Professional Documents
Culture Documents
Disturbances in Circulation
Disturbances in Circulation
Uploaded by
SHERIE ANNE BERNABE0 ratings0% found this document useful (0 votes)
10 views10 pages1. Congenital heart disease (CHD) is the most common birth defect, affecting around 1% of births. Common types include ventricular septal defects (VSD) and atrial septal defects (ASD).
2. An ASD is an abnormal opening between the atria that allows blood to flow from the left atrium to the right atrium, increasing oxygenated blood flow to the right side of the heart and lungs. Small defects may cause no symptoms, while larger defects can lead to heart failure.
3. Surgical repair with a patch is the treatment for ASD, closing the opening between the atria. Nurses educate parents on signs of heart failure or infection and prepare
Original Description:
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Document1. Congenital heart disease (CHD) is the most common birth defect, affecting around 1% of births. Common types include ventricular septal defects (VSD) and atrial septal defects (ASD).
2. An ASD is an abnormal opening between the atria that allows blood to flow from the left atrium to the right atrium, increasing oxygenated blood flow to the right side of the heart and lungs. Small defects may cause no symptoms, while larger defects can lead to heart failure.
3. Surgical repair with a patch is the treatment for ASD, closing the opening between the atria. Nurses educate parents on signs of heart failure or infection and prepare
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
0 ratings0% found this document useful (0 votes)
10 views10 pagesDisturbances in Circulation
Disturbances in Circulation
Uploaded by
SHERIE ANNE BERNABE1. Congenital heart disease (CHD) is the most common birth defect, affecting around 1% of births. Common types include ventricular septal defects (VSD) and atrial septal defects (ASD).
2. An ASD is an abnormal opening between the atria that allows blood to flow from the left atrium to the right atrium, increasing oxygenated blood flow to the right side of the heart and lungs. Small defects may cause no symptoms, while larger defects can lead to heart failure.
3. Surgical repair with a patch is the treatment for ASD, closing the opening between the atria. Nurses educate parents on signs of heart failure or infection and prepare
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
You are on page 1of 10
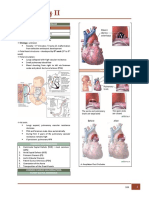
FETAL AND NEONATAL bundle branches
Purkinje fibers/ cells
4 temporary shunts (pathway)
• Terminal point in the conduction system
1.ductus arteriosus - becomes ligamentum
• Specialized to rapidly conduct impulses
arteriosum
through the thick walls of the ventricles
2.Ductus venosus – becomes ligamentum venosum • 30 to 40 impulses per
3.Foramen ovale – becomes ligamentum teres CONGENITAL HEART DEFECTS
(butas sa right ventricle and left atrium)
▪ Most common is VSD
4.Umbilical vessels art vein / umbilical arteries – ▪ Incidence: 1% of or about 40,000 births per
medial umbilical ligaments year
▪ 25% of babies with CHD are critical and
generally needs surgery or other
procedures in their 1st year of life (CDC)
▪ 15% of CHD are associated with genetic
conditions
▪ 28% of kids with CHD have another
recognized anomaly (trisomy 21,)
4 hemodynamic problems
Acyanotic (left to right shunting)
1.Increase of pulmonary blood flow
✓ Atrial septal defect
✓ Ventricular septal defect
✓ Patent ductus arteriosus
✓ Atrioventricular canal
2.Obstruction of blood flow from ventricle
Heart CONDUCTION SYSTEM
Sinoatrial Node (SA node) ✓ Coarctation aorta
✓ Aortic stenosis
• Primary pacemaker of the heart ✓ Pulmonic stenosis
• Inherent firing rate of 60 to 100 impulses per
minute Cyonotic (right to left shunting)
Atrioventricular Node (AV node) 3.Decrease of pulmonary blood flow
✓ Tetralogy of fallot
• Located in the right atrial wall near the
✓ Tricuspid atresia
tricuspid valve
*atresia (sarado)
Coordinates the incoming electrical
impulses from the atria and after a slight 4.Mixed blood flow
delay relays the impulse to ventricles
• 40 to 60 impulses per minute ✓ Transposition of great arteries
✓ Total anomalous pulmonary venous return
Bundle of His ✓ Truncus arteriosus
Specialized conducting tissue ✓ Hypoplastic left heart syndrome
Right bundle branch – conducting impulses to the (makipot,sarado na ang aorta)
right ventricle
Left bundle branch – conducting impulses to the left
ventricle
*Divides into the left anterior and posterior
Congenital heart disease (CHD) 2. NPO WITH IVF
Increased Pulmonary Blood flow (ACYANOTIC) 3. GET HEIGHT AND WEIGHT
1.ATRIAL SEPTAL DEFECT (ASD) 4. MARK THE PEDAL PULSES - DORSALIS AND
POSTERIOR TIBIAL PULSES
6. ORIENT CHILD AND PARENTS TO CC ROOM
POST CARDIAC CATHERIZATION
INTERVENTION
1.CHECK THE VITAL SIGNS
2.GIVE DIURETIC
3.CHECK PEDAL PULSES
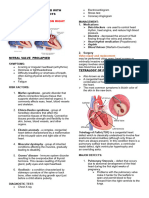
▪ Abnormal opening between atria → blood 4.IMMOBILIZE THE AFFECTED LIMB AMD
from higher pressure (LA) to flow into lower APPLY PRESSURE
pressure (RA).
