Professional Documents
Culture Documents
Anal Fissure: A Common Cause of Anal Pain: Clinical Medicine
Anal Fissure: A Common Cause of Anal Pain: Clinical Medicine
Uploaded by
Erwin CandraCopyright:
Available Formats
You might also like
- Breast Imaging - The RequisitesDocument513 pagesBreast Imaging - The RequisitesEvi Polideras100% (6)
- Perianal Problems: ACS/ASE Medical Student Core Curriculum Perianal ProblemsDocument21 pagesPerianal Problems: ACS/ASE Medical Student Core Curriculum Perianal ProblemsHasti Chande100% (1)
- Hand and Wrist AAOS MCQ. 2019 PDFDocument158 pagesHand and Wrist AAOS MCQ. 2019 PDFantonio ferrer100% (2)
- INGUINAL HERNIA and Umbilical HerniaDocument13 pagesINGUINAL HERNIA and Umbilical HerniaKathNo ratings yet
- Pruritus Ani, Hemorroidet EtjDocument4 pagesPruritus Ani, Hemorroidet EtjKreshnik HAJDARINo ratings yet
- Disease of RectumDocument22 pagesDisease of RectumTalal AbbasiNo ratings yet
- Appendicitis, HasDocument6 pagesAppendicitis, HasHasan MohammedNo ratings yet
- Appendicitis HasanDocument6 pagesAppendicitis HasanHasan MohammedNo ratings yet
- Minilaparoscopic Left Paraduodenal Hernia Repair-A CaseDocument4 pagesMinilaparoscopic Left Paraduodenal Hernia Repair-A CaseAritra PaulNo ratings yet
- Mini Review: Current Concepts in The Management of Anterior Urethral StricturesDocument8 pagesMini Review: Current Concepts in The Management of Anterior Urethral StricturesDwi WiraNo ratings yet
- Hernia CaseDocument9 pagesHernia CaseFatima Love Ariate-Arcasetas100% (1)
- Chapter X.4. Intussusception: Case Based Pediatrics For Medical Students and ResidentsDocument5 pagesChapter X.4. Intussusception: Case Based Pediatrics For Medical Students and ResidentsNawaf Rahi AlshammariNo ratings yet
- Journal Homepage: - : IntroductionDocument5 pagesJournal Homepage: - : IntroductionIJAR JOURNALNo ratings yet
- Final Boerhave SnydromeDocument3 pagesFinal Boerhave SnydromeAnugerah Putra GemilangNo ratings yet
- Textbook of Colon and Rectum-Páginas-219-227Document9 pagesTextbook of Colon and Rectum-Páginas-219-227Elliott Josué Carreón MaldonadoNo ratings yet
- Hernia Ebook FullDocument24 pagesHernia Ebook FullMiguelon GarciaNo ratings yet
- Acute Appendicitis: Review ArticleDocument6 pagesAcute Appendicitis: Review ArticleAinun Jariah FahayNo ratings yet
- Abdominal HerniaDocument33 pagesAbdominal HerniaMohammedNo ratings yet
- Congenital Anomalies 1&2Document40 pagesCongenital Anomalies 1&2Hafez AhmedNo ratings yet
- Anal Fissure - ColoproctoDocument3 pagesAnal Fissure - ColoproctoThomas KlebNo ratings yet
- Perianal Abscess - Abstract - Europe PMCDocument6 pagesPerianal Abscess - Abstract - Europe PMCRidha Aswina DalimuntheNo ratings yet
- Hernias - PPT YenniDocument44 pagesHernias - PPT YenniDhika ArdiansyahNo ratings yet
- 3.1 Acute AppendicitisDocument3 pages3.1 Acute AppendicitisMavi HayalNo ratings yet
- 2.4.5.2.3.a Bowel ObstructionDocument35 pages2.4.5.2.3.a Bowel ObstructionProject ByNo ratings yet
- Common Health Problems That Develop During Infancy MPNDocument14 pagesCommon Health Problems That Develop During Infancy MPNShaii Whomewhat GuyguyonNo ratings yet
- Update On The Management of Anal Fissure: SciencedirectDocument7 pagesUpdate On The Management of Anal Fissure: SciencedirectAndrea RodríguezNo ratings yet
- Appendicitis: Mark W. Jones Hassam Zulfiqar Jeffrey G. DeppenDocument7 pagesAppendicitis: Mark W. Jones Hassam Zulfiqar Jeffrey G. DeppenAndi HairunNo ratings yet
- Clark2016 Benign Anal DiseaseDocument7 pagesClark2016 Benign Anal DiseaseJohana Dellaneira Aucancela RamosNo ratings yet
- Focseneanu2015 PDFDocument3 pagesFocseneanu2015 PDFAniydaNo ratings yet
- Management of Common Benign Anorectal Disease: What All Physicians Need To KnowDocument7 pagesManagement of Common Benign Anorectal Disease: What All Physicians Need To KnowNeri JaramilloNo ratings yet
- Duty AssgnmentDocument1 pageDuty Assgnmentmorphine_24No ratings yet
- Meniere's DiseaseDocument45 pagesMeniere's DiseaseAshish KumarNo ratings yet
- Pathology of EsophagusDocument59 pagesPathology of EsophagusDoc On CallNo ratings yet
- Endometriosis With Salpingitis Simulating Acute AppendicitisDocument20 pagesEndometriosis With Salpingitis Simulating Acute AppendicitisWyendae CliquersNo ratings yet
- SigmoidDocument4 pagesSigmoidFKUPR 2017No ratings yet
- 24 Inguinal HerniaDocument11 pages24 Inguinal Herniaputri0aziqhah0nabillNo ratings yet
- HerniaDocument11 pagesHerniaHapsari Wibawani 'winda'100% (1)
- p1319 PDFDocument4 pagesp1319 PDFSyairodhiNo ratings yet
- Skipidip Skipidap Colonic Hernia WoohooDocument3 pagesSkipidip Skipidap Colonic Hernia WoohooSu-sake KonichiwaNo ratings yet
- Cólica em Neonatos - 2005Document4 pagesCólica em Neonatos - 2005thiago.veterinariaNo ratings yet
- Acute Appendicitis: Michael Alan Cole Robert David HuangDocument10 pagesAcute Appendicitis: Michael Alan Cole Robert David HuangandreaNo ratings yet
- Appendicitis: I. Signs and SymptomsDocument3 pagesAppendicitis: I. Signs and Symptomsslimescared01No ratings yet
