Professional Documents
Culture Documents
Moore R
Moore R
Uploaded by
Elaine IllescasCopyright:
Available Formats
You might also like
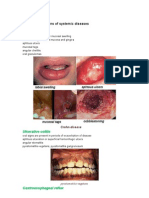
- Oral Manifestations of Systemic DiseasesDocument11 pagesOral Manifestations of Systemic DiseasesMezo Salah100% (2)
- Risk Assessment TemplateDocument3 pagesRisk Assessment TemplateGus VanGeijtenbeekNo ratings yet
- Postoperative Nausea and VomitingDocument33 pagesPostoperative Nausea and Vomitingferlina100% (1)
- Hospital SWOT AnalysisDocument2 pagesHospital SWOT AnalysisKenny Josef96% (26)
- Thailand Traditions and BeliefsDocument6 pagesThailand Traditions and Beliefsapi-316342033100% (1)
- Out 9Document12 pagesOut 9rezkyprayogiNo ratings yet
- Evidence-Based Management of Postoperative Nausea and Vomiting: A ReviewDocument16 pagesEvidence-Based Management of Postoperative Nausea and Vomiting: A ReviewYaclinNo ratings yet
- Relationship Between The Incidence and Risk Factors of Postoperative Nausea and Vomiting in Patients With Intravenous Patient-Controlled AnalgesiaDocument6 pagesRelationship Between The Incidence and Risk Factors of Postoperative Nausea and Vomiting in Patients With Intravenous Patient-Controlled AnalgesiaRandi KhampaiNo ratings yet
- 03 WeilbachDocument3 pages03 WeilbachAmalia Sholihah MukhtarNo ratings yet
- The Management of Postoperative Nausea and Vomiting in Elective Surgery Summary PointsDocument11 pagesThe Management of Postoperative Nausea and Vomiting in Elective Surgery Summary PointsRebecca PiggottNo ratings yet
- The Impact of The Apfel Scoring System For Prophylaxis ofDocument5 pagesThe Impact of The Apfel Scoring System For Prophylaxis ofKrish RendonNo ratings yet
- Nonoperating Room Anesthesia Anesthesia in The Gastrointestinal SuiteDocument16 pagesNonoperating Room Anesthesia Anesthesia in The Gastrointestinal SuiteGustavo ParedesNo ratings yet
- Joint Commission Sentinel Event Alert 8 8 12Document5 pagesJoint Commission Sentinel Event Alert 8 8 12api-244230664No ratings yet
- Week2 Submitter PaperDocument3 pagesWeek2 Submitter Paperapi-299189797No ratings yet
- Bourdaud2014 Pobk SkoruDocument8 pagesBourdaud2014 Pobk SkoruAli ÖzdemirNo ratings yet
- The Assessment of Risk Factors For Postoperative Nausea and VomitingDocument5 pagesThe Assessment of Risk Factors For Postoperative Nausea and VomitingWiedya KristiantiNo ratings yet
- 6887 25815 1 PB PDFDocument7 pages6887 25815 1 PB PDFmochkurniawanNo ratings yet
- Acta Anaesthesiologica Taiwanica: Editorial ViewDocument2 pagesActa Anaesthesiologica Taiwanica: Editorial ViewShuaib AhmedNo ratings yet
- Postoperative Nausea and Vomiting at A Tertiary Care Hospital in North-Western TanzaniaDocument9 pagesPostoperative Nausea and Vomiting at A Tertiary Care Hospital in North-Western TanzaniaAsfaw NurhussenNo ratings yet
- Clinical AuditDocument5 pagesClinical AuditdrskumarNo ratings yet
- Adult PONV and PDNV Process by ASCDocument2 pagesAdult PONV and PDNV Process by ASCHundalHarmanNo ratings yet
- 158 Nausea - Vomiting ScaleDocument9 pages158 Nausea - Vomiting ScaleMas Indra ShuNo ratings yet
- Emergency Physician Awareness of Prehospital ProceDocument8 pagesEmergency Physician Awareness of Prehospital ProceNines RíosNo ratings yet
- A Clinical Audit On Standards For Grading For Risk Assessment Prophylactic Management of Postoperative Nausea and VomitDocument5 pagesA Clinical Audit On Standards For Grading For Risk Assessment Prophylactic Management of Postoperative Nausea and VomitrameshNo ratings yet
- HSR2 5 E649Document9 pagesHSR2 5 E649Samsul BahriNo ratings yet
- Abstract and Introduction: Background: Gabapentinoids Are Widely Used in Perioperative MultimodalDocument22 pagesAbstract and Introduction: Background: Gabapentinoids Are Widely Used in Perioperative MultimodaldianNo ratings yet
- Curatolo2014 Reducing Medication Errors at Admission 3 Cycles To Implement, Improve and Sustain Medication Reconciliation PDFDocument8 pagesCuratolo2014 Reducing Medication Errors at Admission 3 Cycles To Implement, Improve and Sustain Medication Reconciliation PDFJennike ManuelNo ratings yet
- Impact of Pharmacist Interventions On Clinical Outcome and Cost Avoidance in A University Teaching HospitalDocument8 pagesImpact of Pharmacist Interventions On Clinical Outcome and Cost Avoidance in A University Teaching HospitalErick De La RosaNo ratings yet
- 7051N3M126Q411U7Document69 pages7051N3M126Q411U7naldihasibuanNo ratings yet
- Watcharapasorn 2016Document5 pagesWatcharapasorn 2016FranckNo ratings yet
- Post Operative Nausea and Vomiting, Its Causes, and The Way of Its Prevention and TreatmentDocument11 pagesPost Operative Nausea and Vomiting, Its Causes, and The Way of Its Prevention and TreatmentSurendra MaharjanNo ratings yet
- Prospective External Validation of A Predictive Score For Postoperative Pulmonary ComplicationDocument13 pagesProspective External Validation of A Predictive Score For Postoperative Pulmonary ComplicationAthziri GallardoNo ratings yet
- Journal Pre-Proof: International Journal of Medical InformaticsDocument29 pagesJournal Pre-Proof: International Journal of Medical InformaticsDityan KaleNo ratings yet
- Implementation and Function of Acute Pain Management Service: Aga Khan University Hospital ExperienceDocument3 pagesImplementation and Function of Acute Pain Management Service: Aga Khan University Hospital ExperienceMohammad HamidNo ratings yet
- Incidence, Characteristics, and Predictive Factors For Medication Errors in Paediatric Anaesthesia: A Prospective Incident Monitoring StudyDocument8 pagesIncidence, Characteristics, and Predictive Factors For Medication Errors in Paediatric Anaesthesia: A Prospective Incident Monitoring StudyShaikh ZarinNo ratings yet
- Adherence QuestionnaireDocument8 pagesAdherence QuestionnaireDhila FayaNo ratings yet
- PONV Prophylaxis GuidelinesDocument7 pagesPONV Prophylaxis GuidelinesAbby WardNo ratings yet
- Introduction To The Postanaesthetic Care Unit: Review Open AccessDocument7 pagesIntroduction To The Postanaesthetic Care Unit: Review Open AccessSamsul BahriNo ratings yet
- 2 Sba RaquiDocument9 pages2 Sba Raquijoanna medeirosNo ratings yet
- Research ArticleDocument8 pagesResearch ArticleafifahNo ratings yet
- Antiemetic Guideline Consistency and Incidence of Chemotherapy-Induced Nausea and Vomiting in US Community Oncology Practice: INSPIRE StudyDocument10 pagesAntiemetic Guideline Consistency and Incidence of Chemotherapy-Induced Nausea and Vomiting in US Community Oncology Practice: INSPIRE StudyKurnia AnharNo ratings yet
- Principles of Monitoring Postoperative Patients: Oleh: Meity Sarah 2012610108Document8 pagesPrinciples of Monitoring Postoperative Patients: Oleh: Meity Sarah 2012610108Jefry ArieNo ratings yet
