Professional Documents
Culture Documents
117 - Neurology Physiology) Trigeminal Nerve - Cranial Nerve V
117 - Neurology Physiology) Trigeminal Nerve - Cranial Nerve V
Uploaded by
Ussama MD0 ratings0% found this document useful (0 votes)
50 views7 pagesThe document summarizes the trigeminal nerve (cranial nerve V), with a focus on its first branch, the ophthalmic division (V1). It describes the origin and course of V1, including through the cavernous sinus and superior orbital fissure. It provides detailed information on the branches of V1 and the structures each supplies, such as the lacrimal, frontal, and nasociliary nerves supplying different areas of the face, eye, and nasal cavity.
Original Description:
Original Title
117 - Neurology Physiology] Trigeminal Nerve_ Cranial Nerve V
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThe document summarizes the trigeminal nerve (cranial nerve V), with a focus on its first branch, the ophthalmic division (V1). It describes the origin and course of V1, including through the cavernous sinus and superior orbital fissure. It provides detailed information on the branches of V1 and the structures each supplies, such as the lacrimal, frontal, and nasociliary nerves supplying different areas of the face, eye, and nasal cavity.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
0 ratings0% found this document useful (0 votes)
50 views7 pages117 - Neurology Physiology) Trigeminal Nerve - Cranial Nerve V
117 - Neurology Physiology) Trigeminal Nerve - Cranial Nerve V
Uploaded by
Ussama MDThe document summarizes the trigeminal nerve (cranial nerve V), with a focus on its first branch, the ophthalmic division (V1). It describes the origin and course of V1, including through the cavernous sinus and superior orbital fissure. It provides detailed information on the branches of V1 and the structures each supplies, such as the lacrimal, frontal, and nasociliary nerves supplying different areas of the face, eye, and nasal cavity.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
You are on page 1of 7
Last edited: 9/5/2021
52. TRIGEMINAL NERVE | CRANIAL NERVE V
Neurology | Trigeminal Nerve | Cranial Nerve V Medical Editor: Dr. Ana Guerra
OUTLINE II) BRANCHES: COURSE AND STRUCTURES
SUPPLIED
I) ORIGIN OF NERVE
II) BRANCHES: COURSE AND STRUCTURES (A) V1: OPHTHALMIC DIVISIOIN
SUPPLIED
After its origin within the trigeminal ganglia, V1 moves
III) CLINICAL CORRELATION
IV) APPENDIX within the lateral wall of the cavernous sinus.
V) REVIEW QUESTIONS
VII) REFERENCES The Cavernous Sinus
The dura mater is divided into two layers: Periosteum
layer and meningeal layer. The sinus in between both
layers is called the cavernous sinus.
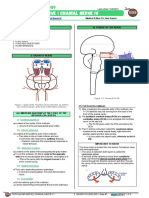
I) ORIGIN OF NERVE The structures that move within the lateral wall of the
cavernous sinus are III CN, IV CN, V1, and V2.
(A) TRIGEMINAL GANGLION The internal carotid artery (ICA) moves through the
foramen lacerum and then it enters the cavity of the
This is the origin of the three trigeminal branches cavernous sinus, next to the abducens nerve.
o V1: Ophthalmic division: GSA fibers.
o V2: Maxillary division: GSA fibers.
o V3: Mandibular division: GSA and SVE fibers.
These are the peripheral processes of the V cranial
nerve.
Nice to know Figure 1-2. The cavernous sinus.
A ganglion is a group of cell bodies located within the
peripheral nervous system. It exits the skull through the superior orbital fissure giving
off three branches:
o Lacrimal branch
(B) NUCLEUS WITHIN THE BRAIN STEM o Frontal branch
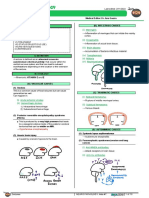
(1) Spinal Nucleus of CN V o Nasociliary branch
Exits the skull from the superior orbital fissure,
Receives information from the peripheral processes, and inside of the Annulus of Zinn.
controls touch, pain, temperature, pression and
proprioception of the entire face. Annulus of Zinn
o One of the most important nucleus of CN V.
Located within the medulla.
(2) Central or Principal Pontine Nucleus of CN V
In charge of picking up touch and proprioception of the
jaw.
Located within the pons.
(3) Mesencephalic Nucleus of CN V
Picks up proprioception of the face.
Located within the midbrain (also known as
mesencephalon).
(4) Trigeminal Motor Nucleus Figure 1-3. The posterior wall of the eyeball seen from an
anterior view: The Annulus of Zinn (green circle), also known
Special Viscera Efferent fibers as the Common tendinous ring.
