Professional Documents
Culture Documents
Case Report
Case Report
Uploaded by
Sara AlvesOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Case Report
Case Report
Uploaded by
Sara AlvesCopyright:
Available Formats
CASE REPORT
3-year-old female, is admitted in the hospital on the 20 th of September of 2022,
presenting with paroxysmal and unproductive cough and rhinorrhea, since the 18th.
The cough started abruptly during the night, from the 18th to the 19th, having a
duration of 3 hours, not allowing the girl to sleep. The cough was like a barking
sound, and, after that, the cough became productive, and the child began to breath
shallowly. The girl took Ventolin syrup 2mg/5ml, a salbutamol, providing short acting
bronchodilation in obstructive airways. On the 19 th an X-ray was done, showing an
emerging infiltration in the right basal segment. That night, the mother gave her
Klacid (clarithromycin). It’s referred that the child was at the pool 2 days before the
symptoms started, and that the very next day she had a cold.
On admission, blood work was done, showing leukocytosis with formula deviation
to the left and a CRP of 14mg/l.
As background, 3 weeks ago she had a strong cough, fever up to 38.5ºC and
rales could be heard. She also had tonsilitis once and she’s vaccinated according to
the plan. Denies allergies and family members are currently healthy.
On the physical exam her condition is moderate. Breathes easily through her nose.
Wheezes can be heard when she takes deeper breaths. On auscultation moist rales
of various calibers can be heard throughout all lungs. Breathing rate is 34 times per
minute. Ear drums are pink, reflexes (+). Saturation of O2 93%. Temperature is
38.4ºC. Heart rate is 138bpm.
Analyses are repeated, showing GBC: leuk 12,6x109/l; Ery 4,54x10*12/l; Hb 112 g/l;
tromb 403x109/l; mon 1%; linf 25 %; gran 67 %. CRP – 22,6 mg/l.
The girl presents herself with 2 days of rhinorrhea and unproductive cough, and,
at the time of admission, she’s showing signs of a lower respiratory tract infection,
with the start of productive cough and high fever. Besides that, the x ray shows an
emerging infiltration in the right basal segment. There’s also, at admission,
leukocytosis with formula deviation to the left and CRP of 14mg/l indicating an
infection in progress. 3 weeks ago, she had a possible superior respiratory tract
infection, with high fever, dry cough and rales.
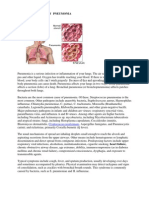
Lower respiratory tract infections (LRTI) include bronchitis, bronchiolitis and
pneumonia, or any combination of the three. Based on the symptoms, such as fever,
respiratory symptoms at the physical exam, such as wheezes, and rales, and
parenchymal involvement, with the presence of infiltrates in the right basal segment
of the lung, the more probable diagnosis is pneumonia. Pneumonia is also more
common in children younger than 5 years of age, and the patient is 3 years old. In
children of this age (<5 years old), viruses are the most common cause. However,
bacterial pathogens, such as Streptococcus pneumoniae, Staphylococcus aureus,
and Streptococcus pyogenes, are also to be taken in consideration. In fact, in viral
pneumonia, fever is usually present, but temperatures are generally lower so,
CASE REPORT SARA GOMES ALVES
despite not being able to fully classify if this pneumonia is viral or bacterial without
further tests, the high temperatures presented by the child and the lobar
consolidation seen in the x ray, are suggestive of bacterial etiology. However,
wheezing is more common in pneumonia caused by atypical bacteria and viruses,
than bacteria. It is also a characteristic feature of bronchiolitis and asthma. Bacterial
pneumonia can be difficult to distinguish from bronchiolitis in young children because
the symptoms and signs of both conditions are nonspecific; children with bacterial
pneumonia may be more ill appearing (higher fever), but clinical features cannot
reliably differentiate bacterial from viral lower respiratory tract infection.
This pneumonia is probably also a community acquired pneumonia (CAP), as the girl
acquired the infection in the community, maybe from the pool she attended 2 days
prior to starting these symptoms, and not from the hospital, as she wasn’t admitted
until the 20th.
The child also presented with nightly cough, not being able to sleep, and that cough
had a very specific barking sound. Croup is a respiratory illness characterized by
inspiratory stridor, barking cough, and hoarseness. These symptoms result from
inflammation in the larynx and subglottic airway. There are two types of croup, the
classical croup (viral croup) and spasmodic croup.