- Prevalence, Risk Factors, and Optimized Management of Moderate To Severe Thirst in The Post Anesthesia Care UnitDocument10 pagesPrevalence, Risk Factors, and Optimized Management of Moderate To Severe Thirst in The Post Anesthesia Care Unitpooria shNo ratings yet
- BCP 14159Document12 pagesBCP 14159dentsavvyNo ratings yet
- 29th International Symposium On Intensive Care and Emergency MedicineDocument209 pages29th International Symposium On Intensive Care and Emergency MedicineYOGINo ratings yet
- Pan 13575Document2 pagesPan 13575Reynaldi HadiwijayaNo ratings yet
- 2014 Article 369Document6 pages2014 Article 369pebinscribdNo ratings yet
- Preventing Ventilator-Associated ICHEDocument8 pagesPreventing Ventilator-Associated ICHEFelix Brian FelixNo ratings yet
- Acta Anaesthesiologica Taiwanica: Research PaperDocument7 pagesActa Anaesthesiologica Taiwanica: Research PaperShuaib AhmedNo ratings yet
- PIIS0007091221004359Document7 pagesPIIS0007091221004359luisfernandoamaya89No ratings yet
- Paper Reintubación Variable Sexo y EdadDocument5 pagesPaper Reintubación Variable Sexo y EdadAres Kinesiology TapeNo ratings yet
- Asa 2013Document1,076 pagesAsa 2013Marwa Mahrous100% (4)
- Research Paper On Ventilator Associated PneumoniaDocument8 pagesResearch Paper On Ventilator Associated PneumoniakwbfbzundNo ratings yet
- Fournel 2020Document9 pagesFournel 2020tim yuNo ratings yet
- 747-Article Text-1365-1-10-20200430Document6 pages747-Article Text-1365-1-10-20200430Yogita DhurandharNo ratings yet
- Perioperative Point of Care Ultrasound From Concept To ApplicationDocument9 pagesPerioperative Point of Care Ultrasound From Concept To Applicationzumbidoslema0qNo ratings yet
- The Preparation and Administration of Intravenous Drugs Before and After Protocol ImplementationDocument8 pagesThe Preparation and Administration of Intravenous Drugs Before and After Protocol ImplementationIvanCompeanVazquezNo ratings yet
- Ade Et AlDocument7 pagesAde Et Alkang.asep008No ratings yet
- Fiorino2000 PDFDocument11 pagesFiorino2000 PDFDiego Antonio Rodriguez CoronadoNo ratings yet
- Dyspnea ProjectDocument20 pagesDyspnea Projectfarah.abd97No ratings yet
- Predicting Weaning and Extubation Outcomes in Long-Term Mechanically Ventilated Patients Using The Modified Burns Wean Assessment Program ScoresDocument7 pagesPredicting Weaning and Extubation Outcomes in Long-Term Mechanically Ventilated Patients Using The Modified Burns Wean Assessment Program ScoresClaudia IsabelNo ratings yet
- Prevention of VAP Use For Bundle Approach 10.1016@j.ajic.2016.04.237Document4 pagesPrevention of VAP Use For Bundle Approach 10.1016@j.ajic.2016.04.237sarintiNo ratings yet
- Journa Generall AneshesiaDocument7 pagesJourna Generall AneshesiaNadya NovianiNo ratings yet
- Payment Instructions For Docs RequestedDocument1 pagePayment Instructions For Docs RequestedElaine IllescasNo ratings yet
- EPM BookmarkDocument2 pagesEPM BookmarkElaine IllescasNo ratings yet
- Outpatient Cheat CodeDocument18 pagesOutpatient Cheat CodeElaine IllescasNo ratings yet
- PAINAD ScaleDocument2 pagesPAINAD ScaleElaine IllescasNo ratings yet
- Functional Actvity ScaleDocument1 pageFunctional Actvity ScaleElaine IllescasNo ratings yet
- Complications After Thigh Sarcoma ResectionDocument7 pagesComplications After Thigh Sarcoma ResectionElaine IllescasNo ratings yet
- CNB Vs IncisionDocument12 pagesCNB Vs IncisionElaine IllescasNo ratings yet
- A Case of Recurrent Mesocolon Myxoid Liposarcoma and Review of The LiteratureDocument7 pagesA Case of Recurrent Mesocolon Myxoid Liposarcoma and Review of The LiteratureElaine IllescasNo ratings yet
- Dinardo 2018Document7 pagesDinardo 2018Elaine IllescasNo ratings yet
- Ni Hms 690786Document17 pagesNi Hms 690786Elaine IllescasNo ratings yet
- Mansoor 2017Document36 pagesMansoor 2017Elaine IllescasNo ratings yet
- AJCC 8th STSDocument5 pagesAJCC 8th STSElaine IllescasNo ratings yet
- BPG Assessment of PainDocument147 pagesBPG Assessment of PainFarah ShamsudinNo ratings yet
- Patient-Centered Care and AdherenceDocument8 pagesPatient-Centered Care and AdherencethinkercolNo ratings yet
- Periodontal Considerations: Presented By: Layan Suleiman Supervisor: Dr. Mohammad AL-Rabab'ahDocument33 pagesPeriodontal Considerations: Presented By: Layan Suleiman Supervisor: Dr. Mohammad AL-Rabab'ahasop06No ratings yet
- Prenatal Care Common Discomforts During PregnancyDocument5 pagesPrenatal Care Common Discomforts During PregnancyKarina MadriagaNo ratings yet
- GastricDocument142 pagesGastricMore MorenoNo ratings yet
- PNPK PNPKDocument3 pagesPNPK PNPKPutri JunitasariNo ratings yet
- Sel ListDocument66 pagesSel Listcharuhans nandgaonkarNo ratings yet
- Reference LetterDocument2 pagesReference Letterapi-400249790No ratings yet
- Laboratorio Clinico Toledo: Patient Number Birthdate SexDocument1 pageLaboratorio Clinico Toledo: Patient Number Birthdate SexMirle BonetNo ratings yet
- DS-10249 ACLS PI Sheet 03ts PDFDocument1 pageDS-10249 ACLS PI Sheet 03ts PDFAsrini Rizky NasutionNo ratings yet
- Hmhub: Food SafetyDocument5 pagesHmhub: Food SafetyJonathan LabutapNo ratings yet
- Embedding AcupunctureDocument5 pagesEmbedding AcupunctureAngela PagliusoNo ratings yet
- NiceDocument45 pagesNiceKenneth Mark B. TevesNo ratings yet
- Republic of The Philippines Tamag, Vigan City 2700 Ilocos Sur Website: MailDocument2 pagesRepublic of The Philippines Tamag, Vigan City 2700 Ilocos Sur Website: MailRenea Joy ArruejoNo ratings yet
- Survival of Atraumatic Restorative Treatment (ART) Sealants and Restorations: A Meta-AnalysisDocument15 pagesSurvival of Atraumatic Restorative Treatment (ART) Sealants and Restorations: A Meta-AnalysisestefaniaNo ratings yet
- Enteral Nutrition of Preterm BabyDocument54 pagesEnteral Nutrition of Preterm Babylordoftheweb100% (5)
- Jurnal Teledentistry 1Document7 pagesJurnal Teledentistry 1Dio Nella ArlinggaNo ratings yet
- Piedmont Medical Center RulingDocument40 pagesPiedmont Medical Center RulingHLMeditNo ratings yet
- Anomalies DentinDocument19 pagesAnomalies DentinHaffie HafiziNo ratings yet
- Leaflet Covid 19 - Pregnant Women PDFDocument2 pagesLeaflet Covid 19 - Pregnant Women PDFBindar AdrianNo ratings yet
- Abdominal Pain A Synthesis of Recommendations ForDocument11 pagesAbdominal Pain A Synthesis of Recommendations Forsakinah mawadahNo ratings yet
- Pregnancy ComplicationsDocument11 pagesPregnancy ComplicationsJosé David Cortez Centeno 20190155No ratings yet
- Diagnosis Short Term Goals Long Term Goals Nursing InterventionsDocument4 pagesDiagnosis Short Term Goals Long Term Goals Nursing Interventionsdanny_ng08100% (9)
