Professional Documents
Culture Documents
Adil Abood: Lec. 7 Gastrointestinal and Liver Diseases Gluten-Sensitive Enteropathy
Adil Abood: Lec. 7 Gastrointestinal and Liver Diseases Gluten-Sensitive Enteropathy
Uploaded by
rania rOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Adil Abood: Lec. 7 Gastrointestinal and Liver Diseases Gluten-Sensitive Enteropathy
Adil Abood: Lec. 7 Gastrointestinal and Liver Diseases Gluten-Sensitive Enteropathy
Uploaded by
rania rCopyright:
Available Formats
Clinical Immunology
4th class
Lec. 7
Gastrointestinal and liver diseases
Gluten-Sensitive Enteropathy
Introduction
Gluten-sensitive enteropathy (GSE), also known as celiac disease (CD) or
celiac sprue, is characterized by inflammatory injury to the mucosa of the
small intestine after ingestion of gluten in genetically predisposed
od
individuals. The inciting agent is gluten, a storage protein commonly
found in wheat, barely and rye. More specifically, GSE is caused by T-
bo
cell-mediated recognition of gliadin, an alcohol-soluble fraction of
gluten.
lA
Removal of gluten from the diet has been found to result in significant
regression of the inflammatory lesion and symptoms seen with the
disease.
di
This disease either limited to intestine or associated with a vesicular skin
rA
disease -DH]
Epidemiology:
1. Currently, it is thought to affect as many as 1 in 100 to 250
oo
individuals worldwide.
2. Predominantly affecting Caucasians and people mainly in North
N
America, Europe, and South America.
3. GSE has also been observed among populations in North Africa,
Iran, and India, which attests to the widespread occurrence of the
disease.
4. It was once thought to occur only in childhood, but GSE can
manifest at any age.
5. Celiac disease is associated with other autoimmune syndromes. For
example, about 7 % of patients with type I diabetes have GSE.
Clinical Immunology
4th class
Etiology:
1. Genetics plays a major role in the pathogenesis of GSE.
2. Individuals expressing the MHC haplotypes -DR3, -DR5, -DR7,
and, more importantly, -DQ2 or -DQ8 are at increased risk of
developing GSE.
3. The disease tends to cluster in families, and the monozygotic twin
concordance rate of 75 percent further emphasizes the strong
od
genetic component.
4. GSE has been associated with a region on the long arm of
bo
chromosome 5 (5q31 33), which is where other candidate
and asthma are also located.
lA
5. It has been speculated that there is some involvement of the gene
that encodes the negative co-stimulatory molecule, cytotoxic T-
di
lymphocyte antigen-4 (CTLA-4).
Clinical features:
rA
1. The myriad of symptoms associated with GSE has made detection
of disease especially difficult. Patients commonly present with
malabsorption, steatorrhea, and weight loss relating to the
oo
flattening of proximal small intestinal villi.
2. Diarrhea is not usually present unless the distal small bowel, in
N
addition to the proximal portion, is affected.
3. Some patients do not present with any gastrointestinal symptoms,
but with effects secondary to malabsorption of vitamins such as
iron, folate, and calcium. These patients may only present with
anemia and osteoporosis, respectively.
Clinical Immunology
4th class
4. In addition, there is a strong association between GSE and
autoimmune disease. Some individuals with GSE also present with
Dermatitis Herpetiformis (DH), Fewer than 10 percent of adults
with gluten-sensitive enteropathy present with dermatitis
herpetiformis. This skin condition may be misdiagnosed as atypical
psoriasis or nonspecific dermatitis. The rash of dermatitis
herpetiformis is intensely pruritic and typically occurs on the back,
od
buttocks, knees, and elbows. Unexcoriated lesions are remarkably
bo
Granular IgA deposition on immunofluorescence of a skin biopsy
specimen is diagnostic. Most DH patients have GSE, whereas all
individuals with GSE do not have DH.
lA
Symptoms of Celiac Disease and Possible Causes
SYMPTOMS POSSIBLE CAUSES
di
Fatigue, malaise Anemia, general immune system activation
Weight loss Nutrient malabsorption
rA
Diarrhea, abdominal pain Accelerated gastrointestinal tract transit time,
steatorrhea, malabsorption
Anemia Most commonly, iron deficiency; less commonly,
vitamin B12 and/or folate deficiency
oo
Bone pain Osteoporosis
Aphthous oral ulcers, glossitis,
stomatitis
N
Infertility Postulated cause: iron, folate, and/or zinc deficiency
Male impotence, decreased libido Peripheral insensitivity to circulating testosterone
Alopecia areata Immunologic attack on hair follicles
Dental enamel defects Demineralization during tooth bud development in
children
Hypoglycemia Delayed absorption of glucose
Gas, flatus, borborygmus Secondary digestion of sugars by intestinal flora
Seizures, gluten ataxia, central Increased affinity of celiac antibodies for brain
nervous system symptoms vasculature
Clinical Immunology
4th class
Pathophysiology (immune mechanism):
1. A strong association exists between celiac disease and two human
leukocyte antigens (HLA) haplotypes (DQ2 and DQ8).