Supplies the first pharyngeal arch Acts as the origin of four extraocular eye muscles:
o Muscles of mastication. Superior recuts, medial rectus, lateral rectus, and
inferior rectus.
Separates the superior orbital fissure into two
compartments: One inside of the Annulus of Zinn
and another one outside of it.
o Structures inside of the Annulus of Zinn:
The superior and inferior branches of CN III.
The nasociliary nerve.
Abducens nerve (CN VI).
o Structures outside of the Annulus of Zinn:
Lacrimal nerve.
Frontal nerve.
Trochlear nerve (CN IV).
Figure 1. Origin of the main divisions of the trigeminal nerve:
Ophthalmic division, maxillary division and mandibular division.
TRIGEMINAL NERVE | CRANIAL NERVE V NEURO PHYSIOLOGY: Note #52. 1 of 7
(iii) Ethmoidal branches
a. Moves upwards to the ethmoid bone
b. Gives off two branches:
i. Posterior ethmoidal nerve
1. Supply innervation to the ethmoid sinuses.
ii. Anterior ethmoidal nerve
1. Medial nasal branch:
a. Supplies touch, pain and temperature
innervation to the medial side of the
nasal cavity.
2. Lateral nasal branch:
a. Supplies touch, pain and temperature
Figure 1-4. Ophthalmic division of the trigeminal nerve: innervation to the lateral side of the
Branches and structures supplied. nasal cavity.
(1) LACRIMAL NERVE 3. External nasal branch:
a. Supplies touch, pain and temperature
Exits the skull through the temple side of the superior
innervation to the tip of the nose.
orbital fissure, outside of the Annulus of Zinn.
Gets to the lacrimal gland and pierces through it.
Gives off two branches:
a. One supplies innervation to the superior palpebra.
b. Another one supplies innervation to the underline
conjunctiva of the temple side of the eye.
(2) FRONTAL NERVE
Exits the skull through the superior orbital fissure, inside
of the Annulus of Zinn.
Gives off two branches:
(i) Supratrochlear nerve
a. Runs above the trochlea. Figure 1-6. Nasal cavity supplied by the Posterior ethmoidal
nerve and branches of the Anterior ethmoidal nerve.
b. Supplies innervation to the skin of the superior
palpebra, the underline conjunctiva, skin of the (iv) Infratrochlear nerve
forehead, and a small part of the scalp.
a. Runs underneath the trochlea.
(ii) Supraorbital nerve b. Gives off three branches:
i. One supplies the medial palpebra and the
a. Supplies innervation to the palpebra, the underline
underline conjunctiva.
conjunctiva, the skin of the forehead, and the skin
ii. The second one supplies to the lacrimal sac.
of the scalp till the vertex of the skull where the
iii. The third one supplies to the lacrimal caruncle.
lambdoid suture is located.
Figure 1-7. Structures supplied by the Infratrochlear nerve.
Figure 1-5. Innervation of the eye by the lacrimal nerve and
frontal nerve.
Table 1. Summary of V1: Branches and structures supplied.
(3) NASOCILIARY NERVE Branches Structures supplied
Exits the skull through the superior orbital fissure, inside
Superior temporal
of the Annulus of Zinn, in between of the superior and
palpebra
anterior branches of CN III. Lacrimal nerve Underline conjunctiva
Gives off four main branches: and temple side of the
eye.
(i) Short ciliary nerves
a. One branch moves with sympathetic and Frontal nerve Skin of superior temporal
parasympathetic fibers: o Supratrochlear nerve palpebra.
o Supraorbital nerve Underline conjunctiva.
i. The ciliary fibers move through the sclera and
Skin of forehead and
supply touch, pain and temperature to the
scalp.
cornea.
ii. Parasympathetic and sympathetic fibers supply Cornea, ciliary muscle
innervation to the ciliary muscle and the and iris.
iris. Nasociliary nerve Ethmoid sinuses.
o Short ciliary nerves Medial and lateral sides
(ii) Long ciliary nerves o Long ciliary nerves of the nasal cavity.
o Ethmoidal branches Tip of the nose.
a. The other branch moves only with sympathetic o Infratrochlear nerve Medial palpebra and
fibers:
underline conjunctiva,
i. Ciliary fibers supply innervation to the cornea. lacrimal sac and lacrimal
ii. Parasympathetic fibers supply innervation to the caruncle.
ciliary muscle and the iris.
(B) V2: MAXILLARY DIVISION
2 of 7 NEURO PHYSIOLOGY: Note #52. TRIGEMINAL NERVE | CRANIAL NERVE V
After its origin within the trigeminal ganglia, V2 moves (5) PTERYGOPALATINE GANGLION BRANCHES
within the lateral wall of the cavernous sinus, right
below V1. (i) Nasopharyngeal branch
V2 then leaves the cavernous sinus but right before a. Innervation to the nasal pharynx
exiting the skull through the foramen rotundum, it b. Innervation to the tympanil tube and a small part of
gives off the Meningeal branch. the skin of the tubal tonsil.