- Test Bank For Porth Pathophysiology Concepts of Altered Health States 1st Canadian Edition HannonDocument15 pagesTest Bank For Porth Pathophysiology Concepts of Altered Health States 1st Canadian Edition Hannonuncapepais16614100% (50)
- 13 Lombe Mumba Ramson 2017 Knowledge Attitude and Practice of Breast Self Examination For Early Detectoin of Breast Cancer Among Women in Roan Constituency in Luanshya Copperbelt Province ZambiaDocument9 pages13 Lombe Mumba Ramson 2017 Knowledge Attitude and Practice of Breast Self Examination For Early Detectoin of Breast Cancer Among Women in Roan Constituency in Luanshya Copperbelt Province ZambiaArick Frendi AndriyanNo ratings yet
- Zygomatic ImplantsDocument3 pagesZygomatic ImplantsDeb SNo ratings yet
Moore R
Moore R
Uploaded by
Elaine IllescasOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Moore R
Moore R
Uploaded by
Elaine IllescasCopyright:
Available Formats
Preventing Postoperative Nausea and Vomiting
During an Ondansetron Shortage
CDR Chad Moore, DNP, CRNA, CHSE, NC, USN
LT Rusty Bledsoe, DNP, CRNA
CDR Raymond Bonds, DNP, CRNA, NEA-BC, CHSE, NC, USN
Margaux Keller, PhD
CAPT Heather King, PhD, CRNA, NC, USN
Postoperative nausea and vomiting (PONV) degrades ondansetron, the most common antiemetic at base-
patient experience and increases healthcare costs. line, was not available in the early postimplementa-
Estimates of PONV range from 10% to 80%. The Apfel tion period, which may partially explain the initial
Simplified Score is an evidence-based instrument for increase in PONV. While ondansetron was unavail-
determining individual risk of PONV. Scoring enables able, providers began using 3 other antiemetics, a
anesthesia providers to match antiemetic strategies practice that persisted once intravenous ondansetron
with the calculated risk of PONV. Data were collected returned. The Apfel score is an evidence-based tool
across 3 times. After the Apfel scoring system was that providers can use to reduce the risk of PONV.
automated into the electronic medical record, provid- This electronic tool and the reminder cards have been
ers were more likely to increase PONV prophylaxis shared across the US Military Health System, foster-
for patients at highest risk and reduce prophylaxis ing an organizational culture that values targeted
for patients at lowest risk. Rates of PONV remained prophylaxis for PONV.
similar at baseline (34.7%) and in the early post-
implementation period (38.8%); a modest reduction Keywords: Acupuncture, medication shortage, PONV,
was observed in the final period (26.5%). Intravenous postoperative nausea and vomiting.
P
ostoperative nausea and vomiting (PONV) rep- that providers will change their antiemetic prophylaxis
resents a substantial physical and financial bur- strategy after receiving education on the Apfel score.5,6
den to patients and healthcare systems. In the Therefore, the use of educational sessions to instruct
US Military Health System, patients with PONV healthcare personnel on the correct use of the Apfel
stay longer and consume more services imme- Simplified Score is important when implementing this
diately after surgery than those without PONV.1 As many practice change. The electronic medical record (EMR) is
as 1 in 3 patients experience PONV, but this unaccept- a readily accessible medium to encourage the use of the
ably high rate can be reduced by matching prophylaxis to Apfel score, and EMR-based reminders have been shown
expected risk. to increase adherence to PONV prophylaxis guidelines.7-9
Widely used in research, the Apfel Simplified Score Such reminders should be enduring, since adherence to
is a validated tool to evaluate risk of PONV. Using 4 in- guidelines and PONV rates return to preimplementation
dependent risk factors—female sex, nonsmoking status, levels when these tools are withdrawn.8,9
history of PONV or motion sickness, and postoperative The addition of an enduring PONV scoring tool and
opioid use—the score is easy for providers to remember training of providers to include evidence when making
and calculate at the bedside. Each of these risk factors clinical decisions will benefit the military healthcare
adds 20% risk of PONV, with the baseline risk never less system and the patients it serves. Training staff is ex-
than 10%; 0, 1, 2, 3, and 4 factors correspond to 10%, pected to produce measurable effects at the facility level,
20%, 40%, 60%, and 80% risk, respectively. Notably, in terms of PONV risk reduction and staff adherence to
the maximum predictable risk is 80%. Each preventive guidelines for PONV prevention. Military staff frequently
treatment can reduce the risk of PONV by approximately relocate, so these interventions should be compatible for
26%.2,3 Targeting high-risk patients with preventive use at any military location to provide for true sustain-
measures also avoids medication overuse.4 Considering ment. We hypothesized that implementing the Apfel
the high frequency of medication shortages in modern scoring system would result in the reduction of PONV
practice, using the right medication for the right patient for patients at Naval Hospital Jacksonville in Florida and
is increasingly important. simultaneously improve medication practices as provid-
Results of previous investigations have demonstrated ers adhere to the guidelines for PONV prevention.
www.aana.com/aanajournalonline AANA Journal April 2021 Vol. 89, No. 2 161
Methods
Postoperative nausea and vomiting are an identified
clinical problem, and education sessions are an impera-
tive aspect of effecting practice change. Formal provider
training sessions on the correct use of the Apfel Simplified
Score occurred in-person for postanesthesia care unit
(PACU) nurses and anesthesia practitioners. These ses-
sions took place in a classroom setting at the Naval
Hospital Jacksonville over 1 hour. In this training, the
local problem of PONV was described, and the following
project interventions were introduced: an EMR-based
PONV risk scoring tool and a PONV algorithm reminder
card (Figure 1). A video-based demonstration showed Figure 1. Reminder Card With Recommendations
anesthesia providers how to use the algorithm for PONV Placed at each Anesthesia Station
prophylaxis. Written knowledge assessments for attend- Abbreviations: Hx, history; IM, intramuscularly; IV, intravenously;
PO, orally; PONV, postoperative nausea and vomiting; postop,
ees were conducted before and after each presentation to
postoperative; pre-op, preoperatively; TD, transdermally; TIVA,
measure how well the information was captured by the total intravenous anesthesia.
