Professional Documents
Culture Documents
Ipm 2-1
Ipm 2-1
Uploaded by
rochmandrg dokter gigiCopyright:
Available Formats
You might also like
- Pulmonary Pathology of Early-Phase 2019 Novel Coronavirus (COVID-19) Pneumonia in Two Patients With Lung CancerDocument5 pagesPulmonary Pathology of Early-Phase 2019 Novel Coronavirus (COVID-19) Pneumonia in Two Patients With Lung Cancermuhammad RidoNo ratings yet
- PIIS1201971220301016Document6 pagesPIIS1201971220301016Gordana PuzovicNo ratings yet
- Complicated Sinusitis With Sphenopalatine Artery Thrombosis in A COVID-19 Patient, A Case ReportDocument3 pagesComplicated Sinusitis With Sphenopalatine Artery Thrombosis in A COVID-19 Patient, A Case ReportNurul Aisyah PaldarNo ratings yet
- Tian Early PhaseDocument12 pagesTian Early PhaseAurelian CârsteaNo ratings yet
- Rli 55 257Document5 pagesRli 55 257WilsonR.CorzoNiñoNo ratings yet
- Unusual Presentation of Covid-19 in Patient With Acute AbdomenDocument4 pagesUnusual Presentation of Covid-19 in Patient With Acute AbdomenCirugía General HGRNo ratings yet
- Episcleritis As An Ocular Manifestation in A Patient With COVID 19Document3 pagesEpiscleritis As An Ocular Manifestation in A Patient With COVID 19Hocie Trinanda SardiNo ratings yet
- MainDocument8 pagesMainWilsonR.CorzoNiñoNo ratings yet
- Articulo Cientifico Derrame Pleural en Covid 19Document10 pagesArticulo Cientifico Derrame Pleural en Covid 19Leyla Barnard LagunaNo ratings yet
- 1 s2.0 S1930043320306208 MainDocument3 pages1 s2.0 S1930043320306208 MainRivaldy BobihuNo ratings yet
- 2019 Novel Coronavirus Disease (COVID-19) in Taiwan: Reports of Two Cases From Wuhan, ChinaDocument4 pages2019 Novel Coronavirus Disease (COVID-19) in Taiwan: Reports of Two Cases From Wuhan, ChinaClaav HugNo ratings yet
- Paper 1Document6 pagesPaper 1ivan.montenegroNo ratings yet
- Coronavirus (COVID-19) OutbreakDocument5 pagesCoronavirus (COVID-19) OutbreakPrima Sarana MedikaNo ratings yet
- International Journal of Infectious DiseasesDocument7 pagesInternational Journal of Infectious Diseaseshardilas kaur behalNo ratings yet
- Emp2 12098Document4 pagesEmp2 12098Miva MaviniNo ratings yet
- REPORTE CASO TBC y COVID 19Document6 pagesREPORTE CASO TBC y COVID 19Farmaco VigilanciaNo ratings yet
- Research Letters: Co-Infection With Sars-Cov-2 and Influenza A Virus in Patient With Pneumonia, ChinaDocument3 pagesResearch Letters: Co-Infection With Sars-Cov-2 and Influenza A Virus in Patient With Pneumonia, Chinajitesh141No ratings yet
- Case Report Scopus CandraDocument6 pagesCase Report Scopus CandraDr.gendjutNo ratings yet
- Perfusie Afwijkingen in Covid 19 Patienten 1603707976Document10 pagesPerfusie Afwijkingen in Covid 19 Patienten 1603707976Muhammad Al-DulaimyNo ratings yet
- Neumonia Intersti CovidDocument11 pagesNeumonia Intersti CovidsantospardogomezNo ratings yet
- Coronavirus (COVID-19) Outbreak: What The Department of Radiology Should KnowDocument5 pagesCoronavirus (COVID-19) Outbreak: What The Department of Radiology Should KnowrezaNo ratings yet
- 10 1513@annalsats 202004-324ocDocument36 pages10 1513@annalsats 202004-324ocDany Daniel Rafael HuamanNo ratings yet
- Functional and Radiological Improvement in A COVID-19 Pneumonia Patient Treated With SteroidsDocument5 pagesFunctional and Radiological Improvement in A COVID-19 Pneumonia Patient Treated With Steroidsmostafa aliNo ratings yet
- Research JournalDocument7 pagesResearch JournalHyacinth A RotaNo ratings yet
- Ibi JurnalDocument9 pagesIbi JurnalRiski Pradika 2017No ratings yet
- JMV 25815Document2 pagesJMV 25815fadil ahmadiNo ratings yet
- The Clinical and Chest CT Features Associated With Severe and Critical COVID-19 PneumoniaDocument5 pagesThe Clinical and Chest CT Features Associated With Severe and Critical COVID-19 PneumoniaNadanNadhifahNo ratings yet
- Conjunctivitis in COVID-19 Patients: Frequency and Clinical PresentationDocument7 pagesConjunctivitis in COVID-19 Patients: Frequency and Clinical PresentationStephanie AureliaNo ratings yet
- Wa0015.4Document7 pagesWa0015.4jeyiy92174No ratings yet
- Clinical Characteristics of COVID-19 Complicated With Pleural EffusionDocument10 pagesClinical Characteristics of COVID-19 Complicated With Pleural EffusionInternal MedicineNo ratings yet
- Cerebrovascular Disease in COVID-19: Adult BrainDocument3 pagesCerebrovascular Disease in COVID-19: Adult BrainUsman Agus PrasetyoNo ratings yet
- COVID-19 Autopsies - Aqaa062Document9 pagesCOVID-19 Autopsies - Aqaa062Pramod BiradarNo ratings yet
- Medical Mycology Case ReportsDocument5 pagesMedical Mycology Case ReportsGUSTI AYU PUTU KRISNA DEWINo ratings yet
- Hemorhagic PRESDocument4 pagesHemorhagic PRESAbdul AzeezNo ratings yet
- USS 2020-I. - Autop - COVID19Document9 pagesUSS 2020-I. - Autop - COVID19Jerry Carhuatanta SaavedraNo ratings yet
- COVID-19 Autopsies, Oklahoma, USADocument9 pagesCOVID-19 Autopsies, Oklahoma, USARhagaraRhaNo ratings yet
