Professional Documents
Culture Documents
12.1 Waste Excretion and Equilibrium: Anatomy of The Urinary System
12.1 Waste Excretion and Equilibrium: Anatomy of The Urinary System
Uploaded by
Vivian TangCopyright:
Available Formats
You might also like
- DR. SEBI KIDNEY FAILURE SOLUTION: Dialysis-Free Living. A Natural Approach to Treating and Preventing Chronic Kidney Disease (2022 Guide for Beginners)From EverandDR. SEBI KIDNEY FAILURE SOLUTION: Dialysis-Free Living. A Natural Approach to Treating and Preventing Chronic Kidney Disease (2022 Guide for Beginners)Rating: 5 out of 5 stars5/5 (2)
- Acute Glomerulonephritis Case StudyDocument12 pagesAcute Glomerulonephritis Case StudyPrincess Tindugan100% (1)
- AAP Module 9 SupplementDocument20 pagesAAP Module 9 Supplementmaryelle conejarNo ratings yet
- Nursing Pharmacology COMPLETEDocument40 pagesNursing Pharmacology COMPLETEMonique Leonardo100% (8)
- Excretion ExcretionDocument7 pagesExcretion ExcretionWaleed Bin KhalidNo ratings yet
- Mechanism of Urine FormationsDocument20 pagesMechanism of Urine FormationsGAURAVNo ratings yet
- Blood Supply of The Urinary Excretory System: AnatomyDocument3 pagesBlood Supply of The Urinary Excretory System: AnatomyJhe CaselNo ratings yet
- The Kidney (Anatomy)Document3 pagesThe Kidney (Anatomy)Nina Ann LiwanagNo ratings yet
- The Human Excretory System Functions To Remove Waste From The Human BodyDocument2 pagesThe Human Excretory System Functions To Remove Waste From The Human BodyrawatanandNo ratings yet
- Excretion (Continued)Document9 pagesExcretion (Continued)t0000123No ratings yet
- Kidney Function: What Do The Kidneys Do?Document4 pagesKidney Function: What Do The Kidneys Do?A Mazid Zabir IINo ratings yet
- Excretion 1Document21 pagesExcretion 1ßéršerK4040 KyùNo ratings yet
- ExcretionDocument15 pagesExcretionAisha Ali - 49549/TCHR/EKNNCNo ratings yet
- The Urinary System: Excretion: The Removal ofDocument18 pagesThe Urinary System: Excretion: The Removal ofRifa YulianiNo ratings yet
- The Excretory SystemDocument15 pagesThe Excretory SystemHarshil PatelNo ratings yet
- The Human Excretory SystemDocument7 pagesThe Human Excretory Systemdonnah_veraNo ratings yet
- Pecularities of Renal Circulation and Acid-Base BalanceDocument17 pagesPecularities of Renal Circulation and Acid-Base Balancekazim786ahmedNo ratings yet
- Anatomy of The KidneyDocument7 pagesAnatomy of The KidneyArgie Arguson IINo ratings yet
- Sken D Blok 20 Kel 2 '17Document18 pagesSken D Blok 20 Kel 2 '17dewi fortuna agustiaNo ratings yet
- Biology Notes IGCSE Excretion NoteDocument9 pagesBiology Notes IGCSE Excretion NoteCorina HuNo ratings yet
- Anatomy and PhysiologyDocument17 pagesAnatomy and PhysiologychardiginNo ratings yet
- Anatomy and Physiology: Location and Basic Structure of The KidneysDocument3 pagesAnatomy and Physiology: Location and Basic Structure of The KidneysarnnieNo ratings yet
- Urinalysis and Body FluidsDocument54 pagesUrinalysis and Body FluidsabdishakurNo ratings yet
- 10 Excretion Biology Notes IGCSE 2014 PDFDocument10 pages10 Excretion Biology Notes IGCSE 2014 PDFJohn DeHans67% (3)
- ExcretionDocument17 pagesExcretionsmbdy tbhhhNo ratings yet
- KidneyDocument8 pagesKidneyRaj JadhavNo ratings yet
- 10 Excretion Biology Notes IGCSE 2014Document10 pages10 Excretion Biology Notes IGCSE 2014pyf2nq6gdrNo ratings yet
- Urine Ingredient Analysis: Name: Yunita Punarisma Class: XI IA 3/ 15Document21 pagesUrine Ingredient Analysis: Name: Yunita Punarisma Class: XI IA 3/ 15ladylomoNo ratings yet