▪ Increase O2 blood into R side of heart *Femoral artery 6-8 hours
RA & RV enlargement
*Femoral vein 4-6 hours
▪ Cardiac failure is unusual in uncomplicated
ASD *Open heart surgery - tatapalan yung butas gamit
▪ May be asymptomatic if small defect ang Teflon material
Dyspnea
▪ Fatigue and poor growth Medication
▪ Soft systolic murmur in pulmonic area 1.Cardiac glycoside (energy drug)
(splitting S2)
▪ May develop CHF Ex: lanoxin
▪ Surgical treatment: Surgical Dacron patch *Below 100 heart beats do not give lanoxin
closure
– Open repair with C-P bypass during 2.Duretics-lasix
school age
3.Antihypertensive
Non-surgical: may be closed using devices
during cardiac catheterization Nursing Management:
TYPES OF ASD • Explain to parents the purpose of tests and
procedures
ASD1 ostium primum - Ang butas ay below of
septum • Teach parents ways to support nutrition,
reduce stress on heart, promote rest, and
ASD2 ostium secundum- gitna ang butas support growth and development during
preoperative period
ASD3 sinus venosus - above ng septum ang
• Teach parents signs of congestive heart
butas
failure and infection
Cardiac catheterization • Prepare parents and child for surgery by
visiting intensive care unit, explaining
Purpose:
equipment and sounds
▪ Diagnostic • Prepare older child for post-operative
▪ Therapeutic/intervention experience, including coughing and deep
▪ Electrophysiologic studies breathing and need for movement
• Teach need for antibiotic prophylaxis to
PRE-CARDIAC CATHERIZATION prevent subacute bacterial endocarditis
INTERVENTION
1.BASELINE VITAL SIGNS
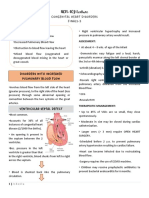
2.VENTRICULAR SEPTAL • DUCTUS closes because increase in
arterial oxygen concentration that follows
• Defect in ventricular septum – error in early
initiation of pulmonary function
fetal development
• Prostaglandin E leads to closure of PDA
• abnormal opening between the right and left
Allows blood to flow from left to right and
ventricles
pulmonary blood flow
• Can occur anywhere in muscle or
• No communication from pulmonary artery to
membranous ventricular septum
aorta
• 20-25% of all CHDs are VSD
• Small PDA: asymptomatic
• Pressure LV → RV and systemic arterial
• Bounding peripheral pulses
circulation resistance → pulmonary
• Widened pulse pressure (>25)
circulation, blood flows through the defect
• Loud machine-like murmur at upper left
and into the pulmonary artery
sternal border (Left intraclavicular area)
• RV becomes enlarged (Hypertrophied), over
• Complication for Large PDA: CHF with
time the RA may also become distended
tachypnea, dyspnea, and hoarse cry
• Symptoms:
• Definitive diagnosis: ECHO
Tachypnea, dyspnea
Medical
Poor growth, reduced fluid intake
(Premature) INDOMETHACIN to close
Palpable thrills
PDA’s; surgical ligation if meds fail
Systolic murmur at left lower sternal border
Prophylactic antibiotics to prevent bacterial
May develop CHF
endocarditis
• Medications:
Surgery >> between age 1-2
Furosemide: a diuretic which removes
year
excess fluid out of the body
Digoxin: helps the heart pump more 2 approaches:
forcefully
Angiotensin-converting enzyme (ACE) 1. Lateral sternotomy
inhibitor: relaxes blood vessels and help 2. Median sternotomy
heart to pump more easily
• Surgical repair with bypass (procedure of 4.OBSTRUCTIVE DEFECTS
choice) • Blood flow in heart meets an area of
• Pulmonary artery banding (if not too anatomic narrowing (stenosis) →
large) or patch obstruction to blood flow
• Eisenmenger syndrome - right to left • Pressure in ventricle & great arteries before
shunting of blood becomes cyanotic obstruction is increased; pressure in area
SMALL DEFECT VSD THERE ARE 2 OPTIONS beyond obstruction is
• Decreased
1. WAIT FOR SPONTANEOUS CLOSURE • Location of narrowing near the valve:
2. OPEN HEART SURGERY THE APPROACH IS Valvular: site of valve itself
PURSE-STRING Subvalvular: narrowing in vent below valve
(ventricular outflow tract)
LARGE DEFECT - OPEN HEART APPROACH Supravalvular: narrowing in great art
DACRON/TEFLON PATCH above valve
• (+) pressure load on ventricle – decrease
3.PATENT DUCTUS ARTERIOSUS (pda)
CO
• Ductus SHOULD close by about age 15 • s/s CHF
hours after birth • Mild obstruction: asymptomatic
• Some shunting of blood may occur up to 24 • Severe stenosis: hypoxemia (rare)
hours of life
5.COARCTATION OF AORTA
Descending aorta - kumikipot
UE/HEAD • Clinical manifestations:
Signs of decreased CO: faint pulses,
1.PINKISH
hypotension, poor feeding, tachycardia
2.BOUNDING PULSE Murmur; exercise intolerance
Chest pain, dizziness with standing
3.WELL DEVELOPED • Treatment
4.HEADACHE – Balloon angioplasty to dilate the valve;
Surgery: Konne procedure (valve