- Clinical and Imaging Features of COVID19Document8 pagesClinical and Imaging Features of COVID19ClaudiaNo ratings yet
- Proning in Non-Intubated (PINI) in Times of COVID-19: Case Series and A ReviewDocument7 pagesProning in Non-Intubated (PINI) in Times of COVID-19: Case Series and A ReviewCarlos ZepedaNo ratings yet
- JR COvid-19 Dan Anosmia Dr. SukriDocument25 pagesJR COvid-19 Dan Anosmia Dr. SukriAlmiraNo ratings yet
- Geriatric Patient With Osteoarthritis and Obesity Survived From Critically Ill of COVID-19: A Case ReportDocument5 pagesGeriatric Patient With Osteoarthritis and Obesity Survived From Critically Ill of COVID-19: A Case Reportnadila raudhani pNo ratings yet
- Piis014067362030920x PDFDocument4 pagesPiis014067362030920x PDFgonzaloNo ratings yet
- Piis014067362030920x PDFDocument4 pagesPiis014067362030920x PDFgonzaloNo ratings yet
- Hypothesis: Hui Li, Liang Liu, Dingyu Zhang, Jiuyang Xu, Huaping Dai, Nan Tang, Xiao Su, Bin CaoDocument4 pagesHypothesis: Hui Li, Liang Liu, Dingyu Zhang, Jiuyang Xu, Huaping Dai, Nan Tang, Xiao Su, Bin CaogonzaloNo ratings yet
- Journal of Clinical and Translational Endocrinology: Case ReportsDocument5 pagesJournal of Clinical and Translational Endocrinology: Case ReportsKartikaa YantiiNo ratings yet
- Essentials For Radiologists OnDocument2 pagesEssentials For Radiologists Onzahra ebrahimiNo ratings yet
- Idcases: Sergio Zaccaria Scalinci, Edoardo Trovato BattagliolaDocument3 pagesIdcases: Sergio Zaccaria Scalinci, Edoardo Trovato BattagliolaMuhamad ZenNo ratings yet
- Estudo DiabetesDocument9 pagesEstudo DiabetesFulano de TalNo ratings yet
- 1 s2.0 S1015958423006000 MainDocument2 pages1 s2.0 S1015958423006000 Mainmodacasper056No ratings yet
- Genomewide Association Study of SevereDocument13 pagesGenomewide Association Study of SevereANANo ratings yet
- EnovaraDocument4 pagesEnovaraenilNo ratings yet
- 2020-Autopsias COVID 4Document6 pages2020-Autopsias COVID 4Mario Martínez TorijaNo ratings yet
- LeukoeritroblastikDocument2 pagesLeukoeritroblastiknadaNo ratings yet
- Misdiagnosis in Covid19 Era JACC PDFDocument6 pagesMisdiagnosis in Covid19 Era JACC PDFRirin Efsa JutiaNo ratings yet
- Correlation Between Ground-Glass Opacity On Pulmonary CT and The Levels of Inflammatory CytokinesDocument7 pagesCorrelation Between Ground-Glass Opacity On Pulmonary CT and The Levels of Inflammatory CytokinesEarlya RifaniNo ratings yet
- Pi Is 0749070421000439Document21 pagesPi Is 0749070421000439Vlady78No ratings yet
- An Adolescent With A Retropharyngeal Swelling ToDocument4 pagesAn Adolescent With A Retropharyngeal Swelling Tolincolnbasilio1No ratings yet
- 1 s2.0 S0924857920301059 MainDocument13 pages1 s2.0 S0924857920301059 MainNini RinNo ratings yet
- Foldes, D., Et Al. (2020) - Plasmacytoid Lymphocytes in SARS CoV 2 Infection (Covid 19) - American Journal of Hematology PDFDocument2 pagesFoldes, D., Et Al. (2020) - Plasmacytoid Lymphocytes in SARS CoV 2 Infection (Covid 19) - American Journal of Hematology PDFRalt MedNo ratings yet
- Letter TO THE Editor: Secondary Organizing Pneumonia After Varicella-Zoster Virus Infection: A Rare AssociationDocument3 pagesLetter TO THE Editor: Secondary Organizing Pneumonia After Varicella-Zoster Virus Infection: A Rare AssociationfatimiahmastaNo ratings yet
- Brit J Clinical Pharma - 2011 - Ardern Jones - Skin Manifestations of Drug AllergyDocument12 pagesBrit J Clinical Pharma - 2011 - Ardern Jones - Skin Manifestations of Drug Allergyrochmandrg dokter gigiNo ratings yet
- Clinical Manifestation of Oral Tuberculosis in Hiv Patient A Review Article 1Document4 pagesClinical Manifestation of Oral Tuberculosis in Hiv Patient A Review Article 1rochmandrg dokter gigiNo ratings yet
- Insights Into Hypersensitivity Reactions In.6Document10 pagesInsights Into Hypersensitivity Reactions In.6rochmandrg dokter gigiNo ratings yet
- A Brief Review of The Mechanisms of Drug HypersensitivityDocument6 pagesA Brief Review of The Mechanisms of Drug Hypersensitivityrochmandrg dokter gigiNo ratings yet
- Aop 157Document4 pagesAop 157rochmandrg dokter gigiNo ratings yet
- Ipm 3Document4 pagesIpm 3rochmandrg dokter gigiNo ratings yet
- Antibiotic Hypersensitivity MechanismsDocument14 pagesAntibiotic Hypersensitivity Mechanismsrochmandrg dokter gigiNo ratings yet
- KARIXA Dentolaser KA 45-01 DLDocument1 pageKARIXA Dentolaser KA 45-01 DLrochmandrg dokter gigiNo ratings yet
- Immunopathogenesis of Delayed-Type HypersensitivityDocument5 pagesImmunopathogenesis of Delayed-Type Hypersensitivityrochmandrg dokter gigiNo ratings yet
- Depression and HIV Disease Progression A Mini-ReviewDocument7 pagesDepression and HIV Disease Progression A Mini-Reviewrochmandrg dokter gigiNo ratings yet
- JAIP Portnoy Et Al PDFDocument3 pagesJAIP Portnoy Et Al PDFrochmandrg dokter gigiNo ratings yet
