Professional Documents
Culture Documents
GI Sim
GI Sim
Uploaded by
Iyath Saeed0 ratings0% found this document useful (0 votes)
8 views5 pagesPyloric stenosis is a narrowing of the pylorus that is not present at birth but develops in infants. It causes non-bilious projectile vomiting after feeding that worsens over time and starts around 3 weeks of age. Diagnosis involves palpating an olive-shaped mass above the umbilicus that is firmer after vomiting. Treatment is pyloromyotomy surgery to cut the pyloric muscle.
Original Description:
Original Title
GI sim
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentPyloric stenosis is a narrowing of the pylorus that is not present at birth but develops in infants. It causes non-bilious projectile vomiting after feeding that worsens over time and starts around 3 weeks of age. Diagnosis involves palpating an olive-shaped mass above the umbilicus that is firmer after vomiting. Treatment is pyloromyotomy surgery to cut the pyloric muscle.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
0 ratings0% found this document useful (0 votes)
8 views5 pagesGI Sim
GI Sim
Uploaded by
Iyath SaeedPyloric stenosis is a narrowing of the pylorus that is not present at birth but develops in infants. It causes non-bilious projectile vomiting after feeding that worsens over time and starts around 3 weeks of age. Diagnosis involves palpating an olive-shaped mass above the umbilicus that is firmer after vomiting. Treatment is pyloromyotomy surgery to cut the pyloric muscle.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
You are on page 1of 5
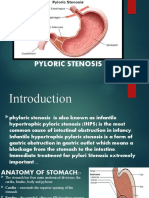
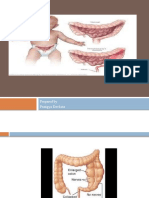
Pyloric Stenosis
Not present at birth.
Associated with eosinophilic gastroenteritis, Apert syndrome, Zellweger
syndrome, trisomy 18, Smith-Lemli-Opitz syndrome, Cornelia de Lange
syndrome.
Use of erythromycin with higher risk if given within first 2 weeks of life.
Female infants of mothers treated with macrolide antibiotics during pregnancy
and breastfeeding.
Abnormal muscle innervation, elevated serum levels of prostaglandins, infant
hypergastrinemia.
Symptoms
o Non-bilious vomiting – initial symptom.
Progressive, occurring immediately after feeding.
Emesis might follow each feeding or intermittent.
Usually stars after 3 weeks of age. (1 week – 5 months).
o Hyperbilirubinemia – unconjugated more than conjugated.
Diagnosis
o Palpating the pyloric mass.
Mass is firm, movable, about 2 cm in length, olive shaped, hard,
best palpated from left side and located above and right of
umbilicus in mid epigastrium beneath liver’s edge.
Best palpated after vomiting.
o Presence of gastric peristaltic wave after eating.
o Ultrasound – confirms.
DDX
o Gastroesophageal reflux with or without hiatal hernia. Differentiated by
radiology.
o Adrenal insufficiency from adrenogenital syndrome. Rule out: absence of
metabolic acidosis and elevated serum potassium and urinary sodium.
o Inborn errors of metabolism – includes emesis with alkalosis or acidosis
and lethargy, coma, seizures.
o Vomiting + diarrhea = gastroenteritis but some may have in pyloric
stenosis.
Treatment
o Preoperative:
Correcting fluid, acid-base, electrolyte losses.
Correction of alkalosis to prevent postoperative apnea associated
with anesthesia. Most infants need 24 hours.
o Surgery: pyloromyotomy
Ramstedt procedure done through short transverse skin incision.
Underlying pyloric mass cut and incision closed.
o Postoperative:
Vomiting – half the infants.
Initiate feeding within 12-24 hrs after surgery.
Maintenance feeding 36-48 hours after.
Atropine IV 0.01 mg/kg 6x/day 5 min before feeding.
o Monitor HR by ECG.
Oral feeding started at 10 mL formula 6x/day.
Gradual increase until patient can tolerate 150 mL/kg/day
unless vomiting occurs more than twice a day.
Once patient can eat 150 mL/kg/day without vomiting, give
atropine 0.02 mg/kg orally 6x/day before feeding.
