Professional Documents
Culture Documents
100%(1)100% found this document useful (1 vote)
19 viewsMaternity and Newborn Nursing Reviewer
Maternity and Newborn Nursing Reviewer
Uploaded by
Cherubim Lei DC FloresImplantation of the blastocyte in the endometrium usually occurs 7 to 9 days after fertilization. During the first trimester of pregnancy from days 14 to 56, organogenesis occurs. Breastfeeding offers infants the benefit of maternal antibodies unlike formula. A breastfeeding mother should allow her infant to breastfeed until satisfied, which may vary from 5 to 20 minutes.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You might also like
- Test Bank For Maternity Nursing 8th Edition, LowdermilkDocument26 pagesTest Bank For Maternity Nursing 8th Edition, LowdermilkILL101100% (3)
- A Community Diagnosis in Level III Group 2Document89 pagesA Community Diagnosis in Level III Group 2Jenny Agustin FabrosNo ratings yet
- Imagine Me Gone by Adam HaslettDocument271 pagesImagine Me Gone by Adam HaslettCherubim Lei DC Flores100% (2)
- Drug Study Augmentin-KidapawanDocument2 pagesDrug Study Augmentin-KidapawanCherubim Lei DC FloresNo ratings yet
- Maternity and Newborn Nursing ReviewerDocument12 pagesMaternity and Newborn Nursing ReviewerCherubim Lei DC FloresNo ratings yet
- Maternity and Newborn Nursing ReviewerDocument20 pagesMaternity and Newborn Nursing ReviewerNick Realino100% (1)
- Med Surg 2 BulletsDocument19 pagesMed Surg 2 BulletsShiraishiNo ratings yet
- Med Surg Chapter 65 Flashcards - QuizletDocument17 pagesMed Surg Chapter 65 Flashcards - QuizletMonica JubaneNo ratings yet
- NCM 106 - DRUG and IVF CALCULATIONS - VIOSDocument3 pagesNCM 106 - DRUG and IVF CALCULATIONS - VIOSIra Velle ViosNo ratings yet
- Drug Administration MIdterm ExamDocument8 pagesDrug Administration MIdterm ExamRettsu GamingNo ratings yet
- COMPETENCY Summary Evaluation Sheet 1Document8 pagesCOMPETENCY Summary Evaluation Sheet 1Rellora Mark AndreiNo ratings yet
- OB - Postterm PregnancyDocument6 pagesOB - Postterm PregnancyDarren Mae MosadaNo ratings yet
- Pharma Long Quiz KeyDocument3 pagesPharma Long Quiz KeyBiatch NebturaNo ratings yet
- Ortho Supplemental NotesDocument6 pagesOrtho Supplemental Notestanya merdeNo ratings yet
- 4.3 InfectiousDocument29 pages4.3 InfectiousJohn Anthony de GùzmanNo ratings yet
- Medical AbbreviationDocument9 pagesMedical AbbreviationDjayNo ratings yet
- Medication and Administration C.NDocument286 pagesMedication and Administration C.NJaleto sunkemoNo ratings yet
- Nclex Bank QuestionsDocument43 pagesNclex Bank QuestionsJANIELA RITCHEL DANIELNo ratings yet
- Maths Numerical Assignment With AnswersDocument3 pagesMaths Numerical Assignment With AnswersAiman SiddiquiNo ratings yet
- Ante Natal Care - 2Document43 pagesAnte Natal Care - 2Dina M ElbakaryNo ratings yet
- Medical Asepsis (Handwashing) Parameters Score 5 4 3 2 1Document36 pagesMedical Asepsis (Handwashing) Parameters Score 5 4 3 2 1Cathrine Mae RamilNo ratings yet
- Generic: Hydromorphone (SC) Brand Name: DilaudidDocument1 pageGeneric: Hydromorphone (SC) Brand Name: DilaudidPreet ChahalNo ratings yet
- Pharma Handouts Rev 3Document34 pagesPharma Handouts Rev 3Aphrill Pearl PacisNo ratings yet
- biophysical-WPS OfficeDocument13 pagesbiophysical-WPS OfficeSandhya GuptaNo ratings yet
- Common Pediatric DisordersDocument2 pagesCommon Pediatric DisordersJean ReyesNo ratings yet
- Icu FlowsheetDocument4 pagesIcu FlowsheetdedeandikaNo ratings yet
- Report Authoring GuideDocument178 pagesReport Authoring GuideabhishekNo ratings yet
- NCM 212 - Dosage CalculationsDocument7 pagesNCM 212 - Dosage CalculationsLYRIZZA LEA BHEA DESIATANo ratings yet
- Med Surge 1Document39 pagesMed Surge 1rave andrei MacanayaNo ratings yet
- Cal Misbah Test 2016 Qa PDFDocument51 pagesCal Misbah Test 2016 Qa PDFSyedKashifAliNo ratings yet
- Maternal/Ob Notes: "Above Success There Is Excellence Beyond Impossible. " Skei Nursing Review & EnhancementDocument53 pagesMaternal/Ob Notes: "Above Success There Is Excellence Beyond Impossible. " Skei Nursing Review & EnhancementAbdullah, Atteya100% (1)
- CP100MEDICALtermPSAbbr. 2Document78 pagesCP100MEDICALtermPSAbbr. 2RAISA N. RASIDNo ratings yet
- Mabini Colleges Inc. College of Midwifery and NursingDocument3 pagesMabini Colleges Inc. College of Midwifery and NursingEmerald IsleNo ratings yet
- NCLEX Review Question 101-200Document14 pagesNCLEX Review Question 101-200Felimon BugtongNo ratings yet
- Growth and DevelopmentDocument32 pagesGrowth and DevelopmentHumera MisterNo ratings yet
- Haad ReviwerDocument20 pagesHaad ReviwerAnjo TranateNo ratings yet
- Module 7 Student Activity SheetDocument7 pagesModule 7 Student Activity SheetJenny Agustin FabrosNo ratings yet
- Understanding Cancer: Jasmin Saragena BetinolDocument104 pagesUnderstanding Cancer: Jasmin Saragena BetinolERAN MARK ROJASNo ratings yet
- Pediatric Medication: Facilitator: Rubina Kousar RN, RM, BSCN Post RNDocument53 pagesPediatric Medication: Facilitator: Rubina Kousar RN, RM, BSCN Post RNRubinaNo ratings yet
- Subcutaneous InjectionDocument16 pagesSubcutaneous InjectionNani KicchaNo ratings yet
- Nursing Care of Clients With Upper Airway or Respiratory DisordersDocument6 pagesNursing Care of Clients With Upper Airway or Respiratory DisordersLuna MarieNo ratings yet
- MCN HandoutsDocument22 pagesMCN HandoutsFRANCYM PRINCESSRICH BATENGANo ratings yet
- Disorders of PancreasDocument41 pagesDisorders of PancreasAbdullah BhattiNo ratings yet
- Routes of Drug Administration and Dosage FormsDocument39 pagesRoutes of Drug Administration and Dosage FormsAditya RathoreNo ratings yet
- Ncma 219 Rle Midterm ReviewerDocument19 pagesNcma 219 Rle Midterm ReviewerAruxi Yoshi100% (1)
- Mohammed H. Eid - The Intensivist-Middle East & ElMarwa For Publishing & Distribution, GN (2019)Document372 pagesMohammed H. Eid - The Intensivist-Middle East & ElMarwa For Publishing & Distribution, GN (2019)Mohamed Moussa100% (1)
- Pointers To ReviewDocument18 pagesPointers To ReviewHegi Ann AlcalaNo ratings yet
- Pressure InjuriesDocument1 pagePressure InjuriesPaola OrtizNo ratings yet
- Pharmacology Drug Dosage CalculationsDocument54 pagesPharmacology Drug Dosage CalculationsMichelle FigueroaNo ratings yet
- NCM 109 SKILLS LAB DAY 5.3 Catheterization22Document33 pagesNCM 109 SKILLS LAB DAY 5.3 Catheterization22Joseph DusichNo ratings yet
- MEDICATION ADMINISTRATION StudentsDocument53 pagesMEDICATION ADMINISTRATION StudentsMary Ann G. CorsanesNo ratings yet
- Postpartal PeriodDocument32 pagesPostpartal PeriodCharrise VoluntadNo ratings yet
- Micro Microbial Mechanisms of Pathogenicity NOTESDocument6 pagesMicro Microbial Mechanisms of Pathogenicity NOTESAriane NobleNo ratings yet
- Lewis - HeartMedical-Surgical Nursing Flashcards - QuizletDocument55 pagesLewis - HeartMedical-Surgical Nursing Flashcards - QuizletNursyNurseNo ratings yet
- 8th Mid McqsDocument25 pages8th Mid McqsMuhammad Uzair GujjarNo ratings yet
- Oxytocin and Other Drugs Acting On UterusDocument37 pagesOxytocin and Other Drugs Acting On UterusRamadi PrameelaNo ratings yet
- NCLEX Practice Questions: D. AspirinDocument15 pagesNCLEX Practice Questions: D. AspirinJackie AbarraNo ratings yet
- Midterm Exam PCT LecDocument5 pagesMidterm Exam PCT LecRichard OcampoNo ratings yet
- DRUG StudyDocument8 pagesDRUG StudyRhobic ManansalaNo ratings yet
- Blood Transfusion and Its ComplicationsDocument31 pagesBlood Transfusion and Its ComplicationsSaima Hasnain MinhasNo ratings yet
- Basic Maternity ConceptsDocument14 pagesBasic Maternity ConceptsDivine Grace Arreglo AbingNo ratings yet
- MCN ReviewerDocument27 pagesMCN ReviewerTresha LabayosNo ratings yet
- Organogenesis Occurs During The First Trimester of Pregnancy, Specifically, Days 14 To 56 ofDocument11 pagesOrganogenesis Occurs During The First Trimester of Pregnancy, Specifically, Days 14 To 56 ofRhea Lyn LamosteNo ratings yet
- Maternity and Newborn Nursing ReviewerDocument12 pagesMaternity and Newborn Nursing ReviewerCherubim Lei DC FloresNo ratings yet
- Paranoid Schizophrenia NCPDocument8 pagesParanoid Schizophrenia NCPCherubim Lei DC Flores75% (4)
- I. Nursing Care Plan Assessment Diagnosis Planning Intervention Evaluation Goal Partially MetDocument3 pagesI. Nursing Care Plan Assessment Diagnosis Planning Intervention Evaluation Goal Partially MetCherubim Lei DC FloresNo ratings yet
- BSN4 NvcfiDocument1 pageBSN4 NvcfiCherubim Lei DC FloresNo ratings yet