- Dehydration Pathway 2016Document3 pagesDehydration Pathway 2016rochmandrg dokter gigiNo ratings yet
- Patch Test ROAT PDFDocument9 pagesPatch Test ROAT PDFrochmandrg dokter gigiNo ratings yet
- I Nyoman Wande, Muhamad Robi'ul Fuadi, Solichul Hadi: Background: ResultsDocument5 pagesI Nyoman Wande, Muhamad Robi'ul Fuadi, Solichul Hadi: Background: Resultsrochmandrg dokter gigiNo ratings yet
- тезисыDocument1 pageтезисыrochmandrg dokter gigiNo ratings yet
- Iufd Lesson PlanDocument21 pagesIufd Lesson PlanBupe LwitaNo ratings yet
- Etool Administration of IV MedicationDocument4 pagesEtool Administration of IV MedicationReeham UsmanNo ratings yet
- Dr. Kiki - Pengantar Trauma UpdateDocument20 pagesDr. Kiki - Pengantar Trauma UpdateRsud Malinau Ppk Blud100% (1)
- (En) 2024 BIOOD Biophilia Tracker X4 MAX FeaturesDocument16 pages(En) 2024 BIOOD Biophilia Tracker X4 MAX FeaturesjsemsamsebouNo ratings yet
- 05 Allama Rozan Firdaus Hortatory Text TaskDocument2 pages05 Allama Rozan Firdaus Hortatory Text TaskAllama Rozan FirdausNo ratings yet
- Optical Coherence Tomography (OCT) in Neurologic DiseasesDocument232 pagesOptical Coherence Tomography (OCT) in Neurologic DiseasesirodalexandraNo ratings yet
- Abruptio Placenta Drug StudyDocument5 pagesAbruptio Placenta Drug StudyJayne Angelie A. NuevaespañaNo ratings yet
- TPN Origin and CalculationsDocument42 pagesTPN Origin and CalculationsmajdNo ratings yet
- TranscriptDocument4 pagesTranscriptGuru PrasadNo ratings yet
- Sepsis and Severe Pneumonia (2022)Document39 pagesSepsis and Severe Pneumonia (2022)rina delsNo ratings yet
- Adult CardDocument4 pagesAdult CardagelsantosNo ratings yet
- Intraoperative Complications: Mandibular Anterior: Intraosseous VesselsDocument2 pagesIntraoperative Complications: Mandibular Anterior: Intraosseous VesselsRoenteiqNo ratings yet
- Untitled DocumentDocument4 pagesUntitled Documentclockstudy5No ratings yet
- Nursing Exam CompreDocument9 pagesNursing Exam ComprerikidbNo ratings yet
- Surat Buat VisaDocument12 pagesSurat Buat VisaNurul FitrianaNo ratings yet
- Drug Administration Route Needle Size EtcDocument1 pageDrug Administration Route Needle Size EtcRon AbuNo ratings yet
- Senarai Nama Anggota Unit Rawatan Rapi, Hospital Queen Elizabeth Ii 2014Document8 pagesSenarai Nama Anggota Unit Rawatan Rapi, Hospital Queen Elizabeth Ii 2014Rosyta DawatNo ratings yet
- Cardiac BiomarkersDocument32 pagesCardiac BiomarkersMaham RehmanNo ratings yet
- Principles For Aseptic Technique - Information For Healthcare Workers - December 2021Document5 pagesPrinciples For Aseptic Technique - Information For Healthcare Workers - December 2021ebubechukwu echefuNo ratings yet
- CNS Stimulants 2023Document10 pagesCNS Stimulants 2023ManWol JangNo ratings yet
- Questions and Answer Group 3 "Glaucoma" Nama: Gustin Ibrahim Umamah Kelas: A S1 FARMASI 2017 NIM: 821417021Document13 pagesQuestions and Answer Group 3 "Glaucoma" Nama: Gustin Ibrahim Umamah Kelas: A S1 FARMASI 2017 NIM: 821417021Afni YunitaNo ratings yet
- High Power CommitteeDocument39 pagesHigh Power CommitteeJaya PrabhaNo ratings yet
- Psych ReportDocument80 pagesPsych ReportPaul Carlo GonzalesNo ratings yet
- Wound Bed Score and Its Correlation With Healing of Chronic WoundsDocument8 pagesWound Bed Score and Its Correlation With Healing of Chronic WoundsErick VásquezNo ratings yet
- Chapter 18 VaccinesDocument29 pagesChapter 18 Vaccineshusseinabdullahahmad99No ratings yet
- RATE LIST of Recognized Private Hospitals and Diagnostic Centres UnderDocument44 pagesRATE LIST of Recognized Private Hospitals and Diagnostic Centres UnderbharatwerulkarNo ratings yet
- Haemostasis and Thrombosis: An Overview: H. RascheDocument5 pagesHaemostasis and Thrombosis: An Overview: H. Rascheshinichi kudoNo ratings yet
- Can Mothers Breastfeed During The COVIDDocument4 pagesCan Mothers Breastfeed During The COVIDAnisa RamdhiniNo ratings yet
- TESDA COVID-19 Health Status Daily Monitoring TESDA COVID - 19 Health Status Daily MonitoringDocument1 pageTESDA COVID-19 Health Status Daily Monitoring TESDA COVID - 19 Health Status Daily MonitoringMICS TVNo ratings yet
- Infectious Diseases II PDFDocument62 pagesInfectious Diseases II PDFhuong LNo ratings yet
Ipm 2-1
Ipm 2-1
Uploaded by
rochmandrg dokter gigiCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Ipm 2-1
Ipm 2-1
Uploaded by
rochmandrg dokter gigiCopyright:
Available Formats
See discussions, stats, and author profiles for this publication at: https://www.researchgate.
net/publication/343856614
Sialadenitis: A Possible Early Manifestation of COVID-19
Article in The Laryngoscope · August 2020
DOI: 10.1002/lary.29083
CITATIONS READS
22 707
4 authors, including:
Alexander Chern
New York Presbyterian Hospital (Columbia/Cornell)
47 PUBLICATIONS 337 CITATIONS
SEE PROFILE
All content following this page was uploaded by Alexander Chern on 28 October 2020.
