Professional Documents
Culture Documents
CSF & Semen
CSF & Semen
Uploaded by
Irish De VeraOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
CSF & Semen
CSF & Semen
Uploaded by
Irish De VeraCopyright:
Available Formats
CLINICAL MICROSCOPY Sir Carl Leoneill A.
Baroma, RMT, DTA, MPH
CSF & SEMEN
CSF
I Formation and Physiology
II Specimen Consideration
III Gross Examination
IV Microscopic Parameters
V Chemistry Tests
VI Other Tests
I. CSF FORMATION AND PHYSIOLOGY
Cerebrospinal fluid
• Imperfect ultrafiltrate of plasma produced in the
choroid plexuses within the ventricles of the brain at
a rate approximately 500 mL per day maintaining
total volume 90-150 mL/day for adults and 10-60 mL
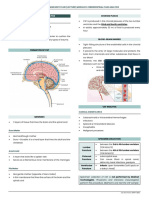
B. Layers of the meninges in the spinal cord
for neonates
• 3rd major body fluid
FORMATION
CSF has particles not seen in urine; not thoroughly
selective • CSF is produced in the choroid plexuses of the
FUNCTIONS: two lumbar ventricles and the third and fourth
• Supply the nutrients to the nervous system ventricles.
• Remove metabolic waste • Blood–brain barrier
• Produce a mechanical barrier to cushion the brain o is the tight-fitting structure of the endothelial cells
and spinal cord against trauma (Protection) in the choroid plexuses that prevent the passage
Meninges of many molecules
• Lines the brain and spinal cord Blood-brain barrier prevents the passage of excessive
• Composed of three layers molecules; since an increase of certain molecules or
o Dura mater (outer layer) particles would indicate an abnormality or malignancy
Counterpart of the glomerulus in the CSF
▪ lines the skull and vertebral canal
• Rate: 500 mL/day or 20 mL/hr
o Arachnoid mater (Spiderweb-like)
• TCV (Total Circulating Volume)
▪ filamentous inner membrane
o Neonates: 10-60 mL/day;
Subarachnoid space – where CSF flows o Adults: 90-150 mL/day
o Pia mater (innermost layer)
▪ lines the surface of the brain and spinal cord II. SPECIMEN CONSIDERATIONS
PHYSIOLOGY SPECIMEN COLLECTION
A. Methods of collection:
• Lumbar Tap
• Cisternal puncture, lateral cervical puncture or
ventricular cannulas
B. Volume collected
A. Layers of the meninges in the brain
DACARA, WINA MARIZ D. | BSMLS3-01 1
TRANSES: CSF & SEMEN
SPECIMEN COLLECTION 4. BLOODY
CSF ORDER OF DRAW • Cause: RBC (↑ >6,000/uL)
• Major Significance:
Purpose Preservation
• Traumatic Tap (Puncture of blood vessel)
TUBE 1 chemical and serologic tests Frozen • Intracranial Hemorrhage (Bleeding within the
braincase)
TUBE 2 microbiology Room Temperature
TRAUMATIC TAP VS. INTRACRANIAL HEMORRHAGE
TUBE 3 Hematology Refrigerated
Distribution of Blood Uneven Even
TUBE 4 Microbiology/ Serology Clot Formation + -
Supernatant Clear Xanthocromic
If only one CSF tube only: Microbiology → HEMATOLOGY →
Erythrophages - +
CHEMICAL AND SEROLOGIC TESTS
D-dimer Negative Positive
5. CLOTTED
• Cause: Due to protein and clotting factors
• Major Significance:
6. XANTHOCHROMIC (YELLOW/PINK/ ORANGE)
• Indicates the presence of RBC degeneration products
or other pigments
SUPERNATANT ASSOCIATED
COLOR DISEASE/DISORDER
• RBC lysis
• Hemoglobin breakdown products
(oxyhemoglobin)
• RBC lysis
• Hemoglobin breakdown products
III. GROSS EXAMINATION (bilirubin)
• Hyperbilirubinemia
• CSF protein >150 mg/dL (1.5 g/L)
A. APPEARANCE
1. NORMAL • RBC lysis (Heavy hemolysis
2. HAZY/TURBID/MILKY/CLOUDY • Hemoglobin breakdown products
3. OILY • Hypervitaminosis
4. BLOODY
5. CLOTTED • Hyperbilirubinemia (biliverdin)
6. XANTHOCHROMIC • Meningeal melanoma
7. PELLICLE
B. VISCOSITY 7. PELLICLE FORMATION