After crossing through the foramen rotundum, V2 moves
through the pterygopalatine fossa and gives
branches to the pterygopalatine ganglion. (ii) Orbital branch
It gives off another three main branches: a. Supplies touch, pain, and temperature to the orbital
a. The posterior superior alveolar nerve. cavity.
b. The infraorbital nerve.
c. The zygomatic nerve.
(iii) Lesser palatine nerve
(1) MENINGEAL/DURA BRANCH a. Supplies innervation to the soft palate and part of
the uvula.
Provides innervation to the dura mater.
(iv) Greater palatine nerve
(2) ZYGOMATIC NERVE
Moves to the orbital cavity through the inferior orbital a. Moves with the lesser palatine nerve.
fissure b. Supplies the posterior part of the hard palate.
Gives off two branches:
(i) Zygomatico temporal (v) Posterior superior nasal branch
nerve a. Enters the nasal cavity through the sphenopalatine
foramen and gives off three branches:
a. Supplies touch, pain and i. Medial nasal branch
temperature of the 1. Supplies the medial
temple. side of the nasal
(ii) Zygomatico facial cavity.
ii. Lateral nasal branch:
nerve 1. Supplies the lateral
a. Supplies touch, pain, side of the nasal
and temperature of the Figure 1-8. Innervation cavity.
cheek area. by the zygomatic nerve. iii. Nasopalatine nerve:
1. Crosses through the
incisive fossa and
Figure 1-9.
supplies the Innervation by the
(3) INFRAORBITAL NERVE
anterior hard posterior superior
Crosses through the inferior orbital fissure alongside palate. nasal branch.
the zygomatic nerve, and runs on the floor of the orbital
cavity. Table 2. Summary of V2: Branches and structures supplied.
Passes through the infraorbital foramen and gives off Branches Structures supplied
five branches:
Meningeal branch Dura mater
(i) Inferior palpebra branch Zygomatic nerve
a. Supplies innervation to the inferior palpebra and o Zygomatico temporal
nerve Temple
the underline conjunctiva.
o Zygomatico facial Cheek area
(ii) Nasal branch nerve
a. Innervation to the nose. Infraorbital nerve
o Inferior palpebra Inferior palpebra and
(iii) Superior labial branch branch underline conjunctiva.
o Nasal branch Nose.
a. Innervation to the upper lips. Upper lips.
o Superior labial
branch Premolars and gingiva.
(iv) Middle superior alveolar nerve (MSAN) Canines, central and
o MSAN
a. Innervation to the premolars and the gingiva o ASAN lateral incisors.
around it.
Posterior superior Hard palate, molars and
(v) Anterior superior alveolar nerve (ASAN) alveolar nerve gingiva.
a. Innervation to the canines, central and lateral Pterygopalatine
incisors. branches Tympanil tube and tubal
o Nasopharyngeal tonsil.
branch Orbital cavity.
o Orbital branch Soft palate.
(4) POSTERIOR SUPERIOR ALVEOLAR NERVE o Lesser palatine Posterior and anterior
nerve hard palate.
Supplies innervation to the hard palate, molars and the o Greater palatine Medial and lateral sides
gingiva around them. nerve of the nasal cavity.
o Posterior superior Anterior part of hard
nasal branch palate.
TRIGEMINAL NERVE | CRANIAL NERVE V NEURO PHYSIOLOGY: Note #52. 3 of 7
(C) V3: MANDIBULAR DIVISION (7) Lingual Nerve
Exits the skull through the foramen ovale. GSA fibers.
Right before leaving the skull, V3 gives off its first Supplies innervation to the anterior 2/3 of the tongue.
branch and it moves with the middle meningeal
artery. Chorda Tympani nerve
After emerging from the foramen oval, V3 gives off Facial nerve (CN VII) motor fibers run through the facial
branches that will provide facial sensation, canal within the middle ear, alongside its sensory
somatosensation from anterior 2/3 of tongue, and (SVA) and parasympathetic fibers called chorda
motor innervation to mastication. tympani.
(1) Nervus spinosus The chorda tympani emerges from the skull moving
from the posterior canaliculus to the anterior
Moves alongside the middle meningeal artery
canaliculus.
a. Supplies sensation to the dura mater.
It joins the pathway of the lingual nerve:
(2) Auriculotemporal nerve o Sensory fibers provide taste to the anterior 2/3 of the
GSA fibers. tongue via the lingual nerve.
a. Supplies innervation to the external ear and temple. o Parasympathetic fibers synapse with the
submandibular ganglion, and the postganglionic
(3) Buccal nerve fibers supply innervation to the submandibular and
GSA fibers. sublingual salivary glands.
a. Supplies innervation to the skin of the cheek.
