucose test a. Encourage parents to take infants to the places
strip: CSF will test positive for glucose whereas children normally accompany parents such as
urine or mucus will not. home relatives shopping or the zoo, because
• Monitor for any increase in head size, measure encouraging children to be as independent as
head circumference as prescribed in the possible as they grow helps them lead an active
preoperative to set a baseline to be used after life as possible
surgery. Mark with an indelible pen the scalp b. Teach parents how to perform passive exercises
above and below the tape measure over both to prevent muscle atrophy and formation of
ears and on the back of the scalp. contractures if a child has impaired lower
extremity motor control.
NURSING INTERVENTION c. Prepare parents emotionally for the possibility of
• Post-operative. use of crutches. Provide patient education
regarding the use of crutches
d. Teach parents to do a daily inspection of child’s
9 CONGENITAL HEART DISEASE
MATERNAL AND CHILD HEALTH NURSING LECTURE
lower extremities and buttocks for any area of • Otoscopic examination may show a level of fluid
irritation or possible infection behind the tympanic membrane and the malleus
e. When in use of wheelchair teach the patient to becomes prominent
press with their arms on the armrests to raise • No movement of typanic membrane (as there
their buttocks off the wheelchair seat at least would be normally)
once every hour to help provide adequate
circulation to the lower extremities. THERAPEUTIC MANAGEMENT
f. To ensure bladder emptying, an intermittent ² Analgesic, antipyretic, decongestants are
clean urinary catheterization technique may be prescribed
taught to parents (inserting a clean catheter
through the urethra into the bladder every 4
hours to drain urine) OTITIS MEDIA WITH EFFUSION
• On early school age, the child can learn to do n This occurs if Otitis Media become chronic
self-catheterization usually occurs to children 3 to 10 years old
• A drug such as oxybutynin chloride (Ditropan) n Epithelial cells of the middle ear begin to secret a
may improve bladder capacity and allow a child to thin watery mucus, becomes glue-like thick and
need less frequent catheterization tenacious
ACUTE OTITIS MEDIA n Some children claim a feeling of fullness or the
n Inflammation of the middle ear is one of the most sound of popping or ringing in the ears; partial
prevalent diseases of childhood loss of hearing 20 to 40dB because of the
n Causative organism: Streptococcus pnuemoniae; inability of the ossicles to function well
Haemophillus influezae; Streptococcus pyogens
n Occurs in children 6 to 36 months and then again THERAPEUTIC MANAGEMENT
at 4 to 6 years ² Control of allergy: antihistamine of decongestant
n Most susceptible groups: male children; Alaskan ² Tympanocentesis
and native American; those with cleft palate, and ² Tubal Myringotomy and insertion of myringotomy
infants who are formula-fed tubes for aeration
n Potentially serious disease of childhood because
permanent damage can occur to middle ear NURSING INTERVENTION
structures, leading to permanent hearing a. Suggest to mother to give prescribed
impairment antihistamine at bedtime. Urge child to sleep with
affected ear up.