1. NORMAL • Causes:
2. CLINICAL SIGNIFICANCE OF VISCOUS CSF
3. METASTATIC MUCIN PRODUCING • Major Significance
ADENOCARCINOMAS
4. CRYPTOCOCCAL MENINGITIS B. VISCOSITY
5. LIQUID NUCLEUS PULPOSUS
• Normal
A. APPEARANCE • Clinical Significance of Viscous CSF
o Metastatic mucin producing adenocarcinomas
1. NORMAL CSF APPERANCE o Cryptococcal meningitis
• Colorless, crystal clear o Liquid nucleus pulposus
2. HAZY/TURBID/MILKY/CLOUDY IV. MICROSCOPIC PARAMETERS
Cause:
• ↑ WBC (>200/ uL)
CSF CELL COUNT
• ↑ RBC (>400/uL) 1. Total Cell Count
• ↑ LIPIDS AND PROTEIN 2. WBC Count
• ↑MICROORGANISMS 3. RBC Count
4. Differential Count
3. OILY
• Major Significance: Radiographic Contrast Media
DACARA, WINA MARIZ D. | BSMLS3-01 2
TRANSES: CSF & SEMEN
1. TOTAL CELL COUNT o -8 mg/dL Total protein concentration for every
• Dilution (using NSS), counting and calculation of the 10,000 RBCs/uL (Henry)
number of uL are done using the same procedure as o -1 mg/dL protein concentration for every 1,200
WBC count RBCs/uL (stras)
• Fuchs-Rosenthal-type chamber may be used • To correct WBC Error:
• An improved Neubauer counting chamber is
routinely used for performing CSF cell counts.
• Cells are counted in the four corner squares and the
center square on both sides of the hemocytometer
Neubauer Counting Chamber
4. DIFFERENTIAL COUNT
a. Concentration technique
• Filtration
o for large volumes of specimens
• Cytocentrifugation
o associated with decreased cellular distortion and
requires addition of _____ to not increase yield
and minimize distortion
b. Smear preparation
c. Examination
• WBC differential count
PREDOMINANT CELLS IN CSF
1. Lymphocytes and Monocytes
2. Neutrophils
3. Erythrophages
2. WBC COUNT 4. RARE: Blast forms, Macrophage, Plasma cells
Procedure:
1. Dilute (3% Acetic acid, NSS)
2. Charge Both side of Hemocytometer
LYMPHOCYTE AND MONOCYTES
• NORMAL VALUES
3. Count in 5 large squares per side
• CLINICAL SIGNIFICANCE:
4. Calculation
Predominant Cells Seen in CSF
Major Clinical Microscopic
Type of Cell
Significance Findings
• Normal • All stages of
Lymphocytes • Viral, tubercular, and development
fungal meningitis may be found
• Multiple sclerosis
• Normal Values:
• Bacterial meningitis • Granules may
• Adult:
• Early cases of viral, be less
• Neonates: prominent
tubercular, and
Neutrophils • fungal meningitis
than in blood
CSF DILUTION • Cerebral hemorrhage • Cells
APPEARANCE DILUTION
AMOUNT OF AMOUNT OF disintegrate
SAMPLE DILUENT rapidly
Clear UNDILUTED
• Normal • Found mixed
Slightly Hazy 1:10 270 uL • Viral, tubercular, and with
Monocytes
fungal meningitis lymphocytes
Hazy 1:20 250 uL
30 uL • Multiple sclerosis
Slightly cloudy 1:100 2,970 uL • RBCs in spinal fluid • May contain
Slightly bloody 1:200 5,970 uL phagocytized
Cloudy, RBCs
1: 10,000 1 mL 9 mL appearing as
Bloody, Turbid
empty
Macrophages • vacuoles or
3. RBC COUNT ghost cells,
• Done in cases of Traumatic Tap hemosiderin
• TCC – WBC ct granules, and
• To correct WBC error: • hematoidin
o -1 WBC for every 700 RBC seen crystals
DACARA, WINA MARIZ D. | BSMLS3-01 3
TRANSES: CSF & SEMEN
• Acute leukemia • Lymphoblasts
Blast forms , myeloblasts,
or monoblasts
• Disseminated • Resemble
Lymphoma lymphomas lymphocytes
cells with cleft
nuclei
• Multiple sclerosis • Traditional
• Lymphocyte and classic
Plasma cells reactions forms seen
• Reactive
lymphs
• Diagnostic • Seen in
Ependymal, procedures clusters with
choroidal, distinct nuclei
and spindle- and distinct
shaped cells cell
• walls
• Metastatic • Seen in
carcinomas clusters with