2. GSE is due to an immune reactivity to certain cereal storage protein
peptides.
3. Endogenous tissue transglutaminase deamidates gliadin into a
negatively charged protein, increasing its immunogenicity.
4. Damage to the intestinal mucosa is seen whene APC present gliadin
od
peptide, that consist of 33 amino acids, by the MHC molecules to helper
T cells that mediate the inflammatory response.
bo
5. TH1 cells producing IFN- -
macrophages to produce pro-inflammatory cytokines such as IL-1 and
TNF-
lA
6. More lymphocytes infiltrate the epithelium (intraepithelial
lymphocytes), and B-cell specific for gliadin will produce IgA
di
antibodies. In addition, other antibodies against transglutaminase
enzymes are also produced.
rA
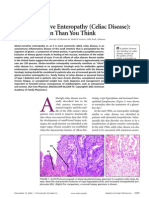
7. Absence of intestinal villi and lengthening of intestinal crypts
characterize mucosal lesions in untreated celiac disease.
oo
N
Clinical Immunology
4th class
Diagnosis
Abnormal Laboratory Findings in Celiac Disease
LABORATORY FINDING PATHOPHYSIOLOGY
Anemia Iron deficiency; vitamin B12 and/or folate deficiency
Elevated alkaline phosphatase level Osteoporosis, osteomalacia
Elevated aspartate transaminase and alanine Minimal elevation common in celiac disease;
transaminase levels presumably autoimmune
Decreased albumin level Malnutrition
od
Elevated calcium level, decreased phosphate Vitamin D deficiency, secondary
level hyperparathyroidism
Thrombocytosis, leukocytosis General inflammatory reaction
bo
Coagulopathy Decreased vitamin K absorption
Low high-density and low-density lipoprotein Decreased fat absorption, decreased hepatic
cholesterol levels lipoprotein production
lA
Serological test:
1. Tissue transglutaminase antibody (TtG), IgA class: the primary
di
test ordered to screen for celiac disease. It is the
mostsensitive and specific blood test for celiac disease.
rA
The IgG class of anti-tTG may be ordered as an alternative in those
who have a deficiency of IgA.
2. Deamidated gliadin peptide (DGP) antibodies (anti-DGP), IgA or
oo
IgG: may be positive in some people with celiac disease who are
negative for anti-tTG, especially children less than 2 years old.
N
3. Anti-endomysial antibodies (EMA): antibodies developed in
reaction to the ongoing damage to the intestinal lining.
4. Anti-reticulin antibody (ARA) test: not as specific or sensitive as
the other autoantibodies; it is found in about 60% of people with
celiac disease and about 25% of those with dermatitis
herpetiformis; it is rarely ordered.
Clinical Immunology
4th class
5. Other tests include:
CBC (complete blood count) to look for anemia.
ESR (erythrocyte sedimentation rate) to evaluate inflammation.
CRP (C-Reactive protein) to evaluate inflammation.
CMP (comprehensive metabolic panel) to determine electrolyte,
protein, and calcium levels, and to verify the status of the kidney
and liver function tests.
od
Vitamin D and B12 and folate to measure vitamin deficiencies
Iron, iron binding capacity or transferrin, and ferritin to detect iron
bo
deficiency.