Viral croup occurs commonly in children from six months to three years of age, and it
is caused by respiratory viruses, having typical viral symptoms as nasal congestion
and fever. Viral croup is usually a self-limited illness and the cough typically resolves
within three day.
Spasmodic croup also occurs in children six months to three years of age and
always occurs at night. The onset and cessation of symptoms are abrupt, and the
duration of symptoms is short. Fever is usually absent. Seeing as the girl had a
strong barking cough during the night, with abrupt onset and cessation, for 3 hours,
she probably had an acute laryngitis with spasmodic croup, although more episodes
are needed to diagnose this condition.
With all these clinical signs and symptoms presented by the 3-year-old girl, the most
probable diagnosis is an acute laryngotracheobronchitis with secondary bacterial
infection: Laryngotracheobronchitis occurs when inflammation extends into the
bronchi, resulting in lower airway signs (wheezing and crackles presented by the girl)
and, sometimes, more severe illness than laryngotracheitis alone. Extension of
inflammation further into the lower airways results in
laryngotracheobronchopneumonitis, which can be complicated by bacterial
superinfection, such as pneumonia.
Bronchiolitis is also a diagnosis to have in consideration and is broadly defined as
a clinical syndrome of respiratory distress that occurs in children <2 years of age,
characterized by upper respiratory symptoms (rhinorrhea) followed by lower
respiratory infection with inflammation, which results in wheezing and/or crackles.
Bronchiolitis typically is caused by a viral infection, being respiratory syncytial virus
(RSV) the most common cause. Bronchiolitis generally presents with fever (usually
≤38.3°C), cough and respiratory distress (wheezing, crackles). It often is preceded
by a one- to three-day history of upper respiratory tract symptoms (nasal
congestion). Typical illness with bronchiolitis begins with upper respiratory tract
CASE REPORT SARA GOMES ALVES
symptoms, followed by lower respiratory tract signs and symptoms on days 2 to 3,
which peak on days 3 to 5 and then gradually resolve. Despite being a valid
differential diagnosis, the type of cough, with the barking sound, doesn’t go with the
type of cough presented in Bronchiolitis, so this diagnosis is less probable.
Foreign body aspiration is to also be taken in consideration, and there often is a
history of the sudden onset of choking and symptoms of upper airway obstruction in
a previously healthy child. If an inhaled foreign body lodges in the larynx, it will
produce hoarseness and stridor. If a large foreign body is swallowed, it may lodge in
the upper esophagus, resulting in distortion of the adjacent soft extrathoracic trachea
and producing a barking cough and inspiratory stridor. However, if the child had
swallowed a foreign body, her symptoms would have a much more acute onset and
she would have more trouble breathing. Also, foreign body aspiration doesn’t explain
the findings of infiltration in the right basal segment in the x-ray.
Asthma is also a differential diagnosis to have in consideration as the child
presented wheezing. However, she didn’t have any previous episodes of
bronchiolitis, doesn’t have allergies and/or family history, therefore, this diagnose is
improbable.
Treatment:
Supportive respiratory care: For children not requiring immediate intubation,
supportive respiratory care consists of providing supplemental oxygen and a trial of
inhaled bronchodilator therapy (nebulized epinephrine if stridor is noted; albuterol if
wheezing is noted)
Supplemental oxygen: For patients with hypoxia and respiratory distress,
supplemental oxygen should be provided to maintain oxygen saturation ( SpO2
≥94%);
Fever control and treatment with antipyretics (oral paracetamol 10-20 mg/kg/toma) or
suppository matched to the weight of the child.
Nebulized epinephrine – For most children presenting with acute respiratory distress
and stridor:
Racemic epinephrine is administered as 0.05 mL/kg per dose (maximum of
0.5 mL) of a 2.25% solution diluted to 3 mL total volume with normal saline. It is
given via nebulizer over 15 minutes.
L-epinephrine (parenteral product) is administered as 0.5 mL/kg per dose
(maximum of 5 mL) using the 1 mg/mL strength (may also be referred to as a 1:1000
dilution). It is given via nebulizer over 15 minutes.
Intubation: Close respiratory monitoring is critical to all children admitted for
management of bacterial tracheitis given the risk for acute airway compromise from
the tracheal exudate and pseudomembranes. However, as the girl isn’t in distress
and is able to breath without any help, this would only be applicable if her situation
worsens.