Malignant • Primary central fusing of cell
cells nervous system borders and
carcinoma nuclei
V. CHEMISTRY TESTS
1. TOTAL PROTEIN
• Normal values:
• ↑ in Cases of:
• ↓ in cases of:
• Major CSF protein: Albumin
• 2nd most abundant
• Alpha globulins: Haptoglobin, ceruloplasmin
• Beta-globulins: Beta2-transferrin (TAU) protein
• Gamma globulins- IgG and some IgA
• Not found in CSF: IgM, Fibrinogen, Lipids
𝑚𝑔
𝐶𝑆𝐹 𝑎𝑙𝑏𝑢𝑚𝑖𝑛 ( )
A𝑙𝑏𝑢𝑚𝑖𝑛 𝑖𝑛𝑑𝑒𝑥 = 𝑑𝐿
𝑔
𝑆𝑒𝑟𝑢𝑚 𝑎𝑙𝑏𝑢𝑚𝑖𝑛 ( )
𝑑𝐿
CSF ELECTROPHORESIS
• Done in conjunction with serum electrophoresis
𝑚𝑔
𝐶𝑆𝐹 𝐼𝑔𝐺 ( ) • For the detection of oligoclonal
𝑑𝐿
𝑔 bands in the gamma region
𝑆𝑒𝑟𝑢𝑚 𝐼𝑔𝐺 ( )
I𝑔𝐺 𝑖𝑛𝑑𝑒𝑥 = 𝑑𝐿 • The presence of 2 or more
𝑚𝑔
𝐶𝑆𝐹 𝑎𝑙𝑏𝑢𝑚𝑖𝑛 ( ) oligoclonal bands in CSF but not
𝑑𝐿
𝑔 in serum is valuable diagnosis of
𝑆𝑒𝑟𝑢𝑚 𝑎𝑙𝑏𝑢𝑚𝑖𝑛 ( )
𝑑𝐿 MS
• Other conditions with oligoclonal
banding in CSF but not in serum
are: Neurosyphilis, encephalitis,
neoplastic disorders, Guillain
barre syndrome
MYELIN BASIC PROTEIN
• Protein component of the lipid-protein complex that
insulate the
• nerve fibers
• Presence of MBP in CSF indicate destruction of
myelin sheath
• Used to monitor the course of MS
DACARA, WINA MARIZ D. | BSMLS3-01 4
TRANSES: CSF & SEMEN
2. GLUCOSE 5. CSF ENZYMES
• Normal values: • Lactate dehydrogenase
• ↑ in Cases of: • CK-BB – increases about 6 hours following ischemia
• ↓ in cases of: and anoxia
• Normal in cases of: • Adenosine deaminase – increased in tubular
meningitis
3. LACTATE • Lysozyme – increased in patients with both bacterial
• Inversely proportional to glucose and tubercular meninges
• Normal values:
• ↑ in Cases of: LACTATE DEHYDROGENASE
• Normal in cases of: • Serum LDH
o Normal: LD 2 > 1 > 3 > 4 > 5
4. GLUTAMINE o Abnormal: LD 1 > 2 > 3 > 4 > 5
• Product of ammonia and alpha-ketoglutarate
• Indirect test for the presence of excess ammonia in • CSF LDH
CSF o Normal: LD 1 > 2 > 3 > 4 > 5
• Normal values: o Neurological M: LD 2 > 1
• ↑ in Cases of: o Bacterial M: LD 5 > 4 > 3 > 2 > 1
SPECIMEN CONSIDERATIONS
• GLUCOSE
• LACTATE
MAJOR LABORATORY REULTS FOR THE DIFFERENTIAL DIAGNOSIS OF MENINGITIS
Bacterial Viral Tubercular Fungal
Predominant Lymphoctes and Lymphocytes and
Neutrophil Lymphocytes
WBC Monocytes Monocytes
Moderate to markedly Moderate to markedly
Protein Markedly elevated Moderately elevated
elevated elevated
Glucose Marked decrease (<40
Normal Decreased (<45 mg/dL) decreased
mg/dL)
Lactate > 35 mg/dL Normal >25 mg/dL > 25 mg/dL
Agents: Enteroviruses Agent: M. tuberculosis Agent: C. neoformans
+ Gram stain ✓ Poliovirus + AFB stain + gram stain = classic
+ culture + Pellicle weblike clot starburst pattern
Other tests: ✓ Echovirus
+ Limulus lysate formation after 12-24 hr + india ink = capsule
✓ Coxsackievirus refrigeration (unstained); background
(black)
DACARA, WINA MARIZ D. | BSMLS3-01 5
TRANSES: CSF & SEMEN
VI. OTHER TESTS
Gram stain
✓ S. pneumonia
✓ H. influenzae
✓ E. coli
✓ N. meningitidis
Lymulus Lysate
• Detects Gram – bacterial endotoxin in body fluids and
surgical instruments
• Regent: Blood of Horseshoe crab REASONS FOR SEMINAL FLUID ANALYSIS
• Principle: in the presence of endotoxin, the • Fertility testing
amoebocytes (WBCs) will release lysate (protein), + • Postvasectomy semen analysis
clumping/ Clot formation • Forensic analysis (alleged rape)
2. COMPOSITION OF SEMEN
SEROLOGY
• ELISA COMPOSITION OF SEMEN
• VDRL (Venereal disease research laboratory test)
• 1. Seminiferous tubules (testes)
• FTA- ABS (fluorescent treponemal antibody o Spermatogenesis site
absorption) 5% Spermatozoa o Sertoli cells
• CAT • 2. Epididymis
