Professional Documents
Culture Documents
eFAST MAC
eFAST MAC
Uploaded by
igd rssaOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
eFAST MAC
eFAST MAC
Uploaded by
igd rssaCopyright:
Available Formats
Traumatic injury is the leading cause of death among individuals younger than 45
years old. Eighty percent of traumatic injury is blunt with the majority of deaths
secondary to hypovolemic shock. In fact, intraperitoneal bleeds occur in 12% of
blunt trauma; therefore, it is essential to identify trauma quickly. The optimal
test should be rapid, accurate, and non-invasive.
Bloom BA, Gibbons RC. Focused Assessment with Sonography for Trauma. [Updated 2020
Jul 31]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing;
2021 Jan-.
Available from: https://www.ncbi.nlm.nih.gov/books/NBK470479/
A.Emergency Indications
Indications for the eFAST include both blunt and penetrating traumatic injuries as
well as presentations of unexplained hypotension as part of an ultrasound shock
protocol (i.e., RUSH exam) to rapidly diagnose the cause of low blood pressure.
B.Contraindications
Contraindications to the eFAST are primarily situations in which performing the
study would delay or interfere with critical life-saving interventions including
emergent surgical intervention.
C.eFAST protocol steps
The premise behind the FAST exam is that free fluid accumulates in the dependent
areas of the abdomen. According to some experts, an extended FAST exam involves
several views. These are;
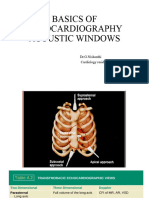
1.Subcostal or Parasternal Long Axis Cardiac
2.Right Upper Quadrant
3.Left Upper Quadrant
4.Suprapubic
5.Thorax for Hemothorax and Pneumothorax
6.IVC for volume status
https://iem-course.org/courses/efast/
*Subcostal Transducer Position*
To obtain this view, use the liver as the acoustic window. The transducer is
curvilinear—the transducer marker (triangle) aims to the right side of the patient.
*Normal Subcostal View*
The right ventricle (RV) is the closest cardiac chamber to the chest wall. The left
ventricle (LV) and both atria (LA and RA) are also visible. The bright white line
is the pericardium. Liver located closest to the top.
*Parasternal Long Axis Transducer Position*
The transducer is placed next to the left sternal border at the 2-4 intercostal
level. The transducer marker, depending on a user preference, can aim to 10 o’clock
(right shoulder) or 4 o’clock (left hip) direction. At this image, the transducer
marker aims to the right shoulder. Images on the right.
*Normal Parasternal Long Axis Cardiac View*
If an adequate subcostal view of the heart cannot be obtained, attempt the
parasternal long axis view. A subcostal view might be difficult in some trauma
patients if they have an abdominal injury, epigastric tenderness or abdominal
distention. In this view, the right ventricle is still the closest cardiac chamber
to the anterior chest wall. The left ventricle left atrium, and aortic outflow
tract are also visible.
*Right Upper Quadrant Transducer Position*
The right upper quadrant is the abdominal view that is the most likely to be
positive. The transducer is placed in the mid-axillary line with the probe marker
pointed toward the patient’s head. A low-frequency, curvilinear, or a phased array
probe should be used to obtain this view.
*Normal Right Upper Quadrant View*
First, identify the kidney and the liver. The kidney is often the easiest structure
to identify. It has a bright white center surrounded by the less echogenic cortex.
The hepatorenal space, the interface between the kidney and liver, is a potential
space that may contain free fluid. In this image, the patient’s head is toward the
left side of the screen, and the feet are toward the right side of the screen. The
diaphragm is the bright white line just superior to the liver. It is important to
visualize the tip of the liver as well as the inferior pole of the kidney to have
an adequate assessment of the hepatorenal space.
Key notes: Make sure to see and evaluate both tips of liver and both poles of right
kidney so we can exclude minimal hemorrhage in this area. If there is a free fluid
(anechoic) we can quickly scan for anomaly structure and find the potential source
of bleeding.
*Normal Hemithorax View*
The image above shows the kidney, liver, and diaphragm. However, as you transition
to the chest cavity at the insertion of the diaphragm, air scatters the ultrasound
beam, and you lose visualization of the spine. In addition, you can see a mirror
image artifact.
