Professional Documents
Culture Documents
International Archives of Urology and Complications Iauc 8 086
International Archives of Urology and Complications Iauc 8 086
Uploaded by
Ikhsan PrialaksanaCopyright:
Available Formats
You might also like
- TB of The TestesDocument2 pagesTB of The Testesntambik21No ratings yet
- Urology MCQs PDFDocument13 pagesUrology MCQs PDFendiNo ratings yet
- Urological Science: Jiun-Hung Geng, Chun-Nung HuangDocument4 pagesUrological Science: Jiun-Hung Geng, Chun-Nung Huangyerich septaNo ratings yet
- University Journal of Surgery and Surgical Specialities: Dhivya Lakshmi S JDocument4 pagesUniversity Journal of Surgery and Surgical Specialities: Dhivya Lakshmi S JYonathanWaisendiNo ratings yet
- Extra Pelvic Endometriosis: Double Ileal and Ileo-Caecal Localization Revealed by Acute Small Bowel Obstruction, A Clinical CaseDocument9 pagesExtra Pelvic Endometriosis: Double Ileal and Ileo-Caecal Localization Revealed by Acute Small Bowel Obstruction, A Clinical CaseIJAR JOURNALNo ratings yet
- Women Genital Tuberculosis: A Study of Two Cases at Mohammed Vi University Hospital in MarrakechDocument5 pagesWomen Genital Tuberculosis: A Study of Two Cases at Mohammed Vi University Hospital in MarrakechIJAR JOURNALNo ratings yet
- Testicular AppendagesDocument4 pagesTesticular AppendagesJohn stamosNo ratings yet
- Testicular Torsion in Undescended TestisDocument5 pagesTesticular Torsion in Undescended TestisjimNo ratings yet
- Laparoschisis: About A Case Report and Literature ReviewDocument10 pagesLaparoschisis: About A Case Report and Literature ReviewIJAR JOURNALNo ratings yet
- La Importancia de La Urografía Por TC en El Diagnóstico Precoz de Variaciones Anatómicas Del Tracto Urogenital Presentación de CasoDocument5 pagesLa Importancia de La Urografía Por TC en El Diagnóstico Precoz de Variaciones Anatómicas Del Tracto Urogenital Presentación de Casojose luis ramirez espinosaNo ratings yet
- Zaid 2013Document3 pagesZaid 2013Teja Laksana NukanaNo ratings yet
- Misdiagnosed Adult Testicular Torsion Case Report PDFDocument5 pagesMisdiagnosed Adult Testicular Torsion Case Report PDFDaylamiNo ratings yet
- Medicine: Intrauterine Device Found in An Ovarian TumorDocument5 pagesMedicine: Intrauterine Device Found in An Ovarian TumorRezky amalia basirNo ratings yet
- Fukui 2016Document13 pagesFukui 2016Aziddin Gani HarahapNo ratings yet
- 1 s2.0 S2221618914600718 MainDocument3 pages1 s2.0 S2221618914600718 MainElizabeth Joan SalimNo ratings yet
- A Rare Case of Colon Cancer in A Young Patient: A Case Report and Literature ReviewDocument5 pagesA Rare Case of Colon Cancer in A Young Patient: A Case Report and Literature ReviewIJAR JOURNALNo ratings yet
- Testicular Torsion: An Analysis of Sixteen Consecutive Cases and A Review of The LiteratureDocument3 pagesTesticular Torsion: An Analysis of Sixteen Consecutive Cases and A Review of The LiteratureLea Bali Ulina SinurayaNo ratings yet
- AgenesiaDocument6 pagesAgenesiaJennifer TorresNo ratings yet
- A Rare Case of Endometriosis in Turners SyndromeDocument3 pagesA Rare Case of Endometriosis in Turners SyndromeElison J PanggaloNo ratings yet
- Complex Case of Ureteropelvic Junction Obstruction 2024 International JournaDocument3 pagesComplex Case of Ureteropelvic Junction Obstruction 2024 International JournaRonald QuezadaNo ratings yet
- 1 s2.0 S221026122100732X MainDocument3 pages1 s2.0 S221026122100732X MainiffaNo ratings yet
- International Journal of Pharmaceutical Science Invention (IJPSI)Document3 pagesInternational Journal of Pharmaceutical Science Invention (IJPSI)inventionjournalsNo ratings yet
- Accepted Manuscript: UrologyDocument12 pagesAccepted Manuscript: UrologyayunikmatulNo ratings yet
- A Rare Case of Appendiceal IntussusceptionDocument6 pagesA Rare Case of Appendiceal IntussusceptionIJAR JOURNALNo ratings yet
- Varicocele 2Document6 pagesVaricocele 2Mella IntaniabellaNo ratings yet
- A Case of Intravaginal Foreign BodyDocument3 pagesA Case of Intravaginal Foreign BodyNara SafaNo ratings yet
- Retroperitoneal Hydatid Cyst Challenging The Dia - 2024 - International JournalDocument4 pagesRetroperitoneal Hydatid Cyst Challenging The Dia - 2024 - International JournalRonald QuezadaNo ratings yet
- Spontaneous Perforated Pyometra With An Intrauterine Device in Menopause: A Case ReportDocument2 pagesSpontaneous Perforated Pyometra With An Intrauterine Device in Menopause: A Case ReportTomy SaputraNo ratings yet
- Case Report: Frican Medical JournalDocument6 pagesCase Report: Frican Medical JournalArief AdamaNo ratings yet
- Corpus Alienum in Rectosigmoid A Case ReportDocument4 pagesCorpus Alienum in Rectosigmoid A Case Reportlina ukagoNo ratings yet
- 1 s2.0 S0022480423002895 MainDocument7 pages1 s2.0 S0022480423002895 Mainlucabarbato23No ratings yet
- Undescended Testis - Current Trends and Guidelines: A Review of The LiteratureDocument11 pagesUndescended Testis - Current Trends and Guidelines: A Review of The LiteratureJihadatul KholilahNo ratings yet
- Diagnosis and Management of An Immature Teratoma During Ovarian Stimulation: A Case ReportDocument3 pagesDiagnosis and Management of An Immature Teratoma During Ovarian Stimulation: A Case Reportmut13No ratings yet
- 5827 16093 1 PBDocument5 pages5827 16093 1 PBTitan LinggastiwiNo ratings yet
- Case ReportDocument3 pagesCase ReportArman MukhtarNo ratings yet
- Managing Ureterocoele in A Teenage GirlDocument6 pagesManaging Ureterocoele in A Teenage GirlAnab Rehan TaseerNo ratings yet
- Medicina 58 01353 v4Document13 pagesMedicina 58 01353 v4PREEDIPAT PHINTHIPNo ratings yet
- Infertility Secondary To An Infected Hydrocele A Case ReportDocument2 pagesInfertility Secondary To An Infected Hydrocele A Case ReportSara AhmedNo ratings yet