CASE REPORT SARA GOMES ALVES
For the bacterial infection:
For appropriately immunized, healthy children younger than five years who are
thought to have bacterial CAP based upon clinical presentation, examination
findings, and supportive radiographic or laboratory data if obtained (lobar
consolidation on radiograph, white blood cell count >15,000/microL, C-reactive
protein >35 to 60 mg/L) but do not require inpatient therapy, amoxicillin is usually
considered the drug of choice. A high-dose amoxicillin, 90 to 100 mg/kg per day,
divided into two or three doses with a maximum dose of 4 g/day.
Sara Gomes Alves
Group 3
Erasmus +
CASE REPORT SARA GOMES ALVES
REFERENCES
Barson, W.J. (2022) Community-acquired pneumonia in children: Clinical features and
diagnosis, UpToDate. Available at: https://www.uptodate.com/contents/community-
acquired-pneumonia-in-children-clinical-features-and-diagnosis?
search=pneumonia+children+sintoma&source=search_result&selectedTitle=2~150&us
age_type=default&display_rank=2 (Accessed: October 10, 2022).
Barson, W.J. (2022) Community-acquired pneumonia in children: Outpatient
treatment, UpToDate. Available at: https://www.uptodate.com/contents/community-
acquired-pneumonia-in-children-outpatient-treatment?
search=pneumonia+bacteriana+crian
%C3%A7as&source=search_result&selectedTitle=1~150&usage_type=default&displa
y_rank=1#H8 (Accessed: October 10, 2022).
Isaacson, G.C. (2020) Congenital anomalies of the larynx, UpToDate. Available at:
https://www.uptodate.com/contents/congenital-anomalies-of-the-larynx?
search=laryngomalacia&source=search_result&selectedTitle=1~24&usage_type=defau
lt&display_rank=1#H3 (Accessed: October 10, 2022).
Woods, C.R. (2021) Bacterial tracheitis in children: Clinical features and
diagnosis, UpToDate. Available at: https://www.uptodate.com/contents/bacterial-
tracheitis-in-children-clinical-features-and-diagnosis?
search=croup+children&topicRef=6002&source=see_link#H11 (Accessed: October 10,
2022).
Woods, C.R. (2021) Bacterial tracheitis in children: Treatment and prevention, UpToDate.
Available at: https://www.uptodate.com/contents/bacterial-tracheitis-in-children-
treatment-and-prevention?
search=laringotraqueobronquite+aguda&source=search_result&selectedTitle=2~17&us
age_type=default&display_rank=2 (Accessed: October 10, 2022).
Woods, C.R. (2022) Croup: Clinical features, evaluation, and diagnosis, UpToDate.
Available at: https://www.uptodate.com/contents/croup-clinical-features-evaluation-
and-diagnosis?
search=croup+children&source=search_result&selectedTitle=2~76&usage_type=defau
lt&display_rank=2 (Accessed: October 10, 2022).
Zyngman, B. (ed.) (no date) Whooping cough (pertussis) in children, Whooping Cough
(Pertussis) in Children - Health Encyclopedia - University of Rochester Medical
Center. Available at: https://www.urmc.rochester.edu/encyclopedia/content.aspx?
contenttypeid=90&contentid=P02533 (Accessed: October 10, 2022).
