Professional Documents
Culture Documents
80141-Article Text-189224-1-10-20120815
80141-Article Text-189224-1-10-20120815
Uploaded by
intanOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
80141-Article Text-189224-1-10-20120815
80141-Article Text-189224-1-10-20120815
Uploaded by
intanCopyright:
Available Formats
SAJS
General Surgery
Oesophageal pouches and diverticula: A pictorial
review
N Khan, FCRad (D)
F Ismail, FCRad (D), MMed Rad (D)
I E A van de Werke, FRCR
Department of Radiology, Kalafong Hospital and University of Pretoria
Diverticula of the oesophagus are rare. They can occur at any Diagnosis
level, and are often defined by their anatomical location. Three Most diverticula are asymptomatic and discovered incidentally
categories are recognised, namely pharyngo-oesophageal, during investigation of unrelated complaints. When suspected, the
parabronchial and epiphrenic. Although these diverticula are investigation of choice is a barium study. It is essential to include
often asymptomatic, patients can develop significant problems the stomach and duodenum in the study to exclude associated
with dysphagia, regurgitation and aspiration. The causation of conditions such as reflux oesophagitis and hiatal hernia.
oesophageal diverticula is controversial; however, the popular
current belief is that most occur because of oesophageal Zenker’s diverticulum (ZD)
dysmotility. This paper demonstrates the categories of Pharangeal diverticulum may be posterior, lateral or posterolateral,
oesophageal diverticula pictorially, including the radiological but the most commonly encountered type is the posterior
features and underlying pathology. pulsion diverticulum. Posterior pulsion diverticulum at the
S Afr J Surg 2012;50(3):71-75. DOI:10.7196/SAJS.1299 cricopharyngeus was first described by Ludlow in 1769. It was
later reclassified by and has since been eponymously linked with
Zenker.1,4,6
Aetiology ZD is an acquired pulsion diverticulum through Killian’s
The classic Rokitansky classification that divides oesophageal dehiscence, an area of congenital weakness through the region of
diverticula into pulsion and traction diverticula still provides the cricopharyngeus muscle (upper oesophageal sphincter; UOS).
useful information as to the aetiopathogenesis. 1 The anatomical
division according to location into pharyngo-oesophageal
(Zenker’s), mid-oesophageal (tracheobronchial) and distal
(epiphrenic) diverticula is the most suitable for radiological
reporting.2,3 There are several areas of structural weakness in the
wall of the pharynx and oesophagus, where either there are gaps
in the muscular walls or the thin strip-like muscles are relatively
unsupported by surrounding neck tissue. Transient protrusions
through these areas of weaknesses are termed pouches, while
persistent protrusions are called diverticula.4,5
Traction diverticula, as the name implies, are the result of
a surrounding inflammatory process with involvement of the
oesophagus, such as tuberculous adenitis. Pulsion diverticula,
on the other hand, occur as a result of an altered pressure
gradient across the oesophageal lumen, which determines the
formation of diverticula through the area of least resistance,
as is naturally present at Killian’s triangle, or due to tearing of
the oesophageal wall above a zone of altered motility, e.g. an
epiphrenic diverticulum.1
Clinical features
Pharyngeal and oesophageal pouches and diverticula are
uncommon before the age of 40; they usually occur in the 7th
and 8th decades of life and are more common in males than
females. Typical symptoms include dysphagia, regurgitation of
undigested food, borborygmi in the cervical region, chronic Fig. 1a. Postero-anterior radiograph of the chest, control view for a barium
coughing, aspiration due to overspill, halitosis and weight swallow study in a patient with a suspected diverticulum. There is an air/
loss.6-8 fluid level in the superior mediastinum (arrow).
VOL 50, NO. 3, AUGUST 2012 SAJS 71
SAJS
constrictor muscle or between the oblique and horizontal fibres
of the cricopharyngeus muscle itself.1,5,6,9 The exact cause of the
defect is not known, the prevailing theory for years having been
inco-ordination between contraction of the pharynx and relaxation
of the upper sphincter, the so-called ‘cricopharyngeal achalasia’.2
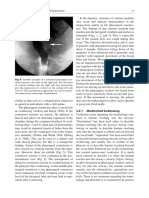
On barium study it is seen as a contrast-filled sac posterior to the
cervical oesophagus, which may extend into the mediastinum (Fig.