The user has requested enhancement of the downloaded file.
The Laryngoscope
© 2020 American Laryngological,
Rhinological and Otological Society Inc,
"The Triological Society" and American
Laryngological Association (ALA)
Case Report
Sialadenitis: A Possible Early Manifestation of COVID-19
Alexander Chern, MD ; Akinrinola O. Famuyide, MD; Gul Moonis, MD; Anil K. Lalwani, MD
Acute sialadenitis may be caused by viruses, including coronaviruses. Although there are anecdotal reports of severe acute
respiratory syndrome coronavirus 2 (SARS-CoV-2) salivary gland infections, there have been no well-documented cases of
sialadenitis in patients with COVID-19 described in the literature. We report a case of parotitis and submandibular gland
sialadenitis, as well as an isolated case of parotitis, in two patients with concurrent SARS-CoV-2 infections. Computed tomogra-
phy imaging demonstrated parotid and submandibular gland enlargement with heterogenous enhancement and attenuation,
consistent with sialadenitis. Medical management was sufficient for successful resolution of the acute sialadenitis.
Key Words: COVID-19, severe acute respiratory syndrome coronavirus 2, sialadenitis, parotitis, submandibular gland,
parotid gland.
Laryngoscope, 130:2595–2597, 2020
INTRODUCTION patients with documented SARS-CoV-2 infections. Insti-
COVID-19 has rapidly spread worldwide since first tutional review board approval was granted for this
identified in December 2019 in Wuhan, China. Caused by study (AAAT0206: Neuroimaging Manifestations of
severe acute respiratory syndrome coronavirus 2 (SARS- COVID-19).
CoV-2), the disease has since been declared a pandemic.
COVID-19 often first presents with otolaryngological
symptoms, including cough, rhinorrhea, sore throat, dys- CASE REPORTS
pnea, anosmia, and dysgeusia.
High viral loads of SARS-CoV-2 have been consistently Case 1
found in saliva specimens of patients with COVID-19.1 An 88-year-old female was admitted for failure to
Animal studies have shown that SARS-CoV, the related thrive and poor oral intake since a recent family member
coronavirus that caused the early 2000s global SARS out- death. Physical examination demonstrated right pre-
break, can infect epithelial cells lining salivary gland ducts.2 auricular swelling and pain; no purulent drainage from
Although these results suggest the possibility of a SARS- Stensen’s duct could be expressed for cultures. Past medi-
CoV-2 salivary gland infection, there is a paucity of reports cal history included diabetes, hypertension, hypothyroid-
in the literature documenting this phenomenon.3,4 Herein, ism, pernicious anemia, autoimmune cirrhosis, and
we report a case of parotitis and submandibular gland diffuse large B cell lymphoma (treated with chemother-
sialadenitis, as well as an isolated case of parotitis, in two apy). Laboratory testing was notable for a positive
COVID-19 real-time polymerase chain reaction (RT-PCR)
test result (nasopharyngeal swab), mild leukocytosis with
From the Department of Otolaryngology–Head and Neck Surgery
(A.C., A.K.L.), New York–Presbyterian/Columbia University Irving Medical lymphopenia and neutrophilic predominance, and blood
Center and Columbia University Vagelos College of Physicians and cultures that grew Micrococcus luteus.
Surgeons, New York, New York, U.S.A.; Department of Otolaryngology–
Head and Neck Surgery (A.C.), New York–Presbyterian/Weill Cornell Computed tomography (CT) imaging of the neck
Medical Center, New York, New York, U.S.A.; Department of Radiology with intravenous (IV) contrast demonstrated an enlarged
(A.O.F., G.M.), Columbia University Irving Medical Center, New York,
New York, U.S.A.; and the Department of Mechanical Engineering (A.K.L.),
right parotid gland with heterogeneous enhancement and
The Fu Foundation School of Engineering and Applied Science, Columbia attenuation, as well as surrounding fat stranding and fas-
University, New York, New York, U.S.A. cial thickening consistent with overlying cellulitis and
Editor’s Note: This Manuscript was accepted for publication on
August 18, 2020.
fasciitis (Fig. 1). No fluid collection or obstructing sialolith
Anil K. Lalwani, MD, serves on the advisory board of Advanced was identified. Chest CT demonstrated peripheral
Bionics, MED EL, and Spiral Therapeutics.
The authors have no other funding, financial relationships, or con-
ground-glass opacities and interstitial thickening consis-
flicts of interest to disclose. tent with COVID-19 pneumonia.
Send correspondence to Anil K. Lalwani, MD, Department of The patient was treated with empiric intravenous
Otolaryngology–Head and Neck Surgery, Columbia University Vagelos
College of Physicians and Surgeons, NewYork–Presbyterian/Columbia antibiotics and supportive therapy. Over the next several
University Irving Medical Center, 180 Fort Washington Avenue, HP8, days, the patient demonstrated improvement in right-
New York, NY 10032. E-mail: akl2144@cumc.columbia.edu
sided facial swelling and pain, resolution of leukocytosis,
DOI: 10.1002/lary.29083 and was transitioned to oral antibiotics upon discharge.
Laryngoscope 130: November 2020 Chern et al.: Sialadenitis: Manifestation of COVID-19
2595
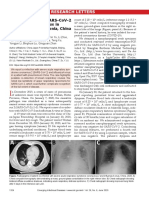
Fig. 1. Case 1. Contrast-enhanced computed tomography (CT) of the soft tissues of the neck. (A) Axial and (B) coronal images show enlarged
right parotid gland with heterogeneous enhancement and attenuation (thin dotted white arrows). There is surrounding fat stranding and fascial
thickening consistent with adjacent cellulitis (curved yellow arrow). There is no sialolith or fluid collection to suggest abscess. (C) Axial CT
image of the chest from the same study demonstrate bilateral upper lobe patchy and peripheral areas of ground glass opacification (thin pur-
ple arrows) consistent with COVID-19 pneumonia. [Color figure can be viewed in the online issue, which is available at www.
laryngoscope.com.]