(4) Nerve to medial pterygoid
SVE fibers.
a. Supplies the medial pterygoid muscle.
(5) Anterior division Figure 1-11. Chorda tympani nerve, a branch of the VII CN:
SVE fibers. Travels alongside the lingual nerve and supplies taste to the
a. Gives off three branches to supply motor innervation anterior 2/3 of the tongue, and the submandibular and
to muscles of mastication: sublingual glands.
(i) Deep temporal nerve:
i. Supplies the temporalis muscle. (8) Nerve to Tensor tympani
SVE fibers.
(ii) Masseteric nerve:
a. Supplies innervation to the tensor tympani muscle.
i. Supplies the masseter muscle. i. It pulls the malleus medially to tense the tympanic
membrane and make the sound less
(iii) Nerve to lateral pterygoid: intrusive.
i. Supplies the lateral pterygoid muscle.
ii. GSA fibers from the buccal nerve move alongside
the NLP. III) CLINICAL CORRELATION
(A) TRIGEMINAL NEURALGIA
(1) Causes:
Idiopathic: 10%
Vascular compression of CN V: 90%
a. Superior cerebellar artery (more commonly) and
Posterior cerebral artery.
b. Maxillary and mandibular divisions are the ones
most commonly affected.
(2) Manifestations
Excruciating pain in V2 and V3 region that can last from
seconds to minutes.
o Can happen up to 100 times a day.
Figure 1-10. Innervation of the mastication muscles by V3.
(3) Treatment
(6) Inferior Alveolar nerve
Medical manage: Carbamazepine, gabapentin.
GSA and SVE fibers.
Surgical manage: Surgical decompression.
a. Moves through the mandibula foramen and gives
Radiofrequency ablation.
off three branches:
(i) Inferior dental nerves:
i. Supply sensation to the inferior teeth.
(ii) Mental nerve:
i. Crosses the mental foramen.
1. Supplies to the skin of the chin.
(iii) Mylohyoid nerve
i. Supplies motor innervation to the mylohyoid
muscle and the anterior belly of digastric.
4 of 7 NEURO PHYSIOLOGY: Note #52. TRIGEMINAL NERVE | CRANIAL NERVE V
IV) APPENDIX
Table 3. Summary of the trigeminal nerve: Branches and structures supplied.
Course Branches Innervations
V1: Ophthalmic Division (GSA fibers)
Lacrimal Nerve
Superior temporal palpebra and the underline conjunctiva.
Frontal Nerve
Anteriorly through
cavernous sinus. Supratrochlear nerve Skin of superior temporal palpebra and underline conjunctiva
Accompanied by CN Supraorbital nerve Skin of forehead and a small part of the scalp.
III, IV, VI and V2.
Exits through the Nasociliary nerve
superior orbital Short ciliary nerves Cornea, ciliary muscle and iris.
fissure and enters Long ciliary nerves Cornea, ciliary muscle and iris.
the orbital cavity.
Ethmoidal branches Sensation to ethmoid sinuses; medial and lateral sides of the nasal
cavity.
Infratrochlear nerve Medial palpebra, lacrimal sac and lacrimal caruncle.
V2: Maxillary Division (GSA fibers)
Meningeal branch
Dura mater
Zygomatic nerve
Zygomatico temporal nerve Sensation to the temple.
Zygomatico facial nerve Sensation to the cheek area.
Infraorbital nerve
Inferior palpebra branch Inferior palpebra and underline conjunctiva.
Moves alongside V1 Nasal branch Sensation to the nose.
through the Superior labial branch nerve Sensation to the upper lips.
cavernous sinus.
Exits the skull Medial superior alveolar nerve Premolars and gingiva around it.
through foramen
rotundum and Anterior superior alveolar nerve Canines, central, and lateral incisors.
enters
pterygopalatine Posterior superior alveolar nerve
fossa. Hard palate, molars and gingiva.
Pterygopalatine branches
Nasopharyngeal branch Tympanil tube and a small portion of the tubal tonsil.
Orbital branch Sensation to the orbital cavity.
Lesser palatine nerve Soft palate.
Greater palatine nerve Posterior part of hard palate.
Posterior superior nasal branch Medial and lateral sides of the nasal cavity.
Anterior part of hard palate.
V3: Mandibular Division (GSA and SVE fibers)
Nervous spinosus (GSA)
Dura mater.
Auriculotemporal nerve (GSA)
External ear and temple.
Buccal nerve (GSA)
Skin of the cheek.
Nerve to medial pterygoid (SVE)
Medial pterygoid muscle.