- 012 090 Groin HerniaDocument8 pages012 090 Groin HerniaxcalibursysNo ratings yet
- HerniaDocument6 pagesHerniaKrizette Ann Cuevo BuanNo ratings yet
- Abdominal Hernia: Jama Patient PageDocument1 pageAbdominal Hernia: Jama Patient PagebasokkaNo ratings yet
- Slide Hernia 2003Document24 pagesSlide Hernia 2003anfaNo ratings yet
- Gastric Volvulus: Bang Chau, Susan DufelDocument2 pagesGastric Volvulus: Bang Chau, Susan DufelmustikaarumNo ratings yet
- Dysphagia Lusoria: A Comprehensive ReviewDocument6 pagesDysphagia Lusoria: A Comprehensive ReviewDante ChavezNo ratings yet
- 8412-Article Text-29472-1-10-20130809Document8 pages8412-Article Text-29472-1-10-20130809NenyNo ratings yet
- Hernias UltrasoundDocument35 pagesHernias UltrasoundRafa Rodríguez AveigaNo ratings yet
- 2016 Usg App PDFDocument9 pages2016 Usg App PDFQonita Aizati QomaruddinNo ratings yet
- 2016 Usg App PDFDocument9 pages2016 Usg App PDFReza ArgoNo ratings yet
- Bicol Medical Center Department of Surgery: AppendicitisDocument60 pagesBicol Medical Center Department of Surgery: AppendicitisHenry Bona100% (1)
- Chronic Pelvic PainDocument18 pagesChronic Pelvic PainWilliam Alfonso Parada VecinoNo ratings yet
- Appendicitis Medical AppendixDocument5 pagesAppendicitis Medical AppendixCordelia NkoroNo ratings yet
- A Simple Guide to Rectal Disorders, Diagnosis, Treatment and Related ConditionsFrom EverandA Simple Guide to Rectal Disorders, Diagnosis, Treatment and Related ConditionsNo ratings yet
- Odynophagia, (Pain on Swallowing) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandOdynophagia, (Pain on Swallowing) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- A Simple Guide To Anal Disorders, Diagnosis, Treatment And Related ConditionsFrom EverandA Simple Guide To Anal Disorders, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Anal Abscess And Fistula, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandAnal Abscess And Fistula, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsRating: 1 out of 5 stars1/5 (1)
- Esophageal Varices, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandEsophageal Varices, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Higuero 2015Document7 pagesHiguero 2015Erwin CandraNo ratings yet
- Jce80002 2413 2422Document10 pagesJce80002 2413 2422Erwin CandraNo ratings yet
- Jce 10016Document8 pagesJce 10016Erwin CandraNo ratings yet
- HHS Public Access: Renal Dysplasia in The NeonateDocument13 pagesHHS Public Access: Renal Dysplasia in The NeonateErwin CandraNo ratings yet
- Sot 1 2011 6Document4 pagesSot 1 2011 6Erwin CandraNo ratings yet
- Images of Primary Angle Closure Glaucoma: Ophthalmology in ViewDocument0 pagesImages of Primary Angle Closure Glaucoma: Ophthalmology in ViewErwin CandraNo ratings yet
- Consensus On Crush1Document7 pagesConsensus On Crush1Erwin CandraNo ratings yet
- Hepatitis G Virus CARDDocument2 pagesHepatitis G Virus CARDErwin CandraNo ratings yet
- Crush Syndrome: Dario Gonzalez, MD, FACEPDocument8 pagesCrush Syndrome: Dario Gonzalez, MD, FACEPMDC101No ratings yet
- Home 11 The Heart Valvular Heart DiseaseDocument1 pageHome 11 The Heart Valvular Heart DiseaseErwin CandraNo ratings yet
- 4.nomenclature of NeoplasmDocument32 pages4.nomenclature of NeoplasmDipo Mas SuyudiNo ratings yet
- Malaria in Pregnancy 4Document35 pagesMalaria in Pregnancy 4api-3705046No ratings yet
- ABC of Clinical Electrocardiography Myocardial IschaemiaDocument6 pagesABC of Clinical Electrocardiography Myocardial IschaemiaShri Mahalaxmi HarishNo ratings yet
- Overview of Mucocutaneous Symptom ComplexDocument5 pagesOverview of Mucocutaneous Symptom ComplexDaphne Jo ValmonteNo ratings yet
- Dissertation On Bronchial AsthmaDocument7 pagesDissertation On Bronchial AsthmaInstantPaperWriterSpringfield100% (1)
- Super Longevity mp3 InstructionsDocument3 pagesSuper Longevity mp3 InstructionsjulioNo ratings yet
- ABO and RH Blood GroupsDocument7 pagesABO and RH Blood GroupsShum Wing Hei JoanneNo ratings yet
- Disaster Nursing SAS Sesion 10Document8 pagesDisaster Nursing SAS Sesion 10Niceniadas CaraballeNo ratings yet
- Medicamente PT RetetaDocument7 pagesMedicamente PT RetetaKaito Noburu ShinNo ratings yet
- JSommers ONLDocument171 pagesJSommers ONLTopaz CompanyNo ratings yet
- Jamaneurology Wang 2023 Oi 230040 1687538249.52757Document9 pagesJamaneurology Wang 2023 Oi 230040 1687538249.52757Mariana VazNo ratings yet
- Mrs. A, 35 Years Old, MR 01 13 45 74, Severity Level IIIDocument18 pagesMrs. A, 35 Years Old, MR 01 13 45 74, Severity Level IIIprimaindra27No ratings yet
- MRCP 2Document26 pagesMRCP 2riyaz414No ratings yet
- Mudra TherapyDocument71 pagesMudra TherapywobblegobbleNo ratings yet
- Hypo Oligo Menorrhea Modern AADocument14 pagesHypo Oligo Menorrhea Modern AAdr anjna takNo ratings yet
- Basic PharmacologyDocument35 pagesBasic PharmacologyPawan PatelNo ratings yet
- Jeyakumar Dhileeban Rrroll 41Document34 pagesJeyakumar Dhileeban Rrroll 41Rupesh TamizhaNo ratings yet
- Rec Letter From ZhylkybaevaDocument2 pagesRec Letter From ZhylkybaevaГулнара УмурзаковаNo ratings yet