- Filtration of Blood in The KidneysDocument12 pagesFiltration of Blood in The KidneysAllan Joseph Bonito CunananNo ratings yet
- Excretion of WaterDocument5 pagesExcretion of WaterKamrul Alam MasumNo ratings yet
- 10 ExcretionDocument3 pages10 ExcretionKavin ManimaranNo ratings yet
- 9.3 NephronDocument15 pages9.3 NephronShehbaaz SinghNo ratings yet
- Excretion HSBDocument9 pagesExcretion HSBNahuuma SmithNo ratings yet
- Urinary System 1. List The Functions of The KidneysDocument6 pagesUrinary System 1. List The Functions of The KidneysheerNo ratings yet
- KidneyDocument5 pagesKidneyecijakaNo ratings yet
- KidneysDocument23 pagesKidneysshaliniNo ratings yet
- Urine FormationDocument3 pagesUrine FormationKatherine Clarisse Carvajal LavariasNo ratings yet
- Excretion: Excretory Organ Excretory ProductDocument3 pagesExcretion: Excretory Organ Excretory ProductKekeletsoNo ratings yet
- Excretion Chapter NotesDocument7 pagesExcretion Chapter NotesMohammad Sayed AliNo ratings yet
- Lecture 4 Excretory SystemDocument18 pagesLecture 4 Excretory Systembabaaijaz01No ratings yet
- The Renal SystemDocument10 pagesThe Renal SystemWahyu Purbo PangestiNo ratings yet
- Human Physiology Ii: School of BiochemistryDocument15 pagesHuman Physiology Ii: School of Biochemistrykeerthana t reddyNo ratings yet
- Acute Glomerulonephritis Case StudyDocument12 pagesAcute Glomerulonephritis Case StudyPrincess Tindugan100% (1)
- Introduction To Excretion in Human BodyDocument11 pagesIntroduction To Excretion in Human Bodyvurn5665No ratings yet
- Introduction To Excretion in Human BodyDocument11 pagesIntroduction To Excretion in Human Bodyvurn5665No ratings yet
- HomeostasisDocument10 pagesHomeostasisSiddhesh YadavNo ratings yet
- ExcretionDocument4 pagesExcretionnisha dolasNo ratings yet
- Diagram of The KidneyDocument3 pagesDiagram of The KidneyElienai de LeonNo ratings yet
- Vocabulary of Urinary System: Ingles Medico Ii - Clase 6Document6 pagesVocabulary of Urinary System: Ingles Medico Ii - Clase 6Agustín Bravo ArreyesNo ratings yet
- Excretory System: ComponentsDocument3 pagesExcretory System: ComponentsKuldeep KMRNo ratings yet
- 1.4 Virtual Patient - Elizabeth Harding: Describe The Structure of The NephronDocument7 pages1.4 Virtual Patient - Elizabeth Harding: Describe The Structure of The NephronAbdullah RajaNo ratings yet
- Uraian Materi Ginjal (English)Document6 pagesUraian Materi Ginjal (English)Novia AnugrahNo ratings yet
- Bio PrsentationDocument1 pageBio Prsentation4L Anisha SieudassNo ratings yet
- Chronic Kidney DiseaseDocument17 pagesChronic Kidney DiseaseAdelle SmithNo ratings yet
- Overview of RENAL: Dr. Wilson Arthur Zein, M. BiomedDocument34 pagesOverview of RENAL: Dr. Wilson Arthur Zein, M. BiomedAnnisNo ratings yet
- Excretory SystemDocument32 pagesExcretory SystemJeanie uyNo ratings yet
- Complete ExcretionDocument61 pagesComplete Excretionethankhoo2007No ratings yet
- Urine Formation Steps Filtration: Dr. Sumaiya KhanDocument4 pagesUrine Formation Steps Filtration: Dr. Sumaiya KhanZeleen Ann SaberonNo ratings yet
- The Formation of UrineDocument4 pagesThe Formation of UrineDanielle Lois Lee YuNo ratings yet
- Kidney NotesDocument5 pagesKidney Notesnad2samNo ratings yet
- Chapter-19 Excretory Products and Their Elimnation: Forms of Nitrogen ExcretionsDocument8 pagesChapter-19 Excretory Products and Their Elimnation: Forms of Nitrogen Excretionsmaryak3050No ratings yet