1, a - c). The diverticulum varies in size from 0.5 cm to 8 cm. Its
opening lies above the cricopharyngeus muscle, which may be
prominent or thickened (Fig. 2).
Fig. 2. Oblique view of a barium swallow study demonstrating a prominent
and thickened cricopharyngeual impression in the cervical oesophagus
(arrow). Note that the mouth of the Zenker’s diverticulum is above and
posterior, while that of a Killian-Jamieson diverticulum is below and anterior
or lateral.
It has recently been postulated that pathophysiology
of the pharyngeal pouches involves altered compliance of the
cricopharyngeus muscle, detected as impaired pharyngeal opening
or raised intrabolus pressure. Histologically it has been observed
that in patients with a pharyngeal pouch the cricopharyngeus
muscle demonstrates fibro-adipose tissue replacement and fibre
degeneration, which it is thought may account for diminished
UOS opening. The inter-relationship between gastro-oesophageal
reflux and hiatal hernia remains unresolved, though an association
has been reported between them.2,6
Killian-Jamieson diverticula or pouches (lateral cervical
c oesophageal pouches)
The Killian-Jamieson (K-J) diverticulum was first described by
Ekberg and Nylander (cited by Chea et al.10) in 1983. These are
Fig. 1, b and c. Barium swallow study in the same patient shows a large transient or persistent protusions through an area of anatomical
contrast-filled sac in the cervical oesophagus (arrow). The position of the weakness, the Killian-Jamieson space (not to be confused with
diverticulum is in keeping with a Zenker’s diverticulum. Killian’s dehiscence), through which the inferior laryngeal nerve
passes. This space is bounded superiorly by the cricopharyngeus
It has been variously described as a protrusion either between muscle, anteriorly by the posterior wall of the cricoid cartilage, and
the thyropharyngeus and cricopharyngeus portion of the inferior inferomedially by the longitudinal tendon of the oesophagus as it
72 SAJS VOL 50, NO. 3, AUGUST 2012
SAJS
inserts onto the cricoid cartilage.5,9,10 It is commonly asymptomatic,
and can be confused clinically with ZD, from which it is easily
distinguished radiologically. On barium study (Fig. 3) it lies below
the level of cricopharyngeus in the anterolateral wall of the cervical
oesophagus, whereas ZD develops at the anatomically weak
posterior zone, Killian’s dehiscence.10 It is 3 - 20 mm in size, fills
during swallowing and empties after swallowing.
Fig. 3. Anteroposterior view of a barium swallow showing a small Killian-
Jamieson diverticulum (arrow).
Mid-oesophageal diverticula
Mid-oesophageal diverticula classically develop at the middle
third of the oesophagus at the level of bifurcation of the trachea.
They were previously believed to be primarily traction in
nature. Traction diverticula are formed when peri-oesophageal
inflammation causes adhesions between inflammatory foci and
the oesophagus. Although traction diverticula do occur, most
mid-oesophageal diverticula are now thought to occur because
of oesophageal dysmotility. The following mechanism has been
described. First, diffuse spasm or hyperactive peristalsis in the
lower two- thirds or half of the oesophagus is associated with
normal or diminished peristalsis in the upper oesophagus. The
b
persistently increased tone in the distal oesophagus usually Fig. 4, a and b. Barium swallow study from two patients, both with mid-
produces epiphrenic diverticula. Second, spasm or hyperactive oesophageal diverticula. The defect illustrated in 4a is also known as a
peristalsis in the lower oesophagus is associated with normal or tracheobronchial diverticulum, pertaining to its location just proximal to the
hyperactive peristalsis in the upper oesophagus. The functional tracheobronchial bifurcation.