- M Mode Vertical DisplacementDocument4 pagesM Mode Vertical Displacementgramachandran186No ratings yet
- IsjsjsDocument13 pagesIsjsjsMarsh MallowNo ratings yet
- The Role of Orthodontics in Temporomandibular DisordersDocument19 pagesThe Role of Orthodontics in Temporomandibular DisordersAngel Rubén Orozco RodríguezNo ratings yet
- Unit 2Document5 pagesUnit 2Phạm Ngọc HuyềnNo ratings yet
- Lesson Plan Lumbar PunctureDocument19 pagesLesson Plan Lumbar PunctureLoma Waghmare (Jadhav)No ratings yet
- J. Antimicrob. Chemother.-2013-Powell-jac Dkt128 2Document10 pagesJ. Antimicrob. Chemother.-2013-Powell-jac Dkt128 2Asri Nikita SariNo ratings yet
- Assessment of HearingDocument30 pagesAssessment of HearingNitin SharmaNo ratings yet
- Jurnal AnalgesikDocument7 pagesJurnal AnalgesikAnung IndrasNo ratings yet
- Blunt AbdominalDocument39 pagesBlunt AbdominalIgnatius JesinNo ratings yet
Anal Fissure: A Common Cause of Anal Pain: Clinical Medicine
Anal Fissure: A Common Cause of Anal Pain: Clinical Medicine
Uploaded by
Erwin CandraOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Anal Fissure: A Common Cause of Anal Pain: Clinical Medicine
Anal Fissure: A Common Cause of Anal Pain: Clinical Medicine
Uploaded by
Erwin CandraCopyright:
Available Formats
available online: www.kp.
org/permanentejournal
Clinical Medicine
Corridor Consult
Anal Fissure: A Common Cause of Anal Pain
By Herman Villalba, MD
Sabrina Villalba, MD
Maher A Abbas, MD, FACS, FASCRS
Vignette Once this cycle sets in, the likelihood of spontaneous
A patient presents with severe anal pain, lasting hours healing decreases and the edges of the fissures become
after each bowel movement. She notices some intermit- more fibrosed, leading to a chronic fissure.
tent bleeding with defecation. She comes to the office Some fissures can be minimally symptomatic, but
with the presumed diagnosis of hemorrhoids. Are her most patients present with severe pain, bleeding, or
symptoms consistent with hemorrhoidal disease, or itching. The pain can be localized to the anus but can
does she have another disorder? radiate to the buttocks, upper posterior thighs, or lower
back. Often the pain is triggered by a bowel movement,
Introduction can last for hours, and can be severe. Bleeding is usu-
Benign anorectal disorders are common and increas- ally not significant. Most patients with fissures have a
ing in incidence. The decreasing intake in dietary fiber history of constipation.
over the 20th century and into the 21st has contributed
to a steady rise in preventable anorectal disorders. It Table 1. Causes of anal pain
is estimated that 20% of the American public has such Thrombosed external hemorrhoids
benign conditions.1 Although hemorrhoids represent Anal fissure
the most common benign anorectal disorder, anal pain Anal abscess
is most often secondary to an acute or chronic anal Herpetic ulceration/other sexually transmitted diseases
fissure and not hemorrhoidal disease.1–14 Crohn’s ulceration and inflammation
Anal, rectal, or pelvic cancer
Pathophysiology and Presentation Lymphoma or leukemia
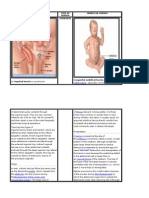
An anal fissure is a tear or a cut in the anoderm (Figure
1). Constipation and passage of hard stools is often the Evaluation
cause of an anal fissure, although diarrhea can also The diagnosis of anal fissure is often made on the
contribute to its development. Most anal fissures are basis of the patient’s medical history. Several anorectal
located in the midline and are posterior more frequently disorders can present with severe anal pain; anal
than anterior. Anterior fissures are seen more often in fissure is the most common cause of pain with or
women. Most fissures heal spontaneously, but some after defecation (Table 1). Anal examination can
persist. It is believed that the decreased blood flow to confirm the diagnosis at the initial visit but is often
the midline portion of the anus contributes to a rela- limited by the patient’s discomfort. The patient is
tively ischemic milieu that becomes more profound sec- usually examined in the prone position. A gentle
ondary to the associated sphincter spasm noted in the spreading of the buttocks can reveal the fissure in
majority of patients with anal fissure.8,10 The anal spasm some patients. If the patient is too apprehensive
is a defense mechanism to prevent further stretching and in much discomfort, the examination should
of the anal canal and worsening of the tear. A vicious be aborted. The patient is treated for the presumed
cycle ensues whereby the anal spasm exacerbates the diagnosis of anal fissure and a complete examina-
ischemia and prevents the fissure from healing, which in tion is deferred to the next visit, usually three or
turn sustains the anal spasm to prevent further tearing. four weeks later. If the fissure is not visualized, li-
Herman Villalba, MD, (left) is a resident in the Department of Surgery, Los Angeles Medical
Center in California. E-mail: herman.a.villalba@kp.org.