attendees. Recovery room nurses were trained separately (Adapted from Gan et al.2,4)
and were instructed to request PONV risk determination
during postanesthesia handoffs. The training gave attend- the recovery room had not yet started, so practitioners
ees the knowledge required to use the project interven- were asked to provide opioid use estimates for their own
tions, which were developed and fully implemented on past cases retroactively. In these cases, the anesthesia pro-
the project start day, after training was complete. vider was also responsible for writing the postoperative
• Interventions Provided at Initial Rollout. The EMR- PACU orders, so this individual would be the person most
based risk scoring tool was integrated into all preanes- capable of predicting whether opioid medications would
thetic assessments and allowed for the assignment of low, be ordered. These estimates were based on limited infor-
moderate, or high risk of PONV. Low risk was defined mation about the case: age, gender, type of surgery, and
as an Apfel score of 0 to1, medium risk was defined as type of anesthesia. Cases were assigned an estimate only
an Apfel score of 2, and high risk was defined as an when the original anesthesia practitioner was available
Apfel score of 3 or greater. These scores correspond to to comment and denied knowledge of any postoperative
the number of antiemetic interventions a patient should opioids administered.
receive. Reminder cards were distributed to anesthe- • Data Collection. Cases were collected from the 5
sia providers to match a patient’s calculated risk with highest-volume surgical services at the facility: orthope-
the appropriate prophylaxis, and cards were affixed to dics, gynecology, general surgery, urology, and otolaryn-
each anesthesia machine and preoperative terminal. gology. In these 5 surgical services, additional inclusion
Interventions were selected based on existing guidelines criteria were applied to nonemergent cases undergoing
for PONV management.4 In an effort to induce a sustain- general anesthesia. Only patients aged 18 to 89 years and
able practice change, these cards included medications scoring between 1 and 3 on the ASA physical classification
that were routinely available and regularly stocked by the system were included. Cases were excluded if they were
hospital pharmacy. outside the 5 highest-volume surgical services, were emer-
• Preimplementation Risk Factor Scoring. Postoperative gencies, used exclusively regional anesthesia or monitored
nausea and vomiting was defined as nausea or vomiting anesthesia care, were in pregnant women, or indicated the
experienced by patient while in the recovery room and presence of nausea on the preanesthetic evaluation.
was scored as an all or none entity. In cases in which Data were collected over 3 periods: baseline (phase 0),
PONV was present, the length and severity of nausea early phase (phase 1), and final phase (phase 2). Baseline
and vomiting were not separately measured. To measure data included cases occurring before provider training
the effectiveness of training, the project team performed took place. Baseline data collection was conducted until
a retrospective chart review to collect data from surgical 30 records per surgical service were collected, working
cases that occurred before training, a period referred to as backward from the project start date, before training.
baseline. For each baseline case, an observed Apfel score The early phase of data collection included cases occur-
was assigned using the following criteria: anticipated ring after training, and data collection continued until 30
postoperative opioids administered in the recovery room, records per surgical service were obtained, approximately
patient history of PONV or motion sickness drawn from 4 months after the initial provider training and project
the preoperative assessment, female sex, and nonsmoking start date. Following baseline and early-phase data collec-
status. Notably, the practice of predicting opioid use in tion and preliminary analysis, a follow-up provider train-
162 AANA Journal April 2021 Vol. 89, No. 2 www.aana.com/aanajournalonline
Phasea Apfel score Guidelines followed, % Guidelines not followed, % N
0-2 0 37.5 62.5 16
1 53.04 46.96 115
2 60.27 39.73 146
3 72.29 27.71 83
4 80.0 20.0 5
0 0 0 100.0 2
1 26.92 73.08 26
2 54.05 45.95 37
3 82.35 17.65 17
4 100.0 0 1
1 0 50.0 50.0 8
1 59.57 40.43 47
2 74.42 25.58 43
3 76.92 23.08 26
4 0 100.0 1
2 0 33.33 66.67 6
1 61.9 38.1 42
2 54.55 45.45 66
3 65.0 35.0 40
4 100.0 0 3
Table 1. Provider Adherence to Guidelines Across Project Phases 0 to 2
aPhase 0 = preintervention baseline; phase 1 = early phase (approximately first 4 months after intervention); phase 2, final phase
(approximately months 4-8 after intervention).
ing was held to update attendees on the project’s status. A
knowledge assessment was administered before and after
this training, and initial results were presented to provid-
ers at this time. Following the provider update, final-
phase data collection began until another 30 records per
service were collected, approximately 8 months after the
project start date.
Provider adherence was determined by reviewing the
antiemetic medications administered in each case, for
which each patient had been categorized as having low,
moderate, or high risk of PONV according to his or her
Apfel score, and then classifying each case as “adherent” or Figure 2. Percentage of Patients Experiencing PONV in
“not adherent” with the evidence-based recommendations Each Apfel Score Category, Across Phases 0 to 2
that were introduced during training. Appropriately treated Abbreviation: PONV, postoperative nausea and vomiting.
patients were those who were given the recommended
number of antiemetics corresponding to their Apfel score. receiving 3 or more (see Figure 1). These interventions
Rates of PONV were derived from recovery room were considered of equal efficacy for the treatment of
nursing records. The incidence of PONV was described nausea and vomiting, and their administration was deter-
as the presence or absence of PONV in the recovery mined solely by the provider. Other data points included
room. Patients needed only to report a single occurrence risk factors within the Apfel score. These data were used
of nausea or vomiting to experience PONV; the duration to make between-group comparisons.
and severity of symptoms were not further considered. • Statistical Analysis. The following primary outcomes
Secondary data included the administration of pro- were measured: provider adherence to the guidelines (cat-
phylactic antiemetic interventions, including haloperi- egories: adherence and nonadherence) and incidence of
dol, promethazine, aprepitant, scopolamine, total intra- PONV (categories: presence or absence). Data were further
venous (IV) anesthesia, ondansetron, dexamethasone, categorized by phase to include baseline, early, and final
and acupressure. In accordance with the guidelines, the subsets. Significance for categorical data was determined
number of interventions is based on risk, with low-risk using χ2 tests. An α value of .05 was considered significant,
patients receiving no interventions and high-risk patients suggesting an association between the categorical variables
www.aana.com/aanajournalonline AANA Journal April 2021 Vol. 89, No. 2 163
Figure 3. Number of Antiemetics Administered in Each Phase
Abbreviations: IV, intravenous; PO, orally; TIVA, total intravenous anesthesia.
aNationwide shortage of IV ondansetron (preferred medication in baseline/phase 0) is reflected in absence of this medication during phase 1.
measured. Odds ratios (ORs) with confidence intervals PONV risk Phase 0 Phase 1 Phase 2
were used to further measure the strength of association. Low (Apfel score 0-1) 1.5 0.5 1.4
The project was deemed exempt by the Navy Medicine Moderate (Apfel score 2) 1.5 1.2 1.2
East institutional review board designee. Analysis was per-
High (Apfel score ≥3) 1.9 1.5 2.0
formed with the Statistical Package for the Social Sciences
(SPSS) version 22.0 for Mac (IBM Corp). Table 2. Mean Number of Antiemetics Administered
During Each Phase
Results Abbreviation: PONV, postoperative nausea and vomiting.