5.HIGH BP replacement)
LE • May require repeat procedures
1.CYANOTIC 7.PULMONARY STENOSIS
2. UNDERDEVELOPED • Pulmonary valve is stenosed
• Narrowing at entrance to pulmonary artery
3. CLOD CLAMMY SKIN >> R ventricular hypertrophy and decreased
pulmonary blood flow
4. LOW BP
• Extreme form of PS: Pulmonary atresia
Approach: (total fusion of the commissures and no
blood flow to lungs)
PGE1- Prostaglandin
• PS >> RVH, R ventricular failure >> R atrial
Cc - balloon angioplasty pressure increases and may reopen
foramen ovale
Valvotomy/valvuloplasty/ commissurotomy
• Shunts unoxygenated blood to L atrium >>
Signs of CHF in infants: systemic cyanosis
• May lead to CHF
• Condition can deteriorate rapidly • Often have PDA as well
• Older kids may complain of dizziness, • Cardiomegaly on CXR
headache, fainting and epistaxis from
hypertension • Treatment: Balloon angioplasty to dilate the
• Patient at risk for ruptured aorta, aortic valve
aneurysm, or stroke Surgical treatment – Breck procedure
• Treatment: non-surgical (Bypass to do valvotomy)
– balloon angioplasty. Usually, effective Usually, can repair with catheterization
• Surgical: does not require bypass since
defect is outside pericardium DEFECTS OF DECREASED PULMONARY
• Post-op complication is hypertension BLOOD FLOW (CYANOTIC)
Usually done before age 2 yrs. • Obstruction of pulmonary blood flow +
Risk of recurrence anatomic defect (ASD/ VSD) between R & L
6.AORTIC STENOSIS side of heart
• Difficulty of blood exiting R heart via
• Narrowing of aortic valve usually malformed pulmonary artery → increase R side
in BI- rather than TRI- cuspid valve pressure > L pressure
• Causes increased resistance in left → desaturated blood shunt R to L →
ventricle, decreased CO, L ventricular desaturated blood in systemic circulation
hypertrophy and pulmonary vascular • Hypoxemia, usually cyanotic
congestion
• L ventricular wall is hypertrophied>> 1.TETRALOGY OF FALLOT
increased pulmonary vascular resistance & four heart defects:
pulmonary hypertension
• LVH >> decrease coronary artery 1. Ventricular Septal Defect
perfusion & increase risk of MI 2. Pulmonary stenosis
3. Right ventricular hypertrophy Continuous infusion of PGE 1 until Sx
4. Overriding aorta Palliative: shunt (pulmonary-to- systemic art
• Hemodynamics vary widely anastamosis)
-Depends on extent of pulmonic valve Pulmonary artery banding
stenosis & size of VSD Modified Fontan procedure
-If VSD is large, pressures are equal in R
TATLONG SAKIT SA PUSO NA AGAD
and L ventricles. Blood is shunted in the
NANGINGITIM
direction of the least resistance (pulmonary
or systemic vascular resistance) 1. TRICUSPID ATRESIA - WALANG PAG
• PVR is > than systemic vascular resistance, DADAANAN NG DUGO MULA SA RIGHT ATRIUM
shunt will be R to L TO R VENTRICLE AND LUNGS
• Clinical manifestations: APPROACH:
• “TET SPELLS” or “blue spells” with acute - PGE1
episodes of cyanosis and hypoxia
Anoxic after feeding or with crying. *FONTAN PROCEDURE - Gumagawa ng
• RISK of emboli, LOC, sudden death, dugtungan sa pagitan ng right atrium to pulmonary
seizures artery
• Repairs: usually indicated when Tet spells *BI-DIRECTIONAL GLEN SHUNT - superior vena
and hyper cyanotic spells increase cava to pulmonary artery
Stage 1: Blalock or modified Blalock
shunt 2.TRANSPOSITION OF THE GREAT VESSELS -
>> blood to pulmonary arteries from L or R *Atrial switching either senning approach (enough
subclavian artery na yung pag dugtong) or mustard approach
Complete repair: usually in 1st year of life. (additional na pag dugtong)
Repair of VSD, resect stenosed area, and
patch R ventricular outflow\ 3.HYPOPLASTIC LEFT HEART SYNDROME
2.TRICUSPID ATRESIA MIXED DEFECTS
• Failure of tricuspid valve to develop • Survival on postnatal period depends on
• No communication from R atrium to R mixing of blood from pulmonary systemic
ventricle circulation within cardiac chambers
• Blood flows thru an ASD or a patent FO to L • Blood is mixed from pulmonary and
side of the heart thru a VSD to R ventricle to systemic circulations within the heart
lungs chambers >> Relative desaturation of blood
• Often associated with PS and TGS in systemic blood flow
• Complete mixing unO2 and O2 blood in L • Cardiac output decreases because of
side of the heart → systemic desaturation, volume load on ventricle
pulmonary obstruction • Signs of desaturation, cyanosis, and CHF,
→ decrease pulmonary blood flow but variable depending on anatomy
• At birth: presence of patent FO (or ASD) is • Degree of cyanosis not always visible &
required to permit blood flow across septum signs of CHF
into L atrium TGA: severe cyanosis in 1st day of life →