Immediately exits
Anterior division (SVE)
the skull through the
foramen ovale. Deep temporal nerve Temporalis muscle
Masseteric nerve Masseter muscle
Nerve to lateral pterygoid Lateral pterygoid muscle.
Lingual nerve (GSA)
Sensation of anterior 2/3 of tongue.
VII CN runs with lingual nerve to supply taste to anterior 2/3 of
tongue.
Nerve to tensor tympani (SVE)
Tensor tympani muscle.
TRIGEMINAL NERVE | CRANIAL NERVE V NEURO PHYSIOLOGY: Note #52. 5 of 7
Figure 1-12. Summary of the trigeminal nerve: Branches and structures supplied.
V) REVIEW QUESTIONS If a person losses sensation of the anterior portion
of hard palate, which of the following nerves would
The following trigeminal nucleus is specifically be most likely to be affected?
responsible of picking sensory information from the a. Lesser palatine nerve.
jaw: b. Greater palatine nerve.
a. The spinal nucleus of CN V. c. Nasopharyngeal branch.
b. The central pontine nucleus. d. Nasopalatine nerve.
c. The mesencephalic nucleus.
d. The trigeminal motor nucleus. Name of the hole through which the mandibular
division exits the skull:
Name of the three branches given off by the a. Superior orbital fissure.
ophthalmic division of CN V: b. Foramen rotundum.
a. Orbital branch, lacrimal branch, and nasociliary c. Foramen ovale.
branch. d. Mandibula foramen.
b. Lacrimal branch, facial branch, and nasociliary
branch. Select the correct statement:
c. Lacrimal branch, frontal branch, and nasociliary a. Trigeminal neuralgia is a extremely painful condition,
branch. and its cause in the majority of cases is still
d. Lacrimal branch, frontal branch, and ciliary branch. idiopathic.
b. Trigeminal neuralgia is a extremely painful condition,
If a person loses sensation of the tip of the nose, and its cause in the majority of cases is the
which division of the nasociliary branch would be compression of V2 and V3 by the PCA.
the affected one? c. Trigeminal neuralgia is a extremely painful condition,
a. Short ciliary nerves. and its cause in the majority of cases is the
b. Long ciliary nerves. compression of V2 and V3 by the SCA.
c. Ethmoidal branches. d. Trigeminal neuralgia is a extremely painful condition,
d. Infratrochlear nerves. and its cause in the majority of cases is
autoimmune.
The following structures receive general somatic
afferent fibers from the maxillary division of V CN CHECK YOUR ANSWERS
EXCEPT for:
a. Dura mater.
b. Temporal side of the superior palpebra.
c. Inferior palpebra.
d. Orbital cavity.
VI) REFRENCES
6 of 7 NEURO PHYSIOLOGY: Note #52. TRIGEMINAL NERVE | CRANIAL NERVE V
● Snell, R. S. (2010). Clinical neuroanatomy (7th ed.).
Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins.
● Sabatine MS. Pocket Medicine: the Massachusetts General
Hospital Handbook of Internal Medicine. Philadelphia: Wolters
Kluwer; 2020.
● Le T. First Aid for the USMLE Step 1 2020. 30th anniversary
edition: McGraw Hill; 2020.
● Williams DA. Pance Prep Pearls. Middletown, DE: Kindle Direct
Publishing Platform; 2020.
● Papadakis MA, McPhee SJ, Rabow MW. Current Medical
Diagnosis & Treatment 2018. New York: McGraw-Hill
Education; 2017.
● Jameson JL, Fauci AS, Kasper DL, Hauser SL, Longo DL,
Loscalzo J. Harrison's Principles of Internal Medicine, Twentieth
Edition (Vol.1 & Vol.2). McGraw-Hill Education / Medical; 2018
● Marieb EN, Hoehn K. Anatomy & Physiology. Hoboken, NJ:
Pearson; 2020.
● Boron WF, Boulpaep EL. Medical Physiology.; 2017.
Netter FH, Felten DL, Józefowicz Ralph F. Netter's Atlas of Human
● Neuroscience. Teterboro, NJ: Icon Learning Systems; 2004.
● Netter FH. Atlas of Human Anatomy. Amsterdam: Elsevier;
2018.
● Westover MB. Pocket Neurology. Lippincott Williams & Wilkins;
2016.
● Guyton and Hall Textbook of Medical Physiology. Philadelphia,
PA: Elsevier; 2021.