• Provider Adherence. Chi-squared tests were used to de-
termine association between provider adherence and the of baseline cases, 67% of early cases, and 59% of final
3 phases of data collection. A significant association was cases were appropriately medicated (P=.006).
found between the baseline and early phases (P=.002). • Antiemetic Interventions. There were 9 interventions
Provider adherence significantly improved between these tracked across each phase: haloperidol, promethazine,
2 phases (OR=2.31, 95% CI=1.33-4.04). Provider adher- aprepitant, scopolamine, total IV anesthesia, IV ondan-
ence was sustained in the final phase, with a nonsignifi- setron, oral ondansetron, dexamethasone, and acupres-
cant decrease in adherence between the early and final sure, and all were used except acupressure (Figure
phases (P=.17, OR=0.71, 95% CI=0.42-1.19). 3). Ondansetron and dexamethasone were the most
• Rates of Postoperative Nausea and Vomiting. Most commonly administered antiemetics across all periods.
patients scored in Apfel categories 1 to 3 (Table 1). Intravenous ondansetron and IV dexamethasone were
Patients with higher Apfel scores experienced higher the only interventions regularly administered in the
rates of PONV in the recovery room (Figure 2). The inci- baseline group. Intravenous ondansetron was unavailable
dence of PONV was 34.7% at baseline, 38.8% in the early for entire time captured by the early phase, because of a
phase, and 26.5% in the final phase. There were no sig- nationwide shortage that persisted for several months.
nificant differences in PONV rates between the baseline An equipotent dose of oral ondansetron (8 mg) had been
and final phase (P=.31, OR=1.18, 95% CI=0.59-2.33) or listed as an alternative to IV ondansetron (4 mg) for both
between the early and final phase (P=.13, OR=1.60, 95% the early and final phases. During the final phase, IV
CI=0.84-3.07). In appropriately treated patients, rates ondansetron became available again but was not admin-
of PONV were lower in the final phase compared with istered as frequently as it had been in the baseline group.
the early phase (P=.044, OR=2.13, 95% CI=0.95-4.85). Oral ondansetron was listed only as a substitute for IV
Furthermore, following the initial training, the propor- ondansetron, and no patients received a combination of
tion of appropriately medicated patients increased; 47% oral and IV ondansetron.
164 AANA Journal April 2021 Vol. 89, No. 2 www.aana.com/aanajournalonline
Figure 4. Number of Antiemetics Administered to Patients in Each Apfel Category, at Baseline
Figure 5. Number of Antiemetics Administered to Patients in Each Apfel Category, in Early Phase
Patients with 0 or 1 risk factors, which translates to a ics. Patients at moderate risk of PONV were more likely
0 or 1 Apfel score, are at lowest risk of PONV. The guide- to receive 2 antiemetics at baseline and 1 antiemetic in
lines suggest these patients may receive no antiemetics. either the early or final phase (see Table 2; Figures 4-6).
Antiemetic prophylaxis for these patients decreased Patients with 3 or more risk factors are at the highest
overall (Table 2; Figures 4-6). Low-risk patients received risk of PONV, and the guidelines indicate these patients
the greatest mean quantity of antiemetic interventions at should receive 3 or more antiemetics. However, at
baseline (1.5), the fewest during the early phase (0.5), baseline, none of the patients with an Apfel score of 3
with a near return to baseline in the final phase (1.4). received 3 or more antiemetics, and they received a mean
Patients with 2 risk factors, and given an Apfel score of only 1.9 antiemetics (see Figure 4). In the early phase,
of 2, are at moderate risk of PONV. The guidelines nearly one-third of high-risk patients received 3 or more
suggest these patients should receive 1 to 2 antiemet- antiemetics (see Figure 5). By the final phase, antiemetic
ics, and across phases, most study participants did. At prophylaxis for these patients had increased to an average
baseline, moderate-risk patients received an average of of 2.0 antiemetics (see Table 2), but nearly half of these
1.5 antiemetics. In the early and final phases, these pa- high-risk patients had received 3 or more antiemetics
tients received slightly less, an average of 1.2 antiemet- (see Figure 6).
www.aana.com/aanajournalonline AANA Journal April 2021 Vol. 89, No. 2 165
Figure 6. Number of Antiemetics Administered to Patients in Each Apfel Category, in Final Phase
Discussion influenced provider estimations. Despite this observa-
The Apfel score is useful for predicting the risk of PONV, tion, the Apfel score continues to be a valid preoperative
and when prophylaxis guidelines are followed, rates of screening tool for estimating the risk of PONV.4,6
PONV tend to decrease. This project made the guide- A common hurdle for providers and hospitals is the
lines and the risk factor scoring readily available and uncertain availability of effective antiemetics. A nation-
demonstrated that provider adherence to the guidelines wide ondansetron shortage coincided with the beginning
increased after implementation. A reduction of PONV in- of the early phase, immediately after implementation,
cidence was seen when comparing baseline with the final which clearly affected the administration of antiemetics
phase, a clinically significant finding that did not reach during this time. Ondansetron was available again during
statistical significance. The multiple points of reference the final phase. Dexamethasone was intermittently avail-
to the Apfel tool may have improved the practitioners’ able during the final phase, but present for most op-
willingness to integrate the tool into their treatment erative cases collected during this period. Small lapses
plans. in availability may have created data artifacts regarding
Since PONV is known to increase facility costs, preven- prescribing habits.
tion of PONV correspondingly results in less expense for In the baseline group, before the EMR-based risk
the hospital.1 Permanent integration of the Apfel tool into scoring tool was integrated into all preanesthetic assess-
the EMR should predictably reduce facility costs through ments, prophylaxis was often administered for patients
this mechanism. This project demonstrated that these at lowest risk of PONV (Apfel categories 0-1). Following
combined points of reference contributed to appropriate training and the commencement of automatic risk cal-
provider adherence, but it is unknown if the card or the culation, providers were more likely to match calculated
EMR-based tool was independently effective in achieving risk with the recommendations, such as no prophylaxis
this goal. Future projects may look to examine the utility of for patients at lowest risk (see Table 1).
a reminder card with or without an EMR-based tool. Also of Most patients included in this project were at moder-
note, providers were taught to use their own preoperative ate risk of PONV, and across all phases, these patients
estimation of whether the patient would require postopera- most often received 1 to 2 antiemetics. At baseline, most
tive opioid use, as part of a commonly employed predictive of these moderate risk patients received 2 antiemetics,
scoring system recommended by current guidelines.4 but in the early and final phases, most received only
The accuracy of personal predictions on whether 1 antiemetic. This may be attributable to the ondanse-
opioids will be used is a valid consideration.5 As part of tron shortage that occurred during the early phase. It
the training given to providers, expected length of surgery is conceivable that some providers would prefer to give
was suggested as a consideration when making these pre- less medication rather than introduce a new medication
dictions. Longer surgeries are associated with more opioid during a shortage, especially when still within the recom-
use, but this factor is not considered an independent sub- mended range of 1 to 2 antiemetics.
stitute for the opioid prediction within the Apfel score.4,5 Perhaps of greatest clinical significance, there was an
It is unknown to what extent this suggestion may have increase in the use of other antiemetics during the early
166 AANA Journal April 2021 Vol. 89, No. 2 www.aana.com/aanajournalonline
phase, including haloperidol, promethazine, aprepitant, 1504. doi:10.1213/ane.0b013e31819e431f
and scopolamine. These medications were not used at all 4. Gan TJ, Diemunsch P, Habib AS, et al. Consensus guidelines for the
management of postoperative nausea and vomiting. Anesth Analg.
at baseline. The guidelines introduced these medications 2014;118(1):85-113. doi:10.1213/ANE.0000000000000002
as additional strategies to prevent PONV, and provided 5. Apfel CC, Läärä E, Koivuranta M, Greim CA, Roewer N. A simplified
a useful algorithm to follow when medication shortages risk score for predicting postoperative nausea and vomiting: conclu-
inevitably occur. In the final phase, providers continued sions from cross-validations between two centers. Anesthesiology.