- Broad Ligament Fibroid - An Unusual Presentation: Case ReportDocument2 pagesBroad Ligament Fibroid - An Unusual Presentation: Case ReportPriyakrishnaVasamsettiNo ratings yet
- Ectopic Abdominal Pregnancies: About 2 CasesDocument10 pagesEctopic Abdominal Pregnancies: About 2 CasesIJAR JOURNALNo ratings yet
- Scrotal Abscess With A Rare Cause: Ase EportDocument3 pagesScrotal Abscess With A Rare Cause: Ase EportTeja Laksana NukanaNo ratings yet
- Suciu 2017Document3 pagesSuciu 2017Teja Laksana NukanaNo ratings yet
- Stuck Up!!! - Case Report of A Rectal Foreign BodyDocument6 pagesStuck Up!!! - Case Report of A Rectal Foreign BodyIJAR JOURNALNo ratings yet
- Artigo Gravidez EctópicaDocument2 pagesArtigo Gravidez EctópicaKevin UchoaNo ratings yet
- Torsio TestisDocument55 pagesTorsio TestisAulia RizkiaNo ratings yet
- Bazo Errante 2016 REVISED Ijtra1601084Document4 pagesBazo Errante 2016 REVISED Ijtra1601084luisalfredo_montesNo ratings yet
- Journal of Pediatric Surgery Case Reports: Moaied A. Hassan, Hasan K. Gatea, Thura K. Ja'afar, Ahmed O. Fahad TDocument3 pagesJournal of Pediatric Surgery Case Reports: Moaied A. Hassan, Hasan K. Gatea, Thura K. Ja'afar, Ahmed O. Fahad TVero MeidyNo ratings yet
- Pelvis Perineum Cases 04Document5 pagesPelvis Perineum Cases 04Uloko ChristopherNo ratings yet
- Final-Galley Proof 2Document3 pagesFinal-Galley Proof 2rvfz9jw649No ratings yet
- Surgical ArticleDocument8 pagesSurgical ArticleKevin Leo Lucero AragonesNo ratings yet
- Fibrothecoma: Clinical, Radiological and Immunohistochemical Data About An ObservationDocument4 pagesFibrothecoma: Clinical, Radiological and Immunohistochemical Data About An ObservationIJAR JOURNALNo ratings yet
- A Case Study On Successful Ayurvedic Management of Heamorrhagic Ovarian CystDocument4 pagesA Case Study On Successful Ayurvedic Management of Heamorrhagic Ovarian CystEditor IJTSRDNo ratings yet
- Atypical Presentation of Genital ChlamydiaDocument5 pagesAtypical Presentation of Genital ChlamydiaIJAR JOURNALNo ratings yet
- Case Obsos SellyDocument24 pagesCase Obsos SellyDwi CahyaNo ratings yet
- 60 TH Male Spermatic Cord HydroceleDocument2 pages60 TH Male Spermatic Cord HydroceleSofie HanafiahNo ratings yet
- Epididymo-Testicular Ischemia Without TorsionDocument3 pagesEpididymo-Testicular Ischemia Without TorsionCarlos Pacichana AgudeloNo ratings yet
- 1 s2.0 S1930043321006816 MainDocument5 pages1 s2.0 S1930043321006816 MainFatimah AssagafNo ratings yet
- Zhang 2021Document5 pagesZhang 2021miraraspopovic020No ratings yet
- Ovarian TorsionDocument4 pagesOvarian TorsionRiko KuswaraNo ratings yet
- Case Report EndometriosisDocument4 pagesCase Report EndometriosischristinejoanNo ratings yet
- Urological Care for the Transgender Patient: A Comprehensive GuideFrom EverandUrological Care for the Transgender Patient: A Comprehensive GuideDmitriy NikolavskyNo ratings yet
- Guidelines On: Paediatric UrologyDocument72 pagesGuidelines On: Paediatric UrologyPatrascu CristiNo ratings yet
- Acute Scrotal Pain in Pediatric Emergency Medicine: Assessment, Diagnosis, Management, and TreatmentDocument13 pagesAcute Scrotal Pain in Pediatric Emergency Medicine: Assessment, Diagnosis, Management, and Treatmentglory haurissaNo ratings yet
- Chapter 151. Manual Testicular DetorsionDocument7 pagesChapter 151. Manual Testicular DetorsionRichard QiuNo ratings yet
- Ultraspund in Pediatric EmergencyDocument22 pagesUltraspund in Pediatric EmergencyAli Akbar RahmaniNo ratings yet
- Testicular Examination OSCE GuideDocument9 pagesTesticular Examination OSCE Guidecharlyn206No ratings yet
- Acute Scrotum, Differential DiagnosisDocument57 pagesAcute Scrotum, Differential DiagnosisRajesh Menon100% (1)
- Srinivasan 2011Document5 pagesSrinivasan 2011miaubooksNo ratings yet
- Emergency Red Flags: DR - Magdy Khames AlyDocument58 pagesEmergency Red Flags: DR - Magdy Khames AlyJerry AbleNo ratings yet
- Abdominal PainDocument26 pagesAbdominal Painsammy_d6No ratings yet
- Acute Appendicitis in Adults - Clinical Manifestations and Differential Diagnosis - UpToDateDocument9 pagesAcute Appendicitis in Adults - Clinical Manifestations and Differential Diagnosis - UpToDateSebastian CamachoNo ratings yet
- Torsio TestisDocument55 pagesTorsio TestisAulia RizkiaNo ratings yet
- Genitourinary Emergency: Prof. Dr. Mostafa Sakr Genitourinary SurgeryDocument83 pagesGenitourinary Emergency: Prof. Dr. Mostafa Sakr Genitourinary SurgeryKeserovic AdmirNo ratings yet
- Acute Scrotum 231016 PDFDocument50 pagesAcute Scrotum 231016 PDFDany Dias100% (1)
- Epididymitis and OrchitisDocument11 pagesEpididymitis and Orchitiscitra08No ratings yet
- Torsion Testicular Patient Characteristics: Research ArticleDocument5 pagesTorsion Testicular Patient Characteristics: Research Articleghani ikhsan MajidNo ratings yet
- Acute Scrotum - Etiology and ManagementDocument5 pagesAcute Scrotum - Etiology and ManagementM. ANDRI PRASETYONo ratings yet
- Surgery Final Year SyllabusDocument6 pagesSurgery Final Year SyllabusMariam NadeemNo ratings yet
- Top 17 Questions in Urology: in This Chapter, We'll Go Over Common Health Problems in UrologyDocument13 pagesTop 17 Questions in Urology: in This Chapter, We'll Go Over Common Health Problems in UrologyadenwijayaNo ratings yet
- Gambar Usg TestisDocument28 pagesGambar Usg TestisIrfan YHNo ratings yet
- Testicular TorsionDocument9 pagesTesticular TorsionSyedKashifAliNo ratings yet
- Epididymo-Orchitis: Epididymo-Orchitis in Heterosexual Men What Is Epidiymo-Orchitis?Document4 pagesEpididymo-Orchitis: Epididymo-Orchitis in Heterosexual Men What Is Epidiymo-Orchitis?Letchumanan L MarimuthuNo ratings yet
- MCQ AtaglanceDocument34 pagesMCQ AtaglanceSaied Galal67% (3)