ASSESSMENT b. Meet with EENT service to consult on cause of
• Child have cold or rhinitis and low grade fever for frequent otitis media
several days, the fever peaks to about 102F c. Instruct mother to administer acetaminophen
(38C) and sharp constant pain begins in one or every 4 hours or ibuprofen every 8 hours and
both ears how to instill saline nose drops
• Infant become extremely irritable and frequently d. Encourage mother to offer liquids and soft foods
tug or pull affected ear in an attempt to gain relief e. Educate the mother about the common
from pain characteristics of otitis media; reassure mother
• External ear is usually free of wax because the the infection will resolve without an antibiotic
warmth of inflammation and fever melts the wax f. Instruct mother to contact the clinic or healthcare
and moves it more readily out of the canal provider if there is no improvement within 24 to
• Tympanic membrane appears inflamed and 48 hours or if the child exhibits increased pain
reddened and may bulge forward into the external
canal
10 CONGENITAL HEART DISEASE
You might also like
- ACLSDocument61 pagesACLSmgthida935100% (1)
- Chapter 32 Assessment of Hematologic Function and Treatment ModalitiesDocument19 pagesChapter 32 Assessment of Hematologic Function and Treatment ModalitiesAira Anne Tonee Villamin100% (3)
- Medicine in Brief: Name the Disease in Haiku, Tanka and ArtFrom EverandMedicine in Brief: Name the Disease in Haiku, Tanka and ArtRating: 5 out of 5 stars5/5 (1)
- Nursing Care of The Child Born With Congenital Heart DisordersDocument3 pagesNursing Care of The Child Born With Congenital Heart DisordersElijah GarciaNo ratings yet
- Diagnosis Depend On: 1-Clinical Features: - Palpation - Auscultation 2 - CXR: - Chamber Enlargement - Plethoric LungDocument11 pagesDiagnosis Depend On: 1-Clinical Features: - Palpation - Auscultation 2 - CXR: - Chamber Enlargement - Plethoric LungYasir Al-KhateebNo ratings yet
- Congenital Heart DiseaseDocument6 pagesCongenital Heart DiseaseSamah KhanNo ratings yet
- Anak 2Document107 pagesAnak 2Nency PurmayaNo ratings yet
- Congenital Heart Defect EDITDocument57 pagesCongenital Heart Defect EDITnicholasacquah680No ratings yet
- Module No. Date: Topic:: Cues/Questions/ Keywords Notes Congenital Heart DisordersDocument28 pagesModule No. Date: Topic:: Cues/Questions/ Keywords Notes Congenital Heart Disordersanon ymousNo ratings yet
- 41 HLHS Ma AaDocument14 pages41 HLHS Ma AaVictor PazNo ratings yet
- Case Scenerio: DR Sourath Munir Malkani Fcps-Ii TraineDocument31 pagesCase Scenerio: DR Sourath Munir Malkani Fcps-Ii TraineSoonh ChannaNo ratings yet
- Cardiovasucular Problems in Children: Niranjana Shalini. M.SC (N) Assistant ProfessorDocument79 pagesCardiovasucular Problems in Children: Niranjana Shalini. M.SC (N) Assistant ProfessorNIRANJANA SHALININo ratings yet
- Tetralogyof FallotDocument43 pagesTetralogyof FallotAlyssa Marie100% (8)
- Acyanoticheartdiseases 180620040047 PDFDocument88 pagesAcyanoticheartdiseases 180620040047 PDFElijahNo ratings yet
- Acyanoticheartdiseases 180620040047 PDFDocument88 pagesAcyanoticheartdiseases 180620040047 PDFElijahNo ratings yet
- Acyanoticheartdiseases 180620040047 PDFDocument88 pagesAcyanoticheartdiseases 180620040047 PDFElijahNo ratings yet
- (I..) KMU Peads CardicDocument88 pages(I..) KMU Peads CardicMuhammadNo ratings yet