At outpatient follow-up, the patient had no further com- peripheral ground glass opacities consistent with COVID-
plaints of parotitis. 19 pneumonia. Bilateral intraparotid lesions consistent
with known Warthin’s tumor were also visualized. These
lesions were stable compared to previous CT imaging
Case 2 (performed 1 week prior for evaluation of facial trauma
A 64-year-old male was admitted for hyponatremia after a fall), which demonstrated multiple bilateral
in the setting of diarrhea and diuretic use and several- intraparotid lesions, with the largest on the right rep-
day history of worsening bilateral preauricular swelling resenting 2.8 × 2.2 cm in axial dimension; no swelling or
accompanied by fever. Physical examination was notable acute inflammatory changes of parotid or submandibular
for bilateral preauricular and submandibular swelling glands were evident.
consistent with parotid and submandibular gland The patient was treated with empiric intravenous
enlargement, respectively; no purulent drainage could be antibiotics, sialogogues, warm compresses/massages to
expressed from Stensen’s or Wharton’s ducts with parotid the parotid region, and hydration. Over his 10-day course
or submandibular gland massage. No decreased neck of admission, he demonstrated clinical improvement in
range of motion, difficulty breathing, or stridor were bilateral facial swelling and pain, as well as decreased
noted. Past medical history was notable for hypertension, inflammatory markers. Patient was transitioned to oral
diabetes, smoking, gastroesophageal reflux disease, and antibiotics upon discharge. At outpatient follow-up, the
Warthin’s tumor (deferred surgery). Laboratory testing patient exhibited near-complete resolution of bilateral
was notable for a positive COVID-19 RT-PCR test result facial swelling; surgical excision of the right-sided
(nasopharyngeal swab), severe leukocytosis with Warthin’s tumor was recommended.
lymphopenia and neutrophilic predominance, and posi-
tive mumps virus immunoglobulin (Ig)G test consistent
with immunization status and/or prior infection. DISCUSSION
CT imaging of the neck with IV contrast demon- Acute sialadenitis is caused by bacterial infection,
strated enlarged parotid glands with areas of hete- viral infection, non-infectious inflammatory processes
rogeneous attenuation and enhancement, as well as (e.g., sarcoidosis) and immune-mediated processes
surrounding fat stranding and fascial thickening compati- (Sjogren syndrome). Viruses causing salivary infection
ble with overlying cellulitis and fasciitis (Fig. 2). No include paramyxovirus (i.e., mumps), influenza A, para-
fluid collection or obstructing sialolith was identified. CT influenza virus, human immunodeficiency virus, and
also demonstrated retropharyngeal edema without rim coronavirus. The findings of parotitis and submandibu-
enhancement as well as enlargement and heterogeneous lar sialadenitis in two patients with documented SARS-
enhancement of the submandibular glands, with the CoV-2 infection by RT-PCR testing suggests that acute,
left greater than the right. Chest CT demonstrated nonsuppurative sialadenitis is a possible manifestation
Laryngoscope 130: November 2020 Chern et al.: Sialadenitis: Manifestation of COVID-19
2596
Fig. 2. Case 2. Contrast-enhanced computed tomography (CT) of the soft tissues of the neck. (A, B) Axial and (C) coronal CT images show
enlarged parotid glands with areas of heterogeneous enhancement and attenuation (thin dotted white arrows) with surrounding fat stranding
and fascial thickening compatible with adjacent cellulitis and fasciitis (curved yellow arrows). There is enlargement and enhancement of the left
submandibular gland consistent with acute sialadenitis (thin long red arrow). There is a mass in the right parotid gland compatible with known,
stable Warthin tumors (short green arrows). Left-sided Warthin’s tumor was also stable (not shown). There is no sialolith or fluid collection to
suggest abscess. There is a low attenuation retropharyngeal effusion without rim enhancement to suggest abscess (thick yellow arrow). [Color
figure can be viewed in the online issue, which is available at www.laryngoscope.com.]
of COVID-19. CT findings suggest that the infection imaging and with parotitis-type symptoms. However,
involves the entire gland without frank abscess formation. they did not have primary parotitis.4 Thus, the current
COVID-19 sialadenitis responded to medical manage- two cases represent the first documented cases of COVID-
ment with complete resolution. 19–related parotid and submandibular gland sialadenitis.
Viral transmission into the salivary glands most
commonly occurs through hematogenous spread, though
retrograde ductal migration may occur with decreased
salivary flow in the dehydrated patient. Animal studies CONCLUSION
have demonstrated SARS-CoV tropism for epithelial cells This case report describes a case of parotitis and
lining salivary gland ducts.2 Moreover, high viral loads of submandibular gland sialadenitis, as well as an isolated
SARS-CoV-2 have been consistently found in saliva case of parotitis, in two patients with concurrent, docu-
specimens.1 Coronaviruses have been detected in saliva mented SARS-CoV-2 infection on RT-PCR testing,
samples with high diagnostic concordance with nasopha- suggesting that acute, nonsuppurative sialadenitis is a
ryngeal specimens, widely considered the standard for possible early manifestation of COVID-19.
diagnostic testing of respiratory viruses.5 However, it
should be noted that saliva contains secretions not only
from the salivary glands, but also the nasopharynx and BIBLIOGRAPHY
the lungs. These findings in toto suggest that SARS-
1. To KKW, Tsang OTY, Yip CYC, et al. Consistent detection of 2019 novel coro-
CoV-2 directly infects salivary glands. navirus in saliva. Clin Infect Dis 2020;71:841–843.
There are two reports in the literature related to 2. Liu L, Wei Q, Alvarez X, et al. Epithelial cells lining salivary gland ducts are
early target cells of severe acute respiratory syndrome coronavirus infec-
SARS-CoV-2 salivary gland infections. One reported a tion in the upper respiratory tracts of rhesus macaques. J Virol 2011;85:
case of parotitis in a COVID-19–negative patient qua- 4025–4030.
3. Capaccio P, Surgery N, Pignataro L, et al. Acute parotitis: a possible preco-
rantined with family members (all COVID-19 positive on cious clinical manifestation of SARS-CoV-2 infection? Otolaryngol Head
RT-PCR testing). The patient was initially COVID-19 Neck Surg 2020;163:182–183.