CASE REPORT SARA GOMES ALVES
You might also like
- Croup Syndrome Nursing Care Planning and Management - Study Guide PDFDocument18 pagesCroup Syndrome Nursing Care Planning and Management - Study Guide PDFSanket TelangNo ratings yet
- LaryngitisDocument40 pagesLaryngitisMikhail Guidicelli100% (1)
- Cases - CoughDocument5 pagesCases - CoughSarthak DubeyNo ratings yet
- Whooping Cough LectureDocument37 pagesWhooping Cough LecturePriyanshu MNo ratings yet
- CroupDocument40 pagesCroupAbigail Basco100% (1)
- CcroupDocument53 pagesCcroupOlivia BernadiNo ratings yet
- Whooping CoughDocument25 pagesWhooping CoughchkiershadiNo ratings yet
- Acute Laryngitis in ChildhoodDocument6 pagesAcute Laryngitis in ChildhoodpinanoeNo ratings yet
- By: Chella May R. SisonDocument11 pagesBy: Chella May R. Sisoncasandra moranteNo ratings yet
- Stridor in ChildrenDocument7 pagesStridor in Childrenp4b5No ratings yet
- Trinity University of Asia St. Luke'S College of Nursing Case Study (Opd) NAME: Marie Deborah Kay B. Chakas CASE: Pneumonia (Pedia)Document19 pagesTrinity University of Asia St. Luke'S College of Nursing Case Study (Opd) NAME: Marie Deborah Kay B. Chakas CASE: Pneumonia (Pedia)MARIE DEBORAH KAY CHAKASNo ratings yet
- AEBADocument6 pagesAEBAAtirah Aa100% (1)
- Croup NcbiDocument6 pagesCroup NcbijefrizalzainNo ratings yet
- Bronkopneumonia Pada Pasien PediatrikDocument5 pagesBronkopneumonia Pada Pasien PediatrikCecilia Evangelista NiluhNo ratings yet
- Histoplasmosis: A Case StudyDocument9 pagesHistoplasmosis: A Case StudyDean ivan ParalesNo ratings yet
- Acute Respiratory InfectionDocument28 pagesAcute Respiratory InfectionMazharNo ratings yet
- What Is Dengue Fever?Document30 pagesWhat Is Dengue Fever?Jeanie Rose AlduesoNo ratings yet
- Case Study PneumoniaDocument53 pagesCase Study PneumoniaWilliam Agoncillo100% (1)
- QCM Ped PulmoDocument8 pagesQCM Ped PulmoWahbi KhalidNo ratings yet
- Miliary Tuberculosis in A Healthy Adult: BstractDocument6 pagesMiliary Tuberculosis in A Healthy Adult: Bstractgustianto hutama pNo ratings yet
- ALRI Control ProgrammeDocument20 pagesALRI Control ProgrammeDr.G.Bhanu PrakashNo ratings yet
- Pulmonary Tuberculosis As A Differential Diagnosis of PneumoniaDocument18 pagesPulmonary Tuberculosis As A Differential Diagnosis of PneumoniaKadek AyuNo ratings yet
- StridorDocument3 pagesStridorDrTarek Mahmoud Abo KammerNo ratings yet
- 1-Case Study - 33-Year-Old Female Presents With Chronic SOB and Cough - StatPearls - NCBI BookshelfDocument7 pages1-Case Study - 33-Year-Old Female Presents With Chronic SOB and Cough - StatPearls - NCBI Bookshelfabdeali hazariNo ratings yet
- NURSING CARE PLAN PneumoniaDocument38 pagesNURSING CARE PLAN PneumoniaLuna JadeNo ratings yet
- Health Info Health Info Medicines Advanced Search Register Login Top of Form User NameDocument24 pagesHealth Info Health Info Medicines Advanced Search Register Login Top of Form User NameAnusha PradhanNo ratings yet
- Acute Bronchitis Chronic Bronchitis: PathophysiologyDocument2 pagesAcute Bronchitis Chronic Bronchitis: PathophysiologyHarimunsyi Anugerah PratamaNo ratings yet
- Acute Cough in Children: Diagnosing Aris SeriesDocument4 pagesAcute Cough in Children: Diagnosing Aris SeriesCzarina Isabela TuazonNo ratings yet
- Pa Tho Physiology of PneumoniaDocument6 pagesPa Tho Physiology of PneumoniaPaula YoungNo ratings yet
- Etiology & EpidemiologyDocument3 pagesEtiology & EpidemiologyHandre PutraNo ratings yet
- Name: Carlo M. Yao Bachelor of Science in NursingDocument33 pagesName: Carlo M. Yao Bachelor of Science in Nursingcarlo24_briggsNo ratings yet