- Conginital Heart DiseaseDocument19 pagesConginital Heart DiseaseSanthosh.S.UNo ratings yet
- Congenital Heart Disorders (Acyanotic)Document53 pagesCongenital Heart Disorders (Acyanotic)Hannah LaputNo ratings yet
- CARDIOVASCULAR-DISEASE Cont.Document6 pagesCARDIOVASCULAR-DISEASE Cont.Kimberly Sharah Mae FortunoNo ratings yet
- Cyanotic Heart Disease 2. Mixed Blood FlowDocument2 pagesCyanotic Heart Disease 2. Mixed Blood FlowJessica Carmela CasugaNo ratings yet
- TOF (Pathophysiology)Document4 pagesTOF (Pathophysiology)Doreen Claire M. WallangNo ratings yet
- Final 3 Congenital Heart DisordersDocument15 pagesFinal 3 Congenital Heart DisordersCAÑADA, JOHANNELYN M.No ratings yet
- Presented by Dona Mathew MSC (N) Govt - College of Nursing KottayamDocument221 pagesPresented by Dona Mathew MSC (N) Govt - College of Nursing KottayamSumathi GopinathNo ratings yet
- Midterm PRT 2 A qq9Document33 pagesMidterm PRT 2 A qq9Reysel MonteroNo ratings yet
- Patent Ductus Arteriosus 6. Aortic Stenosis: Signs and Symptoms: Signs and SymptomsDocument3 pagesPatent Ductus Arteriosus 6. Aortic Stenosis: Signs and Symptoms: Signs and SymptomsKIANA LOUISE ROMANONo ratings yet
- Wk. 10 Alteration in Oxygenation 2 Student Copy 1Document88 pagesWk. 10 Alteration in Oxygenation 2 Student Copy 1evtabarangao8661qcNo ratings yet
- BF - PJB - Yaf Mel Tia NiaDocument20 pagesBF - PJB - Yaf Mel Tia NiaRoberto HutapeaNo ratings yet
- Obstructive LesionsDocument7 pagesObstructive LesionsMaikka IlaganNo ratings yet
- Atrial Septal Defect: Dr. AninditaDocument30 pagesAtrial Septal Defect: Dr. AninditaDadangNoviantoNo ratings yet
- Congenital Heart Defects - CyanoticDocument3 pagesCongenital Heart Defects - Cyanoticr5ss7pq9tpNo ratings yet
- Aortic StenosisDocument8 pagesAortic Stenosisdr.moni.co.ukNo ratings yet
- Midterm PRT 2aDocument24 pagesMidterm PRT 2aReysel MonteroNo ratings yet
- CME Cyanotic Heart DiseaseDocument38 pagesCME Cyanotic Heart DiseaseTan Zhi HongNo ratings yet
- Cardiovascular Disorders & PregnancyDocument6 pagesCardiovascular Disorders & PregnancyChelcee MagsinoNo ratings yet
- 2 - Dr. Winda Azwani, SpA (K) Basic Anatomy and Physiology of Cardiovascular SysDocument18 pages2 - Dr. Winda Azwani, SpA (K) Basic Anatomy and Physiology of Cardiovascular SysnudhakoNo ratings yet
- AcyanoticDocument3 pagesAcyanotic2AAQUINO, PRECIOUS ANGEL F.No ratings yet
- ucu-CHDs 240114 230618Document68 pagesucu-CHDs 240114 230618BrianNo ratings yet
- Pedia Cardio Lecture AidDocument5 pagesPedia Cardio Lecture AidStephanie Pearl AldaNo ratings yet
- Pericardial Diseases 3rd Yr BMTDocument38 pagesPericardial Diseases 3rd Yr BMT211941103014100% (1)
- AV - Congenital Heart DiseaseDocument10 pagesAV - Congenital Heart DiseasebakiralhamdaniNo ratings yet
- Heart-Failure OConnor 11 1Document8 pagesHeart-Failure OConnor 11 1Muhammad Iqbal Al-islamyNo ratings yet
- By: Jacqueline I. Esmundo, R.N.MNDocument32 pagesBy: Jacqueline I. Esmundo, R.N.MNdomlhynNo ratings yet
- Pulmonary Embolism: Here Is Where Your Presentation BeginsDocument39 pagesPulmonary Embolism: Here Is Where Your Presentation BeginsAsmaa ahmedNo ratings yet
- Cardio Vascular DisordersDocument62 pagesCardio Vascular DisordersUday Kumar100% (1)
- 22 Ventricular Septal DefectDocument26 pages22 Ventricular Septal Defectdhiraj parmarNo ratings yet
