Professional Documents
Culture Documents
Oral Pyogenic Granuloma: A Case Report: March 2014
Oral Pyogenic Granuloma: A Case Report: March 2014
Uploaded by
lisa triwardhaniOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Oral Pyogenic Granuloma: A Case Report: March 2014
Oral Pyogenic Granuloma: A Case Report: March 2014
Uploaded by
lisa triwardhaniCopyright:
Available Formats
See discussions, stats, and author profiles for this publication at: https://www.researchgate.
net/publication/315494717
ORAL PYOGENIC GRANULOMA: A CASE REPORT
Article · March 2014
CITATIONS READS
4 182
3 authors:
Swati Kejriwal Rahul Bhandary
4 PUBLICATIONS 35 CITATIONS
Nitte University
15 PUBLICATIONS 67 CITATIONS
SEE PROFILE
SEE PROFILE
Biju Thomas
A.B. Shetty Memorial Institute of Dental Science
185 PUBLICATIONS 528 CITATIONS
SEE PROFILE
Some of the authors of this publication are also working on these related projects:
Periodontics View project
Evaluation of serum and salivary sialic acid and nitric oxide level in chronic periodontitis patients View project
All content following this page was uploaded by Biju Thomas on 15 September 2018.
The user has requested enhancement of the downloaded file.
NUJHS Vol. 4, No.1, March 2014, ISSN 2249-7110
Nitte University Journal of Health Science
Case Report
ORAL PYOGENIC GRANULOMA: A CASE REPORT
1 2 3
Swati Kejriwal , Rahul Bhandary & Biju Thomas
1 2 3
P.G. Student, Professor, Professor & HOD, Department of Periodontics
A.B. Shetty Memorial Institute of Dental Sciences, Nitte University, Deralakatte, Mangalore - 575 018
Correspondence:
Swati Kejriwal
P.G. Student, Department of Periodontics, A.B.Shetty Memorial Institute of Dental Sciences
Nitte University, Deralakatte, Mangalore - 575 018. Karnataka. E-mail : drswatikejriwal@gmail.com
Abstract:
Pyogenic granuloma is an inflammatory hyperplasia affecting the oral tissues. It is a tumour-like growth of the oral cavity, which usually
arises in response to nonspecific infection. Because of the high frequency of pyogenic granuloma in the oral cavity, this case report
describes a pyogenic granuloma in a 59-year-old male patient, discussing the clinical features and histopathologic features that
distinguish this lesion from other similar oral mucosa lesions and also the successful management of the lesion.
Keywords: Pyogenic granuloma, Hyperplasia, granuloma pyogenicum.
Introduction : associated with the growth which increased on chewing
The term “Pyogenic granuloma” or “granuloma food. Medical history was non contributory. Intraoral
1
pyogenicum” was introduced by Hartzell in 1904. It is a examination revealed a solitary red exophytic,
hyperactive benign inflammatory lesion commonly seen in pedunculated growth on the gingiva measuring about 1.5 x
the oral cavity with gingiva being the most common 2 x 1cm present in relation to distal aspect of 47 (Fig. 1) . On
affected site followed by buccal mucosa, tongue and lips. palpation, inspectory findings were confirmed. The growth
was firm on palpation, non tender with absence of
It usually arises in response to various stimuli such as low-
discharge. Bleeding on provocation was positive. Oral
grade local irritation, traumatic injury, hormonal factors, or
hygiene was poor with calculus and stains. Complete
certain kinds of drugs.2 Pyogenic granuloma (PG) may occur
hemogram showed all blood counts within normal limits.
in all age groups, though it is predominantly seen in young
Intraoral periapical radiograph (IOPAR) revealed no
females in the second decade of life because of the
abnormalities (Fig. 2). Oral prophylaxis was performed. In
hormonal changes in this period.2 This article reports the
addition, chemical plaque control measures were advised
case of a 59-year-old male patient with pyogenic
in the form of 0.2% chlorhexidine gluconate mouthwash, to
granuloma successfully managed by surgical intervention.
be used twice daily. Excisional biopsy was performed under
Case Report: local anesthesia and sent for histopathologic examination.