4. Lechien JR, Chetrit A, Chekkoury-Idrissi Y, et al. Parotitis-like symptoms
negative on RT-PCR testing, but weakly positive on IgG associated with COVID-19, France, March–April 2020. Emerg Infect Dis
testing several weeks after onset of symptoms.3 Another 2020;26:2270–2271.
5. To KK, Lu L, Yip CC, et al. Additional molecular testing of saliva specimens
report described three patients with COVID-19 infection improves the detection of respiratory viruses. Emerg Microbes Infect 2017;
with intraparotid lymphadenitis on magnetic resonance 6:1–7.
Laryngoscope 130: November 2020 Chern et al.: Sialadenitis: Manifestation of COVID-19
2597
View publication stats
You might also like
- Pulmonary Pathology of Early-Phase 2019 Novel Coronavirus (COVID-19) Pneumonia in Two Patients With Lung CancerDocument5 pagesPulmonary Pathology of Early-Phase 2019 Novel Coronavirus (COVID-19) Pneumonia in Two Patients With Lung Cancermuhammad RidoNo ratings yet
- PIIS1201971220301016Document6 pagesPIIS1201971220301016Gordana PuzovicNo ratings yet
- Complicated Sinusitis With Sphenopalatine Artery Thrombosis in A COVID-19 Patient, A Case ReportDocument3 pagesComplicated Sinusitis With Sphenopalatine Artery Thrombosis in A COVID-19 Patient, A Case ReportNurul Aisyah PaldarNo ratings yet
- Tian Early PhaseDocument12 pagesTian Early PhaseAurelian CârsteaNo ratings yet
- Rli 55 257Document5 pagesRli 55 257WilsonR.CorzoNiñoNo ratings yet
- Unusual Presentation of Covid-19 in Patient With Acute AbdomenDocument4 pagesUnusual Presentation of Covid-19 in Patient With Acute AbdomenCirugía General HGRNo ratings yet
- Episcleritis As An Ocular Manifestation in A Patient With COVID 19Document3 pagesEpiscleritis As An Ocular Manifestation in A Patient With COVID 19Hocie Trinanda SardiNo ratings yet
- MainDocument8 pagesMainWilsonR.CorzoNiñoNo ratings yet
- Articulo Cientifico Derrame Pleural en Covid 19Document10 pagesArticulo Cientifico Derrame Pleural en Covid 19Leyla Barnard LagunaNo ratings yet
- 1 s2.0 S1930043320306208 MainDocument3 pages1 s2.0 S1930043320306208 MainRivaldy BobihuNo ratings yet
- 2019 Novel Coronavirus Disease (COVID-19) in Taiwan: Reports of Two Cases From Wuhan, ChinaDocument4 pages2019 Novel Coronavirus Disease (COVID-19) in Taiwan: Reports of Two Cases From Wuhan, ChinaClaav HugNo ratings yet
- Paper 1Document6 pagesPaper 1ivan.montenegroNo ratings yet
- Coronavirus (COVID-19) OutbreakDocument5 pagesCoronavirus (COVID-19) OutbreakPrima Sarana MedikaNo ratings yet
- International Journal of Infectious DiseasesDocument7 pagesInternational Journal of Infectious Diseaseshardilas kaur behalNo ratings yet
- Emp2 12098Document4 pagesEmp2 12098Miva MaviniNo ratings yet
- REPORTE CASO TBC y COVID 19Document6 pagesREPORTE CASO TBC y COVID 19Farmaco VigilanciaNo ratings yet
- Research Letters: Co-Infection With Sars-Cov-2 and Influenza A Virus in Patient With Pneumonia, ChinaDocument3 pagesResearch Letters: Co-Infection With Sars-Cov-2 and Influenza A Virus in Patient With Pneumonia, Chinajitesh141No ratings yet
- Case Report Scopus CandraDocument6 pagesCase Report Scopus CandraDr.gendjutNo ratings yet
- Perfusie Afwijkingen in Covid 19 Patienten 1603707976Document10 pagesPerfusie Afwijkingen in Covid 19 Patienten 1603707976Muhammad Al-DulaimyNo ratings yet
- Neumonia Intersti CovidDocument11 pagesNeumonia Intersti CovidsantospardogomezNo ratings yet
- Coronavirus (COVID-19) Outbreak: What The Department of Radiology Should KnowDocument5 pagesCoronavirus (COVID-19) Outbreak: What The Department of Radiology Should KnowrezaNo ratings yet
- 10 1513@annalsats 202004-324ocDocument36 pages10 1513@annalsats 202004-324ocDany Daniel Rafael HuamanNo ratings yet
- Functional and Radiological Improvement in A COVID-19 Pneumonia Patient Treated With SteroidsDocument5 pagesFunctional and Radiological Improvement in A COVID-19 Pneumonia Patient Treated With Steroidsmostafa aliNo ratings yet
- Research JournalDocument7 pagesResearch JournalHyacinth A RotaNo ratings yet
- Ibi JurnalDocument9 pagesIbi JurnalRiski Pradika 2017No ratings yet
- JMV 25815Document2 pagesJMV 25815fadil ahmadiNo ratings yet
- The Clinical and Chest CT Features Associated With Severe and Critical COVID-19 PneumoniaDocument5 pagesThe Clinical and Chest CT Features Associated With Severe and Critical COVID-19 PneumoniaNadanNadhifahNo ratings yet
- Conjunctivitis in COVID-19 Patients: Frequency and Clinical PresentationDocument7 pagesConjunctivitis in COVID-19 Patients: Frequency and Clinical PresentationStephanie AureliaNo ratings yet
- Wa0015.4Document7 pagesWa0015.4jeyiy92174No ratings yet
- Clinical Characteristics of COVID-19 Complicated With Pleural EffusionDocument10 pagesClinical Characteristics of COVID-19 Complicated With Pleural EffusionInternal MedicineNo ratings yet