VOL 50, NO. 3, AUGUST 2012 SAJS 73
SAJS
obstruction created when a peristaltic wave encounters the such diverticula, and later Effer et al. confirmed the consistent
spastic distal oesophagus produces a mid-thoracic diverticulum. hypertrophy of the circular muscle of the terminal oesophagus
Residual congenital attachment between the oesophagus and (cited by Tobin7 and Borrie8). Epiphrenic and mid-oesophageal
the tracheobronchial tree in the area of the carina may add an diverticula have been reported with numerous manometric
element of traction, accentuate the pulsion abnormality, and abnormalities, namely DOS, nutcracker oesophagus, achalasia and
facilitate the formation of a mid-thoracic oesophageal diverticula.11 cardiospasm. Symptoms result from the cause, and rarely from the
Mid-oesophageal diverticula have been associated with several diverticulum per se.7,8
manometric abnormalities, including nutcracker oesophagus, Epiphrenic diverticula are usually single, but it is not
diffuse oesophageal spasm (DOS), achalasia, hypertensive lower infrequent to find two or more synchronous diverticula. They
oesophageal sphincter and nonspecific oesophageal motility are best evaluated on barium radiography as large (more than
disorder. 2,7,8 The position and orientation of mid-thoracic 5 cm) diverticula usually 10 cm from the gastro-oesophageal
diverticula may imply pulsion as a cause. Miskovitz and Steinberg junction (Fig. 5, a and b). When large, they may appear on plain
(cited by Rice and Baker 11) reported that pulsion diverticula radiographs as a soft-tissue mass with or without an air/fluid level,
occur most commonly above the tracheal bifurcation. At this mimicking a hiatal hernia (Fig. 5, c and d).
location they project from the left anterolateral border between
the aortic arch and the left main bronchus and are known as inter- Oesophageal intramural pseudodiverticulosis (OIPD)
aortic-bronchial diverticula.11 Classic mid-oesophageal diverticula This is an unusual condition in which inflammation leads to
are small in size with a large neck, and they rarely become dilation of the ducts of the deep mucous glands. OIPD is most
symptomatic or require surgical intervention (Fig. 4, a and b). likely to be a sequel of chronic oesophagitis, probably reflux. It
occurs in elderly patients, usually males, presenting as intermittent
Epiphrenic diverticula or slowly developing dysphagia.3,7 On barium swallow examination
These occur less frequently than ZD, comprising less than 10% of the ducts appear as tiny 1 - 5 mm flask-shaped out-pouchings
all oesophageal diverticula.8 They were first described by Mondiere arranged in clusters of longitudinal rows. Often the neck is not
in 1833, who attributed them to increased intra luminal pressure. opacified and the diverticulum appears to be separated from the
In 1953 Kay reported muscular hypertrophy immediately below oesophageal lumen by 1 or 2 mm (Fig. 6). Patients with OIPD and
dysphagia respond to dilation of the underlying stricture, while
a b
Fig. 5, a and b. Anteroposterior and lateral views of a barium swallow of a
patient which demonstrates a large epiphrenic diverticulum (arrow).
c d a b c
Fig. 5, c and d. Anteroposterior and lateral radiographs of the chest in a
patient with a large epiphrenic diverticulum, which mimics a hiatus hernia or Fig. 6, a - c. A series of images of a barium swallow study demonstrating
a mass lesion (arrow). oesophageal intramural pseudodiverticulosis (OIPD) (arrows).
74 SAJS VOL 50, NO. 3, AUGUST 2012
SAJS
those with evidence of Candida infection or gastro-oesophageal Disclosure. The authors declare that there are no conflicts of
reflux should be medically treated. interest pertaining to the subject matter of this article.
Conclusion REFERENCES
1. Constantini M, Zaninotto G. Oesophageal diverticula. Best Practice and Research
Oesophageal diverticula are classified radiologically according Clinical Gastroenterology 2004;18:3-17.
to their location as well as their directional orientation. 2. Achkar E. Esophageal diverticula. Gastroenterology and Hepatology 2008;4:691-
693.
Oesophageal disease such as cricopharyngeal inco-ordination, 3. Gore RM, Levine MS. Textbook of Gastrointestinal Radiology. 3rd ed. Philadelphia:
lower oesophageal spasm, achalasia and sliding hiatal hernia Saunders Elsevier, 2008:475-477.
4. Nelson AR. Congenital true esophageal diverticulum. Ann Surg 1956;145:258-263.
have all been associated with proximal oesophageal diverticula, 5. Rubesin SE. The pharynx: Structural disorders. Radiol Clin North Am
be they ZD, mid-oesophageal, epiphrenic or indeed intramural 1994;32:1083-1101.
