Professional Documents
Culture Documents
The Human Heart
The Human Heart
Uploaded by
Frama Intan Miguel0 ratings0% found this document useful (0 votes)
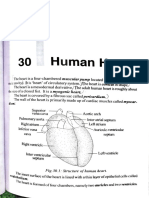
44 views4 pagesThe heart is a hollow, cone-shaped muscle located in the chest cavity between the lungs. It pumps blood through two circulatory systems - systemic circulation provides oxygen and nutrients to the entire body, while pulmonary circulation oxygenates blood in the lungs. The heart has four chambers separated by valves that ensure one-way blood flow. It is surrounded by membranes and receives blood supply from coronary arteries. The cardiac conduction system generates heartbeats that drive rhythmic contractions and pumping of blood to the lungs and body.
Original Description:
Study guide for cardio anaphy
Original Title
The human heart
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThe heart is a hollow, cone-shaped muscle located in the chest cavity between the lungs. It pumps blood through two circulatory systems - systemic circulation provides oxygen and nutrients to the entire body, while pulmonary circulation oxygenates blood in the lungs. The heart has four chambers separated by valves that ensure one-way blood flow. It is surrounded by membranes and receives blood supply from coronary arteries. The cardiac conduction system generates heartbeats that drive rhythmic contractions and pumping of blood to the lungs and body.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
0 ratings0% found this document useful (0 votes)
44 views4 pagesThe Human Heart
The Human Heart
Uploaded by
Frama Intan MiguelThe heart is a hollow, cone-shaped muscle located in the chest cavity between the lungs. It pumps blood through two circulatory systems - systemic circulation provides oxygen and nutrients to the entire body, while pulmonary circulation oxygenates blood in the lungs. The heart has four chambers separated by valves that ensure one-way blood flow. It is surrounded by membranes and receives blood supply from coronary arteries. The cardiac conduction system generates heartbeats that drive rhythmic contractions and pumping of blood to the lungs and body.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
Download as docx, pdf, or txt
You are on page 1of 4
Heart middle layer; primarily cardiac muscle
- a hollow, vaguely cone-shaped, and only contractility/pumping
weighs about 250 to 350 grams blood supply comes from coronary arteries
Location: myocardium of left ventricles are thicker
- rest on the diaphragm mediastinum cardiac bundles of myocardium:
cavity between lungs. function to squeeze blood through
- Oblique position with apex lying left to heart in the proper directions
the midline inferior through the atria
Heart orientation superiorly through ventricles
Apex directed anteriorly, inferiorly and to
the left 3) Endocardium
Base directed posteriorly, superiorly and to Endo = inner
the right Stretches as heart pumps
Anterior surface deep to the sternum and Fibrous skeleton of heart
ribs Dense ct rings surround the valves, fuse
Inferior surface rest on diaphragm and merge with iv septum
Right border faces right lung Supports structure for heart valves
Left border (pulmo border) faces left lung’ Insertion point for cardiac muscle bundles
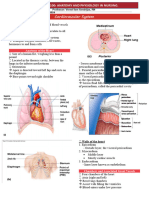
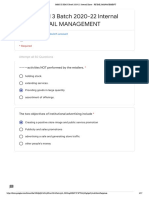
structures of the heart Electrical insulator betweeb atria and
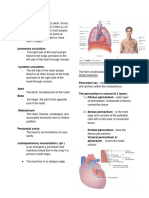
Pericardium ventricle to prevent direct propagation of
(peri=around); protective sac of connective ap’s to ventricles
tissue sulci of the heart
surrounding the heart; confines it to External boundaries are marked by 2 Series of
mediastinum groves on the surface of heart called sulci
2 parts: contain fat and coronary blood vessel
i. the fibrous pericardium- tough a) Coronary sulcus
outer layer thin inelastic, dense Encircles heart and mark boundary
irregular connective tissue. between atria and the ventricles
Anchors heart to mediastinum b) Anterior interventricular sulcus
ii. the serous pericardium- thinner, mark boundary between ventricles
more delicate divided into anteriorly
a. parietal c) posterior interventricular sulcus
b. visceral mark boundary between ventricles
o pericardial cavity- between posteriorly
parietal and visceral layers septum
Walls of the heart: thin Inner partition that divides heart into 2
1) Epicardium sides creating the 4 chambers
- Epi = upon/above interatrial septum partitions the atria
- Outermost; fat to cushion heart interventricular septum partitions
- Visceral layer of serous pericardium. ventricles
- Composed of mesothelium & delicate Chambers of the heart
connective tissue 2 superior atria (low pressure) thin walled
2) Myocardium receiving chambers for the blood coming back
myo = muscle to the heart after circulating
o right atrium blood vessels running through the entire
receives blood from 3 sources (SVC, IVC body.