– PDA allows blood flow to pulmonary CHF (later)
artery for oxygenation Truncus arteriosus: severe CHF 1st few
• Manifestations: cyanosis, tachycardia, weeks of life and mild desaturation
dyspnea, hypoxemia, clubbing
1.HYPOPLASTIC LEFT HEART SYNDROME
At risk for bacterial endocarditis, brain
abcess, stroke • Left side of the heart is underdeveloped
• Treatment: NB – pulmonary blood flow • Left ventricle is small and aortic atresia
depends on PDA
• Most blood flows across patent foramen & pressure in the heart → MYOCARDIAL
ovale to R atrium – to R ventricle and out FAILURE
the pulmonary • Can occur with cardiomyopathy, dysrythmia,
• Descending aorta receives blood from the severe electrolyte imbalances
PDA to supply the systemic circulation • Could also be due to excess demands on a
• PDA closure >> rapid deterioration and CHF normal cardiac muscle (sepsis / severe
anemia)
• Treatment: Keep ductus open with
TYPE OF CONGESTIVE HEART FAILURE
Prostaglandin E infusion
Surgical Treatment: A. RIGHT SIDED HEART FAILURE
Norwood procedure to create a new aorta RV unable to pump blood to Pulmonary
using the main pulmonary artery and Artery → increased pressure in RA and in
creation of large ASD the systemic venous circulation Systemic
Bidirectional Glenn Shunt at 6-9 months venous HPN →
age to reduce volume load on the R hepatosplenomegaly
ventricle B. LEFT SIDED HEART FAILURE
Modified Fontan procedure, similar to – LV unable to pump blood to the systemic
Tricuspid atresia repair circulation → increased LA pressure and
Transplant may be an option for some pulmonary vv → congestion in lungs →
parts. Mortality rate is very high (30%- 50%) increased pulmonary pressure →
pulmonary edema → pulmonary HPN
2.TRANSPOSITION OF THE GREAT VESSELS
Signs and symptoms of CHF
• Pulmonary artery leaves the L ventricle and
the aorta exits from the R ventricle • Each side of the heart depends on the
• No communication between the systemic adequate function of the other
and pulmonary circulations • Failure of one chamber affects the opposite
• Must have PDA or Septal defect to permit chamber
blood flow • If not corrected, it may lead to cardiac
• Rare defect damage → inadequate CO → decreased
Furosemides, Thiazides, Spirinolactone supply to the kidneys → Na and H2O
Fluid restriction resorption → hypervolemia, increased
Sodium restriction workload on the heart, pulmonary and
• Decrease cardiac demands systemic
Bed rest, treat infection
CONGESTIVE HEART FAILURE in Children
Preserve body temperature; reduce effort of
Impaired myocardial function
breathing (semi-fowlers)
Tachycardia, fatigue, weakness, restless, pale, cool
Sedate an irritable child
extremities, decreased BP, decreased urine output
• Improve tissue oxygenation & decrease O2
Pulmonary congestion
consumption
Tachypnea, dyspnea, respiratory distress, exercise
O2 vasodilator
intolerance cyanosis, wheezes
Cool humidified O2
Systemic venous congestion
DISTURBANCES IN CIRCULATION Peripheral and periorbital edema, weight gain,
ACQUIRED CARDIOVASCULAR DISORDERS ascites, hepatomegaly, neck vein distention
1.CONGESTIVE HEART FAILURE CHF Treatment
• Inability of the heart to pump and adequate Goals:
amount of blood to the systemic circulation
• Improved cardiac function
at normal filling pressures to meet the
Digitalize – Digoxin
metabolic demands of the body
• Due to structural deformity in children
(septal defects) → increased blood volume
Increased CO, decreased size and venous • Staph aureus, strep viridians (most
pressure, relieve common), candida albicans, gram negative
edema bacteria
• Lanoxin (Pedia) – more rapid in onset • Enter blood system thru: dental (most
– Oral / IV doses x 24 hours followed by common), UTI, cardiac catheterization,
maintenance dose (BID) to maintain blood surgery, etc.
levels (Digitalizing Dose) • Organism in endocardium → vegetations
• ACE Inhibitors (Capoten / Enalapril) (verrucae) → fibrin deposits → platelet
(-) normal function of R-A system in kidney thrombi → invade adjacent tissues
Blocks conversion of AI to AII (Vasodilator) (mitral/aortic valves)
Captopril – can be given smaller doses → breaks off and embolize elsewhere
• Remove accumulated Fluid and Sodium (spleen, kidney, CNS) → death
✓ Diuretics – mainstay of treatment to • Diagnostics
eliminate excess H2O and salt ✓ Based on clinical manifestations
✓ Bidirectional glenn ✓ Blood c/s: definitive diagnosis
• Keep hct and blood viscosity within ✓ ECG/CXR (cardiomegaly)
acceptable limits (hydrate) ✓ Increased ESR, increased WBC,
• Monitor for anemia, Fe supplementation, anemia, microscopic hematuria
blood transfusion ✓ 2D-echo – vegetations, valve