• Bacterial antigen test • Seminal vesicles
60-70% Seminal o Provide nutrients for sperm & fluid
SEMEN Fluids o Rich in FRUCROSE
o Flavin
• Acidic fluid
20-30% Prostate • Contains ACP, zinc, citric acid & other
I Physiology fluid enzymes
II Composition of Semen • For Coagulation & Liquefaction
III Specimen Collection
5% Bulbourethral • Secretes thick alkaline mucus that
IV Semen Analysis
neutralizes acidity from the prostatic
A. Macroscopic Examination gland
secretions & vagina.
B. Sperm Concentration
C. Sperm Counting
D. Sperm Motility 3. SPECIMEN COLLECTION
E. Sperm Morphology
F. Sperm Viability 1. Abstinence of 2-3 days but not >7 days
G. Seminal fluid fructose 2. Collect the entire ejaculate
H. Antisperm Antibodies Methods of collection:
I. Chemical Testing
J. Microbial Testing o Masturbation
K. Additional Tests o Coitus interruptus
o Condom method
3. Specimen should be delivered to the laboratory within
1. PHYSIOLOGY 1 hour of collection
4. Take note of the time of specimen collection, specimen
receipt and liquefaction.
5. Analysis should be done after liquefaction (usually 30-
60 minutes)
6. Specimen awaiting analysis should be kept at 37° C.
4. SEMEN ANALYSIS
A. Macroscopic Examination
B. Sperm Concentration
C. Sperm Counting
D. Sperm Motility
E. Sperm Morphology
F. Sperm Viability
G. Seminal fluid fructose
H. Antisperm Antibodies
I. Chemical Testing
J. Microbial Testing
K. Additional Tests
DACARA, WINA MARIZ D. | BSMLS3-01 6
TRANSES: CSF & SEMEN
A. MACROSCOPIC EXAMINATION Sperm Count
• Normal Value = ≥ 40 M/ ejaculate
MACROSCOPIC EXAMINATION • Formula: Sperm concentration x specimen volume
Gray-white, • Normal
translucent = ___________
(with musty or • Reporting:
bleach odor) • 0 =
Appearance Increased white Viscosity _________
turbidity = • 4 =
Red or brown _________
coloration =
Yellow coloration
• Normal =
_________
Normal
• ↑pH =
Volume Increased in pH
_________
Decreased in
• ↓pH =
_________
A. Macroscopic Examination
• Liquefaction
o Normal: Clotted semen must liquefy within 30-60
mins after collection
o >60 mins – deficiency on prostatic enzyme
o > 2 hours – Add equal volume of physiologic
Dulbelcco’s phosphate-buffered saline or alpha
chymotrypsin or bromelain (proteolytic enzymes)
D. SPERM MOTILITY
B. SPERM CONCENTRATION
• Normal Values:
• Factors affecting sperm concentration: o Within 1 hour = 50% Motile
o Days of sexual abstinence before collection o Quality = ≥ 2.0
o Infection
o Stress • Computer – Assisted Semen Analysis (CASA)
o Provides objective determination of both sperm
Normal value = 20-160 million/mL o Velocity & trajectory (direction of motion)
1 000 000 000 leukocytes/mL = inflammation or infection o Sperm concentration & morphology
of the reproductive organs
>1 000 000 000 spermatids/mL = disruption of
spermatogenesis
METHODS
1. Improved Neubauer Counting Chamber
o Dilution = 1:20
o Diluents: to immobilize sperm
o Formalin
o Sodium
o Saline
o Distilled water
o Tap water
2. Makler Counting Chamber
o For undiluted specimen – no dilution
o Uses heat to immobilize sperm cells
C. SPERM COUNTING
Sperm Concentration Computation
• 2 WBC squares = # of sperms counted x 100,000
• 5 RBC squares = # of sperms counted x 1,000,000
Sperm Concentration Method using Neubauer
Formula
DACARA, WINA MARIZ D. | BSMLS3-01 7
TRANSES: CSF & SEMEN
E. SPERM MORPHOLOGY H. ANTISPERM ANTIBODIES
1. Mixed agglutination reaction
o Detects the presence of IgG antibodies
o Semen sample + AHG + latex particles or treated
RBCs coated with IgG
o Normal = <10% motile sperm attached to the
particles.