1999;91(3):693-700. doi:10.1097/00000542-199909000-00022
this trend by choosing a variety of antiemetic strategies
6. Sigaut S, Merckx P, Peuch C, Necib S, Pingeon F, Mantz J. Does an
from the list, even after IV ondansetron had returned. educational strategy based on systematic preoperative assessment of
Thus, the practice of giving 2 antiemetics regardless of simplified Apfel’s score decrease postoperative nausea and vomit-
risk changed to reflect a more targeted risk reduction ing? Ann Fr Anesth Reanim. 2010;29(11):765-769. doi:10.1016/j.
annfar.2010.08.004
strategy, and this effect was sustained at 8 months.
7. Kooij FO, Vos N, Siebenga P, Klok T, Hollmann MW, Kal JE. Auto-
As an evidence-based practice improvement initia- mated reminders decrease postoperative nausea and vomiting inci-
tive, this project was successful in its endeavor to change dence in a general surgical population. Br J Anaesth. 2012;108(6):961-
practitioner habits related to PONV prophylaxis at Naval 965. doi:10.1093/bja/aes024
Hospital Jacksonville. As such it can serve as a model for 8. Kooij FO, Klok T, Hollmann MW, Kal JE. Decision support increases
guideline adherence for prescribing postoperative nausea and vomit-
other facilities to follow to implement similar initiatives. ing prophylaxis. Anesth Analg. 2008;106(3):893-898. doi:10.1213/
This project included instances of PONV that occurred ane.0b013e31816194fb
immediately following surgery, in the PACU. Many pa- 9. Kooij FO, Klok T, Hollmann MW, Kal JE. Automated reminders
tients experience PONV within 24 hours of surgery and increase adherence to guidelines for administration of prophylaxis for
postoperative nausea and vomiting. Eur J Anaesthesiol. 2010;27(2):187-
would not be captured here. Patients at highest risk of 191. doi:10.1097/EJA.0b013e32832d6a76
PONV were seldom included in the analysis. No patients
in the highest category, Apfel 4, were included in base- AUTHORS
line or the early phases, as no such records met inclusion CDR Chad Moore, DNP, CRNA, CHSE, NC, USN, is the clinical site
criteria during the period of data collection. Following director for the Uniformed Services University (USU) Nurse Anesthesia
a normal distribution curve, with the fewest patients in Program, Jacksonville, Florida. Email: chad.moore@usuhs.edu.
categories 0 and 4, a much larger sample size would be LT Rusty Bledsoe, DNP, CRNA, is a staff nurse anesthetist at US Naval
Hospital, Okinawa, Japan.
needed to examine the impact on patients with either the
CDR Raymond Bonds, DNP, CRNA, NEA-BC, CHSE, NC, USN, is
lowest or the highest risk of PONV. the director for surgical services at Naval Hospital Beaufort and adjunct
faculty for the Registered Nurse Anesthesia Program at Uniformed Services
Conclusion University.
The Apfel score was successfully implemented into the Margaux Keller, PhD, is a research coordinator with the Henry M.
Jackson Foundation for the Advancement of Military Medicine, Bethesda,
EMR, resulting in significantly increased provider adher-
Maryland. Email: margaux.keller.ctr@usuhs.edu.
ence, but only a slight decrease in PONV. This project
CAPT Heather King, PhD, CRNA, NC, USN, is the executive director
and its associated tools have been shared throughout of the TriService Nursing Research Program, Bethesda, Maryland.
the Military Health System. Since the next generation
of military EMR has the capability to determine the DISCLOSURES
risk of PONV, there is an opportunity for systemwide The authors have declared no financial relationships with any commercial
sustainment. During the next several years the EMR entity related to the content of this article. The authors did not discuss
off-label use within the article. Disclosure statements are available for
is implemented, this project will serve as an introduc-
viewing upon request.
tory springboard to ensuring patients are given effective
PONV prevention. As these findings have been shared
ACKNOWLEDGMENTS
with operational military medical personnel, patients in The authors would like to thank the Tri-Service Nursing Research Program
deployed or isolated settings are expected to experience for providing funding for this project. Guidelines for PONV management
the same high level of care in PONV prevention as their changed after this project was completed. An updated version of Figure 1
is available at shorturl.at/jruJV.
counterparts in the continental United States.
REFERENCES MILITARY DISCLAIMER
1. Moore CB, Hickey AH. Increasing access to auricular acupuncture for The views expressed in this article reflect the results of research conducted
postoperative nausea and vomiting. J Perianesth Nurs. 2017;32(2):96- by the authors and do not necessarily reflect the official policy or position
105. doi:10.1016/j.jopan.2015.06.006 of the Department of the Navy, Department of Defense, nor the United
2. Apfel CC, Korttila K, Abdalla M, et al. A factorial trial of six interven- States Government.
tions for the prevention of postoperative nausea and vomiting. N Engl We are military service members. This work was prepared as part of
J Med. 2004;350(24):2441-2451. doi:10.1056/NEJMoa032196 our official duties. Title 17 U.S.C. 105 provides that “Copyright protection
3. Gan TJ, Sinha AC, Kovac AL, et al. A randomized, double-blind, mul- under this title is not available for any work of the United States Govern-
ticenter trial comparing transdermal scopolamine plus ondansetron ment.” Title 17 U.S.C. 101 defines United States Government work as a
to ondansetron alone for the prevention of postoperative nausea and work prepared by a military service member or employee of the United
vomiting in the outpatient setting. Anesth Analg. 2009;108(5):1498- States Government as part of that person’ s official duties.