- Kidney Diseases, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandKidney Diseases, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- PharynxDocument18 pagesPharynxzenith parmarNo ratings yet
- Sun Touched A Paranormal Vampire Romance A Touch of Vampire Book 4 Becky Moynihan Full Chapter PDF ScribdDocument67 pagesSun Touched A Paranormal Vampire Romance A Touch of Vampire Book 4 Becky Moynihan Full Chapter PDF Scribdpatricia.iglesias588100% (8)
- Module 3 - Neural PhsyiologyDocument49 pagesModule 3 - Neural Phsyiologybuy sellNo ratings yet
- Properties of EnzymesDocument7 pagesProperties of Enzymeslcassidy9074No ratings yet
- Electric Shock ChartDocument1 pageElectric Shock Chartbrsharma100% (2)
- Gas Exchange in PlantsDocument19 pagesGas Exchange in PlantsNaureen Khaliq100% (1)
- Ineffective Breathing PatternDocument8 pagesIneffective Breathing PatternJansen Arquilita Rivera100% (2)
- The Healing Power of HumorDocument3 pagesThe Healing Power of HumorJuan Daniel Yanqui GuerreroNo ratings yet
- 6th Espen SymposiumDocument4 pages6th Espen Symposiumyos_peace86No ratings yet
- Stop SmokingDocument16 pagesStop Smokingeduardo virgilioNo ratings yet
- Embriologija CvjetnicaDocument526 pagesEmbriologija CvjetnicaelviraNo ratings yet
- EmotionsDocument58 pagesEmotionsthivyaashini SellaNo ratings yet
- Chapter 1 - The Nervous SystemDocument8 pagesChapter 1 - The Nervous SystemRadha RamineniNo ratings yet
- 003 Pathology MCQ ACEM Primary CardiovascularDocument5 pages003 Pathology MCQ ACEM Primary Cardiovascularbmhsh100% (2)
- Hematologic Reference Ranges A PDFDocument3 pagesHematologic Reference Ranges A PDFmalaimaxNo ratings yet
- Trigeminal NeuralgiaDocument22 pagesTrigeminal NeuralgiaamandarestykbNo ratings yet
- CH 9 Emotions NCERT PDFDocument19 pagesCH 9 Emotions NCERT PDFrerereNo ratings yet
- Educ 106 Module 8Document3 pagesEduc 106 Module 8Jona Charmele DegilloNo ratings yet
- Test Bank For Laboratory Manual For Seeleys Anatomy Physiology 11th Edition Eric Wise 3 DownloadDocument69 pagesTest Bank For Laboratory Manual For Seeleys Anatomy Physiology 11th Edition Eric Wise 3 Downloadcaseyyoungtoekwmcfdi100% (30)
- Overview Female Reproductive AnatomyDocument45 pagesOverview Female Reproductive AnatomyAbebe TilahunNo ratings yet
- PteridophytesDocument61 pagesPteridophytestapas kunduNo ratings yet
- Flow Sheet TemplateDocument4 pagesFlow Sheet TemplateIulia Tania AndronacheNo ratings yet
- Risk FactorsDocument174 pagesRisk FactorsdevikaNo ratings yet
- Class-10 Revision Test - NutritionDocument4 pagesClass-10 Revision Test - NutritionVarshini PeraNo ratings yet
- Semen Analysis (Seminal Cytology, Sperm CountDocument30 pagesSemen Analysis (Seminal Cytology, Sperm Countabdurae100% (1)
- Approach To HeadacheDocument49 pagesApproach To Headachegea pandhita sNo ratings yet
- 2013 h2 BiologyDocument1,838 pages2013 h2 BiologyJustt Mee100% (1)
- From Wikipedia, The Free Encyclopedia: Ornamental Bulbous Plant Bulb (Disambiguation)Document4 pagesFrom Wikipedia, The Free Encyclopedia: Ornamental Bulbous Plant Bulb (Disambiguation)Alexandra Maria NeaguNo ratings yet
12.1 Waste Excretion and Equilibrium: Anatomy of The Urinary System
12.1 Waste Excretion and Equilibrium: Anatomy of The Urinary System
Uploaded by
Vivian TangOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
12.1 Waste Excretion and Equilibrium: Anatomy of The Urinary System
12.1 Waste Excretion and Equilibrium: Anatomy of The Urinary System
Uploaded by
Vivian TangCopyright:
Available Formats
12.