2. Immunobead test
o Detects the presence of IgG, IgM & IgA
antibodies + location
o Demonstrate what area of the sperm (head, neck,
tail) the autoantibodies are affecting / attached.
I. CHEMICAL TESTING
Decreased
Analyte Normal value
Values Indicate
Fructose ≥ 13 umol / ejaculate ↓Seminal fluid
Neutral α- ≥ 20 mU / ejaculate Epididymis disorder
glucosidase
Zinc ≥ 2.4 umol / ejaculate
• Normal values: Citric acid ≥ 52 umol / ejaculate
o Rountine criteria ↓Prostatic fluid
Acid ≥ 200 units / ejaculate
o Kruger’s strict criteria phosphatase
• Stains for Sperm Morphology:
o Wright’s stain
o Giemsa stain J. MICROBICAL TESTING
o Papanicolau’s stain – Stain of choice
• Round cells
• Head
o WBCs and spermatids (immature cells)
o Normal
o Normal value = 1 million / µL
o Abnormal
▪ > 1 million WBCs/mL = Infection
• Midpiece
▪ > 1 million spermatids/mL = Distraption of
o Contains mitochondria
spermatogenesis
o Tail
• Test for Chlamydia Trachomatis, Mycoplasma
o Abnormal – poor motility
hominis & Ureaplasma urealycticum
F. SPERM VIABILITY/ VITALITY
K. OTHER TESTS
• Modified Bloom’s test
o Preparing a smear and counting the number of
MEDICO LEGAL TESTS
dead cells in 100 sperms Test for detection of semen:
1. Microscopic exam
o Reagents
2. Fluorescene under UV light
o Living sperms = unstained, bluish white
3. Acid phosphatase determination
o Dead sperms = red
o Normal Values: 50% more living cells 4. Glycoprotein p30 = more specific method
5. Florence test (not specific)
o Test for CHOLINE
G. SEMINAL FLUID FRUCTOSE o Reagents: Iodine crystals = KI
o (+) Dark brown rhombic crystals
• SEMINAL FLUID FRUCTOSE
6. Barbiero’s test (very specific)
• Tested within 2 hours or frozen to prevent fructolysis
o Test for SPERMINE
• Screening test
o Reagents: Saturated picric acid + TCA
• Resornicol test = (+) Orange-red color
o (+) Yellow leaf-like crystals
• a.k.a Seliwanoff’s Test
7. ABO blood Grouping
• Low fructose levels are caused by abnormalities of
8. DNA analysis
the seminal vesicles, bilateral congenital absence of
the vas deferens, obstruction of the ejaculatory duct, POSTVASECTOMY SEMEN ANALYSIS
partial retrograde ejaculation, and androgen
• Vasectonomy
deficiency
o Cutting of vas deferens so that the ejaculate will
not contain any sperm cell
DACARA, WINA MARIZ D. | BSMLS3-01 8
TRANSES: CSF & SEMEN
• The only concern is the presence or absence of
sperm
• Done 2 months after vasectomy & continued until 2
consecutive monthly specimens show NO SPERM
TERMINOLOGIES
Terminology Definition
Aspermia No ejaculate
Azoospermia Absence of sperm cells
Necrospermia Immotile/ dead sperm cells
Oligospermia Decreased sperm concentration
DACARA, WINA MARIZ D. | BSMLS3-01 9
You might also like
- TCAR ManualDocument193 pagesTCAR ManualJoe Reed (Game Master)No ratings yet
- Syllabus in Community and Public Health For Medical Laboratory ScienceDocument4 pagesSyllabus in Community and Public Health For Medical Laboratory ScienceIrish De Vera100% (3)
- Clinical Microbiology Laboratory Test RequisitionDocument1 pageClinical Microbiology Laboratory Test RequisitionRhodjane Dela Cruz0% (1)
- Open Common Bile Duct ExplorationDocument51 pagesOpen Common Bile Duct Explorationmathisync100% (4)
- AUBF - Chapter 1Document7 pagesAUBF - Chapter 1Kristin SoquilloNo ratings yet
- WBC AbN MorphologyDocument2 pagesWBC AbN MorphologyTristan Iris100% (2)
- Principles of Teaching 1 (Corpuz, Salandanan 3rd Ed) - Unit 1 Chapter 2Document8 pagesPrinciples of Teaching 1 (Corpuz, Salandanan 3rd Ed) - Unit 1 Chapter 2NiNo_9367% (3)