(A) Right upper quadrant view with normal pleural space. (B) Right upper quadrant
view with evidence of pleural effusion (*) and positive spine sign
*Left Upper Quadrant Transducer Position*
To obtain the left upper quadrant view, position the probe at the left posterior
axillary line near ribs nine and ten. Again, the probe marker is pointed toward the
patient’s head. Since rib shadows may obscure your view, it is sometimes helpful to
angle the probe obliquely in line with the intercostal space.
*Normal Left Upper Quadrant*
This normal view of the left upper quadrant shows the spleen and the kidney (see
image above). As with the right upper quadrant view, the patient’s head is to the
left of the screen, and the patient’s feet are toward the right of the screen.
The diaphragm is a bright white, hyperechoic curving line superior to the spleen.
On the left side, examine the space between the kidney and the spleen for free
fluid. However, it is more likely that fluid will accumulate around the dome of the
spleen and, therefore, you must image the dome of the spleen.
*Pelvic View Transducer Position*
The pelvic view is obtained by placing the transducer in a suprapubic position in
either a transverse or longitudinal orientation. Since the bladder is the acoustic
window, it is helpful to image the patient before the placement of a Foley
catheter.
On the transverse view, the transducer marker aims to the patient’s right side (see
image above). On the longitudinal view, the transducer marker aims to the patient
‘s head. For both exams, the transducer is placed just above the symphysis pubis
and aim downwards inside the pelvis, not toward to abdomen.
*Normal Transverse Pelvic View*
This normal, transverse suprapubic view fans through the bladder. Look for free
fluid lateral or inferior to the bladder.
In the pelvic view, fluid will accumulate in rectouterine space also known as the
pouch of Douglas in females and rectovesical space in males.
*Thorax View Transducer Position*
The extended FAST exam also images each hemithorax for pneumothorax. Using a high
frequency (linear) probe to obtain a longitudinal view of the lung between 3rd and
4th intercostal space, mid-clavicular line is a standard approach. The indicator
(transducer marker) pointed toward the patient’s head.
Since air rises, the transducer should be placed at the most superior region of the
chest. In the supine, trauma patient, this position is usually the third
intercostal space. If the patient is sitting, the apices of the lungs should be
imaged.
*Normal Thorax View*
Grab your transducer with your index finger and thumb like a pen. When you place
your transducer as defined above, you need to find two ribs (HYPERechogenic[white]
curved structures with a HYPOechogenic[gray-black] shadow behind) on the sides and
pleural line (hyperechogenic) in the middle. When you find the view, you need to
stand still at this position by using your other fingers as a tripod.
*Transducer Position for Volume Assessment*
Place the transducer on the abdomen with the probe marker pointed towards the
patient’s head. Visualize the vena cava about 3 cm proximal to the cavoatrial
junction.
*IVC View*
To visualize IVC, you can use various techniques. One of them is to finding the
subcostal 4 chamber view and rotating your transducer marker to 12 o’clock
(patient’s head). At this moment, you can see longitudinal anechoic vessels. If
your transducer tilted to the patient’s left side, this vessel is probably aorta,
and it has thick hyperechogenic borders and pulsates. If your transducers tilted to
the patient’s right side (liver), probably this vessel is inferior vena cava (IVC)
with thinner walls and changes its diameter with respirations. When you see IVC,
now you need to tilt your transducer inside the thorax to find the cavoatrial
junction.