6. Siddiq MA, Sood S, Strachan D. Pharyngeal pouch (Zenker’s diverticulum).
pseudodiverticulosis.The previously popular concept of traction Postgrad Med J 2001;77:506-511.
was a pleasant teaching tool for surgical concepts, but it is is no 7. Tobin RW. Esophageal rings, webs, and diverticula. J Clin Gastroenterol 1998;4:285-
295.
longer tenable as there is an established link with disordered 8. Borrie J, Wilson RLK. Oesophageal diverticula: principal of management and
oesophageal motility. It is therefore pointless to treat the appraisal of classification. Thorax 1980;35:759-767.
9. Perrott J W. Anatomical aspects of hypopharyngeal diverticula. Australian and New
diverticulum without also correcting the cause of the motor Zealand Journal of Surgery 1962;493:304-307.
disorder. 10. Chea CH, Slow SL, Khor TW, Azim NAN. Killian-Jamieson diverticulum: The rare
cervical esophageal diverticulum. Med J Malaysia 2011;66:73-74.
11. Rice TW, Baker ME. Mid-thoracic diverticula. Semin Thorac Cardiovasc Surg
Acknowledgement. The authors would like to thank Professor T 1999;11:352-357.
Mokoena for his valuable contribution.
VOL 50, NO. 3, AUGUST 2012 SAJS 75
You might also like
- Sonography - 2014 - Cartwright - A Sonographer S Guide To The Assessment of Heart DiseaseDocument1 pageSonography - 2014 - Cartwright - A Sonographer S Guide To The Assessment of Heart Diseaseوجدان الدريبيNo ratings yet
- CANINE-Cricopharyngeal Achalasia in DogsDocument6 pagesCANINE-Cricopharyngeal Achalasia in Dogstaner_soysurenNo ratings yet
- Anoto Clinica y QX en HerniasDocument7 pagesAnoto Clinica y QX en HerniasDanielaNo ratings yet
- Kleitsch 1958Document6 pagesKleitsch 1958CojocariNo ratings yet
- Capitulo 2 Radiografia y Ecografia GastrointestinalDocument46 pagesCapitulo 2 Radiografia y Ecografia GastrointestinalLAURA DANIELA VERA BELTRANNo ratings yet
- Hérnia TBDocument3 pagesHérnia TBPietra LocatelliNo ratings yet
- Benign Disease of The Esophagus PDFDocument4 pagesBenign Disease of The Esophagus PDFSpecialNameNo ratings yet
- DiverticulumZenk Slides 100428Document30 pagesDiverticulumZenk Slides 100428Justine NyangaresiNo ratings yet
- Barretts Esophagus - A ReviewDocument14 pagesBarretts Esophagus - A ReviewVytautas LiutvinasNo ratings yet
- 1-s2.0-S1930043323005046-mainDocument3 pages1-s2.0-S1930043323005046-mainAdam DanuartaNo ratings yet
- Textbook of Respiratory Disease in Dogs and Cats Diaphragmatic HerniaDocument9 pagesTextbook of Respiratory Disease in Dogs and Cats Diaphragmatic HerniaDiego CushicóndorNo ratings yet
- Gastric Dilatation Organoaxial Volvulus in A DogDocument6 pagesGastric Dilatation Organoaxial Volvulus in A DogKrlÖz Ändrz Hërëdîa ÖpzNo ratings yet
- Dysphagia Diagnosis 1and Treatment (Olle Ekberg) (Z-Lib - Org) (1) - 83-284Document202 pagesDysphagia Diagnosis 1and Treatment (Olle Ekberg) (Z-Lib - Org) (1) - 83-284Macarena Paz ÁlvarezNo ratings yet
- Hypertrophic Pyloric Stenosis in The Adult: Johannesburg AetiologyDocument3 pagesHypertrophic Pyloric Stenosis in The Adult: Johannesburg AetiologyzapomannNo ratings yet
- Approaches To Esophageal SuturesDocument7 pagesApproaches To Esophageal Suturestaner_soysurenNo ratings yet
- Lecture 5 Zenkers DiverticulumDocument2 pagesLecture 5 Zenkers DiverticulumAmy KochNo ratings yet
- Cisterna Magna SeptaDocument13 pagesCisterna Magna SeptaBRINDUSA CIMPOCANo ratings yet