Sabrina Villalba, MD, (center) is a resident in the Department of Family Medicine, Los Angeles
Medical Center in California. E-mail: sabrina.r.villalba@kp.org.
Maher A Abbas, MD, FACS, FASCRS, (right) is an Assistant Clinical Professor of Surgery at the
University of California, Los Angeles; Chief of Colon and Rectal Surgery and Education Chair in
the Department of Surgery at the Los Angeles Medical Center. E-mail: maher.a.abbas@kp.org.
62 The Permanente Journal/ Fall 2007/ Volume 11 No. 4
Fall07TPJfnl.indd 62 8/14/07 1:00:55 PM
Clinical Medicine
Anal Fissure: A Common Cause of Anal Pain
Table 3. Fiber products
Type of fiber Trade name Fiber content
Psyllium Metamucil 3.4 g/teaspoon
0.5 g/capsule
Konsyl 6 g/teaspoon
0.5 g/capsule
Methylcellulose Citrucel 2 g/teaspoon
0.5 g/caplet
Calcium polycarbophil FiberCon 0.5 g/caplet
Guar gum Benefiber 3 g/tablespoon
1 g/tablet
0.5 g/caplet
the anus. Atypical fissures warrant a complete medi-
cal workup and often require an examination under
anesthesia, with biopsies and cultures.
Figure 1. Anal fissure.
Treatment Options
More than 90% of fissures heal spontaneously.
docaine 2% jelly is used to locally anesthetize the Symptomatic fissures warrant treatment. Conservative
anal opening so that a gentle digital examination can management is the first line of therapy. Increasing
be attempted. Anal spasm is often present. Posterior dietary fiber and water intake should be coupled with
or anterior midline tenderness can be elicited with fiber supplementation. Psyllium-based products are our
gentle palpation. If the patient tolerates the digital preferred fiber supplement. For patients who cannot
examination, then anoscopy can be performed. In tolerate psyllium because of excess gas or bloating, other
addition to direct visualization of the fissure, the fiber products are available (Table 3). Ideally the adult
clinician may note a sentinel pile or tag just distal diet should contain 25 to 35 g of fiber daily (Table 4).
to the fissure and a hypertrophied anal papilla just
proximal to it (Figure 1). The exposed white fibers
of the internal sphincter muscle can be seen in the Table 4. Fiber-rich foods
center of chronic fissures. The clinician should be Food Serving size Fiber content (g)
ready to abort the examination at any time if the Fruits
patient has severe pain. Under such circumstance, Raspberries 1 cup 8.3
carrying out the examination causes needless suf- Pear 1 medium 5
fering and often cannot be completed despite the Figs, dried 2 medium 3.7
perseverance of the examiner. If there are findings Apple 1 medium 3.3
suspicious for other disorders, such as draining pus Strawberries 1 cup 3.3
from anal opening, swelling and erythema of the Orange 1 medium 3
perianal area, or a mass, then the patient should Legumes, beans, grains, and nuts
undergo an examination under anesthesia. Lentils 1 cup, cooked 15.6
It is important to note that benign fissures are located Black beans 1 cup, cooked 15
in the posterior or anterior Spaghetti, whole wheat 1 cup 6.3
midline. Fissures located in Bran flakes 1 cup 6
Table 2. Atypical
the lateral quadrants are re- Bread, whole grain 1 slice 2–5
causes of anal
ferred to as atypical fissures or Oatmeal 1 cup 4
fissure or ulcer
ulcers and are often secondary Almonds 24 nuts 3.3
Syphilis
Vegetables
Tuberculosis to other conditions (Table 2).
Broccoli 1 cup, cooked 10.9
Leukemic infiltrate Atypical fissures can be mul-
Peas 1 cup 8.8
Carcinoma tiple, deep, wide; have irregu-
Yam 1 cup, cooked 5.3
Herpes lar margins; and may present
Spinach 1 cup, cooked 4.3
Crohn’s disease with purulent drainage from
Corn 1 cup 4
The Permanente Journal/ Fall 2007/ Volume 11 No. 4 63
Fall07TPJfnl.indd 63 8/14/07 1:00:56 PM
Clinical Medicine
Anal Fissure: A Common Cause of Anal Pain
In addition to increasing dietary fiber, patients should healing may take up to two months. Patients should
begin fiber supplementation once a day (ie, 6 g psyl- be reassessed at one month; if there is persistent fis-
lium), and if that is tolerated, their dosage should be sure but decreased symptoms, the ointment should be
increased to twice a day within a week. Patients should continued for another month.