You might also like
- Sullair 900RH Parts ManualDocument198 pagesSullair 900RH Parts ManualTamer Elsebaei Ebarhim100% (2)
- Basic of Thorax Imaging - 10 September 2013 - by Robby HermawanDocument126 pagesBasic of Thorax Imaging - 10 September 2013 - by Robby HermawanenriNo ratings yet
- Focused Assessment With Sonography For Trauma (Fast) and Extended-FastDocument49 pagesFocused Assessment With Sonography For Trauma (Fast) and Extended-FastajNo ratings yet
- Us Abdominal AortaDocument16 pagesUs Abdominal AortaRomaNo ratings yet
- Hippo EM Board Review - Ultrasound (New 2017) Written SummaryDocument8 pagesHippo EM Board Review - Ultrasound (New 2017) Written Summarykaylawilliam01No ratings yet
- 2 POCUS in Emergency FAST IVC LUNGresidents December 2022Document92 pages2 POCUS in Emergency FAST IVC LUNGresidents December 2022dr mohd abdul basithNo ratings yet
- PIIS0749070413000729Document25 pagesPIIS0749070413000729Juan Carlos MezaNo ratings yet
- Chest Xray 2Document39 pagesChest Xray 2sushma shresthaNo ratings yet
- Emergency UltrasoundDocument32 pagesEmergency UltrasoundChoga ArlandoNo ratings yet
- Trauma Ultrasound and The FAST ExamDocument7 pagesTrauma Ultrasound and The FAST ExamhaldiszopianNo ratings yet
- UltrasoundTraumaCh02 Fast ExamDocument23 pagesUltrasoundTraumaCh02 Fast Exam108dudleyNo ratings yet
- Basic of Thorax ImagingDocument105 pagesBasic of Thorax ImagingIlham Matoha100% (1)
- Fetal Cardiac Screening Sonography: MethodologyDocument43 pagesFetal Cardiac Screening Sonography: MethodologyUmber AgarwalNo ratings yet
- Echocardiographic ViewsDocument50 pagesEchocardiographic ViewsSheerazNo ratings yet
- Trauma - Fast ScanDocument3 pagesTrauma - Fast ScancsleeNo ratings yet
- Head and Neck Gastrointestinal Lung Pelvic Renal and BladderDocument10 pagesHead and Neck Gastrointestinal Lung Pelvic Renal and BladderAmir AliNo ratings yet
- Fast Scan 2022Document9 pagesFast Scan 2022rosieNo ratings yet
- Diagnostic Imaging - 8 - Radiological Pathology - Lung Pathologies and Radiology in Specific Cases - Prof - Dr.i̇smet TAMERDocument35 pagesDiagnostic Imaging - 8 - Radiological Pathology - Lung Pathologies and Radiology in Specific Cases - Prof - Dr.i̇smet TAMERAly MssreNo ratings yet
- Radiological Investigation of Chest. The Radiological Semiotics of The Chest PathologyDocument169 pagesRadiological Investigation of Chest. The Radiological Semiotics of The Chest PathologyВладимир КурпаянидиNo ratings yet
- Basic of Thorax Imaging - 10 September 2013 - by Robby HermawanDocument126 pagesBasic of Thorax Imaging - 10 September 2013 - by Robby HermawannuradilahyasminNo ratings yet
- 2 1 Diseases of The Respiratory System Radiological Pathology DRDocument43 pages2 1 Diseases of The Respiratory System Radiological Pathology DRNatnael GetahunNo ratings yet
- Chest X-Ray: Confirm DetailsDocument14 pagesChest X-Ray: Confirm DetailsNosheen HafeezNo ratings yet
- Assessment of The Thorax Lungs 1Document6 pagesAssessment of The Thorax Lungs 1Elliejenn EnderesNo ratings yet
- Chest X-Ray Interpretation A Structured Approach Radiology OSCEDocument1 pageChest X-Ray Interpretation A Structured Approach Radiology OSCEValentina SepúlvedaNo ratings yet
- Lung Ultrasound Made Easy Step-By-Step GuideDocument48 pagesLung Ultrasound Made Easy Step-By-Step GuideEL SHITA100% (1)
- Chest RadiographyDocument65 pagesChest RadiographyMunish Dogra100% (1)
- CXR Interpretation WriteupDocument32 pagesCXR Interpretation WriteupArhanNo ratings yet