www.aana.com/aanajournalonline AANA Journal April 2021 Vol. 89, No. 2 167
You might also like
- Oral Manifestations of Systemic DiseasesDocument11 pagesOral Manifestations of Systemic DiseasesMezo Salah100% (2)
- Risk Assessment TemplateDocument3 pagesRisk Assessment TemplateGus VanGeijtenbeekNo ratings yet
- Postoperative Nausea and VomitingDocument33 pagesPostoperative Nausea and Vomitingferlina100% (1)
- Hospital SWOT AnalysisDocument2 pagesHospital SWOT AnalysisKenny Josef96% (26)
- Thailand Traditions and BeliefsDocument6 pagesThailand Traditions and Beliefsapi-316342033100% (1)
- Out 9Document12 pagesOut 9rezkyprayogiNo ratings yet
- Evidence-Based Management of Postoperative Nausea and Vomiting: A ReviewDocument16 pagesEvidence-Based Management of Postoperative Nausea and Vomiting: A ReviewYaclinNo ratings yet
- Relationship Between The Incidence and Risk Factors of Postoperative Nausea and Vomiting in Patients With Intravenous Patient-Controlled AnalgesiaDocument6 pagesRelationship Between The Incidence and Risk Factors of Postoperative Nausea and Vomiting in Patients With Intravenous Patient-Controlled AnalgesiaRandi KhampaiNo ratings yet
- 03 WeilbachDocument3 pages03 WeilbachAmalia Sholihah MukhtarNo ratings yet
- The Management of Postoperative Nausea and Vomiting in Elective Surgery Summary PointsDocument11 pagesThe Management of Postoperative Nausea and Vomiting in Elective Surgery Summary PointsRebecca PiggottNo ratings yet
- The Impact of The Apfel Scoring System For Prophylaxis ofDocument5 pagesThe Impact of The Apfel Scoring System For Prophylaxis ofKrish RendonNo ratings yet
- Nonoperating Room Anesthesia Anesthesia in The Gastrointestinal SuiteDocument16 pagesNonoperating Room Anesthesia Anesthesia in The Gastrointestinal SuiteGustavo ParedesNo ratings yet
- Joint Commission Sentinel Event Alert 8 8 12Document5 pagesJoint Commission Sentinel Event Alert 8 8 12api-244230664No ratings yet
- Week2 Submitter PaperDocument3 pagesWeek2 Submitter Paperapi-299189797No ratings yet
- Bourdaud2014 Pobk SkoruDocument8 pagesBourdaud2014 Pobk SkoruAli ÖzdemirNo ratings yet
- The Assessment of Risk Factors For Postoperative Nausea and VomitingDocument5 pagesThe Assessment of Risk Factors For Postoperative Nausea and VomitingWiedya KristiantiNo ratings yet
- 6887 25815 1 PB PDFDocument7 pages6887 25815 1 PB PDFmochkurniawanNo ratings yet
- Acta Anaesthesiologica Taiwanica: Editorial ViewDocument2 pagesActa Anaesthesiologica Taiwanica: Editorial ViewShuaib AhmedNo ratings yet
- Postoperative Nausea and Vomiting at A Tertiary Care Hospital in North-Western TanzaniaDocument9 pagesPostoperative Nausea and Vomiting at A Tertiary Care Hospital in North-Western TanzaniaAsfaw NurhussenNo ratings yet
- Clinical AuditDocument5 pagesClinical AuditdrskumarNo ratings yet
- Adult PONV and PDNV Process by ASCDocument2 pagesAdult PONV and PDNV Process by ASCHundalHarmanNo ratings yet
- 158 Nausea - Vomiting ScaleDocument9 pages158 Nausea - Vomiting ScaleMas Indra ShuNo ratings yet
- Emergency Physician Awareness of Prehospital ProceDocument8 pagesEmergency Physician Awareness of Prehospital ProceNines RíosNo ratings yet
- A Clinical Audit On Standards For Grading For Risk Assessment Prophylactic Management of Postoperative Nausea and VomitDocument5 pagesA Clinical Audit On Standards For Grading For Risk Assessment Prophylactic Management of Postoperative Nausea and VomitrameshNo ratings yet
- HSR2 5 E649Document9 pagesHSR2 5 E649Samsul BahriNo ratings yet
- Abstract and Introduction: Background: Gabapentinoids Are Widely Used in Perioperative MultimodalDocument22 pagesAbstract and Introduction: Background: Gabapentinoids Are Widely Used in Perioperative MultimodaldianNo ratings yet
- Curatolo2014 Reducing Medication Errors at Admission 3 Cycles To Implement, Improve and Sustain Medication Reconciliation PDFDocument8 pagesCuratolo2014 Reducing Medication Errors at Admission 3 Cycles To Implement, Improve and Sustain Medication Reconciliation PDFJennike ManuelNo ratings yet
- Impact of Pharmacist Interventions On Clinical Outcome and Cost Avoidance in A University Teaching HospitalDocument8 pagesImpact of Pharmacist Interventions On Clinical Outcome and Cost Avoidance in A University Teaching HospitalErick De La RosaNo ratings yet
- 7051N3M126Q411U7Document69 pages7051N3M126Q411U7naldihasibuanNo ratings yet
- Watcharapasorn 2016Document5 pagesWatcharapasorn 2016FranckNo ratings yet
- Post Operative Nausea and Vomiting, Its Causes, and The Way of Its Prevention and TreatmentDocument11 pagesPost Operative Nausea and Vomiting, Its Causes, and The Way of Its Prevention and TreatmentSurendra MaharjanNo ratings yet
- Prospective External Validation of A Predictive Score For Postoperative Pulmonary ComplicationDocument13 pagesProspective External Validation of A Predictive Score For Postoperative Pulmonary ComplicationAthziri GallardoNo ratings yet
- Journal Pre-Proof: International Journal of Medical InformaticsDocument29 pagesJournal Pre-Proof: International Journal of Medical InformaticsDityan KaleNo ratings yet
- Implementation and Function of Acute Pain Management Service: Aga Khan University Hospital ExperienceDocument3 pagesImplementation and Function of Acute Pain Management Service: Aga Khan University Hospital ExperienceMohammad HamidNo ratings yet
- Incidence, Characteristics, and Predictive Factors For Medication Errors in Paediatric Anaesthesia: A Prospective Incident Monitoring StudyDocument8 pagesIncidence, Characteristics, and Predictive Factors For Medication Errors in Paediatric Anaesthesia: A Prospective Incident Monitoring StudyShaikh ZarinNo ratings yet
- Adherence QuestionnaireDocument8 pagesAdherence QuestionnaireDhila FayaNo ratings yet
- PONV Prophylaxis GuidelinesDocument7 pagesPONV Prophylaxis GuidelinesAbby WardNo ratings yet
- Introduction To The Postanaesthetic Care Unit: Review Open AccessDocument7 pagesIntroduction To The Postanaesthetic Care Unit: Review Open AccessSamsul BahriNo ratings yet
- 2 Sba RaquiDocument9 pages2 Sba Raquijoanna medeirosNo ratings yet
- Research ArticleDocument8 pagesResearch ArticleafifahNo ratings yet
- Antiemetic Guideline Consistency and Incidence of Chemotherapy-Induced Nausea and Vomiting in US Community Oncology Practice: INSPIRE StudyDocument10 pagesAntiemetic Guideline Consistency and Incidence of Chemotherapy-Induced Nausea and Vomiting in US Community Oncology Practice: INSPIRE StudyKurnia AnharNo ratings yet
- Principles of Monitoring Postoperative Patients: Oleh: Meity Sarah 2012610108Document8 pagesPrinciples of Monitoring Postoperative Patients: Oleh: Meity Sarah 2012610108Jefry ArieNo ratings yet
- Prevalence, Risk Factors, and Optimized Management of Moderate To Severe Thirst in The Post Anesthesia Care UnitDocument10 pagesPrevalence, Risk Factors, and Optimized Management of Moderate To Severe Thirst in The Post Anesthesia Care Unitpooria shNo ratings yet
- BCP 14159Document12 pagesBCP 14159dentsavvyNo ratings yet