Persistent vomiting = incomplete pyloromyotomy, gastritis,
gastroesophageal reflux disease, some other obstruction.
Do endoscopic balloon dilation for incomplete
pyloromyotomy.
o Conservative management with nasoduodenal feedings who are not
good for surgery.
o Oral and intravenous atropine sulfate (pyloric muscle relaxant).
Pyloric Atresia
Symptoms
o Nonbilious vomiting
o Feeding difficulties
o Abdominal distension during first day of life.
o Gastric aspirate at birth is large (> 20 mL) – remove to prevent aspiration.
o Rupture of stomach may occur as early as first 12 hours of life.
Polyhydramnios + low birth weight.
Diagnosis
o Finding of large, dilated stomach on abdominal plain radiograph or in utero
ultrasonography.
o UGI contrast
Avoid aspiration
o Older children (endoscopy)
Treatment
o All gastric outlet obstruction in neonates start with correction of
dehydration and hypochloremic alkalosis.
o Persistent vomiting relieved with nasogastric decompression.
o Surgical or endoscopic repair only when patient stable.
Intestinal atresia, stenosis, malrotation
Obstruction may be partial or complete and simple or strangulating.
Intrinsic causes
o Inherent abnormalities of intestinal innervation
o Mucus production
o Tubular anatomy (most common and manifest as obliteration or narrowing
of intestinal lumen)
Extrinsic
o Compression of bowel by vessels, organs, cysts
o Abnormalities in intestinal rotation during fetal development.
Symptoms
o Bowel distension – accumulation of food, gas, intestinal secretions
proximal to point of obstruction.
o Absorption of intestinal decreased, secretion of fluid and electrolytes
increased – hypokalemia
o Less blood flow – lack of mucosal integrity – bacterial proliferation
(coliforms, anaerobes). Bacteria can travel – endotoxemia, bacteremia,
sepsis.
o High intestine obstruction:
Large volume, frequent, bilious emesis with little/no abdominal
distension.
Intermittent pain relieved by vomiting.
o Distal bowel small obstruction
Moderate or marked abdominal distension with emesis that is
progressively feculent.
o Both have obstipation.
Diagnosis
o History, PE, radiology.
o Polyhydramnios – high intestinal obstruction.
o Radiology – contrast studies or CT because neonate colonic haustra not
fully developed.
Treatment
o Initial for children and infants – fluid resuscitation and stabilization.
o Nasogastric decompression – for pain and vomiting.
o Broad spectrum antibiotics for ill looking neonates
o No improvement in 12-24 hours, operation.
Duodenal obstruction
Symptoms
You might also like
- Fundamentals of Nursing Outline Chapter 46 Potter and PerryDocument6 pagesFundamentals of Nursing Outline Chapter 46 Potter and PerryAidenhunter05100% (6)
- Hayssen Training ElectricalDocument17 pagesHayssen Training ElectricalRoberto SanchezNo ratings yet
- Esophageal Stricture and ObstructionDocument11 pagesEsophageal Stricture and ObstructionBibi Renu100% (6)
- Intestine ObstructionDocument37 pagesIntestine ObstructionGoesti YudistiraNo ratings yet
- August 14 - Sequencig Using Signal WordsDocument3 pagesAugust 14 - Sequencig Using Signal Wordsshe88% (8)
- Congenital Anomalies of GiDocument94 pagesCongenital Anomalies of GiPadmaNo ratings yet
- Vomiting in ChildrenDocument44 pagesVomiting in ChildrenAstri Faluna SheylavontiaNo ratings yet
- Week 8 Pedia Pediatric GI DisturbancesDocument110 pagesWeek 8 Pedia Pediatric GI DisturbancesJaja ManezNo ratings yet