- Basic of Thorax Imaging - 10 September 2013 - by Robby HermawanDocument126 pagesBasic of Thorax Imaging - 10 September 2013 - by Robby HermawanDwi putri PermatasariNo ratings yet
- Chest Xray BasicsDocument47 pagesChest Xray BasicsPartha GanesanNo ratings yet
- Abdomen Exam DetailsDocument5 pagesAbdomen Exam Detailsdidutza91No ratings yet
- Reading A Chest X-RayDocument2 pagesReading A Chest X-RaySabrinaAyuPutriNo ratings yet
- Imaging Abdominal Trauma Focus On FAST Revisi DR - BahtiarDocument54 pagesImaging Abdominal Trauma Focus On FAST Revisi DR - BahtiarJackson HakimNo ratings yet
- Scrubd 2Document14 pagesScrubd 2Radiant reeNo ratings yet
- Extended Focused Assessment With Sonography in Trauma (eFAST)Document45 pagesExtended Focused Assessment With Sonography in Trauma (eFAST)vimal rajNo ratings yet
- USguidedprocedures EditedDocument7 pagesUSguidedprocedures EditedLex Alejandro Jr.No ratings yet
- Respiratory System ExaminationDocument12 pagesRespiratory System ExaminationHoussemNo ratings yet
- Ultrasound Guided ProceduresDocument71 pagesUltrasound Guided Proceduresg1381821No ratings yet
- Acoustic WindowsDocument54 pagesAcoustic Windowsgovind rajNo ratings yet
- Kuliah Tramed PBLDocument71 pagesKuliah Tramed PBLAgung Ngurah Ray100% (1)
- Advances in Trauma UltrasoundDocument12 pagesAdvances in Trauma UltrasoundBruce Fredy Chino ChambillaNo ratings yet
- EJE2010 - Eco en Enfermedad de AortaDocument14 pagesEJE2010 - Eco en Enfermedad de AortaRaul GascueñaNo ratings yet
- How To Read A Chest X RayDocument11 pagesHow To Read A Chest X RayHilmia Fahma100% (2)
- Echocardiogram: Echocardiogram, Also Known As Echocardiography, or Heart Ultrasound Is ADocument23 pagesEchocardiogram: Echocardiogram, Also Known As Echocardiography, or Heart Ultrasound Is AKarl RobleNo ratings yet
- CardiacDocument47 pagesCardiacJoyzoey100% (2)
- Ldcu Group 4 Buscaino April ShineDocument57 pagesLdcu Group 4 Buscaino April ShineApril Shine BuscainoNo ratings yet
- Respiratory Diagnostic Tests & Procedures.Document32 pagesRespiratory Diagnostic Tests & Procedures.Salman KhanNo ratings yet
- Abdominal Ultrasound Anatomy.: DR/ Abd Allah Nazeer. MDDocument50 pagesAbdominal Ultrasound Anatomy.: DR/ Abd Allah Nazeer. MDAri Dwi PrasetyoNo ratings yet
- Chest X-Ray Analysis 2023Document63 pagesChest X-Ray Analysis 2023CHARLOTTE DU PREEZNo ratings yet
- CHEST X-RAY Presentation CVSDocument45 pagesCHEST X-RAY Presentation CVSNorsafrini Rita Ahmad100% (1)
- Chest X Ray Techniques and PositioningDocument67 pagesChest X Ray Techniques and PositioningSandeep ChaudharyNo ratings yet
- Chest X-Rays: Anusuya R. Radiograher, Department of Radiology, MMCH & RiDocument36 pagesChest X-Rays: Anusuya R. Radiograher, Department of Radiology, MMCH & RiHafis NasarNo ratings yet
- Interpretation of CXray 2021Document250 pagesInterpretation of CXray 2021osamayasser82No ratings yet
- XrayDocument28 pagesXrayPravinNo ratings yet
- Basics of Chest Xrays DR Divya 2Document48 pagesBasics of Chest Xrays DR Divya 2tanmaylawandpvtNo ratings yet
- Respiratory SystemDocument43 pagesRespiratory SystemLyht TVNo ratings yet
- X RayDocument18 pagesX RayAbdul Ghaffar AbdullahNo ratings yet
- Chest Xray PDFDocument8 pagesChest Xray PDFOvi SharmaNo ratings yet
- Fetal Cardiology: A Practical Approach to Diagnosis and ManagementFrom EverandFetal Cardiology: A Practical Approach to Diagnosis and ManagementNo ratings yet