- 29th International Symposium On Intensive Care and Emergency MedicineDocument209 pages29th International Symposium On Intensive Care and Emergency MedicineYOGINo ratings yet
- Pan 13575Document2 pagesPan 13575Reynaldi HadiwijayaNo ratings yet
- 2014 Article 369Document6 pages2014 Article 369pebinscribdNo ratings yet
- Preventing Ventilator-Associated ICHEDocument8 pagesPreventing Ventilator-Associated ICHEFelix Brian FelixNo ratings yet
- Acta Anaesthesiologica Taiwanica: Research PaperDocument7 pagesActa Anaesthesiologica Taiwanica: Research PaperShuaib AhmedNo ratings yet
- PIIS0007091221004359Document7 pagesPIIS0007091221004359luisfernandoamaya89No ratings yet
- Paper Reintubación Variable Sexo y EdadDocument5 pagesPaper Reintubación Variable Sexo y EdadAres Kinesiology TapeNo ratings yet
- Asa 2013Document1,076 pagesAsa 2013Marwa Mahrous100% (4)
- Research Paper On Ventilator Associated PneumoniaDocument8 pagesResearch Paper On Ventilator Associated PneumoniakwbfbzundNo ratings yet
- Fournel 2020Document9 pagesFournel 2020tim yuNo ratings yet
- 747-Article Text-1365-1-10-20200430Document6 pages747-Article Text-1365-1-10-20200430Yogita DhurandharNo ratings yet
- Perioperative Point of Care Ultrasound From Concept To ApplicationDocument9 pagesPerioperative Point of Care Ultrasound From Concept To Applicationzumbidoslema0qNo ratings yet
- The Preparation and Administration of Intravenous Drugs Before and After Protocol ImplementationDocument8 pagesThe Preparation and Administration of Intravenous Drugs Before and After Protocol ImplementationIvanCompeanVazquezNo ratings yet
- Ade Et AlDocument7 pagesAde Et Alkang.asep008No ratings yet
- Fiorino2000 PDFDocument11 pagesFiorino2000 PDFDiego Antonio Rodriguez CoronadoNo ratings yet
- Dyspnea ProjectDocument20 pagesDyspnea Projectfarah.abd97No ratings yet
- Predicting Weaning and Extubation Outcomes in Long-Term Mechanically Ventilated Patients Using The Modified Burns Wean Assessment Program ScoresDocument7 pagesPredicting Weaning and Extubation Outcomes in Long-Term Mechanically Ventilated Patients Using The Modified Burns Wean Assessment Program ScoresClaudia IsabelNo ratings yet
- Prevention of VAP Use For Bundle Approach 10.1016@j.ajic.2016.04.237Document4 pagesPrevention of VAP Use For Bundle Approach 10.1016@j.ajic.2016.04.237sarintiNo ratings yet
- Journa Generall AneshesiaDocument7 pagesJourna Generall AneshesiaNadya NovianiNo ratings yet
- Payment Instructions For Docs RequestedDocument1 pagePayment Instructions For Docs RequestedElaine IllescasNo ratings yet
- EPM BookmarkDocument2 pagesEPM BookmarkElaine IllescasNo ratings yet
- Outpatient Cheat CodeDocument18 pagesOutpatient Cheat CodeElaine IllescasNo ratings yet
- PAINAD ScaleDocument2 pagesPAINAD ScaleElaine IllescasNo ratings yet
- Functional Actvity ScaleDocument1 pageFunctional Actvity ScaleElaine IllescasNo ratings yet
- Complications After Thigh Sarcoma ResectionDocument7 pagesComplications After Thigh Sarcoma ResectionElaine IllescasNo ratings yet
- CNB Vs IncisionDocument12 pagesCNB Vs IncisionElaine IllescasNo ratings yet
- A Case of Recurrent Mesocolon Myxoid Liposarcoma and Review of The LiteratureDocument7 pagesA Case of Recurrent Mesocolon Myxoid Liposarcoma and Review of The LiteratureElaine IllescasNo ratings yet
- Dinardo 2018Document7 pagesDinardo 2018Elaine IllescasNo ratings yet
- Ni Hms 690786Document17 pagesNi Hms 690786Elaine IllescasNo ratings yet
- Mansoor 2017Document36 pagesMansoor 2017Elaine IllescasNo ratings yet
- AJCC 8th STSDocument5 pagesAJCC 8th STSElaine IllescasNo ratings yet
- BPG Assessment of PainDocument147 pagesBPG Assessment of PainFarah ShamsudinNo ratings yet
- Patient-Centered Care and AdherenceDocument8 pagesPatient-Centered Care and AdherencethinkercolNo ratings yet
- Periodontal Considerations: Presented By: Layan Suleiman Supervisor: Dr. Mohammad AL-Rabab'ahDocument33 pagesPeriodontal Considerations: Presented By: Layan Suleiman Supervisor: Dr. Mohammad AL-Rabab'ahasop06No ratings yet
- Prenatal Care Common Discomforts During PregnancyDocument5 pagesPrenatal Care Common Discomforts During PregnancyKarina MadriagaNo ratings yet
- GastricDocument142 pagesGastricMore MorenoNo ratings yet
- PNPK PNPKDocument3 pagesPNPK PNPKPutri JunitasariNo ratings yet
- Sel ListDocument66 pagesSel Listcharuhans nandgaonkarNo ratings yet
- Reference LetterDocument2 pagesReference Letterapi-400249790No ratings yet
- Laboratorio Clinico Toledo: Patient Number Birthdate SexDocument1 pageLaboratorio Clinico Toledo: Patient Number Birthdate SexMirle BonetNo ratings yet
- DS-10249 ACLS PI Sheet 03ts PDFDocument1 pageDS-10249 ACLS PI Sheet 03ts PDFAsrini Rizky NasutionNo ratings yet
- Hmhub: Food SafetyDocument5 pagesHmhub: Food SafetyJonathan LabutapNo ratings yet
- Embedding AcupunctureDocument5 pagesEmbedding AcupunctureAngela PagliusoNo ratings yet
- NiceDocument45 pagesNiceKenneth Mark B. TevesNo ratings yet
- Republic of The Philippines Tamag, Vigan City 2700 Ilocos Sur Website: MailDocument2 pagesRepublic of The Philippines Tamag, Vigan City 2700 Ilocos Sur Website: MailRenea Joy ArruejoNo ratings yet
- Survival of Atraumatic Restorative Treatment (ART) Sealants and Restorations: A Meta-AnalysisDocument15 pagesSurvival of Atraumatic Restorative Treatment (ART) Sealants and Restorations: A Meta-AnalysisestefaniaNo ratings yet
- Enteral Nutrition of Preterm BabyDocument54 pagesEnteral Nutrition of Preterm Babylordoftheweb100% (5)
- Jurnal Teledentistry 1Document7 pagesJurnal Teledentistry 1Dio Nella ArlinggaNo ratings yet
- Piedmont Medical Center RulingDocument40 pagesPiedmont Medical Center RulingHLMeditNo ratings yet
- Anomalies DentinDocument19 pagesAnomalies DentinHaffie HafiziNo ratings yet
- Leaflet Covid 19 - Pregnant Women PDFDocument2 pagesLeaflet Covid 19 - Pregnant Women PDFBindar AdrianNo ratings yet
- Abdominal Pain A Synthesis of Recommendations ForDocument11 pagesAbdominal Pain A Synthesis of Recommendations Forsakinah mawadahNo ratings yet
- Pregnancy ComplicationsDocument11 pagesPregnancy ComplicationsJosé David Cortez Centeno 20190155No ratings yet
- Diagnosis Short Term Goals Long Term Goals Nursing InterventionsDocument4 pagesDiagnosis Short Term Goals Long Term Goals Nursing Interventionsdanny_ng08100% (9)
- Test Bank For Porth Pathophysiology Concepts of Altered Health States 1st Canadian Edition HannonDocument15 pagesTest Bank For Porth Pathophysiology Concepts of Altered Health States 1st Canadian Edition Hannonuncapepais16614100% (50)
- 13 Lombe Mumba Ramson 2017 Knowledge Attitude and Practice of Breast Self Examination For Early Detectoin of Breast Cancer Among Women in Roan Constituency in Luanshya Copperbelt Province ZambiaDocument9 pages13 Lombe Mumba Ramson 2017 Knowledge Attitude and Practice of Breast Self Examination For Early Detectoin of Breast Cancer Among Women in Roan Constituency in Luanshya Copperbelt Province ZambiaArick Frendi AndriyanNo ratings yet
- Zygomatic ImplantsDocument3 pagesZygomatic ImplantsDeb SNo ratings yet