1 Waste Excretion and Equilibrium
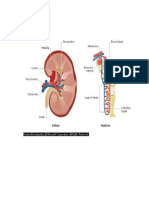
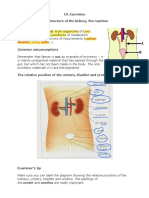
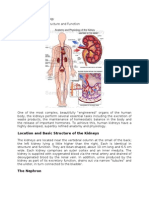
When the body converts large organic molecules into simpler ones, some of these simpler molecules are harmful to the body. In order for life to continue, the body must successfully excrete these toxic substances. The kidneys play a crucial role in removing waste, balancing blood pH, and maintaining water balance. Canadians consume more protein than is required. Protein contains nitrogen. The amino group (NH2) must be excreted from the body. The liver begins this process by converting NH2 to ammonia. This is referred to as deamination. Ammonia is a water-soluble gas and is extremely toxic. In the liver molecules of ammonia combine with carbon dioxide to form urea which is much less toxic. Uric acid is another waste product produced in the liver from the breakdown of nucleic acids, like DNA, for example. The kidneys play a very important role in regulating water balance in the body. You would die in a few days without ingesting water. In order to maintain proper water levels in the body, humans must consume 2 L of fluids each day. Anatomy of the Urinary System Renal arteries bring blood to the kidneys. The kidneys may hold up to 25% of the bodys blood at any one time. Wastes are filtered out of the blood and are carried to the bladder by the ureters. The bladder has a sphincter muscle that helps to control the time of urination. As the bladder fills up, messages are sent to the brain, creating the sensation of having to go. The more full it gets, the stronger the sensation. When urination occurs, urine enters the urethra to be voided from the body. The kidney has an outer layer called the renal cortex. The middle layer is called the renal medulla. The innermost, hollow area is called the renal pelvis. It is from here that urine exits the kidney through the ureter. Nephrons Your kidneys have about 1 000 000 nephrons. They are the functional units, doing the processing required to make urine. A small branch off the renal artery called the afferent arteriole, brings blood to the nephron. The afferent arterioles branch into a capillary bed called the glomerulus. Blood leaves the glomerulus again through the efferent arteriole. Blood then travels through a capillary net called the peritubular capillaries that wrap around the kidney tubule. Blood then leaves the nephron through a venule that meets the renal vein. The glomerulus is surrounded by a funnel-shaped portion of the nephron called the Bowmans capsule. The Bowmans capsule, afferent arteriole, and the efferent arteriole are located in the cortex of the kidney. Fluid to be processed leaves the bloodstream and enters the Bowmans capsule.
The fluid then travels to the proximal tubule. From there it moves on to the loop of Henle (this loop decends into the renal medulla). Urine then moves on to the distal tubule, the last part of the nephron, into the collecting ducts. The collecting ducts drain urine into the renal pelvis. Formation of Urine There are three steps to urine formation. Filtration As blood flows through the glomerulus, fluid moves from it into the Bowmans capsule due to the pressure gradient. Small dissolved molecules move from the glomerulus into the Bowmans capsule. Plasma proteins, blood cells, and platelets are too big to leave the glomerulus and stay behind in the blood. Below is a table that illustrates the presence of various substances in the glomerulus versus the Bowmans capsule: Reabsorption Solute Glomerulus Bowmans Capsule About 20% of the fluid that enters the glomerulus is Water Yes Yes filtered into the nephron. Sodium Yes Yes It is necessary for much of that fluid to be reabsorbed into chloride the bloodstream, otherwise you would create massive Glucose Yes Yes amounts of urine and be constantly dehydrated. Amino acids Yes Yes Aldosterone is a hormone that is essential for proper Hydrogen ions Yes Yes reabsorption. It causes the reabsoption of Na+ ions into the bloodstream. This changes the osmotic balance and as Urea Yes Yes a result, more water moves into the blood from the Plasma Yes No nephron. proteins Erythrocytes Yes No Na+ ions are brought into the nephron by carrier molecules. Negative ions like Cl- and HCO3- are attracted Platelets Yes No to the positive ions and follow them into the nephron as well. The nephron is lined with mitochondria to supply the necessary ATP for this active transport. Reabsorption occurs until the threshold level (the maximum amount of a substance that can be moved into the nephron) is reached. Excess salt is excreted in the urine. Other substances are actively transported from the proximal tubule . Glucose and amino acids attach to carrier molecules that transport them into the blood. Only so much can be reabsorbed though. The rest will be excreted in urine. The more solutes there are in the bloodstream draw water back into the blood as well due to the osmotic gradient. The plasma proteins that stay in the blood also draw water back into the bloodstream from the interstitial fluid as well. As water leaves the nephron and gets reabsorbed, the solutes left in the nephron become very concentrated. Some molecules of urea and uric acid diffuse back into the blood. Secretion Secretion is the movement of wastes from the blood back into the nephron. This includes ammonia, excess H+ ions, and minerals like K+. Even drugs, such as penicillin, can be secreted.