- 2017 Pediatric Testicular TorsionDocument12 pages2017 Pediatric Testicular TorsionVladimir BasurtoNo ratings yet
- The Acute ScrotumDocument9 pagesThe Acute ScrotumAnastasia FebriantiNo ratings yet
- Testicular TorsionDocument24 pagesTesticular Torsionamal.fathullah100% (1)
- Male Pelvic Organ 1Document73 pagesMale Pelvic Organ 1Juhar AhamedNo ratings yet
- Orchitis Vs Testicular Torsion Urology ReportDocument13 pagesOrchitis Vs Testicular Torsion Urology ReportRem AlfelorNo ratings yet
- Testicular Torsion Fani FinalDocument31 pagesTesticular Torsion Fani Finalrockblaster80No ratings yet
- Types of Scrotal ConditionsDocument50 pagesTypes of Scrotal ConditionsTaha ERDOĞANNo ratings yet
International Archives of Urology and Complications Iauc 8 086
International Archives of Urology and Complications Iauc 8 086
Uploaded by
Ikhsan PrialaksanaOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
International Archives of Urology and Complications Iauc 8 086
International Archives of Urology and Complications Iauc 8 086
Uploaded by
Ikhsan PrialaksanaCopyright:
Available Formats
ISSN: 2469-5742
Congote et al. Int Arch Urol Complic 2022, 8:086
DOI: 10.23937/2469-5742/1510086
Volume 8 | Issue 2
International Archives of Open Access
Urology and Complications
Case Report
Polyorchidism: A Rare Cause of Testicular Torsion
Juliana Villanueva Congote, MD1*, Stefania Prada1,2, Juliana Arenas1,2, Daniela Varela1, German
Patiño1,2 and Nicolás Fernandez1,2,3
1
Division of Urology, Pontificia Universidad Javeriana, Colombia
Check for
2
Urology Department, Hospital Universitario San Ignacio, Colombia updates
3
Division of Urology, Seattle Children’s Hospital, University of Washington, USA
*Corresponding author: Juliana Villanueva Congote, MD, Division of Urology, Pontificia Universidad Javeriana, Carrera
7 No. 40-62, Bogotá, Colombia, Tel: +57-3017-843-335
Abstract was first described in the XVI century on an autopsy [1].
Later, in 1880,it was confirmed on histological labeling
Background: Polyorchidism is a rare congenital anomaly
[2]. Different theories currently have been proposed to
of the urogenital tract. Usually, it requires conservative
management; however, this varies according to each patient. understand this developmental anomaly. However, the
This report summarizes the possible clinical presentation exact cause is still unknown [3].
and the feasible management options depending on the
patients and testicular characteristics. Concerning the diagnosis, supernumerary testes can
be suspected on clinical examination. Although, in some
Case presentation: 23 years old young male presented
to our outpatient clinic with intermittent left testicular pain cases, testicular pain secondary to torsion can be the
associated with tenderness to palpation. On the physical only positive finding on the physical examination [4].
exam, he had a palpable mass at the upper pole of the left Testicular torsion represents the more frequent cause
testis. He was taken to an MRI, which showed a normal right
for testicular loss. It is considered a surgical emergency
testis with a left mass-dependent of the upper pole of the left
testis. He was discharged after pain control was achieved; because of the opportunity of testicle salvage [5]. The
however, he presented again to the Emergency Room diagnosis should be made clinically, and other causes
with acute left testicular pain one week later. The physical of acute scrotum should be ruled out. In the case of
exam was suggestive of left testicular torsion. He was taken
polyorchidism, testicular torsion may occur by rotation
to surgery for scrotal exploration and bilateral testicular
fixation. Polyorchidism was confirmed intraoperatively. of the entire content of the hemiscrotum or only of the
supernumerary testicle [6].
Conclusions: Polyorchidism is a rare pathology of the male
genitalia. When suspected, a thorough physical examination Most authors suggest that polyorchidism should be
is always mandatory. It is essential to individualize the
confirmed histological and that prophylactic orchidopexy
patients’ cases to decide whether conservative management
is attainable, with radiologic studies support. is necessary. To date, there is no known systematic
analysis that shows the occurrence of polyorchidism,
Keywords
concomitant to malignancies, the reason why more
Gonadal disorders, Urogenital abnormalities, Testis, conservative management has been proposed [4].
Congenital abnormalities, Gonads
We present a case report of a young male of 23 years
Background old with intraoperatively confirmed polyorchidism, along
with a comprehensive literature review. We summarize
Polyorchidism or supplementary testis is a the possible clinical presentation of the pathology
developmental anomaly defined as the presence of along with its feasible management depending on the
more than two testicles [1]. There are several forms of patient’s testicular characteristics.
this feature, being triorchidism the most common one. It
Citation: Congote JV, Prada S, Arenas J, Varela D, Patiño G, et al. (2022) Polyorchidism: A Rare Cause of
Testicular Torsion. Int Arch Urol Complic 8:086. doi.org/10.23937/2469-5742/1510086
Accepted: July 11, 2022; Published: July 13, 2022
Copyright: © 2022 Congote JV, et al. This is an open-access article distributed under the terms of the
Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction
in any medium, provided the original author and source are credited
Congote et al. Int Arch Urol Complic 2022, 8:086 • Page 1 of 6 •
DOI: 10.23937/2469-5742/1510086 ISSN: 2469-5742
Figure 1: US. LT, Left testicle. SLT, Supernumerary left testicle. SLT located in the upper pole of the LT, both with similar
echogenicity.