- Acyanotic Heart Diseases ASD-Atrial Septal DefectDocument5 pagesAcyanotic Heart Diseases ASD-Atrial Septal DefectPrincess LegansonNo ratings yet
- Congenital Heart Diseases.Document86 pagesCongenital Heart Diseases.Salman KhanNo ratings yet
- CHD by GetasewDocument35 pagesCHD by Getasewshimeles teferaNo ratings yet
- [20550464 - Echo Research and Practice] EDUCATIONAL SERIES IN CONGENITAL HEART DISEASE_ Echocardiographic assessment of left to right shunts_ atrial septal defect, ventricular septal defect, atrioventricular septalDocument16 pages[20550464 - Echo Research and Practice] EDUCATIONAL SERIES IN CONGENITAL HEART DISEASE_ Echocardiographic assessment of left to right shunts_ atrial septal defect, ventricular septal defect, atrioventricular septalFarida FaradillaNo ratings yet
- Pathophysiology Congenital Heart Disease-1Document54 pagesPathophysiology Congenital Heart Disease-1single_ladyNo ratings yet
- CCHDDocument69 pagesCCHDchebetnaomi945No ratings yet
- Case StudyDocument10 pagesCase StudyEMANUEL SAGUIPEDNo ratings yet
- Congenital Heart Disease - Part IDocument95 pagesCongenital Heart Disease - Part IMeraol HusseinNo ratings yet
- Cardio Day 1 TemplateDocument18 pagesCardio Day 1 TemplateMikeNo ratings yet
- Congenital Heart Disease NotesDocument7 pagesCongenital Heart Disease NotesFarisa Jane BanggoNo ratings yet
- Atrial Septal Defect (ASD) Dan Ventricular Septal Defect (VSD)Document10 pagesAtrial Septal Defect (ASD) Dan Ventricular Septal Defect (VSD)Anis Syafa'atul HusnaNo ratings yet
- CardioDocument8 pagesCardioThomas KearneyNo ratings yet
- Congenital Heart DiseaseDocument3 pagesCongenital Heart DiseaseKarisaNo ratings yet
- Acynotic Heart DiseasesDocument13 pagesAcynotic Heart DiseasesSimran JosanNo ratings yet
- JVP Rajesh - 2Document16 pagesJVP Rajesh - 2bminor7No ratings yet
- Pedia Quiz 3Document4 pagesPedia Quiz 34xh8f9mng7No ratings yet
- Instructional Module: IM-IST1 - 1-2NDSEM-2020-2021Document24 pagesInstructional Module: IM-IST1 - 1-2NDSEM-2020-2021Ramos, Janica De VeraNo ratings yet
- Case AnalysisDocument2 pagesCase AnalysisRamos, Janica De VeraNo ratings yet
- Reflect and Share From ExperiencesDocument3 pagesReflect and Share From ExperiencesRamos, Janica De VeraNo ratings yet
- AL1 Activity For IM5 DiagnosingLDS CoH 1Document1 pageAL1 Activity For IM5 DiagnosingLDS CoH 1Ramos, Janica De VeraNo ratings yet
- Reflect and Share From ExperiencesDocument2 pagesReflect and Share From ExperiencesRamos, Janica De Vera100% (1)
- Reflect and Share From ExperiencesDocument2 pagesReflect and Share From ExperiencesRamos, Janica De VeraNo ratings yet
- Restaurant Business Proposal TemplateDocument1 pageRestaurant Business Proposal TemplateRamos, Janica De VeraNo ratings yet
- Health Problems Common in ToddlersDocument10 pagesHealth Problems Common in ToddlersRamos, Janica De VeraNo ratings yet
- Communicable Non Communicable DiseasesDocument23 pagesCommunicable Non Communicable DiseasesRamos, Janica De VeraNo ratings yet
- Nih GrantDocument14 pagesNih Grantapi-649553353No ratings yet
- Tuberculosis: Mariana Ngundju AwangDocument23 pagesTuberculosis: Mariana Ngundju AwangansyNo ratings yet
- Family Planning Case StudyDocument5 pagesFamily Planning Case StudyBreen GreenNo ratings yet
- 39 HelminthiasisDocument87 pages39 HelminthiasisArlini Nurul YuliantiNo ratings yet