• Respiratory infection or reduce pulmonary function
function can worsen hypoxemia • Clinical manifestation
✓ Aggressive pulmonary hygiene ✓ Insidious onset, unexplained fever
✓ CPT, antibiotics (low grade, intermittent)
✓ O2 ✓ Anorexia, malaise, weight loss
✓ Extracardiac emboli
OBJECTIVE IN THE MANAGEMENT OF CHF ✓ Splinter h’ge – thin black lines under
1. Increase myocardial contractility by giving nails
cardiac glucoside ✓ Osler nodes – red, painful,
intradermal nodes on pads of
2. Decrease fluid overload - diuretic/weighing phalanges
3. decrease oxygen demands - complete bed rest ✓ Laneway lesions – painless h’ges on
without bathroom privilege, do all nursing care panes and soles
✓ Petechiae on oral mucous membrane
4. Prevent respiratory infection - reposition ✓ May be present: CHF, dysrythmia,
new murmur
5. Collaboration with dietician
• Therapeutic management
6. Emotional support
✓ High dose antibiotics: Penicillin,
2.ENDOCARDITIS (Bacterial Infective ampicillin, methicillin, cloxacillin,
Endocarditis) streptomycin, or gentamycin
• BE, IE or subacute bacterial endocarditis ✓ IV/IM x 4 weeks at least
(SBE) ✓ Amphoterecin or flucytosine for
• Infection in valves and endocardium fungal infections
✓ Treat 2-8 weeks. If antibiotics is
• Sequelae of sepsis in child with cardiac
unsuccessful
disease of congenital anomaly
>> CHF develops, vulvular
• Affects children with valvular abnormalities,
damage
prosthetic valves, recent heart surgery with
✓ Should be instituted immediately
invasive lines and RHD with valve
✓ Blood c/s periodically to evaluate
involvement, drug abuse
response to antibiotics
✓ Prophylaxis before dental infection
procedures, bronchoscopy, T&A, MAJOR
surgeries, childbirth Carditis – tachycardia out of proportion to degree of
✓ Prophylaxis: 1 hour before fever
procedures (IV) or may use PO in
-Cardiomegaly, murmur, muffled heart sounds
some cases
-Pericardial friction rub, pericardial pain, changes in
✓ Family dentist should be advised of
existing heart problems ECG
-Involves endocardium, pericardium, and
3.Rheumatic Fever (RF) myocardium
» Most commonly the mitral valve
Inflammatory disease occurs after Group A Beta-
Polyarthritis
haemolytic streptococcal throat infection
- Arthritis is reversible and migrates, especially in
Self-limiting
large joints (knees, elbow, hips, shoulders, wrists)
– Affects joints, skin, brain,
- Swollen, hot, red, painful joints, after 1-2 days →
serious surfaces, and heart affects different joints
Risk factors:
Age and sex: (5-15 years old) female Clinical Manifestations (Modified Jones Criteria)
Housing and socioeconomic status MAJOR
Season: rainy season Erythma marginatum – rash
Genetic predisposition
• Transitory, non pruritic
4 affectations • Trunk and proximal portion of extremities
• Red macule with clear center wavy, well-
• Heart, pan carditis, joints - polyarthralgia
dermacated border
and SC nodules, skin - erythma
marginatum, cnd - syndenhams chore Subcutaneous nodules
Clinical Manifestations • Small nontender nodules
✓ Acute febrile-like illness (2-3 weeks after • Bony prominences – hands, feet, elbows,
streptococcal throat infection) scalp, scapulae, vertebrae
✓ Non-specific • Persistent indefinitely after onset of the
Fever disease and resolve with no resulting
Joint pain damage
Loss of appetite St. Vitus Dance – The Fifth Manifestation
Muscle ache (Sydenham’s
✓ Specific Chorea)
Joints (swelling and pain of larger joints like
knee, ankle, elbow and wrist occurring in • St. Vitus Dance (aka, chorea) reflects CNS
rapid succession – “migratory arthritis”) involvement
Heart (causes inflammation of the whole • Definition: Chorea refers to sudden, aimless
layers of the heart – PANCARDITIS) – movements of extremities, involuntary facial
Palpitation, chest pain, shortness of breath, grimaces, speech disturbances, emotional
leg swelling, etc. lability and muscle weakness
Skin & subcutaneous tissues (non-itching • Worse with anxiety and relieved by rest
macular rash and painless mobile nodules
MINOR
over joints and spines)
Central Nervous System (a late • Arthralgia
manifestation) – abnormal movements of • Fever
the limbs with muscle weakness and
emotional labiality.
Diagnostic approach: Modified Jones Criteria
2 major or 1 major + 2 minor manifestations + strep
LABORATORY • Stress parents and teachers: illness is
temporary and disappears in time
• Increased ESR, CRP
– Supporting evidence of antecedent group, Rheumatic Heart Disease (RHD)
A Strep Infection - Most common complication of RF
• Throat c/s, rapid Ag test - Damage to valves leading to stenosis or
• ASO titer (most reliable – 80% children) regurgitation with resultant hemodynamic dist.