Figure 2: Figure 2A and 2B MRI. LT, Left testicle. SLT, Supernumerary left testicle, and left testicle showing similar
echogenicity. SLT is located adjacent to the lower pole of the left testicle.
Case Presentation He presented to the Emergency Room with acute
severe left testicular pain one week later. Physical
A healthy 23-year-old male showed to the outpatient
examination was suggestive of left testicular torsion.
clinic presenting a two-year-long left scrotal mass
A new Doppler US was performed, which showed the
sensation and intermittent pain. A solid mass from the
supernumerary testicle in the upper pole of the left
inferior pole of the left testicle was found palpated on
testicle and with decreased vascular flow, supporting
physical examination. It was painless when palpated and
the diagnosis. The patient was taken to the OR and
independent from the epididymis. Testicular ultrasound
underwent scrotal exploration surgery confirming
was performed in the urology department, evidencing
testicular torsion with a supernumerary testicle on the
a left-sided testicle’s lower pole round mass, with the
same echogenicity as the rest of the testicle. The right left side. Testicular fixation was performed bilaterally
testicle was normal, with dimensions of 50 × 31 × 33 using a dartos pouch and fixation of the tunica
mm with a volume of 27 cm3.The left testicle was 36 × albuginea to the dartos layer in the inferior aspect of
24 × 29 for 13 cm3, and the upper pole mass ipsilateral the testicle with 3-0 absorbable sutures. During surgery,
to the left testicle was 14 × 13 × 16 mm with a volume the continuity in the albuginea was evident, so it was
of 1.5 cm3 (Figure 1). Considering the findings suggesting considered that taking the supernumerary testicle out
a peritesticular mass, tumoral markers and a pelvic MRI represented a risk for the integrity of the left testicle,
were ordered. leading to injury or other complications, therefore the
supernumerary testicle was not removed. Intraoperative
Tumor markers were within normal ranges. The MRI findings are described in Figure 3.
showed a right testicle with dimensions of 50 × 31 × 33
mm, a volume of 27 cm3, and a regular right epididymis. The patient attended a post-operatory consultation
The left testicle had a volume of 13 cm3, an image in nine days after surgery. The pain was controlled, and
the inferior pole with similar characteristics to the no other complications were addressed. After four
testicular parenchyma was found, corresponding to an months, the patient went to another appointment;
accessory testicle of 1.5 cm3 (Figure 2). Testicular biopsy this time, he presented with testicular pain. He had a
was omitted considering the markers and the imaging Doppler ultrasound with no changes from the previous
characteristics. one. Therefore, pain management was prescribed
Congote et al. Int Arch Urol Complic 2022, 8:086 • Page 2 of 6 •
DOI: 10.23937/2469-5742/1510086 ISSN: 2469-5742
Figure 3: Operative findings A-D. LT, Left testicle. RT, Right testicle. SLT, Supernumerary left testicle. LE, Left Epididymis.
with sertraline and a short cycle of non-steroidal anti- testosterone levels and the Mullerian Inhibiting
inflammatory drugs. Factor (MIF), the male genital systems will derive
from the Wolffian ducts. In contrast, the potentially
Discussion and Literature Review preprogrammed Mullerian ducts will be inhibited to
We conducted a literature review in Embase using enhance testes’ production instead of ovaries. Thus,
‘polyorchidism’, finding 278 results dating from 1948 the male paramesonephric (Mullerian) duct disappears
to January 2021. Only cases reports were considered; except its upper end, which will persist as an appendix
200 case reports worldwide were found. A language [7].
filter was included during the literature search; only
The physiologic process to develop normal testes
case reports written in English were included. The
has been widely described. Moreover, the embryologic
present manuscript aims to depict the current available
sequences that enable supernumerary testicles are
understanding of this unusual feature.
yet to be elucidated. The current debate about the
Embryologic and developmental considerations matter includes theories involving irregular migrations
of cell populations inducing a longitudinal duplication
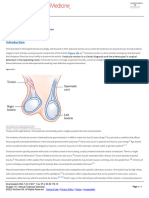
In the fifth to sixth week of development, both the
of the genital ridge and the presence of peritoneal
right and left intermediate mesoderm gives rise to a
mesenchymal expansions causing transverse division
structure called the urogenital ridge. It has two portions,
over the genital ridge [2,7]. The above can result in
a lateral and wider nephrogenic portion and a more
a complete or incomplete duplication with a fully
medial one, the gonadal portion. This primitive gonadal
separated testis and epididymis [2]. Patients with
structure will receive the migration of the primordial
polyorchidism often present with other anomalies
germ cells formed in the yolk sack. Future gonads will be
such as cryptorchidism, spermatic cord torsions, or
developed after induction and differentiation [7]. In this
neoplasms [2].
sense, the gonadal development in terms of quality and
quantity depends significantly on an induction process. Classification systems
In the male embryo case, this process is determined by
No consensus on the classification of polyorchidism
the presence of the SRY gene [8].
has been stated. However, different authors have created
In a subsequent process, dependent on high distinct categorizations. In 1988, Leung, et al. described
Congote et al. Int Arch Urol Complic 2022, 8:086 • Page 3 of 6 •
DOI: 10.23937/2469-5742/1510086 ISSN: 2469-5742
the first anatomical classification of polyorchidism intermittent pain in the left groin, associated with
according to anatomical variations [9]. Later on, in long-standing mass sensation, exacerbated in a short
1991, Thum, et al. published a new classification based period [14]. In other cases, the patient presented with
on the embryologic origin and functionality [10,11]. left scrotal pain without scrotal swelling or severe
Even though these two classifications helped sort this pain in the scrotum of short-time evolution [15]. Our
developmental anomaly, no surgical management patient reported a two-year left scrotal mass sensation
guidance was proposed. with intermittent pain, exacerbated one week before
admission to the emergency room for testicular torsion
One year after Thum’s classification system was
on the left side. In the above-reported cases, there is
described, Singer, et al. created a new classification
no history of trauma. Severe pain has been present
based on the testes’ anatomy and reproductive potential
for a short time, and patients’ primary concern in the
to help surgical management [7]. This system is based
emergency room was the severe onset of scrotal or groin
on the anatomic and functional arrangements and
pain. Furthermore, Bergholz, et al. found an association
the drainage systems combined with possible surgical
of polyorchidism with pseudohermaphroditism,
complications. This classification helped elucidate a
nephrolithiasis, and infertility. Additionally, of the
management strategy [7].