- North Valley College Foundation Cover FormatDocument2 pagesNorth Valley College Foundation Cover FormatCherubim Lei DC FloresNo ratings yet
- Case Study For Paranoid SchizophreniaDocument30 pagesCase Study For Paranoid SchizophreniaCherubim Lei DC FloresNo ratings yet
- NCP Drug Study Final Paranoid SchizophreniaDocument11 pagesNCP Drug Study Final Paranoid SchizophreniaCherubim Lei DC FloresNo ratings yet
- I. Nursing Care Plan Assessment Diagnosis Planning Intervention EvaluationDocument4 pagesI. Nursing Care Plan Assessment Diagnosis Planning Intervention EvaluationCherubim Lei DC FloresNo ratings yet
- A Beautiful Mind SummaryDocument2 pagesA Beautiful Mind SummaryCherubim Lei DC FloresNo ratings yet
- I. Nursing Care Plan Assessment Diagnosis Planning Intervention EvaluationDocument3 pagesI. Nursing Care Plan Assessment Diagnosis Planning Intervention EvaluationCherubim Lei DC FloresNo ratings yet
- Nursing Psychiatric Case StudyDocument19 pagesNursing Psychiatric Case StudyCherubim Lei DC FloresNo ratings yet
- Rizal Book by Zayde 2nd EditionDocument207 pagesRizal Book by Zayde 2nd EditionCherubim Lei DC FloresNo ratings yet
- Drug Study For AsthmaDocument4 pagesDrug Study For AsthmaCherubim Lei DC FloresNo ratings yet
- Subjective Objective Assessment Planning Nursing Intervention Rationale EvaluationDocument7 pagesSubjective Objective Assessment Planning Nursing Intervention Rationale EvaluationCherubim Lei DC FloresNo ratings yet
- Pinaka Final NresDocument28 pagesPinaka Final NresCherubim Lei DC FloresNo ratings yet
- I. Nursing Care Plan Assessment Diagnosis Planning Intervention EvaluationDocument3 pagesI. Nursing Care Plan Assessment Diagnosis Planning Intervention EvaluationCherubim Lei DC FloresNo ratings yet
- Paranoid Schizophrenia Case StudyDocument33 pagesParanoid Schizophrenia Case StudyCherubim Lei DC Flores50% (4)
- Dawwwwwwwwwwwwwwww PDFDocument442 pagesDawwwwwwwwwwwwwwww PDFCherubim Lei DC FloresNo ratings yet
- 10 Nursing TheoristsDocument6 pages10 Nursing TheoristsCherubim Lei DC FloresNo ratings yet
- PrognosisDocument3 pagesPrognosisCherubim Lei DC FloresNo ratings yet
- Pinaka Final NresDocument28 pagesPinaka Final NresCherubim Lei DC FloresNo ratings yet
- Blastocyst ANA 205Document27 pagesBlastocyst ANA 205Ogundipe olorunfemiNo ratings yet
- 2ND Q Grade 5 Epp and ScienceDocument7 pages2ND Q Grade 5 Epp and ScienceHAZEL JANE BAGUIONo ratings yet
- Norethisterone JournalDocument29 pagesNorethisterone JournalAditya Syah PutraNo ratings yet
- 20 Perimenopause & MenopauseDocument14 pages20 Perimenopause & MenopauseGirum SolomonNo ratings yet
- Final Obstetrics and GynacologyDocument88 pagesFinal Obstetrics and Gynacologysis8100% (2)
- 0308 Repro101Document3 pages0308 Repro101thidingNo ratings yet
- Fuck Better A Simple Guide To Superior SexDocument86 pagesFuck Better A Simple Guide To Superior SexMarc Joel80% (5)
- Medicine Lecture 1 - History Taking (Colored)Document4 pagesMedicine Lecture 1 - History Taking (Colored)miguel cuevas100% (2)
- Science10 q3 Mod2 Week2 Menstrual-Cycle-Version-3Document24 pagesScience10 q3 Mod2 Week2 Menstrual-Cycle-Version-3nadia doropanNo ratings yet
- The Menstrual Cycle ForDocument4 pagesThe Menstrual Cycle ForAngelica Calamba CalicaNo ratings yet
- Human Reproduction Neet Special BioDocument75 pagesHuman Reproduction Neet Special BioAnil KumarNo ratings yet
- Cambridge IGCSE: BIOLOGY 0610/42Document20 pagesCambridge IGCSE: BIOLOGY 0610/42Tanish KanojiaNo ratings yet
- Ethical Concerns Relating To Taking Birth Control PillsDocument8 pagesEthical Concerns Relating To Taking Birth Control PillsMichael MbithiNo ratings yet
- Nle Notes MCNDocument33 pagesNle Notes MCNjosephmary09No ratings yet
- Reproductive System Notes - 2014-15 DraftDocument62 pagesReproductive System Notes - 2014-15 DraftMiguel MenendezNo ratings yet
- Maternity Nursing ReviewDocument37 pagesMaternity Nursing Reviewshenric16No ratings yet
- Embryology Chapter 3Document23 pagesEmbryology Chapter 3Abdisamed AllaaleNo ratings yet
- Normal Menstrual CycleDocument28 pagesNormal Menstrual CycleCristóbal Concha100% (1)
- SituationdDocument64 pagesSituationdIvory SantiagoNo ratings yet
- Premenstrual Syndrome (PMS)Document4 pagesPremenstrual Syndrome (PMS)Nick BantoloNo ratings yet
- 1Document21 pages1beatrice.laalNo ratings yet
- Optimize The Stages of Your Menstrual CycleDocument11 pagesOptimize The Stages of Your Menstrual CycleAnabel VizcarraNo ratings yet
- Science Short Notes Grade 10Document32 pagesScience Short Notes Grade 10Mallindu PereraNo ratings yet
- CombinepdfDocument40 pagesCombinepdfShaira UntalanNo ratings yet
- 2 Study of Female Pelvic Pain ..Document69 pages2 Study of Female Pelvic Pain ..Ghofran Ibrahim HassanNo ratings yet
- Grade 8 Integrated Science Week 2 Lesson 2Document5 pagesGrade 8 Integrated Science Week 2 Lesson 2Balram HaroldNo ratings yet
- Midterm Module SocSci 111Document40 pagesMidterm Module SocSci 111Frances Georgina FabaleNo ratings yet
- Greendale-1999-The MenopauseDocument10 pagesGreendale-1999-The MenopauseRya RatnaNo ratings yet
- IMAT 2015 - Shuffled - EdiSESDocument31 pagesIMAT 2015 - Shuffled - EdiSESSalvatore SinatraNo ratings yet
Maternity and Newborn Nursing Reviewer
Maternity and Newborn Nursing Reviewer
Uploaded by
Cherubim Lei DC Flores100%(1)100% found this document useful (1 vote)
19 views21 pagesImplantation of the blastocyte in the endometrium usually occurs 7 to 9 days after fertilization. During the first trimester of pregnancy from days 14 to 56, organogenesis occurs. Breastfeeding offers infants the benefit of maternal antibodies unlike formula. A breastfeeding mother should allow her infant to breastfeed until satisfied, which may vary from 5 to 20 minutes.
Original Description:
Maternity and Newborn Nursing Reviewer
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentImplantation of the blastocyte in the endometrium usually occurs 7 to 9 days after fertilization. During the first trimester of pregnancy from days 14 to 56, organogenesis occurs. Breastfeeding offers infants the benefit of maternal antibodies unlike formula. A breastfeeding mother should allow her infant to breastfeed until satisfied, which may vary from 5 to 20 minutes.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
100%(1)100% found this document useful (1 vote)
19 views21 pagesMaternity and Newborn Nursing Reviewer
Maternity and Newborn Nursing Reviewer
Uploaded by
Cherubim Lei DC FloresImplantation of the blastocyte in the endometrium usually occurs 7 to 9 days after fertilization. During the first trimester of pregnancy from days 14 to 56, organogenesis occurs. Breastfeeding offers infants the benefit of maternal antibodies unlike formula. A breastfeeding mother should allow her infant to breastfeed until satisfied, which may vary from 5 to 20 minutes.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
Download as pdf or txt
You are on page 1of 21
Maternity and Newborn Nursing Reviewer 12.
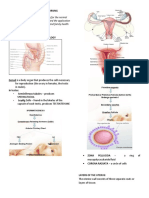
Implantation occurs when the
cellular walls of the blastocyte
implants itself in the
Basic Maternity Concepts endometrium, usually 7 to 9
days after fertilization.
1. The male sperm contributes an
X or a Y chromosome; the
female ovum contributes an X
chromosome. 13. Heart development in the
2. Fertilization produces a total of embryo begins at 2 to 4 weeks
46 chromosomes, including an and is complete by the end of
XY combination (male) or an XX the embryonic stage.
combination (female). Menstruation
3. Organogenesis occurs during the
first trimester of pregnancy, 14. If a patient misses a menstrual
specifically, days 14 to 56 of period while taking an oral
gestation. contraceptive exactly as
4. Implantation in the uterus prescribed, she should continue
occurs 6 to 10 days after ovum taking the contraceptive.
fertilization. 15. The first menstrual flow is called
5. The chorion is the outermost menarche and may be
extraembryonic membrane that anovulatory (infertile).
gives rise to the placenta. Breastfeeding
6. The corpus luteum secretes
large quantities 16. When both breasts are used
of progesterone. for breastfeeding, the infant
7. From the 8th week of usually doesn’t empty the
gestation through delivery, the second breast. Therefore, the
developing cells are known as a second breast should be used
fetus. first at the next feeding.
8. The union of a male and a 17. Stress, dehydration,
female gamete produces a and fatigue may reduce a
zygote, which divides into the breastfeeding mother’s milk
fertilized ovum. supply.