- Pyloric Stenosis Case StudyDocument37 pagesPyloric Stenosis Case StudyFaith Torralba100% (3)
- Nursing MGT of PT With Lower Git DisordersDocument65 pagesNursing MGT of PT With Lower Git DisordersCarlos LorenzoNo ratings yet
- Congenital Development Disorder of Esophagus, Stomach, Duodenum, Abdomen Wall, Anus and RectumDocument56 pagesCongenital Development Disorder of Esophagus, Stomach, Duodenum, Abdomen Wall, Anus and RectumSarah Nabella PutriNo ratings yet
- Nursing Care of The Child With A Gastrointestinal DisordersDocument46 pagesNursing Care of The Child With A Gastrointestinal Disorderstalaekrema01No ratings yet
- Obstruksi IntestinalDocument37 pagesObstruksi IntestinalkrisandiNo ratings yet
- Omphalocelevsgastroschisis 160810122732Document23 pagesOmphalocelevsgastroschisis 160810122732LNICCOLAIO100% (1)
- 1 NCM+116n+Lecture+Care+of+the+Clients+with+Problems+GI+Function+and+NutritionDocument6 pages1 NCM+116n+Lecture+Care+of+the+Clients+with+Problems+GI+Function+and+NutritionKylle AlimosaNo ratings yet
- Intestinal Obstruction in Paediatrics - James GathogoDocument21 pagesIntestinal Obstruction in Paediatrics - James GathogoMalueth Angui100% (1)
- Gastro NephroDocument93 pagesGastro Nephrohasanatiya41No ratings yet
- Common Laboratory ProceduresDocument4 pagesCommon Laboratory ProceduresrahafNo ratings yet
- Open Cholecystectomy: By: Santoyo, Sarah Jane R. BSN 3-B Group 6-Operating RoomDocument6 pagesOpen Cholecystectomy: By: Santoyo, Sarah Jane R. BSN 3-B Group 6-Operating RoomJullie Anne SantoyoNo ratings yet
- Case Presentation About Calculous CholecyctitisDocument23 pagesCase Presentation About Calculous CholecyctitiskarenNo ratings yet
- Digestive DiseasesDocument10 pagesDigestive Diseaseskate_5182178No ratings yet
- Pedia Surg Module, Grp11&2Document91 pagesPedia Surg Module, Grp11&2Jelyn ManipisNo ratings yet
- Pyloric StenosisDocument47 pagesPyloric StenosisgeethsreesatNo ratings yet
- Paediatric Surgery 2Document38 pagesPaediatric Surgery 2عمار عارفNo ratings yet
- Hirsch SprungDocument4 pagesHirsch SprungRy AnneNo ratings yet
- 5 Review Gi DigestiveDocument97 pages5 Review Gi DigestiveSaif AlzateemhNo ratings yet
- Gi NclexDocument14 pagesGi NclexYoke W Khoo100% (3)
- Pyloric StenosisDocument18 pagesPyloric StenosisAnkita Samanta0% (1)
- Small Bowel: Alaa MaaliDocument78 pagesSmall Bowel: Alaa MaaliHalima AssiNo ratings yet
- Hirsch SprungDocument3 pagesHirsch SprungBheru LalNo ratings yet
- Gastro - NelsonDocument14 pagesGastro - NelsonGemma OrquioNo ratings yet
- Alteration in MetabolismDocument26 pagesAlteration in MetabolismAileen MonaresNo ratings yet
- CH 38 - Bowel EliminationDocument10 pagesCH 38 - Bowel EliminationJose GonzalezNo ratings yet
- Gastrointestinal Tract: Monometric StudiesDocument9 pagesGastrointestinal Tract: Monometric StudiesJosh LimNo ratings yet
- PBL No Bowel Output in NeonatesDocument24 pagesPBL No Bowel Output in NeonatesOTOH RAYA OMARNo ratings yet
- Hirschsprung'S Disease OR Congenital Aganglionic MegacolonDocument59 pagesHirschsprung'S Disease OR Congenital Aganglionic MegacolonHarshika KDGNo ratings yet
- Emergencies in GITDocument7 pagesEmergencies in GITsssajiNo ratings yet
- SG3 Paediatric Surgical EmergenciesDocument69 pagesSG3 Paediatric Surgical EmergenciesDiyana ZatyNo ratings yet
- Hypertrophic Pyloric StenosisDocument17 pagesHypertrophic Pyloric StenosisMohammed Fareed100% (1)