- Vaccinations in PregnancyDocument137 pagesVaccinations in PregnancyAmine YounisNo ratings yet
- Proper Collection and Preservation of SpecimenDocument6 pagesProper Collection and Preservation of SpecimenDavid SantosNo ratings yet
- CSF & Body FluidDocument42 pagesCSF & Body FluidlopaNo ratings yet
- Malarial ParasitesDocument5 pagesMalarial ParasitesZette ArañaNo ratings yet
- Body FluidsDocument81 pagesBody FluidsAris ResurreccionNo ratings yet
- Microtomy and Cutting Sections ChapterDocument28 pagesMicrotomy and Cutting Sections ChapterAlex LiganNo ratings yet
- CSF ExaminationDocument38 pagesCSF ExaminationAmaan KhanNo ratings yet
- Aubf Lec (2 Week) Physical Examination of Urine: Color, Clarity Specific GravityDocument38 pagesAubf Lec (2 Week) Physical Examination of Urine: Color, Clarity Specific GravityAngela ReyesNo ratings yet
- Blood Bottles GuideDocument9 pagesBlood Bottles GuideLohJNo ratings yet
- Urine Specimen Collection: Ms. Sneha SehrawatDocument36 pagesUrine Specimen Collection: Ms. Sneha SehrawatRajaNo ratings yet
- Diagnostic Microbiology - : University of Santo Tomas - Medical TechnologyDocument6 pagesDiagnostic Microbiology - : University of Santo Tomas - Medical TechnologyWynlor AbarcaNo ratings yet
- Sputum Analysis and BalDocument41 pagesSputum Analysis and BalClaire GonoNo ratings yet
- Intro To ImmunohematoDocument48 pagesIntro To Immunohematojong188No ratings yet
- AUBF Finals Vaginal SecretionsDocument37 pagesAUBF Finals Vaginal SecretionsLyra Dennise LlidoNo ratings yet
- Histopathology InstrumentsDocument6 pagesHistopathology InstrumentsLawrence LeeNo ratings yet
- Clinical Parasitology LaboratoryDocument4 pagesClinical Parasitology LaboratoryLyka ReyesNo ratings yet
- Notes Cerebrospinal FluidDocument10 pagesNotes Cerebrospinal FluidsusuigenerisNo ratings yet
- Microscopic Examination of UrineDocument4 pagesMicroscopic Examination of UrineGlaiza Erika Baes GudaNo ratings yet
- Prathama Blood Bank, Management Practice and Donors Behavior.Document183 pagesPrathama Blood Bank, Management Practice and Donors Behavior.Bohra Nilesh100% (2)
- Bacteriology PDFDocument49 pagesBacteriology PDFKat JornadalNo ratings yet
- CLM.20 Microbiology Specimen CollectionDocument19 pagesCLM.20 Microbiology Specimen Collectionfldos universeNo ratings yet
- Histochemistry Chapter 5Document48 pagesHistochemistry Chapter 5Zelalem DejazmachNo ratings yet
- Bacteriology HandoutDocument30 pagesBacteriology HandoutMoonyeen Jann Casera BalicNo ratings yet
- Chapter 18 Anemia HematologyDocument30 pagesChapter 18 Anemia HematologyYelnats DatsimaNo ratings yet
- Connective TissueDocument7 pagesConnective TissueSheena Pasion100% (1)
- Bone Marrow ExaminationDocument88 pagesBone Marrow ExaminationSravani PeddagangannagariNo ratings yet
- Pre-Analytical Consideration and Venipuncture ComplicationsDocument52 pagesPre-Analytical Consideration and Venipuncture ComplicationsVenom100% (1)
- Accurate Diagnosis of Parasitic Infections Is Important To Decrease The Prevalence andDocument4 pagesAccurate Diagnosis of Parasitic Infections Is Important To Decrease The Prevalence andManulat VicaiiNo ratings yet
- Culture Media FinalDocument25 pagesCulture Media FinalRaghu KumarNo ratings yet
- Bacteria - Morphology & ClassificationDocument38 pagesBacteria - Morphology & ClassificationAfshan NasirNo ratings yet
- Solid Waste Management For Hospitals: Presented By: Faisal V A MT15CTM004Document46 pagesSolid Waste Management For Hospitals: Presented By: Faisal V A MT15CTM004vnitceNo ratings yet
- Urine Sediment Particles PDFDocument119 pagesUrine Sediment Particles PDFambadepravinNo ratings yet