9. Spermatozoa (or their 18. To help a mother break the
fragments) remain in the vagina suction of her breastfeeding
for 72 hours after sexual infant, the nurse should teach
intercourse. her to insert a finger at the
10. If the ovum is fertilized by a corner of the infant’s mouth.
spermatozoon carrying a Y 19. Cow’s milk shouldn’t be given to
chromosome, a male zygote is infants younger than age one
formed. (1) because it has a low linoleic
11. Implantation occurs when the acid content and its protein is
cellular walls of the blastocyte difficult for infants to digest.
implants itself in the 20. A woman who is breastfeeding
endometrium, usually 7 to 9 should rub a mild emollient
days after fertilization. cream or a few drops of breast
milk (or colostrum) on the
nipples after each feeding. She Neonatal Care
should let the breasts air-dry to
prevent them from cracking. 32. The initial weight loss for a
21. Breastfeeding mothers should healthy neonate is 5% to 10% of
increase their fluid intake to 2½ birth weight.
to 3 qt (2,500 to 3,000 ml) daily. 33. The normal hemoglobin value in
22. After feeding an infant with neonates is 17 to 20 g/dl.
a cleft lip or palate, the nurse 34. The circumference of a
should rinse the infant’s mouth neonate’s head is normally 2 to
with sterile water. 3 cm greater than the
23. Human immunodeficiency virus circumference of the chest.
(HIV) has been cultured in 35. After delivery, the first nursing
breast milk and can be action is to establish the
transmitted by an HIV-positive neonate’s airway.
mother who breast-feeds her 36. The specific gravity of a
infant. neonate’s urine is 1.003 to
24. Colostrum, the precursor of 1.030. A lower specific gravity
milk, is the first secretion from suggests overhydration; a
the breasts after delivery. higher one
25. A mother should allow her suggests dehydration.
infant to breastfeed until the 37. During the first hour after birth
infant is satisfied. The time may (the period of reactivity),
vary from 5 to 20 minutes. the neonate is alert and awake.
26. Most drugs that a breastfeeding 38. The neonatal period extends
mother takes appear in breast from birth to day 28. It’s also
milk. called the first four (4) weeks or
27. Prolactin stimulates and first month of life.
sustains milk production. 39. A low-birth-weight
28. Breastfeeding of a premature neonate weighs 2,500 g (5 lb 8
neonate born at 32 weeks oz) or less at birth.
gestation can be accomplished 40. A very-low-birth-weight
if the mother expresses milk neonate weighs 1,500 g (3 lb 5
and feeds the neonate by oz) or less at birth.
gavage. 41. Administering high levels of
29. A mother who has a positive oxygen to a premature neonate
human immunodeficiency virus can cause blindness as a result
test result shouldn’t breastfeed of retrolental fibroplasia.
her infant. 42. An Apgar score of 7 to 10
30. Hot compresses can help to indicates no immediate distress,
relieve breast tenderness after 4 to 6 indicates moderate
breastfeeding. distress, and 0 to 3 indicates
31. Unlike formula, breast milk severe distress.
offers the benefit of maternal 43. To elicit Moro’s reflex, the nurse
antibodies. holds the neonate in both hands
and suddenly, but gently, drops
the neonate’s head backward.
Normally, the neonate abducts
and extends all extremities
bilaterally and symmetrically, 52. The nurse should count a
forms a C shape with the thumb neonate’s respirations for
and forefinger, and first adducts one (1) full minute.
and then flexes the extremities. 53. Chlorpromazine (Thorazine) is
44. An Apgar score of 7 to 10 used to treat neonates who are
indicates no immediate distress, addicted to narcotics.
4 to 6 indicates moderate 54. The nurse should provide a
distress, and 0 to 3 indicates dark, quiet environment for a
severe distress. neonate who is
45. If jaundice is suspected in a experiencing narcotic
neonate, the nurse should withdrawal.
examine the infant under 55. Drugs used to treat withdrawal
natural window light. If natural symptoms in neonates
light is unavailable, the nurse include phenobarbital (Luminal),
should examine the infant camphorated opium tincture
under a white light. (paregoric), and diazepam
46. Vitamin K is administered to (Valium).
neonates to prevent 56. In a premature neonate, signs
hemorrhagic disorders because of respiratory distress include
a neonate’s intestine can’t nostril flaring, substernal
synthesize vitamin K. retractions, and inspiratory
47. Variability is any change in the grunting.
fetal heart rate (FHR) from its 57. Respiratory distress
normal rate of 120 to 160 syndrome (hyaline membrane
beats/minute. Acceleration is disease) develops in premature
increased FHR; deceleration is infants because their pulmonary
decreased FHR. alveoli lack surfactant.
48. Fetal alcohol syndrome presents 58. Whenever an infant is being put
in the first 24 hours after birth down to sleep, the parent or
and produces lethargy, seizures, caregiver should position
poor sucking reflex, abdominal the infant on the back.
distention, and respiratory Remember the mnemonic “back
difficulty. to sleep.”
49. In a neonate, the symptoms 59. The percentage of water in a
of heroin withdrawal may begin neonate’s body is about 78% to
several hours to 4 days after 80%.
birth. 60. To perform nasotracheal
50. In a neonate, the symptoms suctioning in an infant, the
of methadone withdrawal may nurse positions the infant with
begin 7 days to several weeks his neck slightly hyperextended
after birth. in a “sniffing” position, with his
51. In a neonate, the cardinal signs chin up and his head tilted back
of narcotic withdrawal include slightly.
coarse, flapping tremors; 61. After birth, the neonate’s
sleepiness; restlessness; umbilical cord is tied 1″ (2.5 cm)
prolonged, persistent, high- from the abdominal wall with a
pitched cry; and irritability. cotton cord, plastic clamp, or
rubber band.
62. When teaching parents to radiant warmer. In a radiant
provide umbilical cord care, the warmer, a heat-sensitive probe
nurse should teach them to taped to the neonate’s skin
clean the umbilical area with a activates the heater unit
cotton ball saturated with automatically to maintain the
alcohol after every diaper desired temperature.
change to prevent infection and 70. Neonates who are delivered
promote drying. by cesarean birth have a higher
63. Ortolani’s sign (an audible click incidence of respiratory distress
or palpable jerk that occurs with syndrome.
thigh abduction) confirms 71. When providing phototherapy
congenital hip dislocation in a to a neonate, the nurse should
neonate. cover the neonate’s eyes and
64. Cutis marmorata is mottling or genital area.
purple discoloration of the skin. 72. The narcotic antagonist
It’s a transient vasomotor naloxone (Narcan) may be given
response that occurs primarily to a neonate to correct
in the arms and legs of infants respiratory depression caused
who are exposed to cold. by narcotic administration to
65. The first immunization for a the mother during labor.
neonate is the hepatitis 73. In a neonate, symptoms of
B vaccine, which is administered respiratory distress syndrome
in the nursery shortly after include expiratory grunting or
birth. whining, sandpaper breath
66. Infants with Down sounds, and seesaw retractions.
syndrome typically have marked 74. Cerebral palsy presents as
hypotonia, floppiness, slanted asymmetrical movement,
eyes, excess skin on the back of irritability, and excessive, feeble
the neck, flattened bridge of the crying in a long, thin infant.
nose, flat facial features, spade- 75. The nurse should assess a
like hands, short and broad feet, breech-birth neonate
small male genitalia, absence of for hydrocephalus, hematomas,
Moro’s reflex, and a simian fractures, and other anomalies
crease on the hands. caused by birth trauma.
67. The nurse 76. In a neonate, long, brittle
instills erythromycin in a fingernails are a sign of
neonate’s eyes primarily to postmaturity.
prevent blindness caused by 77. Desquamation (skin peeling) is
gonorrhea or chlamydia. common in postmature
68. A fever in the first 24 neonates.
hours postpartum is most likely 78. The average birth weight of
caused by dehydration rather neonates born to mothers who
than infection. smoke is 6 oz (170 g) less than
69. Preterm neonates or neonates that of neonates born to
who can’t maintain a skin nonsmoking mothers.
temperature of at least 97.6° F 79. Neonatal jaundice in the first 24
(36.4° C) should receive care in hours after birth is known as
an incubator (Isolette) or a
pathological jaundice and is a minute and 5 minutes after
sign of erythroblastosis fetalis. delivery. The score is based on
80. Lanugo covers the fetus’s body respiratory effort, heart
until about 20 weeks gestation. rate, muscle tone, reflex
Then it begins to disappear from irritability, and color.
the face, trunk, arms, and legs, 91. Erythromycin is given at birth to
in that order. prevent ophthalmia
81. In a neonatorum.
neonate, hypoglycemia causes 92. In the neonate, the
temperature instability, normal blood glucose level is 45
hypotonia, jitteriness, and to 90 mg/dl.
seizures. Premature, 93. Hepatitis B vaccine is usually
postmature, small-for- given within 48 hours of birth.
gestational-age, and large-for- 94. Hepatitis B immune globulin is
gestational-age neonates are usually given within 12 hours of
susceptible to this disorder. birth.
82. Neonates typically need to 95. Boys who are born
consume 50 to 55 cal per pound with hypospadias shouldn’t be
of body weight daily. circumcised at birth because the
83. During fetal heart rate foreskin may be needed for
monitoring, variable constructive surgery.
decelerations indicate 96. In neonates, cold stress affects
compression or prolapse of the the circulatory, regulatory, and
umbilical cord. respiratory systems.