There are many mitochondria in the cells that line the distal tubule. They supply the energy required by carrier molecules to move substances against their concentration gradient back into the nephron. Study Table 3, pg. 383. pH Balance The kidneys also help to restore proper pH in the blood. The body produces several substances that would affect pH levels, such as carbonic acid (from respiration). Carbonic acid and other acids produce H+ ions which lowers pH. The pH balance is maintained by buffer systems that absorb excess H+ ions, or negative ions that act a bases. Bicarbonate ions, HCO3-, buffer excess H+ ions in the blood. This produces carbonic acid. The carbonic acid then breaks down to form carbon dioxide and water. The kidneys reverse this reaction to help restore this buffer system. Carbon dioxide is actively transported from the peritubular capillaries into the nephron. The carbon dioxide then combines with water, generating HCO3- and H+ ions. The bicarbonate ions then diffuse back into the bloodstream where they can be used again to buffer the blood. The H+ ions are excreted in urine.
12.2 Kidney Dysfunction
Many kidney disorders can be diagnosed through urinalysis. Diabetes Mellitus Diabetes mellitus is caused by a low to no secretion of insulin from the islet cells of the pancreas. This causes blood glucose levels to rise. Sufferers need to have daily injections of insulin to control their blood glucose. Reabsorption can move only so much glucose back into the blood. Sufferers of diabetes mellitus have very high blood glucose levels, so there is a lot of glucose that cant be reabsorbed into the blood. As a result, glucose is excreted in their urine. This sets up an osmotic gradient causing a lot of water to be excreted in urine. Therefore, suffers are often dehydrated and thirsty. Diabetes Insipidus Diabetes insipidus is caused by the undersecretion of ADH (antidiuretic hormone) from the pituitary gland. ADH makes the distal tubule and collecting ducts more permeable to water, so urine becomes more concentrated when it is released. People with diabetes insipidus excrete abnormally high amounts of dilute urine, up to 20 L per day. Nephritis The term nephritis is used to describe a number of disorders, all of which cause the inflammation of nephrons. Capillaries in the nephron break and allow blood cells and other large components of blood to find way into the Bowmans capsule, and eventually, urine. Urine will contain blood and test positive for the presence of protein. Protein molecules (among other things) draw more water into the nephron. This increases urine output. Nephritis can lead to kidney failure are even death. Kidney Stones Kidney stones are caused by the precipitation of mineral solutes from the blood. If these stones lodge in the renal pelvis they may block urine from reaching the ureter and being excreted by the body. As the stone moves, it damages tissues and causes terrible pain. To treat kidney stones in the past, surgery was required.
However, nowadays doctors may use high frequency sound waves to blast the stones apart. The smaller granules may be able to be passed without the requirement of surgery. Dialysis Technology If a person cant normally process waste a dialysis machine can help restore the normal solute balance in blood. In dialysis, substances are exchanged across a semipermeable membrane. There are two types of dialysis: hemodialysis and peritoneal dialysis. In hemodialysis, a machine is connected to a patients vein. The patients blood flows through a machine where solutes diffuse out the blood into dialysis solution. As the solution is frequently changed, things like urea and uric acid are being constantly diffused out of the blood. During this dialysis, hormones the kidneys normally make get added to the patients blood. In peritoneal dialysis, 2 L of dialysis fluid is pumped into the abdomen. Urea and other wastes diffuse from tissue into the fluid. Over the course of a day, the fluid is replaced several times. While dialysis has allowed many people to survive long enough to allow their kidneys to heal, or to get a kidney transplant, it is not perfect. It cant produce the hormones that the kidneys make. Kidney Transplants Kidney transplants are successful in about 85% of all cases. A transplanted kidney does a much better job than dialysis. However, kidney transplant patients must take immunosuppressant drugs that have a host of complications. A simple cold becomes a big issue for a transplant patient. In a kidney transplant, a new kidney and new ureter are placed in the lower abdomen, near the groin. The old kidneys are rarely removed.