140 cases with histological confirmation reported in
Finally, in 2007, Bergholz and colleagues presented the study mentioned above, only 23 patients (16%)
a new anatomical system regarding polyorchidism’s presented with painless scrotal or inguinal swelling
functional taxonomy. Testis being drained by a deferent without any other symptoms or disease [16].
duct were classified as a type A divided into three
It is worth mentioning that most patients with
subcategories. In A1, the drained supernumerary testis
polyorchidism have a standard 46, XY karyotype.
had its epididymis and vas. If the drained supernumerary
Nevertheless, chromosomal irregularities such as 46,
testis had its epididymis but shared a common deferent
XX, XY mosaicism, and deletion of the long arm of the
duct, it is A2. In A3, the drained supernumerary testis
21st chromosome have been reported [17].
shared a common epididymis. The testes that were not
drained by a deferent duct were classified as a type B, Diagnosis
divided into B1 and B2. In B1, the testis did have its own
In most cases, polyorchidism is suspected by clinical
epididymis, while in B2, the testis did not have its own
examination as an incidental finding. Still, according to
epididymis; Therefore, consisting of testicular tissue
Bergholz, et al. the diagnoses should be supported by
only [4]. Our patient is a polyorchidism type A3.
images. Hydrocele, spermatocele, varicocele, Morgagni
Clinical manifestations cyst, or testicular neoplasm can be mistaken for a
Commonly, patients with polyorchidism are supernumerary testis. Additionally, an undescended
diagnosed in childhood or teenage years due to the testis in the groin area can be wrongly diagnosed as an
appearance of intermittent testicular pain associated inguinal hernia [16].
with a palpable mass [1]. However, our patient was an Some authors argue that ultrasound alone is enough
adult that presented to the Emergency Room with new- to make the final diagnosis [18]. However, a Doppler
onset testicular pain. The most frequent presentation ultrasound or an MRI can also be helpful for diagnosis.
is triorchidism, and the supernumerary testis is most The ultrasound will identify a scrotal mass identical to
frequently located on the left side [12], as in our patient. the ipsilateral testis on every ultrasonographic technique
The location explanation might be that the left testis is performed, as is shown in our case in Figure 1 [19]. The
more prone to subdivision because of its greater size Doppler will report a mass separated from the testis
and different vascular topographic anatomy. However, with a gray-scale ultrasound pattern, showing similar
this has not been proved [12,13]. echogenicity or slightly less echogenic than the normal
Congenital anomaly has been associated with testis, and provides information on the vascularity and
cryptorchidism (40%), hernias (30%), torsion (15%), viability of the gonad [20]. Meanwhile, on the MRI, a
hydrocele (9%), and malignancy in 6% of cases [1]. This typical oval or round structure can be observed with the
case is clinically relevant because the extra testicle signal characteristics of the testicles: a homogeneous
caused the left testicle torsion. It corresponds to an intermediate signal intensity on T1 and high intensity on
unusual presentation, but it is a differential diagnosis that T2. In some cases, the MRI will not provide additional
should be considered. Additionally, in some patients, information than the one found on the sonography.
polyorchidism might present as persistent fertility However, the MRI would play a confirmative diagnosis
after vasectomy, retractable testes, or ureteropelvic role [21].
duplicity, which would be explained by the common Furthermore, new techniques cannot always
embryologic origin of the ureter and the vas [11]. differentiate between supernumerary testes and other
Our literature review found that in two reported kinds of testicular masses. Therefore, a close follow-up,
cases, the patients presented to the urologist with including serological markers for malignancy, must be
Congote et al. Int Arch Urol Complic 2022, 8:086 • Page 4 of 6 •
DOI: 10.23937/2469-5742/1510086 ISSN: 2469-5742
done if the patient does not undergo surgical exploration Competing Interests
or biopsy [12].
The authors declare that they have no competing
Management interests.
Management of polyorchidism has been Author Contribution
controversial since this congenital anomaly of the male
All authors made a significant contribution to the
urogenital tract was first described [22]. Previously, it
work reported, whether that is in the conception, study
was reasonable to remove the supernumerary testis
design, execution, acquisition of data, analysis and
regardless of its location because of the incidence of
interpretation, or in all these areas; took part in drafting,
testicular torsion and the suspected malignancy [16]. revising or critically reviewing the article; gave final
However, in 1987, more conservative management approval of the version to be published; have agreed on
was proposed with the advent of ultrasound and MRI the journal to which the article has been submitted; and
[16]. Some authors have suggested that if there is no agree to be accountable for all aspects of the work.
coexistent disorder and testicular tumor markers are
Funding
negative for a malignant disease, surgical exploration or
biopsy is unnecessary, and patients can be followed up This research did not receive any specific grant from
conservatively [12]. funding agencies in the public, commercial, or not-for-
profit sectors.
In 2008, Khedis, et al. proposed polyorchidism
management based on a simple Polyorchidism References
classification or a Complicated Polyorchidism. A simple 1. Olano Grasa I, Llarena Ibarguren R, García-Olaverri
case is when the supernumerary testes were in an Rodríguez J, Azurmendi Arin I, Cantón Aller E, et al. (2009)
orthotopic position without any malignancy signs or Poliorquidismo. Archivos Españoles de Urología (Ed.
impresa) 62: 59-62.
association with other abnormalities. They suggested
2. Uğuz S, Gürağaç A, Demirer Z, Yilmaz S, Aydur E (2017)
surveillance with physical examination and testicular
Bilateral polyorchidism with ipsilateral two undescended
ultrasound in these patients. Complicated polyorchidism testes: A rare congenital anomaly. Andrologia 49.
is defined as supernumerary testis associated with
3. Ojili V, Shanbhogue AKP, Doherty GP (2009) An unusual
malignancy or abnormalities. In this case, they case of polyorchidism with three homolateral testes and
considered radical orchiectomy of all testes on the contralateral anorchia. Eur J Radiol Extra 72: e129-e131.
suspicious side [23]. Finally, Khedis, et al. propose that in 4. Bergholz R, Koch B, Spieker T, Lohse K (2007)
young patients with polyorchidism plus cryptorchidism, Polyorchidism: A case report and classification. J Pediatr
orchidopexy and observation should be done, if feasible Surg 42: 1933-1935.