- Trilogy of Foregut Midgut and Hindgut Atresias PreDocument5 pagesTrilogy of Foregut Midgut and Hindgut Atresias PreEriekafebriayana RNo ratings yet
- Cricopharyngeal DysphagiaDocument8 pagesCricopharyngeal Dysphagiataner_soysurenNo ratings yet
- Bedside Water Swallow Test ArticleDocument4 pagesBedside Water Swallow Test ArticleJU WSDNo ratings yet
- Fundoplication For The TreatmentDocument5 pagesFundoplication For The TreatmentDaniel FloreaNo ratings yet
- Laparoscopic Heller Myotomy For Achalasia: Robert N. Cacchione, M.D., Dan N. Tran, M.D., Diane H. Rhoden, M.DDocument5 pagesLaparoscopic Heller Myotomy For Achalasia: Robert N. Cacchione, M.D., Dan N. Tran, M.D., Diane H. Rhoden, M.Dgabriel martinezNo ratings yet
- 10 CR Killian Jamieson DiverticulumDocument2 pages10 CR Killian Jamieson DiverticulumUmesh BabuNo ratings yet
- Andolfi Et Al. - 2016 - Surgical Treatment of Paraesophageal Hernias A ReDocument6 pagesAndolfi Et Al. - 2016 - Surgical Treatment of Paraesophageal Hernias A ReDaniel PredaNo ratings yet
- The Misplaced Caecum and The Root of The MesenteryDocument8 pagesThe Misplaced Caecum and The Root of The MesenteryKrsna DharmasyaNo ratings yet
- Caudal Duplication SyndromeDocument3 pagesCaudal Duplication Syndromekhumaira1982No ratings yet
- MRI Findings in Fetuses With An Abdominal Wall Defect: Gastroschisis, Omphalocele, and Cloacal ExstrophyDocument7 pagesMRI Findings in Fetuses With An Abdominal Wall Defect: Gastroschisis, Omphalocele, and Cloacal ExstrophyIngrid TanasaNo ratings yet
- Differential Diagnosis of Intracranial AnomaliesDocument4 pagesDifferential Diagnosis of Intracranial AnomaliesFitrianidilaNo ratings yet
- 0 1 The Pathophysiology of Shoulder Instability 2800953368Document8 pages0 1 The Pathophysiology of Shoulder Instability 2800953368César ArveláezNo ratings yet
- Jurnal THTDocument46 pagesJurnal THTShida ZakariaNo ratings yet
- Anatomy and Physiology of PharynxDocument16 pagesAnatomy and Physiology of Pharynxaleeza nomanNo ratings yet
- Diagnosis and Management of Esophageal Rings and WebsDocument4 pagesDiagnosis and Management of Esophageal Rings and WebsIt's MeNo ratings yet
- DOLICHOCOLONDocument6 pagesDOLICHOCOLONCassNo ratings yet
- Duplication Cyst of Pyloric Canal: A Rare Cause of Pediatric Gastric Outlet Obstruction: Rare Case ReportDocument4 pagesDuplication Cyst of Pyloric Canal: A Rare Cause of Pediatric Gastric Outlet Obstruction: Rare Case Reportfebyan yohanesNo ratings yet
- Anatomyand Physiologyofthe Larynxand HypopharynxDocument13 pagesAnatomyand Physiologyofthe Larynxand HypopharynxAngela PetreskaNo ratings yet
- 556 - Breechwilliams Obstetrics 25th Edition (2018)Document12 pages556 - Breechwilliams Obstetrics 25th Edition (2018)yayayanizaNo ratings yet
- Hernia Femoralis IncarserataDocument2 pagesHernia Femoralis IncarserataSa FariNo ratings yet
- Embryology of RotationDocument5 pagesEmbryology of RotationmikeNo ratings yet
- Cricopharyngeal Myotomy Surgical TechniqueDocument8 pagesCricopharyngeal Myotomy Surgical TechniqueDANDYNo ratings yet
- Conventional and Laparoscopic Epigastric Hernia RepairDocument4 pagesConventional and Laparoscopic Epigastric Hernia RepairOhana S.No ratings yet
- Abdomen UltrasoundDocument9 pagesAbdomen UltrasoundRADIOLOGI RSUD CILEUNGSINo ratings yet
- Surgery For Pharyngeal Pouch or Zekers DivertulaDocument19 pagesSurgery For Pharyngeal Pouch or Zekers DivertulaKumaran Bagavathi RagavanNo ratings yet