• AntiDNAse. ESR, CRP
4.KAWASAKI DISEASE
ECG, CXR – evidence of heart involvement
• Mucocutaneous LN syndrome
TREATMENT
• Acute systemic vasculitis
Goals:
• < 5 y/o (Peak: toddlers)
✓ Eradication of haemolytic strep • Self-limiting but 20% children without
✓ Prevention of permanent cardiac treatment develop
damage
✓ Palliation of other symptoms
✓ Prevention or recurrence of RF
Prevention of RHD
Treatment of streptococcal tonsillitis / pharyngitis
✓ Penicillin G – IM x 1
✓ Penicillin V – oral x 10 days
✓ Sulfa – oral x 10 days Area involved: CVS
✓ Erythromycin (if allergic to above) – oral x Initially: Inflammation arterioles, venules,
10 days capilliaries → formation coronary artery aneurysm
Treatment of recurrent RF Death: result of coronary thrombosis or severe scar
– Same as above formation & stenosis of main coronary artery
Myocardial infarction from thrombosis
Salicylates (ASA) – control inflammatory process No specific diagnostic test
esp. joints, dec fever and discomfort IRRITABILITY – hallmark of Kawasaki Disease
Bed rest – during febrile phase but need not be Persists in 2 weeks
strict
Should be followed medically x 5 years at least
NURSING CONSIDERATIONS - Help family adjust to the disorder
- Educate family
• Encourage compliance with drug - Help family cope with effects of the disorder
• Encourage adherence to tx’c plan - Prepare child and family for surgery
(+) poor compliance: monthly injections
• Facilitate recovery from illness Surgical Interventions
• Provide emotional support - Open-Heart
• Prevent disease - Closed heart procedures
- Staged procedures
Interventions during homecare
- Prepare child and family for procedures
• Provide rest and adequate nutrition
Postoperative Care of the Child
• Once fever is over, resume moderate
activities, improve appetite - Monitor vital signs and A/V pressures
• Carditis: most disturbing and frustrating - Intraarterial monitoring of BP
manifestation - Intracardiac monitoring
• Gradual - Respiratory needs
• Mistaken for nervousness, clumsiness, - Rest, comfort and pain management
inattentiveness - Fluid management
• Limits physical activity - Progression of activity
Postoperative Complications
CHF – due to excessive pulmonary blood flow or
fluid overload
Hypoxia – inadequate pulmonary blood flow /
respiratory problems
Dysrythmias
- Early post op period
- Due to electrolyte imbalance (hypokalemia)
& surgical intervention to septum /
myocardium
- ECG pattern, apical pulses x 1 minute
Cardiac tamponade
- Compression of heart by blood and other
effusion (clots) in pericardial sac → restricts
normal heart movement
- Rising and equalizing RA and LA pressures,
narrowing pulse pressure, tachycardia,
dyspnea, apprehension, abrupt stop to
chest tube drainage from mediastinal tubes
- 2-D echo to confirm the diagnosis
Decreased cardiac output syndrome
Signs of Shock: decreased BP, decreased pulse
pressure,
cool extremities, metabolic acidosis, oliguria
Aggressively treated with IV inotropes (dopamine,
dobutamine, milrinone)
Decreased peripheral perfusion
Capillary refill time, skin color, warm/cold
extremities, pulses (strong/weak)
Pulmonary changes
Areas of atelectasis common after Sx
Treatment: Pericardiocentesis
6 criteria
1.fever 5days or more
2. Polymorphous rashes
3. Bilateral conjunctivitis without exudates
4. Cervical lymph node
5. Changes mucous membrane - strawberry
younger peeling of skin
3 stages
1. Acute stage last for the 1st to 10 days of illness;
give immunoglobulin
2. Subacute stage
3. Convalescent
You might also like
- Handbook of Psychocardiology PDFDocument1,147 pagesHandbook of Psychocardiology PDFLaura Rodriguez100% (1)
- PrescriptionDocument2 pagesPrescriptionELvin LozandeNo ratings yet
- Nursing Care of The Child Born With Congenital Heart DisordersDocument3 pagesNursing Care of The Child Born With Congenital Heart DisordersElijah GarciaNo ratings yet
- Lecture CardiologyDocument65 pagesLecture CardiologyshinhyejjNo ratings yet
- How To Lose Weight and Keep It OffDocument2 pagesHow To Lose Weight and Keep It OffLUMINITA GIUCANo ratings yet
- Congenital Heart DefectsDocument7 pagesCongenital Heart DefectsJulia Rae Delos SantosNo ratings yet
- CME Cyanotic Heart DiseaseDocument38 pagesCME Cyanotic Heart DiseaseTan Zhi HongNo ratings yet
- Cardio (1) - 240326 - 233643Document12 pagesCardio (1) - 240326 - 233643Taif SalimNo ratings yet
- Final Exam NotesDocument24 pagesFinal Exam NotesNicholeGarcesCisnerosNo ratings yet
- Acyanotic Congenital Heart DiseaseDocument48 pagesAcyanotic Congenital Heart DiseasenabillagusrinaNo ratings yet
- Feeling Blue, A Presentation: Ronald MbwasiDocument29 pagesFeeling Blue, A Presentation: Ronald MbwasiALL KINDS By Milseni KNo ratings yet
- Congenital Heart Defect EDITDocument57 pagesCongenital Heart Defect EDITnicholasacquah680No ratings yet