You might also like
- DR. SEBI KIDNEY FAILURE SOLUTION: Dialysis-Free Living. A Natural Approach to Treating and Preventing Chronic Kidney Disease (2022 Guide for Beginners)From EverandDR. SEBI KIDNEY FAILURE SOLUTION: Dialysis-Free Living. A Natural Approach to Treating and Preventing Chronic Kidney Disease (2022 Guide for Beginners)Rating: 5 out of 5 stars5/5 (2)
- Acute Glomerulonephritis Case StudyDocument12 pagesAcute Glomerulonephritis Case StudyPrincess Tindugan100% (1)
- AAP Module 9 SupplementDocument20 pagesAAP Module 9 Supplementmaryelle conejarNo ratings yet
- Nursing Pharmacology COMPLETEDocument40 pagesNursing Pharmacology COMPLETEMonique Leonardo100% (8)
- Excretion ExcretionDocument7 pagesExcretion ExcretionWaleed Bin KhalidNo ratings yet
- Mechanism of Urine FormationsDocument20 pagesMechanism of Urine FormationsGAURAVNo ratings yet
- Blood Supply of The Urinary Excretory System: AnatomyDocument3 pagesBlood Supply of The Urinary Excretory System: AnatomyJhe CaselNo ratings yet
- The Kidney (Anatomy)Document3 pagesThe Kidney (Anatomy)Nina Ann LiwanagNo ratings yet
- The Human Excretory System Functions To Remove Waste From The Human BodyDocument2 pagesThe Human Excretory System Functions To Remove Waste From The Human BodyrawatanandNo ratings yet
- Excretion (Continued)Document9 pagesExcretion (Continued)t0000123No ratings yet
- Kidney Function: What Do The Kidneys Do?Document4 pagesKidney Function: What Do The Kidneys Do?A Mazid Zabir IINo ratings yet
- Excretion 1Document21 pagesExcretion 1ßéršerK4040 KyùNo ratings yet
- ExcretionDocument15 pagesExcretionAisha Ali - 49549/TCHR/EKNNCNo ratings yet
- The Urinary System: Excretion: The Removal ofDocument18 pagesThe Urinary System: Excretion: The Removal ofRifa YulianiNo ratings yet
- The Excretory SystemDocument15 pagesThe Excretory SystemHarshil PatelNo ratings yet
- The Human Excretory SystemDocument7 pagesThe Human Excretory Systemdonnah_veraNo ratings yet
- Pecularities of Renal Circulation and Acid-Base BalanceDocument17 pagesPecularities of Renal Circulation and Acid-Base Balancekazim786ahmedNo ratings yet
- Anatomy of The KidneyDocument7 pagesAnatomy of The KidneyArgie Arguson IINo ratings yet
- Sken D Blok 20 Kel 2 '17Document18 pagesSken D Blok 20 Kel 2 '17dewi fortuna agustiaNo ratings yet
- Biology Notes IGCSE Excretion NoteDocument9 pagesBiology Notes IGCSE Excretion NoteCorina HuNo ratings yet
- Anatomy and PhysiologyDocument17 pagesAnatomy and PhysiologychardiginNo ratings yet
- Anatomy and Physiology: Location and Basic Structure of The KidneysDocument3 pagesAnatomy and Physiology: Location and Basic Structure of The KidneysarnnieNo ratings yet
- Urinalysis and Body FluidsDocument54 pagesUrinalysis and Body FluidsabdishakurNo ratings yet
- 10 Excretion Biology Notes IGCSE 2014 PDFDocument10 pages10 Excretion Biology Notes IGCSE 2014 PDFJohn DeHans67% (3)
- ExcretionDocument17 pagesExcretionsmbdy tbhhhNo ratings yet
- KidneyDocument8 pagesKidneyRaj JadhavNo ratings yet
- 10 Excretion Biology Notes IGCSE 2014Document10 pages10 Excretion Biology Notes IGCSE 2014pyf2nq6gdrNo ratings yet
- Urine Ingredient Analysis: Name: Yunita Punarisma Class: XI IA 3/ 15Document21 pagesUrine Ingredient Analysis: Name: Yunita Punarisma Class: XI IA 3/ 15ladylomoNo ratings yet