- Cancer Cell WebquestDocument4 pagesCancer Cell Webquestapi-327342342No ratings yet
- Au Di Minor Case Study Myasthenia GravisDocument17 pagesAu Di Minor Case Study Myasthenia Gravisapi-301816885No ratings yet
- GURPS 4e - Injury Template V4Document7 pagesGURPS 4e - Injury Template V4Luca LiperiNo ratings yet
- Laboratory Investigation Report::: Patient Name: Age/Sex:: Order Date Uhid: Ref. DoctorDocument2 pagesLaboratory Investigation Report::: Patient Name: Age/Sex:: Order Date Uhid: Ref. DoctorSanchita AdhikariNo ratings yet
- Hepatocellular CarcinomaDocument18 pagesHepatocellular CarcinomaIngrid González EfronNo ratings yet
- Neurology MnemonicsDocument2 pagesNeurology MnemonicsJan Taplin100% (1)
- Biology of Blood and Marrow Transplantation: PediatricDocument8 pagesBiology of Blood and Marrow Transplantation: PediatricMichael John AguilarNo ratings yet
- Eastern Equine Encephalitis (EEE) Stats For MassachusettsDocument3 pagesEastern Equine Encephalitis (EEE) Stats For MassachusettsGarrett QuinnNo ratings yet
- Acute PainDocument4 pagesAcute PainCuttie Anne GalangNo ratings yet
- KRAEPELIN Clinical PsychiatryDocument628 pagesKRAEPELIN Clinical Psychiatrylizardocd100% (3)
- Wa0029.Document6 pagesWa0029.anusha.veldandiNo ratings yet
- Congestive Heart Failure PDFDocument9 pagesCongestive Heart Failure PDFSheryl Ann Mae BombalesNo ratings yet
- 35 Golden Eye RulesDocument7 pages35 Golden Eye RulesJethro WuNo ratings yet
- Diagnosis Dan Resusitasi Pada Pasien Syok Perdarahan & Syok DehidrasiDocument29 pagesDiagnosis Dan Resusitasi Pada Pasien Syok Perdarahan & Syok DehidrasiAris Dwi RahimNo ratings yet
- Major Review: Primary and Secondary Lacrimal Canaliculitis: A Review of LiteratureDocument12 pagesMajor Review: Primary and Secondary Lacrimal Canaliculitis: A Review of LiteratureBernardo RomeroNo ratings yet
- PassPACES Ophthalmology For Station 5 of The PACESExaminationDocument2 pagesPassPACES Ophthalmology For Station 5 of The PACESExaminationIbrahim AbbassNo ratings yet
- Daftar Pasien Exitus Bayi Dan Anak Di RS HAM Dan RS CPL USU Jumat Pagi, 24 Mei 2024Document9 pagesDaftar Pasien Exitus Bayi Dan Anak Di RS HAM Dan RS CPL USU Jumat Pagi, 24 Mei 2024Putri Nahrisa NstNo ratings yet
- PDF TextDocument2 pagesPDF TextchnmthakurNo ratings yet
- Case StudyDocument7 pagesCase StudyAaron WallaceNo ratings yet
- Prevalence of Adentia in The Elderly and Development FactorsDocument4 pagesPrevalence of Adentia in The Elderly and Development FactorsCentral Asian StudiesNo ratings yet
- Skin LesionsDocument4 pagesSkin LesionsRose Marceline Patague TalubanNo ratings yet
- Nursing Care Plan Funds 2Document7 pagesNursing Care Plan Funds 2Yash RamawatNo ratings yet
- Blood Component TherapyDocument73 pagesBlood Component TherapySaikat Prasad DattaNo ratings yet
- Child Protection - Dr. GarciaDocument55 pagesChild Protection - Dr. GarciaGio GelilangNo ratings yet














































![[20550464 - Echo Research and Practice] EDUCATIONAL SERIES IN CONGENITAL HEART DISEASE_ Echocardiographic assessment of left to right shunts_ atrial septal defect, ventricular septal defect, atrioventricular septal](https://imgv2-2-f.scribdassets.com/img/document/540346879/149x198/de08a1f760/1710537255?v=1)
















