TRIGEMINAL NERVE | CRANIAL NERVE V NEURO PHYSIOLOGY: Note #52. 7 of 7
You might also like
- Advance Statistics ProjectDocument9 pagesAdvance Statistics Projectrishit100% (9)
- The Esthetic Biological Contour Concept (Blatz) (2021)Document12 pagesThe Esthetic Biological Contour Concept (Blatz) (2021)Sofia Avila86% (7)
- Acute PancreatitisDocument31 pagesAcute PancreatitisAmoroso, Marian Corneth D.No ratings yet
- Maxillary Injection Techniques PPT I Sas 11-14Document45 pagesMaxillary Injection Techniques PPT I Sas 11-14mavirosemandawe08No ratings yet
- MCQs PDFDocument234 pagesMCQs PDFPeter Osundwa Kiteki100% (4)
- HEENT Cheat SheetDocument22 pagesHEENT Cheat SheetKatrina FeriNo ratings yet
- 2023.neuroscience - Trans10.posterior Fossa Level Brainstem Cranial Nuclei and NervesDocument7 pages2023.neuroscience - Trans10.posterior Fossa Level Brainstem Cranial Nuclei and NervesstellaNo ratings yet
- The Brainstem: Ot1024: NeuroscienceDocument6 pagesThe Brainstem: Ot1024: NeuroscienceReyna MedinaNo ratings yet
- 115 - Neurology Physiology) Oculomotor Nerve - Cranial Nerve IIIDocument6 pages115 - Neurology Physiology) Oculomotor Nerve - Cranial Nerve IIIUssama MDNo ratings yet
- Preparing For The PANCEDocument46 pagesPreparing For The PANCEJay plNo ratings yet
- Neuron Anatomy & Function AtfDocument5 pagesNeuron Anatomy & Function AtfGavin MuhammadNo ratings yet
- The Audio PANCE and PANRE Episode 23 - The Physician Assistant LifeDocument5 pagesThe Audio PANCE and PANRE Episode 23 - The Physician Assistant LifeThe Physician Assistant LifeNo ratings yet
- Blood Supply of BrainDocument15 pagesBlood Supply of Braincdeepak71No ratings yet
- 132 - Neurology Pathology - Stroke Syndromes - MCA, ACA, ICA, PCA, Vertebrobasilar Artery SDocument4 pages132 - Neurology Pathology - Stroke Syndromes - MCA, ACA, ICA, PCA, Vertebrobasilar Artery SUsman AR VainceNo ratings yet
- 7th Grade Tri 2 Infectious DiseasesDocument3 pages7th Grade Tri 2 Infectious Diseasesapi-278126127No ratings yet
- Critical Care: Version 2 (2020)Document56 pagesCritical Care: Version 2 (2020)yazzNo ratings yet
- Medical MneumonicsDocument139 pagesMedical MneumonicsdrtpkNo ratings yet
- 4 Cerebellum 2022Document40 pages4 Cerebellum 2022Gregory Wiggins100% (1)
- Open Folder 07. NeurologyDocument5 pagesOpen Folder 07. NeurologyAfrah AbdulNo ratings yet
- Lesson AssignmentDocument22 pagesLesson AssignmentFatima AzziffNo ratings yet
- CVS Physiology - 220505 - 061700Document131 pagesCVS Physiology - 220505 - 061700Jinnah SheriffNo ratings yet
- IM 3A PE Cardiology Dr. JumangitDocument12 pagesIM 3A PE Cardiology Dr. JumangitCzara DyNo ratings yet
- 140 - Neurology Pathology) Seizures - Etiology, Pathophysiology, Clinical Features, Treatment, ComplicationsDocument10 pages140 - Neurology Pathology) Seizures - Etiology, Pathophysiology, Clinical Features, Treatment, ComplicationsUssama MDNo ratings yet
- Cardiac ExaminationDocument23 pagesCardiac ExaminationAreza Eka PermanaNo ratings yet
- 3.0 Grand Physiology Finals Compilation - Batch 2017Document89 pages3.0 Grand Physiology Finals Compilation - Batch 2017Sheryl Layne Lao-SebrioNo ratings yet
- Vertebral Arteries, and Their Divisions. Arteries Fuse To Form The Basilar ArteryDocument6 pagesVertebral Arteries, and Their Divisions. Arteries Fuse To Form The Basilar Arterymurali_bharadwazNo ratings yet
- Diagnoses and Management Acute Headache Emergency DepartmentDocument37 pagesDiagnoses and Management Acute Headache Emergency DepartmentBendy Dwi IrawanNo ratings yet
- Cardiovascular SystemDocument58 pagesCardiovascular Systemsultan khabeebNo ratings yet
- Cerebral Aneurysm: Junchen ZhangDocument37 pagesCerebral Aneurysm: Junchen ZhangsanjivdasNo ratings yet