- Filtration of Blood in The KidneysDocument12 pagesFiltration of Blood in The KidneysAllan Joseph Bonito CunananNo ratings yet
- Excretion of WaterDocument5 pagesExcretion of WaterKamrul Alam MasumNo ratings yet
- 10 ExcretionDocument3 pages10 ExcretionKavin ManimaranNo ratings yet
- 9.3 NephronDocument15 pages9.3 NephronShehbaaz SinghNo ratings yet
- Excretion HSBDocument9 pagesExcretion HSBNahuuma SmithNo ratings yet
- Urinary System 1. List The Functions of The KidneysDocument6 pagesUrinary System 1. List The Functions of The KidneysheerNo ratings yet
- KidneyDocument5 pagesKidneyecijakaNo ratings yet
- KidneysDocument23 pagesKidneysshaliniNo ratings yet
- Urine FormationDocument3 pagesUrine FormationKatherine Clarisse Carvajal LavariasNo ratings yet
- Excretion: Excretory Organ Excretory ProductDocument3 pagesExcretion: Excretory Organ Excretory ProductKekeletsoNo ratings yet
- Excretion Chapter NotesDocument7 pagesExcretion Chapter NotesMohammad Sayed AliNo ratings yet
- Lecture 4 Excretory SystemDocument18 pagesLecture 4 Excretory Systembabaaijaz01No ratings yet
- The Renal SystemDocument10 pagesThe Renal SystemWahyu Purbo PangestiNo ratings yet
- Human Physiology Ii: School of BiochemistryDocument15 pagesHuman Physiology Ii: School of Biochemistrykeerthana t reddyNo ratings yet
- Acute Glomerulonephritis Case StudyDocument12 pagesAcute Glomerulonephritis Case StudyPrincess Tindugan100% (1)
- Introduction To Excretion in Human BodyDocument11 pagesIntroduction To Excretion in Human Bodyvurn5665No ratings yet
- Introduction To Excretion in Human BodyDocument11 pagesIntroduction To Excretion in Human Bodyvurn5665No ratings yet
- HomeostasisDocument10 pagesHomeostasisSiddhesh YadavNo ratings yet
- ExcretionDocument4 pagesExcretionnisha dolasNo ratings yet
- Diagram of The KidneyDocument3 pagesDiagram of The KidneyElienai de LeonNo ratings yet
- Vocabulary of Urinary System: Ingles Medico Ii - Clase 6Document6 pagesVocabulary of Urinary System: Ingles Medico Ii - Clase 6Agustín Bravo ArreyesNo ratings yet
- Excretory System: ComponentsDocument3 pagesExcretory System: ComponentsKuldeep KMRNo ratings yet
- 1.4 Virtual Patient - Elizabeth Harding: Describe The Structure of The NephronDocument7 pages1.4 Virtual Patient - Elizabeth Harding: Describe The Structure of The NephronAbdullah RajaNo ratings yet
- Uraian Materi Ginjal (English)Document6 pagesUraian Materi Ginjal (English)Novia AnugrahNo ratings yet
- Bio PrsentationDocument1 pageBio Prsentation4L Anisha SieudassNo ratings yet
- Chronic Kidney DiseaseDocument17 pagesChronic Kidney DiseaseAdelle SmithNo ratings yet
- Overview of RENAL: Dr. Wilson Arthur Zein, M. BiomedDocument34 pagesOverview of RENAL: Dr. Wilson Arthur Zein, M. BiomedAnnisNo ratings yet
- Excretory SystemDocument32 pagesExcretory SystemJeanie uyNo ratings yet
- Complete ExcretionDocument61 pagesComplete Excretionethankhoo2007No ratings yet
- Urine Formation Steps Filtration: Dr. Sumaiya KhanDocument4 pagesUrine Formation Steps Filtration: Dr. Sumaiya KhanZeleen Ann SaberonNo ratings yet
- The Formation of UrineDocument4 pagesThe Formation of UrineDanielle Lois Lee YuNo ratings yet
- Kidney NotesDocument5 pagesKidney Notesnad2samNo ratings yet