- Pediatric Community-Acquired Pneumonia: Nelson 20 EdDocument43 pagesPediatric Community-Acquired Pneumonia: Nelson 20 EdRazel Kinette AzotesNo ratings yet
- Acute Upper Respiratory Infection (AURI)Document58 pagesAcute Upper Respiratory Infection (AURI)api-19916399No ratings yet
- Tosse Cronica em CriançasDocument17 pagesTosse Cronica em CriançasEdvaldo Pereira da Silva JúniorNo ratings yet
- READINGS PcapDocument2 pagesREADINGS PcapEden RelacionNo ratings yet
- Pertussis: Infected Individuals Do Not "Whoop"!Document4 pagesPertussis: Infected Individuals Do Not "Whoop"!marcusNo ratings yet
- BronchiolitisDocument5 pagesBronchiolitisreshianeNo ratings yet
- The Flu: A Guide for Prevention and TreatmentFrom EverandThe Flu: A Guide for Prevention and TreatmentRating: 5 out of 5 stars5/5 (1)
- Acute Laryngeal Infection in ChildrenDocument19 pagesAcute Laryngeal Infection in ChildrenfaradillaNo ratings yet
- Case Report Acute Laryngitis: Presentator: Dr. Hermawan Surya D Moderator: Dr. Rio Heryanto GunawanDocument8 pagesCase Report Acute Laryngitis: Presentator: Dr. Hermawan Surya D Moderator: Dr. Rio Heryanto GunawanHermawan Surya DharmaNo ratings yet
- Pulm Board ReviewDocument19 pagesPulm Board ReviewAli LaftaNo ratings yet
- Upper Airway Obstruction: Ref.: Nelson Essentials of Pediatrics 7 - Edit. Nelson's Textbook of Pediatrics 20 - EditDocument5 pagesUpper Airway Obstruction: Ref.: Nelson Essentials of Pediatrics 7 - Edit. Nelson's Textbook of Pediatrics 20 - EditAli Abd AlrezaqNo ratings yet
- Pneumonia Case StudyDocument5 pagesPneumonia Case StudycrisolandNo ratings yet
- Whooping CoughDocument7 pagesWhooping Coughmughaltalha01249212015No ratings yet
- Community-Acquired Pneumonia in Infants and ChildrenDocument9 pagesCommunity-Acquired Pneumonia in Infants and ChildrenLorenn AdarnaNo ratings yet
- Case Files® StreptokokusDocument4 pagesCase Files® StreptokokusAHMAD ADE SAPUTRANo ratings yet
- Case Study PneumoniaDocument8 pagesCase Study PneumoniaThesa FedericoNo ratings yet
- BronchitisDocument2 pagesBronchitisNica BaldicanasNo ratings yet
- MEASLES IN CHILDREN in English Dr. Dinda Yuliasari FIXDocument8 pagesMEASLES IN CHILDREN in English Dr. Dinda Yuliasari FIXDinda yuliasariNo ratings yet
- Lower Respiratory Tract Infections (Lrtis) BronchitisDocument11 pagesLower Respiratory Tract Infections (Lrtis) BronchitisAhmed Gh Al-zechrawiNo ratings yet
- W1 L1 URTI (Outdated)Document41 pagesW1 L1 URTI (Outdated)Anas FikriNo ratings yet
- HH2 Pediatric Asthma Case StudyDocument3 pagesHH2 Pediatric Asthma Case Studyshazel chiasaokwuNo ratings yet
- Pertusis Al 4Document23 pagesPertusis Al 4Pratita Jati PermatasariNo ratings yet
- Bronchiolitis EtiologyDocument6 pagesBronchiolitis EtiologyRonNo ratings yet
- Laporan Kasus: Disusun Oleh: Annisa Nadya Pradita NPM 1102013037Document14 pagesLaporan Kasus: Disusun Oleh: Annisa Nadya Pradita NPM 1102013037ZuraidaNo ratings yet
- The Wheezing Infant: Airway Problems in ChildrenDocument4 pagesThe Wheezing Infant: Airway Problems in ChildrenDenise DelaneyNo ratings yet
- VSIM Nursing Clinical Rotation WorksheetDocument13 pagesVSIM Nursing Clinical Rotation WorksheetVin Lorenzo CampbellNo ratings yet
- Pulmonology - Cases With AnswersDocument4 pagesPulmonology - Cases With AnswersSimran PiñheiroNo ratings yet
- Typhoid Fever Final 2Document28 pagesTyphoid Fever Final 2gAARaNo ratings yet
- Diagnosis and Treatment of Chronic CoughFrom EverandDiagnosis and Treatment of Chronic CoughSang Heon ChoNo ratings yet
- Scarlet Fever, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandScarlet Fever, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Acute Inflammatory Upper Airway ObstuctionDocument8 pagesAcute Inflammatory Upper Airway ObstuctionSara AlvesNo ratings yet