and Coronary Sinus) Blood vessels:
o left atrium Arteries
forms most of the base of the heart carry blood away from the heart to tissues
receives blood from lungs, 4 pulmonary of body
veins (2 R+ 2L) large vessel carrying oxygen rich blood,
2 inferior ventricles (high pressure) thick walled with exception of pulmonary arteries
discharging chambers that push blood back out thick walled need to withstand pressure
the heart produced when heart pushes blood into
o right ventricle them
forms most of anterior surface of the heart Veins
o left ventricle carry it back to heart
myocardium of LV is thicker than thr right From capillary system blood returned to
Heart valves heart via veins
Each chamber has corresponding valves. Largest vein contains one way valves that
Connected to the inner walls of the heart keep blood flowing to the heart
by tough tendons that allows valves to (3 layers of artery/veins: The outer layer is tunica
close and hold the valve flaps in place (like Externa, the middle layer—called tunica media—
arm holding a door!) is muscle and fiber. The innermost layer, tunica
Mnemonics: (try puling my aorta) intima, is the one that comes in direct contact
2 atrioventricular valves that close at the with blood)
beginning of ventricular contraction. They Capillaries
prevent blood from flowing back into the link arterioles to veins.
atria Smallest blood vessel
a) Tricuspid valve- right side, separates Important for bringing nutrients and
right atrium to right ventricle oxygen to tissues and absorbing co2 and
b) Mitral valve- left, separates left atrium to other waste products
left ventricle There are 2 blood circulatory system in the
2 semilunar valves that prevents blood from human body which are connected:
flowing back into ventricles during 1) The systemic circulation
relaxation: provides organs, tissues and cells with
c) Pulmonic semilunar valve- separates blood so that they get oxygen and other
right ventricle from pulmonary artery vital substances.
d) Aortic valve= left side, separates left blood flows from the heart to all parts of
ventricle from aorta the body and back to the heart
Lub dub- sounds of valve opening and closing 2) The pulmonary circulation
where the fresh oxygen we breathe in
enters the blood. At the same time, carbon
dioxide is released from the blood.
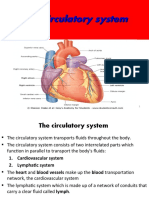
The blood circulatory system blood flows from the heart to the lungs and
delivers nutrients and oxygen to all cells in back to the heart
the body. It consists of the heart and the
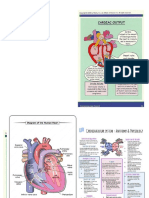
There are 14 steps in a circle of blood for easy Cardiac output calculation
illustration: Co = sv x hr
Ml/min ml/beat beats/min
1. Superior/ Inferior Vena Cava Cardiac output is normally 5l/min and is
2. (deoxygenated blood) right atrium determined by multiplying the hr by sv
3. Tricuspid valve Co- Cardiac output: amount blood pumped
4. right ventricle by ventricles in 1 min
5. pulmonary valve Sv- stroke volume: amount of blood
6. pulmonic artery pumped out of a ventrical during each
7. (oxygenated blood) lungs contraction
8. pulmonary veins Hr- heart rate: number of beats per min.