84. A neonate whose mother 97. Fetal embodiment is a maternal
has diabetes should be assessed developmental task that occurs
for hyperinsulinism. in the second trimester. During
85. The best technique for assessing this stage, the mother may
jaundice in a neonate is to complain that she never gets to
blanch the tip of the nose or the sleep because the fetus always
area just above the umbilicus. gives her a thump when she
86. Milia may occur as pinpoint tries.
spots over a neonate’s nose. 98. Mongolian spots can range from
87. Strabismus is a normal finding in brown to blue. Their color
a neonate. depends on how close
88. Respiratory distress syndrome melanocytes are to the surface
develops in premature neonates of the skin. They most
because their alveoli lack commonly appear as patches
surfactant. across the sacrum, buttocks,
89. Rubella infection in a pregnant and legs.
patient, especially during the 99. Mongolian spots are common in
first trimester, can lead to non-white infants and usually
spontaneous abortion or stillbirt disappear by age 2 to 3 years.
h as well as fetal cardiac and 100. Vernix caseosa is a
other birth defects. cheeselike substance that
90. The Apgar score is used to covers and protects the fetus’s
assess the neonate’s vital skin in utero. It may be rubbed
functions. It’s obtained at 1 into the neonate’s skin or
washed away in one or two to the heart, resulting in supine
baths. hypotensive syndrome, or
101. Caput succedaneum is inferior vena cava syndrome.
edema that develops in and 109. Tocolytic agents used to
under the fetal scalp during treat preterm labor
labor and delivery. It resolves include terbutaline (Brethine),
spontaneously and presents no ritodrine (Yutopar), and
danger to the neonate. The magnesium sulfate.
edema doesn’t cross the suture 110. A pregnant woman who
line. has hyperemesis gravidarum
102. Nevus flammeus, or may require hospitalization to
port-wine stain, is a diffuse pink treat dehydration and
to dark bluish red lesion on a starvation.
neonate’s face or neck. 111. Diaphragmatic hernia is
103. The Guthrie test (a one of the most urgent neonatal
screening test surgical emergencies. By
for phenylketonuria) is most compressing and displacing the
reliable if it’s done between the lungs and heart, this disorder
second and sixth days after birth can cause respiratory distress
and is performed after the shortly after birth.
neonate has ingested protein. 112. Common complications
104. To assess coordination of early pregnancy (up to 20
of sucking and swallowing, the weeks gestation) include fetal
nurse should observe the loss and serious threats to
neonate’s first breastfeeding or maternal health.
sterile water bottle-feeding. 113. If the neonate is stable,
105. To establish a milk the mother should be allowed
supply pattern, the mother to breast-feed within the
should breast-feed her infant at neonate’s first hour of life.
least every 4 hours. During the 114. The nurse should check
first month, she should breast- the neonate’s temperature
feed 8 to 12 times daily every 1 to 2 hours until it’s
(demand feeding). maintained within normal limits.
106. To avoid contact with At birth, a neonate normally
blood and other body fluids, the weighs 5 to 9 lb (2 to 4 kg),
nurse should wear gloves when measures 18″ to 22″ (45.5 to 56
handling the neonate until after cm) in length, has a head
the first bath is given. circumference of 13½” to 14″
107. If a breast-fed infant is (34 to 35.5 cm), and has a chest
content, has good skin turgor, circumference that’s 1″ (2.5 cm)
an adequate number of wet less than the head
diapers, and normal weight circumference.
gain, the mother’s milk supply is 115. In the neonate,
assumed to be adequate. temperature normally ranges
108. In the supine position, a from 98° to 99° F (36.7° to 37.2°
pregnant patient’s enlarged C), apical pulse rate averages
uterus impairs venous return 120 to 160 beats/minute, and
from the lower half of the body
respirations are 40 to 60 124. Because of the anti-
breaths/minute. insulin effects of placental
116. The diamond-shaped hormones, insulin requirements
anterior fontanel usually closes increase during the third
between ages 12 and 18 trimester.
months. The triangular posterior 125. Gestational age can be
fontanel usually closes by age 2 estimated by ultrasound
months. measurement of maternal
117. In the neonate, a abdominal circumference, fetal
straight spine is normal. A tuft femur length, and fetal head
of hair over the spine is an size. These measurements are
abnormal finding. most accurate between 12 and
118. Prostaglandin gel may 18 weeks gestation.
be applied to the vagina or 126. Skeletal
cervix to ripen an unfavorable system abnormalities and
cervix before labor induction ventricular septal defects are
with oxytocin (Pitocin). the most common disorders of
119. Supernumerary nipples infants who are born to diabetic
are occasionally seen on women. The incidence of
neonates. They usually appear congenital malformation is
along a line that runs from each three times higher in these
axilla, through the normal infants than in those born to
nipple area, and to the groin. nondiabetic women.
120. Meconium is a material 127. Skeletal system
that collects in the fetus’s abnormalities and ventricular
intestines and forms the septal defects are the most
neonate’s first feces, which are common disorders of infants
black and tarry. who are born to diabetic
121. The presence of women. The incidence of
meconium in the amniotic fluid congenital malformation is
during labor indicates possible three times higher in these
fetal distress and the need to infants than in those born to
evaluate the neonate for nondiabetic women.
meconium aspiration. 128. The patient
122. To assess a with preeclampsia usually has
neonate’s rooting reflex, the puffiness around the eyes or
nurse touches a finger to the edema in the hands (for
cheek or the corner of the example, “I can’t put my
mouth. Normally, the neonate wedding ring on.”).
turns his head toward the 129. Kegel exercises require
stimulus, opens his mouth, and contraction and relaxation of
searches for the stimulus. the perineal muscles. These
123. Harlequin sign is exercises help strengthen pelvic
present when a neonate who is muscles and improve urine
lying on his side appears red on control in postpartum patients.
the dependent side and pale on 130. Symptoms
the upper side. of postpartum depression range
from mild postpartum blues to
intense, 139. Lightening is settling of
suicidal, depressive psychosis. the fetal head into the brim of
131. The preterm neonate the pelvis.
may require gavage feedings Prenatal Care
because of a weak sucking
reflex, uncoordinated sucking, 140. In a full-term neonate,
or respiratory distress. skin creases appear over two-
132. Acrocyanosis (blueness thirds of the neonate’s feet.
and coolness of the arms and Preterm neonates have heel
legs) is normal in neonates creases that cover less than
because of their immature two-thirds of the feet.
peripheral circulatory system. 141. At 20 weeks gestation,
133. To prevent ophthalmia the fundus is at the level of the
neonatorum (a umbilicus.
severe eye infection caused by 142. At 36 weeks gestation,
maternal gonorrhea), the nurse the fundus is at the lower
may administer one of three border of the rib cage.
drugs, as prescribed, in the 143. A premature neonate is
neonate’s eyes: tetracycline, one born before the end of the
silver nitrate, or erythromycin. 37th week of gestation.
Neonatal testing for 144. Gravida is the number
phenylketonuria is mandatory in of pregnancies a woman has
most states. had, regardless of outcome.
134. The nurse should place 145. Para is the number of
the neonate in a 30-degree pregnancies that reached
Trendelenburg position to viability, regardless of whether
facilitate mucus drainage. the fetus was delivered alive or
135. The nurse may suction stillborn. A fetus is considered
the neonate’s nose and mouth viable at 20 weeks gestation.
as needed with a bulb syringe or 146. A multipara is a woman
suction trap. who has had two or more
136. To prevent heat loss, pregnancies that progressed to
the nurse should place the viability, regardless of whether
neonate under a radiant the offspring were alive at birth.
warmer during suctioning and 147. Positive signs of
initial delivery-room care, and pregnancy include ultrasound
then wrap the neonate in a evidence, fetal heart tones, and
warmed blanket for transport to fetal movement felt by the
the nursery. examiner (not usually present
137. The umbilical cord until 4 months gestation
normally has two arteries and 148. Quickening, a
one vein. presumptive sign of pregnancy,
138. When providing care, occurs between 16 and 19
the nurse should expose only weeks gestation.
one part of an infant’s body at a 149. Goodell’s sign is
time. softening of the cervix.
150. Quickening, a
presumptive sign of pregnancy,
occurs between 16 and 19 160. Linea nigra, a dark line
weeks gestation. that extends from the umbilicus
151. Ovulation ceases during to the mons pubis, commonly
pregnancy. appears during pregnancy and
152. Immunity to rubella can disappears after pregnancy.
be measured by 161. Culdoscopy is
a hemagglutination inhibition visualization of the pelvic organs
test (rubella titer). This test through the posterior vaginal
identifies exposure to rubella fornix.
infection and determines 162. The nurse should teach
susceptibility in pregnant a pregnant vegetarian to obtain
women. In a woman, a titer protein from alternative
greater than 1:8 indicates sources, such as nuts, soybeans,
immunity. and legumes.
153. To estimate the date of 163. The nurse should
delivery using Naegele’s rule, instruct a pregnant patient to
the nurse counts backward take only prescribed prenatal
three (3) months from the first vitamins because over-the-
day of the last menstrual period counter high-potency vitamins
and then adds seven (7) days to may harm the fetus.
this date. 164. High-sodium foods can
154. During pregnancy, cause fluid retention, especially
weight gain averages 25 to 30 lb in pregnant patients.
(11 to 13.5 kg). 165. A pregnant patient can
155. Rubella has a avoid constipation and
teratogenic effect on the fetus hemorrhoids by adding fiber to
during the first trimester. It her diet.
produces abnormalities in up to 166. A pregnant woman
40% of cases without should drink at least eight 8-oz
interrupting the pregnancy. glasses (about 2,000 ml) of
156. At 12 weeks gestation, water daily.
the fundus should be at the top 167. Cytomegalovirus is the
of the symphysis pubis. leading cause of congenital viral
157. Chloasma, the mask of infection.
pregnancy, is pigmentation of a 168. Tocolytic therapy is
circumscribed area of skin indicated in premature labor,
(usually over the bridge of the but contraindicated in fetal
nose and cheeks) that occurs in death, fetal distress, or severe
some pregnant women. hemorrhage.
158. The gynecoid pelvis is 169. Through
most ideal for delivery. Other ultrasonography, the
types include platypelloid (flat), biophysical profile assesses fetal
anthropoid (ape-like), and well-being by measuring fetal
android (malelike). breathing movements, gross
159. Pregnant women body movements, fetal tone,
should be advised that there reactive fetal heart rate
is no safe level of alcohol intake. (nonstress test), and qualitative
amniotic fluid volume.
170. Pica is a craving to eat during oral sex because of the
nonfood items, such as dirt, possibility of air embolism.
crayons, chalk, glue, starch, or 178. The presence of
hair. It may occur during human chorionic
pregnancy and can endanger gonadotropin in the blood or
the fetus. urine is a probable sign of
171. A pregnant patient pregnancy.
should take folic acid because 179. Radiography isn’t
this nutrient is required for usually used in a pregnant
rapid cell division. woman because it may harm
172. A woman who is taking the developing fetus. If
clomiphene (Clomid) to induce radiography is essential, it
ovulation should be informed of should be performed only after
the possibility of multiple births 36 weeks gestation.
with this drug. 180. A pregnant patient who
173. During the first has had rupture of the
trimester, a pregnant woman membranes or who is
should avoid all drugs unless experiencing
doing so would adversely affect vaginal bleeding shouldn’t
her health. engage in sexual intercourse.