- CVS, Respi Heent ExamDocument8 pagesCVS, Respi Heent ExamDranreb Berylle MasangkayNo ratings yet
- EmergencyDocument86 pagesEmergencyyazzNo ratings yet
- Chapter 21 AddqDocument12 pagesChapter 21 AddqLenel John Giban Bagunas100% (1)
- HEART MURMURS by NISHDocument41 pagesHEART MURMURS by NISHurtikikeNo ratings yet
- Day-17-Pedigree Analysis Answer Key: Generation-IDocument2 pagesDay-17-Pedigree Analysis Answer Key: Generation-IalishNo ratings yet
- Step 1: Lecture NotesDocument7 pagesStep 1: Lecture NotesHo Hoang VuNo ratings yet
- Co PDFDocument4 pagesCo PDFReginaJacobNo ratings yet
- Manual of Common Bedside Surgical Procedures-CHAPTER 6 Neurosurgical ProceduresDocument30 pagesManual of Common Bedside Surgical Procedures-CHAPTER 6 Neurosurgical ProceduresCosti TanaseNo ratings yet
- Lecture 6 Cardiovascular: Vascular System - The HemodynamicsDocument70 pagesLecture 6 Cardiovascular: Vascular System - The HemodynamicsAndreea ŞtefănescuNo ratings yet
- Inguinal CanalDocument4 pagesInguinal CanalspiraldaoNo ratings yet
- Thyroid Examination and ThyroidectomyDocument9 pagesThyroid Examination and ThyroidectomyAhmadNo ratings yet
- PANCE or PANRE PA Exam What Do Zebras Have To Do With My SuccessDocument2 pagesPANCE or PANRE PA Exam What Do Zebras Have To Do With My SuccessHELP PANCE PANRE Online PA Exam Review CourseNo ratings yet
- Trochlear Nerve Cranial Nerve IV AtfDocument4 pagesTrochlear Nerve Cranial Nerve IV AtfRishi VermaNo ratings yet
- Accessory Nerve: Cranial Nerve XIDocument3 pagesAccessory Nerve: Cranial Nerve XIRubin kasmiNo ratings yet
- Accessory Nerve - Cranial Nerve XI AtfDocument3 pagesAccessory Nerve - Cranial Nerve XI AtfCathy SolivarNo ratings yet
- Abducens Nerve Cranial Nerve VI AtfDocument4 pagesAbducens Nerve Cranial Nerve VI AtfAfrah AbdulNo ratings yet
- 094 - Neurology Physiology) Descending Tracts - Corticobulbar TractDocument3 pages094 - Neurology Physiology) Descending Tracts - Corticobulbar TractNikki Lin LiuNo ratings yet
- 084 - Neurology Physiology) Medulla Anatomy & FunctionDocument14 pages084 - Neurology Physiology) Medulla Anatomy & Functionice.bear.wolfoNo ratings yet
- Abducens Nerve - Cranial Nerve VI AtfDocument4 pagesAbducens Nerve - Cranial Nerve VI AtfCathy SolivarNo ratings yet
- Vagus Nerve Cranial Nerve X AtfDocument3 pagesVagus Nerve Cranial Nerve X AtfRishi VermaNo ratings yet
- Cranial Nerve III - Oculomotor Nerve - FRCEM SuccessDocument1 pageCranial Nerve III - Oculomotor Nerve - FRCEM SuccessJohn CoxNo ratings yet
- Anatomy AssignmentDocument10 pagesAnatomy AssignmentObansa JohnNo ratings yet
- Pinna or Auricle (Fig. 31.1) : Ssion)Document12 pagesPinna or Auricle (Fig. 31.1) : Ssion)Myat NyanNo ratings yet
- Handout Cranial NervesDocument95 pagesHandout Cranial NervesWongelNo ratings yet
- Edited Handout Cranial Nerves & Tastebude Olafactory EpitheliumDocument139 pagesEdited Handout Cranial Nerves & Tastebude Olafactory EpitheliumWongelNo ratings yet
- Cranial Nerves - AADocument71 pagesCranial Nerves - AARaif RizqullahNo ratings yet
- Neurology - Hypoglossal Nerve - CN XIIDocument3 pagesNeurology - Hypoglossal Nerve - CN XIIRubin kasmiNo ratings yet
- Brainstem Lesions Trans 2019 PDFDocument8 pagesBrainstem Lesions Trans 2019 PDFVon HippoNo ratings yet
- Lecture 1: NeuroembryologyDocument13 pagesLecture 1: NeuroembryologyRaul Docto100% (1)
- Tutor 16.2 GRACE NASYA (18-091) 4BDocument92 pagesTutor 16.2 GRACE NASYA (18-091) 4BGrace HerlisNo ratings yet
- Upper Motor Neuron Vs Lower Motor Neuron AtfDocument4 pagesUpper Motor Neuron Vs Lower Motor Neuron AtfRishi Verma100% (1)
- 6.nerves of Head and NeckDocument36 pages6.nerves of Head and NeckDr P N N ReddyNo ratings yet