A 59-year-old male patient reported to the Department of Histopathological examination showed a hyperplastic,
Periodontics with a complaint of growth in the lower right parakeratinized stratified squamous epithelium. The
back region of the mouth since 2 months. The growth was connective tissue was loose fibrillar and comprised of
initially small in size and slowly growing attaining the numerous proliferating capillaries, dense mixed
present size. The patient inflammatory infiltrate, and extravasated red blood cells
Access this article online
gave history of a similar (Fig. 3,4). The histopathological examination confirmed the
Quick Response Code
lesion 5 months back for clinical diagnosis of Pyogenic granuloma. The patient was
which the patient had recalled after a week and the excised area was evaluated
undergone surgical excision for healing. Healing was satisfactory. The patient was
3 months back. Patient recalled periodically at two weeks, 1 month, three months
reported discomfort and six months. At each visit, oral prophylaxis and oral
Keywords: Pyogenic granuloma, Hyperplasia, granuloma 123
pyogenicum. - Swati Kejriwal
NUJHS Vol. 4, No.1, March 2014, ISSN 2249-7110
Nitte University Journal of Health Science
hygiene instructions were reinforced. Even after six
months, there was no recurrence of the lesion (Fig.5).
Fig.4: Photomicrograph showing epithelium and
connective tissue (H & E stain, 40X magnification).
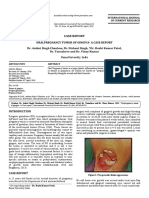
Fig.1: Pre-operative photograph showing the lesion distal
to 47
Fig.2: Intraoral periapical radiograph.
Fig.5: Six months postoperative view
Discussion :
Gingival enlargement is defined as an increase in size of the
gingiva. Depending on etiologic factors, gingival
enlargement can be of many types like inflammation, drug
induced effects, neoplasm, hormonal imbalance, non
specific conditioned enlargement and systemic
involvement like Leukemia, Wegener's granulomatosis
etc.2 Nonspecific conditioned enlargement, or pyogenic
Fig.3: Photomicrograph showing hyperplastic,
granuloma, is a benign, localized mass of exuberant
parakeratinized stratified squamous epithelium and
connective tissue with numerous proliferating capillaries, granulation tissue. It is considered as an exaggerated
dense mixed inflammatory infiltrate, and extravasated red conditioned response to minor trauma or chronic
blood cells (H & E stain, 4X magnification).
irritation.3 However, the term is a misnomer since the
condition is not associated with pus formation and does
Keywords: Pyogenic granuloma, Hyperplasia, granuloma 124
pyogenicum. - Swati Kejriwal
NUJHS Vol. 4, No.1, March 2014, ISSN 2249-7110
Nitte University Journal of Health Science
not represent a granuloma histologically. 4 PG is PG may be confused with other benign and malignant
predominantly seen in the second decade of life though it conditions because of its appearance and evolution of
2
may occur in all age groups. In contrast, Epivatianos et al growth; hence, biopsy findings are important in
reported that the average patient age was 52 years with a establishing diagnosis.2The clinical and histopathological
peak incidence of occurrence in the sixth decade of life.5 In finding led to a final diagnosis of PG. Treatment of PG
the present case, the patient was 59 years old. Oral PG involves a complete surgical excision. After excision,
shows a predilection for the gingiva accounting for 75% of recurrence rate has been reported in up to 16% of lesions.
6
all cases followed by buccal mucosa, tongue and lips. Here, Recurrence is believed to result from incomplete excision,
the lesion was present on the gingiva distal of 47. Rarely, PG failure to remove etiologic factors, or re-injury of the area.
7
may cause significant bone loss. Here, IOPAR revealed no Also gingival lesions show a much higher recurrence rate
abnormalities. Studies have shown that PG may occur as a than lesions from other oral mucosal sites.6 Here the
result of an exaggerated localized connective tissue patient gave history of similar lesion which was excised 3
reaction to a minor injury or any underlying irritation. The months back. The patient was recalled for regular
irritating factor can be poor oral hygiene, nonspecific maintenance visits, and after 6 months of the treatment
infection, over hanging restorations, cheek biting etc. there was no recurrence seen.
Because of this irritation, the underlying fibrovascular
Conclusion:
connective tissue becomes hyperplastic and there is
From the present case report it is concluded that pyogenic
proliferation of granulation tissue which leads to the
granuloma can be adequately treated with the correct
formation of a pyogenic granuloma.8 In the present case,
diagnosis and proper treatment planning. A careful
patient's oral hygiene was poor. Chronic irritation resulting
management of the lesion also helps in preventing the
from accumulated plaque and calculus could have
recurrence of this benign lesion.
contributed to the development of PG.