- Piazza 2010Document11 pagesPiazza 2010Israel BlancoNo ratings yet
- 8095 28575 1 SMDocument2 pages8095 28575 1 SMPatrick JohnNo ratings yet
- J Thorsurg 2018 07 001Document7 pagesJ Thorsurg 2018 07 001Gabriel RangelNo ratings yet
- Trichobezoars: Case Reports and Review of LiteratureDocument4 pagesTrichobezoars: Case Reports and Review of LiteratureSajag GuptaNo ratings yet
- 1 s2.0 S0002961004004295 MainDocument6 pages1 s2.0 S0002961004004295 MainResidentes CirugíaNo ratings yet
- Congenital Eventration of The Diaphragm+++Document13 pagesCongenital Eventration of The Diaphragm+++TommyNo ratings yet
- Comisuritis Posterior 2Document8 pagesComisuritis Posterior 2VORTIZNo ratings yet
- FP 34 08 33Document3 pagesFP 34 08 33ZakiNo ratings yet
- Dehiscence or Thinning of Bone Overlying The Superior Semicircular Canal in A Temporal Bone SurveyDocument11 pagesDehiscence or Thinning of Bone Overlying The Superior Semicircular Canal in A Temporal Bone SurveyEnrico ArmatoNo ratings yet
- Congental Abdominal Wall DefectsDocument38 pagesCongental Abdominal Wall DefectsAhmad Abu KushNo ratings yet
- Vascular AccententDocument2 pagesVascular Accententwp4saleNo ratings yet
- Anatomy and Physiology of The Larynx and Hypopharynx: January 2010Document13 pagesAnatomy and Physiology of The Larynx and Hypopharynx: January 2010Listya ParamitaNo ratings yet
- Caudal Regression Syndrome: DiseaseDocument5 pagesCaudal Regression Syndrome: DiseaseLisnainiMuchlisNo ratings yet
- Obstruction. DidacticsDocument87 pagesObstruction. DidacticsJoher MendezNo ratings yet
- Pedia 2023Document14 pagesPedia 2023paiskopaxiew888No ratings yet
- Study On Clinical Profile, Management & Outcome of Gastrointestinal Duplication in ChildrenDocument35 pagesStudy On Clinical Profile, Management & Outcome of Gastrointestinal Duplication in ChildrenIJAR JOURNALNo ratings yet
- Postmedj00278 0033Document3 pagesPostmedj00278 0033himNo ratings yet
- Hydrocephalus in An American Miniature Horse Foal A Case Report and Review 2011 Journal of Equine Veterinary ScienceDocument4 pagesHydrocephalus in An American Miniature Horse Foal A Case Report and Review 2011 Journal of Equine Veterinary SciencealarochaNo ratings yet
- Sticky Bone For Space Maintenance in The Treatment of Miller's Class I Gingival Recession Defects With VISTA Technique A Case SeriesDocument4 pagesSticky Bone For Space Maintenance in The Treatment of Miller's Class I Gingival Recession Defects With VISTA Technique A Case SeriesInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Access, Orientation and Security.: Tri-Tome PCDocument2 pagesAccess, Orientation and Security.: Tri-Tome PCNorberto MartinezNo ratings yet
- CPR Training Errors: Maria Rosario C. Soriano, RN, RM LORMA Colleges - Senior High SchoolDocument22 pagesCPR Training Errors: Maria Rosario C. Soriano, RN, RM LORMA Colleges - Senior High SchoolSteffie Anne GavinaNo ratings yet
- Advanced Cardiac Life Support (ACLS) : Dr. Martha Regisna Silalahi RSUD BintanDocument19 pagesAdvanced Cardiac Life Support (ACLS) : Dr. Martha Regisna Silalahi RSUD BintangisnamarthaNo ratings yet
- (Download PDF) Plastic Surgery Hand and Upper Extremity 4Th Edition Geoffrey C Gurtner Full Chapter PDFDocument62 pages(Download PDF) Plastic Surgery Hand and Upper Extremity 4Th Edition Geoffrey C Gurtner Full Chapter PDFpjesmenessro100% (7)