- 0327 Congenital Anomalies Rutter Congenital Anomalies Tracheoesophageal Fistula and Esophageal AtresiaDocument6 pages0327 Congenital Anomalies Rutter Congenital Anomalies Tracheoesophageal Fistula and Esophageal AtresiaYvonne ChuehNo ratings yet
- Intussuseption and Hirschprung's DiseaseDocument5 pagesIntussuseption and Hirschprung's DiseaseAris Magallanes100% (2)
- Nursing Care of The Child With Gastrointestinal DisordersDocument50 pagesNursing Care of The Child With Gastrointestinal Disordersمهند الرحيليNo ratings yet
- Diverticular Disease and Intestinal ObstructionDocument31 pagesDiverticular Disease and Intestinal ObstructionPauLa Cheneree Peña ÜNo ratings yet
- Paralytic IleusDocument2 pagesParalytic Ileusrjalavazo100% (2)
- Alterations in Nutrition and GastrointestinalDocument7 pagesAlterations in Nutrition and GastrointestinalChriszanie CruzNo ratings yet
- Hirschprung DiseaseDocument61 pagesHirschprung DiseaseAdditi Satyal100% (1)
- VomitingDocument4 pagesVomitingMax BrownNo ratings yet
- In Partial Fulfillment For The Requirements in R.L.E: Submitted By: Elaine Blanche R. GonzalezDocument6 pagesIn Partial Fulfillment For The Requirements in R.L.E: Submitted By: Elaine Blanche R. GonzalezBlanche GonzalezNo ratings yet
- G.I Disorders Part 2Document53 pagesG.I Disorders Part 2شبلي غرايبهNo ratings yet
- Chapter 28 Child With A Gastrointestinal ConditionDocument85 pagesChapter 28 Child With A Gastrointestinal Conditionsey_scottNo ratings yet
- Hypertrophic Pyloric StenosisDocument23 pagesHypertrophic Pyloric StenosisRahel Imelda PanggabeanNo ratings yet
- Neonatal Intestinal ObstructionDocument25 pagesNeonatal Intestinal ObstructionnlwhtdcsnvuvbkxmtpNo ratings yet
- Medical Surgical Nursing Module 1 Lesson 1 Upper Gastrointestinal DisordersDocument34 pagesMedical Surgical Nursing Module 1 Lesson 1 Upper Gastrointestinal DisordersRomelyn Ordillas100% (2)
- ND RDDocument22 pagesND RDKatie Marie Wilson100% (1)
- Intestinal Obstruction 2Document46 pagesIntestinal Obstruction 2Lawrence WanderiNo ratings yet
- KONSTIPASI (Medscape) : The Paris Consensus On Childhood Constipation Terminology (PACCT) Defines Constipation AsDocument5 pagesKONSTIPASI (Medscape) : The Paris Consensus On Childhood Constipation Terminology (PACCT) Defines Constipation AsGilang Nesta PersempreNo ratings yet
- Disorders of The ColonDocument47 pagesDisorders of The ColonGieve BlasurcaNo ratings yet
- Hirschprung's DiseaseDocument26 pagesHirschprung's DiseaseAbdur RaqibNo ratings yet
- Gi SMB - Clin MedDocument5 pagesGi SMB - Clin MedSohil PatelNo ratings yet
- Pyloric StenosisDocument3 pagesPyloric Stenosismagisasamundo100% (1)
- Visayas Community Medical Center Department of Surgery: Curan, Jan Kleen Ediza, Janseen Tortugo, Andrea MarieDocument43 pagesVisayas Community Medical Center Department of Surgery: Curan, Jan Kleen Ediza, Janseen Tortugo, Andrea MarieJanseen EdizaNo ratings yet
- Dysphagia, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandDysphagia, A Simple Guide To The Condition, Treatment And Related ConditionsRating: 5 out of 5 stars5/5 (1)
- The Sabbath As FreedomDocument14 pagesThe Sabbath As Freedomapi-232715913No ratings yet
- 50 Programing QuotesDocument3 pages50 Programing QuotesFreddy MoncadaNo ratings yet
- Challenges of Copyright in A Digital Age by Wandi KawecheDocument5 pagesChallenges of Copyright in A Digital Age by Wandi Kawechepoppy peterNo ratings yet