References:
1. Hartzell MB. Granuloma pyogenicum. J Cutan Dis Syph 1904;22:520-
525.
2. Sumanth Shivaswamy, Nazia Siddiqui, A. Sanjay Jain, Ajit Koshy, Sonal
Tambwekar, Akhil Shankar. A rare case of generalized pyogenic
granuloma: A case report. Quintessence Int 2011;42:493–499.
3. Ningappa Chinnannavar Sangamesh, Bellguppa Poornima, Kodige
Chandrashekar Vidya, Santosh Bhopal Sakri. Extragingival pyogenic
granuloma: A rare case report. Journal of the Scientific Society
2013;40(1):49-51.
4. Reet Kamal, Parveen Dahiya, Abhiney Puri. Oral pyogenic granuloma:
various concepts of etiopathogenesis. Journal of Oral and
Maxillofacial Pathology 2012;16(1):79-82.
5. Epivatianos A, Antoniades D, Zaraboukas T, Zairi E, Poulopoulos A,
Kiziridou A, Iordanidis S. Pyogenic granuloma of the oral cavity:
comparative study of its clinicopathological and
immunohistochemical features. Pathol Int 2005;55:391-7.
6. Hamid Jafarzadeh, Majid Sanatkhani, Nooshin Mohtasham. Oral
pyogenic granuloma: a review. Journal of Oral Science 2006;48(4):167-
175.
7. Goodman-Topper ED, Bimstein E. Pyogenic granuloma as a cause of
bone loss in a twelve-year-old child: report of case. ASDC J Dent Child
1994;61:65-67.
8. Pushpendra Kumar Verma, Ruchi Srivastava, HC Baranwal, TP
Chaturvedi, Anju Gautam, Amit Singh. Pyogenic Granuloma -
Hyperplastic Lesion of the Gingiva: Case Reports. Open Dent J. 2012;
6: 153–156.
Keywords: Pyogenic granuloma, Hyperplasia, granuloma 125
pyogenicum. - Swati Kejriwal
View publication stats
You might also like
- Caterpillar 910 Wheel LoaderDocument4 pagesCaterpillar 910 Wheel LoaderAya Mariati100% (1)
- The Joker and The Queen - Ed Sheeran Piano-Vocal-GuitarDocument3 pagesThe Joker and The Queen - Ed Sheeran Piano-Vocal-GuitarAngela HallNo ratings yet
- Turbocharger PresentationDocument18 pagesTurbocharger PresentationShrwan Gyawali100% (3)
- Hospital Management System SrsDocument71 pagesHospital Management System SrsYash Kapoor77% (13)
- Unusual Case of Postpartum Gingival Enlargement: Diagnosis and ManagementDocument5 pagesUnusual Case of Postpartum Gingival Enlargement: Diagnosis and ManagementAzizah Nurul HusnaNo ratings yet
- 10 Squamouspapilloma-ReportoftwocasesDocument7 pages10 Squamouspapilloma-ReportoftwocasesAyik DarkerThan BlackNo ratings yet
- Focal Reactive OvergrowthsDocument5 pagesFocal Reactive OvergrowthsLjubomirErdoglijaNo ratings yet
- Granuloma ArticleDocument3 pagesGranuloma ArticleRamanpreet KourNo ratings yet
- Tangible Results Following Scaling and Root Planing in Treating: Generalized Aggressive Periodontitis (GAP) - A Case ReportDocument8 pagesTangible Results Following Scaling and Root Planing in Treating: Generalized Aggressive Periodontitis (GAP) - A Case ReportDeanita PutriNo ratings yet
- Inflammatory Gingival Enlargement and Management: A Case ReportDocument4 pagesInflammatory Gingival Enlargement and Management: A Case ReportErfinaNo ratings yet
- Management of Puberty Associated Gingival Enlargement in An Adolescent Female - A Case Report With A Follow-Up of 1 YearDocument4 pagesManagement of Puberty Associated Gingival Enlargement in An Adolescent Female - A Case Report With A Follow-Up of 1 YearDha Dina SevofrationNo ratings yet
- Cappillary HemangiomaDocument4 pagesCappillary HemangiomaANUP LAL RAJBAHAKNo ratings yet
- Pyogenic Granuloma A Case ReportDocument9 pagesPyogenic Granuloma A Case ReportSafira HlwNo ratings yet
- October 2018 1538385165 481 PDFDocument4 pagesOctober 2018 1538385165 481 PDFKiyRizkikaNo ratings yet