174. The Food and Drug 181. A pregnant staff
Administration has established member should not be assigned
the following five categories of to work with a patient who has
drugs based on their potential cytomegalovirus infection
for causing birth defects: A, no because the virus can be
evidence of risk; B, no risk found transmitted to the fetus.
in animals, but no studies have 182. A pregnant patient
been done in women; C, animal should take an iron supplement
studies have shown an adverse to help prevent anemia.
effect, but the drug may be 183. Nausea and vomiting
beneficial to women despite the during the first trimester of
potential risk; D, evidence of pregnancy are caused by rising
risk, but its benefits may levels of the hormone human
outweigh its risks; and X, fetal chorionic gonadotropin.
anomalies noted, and the risks 184. The duration of
clearly outweigh the potential pregnancy averages 280 days,
benefits. 40 weeks, 9 calendar months, or
175. A probable sign of 10 lunar months.
pregnancy, McDonald’s sign is 185. Before performing a
characterized by an ease in Leopold maneuver, the nurse
flexing the body of the uterus should ask the patient to empty
against the cervix. her bladder.
176. Amenorrhea is a 186. Pelvic-tilt exercises can
probable sign of pregnancy. help to prevent or relieve
177. A pregnant woman’s backache during pregnancy.
partner should avoid 187. The nurse must place
introducing air into the vagina identification bands on both the
mother and the neonate before 199. A major developmental
they leave the delivery room. task for a woman during the
188. Dinoprostone (Cervidil) first trimester of pregnancy is
is used to ripen the cervix. accepting the pregnancy.
189. Because women 200. A pregnant patient with
with diabetes have a higher vaginal bleeding shouldn’t have
incidence of birth anomalies a pelvic examination.
than women without diabetes, 201. In the early stages of
an alpha-fetoprotein level may pregnancy, the finding of
be ordered at 15 to 17 weeks glucose in the urine may be
gestation. related to the increased
190. Painless vaginal shunting of glucose to the
bleeding during the last developing placenta, without a
trimester of pregnancy may corresponding increase in the
indicate placenta previa. reabsorption capability of the
191. The hormone human kidneys.
chorionic gonadotropin is a 202. A patient who has
marker for pregnancy. premature rupture of the
192. With advanced membranes is at significant risk
maternal age, a common for infection if labor doesn’t
genetic problem is Down begin within 24 hours.
syndrome. 203. Infants of diabetic
193. Methergine stimulates mothers are susceptible
uterine contractions. to macrosomia as a result of
194. The administration of increased insulin production in
folic acid during the early stages the fetus.
of gestation may prevent neural 204. To prevent heat loss in
tube defects. the neonate, the nurse should
195. A clinical manifestation bathe one part of his body at a
of a prolapsed umbilical cord is time and keep the rest of the
variable decelerations. body covered.
196. The nurse should keep 205. A patient who has a
the sac of meningomyelocele cesarean delivery is at greater
moist with normal risk for infection than the
saline solution. patient who gives birth
197. If fundal height is at vaginally.
least 2 cm less than expected, 206. The occurrence of
the cause may be growth thrush in the neonate is
retardation, missed abortion, probably caused by contact with
transverse lie, or false the organism during delivery
pregnancy. through the birth canal.
198. Fundal height that 207. Maternal serum alpha-
exceeds expectations by more fetoprotein is detectable at 7
than 2 cm may be caused by weeks of gestation and peaks in
multiple gestation, the third trimester. High levels
polyhydramnios, uterine detected between the 16th and
myomata, or a large baby. 18th weeks are associated with
neural tube defects. Low levels
are associated with Down shorten and lengthen in a
syndrome. synchronized pattern.
208. An arrest of descent 216. During crowning, the
occurs when the fetus doesn’t presenting part of the fetus
descend through the pelvic remains visible during the
cavity during labor. It’s interval between contractions.
commonly associated with 217. Uterine atony is failure
cephalopelvic disproportion, of the uterus to remain firmly
and cesarean delivery may be contracted.
required. 218. The major cause of
209. A late sign of uterine atony is a full bladder.
preeclampsia is 219. If the mother wishes to
epigastric pain as a result of breastfeed, the neonate should
severe liver edema. be nursed as soon as possible
210. In the patient with after delivery.
preeclampsia, blood pressure 220. A smacking sound, milk
returns to normal during the dripping from the side of the
puerperal period. mouth, and sucking noises all
211. To obtain an estriol indicate improper placement of
level, urine is collected for 24 the infant’s mouth over the
hours. nipple.
212. An estriol level is used 221. Before feeding is
to assess fetal well-being and initiated, an infant should be
maternal renal functioning as burped to expel air from the
well as to monitor a pregnancy stomach.
that’s complicated by diabetes. 222. Most authorities
213. The period between strongly encourage the
contractions is referred to as continuation of breastfeeding
the interval, or resting phase. on both the affected and the
During this phase, the uterus unaffected breast of patients
and placenta fill with blood and with mastitis.
allow for the exchange of 223. Neonates are
oxygen, carbon dioxide, and nearsighted and focus on items
nutrients. that are held 10″ to 12″ (25 to
214. In a patient who 30.5 cm) away.
has hypertonic contractions, the 224. In a neonate, low-set
uterus doesn’t have an ears are associated with
opportunity to relax and there is chromosomal abnormalities
no interval between such as Down syndrome.
contractions. As a result, the 225. Meconium is usually
fetus may experience hypoxia or passed in the first 24 hours;
rapid delivery may occur. however, passage may take up
215. Two qualities of the to 72 hours.
myometrium are elasticity, 226. Obstetric data can be
which allows it to stretch yet described by using the F/TPAL
maintain its tone, and system:
contractility, which allows it to F/T: Full-term delivery at 38
weeks or longer
P: Preterm delivery between 20 the mother imagines what the
and 37 weeks child she’s carrying is like and
A: Abortion or loss of fetus becomes acquainted with it.
before 20 weeks 234. Mean arterial pressure
L: Number of children living (if a of greater than 100 mm Hg after
child has died, further 20 weeks of pregnancy is
explanation is needed to clarify considered hypertension.
the discrepancy in numbers). 235. Laden’s sign, an early
227. Parity doesn’t refer to indication of pregnancy, causes
the number of infants delivered, softening of a spot on the
only the number of deliveries. anterior portion of the uterus,
228. Women who are just above the uterocervical
carrying more than one fetus juncture.
should be encouraged to gain 236. During pregnancy, the
35 to 45 lb (15.5 to 20.5 kg) abdominal line from the
during pregnancy. symphysis pubis to the
229. The recommended umbilicus changes from linea
amount of iron supplement for alba to linea nigra.
the pregnant patient is 30 to 60 237. The treatment for
mg daily. supine hypotension syndrome
230. Drinking six alcoholic (a condition that sometimes
beverages a day or a single occurs in pregnancy) is to have
episode of binge drinking in the the patient lie on her left side.
first trimester can cause fetal 238. A contributing factor in
alcohol syndrome. dependent edema in the
Chorionic villus sampling is pregnant patient is the increase
performed at 8 to 12 weeks of of femoral venous pressure
pregnancy for early from 10 mm Hg (normal) to 18
identification of genetic defects. mm Hg (high).
231. In percutaneous 239. Hyperpigmentation of
umbilical blood sampling, a the pregnant patient’s face,
blood sample is obtained from formerly called chloasma and
the umbilical cord to now referred to as melasma,
detect anemia, genetic defects, fades after delivery.
and blood incompatibility as 240. The hormone relaxin,
well as to assess the need for which is secreted first by the
blood transfusions. corpus luteum and later by the
232. Hemodilution of placenta, relaxes the connective
pregnancy is the increase in tissue and cartilage of the
blood volume that occurs during symphysis pubis and the
pregnancy. The increased sacroiliac joint to facilitate
volume consists of plasma and passage of the fetus during
causes an imbalance between delivery.
the ratio of red blood cells to 241. Progesterone maintains
plasma and a resultant decrease the integrity of the pregnancy
in hematocrit. by inhibiting uterine motility.
233. Visualization in
pregnancy is a process in which
Labor and Delivery 250. When used to describe
the degree of fetal descent,
242. During labor, to relieve engagement means when the
supine hypotension manifested largest diameter of the
by nausea and vomiting and presenting part has passed
paleness, turn the patient on through the pelvic inlet.
her left side. 251. Fetal stations indicate
243. During the transition the location of the presenting
phase of the first stage of labor, part in relation to the ischial
the cervix is dilated 8 to 10 cm spine. It’s described as –1, –2, –
and contractions usually occur 2 3, –4, or –5 to indicate the
to 3 minutes apart and last for number of centimeters above
60 seconds. the level of the ischial spine;
244. The first stage of station –5 is at the pelvic inlet.
labor begins with the onset of 252. Fetal stations are
labor and ends with full cervical also described as +1, +2, +3, +4,
dilation at 10 cm. or +5 to indicate the number of
245. The second stage of centimeters it is below the level
labor begins with full cervical of the ischial spine; station 0 is
dilation and ends with the at the level of the ischial spine.
neonate’s birth. 253. Any vaginal
246. The third stage of bleeding during pregnancy
labor begins after the neonate’s should be considered a
birth and ends with expulsion of complication until proven
the placenta. otherwise.
247. The fourth stage of 254. During delivery, if the
labor (postpartum stabilization) umbilical cord can’t be loosened
lasts up to 4 hours after the and slipped from around the
placenta is delivered. This time neonate’s neck, it should be
is needed to stabilize the clamped with two clamps and
mother’s physical and cut between the clamps.
emotional state after the stress 255. During the first stage of
of childbirth. labor, the side-lying
248. Unlike false labor, true position usually provides the
labor produces regular rhythmic greatest degree of comfort,
contractions, abdominal although the patient may
discomfort, progressive descent assume any comfortable
of the fetus, bloody show, and position.
progressive effacement and 256. Fetal stations are
dilation of the cervix. also described as +1, +2, +3, +4,
249. When used to describe or +5 to indicate the number of
the degree of fetal descent centimeters it is below the level
during labor, floating means the of the ischial spine; station 0 is
presenting part is not engaged at the level of the ischial spine.
in the pelvic inlet, but is freely 257. Fetal stations indicate
movable (ballotable) above the the location of the presenting
pelvic inlet. part in relation to the ischial
spine. It’s described as –1, –2, –
3, –4, or –5 to indicate the and are more likely than older
number of centimeters above mothers to have nutritional
the level of the ischial spine; deficiencies.
station –5 is at the pelvic inlet. 265. The narrowest diameter
258. When used to describe of the pelvic inlet is the
the degree of fetal descent, anteroposterior (diagonal
engagement means when the conjugate).
largest diameter of the 266. During labor, the resting
presenting part has passed phase between contractions is
through the pelvic inlet. at least 30 seconds.