9. left atrium Control of cardiac output
10. mitral valve Factors affecting stroke volume
11. left ventricle Preload
12. aortic valve - Volume of blood inn ventricles at the
13. aorta and coronary arteries end of diastole (end diastolic pressure)
14. body Increased in:
15. back to heart via vena cava Hypovolemia
Regurgitation of cardiac valves
Heart failure
Conduction system Afterload
The heartbeat is generated by cardiac - Resistance left ventricle must overcome
conduction to force blood out of the heart and to circulate blood
to the rest of the body. - Increased in: hypertension,
1) Sinoatrial (sa) node vasoconstriction
2) Atrioventricular (av) node - Increased afterload = increased cardiac
3) Bundle of his workload
4) L and R bundle branch Contractility
5) Purkinje fibers - Amount of force generated by
myocardium to eject blood into
Heart sounds circulation. Ventricular compliance and
Each valve sound is best heard in diff. filling pressure affect the stroke volume
corners Increasing cardiac output
Pulmo. Valve= superior left Incre. Preload- blood returning to right
Aortic valve= superior right atrium
Mitral (bicuspid) = apex Inre. Contractility
Tricuspid= inferior right Decre. Afterload- pressure heart pump
Co-ordination of the heartbeat against
One complete sequence of contraction and Factors affecting heart rate
relaxation is called heartbeat Hr affects co by causing a decrease or
Lub is a softer sound of atria contracting increase in stroke volume
Dub is louder sound of ventricles Controlled by baroreceptors in aortic arch
contracting which are sensitive to changes in bp
Parasympathetic ns stimulation= slow hr
sympathetic ns stimulation= increase hr
You might also like
- Zollinger EllisonDocument2 pagesZollinger EllisonFrama Intan MiguelNo ratings yet
- Turnip28 V16a Core RulesDocument73 pagesTurnip28 V16a Core RulesСлавік БачинськийNo ratings yet
- Chapter 12: Heart: Functions of The HeartDocument12 pagesChapter 12: Heart: Functions of The Heartchristian anchetaNo ratings yet
- Linking Words ExercisesDocument4 pagesLinking Words ExercisesNLBekvalac100% (1)
- CARDIOVASDocument3 pagesCARDIOVASFrama Intan MiguelNo ratings yet
- Heart: Size, Form, and Location: Cardiovascular SystemDocument3 pagesHeart: Size, Form, and Location: Cardiovascular Systemskyler andradaNo ratings yet
- Cardiovascular SystemDocument26 pagesCardiovascular SystemumerjicNo ratings yet
- The Circulatory System ZooDocument9 pagesThe Circulatory System Zoopierre TritzNo ratings yet
- Lecture 3 Cardiovascular System 1Document54 pagesLecture 3 Cardiovascular System 1hafiz patah100% (1)
- Acfrogb 7ik4ojriyfu8nvvwmohozvp1pcb2hjyh47jdwvhnpmnhiyornnhy - Xeyhodxnx4wlzdu5sc59 1gvhetgkpoh5ws31c2bftcevdfose32075g4qf78x9c08Document60 pagesAcfrogb 7ik4ojriyfu8nvvwmohozvp1pcb2hjyh47jdwvhnpmnhiyornnhy - Xeyhodxnx4wlzdu5sc59 1gvhetgkpoh5ws31c2bftcevdfose32075g4qf78x9c08Bala GanapathyNo ratings yet
- Cardiovascular SystemDocument4 pagesCardiovascular Systembuhia.quennieNo ratings yet
- Lect 8. Cardiovascular SystemDocument35 pagesLect 8. Cardiovascular Systemrukhsanatariq299No ratings yet
- Cardiovascular - SummaryDocument18 pagesCardiovascular - Summarys.tinaja.marieantonetteNo ratings yet
- Heart and Neck VesselsDocument3 pagesHeart and Neck VesselsMark ElbenNo ratings yet
- Syok Hipovolemik EnglishDocument25 pagesSyok Hipovolemik Englishatmarida 123No ratings yet
- 0.8 Sec. The HeartDocument9 pages0.8 Sec. The Heartmary lee gumapacNo ratings yet
- Cardiovascular SystemDocument16 pagesCardiovascular SystemMa Ellen LumauagNo ratings yet
- Anaphysio MC1Document12 pagesAnaphysio MC1KRISTINE CHAD NAVALES CANTALEJONo ratings yet
- Cardiovascular System: Anatomy and PhysiologyDocument10 pagesCardiovascular System: Anatomy and PhysiologyDavid PunzalanNo ratings yet