- Case Report: Rama University, IndiaDocument2 pagesCase Report: Rama University, IndiaPutri YingNo ratings yet
- Assessment of Alveolar Bone Augmentation in Intrabony Defects Employing Platelet-Rich Fibrin (PRF) Membrane and Sticky Bone (Injectable-PRF & Demineralized Freeze-Dried Bone Graft) - A Case ReportDocument4 pagesAssessment of Alveolar Bone Augmentation in Intrabony Defects Employing Platelet-Rich Fibrin (PRF) Membrane and Sticky Bone (Injectable-PRF & Demineralized Freeze-Dried Bone Graft) - A Case ReportInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- JORGaggingDF PDFDocument8 pagesJORGaggingDF PDFCrisu CrisuuNo ratings yet
- JOHCD PregnancyAssociatedGingivalEnlargementDocument5 pagesJOHCD PregnancyAssociatedGingivalEnlargementAZWAN RAHMADHAN PUTRANo ratings yet
- PeriodontitisDocument14 pagesPeriodontitisDanni MontielNo ratings yet
- 04 Ravneet KRandhawapolishingDocument9 pages04 Ravneet KRandhawapolishingLatifa Hanif ZuhriNo ratings yet
- Full-Mouth Rehabilitation of Worn Dentition by HobDocument9 pagesFull-Mouth Rehabilitation of Worn Dentition by Hobdea swastikaNo ratings yet
- Endoscopic Findings of The Gastric Mucosa During Long Term Use of Proton Pump Inhibitor A Multicenter StudyDocument6 pagesEndoscopic Findings of The Gastric Mucosa During Long Term Use of Proton Pump Inhibitor A Multicenter StudySamuel0651No ratings yet
- Management of Puberty Associated Gingival Enlargement in The Aesthetic Zone in An Adolescent FemaleDocument3 pagesManagement of Puberty Associated Gingival Enlargement in The Aesthetic Zone in An Adolescent Femalehelen mrbnNo ratings yet
- Epidemiology of Secondary Peritonitis: Analysis of 545 CasesDocument6 pagesEpidemiology of Secondary Peritonitis: Analysis of 545 CasesIntan KarmilaNo ratings yet
- Warthins Tumorof Parotid GlandDocument5 pagesWarthins Tumorof Parotid GlandWahyuni NaharuddinNo ratings yet
- Gingival Epulis: Report of Two Cases.: Dr. Praful Choudhari, Dr. Praneeta KambleDocument5 pagesGingival Epulis: Report of Two Cases.: Dr. Praful Choudhari, Dr. Praneeta KambleAnandNo ratings yet
- CR 4Document4 pagesCR 4Fitrah AndiNo ratings yet
- Evaluation of Effects of 1.2% Atorvastatin As A Local Drug Delivery: A Randomized Controlled Clinical StudyDocument8 pagesEvaluation of Effects of 1.2% Atorvastatin As A Local Drug Delivery: A Randomized Controlled Clinical StudyIJAR JOURNALNo ratings yet
- Sahrmann 2010Document12 pagesSahrmann 2010Dragos CiongaruNo ratings yet
- Ramesh Amitha Local Drug Delivery in PeriodontalDocument6 pagesRamesh Amitha Local Drug Delivery in Periodontalsobhan hajianNo ratings yet
- PregnancyTumor GeneralDentistryDocument4 pagesPregnancyTumor GeneralDentistryNguyên TrầnNo ratings yet
- Evaluation of Role of Oxitard Capsules in The Treatment of OSMFDocument5 pagesEvaluation of Role of Oxitard Capsules in The Treatment of OSMFsevattapillaiNo ratings yet
- JIndianSocPeriodontol214326-4026404 010706Document3 pagesJIndianSocPeriodontol214326-4026404 010706Fatma HandayaniNo ratings yet
- Ars Lan 2019Document3 pagesArs Lan 2019khadidja BOUTOUILNo ratings yet
- Lobular Capillary Hemangioma of TongueDocument3 pagesLobular Capillary Hemangioma of TongueShreya DasguptaNo ratings yet
- Pyogenic Granuloma A Clinicopathological AnalysisDocument4 pagesPyogenic Granuloma A Clinicopathological AnalysisconsendoNo ratings yet
- Journal of Periodontology - 2018 - Lang - Periodontal HealthDocument8 pagesJournal of Periodontology - 2018 - Lang - Periodontal HealthMonica MartínezNo ratings yet