259. Amniotomy is artificial 267. The length of the uterus
rupture of the amniotic increases from 2½” (6.3 cm)
membranes. before pregnancy to 12½” (32
260. The three phases of a cm) at term.
uterine contraction are 268. To estimate the true
increment, acme, and conjugate (the smallest inlet
decrement. measurement of the pelvis),
261. The intensity of a labor deduct 1.5 cm from the
contraction can be assessed by diagonal conjugate (usually 12
the indentability of the uterine cm). A true conjugate of 10.5
wall at the contraction’s peak. cm enables the fetal head
Intensity is graded as mild (usually 10 cm) to pass.
(uterine muscle is somewhat 269. The smallest outlet
tense), moderate (uterine measurement of the pelvis is
muscle is moderately tense), or the intertuberous diameter,
strong (uterine muscle is which is the transverse
boardlike). diameter between the ischial
262. The frequency of tuberosities.
uterine contractions, which is 270. Electronic fetal
measured in minutes, is the monitoring is used to assess
time from the beginning of one fetal well-being during labor. If
contraction to the beginning of compromised fetal status is
the next. suspected, fetal blood pH may
263. Before internal fetal be evaluated by obtaining a
monitoring can be performed, a scalp sample.
pregnant patient’s cervix must 271. In an emergency
be dilated at least 2 cm, the delivery, enough pressure
amniotic membranes must be should be applied to the
ruptured, and the presenting emerging fetus’s head to guide
part of the fetus (scalp or the descent and prevent a rapid
buttocks) must be at station –1 change in pressure within the
or lower, so that a small molded fetal skull.
electrode can be attached. 272. Massaging the uterus
264. Teenage mothers are helps to stimulate contractions
more likely to have low-birth- after the placenta is delivered.
weight neonates because they 273. When a patient is
seek prenatal care late in admitted to the unit in active
pregnancy (as a result of denial)
labor, the nurse’s first action is uterine contractions during
to listen for fetal heart tones. labor, it must be administered
274. Nitrazine paper is used under close observation to help
to test the pH of vaginal prevent maternal and fetal
discharge to determine the distress.
presence of amniotic fluid. 282. Molding is the process
275. A pregnant patient by which the fetal head changes
normally gains 2 to 5 lb (1 to 2.5 shape to facilitate movement
kg) during the first trimester through the birth canal.
and slightly less than 1 lb (0.5 283. If a woman suddenly
kg) per week during the last two becomes hypotensive during
trimesters. labor, the nurse should increase
276. Precipitate labor lasts the infusion rate of I.V. fluids as
for approximately 3 hours and prescribed.
ends with delivery of the 284. During fetal heart
neonate. monitoring, early deceleration is
277. As emergency caused by compression of the
treatment for excessive uterine head during labor.
bleeding, 0.2 mg of 285. After the placenta is
methylergonovine (Methergine) delivered, the nurse may add
is injected I.V. over 1 minute oxytocin (Pitocin) to the
while the patient’s blood patient’s I.V. solution, as
pressure and uterine prescribed, to promote
contractions are monitored. postpartum involution of the
278. Braxton Hicks uterus and stimulate lactation.
contractions are usually felt in 286. If needed, cervical
the abdomen and don’t cause suturing is usually done
cervical change. True labor between 14 and 18 weeks
contractions are felt in the front gestation to reinforce
of the abdomen and back and an incompetent cervix and
lead to progressive cervical maintain pregnancy. The
dilation and effacement. suturing is typically removed by
279. If a fetus has late 35 weeks gestation.
decelerations (a sign of fetal 287. The Food and Drug
hypoxia), the nurse should Administration has established
instruct the mother to lie on her the following five categories of
left side and then administer 8 drugs based on their potential
to 10 L of oxygen per minute by for causing birth defects: A, no
mask or cannula. The nurse evidence of risk; B, no risk found
should notify the physician. The in animals, but no studies have
side-lying position removes been done in women; C, animal
pressure on the inferior vena studies have shown an adverse
cava. effect, but the drug may be
280. Oxytocin (Pitocin) beneficial to women despite the
promotes lactation and uterine potential risk; D, evidence of
contractions. risk, but its benefits may
281. Because oxytocin outweigh its risks; and X, fetal
(Pitocin) stimulates powerful anomalies noted, and the risks
clearly outweigh the potential (RhoGAM) after delivering an
benefits. Rh-positive neonate.
288. The mechanics of 297. When informed that a
delivery are engagement, patient’s amniotic membrane
descent and flexion, internal has broken, the nurse should
rotation, extension, external check fetal heart tones and then
rotation, restitution, and maternal vital signs.
expulsion. 298. Crowning is the
289. The duration of a appearance of the fetus’s head
contraction is timed from the when its largest diameter is
moment that the uterine encircled by the vulvovaginal
muscle begins to tense to the ring.
moment that it reaches full 299. Subinvolution may
relaxation. It’s measured in occur if the bladder is distended
seconds. after delivery.
290. Fetal demise is death of 300. For an extramural
the fetus after viability. delivery (one that takes place
291. The most common outside of a normal delivery
method of inducing labor after center), the priorities for care of
artificial rupture of the the neonate include maintaining
membranes is oxytocin (Pitocin) a patent airway, supporting
infusion. efforts to breathe, monitoring
292. After the amniotic vital signs, and maintaining
membranes rupture, the initial adequate body temperature.
nursing action is to assess the 301. The administration of
fetal heart rate. oxytocin (Pitocin) is stopped if
293. The most common the contractions are 90 seconds
reasons for cesarean birth are or longer.
malpresentation, fetal distress, 302. If a pregnant patient’s
cephalopelvic disproportion, rubella titer is less than 1:8, she
pregnancy- should be immunized after
induced hypertension, previous delivery.
cesarean birth, and inadequate 303. During the transition
progress in labor. phase of labor, the woman
294. Amniocentesis usually is irritable and restless.
increases the risk of 304. Maternal hypotension is
spontaneous abortion, trauma a complication of spinal block.
to the fetus or placenta, 305. The mother’s Rh factor
premature labor, infection, and should be determined before an
Rh sensitization of the fetus. amniocentesis is performed.
295. After amniocentesis, 306. With early maternal
abdominal cramping or age, cephalopelvic
spontaneous vaginal bleeding disproportion commonly occurs.
may indicate complications. 307. Spontaneous rupture of
296. To prevent her from the membranes increases the
developing Rh antibodies, an risk of a prolapsed umbilical
Rh-negative primigravida should cord.
receive Rho(D) immune globulin
Postpartum Care glucose but positive for
acetone, the nurse should
308. Lochia rubra is the assess the patient’s diet for
vaginal discharge of almost pure inadequate caloric intake.
blood that occurs during the 318. Direct antiglobulin
first few days after childbirth. (direct Coombs’) test is used to
309. Lochia serosa is the detect maternal antibodies
serous vaginal discharge that attached to red blood cells in
occurs 4 to 7 days after the neonate.
childbirth. 319. Before discharging a
310. Lochia alba is the patient who has had an
vaginal discharge of decreased abortion, the nurse should
blood and increased leukocytes instruct her to report bright red
that’s the final stage of lochia. It clots, bleeding that lasts longer
occurs 7 to 10 days after than 7 days, or signs of
childbirth. infection, such as a temperature
311. After delivery, a of greater than 100° F (37.8° C),
multiparous woman is more foul-smelling vaginal discharge,
susceptible to bleeding than a severe uterine cramping,
primiparous woman because nausea, or vomiting.
her uterine muscles may be 320. The fundus of a
overstretched and may not postpartum patient is massaged
contract efficiently. to stimulate contraction of the
312. The nurse should uterus and prevent
suggest ambulation to a hemorrhage.
postpartum patient who has gas 321. Laceration of the
pain and flatulence. vagina, cervix, or perineum
313. Methylergonovine produces bright red bleeding
(Methergine) is an oxytocic that often comes in spurts. The
agent used to prevent and bleeding is continuous, even
treat postpartum when the fundus is firm.
hemorrhage caused by uterine 322. To avoid puncturing the
atony or subinvolution. placenta, a vaginal examination
314. After a stillbirth, the should not be performed on a
mother should be allowed to pregnant patient who is
hold the neonate to help her bleeding.
come to terms with the death. 323. A patient who has
315. If a woman receives a postpartum hemorrhage caused
spinal block before delivery, the by uterine atony should be
nurse should monitor the given oxytocin as prescribed.
patient’s blood pressure closely. 324. After delivery, if the
316. A postpartum patient fundus is boggy and deviated to
may resume sexual intercourse the right side, the patient
after the perineal or uterine should empty her bladder.
wounds heal (usually within 4 325. In the early postpartum
weeks after delivery). period, the fundus should be
317. If a pregnant patient’s midline at the umbilicus.
test results are negative for
Pregnancy Complications to avoid becoming pregnant for
3 months.
326. An ectopic pregnancy is Nonstress Test
one that implants abnormally,
outside the uterus. 336. A nonstress test is
327. A habitual aborter is a considered nonreactive
woman who has had three or (positive) if fewer than two fetal
more consecutive spontaneous heart rate accelerations of at
abortions. least 15 beats/minute occur in
328. Threatened 20 minutes.
abortion occurs when bleeding 337. A nonstress test is
is present without cervical considered reactive (negative) if
dilation. two or more fetal heart rate
329. A complete accelerations of 15
abortion occurs when all beats/minute above baseline
products of conception are occur in 20 minutes.
expelled. 338. A nonstress test is
330. Hydramnios (polyhydra usually performed to assess
mnios) is excessive amniotic fetal well-being in a pregnant
fluid of more than 2,000 ml in patient with a prolonged
the third trimester. pregnancy (42 weeks or more),
331. In an incomplete diabetes, a history of poor
abortion, the fetus is expelled, pregnancy outcomes, or
but parts of the placenta and pregnancy-induced
membrane remain in the uterus. hypertension.