- Cardiovascular System - The HeartDocument37 pagesCardiovascular System - The HeartCecil AlbaNo ratings yet
- Cardiovascular System WordDocument18 pagesCardiovascular System WordLapitan Jared Anne S.No ratings yet
- Cardiovascular SystemDocument10 pagesCardiovascular SystemGlen DaleNo ratings yet
- Scan Dec 12, 2022Document6 pagesScan Dec 12, 2022Saktheeswaran VNo ratings yet
- #3 Cardiovascular SystemDocument18 pages#3 Cardiovascular SystemLapitan Jared Anne S.No ratings yet
- Mc1 Reviewer (Cardiovascular System) - MidtermsDocument2 pagesMc1 Reviewer (Cardiovascular System) - MidtermsFrancine Dominique CollantesNo ratings yet
- ANATOMY Final pt.1Document26 pagesANATOMY Final pt.1Gladys Mae S. BañesNo ratings yet
- Anatomy & Physiology NotesDocument56 pagesAnatomy & Physiology NotesChristina Gonez100% (2)
- Circulatory SystemDocument47 pagesCirculatory Systemeliassultan3No ratings yet
- Cardiovascular System Anatomy and PhysiologyDocument14 pagesCardiovascular System Anatomy and PhysiologyKIRSTEN CHAVEZ100% (1)
- 10th Week Practical LessonsDocument11 pages10th Week Practical LessonstheodorastanerNo ratings yet
- Cardiovascular / Circulatory System: Upper Chambers or Receiving ChambersDocument2 pagesCardiovascular / Circulatory System: Upper Chambers or Receiving ChambersRashid DayaoNo ratings yet
- 8 CardiovascularDocument44 pages8 CardiovascularleonardodataguroNo ratings yet
- Chapter 19 Heart Marie BDocument29 pagesChapter 19 Heart Marie BomarNo ratings yet
- Anatomy & Physiology of The Cardiovascular SystemDocument3 pagesAnatomy & Physiology of The Cardiovascular SystemluaNo ratings yet
- CARDIOLOGYDocument15 pagesCARDIOLOGYPatty RomeroNo ratings yet
- 8.cardiovascular SystemDocument13 pages8.cardiovascular Systempodki gurungNo ratings yet
- Lecture 5 & 6Document32 pagesLecture 5 & 6raja11160No ratings yet
- HEARTDocument8 pagesHEARTSJane FeriaNo ratings yet
- Heart Reviewer 1Document6 pagesHeart Reviewer 1tokzzNo ratings yet
- HeartDocument45 pagesHeartlilac.poppy.48No ratings yet
- Ana CardioDocument3 pagesAna CardioFIONA DANE MAURERANo ratings yet
- Circulatory SDocument110 pagesCirculatory SMohammed HabibNo ratings yet
- Anatomy Circulatory SystemDocument131 pagesAnatomy Circulatory Systemanduamlakmolalgn332No ratings yet
- Lesson 12 HeartDocument9 pagesLesson 12 HeartEly FructuosoNo ratings yet
- Anatomy5.heart and Large VesselesDocument73 pagesAnatomy5.heart and Large VesselesAhmadNo ratings yet
- HeartDocument7 pagesHeartlilac.poppy.48No ratings yet
- PRINTED Cardiovascular System (Heart) HandoutsDocument7 pagesPRINTED Cardiovascular System (Heart) HandoutsKate GutierrezNo ratings yet
- The Circulatory SystemDocument114 pagesThe Circulatory SystemKhant Si ThuNo ratings yet
- Cardio 1Document7 pagesCardio 1Moon KillerNo ratings yet
- Heart Finals ReviewerDocument7 pagesHeart Finals ReviewershannenmaehfajanilanNo ratings yet
- Anatomy and Physiology of The HeartDocument9 pagesAnatomy and Physiology of The HeartNina Anne ParacadNo ratings yet
- Anaphy CardioDocument6 pagesAnaphy CardioDianne DimaanoNo ratings yet
- Blood Vessels CirculationDocument6 pagesBlood Vessels Circulationskyler andradaNo ratings yet
- Anterolateral Posteriorly Superiorly Inferiorly:: Cardiovascular System DR - Nadia HameedDocument7 pagesAnterolateral Posteriorly Superiorly Inferiorly:: Cardiovascular System DR - Nadia HameedIIAhmedIINo ratings yet
- Anatomia Del CorazonDocument21 pagesAnatomia Del CorazonAndrea OrtizNo ratings yet
- CHAP11Document12 pagesCHAP11Crystal ARIETANo ratings yet
- Anatomy NstemiDocument3 pagesAnatomy NstemiSheana Tmpl100% (1)
- HeartDocument18 pagesHeartCORONEL, SOPHIANo ratings yet