- DOH 1 Ozident Einas 2020Document15 pagesDOH 1 Ozident Einas 2020Farha Navas100% (1)
- International Patient Safety Goals IPSGDocument20 pagesInternational Patient Safety Goals IPSGShafique HussainNo ratings yet
- ASE HCM Poster FINALDocument2 pagesASE HCM Poster FINALBandar Alamri100% (1)
- Ism PresentationDocument22 pagesIsm Presentationapi-277297976100% (1)
- My Updated CVDocument3 pagesMy Updated CVsyed imdadNo ratings yet
- Endolift ALP2Document2 pagesEndolift ALP2juanenrique.martinezmezaNo ratings yet
- CraniotomyDocument5 pagesCraniotomyReylan AtcNo ratings yet
- SNB Reviewer Updated July 2023Document53 pagesSNB Reviewer Updated July 2023Maria Julryn Jariol PaterezNo ratings yet
- GIT Portal HypertensionDocument24 pagesGIT Portal HypertensionDr.P.NatarajanNo ratings yet
- Jejunoileal Shunt in Surgical Treatment of Morbid ObesityDocument11 pagesJejunoileal Shunt in Surgical Treatment of Morbid ObesityTiago VieiraNo ratings yet
- (Essentials in Ophthalmology) Ahmad A. Aref, Rohit Varma (Eds.) - Advanced Glaucoma Surgery-Springer International Publishing (2015)Document140 pages(Essentials in Ophthalmology) Ahmad A. Aref, Rohit Varma (Eds.) - Advanced Glaucoma Surgery-Springer International Publishing (2015)Inna Bujor100% (1)
- Lesson 7 - Capillary Puncture Equipment and ProcedureDocument2 pagesLesson 7 - Capillary Puncture Equipment and ProcedurekhakimagdalenaNo ratings yet
- Anatomical Basis of Cranial Neurosurgery (PDFDrive)Document463 pagesAnatomical Basis of Cranial Neurosurgery (PDFDrive)Alkawthar M. AbdulsadaNo ratings yet
- Surgical Instruments-2Document55 pagesSurgical Instruments-2Philip Gene II MalacasNo ratings yet
- Leiomyoma Types, Incidence and Clinical Presentation - A Study at A Tertiary Care HospitalDocument6 pagesLeiomyoma Types, Incidence and Clinical Presentation - A Study at A Tertiary Care HospitalIJAR JOURNALNo ratings yet
- Etiology and Diagnosis of Ascites of Undetermined Origin in A Developing Country: A Prospective StudyDocument9 pagesEtiology and Diagnosis of Ascites of Undetermined Origin in A Developing Country: A Prospective StudyIJAR JOURNALNo ratings yet
- The Study of Operation Theatre Utilization Amri Hospital BhubaneswarDocument46 pagesThe Study of Operation Theatre Utilization Amri Hospital BhubaneswarRakesh Kumar AcharjyaNo ratings yet
- Heart Transplantation: Dr. K V Siva KrishnaDocument133 pagesHeart Transplantation: Dr. K V Siva KrishnaRahul K. JagaNo ratings yet
- NO Nama Barang Satuan VOL Harga JumlahDocument14 pagesNO Nama Barang Satuan VOL Harga Jumlahecko hajaNo ratings yet
- PDF Human Anatomy Color Atlas and Textbook John A Gosling Ebook Full ChapterDocument53 pagesPDF Human Anatomy Color Atlas and Textbook John A Gosling Ebook Full Chaptersalvatore.dorsey816100% (2)
- Memahami Farmakoterapi Jantung PDFDocument31 pagesMemahami Farmakoterapi Jantung PDFRahayu WijayantiNo ratings yet
- Dentoalveoar SurgeryDocument131 pagesDentoalveoar SurgeryRujan Mirela AmaliaNo ratings yet
- Doppler-Atlas Stroke ManagementDocument7 pagesDoppler-Atlas Stroke ManagementdanielNo ratings yet
- Full Chapter Laparoscopic Colon Surgery Milestones Education Best Practice Gregory Kouraklis PDFDocument46 pagesFull Chapter Laparoscopic Colon Surgery Milestones Education Best Practice Gregory Kouraklis PDFbernard.davis529100% (4)