Stool fat, to help evaluate malabsorption.
lA
To confirm a diagnosis of celiac disease, a four biopsies were
taken from the seconed portion of duodenum, are examined to
detect damage to the intestinal villi.
di
Distal duodenal biopsy is the gold standard for the diagnosis of
celiac disease. Biopsy should be performed in most patients with
rA
suspected gluten-sensitive enteropathy. In determining the need for
biopsy, family physicians should consult a gastroenterologist who
oo
is experienced in the diagnosis and management of celiac disease
N
You might also like
- Bicom For ChildrenDocument11 pagesBicom For ChildrenAnahata Fraydon100% (3)
- Bio Resonance Therapy by BurkiDocument10 pagesBio Resonance Therapy by BurkiHayatFaqeerNo ratings yet
- Baking TechnologyDocument124 pagesBaking Technologyfekremariam Ambaw100% (4)
- Case StudyDocument12 pagesCase Studyapi-242211536100% (1)
- COC 1 Prepare and Produce Bakery ProductsDocument81 pagesCOC 1 Prepare and Produce Bakery Productszander prospero88% (8)
- Celiac DiseaseDocument42 pagesCeliac DiseaseTri P BukerNo ratings yet
- Celiac Disease: Mobin Ur RehmanDocument46 pagesCeliac Disease: Mobin Ur RehmanMobin Ur Rehman KhanNo ratings yet
- Approaches To Diagnosis Celiac DiseaseDocument16 pagesApproaches To Diagnosis Celiac DiseaseJunior GrobeNo ratings yet
- 09 - Celiac DiseaseDocument18 pages09 - Celiac DiseaseSheila Lucya100% (1)
- Celiac DiseaseDocument37 pagesCeliac DiseaseTaj lamajed100% (1)
- Celiac DiseaseDocument10 pagesCeliac DiseaseAnonymous NA6cn5s8No ratings yet
- Celiac Disease FinalDocument7 pagesCeliac Disease FinalacholineNo ratings yet
- Gastro PDFDocument304 pagesGastro PDFAri Syuhada PutraNo ratings yet
- Celiac DiseaseDocument14 pagesCeliac Diseaseraed faisalNo ratings yet
- Gastroenterolgy Reference Guide PDFDocument0 pagesGastroenterolgy Reference Guide PDFbibicul1958No ratings yet
- Orphanet Journal of Rare Diseases: Celiac DiseaseDocument8 pagesOrphanet Journal of Rare Diseases: Celiac DiseaseFauzi NoviaNo ratings yet
- Report DISORDERS OF MALABSORPTIONDocument8 pagesReport DISORDERS OF MALABSORPTIONKathleen Anzhelika B. NemenzoNo ratings yet
- Celiac Disease - 2024Document9 pagesCeliac Disease - 2024khaleelNo ratings yet
- Celiac Disease Celiac Sprue Gluten SensiDocument2 pagesCeliac Disease Celiac Sprue Gluten SensiNərmin ŞahverdiyevaNo ratings yet
- Celiac Disease (Gluten-Sensitive Enteropathy)Document6 pagesCeliac Disease (Gluten-Sensitive Enteropathy)Cricket Trick & FitnessNo ratings yet
- Booklet On Coeliac DiseaseDocument12 pagesBooklet On Coeliac DiseaseQiliang Liu100% (1)
- رابعDocument67 pagesرابععلي عليNo ratings yet
- SlidesDocument43 pagesSlidessidhhikaNo ratings yet
- Non Celiac Enteropathy Level 2 - July 2016Document7 pagesNon Celiac Enteropathy Level 2 - July 2016احمد ليمونهNo ratings yet
- Celiac Disease Gluten Related DisordersDocument49 pagesCeliac Disease Gluten Related Disordersxaviermargarida100% (1)
- Celiac Disease: DR Ajeet Kumar Lohana Senior Registrar Gastroenterology AtmcDocument59 pagesCeliac Disease: DR Ajeet Kumar Lohana Senior Registrar Gastroenterology AtmcAjeet LohanaNo ratings yet
- Celiac Disease - Case StudyDocument29 pagesCeliac Disease - Case StudyRye HanaNo ratings yet
- Chronic Diarrhea in ChildrenDocument30 pagesChronic Diarrhea in ChildrenRyan KadavilNo ratings yet
- Celiacdiseaseand Nonceliacgluten Sensitivity: Runa D. Watkins,, Shamila ZawahirDocument14 pagesCeliacdiseaseand Nonceliacgluten Sensitivity: Runa D. Watkins,, Shamila ZawahirVicky MacNo ratings yet
- Celiac Disease: Clinical PracticeDocument8 pagesCeliac Disease: Clinical PracticeRo RojasNo ratings yet