- 02 Diagnostic MycologyDocument78 pages02 Diagnostic MycologyNilda Quitquitan PatriarcaNo ratings yet
- Aubf Lab Types of Urine SpecimenDocument18 pagesAubf Lab Types of Urine SpecimenNerizaNo ratings yet
- Mycobacteria: Nocardia, Rhodococcus, Tsukamurella and GordoniaDocument7 pagesMycobacteria: Nocardia, Rhodococcus, Tsukamurella and Gordonia20C – Gorospe, Rhai Chezka V.No ratings yet
- Molecular Biology and Diagnostic Intro To CytogeneticsDocument6 pagesMolecular Biology and Diagnostic Intro To Cytogeneticselijah montefalcoNo ratings yet
- Cytology I - Techniques and Application: Peter NG Cyto Lab Ic, MT, PYNEHDocument201 pagesCytology I - Techniques and Application: Peter NG Cyto Lab Ic, MT, PYNEHbusiness onlyyouNo ratings yet
- Sputum ExaminationDocument9 pagesSputum ExaminationDr. Ashish JawarkarNo ratings yet
- Red Blood Cells "Best Module Ever"Document4 pagesRed Blood Cells "Best Module Ever"Jose Emmanuel Dolor100% (1)
- Group 3 - ParasitologyDocument8 pagesGroup 3 - Parasitologyjulo_05No ratings yet
- Topic 02 Urinalysis I Review of Ana and Phy of KidneysDocument6 pagesTopic 02 Urinalysis I Review of Ana and Phy of KidneysNatasha MendozaNo ratings yet
- Diploma in Medical Laboratory Technology PDFDocument52 pagesDiploma in Medical Laboratory Technology PDFMayur Parmar100% (1)
- Group 4 - General Pathology, Logic and Cytologic TechniquesDocument11 pagesGroup 4 - General Pathology, Logic and Cytologic Techniquesjulo_05No ratings yet
- 11 PathologyDocument26 pages11 PathologyRocky BullNo ratings yet
- Specimen Collection and ProcessingDocument40 pagesSpecimen Collection and ProcessingHersey MiayoNo ratings yet
- CLS 400 - Test 4 (Extra Credit)Document8 pagesCLS 400 - Test 4 (Extra Credit)McNeeseInsiderNo ratings yet
- Impregnation and EmbeddingDocument5 pagesImpregnation and EmbeddingOsannah Irish InsongNo ratings yet
- Mod 1Document26 pagesMod 1SEAN MELNOR LOSBAÑESNo ratings yet
- Histopath Lec (Module 1) : Iintroduction To PathologyDocument17 pagesHistopath Lec (Module 1) : Iintroduction To PathologyAngela ReyesNo ratings yet
- Performance Rubrics For EtsDocument2 pagesPerformance Rubrics For EtsKim G. SarongNo ratings yet
- Cytology and Cytological TechniquesDocument29 pagesCytology and Cytological TechniquesNgotelo FunwiNo ratings yet
- Lab 7 Blood Smear and Morphology AnalysisDocument8 pagesLab 7 Blood Smear and Morphology Analysisapi-309917909100% (1)
- Specimen CollectionDocument60 pagesSpecimen Collectionmyla adapNo ratings yet
- Student Notes: GPHCT: Davao Doctors College Medical Laboratory Science DepartmentDocument7 pagesStudent Notes: GPHCT: Davao Doctors College Medical Laboratory Science DepartmentFedz FederisoNo ratings yet
- Types of ImmunityDocument35 pagesTypes of ImmunityKailash NagarNo ratings yet
- Leukaemoid Reaction Lecture by DRDocument35 pagesLeukaemoid Reaction Lecture by DRapi-273068056100% (1)
- Mtap AubfDocument10 pagesMtap AubfMarjorie Balangue MacadaegNo ratings yet
- Aubf Lecture (2024) - M8 - Cerebrospinal Fluid AnalysisDocument7 pagesAubf Lecture (2024) - M8 - Cerebrospinal Fluid Analysiszv84n8kqz2No ratings yet
- Non FermentativeDocument13 pagesNon FermentativeIrish De VeraNo ratings yet
- Fresh Tissue Examination - HistopathDocument4 pagesFresh Tissue Examination - HistopathIrish De VeraNo ratings yet
- Teaching Medical Students Basic Principles of Laboratory MedicineDocument14 pagesTeaching Medical Students Basic Principles of Laboratory MedicineIrish De VeraNo ratings yet