- Lo Han Guo FruitDocument9 pagesLo Han Guo FruitInten KusumaNo ratings yet
- Caz PatologieDocument5 pagesCaz PatologieBarbulescu Anca DianaNo ratings yet
- Kees Tra 2014Document21 pagesKees Tra 2014Marco Antonio García LunaNo ratings yet
- Art 2Document21 pagesArt 2xdxdxdxdNo ratings yet
- 10 1093@qjmed@hcx164 PDFDocument2 pages10 1093@qjmed@hcx164 PDFAida Juniati SyafniNo ratings yet
- Two Cases of An Atypical Presentation of Necrotizing StomatitisDocument5 pagesTwo Cases of An Atypical Presentation of Necrotizing StomatitisSamehada SamaNo ratings yet
- Apgh 3 1Document2 pagesApgh 3 1Rashmi Ranjan BeheraNo ratings yet
- OperculectomyDocument4 pagesOperculectomyshania arifinNo ratings yet
- Granuloma Pyogenicum - A Case ReportDocument4 pagesGranuloma Pyogenicum - A Case ReportInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Fissure DilationDocument5 pagesFissure DilationIbrahim AlmoosaNo ratings yet
- Clinical Efficacy of Local Delivered Minocycline in The Treatment of Chronic Periodontitis Smoker PatientsDocument5 pagesClinical Efficacy of Local Delivered Minocycline in The Treatment of Chronic Periodontitis Smoker PatientsvivigaitanNo ratings yet
- KuretaseDocument3 pagesKuretaserindaNo ratings yet
- Journal of Drug Discovery and Therapeutics 1 (4) 2013, 01-02Document2 pagesJournal of Drug Discovery and Therapeutics 1 (4) 2013, 01-02Bayu SaputroNo ratings yet
- Case Report AnugDocument6 pagesCase Report AnugAzi Pertiwi HussainNo ratings yet
- Clinical Trial of Regeneration of Aged Vocal Folds With Growth Factor TherapyDocument5 pagesClinical Trial of Regeneration of Aged Vocal Folds With Growth Factor Therapydr.hungsonNo ratings yet
- Efficacy of Photodynamic Therapy and Periodontal TDocument10 pagesEfficacy of Photodynamic Therapy and Periodontal Thafizhuddin muhammadNo ratings yet
- The New Periodontal Disease Classification: Analysis and ReviewDocument6 pagesThe New Periodontal Disease Classification: Analysis and ReviewRuxandra FitaNo ratings yet
- Risk Assessment: A Mandatory Evaluation and Analysis of Periodontal Tissue in General Population - A SurveyDocument7 pagesRisk Assessment: A Mandatory Evaluation and Analysis of Periodontal Tissue in General Population - A SurveyAnonymous izrFWiQNo ratings yet
- Low Lying Fistula-In-Ano - Fistulotomy or FistulectomyDocument4 pagesLow Lying Fistula-In-Ano - Fistulotomy or FistulectomyApjhs ApjhsNo ratings yet
- Periodontal Health: Niklaus P. Lang P. Mark BartoldDocument8 pagesPeriodontal Health: Niklaus P. Lang P. Mark BartoldChristine LomuntadNo ratings yet
- The Epidemiology, Antibiotic Resistance and Post-Discharge Course of Peritonsillar Abscesses in London, OntarioDocument7 pagesThe Epidemiology, Antibiotic Resistance and Post-Discharge Course of Peritonsillar Abscesses in London, OntarioMaharaniNo ratings yet
- Atrophican Rhinitis JournalDocument8 pagesAtrophican Rhinitis JournalYola SurbaktiNo ratings yet
- KeratitisDocument11 pagesKeratitisAnonymous mvNUtwidNo ratings yet
- Acute Urinary Retention in An Adolescent Girl Secondary To Hematocolpos: A Case ReportDocument3 pagesAcute Urinary Retention in An Adolescent Girl Secondary To Hematocolpos: A Case ReportLailatuz ZakiyahNo ratings yet
- Hyaluronic Acid As An Adjunct After Scaling and Root Planing A Prospective Randomized Clinical TrialDocument9 pagesHyaluronic Acid As An Adjunct After Scaling and Root Planing A Prospective Randomized Clinical TrialAdriana Segura DomínguezNo ratings yet