drink at least two glasses of water or fluids each time Patients in whom medical therapy fails may be
they take a fiber supplement dose. A laxative, such candidates for surgical intervention. The timing of
as two tablespoons milk of magnesia once or twice a intervention depends on the initial response to conser-
day, is added for patients with persistent constipation vative therapy and on symptom severity. Patients with
despite increased fiber intake. Stool softeners such as severe anal pain can be offered surgical intervention
docusate can also be added to the fiber regimen. A if no improvement is seen within a week. Injection of
sitz bath in warm water once or twice a day for ten botulinum toxin type A into the internal sphincter can
minutes may offer some relief. Lidocaine 2% jelly is lead to symptomatic relief and healing of some fis-
prescribed to reduce pain as needed before and after sures. Overall, it is safe and rarely causes any degree
bowel movements. Steroid-based creams and hemor- of incontinence. The paralysis that it causes occurs
rhoidal ointments are usually not effective. Ointments within hours of injection, reaches its peak within a
such as nitroglycerin 0.2% to 0.3%, diltiazem 2%, and week, and can last between one and three months.8
nifedipine 0.03% can heal symptomatic fissures; their However, in many patients the relief is temporary and
reported success rate is between 30% and 70%.2–4,7–11 long-term fissure recurrence is common, often making
Most of these medications must be compounded as additional injections necessary.8 Furthermore, botuli-
an ointment preparation by a pharmacy. Gel or liquid num is expensive; the cost of 100 units is $558 at our
preparations are not as effective because of a shorter institution. Because of these reasons, we do not offer
duration of action. Furthermore, they are cumbersome injection as a sole treatment. However, for a subgroup
to use and do not adhere to the anal area as well as of patients with fissures refractory to medical therapy
ointments do. Diltiazem 2%, applied three times daily who are at risk of incontinence or are reluctant to
and five minutes prior to a bowel movement, is our undergo the gold standard surgical treatment of lateral
ointment of choice and has a higher rate of fissure heal- internal sphincterotomy (LIS), we have combined in-
ing than nitroglycerin does and can heal fissures that jection of botulinum with fissurectomy. Debridement
have been unsuccessfully treated with nitroglycerin.10 of the fibrotic edges of a chronic fissure can stimulate
Headache is a common side effect with nitroglycerin, healing when combined with fissurectomy.11 Typically
experienced by up to 50% of patients.8 About 10% we inject 60 to 80 units of botulinum toxin type A into
of patients using diltiazem ointment will experience the internal sphincter muscle; we have seen complete
itching.10 Patients should wear a glove or a finger cot fissure resolution in many patients.
to apply the medication. The relaxation of sphincter The most effective surgical treatment of chronic anal
tone induced by diltiazem, nitroglycerin, and nifedipine fissure is LIS (Figure 2). LIS can heal more than 90%
can relieve the pain within a few days, but complete of fissures refractory to medical therapy within eight
Figure 2a. Lateral internal sphincterotomy. Figure 2b. Lateral internal sphincterotomy.
64 The Permanente Journal/ Fall 2007/ Volume 11 No. 4
Fall07TPJfnl.indd 64 8/14/07 1:00:58 PM
Clinical Medicine
Anal Fissure: A Common Cause of Anal Pain
weeks and is associated with a very low recurrence rate anal fissure. Br J Surg 2007 Feb;94(2):162–7.
of less than 10%.7 LIS involves cutting a small portion 5. Giral A, Memisoglu K, Gültekin Y, et al. Botulinum toxin
injection versus lateral internal sphincterotomy in the treat-
of the distal aspect of the internal sphincter muscle
ment of chronic anal fissure: a non-randomized controlled
(Figure 2). The internal sphincter muscle contributes to trial. BMC Gastroenterol 2004 Mar;22:4–7.
baseline and resting continence. Spasm of this muscle 6. Arroyo A, Pérez F, Serrano P, et al. Surgical versus chemical
results in severe anal pain and constricts blood flow (botulinum toxin) sphincterotomy for chronic anal fissure:
to the fissure area. Releasing a portion of the muscle long-term results of a prospective randomized clinical and
yields rapid symptomatic relief and heals the fissure. manometric study. Am J Surg 2005 Apr;189(4):429–34.
7. Brown CJ, Dubreuil D, Santoro L, et al. Lateral internal
Overall, the procedure is safe and can be done under
sphincterotomy is superior to topical nitroglycerin for
local anesthesia with intravenous sedation in most healing chronic anal fissure and does not compromise long-
patients. The complication rate is low.7,12–14 A subgroup term fecal continence: six-year follow-up of a multicenter, Releasing a
of patients may experience transient and temporary gas randomized, controlled trial. Dis Colon Rectum 2007 portion of
incontinence. In rare cases, the incontinence can be Apr;50(4):442–8. the muscle
more severe or permanent. A careful evaluation of the 8. De Nardi PD, Ortolano E, Radaelli G, Staudacher C. Com- yields rapid
parison of glycerine trinitrate and botulinum toxin-A for
patient’s baseline continence level is important before
the treatment of chronic anal fissure: long-term results. Dis
symptomatic
deciding on surgery. If the patient has any pre-existing Colon Rectum 2006 Apr;49(4):427–32. relief and
degree of incontinence, it is best to consider injection 9. Bailey HR, Beck DE, Billingham RP, et al. A study to deter- heals the
of botulinum toxin type A with fissurectomy or, alter- mine the nitroglycerin ointment dose and dosing interval fissure.
natively, a flap procedure to cover the fissure. that best promote the healing of chronic anal fissures. Dis
Colon Rectum 2002 Sep;45(9):1192–9.