- Final 3 Congenital Heart DisordersDocument15 pagesFinal 3 Congenital Heart DisordersCAÑADA, JOHANNELYN M.No ratings yet
- Surgery II: Congenital Heart DiseaseDocument10 pagesSurgery II: Congenital Heart DiseaseRea Dominique CabanillaNo ratings yet
- Clinical Aspect of Maternal and Child NursingDocument21 pagesClinical Aspect of Maternal and Child NursingMarianne CoracheaNo ratings yet
- Cardiac DiseasesDocument8 pagesCardiac DiseasesTJ NgNo ratings yet
- Acyanotic Heart Diseases ASD-Atrial Septal DefectDocument5 pagesAcyanotic Heart Diseases ASD-Atrial Septal DefectPrincess LegansonNo ratings yet
- Zuñega - Congenital Heart Disease Educational MaterialsDocument13 pagesZuñega - Congenital Heart Disease Educational MaterialsAprilene Angel Balaque ZunegaNo ratings yet
- Congenital Heart Disorders (Acyanotic)Document53 pagesCongenital Heart Disorders (Acyanotic)Hannah LaputNo ratings yet
- Pediatric Cardiology: D R J O S E M N U Ñ E ZDocument24 pagesPediatric Cardiology: D R J O S E M N U Ñ E ZTim HoseinNo ratings yet
- Cardiopatii Congenitale 17-18 enDocument74 pagesCardiopatii Congenitale 17-18 enMatei PopescuNo ratings yet
- Congenital Heart Disease NotesDocument7 pagesCongenital Heart Disease NotesFarisa Jane BanggoNo ratings yet
- CVS Last Version (25-9)Document182 pagesCVS Last Version (25-9)DaNy Chiriac0% (1)
- Life Threatening Congenital Heart Disease Edisi II Dr. Heny Martini, SPJP (K)Document66 pagesLife Threatening Congenital Heart Disease Edisi II Dr. Heny Martini, SPJP (K)Faruz Faruz RomadhonNo ratings yet
- 13 Congenital Heart Disorders TransesDocument11 pages13 Congenital Heart Disorders TransesKeana DacayanaNo ratings yet
- Cardiovascular Disorders & PregnancyDocument6 pagesCardiovascular Disorders & PregnancyChelcee MagsinoNo ratings yet
- CardiovascularDocument182 pagesCardiovascularCengiz AryanNo ratings yet
- CVS Examination - 16-11-2021Document60 pagesCVS Examination - 16-11-2021KUMUTHA MALAR A/P PARMESWARANNo ratings yet
- Congenital Cardiac Disease: A Guide To Evaluation, Treatment and Anesthetic ManagementDocument87 pagesCongenital Cardiac Disease: A Guide To Evaluation, Treatment and Anesthetic ManagementJZNo ratings yet
- Pda TofDocument56 pagesPda TofPritam PanigrahiNo ratings yet
- Congenital Heart DiseaseDocument12 pagesCongenital Heart DiseaseNinna Isabel VictorioNo ratings yet
- NSG124 - Pedia Written ReportDocument12 pagesNSG124 - Pedia Written Reportlaurie.charlynjaneNo ratings yet
- Congenital Heart DefectDocument12 pagesCongenital Heart Defectsangkularosmina837No ratings yet
- Non-Cyanotic Congenital Heart Disease-UpDate 4-22-53Document136 pagesNon-Cyanotic Congenital Heart Disease-UpDate 4-22-53getnusNo ratings yet
- 2 - Dr. Winda Azwani, SpA (K) Basic Anatomy and Physiology of Cardiovascular SysDocument18 pages2 - Dr. Winda Azwani, SpA (K) Basic Anatomy and Physiology of Cardiovascular SysnudhakoNo ratings yet
- Heart Failure: Andi Wahjono Adi, MD, FIHADocument46 pagesHeart Failure: Andi Wahjono Adi, MD, FIHAYuanita WahyuningsihNo ratings yet
- Valvular Heart DiseaseDocument33 pagesValvular Heart Diseasesimran kaurNo ratings yet
- Midterm PRT 2aDocument24 pagesMidterm PRT 2aReysel MonteroNo ratings yet
- Congenital Heart Diseases Practical Approach in Children With Heart MurmurDocument51 pagesCongenital Heart Diseases Practical Approach in Children With Heart Murmurdennyyy175No ratings yet
- Dr. Musnidarti, SPJP, FihaDocument72 pagesDr. Musnidarti, SPJP, FihasovianNo ratings yet
- Congenital Heart DiseaseDocument5 pagesCongenital Heart Diseasesarguss14100% (1)
- Midterm PRT 2 A qq9Document33 pagesMidterm PRT 2 A qq9Reysel MonteroNo ratings yet
- Pediatric Congenital Heart DiseaseDocument95 pagesPediatric Congenital Heart DiseaseShikya AbnasNo ratings yet
- Congenital Heart Disease (CHD) : by Alireza PourtalebiDocument69 pagesCongenital Heart Disease (CHD) : by Alireza PourtalebiAswathy AswathyNo ratings yet
- Module No. Date: Topic:: Cues/Questions/ Keywords Notes Congenital Heart DisordersDocument28 pagesModule No. Date: Topic:: Cues/Questions/ Keywords Notes Congenital Heart Disordersanon ymousNo ratings yet
- Congenital Heart DiseasesDocument52 pagesCongenital Heart DiseasesCristina Maria100% (1)
- Anak 2Document107 pagesAnak 2Nency PurmayaNo ratings yet
- AcyanoticDocument3 pagesAcyanotic2AAQUINO, PRECIOUS ANGEL F.No ratings yet
- Where Problems With The Heart Mean There Isn't Enough Oxygen Present in The BloodDocument6 pagesWhere Problems With The Heart Mean There Isn't Enough Oxygen Present in The BloodRizalyn Padua ReyNo ratings yet
- 4 Valvular Heart Disease ICMPD (Autosaved)Document30 pages4 Valvular Heart Disease ICMPD (Autosaved)mus zaharaNo ratings yet
- Congenital Heart DefectsDocument6 pagesCongenital Heart DefectsJohiarra Madanglog TabigneNo ratings yet