[23]. The management of polyorchidism depends on 5. Sharp VJ, Kieran K, Arlen AM (2013) Testicular Torsion:
the patient’s age, the testicular location, size, and the Diagnosis, Evaluation, and Management. Am Fam
Physician 88: 835-840.
anatomical organization of its drainage system [24].
6. Amodio JB, Maybody M, Slowotsky C, Fried K, Foresto C
Conclusions (2004) Polyorchidism. J Ultrasound Med 23: 951-957.
Polyorchidism is a rare developmental anomaly 7. Singer BR, Donaldson JG, Jackson DS (1992)
Polyorchidism: Functional classification and management
of the male genital tract whose exact causes remain strategy. Urology 39: 384-388.
unknown. Typically, patients will present to the
8. Morton CC, Lee C (2009) Cytogenetics in reproduction.
urologist with intermittent scrotal pain associated with In: Strauss JF, Barbieri RLBT-Y, JRE, WB Saunders
a mass sensation. Testicular torsion might be present in Philadelphia, 777-799.
15% of the patients. In testicular torsion symptomatic 9. Tonape T, Singh G, Koushik P, Tumepalli T (2012)
patients’ scrotal exploration and fixation of the testicle Triorchidism: A rare genitourinary abnormality. J Surg Tech
is recommended. Patients must continue active Case Rep 4: 126-128.
surveillance after surgery. However, there is no evidence 10. Thum G (1991) Polyorchidism: Case report and review of
to determine how long a patient with polyorchidism literature. J Urol 145: 370-372.
must be followed up. 11. Garza-Montúfar ME, Olvera-Posada D (2017)
Polyorchidism: A case presentation and review of the
Ethics Approval and Consent to Participate literature. Rev Mex Urol 77: 143-150.
Not applicable. 12. Bayraktar A, Olcucuoglu E, Sahin I, Bayraktar Y, Tastemur
S, et al. (2010) Management of polyorchidism: Surgery or
Consent for Publication conservative management. J Hum Reprod Sci 3: 162-163.
Written informed consent was obtained from the 13. Shah SN, Miller BM, Geisler E (1992) Polyorchidism
discovered as testicular torsion. Urology 39: 543-544.
patient for publication of this case report and images
usage. 14. Wilson WA, Littler J (1953) Polyorchidism a report of two
cases with torsion. Br J Surg 41: 302-307.
Congote et al. Int Arch Urol Complic 2022, 8:086 • Page 5 of 6 •
DOI: 10.23937/2469-5742/1510086 ISSN: 2469-5742
15. Kumar K, Das D, Shivaraj (2012) Triorchidism with torsion. 21. Yalçinkaya S, Şahin C, Şahin AF (2011) Polyorchidism:
Ann Med Health Sci Res 2: 199-201. Sonographic and magnetic resonance imaging findings. J
Can Urol Assoc 5: 84-86.
16. Bergholz R, Wenke K (2009) Polyorchidism: A meta-
analysis. J Urol 182: 2422-2427. 22. Lawrentschuk N, MacGregor RJ (2004) Polyorchidism: A
case report and review of the literature. ANZ J Surg 74:
17. Artul S, Habib G (2015) Polyorchidism: Two case reports
1130-1132.
and a review of the literature. J Med Case Rep 8.
23. Khedis M, Nohra J, Dierickx L, Walschaerts M, Soulié M, et
18. Myers A, Morganstern B, Fine R (2017) A unique case of
al. (2008) Polyorchidism: Presentation of 2 cases, review
pentaorchidism. Urology 104: 196-197.
of the literature and a new management strategy. Urol Int
19. Rafailidis V, Arvaniti M, Rafailidis D, Sfoungaris D (2017) 80: 98-101.
Multiparametric ultrasound findings in a patient with
24. Savas M, Yeni E, Ciftci H, Cece H, Topal U, et al. (2010)
polyorchidism. Ultrasound 25: 177-181.
Polyorchidism: A three-case report and review of the
20. Fonseca-sosa FK (2019) Casos Clínicos 72: 616-618. literature. Andrologia 42: 57-61.
Congote et al. Int Arch Urol Complic 2022, 8:086 • Page 6 of 6 •
You might also like
- TB of The TestesDocument2 pagesTB of The Testesntambik21No ratings yet
- Urology MCQs PDFDocument13 pagesUrology MCQs PDFendiNo ratings yet
- Urological Science: Jiun-Hung Geng, Chun-Nung HuangDocument4 pagesUrological Science: Jiun-Hung Geng, Chun-Nung Huangyerich septaNo ratings yet
- University Journal of Surgery and Surgical Specialities: Dhivya Lakshmi S JDocument4 pagesUniversity Journal of Surgery and Surgical Specialities: Dhivya Lakshmi S JYonathanWaisendiNo ratings yet
- Extra Pelvic Endometriosis: Double Ileal and Ileo-Caecal Localization Revealed by Acute Small Bowel Obstruction, A Clinical CaseDocument9 pagesExtra Pelvic Endometriosis: Double Ileal and Ileo-Caecal Localization Revealed by Acute Small Bowel Obstruction, A Clinical CaseIJAR JOURNALNo ratings yet
- Women Genital Tuberculosis: A Study of Two Cases at Mohammed Vi University Hospital in MarrakechDocument5 pagesWomen Genital Tuberculosis: A Study of Two Cases at Mohammed Vi University Hospital in MarrakechIJAR JOURNALNo ratings yet
- Testicular AppendagesDocument4 pagesTesticular AppendagesJohn stamosNo ratings yet
- Testicular Torsion in Undescended TestisDocument5 pagesTesticular Torsion in Undescended TestisjimNo ratings yet
- Laparoschisis: About A Case Report and Literature ReviewDocument10 pagesLaparoschisis: About A Case Report and Literature ReviewIJAR JOURNALNo ratings yet
- La Importancia de La Urografía Por TC en El Diagnóstico Precoz de Variaciones Anatómicas Del Tracto Urogenital Presentación de CasoDocument5 pagesLa Importancia de La Urografía Por TC en El Diagnóstico Precoz de Variaciones Anatómicas Del Tracto Urogenital Presentación de Casojose luis ramirez espinosaNo ratings yet