- Non-IgE-Mediated Gastrointestinal Food Allergies in ChildrenDocument28 pagesNon-IgE-Mediated Gastrointestinal Food Allergies in ChildrenSara AlvesNo ratings yet
- Suicidal BehaviorDocument8 pagesSuicidal BehaviorSara AlvesNo ratings yet
- Diagnostic Tools in Ocular AllergyDocument14 pagesDiagnostic Tools in Ocular AllergySara AlvesNo ratings yet
- Hearing Aid PDFDocument43 pagesHearing Aid PDFBILAL DIFNo ratings yet
- Imaging Hearing LossDocument20 pagesImaging Hearing LossmenafabNo ratings yet
- A Few Secrets About Bone Conduction Testing Traducir¡¡Document5 pagesA Few Secrets About Bone Conduction Testing Traducir¡¡Pamela Tamara Fernández EscobarNo ratings yet
- Therapy Techniques For Cleft PalateDocument5 pagesTherapy Techniques For Cleft Palateapi-438091798100% (1)
- Titles List of E N T Branch at StudentDocument1 pageTitles List of E N T Branch at Studentheba youssefNo ratings yet
- ENT-Summary AOMDocument14 pagesENT-Summary AOMGio BalisiNo ratings yet
- New Phonetics PresentationDocument16 pagesNew Phonetics PresentationAryNo ratings yet
- Trans SaVi Oto Lec 03 Diseases of The External and Middle EarDocument13 pagesTrans SaVi Oto Lec 03 Diseases of The External and Middle EarJoherNo ratings yet
- EntDocument6 pagesEntibrahimNo ratings yet
- Admin, JPHV VESTIBULAR NEURONITIS 3Document5 pagesAdmin, JPHV VESTIBULAR NEURONITIS 3williams papilayaNo ratings yet
- 4 Kuliah-Slide Vestibular Disorder - 2018 - English VersionDocument68 pages4 Kuliah-Slide Vestibular Disorder - 2018 - English VersionSalma Maha RhaniNo ratings yet
- 5 Best ENT Specialists in HyderabadDocument3 pages5 Best ENT Specialists in HyderabadbsrhospitalsNo ratings yet
- OtosclerosisDocument31 pagesOtosclerosisashry909100% (1)
- Science Class 8 Sound and HearingDocument4 pagesScience Class 8 Sound and HearingSangeeta SharmaNo ratings yet
- Lecture 1 - Introduction To Phonetics & ArticulatorsDocument10 pagesLecture 1 - Introduction To Phonetics & ArticulatorsbeehornetNo ratings yet
- Laryngeal Diseases: Laryngitis, Vocal Cord Nodules / Polyps, Carcinoma LarynxDocument52 pagesLaryngeal Diseases: Laryngitis, Vocal Cord Nodules / Polyps, Carcinoma LarynxjialeongNo ratings yet
- Benign Diseases of LarynxDocument76 pagesBenign Diseases of Larynxranjeet kumar lalNo ratings yet
- Otosclerosis An Update On Diagnosis and Treatment.3Document6 pagesOtosclerosis An Update On Diagnosis and Treatment.3andiNo ratings yet
- 2021 CovidDocument79 pages2021 Covidma. vidiaNo ratings yet
- Bài Kt 1 Ngữ Âm HọcDocument10 pagesBài Kt 1 Ngữ Âm HọcLệ ThứcNo ratings yet
- Hearing Conservation Rev.Document10 pagesHearing Conservation Rev.Anthony BasantaNo ratings yet
- Hearing Status of Children Under Five Years Old in Jatinangor DistrictDocument5 pagesHearing Status of Children Under Five Years Old in Jatinangor DistricterickNo ratings yet
- Amendment Concept BookDocument818 pagesAmendment Concept BookFourth YearNo ratings yet
- 1.2 URTI ApproachDocument90 pages1.2 URTI ApproachMohammad AlrefaiNo ratings yet
- Vehicular Vocalizing To Start Your Day: Voice PedagogyDocument6 pagesVehicular Vocalizing To Start Your Day: Voice PedagogyJulia Gavrashenko100% (1)
- Hoarseness of VoiceDocument6 pagesHoarseness of VoiceJayantiNo ratings yet
- Laryngomalacia With Epiglottic Prolapse Obscuring The Laryngeal InletDocument3 pagesLaryngomalacia With Epiglottic Prolapse Obscuring The Laryngeal Inletwawa chenNo ratings yet
- T10 MaskingDocument2 pagesT10 Maskingshel29No ratings yet
- Theory and Practice of Pure Tone Audiometry - PTADocument12 pagesTheory and Practice of Pure Tone Audiometry - PTAsolhazNo ratings yet