10. Jonas M, Speake W, Scholefield JH. Diltiazem heals glyceryl
Conclusion trinitrate-resistant chronic anal fissures: a prospective study.
Anal fissure is the most common cause of severe anal Dis Colon Rectum 2002 Aug;45(8):1091–5.
pain and bleeding seen in the primary care setting, 11. Lindsey I, Cunningham C, Jones OM, Francis C, Mortensen
in urgent care and surgical clinics, and in Emergency NJ. Fissurectomy-botulinum toxin: a novel sphincter-sparing
Departments. Most fissures heal spontaneously, but con- procedure for medically resistant chronic anal fissure. Dis
Colon Rectum 2004 Nov;47(11):1947–52.
servative management with ointment and fiber supple-
12. Hyman N. Incontinence after lateral internal sphincteroto-
mentation will relieve the pain and promote healing of
my: a prospective study and quality of life assessment. Dis
those that do not. Surgical intervention is reserved for Colon Rectum 2004 Jan;47(1):35–8.
patients in whom conservative treatment fails. v 13. Arroyo A, Pérez F, Serrano P, Candela F, Calpena R. Open
versus closed lateral sphincterotomy performed as an
Acknowledgment outpatient procedure under local anesthesia for chronic
Katharine O’Moore-Klopf of KOK Edit provided editorial anal fissure: prospective randomized study of clinical
assistance. and manometric longterm results. J Am Coll Surg 2004
Sep;199(3):361–7.
References 14. Sánchez Romero A, Arroyo Sebastián A, Pérez Vicente F, et
1. Nelson RL, Abcarian H, Davis FG, Persky V. Prevalence of al. Open lateral internal anal sphincterotomy under local
benign anorectal disease in a randomly selected population. anesthesia as the gold standard in treatment of chronic anal
Dis Colon Rectum 1995 Apr;38(4):341–4. fissures. A prospective clinical and manometric study. Rev
2. Perrotti P, Bove A, Antropoli C, et al. Topical nifedipine with Esp Enferm Dig 2004 Dec;96(12):856–63.
lidocaine ointment vs. active control for treatment of chron-
ic anal fissure: results of a prospective, randomized, double- Suggested Reading
blind study. Dis Colon Rectum 2002 Nov;45(11):1468–75. 1. Madoff RD, Fleshman JW. AGA technical review on the
3. Bielecki K, Kolodziejczak M. A prospective randomized trial diagnosis and care of patients with anal fissure. Gastroen-
of diltiazem and glyceryltrinitrate ointment in the treatment terology 2003 Jan;124(1):235–45.
of chronic anal fissure. Colorectal Dis 2003 May;5(3):256–7. 2. Lund JN, Scholefield JH. Aetiology and treatment of anal
4. Brisinda G, Cadeddu F, Brandara F, Marniga G, Maria G. fissure. Br J Surg 1996 Oct;83(10):1335–44.
Randomized clinical trial comparing botulinum toxin injec-
tions with 0.2 per cent nitroglycerin ointment for chronic
The Permanente Journal/ Fall 2007/ Volume 11 No. 4 65
Fall07TPJfnl.indd 65 8/14/07 1:00:58 PM
You might also like
- Breast Imaging - The RequisitesDocument513 pagesBreast Imaging - The RequisitesEvi Polideras100% (6)
- Perianal Problems: ACS/ASE Medical Student Core Curriculum Perianal ProblemsDocument21 pagesPerianal Problems: ACS/ASE Medical Student Core Curriculum Perianal ProblemsHasti Chande100% (1)
- Hand and Wrist AAOS MCQ. 2019 PDFDocument158 pagesHand and Wrist AAOS MCQ. 2019 PDFantonio ferrer100% (2)
- INGUINAL HERNIA and Umbilical HerniaDocument13 pagesINGUINAL HERNIA and Umbilical HerniaKathNo ratings yet
- Pruritus Ani, Hemorroidet EtjDocument4 pagesPruritus Ani, Hemorroidet EtjKreshnik HAJDARINo ratings yet
- Disease of RectumDocument22 pagesDisease of RectumTalal AbbasiNo ratings yet
- Appendicitis, HasDocument6 pagesAppendicitis, HasHasan MohammedNo ratings yet
- Appendicitis HasanDocument6 pagesAppendicitis HasanHasan MohammedNo ratings yet
- Minilaparoscopic Left Paraduodenal Hernia Repair-A CaseDocument4 pagesMinilaparoscopic Left Paraduodenal Hernia Repair-A CaseAritra PaulNo ratings yet
- Mini Review: Current Concepts in The Management of Anterior Urethral StricturesDocument8 pagesMini Review: Current Concepts in The Management of Anterior Urethral StricturesDwi WiraNo ratings yet
- Hernia CaseDocument9 pagesHernia CaseFatima Love Ariate-Arcasetas100% (1)
- Chapter X.4. Intussusception: Case Based Pediatrics For Medical Students and ResidentsDocument5 pagesChapter X.4. Intussusception: Case Based Pediatrics For Medical Students and ResidentsNawaf Rahi AlshammariNo ratings yet
- Journal Homepage: - : IntroductionDocument5 pagesJournal Homepage: - : IntroductionIJAR JOURNALNo ratings yet
- Final Boerhave SnydromeDocument3 pagesFinal Boerhave SnydromeAnugerah Putra GemilangNo ratings yet