- Chronic Liver DiseaseDocument75 pagesChronic Liver DiseasebitspurNo ratings yet
- Protein-Losing Enteropathy: Francisco A. SylvesterDocument10 pagesProtein-Losing Enteropathy: Francisco A. SylvesterNIKEN PUSPITASARINo ratings yet
- Malabsorption SyndromesDocument29 pagesMalabsorption SyndromesuouoNo ratings yet
- DC Mais Comum Do Que Se PensaDocument8 pagesDC Mais Comum Do Que Se PensaMary Jane NascimentoNo ratings yet
- Doença Celíaca Revisão 2017Document14 pagesDoença Celíaca Revisão 2017Bianca CorreaNo ratings yet
- Autoimmune HepatitisDocument3 pagesAutoimmune HepatitisMohammed FaragNo ratings yet
- Systemic Lupus Erythematosus (SLE)Document5 pagesSystemic Lupus Erythematosus (SLE)Daniel MazariegoNo ratings yet
- Celiac Disease: Reporter: Joefer C. Traya, SNDocument8 pagesCeliac Disease: Reporter: Joefer C. Traya, SNjoe_ferNo ratings yet
- Chronic Constipation in A 7-Year-Old Boy: Judy-April Oparaji, MD, RDN, CSP, Theresa Heifert, MDDocument5 pagesChronic Constipation in A 7-Year-Old Boy: Judy-April Oparaji, MD, RDN, CSP, Theresa Heifert, MDbella friscaamaliaNo ratings yet
- The Present and The Future in The Diagnosis and Management of Celiac DiseaseDocument9 pagesThe Present and The Future in The Diagnosis and Management of Celiac Diseaseمودة المنعميNo ratings yet
- Intestinal Strongyloidiasis and Hyperinfection SyndromeDocument26 pagesIntestinal Strongyloidiasis and Hyperinfection Syndromeanon-169801100% (2)
- Neonatal Jaundice: AuthorsDocument9 pagesNeonatal Jaundice: AuthorsRam Kumar ShresthaNo ratings yet
- Celiac Disease: GeneticsDocument10 pagesCeliac Disease: Geneticslotp12No ratings yet
- Glycogen Storage Disorders PDFDocument4 pagesGlycogen Storage Disorders PDFAHMEDNo ratings yet
- Autoimmune Hepatitis LectureDocument21 pagesAutoimmune Hepatitis LectureAbdul hadiNo ratings yet
- Pharmaceutical Sciences: Celiac Disease: From Pathophysiology To TreatmentDocument4 pagesPharmaceutical Sciences: Celiac Disease: From Pathophysiology To TreatmentiajpsNo ratings yet
- 8 - Autoimmune DiseasesDocument20 pages8 - Autoimmune Diseasesvirag.patilNo ratings yet
- Chronic Liver DiseasesDocument24 pagesChronic Liver DiseasestabarekNo ratings yet
- Presented To CD4+ T Cells. (MCQ) Damage and The Characteristic Mucosal PathologyDocument3 pagesPresented To CD4+ T Cells. (MCQ) Damage and The Characteristic Mucosal Pathologymurali_bharadwazNo ratings yet
- AJGP 2018 0102 Clinical CoeliacDocument6 pagesAJGP 2018 0102 Clinical CoeliacAngie Viquez BeitaNo ratings yet
- 4 Approach To Immunodeficiency in PediatricsDocument64 pages4 Approach To Immunodeficiency in Pediatricsaj1998aj100% (1)
- Cellular Mechanism of DM FinalDocument70 pagesCellular Mechanism of DM FinalJamil Muqtadir BhattiNo ratings yet
- Diabetes Mellitus PatientsDocument33 pagesDiabetes Mellitus PatientsShabeel PnNo ratings yet
- Immune DeficiencyDocument18 pagesImmune DeficiencyDr anas AbdullahNo ratings yet
- Going Gluten Free in Non Celiac Autoimmune Diseases The Missing IngredientDocument4 pagesGoing Gluten Free in Non Celiac Autoimmune Diseases The Missing IngredientLisa GonçalvesNo ratings yet
- Immuno DeficienciesDocument13 pagesImmuno DeficienciesNikhil TyagiNo ratings yet
- Autoimmune Hepatitis (AIH)Document18 pagesAutoimmune Hepatitis (AIH)Ahmed AliNo ratings yet
- Coeliac Disease & Its Homoeopathic Management.20201030124904Document9 pagesCoeliac Disease & Its Homoeopathic Management.20201030124904elifNo ratings yet
- Ple 2015 Board Review May 2015 Patho OnlyDocument10 pagesPle 2015 Board Review May 2015 Patho OnlyMa Katherina ArellanoNo ratings yet
- 2008 Wieser de CititDocument13 pages2008 Wieser de CititElisabeta StamateNo ratings yet