- Cerebrovascular Disease in COVID-19: Adult BrainDocument3 pagesCerebrovascular Disease in COVID-19: Adult BrainUsman Agus PrasetyoNo ratings yet
- COVID-19 Autopsies - Aqaa062Document9 pagesCOVID-19 Autopsies - Aqaa062Pramod BiradarNo ratings yet
- Medical Mycology Case ReportsDocument5 pagesMedical Mycology Case ReportsGUSTI AYU PUTU KRISNA DEWINo ratings yet
- Hemorhagic PRESDocument4 pagesHemorhagic PRESAbdul AzeezNo ratings yet
- USS 2020-I. - Autop - COVID19Document9 pagesUSS 2020-I. - Autop - COVID19Jerry Carhuatanta SaavedraNo ratings yet
- COVID-19 Autopsies, Oklahoma, USADocument9 pagesCOVID-19 Autopsies, Oklahoma, USARhagaraRhaNo ratings yet
- Clinical and Imaging Features of COVID19Document8 pagesClinical and Imaging Features of COVID19ClaudiaNo ratings yet
- Proning in Non-Intubated (PINI) in Times of COVID-19: Case Series and A ReviewDocument7 pagesProning in Non-Intubated (PINI) in Times of COVID-19: Case Series and A ReviewCarlos ZepedaNo ratings yet
- JR COvid-19 Dan Anosmia Dr. SukriDocument25 pagesJR COvid-19 Dan Anosmia Dr. SukriAlmiraNo ratings yet
- Geriatric Patient With Osteoarthritis and Obesity Survived From Critically Ill of COVID-19: A Case ReportDocument5 pagesGeriatric Patient With Osteoarthritis and Obesity Survived From Critically Ill of COVID-19: A Case Reportnadila raudhani pNo ratings yet
- Piis014067362030920x PDFDocument4 pagesPiis014067362030920x PDFgonzaloNo ratings yet
- Piis014067362030920x PDFDocument4 pagesPiis014067362030920x PDFgonzaloNo ratings yet
- Hypothesis: Hui Li, Liang Liu, Dingyu Zhang, Jiuyang Xu, Huaping Dai, Nan Tang, Xiao Su, Bin CaoDocument4 pagesHypothesis: Hui Li, Liang Liu, Dingyu Zhang, Jiuyang Xu, Huaping Dai, Nan Tang, Xiao Su, Bin CaogonzaloNo ratings yet
- Journal of Clinical and Translational Endocrinology: Case ReportsDocument5 pagesJournal of Clinical and Translational Endocrinology: Case ReportsKartikaa YantiiNo ratings yet
- Essentials For Radiologists OnDocument2 pagesEssentials For Radiologists Onzahra ebrahimiNo ratings yet
- Idcases: Sergio Zaccaria Scalinci, Edoardo Trovato BattagliolaDocument3 pagesIdcases: Sergio Zaccaria Scalinci, Edoardo Trovato BattagliolaMuhamad ZenNo ratings yet
- Estudo DiabetesDocument9 pagesEstudo DiabetesFulano de TalNo ratings yet
- 1 s2.0 S1015958423006000 MainDocument2 pages1 s2.0 S1015958423006000 Mainmodacasper056No ratings yet
- Genomewide Association Study of SevereDocument13 pagesGenomewide Association Study of SevereANANo ratings yet
- EnovaraDocument4 pagesEnovaraenilNo ratings yet
- 2020-Autopsias COVID 4Document6 pages2020-Autopsias COVID 4Mario Martínez TorijaNo ratings yet
- LeukoeritroblastikDocument2 pagesLeukoeritroblastiknadaNo ratings yet
- Misdiagnosis in Covid19 Era JACC PDFDocument6 pagesMisdiagnosis in Covid19 Era JACC PDFRirin Efsa JutiaNo ratings yet
- Correlation Between Ground-Glass Opacity On Pulmonary CT and The Levels of Inflammatory CytokinesDocument7 pagesCorrelation Between Ground-Glass Opacity On Pulmonary CT and The Levels of Inflammatory CytokinesEarlya RifaniNo ratings yet
- Pi Is 0749070421000439Document21 pagesPi Is 0749070421000439Vlady78No ratings yet
- An Adolescent With A Retropharyngeal Swelling ToDocument4 pagesAn Adolescent With A Retropharyngeal Swelling Tolincolnbasilio1No ratings yet
- 1 s2.0 S0924857920301059 MainDocument13 pages1 s2.0 S0924857920301059 MainNini RinNo ratings yet
- Foldes, D., Et Al. (2020) - Plasmacytoid Lymphocytes in SARS CoV 2 Infection (Covid 19) - American Journal of Hematology PDFDocument2 pagesFoldes, D., Et Al. (2020) - Plasmacytoid Lymphocytes in SARS CoV 2 Infection (Covid 19) - American Journal of Hematology PDFRalt MedNo ratings yet
- Letter TO THE Editor: Secondary Organizing Pneumonia After Varicella-Zoster Virus Infection: A Rare AssociationDocument3 pagesLetter TO THE Editor: Secondary Organizing Pneumonia After Varicella-Zoster Virus Infection: A Rare AssociationfatimiahmastaNo ratings yet
- Brit J Clinical Pharma - 2011 - Ardern Jones - Skin Manifestations of Drug AllergyDocument12 pagesBrit J Clinical Pharma - 2011 - Ardern Jones - Skin Manifestations of Drug Allergyrochmandrg dokter gigiNo ratings yet
- Clinical Manifestation of Oral Tuberculosis in Hiv Patient A Review Article 1Document4 pagesClinical Manifestation of Oral Tuberculosis in Hiv Patient A Review Article 1rochmandrg dokter gigiNo ratings yet
- Insights Into Hypersensitivity Reactions In.6Document10 pagesInsights Into Hypersensitivity Reactions In.6rochmandrg dokter gigiNo ratings yet
- A Brief Review of The Mechanisms of Drug HypersensitivityDocument6 pagesA Brief Review of The Mechanisms of Drug Hypersensitivityrochmandrg dokter gigiNo ratings yet
- Aop 157Document4 pagesAop 157rochmandrg dokter gigiNo ratings yet
- Ipm 3Document4 pagesIpm 3rochmandrg dokter gigiNo ratings yet