- Transplantation SurgeryFrom EverandTransplantation SurgeryGabriel C. OniscuNo ratings yet
- Cds13041 Yamaha PWC Plug-In EcuDocument1 pageCds13041 Yamaha PWC Plug-In EcuGérôme ZélateurNo ratings yet
- StarUML 5.0 Developer GuideDocument123 pagesStarUML 5.0 Developer GuideJohn ZiziNo ratings yet
- S7-SCL - Working With S7-SCL PDFDocument28 pagesS7-SCL - Working With S7-SCL PDFPirvu Ioan DanielNo ratings yet
- Phonemic Transcription Is The Most Common Type Of: Allophonic & Phonemic Transcription A Broad Transcription, Also CalledDocument2 pagesPhonemic Transcription Is The Most Common Type Of: Allophonic & Phonemic Transcription A Broad Transcription, Also CalledMuhammad DelvinNo ratings yet
- Durst Rho 600 Pictor - SM - 4-HeadAdjustment - V1.3 - 1Document25 pagesDurst Rho 600 Pictor - SM - 4-HeadAdjustment - V1.3 - 1Anonymous aPZADS4No ratings yet
- VSMDocument2 pagesVSMaimun rasheedNo ratings yet
- IT Practical File Main 2023-24Document45 pagesIT Practical File Main 2023-24princethakan9No ratings yet
- AbarisDocument6 pagesAbarisЛеонид Жмудь100% (1)
- Shielding Gases Selection Chart 2013Document1 pageShielding Gases Selection Chart 2013Lachie TaylorNo ratings yet
- Chapter 5 Concurrency 1: Mutual Exclusion and SynchronizationDocument10 pagesChapter 5 Concurrency 1: Mutual Exclusion and SynchronizationAri BaderNo ratings yet
- Foundation EngineeringDocument2 pagesFoundation EngineeringqwfqefwqefgefqeNo ratings yet
- TWJO-1-TCD-ST1-0004-Rev E-A6Document61 pagesTWJO-1-TCD-ST1-0004-Rev E-A6Anang AprizalNo ratings yet
- FRGU Tech SpecDocument11 pagesFRGU Tech SpecAdin AlayubiNo ratings yet
- FB6100 DSCDocument132 pagesFB6100 DSCTahir FadhilNo ratings yet
- 992D Valve Set InstructionsDocument7 pages992D Valve Set InstructionsJohn GrayNo ratings yet
- Design For Testability and Design For Testability and Built Built - in Self in Self - Test TestDocument74 pagesDesign For Testability and Design For Testability and Built Built - in Self in Self - Test TestSyed Waqas Arif Shah100% (1)
- Principles of Environmental Science 8th Edition Cunningham Solutions Manual 1Document36 pagesPrinciples of Environmental Science 8th Edition Cunningham Solutions Manual 1kaylanunezorjsgzqmti100% (31)
- Update UI Components With NavigationUIDocument21 pagesUpdate UI Components With NavigationUISanjay PatelNo ratings yet
- Basic Probability and Statistics A Short CourseDocument128 pagesBasic Probability and Statistics A Short CourseangladaxNo ratings yet
- Molar Solutions: Questionsheet 1Document10 pagesMolar Solutions: Questionsheet 1thegreatwardiniNo ratings yet
- Melamine Test (HPLC GC)Document5 pagesMelamine Test (HPLC GC)widodoNo ratings yet
- IDES MK Cable Scenario MTODocument16 pagesIDES MK Cable Scenario MTOaprian100% (1)
- Ac Bridge: EEE 457: Measurement & InstrumentationDocument13 pagesAc Bridge: EEE 457: Measurement & InstrumentationTareqNo ratings yet
- Checkweigher RFQ FormDocument2 pagesCheckweigher RFQ Formwasim KhokharNo ratings yet
- Exam-Style Question:: Mathematical ModellingDocument4 pagesExam-Style Question:: Mathematical ModellingFadi AyyoubNo ratings yet
- Python Quick ReferenceDocument3 pagesPython Quick ReferenceBill Havanki100% (1)
- Leister Plastic Welding BR Hot Air Hand Tools PlastralDocument28 pagesLeister Plastic Welding BR Hot Air Hand Tools PlastralCristian FerchiuNo ratings yet
- MT7621 PDFDocument43 pagesMT7621 PDFCami DragoiNo ratings yet
- (2016) Method Development For FeODocument5 pages(2016) Method Development For FeODoreya MorenoNo ratings yet