- Celiac - Word - TrixieDocument3 pagesCeliac - Word - TrixieAirah Mae SabileNo ratings yet
- The Spectrum of Autoimmune Enteropathy: Natalia Nedelkopoulou, Evangelia Farmaki, Maesha Deheragoda and Babu VadamalayanDocument11 pagesThe Spectrum of Autoimmune Enteropathy: Natalia Nedelkopoulou, Evangelia Farmaki, Maesha Deheragoda and Babu VadamalayanjessicaNo ratings yet
- Mal AbsorptionDocument6 pagesMal AbsorptionDiane CheongNo ratings yet
- Presentation 1Document5 pagesPresentation 1Rani KhandelwalNo ratings yet
- Celiac SprueDocument19 pagesCeliac SprueKavita sharmaNo ratings yet
- Et 32Document10 pagesEt 32NaveenNo ratings yet
- Systemic Diseases With Oral Manifestations 19Document141 pagesSystemic Diseases With Oral Manifestations 19Hanin AbukhiaraNo ratings yet
- Gluten and Celiac Disease: Gluten-Free Certification Guide & Terms of CertificationsDocument9 pagesGluten and Celiac Disease: Gluten-Free Certification Guide & Terms of CertificationsKSXNo ratings yet
- Studies About Obtaining Safe and Healthy Bakery Products Using The Beneficial Properties of EnzymesDocument5 pagesStudies About Obtaining Safe and Healthy Bakery Products Using The Beneficial Properties of EnzymesDanaNo ratings yet
- Semi Sweet and Short Dough BiscuitDocument25 pagesSemi Sweet and Short Dough Biscuitgull hassanNo ratings yet
- The Technology of Cake Making (A.j. Bent, E.B. Bennion, G.S.T. Bamford)Document436 pagesThe Technology of Cake Making (A.j. Bent, E.B. Bennion, G.S.T. Bamford)nawresnoussaNo ratings yet
- Foods That Burn Fat, Foods That Turn To Fat, Part 1Document8 pagesFoods That Burn Fat, Foods That Turn To Fat, Part 1S SPEEDNo ratings yet
- Herbal Formulation Considerations For Autoimmune DisordersDocument26 pagesHerbal Formulation Considerations For Autoimmune Disordershitesh mendirattaNo ratings yet
- "Senza Il Pane Tutto Diventa Orfano": Gluten Sensitivity, Coeliac DiseaseDocument87 pages"Senza Il Pane Tutto Diventa Orfano": Gluten Sensitivity, Coeliac DiseaseAmy Ruskoski HendersonNo ratings yet
- Production of Nutritional Bars With Different Proportions of Oat Flour and Brown Rice FlourDocument11 pagesProduction of Nutritional Bars With Different Proportions of Oat Flour and Brown Rice FlourasclepiuspdfsNo ratings yet
- Pepti Junior Aptamil - Recipe - Booklet 1Document27 pagesPepti Junior Aptamil - Recipe - Booklet 1sorinsoareNo ratings yet
- Food Intolerance - Causes, Types, Symptoms, and DiagnosisDocument5 pagesFood Intolerance - Causes, Types, Symptoms, and DiagnosisHannah Denise BatallangNo ratings yet
- Combine Enzyme To Increase Loaf VolumeDocument11 pagesCombine Enzyme To Increase Loaf VolumeTrinh LamNo ratings yet
- Thyroid Diet Quick Start GuideDocument7 pagesThyroid Diet Quick Start GuideDruštvo PlusPet100% (1)
- Case Questions and Case StudyDocument15 pagesCase Questions and Case Studyapi-240616135No ratings yet
- Training Dataset Assessment - 2Document34 pagesTraining Dataset Assessment - 2Peter Kaydee MatthewsNo ratings yet
- Array 3Document2 pagesArray 3api-247458670No ratings yet
- Lesson PlanDocument2 pagesLesson PlanbryantmontorioNo ratings yet
- PM Unit 3Document2 pagesPM Unit 3Christina BinoboNo ratings yet
- Body of ThesisDocument41 pagesBody of Thesisyasas100% (2)
- Ancillary Document Pizza BookDocument24 pagesAncillary Document Pizza BookSoham DasguptaNo ratings yet
- Food Science Final PaperDocument18 pagesFood Science Final Paperapi-239706380No ratings yet
- NEUROGLUTEN 6pDocument6 pagesNEUROGLUTEN 6pEneko LandaburuNo ratings yet
- BASF Nutrition Ingredients - Global Product Catalog - Human January - 2009Document9 pagesBASF Nutrition Ingredients - Global Product Catalog - Human January - 2009zamocoolNo ratings yet