- Antibiotic Hypersensitivity MechanismsDocument14 pagesAntibiotic Hypersensitivity Mechanismsrochmandrg dokter gigiNo ratings yet
- KARIXA Dentolaser KA 45-01 DLDocument1 pageKARIXA Dentolaser KA 45-01 DLrochmandrg dokter gigiNo ratings yet
- Immunopathogenesis of Delayed-Type HypersensitivityDocument5 pagesImmunopathogenesis of Delayed-Type Hypersensitivityrochmandrg dokter gigiNo ratings yet
- Depression and HIV Disease Progression A Mini-ReviewDocument7 pagesDepression and HIV Disease Progression A Mini-Reviewrochmandrg dokter gigiNo ratings yet
- JAIP Portnoy Et Al PDFDocument3 pagesJAIP Portnoy Et Al PDFrochmandrg dokter gigiNo ratings yet
- Dehydration Pathway 2016Document3 pagesDehydration Pathway 2016rochmandrg dokter gigiNo ratings yet
- Patch Test ROAT PDFDocument9 pagesPatch Test ROAT PDFrochmandrg dokter gigiNo ratings yet
- I Nyoman Wande, Muhamad Robi'ul Fuadi, Solichul Hadi: Background: ResultsDocument5 pagesI Nyoman Wande, Muhamad Robi'ul Fuadi, Solichul Hadi: Background: Resultsrochmandrg dokter gigiNo ratings yet
- тезисыDocument1 pageтезисыrochmandrg dokter gigiNo ratings yet
- Iufd Lesson PlanDocument21 pagesIufd Lesson PlanBupe LwitaNo ratings yet
- Etool Administration of IV MedicationDocument4 pagesEtool Administration of IV MedicationReeham UsmanNo ratings yet
- Dr. Kiki - Pengantar Trauma UpdateDocument20 pagesDr. Kiki - Pengantar Trauma UpdateRsud Malinau Ppk Blud100% (1)
- (En) 2024 BIOOD Biophilia Tracker X4 MAX FeaturesDocument16 pages(En) 2024 BIOOD Biophilia Tracker X4 MAX FeaturesjsemsamsebouNo ratings yet
- 05 Allama Rozan Firdaus Hortatory Text TaskDocument2 pages05 Allama Rozan Firdaus Hortatory Text TaskAllama Rozan FirdausNo ratings yet
- Optical Coherence Tomography (OCT) in Neurologic DiseasesDocument232 pagesOptical Coherence Tomography (OCT) in Neurologic DiseasesirodalexandraNo ratings yet
- Abruptio Placenta Drug StudyDocument5 pagesAbruptio Placenta Drug StudyJayne Angelie A. NuevaespañaNo ratings yet
- TPN Origin and CalculationsDocument42 pagesTPN Origin and CalculationsmajdNo ratings yet
- TranscriptDocument4 pagesTranscriptGuru PrasadNo ratings yet
- Sepsis and Severe Pneumonia (2022)Document39 pagesSepsis and Severe Pneumonia (2022)rina delsNo ratings yet
- Adult CardDocument4 pagesAdult CardagelsantosNo ratings yet
- Intraoperative Complications: Mandibular Anterior: Intraosseous VesselsDocument2 pagesIntraoperative Complications: Mandibular Anterior: Intraosseous VesselsRoenteiqNo ratings yet
- Untitled DocumentDocument4 pagesUntitled Documentclockstudy5No ratings yet
- Nursing Exam CompreDocument9 pagesNursing Exam ComprerikidbNo ratings yet
- Surat Buat VisaDocument12 pagesSurat Buat VisaNurul FitrianaNo ratings yet
- Drug Administration Route Needle Size EtcDocument1 pageDrug Administration Route Needle Size EtcRon AbuNo ratings yet
- Senarai Nama Anggota Unit Rawatan Rapi, Hospital Queen Elizabeth Ii 2014Document8 pagesSenarai Nama Anggota Unit Rawatan Rapi, Hospital Queen Elizabeth Ii 2014Rosyta DawatNo ratings yet
- Cardiac BiomarkersDocument32 pagesCardiac BiomarkersMaham RehmanNo ratings yet
- Principles For Aseptic Technique - Information For Healthcare Workers - December 2021Document5 pagesPrinciples For Aseptic Technique - Information For Healthcare Workers - December 2021ebubechukwu echefuNo ratings yet
- CNS Stimulants 2023Document10 pagesCNS Stimulants 2023ManWol JangNo ratings yet
- Questions and Answer Group 3 "Glaucoma" Nama: Gustin Ibrahim Umamah Kelas: A S1 FARMASI 2017 NIM: 821417021Document13 pagesQuestions and Answer Group 3 "Glaucoma" Nama: Gustin Ibrahim Umamah Kelas: A S1 FARMASI 2017 NIM: 821417021Afni YunitaNo ratings yet
- High Power CommitteeDocument39 pagesHigh Power CommitteeJaya PrabhaNo ratings yet
- Psych ReportDocument80 pagesPsych ReportPaul Carlo GonzalesNo ratings yet
- Wound Bed Score and Its Correlation With Healing of Chronic WoundsDocument8 pagesWound Bed Score and Its Correlation With Healing of Chronic WoundsErick VásquezNo ratings yet
- Chapter 18 VaccinesDocument29 pagesChapter 18 Vaccineshusseinabdullahahmad99No ratings yet
- RATE LIST of Recognized Private Hospitals and Diagnostic Centres UnderDocument44 pagesRATE LIST of Recognized Private Hospitals and Diagnostic Centres UnderbharatwerulkarNo ratings yet
- Haemostasis and Thrombosis: An Overview: H. RascheDocument5 pagesHaemostasis and Thrombosis: An Overview: H. Rascheshinichi kudoNo ratings yet
- Can Mothers Breastfeed During The COVIDDocument4 pagesCan Mothers Breastfeed During The COVIDAnisa RamdhiniNo ratings yet
- TESDA COVID-19 Health Status Daily Monitoring TESDA COVID - 19 Health Status Daily MonitoringDocument1 pageTESDA COVID-19 Health Status Daily Monitoring TESDA COVID - 19 Health Status Daily MonitoringMICS TVNo ratings yet
- Infectious Diseases II PDFDocument62 pagesInfectious Diseases II PDFhuong LNo ratings yet