- Textbook of Colon and Rectum-Páginas-219-227Document9 pagesTextbook of Colon and Rectum-Páginas-219-227Elliott Josué Carreón MaldonadoNo ratings yet
- Hernia Ebook FullDocument24 pagesHernia Ebook FullMiguelon GarciaNo ratings yet
- Acute Appendicitis: Review ArticleDocument6 pagesAcute Appendicitis: Review ArticleAinun Jariah FahayNo ratings yet
- Abdominal HerniaDocument33 pagesAbdominal HerniaMohammedNo ratings yet
- Congenital Anomalies 1&2Document40 pagesCongenital Anomalies 1&2Hafez AhmedNo ratings yet
- Anal Fissure - ColoproctoDocument3 pagesAnal Fissure - ColoproctoThomas KlebNo ratings yet
- Perianal Abscess - Abstract - Europe PMCDocument6 pagesPerianal Abscess - Abstract - Europe PMCRidha Aswina DalimuntheNo ratings yet
- Hernias - PPT YenniDocument44 pagesHernias - PPT YenniDhika ArdiansyahNo ratings yet
- 3.1 Acute AppendicitisDocument3 pages3.1 Acute AppendicitisMavi HayalNo ratings yet
- 2.4.5.2.3.a Bowel ObstructionDocument35 pages2.4.5.2.3.a Bowel ObstructionProject ByNo ratings yet
- Common Health Problems That Develop During Infancy MPNDocument14 pagesCommon Health Problems That Develop During Infancy MPNShaii Whomewhat GuyguyonNo ratings yet
- Update On The Management of Anal Fissure: SciencedirectDocument7 pagesUpdate On The Management of Anal Fissure: SciencedirectAndrea RodríguezNo ratings yet
- Appendicitis: Mark W. Jones Hassam Zulfiqar Jeffrey G. DeppenDocument7 pagesAppendicitis: Mark W. Jones Hassam Zulfiqar Jeffrey G. DeppenAndi HairunNo ratings yet
- Clark2016 Benign Anal DiseaseDocument7 pagesClark2016 Benign Anal DiseaseJohana Dellaneira Aucancela RamosNo ratings yet
- Focseneanu2015 PDFDocument3 pagesFocseneanu2015 PDFAniydaNo ratings yet
- Management of Common Benign Anorectal Disease: What All Physicians Need To KnowDocument7 pagesManagement of Common Benign Anorectal Disease: What All Physicians Need To KnowNeri JaramilloNo ratings yet
- Duty AssgnmentDocument1 pageDuty Assgnmentmorphine_24No ratings yet
- Meniere's DiseaseDocument45 pagesMeniere's DiseaseAshish KumarNo ratings yet
- Pathology of EsophagusDocument59 pagesPathology of EsophagusDoc On CallNo ratings yet
- Endometriosis With Salpingitis Simulating Acute AppendicitisDocument20 pagesEndometriosis With Salpingitis Simulating Acute AppendicitisWyendae CliquersNo ratings yet
- SigmoidDocument4 pagesSigmoidFKUPR 2017No ratings yet
- 24 Inguinal HerniaDocument11 pages24 Inguinal Herniaputri0aziqhah0nabillNo ratings yet
- HerniaDocument11 pagesHerniaHapsari Wibawani 'winda'100% (1)
- p1319 PDFDocument4 pagesp1319 PDFSyairodhiNo ratings yet
- Skipidip Skipidap Colonic Hernia WoohooDocument3 pagesSkipidip Skipidap Colonic Hernia WoohooSu-sake KonichiwaNo ratings yet
- Cólica em Neonatos - 2005Document4 pagesCólica em Neonatos - 2005thiago.veterinariaNo ratings yet
- Acute Appendicitis: Michael Alan Cole Robert David HuangDocument10 pagesAcute Appendicitis: Michael Alan Cole Robert David HuangandreaNo ratings yet
- Appendicitis: I. Signs and SymptomsDocument3 pagesAppendicitis: I. Signs and Symptomsslimescared01No ratings yet
- 012 090 Groin HerniaDocument8 pages012 090 Groin HerniaxcalibursysNo ratings yet
- HerniaDocument6 pagesHerniaKrizette Ann Cuevo BuanNo ratings yet
- Abdominal Hernia: Jama Patient PageDocument1 pageAbdominal Hernia: Jama Patient PagebasokkaNo ratings yet
- Slide Hernia 2003Document24 pagesSlide Hernia 2003anfaNo ratings yet
- Gastric Volvulus: Bang Chau, Susan DufelDocument2 pagesGastric Volvulus: Bang Chau, Susan DufelmustikaarumNo ratings yet
- Dysphagia Lusoria: A Comprehensive ReviewDocument6 pagesDysphagia Lusoria: A Comprehensive ReviewDante ChavezNo ratings yet
- 8412-Article Text-29472-1-10-20130809Document8 pages8412-Article Text-29472-1-10-20130809NenyNo ratings yet
- Hernias UltrasoundDocument35 pagesHernias UltrasoundRafa Rodríguez AveigaNo ratings yet
- 2016 Usg App PDFDocument9 pages2016 Usg App PDFQonita Aizati QomaruddinNo ratings yet
- 2016 Usg App PDFDocument9 pages2016 Usg App PDFReza ArgoNo ratings yet
- Bicol Medical Center Department of Surgery: AppendicitisDocument60 pagesBicol Medical Center Department of Surgery: AppendicitisHenry Bona100% (1)
- Chronic Pelvic PainDocument18 pagesChronic Pelvic PainWilliam Alfonso Parada VecinoNo ratings yet
- Appendicitis Medical AppendixDocument5 pagesAppendicitis Medical AppendixCordelia NkoroNo ratings yet
- A Simple Guide to Rectal Disorders, Diagnosis, Treatment and Related ConditionsFrom EverandA Simple Guide to Rectal Disorders, Diagnosis, Treatment and Related ConditionsNo ratings yet