- Acyanoticheartdiseases 180620040047 PDFDocument88 pagesAcyanoticheartdiseases 180620040047 PDFElijahNo ratings yet
- Acyanoticheartdiseases 180620040047 PDFDocument88 pagesAcyanoticheartdiseases 180620040047 PDFElijahNo ratings yet
- Acyanoticheartdiseases 180620040047 PDFDocument88 pagesAcyanoticheartdiseases 180620040047 PDFElijahNo ratings yet
- Congenital Heart Disease: Thoracic Conference Frank Nami, M.DDocument49 pagesCongenital Heart Disease: Thoracic Conference Frank Nami, M.DMarie CrystallineNo ratings yet
- Chapter 41. Nursing Care of The Child With A Cardiovascular Disorder TermDocument11 pagesChapter 41. Nursing Care of The Child With A Cardiovascular Disorder TermJœnríčk AzueloNo ratings yet
- Congenital Heart DiseaseDocument21 pagesCongenital Heart DiseaseRajwinder KaurNo ratings yet
- Pediatric Cardiac DisordersDocument55 pagesPediatric Cardiac DisordersgraciaNo ratings yet
- Cardiovascular Disorders in Children - StudentDocument53 pagesCardiovascular Disorders in Children - StudentKeanu Win CatipayNo ratings yet
- Cardiac SurgeryDocument110 pagesCardiac SurgeryChristopher McAndrew100% (1)
- AV - Congenital Heart DiseaseDocument10 pagesAV - Congenital Heart DiseasebakiralhamdaniNo ratings yet
- Cardiovascular Diseases VSD Asd 2022 1Document16 pagesCardiovascular Diseases VSD Asd 2022 1Boyu GrtrNo ratings yet
- Immediate Life Support for healthcare Practitioners: A Step-By-Step GuideFrom EverandImmediate Life Support for healthcare Practitioners: A Step-By-Step GuideNo ratings yet
- Effects of Surgical Sterilization On Canine and Feline Health and On SocietyDocument9 pagesEffects of Surgical Sterilization On Canine and Feline Health and On SocietyNadhim Jawad HasanNo ratings yet
- Sample RUDocument25 pagesSample RUmaria riza lagromaNo ratings yet
- Biochemic CombinationDocument5 pagesBiochemic CombinationTahir Naqvi0% (1)
- Chapter Immunological ToleranceDocument33 pagesChapter Immunological TolerancemkmicroduNo ratings yet
- Ranbaxy Takes The Lions Share: Win A Press & Go Nails PackDocument3 pagesRanbaxy Takes The Lions Share: Win A Press & Go Nails Packapi-139438053No ratings yet
- LP 4-ImmunoprophylaxisDocument15 pagesLP 4-ImmunoprophylaxismlinaballerinaNo ratings yet
- Acute Leukemia - Knowledge at AMBOSSDocument1 pageAcute Leukemia - Knowledge at AMBOSSRenad AlharbiNo ratings yet
- History of MedicineDocument108 pagesHistory of MedicineAlexandra Constantin100% (2)
- Management of Sore ThroatDocument11 pagesManagement of Sore ThroatSheera EiyraaNo ratings yet
- Kasus Farmakokinetika Klinik AntibiotikaDocument2 pagesKasus Farmakokinetika Klinik AntibiotikaMr-Eng DeathbatthefallensevenfoldismNo ratings yet
- Evidence-Based Medicine Dan Biostatistik: PengajarDocument1 pageEvidence-Based Medicine Dan Biostatistik: PengajarAnugrah TrianandaNo ratings yet
- Vitiligo TreatmentDocument3 pagesVitiligo TreatmentAnonymous d9GP3q5Z8PNo ratings yet
- Bipolar DisorderDocument349 pagesBipolar Disorders3149521696100% (1)
- Drugs To Avoid in Myasthenia GravisDocument3 pagesDrugs To Avoid in Myasthenia GravispapitomalosoNo ratings yet
- Food Handler Teach and TestDocument2 pagesFood Handler Teach and TestSavitri Maharani BudimanNo ratings yet
- Thrombosis and Thromboprophylaxis in Gynecology SurgeryDocument9 pagesThrombosis and Thromboprophylaxis in Gynecology Surgerymanuel peraltaNo ratings yet
- DMG Catalog DentalDocument64 pagesDMG Catalog DentalErdeli StefaniaNo ratings yet
- Aipg 2016Document115 pagesAipg 2016Gowri ShankarNo ratings yet
- Diabetes Mellitus Type 1Document12 pagesDiabetes Mellitus Type 1Burhan RiazNo ratings yet
- USFDA Regulatory Toxicology OverviewDocument100 pagesUSFDA Regulatory Toxicology OverviewHarsh KoshtiNo ratings yet
- Colorectal Cancer: - Dr. Suneet KhuranaDocument36 pagesColorectal Cancer: - Dr. Suneet KhuranaCarlo ToledooNo ratings yet
- Histopathology & Cytopathology Flowchart-1Document4 pagesHistopathology & Cytopathology Flowchart-1shivam jaiswalNo ratings yet
- S1 2013 280476 BibliographyDocument4 pagesS1 2013 280476 BibliographyrizkaNo ratings yet
- DR Sara Gottfried How To Optimize Female Hormone Health For Vitality & LongevityDocument56 pagesDR Sara Gottfried How To Optimize Female Hormone Health For Vitality & Longevitywaheed khanNo ratings yet
- Nut Ric ScoreDocument1 pageNut Ric ScoreClaudia M FernandezNo ratings yet
- Anusuchi 9 (Payment Mechanism and Rates) UploadDocument61 pagesAnusuchi 9 (Payment Mechanism and Rates) UploadAmit OjhaNo ratings yet
- Progress in Orthodontics-Oussama Sandid-Mohamad Aboualnaser - Progres en Orthodontie-Orthodontists DentistsDocument39 pagesProgress in Orthodontics-Oussama Sandid-Mohamad Aboualnaser - Progres en Orthodontie-Orthodontists DentistsAnonymous oD9H6T8p100% (1)