- Heart and Neck VesselsDocument31 pagesHeart and Neck Vesselsshellacayetano2No ratings yet
- Mammalian Heart PDFDocument5 pagesMammalian Heart PDFKhaled TurkNo ratings yet
- Chapter 13 - HeartDocument5 pagesChapter 13 - Heartbussniesm05No ratings yet
- L2 Cardiovascular SystemDocument32 pagesL2 Cardiovascular SystemGlen DaleNo ratings yet
- CARDIOVASDocument3 pagesCARDIOVASFrama Intan MiguelNo ratings yet
- CardiovascularDocument2 pagesCardiovascularFrama Intan MiguelNo ratings yet
- CellDocument3 pagesCellFrama Intan MiguelNo ratings yet
- UcosDocument18 pagesUcoskks12No ratings yet
- Using MLAG in Dell Networks v1.3Document33 pagesUsing MLAG in Dell Networks v1.3Damian CostantinoNo ratings yet
- Ds 1Document8 pagesDs 1michaelcoNo ratings yet
- Da Vinci Surgical System Power PointDocument23 pagesDa Vinci Surgical System Power PointJaed CaraigNo ratings yet
- Figure Skating Spirals in CompetitionDocument2 pagesFigure Skating Spirals in CompetitionAlexandra PurcaroiuNo ratings yet
- Elln Matrix: Valenzuela South District Ilang-Ilang St. Karuhatan, Valenzuela City Tel/fax No. 2944246Document1 pageElln Matrix: Valenzuela South District Ilang-Ilang St. Karuhatan, Valenzuela City Tel/fax No. 2944246rafaela villanuevaNo ratings yet
- State Senator Darryl Rouson Aug. 27 LetterDocument1 pageState Senator Darryl Rouson Aug. 27 LetterWTSP 10No ratings yet
- ReadmeDocument6 pagesReadmegabyorNo ratings yet
- 2000girls tcm77-254006Document92 pages2000girls tcm77-254006ВладиславNo ratings yet
- As I Follow Christ by Dwain N. EsmondDocument138 pagesAs I Follow Christ by Dwain N. EsmondGabor KovacsNo ratings yet
- Important Safeguards. Instrucciones Importantes de SeguridadDocument2 pagesImportant Safeguards. Instrucciones Importantes de SeguridadLUISA MALDONADO ROANo ratings yet
- ArtsDocument71 pagesArtsits.me.brader07No ratings yet
- Retail Management Final ExamDocument17 pagesRetail Management Final ExamAkhilesh JadhavNo ratings yet
- Pub - Green Advertising and Green Public Relations As Integration PropagandaDocument16 pagesPub - Green Advertising and Green Public Relations As Integration PropagandagbthomasonNo ratings yet
- Senate Bill 1483Document15 pagesSenate Bill 1483SAS NwSSUNo ratings yet
- 3 Experiment ChemistryDocument30 pages3 Experiment ChemistryThangavel SarujanNo ratings yet
- GP Maths Grade 10 June 2023 P2 and MemoDocument11 pagesGP Maths Grade 10 June 2023 P2 and Memoshaybusiness022No ratings yet
- Menz Issue 1Document40 pagesMenz Issue 1Dan Moore100% (2)
- The Massive Korean Wave in Indonesia and Its Effects in The Term of CultureDocument6 pagesThe Massive Korean Wave in Indonesia and Its Effects in The Term of CultureRaven RhythmNo ratings yet
- Practical-1: AIM: Implement A Program Which Can Decrypt The Original Message From The GivenDocument65 pagesPractical-1: AIM: Implement A Program Which Can Decrypt The Original Message From The GivenprogrammerNo ratings yet
- 3:3Document15 pages3:3Nicholas CemenenkoffNo ratings yet
- Cell Phone Radiation PresentationDocument16 pagesCell Phone Radiation PresentationCeasar CoolNo ratings yet
- Scope of WorkDocument5 pagesScope of WorkKausik DewanNo ratings yet
- That Palastic Bag Should Be BannedDocument12 pagesThat Palastic Bag Should Be Bannedlili afidaNo ratings yet
- Padlet Crib Sheet v0.2Document2 pagesPadlet Crib Sheet v0.2Abdou OsseniNo ratings yet
- Lecture3 - Logic Operation FundamentalsDocument64 pagesLecture3 - Logic Operation FundamentalsTrần Quốc ToảnNo ratings yet
- Social Media and The New Product Development Dur 2021 Technological ForecastDocument15 pagesSocial Media and The New Product Development Dur 2021 Technological ForecastFaisal KeryNo ratings yet
- Fso RF - Out RXRDocument11 pagesFso RF - Out RXRRF_RAJANo ratings yet