- Chapter-19 Excretory Products and Their Elimnation: Forms of Nitrogen ExcretionsDocument8 pagesChapter-19 Excretory Products and Their Elimnation: Forms of Nitrogen Excretionsmaryak3050No ratings yet
- Kidney Diseases, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandKidney Diseases, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- PharynxDocument18 pagesPharynxzenith parmarNo ratings yet
- Sun Touched A Paranormal Vampire Romance A Touch of Vampire Book 4 Becky Moynihan Full Chapter PDF ScribdDocument67 pagesSun Touched A Paranormal Vampire Romance A Touch of Vampire Book 4 Becky Moynihan Full Chapter PDF Scribdpatricia.iglesias588100% (8)
- Module 3 - Neural PhsyiologyDocument49 pagesModule 3 - Neural Phsyiologybuy sellNo ratings yet
- Properties of EnzymesDocument7 pagesProperties of Enzymeslcassidy9074No ratings yet
- Electric Shock ChartDocument1 pageElectric Shock Chartbrsharma100% (2)
- Gas Exchange in PlantsDocument19 pagesGas Exchange in PlantsNaureen Khaliq100% (1)
- Ineffective Breathing PatternDocument8 pagesIneffective Breathing PatternJansen Arquilita Rivera100% (2)
- The Healing Power of HumorDocument3 pagesThe Healing Power of HumorJuan Daniel Yanqui GuerreroNo ratings yet
- 6th Espen SymposiumDocument4 pages6th Espen Symposiumyos_peace86No ratings yet
- Stop SmokingDocument16 pagesStop Smokingeduardo virgilioNo ratings yet
- Embriologija CvjetnicaDocument526 pagesEmbriologija CvjetnicaelviraNo ratings yet
- EmotionsDocument58 pagesEmotionsthivyaashini SellaNo ratings yet
- Chapter 1 - The Nervous SystemDocument8 pagesChapter 1 - The Nervous SystemRadha RamineniNo ratings yet
- 003 Pathology MCQ ACEM Primary CardiovascularDocument5 pages003 Pathology MCQ ACEM Primary Cardiovascularbmhsh100% (2)
- Hematologic Reference Ranges A PDFDocument3 pagesHematologic Reference Ranges A PDFmalaimaxNo ratings yet
- Trigeminal NeuralgiaDocument22 pagesTrigeminal NeuralgiaamandarestykbNo ratings yet
- CH 9 Emotions NCERT PDFDocument19 pagesCH 9 Emotions NCERT PDFrerereNo ratings yet
- Educ 106 Module 8Document3 pagesEduc 106 Module 8Jona Charmele DegilloNo ratings yet
- Test Bank For Laboratory Manual For Seeleys Anatomy Physiology 11th Edition Eric Wise 3 DownloadDocument69 pagesTest Bank For Laboratory Manual For Seeleys Anatomy Physiology 11th Edition Eric Wise 3 Downloadcaseyyoungtoekwmcfdi100% (30)
- Overview Female Reproductive AnatomyDocument45 pagesOverview Female Reproductive AnatomyAbebe TilahunNo ratings yet
- PteridophytesDocument61 pagesPteridophytestapas kunduNo ratings yet
- Flow Sheet TemplateDocument4 pagesFlow Sheet TemplateIulia Tania AndronacheNo ratings yet
- Risk FactorsDocument174 pagesRisk FactorsdevikaNo ratings yet
- Class-10 Revision Test - NutritionDocument4 pagesClass-10 Revision Test - NutritionVarshini PeraNo ratings yet
- Semen Analysis (Seminal Cytology, Sperm CountDocument30 pagesSemen Analysis (Seminal Cytology, Sperm Countabdurae100% (1)
- Approach To HeadacheDocument49 pagesApproach To Headachegea pandhita sNo ratings yet
- 2013 h2 BiologyDocument1,838 pages2013 h2 BiologyJustt Mee100% (1)
- From Wikipedia, The Free Encyclopedia: Ornamental Bulbous Plant Bulb (Disambiguation)Document4 pagesFrom Wikipedia, The Free Encyclopedia: Ornamental Bulbous Plant Bulb (Disambiguation)Alexandra Maria NeaguNo ratings yet