332. When a pregnant Placental Abnormalities
patient has undiagnosed vaginal
bleeding, vaginal examination 339. Placenta previa is
should be avoided until abnormally low implantation of
ultrasonography rules out the placenta so that it
placenta previa. encroaches on or covers the
333. A patient with a cervical os.
ruptured ectopic pregnancy 340. In complete (total)
commonly has sharp pain in the placenta previa, the placenta
lower abdomen, with spotting completely covers the cervical
and cramping. She may have os.
abdominal rigidity; rapid, 341. In partial (incomplete or
shallow respirations; marginal) placenta previa, the
tachycardia; and shock. placenta covers only a portion
334. A 16-year-old girl who is of the cervical os.
pregnant is at risk for having a 342. Abruptio placentae is
low-birth-weight neonate. premature separation of a
335. A rubella vaccine normally implanted placenta. It
shouldn’t be given to a pregnant may be partial or complete, and
woman. The vaccine can be usually causes abdominal pain,
administered after delivery, but vaginal bleeding, and a
the patient should be instructed boardlike abdomen.
343. In placenta previa, 350. The classic triad of
bleeding is painless and seldom symptoms of preeclampsia are
fatal on the first occasion, but it hypertension, edema,
becomes heavier with each and proteinuria. Additional
subsequent episode. symptoms of severe
344. Nursing preeclampsia include
interventions for a patient hyperreflexia, cerebral and
with placenta previa include vision disturbances, and
positioning the patient on her epigastric pain.
left side for maximum fetal 351. After
perfusion, monitoring fetal administering magnesium
heart tones, and administering sulfate to a pregnant patient for
I.V. fluids and oxygen, as hypertension or preterm labor,
ordered. the nurse should monitor the
345. Treatment for abruptio respiratory rate and deep
placentae is usually immediate tendon reflexes.
cesarean delivery. 352. Eclampsia is the
346. A classic difference occurrence of seizures that
between abruptio placentae aren’t caused by a cerebral
and placenta previa is the disorder in a patient who has
degree of pain. Abruptio pregnancy-induced
placentae causes pain, whereas hypertension.
placenta previa causes painless 353. In a patient with
bleeding. preeclampsia, epigastric pain is
347. Because a major role of a late symptom and requires
the placenta is to function as a immediate medical
fetal lung, any condition that intervention.
interrupts normal blood flow to 354. In a pregnant patient,
or from the placenta increases preeclampsia may progress to
fetal partial pressure of arterial eclampsia, which is
carbon dioxide and decreases characterized by seizures and
fetal pH. may lead to coma.
Preeclampsia
355. HELLP (hemolysis,
348. Pregnancy-induced elevated liver enzymes, and low
hypertension is a leading cause platelets) syndrome is an
of maternal death in the United unusual variation of pregnancy-
States. induced hypertension.
349. Pregnancy-induced Contraceptives
hypertension (preeclampsia) is
an increase in blood pressure of 356. The failure rate of a
30/15 mm Hg over baseline or contraceptive is determined by
blood pressure of 140/95 mmHg the experience of 100 women
on two occasions at least 6 for 1 year. It’s expressed as
hours apart accompanied by pregnancies per 100 woman-
edema and albuminuria after 20 years.
weeks gestation. 357. Before providing a
specimen for a sperm count, the
patient should avoid ejaculation
for 48 to 72 hours.
358. If a patient misses two
consecutive menstrual periods
while taking an oral
contraceptive, she should
discontinue the contraceptive
and take a pregnancy test.
359. If a patient who is
taking an oral contraceptive
misses a dose, she should take
the pill as soon as she
remembers or take two at the
next scheduled interval and
continue with the normal
schedule.
360. If a patient who is
taking an oral contraceptive
misses two consecutive doses,
she should double the dose for
2 days and then resume her
normal schedule. She also
should use an additional birth
control method for 1 week.
You might also like
- Test Bank For Maternity Nursing 8th Edition, LowdermilkDocument26 pagesTest Bank For Maternity Nursing 8th Edition, LowdermilkILL101100% (3)
- A Community Diagnosis in Level III Group 2Document89 pagesA Community Diagnosis in Level III Group 2Jenny Agustin FabrosNo ratings yet
- Imagine Me Gone by Adam HaslettDocument271 pagesImagine Me Gone by Adam HaslettCherubim Lei DC Flores100% (2)
- Drug Study Augmentin-KidapawanDocument2 pagesDrug Study Augmentin-KidapawanCherubim Lei DC FloresNo ratings yet
- Maternity and Newborn Nursing ReviewerDocument12 pagesMaternity and Newborn Nursing ReviewerCherubim Lei DC FloresNo ratings yet
- Maternity and Newborn Nursing ReviewerDocument20 pagesMaternity and Newborn Nursing ReviewerNick Realino100% (1)
- Med Surg 2 BulletsDocument19 pagesMed Surg 2 BulletsShiraishiNo ratings yet
- Med Surg Chapter 65 Flashcards - QuizletDocument17 pagesMed Surg Chapter 65 Flashcards - QuizletMonica JubaneNo ratings yet
- NCM 106 - DRUG and IVF CALCULATIONS - VIOSDocument3 pagesNCM 106 - DRUG and IVF CALCULATIONS - VIOSIra Velle ViosNo ratings yet
- Drug Administration MIdterm ExamDocument8 pagesDrug Administration MIdterm ExamRettsu GamingNo ratings yet
- COMPETENCY Summary Evaluation Sheet 1Document8 pagesCOMPETENCY Summary Evaluation Sheet 1Rellora Mark AndreiNo ratings yet
- OB - Postterm PregnancyDocument6 pagesOB - Postterm PregnancyDarren Mae MosadaNo ratings yet
- Pharma Long Quiz KeyDocument3 pagesPharma Long Quiz KeyBiatch NebturaNo ratings yet
- Ortho Supplemental NotesDocument6 pagesOrtho Supplemental Notestanya merdeNo ratings yet
- 4.3 InfectiousDocument29 pages4.3 InfectiousJohn Anthony de GùzmanNo ratings yet
- Medical AbbreviationDocument9 pagesMedical AbbreviationDjayNo ratings yet
- Medication and Administration C.NDocument286 pagesMedication and Administration C.NJaleto sunkemoNo ratings yet
- Nclex Bank QuestionsDocument43 pagesNclex Bank QuestionsJANIELA RITCHEL DANIELNo ratings yet
- Maths Numerical Assignment With AnswersDocument3 pagesMaths Numerical Assignment With AnswersAiman SiddiquiNo ratings yet
- Ante Natal Care - 2Document43 pagesAnte Natal Care - 2Dina M ElbakaryNo ratings yet
- Medical Asepsis (Handwashing) Parameters Score 5 4 3 2 1Document36 pagesMedical Asepsis (Handwashing) Parameters Score 5 4 3 2 1Cathrine Mae RamilNo ratings yet
- Generic: Hydromorphone (SC) Brand Name: DilaudidDocument1 pageGeneric: Hydromorphone (SC) Brand Name: DilaudidPreet ChahalNo ratings yet
- Pharma Handouts Rev 3Document34 pagesPharma Handouts Rev 3Aphrill Pearl PacisNo ratings yet
- biophysical-WPS OfficeDocument13 pagesbiophysical-WPS OfficeSandhya GuptaNo ratings yet
- Common Pediatric DisordersDocument2 pagesCommon Pediatric DisordersJean ReyesNo ratings yet
- Icu FlowsheetDocument4 pagesIcu FlowsheetdedeandikaNo ratings yet
- Report Authoring GuideDocument178 pagesReport Authoring GuideabhishekNo ratings yet
- NCM 212 - Dosage CalculationsDocument7 pagesNCM 212 - Dosage CalculationsLYRIZZA LEA BHEA DESIATANo ratings yet
- Med Surge 1Document39 pagesMed Surge 1rave andrei MacanayaNo ratings yet
- Cal Misbah Test 2016 Qa PDFDocument51 pagesCal Misbah Test 2016 Qa PDFSyedKashifAliNo ratings yet
- Maternal/Ob Notes: "Above Success There Is Excellence Beyond Impossible. " Skei Nursing Review & EnhancementDocument53 pagesMaternal/Ob Notes: "Above Success There Is Excellence Beyond Impossible. " Skei Nursing Review & EnhancementAbdullah, Atteya100% (1)
- CP100MEDICALtermPSAbbr. 2Document78 pagesCP100MEDICALtermPSAbbr. 2RAISA N. RASIDNo ratings yet
- Mabini Colleges Inc. College of Midwifery and NursingDocument3 pagesMabini Colleges Inc. College of Midwifery and NursingEmerald IsleNo ratings yet
- NCLEX Review Question 101-200Document14 pagesNCLEX Review Question 101-200Felimon BugtongNo ratings yet
- Growth and DevelopmentDocument32 pagesGrowth and DevelopmentHumera MisterNo ratings yet
- Haad ReviwerDocument20 pagesHaad ReviwerAnjo TranateNo ratings yet
- Module 7 Student Activity SheetDocument7 pagesModule 7 Student Activity SheetJenny Agustin FabrosNo ratings yet
- Understanding Cancer: Jasmin Saragena BetinolDocument104 pagesUnderstanding Cancer: Jasmin Saragena BetinolERAN MARK ROJASNo ratings yet
- Pediatric Medication: Facilitator: Rubina Kousar RN, RM, BSCN Post RNDocument53 pagesPediatric Medication: Facilitator: Rubina Kousar RN, RM, BSCN Post RNRubinaNo ratings yet