- Odynophagia, (Pain on Swallowing) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandOdynophagia, (Pain on Swallowing) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- A Simple Guide To Anal Disorders, Diagnosis, Treatment And Related ConditionsFrom EverandA Simple Guide To Anal Disorders, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Anal Abscess And Fistula, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandAnal Abscess And Fistula, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsRating: 1 out of 5 stars1/5 (1)
- Esophageal Varices, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandEsophageal Varices, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Higuero 2015Document7 pagesHiguero 2015Erwin CandraNo ratings yet
- Jce80002 2413 2422Document10 pagesJce80002 2413 2422Erwin CandraNo ratings yet
- Jce 10016Document8 pagesJce 10016Erwin CandraNo ratings yet
- HHS Public Access: Renal Dysplasia in The NeonateDocument13 pagesHHS Public Access: Renal Dysplasia in The NeonateErwin CandraNo ratings yet
- Sot 1 2011 6Document4 pagesSot 1 2011 6Erwin CandraNo ratings yet
- Images of Primary Angle Closure Glaucoma: Ophthalmology in ViewDocument0 pagesImages of Primary Angle Closure Glaucoma: Ophthalmology in ViewErwin CandraNo ratings yet
- Consensus On Crush1Document7 pagesConsensus On Crush1Erwin CandraNo ratings yet
- Hepatitis G Virus CARDDocument2 pagesHepatitis G Virus CARDErwin CandraNo ratings yet
- Crush Syndrome: Dario Gonzalez, MD, FACEPDocument8 pagesCrush Syndrome: Dario Gonzalez, MD, FACEPMDC101No ratings yet
- Home 11 The Heart Valvular Heart DiseaseDocument1 pageHome 11 The Heart Valvular Heart DiseaseErwin CandraNo ratings yet
- 4.nomenclature of NeoplasmDocument32 pages4.nomenclature of NeoplasmDipo Mas SuyudiNo ratings yet
- Malaria in Pregnancy 4Document35 pagesMalaria in Pregnancy 4api-3705046No ratings yet
- ABC of Clinical Electrocardiography Myocardial IschaemiaDocument6 pagesABC of Clinical Electrocardiography Myocardial IschaemiaShri Mahalaxmi HarishNo ratings yet
- Overview of Mucocutaneous Symptom ComplexDocument5 pagesOverview of Mucocutaneous Symptom ComplexDaphne Jo ValmonteNo ratings yet
- Dissertation On Bronchial AsthmaDocument7 pagesDissertation On Bronchial AsthmaInstantPaperWriterSpringfield100% (1)
- Super Longevity mp3 InstructionsDocument3 pagesSuper Longevity mp3 InstructionsjulioNo ratings yet
- ABO and RH Blood GroupsDocument7 pagesABO and RH Blood GroupsShum Wing Hei JoanneNo ratings yet
- Disaster Nursing SAS Sesion 10Document8 pagesDisaster Nursing SAS Sesion 10Niceniadas CaraballeNo ratings yet
- Medicamente PT RetetaDocument7 pagesMedicamente PT RetetaKaito Noburu ShinNo ratings yet
- JSommers ONLDocument171 pagesJSommers ONLTopaz CompanyNo ratings yet
- Jamaneurology Wang 2023 Oi 230040 1687538249.52757Document9 pagesJamaneurology Wang 2023 Oi 230040 1687538249.52757Mariana VazNo ratings yet
- Mrs. A, 35 Years Old, MR 01 13 45 74, Severity Level IIIDocument18 pagesMrs. A, 35 Years Old, MR 01 13 45 74, Severity Level IIIprimaindra27No ratings yet
- MRCP 2Document26 pagesMRCP 2riyaz414No ratings yet
- Mudra TherapyDocument71 pagesMudra TherapywobblegobbleNo ratings yet
- Hypo Oligo Menorrhea Modern AADocument14 pagesHypo Oligo Menorrhea Modern AAdr anjna takNo ratings yet
- Basic PharmacologyDocument35 pagesBasic PharmacologyPawan PatelNo ratings yet
- Jeyakumar Dhileeban Rrroll 41Document34 pagesJeyakumar Dhileeban Rrroll 41Rupesh TamizhaNo ratings yet
- Rec Letter From ZhylkybaevaDocument2 pagesRec Letter From ZhylkybaevaГулнара УмурзаковаNo ratings yet
- M Mode Vertical DisplacementDocument4 pagesM Mode Vertical Displacementgramachandran186No ratings yet
- IsjsjsDocument13 pagesIsjsjsMarsh MallowNo ratings yet
- The Role of Orthodontics in Temporomandibular DisordersDocument19 pagesThe Role of Orthodontics in Temporomandibular DisordersAngel Rubén Orozco RodríguezNo ratings yet
- Unit 2Document5 pagesUnit 2Phạm Ngọc HuyềnNo ratings yet
- Lesson Plan Lumbar PunctureDocument19 pagesLesson Plan Lumbar PunctureLoma Waghmare (Jadhav)No ratings yet
- J. Antimicrob. Chemother.-2013-Powell-jac Dkt128 2Document10 pagesJ. Antimicrob. Chemother.-2013-Powell-jac Dkt128 2Asri Nikita SariNo ratings yet
- Assessment of HearingDocument30 pagesAssessment of HearingNitin SharmaNo ratings yet
- Jurnal AnalgesikDocument7 pagesJurnal AnalgesikAnung IndrasNo ratings yet
- Blunt AbdominalDocument39 pagesBlunt AbdominalIgnatius JesinNo ratings yet