- Zaid 2013Document3 pagesZaid 2013Teja Laksana NukanaNo ratings yet
- Misdiagnosed Adult Testicular Torsion Case Report PDFDocument5 pagesMisdiagnosed Adult Testicular Torsion Case Report PDFDaylamiNo ratings yet
- Medicine: Intrauterine Device Found in An Ovarian TumorDocument5 pagesMedicine: Intrauterine Device Found in An Ovarian TumorRezky amalia basirNo ratings yet
- Fukui 2016Document13 pagesFukui 2016Aziddin Gani HarahapNo ratings yet
- 1 s2.0 S2221618914600718 MainDocument3 pages1 s2.0 S2221618914600718 MainElizabeth Joan SalimNo ratings yet
- A Rare Case of Colon Cancer in A Young Patient: A Case Report and Literature ReviewDocument5 pagesA Rare Case of Colon Cancer in A Young Patient: A Case Report and Literature ReviewIJAR JOURNALNo ratings yet
- Testicular Torsion: An Analysis of Sixteen Consecutive Cases and A Review of The LiteratureDocument3 pagesTesticular Torsion: An Analysis of Sixteen Consecutive Cases and A Review of The LiteratureLea Bali Ulina SinurayaNo ratings yet
- AgenesiaDocument6 pagesAgenesiaJennifer TorresNo ratings yet
- A Rare Case of Endometriosis in Turners SyndromeDocument3 pagesA Rare Case of Endometriosis in Turners SyndromeElison J PanggaloNo ratings yet
- Complex Case of Ureteropelvic Junction Obstruction 2024 International JournaDocument3 pagesComplex Case of Ureteropelvic Junction Obstruction 2024 International JournaRonald QuezadaNo ratings yet
- 1 s2.0 S221026122100732X MainDocument3 pages1 s2.0 S221026122100732X MainiffaNo ratings yet
- International Journal of Pharmaceutical Science Invention (IJPSI)Document3 pagesInternational Journal of Pharmaceutical Science Invention (IJPSI)inventionjournalsNo ratings yet
- Accepted Manuscript: UrologyDocument12 pagesAccepted Manuscript: UrologyayunikmatulNo ratings yet
- A Rare Case of Appendiceal IntussusceptionDocument6 pagesA Rare Case of Appendiceal IntussusceptionIJAR JOURNALNo ratings yet
- Varicocele 2Document6 pagesVaricocele 2Mella IntaniabellaNo ratings yet
- A Case of Intravaginal Foreign BodyDocument3 pagesA Case of Intravaginal Foreign BodyNara SafaNo ratings yet
- Retroperitoneal Hydatid Cyst Challenging The Dia - 2024 - International JournalDocument4 pagesRetroperitoneal Hydatid Cyst Challenging The Dia - 2024 - International JournalRonald QuezadaNo ratings yet
- Spontaneous Perforated Pyometra With An Intrauterine Device in Menopause: A Case ReportDocument2 pagesSpontaneous Perforated Pyometra With An Intrauterine Device in Menopause: A Case ReportTomy SaputraNo ratings yet
- Case Report: Frican Medical JournalDocument6 pagesCase Report: Frican Medical JournalArief AdamaNo ratings yet
- Corpus Alienum in Rectosigmoid A Case ReportDocument4 pagesCorpus Alienum in Rectosigmoid A Case Reportlina ukagoNo ratings yet
- 1 s2.0 S0022480423002895 MainDocument7 pages1 s2.0 S0022480423002895 Mainlucabarbato23No ratings yet
- Undescended Testis - Current Trends and Guidelines: A Review of The LiteratureDocument11 pagesUndescended Testis - Current Trends and Guidelines: A Review of The LiteratureJihadatul KholilahNo ratings yet
- Diagnosis and Management of An Immature Teratoma During Ovarian Stimulation: A Case ReportDocument3 pagesDiagnosis and Management of An Immature Teratoma During Ovarian Stimulation: A Case Reportmut13No ratings yet
- 5827 16093 1 PBDocument5 pages5827 16093 1 PBTitan LinggastiwiNo ratings yet
- Case ReportDocument3 pagesCase ReportArman MukhtarNo ratings yet
- Managing Ureterocoele in A Teenage GirlDocument6 pagesManaging Ureterocoele in A Teenage GirlAnab Rehan TaseerNo ratings yet
- Medicina 58 01353 v4Document13 pagesMedicina 58 01353 v4PREEDIPAT PHINTHIPNo ratings yet
- Infertility Secondary To An Infected Hydrocele A Case ReportDocument2 pagesInfertility Secondary To An Infected Hydrocele A Case ReportSara AhmedNo ratings yet
- Broad Ligament Fibroid - An Unusual Presentation: Case ReportDocument2 pagesBroad Ligament Fibroid - An Unusual Presentation: Case ReportPriyakrishnaVasamsettiNo ratings yet
- Ectopic Abdominal Pregnancies: About 2 CasesDocument10 pagesEctopic Abdominal Pregnancies: About 2 CasesIJAR JOURNALNo ratings yet
- Scrotal Abscess With A Rare Cause: Ase EportDocument3 pagesScrotal Abscess With A Rare Cause: Ase EportTeja Laksana NukanaNo ratings yet
- Suciu 2017Document3 pagesSuciu 2017Teja Laksana NukanaNo ratings yet
- Stuck Up!!! - Case Report of A Rectal Foreign BodyDocument6 pagesStuck Up!!! - Case Report of A Rectal Foreign BodyIJAR JOURNALNo ratings yet
- Artigo Gravidez EctópicaDocument2 pagesArtigo Gravidez EctópicaKevin UchoaNo ratings yet
- Torsio TestisDocument55 pagesTorsio TestisAulia RizkiaNo ratings yet
- Bazo Errante 2016 REVISED Ijtra1601084Document4 pagesBazo Errante 2016 REVISED Ijtra1601084luisalfredo_montesNo ratings yet
- Journal of Pediatric Surgery Case Reports: Moaied A. Hassan, Hasan K. Gatea, Thura K. Ja'afar, Ahmed O. Fahad TDocument3 pagesJournal of Pediatric Surgery Case Reports: Moaied A. Hassan, Hasan K. Gatea, Thura K. Ja'afar, Ahmed O. Fahad TVero MeidyNo ratings yet