- Subcutaneous InjectionDocument16 pagesSubcutaneous InjectionNani KicchaNo ratings yet
- Nursing Care of Clients With Upper Airway or Respiratory DisordersDocument6 pagesNursing Care of Clients With Upper Airway or Respiratory DisordersLuna MarieNo ratings yet
- MCN HandoutsDocument22 pagesMCN HandoutsFRANCYM PRINCESSRICH BATENGANo ratings yet
- Disorders of PancreasDocument41 pagesDisorders of PancreasAbdullah BhattiNo ratings yet
- Routes of Drug Administration and Dosage FormsDocument39 pagesRoutes of Drug Administration and Dosage FormsAditya RathoreNo ratings yet
- Ncma 219 Rle Midterm ReviewerDocument19 pagesNcma 219 Rle Midterm ReviewerAruxi Yoshi100% (1)
- Mohammed H. Eid - The Intensivist-Middle East & ElMarwa For Publishing & Distribution, GN (2019)Document372 pagesMohammed H. Eid - The Intensivist-Middle East & ElMarwa For Publishing & Distribution, GN (2019)Mohamed Moussa100% (1)
- Pointers To ReviewDocument18 pagesPointers To ReviewHegi Ann AlcalaNo ratings yet
- Pressure InjuriesDocument1 pagePressure InjuriesPaola OrtizNo ratings yet
- Pharmacology Drug Dosage CalculationsDocument54 pagesPharmacology Drug Dosage CalculationsMichelle FigueroaNo ratings yet
- NCM 109 SKILLS LAB DAY 5.3 Catheterization22Document33 pagesNCM 109 SKILLS LAB DAY 5.3 Catheterization22Joseph DusichNo ratings yet
- MEDICATION ADMINISTRATION StudentsDocument53 pagesMEDICATION ADMINISTRATION StudentsMary Ann G. CorsanesNo ratings yet
- Postpartal PeriodDocument32 pagesPostpartal PeriodCharrise VoluntadNo ratings yet
- Micro Microbial Mechanisms of Pathogenicity NOTESDocument6 pagesMicro Microbial Mechanisms of Pathogenicity NOTESAriane NobleNo ratings yet
- Lewis - HeartMedical-Surgical Nursing Flashcards - QuizletDocument55 pagesLewis - HeartMedical-Surgical Nursing Flashcards - QuizletNursyNurseNo ratings yet
- 8th Mid McqsDocument25 pages8th Mid McqsMuhammad Uzair GujjarNo ratings yet
- Oxytocin and Other Drugs Acting On UterusDocument37 pagesOxytocin and Other Drugs Acting On UterusRamadi PrameelaNo ratings yet
- NCLEX Practice Questions: D. AspirinDocument15 pagesNCLEX Practice Questions: D. AspirinJackie AbarraNo ratings yet
- Midterm Exam PCT LecDocument5 pagesMidterm Exam PCT LecRichard OcampoNo ratings yet
- DRUG StudyDocument8 pagesDRUG StudyRhobic ManansalaNo ratings yet
- Blood Transfusion and Its ComplicationsDocument31 pagesBlood Transfusion and Its ComplicationsSaima Hasnain MinhasNo ratings yet
- Basic Maternity ConceptsDocument14 pagesBasic Maternity ConceptsDivine Grace Arreglo AbingNo ratings yet
- MCN ReviewerDocument27 pagesMCN ReviewerTresha LabayosNo ratings yet
- Organogenesis Occurs During The First Trimester of Pregnancy, Specifically, Days 14 To 56 ofDocument11 pagesOrganogenesis Occurs During The First Trimester of Pregnancy, Specifically, Days 14 To 56 ofRhea Lyn LamosteNo ratings yet
- Maternity and Newborn Nursing ReviewerDocument12 pagesMaternity and Newborn Nursing ReviewerCherubim Lei DC FloresNo ratings yet
- Paranoid Schizophrenia NCPDocument8 pagesParanoid Schizophrenia NCPCherubim Lei DC Flores75% (4)
- I. Nursing Care Plan Assessment Diagnosis Planning Intervention Evaluation Goal Partially MetDocument3 pagesI. Nursing Care Plan Assessment Diagnosis Planning Intervention Evaluation Goal Partially MetCherubim Lei DC FloresNo ratings yet
- BSN4 NvcfiDocument1 pageBSN4 NvcfiCherubim Lei DC FloresNo ratings yet
- North Valley College Foundation Cover FormatDocument2 pagesNorth Valley College Foundation Cover FormatCherubim Lei DC FloresNo ratings yet
- Case Study For Paranoid SchizophreniaDocument30 pagesCase Study For Paranoid SchizophreniaCherubim Lei DC FloresNo ratings yet
- NCP Drug Study Final Paranoid SchizophreniaDocument11 pagesNCP Drug Study Final Paranoid SchizophreniaCherubim Lei DC FloresNo ratings yet
- I. Nursing Care Plan Assessment Diagnosis Planning Intervention EvaluationDocument4 pagesI. Nursing Care Plan Assessment Diagnosis Planning Intervention EvaluationCherubim Lei DC FloresNo ratings yet
- A Beautiful Mind SummaryDocument2 pagesA Beautiful Mind SummaryCherubim Lei DC FloresNo ratings yet
- I. Nursing Care Plan Assessment Diagnosis Planning Intervention EvaluationDocument3 pagesI. Nursing Care Plan Assessment Diagnosis Planning Intervention EvaluationCherubim Lei DC FloresNo ratings yet
- Nursing Psychiatric Case StudyDocument19 pagesNursing Psychiatric Case StudyCherubim Lei DC FloresNo ratings yet
- Rizal Book by Zayde 2nd EditionDocument207 pagesRizal Book by Zayde 2nd EditionCherubim Lei DC FloresNo ratings yet
- Drug Study For AsthmaDocument4 pagesDrug Study For AsthmaCherubim Lei DC FloresNo ratings yet
- Subjective Objective Assessment Planning Nursing Intervention Rationale EvaluationDocument7 pagesSubjective Objective Assessment Planning Nursing Intervention Rationale EvaluationCherubim Lei DC FloresNo ratings yet
- Pinaka Final NresDocument28 pagesPinaka Final NresCherubim Lei DC FloresNo ratings yet
- I. Nursing Care Plan Assessment Diagnosis Planning Intervention EvaluationDocument3 pagesI. Nursing Care Plan Assessment Diagnosis Planning Intervention EvaluationCherubim Lei DC FloresNo ratings yet
- Paranoid Schizophrenia Case StudyDocument33 pagesParanoid Schizophrenia Case StudyCherubim Lei DC Flores50% (4)
- Dawwwwwwwwwwwwwwww PDFDocument442 pagesDawwwwwwwwwwwwwwww PDFCherubim Lei DC FloresNo ratings yet
- 10 Nursing TheoristsDocument6 pages10 Nursing TheoristsCherubim Lei DC FloresNo ratings yet
- PrognosisDocument3 pagesPrognosisCherubim Lei DC FloresNo ratings yet
- Pinaka Final NresDocument28 pagesPinaka Final NresCherubim Lei DC FloresNo ratings yet
- Blastocyst ANA 205Document27 pagesBlastocyst ANA 205Ogundipe olorunfemiNo ratings yet
- 2ND Q Grade 5 Epp and ScienceDocument7 pages2ND Q Grade 5 Epp and ScienceHAZEL JANE BAGUIONo ratings yet
- Norethisterone JournalDocument29 pagesNorethisterone JournalAditya Syah PutraNo ratings yet
- 20 Perimenopause & MenopauseDocument14 pages20 Perimenopause & MenopauseGirum SolomonNo ratings yet
- Final Obstetrics and GynacologyDocument88 pagesFinal Obstetrics and Gynacologysis8100% (2)
- 0308 Repro101Document3 pages0308 Repro101thidingNo ratings yet
- Fuck Better A Simple Guide To Superior SexDocument86 pagesFuck Better A Simple Guide To Superior SexMarc Joel80% (5)
- Medicine Lecture 1 - History Taking (Colored)Document4 pagesMedicine Lecture 1 - History Taking (Colored)miguel cuevas100% (2)
- Science10 q3 Mod2 Week2 Menstrual-Cycle-Version-3Document24 pagesScience10 q3 Mod2 Week2 Menstrual-Cycle-Version-3nadia doropanNo ratings yet
- The Menstrual Cycle ForDocument4 pagesThe Menstrual Cycle ForAngelica Calamba CalicaNo ratings yet
- Human Reproduction Neet Special BioDocument75 pagesHuman Reproduction Neet Special BioAnil KumarNo ratings yet
- Cambridge IGCSE: BIOLOGY 0610/42Document20 pagesCambridge IGCSE: BIOLOGY 0610/42Tanish KanojiaNo ratings yet
- Ethical Concerns Relating To Taking Birth Control PillsDocument8 pagesEthical Concerns Relating To Taking Birth Control PillsMichael MbithiNo ratings yet
- Nle Notes MCNDocument33 pagesNle Notes MCNjosephmary09No ratings yet
- Reproductive System Notes - 2014-15 DraftDocument62 pagesReproductive System Notes - 2014-15 DraftMiguel MenendezNo ratings yet
- Maternity Nursing ReviewDocument37 pagesMaternity Nursing Reviewshenric16No ratings yet
- Embryology Chapter 3Document23 pagesEmbryology Chapter 3Abdisamed AllaaleNo ratings yet
- Normal Menstrual CycleDocument28 pagesNormal Menstrual CycleCristóbal Concha100% (1)
- SituationdDocument64 pagesSituationdIvory SantiagoNo ratings yet
- Premenstrual Syndrome (PMS)Document4 pagesPremenstrual Syndrome (PMS)Nick BantoloNo ratings yet
- 1Document21 pages1beatrice.laalNo ratings yet
- Optimize The Stages of Your Menstrual CycleDocument11 pagesOptimize The Stages of Your Menstrual CycleAnabel VizcarraNo ratings yet
- Science Short Notes Grade 10Document32 pagesScience Short Notes Grade 10Mallindu PereraNo ratings yet
- CombinepdfDocument40 pagesCombinepdfShaira UntalanNo ratings yet
- 2 Study of Female Pelvic Pain ..Document69 pages2 Study of Female Pelvic Pain ..Ghofran Ibrahim HassanNo ratings yet
- Grade 8 Integrated Science Week 2 Lesson 2Document5 pagesGrade 8 Integrated Science Week 2 Lesson 2Balram HaroldNo ratings yet
- Midterm Module SocSci 111Document40 pagesMidterm Module SocSci 111Frances Georgina FabaleNo ratings yet
- Greendale-1999-The MenopauseDocument10 pagesGreendale-1999-The MenopauseRya RatnaNo ratings yet
- IMAT 2015 - Shuffled - EdiSESDocument31 pagesIMAT 2015 - Shuffled - EdiSESSalvatore SinatraNo ratings yet