- Chapter 3 Anatomical Organization of Cranial Nerves 2009 Manual Therapy For The Cranial NervesDocument4 pagesChapter 3 Anatomical Organization of Cranial Nerves 2009 Manual Therapy For The Cranial NervesDaniela Bustos PéndolaNo ratings yet
- Spinal Cord (3 of 5)Document24 pagesSpinal Cord (3 of 5)j53934762No ratings yet
- Foramen Structures Conducted Cranial Fossa Cranial Bone Cribriform ForaminaDocument8 pagesForamen Structures Conducted Cranial Fossa Cranial Bone Cribriform ForaminaAchiever FayeNo ratings yet
- 24 Month JADAfissealantsibelDocument10 pages24 Month JADAfissealantsibelDani BrenerNo ratings yet
- OMSB 9 Nov 2018Document3 pagesOMSB 9 Nov 2018Subhajit SahaNo ratings yet
- Trigeminal Nerve FinalDocument101 pagesTrigeminal Nerve FinalShraddha PatilNo ratings yet
- Pedodontic TriangleDocument3 pagesPedodontic Triangleewretrdf0% (1)
- Classification of Instruments Used in Operative DentistryDocument19 pagesClassification of Instruments Used in Operative Dentistryدكتور فاروقNo ratings yet
- Materiais Alinhadores EstéticosDocument3 pagesMateriais Alinhadores EstéticosDr FernandoNo ratings yet
- Sivakumar 2012Document5 pagesSivakumar 2012Adriiana Jaimes JaimesNo ratings yet
- A Review of Implant Abutments - Abutment Classification To Aid Prosthetic Selection. Karunagaran 2013Document6 pagesA Review of Implant Abutments - Abutment Classification To Aid Prosthetic Selection. Karunagaran 2013Sofi Fuentes CarboneNo ratings yet
- Swinglock DentureDocument7 pagesSwinglock DentureLouis HutahaeanNo ratings yet
- Jurnal Tara SyifaDocument4 pagesJurnal Tara SyifaMuhammad Fauzan IhsanNo ratings yet
- Lecture3Y4S7 ENGDocument25 pagesLecture3Y4S7 ENGShany SchwarzwaldNo ratings yet
- Proteze MobileDocument12 pagesProteze MobileAndreea IoanaNo ratings yet
- Mechanical Evaluation of Peek Compared With Zirconia As A Dental Implant MaterialDocument6 pagesMechanical Evaluation of Peek Compared With Zirconia As A Dental Implant MaterialDiaa M. ZahranNo ratings yet
- The Caries ProcessDocument4 pagesThe Caries ProcessAdriiana Jaimes JaimesNo ratings yet
- Four Rooted Maxillary Third Molar A Case Report ofDocument3 pagesFour Rooted Maxillary Third Molar A Case Report ofghinaNo ratings yet
- Appropriate Oral Health CareDocument21 pagesAppropriate Oral Health CareSupriya BhataraNo ratings yet
- Adhesive Cementation Protocol of Zirconia RestorationsDocument6 pagesAdhesive Cementation Protocol of Zirconia RestorationsStefan PopescuNo ratings yet
- Articulo American Academy of Pediatric Pediatric Restorative DentistryDocument14 pagesArticulo American Academy of Pediatric Pediatric Restorative DentistrykbladimirzmNo ratings yet
- Lec 7 BondingDocument8 pagesLec 7 BondingAbdur RehmanNo ratings yet
- Prevention Strategies For Periodontal Disease - Chapter 16Document10 pagesPrevention Strategies For Periodontal Disease - Chapter 16Daniah MNo ratings yet
- Health6 - q1 - Mod5 - Identifies Community Health Resources and Facilities - FINAL.Document24 pagesHealth6 - q1 - Mod5 - Identifies Community Health Resources and Facilities - FINAL.vamps sier100% (1)
- Muscles of Facial ExpressionDocument3 pagesMuscles of Facial ExpressionJOHN HAROLD CABRADILLANo ratings yet
- IMB633-PDF-ENG - Positioning and BehavoirDocument12 pagesIMB633-PDF-ENG - Positioning and Behavoir2301389No ratings yet
- Textbook Ebook Advanced Dental Biomaterials Khurshid All Chapter PDFDocument43 pagesTextbook Ebook Advanced Dental Biomaterials Khurshid All Chapter PDFdollie.serrano826100% (9)
- Using Shimbashi Number and CephalometricDocument8 pagesUsing Shimbashi Number and Cephalometricsolodont1No ratings yet
- Ohi Case StudyDocument11 pagesOhi Case Studyapi-308499727100% (1)