- Soal BAHASA INGGRIS XIIDocument5 pagesSoal BAHASA INGGRIS XIIZiyad Frnandaa SyamsNo ratings yet
- Final Project On Employee EngagementDocument97 pagesFinal Project On Employee EngagementSanju DurgapalNo ratings yet
- Shotgun StatisticsDocument1 pageShotgun Statistics-No ratings yet
- POTTER ROEMER® 2500 Series 1 '' HOSE RACK ASSEMBLIESDocument1 pagePOTTER ROEMER® 2500 Series 1 '' HOSE RACK ASSEMBLIESrvalentino2012No ratings yet
- Brachy Quality GuideDocument270 pagesBrachy Quality GuideTejinder SinghNo ratings yet
- CH 12Document31 pagesCH 12asin12336No ratings yet
- The EI SLP Therapy BundleDocument14 pagesThe EI SLP Therapy BundlelevyNo ratings yet
- Evaluation of Trajectory Model For Differential Steering Using Numerical MethodDocument6 pagesEvaluation of Trajectory Model For Differential Steering Using Numerical MethodNaufal RachmatullahNo ratings yet
- 5db83ef1f71e482 PDFDocument192 pages5db83ef1f71e482 PDFRajesh RoyNo ratings yet
- Fragment D Une Statue D Osiris ConsacreDocument11 pagesFragment D Une Statue D Osiris ConsacrePedro Hernández PostelNo ratings yet
- Brazil Is Samba: Rhythm, Percussion, and Samba in The Formation of Brazilian National Identity (1902-1958)Document135 pagesBrazil Is Samba: Rhythm, Percussion, and Samba in The Formation of Brazilian National Identity (1902-1958)Carlos Barrientos100% (1)
- Adverb Worksheet For Class 4 With AnswersDocument10 pagesAdverb Worksheet For Class 4 With Answersrodolfo penaredondoNo ratings yet
- EXEMPLAR - 1006HSV - Assessment 1a - Critical Analysis Reflective Essay - Draft Template - T323Document5 pagesEXEMPLAR - 1006HSV - Assessment 1a - Critical Analysis Reflective Essay - Draft Template - T323aryanrana20942No ratings yet
- How To Extend A BrandDocument7 pagesHow To Extend A BrandDhruv AggarwalNo ratings yet
- Glory To God Light From Light With LyricsDocument13 pagesGlory To God Light From Light With LyricsRodolfo DeriquitoNo ratings yet
- Fizika RadiologijaDocument9 pagesFizika RadiologijaBorislav TapavičkiNo ratings yet
- The Duality of Human Nature in Oscar Wilde's The Importance of Being EarnestDocument28 pagesThe Duality of Human Nature in Oscar Wilde's The Importance of Being EarnestSowmya ShreeNo ratings yet
- Versatile, Efficient and Easy-To-Use Visual Imu-Rtk: Surveying & EngineeringDocument4 pagesVersatile, Efficient and Easy-To-Use Visual Imu-Rtk: Surveying & EngineeringMohanad MHPSNo ratings yet
- (First Mas) (Call Center) LP/PP: Panel Load ScheduleDocument1 page(First Mas) (Call Center) LP/PP: Panel Load ScheduleyasserNo ratings yet
- System Development Invoice - Audit ToolDocument2 pagesSystem Development Invoice - Audit ToolVictorNo ratings yet
- Interest InventoriesDocument7 pagesInterest Inventoriesandrewwilliampalileo@yahoocomNo ratings yet
- JAMA 1990 Meshberger 1837 41 PDFDocument5 pagesJAMA 1990 Meshberger 1837 41 PDFNicholas TorreyNo ratings yet
- 1884 Journey From Heraut To Khiva Moscow and ST Petersburgh Vol 2 by Abbott S PDFDocument342 pages1884 Journey From Heraut To Khiva Moscow and ST Petersburgh Vol 2 by Abbott S PDFBilal AfridiNo ratings yet
- Ave Maria CollegeDocument6 pagesAve Maria CollegeMylene EsicNo ratings yet
- Economists' Corner: Weighing The Procompetitive and Anticompetitive Effects of RPM Under The Rule of ReasonDocument3 pagesEconomists' Corner: Weighing The Procompetitive and Anticompetitive Effects of RPM Under The Rule of ReasonHarsh GandhiNo ratings yet