- Lec 2 CarbohydratesDocument10 pagesLec 2 CarbohydratesIrish De VeraNo ratings yet
- Principles of Teaching 1Document7 pagesPrinciples of Teaching 1Irish De VeraNo ratings yet
- S M L S: WhiteDocument9 pagesS M L S: WhiteIrish De VeraNo ratings yet
- Footnote To YouthDocument6 pagesFootnote To YouthIrish De VeraNo ratings yet
- Elective 2 Lecture 1 Concept of IllnessDocument9 pagesElective 2 Lecture 1 Concept of IllnessMelchor Felipe Salvosa100% (1)
- Systemic Lupus ErythematosusDocument40 pagesSystemic Lupus ErythematosusAkshan SentinelNo ratings yet
- Aspek Legal & Etik Keperawatan Komplementer. Hengky IrawanDocument40 pagesAspek Legal & Etik Keperawatan Komplementer. Hengky IrawanBella OctaviaNo ratings yet
- Aranas - Geriatric Assessment ToolDocument14 pagesAranas - Geriatric Assessment ToolNicko Pazon AranasNo ratings yet
- Treatment Efficacy Summary: Dysarthria (Neurological Motor Speech Impairment)Document1 pageTreatment Efficacy Summary: Dysarthria (Neurological Motor Speech Impairment)Mara CadinoiuNo ratings yet
- JC Severe Scrub TyphusDocument27 pagesJC Severe Scrub TyphusAakarsh RastogiNo ratings yet
- Glasgow Coma Scale (GCS) NCLEX Questions Quiz NursingDocument14 pagesGlasgow Coma Scale (GCS) NCLEX Questions Quiz NursingGabrielle G. MaldoNo ratings yet
- 2013 Pneumonia Due To Multidrug-Resistant Leclercia AdecarboxylataDocument3 pages2013 Pneumonia Due To Multidrug-Resistant Leclercia AdecarboxylataLexotanyl LexiNo ratings yet
- Special Needs in The General Education ClassroomDocument15 pagesSpecial Needs in The General Education Classroomapi-267526572No ratings yet
- Clostridium TetaniDocument5 pagesClostridium TetaniMaria Edessa TumbaliNo ratings yet
- Blood Safety IndicatorDocument7 pagesBlood Safety IndicatorCorachea LabNo ratings yet
- Kidney DiseasesDocument45 pagesKidney DiseasesSai ViswasNo ratings yet
- Copy of EnterobiasisDocument1 pageCopy of EnterobiasisCelina GonzalesNo ratings yet
- Respiratory Disorder in PregnancyDocument52 pagesRespiratory Disorder in Pregnancyjhon heriansyahNo ratings yet
- Staphylococci & MicrococciDocument52 pagesStaphylococci & Micrococcihoneylemon.coNo ratings yet
- Infanrix-Hexa SMPC 09 2020Document15 pagesInfanrix-Hexa SMPC 09 2020walkrogNo ratings yet
- Acute Coronary SyndromeDocument59 pagesAcute Coronary SyndromeLouis EkaputraNo ratings yet
- CH 21Document19 pagesCH 21Lisa Evitt CoxNo ratings yet
- NRSG 780 - Health Promotion and Population Health: Module 3: EpidemiologyDocument34 pagesNRSG 780 - Health Promotion and Population Health: Module 3: EpidemiologyjustdoyourNo ratings yet
- Pediatric DosaPediatric Dosages Based On Body Weightges Based On Body WeightDocument7 pagesPediatric DosaPediatric Dosages Based On Body Weightges Based On Body WeightdjbhetaNo ratings yet
- NSG 506 - Cmo 10 Series 1998Document69 pagesNSG 506 - Cmo 10 Series 1998mvfigueroaNo ratings yet
- Principles of Continuous Renal Replacement Therapy For AkiDocument43 pagesPrinciples of Continuous Renal Replacement Therapy For AkiFelicia Risca RyandiniNo ratings yet
- 266-File Utama Naskah-502-1-10-20220701Document9 pages266-File Utama Naskah-502-1-10-20220701cah bagusNo ratings yet
- THE INTEGUMENT ORGAN: The Integument As An Organ and Is An Alternative Name ForDocument16 pagesTHE INTEGUMENT ORGAN: The Integument As An Organ and Is An Alternative Name ForPdianghunNo ratings yet
- Fundamentals of Cardiology For The USMLE and General Medics PDFDocument287 pagesFundamentals of Cardiology For The USMLE and General Medics PDFCharles Vindo100% (2)
- Ayurveda TipsDocument3 pagesAyurveda Tipsgautam_amitNo ratings yet