- Pelvis Perineum Cases 04Document5 pagesPelvis Perineum Cases 04Uloko ChristopherNo ratings yet
- Final-Galley Proof 2Document3 pagesFinal-Galley Proof 2rvfz9jw649No ratings yet
- Surgical ArticleDocument8 pagesSurgical ArticleKevin Leo Lucero AragonesNo ratings yet
- Fibrothecoma: Clinical, Radiological and Immunohistochemical Data About An ObservationDocument4 pagesFibrothecoma: Clinical, Radiological and Immunohistochemical Data About An ObservationIJAR JOURNALNo ratings yet
- A Case Study On Successful Ayurvedic Management of Heamorrhagic Ovarian CystDocument4 pagesA Case Study On Successful Ayurvedic Management of Heamorrhagic Ovarian CystEditor IJTSRDNo ratings yet
- Atypical Presentation of Genital ChlamydiaDocument5 pagesAtypical Presentation of Genital ChlamydiaIJAR JOURNALNo ratings yet
- Case Obsos SellyDocument24 pagesCase Obsos SellyDwi CahyaNo ratings yet
- 60 TH Male Spermatic Cord HydroceleDocument2 pages60 TH Male Spermatic Cord HydroceleSofie HanafiahNo ratings yet
- Epididymo-Testicular Ischemia Without TorsionDocument3 pagesEpididymo-Testicular Ischemia Without TorsionCarlos Pacichana AgudeloNo ratings yet
- 1 s2.0 S1930043321006816 MainDocument5 pages1 s2.0 S1930043321006816 MainFatimah AssagafNo ratings yet
- Zhang 2021Document5 pagesZhang 2021miraraspopovic020No ratings yet
- Ovarian TorsionDocument4 pagesOvarian TorsionRiko KuswaraNo ratings yet
- Case Report EndometriosisDocument4 pagesCase Report EndometriosischristinejoanNo ratings yet
- Urological Care for the Transgender Patient: A Comprehensive GuideFrom EverandUrological Care for the Transgender Patient: A Comprehensive GuideDmitriy NikolavskyNo ratings yet
- Guidelines On: Paediatric UrologyDocument72 pagesGuidelines On: Paediatric UrologyPatrascu CristiNo ratings yet
- Acute Scrotal Pain in Pediatric Emergency Medicine: Assessment, Diagnosis, Management, and TreatmentDocument13 pagesAcute Scrotal Pain in Pediatric Emergency Medicine: Assessment, Diagnosis, Management, and Treatmentglory haurissaNo ratings yet
- Chapter 151. Manual Testicular DetorsionDocument7 pagesChapter 151. Manual Testicular DetorsionRichard QiuNo ratings yet
- Ultraspund in Pediatric EmergencyDocument22 pagesUltraspund in Pediatric EmergencyAli Akbar RahmaniNo ratings yet
- Testicular Examination OSCE GuideDocument9 pagesTesticular Examination OSCE Guidecharlyn206No ratings yet
- Acute Scrotum, Differential DiagnosisDocument57 pagesAcute Scrotum, Differential DiagnosisRajesh Menon100% (1)
- Srinivasan 2011Document5 pagesSrinivasan 2011miaubooksNo ratings yet
- Emergency Red Flags: DR - Magdy Khames AlyDocument58 pagesEmergency Red Flags: DR - Magdy Khames AlyJerry AbleNo ratings yet
- Abdominal PainDocument26 pagesAbdominal Painsammy_d6No ratings yet
- Acute Appendicitis in Adults - Clinical Manifestations and Differential Diagnosis - UpToDateDocument9 pagesAcute Appendicitis in Adults - Clinical Manifestations and Differential Diagnosis - UpToDateSebastian CamachoNo ratings yet
- Torsio TestisDocument55 pagesTorsio TestisAulia RizkiaNo ratings yet
- Genitourinary Emergency: Prof. Dr. Mostafa Sakr Genitourinary SurgeryDocument83 pagesGenitourinary Emergency: Prof. Dr. Mostafa Sakr Genitourinary SurgeryKeserovic AdmirNo ratings yet
- Acute Scrotum 231016 PDFDocument50 pagesAcute Scrotum 231016 PDFDany Dias100% (1)
- Epididymitis and OrchitisDocument11 pagesEpididymitis and Orchitiscitra08No ratings yet
- Torsion Testicular Patient Characteristics: Research ArticleDocument5 pagesTorsion Testicular Patient Characteristics: Research Articleghani ikhsan MajidNo ratings yet
- Acute Scrotum - Etiology and ManagementDocument5 pagesAcute Scrotum - Etiology and ManagementM. ANDRI PRASETYONo ratings yet
- Surgery Final Year SyllabusDocument6 pagesSurgery Final Year SyllabusMariam NadeemNo ratings yet
- Top 17 Questions in Urology: in This Chapter, We'll Go Over Common Health Problems in UrologyDocument13 pagesTop 17 Questions in Urology: in This Chapter, We'll Go Over Common Health Problems in UrologyadenwijayaNo ratings yet
- Gambar Usg TestisDocument28 pagesGambar Usg TestisIrfan YHNo ratings yet
- Testicular TorsionDocument9 pagesTesticular TorsionSyedKashifAliNo ratings yet
- Epididymo-Orchitis: Epididymo-Orchitis in Heterosexual Men What Is Epidiymo-Orchitis?Document4 pagesEpididymo-Orchitis: Epididymo-Orchitis in Heterosexual Men What Is Epidiymo-Orchitis?Letchumanan L MarimuthuNo ratings yet
- MCQ AtaglanceDocument34 pagesMCQ AtaglanceSaied Galal67% (3)
- 2017 Pediatric Testicular TorsionDocument12 pages2017 Pediatric Testicular TorsionVladimir BasurtoNo ratings yet
- The Acute ScrotumDocument9 pagesThe Acute ScrotumAnastasia FebriantiNo ratings yet
- Testicular TorsionDocument24 pagesTesticular Torsionamal.fathullah100% (1)
- Male Pelvic Organ 1Document73 pagesMale Pelvic Organ 1Juhar AhamedNo ratings yet
- Orchitis Vs Testicular Torsion Urology ReportDocument13 pagesOrchitis Vs Testicular Torsion Urology ReportRem AlfelorNo ratings yet
- Testicular Torsion Fani FinalDocument31 pagesTesticular Torsion Fani Finalrockblaster80No ratings yet
- Types of Scrotal ConditionsDocument50 pagesTypes of Scrotal ConditionsTaha ERDOĞANNo ratings yet