- A Systematic Review of Non-Surgical Management in Peyronie S DiseaseDocument11 pagesA Systematic Review of Non-Surgical Management in Peyronie S DiseaseJad DegheiliNo ratings yet
- Post-cholecystectomy Bile Duct InjuryFrom EverandPost-cholecystectomy Bile Duct InjuryVinay K. KapoorNo ratings yet
- Empowerment DLP (August 01, 2019)Document2 pagesEmpowerment DLP (August 01, 2019)Clars Ramos Beldad100% (2)
- Online Library PowerPoint TemplatesDocument49 pagesOnline Library PowerPoint Templateskhozin albatawiNo ratings yet
- Classification of CementDocument7 pagesClassification of CementMonzer HussainNo ratings yet
- ACN Micro Project-1Document23 pagesACN Micro Project-1ashutosh dudhaneNo ratings yet
- Brazil Ventilaton MineDocument6 pagesBrazil Ventilaton MineNaufi SyifaNo ratings yet
- Torbela v. Sps. Rosario Banco Filipino G.R. No. 140528Document17 pagesTorbela v. Sps. Rosario Banco Filipino G.R. No. 140528Ace MereriaNo ratings yet
- RA RME LUCENA Apr2018 PDFDocument8 pagesRA RME LUCENA Apr2018 PDFPhilBoardResultsNo ratings yet
- The Sociology of C. Wright Mills: Max WeberDocument16 pagesThe Sociology of C. Wright Mills: Max WeberMuhammad YaseenNo ratings yet
- Ai in EduDocument14 pagesAi in EduKang YihyunNo ratings yet
- Aircraft Conformity WorksheetDocument14 pagesAircraft Conformity WorksheetMarcus DragoNo ratings yet
- 3 Ways To View Your Shared Folders in Windows (All Versions) - Digital CitizenDocument7 pages3 Ways To View Your Shared Folders in Windows (All Versions) - Digital CitizenSelvakumar RNo ratings yet
- Husqvarna TC 142T - 96051014600 (2016-08) Parts Diagram For CHASSIS - FRAMEDocument7 pagesHusqvarna TC 142T - 96051014600 (2016-08) Parts Diagram For CHASSIS - FRAMEmarcos garciaNo ratings yet
- Palawan BranchesDocument28 pagesPalawan Branchesxdmhundz9990% (1)
- Rakes vs. Atlantic GulfDocument2 pagesRakes vs. Atlantic GulfPia SarconNo ratings yet
- People of The Philippines Vs Honesto Dimagiba y WayanDocument4 pagesPeople of The Philippines Vs Honesto Dimagiba y WayanCherry Merce S. TanNo ratings yet
- Nanotechnology Military Applications 16 PDFDocument2 pagesNanotechnology Military Applications 16 PDFLUIS GONZALEZ PEREZNo ratings yet
- Mitchell e Villet, 1987 - Reinforcement of Earth Slopes and EmbankmentsDocument330 pagesMitchell e Villet, 1987 - Reinforcement of Earth Slopes and EmbankmentsJordana Furman100% (1)
- Glossary of Pharmaceutical TermsDocument140 pagesGlossary of Pharmaceutical Termsmohammed goudaNo ratings yet
- TERPS PANS-OPS Approach Brief With Circling Considerations - NBAADocument39 pagesTERPS PANS-OPS Approach Brief With Circling Considerations - NBAAMos DetNo ratings yet
- Crankshaft Alignment MeasurementDocument1 pageCrankshaft Alignment MeasurementmohamedNo ratings yet
- Lab Policies KOH Prep For Fungal Elements Affiliate Lab 8649 4Document3 pagesLab Policies KOH Prep For Fungal Elements Affiliate Lab 8649 4Geby JeonNo ratings yet
- Social Responsibility Theory FixDocument8 pagesSocial Responsibility Theory Fixsyifa fauziahNo ratings yet
- Rudolf Elmer's Complaint To The ECHR v. Jersey (Standard Bank)Document13 pagesRudolf Elmer's Complaint To The ECHR v. Jersey (Standard Bank)David LeloupNo ratings yet
- Product GuideDocument52 pagesProduct GuidePham Cao ThanhNo ratings yet
- 2nd Quarter Exam Gen MathDocument5 pages2nd Quarter Exam Gen Mathargie joy marie100% (1)
- Textbook Materials - ch9Document35 pagesTextbook Materials - ch9OZZYMANNo ratings yet